
Substance Use Disorder Treatment for
People With Co-Occurring Disorders
UPDATED 2020
TREATMENT IMPROVEMENT PROTOCOL
TIP 42
This page intentionally left blank.
This page intentionally left blank.

TIP 42
Contents
Foreword ..................................................................vii
Executive Summary .......................................................... ix
Overall Key Messages ....................................................... ix
Content Overview...........................................................x
Consensus Panel .......................................................... xvii
TIP Development Participants ................................................. xvii
KAP Expert Panel and Federal Government Participants ........................ xviii
Publication Information..................................................... xxvii
Chapter 1—Introduction to Substance Use Disorder Treatment for
People With Co-Occurring Disorders
.........................................1
Scope of This TIP............................................................2
Terminology in This TIP ......................................................3
Important Developments That Led to This TIP Update ............................6
Why Do We Need a TIP on CODs? .............................................7
The Complex, Unstable, and Bidirectional Nature of CODs ........................11
Conclusion................................................................12
Chapter 2— Guiding Principles for Working With People Who Have
Co-Occurring Disorders
.....................................................13
General Guiding Principles ...................................................14
Guidelines for Counselors and Other Providers ..................................16
Guidelines for Administrators and Supervisors ..................................21
Conclusion................................................................29
Chapter 3—Screening and Assessment of Co-Occurring Disorders .............31
Screening and Basic Assessment for CODs ......................................32
The Complete Screening and Assessment Process ................................36
Considerations in Treatment Matching.........................................65
Conclusion................................................................68
Chapter 4—Mental and Substance-Related Disorders: Diagnostic
and Cross-Cutting Topics
........................................................69
Depressive Disorders .......................................................71
Bipolar I Disorder ..........................................................76
Posttraumatic Stress Disorder ................................................83
Personality Disorders .......................................................89
Anxiety Disorders . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . .98
Schizophrenia and Other Psychotic Disorders ..................................104
Attention Decit Hyperactivity Disorder.......................................110
iii

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
Feeding and Eating Disorders ...............................................114
Substance-Related Disorders ................................................121
Cross-Cutting Topics: Suicide and Trauma......................................129
Conclusion...............................................................140
Chapter 5—Strategies for Working With People Who Have
Co-Occurring Disorders
....................................................141
Competencies for Working With Clients Who Have CODs
Guidance for Working With Clients Who Have Specic
........................142
Guidelines for a Successful Therapeutic Relationship ............................142
Protect Condentiality .....................................................148
Co-Occurring Mental Disorders ............................................160
Conclusion...............................................................163
Chapter 6—Co-Occurring Disorders Among Special Populations ..............165
People Experiencing Homelessness ...........................................166
People Involved in the Criminal Justice System .................................170
Women .................................................................172
People of Diverse Racial/Ethnic Backgrounds...................................179
Conclusion...............................................................182
Chapter 7—Treatment Models and Settings for People With
Co-Occurring Disorders
...................................................183
Treatment Overview.......................................................184
Treatment Models ........................................................188
Empirical Evidence for ACT .................................................192
Treatment Settings ....................................................... 203
Pharmacotherapy ........................................................ 220
Chapter 8—Workforce and Administrative Concerns in Working
With People Who Have Co-Occurring Disorders
............................ 229
Recruitment, Hiring, and Retention ......................................... 230
Avoiding Burnout ........................................................ 233
Competency and Professional Development .................................. 234
Conclusion...............................................................243
Appendix A—Bibliography....................................................245
Appendix B—Resources ..................................................... 285
Training for Providers and Administrators .................................... 285
Other Resources for Counselors, Providers, and Programs ........................287
Client and Family Resources................................................ 293
iv

TIP 42
Appendix C—Provider Forms, Measures, and Tools ................................297
Biopsychosocial Intake Forms ...............................................297
Suicide and Safety Screening and Assessment Tools .............................297
Mental Disorder Screening and Assessment Tools ...............................297
Substance Use/Misuse Screening and Assessment Tools..........................297
Trauma Screening and Assessment Tools ..................................... 299
Levels of Care Tool ....................................................... 299
Functioning and Disability Tools .............................................310
Stage of Change Tools .....................................................310
Additional Screening Tools for Common Mental Disorders........................313
Exhibits
Exhibit 1.1. Key Terms..........................................................3
EXHIBIT 1.2. Co-Occurring Substance Misuse in Adults Ages 18 and Older
With and Without any Mental Illness and SMI (in 2018)............................7
Exhibit 2.1. Six Guiding Principles in Treating Clients With CODs ......................16
Exhibit 2.2. Making “No Wrong Door” a Reality ...................................19
Exhibit 2.3. The Four Quadrants Model ..........................................20
Exhibit 2.4. SAMHSA Practice Principles of Integrated Treatment for CODs .............21
Exhibit 2.5. Levels of Program Capacity in CODs ...................................31
Exhibit 3.1. Assessment Considerations for Clients With CODs ........................39
Exhibit 3.2. Biopsychosocial Sources of Information in the Assessment of CODs .........40
Exhibit 3.3. Recommended Screening Tools To Help Detect CODs ................... 44
Exhibit 3.4. The Suicide Behaviors Questionnaire-Revised (SBQ-R) - Overview ...........46
Exhibit 3.5. SBQ-R-Scoring .....................................................46
Exhibit 3.6. SBQ-R Suicide Behaviors Questionnaire - Revised.........................47
Exhibit 3.7. Mental HSF-III .....................................................52
Exhibit 3.8. Level of Care Quadrants ............................................57
Exhibit 3.9. Sample Treatment Plan for Case Example George T.......................68
Exhibit 3.10. Considerations in Treatment Matching ................................68
Exhibit 4.1. Diagnostic Criteria for MDD .........................................74
Exhibit 4.2. Diagnostic Criteria for PDD ..........................................76
Exhibit 4.3. Diagnostic Criteria for Bipolar I Disorder ...............................80
Exhibit 4.4. Diagnostic Criteria for PTSD .........................................86
Exhibit 4.5 Diagnostic Criteria for General PD .....................................92
Exhibit 4.6 Diagnostic Criteria for BPD ...........................................95
v

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
Exhibit 4.7. Diagnostic Criteria for ASPD .........................................99
Exhibit 4.8. Diagnostic Criteria for GAD .........................................101
Exhibit 4.9. Diagnostic Criteria for Panic disorder .................................102
Exhibit 4.10. Diagnostic Criteria for SAD.........................................103
Exhibit 4.11. Diagnostic Criteria for Schizophrenia.................................108
Exhibit 4.12. Diagnostic Criteria for ADHD .......................................113
Exhibit 4.13. Diagnostic Criteria for AN .........................................117
Exhibit 4.14. Diagnostic Criteria for BN..........................................118
Exhibit 4.15. Diagnostic Criteria for BED.........................................119
Exhibit 4.16. Substances and Corresponding Substance-Induced Mental Disorders .....124
Exhibit 4.17. Substance-Induced Mental Disorder Symptoms (by Substance) ...........125
Exhibit 4.18. Features of DSM-5 Substance-Induced Mental Disorders ................127
Exhibit 4.19. Substances That Precipitate or Mimic Common Mental Disorders ........128
Exhibit 4.20. Veterans and CODs ..............................................141
Exhibit 6.1. Adapting Treatment Services to Women’s Needs .......................177
Exhibit 7.1. The Four Quadrants of Care.........................................187
Exhibit 7.2. TC Activities and Components.......................................207
Exhibit 7.3. TC Modications for People With CODs ............................. 208
Exhibit 7.4. Traditional Mental Health Settings Versus Integrated Mental
Health–Primary Care Settings .............................................. 220
Exhibit 7.5. Redesigning Addiction Services for Integration With Primary Care:
Questions for Addiction Providers and Administrators To Consider.................221
Exhibit 7.6. Side Eects of Antidepressants .....................................224
Exhibit 8.1. Building an Eective Recruitment and Retention Plan for
Behavioral Health Service Providers ......................................... 233
Exhibit 8.2. Reducing Sta Turnover in Programs for Clients With CODs ............. 235
Exhibit 8.3. Essential Attitudes and Values for Providers Serving Clients With CODs .....237
Exhibit 8.4. Examples of Basic Competencies Needed To Treat People With CODs ..... 239
Exhibit 8.5. Six Intermediate Competencies for Treating People With CODs ...........240
Exhibit 8.6. Examples of Advanced Competencies for Treatment of People With CODs ..240
Exhibit 8.7. Certication for Health Professions ................................. 244
vi

TIP 42
Foreword
The Substance Abuse and Mental Health Services Administration (SAMHSA) is the U.S. Department of
Health and Human Services agency that leads public health efforts to reduce the impact of substance
abuse and mental illness on America’s communities. An important component of SAMHSA’s work is
focused on dissemination of evidence-based practices, and providing training and technical assistance to
healthcare practitioners on implementation of these best practices.
The Treatment Improvement Protocol (TIP) series contributes to SAMHSA’s mission by providing science-
based, best-practice guidance to the behavioral health field. TIPs reflect careful consideration of all
relevant clinical and health service research, demonstrated experience, and implementation requirements.
Select nonfederal clinical researchers, service providers, program administrators, and patient advocates
comprising each TIP’s consensus panel discuss these factors, offering input on the TIP’s specific topics in
their areas of expertise to reach consensus on best practices. Field reviewers then assess draft content and
the TIP is finalized.
The talent, dedication, and hard work that TIP panelists and reviewers bring to this highly participatory
process have helped bridge the gap between the promise of research and the needs of practicing
clinicians and administrators to serve, in the most scientifically sound and effective ways, people in need of
care and treatment of mental and substance use disorders. My sincere thanks to all who have contributed
their time and expertise to the development of this TIP. It is my hope that clinicians will find it useful and
informative to their work.
Elinore F. McCance-Katz, M.D., Ph.D.
Assistant Secretary for Mental Health and Substance Use
U.S. Department of Health and Human Services
Substance Abuse and Mental Health Services Administration
vii
This page intentionally left blank.

TIP 42
Executive Summary
This Treatment Improvement Protocol (TIP) update is intended to provide addiction counselors and other
providers, supervisors, and administrators with the latest science in the screening, assessment, diagnosis,
and management of co-occurring disorders (CODs). For purposes of this TIP, the term CODs refers to
co-occurring substance use disorders (SUDs) and mental disorders. Clients with CODs have one or more
disorders relating to the use of alcohol or other substances with misuse potential as well as one or more
mental disorders. A diagnosis of CODs occurs when at least one disorder of each type can be established
independently of the other and is not simply a cluster of symptoms resulting from the one disorder.
Many may think of the typical person with CODs as having a serious mental illness (SMI) combined with
a severe SUD, such as schizophrenia combined with alcohol use disorder (AUD). However, counselors
working in addiction agencies are more likely to see people with severe addiction combined with mild- to
moderate-severity mental disorders. An example would be a person with AUD combined with attention
deficit hyperactivity disorder (ADHD) or an anxiety disorder. Efforts to provide treatment that will meet
the unique needs of people with CODs have gained momentum over the past two decades in both SUD
treatment and mental health services settings.
An expert panel developed the TIP’s content based on a review of the most up-to-date literature and on
their extensive experience in the field of SUD treatment. Other professionals also generously contributed
their time and commitment to this publication.
This TIP is organized to guide counselors and other addiction professionals sequentially through the
primary components of proper identification and management of CODs. The TIP is divided into chapters
so that readers can easily find the material they need. Following is a summary of the TIP’s overall main
points and summaries of each of the eight TIP chapters.
The primary focus of this TIP is co-occurring SUDs and mental disorders, not physical disorders. People
with mental illness also frequently develop physical conditions that, like SUDs, can exacerbate or induce
symptoms (e.g., HIV, hepatitis C virus, hypothyroidism). However, physical conditions are beyond the scope
of this publication and are excluded.
Overall Key Messages
People with SUDs are more likely than those without SUDs to have co-occurring mental disorders.
Addiction counselors encounter clients with CODs as a rule, not an exception. Mental disorders likely
to co-occur with addiction include depressive disorders, bipolar I disorder, posttraumatic stress disorder
(PTSD), personality disorders (PDs), anxiety disorders, schizophrenia and other psychotic disorders, ADHD,
and eating and feeding disorders.
Serious gaps exist between the treatment and service needs of people with CODs and the actual care
they receive. Many factors contribute to the gap, such as lack of awareness about and training in CODs by
addiction counselors, as well as workforce factors like labor shortages and professional burnout.
Failure to routinely screen clients receiving behavioral health services for mental disorders and SUDs
creates a problematic domino effect. A lack of screening means a lack of assessment, which results
in a lack of diagnosis, which leads to a lack of treatment, which then reduces a person’s chances of
achieving long-term recovery for either or both disorders. Counselors and other providers can prevent
this cascade of negative events by understanding how and why to screen, how to perform a full
assessment, and how to recognize diagnostic symptoms of mental disorders and SUDs.
ix

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
CODs are treatable conditions, and a range
of treatment modalities exists that can be
implemented across numerous inpatient and
outpatient settings. Counselors may need to
adapt interventions based on the treatment
setting as well as the unique needs and
characteristics of clients, including their
gender, race/ethnicity, life circumstance (e.g.,
homelessness, involvement in the criminal justice
system), symptoms, functioning, stage of change,
risk of suicidality, and trauma history.
People with CODs are at an elevated risk for
self-harm, especially if they have a history of
trauma. Counselors, other providers, supervisors,
and administrators should make client safety
a priority and ensure that providers have the
necessary training to detect and respond to
suicidal thoughts, gestures, and attempts in COD
clientele.
Essential services for people with CODs are
person centered, trauma informed, culturally
responsive, recovery oriented, comprehensive, and
continuously offered across all levels of care and
disease course.
There is no “wrong door” by which people
with CODs arrive at treatment. Counselors and
programs should have a range of interventions and
services in their “toolbox” with which they can help
all clients.
Administrators and supervisors play a critical
role in responding to workforce challenges,
such as unmet training needs, low employee
retention, staff burnout, and low competency in
advanced COD management skills. Such workforce
matters are directly tied to treatment availability
and quality, so these challenges should be taken
seriously and addressed actively by all COD
treatment programs.
Content Overview
This TIP is divided into eight chapters designed
to thoroughly cover all relevant aspects of
screening, assessment, diagnosis, treatment, and
programming.
Chapter 1: Introduction to SUD Treatment
for People With CODs
This chapter provides a broad introduction to
CODs and to SUD treatment for people with
CODs. It serves as an outline of the main focus
of this TIP. The intended audiences are addiction
counselors and other SUD treatment professionals
(e.g., psychologists, psychiatrists, licensed clinical
social workers, licensed marriage and family
therapists, psychiatric and mental health nurses
[specialty practice registered nurses]), supervisors,
and administrators.
Mental illness is highly comorbid in people
with addiction and associated with low rates of
treatment engagement, retention, and completion.
CODs are linked to numerous negative health
outcomes and life circumstances, like elevated
risk of homelessness, trauma, and self-harm. To
close treatment gaps and ensure that people with
SUDs and mental disorders achieve long-lasting
recovery, educating counselors, supervisors,
and administrators about the prevalence and
seriousness of these conditions is essential.
In Chapter 1, readers will learn about:
•
The appropriate terminology surrounding CODs
and COD treatment approaches.
•
The numerous factors that led to the creation of
this TIP update.
•
The need for this TIP, which addresses CODs
and summarizes prevalence and treatment
rates, trends in programming, and negative
events associated with CODs (e.g., increased
hospitalization).
•
The complicated and bidirectional relationship
between mental disorders and SUDs that can
make diagnosing and treating these conditions
difficult.
Chapter 2: Guiding Principles for Working
With People Who Have CODs
This chapter reviews strategies and recommended
guidelines for effective COD services. The
intended audiences are counselors and other
behavioral health service providers, supervisors,
and administrators.
x

TIP 42
Service provision guidelines help safeguard the
well-being of clients with CODs and ensure that
they receive high-quality, evidence-based care.
Counselors and other providers, supervisors, and
administrators can take small but powerful steps
to increase the likelihood that clients with CODs
get the services they need, such as using person-
centered approaches, providing comprehensive
care, and integrating research into clinical services.
These strategies can have a large impact in terms
of generating positive treatment outcomes.
In Chapter 2, readers will learn that:
•
Essential services for people with CODs must
be recovery oriented, culturally responsive, and
inclusive of clients’ families or support system
(including mutual-help and peer recovery
supports).
•
Counselors should ensure that they are
providing clients full access to treatments;
routine screening and complete assessments;
services tailored to clients’ symptoms and stage
of change; and services that are integrated,
comprehensive, and continuous across
treatment settings and disease course.
•
Administrators and supervisors can increase
the odds of clients achieving optimal recovery
outcomes by ensuring that providers possess
the appropriate basic, intermediate, and
advanced competencies and have access to
training opportunities—both of which are
essential if counselors are to confidently and
competently manage CODs.
•
Integration of evidence-based care into COD
programming increases the chances of clients
receiving effective therapies that improve their
odds of lifelong recovery.
•
In addition to establishing essential services
(e.g., screening and assessment, onsite
prescribing, psychoeducation, mutual support),
program developers and administrators should
engage in ongoing assessment to ensure that
their organization has the capacity to serve
clients with CODs and is faithfully following
service implementation guidelines.
Chapter 3: Screening and Assessment of
CODs
This chapter describes the screening and full
assessment process for identifying people with and
at risk for mental illnesses and SUDs. The intended
audiences are addiction counselors and other
providers, supervisors, and administrators.
To reduce gaps in treatment access and provision,
counselors must appropriately engage in timely,
evidence-based screening and assessment. This
multistep process is designed to help counselors
thoroughly explore all areas of clients’ history,
symptoms, functioning, readiness for treatment,
and other service needs so that treatment decision
making is fully informed and tailored to each
individual’s clinical situation. In short, without
timely and effective screening and assessment,
the chances of clients receiving appropriate care
decrease significantly.
In Chapter 3, readers will learn that:
•
All SUD treatment clients should be screened at
least annually for SUDs, mental disorders, risk of
harm to self and others, functional impairment,
and trauma.
•
Screening is an informal yet highly effective
process of initially identifying people with CODs
who may ultimately need formal treatment or
other services.
•
A full biopsychosocial approach to assessment
helps counselors thoroughly explore clients’
physical, substance use–related, psychiatric,
social, educational/vocational, and family
histories for indications of addiction, mental
illness, or both.
•
Numerous screening and assessment measures
are validated for use with people who have
mental disorders and SUDs to help counselors
make diagnostic determinations and guide
decisions about referral for further evaluation
(e.g., psychiatric, medical).
•
Assessment is more than just administering
questionnaires; it includes exploring clients’
risk of harm to self and others, trauma history,
strengths and supports, cultural needs, and
readiness for change.
xi

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
•
When performed correctly, a full assessment
should help build rapport between the
counselor and the client and foster shared
decision making for treatment or other services.
Chapter 4: Mental and Substance-Related
Disorders: Diagnostic and Cross-Cutting
Topics
This chapter will help readers learn the Diagnostic
and Statistical Manual of Mental Disorders (5th ed.;
American Psychiatric Association, 2013) diagnostic
criteria for mental disorders that commonly occur
alongside SUDs, as well as symptoms of substance-
related disorders. The intended audiences
are addiction counselors and other providers,
supervisors, and administrators.
Not all addiction counselors are permitted to
diagnose mental disorders (regulations vary by
state). However, all addiction counselors and
other providers should become familiar with
the diagnostic criteria for mental illnesses that
commonly co-occur with SUDs so that they
can refer clients for a full psychiatric evaluation
(if needed) and tailor treatment and services
accordingly.
Someone with CODs will sometimes need
treatment approaches that differ slightly from
those for a person who has either an SUD or a
mental disorder but not both. Counselors and
other providers must understand how to recognize
signs of highly comorbid mental illnesses, know
how these disorders affect treatment decision
making, and recognize the trauma history and
risk of self-harm associated with these disorders.
Equally important, clinicians should learn how to
differentiate independent mental disorders from
substance-induced mental disorders, as the latter
are often treated differently than the former (if they
require treatment at all, given that many substance-
induced conditions remit once substance use has
ended).
In Chapter 4, readers will learn that:
•
Mental disorders that most commonly co-occur
with SUDs include major depressive disorder,
persistent depressive disorder (dysthymia),
bipolar I disorder, PTSD, borderline and
antisocial PDs, schizophrenia and other
psychotic disorders, generalized anxiety
disorder, panic disorder, social anxiety disorder,
ADHD, anorexia nervosa, bulimia nervosa, and
binge eating disorder.
•
Although less common in the general
population, all of these mental disorders are
likely to be seen by counselors working in SUD
treatment settings.
•
Counselors may need to treat SUDs in the
presence of a mental disorder in slightly
different ways than they would treat addiction
without comorbid mental illness. The way in
which treatment proceeds can vary depending
on the mental illness.
•
Nearly all CODs carry an increased risk of
suicide, and counselors are obligated to
thoroughly assess and respond to a current
report or history of self-harm.
•
Trauma is ubiquitous across CODs and needs to
be managed using trauma-informed techniques.
•
Many mental disorder symptoms mimic
symptoms of SUDs, and vice versa. Being able
to differentiate between the two is a core
competency.
•
Similarly, many mental disorders may appear
in the context of substance intoxication or
withdrawal. Treatment approaches for these
substance-induced disorders can differ from the
treatment of independent mental disorders,
so counselors must recognize the difference
between the two.
Chapter 5: Strategies for Working With
People Who Have CODs
This chapter summarizes the importance of
establishing a therapeutic alliance with clients
who have CODs and discusses how providers
can do so. The intended audiences are addiction
counselors and other providers, supervisors, and
administrators.
Good provider–client rapport can enhance
treatment outcomes and completion and is a
cornerstone of providing high-quality care. When
working with clients who have CODs, counselors
and other providers should be aware of clinical
factors and concerns—like confidentiality matters,
use of empathy, and cultural responsiveness—that
xii

TIP 42
can make the therapeutic relationship more
successful and increase the chances that clients will
achieve and maintain recovery.
For co-occurring mental disorders, like depression,
anxiety disorders, PTSD, and SMIs, specific
treatment strategies (e.g., selecting appropriate
therapeutic interventions; structuring clinical
sessions) can improve client adherence and
outcomes. Counselors and other providers should
learn these techniques and approaches before
treating individuals with CODs so that they are
prepared to best respond to clients’ needs and
help establish good therapeutic alliance from the
outset.
In Chapter 5, readers will learn that:
•
Rapport building is essential in helping clients
achieve and sustain positive behavior change.
•
Working with people who have CODs can be
challenging given clients’ feelings of mistrust
or shame. CODs can be complex and lifelong,
causing a range of difficulties for people living
with them.
•
A successful therapeutic alliance is built on
empathy and support and by providing services
fully responsive to all clients’ needs.
•
Relapse prevention and skill building are critical
components of comprehensive care.
•
Culturally sensitive techniques can help build
rapport and trust between counselors and
clients from various cultural, racial, and ethnic
backgrounds.
•
For clients with depression, cognitive–behavioral
techniques, behavioral activation, and
medication evaluation are core services.
•
Clients with anxiety may need treatments
tailored to their anxiety diagnosis, such as
individual therapy for a client with social anxiety
and fear of group settings.
•
Safety and trust are cornerstones of effective
treatment for people with trauma and PTSD.
•
People with SMI may have cognitive limitations
that undermine treatment participation and
adherence and may need help with basic living
needs (e.g., housing, employment).
Chapter 6: CODs Among Special
Populations
This chapter discusses four populations with CODs
who may be especially susceptible to treatment
challenges and negative outcomes: people
experiencing homelessness, people involved in
the criminal justice system, women, and racial/
ethnic minorities. The intended audiences are SUD
counselors and other providers, supervisors, and
administrators.
Although all people with CODs are vulnerable to
treatment difficulties and poor outcomes because
of the complex and chronic nature of their illnesses,
certain COD populations are especially susceptible
and may benefit from tailored services. Counselors
and other providers need to be sensitive to specific
treatment needs of such populations and make
adjustments in their assessment, diagnosis, referral,
and service provision accordingly.
In Chapter 6, readers will learn that:
•
CODs are highly prevalent in people who are
experiencing homelessness, but several service
models exist to help counselors address clients’
behavioral health concerns and their housing
needs.
•
People involved in the criminal justice system
are at risk for CODs both during incarceration
and after release into the community.
•
Treatment of CODs among justice system–
involved people is important because, if left
untreated, CODs can increase their risk of
recidivism, rearrest, and reincarceration.
•
Women are a vulnerable population because
of the increased likelihood that they will face
trauma, which heightens the occurrence of
CODs, and pregnancy/child care-related
factors, which can also exacerbate CODs or
otherwise affect treatment provision (such as
pharmacotherapy).
•
Although research suggests that COD treatment
outcomes for men and women are generally
equivalent, women may benefit from gender-
specific services in order to stay engaged in (and
thus benefit from) interventions.
•
Compared with U.S. Whites, people from racial/
ethnic minorities face significantly greater
xiii

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
mental health service and SUD treatment
access barriers and are likelier to have negative
treatment outcomes.
•
Counselors and other providers should
learn how to provide culturally responsive
assessments and treatments or other services to
meet the unique needs facing clients of diverse
racial/ethnic backgrounds who have CODs.
Chapter 7: Treatment Models and
Settings for People With CODs
This chapter is an overview of treatment models
and settings for clients with CODs. It will help
counselors and administrators offer empirically
supported care for this population. The intended
audiences are counselors and other providers,
supervisors, and administrators in addiction
programs.
CODs are complex conditions, and clients can
engage in services across a multitude of inpatient
and outpatient settings. Counselors and other
providers have at their disposal several empirically
validated treatment approaches designed to
address the full scope of needs of people with
CODs, including services to reduce symptoms,
increase abstinence, achieve stable housing,
and help clients make meaningful connections
with resources and networks of support in the
community. Although not appropriate for all
clients with CODs, pharmacotherapies are a
treatment option that, for certain conditions like
AUD and opioid use disorder (OUD), can not only
improve functioning but also reduce mortality and
morbidity. Counselors and other providers who
do not prescribe medication for clients with CODs
should nonetheless be aware of their uses, side
effects, and interactions/warnings so that they can
help monitor clients for safety and offer referrals
for medication evaluation as needed.
In Chapter 7, readers will learn that:
•
COD treatment can be sequential, simultaneous
(but in parallel), or concurrent (and integrated).
•
People with CODs face a multitude of individual,
logistic, socioeconomic, cultural, organizational,
systemic, and policy-related barriers to
accessing and using SUD treatment and mental
health services. Counselors and administrators
play important roles in reducing these barriers
and helping clients overcome such challenges.
•
Integrated care is recommended as a best
practice for serving people with CODs.
•
Assertive community outreach and intensive
case management are multidisciplinary
approaches that can be easily adapted to
integrated settings and thus offer clients
comprehensive, continuous care. They can also
be adapted to populations vulnerable to CODs
and poor outcomes, like people without stable
housing and those involved in the criminal
justice system.
•
Mutual supports, including from peer recovery
support specialists, are critical because they
offer clients information and support from
others with a lived experience with mental
illness, SUDs, or both. Many COD-specific
mutual-support programs are available, and
counselors should keep referral information on
hand so they can readily refer clients interested
in these services.
•
Providers can offer COD services in many
different settings, including therapeutic
communities, outpatient addiction centers,
residential treatment facilities, and acute
medical care facilities.
•
Pharmacotherapy is often a core part of
COD treatment, especially for people with
depression, bipolar I disorder, anxiety,
schizophrenia/psychotic disorders, AUD, or
OUD. Counselors do not prescribe medication,
but they should understand what medications
their clients are likely to take and the side
effects clients are likely to experience so they
can offer proper psychoeducation, help monitor
for unsafe side effects, and refer clients to
prescribers for medication management as
needed.
Chapter 8: Workforce and Administrative
Concerns in Working With People Who
Have CODs
This chapter reviews major issues facing the mental
health service and SUD treatment labor force
and demonstrates how workforce matters can
negatively affect clients with CODs. The intended
audiences are supervisors and administrators in
SUD treatment.
xiv

