
WHEN YOU HAVE MEDICAID
AND OTHER INSURANCE
Balance Billing, Choosing Providers
and Other Advice on Third Party Liability (TPL)
A guide to understanding health coverage in New Jersey
if you have Medicaid and Medicare and/or Other Health Insurance.
Prepared by DHS Office of Publications (revised 1/16)

TABLE OF CONTENTS
Introduction ................................................................................................1
Health Plan contact information ........................................................1
When you have Medicare and Medicaid .............................................. 2-8
Choosing Providers ..........................................................................2
Health Insurance Cards ....................................................................2
Balance Billing .............................................................................. 2-3
Coverage Responsibility ...................................................................4
Referrals ...........................................................................................5
Medicare and Medicaid Reference Chart ..................................... 6-8
When you have Other Health Insurance and Medicaid .................... 9-15
Choosing Providers ......................................................................…9
Health Insurance Cards ....................................................................9
Balance Billing .......................................................................... 10-11
Coverage Responsibility .................................................................12
Referrals .........................................................................................13
Other Health Insurance and Medicaid Reference Chart ........... 14-15
When you have Other Health Insurance, Medicare
and Medicaid ...................................................................................... 16-19
Choosing Providers ........................................................................16
Health Insurance Cards ..................................................................17
Balance Billing ................................................................................17
Coverage Responsibility .................................................................18
Referrals .........................................................................................19
WHEN YOU HAVE MEDICAID AND OTHER INSURANCE

INTRODUCTION
If you have Medicaid and other health insurance coverage, each type of coverage is
called a “payer.” When there is more than one payer, there are rules that decide how
payments are coordinated and how much each payer pays for each service. In some
cases, a member may have only one payer, Medicaid. In some cases, a member may
have a second or third payer, which may include but not be limited to Medicare, or other
health insurance.
1
Many members have other health insurance or Medicare as their primary payer, as well as
Medicaid Fee-for-Service (FFS) as their secondary or tertiary payer. This includes people
who belong to a Medicare Advantage (MA) Health Plan
2
as their primary insurance.
In New Jersey, Medicaid Health Plans are replacing Medicaid FFS as the secondary (or
tertiary) payer. When you enroll in a Medicaid Health Plan, MEDICAID IS GENERALLY
THE PAYER OF LAST RESORT. This means that Medicare and/or your other health
insurance pay for covered services first, and your Medicaid Health Plan generally pays
for covered services last.
YOU CAN NEVER BE DENIED MEDICALLY NECESSARY COVERED SERVICES
BECAUSE OF ISSUES OR CONFUSION WITH MULTIPLE PAYERS.
If you receive a bill for any services, you should contact your Medicaid Health Plan member
services department right away:
Aetna Better Health 1-855-232-3596 TTY/TDD 711
Amerigroup 1-800-600-4441 TTY/TDD 1-800-855-2880
Horizon NJ Health 1-877-765-4325 TTY/TDD 1-800-654-5505
UnitedHealthcare 1-800-941-4647 TTY/TDD 711
WellCare 1-888-453-2534 TTY/TDD 1-877-247-6272
When You Have Medicaid And Other Insurance is meant to assist Medicaid Health Plan
members and families in understanding the details with service payments. If you need
assistance understanding some of the information, please share this guide with a family
member, friend, and healthcare provider or call your Medicaid Health Plan with any
questions.
WHEN YOU HAVE MEDICAID AND OTHER INSURANCE
1
1
Examples of other health insurance: employee health insurance, automobile insurance, Veteran’s
benefits
2
Medicare Advantage is a Medicare Health Plan which includes benefits covered under Medicare Parts
A and B, and may include Medicare Part D and additional benefits.

WHEN YOU HAVE MEDICARE AND MEDICAID
CHOOSING PROVIDERS
You may continue to see your Medicare providers for Medicare covered services, even
when those providers are not in the Medicaid Health Plan provider network. TO ENSURE
THAT YOU WILL NOT BE BILLED, YOU MAY WANT TO CHOOSE MEDICARE
PROVIDERS THAT ARE ALSO IN YOUR MEDICAID HEALTH PLAN PROVIDER
NETWORK.
There are some services which are covered by your Medicaid Health Plan, but not by
Medicare. For example, dental services, vision services, hearing aids and incontinence
supplies are covered by your Medicaid Health Plan, but not by Medicare. YOU SHOULD
ONLY USE MEDICAID HEALTH PLAN PROVIDERS FOR THESE SERVICES/
SUPPLIES. MEDICAID HEALTH PLAN PROVIDERS ARE PROHIBITED FROM
BILLING YOU FOR MEDICAID COVERED SERVICES.
Please note: Medicare providers who do not participate with Medicaid have the right not to
accept you as a patient. You must find Medicare providers who are willing to treat patients
who have Medicare and Medicaid.
HEALTH INSURANCE CARDS
When you enroll in a Medicaid Health Plan, you will receive a Medicaid Health Plan
identification (ID) card. All Medicaid Health Plan ID cards will list a Medicaid Health Plan
primary care provider (PCP). YOU SHOULD CONTINUE TO SEE YOUR MEDICARE
PCP, REGARDLESS OF THE INFORMATION ON THE MEDICAID HEALTH PLAN ID
CARD. You are only required to see your Medicaid Health Plan PCP when the needed
service is not covered by Medicare, but is covered by your Medicaid Health Plan.
If you have Medicare and Medicaid, you should show all health insurance cards any time
you visit a doctor, hospital, pharmacy, lab or other service provider. This will ensure that
all providers know how to bill for that particular service, supply or prescription.
BALANCE BILLING
All providers who accept Medicare and Medicaid cannot bill individuals who have dual
coverage (both Medicare and Medicaid) for the balance of a bill. Individuals with dual
coverage are protected from being billed for the balance due on a medical claim for
medically necessary, covered services. If a provider does not know you have Medicaid,
they may send you a bill to pay the balance of the claim in error. Therefore, always
present your Medicare, Medicaid Health Plan, and plastic Medicaid Health Benefits
Identification (HBID) cards when you check in for a medical visit.
WHEN YOU HAVE MEDICAID AND OTHER INSURANCE
2

The medical office, hospital or pharmacy will need to know all of the health insurance
coverage you have to know how to submit the claim for payment.
Here are examples of how a Medicare and Medicaid provider should handle the balance
on a medical bill when you have Medicare and Medicaid:
For an office visit:
If the charge for a service is $80.00 and the Medicare payment is $64.00 (80%
of the charge), your Medicaid Health Plan will pay the 20% co-insurance or the
difference between the Medicare reimbursement and the Medicaid Health Plan
rate, whichever is less. In this example, let’s say the Medicaid Health Plan
reimbursement rate for the service is $70.00. In that case, the Medicaid Health
Plan would pay $6.00 toward the bill (The difference between the $70.00 Medicaid
Health Plan rate and the amount Medicare paid $64.00 = $6.00). You are not
responsible for any additional payment. If the Medicaid Health Plan rate is
lower than the Medicare 80% payment, no payment is made to the Medicare/
Medicaid provider. As long as you have informed the Medicare/Medicaid
provider of your Medicaid Health Plan status, the doctor will know that you
are not responsible for a co-insurance payment.
For a hospital stay:
If the charge for a hospital stay is $500.00
and the Medicare payment is $400.00 (80%
of the charge), your Medicaid Health Plan will
pay the 20% co-insurance or the difference
between the Medicare reimbursement and the
Medicaid Health Plan rate, whichever is less.
In this example, let’s say the Medicaid Health
Plan reimbursement rate for the hospital stay
is $350.00. In that case, the Medicaid Health
Plan would pay $0.00 toward the bill (The
cost of the hospital stay exceeds the Medicaid
Health Plan rate). You are not responsible
for any additional payment. As long as
you have informed the Medicare/Medicaid
provider of your Medicaid Health Plan
status, the hospital/doctor will know you
are not responsible for a co-insurance
payment.
FOR ALL SCENARIOS, MEDICAID HEALTH PLANS WILL FOLLOW THE SAME
PAYMENT RULES THAT MEDICAID FFS DID IN DETERMINING THE PAYMENT OF
THE CO-INSURANCE AMOUNT.
WHEN YOU HAVE MEDICAID AND OTHER INSURANCE
3

COVERAGE RESPONSIBILITY
Based on a regulation that has been in effect since January 2006, you can be billed for
services rendered by a provider if the following criteria exist:
3
1 – You have been paid for the service by a health insurance company or other
third party and you have failed or refused to remit to the provider that portion of the
third party’s payment to which the provider is entitled by law.
You may also be billed for services if the following criteria exist:
1 – Either:
A – The service is not covered by any of your payers; OR
B – The service is determined to be medically unnecessary before it is
rendered; OR
C – The provider does not participate with the Medicaid Health Plan, either
generally or for that service;
AND
2 – You are informed in writing before the service is rendered that either A, B or C
above exists and you voluntarily agree in writing before the service is rendered to
pay for all or part of the provider’s charges; AND
3 – The service is not an emergency service as defined in State and federal law;
AND
4 – The service is not a trauma service as defined by State law; AND
5 – The additional protections under federal and State law
4
do not apply; AND
6 – The provider has received no program payment from either Medicaid FFS or
your Medicaid Health Plan.
Example:
If you have Medicare and Medicaid and receive a cosmetic surgery from a Medicare
provider who is also in your Medicaid Health Plan provider network, this service will
not be paid for by Medicare or your Medicaid Health Plan. Cosmetic surgeries are
not covered by Medicare or your Medicaid Health Plan. However, the service must
meet the criteria listed above and you must agree in writing to pay for the service
prior to the service being rendered.
WHEN YOU HAVE MEDICAID AND OTHER INSURANCE
4
3
Adapted from N.J.A.C. 10:74-8.7
4
42 U.S.C. § 1396u-2(b)(6), 42 CFR 438.106, N.J.A.C. 11:24-9.1(d)9 and/or 15.2(b)7ii