TIP 42
Projections about the behavioral health workforce
suggest that serious gaps will only increase as
the number of people entering and staying in the
profession is outpaced by the number of people
needing those professionals’ services. This trend
will continue unless there are interventions to
support the growing capacity and training needs
of the field. These gaps have resulted in people
with CODs having fewer opportunities to access
high-quality, evidence-based care across a broad
continuum of settings and services. Further,
unmet training, education, and credentialing in
CODs means that there is an insufficient number
of counselors and supervisors who understand
the treatment needs of this population and
how best to manage their conditions. Ensuring
better recruitment and retention of well-trained
behavioral health professionals is paramount
and will help broaden and strengthen the SUD
treatment and mental health services systems.
In Chapter 8, readers will learn that:
•
This country has a major shortage of mental
health and addiction professionals, and the
shortage will only continue to grow unless the
field uses strategies to increase the size of the
workforce and retain current professionals.
Workforce shortages partly account for why
people with CODs face challenges in accessing,
engaging in, adhering to, and benefitting from
services.
•
Recruitment, hiring, and retention techniques
can help programs attract and keep the right
candidates while reducing turnover.
•
Burnout is a major component of turnover and
is prominent in these fields because of the
complex and challenging nature of the client
population.
•
Many professionals working with clients who
have CODs feel uncomfortable or inadequately
prepared to offer effective COD services, but
better training and active clinical supervision can
remedy this.
•
Supervisors and administrators must ensure
that counselors are properly trained if good
client outcomes are to be achieved. Numerous
training resources are available to assist with this
process.
•
Professional certification and credentialing give
counselors and supervisors the necessary skills
to provide effective COD services and convey a
sense of staff competency and professionalism
within an organization.
xv
TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
TIP ORGANIZATION BY KEY TOPIC AREAS OF INTEREST
The expansive scope of this TIP covers clinically relevant and program-related concepts, guidelines, and
topic areas. The section “Content Overview,” broadly outlines the layout of the publication. The following
bullets will orient readers to the location of specific subject matter likely to be of high interest. Note
that some of the following content may be mentioned or discussed briefly in other chapters; this listing
reflects the primary locations in the TIP.
•
Ensuring continuity of care: Chapter 2
•
Providing essential program services for people with CODs: Chapter 2
•
Determining level of service and how to match treatment: Chapter 3
•
Screening and assessing for CODs: Chapter 3 (selected tools are located in Appendix C)
•
Addressing suicide risk: Chapter 3 (screening and assessment) and Chapter 4 (prevention and
management)
•
Using motivational enhancement: Chapter 5
•
Using relapse prevention techniques: Chapter 5
•
Dealing with common clinical challenges in working with clients who have CODs: Chapter 5
•
Understanding culture-specific matters, including how to provide culturally competent services:
Chapters 5 and 6
•
Modifying treatments for clients with CODs based on treatment setting and model: Chapter 7
•
Removing treatment barriers and improving service access for people with CODs: Chapter 7
•
Offering integrated care: Chapter 7
•
Designing residential and outpatient treatment programs: Chapter 7
•
Achieving core provider competencies in working with clients who have CODs: Chapter 8
xvi

TIP 42
TIP Development Participants
Note: The information given indicates participants’ affiliations
at the time of their participation in this TIP’s original
development and may not reflect their current affiliations.
Consensus Panel
Each TIP consensus panel is a group of primarily
nonfederal addiction-focused clinical, research,
administrative, and recovery support experts with
deep knowledge of the TIP’s topic. With SAMHSA’s
Knowledge Application Program team, members
of the consensus panel develop each TIP via a
consensus-driven, collaborative process that blends
evidence-based, best, and promising practices
with the panel members’ expertise and combined
wealth of experience.
Chair
Stanley Sacks, Ph.D.
Director
Center for the Integration of Research and Practice
National Development and Research Institutes, Inc.
New York, New York
Co-Chair
Richard K. Ries, M.D.
Director/Professor
Outpatient Mental Health Services
Dual Disorder Programs
Harborview Medical Center
Seattle, Washington
Workgroup Leaders
Donna Nagy McNelis, Ph.D.
Director, Behavioral Healthcare Education
Associate Professor, Psychiatry
Drexel University
School of Medicine
Philadelphia, Pennsylvania
David Mee-Lee, M.D., FASAM
DML Training and Consulting
Davis, California
James L. Sorenson, Ph.D.
Department of Psychiatry
San Francisco General Hospital
San Francisco, California
Douglas Ziedonis, M.D.
Director, Addiction Services
University Behavioral Healthcare System
Piscataway, New Jersey
Joan E. Zweben, Ph.D.
Executive Director
The 14th Street Clinic and Medical Group
East Bay Community Recovery Project
University of California
Berkeley, California
Panelists
Betty Blackmon, M.S.W., J.D.
Parker-Blackmon and Associates
Kansas City, Missouri
Steve Cantu, LCDC, CADAC, RAS
Clinical Program Coordinator
South Texas Rural Health Services, Inc.
Cotulla, Texas
Catherine S. Chichester, M.S.N., R.N., CS
Executive Director
Co-Occurring Collaborative of Southern Maine
Portland, Maine
Colleen Clark, Ph.D.
Research Associate
Department of Community Mental Health
University of South Florida
Tampa, Florida
xvii

TIP 42
KAP Expert Panel and Federal
Government Participants
Substance Use Disorder Treatment for People With Co-Occurring Disorders
Christie A. Cline, M.D., M.B.A.
Medical Director
Behavioral Health Sciences Division
New Mexico Department of Health
Santa Fe, New Mexico
Raymond Daw, M.A.
Executive Director
Na’nizhoozhi Center, Inc.
Gallup, New Mexico
Sharon C. Ekleberry, LCSW, LSATP, BCD
Division Director
Adult Outpatient Services
Fairfax County Mental Health Services
Fairfax/Falls Church Community Services Board
Centreville, Virginia
Byron N. Fujita, Ph.D.
Senior Psychologist
Clackamas County Mental Health Center
Oregon City, Oregon
Lewis E. Gallant, Ph.D.
Executive Director
National Association of State Alcohol and Drug
Abuse Directors, Inc.
Washington, DC
Michael Harle, M.H.S.
President/Executive Director
Gaudenzia, Inc.
Norristown, Pennsylvania
Michael W. Kirby, Jr., Ph.D.
Chief Executive Officer
Arapahoe House, Inc.
Thornton, Colorado
Kenneth Minkoff, M.D.
Medical Director
Choate Health Management
Woburn, Massachusetts
Lisa M. Najavits, Ph.D.
Associate Professor of Psychology
Harvard Medical School/McLean Hospital
Belmont, Massachusetts
Tomas A. Soto, Ph.D.
Director
Behavioral Sciences
The CORE Center
Chicago, Illinois
The Chair and Co-Chair would like to thank
Kenneth Minkoff, M.D., for his valuable
contributions to Chapter 3 of this TIP.
Special thanks go to Donna Nagy McNelis, Ph.D.,
for providing content on workforce development;
Tim Hamilton, for providing content about COD
mutual-support groups; Theresa Moyers, Ph.D.,
for her critical review of motivational interviewing
content; George A. Parks, Ph.D., for his input
about relapse prevention; Cynthia M. Bulik, Ph.D.,
for writing content about eating disorders; Lisa M.
Najavits, Ph.D., for her contributions addressing
PTSD; Barry S. Brown, Ph.D., for providing
consultation to the Chair; and Jo Scraba for her
editorial assistance to the Chair.
Barry S. Brown, Ph.D.
Adjunct Professor
University of North Carolina at Wilmington
Carolina Beach, North Carolina
Jacqueline Butler, M.S.W., LISW, LPCC, CCDC III,
CJS
Professor of Clinical Psychiatry College of Medicine
University of Cincinnati
Cincinnati, Ohio
Deion Cash
Executive Director
Community Treatment and Correction Center, Inc.
Canton, Ohio
Debra A. Claymore, M.Ed.Adm.
Owner/Chief Executive Officer WC Consulting, LLC
Loveland, Colorado
xviii

TIP 42
Carlo C. DiClemente, Ph.D.
Chair
Department of Psychology
University of Maryland–Baltimore County
Baltimore, Maryland
Catherine E. Dube, Ed.D.
Independent Consultant
Brown University
Providence, Rhode Island
Jerry P. Flanzer, D.S.W., LCSW, CAC
Chief, Services
Division of Clinical and Services Research
National Institute on Drug Abuse
Bethesda, Maryland
Michael Galer, D.B.A.
Chairman of the Graduate School of Business
University of Phoenix—Greater Boston Campus
Braintree, Massachusetts
Renata J. Henry, M.Ed.
Director
Division of Alcoholism, Drug Abuse, and Mental
Health
Delaware Department of Health and Social Services
New Castle, Delaware
Joel Hochberg, M.A.
President
Asher & Partners
Los Angeles, California
Jack Hollis, Ph.D.
Associate Director
Center for Health Research Kaiser Permanente
Portland, Oregon
Mary Beth Johnson, M.S.W.
Director
Addiction Technology Transfer Center
University of Missouri—Kansas City
Kansas City, Missouri
Eduardo Lopez, B.S.
Executive Producer
EVS Communications
Washington, DC
Holly A. Massett, Ph.D.
Academy for Educational Development
Washington, DC
Diane Miller
Chief
Scientific Communications Branch
National Institute on Alcohol Abuse and Alcoholism
Bethesda, Maryland
Harry B. Montoya, M.A.
President/Chief Executive Officer
Hands Across Cultures
Española, New Mexico
Richard K. Ries, M.D.
Director/Professor
Outpatient Mental Health Services
Dual Disorder Programs
Seattle, Washington
Gloria M. Rodriguez, D.S.W.
Research Scientist
Division of Addiction Services
New Jersey Department of Health and Senior
Services
Trenton, New Jersey
Everett Rogers, Ph.D.
Center for Communications Programs
Johns Hopkins University
Baltimore, Maryland
Jean R. Slutsky, P.A., M.S.P.H.
Senior Health Policy Analyst
Agency for Healthcare Research & Quality
Rockville, Maryland
Nedra Klein Weinreich, M.S.
President
Weinreich Communications
Canoga Park, California
Clarissa Wittenberg
Director
Office of Communications and Public Liaison
National Institute of Mental Health
Kensington, Maryland
xix

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
Consulting Members
Paul Purnell, M.A.
Social Solutions, LLC
Potomac, Maryland
Scott Ratzan, M.D., M.P.A., M.A.
Academy for Educational Development
Washington, DC
Thomas W. Valente, Ph.D.
Director, Master of Public Health Program
Department of Preventive Medicine
School of Medicine
University of Southern California
Alhambra, California
Patricia A. Wright, Ed.D.
Independent Consultant
Baltimore, Maryland
Field Reviewers
Field reviewers represent each TIP’s intended
target audiences. They work in addiction, mental
health, primary care, and adjacent fields. Their
direct frontline experience related to the TIP’s
topic allows them to provide valuable input on a
TIP’s relevance, utility, accuracy, and accessibility.
Additional advisors to this TIP include members of
a resource panel and an editorial advisory board.
Calvin Baker
Addicted Homeless Project
Program Coordinator
Division of Addictions and Mental Health
Prince George’s County Health Department
Forestville, Maryland
Richard J. Bilangi, M.S.
Executive Director/President
Connecticut Counseling Centers, Inc.
Middlebury, Connecticut
Dennis L. Bouffard, Ph.D.
Program Manager
Connecticut Valley Hospital
Addiction Services Division
Middletown, Connecticut
Kim P. Bowman, M.S.
Executive Director
Chester County Department of Drug and Alcohol
Services
West Chester, Pennsylvania
Patricia Hess Bridgman, M.A., CCDC IIIE
Associate Director
Ohio Council of Behavioral Healthcare Providers
Columbus, Ohio
Barry S. Brown, Ph.D.
Adjunct Professor
University of North Carolina at Wilmington
Carolina Beach, North Carolina
Vivian B. Brown, Ph.D.
President/Chief Executive Officer
PROTOTYPES
Culver City, California
Tamara J. Cadet, M.S.W., M.P.H.
Web Content Manager
Free to Grow: Head Start Partnerships to Promote
Substance-Free Communities
Columbia University
Andover, Massachusetts
Sharon M. Cadiz, Ed.D.
Senior Director of Special Projects
Project Return Foundation, Inc.
New York, New York
Jerome F. X. Carroll, Ph.D.
Private Practice
Brooklyn, New York
Bruce Carruth, Ph.D., LCSW
Private Practice
Laredo, Texas
Michael Cartwright, Ph.D.
Executive Director
Foundations Associates
Nashville, Tennessee
Catherine S. Chichester, M.S.N., R.N., CS
Executive Director
Co-Occurring Collaborative of Southern Maine
Portland, Maine
xx

TIP 42
CAPT Carol Coley, M.S., USPHS
Senior Program Management Advisor
Division of State and Community Assistance
Systems Improvement Branch
Center for Substance Abuse Treatment
Substance Abuse and Mental Health Services
Administration
Rockville, Maryland
Margaret A. Cramer, Ph.D.
Clinical Psychologist/Instructor
Melrose, Massachusetts
George De Leon, Ph.D.
Director
Center for Therapeutic Community Research
National Development and Research Institutes, Inc.
New York, New York
Janice M. Dyehouse, Ph.D., R.N., M.S.N.
Professor and Department Head
College of Nursing
University of Cincinnati
Cincinnati, Ohio
Benjam in M. Eiland, M.A., CATS, EAP
Director of Substance Abuse Services
Haight Ashbury Free Clinic
San Francisco, California
Dorothy J. Farr
Clinical Director
Bucks County Drug and Alcohol Commission, Inc.
Warminster, Pennsylvania
Michael I. Fingerhood, M.D., FACP
Associate Professor
Department of Medicine
Center for Chemical Dependence School of Medicine
Johns Hopkins Bayview Medical Center
Baltimore, Maryland
Jerry P. Flanzer, D.S.W., LCSW, CAC
Chief, Services
Division of Clinical and Services Research
National Institute on Drug Abuse
Bethesda, Maryland
Byron N. Fujita, Ph.D.
Senior Psychologist
Clackamas County Mental Health Center
Oregon City, Oregon
Gerard Gallucci, M.D., M.H.S.
Medical Director
Community Psychiatry Program
Bayview Medical Center
Johns Hopkins University
Baltimore, Maryland
Mary Gillespie, Psy.D., CASAC
Psychologist
Saratoga Springs, New York
Karen Scott Griffin, M.S.
Director of Administration
Gaudenzia, Inc.
Norristown, Pennsylvania
Valerie A. Gruber, Ph.D., M.P.H.
Assistant Clinical Professor
University of California, San Francisco
San Francisco, California
Nancy Handmaker, Ph.D.
Professor
Department of Psychology
University of New Mexico
Albuquerque, New Mexico
Edward Hendrickson, LMFT, MAC
Clinical Supervisor
Arlington County MHSASD
Arlington, Virginia
David Hodgins, Ph.D.
Professor
Department of Psychology
University of Calgary
Calgary, Canada
Kimberly A. Johnson
Director
Maine Office of Substance Abuse
Augusta Mental Health Complex
Augusta, Maine
xxi

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
Edith Jungblut
Public Health Advisor
Center for Substance Abuse Treatment
Substance Abuse and Mental Health Services
Administration
Rockville, Maryland
George A. Kanuck
Public Health Analyst
Co-Occurring and Homeless Branch
Division of State and Community Assistance
Center for Substance Abuse Treatment
Substance Abuse and Mental Health Services
Administration
Rockville, Maryland
Michael W. Kirby, Jr., Ph.D.
Chief Executive Officer
Arapahoe House, Inc.
Thornton, Colorado
Daniel R. Kivlahan, Ph.D.
Director
VA Center of Excellence in Substance Abuse
Treatment and Education
VA Puget Sound Health Care System
Seattle, Washington
TingFun May Lai, M.S.W., CSW, CASAC
Director
Chinatown Alcoholism Services
New York, New York
Linda Lantrip, D.O., R.N.
Medical Director
Central Oklahoma Community Mental Health Center
Norman, Oklahoma
Robert M. Long, M.S., LCDC, LADC
Director
Substance Abuse and Dual Diagnosis Services
Kennebee Valley Mental Health Center
Augusta, Maine
Russell P. MacPherson, Ph.D., CAP, CAPP, CCP,
CDVC, DAC
President
RPM Addiction Prevention Training
Sanford, Florida
Philip R. Magaletta, Ph.D.
Clinical Training Coordinator
Federal Bureau of Prisons
Washington, DC
G. Alan Marlatt, Ph.D.
Professor of Psychology
Director
The Addictive Behaviors Research Center
University of Washington
Seattle, Washington
Julia W. Maxwell, LICSW, CAS
Branch Manager
Department of Mental Health/Community Services
Mental Health and Addiction Services
St. Elizabeth’s Campus
Washington, DC
Frank A. McCorry, Ph.D.
Director
Clinical Services Unit
N.Y.S. Office of Alcoholism and Substance Abuse
Services
New York, New York
Gregory J. McHugo, Ph.D.
Research Associate Professor
Dartmouth Medical School
New Hampshire-Dartmouth Psychiatric Research
Center
Lebanon, New Hampshire
David Mee-Lee, M.D., FASAM
DML Training and Consulting
Davis, California
Kenneth Minkoff, M.D.
Medical Director
Choate Health Management
Woburn, Massachusetts
Theresa Moyers, Ph.D.
Assistant Research Professor
Department of Psychology
University of New Mexico
Albuquerque, New Mexico
xxii

TIP 42
Ethan Nebelkopf, Ph.D., MFCC
Clinic Director
Family and Child Guidance Center
Native American Health Center
Oakland, California
Gwen M. Olitsky, M.S.
Chief Executive Officer
The Self-Help Institute for Training and Therapy
Lansdale, Pennsylvania
Thomas A. Peltz, M.Ed., LMHC, CAS
Private Practice Therapist
Beverly Farms, Massachusetts
Stephanie W. Perry, M.D.
Assistant Commissioner of Health
Bureau of Alcohol and Drug Abuse Services
Tennessee Department of Health
Nashville, Tennessee
Lawrence D. Rickards, Ph.D.
CoOccurring Disorders Program Manager
Homeless Programs Branch
Center for Substance Abuse Treatment
Substance Abuse and Mental Health Services
Administration
Rockville, Maryland
Jeffery L. Rohacek, M.S., CASAC
Psychologist II
McPike Addiction Treatment Center
Utica, New York
Edwin M. Rubin, Psy.D.
Psychologist
Aurora Behavioral Health Services
Aurora Health Care
Milwaukee, Wisconsin
Theresa Rubin-Ortiz, LCSW
Clinical Director
Bonita House, Inc.
Oakland, California
Margaret M. Salinger, M.S.N., R.N., CARN
Unit/Program Manager
Coatesville VA Medical Center
Coatesville, Pennsylvania
Steven V. Sawicki
Assistant Program Director
Center for Human Development
Connecticut Outreach-West
Waterbury, Connecticut
Anna M. Scheyett, M.S.W., LCSW, CASWCM
Clinical Assistant Professor
School of Social Work
University of North Carolina
Chapel Hill, North Carolina
Marilyn S. Schmal, M.A., CSAC
Mental Health Therapist II
Arlington County Mental Health
Substance Abuse Services
Arlington, Virginia
Darren C. Skinner, Ph.D., LSW, CAC
Director
Gaudenzia, Inc.
Gaudenzia House West Chester
West Chester, Pennsylvania
David E. Smith, M.D.
Founder and President
Haight Ashbury Free Clinics, Inc.
San Francisco, California
Antony P. Stephen, Ph.D.
Executive Director
Mental Health and Behavioral Sciences
New Jersey Asian American Association for Human
Services, Inc.
Elizabeth, New Jersey
Norm Suchar
Program and Policy Analyst
National Alliance to End Homelessness
Washington, DC
Richard T. Suchinsky, M.D.
Associate Chief for Addictive Disorders and
Psychiatric Rehabilitation
Mental Health and Behavioral Science Services
Department of Veterans Affairs
Washington, DC
xxiii

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
Kimberly N. Sutton, Ph.D.
Director/Associate Professor of Psychiatry
Cork Institute on Alcohol and Other Drug Abuse
Morehouse School of Medicine
Atlanta, Georgia
Mary Lynn Ulrey, M.S., ARNP
Chief Operating Officer
Operation PAR, Inc.
Pinellas Park, Florida
Robert Walker, M.S.W., LCSW
Assistant Professor
Center on Drug and Alcohol Research
University of Kentucky
Lexington, Kentucky
Verner Stuart Westerberg, Ph.D.
President
Addiction Services Research
Albuquerque, New Mexico
Aline G. Wommack, R.N., M.S.
Deputy Director
Division of Substance Abuse and Addiction
Medicine
UCSF Deputy Department of Psychiatry
San Francisco, California
Ann S. Yabusaki, Ph.D.
Director
Coalition for a DrugFree Hawaii
Honolulu, Hawaii
Mariko Yamada, LCSW
Clinical Supervisor
Asian American Drug Abuse Program Inc.
Gardena, California
Debby Young
Windsor, California
Joan E. Zweben, Ph.D.
Executive Director
The 14th Street Clinic and Medical Group
East Bay Community Recovery Project
University of California
Berkley, California
Resource Panel
Robert E. Anderson
Director
Research and Program Applications
National Association of State Alcohol and Drug
Abuse Directors
Washington, DC
Nancy Bateman, LCSWC, CAC
Senior Staff Associate
Division of Professional Development and Advocacy
National Association of Social Workers
Washington, DC
James F. Callahan, D.P.A.
Executive Vice President
American Society of Addiction Medicine
Chevy Chase, Maryland
Frank Canizales, M.S.W.
Management Analyst, Alcohol Program
Division of Clinical and Preventive Services
Indian Health Service
Rockville, Maryland
Cathi Coridan, M.A.
Senior Director
Substance Abuse Programs and Policy
National Mental Health Association
Alexandria, Virginia
Jennifer Fiedelholtz
Public Health Analyst
Office of Policy and Program Coordination
Substance Abuse and Mental Health Services
Administration
Rockville, Maryland
Ingrid D. Goldstrom, M.Sc.
Center for Substance Abuse Treatment
Substance Abuse and Mental Health Services
Administration
Rockville, Maryland
xxiv

TIP 42
Lynne M. Haverkos, M.D., M.P.H.
Program Director
Behavioral Pediatrics and Health Promotion
Research Program
National Institute of Child Health and Human
Development
Bethesda, Maryland
Edward Hendrickson, LMFT, MAC
Clinical Supervisor
Arlington County Mental Health and Substance
Abuse Services Division
Arlington, Virginia
Kevin D. Hennessy, Ph.D.
Senior Health Policy Analyst
Office of the Assistant Secretary for Planning and
Evaluation
Department of Health and Human Services
Washington, DC
James (Gil) Hill, Ph.D.
Director
Office of Rural Health and Substance Abuse
American Psychological Association
Washington, DC
Hendree E. Jones, Ph.D.
Assistant Professor
Department of Psychiatry and Behavioral Sciences
Johns Hopkins University Center
Baltimore, Maryland
Diane M. Langhorst
Clinical Supervisor Substance Abuse Services
Henrico Area Mental Health and Retardation Services
Richmond, Virginia
Tom Leibfried, M.P.A.
Vice President of Government Relations
National Council for Community Behavioral
Healthcare
Rockville, Maryland
James J. Manlandro, D.O.
Director
Family Addiction Treatment Services, Inc.
Dennisville, New Jersey
Julia W. Maxwell, LICSW, CAS
Branch Director
Mental Health Addiction and Services Branch
Commission on Mental Health Services District of
Columbia
Washington, DC
William F. Northey, Jr., Ph.D.
Research Specialist
American Association for Marriage and Family
Therapy
Alexandria, Virginia
Fred C. Osher, M.D.
Director
Center for Behavioral Health, Justice and Public
Policy
University of Maryland
Jessup, Maryland
Terry C. Pellmar, Ph.D.
Director
Board on Neuroscience and Behavioral Health
Institute of Medicine
Washington, DC
Ernst Quimby, Ph.D.
Associate Professor
Department of Sociology and Anthropology
Howard University
Washington, DC
Susan E. Salasin
Director
Mental Health and Criminal Justice Program
Center for Substance Abuse Treatment
Substance Abuse and Mental Health Services
Administration
Rockville, Maryland
Laurel L. Stine, J.D., M.A.
Director of Federal Relations
Bazelon Center for Mental Health Law
Washington, DC
xxv

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
Richard T. Suchinsky, M.D.
Associate Director for Addictive Disorders and
Psychiatric Rehabilitation
Mental Health and Behavioral Sciences Services
Department of Veterans Affairs
Washington, DC
Jan Towers, Ph.D., CRNP
Director
Health Policy
American Academy of Nurse Practitioners
Washington, DC
Steve Wing
Senior Advisor for Drug Policy
Office of Policy and Program Coordination
Substance Abuse and Mental Health Services
Administration
Rockville, Maryland
Cultural Competency and Diversity
Network Participants
Raymond Daw, M.A.
Executive Director
Na’nizhoozhi Center, Inc.
Gallup, New Mexico
Disabilities Work Group
Michael I. Fingerhood, M.D., FACP
Associate Professor
Department of Medicine
Center for Chemical Dependence School of
Medicine
Johns Hopkins Bayview Medical Center
Baltimore, Maryland
Aging Work Group
Ting-Fun May Lai, M.S.W., CSW, CASAC
Director
Chinatown Alcoholism Center
Hamilton-Madison House
New York, New York
Asian and Pacific Islanders Work Group
Antony P. Stephen, Ph.D.
Executive Director
Mental Health & Behavioral Sciences
New Jersey Asian American Association for Human
Services, Inc.
Elizabeth, New Jersey
Asian and Pacific Islanders Workgroup
Richard T. Suchinsky, M.D.
Associate Chief for Addictive Disorders and
Psychiatric Rehabilitation
Mental Health and Behavioral Sciences Services
Department of Veterans Affairs
Washington, DC
Disabilities Work Group
Ann S. Yabusaki, Ph.D.
Director
Coalition for a DrugFree Hawaii
Honolulu, Hawaii
Asian and Pacific Islanders Work Group
xxvi

TIP 42
Publication Information
Acknowledgments
This publication was prepared under the
Knowledge Application Program (KAP) for the
Center for Substance Abuse Treatment, Substance
Abuse and Mental Health Services Administration
(SAMHSA). Karl D. White, Ed.D., and Andrea
Kopstein, Ph.D., M.P.H., served as the Contracting
Officer’s Representatives (CORs) for initial TIP
development. Content was reviewed and updated
in 2020. Suzanne Wise served as the COR, Candi
Byrne served as the Alternate COR, and Valerie
Tarantino, LCSW-C, as the Product Champion.
Disclaimer
The views, opinions, and content expressed herein
are the views of the consensus panel members and
do not necessarily reflect the official position of
SAMHSA. No official support of or endorsement by
SAMHSA for these opinions or for the instruments
or resources described is intended or should be
inferred. The guidelines presented should not be
considered substitutes for individualized client care
and treatment decisions.
Public Domain Notice
All materials appearing in this volume except those
taken directly from copyrighted sources are in the
public domain and may be reproduced or copied
without permission from SAMHSA or the authors.
Citation of the source is appreciated. However, this
publication may not be reproduced or distributed
for a fee without the specific, written authorization
of the Office of Communications, SAMHSA,
Department of Health and Human Services.
Electronic Access and Copies of Publicaon
This publication may be ordered or downloaded
from SAMHSA’s Publications and Digital Products
webpage at store.samhsa.gov. Or, please call
SAMHSA at 1-877-SAMHSA-7 (1-877-726-4727)
(English and Español).
Recommended Citation
Substance Abuse and Mental Health Services
Administration. Substance Use Disorder Treatment
for People With Co-Occurring Disorders. Treatment
Improvement Protocol (TIP) Series, No. 42.
SAMHSA Publication No. PEP20-02-01-004.
Rockville, MD: Substance Abuse and Mental Health
Services Administration, 2020.
Originating Oce
Quality Improvement and Workforce Development
Branch, Division of Services Improvement, Center
for Substance Abuse Treatment, Substance Abuse
and Mental Health Services Administration, 5600
Fishers Lane, Rockville, MD 20857.
Nondiscrimination Notice
SAMHSA complies with applicable federal civil
rights laws and does not discriminate on the basis
of race, color, national origin, age, disability, or
sex. SAMHSA cumple con las leyes federales
de derechos civiles aplicables y no discrimina
por motivos de raza, color, nacionalidad, edad,
discapacidad, o sexo.
SAMHSA Publication No. PEP20-02-01-004
First printed 2005
Updated 2020
xxvii
This page intentionally left blank.