REFERRALS
WHEN YOUR MEDICARE PCP REFERS YOU TO SEE A MEDICARE SPECIALIST FOR
A MEDICARE–ONLY COVERED SERVICE OR FOR A MEDICARE AND MEDICAID
HEALTH PLAN COVERED SERVICE, YOU DO NOT NEED TO OBTAIN A REFERRAL
FROM YOUR MEDICAID HEALTH PLAN PCP. The same billing standards apply and
you cannot be billed for a Medicare only or for a Medicare and Medicaid Health Plan
covered service, when that service is received from a Medicare provider.
However, if you need health services that are not covered by Medicare, you may need a
referral from your Medicaid Health Plan PCP. These are examples of services that are not
covered by Medicare, but are covered by your Medicaid Health Plan: hearing aids, vision
exams, incontinence supplies, and personal care assistance services.
Each Medicaid Health Plan has established different guidelines regarding referrals to see
specialists within the Medicaid Health Plan network. Please contact your Medicaid Health
Plan for more information:
Aetna Better Health 1-855-232-3596 TTY/TDD 711
Amerigroup 1-800-600-4441 TTY/TDD 1-800-855-2880
Horizon NJ Health 1-877-765-4325 TTY/TDD 1-800-654-5505
UnitedHealthcare 1-800-941-4647 TTY/TDD 711
WellCare 1-888-453-2534 TTY/TDD 1-877-247-6272
REMEMBER:
YOU CAN NEVER BE DENIED MEDICALLY NECESSARY COVERED SERVICES
BECAUSE OF ISSUES OR CONFUSION WITH MULTIPLE PAYERS.
If you receive a bill for any services, you should contact your Medicaid Health Plan member
services department right away:
Aetna Better Health 1-855-232-3596 TTY/TDD 711
Amerigroup 1-800-600-4441 TTY/TDD 1-800-855-2880
Horizon NJ Health 1-877-765-4325 TTY/TDD 1-800-654-5505
UnitedHealthcare 1-800-941-4647 TTY/TDD 711
WellCare 1-888-453-2534 TTY/TDD 1-877-247-6272
WHEN YOU HAVE MEDICAID AND OTHER INSURANCE
5
WHEN YOU HAVE MEDICAID AND OTHER INSURANCE
6
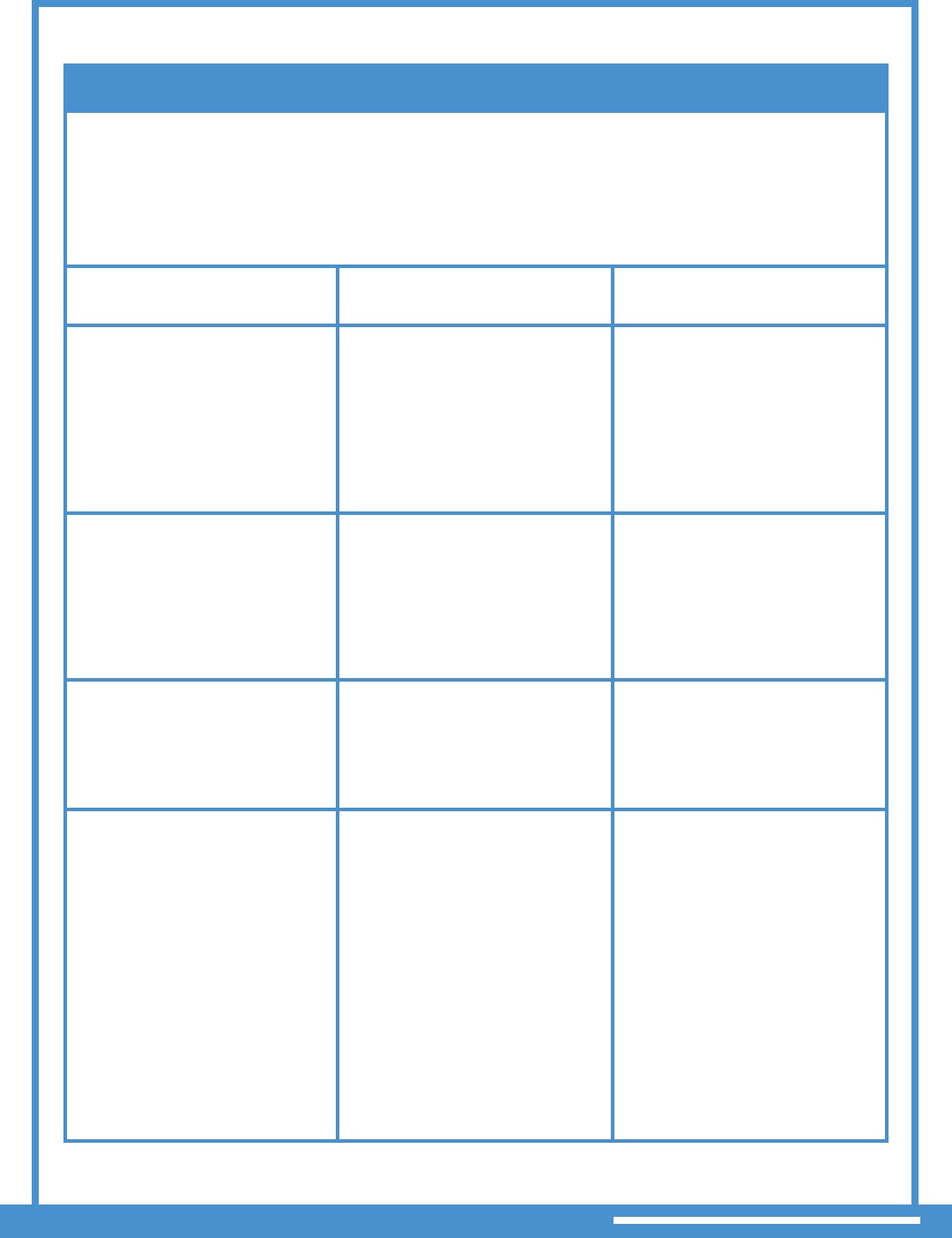
IF SERVICE IS
An approved, Medicare
covered benefit
(Examples: outpatient
hospital service, primary
care, specialists,
lab tests, radiology)
Inpatient hospital care
Emergency care received
at a hospital emergency
department
A medically necessary
service which is not
covered by Medicare
but is covered by your
Medicaid Health Plan
(Examples: dental
services, hearing aids,
personal care assistant
services, medical day care
services, incontinence
supplies, family planning
services)
THEN
Medicare is the primary
payer and Medicaid
Health Plan is the
secondary payer.
Medicare is the primary
payer and Medicaid
Health Plan is the
secondary payer.
Medicare is the primary
payer and Medicaid
Health Plan is the
secondary payer.
Medicaid Health Plan is
the only payer.
PROVIDER GUIDANCE
Use a Medicare provider
who does not need to be
in your Medicaid Health
Plan’s provider network.
Use a hospital that is
affiliated with Medicare. If
possible, use a hospital
that is also in your
Medicaid Health Plan
provider network.
Go to the nearest hospital.
Use a provider in your
Medicaid Health Plan
provider network.
WHEN YOU HAVE BOTH MEDICARE AND MEDICAID
If you have both Medicare and Medicaid, you should always choose providers in
your Medicare provider network for Medicare covered, medically necessary services.
When receiving Medicare covered services, all Medicare guidelines must be followed
to ensure Medicare coverage. See http://www.medicare.gov for more information.
WHEN YOU HAVE MEDICAID AND OTHER INSURANCE
7
5
A provider who has opted out of Medicare is one that does not accept Medicare beneficiaries for any
services.
6
Generally, when a service is rendered by a provider who has opted out of Medicare, and is not in your
Medicaid Health Plan network, the service will not be covered by Medicare or your Medicaid Health Plan.
7
Medicare Advantage is a Medicare Health Plan which includes benefits covered under Medicare Parts A
and B, and may include Medicare Part D and additional benefits.
8
Creditable drug coverage is coverage from an employer or union plan in place of Medicare Part D.
9
Exceptions: benzodiazepines, barbiturates, smoking cessation drugs, and certain vitamins are not
covered by Medicare Part D but are covered by your Medicaid Health Plan. Co-pays do not apply.
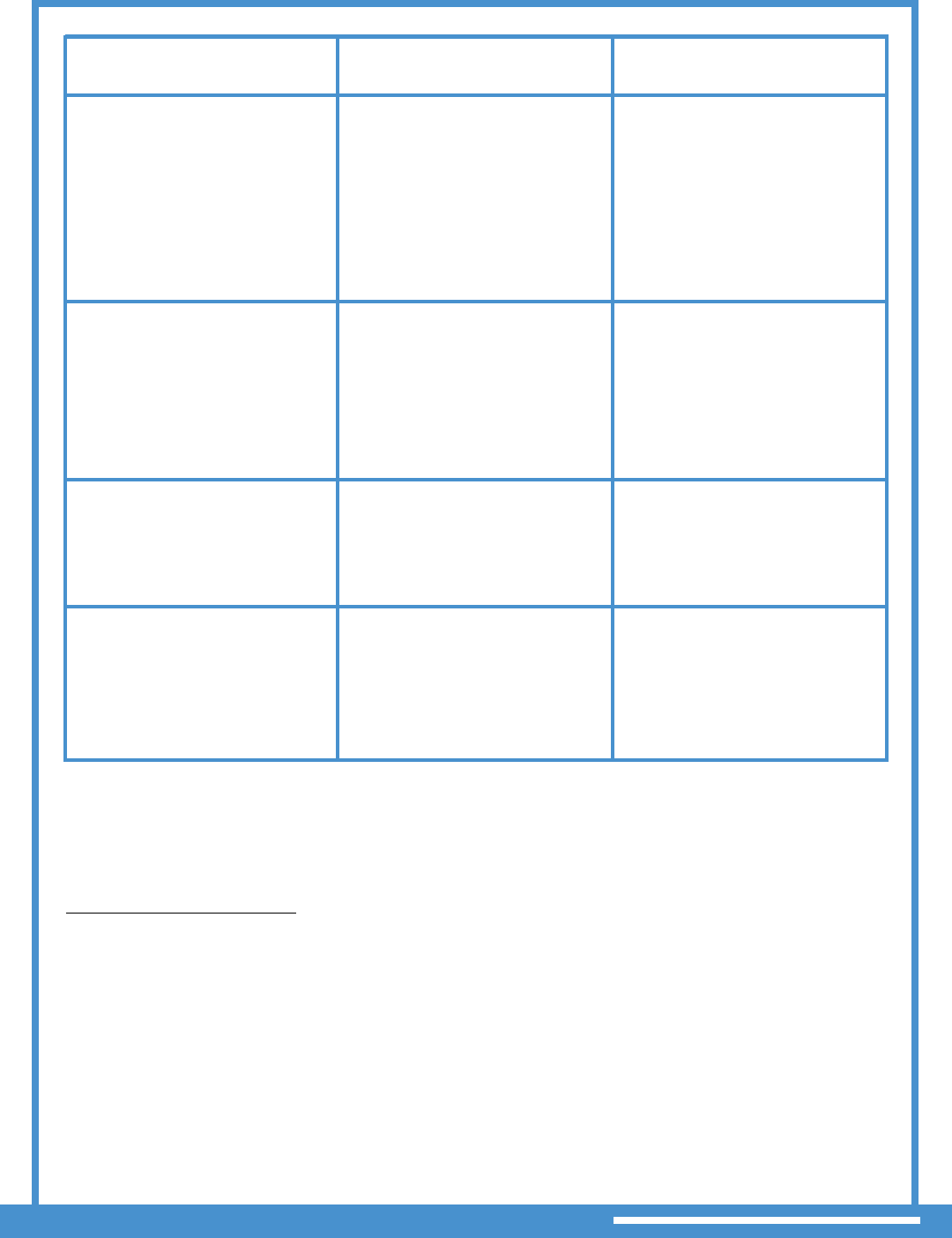
IF SERVICE IS
Rendered by a provider
who has opted out of
Medicare for Medicare
Parts A and B members
5
and is not in your
Medicaid Health Plan
provider network
Rendered to a Medicare
Advantage Health
Plan
7
member by an
unapproved, uncovered
out-of-network provider
A prescription drug
covered under Medicare
Part D
A prescription drug not
covered under Medicare
Part D or creditable drug
coverage
8
THEN
Member is responsible
for payment if properly
informed and signed
private contract.
6
Member is responsible for
payment.
Medicare is the primary
payer. Member must pay
a small prescription co-
pay, if applicable.
Member is responsible
for payment.
9
Some
exceptions apply. See
footnote at the bottom of
this page.
PROVIDER GUIDANCE
To avoid being
responsible for medical
bills, be sure to use
providers who participate
in Medicare.
To avoid being responsible
for medical bills, be sure to
use providers who are in
the Medicare Advantage
Health Plan’s provider
network.
Use a Medicare
participating pharmacy to
receive prescription drugs.
N/A