Chapter 1—Introduction to Substance Use
Disorder Treatment for People With
Co-Occurring Disorders
KEY MESSAGES
TIP 42
SUBSTANCE USE DISORDER TREATMENT FOR
PEOPLE WITH CO-OCCURRING DISORDERS
• People with mental illness are likely to have
comorbid substance use disorders (SUDs) and
vice versa. Addiction counselors should expect
to encounter mental illness in their client
population.
• Co-occurring disorders (CODs) are
burdensome conditions that have significant
physical, emotional, functional, social, and
economic consequences for the people who
live with these disorders and their loved ones.
Society as a whole is also affected by the
prevalence of CODs.
• Over the past two decades, the behavioral health
field’s knowledge of the outcomes, service
needs, and treatment approaches for individuals
with CODs has expanded considerably. But gaps
remain in ready access to services and provision
of timely, appropriate, effective, evidence-based
care for people with CODs.
• CODs are complex and bidirectional. They
can wax and wane over time. Providers,
supervisors, and administrators should be
mindful of this when helping clients make
decisions about treatment and level of care.
What is health? The World Health Organization
(WHO) considers healthy states ones characterized
by “complete physical, mental, and social well-being
and not merely the absence of disease or infirmity”
(WHO, n.d.). The Department of Health and Human
Services’ (HHS) Healthy People 2020 initiative
also supports a broad definition of optimal health,
reflected by its overarching goals of (Centers for
Disease Control and Prevention [CDC], 2014):
•
Helping people achieve high-quality, long lives
free of preventable disease, disability, injury, and
premature death.
•
Establishing health equity, eliminating
disparities, and improving the health of all
groups.
•
Promoting quality of life, healthy development,
and healthy behaviors across all life stages.
The concept of “well-being” extends beyond
one’s physical condition and includes other
important areas of functioning and quality of life,
such as mental illness and SUDs. Healthy People
2020 policy and prevention goals include reducing
substance use among all Americans (especially
children) and decreasing the prevalence of mental
disorders (particularly suicidality and depression)
while increasing treatment access (Office of
Disease Prevention and Health Promotion, 2019).
SUDs and mental disorders are detrimental to the
health of individuals and to society as a whole.
The tendency of these disorders to co-occur can
make the damage they cause more extensive
and complex. As knowledge of CODs continues
to evolve, new challenges have arisen: What is
the best way to manage CODs and reduce lags
in treatment? How do we manage especially
vulnerable populations with CODs, such as people
experiencing homelessness and those in our
criminal justice system? What about people with
addiction and serious mental illness (SMI), such as
bipolar disorder or schizophrenia? What are the
best treatment environments and modalities? How
can we build an integrated system of care?
The main purpose of this Treatment Improvement
Protocol (TIP) is to attempt to answer these and
related questions by providing current, evidence-
based, practice-informed knowledge about the
rapidly advancing field of COD research. This
1

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
TIP is primarily for SUD treatment and mental
health service providers, clinical supervisors, and
program administrators.
This chapter introduces the TIP and is addressed
to all potential audiences of the TIP: counselors,
other treatment/service providers, supervisors,
and administrators. It describes the scope of this
TIP (both what is included and what is excluded
by design), its intended audience, and the
basic approach that has guided the selection of
strategies, techniques, and models highlighted in
the text. Next, a section on terminology, including
a box of key terms, will help provide a common
language and facilitate readers’ understanding
of core concepts in this TIP. The chapter also
addresses the developments that led to this TIP
revision as well as the underlying rationale for
developing a publication on CODs specifically.
Scope of This TIP
The TIP summarizes state-of-the-art diagnosis,
treatment, and service delivery for CODs in the
addiction and mental health fields. It contains
chapters on screening and assessment, diagnosis,
and treatment settings and models, as well as
recommendations to address workforce and
administration needs. It is not intended for trainees
or junior professionals lacking a basic background
in mental illness and addiction (see the “Audience”
section that follows). It therefore excludes generic,
introductory information about mental disorders
and SUDs. Of note:
•
The primary concern of this TIP is co-occurring
SUDs and mental disorders, even though
the vulnerable population with CODs is also
subject to many other physical conditions. As
such, co-occurring physical disorders common
in individuals with SUDs, mental disorders, or
both (e.g., HIV, hepatitis C virus) are beyond the
scope of this publication and excluded.
•
Tobacco use disorder, which was treated in
the original TIP as an important cross-cutting
issue, is omitted from this update. Since the
original development of this TIP, considerable
and comprehensive treatment resources have
become available specific to nicotine cessation.
•
Pathological gambling, which the Diagnostic
and Statistical Manual of Mental Disorders (5th
ed.; DSM-5; American Psychiatric Association,
2013) classifies along with other SUDs and which
was included in the original TIP, is not addressed
in this update because behavioral addictions are
outside its scope.
•
Although the TIP addresses several specific
populations (i.e., people experiencing
homelessness; people involved in the criminal
justice system; people from diverse racial,
ethnic, and cultural backgrounds; women;
active duty and veteran military personnel), it
does so briefly. It also omits content specifically
for adolescents. The authors fully recognize,
and the TIP states repeatedly, that all COD
treatment must be culturally responsive.
Audience
The primary audience for this TIP is SUD treatment
providers. It is meant to meet the needs of those
with basic education/experience as well as the
differing needs of those with intermediate or
advanced education. SUD treatment providers
include drug and alcohol counselors, licensed clinical
social workers and psychologists who specialize in
addiction treatment, and specialty practice registered
nurses [psychiatric and mental health nurses]). Many
such providers have addiction counseling certification
or related professional licenses. Some may have
credentials in the treatment of mental disorders or in
criminal justice services.
Other main audiences for this TIP are mental
health service providers, as well as primary
care providers (e.g., general practitioners,
internal medicine specialists, family physicians,
nurse practitioners), who may encounter patients
with CODs in their clinics, private practices, or
emergency medicine settings.
Secondary audiences include administrators,
supervisors, educators, researchers, criminal justice
staff, and other healthcare and social service
providers who work with people who have CODs.
Approach
The TIP uses three criteria for including a
particular strategy, technique, or model:
1. Definitive research (i.e., evidence-based
treatments)
Chapter 1 2
TIP 42
Chapter 1—Introduction to SUD Treatment for People With Co-Occurring Disorders
2. Well-articulated approaches with empirical
support
3. Consensus panel agreement about established
clinical practice
The information in this TIP derives from a variety
of sources, including the research literature,
conceptual writings, descriptions of established
program models, accumulated clinical experience
and expertise, government reports, and other
available empirical evidence. It reflects the current
state of clinical wisdom regarding the treatment of
clients with CODs.
Guidance for the Reader
This TIP is a resource document and a guide on
CODs. It contains up-to-date knowledge and
instructive material, reviews selected literature,
summarizes many COD treatment approaches,
and covers some empirical information. The scope
of CODs generated a complex and extensive TIP
that is probably best read by chapter or section.
It contains text boxes, case histories, illustrations,
and summaries to synthesize knowledge that is
EXHIBIT 1.1. Key Terms
grounded in the practical realities of clinical cases
and real situations.
A special feature throughout the TIP—“Advice
to the Counselor” boxes—provides direct and
accessible guidance for the counselor. Readers
can study these boxes to obtain concise practical
guidance. Advice to the Counselor boxes distill what
the counselor needs to know and what steps to
take; they are enriched by more detailed reading of
the relevant material in each section or chapter.
The chair and co-chair of the TIP consensus panel
encourage collaboration among providers and
treatment agencies to translate the concepts
and methods of this TIP into other useable tools
specifically shaped to the needs and resources
of each agency and situation. The consensus
panel hopes that the reader will gain from this
TIP increased knowledge, encouragement, and
resources for the important work of treating people
with CODs.
Terminology in This TIP
Exhibit 1.1 defines key terms that appear in this TIP.
•
Addiction*: The most severe form of SUD, associated with compulsive or uncontrolled use of one or more
substances. Addiction is a chronic brain disease that has the potential for both recurrence (relapse) and
recovery.
•
Binge drinking*: A drinking pattern that leads to blood alcohol concentration levels of 0.08 grams per
deciliter or greater. This usually takes place after four or more drinks for women and five or more drinks
for men (National Institute on Drug Abuse, n.d.; Center for Behavioral Health Statistics and Quality, 2019).
However, older adults are more sensitive to the effects of alcohol and treatment providers may need to
lower these numbers when screening for alcohol misuse (Kaiser Permanente, 2019). Additionally, other
factors such as weight, decrease in enzyme activity, and body composition, (e.g. amount of muscle tissue
present in the body) can also affect alcohol absorption rates.
•
Continuing care: Care that supports a client’s progress, monitors his or her condition, and can respond to
a return to substance use or a return of symptoms of a mental disorder. Continuing care is both a process
of posttreatment monitoring and a form of treatment itself. It is sometimes referred to as aftercare.
•
Co-occurring disorders: In this TIP, this term refers to co-occurring SUDs and mental disorders. Clients
with CODs have one or more mental disorders as well as one or more SUDs.
•
Heavy drinking*: Consuming five or more drinks for men and four or more drinks for women in one
period on each of 5 or more days in the past 30 days (NIAAA, n.d.).
•
Integrated interventions: Specific treatment strategies or therapeutic techniques in which interventions for
the SUD and mental disorder are combined in one session or in a series of interactions or multiple sessions.
•
Mutual support programs: Mutual support programs consist of groups of people who work together to
achieve and maintain recovery. Unlike peer support (e.g., use of recovery coaches), mutual support groups
Chapter 1 3

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
consist only of people who volunteer their time and typically have no official connection to treatment
programs. Most are self-supporting. Although 12-Step groups (e.g., Alcoholics Anonymous and Narcotics
Anonymous) are the most widespread and well researched type of mutual support groups, other groups
may be available in some areas. They range from groups affiliated with a religion or church (e.g., Celebrate
Recovery, Millati Islami) to purely secular groups (e.g., SMART Recovery, Women for Sobriety).
•
Peer recovery support services: The entire range of SUD treatment and mental health services that help
support individuals’ recovery and that are provided by peers. The peers who provide these services are called
peer recovery support specialists (“peer specialists” for brevity), peer providers, or recovery coaches.
•
Relapse*: A return to substance use after a significant period of abstinence.
•
Recovery*: A process of change through which individuals improve their health and wellness, live a
self-directed life, and strive to reach their full potential. Even individuals with severe and chronic SUDs
can, with help, overcome their SUD and regain health and social function. This is called remission. When
those positive changes and values become part of a voluntarily adopted lifestyle, that is called “being in
recovery.” Although abstinence from all substance misuse is a cardinal feature of a recovery lifestyle, it is
not the only healthy, pro-social feature.
•
Standard drink*: Based on the 2015–2020 Dietary Guidelines for Americans (HHS, U.S. Department of
Agriculture, 2015) one standard drink contains 14 grams (0.6 ounces) of pure alcohol:
12 fl oz. of
regular beer
about 5%
alcohol
8-9 fl oz. of
malt liquor
(shown in a
12 oz glass)
about 7%
alcohol
5 fl oz. of
table wine
about 12%
alcohol
1.5 fl oz. shot
of 80-proof
distilled spirits
(gin, rum, tequila,
vodka, whiskey, etc.)
40% alcohol
The percent of “pure” alcohol, expressed here as alcohol by
volume (alc/vol), varies by beverage.
•
Substance*: A psychoactive compound with the potential to cause health and social problems, including
SUDs (and their most severe manifestation, addiction). The insert at the bottom of this exhibit lists
common examples of such substances.
•
Substance misuse*: The use of any substance in a manner, situation, amount, or frequency that can
cause harm to users or to those around them. For some substances or individuals, any use would
constitute misuse (e.g., underage drinking, injection drug use).
•
Substance use*: The use—even one time—of any of the substances listed in the insert.
•
Substance use disorder*: A medical illness caused by repeated misuse of a substance or substances.
According to the DSM-5 (American Psychiatric Association [APA], 2013), SUDs are characterized by
clinically significant impairments in health, social function, and impaired control over substance use and
are diagnosed through assessing cognitive, behavioral, and psychological symptoms. SUDs range from
mild to severe and from temporary to chronic. They typically develop gradually over time with repeated
misuse, leading to changes in brain circuits governing incentive salience (the ability of substance-
associated cues to trigger substance seeking), reward, stress, and executive functions like decision making
and self-control. Multiple factors influence whether and how rapidly a person will develop an SUD. These
Chapter 1 4

TIP 42
•
•
•
•
•
•
•
Chapter 1—Introduction to SUD Treatment for People With Co-Occurring Disorders
factors include the substance itself; the genetic vulnerability of the user; and the amount, frequency, and
duration of the misuse. Note: A severe SUD is commonly called an addiction.
Categories and examples of substances
SUBSTANCE CATEGORY REPRESENTATIVE EXAMPLES
Alcohol
•
•
•
•
Beer
Wine
Malt liquor
Distilled spirits
Illicit Drugs Cocaine, including crack
Her
oin
Hallucinogens, including LSD (lysergic acid
dieth
ylamide), PCP (ph
encyclidine), ecstasy,
peyote, mescaline, psilocybin
Methamphetamines, including crystal meth
Marijuana, including hashish
†
Synthetic drugs, including K2, Spice, and “bath salts”
Prescription-type medications that are used for
nonm
edical purposes
-
-
-
-
Pain relievers—Synthetic, semisynthetic, and
nonsynthetic opioid medications, including
fentanyl, codeine, oxycodone, hydrocodone, and
tramadol products
Tranquilizers, including benzodiazepines,
meprobamate products, and muscle relaxants
Stimulants and methamphetamine, including
amphetamine, dextroamphetamine, and
phentermine products; mazindol products;
and methylphenidate or dexmethylphenidate
products
Sedatives, including temazepam, flurazepam, or
triazolam and any barbiturates
Over
-the-Counter Drugs and Other Substances
•
•
Cough and cold medicines
Inhalants, including amyl nitrite, cleaning fluids,
gasoline and lighter gases, anesthetics, solvents,
spray paint, nitrous oxide
†
As of March 2020, most states and the District of Columbia have legalized medical marijuana use, although some
states have stricter limitations than others. Additionally, a significant number of states and the District of Columbia
also allow recreational use and home cultivation. It should be noted that none of the permitted uses under state laws
alter the status of marijuana and its constituent compounds as illicit drugs under Schedule I of the federal Controlled
Substances Act.
Source: HHS Office of the Surgeon General (2016).
*The definitions of all terms marked with an asterisk correspond closely to those given in Facing Addiction in America: The
Surgeon General’s Report on Alcohol, Drugs, and Health. The standard drink image and the table depicting substance
types and categories come from the same source, which is in the public domain. This resource provides a great deal of
useful information about substance misuse and its impact on U.S. public health. The report is available online (https://
addiction.surgeongeneral.gov/sites/default/files/surgeon-generals-report.pdf).
Chapter 1 5

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
The behavioral health field has used many terms to
describe the group of individuals who have CODs.
Some of these terms do not appear in this TIP,
which attempts to reflect a “person-first” approach
(see the “Person-Centered Terminology” section).
Providers and other professionals working with
people who have CODs need to understand that
some terms that have been commonly related
to CODs may now be outdated and, in certain
cases, pejorative. Such terms include:
Person-Centered Terminology
•
Dual diagnosis.
•
Dually diagnosed.
•
Dually disordered.
•
Mentally ill chemical abuser.
•
Mentally ill chemically dependent.
•
Mentally ill substance abuser.
•
Mentally ill substance using.
•
Chemically abusing mentally ill.
•
Chemically addicted and mentally ill.
•
Substance abusing mentally ill.
All of these terms have their uses, but many have
connotations that are unhelpful or too broad or
varied in interpretation to be useful. For example,
“dual diagnosis” also can mean having both mental
and developmental disorders. Outside of this
TIP, readers should not assume that these terms
all have the same meaning as CODs and should
clarify the client characteristics associated with a
particular term. Readers should also realize that the
term “co-occurring disorder” is not always precise.
As with other terms, it may become distorted over
time by common use and come to refer to other
conditions; after all, clients and consumers may
have a number of health conditions that “co-
occur,” including physical illness. Nevertheless, for
the purpose of this TIP, CODs refers only to SUDs
and mental disorders.
Some clients’ mental illness symptoms may not
fully meet strict definitions of co-occurring SUDs
and mental disorders or criteria for diagnoses in
DSM-5 categories. However, many of the relevant
principles that apply to the treatment of CODs will
also apply to these individuals. Careful assessment
and treatment planning to take each disorder into
account will still be important.
This TIP uses only person-first language—such as
“person with CODs.” In recent years, consumer
advocacy groups have expressed concerns
about how clients are classified. Many object to
terminology that seems to put them in a “box”
with a label that follows them through life, that
does not capture the fullness of their identities.
A person with CODs may also be a mother, a
plumber, a pianist, a student, or a person with
diabetes, to cite just a few examples. Referring
to an individual as a person who has a specific
disorder—a person with depression rather than “a
depressive,” a person with schizophrenia rather
than “a schizophrenic,” or a person who uses
heroin rather than “a heroin addict”—is more
acceptable to many clients because it implies
that they have many characteristics beyond a
stigmatized illness, and therefore they are not
defined by this illness.
Because this TIP’s primary audience is
counselors in the addiction and mental health
fields, this publication uses the term “client,”
rather than “patient” or “consumer.”
Important Developments That
Led to This TIP Update
Important developments in a number of areas
pointed to the need for a revised TIP on CODs:
•
The revisions to the diagnostic classification of
and diagnostic criteria for mental disorders in
DSM-5 made an update necessary. See Chapter
4 for an indepth discussion of DSM-5 diagnoses.
•
This update to TIP 42 offers a greater emphasis
on integrated care or concurrent treatment
(e.g., treating a client’s alcohol use disorder
[AUD] at the same time that you treat his or
her posttraumatic stress disorder [PTSD]), as
this is a larger focus of the research and clinical
field today than when this TIP was originally
published. More information about treatment
approaches is in Chapter 7.
Chapter 1 6
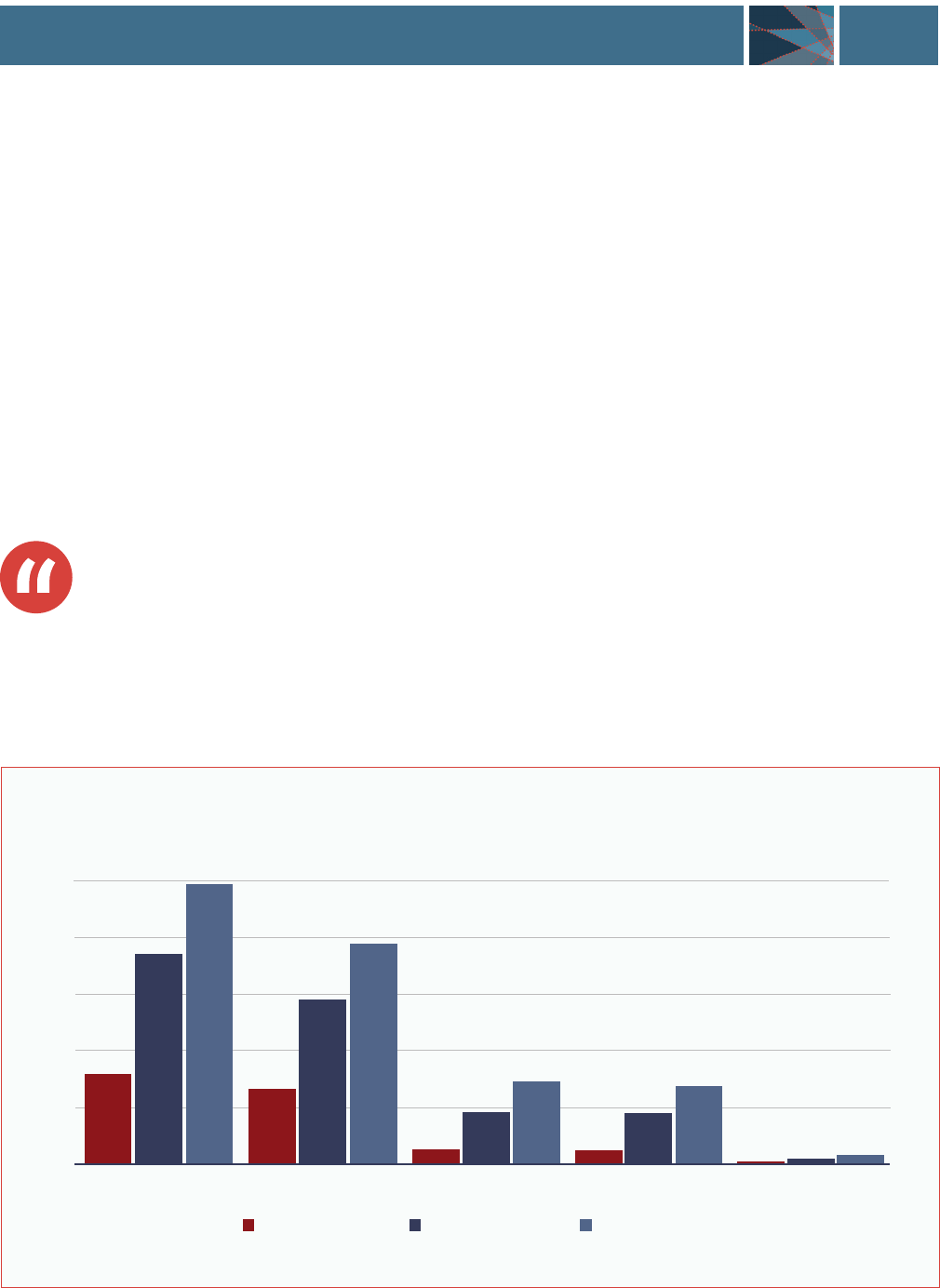
TIP 42
5.6M
50%
40%
30%
20%
10%
0%
Heroin
Illicit Drugs
Cannabis
Opioid Misuse
Prescription Pain
Reliever Misuse
31.5M
17.5M
26.5M
13.9M
4.4M
5.2M
4.4M
1.7M
5.0M
4.2M
1.6M
367K
430K
206K
15.7%
13.2%
2.6%
2.5%
0.2%
0.9%+
1.8%+
13.9%+
8.9%+
36.7%
49.4%+
29.2%+
38.9%+
9.2%+
14.6%+
No Mental Illness Any Mental Illness SMI
Source: McCance-Katz (2019). Adapted from material in the public domain.
Chapter 1—Introduction to SUD Treatment for People With Co-Occurring Disorders
•
This update reflects a wealth of new data about
effective treatment options for people with
CODs, including those with SMI (see especially
Chapter 7).
Why Do We Need a TIP on CODs?
Empirical evidence confirms that CODs are
serious problems in need of better management.
Treatment rates are markedly low and outcomes
often suboptimal, underscoring the importance of
advancing the field’s knowledge about and use of
appropriate, specialized techniques for screening,
assessment, diagnosis, and coordinated care of this
population. Findings from four key areas are borne
out by prevalence statistics and other nationally
representative survey data and reveal the stark
reality of underservice in this population.
“Comorbidity is important because
it is the rule rather than the
exception with mental health
disorders.”
Source: Lai, Cleary, Sitharthan, & Hunt, 2015; p. 8
1. Prevalence and Treatment Need of CODs
National surveys suggest that mental illness
(and SMI in particular) commonly co-occurs
with substance misuse in the general adult
population, and many individuals with CODs
go untreated. The National Survey on Drug Use
and Health (NSDUH), based on a sample of more
than 67,700 U.S. civilians ages 12 or older in
noninstitutionalized settings (Center for Behavioral
Health Statistics and Quality [CBHSQ], 2019), offers
revealing insights. Notable statistics from the latest
survey include the following (CBHSQ, 2019):
•
In 2018, 47.6 million (19.1 percent of all adults)
adults ages 18 and older had any mental illness
during the previous year, including 11.4 million
(4.6 percent of all adults) with SMI.
- Among these 47.6 million adults with any
past-year mental disorder, 9.2 million (19.3
percent) also had an SUD, but only 5 percent
of adults without any mental illness in the
past year had an SUD.
- Of the 11.4 million adults with an SMI in the
previous year, approximately 28 percent also
had an SUD.
EXHIBIT 1.2. Co-Occurring Substance Misuse in Adults Ages 18 and
Older With and Without Any Mental Illness and SMI (in 2018)
Chapter 1 7

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
•
SMI is highly correlated with substance misuse
(Exhibit 1.2; McCance-Katz, 2019). Adults ages
18 and older with any past-year mental illness
were more likely than those without to use illicit
drugs or misuse prescription medication. This
pattern was even more pronounced among
people with SMI. Of the 47.6 million adults with
any past-year mental illness, more than half
(56.7 percent) received no treatment, and over
one-third (35.9 percent) of adults with an SMI
in the past year received no treatment. Further,
nearly all (more than 90 percent) of the 9.2
million adults with both a past-year mental
illness and SUD did not receive services for
both conditions (McCance-Katz, 2019).
•
About 14.2 million adults (about 5.7 percent of
all adults) saw themselves as needing mental
health services at some point in the previous
year but did not receive it (CBHSQ, 2019):
-
Of adults with any mental disorder, 11.2
million (almost 24 percent), or nearly 1
in 4 adults with any mental illness, had a
perceived unmet need for mental health
services in the past year.
-
Of adults with an SMI, 5.1 million (about 45
percent), or more than 2 out of every 5 adults
with SMI, had a perceived unmet need for
mental health services in the previous year.
•
More than 18 million people ages 12 and older
needed but did not receive SUD treatment in
the previous year (e.g., they had an SUD or
problems related to substance use). Most of
those individuals did not see themselves as
needing treatment (only 5 percent thought they
needed it).
•
Almost half (48.6 percent) of adults ages
18 and older with any mental illness and
co-occurring SUD received no treatment at
all in 2018. About 41 percent received mental
health services only, 3.3 percent received SUD
treatment only, and 7 percent received both.
•
Of adults with SMI and co-occurring SUDs,
30.5 percent received no treatment. About 56
received mental health services only; almost 3
percent received SUD treatment only; and about
11 percent received both.
Other nationally representative survey datasets
confirm the high rate of comorbidity and treatment
need for mental disorders and SUDs in the general
adult population. An analysis of Wave 3 of the
National Epidemiologic Survey on Alcohol and
Related Conditions (NESARC-III; Grant et al.,
2015) revealed an increased risk of comorbid
mental illness among people with 12-month and
lifetime AUD. Specifically, the odds of having major
depression, bipolar disorder, antisocial personality
disorder (PD), borderline PD (BPD), panic disorder,
specific phobia, or generalized anxiety disorder
(GAD) ranged from 1.2 to 6.4. Only 20 percent of
people with lifetime AUD and 8 percent of people
with 12-month AUD received treatment.
From the same survey, any 12-month drug use
disorder (i.e., SUD not involving alcohol) was
associated with significantly increased odds of also
having a co-occurring mental disorder, including
1.3 times the odds of having major depressive
disorder (MDD), 1.5 odds of dysthymia, 1.5 odds
of bipolar I disorder, 1.6 odds of PTSD, 1.4 odds
of antisocial PD, and 1.8 odds of BPD (Grant et
al., 2016). Lifetime drug use disorder had similar
comorbidities but also was associated with a
1.3 increase in odds of also having GAD, panic
disorder, or social phobia. Only 13.5 percent of
people with a 12-month drug use disorder and
about a quarter of people with any lifetime drug
use disorder received treatment in the past year.
2. CODs and Hospitalizations
Compared with people with mental disorders or
SUDs alone, people with CODs are more likely
to be hospitalized. Some evidence suggests that
the hospitalization rate for people with CODs is
increasing.
Since the 1960s, treatment for mental disorders
and SUDs in the United States has shifted away
from state-owned facilities to psychiatric units in
general hospitals and private psychiatric hospitals
(Parks & Radke, 2014). Psychiatric bed capacity
has continued to shrink over the past few
decades in the United States and elsewhere
(Allison, & Bastiampillai, 2017; Lutterman, Shaw,
Fisher, & Manderscheid, 2017; Tyrer, Sharfstein,
O’Reilly, Allison, & Bastiampillai, 2017), despite
Chapter 1 8

TIP 42
Chapter 1—Introduction to SUD Treatment for People With Co-Occurring Disorders
OPIOID USE DISORDER AND THE PROBLEM OF CODs
Opioid addiction and overdose are a public health crisis and the target of numerous federal prevention
and treatment campaigns. Among the causes for concern is the high rate of CODs among people with
opioid use disorder (OUD). Of 2 million U.S. adults with OUD in the 2015 to 2017 NSDUH (Jones & McCance-
Katz, 2019):
• 77 percent also had another SUD or nicotine dependence in the past year.
• 64 percent also had any co-occurring mental illness in the past year.
• 27 percent had a past-year comorbid SMI.
In terms of service provision, 38 percent of people with OUD and any past-year mental illness or SMI
received SUD treatment in the previous year. Mental health services were more common, with 55 percent
of people with OUD and any mental illness and 65 percent of those with OUD and SMI receiving care in the
previous year. However, comprehensive treatment for both disorders was low and reported by only one-
quarter of people with OUD and any mental illness and 30 percent of people with OUD and SMI.
an upsurge in mental disorder/SUD-related
hospitalizations:
•
The Agency for Healthcare Research and Quality
found that from 2005 to 2014, the number of
hospital inpatient stays for people with mental
disorders or SUDs increased by 12 percent, and
the proportion of total inpatient stays accounted
for by mental disorders or SUDs also increased,
by 20 percent (McDermott, Elixhauser, & Sun,
2017).
•
CODs are also linked to rehospitalizations for
non-behavioral-health reasons (i.e., for physical
health conditions). Among a large sample of
Florida Medicaid recipients (Becker, Boaz,
Andel, & Hafner, 2017), 28 percent of people
with SMI and an SUD were rehospitalized within
30 days of discharge, whereas rehospitalization
occurred in only 17 percent of people with
neither disorder, 22 percent of people with
SMI only, 27 percent of people with a drug use
disorder, and 24 percent of people with AUD.
•
In the 2000 to 2012 Treatment Episode Data Set
(TEDS), SUD treatment-related admissions of
adults ages 55 and older that also involved co-
occurring psychiatric problems nearly doubled,
from 17 percent to 32 percent (Chhatre, Cook,
Mallik, & Jayadevappa, 2017).
•
As reported in the 2012 Healthcare Cost
and Utilization Project (Heslin, Elixhauser, &
Steiner, 2015), almost 6 percent of all inpatient
hospitalizations in the United States involved a
COD, 21 percent a mental disorder diagnosis
only, and about 6 percent an SUD only. Of
inpatient stays involving a primary diagnosis of
mental illness or SUD, 46 percent were because
of a COD, whereas 40 percent of inpatient stays
involved a mental disorder only and 15 percent
an SUD only (Heslin et al., 2015).
Hospitalizations and early readmissions are costly,
potentially preventable occurrences. Identifying
individuals at risk for either or both (such as
individuals with CODs) could inform more effective
discharge planning and wraparound services.
3. Trends in COD Programming
Some evidence supports an increased prevalence
of people with CODs in treatment settings
and of more programs for people with CODs.
However, treatment gaps remain.
Data from the Nationwide Inpatient Sample of the
Healthcare Cost and Utilization Project (Zhu & Wu,
2018) found that the number of people ages 12
and older hospitalized for inpatient detoxification
who had a co-occurring mental disorder diagnosis
increased significantly from 43 percent in 2003
to almost 59 percent in 2011. This included a
significant rise in co-occurring anxiety disorders
(8 percent vs. 17 percent) and nonsignificant
but notable increases in mood disorders (35
Chapter 1 9