WHEN YOU HAVE MEDICAID AND OTHER INSURANCE
8
IF SERVICE IS
For nursing facility care,
including short-term in-
patient rehabilitation
settings
THEN
Medicare and Medicaid
cover some days in a
nursing facility. For more
information, contact
SHIP at 1-800-792-8820
(TTY 711), Medicare at
1-800-MEDICARE (1-
800-633-4227) (TTY
1-877-486-2048) or
your Medicaid Health
Plan member services
department.
PROVIDER GUIDANCE
Contact the State Health
Insurance Assistance
Program (SHIP) at
1-800-792-8820 (TTY
711), Medicare at
1-800-MEDICARE (1-
800-633-4227) (TTY
1-877-486-2048) or
your Medicaid Health
Plan member services
department for guidance.

WHEN YOU HAVE OTHER HEALTH INSURANCE AND MEDICAID
CHOOSING PROVIDERS
You should always choose providers in your other health insurance provider network for
services covered by your other health insurance. You may continue to see your other
health insurance provider, even when those providers are not in your Medicaid Health
Plan provider network. When possible, if you are choosing new providers, you may want
to choose providers that are in your other health insurance provider network and also
in your Medicaid Health Plan provider network. GENERALLY, WHEN YOU CHOOSE
PROVIDERS IN BOTH NETWORKS FOR MEDICAID HEALTH PLAN COVERED
SERVICES, YOU CANNOT BE BILLED.
Under limited circumstances, you may be responsible for a portion of the payment. See
pages 10-11 for details and billing examples.
There are some services which are covered by your Medicaid Health Plan, but may not be
covered by your other health insurance. For example, private duty nursing, personal care
assistance and incontinence supplies are covered by your Medicaid Health Plan, but may
not be covered by your other health insurance. WHEN YOU USE MEDICAID HEALTH
PLAN PROVIDERS FOR THESE SERVICES/SUPPLIES, YOU CANNOT BE BILLED
FOR THE BALANCE.
HEALTH INSURANCE CARDS
When you enroll in a Medicaid Health Plan, you will receive a Medicaid Health Plan
identification (ID) card. All Medicaid Health Plan ID cards will list a Medicaid Health
Plan primary care provider (PCP). YOU SHOULD CONTINUE TO SEE YOUR OTHER
HEALTH INSURANCE PCP, REGARDLESS OF THE INFORMATION ON THE
MEDICAID HEALTH PLAN ID CARD, EVEN WHEN THE OTHER HEALTH INSURANCE
PCP DOES NOT PARTICIPATE WITH THE MEDICAID HEALTH PLAN. You are only
required to see your Medicaid Health Plan PCP when the needed service is not covered
by your other health insurance, but is covered by your Medicaid Health Plan.
If you have other health insurance and Medicaid, we recommend you show all health
insurance cards anytime you visit a doctor, hospital, pharmacy, lab or other service
provider. However, if you have other health insurance and Medicaid, AND YOU CHOOSE
NOT TO SHOW A PROVIDER YOUR MEDICAID HEALTH PLAN ID CARD, YOU MAY
BE HELD RESPONSIBLE FOR ANY APPLICABLE CO-INSURANCE PAYMENTS FOR
THE SERVICE RENDERED. By showing both cards, you should not be responsible for
any payments; however under limited circumstances, you may be responsible for a portion
of the payment. See pages 10-11 for details and billing examples.
WHEN YOU HAVE MEDICAID AND OTHER INSURANCE
9

BALANCE BILLING
Providers who are in your other health insurance provider network and your Medicaid
Health Plan provider network are prohibited from billing individuals for the balance of a bill
for Medicaid Health Plan covered services. In order to prevent being billed for Medicaid
Health Plan covered services, providers in your other health insurance network who are
not in your Medicaid Health Plan network must be informed of your Medicaid status.
Individuals on Medicaid are protected from being billed for the balance due on a medical
claim for medically necessary, covered services. If a provider does not know you have
Medicaid, they may send you a bill to pay the balance of the claim in error. Therefore,
always present your Other Health Insurance, Medicaid Health Plan, and plastic
Medicaid HBID cards when you check in for a medical visit. The medical office, hospital
or pharmacy will need to know all of the health insurance coverage you have to know how
to submit the claim for payment.
After an other health insurance provider bills your other health insurance and receives
payment, they will submit a claim for the unpaid balance to your Medicaid Health Plan. In
the past, if the provider was not also a Medicaid provider, they may have been unable to bill
Medicaid because they were not set up in the Medicaid FFS claims system. The Medicaid
Health Plan can process claims of providers who are not in their provider network.
At the same time, Medicaid Health Plans cannot exceed the maximum reimbursement that
the Medicaid Health Plan would have covered if it had been the primary payer.
Children under agreement with the
Department of Children and Families/
Division of Youth and Family Services
(DCF/DYFS) who have other health
insurance and Medicaid do not pay
any co-insurance.
Here are examples of how a provider
should handle the balance on a
medical bill when you have other
health insurance and Medicaid:
WHEN YOU HAVE MEDICAID AND OTHER INSURANCE
10

For an office visit:
If the charge for a service is $80.00 and the other health insurance payment
is $64.00 (80% of the charge), your Medicaid Health Plan will pay the 20% co-
insurance or the difference between the other health insurance reimbursement
and the Medicaid Health Plan rate, whichever is less. In this example, let’s say
the Medicaid Health Plan rate for the service is $70.00. In that case, the Medicaid
Health Plan would pay $6.00 toward the bill (The difference between the $70.00
Medicaid Health Plan rate and the amount your other health insurance paid $64.00
= $6.00). Generally, if the provider is in your other health insurance network
AND your Medicaid Health Plan network, you are not responsible for any
additional payment. If the provider is in your other health insurance network,
but NOT your Medicaid Health Plan network, you may be responsible for
a portion of payment. If the Medicaid Health Plan rate is lower than the other
health insurance 80% payment, no payment is made to the other health insurance
provider. If the provider is in your other health insurance network AND your
Medicaid Health Plan network, you are not responsible for any additional
payment. If the provider is in your other health insurance network, but NOT
your Medicaid Health Plan network, you may be responsible for a portion of
payment.
For a hospital stay:
If the charge for a hospital stay is $500.00 and the other health insurance payment
is $400.00 (80% of the charge), your Medicaid Health Plan will pay the 20% co-
insurance or the difference between the other health insurance reimbursement
and the Medicaid Health Plan rate, whichever is less. In this example, let’s say
the Medicaid Health Plan rate for the hospital stay is $350.00. In that case, the
Medicaid Health Plan would pay $0.00 toward the bill (The cost of the hospital stay
exceeds the Medicaid Health Plan rate). Generally, if the provider is in your
other health insurance network AND your Medicaid Health Plan network, you
are not responsible for any additional payment. If the provider is in your
other health insurance network, but NOT your Medicaid Health Plan network,
you may be responsible for a portion of payment.
FOR ALL SCENARIOS, MEDICAID HEALTH PLANS WILL FOLLOW THE SAME
PAYMENT RULES THAT MEDICAID FFS DID IN DETERMINING THE PAYMENT OF
THE CO-INSURANCE AMOUNT.
WHEN YOU HAVE MEDICAID AND OTHER INSURANCE
11

COVERAGE RESPONSIBILITY
Based on a regulation that has been in effect since January 2006, you can be billed for
services rendered by a provider if the following criteria exist:
10
1 – You have been paid for the service by a health insurance company or other
third party and you have failed or refused to remit to the provider that portion of the
third party’s payment to which the provider is entitled by law.
You may also be billed for services if the following criteria exist:
1 – Either:
A – The service is not covered by any of your payers; OR
B – The service is determined to be medically unnecessary before it is
rendered; OR
C – The provider does not participate with the Medicaid Health Plan, either
generally or for that service;
AND
2 – You are informed in writing before the service is rendered that either A, B or C
above exists and you voluntarily agree in writing before the service is rendered to
pay for all or part of the provider’s charges; AND
3 – The service is not an emergency service as defined in State and federal law;
AND
4 – The service is not a trauma service as defined by State law; AND
5 – The additional protections under federal and State law
11
do not apply; AND
6 – The provider has received no program payment from either Medicaid FFS or
your Medicaid Health Plan.
Example:
If you have other health insurance and Medicaid and receive medically necessary
knee replacement surgery by a provider in your other health insurance provider
network, and the service is covered by your other health insurance, your other
health insurance will be the primary payer for the surgery and the inpatient hospital
stay. Your Medicaid Health Plan will pay the difference for any Medicaid covered
services received during the surgery and inpatient hospital stay, provided that the
total reimbursement does not exceed the pre-determined Medicaid Health Plan
rate for that/those service(s).
WHEN YOU HAVE MEDICAID AND OTHER INSURANCE
12
10
Adapted from N.J.A.C. 10:74-8.7
11
42 U.S.C. § 1396u-2(b)(6), 42 CFR 438.106, N.J.A.C. 11:24-9.1(d)9 and/or 15.2(b)7ii

REFERRALS
WHEN YOUR OTHER HEALTH INSURANCE PCP REFERS YOU TO SEE AN OTHER
HEALTH INSURANCE SPECIALIST FOR AN OTHER HEALTH INSURANCE-ONLY
SERVICE OR FOR AN OTHER HEALTH INSURANCE AND MEDICAID HEALTH PLAN
COVERED SERVICE, YOU DO NOT NEED A REFERRAL FROM YOUR MEDICAID
HEALTH PLAN PCP. The same billing standards apply and you can only be billed for
services when the service meets the criteria discussed in the sections on Balance Billing
(pages 10-11) and Coverage Responsibility (page 12).
However, if you need health services that are not covered by your other health insurance,
you may need a referral from your Medicaid Health Plan PCP. These are examples of
services that may not be covered by your other health insurance, but are covered by your
Medicaid Health Plan: incontinence supplies, private duty nursing, medical day care and
personal care assistance services.
Each Medicaid Health Plan has established different guidelines regarding referrals to see
specialists within the Medicaid Health Plan network. Please contact your Medicaid Health
Plan for more information:
Aetna Better Health 1-855-232-3596 TTY/TDD 711
Amerigroup 1-800-600-4441 TTY/TDD 1-800-855-2880
Horizon NJ Health 1-877-765-4325 TTY/TDD 1-800-654-5505
UnitedHealthcare 1-800-941-4647 TTY/TDD 711
WellCare 1-888-453-2534 TTY/TDD 1-877-247-6272
REMEMBER:
YOU CAN NEVER BE DENIED MEDICALLY NECESSARY COVERED SERVICES
BECAUSE OF ISSUES OR CONFUSION WITH MULTIPLE PAYERS.
If you receive a bill for any services, you should contact your Medicaid Health Plan member
services department right away:
Aetna Better Health 1-855-232-3596 TTY/TDD 711
Amerigroup 1-800-600-4441 TTY/TDD 1-800-855-2880
Horizon NJ Health 1-877-765-4325 TTY/TDD 1-800-654-5505
UnitedHealthcare 1-800-941-4647 TTY/TDD 711
WellCare 1-888-453-2534 TTY/TDD 1-877-247-6272
WHEN YOU HAVE MEDICAID AND OTHER INSURANCE
13