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
percent vs. 46 percent) and schizophrenia or other
psychotic disorders (3 percent vs. 5 percent).
Recent survey data (Substance Abuse and Mental
Health Services Administration [SAMHSA], 2018e)
revealed a significant increase in the proportion of
clients with CODs in SUD treatment facilities from
2007 (37 percent) to 2017 (50 percent).
COD programming has not kept pace with the
increase in clients needing such services. In 2018,
almost every SUD treatment facility surveyed
through the National Survey of Substance Abuse
Treatment Services (99.8 percent) reported
having clients in treatment with a diagnosed
COD (SAMHSA, 2019a). However, only 50
percent of the facilities indicated that they
provided specifically tailored programs or group
treatments for clients with CODs.
The 2018 National Mental Health Services Survey
(SAMHSA, 2019b) reported similar findings: Only
46 percent of mental health service facilities
offered COD-specific programming. Facilities
most likely to offer COD programming were
private psychiatric hospitals (65 percent), Veterans
Administration medical centers (56 percent), and
multisetting mental health facilities (59 percent),
and community mental health centers (54 percent).
Among those least likely to offer COD programs
were partial hospitalization/day treatment facilities
(37 percent) and general hospitals (40 percent). A
national survey of 256 SUD treatment and mental
health service programs (McGovern, Lambert-
Harris, Gotham, Claus, & Xie, 2014) found only 18
percent of addiction programs and 9 percent
of mental health services programs were rated
as COD “capable” (in terms of their capacity to
adequately deliver COD services).
The types of assessment and pretreatment
services at SUD treatment facilities varied
in 2018 (SAMHSA, 2019a), with 96 percent
providing screening for substance misuse, 93
percent providing comprehensive substance
misuse assessment or SUD diagnosis, 75 percent
screening for mental disorders, and 53 percent
providing comprehensive psychiatric assessment or
diagnosis.
4. Complications of CODs
CODs can complicate treatment and, if poorly
managed, can hinder recovery. Further, rates of
mental disorders appear to increase as the number
of SUDs increases, meaning people with polysub-
stance use are especially vulnerable to CODs.
Epidemiologists have observed increasing rates
of SUD treatment admissions among people with
multiple SUDs. Analyses of TEDS data (SAMHSA,
CBHSQ, 2019) reveal that in 2017, more than 25
percent of people ages 12 and older admitted for
SUD treatment reported both alcohol and other
substance misuse. This could partially account for
the increase in clients with CODs in SUD treatment
settings, as it appears that having multiple mental
disorders increases the odds of having multiple
SUDs or vice versa. In the NESARC-III (McCabe,
West, Jutkiewicz, & Boyd, 2017), people with
one lifetime mental disorder had more than three
times the odds of having multiple past-year SUDs
compared with people with no lifetime mental
disorders. But people with multiple mental
disorders (particularly mood disorders, PDs, and
PTSD) are nearly nine times more likely to have
multiple past-year SUDs. Individuals with multiple
previous SUDs were also less likely to experience
remission from substance misuse than were people
with a single SUD.
SUD treatment facilities are increasingly seeing
nonalcohol substances as the primary substance
of misuse among people entering treatment.
For instance, from 2005 to 2015, the proportion
of alcohol admissions decreased from about 40
percent to 34 percent and opiate admissions
increased from 18 percent to 34 percent (with
opiates other than heroin increasing from 4 percent
to 8 percent) (SAMHSA, 2017). This and the trend
of increased polysubstance misuse are worrisome,
as NESARC-III data clearly demonstrate both
drug use disorders and AUD each independently
confer an exaggerated risk of co-occurring mental
disorders (Grant et al., 2015; Grant et al., 2016).
CODs can be an obstacle to addiction recovery,
especially when untreated. Data from the 2009
to 2011 TEDS-Discharges show that, of people
admitted to SUD treatment, 28 percent had a
co-occurring psychiatric condition (Krawczyk et
Chapter 1 10

TIP 42
Chapter 1—Introduction to SUD Treatment for People With Co-Occurring Disorders
al., 2017). Prevalence rates of CODs varied across
individual states and ranged from 8 percent to 62
percent. People with a psychiatric comorbidity
were significantly more likely than those without
a psychiatric comorbidity to report using three
or more substances (27 percent vs. 17 percent).
Of people who did not complete treatment, 42
percent had a COD, versus 36 percent without.
This translated to about a 1.3 increase in odds of
not completing treatment and a 1.1 increase in
odds of earlier time to attrition for people with
CODs compared with those with an SUD only.
CODs are strongly associated with socioeconom-
ic and health factors that can challenge recovery,
such as unemployment, homelessness, incarcer-
ation/criminal justice system involvement, and
suicide.
•
According to SAMHSA’s Mental Health Annual
Report, in 2017, 29 percent of people with
CODs were unemployed and 50 percent
were not in the labor force (e.g., disabled,
retired, student) (SAMHSA, 2019d). The current
national unemployment rate at the time of this
publication is 3.8 percent (Bureau of Labor
Statistics, March 3, 2020).
•
Of people 12 and older with CODs, 7.5
percent experience homelessness, including
8.3 percent of people with an SUD and
schizophrenia or other psychotic disorder, 6.9
percent with an SUD and bipolar disorders,
and 7.8 percent with an SUD and depressive
disorders (SAMHSA, 2019d). Rates of lifetime
and past-year homelessness in the general
community per NESARC-III (Tsai, 2018) are
about 4 percent and 1.5 percent, respectively.
The 2017 Annual Homeless Assessment Report
to Congress (Henry, Watt, Rosenthal, & Shivji,
2017) found that almost 23 percent of adults in
permanent supportive housing programs had
transferred from an SUD treatment center; 15
percent, from a mental health services facility.
Furthermore, of the 552,830 total individuals
experiencing homelessness, about 20 percent
(111,122) had an SMI and about 16 percent
(86,647) had a chronic SUD (U.S. Department of
Housing and Urban Development, 2018).
•
Of people incarcerated in U.S. state prisons
(Al-Rousan, Rubenstein, Sieleni, Deol, &
Wallace, 2017), about 48 percent have a history
of mental illness (of whom 29 percent had an
SMI), 26 percent, a history of an SUD. Of those
with mental illness, 49 percent also have a co-
occurring SUD.
•
Mental disorders that commonly co-occur
with SUDs—including depression, anxiety
disorders, bipolar disorders, schizophrenia,
and PTSD—are highly prevalent in people who
have completed suicide, (Stone, Chen, Daumit,
Linden, & McGinty, 2019). Suicide is also a
well-known risk factor in SUDs and a leading
cause of death for people with addiction (Center
for Substance Abuse Treatment, 2009; Yuodelis-
Flores & Ries, 2015). In CDC’s National Vital
Statistics System dataset (Stone et al., 2019),
46 percent of all individuals in the United States
who died by suicide between 2014 and 2016
had a known mental condition, and 28 percent
misused substances, and of this 28 percent
almost one-third (32 percent) also had a known
mental health condition.
These figures reflect the need for specifically
tailored COD assessments, interventions, treatment
approaches, and clinical considerations (e.g.,
COD programming specific to people without
stable housing; COD interventions designed for
implementation in criminal justice settings). More
information about how these variables factor into
service provision and outcomes can be found in
Chapters 4 and 6.
The Complex, Unstable, and
Bidirectional Nature of CODs
Counselors working with clients who have CODs
often want to know which disorder developed
first. The answer is not always clear because the
temporal nature of CODs can be inconsistent and
nuanced. In some cases, a mental disorder may
obviously have led to the development of an SUD.
An example would be someone with long-standing
major depressive disorder who starts using alcohol
excessively to cope and develops AUD. In other
instances, substance use clearly precipitated the
mental disorder—such as when someone develops
a cocaine-induced psychotic disorder. In many cases,
it will be uncertain which disorder occurred first.
Chapter 1 11
TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
Furthermore, CODs can be bidirectional. For
some clients, there may be a third condition that
is influencing both or either of the two comorbid
disorders (e.g., HIV, chronic pain). Environmental
factors, like homelessness or extreme stress, can
also affect one or both disorders. Thus, even when
it is clear which disorder developed first, the causal
relationship may be unknown. Regardless of the
temporal-causal relationship between a client’s SUD
and mental illness, the two are likely to affect, and
possibly exacerbate, one another. This means that
both need to be treated with equal seriousness.
In addition to inducing a mental disorder,
substance misuse can sometimes mimic
a mental disorder. Thus, it is important to
use thorough screening and assessment
approaches to help disentangle all symptoms
and make an accurate diagnosis. Learn more
about screening and assessment for CODs in
Chapter 3.
CODs are not necessarily equal in severity.
Often, one disorder is more severe, distressing,
or impairing than the other. Recognizing this is
important for treatment planning and requires
a person-centered rather than cookie-cutter
approach to determining diagnosis, comorbidities,
functioning, treatment and referral needs, and
stage of change. Models are available to help
counselors make such decisions based on the
severity and impact of each disorder. For instance,
the Four Quadrants Model (National Association of
State Mental Health Program Directors & National
Association of State Alcohol and Drug Abuse
Directors, 1999) classifies clients in four basic
groups based on relative symptom severity, not
diagnosis:
•
Category I: Less severe mental disorder/less
severe substance disorder
•
Category II: More severe mental disorder/less
severe substance disorder
•
Category III: Less severe mental disorder/more
severe substance disorder
•
Category IV: More severe mental disorder/more
severe substance disorder
For a more detailed description of this model, see
Chapter 2. To learn how to integrate the quadrants
of care framework into assessment and treatment
decision-making processes, see Chapter 3.
SUDs, Mental Illness, and “Self-
Medicating”
The notion that SUDs are caused, in whole or
in part, by one’s attempts to “self-medicate”
symptoms with alcohol or illicit drugs has been a
source of debate. The consensus panel cautions
that the term “self-medication” should not be
used, as it equates drugs of misuse (which usually
worsen health) with true medications (which are
designed to improve health). Although some
people with mental conditions may misuse
substances to alleviate their symptoms or
otherwise cope (Sarvet et al., 2018; Simpson,
Stappenbeck, Luterek, Lehavot, & Kaysen, 2014),
this is not always the case. Counselors should not
assume self-medication is the causal link between a
client’s mental disorder and SUD.
Conclusion
The COD recovery trajectory often has pitfalls,
but our understanding of CODs and COD-specific
service delivery has improved over the past 20
years. Despite these advances, significant gaps
remain in the accurate and timely assessment,
diagnosis, and treatment of people with CODs.
To achieve lower cost mental health services and
SUD treatment, better client outcomes, and a
more positive treatment experience, providers and
administrators must collectively place more focus
on CODs in their work. By better understanding
the risks and responding to the service needs
of people with CODs, behavioral health service
providers can help make long-term recovery an
attainable goal for all clients with CODs.
Chapter 1 12

Chapter 2— Guiding Principles for Working
With People Who Have Co-Occurring Disorders
KEY MESSAGES
TIP 42
SUBSTANCE USE DISORDER TREATMENT FOR
PEOPLE WITH CO-OCCURRING DISORDERS
• General guiding principles of good care for
people with co-occurring disorders (CODs)
ensure that counselors and other providers,
administrators, and supervisors fully meet
clients’ comprehensive needs—effectively and
ethically.
• Counselors should offer clients full access to
a range of integrated services through the
continuum of recovery.
• Administrators and supervisors are responsible
for the training, professional development,
recruitment, and retention of qualified
counselors and other professional staff
working with people who have CODs. Failure
to attend to these workforce matters will only
further inhibit client access to care.
• Several core essential services exist for clients
with comorbid conditions, and supervisors
and administrators should regularly evaluate
their program’s capacity and performance to
monitor its effectiveness in providing these
services and correct course when needed.
Many treatment providers and agencies recognize
the need to provide quality care to people
with CODs but see it as a daunting challenge
beyond their resources. Programs that already
have incorporated some elements of integrated
services and want to do more may lack a clear
framework for determining priorities. Addiction
counselors might recognize the need to be able
to effectively treat clients with CODs but not fully
understand the best approaches to doing so. As
counselors and programs look to improve their
effectiveness in treating this population, what
should they consider? How could the experience of
other agencies or counselors inform their planning
process? Are resources available that could help
turn such a vision into reality? This chapter is
designed to help both providers and agencies
that want to improve services for their clients with
CODs, whether that means establishing services
where there currently are none or learning to
improve existing ones.
The chapter is designed for counselors, other
treatment/service providers, supervisors, and
administrators and begins with a review of general
guiding principles derived from proven models,
clinical experience, and the growing base of
empirical evidence. Building on these guiding
principles, the chapter turns to the specific core
components for effective service delivery for
addiction counselors and other providers and for
administrators and supervisors, respectively. For
providers, this includes addressing in concrete
terms the challenges of providing access,
screening and assessment, appropriate level
of care, integrated treatment, comprehensive
services, and continuity of care. For supervisors and
administrators, effective service delivery requires
staff to develop essential core competencies
and take advantage of opportunities for
professional development. Achieving optimal
COD programming means integrating research
into clinical services to ensure that practices are
evidence based, establishing essential services
to meet the varied needs of people with CODs,
and conducting program assessments to gauge
whether services adequately fulfill clients’ access
and treatment needs.
13
TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
General Guiding Principles
The consensus panel developed a list of guiding
principles to serve as fundamental building blocks
for working with clients who have CODs (Exhibit
2.1). These principles are derived from a variety
of sources: conceptual writings, well-articulated
program models, a growing understanding of the
essential features of CODs, elements common to
separate treatment models, clinical experience, and
available empirical evidence. These principles may
be applied at both a program level (e.g., providing
literature for people with cognitive impairments) or
at the individual level (e.g., addressing the client’s
basic needs).
Exhibit 2.1. Six Guiding Principles
in Treating Clients With CODs
1. Use a recovery perspective.
2. Adopt a multiproblem viewpoint.
3. Develop a phased approach to treatment.
4. Address specific real-life problems early in
treatment.
5. Plan for the client’s cognitive and functional
impairments.
6. Use support systems to maintain and extend
treatment effectiveness.
The following section discusses the six principles
and the related field experience underlying each
one.
Use a Recovery Perspective
The recovery perspective has two main features: It
acknowledges that recovery is a long-term process
of internal change, and it recognizes that these
internal changes proceed through various stages.
(See De Leon [1996] and Prochaska, DiClemente, &
Norcross [1992] for a detailed description. Also see
Chapter 5 of this Treatment Improvement Protocol
(TIP) for a discussion of the recovery perspective as
a guideline for establishing therapeutic alliance.)
The recovery perspective applies to clients with
CODs and generates two main practice principles:
•
Develop a treatment plan that provides for
continuity of care over time. In preparing
this plan, the provider should recognize that
treatment may occur in different settings over
time (e.g., residential, outpatient) and that
much of the recovery process typically occurs
outside of or following treatment (e.g., through
participation in mutual-support programs,
through family, peer, and community support,
including the faith community). The provider
needs to reinforce long-term participation in
these continuous care settings.
•
Devise treatment interventions that are specific
to the tasks and challenges faced at each
stage of the COD recovery process. Whether
within the substance use disorder (SUD)
treatment or mental health services system, the
provider is advised to use sensible stepwise
approaches in developing and using treatment
protocols. In addition, markers that are unique
to individuals—such as those related to their
cultural, social, or spiritual context—should be
considered. The provider needs to engage the
client in defining markers of progress that are
meaningful to him or her and to each stage of
recovery.
Adopt a Multiproblem Viewpoint
People with CODs generally have an array of
mental, medical, substance use, family, and social
problems. Most need substantial rehabilitation
and habilitation (i.e., initial learning and acquisition
of skills). Treatment should address immediate
and long-term needs for housing, work, health
care, and a supportive network. Therefore,
services should be comprehensive to meet the
multidimensional problems typically presented by
clients with CODs.
Develop a Phased Approach to Treatment
Using a staged or phased approach to
COD treatment helps counselors optimize
comprehensive, appropriate, and effective care for
all client needs. Generally, three to five phases are
identified, including engagement, stabilization/
persuasion, active treatment, and continuing care
Chapter 2 14

TIP 42
Chapter 2—Guiding Principles for Working With People Who Have CODs
or continuing care/relapse prevention (Mueser &
Gingerich, 2013; Substance Abuse and Mental
Health Services Administration [SAMHSA], 2009a).
These phases are consistent with, and parallel to,
stages identified in the recovery perspective. The
use of these phases enables the provider (whether
within the SUD treatment or mental health
services system) to develop and use effective,
stage-appropriate treatment protocols. (See the
revised TIP 35, Enhancing Motivation for Change
in Substance Use Disorder Treatment [SAMHSA,
2019c]).
Address Specic Real-Life Problems Early
in Treatment
Growing recognition that CODs arise in a context
of personal and social problems, with disruption of
personal and social life, has prompted approaches
that address specific life problems early in
treatment. These approaches may incorporate
case management and intensive case management
to help clients surmount bureaucratic hurdles
or handle legal and family matters. Specialized
interventions that target important areas of client
need, such as housing-related support services
(Clark, Guenther, & Mitchell, 2016), can also
help. Vocational services help clients with CODs
make concrete improvements in career goal
setting, job seeking, work attainment, and earned
wages (Luciano & Carpenter-Song, 2014; Mueser,
Campbell, & Drake, 2011).
For people in recovery from mental disorders
or SUDs, workforce participation is not only
valuable because of its economic contributions; it
can also enhance individual self-efficacy, improve
self-identity (e.g., help people feel “normal”
as opposed to “like a patient”), offer a sense of
belonging with society at large, provide a way
for people to build relationships with others, and
improve quality of life (Charzynska, Kucharska, &
Mortimer, 2015; Walsh & Tickle, 2013). A review of
the effects of employment interventions for people
with SUDs found that employment was associated
with reduced substance use and more stable
housing (Walton & Hall, 2016).
Solving financial, housing, occupational, and other
problems of everyday living is often an important
first step toward achieving client engagement in
continuing treatment. Engagement is a critical part
of SUD treatment generally and of treatment for
CODs specifically, because remaining in treatment
for an adequate length of time is essential to
achieving behavioral change.
Plan for Clients’ Cognitive and Functional
Impairments
Services for clients with CODs, especially those
with more serious mental disorders, must be
tailored to individual needs and functioning.
Clients with CODs often display cognitive and
other functional impairments that affect their ability
to comprehend information or complete tasks
(Duijkers, Vissers, & Egger, 2016). The manner
in which interventions are presented must be
compatible with client needs and functioning.
Such impairments frequently call for relatively
short, highly structured treatment sessions that
are focused on practical life problems. Gradual
pacing, visual aids, and repetition are often helpful.
Even impairments that are comparatively subtle
(e.g., certain learning disabilities) may still have
significant impact on treatment success. Careful
assessment of such impairments and a treatment
plan consistent with the assessment are therefore
essential.
Use Support Systems To Maintain and
Extend Treatment Eectiveness
The mutual-support movement, the family, peer
providers, the faith community, and other resources
that exist within the client’s community can play an
invaluable role in recovery. This can be particularly
true for clients with CODs, many of whom have not
enjoyed a consistently supportive environment for
decades. In some cultures, the stigma surrounding
SUDs or mental disorders is so great that the client
and even the entire family may be ostracized by
the immediate community. For instance, some
mutual- support programs are not very accepting
of members with CODs who take psychiatric
medication. Furthermore, the behaviors associated
with active substance use may have alienated the
client’s family and community. The provider plays a
role in ensuring that the client is aware of available
support systems and motivated to use them
effectively.
Chapter 2 15

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
Mutual Support
Based on the Alcoholics Anonymous (AA) model,
the mutual-support movement has grown to
encompass a wide variety of addictions. AA and
Narcotics Anonymous are two of the largest
mutual-support organizations for SUDs; Dual
Recovery Anonymous is most known for CODs.
Personal responsibility, self-management, and
helping one another are the basic tenets of mutual-
support approaches. Such programs apply a broad
spectrum of personal responsibility and peer
support principles. However, in the past, clients
with CODs felt that either their mental or their
substance use problems could not be addressed in
a single-themed mutual-support program. That has
changed.
Mutual-support principles, highly valued in the
SUD treatment field, are now widely recognized
as important components in the treatment of
CODs. Mutual support can be used as an adjunct
to primary treatment, as a continuing feature
of treatment in the community, or both. These
programs not only provide a vital means of support
during outpatient treatment but also are commonly
used in residential programs such as therapeutic
communities (TCs). As clients gain employment,
travel, or relocate, mutual support can become
the most easily accessible means of providing
continuity of care. For a more extensive discussion
of dual recovery mutual-support programs
applicable to people with CODs, including those
structured around peer-recovery support services,
see Chapter 7.
Building Community
The need to build an enduring community arises
from three interrelated factors: the persistent
nature of CODs, the recognized effectiveness of
mutual-support principles, and the importance of
client empowerment. The TC, modified mutual
programs for CODs (e.g., Double Trouble in
Recovery), and the client consumer movement
all reflect an understanding of the critical role
clients play in their own recovery, as well as the
recognition that support from other clients with
similar problems promotes and sustains change.
Reintegration With Family and Community
The client with CODs who successfully completes
treatment must face the fragility of recovery,
the potential toxicity of the past or current
environment, and the negative impact of previous
associates who might encourage substance use
and illicit or maladaptive behaviors. Groups and
activities that support change are needed. In
this context, clients should receive support from
family and significant others where that support is
available or can be developed. Clients also need
help reintegrating into the community through
such resources as spiritual, recreational, and social
organizations.
Peer-Based Services
Peer recovery support services typically refers
to services provided by people with a lived
experience with substance misuse, mental
disorders, or both (or, in the case of family peer
services, people who have a lived experience
of having a loved one with substance misuse,
mental disorders, or both). Peer recovery support
specialists are nonclinical professionals who help
individuals both initiate and maintain long-term
recovery by offering support, education, and
linkage to resources. Peers also serve as role
models for successful recovery and healthy living.
For more information on peer recovery support
services for CODs and the potential role of peer
recovery support specialists in promoting and
maintaining recovery, see Chapter 7.
Guidelines for Counselors and
Other Providers
The general guiding principles described previ-
ously serve as the fundamental building blocks
for effective treatment, but ensuring effective
treatment requires counselors and other providers
to attend to other variables. This section discusses
six core components that form the ideal delivery
of addiction counseling services for clients with
CODs. These are:
1. Providing access.
2. Completing a full assessment.
Chapter 2 16

TIP 42
Chapter 2—Guiding Principles for Working With People Who Have CODs
3. Providing an appropriate level of care.
4. Achieving integrated treatment.
5. Providing comprehensive services.
6. Ensuring continuity of care.
Providing Access
“Access” refers to the process by which a person
with CODs makes initial contact with the service
system, receives an initial evaluation, and is
welcomed into services that are appropriate for his
or her needs. There are four main types of access:
1. Routine access for individuals seeking services
who are not in crisis
2. Crisis access for individuals requiring immediate
services because of an emergency
3. Outreach, in which agencies target individuals
in great need (e.g., people experiencing
homelessness) who are not seeking services or
cannot access ordinary or crisis services
4. Access that is involuntary, coerced, or mandated
by the criminal justice system, employers, or the
child welfare system
Treatment access may be complicated by clients’
criminal justice involvement, homelessness, or
health status. A “no wrong door” policy should be
applied to the full range of clients with CODs, and
counselors (as well as programs) should address
obstacles that bar entry to treatment for those with
either a mental disorder or an SUD. (See Chapter 7
for recommendations on removing systemic barriers
to care and Exhibit 2.2 for more on the “no wrong
door” approach to behavioral health services.)
Exhibit 2.2. Making “No Wrong Door” a Reality
The consensus panel strongly endorses a “no wrong door” policy: effective systems must ensure that an
individual needing treatment will be identified and assessed and will receive treatment, either directly
or through appropriate referral, no matter where he or she enters the realm of services (Center for
Substance Abuse Treatment [CSAT], 2000a).
The focus of the “no wrong door” imperative is on constructing the healthcare delivery system so
that treatment access is available at any point of entry. A client with CODs needing treatment might
enter the service system by means of a primary care facility, homeless shelter, social service agency,
emergency room, or criminal justice setting. Some clients require creation of a “right door” to enter
treatment. For example, mobile outreach teams can access clients with CODs who are otherwise
unlikely to seek treatment on their own.
The “no wrong door” approach has five major implications for service planning:
1. Assessment, referral, and treatment planning across settings is consistent with a “no wrong door”
policy.
2. Creative outreach strategies are available to encourage people to engage in treatment.
3. Programs and staff can change expectations and program requirements to engage reluctant and
“unmotivated” clients.
4. Treatment plans are based on clients’ needs and respond to changes as they progress through
stages of treatment.
5. The overall system of care is seamless, providing continuity of care across service systems. This is
only possible via established patterns of interagency cooperation or clear willingness to attain that
cooperation.
Source: CSAT (2000a).
Chapter 2 17

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
Completing a Full Assessment
Whereas Chapter 3 provides a complete de-
scription of the assessment process, this section
highlights several important features of assessment
that support effective service delivery. Assessment
of individuals with CODs involves a combination of:
•
Screening to detect the presence of CODs
in the setting where the client is first seen for
treatment.
•
Evaluating background factors (e.g., family
history, trauma history, marital status, health,
education, work history), mental disorders,
SUDs, and related medical and psychosocial
problems (e.g., living circumstances,
employment) that are critical to address in
treatment planning.
•
Diagnosing the type and severity of SUDs and
mental disorders.
•
Initial matching of individual client to
services. (Often, this must be done before a
full assessment is completed and diagnoses
clarified. Also, the client’s motivation to change
with regard to one or more of the CODs may
not be well established.)
•
Appraising existing social and community
support systems.
•
Conducting continuous evaluation (that is,
reevaluating over time as needs and symptoms
change and as more information becomes
available).
The challenge of assessment for individuals
with CODs in any system involves maximizing
the likelihood of the identification of CODs,
immediately facilitating accurate treatment
planning, and revising treatment over time as the
client’s needs change.
Providing an Appropriate Level of Care
Clients enter the treatment system at various levels
of need and encounter agencies with varying
capacity to meet those needs. Ideally, clients
should be placed in the level of care appropriate
to the severity of both their SUD and their mental
illness.
The American Association of Community
Psychiatry’s Level of Care Utilization System
(LOCUS) is one standard way of identifying
appropriate levels of care and service intensity. The
LOCUS describes six levels of care sequentially
increasing in intensity, based on the client’s
individually assessed needs across six dimensions.
Further, a treatment program’s ability to address
CODs as “addiction-only services,” “dual diagnosis
capable,” and “dual diagnosis enhanced” is
another useful perspective in care determination
and decision making (Chapter 3 discusses
frameworks to help with treatment placement).
Severity and Levels of Care
Models are available to help counselors make
treatment and referral decisions based on the
severity and impact of each disorder. For instance,
the quadrants of care (also called the Four
Quadrants Model) is a conceptual framework that
classifies clients in four basic groups based on
relative symptom severity, not diagnosis (Exhibit
2.3). The quadrants of care were derived from
a conference, the National Dialogue on Co-
Occurring Mental Health and Substance Abuse
Disorders, which was supported by SAMHSA
and two of its centers—CSAT and the Center for
Mental Health Services—and co-sponsored by
the National Association of State Mental Health
Program Directors and the National Association
of State Alcohol and Drug Abuse Directors. The
quadrants of care is a model originally developed
by Ries (1993).
EXHIBIT 2.3. The Four Quadrants Model
III—Less severe mental disorder/more severe SUD IV—More severe mental disorder/more severe SUD
I—Less severe mental disorder/less severe SUD II—More severe mental disorder/less severe SUD
Chapter 2 18