WHEN YOU HAVE MEDICAID AND OTHER INSURANCE
14
IF SERVICE IS
An approved, other
health insurance covered
benefit, including referrals
from your other health
insurance PCP
A medically necessary
service which may not
be covered by other
health insurance but is
covered by your Medicaid
Health Plan (Examples:
incontinence supplies,
personal care assistant
services, medical day care
services, family planning
services)
THEN
Other health insurance
is the primary payer and
Medicaid Health Plan is
the secondary payer. A
Medicaid Health Plan
referral is not required.
Medicaid Health Plan is
the primary payer.
PROVIDER GUIDANCE
Use a provider in your
other health insurance
provider network. Your
Medicaid Health Plan ID
card will have a Medicaid
Health Plan PCP on it.
You should still use your
other health insurance
PCP for all other health
insurance covered
services regardless of the
Medicaid Health Plan PCP
listed on your Medicaid
Health Plan ID card.
Use a provider in your
Medicaid Health Plan
provider network.
WHEN YOU HAVE BOTH OTHER HEALTH INSURANCE AND MEDICAID
If you have both Other Health Insurance and Medicaid, you should always choose
providers in your other health insurance provider network for other health insurance
covered, medically necessary services. If possible, finding providers in both your other
health insurance provider network and your Medicaid Health Plan provider network
should eliminate any chance of being billed for other health insurance and Medicaid
covered services. There are many different types of other health insurance and each
type of other health insurance will have different guidelines and types of coverage.
Refer to your other health insurance member materials for more information. Generally,
when your other health insurance covers a Medicaid Health Plan covered service, your
Medicaid Health Plan will also cover the service, provided the service does not exceed
the Medicaid Health Plan reimbursement rate for that service. See Balance Billing on
pages 10-11 for more information.
WHEN YOU HAVE MEDICAID AND OTHER INSURANCE
15
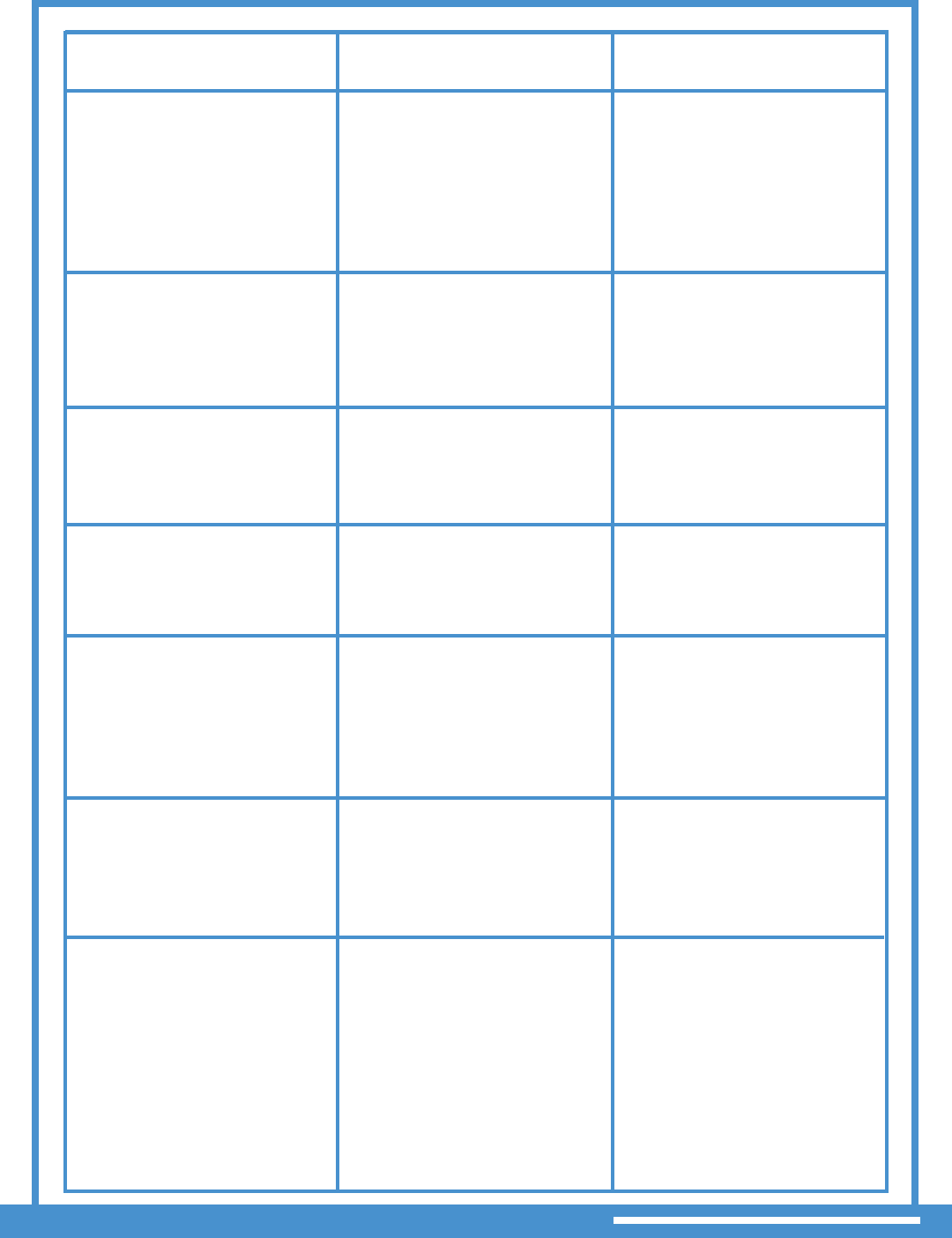
IF SERVICE IS
Rendered by a provider that
is not in your other health
insurance provider network
and is not in your Medicaid
Health Plan provider network
and was not authorized by
your other health insurance
A prescription drug covered
by your other health
insurance
A prescription drug not
covered by your other health
insurance, but covered by
your Medicaid Health Plan
A prescription drug not
covered by your other health
insurance or your Medicaid
Health Plan.
An inpatient stay in an
other health insurance
provider hospital
Emergency care received
at a hospital emergency
department
For nursing facility care
THEN
Member is responsible
for payment.
Other health insurance is
primary payer. Medicaid
Health Plan is secondary
payer and covers the drug
co-pay.
Medicaid Health Plan
is only payer.
Member is responsible
for payment.
Other health insurance is
the primary payer. Medicaid
Health Plan is the
secondary payer.
Other health insurance is the
primary payer and Medicaid
Health Plan is the
secondary payer.
Other health insurance
and your Medicaid Health
Plan may both cover
nursing facility care. For
more information about
payments, contact your
other health insurance
service representative
or your Medicaid Health
Plan member services
department.
PROVIDER GUIDANCE
To avoid being responsible
for medical bills, be sure to
use providers who are in
your other health insurance’s
provider network.
Use an other health
insurance participating
pharmacy to receive
prescription drugs.
Use a pharmacy in your
Medicaid Health Plan
provider network.
N/A
Use a hospital that is in
your other health insurance
provider network. If
possible, use a hospital
that is also in your Medicaid
Health Plan provider network
Go to the nearest hospital.
Use a facility that is in your
other health insurance
and Medicaid Health Plan
provider networks.

WHEN YOU HAVE OTHER HEALTH INSURANCE,
MEDICARE AND MEDICAID
CHOOSING PROVIDERS
When you have other health insurance, Medicare and Medicaid, either your other
health insurance or Medicare is the primary payer for most covered services. To
determine which health coverage is your primary payer, please use the following resources:
1) Call Medicare’s State Health Insurance Assistance Program (SHIP) at
1-800-792-8820 (TTY 711)
2) Call Medicare at 1-800-MEDICARE (1-800-633-4227) (TTY 1-877-486-2048)
3) The Medicare Guide to Who Pays First:
http://www.medicare.gov/Publications/Pubs/pdf/02179.pdf
You should always choose providers from your primary provider network for services
covered by your primary health coverage. When possible, it is recommended that you
choose providers that are in your other health insurance provider network that are also
Medicare providers. WHEN YOU CHOOSE PROVIDERS IN BOTH NETWORKS FOR
MEDICAID HEALTH PLAN COVERED SERVICES, YOU CANNOT BE BILLED.
There are some services which are covered by your Medicaid Health Plan, but may not
be covered by your other health insurance or Medicare. For example, dental services,
personal care assistance services, medical day care and incontinence supplies are
covered by your Medicaid Health Plan, but may not be covered by your other health
insurance or Medicare. WHEN YOU USE MEDICAID HEALTH PLAN PROVIDERS FOR
THESE SERVICES/SUPPLIES, YOU CANNOT BE BILLED FOR THE BALANCE.
WHEN YOU HAVE MEDICAID AND OTHER INSURANCE
16

HEALTH INSURANCE CARDS
When you enroll in a Medicaid Health Plan, you will receive a Medicaid Health Plan
identification (ID) card. All Medicaid Health Plan ID cards will include a Medicaid Health
Plan primary care provider (PCP). YOU SHOULD CONTINUE TO SEE YOUR OTHER
HEALTH INSURANCE OR MEDICARE PCP, REGARDLESS OF THE INFORMATION
ON THE MEDICAID HEALTH PLAN ID CARD. You are only required to see your
Medicaid Health Plan PCP when the needed service is not covered by your other health
insurance but is covered by your Medicaid Health Plan.
If you have other health insurance, Medicare and Medicaid, we recommend you show all
health insurance cards anytime you visit a doctor, hospital, pharmacy, lab or other service
provider. However, if you have other health insurance, Medicare and Medicaid, you can
choose if you prefer NOT TO SHOW A PROVIDER YOUR MEDICAID HEALTH PLAN ID
CARD, IN WHICH CASE YOU MAY BE HELD RESPONSIBLE FOR ANY APPLICABLE
CO-INSURANCE PAYMENTS FOR THE SERVICE RENDERED. By showing all cards,
you should not be responsible for any payments; however under limited circumstances,
you may be responsible for a portion of the payment. See below for details.
BALANCE BILLING
If you have other health insurance, Medicare and Medicaid, the rules that apply to members
with Medicare and Medicaid apply to you as well. Members with both Medicare and
Medicaid cannot be billed for services rendered by providers that accept Medicare.
It is recommended that you receive services from providers in your other health insurance
network that accept Medicare. For any service which is covered by your other health
insurance, your other health insurance is the primary payer, Medicare is the second payer,
and your Medicaid Health Plan is the last payer. Contact the Medicare Coordination of
Benefits Call Center at 1-800-999-1118 (TTY 1-800-318-8782) to determine if, in your
situation, Medicare or the other health insurance is the primary payer.
FOR ALL SCENARIOS, MEDICAID HEALTH PLANS WILL FOLLOW THE SAME
PAYMENT RULES THAT MEDICAID FFS DID IN DETERMINING THE PAYMENT OF
THE CO-INSURANCE AMOUNT.
WHEN YOU HAVE MEDICAID AND OTHER INSURANCE
17

COVERAGE RESPONSIBILITY
Based on a regulation that has been in effect since January 2006, you can be billed for
services rendered by a provider if the following criteria exist:
12
1 – You have been paid for the service by a health insurance company or other
third party and you have failed or refused to remit to the provider that portion of the
third party’s payment to which the provider is entitled by law.
You may also be billed for services if the following criteria exist:
1 – Either:
A – The service is not covered by any of your payers; OR
B – The service is determined to be medically unnecessary before it is
rendered; OR
C – The provider does not participate with the Medicaid Health Plan, either
generally or for that service;
AND
2 – You are informed in writing before the service is rendered that either A, B or C
above exists and you voluntarily agree in writing before the service is rendered to
pay for all or part of the provider’s charges; AND
3 – The service is not an emergency service as defined in State and federal law;
AND
4 – The service is not a trauma service as defined by State law; AND
5 – The additional protections under federal and State law
13
do not apply; AND
6 – The provider has received no program payment from either Medicaid FFS or
your Medicaid Health Plan.
WHEN YOU HAVE MEDICAID AND OTHER INSURANCE
18
12
Adapted from N.J.A.C. 10:74-8.7
13
42 U.S.C. § 1396u-2(b)(6), 42 CFR 438.106, N.J.A.C. 11:24-9.1(d)9 and/or 15.2(b)7ii

REFERRALS
WHEN YOUR OTHER HEALTH INSURANCE OR MEDICARE PCP REFERS YOU
TO SEE AN OTHER HEALTH INSURANCE OR MEDICARE SPECIALIST FOR AN
OTHER HEALTH INSURANCE OR MEDICARE ONLY OR FOR AN OTHER HEALTH
INSURANCE /MEDICARE AND MEDICAID HEALTH PLAN COVERED SERVICE,
YOU DO NOT NEED TO OBTAIN A REFERRAL FROM YOUR MEDICAID HEALTH
PLAN PCP. The same billing standards apply and you generally cannot be billed for an
other health insurance/Medicare and Medicaid Health Plan covered service, when that
service is received from an other health insurance/Medicare provider. Additionally, you
can only be billed for services received from a non other health insurance /Medicare and
non Medicaid Health Plan provider when the service meets the criteria discussed in the
sections on Balance Billing (page 17) and Coverage Responsibility (page 18).
However, if you need health services that are not covered by your other health insurance
or by Medicare, you many need a referral from your Medicaid Health Plan PCP. These
are examples of services that may not be covered by your other health insurance or
Medicare, but are covered by your Medicaid Health Plan: incontinence supplies, private
duty nursing, medical day care and personal care assistance services.
Each Medicaid Health Plan has established different guidelines regarding referrals to see
specialists in the Medicaid Health Plan network. Please contact your Medicaid Health
Plan for more information:
Aetna Better Health 1-855-232-3596 TTY/TDD 711
Amerigroup 1-800-600-4441 TTY/TDD 1-800-855-2880
Horizon NJ Health 1-877-765-4325 TTY/TDD 1-800-654-5505
UnitedHealthcare 1-800-941-4647 TTY/TDD 711
WellCare 1-888-453-2534 TTY/TDD 1-877-247-6272
REMEMBER:
YOU CAN NEVER BE DENIED MEDICALLY NECESSARY COVERED SERVICES
BECAUSE OF ISSUES OR CONFUSION WITH MULTIPLE PAYERS.
If you receive a bill for any services, you should contact your Medicaid Health Plan member
services department right away:
Aetna Better Health 1-855-232-3596 TTY/TDD 711
Amerigroup 1-800-600-4441 TTY/TDD 1-800-855-2880
Horizon NJ Health 1-877-765-4325 TTY/TDD 1-800-654-5505
UnitedHealthcare 1-800-941-4647 TTY/TDD 711
WellCare 1-888-453-2534 TTY/TDD 1-877-247-6272
WHEN YOU HAVE MEDICAID AND OTHER INSURANCE
19

Note: When You Have Medicaid And Other Insurance is not a legal document.
The official Medicaid program provisions are contained in the relevant laws and
regulations. The information in this document is correct as of October 1, 2011.
WHEN YOU HAVE MEDICAID AND OTHER INSURANCE
20