TIP 42
Chapter 2—Guiding Principles for Working With People Who Have CODs
Chapter 3 offers more detail about the four
quadrants and their use in comprehensive
assessment.
Achieving Integrated Treatment
The seminal concept of integrated treatment for
people with severe mental disorders and SUDs,
as articulated by Minkoff (1989), emphasized the
need for correlation between the treatment models
for mental health services and SUD treatment in
a residential setting. Minkoff’s model stressed the
importance of well-coordinated, stage-specific
treatment (i.e., engagement, primary treatment,
continuing care) of SUDs and mental disorders,
with emphasis on dual recovery goals as well as
the use of effective treatment strategies from the
mental health and SUD treatment fields.
During the last decade, integrated treatment
continued to evolve. Several models have shown
success in community addiction treatment and
mental health service programs (Chow, Wieman,
Cichocki, Qvicklund, & Hiersteiner, 2013; Kelly &
Daley, 2013; McGovern et al., 2014), including
programs in which COD services were combined
with supportive housing services (Pringle, Grasso,
& Lederer, 2017); programs serving people in
the criminal justice system (Peters, Young, Rojas,
& Gorey, 2017); programs in outpatient and
residential settings (Hunt, Siegfried, Morley,
Sitharthan, & Cleary, 2014; Morse & Bride, 2017);
TCs (Dye, Roman, Knudsen, & Johnson, 2012); and
opioid treatment programs (Brooner et al., 2013;
Kidorf et al., 2013).
The literature from the addiction and mental health
fields has evolved to describe integrated treatment
as a unified treatment approach to meet clients’
addiction, mental disorder, and related needs
(Exhibit 2.4). It is the preferred model of treatment.
Chapter 7 further discusses integrated treatment
models.
Exhibit 2.4. SAMHSA Practice
Principles of Integrated
Treatment for CODs
•
Mental illness and SUDs are both treated
concurrently to meet the full range of clients’
symptoms equally.
•
Providers of integrated care receive training
in the treatment of both SUDs and mental
disorders.
•
CODs are treated with a stage-wise approach
that is tailored to the client’s stage of readiness
for treatment (e.g., engagement, persuasion,
active treatment, relapse prevention).
•
Motivational techniques (e.g., motivational
interviewing [MI], motivational counseling) are
integrated into care to help clients reach their
goals—and particularly at the engagement
stage of treatment.
•
Addiction counseling is used to help clients
develop healthier, more adaptive thoughts and
behaviors in support of long-term recovery.
•
Clients are offered multiple treatment formats,
including individual, group, family, and peer
support, as they move through the various
stages of treatment.
•
Pharmacotherapy is discussed in
multidisciplinary teams, offered to clients as
appropriate, and monitored for safety (e.g.,
interactions), adherence, and response.
Source: SAMHSA (2009a).
Providing Comprehensive Services
People with CODs have a range of medical and
social problems—multidimensional problems
that require comprehensive services. In addition
to treatment for SUDs and mental disorders,
these clients often require various other services
to address social problems and stabilize living
conditions. Treatment providers should prepare
to help clients access an array of services,
including life skills development, English as
a second language, parenting, nutrition, and
employment assistance. Two areas of particular
value are housing and work. (See Chapter 6 for a
Chapter 2 19

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
discussion about people with CODs experiencing
homelessness and Chapter 7 for further information
about vocational services as a part of treatment.)
Ensuring Continuity of Care
Continuity of care implies coordination of care as
clients move across different service systems (Puntis,
Rugkåsa, Forrest, Mitchell, & Burns, 2015; Weaver,
Coffey, & Hewitt, 2017). Both SUDs and mental
disorders frequently are long-term conditions, so
treatment for people with CODs should take into
consideration rehabilitation and recovery over a
significant period of time. Therefore, to be effective,
treatment must address the three features that
characterize continuity of care:
•
Consistency between primary treatment and
ancillary services
•
Seamlessness as clients move across levels of care
(e.g., from residential to outpatient treatment)
•
Coordination of present and past treatment
episodes (i.e., making sure you are aware of
previous treatments given, how the client
responded, and the client’s treatment preferences)
It is important to set up systems that prevent gaps
between service system levels and between clinic-
based services and those outside the clinic. The ideal
is to include outreach, employment, housing, health
care and medication, financial supports, recreational
activities, and social networks in a comprehensive and
integrated service delivery system.
Continuity of Care and Outpatient Treatment
Settings
Continuing care and relapse prevention are
especially important with this population given
that mental disorders are often cyclical, recurring
illnesses and substance misuse is likewise a
chronic condition subject to periods of relapse
and remission. Clients with CODs often require
long-term continuity of care that supports their
progress, monitors their condition, and can
respond to a return to substance use or a return
of symptoms of mental disorder. Continuing care
is both a process of posttreatment monitoring and
a form of treatment itself. (In the present context,
the term “continuing care” is used to describe the
treatment options available to a client after leaving
one program for another, less intense, program.)
The relative seriousness of a client’s mental disorders
and SUDs may be very different at the time he
or she leaves a primary treatment provider; thus,
different levels of intervention will be appropriate.
After leaving an outpatient program, some clients
with CODs may need to continue intensive mental
health services but can manage their SUD through
mutual-support group participation. Others may need
minimal mental health services but require continued
formal SUD treatment. For people with serious
mental illness (SMI), continued treatment often is
warranted. A treatment program can provide these
clients with structure and varied services not usually
available from mutual support-groups.
Encourage clients with CODs who leave a program
to return if they need assistance with either
disorder. The status of these individuals can be
fragile; they need quick access to help in times of
crisis. Regular informal check-ins with clients also
can help alleviate potential problems before they
become serious enough to threaten recovery. A
good continuing care plan will include steps for
when and how to reconnect with services. The
plan and provision of these services also makes
readmission easier for clients with CODs who need
to come back. Clients with CODs should maintain
contact postdischarge (even if only by telephone
or informal gatherings). Increasingly, addiction
programs are using follow-up contacts and periodic
group meetings to monitor client progress and
assess the need for further service.
Continuity of Care and Residential Treatment
Settings
Returning to life in the community after residential
placement is a major undertaking for clients with
CODs, with relapse an ever-present risk. The goals
of continuing care programming are:
•
Sustaining abstinence.
•
Continuing recovery.
•
Mastering community living.
•
Developing vocational skills.
•
Obtaining gainful employment.
•
Deepening psychological understanding.
•
Assuming increasing responsibility.
•
Resolving family difficulties.
•
Consolidating changes in values and identity.
Chapter 2 20

TIP 42
Chapter 2—Guiding Principles for Working With People Who Have CODs
The key services are life skills education, relapse
prevention, mutual-support programs, case
management (especially for housing), and
vocational training and employment.
Empirical Evidence Related to Continuity of
Care
A systematic review (McCallum, Mikocka-Walus,
Turnbull, & Andrews, 2015) investigating the effects
of continuity of care on treatment outcomes for
people with CODs showed mixed results. Putting
in place continuity of care has generally involved
linking clients from one level of care to another
and providing multidimensional services. Positive
associations reported by some studies included
better treatment commitment, reduced violent
behavior, improved service satisfaction, better
generic and disease-specific quality of life, and
enhanced community functioning. However, there
was no consistent evidence that continuity of care
was associated with abstinence.
The belief that continuous care benefits people
with CODs is also informed by positive research
findings on continuity of care for addiction
populations and SMI populations separately. A
meta-analysis of studies exploring continuing care
among people with substance misuse found a small
but positive effect on substance-related outcomes
(Blodgett, Maisel, Fuh, Wilbourne, & Finney,
2014). Continuity of care following residential
detoxification is associated with decreased rates
of readmission for detoxification (Lee et al., 2014).
More recently, a continuing care intervention for
people in the first year of SUD recovery (McKay,
Knepper, Deneke, O’Reilly, & DuPont, 2016)
found a 70-percent adherence rate over 1 year
for providing urine samples and a mere 4-percent
positive urine sample rate (for drugs or alcohol).
A review of international studies examining
continuity of care and patient outcomes in mental
health found wide variability in the research
methodology and outcomes (Puntis et al., 2015). In
studies conducted in the United States, continuity
of care (in some but not all of the U.S. studies)
was associated with reduced psychiatric symptom
severity, lower risk of rehospitalization, improved
functioning, reduced Medicaid expenditures, and
fewer violent behaviors.
Guidelines for Administrators and
Supervisors
This section focuses on some key matters ad-
ministrators and supervisors face in developing a
workforce able to meet the needs of clients with
CODs. Guidelines to address these core topics
include:
1. Identifying and providing to counselors the
essential competencies (basic, intermediate, and
advanced), values, and attitudes to be successful
in COD service delivery.
2. Offering opportunities for professional
development, including staff training and
education.
3. Using effective burnout and turnover reduction
techniques, as these are common problems for
any SUD treatment provider, but particularly so
for those who work with clients who have CODs.
Critical challenges face SUD treatment systems and
programs that aim to improve care for clients with
CODs. This section addresses these challenges by
discussing how supervisors and administrators can
foster more effective COD programming, such as:
1. Integrating research and practice into
programming.
2. Establishing essential services for people with
CODs.
3. Assessing agency potential to serve clients
with CODs via adequate and responsive
programming.
This section only briefly addresses guidelines for
administrators and supervisors. More detailed
discussions about workforce improvement and
administrative matters, including descriptions of
provider competencies, supervision, staff training,
hiring, turnover, and retention, are in Chapter 8.
Providers’ Competencies
Provider competencies are measurable skills and
specific attitudes and values counselors should
learn and develop. Attitudes and values guide
how providers meet client needs and affect overall
treatment climate. They are particularly important
in working with clients who have CODs because
Chapter 2 21

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
the counselor is confronted with two disorders that
require complex interventions. Essential values
and attitudes that inform effective care for clients
with CODs include a desire and willingness to
work with populations with CODs, an appreciation
for the complexity of CODs, and an awareness of
one’s own personal feelings about and reactions to
working with people who have CODs. These are
discussed primarily in Chapter 8.
Basic competencies are rudimentary, introductory
skills all counselors should possess, such as:
•
Performing a basic screening and assessment
to determine whether CODs might exist and, if
needed, referring for more thorough and formal
diagnostic testing.
•
Conducting a preliminary screening to
determine whether a client poses an immediate
danger to self or others and coordinating any
subsequent assessment with appropriate staff or
consultants.
•
Referring a client to the appropriate mental
health services or SUD treatment and following
up to ensure that the client receives needed
care.
•
Coordinating care with a mental health
counselor serving the same client to ensure
that the interaction of the client’s disorders is
well understood and that treatment plans are
coordinated.
Intermediate competencies encompass skills
such as:
•
Performing more indepth screening.
•
Treatment planning.
•
Discharge planning.
•
Linking clients to other mental health system
services.
Advanced competencies go beyond an awareness
of the addiction and mental health fields as individ-
ual disciplines to a more sophisticated appreciation
for how CODs interact in an individual. This can
include:
•
Understanding the effects of level of functioning
and degree of disability related to both
substance-related and mental disorders,
separately and combined.
•
Using integrated models of assessment,
intervention, and recovery for people with both
substance-related and mental disorders, as
opposed to parallel treatment efforts that resist
integration.
•
Collaboratively developing and implementing
an integrated treatment plan based on thorough
assessment that addresses both/all disorders
and establishes sequenced goals based on
urgent needs, considering the stage of recovery
and level of engagement.
•
Involving the person, family members, and
other supports and service providers (including
peer supports and those in the natural support
system) in establishing, monitoring, and refining
the treatment plan.
Continuing Professional Development
Given the complexity of CODs and lagging
treatment rates, there is a pressing need for
professionals to develop the necessary skills
to accurately identify and manage these
conditions. This TIP makes an effort to integrate
available information on continuing professional
development. Counselors reading this TIP can
review their own knowledge and determine
what they need to continue their professional
development. More information can also be found
in Chapter 8.
Education and Training
Education and training are critical to ensuring
professional development and competency of
providers and should take place throughout the
continuum of one’s formal education and career.
Various forms of education and training are central
to evidence-based, high-quality care for people
with CODs:
•
Staff education and training are fundamental
to all SUD treatment programs. Few university-
based programs offer a formal curriculum on
CODs, although the past decade has seen some
improvement.
•
Many SUD treatment counselors learn through
continuing education and facility-sponsored
training. Continuing education is useful
because it can respond rapidly to the needs
of a workforce that has diverse educational
Chapter 2 22

TIP 42
Chapter 2—Guiding Principles for Working With People Who Have CODs
backgrounds and experience. To have practical
utility, competency training must address the day-
to-day concerns that counselors face in working
with clients who have CODs. The educational
context must be rich with information, culturally
sensitive, and designed for adult students, and
must include examples and role models. Ideally,
the instructors will have extensive experience as
practitioners in the field. Continuing education is
also essential for effective provision of services to
people with CODs, but it is not sufficient in and
of itself. Counselors must have ongoing support,
supervision, and opportunity to practice new
skills if they are to truly integrate COD content
into their practice.
•
Cross-training is simultaneous provision of
material and training in more than one discipline
(e.g., addiction and social work counselors,
addiction counselors and corrections officers).
Counselors with primary expertise in either
addiction or mental health can work far more
effectively with clients who have CODs if they
have some cross-training in the other field. The
consensus panel suggests that counselors of
either field receive at least basic level cross-
training in the other field to better assess, refer,
understand, and work effectively with the large
number of clients with CODs.
Program Orientation and Ongoing
Supervision
Staff education and training have two additional
components: (1) program orientation that clearly
presents the mission, values, and aims of service
delivery; and (2) strong, ongoing supervision. The
orientation can use evidence-based initiatives as
well as promising practices. Successful program
orientation for working with clients who have CODs
will equip staff members with skills and decision-
making tools that will enable them to provide
optimal services in real-world environments.
Skills best learned through direct supervision and
modeling include active listening, interviewing
techniques, the ability to summarize, and the
capacity to provide feedback. Strong, active
supervision of ongoing cases is a key element in
assisting staff to develop, maintain, and enhance
relational skills.
Avoiding Burnout and Reducing Sta
Turnover
Burnout
Assisting clients who have CODs is difficult and
emotionally taxing; the danger of burnout is
considerable. Among mental health and SUD
clinicians, the effects of working with clients with
trauma can lead to compassion fatigue, vicarious
traumatization, or secondary traumatic stress
(Huggard, Law, & Newcombe, 2017; Newell,
Nelson-Gardell, & MacNeil, 2016). If untreated,
these can have profound negative effects on a
clinician’s ability to function at work effectively, care
for clients, and care for oneself (Baum, 2016).
Program administrators must stay aware of burnout
and the benefits of reducing turnover. In order for
staff to sustain their morale and esprit de corps,
they need to feel that program administrators are
interested in their well-being. Most important,
supervision should be supportive, providing
guidance and technical knowledge. Programs can
proactively address burnout by placing high value
on staff well-being; routinely discussing well-being;
providing activities such as retreats, weekend
activities, yoga, and other healing activities at
the worksite; and creating a network of ongoing
support.
Turnover
The issue of staff turnover is especially important
for staff working with clients who have CODs
because of the limited workforce pool and the high
investment of time and effort involved in develop-
ing a trained workforce. Rapid turnover disrupts
the context in which recovery occurs. Clients in
such agencies may become discouraged about
the possibility of being helped by others. Ways to
reduce staff turnover in programs for clients with
CODs can include:
•
Hiring staff members familiar with both SUD and
mental disorders who have a positive regard for
clients with either or both disorders.
•
Ensuring that staff have realistic expectations for
the progress of clients with CODs.
•
Ensuring that supervisory staff members are
supportive and knowledgeable about problems
and concerns specific to clients with CODs.
Chapter 2 23

TIP 42
-
-
-
-
-
Substance Use Disorder Treatment for People With Co-Occurring Disorders
•
Providing and supporting opportunities for
further education and training.
•
Offering a desirable work environment through:
Adequate compensation.
Salary incentives for COD expertise.
Opportunities for training and for career
advancement.
Involvement in quality improvement or clinical
r
esear
ch activities.
Efforts to adjust workloads.
Integrating Research and Practice
To be effective, resources must be used to
implement the evidence-based practices most
appropriate to the client population and the
program needs. The importance of the transfer of
knowledge and technology has come to be well
understood. Conferences to explore “bridging the
gap” between research and field practice are now
common. Although not specific to CODs, these
efforts have clear implications for our attempts
to share knowledge of what is working for clients
with CODs. For instance, since 2007, the National
Institutes of Health has cosponsored the Annual
Conference on the Science of Dissemination and
Implementation in Health, designed to foster better
integration of healthcare research into practice
and policy. CODs have been an underrepresented
topic at these gatherings, but presentations on
implementation studies in addiction and in mental
health, separately, likely will still be informative for
enhancing the use and measurement of research-
based practices for CODs.
In the SUD treatment field, implementation
research has accelerated in response to evidence
suggesting that the uptake of empirical findings
into actual practice is lagging (McGovern,
Saunders, & Kim, 2013). This lag has persisted
despite the availability of research supporting
the efficacy and effectiveness of SUD treatment,
including pharmacotherapies and psychosocial
interventions. In mental health, significant efforts
over the previous two decades have led to
increased utilization of evidence-based practices
and program evaluation strategies to monitor
fidelity and outcomes (Stirman, Gutner, Langdon,
& Graham, 2016). But more research–practice
partnerships in mental health are needed,
because many clients still cannot access or do
not receive evidence-based care. Similarly, within
COD treatment settings, more work is needed to
provide research-based services that are feasible,
acceptable, effective, and sustainable. SAMHSA
(2009a) developed an evidence-based practice
toolkit to help SUD and mental disorder treatment
programs incorporate empirically supported
policies and practices into their organizations,
with the aim of giving clients the best chances at
achieving long-term abstinence by translating COD
knowledge into practice.
Establishing Essential Services for People
With CODs
Individuals with CODs are found in all SUD
treatment settings, at every level of care. Although
some of these individuals have SMI or disabilities,
many have disorders of mild to moderate severity.
As SUD treatment programs serve the increasing
number of clients with CODs, the essential
program elements required to meet their needs
must be defined clearly and set in place.
ADVICE TO ADMINISTRATORS: RECOMMENDATIONS FOR PROVIDING
ESSENTIAL SERVICES FOR PEOPLE WITH CODs
Develop a COD program with these components: 5. Relapse prevention
6.
Case management
1. Screening, assessment, and referral for people
with CODs
7.
COD-specific treatment components
2.
Physical and mental health consultation
8. Continuing care services
3.
Prescribing onsite psychiatrist
9.
Double Trouble groups (onsite)
4. Psychoeducational classes
10.
Dual recovery mutual-help groups (offsite)
Chapter 2 24

TIP 42Chapter 2—Guiding Principles for Working With People Who Have CODs
Program components described in this section
should inform any SUD treatment program seeking
to provide integrated addiction and mental health
services to clients with CODs. These elements
reflect a variety of strategies, approaches, and
models that the consensus panel discussed and
that often appear in current clinical programming.
The consensus panel believes these elements
constitute the best practices for designing COD
programs in SUD treatment agencies. What follows
are program considerations for implementing these
essential components. Information about designing
residential and outpatient treatment services can
be found in Chapter 7.
Screening, Assessment, and Referral for
People With CODs
All SUD treatment programs should have
appropriate procedures for screening, assessing,
and referring clients with CODs. Each provider
must be able to identify clients with both mental
disorders and SUDs and ensure their access to
the care needed for each disorder. For a detailed
discussion, see Chapter 3.
If the screening and assessment process establishes
an SUD or mental disorder beyond the capacity
and resources of the agency, referral should be
made to a suitable residential or mental health
facility, or other community resource. Mechanisms
for ongoing consultation and collaboration are
needed to ensure that the referral is suitable to the
treatment needs of people with CODs.
Physical and Mental Health Consultation
Any SUD treatment program that serves a
significant number of clients with CODs would do
well to expand standard staffing to include mental
health specialists and to incorporate consultation
(for assessment, diagnosis, and medication) into
treatment services.
Adding a master’s level clinical specialist with
strong diagnostic skills and expertise in working
with clients who have CODs can strengthen an
agency’s ability to provide services for these
clients. These staff members could function as
consultants to the rest of the team on matters
related to mental disorders, in addition to being
the liaison for a mental health consultant and
provision of direct services.
A psychiatrist provides services crucial to
sustaining recovery and stable functioning for
people with CODs: assessment, diagnosis,
periodic reassessment, medication, and rapid
response to crises. If lack of funding prevents the
SUD treatment agency from hiring a consultant
psychiatrist, the agency could establish a
collaborative relationship with a mental health
agency to provide those services. A memorandum
of agreement formalizes this arrangement and
ensures the availability of a comprehensive service
package for clients with CODs.
Prescribing Onsite Psychiatrist
An onsite psychiatrist brings diagnostic,
prescribing, and mental health counseling services
directly to the location at which clients receive
most of their treatment. An onsite psychiatrist
can reduce barriers presented by offsite referral,
including distance and travel limitations, the
inconvenience of enrolling in another agency,
separation of clinical services (more “red tape”),
fears of being seen as “mentally ill” (if referred to a
mental health agency), cost, and difficulty getting
comfortable with different staff.
The consensus panel is aware that the cost of an
onsite psychiatrist is a concern for many programs.
Many agencies that use the onsite psychiatrist
model find that they can afford to hire a psychiatrist
part time, even 4 to 16 hours per week, and that
a significant number of clients can be seen that
way. A certain amount of that cost can be billed
to Medicaid, Medicare, insurance agencies, or
other funders. For larger agencies, the psychiatrist
may be full time or share a full-time position with
a nurse practitioner. The psychiatrist can also be
employed concurrently by the local mental health
program, an arrangement that helps to facilitate
access to other mental health services such as
intensive outpatient treatment, psychosocial
programs, and even inpatient psychiatric care if
needed.
Ideally, SUD treatment agencies should hire a
psychiatrist with SUD treatment expertise to work
onsite. Finding psychiatrists with this background
Chapter 2 25

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
may present a challenge. Psychiatrists certified by
the American Society of Addiction Medicine or the
American Osteopathic Association (for osteopathic
physicians) can provide leadership, advocacy,
development, and consultation for SUD treatment
staff.
Medication and Medication Monitoring
Many clients with CODs require medication
to control their psychiatric symptoms and to
stabilize their mental status. The importance
of stabilizing clients with CODs on psychiatric
medication when indicated is now well established
in the SUD treatment field. (Chapter 7 covers in
more depth the role of medication in treating
CODs.) One important role of psychiatrists in
SUD treatment settings is to provide medication
based on the assessment and diagnosis of the
client, with subsequent regular contact and review
of medication. These activities include careful
monitoring and review of medication adherence.
Psychoeducational Classes
Psychoeducational classes on mental disorders
and SUDs are important elements in basic COD
programs. These classes typically focus on the signs
and symptoms of mental disorders, medication,
and the effects of mental disorders on substance
misuse. Psychoeducational classes of this kind
increase client awareness of their specific problems
and do so in a safe and positive context. Most
important, however, is that education about mental
disorders be open and generally available within
SUD treatment programs. Information should be
presented in a factual manner. Some mental health
clinics have prepared synopses of mental illnesses
for clients in terms that are factual but unlikely to
cause distress. A range of literature written for the
layperson is also available through government
agencies and advocacy groups (see Appendix
B). This material provides useful background
information for the SUD treatment counselor as
well as for the client.
Relapse Prevention
Programs can adopt strategies to help clients
become aware of cues or “triggers” that make
them more likely to misuse substances and help
them develop alternative coping responses to
those cues. Some providers use “mood logs” to
increase clients’ awareness of situational factors
that underlie urges to use substances. These logs
help answer the question, “When I have an urge to
drink or use, what is happening?” Basic treatment
programs can train clients to recognize cues for
the return of psychiatric symptoms, to manage
emotions, and to identify, contain, and express
feelings appropriately. (For more information about
relapse prevention and COD services, turn to
Chapter 5.)
Case Management
CODs are complex conditions that affect many
areas of a person’s life, including his or her
physical and emotional functioning, vocation/
education, social and family relationships, and
daily functioning. Case management is needed
to ensure that clients receive a continuum of
support services at the intensity and level needed
to meet their service needs and readiness for
change. Administrators should ensure that
staff case managers are service providers and
advocates for the specific needs of clients with
CODs. Additionally, programs should offer case
management that facilitates client transitions from
one level of care to the next and that is responsive
to all recovery-related needs.
COD-Specic Treatment Components
People with CODs face unique challenges compared
with individuals who have only a mental illness or
an SUD. For instance, their risk of homelessness,
incarceration, and recovery relapse are particularly
high. Further, symptoms of one condition can
exacerbate the other (especially if untreated), and
treatment components should comprehensively
address all diagnoses and symptoms. Administrators
should ensure that program elements speak directly
to CODs by hiring staff with COD training and
experience and implementing programs adapted
to the particular needs of COD populations.
(See Chapter 7 for guidance on adapting various
treatment models for CODs.)
Continuing Care Services
Long-term follow-up is critical to recovery. SUDs
and mental illness are chronic diseases, and clients
will likely face struggles (including relapse) long
Chapter 2 26

TIP 42
Chapter 2—Guiding Principles for Working With People Who Have CODs
after they leave treatment. Programs have many
options for providing continuing care, including
mutual support and peer recovery support
programs, relapse prevention groups, ongoing
individual or group counseling, and mental health
services (e.g., medication checks). For inpatient
settings, long-term follow-up should be discussed
collaboratively as part of clients’ discharge plan so
clients are fully aware of the supports and services
in place to help them succeed. (Also see the
section “Ensuring Continuity of Care.”)
Dual Recovery Mutual-Support Groups
(Osite)
Double Trouble Groups (Onsite)
Onsite groups such as Double Trouble in Recovery
provide a forum for discussing the interrelated
problems of mental disorders and SUDs, helping
participants to identify triggers for relapse. Clients
describe their psychiatric symptoms (e.g., hearing
voices) and their urges to use drugs. They are
encouraged to discuss, rather than to act on, these
impulses. Double Trouble groups can also be used
to monitor medication adherence, psychiatric
symptoms, substance use, and adherence to
scheduled activities. Double Trouble provides a
constant framework for assessment, analysis, and
planning. Through participation, the individual with
CODs develops perspective on the interrelated
nature of mental disorders and SUDs and becomes
better able to view his or her behavior within this
framework.
Various dual recovery mutual-support groups exist
in many communities. SUD treatment programs
can refer clients to dual recovery mutual-support
groups tailored to the special needs of people
with CODs. These groups provide a safe forum for
discussion about medication, mental health, and
substance misuse problems in an understanding,
supportive environment where coping skills can be
shared. Chapter 7 contains a more comprehensive
description of this approach.
Assessing the Agency’s Capacity To Serve
Clients With CODs
Every agency that already is treating or planning to
treat clients with CODs should assess the current
profile of its clients, as well as the estimated
number and type of potential new clients in
the community. It must also consider its current
capabilities, its resources and limitations, and
the services it wants to provide in the future.
Organizational tasks to determine service capacity
include:
•
Conducting a needs assessment to determine
the prevalence of CODs in the client population,
the demographics of those clients, and the
nature of the disorders and accompanying
problems they present. Data gathered can be
used to support grant proposals for increasing
service capacity.
12STEP FACILITATION AND CODs
12-Step facilitation (TSF) is a treatment engagement strategy designed to move clients toward
participation in mutual support as a part of their plan for achieving and sustaining long-term recovery.
Less research has been conducted on TSF for COD populations than for SUD-only populations, but early
findings suggest that it may be helpful in teaching clients with CODs about their illnesses and about the
benefits of mutual-support program participation (Hagler et al., 2015).
In one randomized, controlled trial (Bogenschutz et al., 2014b), people with alcohol use disorder and SMI
were exposed to 12 weeks of TSF adapted for CODs. Compared with treatment as usual, those in the TSF
condition were more than twice as likely to participate in 12-Step groups (65.8 percent vs. 29.4 percent)
and, on average, attended more meetings. Although there were no differences in substance use between
the two conditions, 12-Step participation was a significant predictor of future proportion of days abstinent
and drinking intensity (i.e., number of drinks per drinking day).
Chapter 2 27

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
•
Determining what changes need to be made in
staff, training, accreditation, and other factors to
provide effective services for clients with CODs.
•
Assessing community capacity to understand
what resources and services are already
available within their local and state systems of
care before deciding what services to provide.
•
Identifying missing levels of care/gaps in
services to help programs better respond to
client needs.
SAMHSA’s Dual Diagnosis Capability in Addiction
Treatment (DDCAT) Toolkit (SAMHSA, 2011b) helps
SUD treatment systems and programs assess and
enhance their capacity to effectively serve clients
with CODs. The toolkit features an assessment
measure (the DDCAT Index) that provides
feedback on numerous program elements critical
to implementation and maintenance of competent
service delivery for CODs. To clarify the guiding
principles and approaches that optimize COD
programming success, these elements are further
classified into seven dimensions:
1. A structure that offers unrestricted, integrated,
collaborative services to clients with CODs
2. A culture that is welcoming to clients with
CODs and readily offers education about CODs
3. Use of routine screening, assessment, and
diagnosis (or referral to diagnosis, if needed) for
clients with CODs that takes into account each
client’s severity and persistence of symptoms
4. A clinical process that includes stage-wise
treatment planning; ongoing assessment
and monitoring of symptoms of both
disorders throughout the course of care;
and numerous approaches to interventions,
such as pharmacotherapy management,
psychoeducation and support (for the client
and for family), specialized interventions in
behavioral health, and peer-based services
5. Provision of continuous care through
collaborative approaches, recovery maintenance
strategies, and follow-up services (including
community-based and peer-based services)
6. Attention to staffing needs, such as including
prescribers; ensuring that clinicians possess
required licensure, competency, and experience;
and implementing supervision or other
professional consultation processes (like case
reviews or other formal approaches to staff
monitoring and support) to ensure ethical,
evidence-based care
7. Staff training on CODs, including training
that imparts basic skills and knowledge
(e.g., screening and assessment, symptoms,
prevalence rates) as well as advanced training
(e.g., specific interventions, including basic
understanding of pharmacotherapies)
Trauma-informed care should be the standard
among all programs providing COD services.
Trauma is exceedingly common among
people with co-occurring mental disorders
and SUDs and, if untreated, can make recovery
very challenging. For more information
about integrating trauma-informed services,
like assessments and treatments, into COD
programming, see TIP 57, Trauma-Informed
Care in Behavioral Health Services, as well as
Chapters 3 and 6 of this TIP.
The consensus panel suggests the following
classification system: basic, intermediate, advanced
or fully integrated. As conceived by the consensus
panel:
•
A basic program has the capacity to provide
treatment for one disorder but also screens for
the other disorder and can access necessary
consultations.
•
A program with an intermediate level of
capacity tends to focus primarily on one
disorder without substantial modification to its
usual treatment, but also explicitly addresses
some specific needs related to the other
disorder. For example, an SUD treatment
program may recognize the importance of
continued use of psychiatric medications in
recovery, or a psychiatrist could provide MI
regarding substance use while prescribing
medication for mental disorders.
•
A program with advanced capacity provides
integrated SUD treatment and mental health
services for clients with CODs. Chapter 7
Chapter 2 28
TIP 42
•
Chapter 2—Guiding Principles for Working With People Who Have CODs
EXHIBIT 2.5. Levels of Program Capacity in CODs
More Treatment for More Treatment
Mental Disorders for SUDs
Fully Integrated
COD
Integrated
Advanced
COD
Enhanced
Advanced
COD
Enhanced
Intermediate
COD
Basic
Capable
Mental
Disorder Only
Treatment
Basic
Addiction
Intermediate
Only
Treatment
Capable
COD
Level of Program Capacity Mental Disorder Treatment
in CODs for SUD Treatment Providers
Providers
describes several such program models. These
programs address CODs from an integrated
perspective and provide services for both
disorders. For some programs, this means
strengthening SUD treatment in the mental
health services setting by adding interventions
that target specific COD symptoms or
disorders and relapse prevention strategies
that intertwine identification of cues, warning
signs, and coping skills for both disorders. For
other programs, it means adding mental health
services, such as psychoeducational classes
on mental disorder symptoms and groups
for medication monitoring, in SUD treatment
settings. Collaboration with other agencies can
aid comprehensiveness of services.
A fully integrated program actively combines
SUD and mental illness interventions to treat
disor
ders, related problems, and the whole
person more effectively.
The suggested classification has several
advantages. For one, it avoids use of the term
“dual diagnosis” and allows a more general,
flexible approach to describing capacity without
specific criteria. In addition, the classification
system reflects a bidirectionality of movement
wherein either addiction or mental health agencies
can advance toward more integrated care for
clients with CODs, as shown in Exhibit 2.5.
Conclusion
Co-occurring mental disorders and SUDs are
complex. They present significant clinical,
functional, social, and economic challenges
for people living with them as well as for the
counselors, administrators, supervisors, and
programs who treat them. To help address the
full range of symptoms clients experience and
optimize outcomes, providers and programs must
understand the components of comprehensive,
high-quality care for CODs and have plans in place
to implement core strategies, skills, and services.
By using treatment frameworks, philosophies,
and approaches empirically shown to net the best
outcomes for people living with CODs, the SUD
treatment and mental health service fields can
close gaps in access and treatment so that people
with CODs can live healthier, more functional lives.
Chapter 2 29
This page intentionally left blank.

Chapter 3—Screening and Assessment of
Co-Occurring Disorders
KEY MESSAGES
•
Screening and assessment are central to
identifying and treating clients with co-
occurring disorders (CODs) in a manner that
is timely, effective, and tailored to all of their
needs. The assessment process helps fulfill
a critical need, as most people with CODs
receive either treatment for only one disorder
or no treatment at all.
• Most counseling professionals can initiate the
screening process. Understanding why, whom,
and when to screen and which validated tools
to use are the keys to success.
• The assessment process is a multifactor,
biopsychosocial approach to determining
which symptoms and diagnoses might be
present and how to tailor decisions about
treatment and follow-up care based on
assessment results.
• The 12 steps of assessment are designed to
foster a thorough investigation of pertinent
biopsychosocial factors contributing to,
exacerbating, and mitigating the client’s
current symptomatology and functional
status. At its core is the client’s chronological
history of past symptoms of substance use
disorders (SUDs) or mental illness, as well
as diagnosis, treatment, and impairment
related to these issues. Counselors should get
a detailed description of current strengths,
supports, limitations, skill deficits, and cultural
barriers. Identification of a client’s stage of
change and readiness to engage in services
will inform treatment planning and optimize
adherence and outcomes.
TIP 42
SUBSTANCE USE DISORDER TREATMENT FOR
PEOPLE WITH CO-OCCURRING DISORDERS
A serious treatment gap exists between the mental
disorder and SUD needs of people with CODs
and the number of people who actually receive
services. According to the 2018 National Survey
on Drug Use and Health, of the 9.2 million U.S.
adults ages 18 and older who had CODs in the
past year, more than 90 percent did not receive
treatment for both disorders, and approximately
50 percent received no treatment at all (Center
for Behavioral Health Statistics and Quality, 2019).
Underlying these statistics is the failure of addiction
and mental health professionals to adequately
recognize CODs.
Screening and assessment are critical components
of establishing diagnosis and getting people on the
right path to treatment or other needed services.
This chapter, whose audiences are counselors,
other treatment/service providers, supervisors, and
administrators, offers guidance to help addiction
counselors understand the purpose and process for
effective screening and assessment of clients for
possible CODs. It has three parts:
1. An overview of the basic screening and
assessment approach that should be a part of
any program for clients with CODs
2. An outline of the 12 steps to an ideal complete
screening and assessment, including some
instruments that can be used in assessing CODs
(see Appendix C for select screening tools)
3. A discussion of key considerations in treatment
matching
Ideally, information needs to be collected
continually and assessments revised and monitored
as clients move through recovery. A comprehensive
assessment, as described in the main section of
this chapter, leads to improved treatment planning
and this chapter aims to provide a model of the
optimal process of evaluation for clients with
CODs and to encourage the field to move toward
31

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
this ideal. Nonetheless, the panel recognizes that
not all agencies and providers have the resources
to conduct immediate and thorough screenings.
Therefore, the chapter provides a description
of the initial screening and the basic or minimal
assessment of CODs necessary for the initial
treatment planning.
Note that medical problems (including physical
disability and sexually transmitted diseases),
cultural topics, gender-specific and sexual
orientation matters, and legal concerns always
must be addressed, whether basic or more
comprehensive assessment is performed. The
consensus panel assumes that appropriate
procedures are in place to address these and other
important areas that must be included in treatment
planning. However, the focus of this chapter,
in keeping with the purpose of this Treatment
Improvement Protocol (TIP), is on screening and
assessment for CODs.
Screening and Basic Assessment
for CODs
This section provides an overview of the screening
and basic assessment process for CODs. A basic
assessment covers the key information required
for treatment matching and treatment planning.
Specifically, the basic assessment offers a structure
for obtaining:
•
Demographic and historical information,
established or probable diagnoses, and associated
impairments.
•
General strengths and problem areas.
•
Stage of change or level of service needed for
both substance misuse and mental illness.
•
Preliminary determination of the severity
of CODs as a guide to final level of care
determination.
In carrying out these processes, counselors
should understand the limitations of their
licensure or certification authority to diagnose
or assess mental disorders. Generally, however,
collecting screening and assessment information is
a legitimate and legal activity even for unlicensed
providers, as long as they do not use diagnostic
labels as conclusions or opinions about the
client. Information gathered in this way is needed
to ensure that the client is placed in the most
appropriate treatment setting (see the section
“Step 5: Determine Level of Care”) and to assist in
providing mental disorder and addiction care that
addresses each disorder.
In addition, a number of circumstances that can
affect validity and test responses may not be
obvious to the beginning counselor, such as the
manner in which instructions are given to the client,
the setting where the screening or assessment
takes place, privacy (or the lack thereof), and trust
and rapport between the client and counselor.
Throughout the process be sensitive to cultural
context and to the different presentations of both
SUDs and mental disorders that may occur in
various cultures (see Chapter 5 of this TIP for more
information about culturally sensitive care for clients
with CODs). Detailed discussions of these important
screening/assessment and cultural matters are
beyond the scope of this TIP.
For more information on screening and assessment
for CODs, see Screening and Assessment of
Co-Occurring Disorders in the Justice System
(Substance Abuse and Mental Health Services
Administration [SAMHSA], 2015b). For information
on cultural topics, see TIP 59, Improving Cultural
Competence (SAMHSA, 2014a).
Screening
For the purposes of this TIP, screening is a formal
process of testing to determine whether a client
warrants further because of a co-occurring SUD or
mental disorder. The screening process for CODs
seeks to answer a “yes” or “no” question: Does
the substance misuse (or mental disorder) client
being screened show signs of a possible mental (or
substance misuse) problem?
Although both screening and assessment are
ways of gathering information about the client in
order to better treat him or her, assessment differs
from screening in that screening is a process for
evaluating the possible presence of a particular
problem and typically precedes assessment,
whereas assessment is a process for defining the
nature of that problem and developing specific
Chapter 3 32

TIP 42
Chapter 3—Screening and Assessment of Co-Occurring Disorders
ADVICE TO THE COUNSELOR: DOS AND DON’TS OF ASSESSMENT
FOR CODs
• Do keep in mind that assessment is about getting to know a person with complex and individual
needs. Tools alone cannot produce a comprehensive assessment.
• Do always make every effort to contact all involved parties, including family members, people who
have treated the client previously, and probation officers, as quickly as possible in the assessment
process. (These other sources of information will henceforth be referred to as collaterals.)
• Don’t allow preconceptions about addiction to interfere with learning about what the client
really needs. CODs are as likely to be underrecognized as overrecognized. Assume initially that an
established diagnosis and treatment regimen for mental illness is correct, and advise clients to
continue with those recommendations until careful reevaluation has taken place.
• Do become familiar with the diagnostic criteria for common mental disorders, including serious mental
illness (SMI) (e.g., bipolar disorder, schizophrenia, other psychotic disorders). Also become familiar with
the names and indications of common psychiatric medications and with the criteria in your own state
for determining who is a mental disorder priority client. Know the process for referring clients for mental
illness case management services or for collaborating with mental health services providers.
• Don’t assume there is one correct treatment approach or program for any type of COD. The purpose
of assessment is to collect information on multiple variables, enabling individualized treatment
matching. Assess stage of change for each problem and clients’ level of ability to follow treatment
recommendations.
• Do get familiar with the specific role your program plays in delivering services related to CODs in the
wider context of the system of care. This allows you to have a clearer idea of what clients your program
will best serve and helps you to facilitate access to other settings for clients who might be better
served elsewhere.
• Don’t be afraid to admit when you don’t know, either to the client or yourself. If you do not
understand what is going on with a client, acknowledge that to the client, indicate that you will
work with the client to find the answers, and then ask for help. Identify at least one supervisor who is
knowledgeable about CODs as a resource for asking questions.
• Most important, do remember that empathy and hope are the most valuable components of your
work with a client. When in doubt about how to manage a client with COD, stay connected, be
empathic and hopeful, and work with the client and the treatment team to try to figure out the best
approach over time.
treatment recommendations for addressing the
problem. Thus, assessment is a more thorough and
comprehensive process than screening.
The consensus panel recommends that all clients
presenting for SUD treatment, mental health
services, or both be screened at least annually
by SUD treatment and mental health services
providers for past and present substance misuse
and mental disorders. SUD treatment and mental
health counselors should also screen clients who
report experiencing or otherwise show signs or
symptoms of an SUD or a mental disorder.
Counselors can conduct screening processes, if
properly designed (see next paragraph), using
their basic counseling skills. All counselors can
be trained to screen for COD. There are seldom
Chapter 3 33

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
ADVICE TO THE COUNSELOR: KNOW THE BASICS OF SCREENING
•
What is screening? Screening is a simple process of determining whether more indepth assessment is
needed, often consisting of asking the client basic “yes” or “no” questions.
• Who should conduct screening? Nearly any counselor can screen. Generally, no special training is
required.
• When does screening take place? The consensus panel recommends that all SUD treatment clients
and mental disorder treatment clients be screened for CODs at least annually. Screening is also needed
when clients report or exhibit symptoms suggesting another disorder may be present.
• Where does screening occur? Screening can happen anywhere that services are offered.
• Why screen? Screening is a necessary first step to ensure that clients receive the right diagnosis and
treatment.
• How should screening be performed? A variety of easy-to-administer screening tools are available and
are located or linked to throughout this chapter as well as in Appendix C.
any legal or professional restraints on who can
be trained to conduct a screening. Counselors
should work with their program administrators to
determine how often to screen, which tools to use,
and who will perform the screening.
The purpose of screening is not necessarily
to identify what kind of disorder the person
might have or how serious it might be.
Rather, screening determines whether further
assessment is warranted. Screening processes
always should define a protocol for determining
which clients screen positive and for ensuring that
those clients receive a thorough assessment. That
is, a professionally designed screening process
establishes precisely how any screening tools or
questions are to be scored and indicates what
constitutes scoring positive for a particular possible
problem (often called “establishing cutoff scores”).
The screening protocol details exactly what takes
place after a client scores in the positive range and
provides the necessary standard forms to be used
to record the results of all later assessments and to
document that each staff member has carried out
his or her responsibilities in the process.
So, what can an SUD treatment or mental health
counselor do to screen clients? Screening often
entails having a client respond to a specific set of
questions, scoring those questions according to the
counselor’s training, and then taking the next step
in the process depending on the results and the
design of the screening process. In SUD treatment
or mental health service settings, every counselor
or clinician who conducts intake or assessment
should be able to screen for the most common
CODs and know the protocol for obtaining COD
assessment information and recommendations. For
SUD treatment agencies instituting mental disorder
screening or mental health service programs
instituting substance misuse screening, see the
section, “Assessment Step 3: Screen for and Detect
COD.” Selected instruments from that section
appear in this chapter and in Appendix C.
Basic Assessment
A basic assessment assessment consists of
gathering key information and engaging clients in
a process that enables counselors to understand
clients’ readiness for change, problem areas,
COD diagnoses, disabilities, and strengths. An
assessment typically involves a clinical examination
of the functioning and well-being of the client and
includes a number of tests and written and oral
exercises. The COD diagnosis is established by
referral to a psychiatrist, clinical psychologist, or
other qualified healthcare professional. Assessment
of the client with CODs is an ongoing process
that should be repeated over time to capture
the changing nature of the client’s status. Intake
information includes:
Chapter 3 34

TIP 42
Chapter 3—Screening and Assessment of Co-Occurring Disorders
•
Background—family, trauma history, history
of domestic violence (as either a perpetrator
or a victim), marital status, legal involvement
and financial situation, health, education,
housing status, strengths and resources, and
employment.
•
Substance use—age of first use, primary
substance(s) used (including alcohol), patterns of
substance use, treatment episodes, and family
history of substance use problems.
•
Mental illness—family history of mental illness;
client history of mental illness, including
diagnosis, hospitalization and other treatment;
current symptoms and mental status; and
medications and medication adherence.
In addition, the basic information can be
augmented by some objective measurement
(see “Step 3: Screen for and Detect COD”
and Appendix C). It is essential for treatment
planning that the counselor organize the collected
information in a way that helps identify established
mental disorder diagnoses and current treatment.
The following text box highlights the role of
instruments in assessment.
Careful attention to the characteristics of past
episodes of substance misuse and abstinence with
regard to mental disorder symptoms, impairments,
diagnoses, and treatments can illuminate the role
of substance misuse in maintaining, worsening,
and interfering with the treatment of any mental
disorder. Understanding a client’s mental disorder
symptoms and impairments that persist during
periods of abstinence of 30 days or more can be
useful, particularly in understanding what the client
copes with even when the acute effects of substance
misuse are not present. For any period of abstinence
that lasts a month or longer, ask the client about
mental health services, SUD treatment, or both.
If mental disorder symptoms (even suicidality or
hallucinations) occur within 30 days of intoxication or
withdrawal from the substance, symptoms may be
substance induced. The best way to manage them is
by maintaining abstinence from substances. Even if
symptoms are substance induced, formal treatment
strategies should be applied to help the client newly
in recovery best manage the symptoms.
THE ROLE OF ASSESSMENT
TOOLS
Providers frequently ask, what is the best
assessment tool for COD? The answer is that
there is no single gold standard assessment
tool for COD.
•
Many traditional clinical tools focus narrowly
on a specific problem. An example of such a
tool is the Beck Depression Inventory (Beck &
Steer, 1987), a list of 21 questions about mood
and other symptoms of feeling depressed.
•
Other tools have a broader focus and
organize a range of information so that the
collection of such information is done in
a standard, regular way by all counselors.
The Addiction Severity Index (ASI), which is
not a comprehensive assessment tool but
a measure of addiction severity in multiple
problem domains, is an example of this type
of tool (McLellan et al., 1992). Not only does a
tool such as the ASI help a counselor, through
repetition, become adept at collecting the
information, it also helps the counselor refine
his or her sense of similarities and differences
among clients.
•
Knowing the appropriateness of a tool is
also critical. Has the assessment been well
studied? Is it considered valid and reliable? Is
it validated for use in a population the client
represents? If the answer to any of these
questions is “no,” that might mean that the
results from the assessment are not reliable,
valid, interpretable, applicable to the client, or
some combination thereof. This is especially
true with clients from diverse populations.
Race/ethnicity, educational background,
age, gender—all of these factors affect life
experiences and can affect the answers a
person gives to a questionnaire. Wherever
possible, be sure to use tools that are
appropriately matched to the client.
•
A standard mental status examination can
also collect information on current mental
health. Some very good tools exist, but no
one tool stands in for comprehensive clinical
assessment.
Provider and client together should try to
understand the specific effects that substances
Chapter 3 35

TIP 42
−
−
−
Substance Use Disorder Treatment for People With Co-Occurring Disorders
have had on mental disorder symptoms, including
possible triggering of psychiatric symptoms
through substance use. The consensus panel
notes that many individuals with CODs have
well-established diagnoses when they enter SUD
treatment and encourages counselors to find out
about any known diagnoses.
As part of basic assessment, assess clients’
mental health and SUD history by asking
questions like:
•
“Tell me about your mental ‘ups and downs’.
What is it like for you when things are worse?
What is it like when things are better or stable?”
•
“How do you notice using alcohol (or whatever
substance the client is misusing) affects your
depression (or whichever mental disorder
symptom the client is experiencing)?”
•
“What mental disorders have you been
diagnosed with in the past? When was that,
and what happened after you received the
diagnosis?”
•
“What (mental disorder or substance misuse)
treatment seemed to work best for you?”
•
“What treatment did you like or dislike? Why?”
The Complete Screening and
Assessment Process
This chapter is organized around 12 specific steps
in the assessment process. Through these steps,
the counselor seeks to:
•
Get a more detailed chronological history of
mental symptoms, diagnosis, treatment, and
impairment, particularly preceding substance
misuse and during periods of extended
abstinence.
•
Get a more detailed description of current
strengths, supports, limitations, skill deficits,
and cultural barriers related to following a
recommended treatment regimen for a disorder
or problem.
ADVICE TO THE COUNSELOR: HOW TO MAKE THE ASSESSMENT PROCESS
A SUCCESS
Counselors can increase the chances of a successful assessment process by taking some basic steps to
help clients feel relaxed and open.
• First, create a welcoming environment by taking an open, nonjudgmental attitude.
SUD and mental illness each carry their own stigma, and people who have both disorders may feel
even more marginalized, leading to underreporting or denial of symptoms and treatment needs.
Research suggests that some mental health professionals possess especially negative attitudes and
beliefs about individuals with SMI, like psychotic disorders, and SUDs (Avery, Zerbo, & Ross, 2016).
By being aware of personal biases and taking steps to create a warm and open environment,
counselors can increase the likelihood that clients will feel comfortable discussing distressing
symptoms and dysfunctions, which can better inform treatment needs.
• Use open-ended rather than just “yes” or “no” questions. Open-ended questions will allow counselors
to elicit a greater depth of information and will feel more conversational in tone to the client. “Yes” or
“no” questions can feel more judgmental and detached. Open-ended questions are also more thought
provoking and can lead the client to greater self-exploration and self-awareness.
• Furthermore, be sure to address motivation by talking with clients about their ambivalence toward
engaging in services. More information about motivational interviewing techniques can be found in the
update of TIP 35, Enhancing Motivation for Change in Substance Use Disorder Treatment (SAMHSA, 2019c).
Chapter 3 36
TIP 42
Chapter 3—Screening and Assessment of Co-Occurring Disorders
•
Determine stage of change for each problem
and identify external contingencies that might
help promote treatment adherence.
Assessment steps appear sequential, but some
can occur simultaneously or in a different order,
depending on the situation. Providers should
identify and attend to acute safety needs, which
often must be addressed before a more compre-
hensive assessment process can occur. Sometimes,
however, components of the assessment process
are essential to address clients’ specific safety
needs. Furthermore, counselors should recognize
that although the assessment seeks to identify
individual needs and vulnerabilities as quickly
as possible to initiate appropriate treatment,
assessment is an ongoing process. As treatment
proceeds and as other changes occur in clients’
lives and mental status, counselors must actively
seek current information rather than proceed on
assumptions that might be no longer valid. Exhibit
3.1 lists general considerations for the assessment
of clients with CODs.
The following section discusses the availability
and utility of validated assessment tools to assist
counselors in this process. A number of tools
are required by various states for use in their
SUD treatment systems (e.g., ASI, [McLellan et
al., 1992]; American Association of Community
Psychiatry – Level of Care Utilization System
[LOCUS]). Particular attention will be given to the
role of these tools in the COD assessment process,
with suggested strategies for reducing duplication
of effort when possible.
It is beyond the scope of this TIP to provide
detailed instructions for administering the tools
mentioned, but select information about cutoff
scores is included in this chapter (and select
measures are included in Appendix C). Basic
information about each instrument is also given
in this chapter, and readers can obtain more
detailed information about administration and
interpretation from the sources given for obtaining
these instruments.
This discussion is directed toward providers
working in SUD treatment settings, although
many of the steps apply equally well to mental
health clinicians in mental health service settings.
At certain key points in the discussion, particular
information relevant to mental health clinicians is
identified and described.
EXHIBIT 3.1. Assessment Considerations for Clients With CODs
•
Providers should maintain a nonjudgmental attitude while taking a matter-of-fact approach to asking
about past and current substance misuse and mental illness.
•
First asking about past substance misuse and mental illness could help clients feel more open and
amenable to discussing current problems, which people sometimes minimize.
•
Counselors should explain to clients why they are asking about substance misuse and mental illness and
discuss the role of such information in treatment planning.
•
Self-report assessments can be informative, but counselors should gather laboratory data and collateral
information from family and friends as needed.
•
Counselors should be able to recognize the common demographic correlates of COD, such as gender,
younger age, lower educational attainment, and single marital status. These give counselors an idea
of which clients may be more vulnerable to these disorders and potentially in need of screening and
assessment. However, these factors should not be used to justify not screening or assessing certain
people. Screen all clients for substance misuse and mental illness at least once per year. All clients
who screen positive for symptoms, functional impairment, or other service needs should be fully
assessed.
Source: Mueser & Gingerich (2013).
Chapter 3 37

TIP 42
•
•
•
•
•
•
•
Substance Use Disorder Treatment for People With Co-Occurring Disorders
Using a Biopsychosocial Approach
Because addictions and mental disorders are
complex conditions with multiple contributing
factors, clinicians should conduct assessments
using a biopsychosocial approach that thoroughly
investigates clients’ history and current status in a
holistic manner. “Biopsychosocial” in this context
refers to a clinical philosophy and approach to
care that seeks to understand clients and their
experience through a medical, psychological,
emotional, sociocultural, and socioeconomic lens.
This is particularly important when assessing and
treating CODs given that numerous determinants
and exacerbating and mitigating factors may
potentially be relevant to diagnosis, treatment
planning, and outcomes. Biopsychosocial
assessment is evidence based and the standard
of care. It is comprehensive and widely addresses
all aspects of clients’ lives that may be relevant
to his or her symptoms and service needs.
By definition, a biopsychosocial assessment
will rely on input from multidisciplinary team
members including physicians and nurses
(including psychiatric and mental health
nurses [specialty practice registered nurses]);
psychologists, psychiatrists, and other mental
health professionals; social workers; and addiction
counselors and other SUD treatment professionals.
Addiction counselors will not be able to assess all
biopsychosocial assessment areas (Exhibit 3.2) and
will focus primarily on the psychological and social
sources of information. Appendix C contains links
to sample biopsychosocial assessment forms.
EXHIBIT 3.2. Biopsychosocial Sources of Information in the Assessment
of CODs
TOPIC AREA SUD AREAS OF ASSESSMENT MENTAL DISORDER AREAS OF
ASSESSMENT
Biological
Alcohol on the breath
Positive urine tests
Abnormal laboratory tests
Withdrawal symptoms
Injuries and trauma
Medical signs and symptoms of toxicity
and withdrawal
Impaired cognition
•
•
•
Abnormal laboratory tests (e.g.,
magnetic resonance imaging)
Neurological exams
Use of psychiatric and other medications
Psychological
•
•
•
•
•
Intoxicated behavior
Functional impairment
Responses to SUD assessments
Documented substance misuse history
History of trauma
•
•
•
•
•
•
Mental status exam results
Responses to mental disorder/symptom
screens (e.g., depressed mood,
psychosis, anxiety)
History of or current diagnosis of and
treatment for mental illness
Stress and situational factors
Self-image and personality
History of trauma
Continued on next page
Chapter 3 38

TIP 42
•
•
•
•
•
•
•
•
•
•
•
•
•
•
•
•
Chapter 3—Screening and Assessment of Co-Occurring Disorders
Continued
TOPIC AREA SUD AREAS OF ASSESSMENT MENTAL DISORDER AREAS OF
ASSESSMENT
Social Collateral information from others (e.g.,
family, caregivers)
Social interactions, recreation/interests,
lifest
yle
Family history of SUDs
Availability of support systems (e.g.,
family
, friends, close others)
Housing, education, and job histories
Military history
Ethnic and cultural background
Legal history (e.g., involvement in the
criminal justic
e system)
Collateral information from others (e.g.,
family
, caregivers)
Social interactions, recreation/interests,
lifest
yle
Family history of mental disorders
Availability of support systems (e.g.,
family
, friends, close others)
Housing, education, and employment
histor
ies
Military history
Ethnic and cultural background
Legal history (e.g., involvement in the
criminal justic
e system)
TWELVE STEPS IN THE
ASSESSMENT PROCESS
Step 1: Engage the client.
Step 2: Identify and contact collaterals (family,
friends, other providers) to gather additional
information.
Step 3: Screen for and detect CODs.
Step 4: Determine quadrant and locus of
responsibility.
Step 5: Determine level of care.
Step 6: Determine diagnosis.
Step 7: Determine disability and functional
impairment.
Step 8: Identify strengths and supports.
Step 9: Identify cultural and linguistic needs
and supports.
Step 10: Identify problem domains.
Step 11: Determine stage of change.
Step 12: Plan treatment.
Assessment Step 1: Engage the Client
The first step in the assessment process is to
engage the client in an empathic, welcoming
manner and build rapport to facilitate open
disclosure of information regarding mental illness,
SUDs, and related concerns. The aim is to create
a safe and nonjudgmental environment in which
sensitive personal information may be discussed.
Counselors should recognize that cultural matters,
including the use of the client’s preferred language,
play a role in creating a sense of safety and
promote accurate understanding of the client’s
situation and options. Such topics therefore
must be addressed sensitively at the outset and
throughout the assessment process.
The consensus panel identified five key concepts
that underlie effective engagement during initial
clinical contact:
•
Universal access (“no wrong door”)
•
Empathic detachment
•
Person-centered assessment
•
Cultural sensitivity
•
Trauma-informed services
Chapter 3 39

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
All staff, including SUD treatment providers and
mental health clinicians, in any service setting
need to develop competency in engaging and
welcoming individuals with CODs. (See Chapter 5
for a discussion of working successfully with people
who have CODs and establishing a therapeutic
alliance.) Whereas engagement is presented here
as the first necessary step for assessment to take
place, in a larger sense engagement represents an
ongoing concern of the counselor—to understand
the client’s experience and to keep him or her
positive and engaged relative to the prospect of
better health and recovery.
No Wrong Door
“No wrong door” refers to formal recognition by
a service system that individuals with CODs may
enter through a range of community service sites,
that they are a high priority for engagement in
treatment, and that proactive efforts are necessary
to welcome them into treatment and prevent
them from falling through the cracks. Addiction
and mental health counselors are encouraged to
identify individuals with CODs, welcome them
into the service system, and initiate proactive
efforts to help them access appropriate treatment
in the system, regardless of their initial site
of presentation. The recommended attitude
counselors should embody is, “The purpose of this
assessment is not just to determine whether the
client fits in my program but to help the client
figure out where he or she fits in the system of
care and to help him or her get there.”
Empathic Detachment
Empathic detachment requires the assessing
clinician to:
•
Acknowledge that the provider and client are
working together to make decisions to support
the client’s best interest.
•
Recognize that the provider cannot transform
the client into a different person but can only
support change that he or she is already making.
•
Maintain an empathic connection even if the
client does not seem to fit into the provider’s
expectations, treatment categories, or preferred
methods of working.
Providers should be prepared to demonstrate
responsiveness to the requirements of treating
clients with CODs. Counselors should be careful
not to label mental disorder symptoms immediately
as caused by addiction but instead should be
comfortable with the strong possibility that a
mental disorder may be present independently and
encourage disclosure of information that will help
clarify the meaning of any CODs for that client.
(See Chapter 4 for guidance on distinguishing
independent mental disorders from substance-
induced mental disorders.)
Person-Centered Assessments
Person-centered assessments emphasize that the
focus of initial contact is not on getting forms filled
out or answering a battery of questions, or on
establishing program fit. Instead the focus is on
finding out what the client wants, seen from his or
her perspective on the problem, what he or she
wants to change, and how he or she thinks that
change will occur.
Ewing, Austin, Diffin, and Grande (2015) developed
an evidence-based practice tool for conducting
person-centered assessment and planning with
caregivers of palliative care patients. The framework
and key approaches they propose could be
generalized to other health issues—including mental
illness and substance misuse—and offer useful
guidance for ensuring assessment processes are
focused on the client and his or her problems, goals,
and needs. However, research is needed on the use
of their framework in people with CODs.
Sensitivity to Culture, Gender, and Sexual
Orientation
An important component of a person-centered
assessment is always recognizing the significant
role of culture on a client’s view of problems and
treatments. Cultures differ significantly in their
views of SUDs and mental disorders, which may
affect how a client presents. Clients may participate
in treatment cultures (mutual-support programs,
Dual Recovery Self-Help, psychiatric rehabilitation)
that also affect their view of treatment. Cultural
sensitivity requires recognizing one’s own cultural
perspective and having a genuine spirit of inquiry
into how cultural factors influence the clients’
requests for help.
Chapter 3 40

TIP 42
Chapter 3—Screening and Assessment of Co-Occurring Disorders
During the assessment process, counselors should
learn about clients’ sexual orientation and any
gender identity matters, as part of understanding
the clients’ personal identity, living situation, and
relationships. Counselors should also be aware
that clients often have family-related and other
concerns that must be addressed to engage them
in treatment, such as the need for child care.
For more information about culturally competent
treatment, see Chapters 5 and 6 of this TIP as
well as TIP 59, Improving Cultural Competence
(SAMHSA, 2014a) and TIP 51, Substance Abuse
Treatment: Addressing the Specific Needs of
Women (SAMHSA, 2009c).
Trauma-Informed Care
The high prevalence of trauma in individuals with
CODs requires a clinician to consider the possibility
of a trauma history even before beginning to assess
the client. Trauma may include early childhood
physical, sexual, or emotional abuse; experiences
of rape or interpersonal violence as an adult; and
traumatic experiences associated with political
oppression, as might be the case in refugee or
other immigrant populations. The approach to the
client must be sensitive to the possibility that the
client has suffered previous traumatic experiences
that may interfere with his or her ability to trust the
counselor. A clinician who observes guardedness on
the part of the client should consider the possibility
of trauma and try to promote safety in the interview
by providing support and gentleness, rather than
trying to “break through” evasiveness that might
look like resistance or denial. All questioning should
avoid “retraumatizing” the client.
See Chapter 4 for information about trauma-
informed care, Chapter 6 for information on
women’s concerns in CODs, and TIP 57, Trauma-
Informed Care in Behavioral Health Services
(SAMHSA, 2014b).
Assessment Step 2: Identify and
Contact Collaterals (Family, Friends,
Other Providers) To Gather Additional
Information
Clients presenting for SUD treatment, particularly
those who have current or past mental disorder
symptoms, may be unable or unwilling to report
past or present circumstances accurately. For this
reason, all assessments should include routine
procedures for identifying and contacting family
and other collaterals (with clients’ permission) who
may have useful information.
Information from collaterals is valuable as a
supplement to the client’s own report in all of the
assessment steps listed in the remainder of this
chapter. It is valuable particularly in evaluating the
nature and severity of mental disorder symptoms
when the client may be so impaired that he or she
is unable to provide that information accurately.
Note, however, that the process of seeking
such information must be carried out strictly in
accordance with applicable guidelines and laws
regarding confidentiality
1
and with the client’s
permission.
Assessment Step 3: Screen for and
Detect CODs
Because of the high prevalence of co-occurring
mental disorders in SUD treatment settings, and
because treatment outcomes for individuals with
multiple problems improve if each problem is
addressed specifically, the consensus panel recom-
mends that:
•
SUD treatment providers screen all new
clients for co-occurring mental disorders.
•
Mental disorder treatment providers screen all
new clients for any substance misuse.
The type of screening will vary by setting.
Substance misuse screening in mental disorder
service settings should:
•
Screen for acute safety risk related to serious
intoxication or withdrawal.
1
Confidentiality is governed by the federal “Confidentiality of Alcohol and Drug Abuse Patient Records” regulations (42 C.F.R.
Part 2) and the federal “Standards for Privacy of Individually Identifiable Health Information” (45 C.F.R. Parts 160 and 164).
Chapter 3 41

TIP 42
-
-
-
-
-
•
•
Substance Use Disorder Treatment for People With Co-Occurring Disorders
•
Screen for past and present substance use,
substance-related problems, and substance-
related disorders (i.e., SUDs and substance-
induced mental disorders).
Mental disorder screening has four major
components in SUD treatment settings:
•
Screen for acute safety risk, including for:
Suicide.
Violence to others.
Inability to care for oneself.
Risky behaviors.
Danger of physical or sexual victimization.
•
Screen for past and present mental illness
symptoms and disorders.
•
Screen for cognitive and learning deficits.
•
Regardless of setting, screen all clients for past
and present victimization and trauma.
Exhibit 3.3 lists recommended, validated screening
tools across behavioral health service settings.
EXHIBIT 3.3. Recommended Screening Tools To Help Detect CODs
Client safety
•
Columbia-Suicide Severity Rating Scale (C-SSRS)
•
Suicide Behaviors Questionnaire-Revised (SBQ-R)
•
Risk of harm section of the LOCUS
•
Humiliation, Afraid, Rape, and Kick
Past or present mental disorders
•
ASI
•
Mental Health Screening Form-III (MHSF-III)
•
Modified Mini Screen
•
Diagnostic and Statistical Manual of Mental Disorders (5th ed. [DSM-5]; American Psychiatric
Association, 2013) Cross-Cutting Symptom Measure
Past or present substance misuse
•
10-item Drug Abuse Screening Test (DAST-10)
•
Alcohol Use Disorders Identification Test (AUDIT) and Alcohol Use Disorders Identification
Test—Concise (AUDIT-C)
•
CAGE Questionnaire Adapted To Include Drugs
•
Michigan Alcoholism Screening Test (MAST)
•
National Institute on Drug Abuse (NIDA)-Modified Alcohol, Smoking, and Substance Involvement
Screening Test (ASSIST)
•
Simple Screening Instrument for Substance Abuse (SSI-SA)
Trauma
•
The Primary Care PTSD Screen for DSM-5
•
The PTSD Checklist for DSM-5
Level of care
LOCUS
Fun
ctioning and impairment
World Health Organization (WHO) Disability Assessment Schedule 2.0
Chapter 3 42

TIP 42
Chapter 3—Screening and Assessment of Co-Occurring Disorders
Safety Screening
Safety screening requires that, early in the
interview, the provider specifically ask the client
whether he or she has any immediate impulse
to engage in violent or self-injurious behavior,
or whether he or she is in any immediate danger
from others. These questions should be asked
directly of the client and of anyone else who is
providing information. If the answer is yes, the
provider should obtain more detailed information
about the nature and severity of the danger, the
client’s ability to avoid the danger, the immediacy
of the danger, what the client needs to do to
be safe and feel safe, and any other information
relevant to safety. Additional information can be
gathered depending on counselor/staff training for
crisis/emergency situations and the interventions
appropriate to the treatment provider’s particular
setting and circumstances. Once this information
is gathered, if it appears that the client is at
immediate risk, the provider should arrange
for a more indepth risk assessment by a mental
health–trained clinician, and the client should not
be left alone or unsupervised.
Screening for Risk of Suicide or Self-Harm
A variety of validated tools are available for
screening for risk of suicide or other self-harm:
•
C-SSRS is a commonly used, well-supported tool
to quickly assess suicidal ideation, behavior, and
lethality in adult and adolescent populations
(Posner et al., 2011). It is available in over 100
languages and has been used in many settings
that serve people with CODs, including primary
care, military hospitals, and the criminal justice
system. Screeners can be selected based on
the setting in which they are being used, the
population being screened, and the language
needed. Columbia University maintains versions
of the C-SSRS at http://cssrs.columbia.edu/
the-columbia-scale-c-ssrs/cssrs-for-communities-
and-healthcare/#filter=.general-use.english.
•
SBQ-R (Osman et al., 2001) has demonstrated
good reliability and validity in measuring past
suicide attempts, frequency of suicidal ideation,
previous suicidal communication, and likelihood
of future suicide attempt in adults in inpatient
and community settings (Batterham et al., 2015).
For the full instrument with an overview and
scoring instructions, see Exhibits 3.4 through
3.6, beginning on page 44.
•
Some systems use the LOCUS (Sowers, 2016)
to determine level of care for both mental
disorders and addiction. One dimension of
LOCUS specifically provides guidance for
scoring severity of risk of harm.
Chapter 3 43

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
EXHIBIT 3.4. The Suicide Behaviors Questionnaire-Revised (SBQ-R) -
Overview
The SBQ-R has 4 items, each tapping a different dimension of suicidality:*
•
Item 1 taps into lifetime suicide ideation and/or suicide attempt.
•
Item 2 assesses the frequency of suidical ideation over the past twelve months.
•
Item 3 assesses the threat of suicide attempt.
•
Item 4 evaluates self-reported likelihood of suidical behavior in the future.
Clinical Utility
Due to the wording of the four SBQ-R items, a broad range of information is obtained in a very brief
administration. Responses can be used to identify at-risk individuals and specific risk behaviors.
Scoring
See scoring guideline on the following page.
Psychometric Properties*
Cutoff Score Sensitivity Specificity
Adult General Population
Adult Psychiatric Inpatients
≥7
≥8
93%
80%
95%
91%
*Osman A, Bagge CL, Gutierrez PM, Konick LC, Kooper BA, Barrios FX. The Suicidal Behaviors Questionnaire-Revised
(SBQ-R): Validation with clinical and nonclinical samples. Assessment, 2001, (5), 443-454.
Source: Center for Quality Assessment and Improvement in Mental Health (2007).
EXHIBIT 3.5. SBQ-R-Scoring
ITEM 1: TAPS INTO LIFETIME SUICIDE IDEATION ANDOR SUICIDE ATTEMPTS
Selected response 1 Non-Suicidal subgroup 1 point
Selected response 2 Suicide Risk Ideation group 2 points
Selected response 3a or 3b Suicide Plan subgroup 3 points
Selected response 4a or 4b Suicide Attempt subgroup 4 points Total Points
ITEM 2: ASSESSES THE FREQUENCY OF SUICIDAL IDEATION OVER THE PAST 12 MONTHS
Selected Response:
Never 1 point
Rarely (1 time) 2 points
Sometimes (2 times) 3 points
Often (3-4 times) 4 points
Very often (5 or more times) 5 points Total Points
Chapter 3 44

TIP 42
□
□
□
Chapter 3—Screening and Assessment of Co-Occurring Disorders
ITEM 3: TAPS INTO THE THREAT OF SUICIDE ATTEMPT
Selected response 1 1 point
Selected response 2a or 2b 2 points
Selected response 3a or 3b 3 points Total Points
ITEM 4: EVALUATES SELF-REPORTED LIKELIHOOD OF SUICIDAL BEHAVIOR IN THE FUTURE
Selected Response:
Never 0 point
No chance at all 1 points
Rather unlikely 2 points
Unlikely 3 points
Likely 4 points
Rather Likely 5 points
Very Likely 6 points Total Points
Sum all the scores circled/checked by the respondents.
The total score should range from 3-18.
Total Score
AUC = AREA UNDER THE RECEIVER OPERATING CHARACTERISTIC CURVE; THE AREA MEASURES
DISCRIMINATION, THAT IS, THE ABILITY OF THE TEST TO CORRECTLY CLASSIFY THOSE WITH AND
WITHOUT THE RISK. .901.0 = EXCELLENT; .80.90 = GOOD; .70.80 = FAIR; .60.70 = POOR
Sensitivity Specificity PPV AUC
Item 1: a cutoff score of ≥ 2
Validation Reference: Adult Inpatient
Validation Reference: Undergraduate College
0.80
1.00
0.97
1.00
.95
1.00
0.92
1.00
Total SBQ-R: a cutoff score of ≥ 7
Validation Reference: Undergraduate College 0.93 0.95 0.70 0.96
Total SBQ-R: a cutoff score of ≥ 8
Validation Reference: Adult Inpatient
0.80 0.91 0.70 0.96
EXHIBIT 3.6. SBQ-R Suicide Behaviors Questionnaire—Revised
Patient Name _____________ Date of Visit _________________
Instructions: Please check the number beside the statement or phrase that best applies to you.
Have you ever thought about or attempted to kill yourself? (check one only)
1. Never
2. It was just a brief passing thought
3a. I have had a plan at least once to kill myself but did not try to do it
Continued on next page
Chapter 3 45
TIP 42
□
□
□
Substance Use Disorder Treatment for People With Co-Occurring Disorders
Continued
3b. I have had a plan at least once to kill myself and really wanted to die
4a. I have attempted to kill myself, but did not want to die
4b. I have attempted to kill myself, and really hoped to die
How often have y
ou thought about killing yourself in the past year? (check one only)
□
□
□
□
□
1. Never
2. Rarely (1 time)
3. Sometimes (2 times)
4. Often (3-4 times)
5. Very Often (5 or more times)
Have you ever told someone that you were going to commit suicide, or that you might do it? (check
one only)
□
□
□
□
□
1. No
2a. Yes, at one time, but did not really want to die
2b. Yes, at one time, and really wanted to die
3a. Yes, more than once, but did not want to do it
3b. Yes, more than once, and really wanted to do it
How lik
ely is it that you will attempt suicide someday? (check one only)
□
□
□
□
□
□
□
0. Never
1. No chance at all
2. Rather unlikely
3. Unlikely
4. Likely
5. Rather likely
6. Very likely
Copyright © Osman et al. (2001). All Rights Reserved.
For more indepth discussion of how to manage
suicidal ideation and behaviors in clients seeking
treatment for substance misuse, see Chapter 4
of this TIP as well as TIP 50, Addressing Suicidal
Thoughts and Behaviors in Substance Abuse
Treatment (Center for Substance Abuse Treatment
[CSAT], 2009).
No tool is definitive for safety screening. Providers
and programs should use one of these tools only
as a starting point, and then use more detailed
questions to get all relevant information.
Providers should not underestimate risk because
the client is actively using substances. For example,
although people who are intoxicated might only
seem to be making threats of self-harm (e.g., “I’m
just going to go home and blow my head off if
nobody around here can help me”), all statements
about harming oneself or others must be taken
seriously. Individuals who have suicidal or aggressive
impulses when intoxicated may act on those
impulses. Remember, alcohol and drug misuse are
among the highest predictors of danger to self
or others—even without any co-occurring mental
disorder.
Chapter 3 46

TIP 42
-
-
-
-
-
-
-
-
-
-
-
-
-
Chapter 3—Screening and Assessment of Co-Occurring Disorders
Determining whether and to what extent an
intoxicated client may be suicidal requires a skilled
mental health assessment, plus information from
collaterals who know the client best. (See Chapter
4 for a more detailed discussion of suicidality in
people with CODs.) In addition, remember that the
vast majority of people who are misusing substances
will experience at least transient symptoms of
depression, anxiety, and other mental disorders.
Moreover, even a skilled clinician may not be able to
determine whether an intoxicated suicidal patient is
making a serious threat of self-harm; however, safety
is a critical and paramount concern.
Positive Suicide Screens
If a client screens positive for suicide risk,
counselors should conduct a suicide risk as-
sessment to more thoroughly determine the
client’s potential for self-harm. No generally
accepted and standardized suicide assessment
has been shown to be reliable and valid, but
most established suicide assessments contain
similar elements. The assessment questions below
are drawn from the National Institute of Mental
Health's Ask Suicide-Screening Questions (ASQ)
Toolkit (n.d.; https://www.nimh.nih.gov/research/
research-conducted-at-nimh/asq-toolkit-materials/
index.shtml).
Ask questions about the client’s feelings about
living, such as:
•
Ask questions about the client’s feelings about
living, such as:
“Do you ever wish you weren’t alive?”
“Have you ever felt that your life wasn’t
worth living any longer?”
•
For people who endorse thoughts of suicide or
self-harm questions, ask questions like:
“Do you have any thoughts of killing yourself
now?”
“Do you have a plan for how you would kill
yourself?”
“If you decided to kill yourself, how would
you do it?”
•
For people who have tried to commit suicide in
the past, ask:
“Why did you try to commit suicide? When
was this? What were the circumstances? What
did you do?”
-
-
-
“What happened after you tried to kill
yourself?”
“Did you want to die?”
“Did you get medical or psychiatric treatment
after? Was tr
eatment offered to you? (If yes)
How did that go for you?”
•
Also be sure to ask about other symptoms and
factors that might increase or decrease risk of
dying by suicide, such as:
“What are some reasons you would not kill
yourself?”
“Do you know anyone who has killed
themselves or tried to?”
“In the past few weeks, have you felt so sad
or down that it was hard to do things you
normally enjoy?”
“In the past few weeks, have you felt
hopeless or as though things will never get
better?”
“Do you often act without thinking?”
“Is there a trusted adult or other person you
can talk to?”
“Are there any problems in your household
that ar
e hard to handle?”
The provider needs to determine, based on the
client’s assessment responses, whether the risk of
imminent suicide is mild, moderate, or high. The
provider must also determine to what degree the
client is willing and able to follow through with
a set of interventions to keep safe. Screening
personnel should also assess whether suicidal
feelings are transitory or reflect a chronic condition.
Factors that may predispose a client toward
suicide should also be considered in client
evaluation. Vulnerable populations include (U.S.
Department of Health and Human Services, 2012):
•
American Indians/Alaska Natives.
•
Individuals who have lost a loved one to suicide.
•
Individuals involved in the criminal justice system
or child welfare system.
•
Individuals who engage in nonsuicidal self-injury
(see Section III of DSM-5).
•
Individuals with a history of suicide attempts.
•
Individuals with debilitating physical conditions.
•
Individuals with mental disorders, SUDs, or both.
•
Individuals in the lesbian/gay/bisexual/
transgender/questioning community.
Chapter 3 47
TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
•
Members of the armed forces and veterans.
•
Middle-aged and older men.
Asking people about thoughts of suicide
does not make them more likely to try to kill
themselves. On the contrary, asking about
suicide displays a level of care and concern that
can help people with suicidal thoughts and
intentions open up and feel more receptive to
help. Counselors should not avoid asking such
questions out of fear that asking them will “put
the idea” of suicide into their clients’ minds; this
is simply not true.
Counselors should also be prepared to probe the
client’s likelihood of inflicting harm on another
person. Specifically, counselors should ask
questions that establish whether homicidal
ideation, plans, means, access, and protective
factors are present. Also ask about past expe-
riences and future expectations. Questions can
include the following:
•
“Have you had any thoughts of harming
others?”
•
“Have you had any thoughts of harming anyone
specific? Who?”
•
“If you decided to harm (name of person), how
would you do it?”
•
“On a scale of 0 to 10, with 0 meaning ‘not
likely at all,’ how likely are you to harm this
person in the next week?”
•
“What reasons do you have to not harm this
person? What might stop you from harming
him/her?”
•
“What else could you do to deal with your anger
(or name whatever other feelings the client
reports feeling) instead of harming this person?”
•
“In the past, have you acted on thoughts of
harming someone? What happened?”
•
“How might your life change if you harm this
person? What might happen to you or to your
family? What might happen to this person’s
family?”
•
“Would you be willing to agree to tell someone
before you do this?”
•
“How confident are you in remaining sober over
the next week? What can you do to increase the
chances you will remain sober? (for example, use
of 12-Step meetings, supports, or treatment).”
Screening for Risk of Violence
The U.S. Preventive Services Task Force (USPSTF)
recommends that providers routinely screen all
women of childbearing age for risk of intimate
partner violence (USPSTF, 2016). Similarly,
addiction counselors and mental health counselors
should be vigilant for risk of victimization among
female clients, although men too can and do
experience intimate partner violence and should
be screened if counselors suspect victimization.
The screener recommended for high sensitivity
and specificity (Arkins, Begley, & Higgins, 2016;
USPSTF, 2016) is called Humiliation, Afraid, Rape,
and Kick. This four-question tool (which has been
validated only for women) screens for emotional,
physical, and sexual violence (Sohal, Eldridge, &
Feder, 2007). See Appendix C for the tool.
Screening for Past and Present Mental
Disorders
Screening for past and present mental disorders
accomplishes three goals:
1. To understand a client’s history and, if the
history is positive for a mental disorder, to
alert the counselor and treatment team to the
types of symptoms that may reappear so that
the counselor, client, and staff can watch out for
the emergence of any such symptoms.
2. To identify clients who may have a current
mental disorder and need assessment to
determine the nature of the disorder and an
evaluation to plan for its treatment.
3. To determine the nature of the symptoms
that may increase and decrease to help clients
with current CODs monitor their symptoms—
especially how the symptoms improve or
worsen in response to medications, “slips” (i.e.,
substance use), and treatment interventions. For
example, clients often need help seeing that the
treatment goal of avoiding isolation improves
their mood. So, when they call their sponsor
and go to a meeting, they break the cycle of
depressed mood, seclusion, dwelling on oneself
Chapter 3 48
TIP 42
Chapter 3—Screening and Assessment of Co-Occurring Disorders
and one’s mood, increased depression, and
other symptoms or consequences of depression.
Several screening, assessment, and treatment
planning tools are available to assist the SUD
treatment team (see Appendix C). Hundreds of
assessment and treatment planning tools exist for
assessment of specific disorders and for differential
diagnosis and treatment planning. The National
Institute on Alcohol Abuse and Alcoholism offers
professional education materials that address
screening and assessment for alcohol misuse,
including links to several screening instruments
(www.niaaa.nih.gov/publications/clinical-guides-
and-manuals). A NIDA research report (NIDA,
2018a) provides broad background information
on assessment processes pertinent to CODs and
specific information on many mental disorders,
treatment planning, and substance misuse
tools. The mental health field contains a vast
array of screening and assessment devices, and
subfields are devoted primarily to the study and
development of evaluative methods.
Almost all SAMHSA TIPs, available online
(https://store.samhsa.gov/series/tip-series-
treatment-improvement-protocols-tips), have a
section on assessment; many have appendixes
with wholly reproduced assessment tools or
information about locating such tools.
Advanced assessment techniques include
assessment instruments for general and specific
purposes and advanced guides to differential
diagnosis. Most highpower assessment techniques
center on a specific type of problem or set of
symptoms, are typically lengthy, often require
specific doctoral training to use, and can be
difficult to adapt properly for some SUD treatment
settings. For these reasons, such assessments are
not included in this publication.
When using any of the wide array of tools that
detect symptoms of mental disorders, counselors
should bear in mind that symptoms of a mental
disorder can be mimicked by substances. For
example, hallucinogens may produce symptoms
that resemble psychosis, and depression commonly
occurs during withdrawal from many substances.
Even with well-tested tools, distinguishing between
a mental disorder and a substance-related disorder
can be difficult without additional information
such as the history and chronology of symptoms.
In addition to interpreting the results of such
instruments in the broader context of what is
known about the client’s history, counselors are
also reminded that retesting often is important,
particularly to confirm diagnostic conclusions for
clients who have used substances.
The next section briefly highlights some instruments
available for mental disorder screening.
Mental Health Screening Tools
MHSF-III
MHSF-III (Exhibit 3.7) has only 17 simple questions
and is designed to screen for present or past
symptoms of most major mental disorders (Carroll
& McGinley, 2001). The MHSF-III was developed in
an SUD treatment setting, and it has face validity—
that is, if a knowledgeable diagnostician reads each
item, it is clear that a “yes” would warrant further
evaluation of the client for the mental disorder for
which the item represents typical symptomatology.
It has been used as a part of integrated behavioral
health and physical health services (Chaple, Sacks,
Randell, & Kang, 2016) and in behavioral health
courts (Miller & Khey, 2016). The MHSF-III is
reprinted in Appendix C.
The MHSF-III is only a screening device, because
it asks only one question for each disorder for
which it attempts to screen. If a client answers “no”
because of a misunderstanding of the question or a
momentary lapse in memory focus, the screen will
produce a “false negative.” This means the client
might have the mental disorder, but the screen
falsely indicates that he or she probably does not
have the disorder.
The MHSF-III is scored by totaling the “yes”
responses (1 point each), for a maximum score
of 17. A “yes” response to any of the items on
questions 3 through 17 suggests that a qualified
mental health specialist should be consulted
to determine whether follow-up, including a
diagnostic interview, is warranted.
Chapter 3 49

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
EXHIBIT 3.7. Mental Health Screening Form-III
Please circle “yes” or “no” for each question.
1. Have you ever talked to a psychiatrist, psychologist, therapist, social worker, or counselor Yes No
about an emotional problem?
2. Have you ever felt you needed help with your emotional problems, or have you had Yes No
people tell you that you should get help for your emotional problems?
3. Have you ever been advised to take medication for anxiety, depression, hearing voices, or Yes No
for any other emotional problem?
4. Have you ever been seen in a psychiatric emergency room or been hospitalized for Yes No
psychiatric reasons?
5. Have you ever heard voices no one else could hear or seen objects or things which others Yes No
could not see?
6. (a) Have you ever been depressed for weeks at a time, lost interest or pleasure in most Yes No
activities, had trouble concentrating and making decisions, or thought about killing
yourself?
Yes No
(b) Did you ever attempt to kill yourself?
7. Have you ever had nightmares or flashbacks as a result of being involved in some Yes No
traumatic/terrible event? For example, warfare, gang fights, fire, domestic violence, rape,
incest, car accident, being shot or stabbed?
8. Have you ever experienced any strong fears? For example, of heights, insects, animals, dirt, Yes No
attending social events, being in a crowd, being alone, being in places where it may be
hard to escape or get help?
9. Have you ever given in to an aggressive urge or impulse, on more than one occasion, that Yes No
resulted in serious harm to others or led to the destruction of property?
10. Have you ever felt that people had something against you, without them necessarily Yes No
saying so, or that someone or some group may be trying to influence your thoughts or
behavior?
11. Have you ever experienced any emotional problems associated with your sexual interests, Yes No
your sexual activities, or your choice of sexual partner?
12. Was there ever a period in your life when you spent a lot of time thinking and worrying Yes No
about gaining weight, becoming fat, or controlling your eating? For example, by
repeatedly dieting or fasting, engaging in much exercise to compensate binge eating,
taking enemas, or forcing yourself to throw up?
13. Have you ever had a period of time when you were so full of energy and your ideas came Yes No
very rapidly, when you talked nearly nonstop, when you moved quickly from one activity
to another, when you needed little sleep, and when you believed you could do almost
anything?
14. Have you ever had spells or attacks when you suddenly felt anxious, frightened, or uneasy Yes No
to the extent that you began sweating, your heart began to beat rapidly, you were shaking
or trembling, your stomach was upset, or you felt dizzy or unsteady, as if you would faint?
Continued on next page
Chapter 3 50
TIP 42
Chapter 3—Screening and Assessment of Co-Occurring Disorders
Continued
15. Have you ever had a persistent, lasting thought or impulse to do something over and over
that caused you considerable distress and interfered with normal routines, work, or social
relations? Examples would include repeatedly counting things, checking and rechecking
on things you had done, washing and rewashing your hands, praying, or maintaining a
very rigid schedule of daily activities from which you could not deviate.
Yes No
16. Have you ever lost considerable sums of money through gambling or had problems at
work, in school, or with your family and friends as a result of your gambling?
Yes No
17. Have you ever been told by teachers, guidance counselors, or others that you have a
special learning problem?
Yes No
Source: Carroll & McGinley (2000). The MHSF-III may be reproduced or copied, in entirety, without permission.
Counselors should bear in mind that symptoms
of substance misuse can mimic symptoms of
mental disorders.
Modied Mini Screen
The Mini-International Neuropsychiatric Interview
(M.I.N.I.) is a simple tool that takes 15 to 30
minutes to administer and that covers 20 mental
disorders and SUDs. Considerable validation
research exists on the M.I.N.I. (Sheehan et
al., 1998). However, a modified version of the
M.I.N.I.—the Modified Mini Screen (MMS)—that
contains only 22 items can be used to screen
even more quickly for mental disorders in three
diagnostic areas: mood disorders, anxiety
disorders, and psychotic disorders. The MMS
has been validated for use with adults in SUD
treatment, social service, and criminal justice
settings (Alexander, Layman, & Haugland, 2013;
SAMHSA, 2015b).
ASI
The ASI (McLellan et al., 1992) does not screen for
mental disorders and provides only a lowpower
screen for generic mental health concerns. Use
of the ASI ranges widely. Some SUD treatment
programs use a scaleddown approach to gather
basic information about a client’s alcohol use;
drug use; legal status; and employment, family/
social, medical, and psychiatric status. Other
programs use the ASI as an indepth assessment
and treatment planning instrument, with a trained
interviewer administering it and making complex
judgments about the client’s presentation and
attitudes about and willingness to take the
ASI. Counselors can be trained to make clinical
judgments about how the client comes across,
how genuine and legitimate the client’s way of
responding seems, whether there are any safety or
selfharm concerns requiring further investigation,
and where the client falls on a nine-point scale for
each dimension.
With about 200 items, the ASI is a lowpower
instrument with a broad range, covering the seven
areas mentioned previously and requiring about
1 hour to complete. The continuing development
of and research into the ASI includes training
programs, computerization, and critical analyses.
It is a public domain document that has been
used widely for two decades. It has been found
to be effective in predicting inpatient psychiatric
admissions among people seeking SUD treatment
(Drymalski & Nunley, 2016).
DSM-5 Cross-Cutting Symptom Measure
Among the major revisions to DSM-5 was the
inclusion of a newly developed patient assessment
tool to help providers screen for common mental
Chapter 3 51

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
disorders and symptoms needing treatment,
including major depression, generalized anxiety,
mania, somatic conditions, sleep disturbance,
cognitive dysfunction, and substance misuse. The
DSM-5 Self-Rated Level 1 Cross-Cutting Symptom
Measure—Adult contains 23 items that correspond
to diagnostic categories in DSM-5 (e.g., depressive
disorders, psychotic disorders) or to specific symptom
domains (e.g., mania, anger, suicidal ideation).
Because the screener is included in DSM-5’s
Section III for “emerging measures,” meaning
it requires further research before being
implemented in routine clinical practice, little
is known about its validation. No published
studies to date have examined its use with
COD populations. Nonetheless, the measure is
worthy of consideration, especially in research
settings. It is available online with scoring
information (https://www.psychiatry.org/
psychiatrists/practice/dsm/educational-resources/
assessment-measures#Disorder).
Screening for Past and Present SUDs
This section is intended primarily for counselors
working in mental health service settings and
suggests ways to screen clients for substance misuse.
Screening begins with inquiry about past and
present substance use and related problems and
disorders. If the client answers “yes” to having
problems or a disorder, further assessment is
warranted. If the client acknowledges a past
substance problem but states that it is now
resolved, assessment is still required. Careful
exploration of what current strategies the individual
is using to prevent relapse is warranted. Such
information can help ensure that the individual
continues to use those strategies while focusing on
mental health services.
Screening for the presence of substance misuse
involves four components, which are:
•
Substance misuse symptom checklists.
•
Substance misuse severity assessment.
•
Formal screening tools that work around denial.
•
Screening of urine, saliva, or hair samples.
Symptom Checklists
Checklists address common categories of
substances, problems associated with use for a
given substance, and a history of meeting SUD
criteria. Overly detailed checklists are unhelpful;
they lose value as simple screening tools. Including
misuse of over-the-counter medication (e.g., cold
medications) and of prescribed medication is
helpful.
Severity Assessment
Monitor the severity of an SUD (if present). This
process can begin with simple questions about
past or present diagnosis of an SUD and the
client’s experience of associated difficulties.
DSM-5 offers guidance on assessing SUD severity
based on symptom count. Specifically, two to
three symptoms would be considered a mild SUD,
four or five a moderate SUD, and six or more a
severe SUD (American Psychiatric Association
[APA], 2013). Some programs may use formal SUD
diagnostic tools; others use the ASI (McLellan et
al., 1992) or similar instruments, even in the mental
disorder service setting.
SCREENING AND
INTOXICATIONWITHDRAWAL
Counselors cannot formally screen or assess
clients who are actively intoxicated. If clients are
obviously intoxicated, treat them with empathy
and firmness, and ensure their physical safety.
If clients report that they are experiencing
withdrawal, or appear to be exhibiting signs
of withdrawal, formal withdrawal scales
can help even inexperienced providers
gather information from which medically
trained personnel can determine if medical
intervention is required. Such tools include
the Clinical Institute Withdrawal Assessment
of Alcohol Scale, Revised (Sullivan, Sykora,
Schneiderman, Naranjo, & Sellers, 1989) for
alcohol withdrawal and the Clinical Institute
Narcotic Assessment (Zilm & Sellers, 1978)
for opioid withdrawal. These are included in
Appendix C.
Chapter 3 52

TIP 42Chapter 3—Screening and Assessment of Co-Occurring Disorders
Substance Misuse Screening Tools
answers as at risk on the Quick Screen, the full
NIDA-Modified ASSIST should be administered.
AUDIT and AUDIT-C
The AUDIT (Babor, Higgins-Biddle, Saunders,
& Monteiro, 2001) and its abbreviated version,
the AUDIT-C (Bush, Kivlahan, McDonell, Fihn, &
Bradley, 1998), have been validated for use in
screening adults at risk for alcohol misuse (Dawson,
Smith, Saha, Rubinsky, & Grant, 2012; Johnson,
Lee, Vinson, & Seale, 2013). These instruments
measure current alcohol use, drinking behaviors,
and consequences of drinking. Cutoff scores
suggesting hazardous alcohol use are 8 or higher
on the AUDIT (Babor et al., 2001) and 3 or higher
on the AUDIT-C for SUD or heavy drinking (Bush et
al., 1998). Both measures are in Appendix C.
DAST-10
CAGE-AID
The CAGE-AID (Cut Down, Annoyed, Guilty, Eye-
opener—Adapted to Include Drugs) is a variation
of the four-question CAGE screener, which focuses
solely on detecting alcohol misuse. The CAGE-AID
instead screens for drug use and alcohol misuse. It
is brief, valid, and reliable (Mdege & Lang, 2011),
and recommended by the USPSTF and others for
substance misuse screening, particularly in primary
care populations (Halloran, 2013; Lanier & Ko,
2008). Respondents who endorse one or more
items on the CAGE-AID should be considered
for full assessment of substance misuse. The
CAGE-AID is online at https://www.hiv.uw.edu/
page/substance-use/cage-aid.
NIDA-Modied ASSIST
WHO’s ASSIST tool (WHO ASSIST Working
Group, 2002) is an effective measure for lifetime
and current substance misuse, but its length and
complex computer scoring system have hindered
its widespread adoption. NIDA developed an
abbreviated version called the NIDA-Modified
ASSIST, which is recommended by APA for use
with DSM-5 (NIDA, 2015) and is recommended for
primary care as well as general medical populations
(NIDA, 2012; Zgierska, Amaza, Brown, Mundt, &
Fleming, 2014).
The NIDA-Modified ASSIST can be completed
online (www.drugabuse.gov/nmassist/) or on paper.
It opens with a Quick Screen to determine whether
further assessment is warranted. If the client
The DAST-10 (Skinner, 1982) is a moderately-to-
highly reliable and valid measure that has been
widely used in practice and research (Mdege &
Lang, 2011; Yudko, Lozhkina, & Fouts, 2007). It
assesses past-year use of substances other than
alcohol and can be administered quickly. Scores
of 3 or higher warrant consideration of further
assessment for a possible SUD (Skinner, 1982). The
DAST-10 can be accessed online (https://www.hiv.
uw.edu/page/substance-use/dast-10).
MAST
The MAST (Selzer, 1971) is a widely used self-
report screening tool for problematic substance
use. A systematic review of its psychometric
properties suggests the MAST is moderate to
robust in reliability and validity (Minnich, Erford,
Bardhoshi, & Atalay, 2018).
This 25-item measure asks about lifetime alcohol
use and consequences. It takes 8 to 10 minutes to
complete. A score of 0 to 3 suggests no drinking
problems. A score of 4 suggests early or moderate
problems. A score of 5 or higher indicates problem
drinking and warrants further assessment. See
Appendix C for the measure.
SSI-SA
Developed by CSAT, the SSI-SA (CSAT, 1994)
screens for alcohol consumption and other
substance use, preoccupation and loss of control,
negative consequences of substance use, problem
recognition, and tolerance and withdrawal.
The SSI-SA has strong psychometric properties
(Boothroyd, Peters, Armstrong, Rynearson-Moody,
& Caudy, 2015) and includes items drawn from
existing validated substance screeners, including
the AUDIT, CAGE, DAST, and MAST. It is often
used in criminal justice settings (SAMHSA, 2015b)
but also has been found effective in hospital
settings (Mdege & Lang, 2011). A score of 4 or
higher is considered indicative of moderate to
high risk of substance misuse and warrants further
assessment (Boothroyd et al., 2015). See Appendix
C for this instrument.
Chapter 3 53

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
Trauma Screening
Trauma refers to an event or circumstance
experienced, witnessed, or learned of by an
individual that has a protracted, negative influence
on his or her physical, emotional, psychological,
social, spiritual, or functional well-being. Common
traumatic events include childhood maltreatment
(e.g., physical, sexual, or emotional abuse; neglect);
being a victim of physical or sexual assault;
experiencing a terrorist event, natural or man-made
disaster, accident, fire, or mass casualty event;
repeatedly being exposed to details of horrific
or violent events (e.g., first responders seeing
injured or dead victims, police officials repeatedly
hearing details about child abuse); or learning that
something extremely disturbing happened to a
loved one or close friend (e.g., learning that your
child has died).
Trauma is common in individuals with SUDs,
mental disorders, or both, particularly women and
military populations (Berenz & Coffey, 2012; Carter,
Capone, & Short, 2011; Gilmore et al., 2016; Kline
et al., 2014; Konkoly Thege et al., 2017; Mandavia,
Robinson, Bradley, Ressler, & Powers, 2016;
Mason & Du Mont, 2015; Palmer et al., 2016; Vest,
Hoopsick, Homish, Daws, & Homish, 2018; Walsh,
McLaughlin, Hamilton, & Keyes, 2017; see also
Chapter 4 for more discussion).
To determine whether trauma screening is
warranted, counselors can ask clients about past
traumatizing events directly or use a structured
tool, like the Adverse Childhood Experiences
Study Score Calculator (available online at https://
acestoohigh.com/got-your-ace-score/). In screening
for a history of trauma or obtaining a preliminary
diagnosis of PTSD, asking clients to describe
traumatic events in detail can be traumatizing. Limit
questioning to very brief and general questions,
such as “Have you ever experienced childhood
physical abuse? Sexual abuse? A serious accident?
Violence or the threat of it? Have there been
experiences in your life that were so traumatic they
left you unable to cope with day-to-day life?”
To screen for PTSD, assuming the client has a
positive trauma history, consider using these scales:
•
The Primary Care PTSD Screen for DSM-5 (Prins
et al., 2015) and administration and scoring
information are available online (www.ptsd.
va.gov/professional/assessment/documents/pc-
ptsd5-screen.pdf).
•
The PTSD Checklist for DSM-5 (Weathers
et al., 2013) and administration and scoring
information are available online (https://www.
ptsd.va.gov/professional/assessment/adult-sr/
ptsd-checklist.asp).
See TIP 57, Trauma-Informed Care in Behavioral
Health Services (SAMHSA, 2014b), for more indepth
discussion of screening, assessment, and manage-
ment of trauma in behavioral health populations.
Valuable guidance about counseling people with
CODs and trauma is in Chapter 7 of this TIP.
Assessment Step 4: Determine Quadrant
and Locus of Responsibility
Quadrants of care (i.e., Four Quadrants Model) is a
conceptual framework that classifies clients in four
basic groups based on relative symptom severity,
not diagnosis (Exhibit 3.8).
Quadrant assignment is based on the severity of
the mental disorders and SUDs as follows:
•
Category/Quadrant I: This quadrant includes
individuals with low-severity substance misuse
and low-severity mental disorders. These
low-severity individuals can be accommodated
in intermediate outpatient settings of either
mental disorder or chemical dependency
programs, with consultation or collaboration
between settings if needed. Alternatively,
some people will be identified and managed
in primary care settings with consultation
from mental health service or SUD treatment
providers.
•
Quadrant II: This quadrant includes individuals
with high-severity mental disorders who are
usually identified as priority clients within the
mental health system and who also have low-
severity SUDs (e.g., SUD in remission or partial
remission). These individuals ordinarily receive
continuing care in the mental health system
and are likely to be well served in a variety of
intermediate-level mental health programs using
integrated case management.
Chapter 3 54
TIP 42
Alcohol and Drug Use Disorders
Category IV
Mental disorders more severe
SUDs more severe Locus of care
State hospitals, jails/prisons,
emergency rooms, etc.
Mental disorders more severe
SUDs less severe Locus of care
Mental health system
high
severity
low
severity
Category III
Mental disorders less severe
SUDs more severe Locus of care
SUD Treatment System
Category I
Mental disorders less severe
SUDs less severe Locus of care
Primary healthcare settings
Mental Illness
Category II
high
severity
Chapter 3—Screening and Assessment of Co-Occurring Disorders
EXHIBIT 3.8. Level of Care Quadrants
•
Quadrant III: This quadrant includes
individuals who have severe SUDs and low- or
moderate-severity mental disorders. They are
generally well accommodated in intermediate-
level SUD treatment programs. In some cases,
coordination and collaboration with affiliated
mental health programs are needed to provide
ongoing treatment of the mental disorders.
•
Quadrant IV: Quadrant IV has two subgroups.
One includes people with serious, persistent
mental illness (SPMI) who also have severe
and unstable SUDs. The other includes people
with severe and unstable SUDs and severe and
unstable behavioral problems (e.g., violence,
suicidality) who do not (yet) meet criteria for
SPMI. These individuals require intensive,
comprehensive, and integrated services for both
their SUDs and mental disorders. The locus of
treatment can be specialized residential SUD
treatment programs such as modified therapeutic
communities in state hospitals, jails, or even
in settings that provide acute care such as
emergency departments (EDs).
The quadrants of care were derived from a con-
ference, the National Dialogue on Co-Occurring
Mental Health and Substance Abuse Disorders,
supported by SAMHSA and two of its centers—
CSAT and the Center for Mental Health Services—
and co-sponsored by the National Association of
State Mental Health Program Directors (NASMHPD)
and the National Association of State Alcohol
and Drug Abuse Directors (NASADAD). The
quadrants of care model was originally developed
by Ries (1993) and used by the State of New York
(NASMHPD & NASADAD, 1999; see also Rosenthal,
1992). It has two distinct uses:
•
To help conceptualize an individual client’s
treatment and to guide improvements in system
integration (for example, if the client has acute
psychosis and is known to the treatment staff
to have a history of alcohol use disorder (AUD),
the client will clearly fall into Category IV—that
is, severe mental disorder and severe SUD).
However, the severity of the client’s needs,
diagnosis, symptoms, and impairments all
determine level of care placement.
•
To guide improvements in systems integration,
including efficient allocation of resources.
The model is considered valid, reliable, and
feasible (McDonell et al., 2012), which is
Chapter 3 55

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
particularly beneficial for clients with CODs
given that conditions tend to fluctuate over time,
underscoring the need for a stable framework that
can accurately classify individuals and capture their
potential treatment needs throughout the course
of their illnesses.
Step 2 will collect most information necessary
to make this determination, but there will
sometimes be additional nuances to consider.
Certain states formally specify procedures for
quadrant determination. In the absence of formal
procedures, SUD treatment providers in any setting
can follow Exhibit 3.8.
Determination of SMI Status
Every state mental health system has developed
a set of specific criteria for determining who can
be considered seriously mentally ill and therefore
eligible to be considered a mental health priority
client. These criteria are based on combinations
of specific diagnoses, severity of disability, and
duration of disability (usually 6 months to 1 year).
Some require that the condition be independent of
an SUD. These criteria are different for every state.
It would be helpful for SUD treatment providers to
obtain copies of the criteria for their own states, as
well as copies of the specific procedures by which
eligibility is established by their states’ mental health
systems. By determining that a client might be
eligible for consideration as a mental health priority
client, the SUD treatment counselor can assist the
client in accessing various services and benefits the
client may not know are open to her or him.
To gauge SMI status, start by asking whether
the client already gets mental health priority
services (e.g., “Do you have a mental health case
manager?” “Are you a Department of Mental
Health client?”).
•
If the client already is a mental health client,
then he or she will be assigned to quadrant II
or IV. Contact the mental health case manager
and establish collaboration to promote case
management.
•
If the client is not already a mental health client
but appears to be eligible, and the client and
family are willing, arrange a referral for eligibility
determination.
•
Clients who present in SUD treatment settings
who look as if they might have SMI, but have
not been so determined, should be considered
to belong to quadrant IV.
For assistance in determining the severity of
symptoms and disability, the SUD treatment
provider can use the severity criteria listed
in DSM-5. For disorders in which DSM-5 does
not offer any guidance on determining severity,
counselors can use Dimension 3 (Co-Morbidity)
subscales in the LOCUS (see the section
“Assessment Step 5: Determine Level of Care”),
particularly the levels of severity of comorbidity
and impairment/functionality.
Determination of Severity of SUDs
Presence of active or unstable substance misuse
or serious substance misuse as indicated by a
DSM-5 severity rating of “severe” would identify
the individual as being in quadrant III or IV. Less
serious SUD (a DSM-5 severity rating of “mild” or
“moderate”) identifies the individual as being in
quadrant I or II.
If the client is determined to have SMI with a
serious SUD, he or she falls in quadrant IV; those
with SMI and a mild SUD fall in quadrant II. A
client with a serious SUD who has mental disorder
symptoms that do not constitute SMI falls into
quadrant III. A client with mild to moderate mental
disorder symptoms and a less serious SUD falls into
quadrant I.
Clients in quadrant III who present in SUD
treatment settings are often best managed by
receiving care in the SUD treatment setting, with
collaborative or consultative support from mental
health providers. Individuals in quadrant IV usually
require intensive intervention to stabilize and
determine eligibility for mental health services
and appropriate locus of continuing care. If they
do not meet SMI criteria, once their more serious
mental symptoms have stabilized and substance
use is controlled initially, they begin to look like
individuals in quadrant III, and can respond to
similar services.
Note, however, that this discussion of quadrant
determination is not validated by clinical research.
It is merely a practical approach to adapting an
Chapter 3 56
TIP 42
Chapter 3—Screening and Assessment of Co-Occurring Disorders
ASSESSMENT STEP 5APPLICATION TO CASE EXAMPLES JANE B.
Jane B. is a 28-year-old single White woman diagnosed with paranoid schizophrenia, AUD, and
cocaine use disorder. She has a history of multiple episodes of sexual victimization. She is experiencing
homelessness (living in a shelter), is actively psychotic, and will not admit to substance misuse. She often
visits the local ED for mental and medical complaints but refuses follow-up treatment. Her main requests
are for money and food, not treatment. Jane has been offered involvement in a housing program that
requires no treatment engagement or sobriety but has refused because of paranoia about working
with staff in this setting. Jane B. declines medication, given her paranoia, but does not seem acutely
dangerous to herself or others.
The severity of Jane B.’s condition and her psychosis, homelessness, and lack of stability may lead the
provider initially to consider psychiatric hospitalization or referral for residential SUD treatment. In
fact, application of assessment criteria in the LOCUS might have led easily to that conclusion. In the
LOCUS, more flexible matching is possible. The first consideration is whether the client meets criteria for
involuntary psychiatric commitment (usually, suicidal or homicidal impulses, or inability to feed oneself
or obtain shelter). In this instance, she is psychotic and experiencing homelessness but has been able to
find food and shelter; she is unwilling to accept voluntary mental health services. Further, residential SUD
treatment is inappropriate, both because she is completely unmotivated to get help and because she is
likely to be too psychotic to participate in treatment effectively. The LOCUS would therefore recommend
Level 3 – “High Intensity Community Based Services.”
If after extended participation in the engagement strategies described earlier, she began to take
antipsychotic medication, after some time her psychosis might clear up, and she might begin to express
interest in getting sober. In that case, if she had determined that she is unable to get sober on the street,
residential SUD treatment would be indicated. Because of the longstanding severity of her mental illness,
she likely would continue to have some level of symptoms of her mental disorder and disability even
when medicated. In this case, Jane B. probably would require a residential program able to supply an
enhanced level of services.
existing framework for clinical use, in advance of
more formal processes being developed, tested,
and disseminated.
In many systems, the process of assessment
stops largely after assessment Step 4 with the
determination of placement. Some information
from subsequent steps (especially Step 7) may be
included in this initial process, but usually more
indepth or detailed consideration of treatment
needs may not occur until after “placement” in an
actual treatment setting.
Assessment Step 5: Determine Level of Care
Client placement in the appropriate care setting for
his or her needs is necessary to optimize treatment
completion and desirable outcomes. Placing
a client in a level of care is also often required
by private and public payers (i.e., Medicaid) for
authorization of mental health services or SUD
treatment decisions. Thus, the availability of valid
and reliable commonly used tools can not only help
increase the odds of effective treatment matching
but can help providers meet documentation
requirements for reimbursement.
Tools for Determining Level of Care
LOCUS
The LOCUS Adult Version 20 (Sowers, 2016) can
be used as a systemwide level of care assessment
instrument for either mental disorder service
settings only or for both mental disorder service
and SUD treatment settings. The LOCUS uses
multiple dimensions of assessment, including:
•
Risk of harm.
•
Functional status.
•
Comorbidity (medical, addictive, psychiatric).
•
Recovery environment.
•
Treatment and recovery history.
•
Engagement and recovery status.
Chapter 3 57

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
The LOCUS (Plakun, 2018) helps:
•
Determine a client’s level of service needs.
•
Describe all levels of care, from short-term
outpatient services to inpatient residential care.
•
Provide a quantified approach to defining level
of care based on scores on its six dimensions.
LOCUS has a point system for each dimension
that permits aggregate scoring to suggest level of
service intensity. It permits level of care assessment
for clients with mental disorders or SUDs only, as
well as for those with CODs. It is highly correlated
with the DSM-IV-TR Global Assessment of
Functioning scale and has demonstrated good
sensitivity in assessing severity of symptoms,
particularly those that are psychiatric in nature
(Thurber, Wilson, Realmuto, & Specker, 2018).
Assessment Step 6: Determine Diagnosis
Determining the diagnosis can be a formidable
clinical challenge in the assessment of CODs.
Clinicians in both mental disorder services and SUD
treatment settings recognize that it can be impos-
sible to establish a firm diagnosis when confronted
with the mixed presentation of mental symptoms
and ongoing substance misuse. Of course,
substance misuse contributes to the emergence
or severity of mental symptoms and therefore
confounds the diagnostic picture. Therefore, this
step often includes dealing with confusing diagnos-
tic presentations. Three guiding principles can help
counselors thoroughly assess the client’s current
and past history of mental and substance-related
symptoms and problems:
1. Conduct a thorough interview to establish past
mental and SUD diagnoses and treatments.
2. Document all past diagnoses, including their
relationship to certain time periods (e.g., just
before the diagnosis, just after the diagnosis,
during symptomatic phases) and events,
symptoms, and levels of functioning during
those time periods.
3. Determine the timing of mental disorder
symptoms, particularly in relationship to periods
of substance use and SUDs (e.g., during periods
of abstinence, within 30 days of onset of an SUD).
Addiction counselors who want to improve their
competencies to address CODs are urged to
become conversant with the basic resource used
to diagnose mental disorders, DSM5 (APA, 2013).
Indepth discussion of what counselors need
to know concerning DSM-5 diagnostic criteria,
differential diagnosis, and management of mental
disorders in the context of co-occurring addiction
is in Chapter 4.
Principles of Determining Diagnosis
1. The Importance of Client History
Diagnosis is established more by history than
by current symptom presentation. This applies
to both mental disorders and SUDs. The first
step in determining the diagnosis is to determine
whether the client has an established diagnosis or
is receiving ongoing treatment for an established
disorder. This information can be obtained by the
counselor as part of the routine intake process. If
there is evidence of a disorder but the diagnosis
or treatment recommendations are unclear, the
counselor should immediately begin the process of
obtaining this information from collaterals. If there
is a valid history of a mental disorder diagnosis
at admission to SUD treatment, that diagnosis
should be considered presumptively valid for initial
treatment planning, and any existing stabilizing
treatment should be maintained. In addition to
confirming an established diagnosis, the client’s
history can provide insight into patterns that may
emerge and add depth to knowledge of the client.
For example, if a client comes into the clinician’s
office and says she hears voices (whether or not
she is sober currently), no diagnosis should be
made on that basis alone. People hear voices for
many reasons. They may be related to substance-
related syndromes (e.g., substance-induced
psychosis or hallucinosis, which is the experience
of hearing voices that the client knows are not
real, and that may say things that are distressing
or attacking—particularly when the client has a
history of trauma—but are not bizarre). With CODs,
most causes will be independent of substance
use (e.g., schizophrenia, schizoaffective disorder,
affective disorder with psychosis or dissociative
hallucinosis related to PTSD). Psychosis usually
involves loss of ability to tell that the voices are
Chapter 3 58

TIP 42
Chapter 3—Screening and Assessment of Co-Occurring Disorders
not real and increased likelihood that they are
bizarre in content. Methamphetamine psychosis
is particularly confounding because it can mimic
schizophrenia. Many clients with psychotic
disorders will still hear voices when on medication,
but the medication makes the voices less bizarre
and helps clients know they are not real.
If clients state, for example, that they have heard
voices, although not as much as they used to; have
been abstinent for 4 years; have remembered to
take medication most days, but may forget; and
have had multiple hospitalizations for psychosis
10 years ago but none since, then they clearly
have a diagnosis of psychotic illness (probably
schizophrenia or schizoaffective disorder). Given
their continuing symptoms while abstinent and on
medication, it is quite possible that the diagnosis
will persist.
Chapter 4 offers additional information about
differential diagnosis.
2. Documenting Prior Diagnoses
Even though SUD treatment counselors may not
be licensed to make a mental disorder diagnosis,
they should document prior diagnoses and gather
information related to current diagnoses.
Diagnoses established by history should not be
changed at the point of initial assessment. If the
clinician has a suspicion that a long-established
diagnosis may be invalid, he or she needs to take
time to gather additional information, consult with
collaterals, get more careful and detailed history,
and develop a better relationship with the client
before recommending diagnostic reevaluation.
The counselor should raise concerns related to
diagnosis with the clinical supervisor or at a team
meeting.
In many instances, no well-established mental
disorder diagnosis exists, or multiple diagnoses
confuse the picture. Even with an established
diagnosis, gathering information to confirm that
diagnosis is helpful. During initial assessment,
SUD treatment counselors can gather data that
can assist diagnosis, either by supporting the
findings of the existing mental health assessment
or by providing useful background information
in the event a new mental health assessment is
conducted. The key is not merely to gather lists
of past and present symptoms but to connect
those symptoms to periods in the client’s life that
are helpful in the diagnostic process—namely,
before the onset of an SUD and during periods
of abstinence (or very limited use) or after SUD
onset and persisting for more than 30 days.
The clinician should determine whether mental
disorder symptoms occur only when the client is
using substances actively. Therefore, it is important
to determine the nature and severity of the
symptoms of the mental disorder when the SUD
is stabilized. Note whether the client recently had
a complete physical, including appropriate labs.
Physical diseases can also present with or mimic
mental disorders (e.g., hypothyroidism presenting
with or like depression) and need to be identified
and treated accordingly.
3. Linking Mental Symptoms to Specic Periods
For diagnostic purposes, it is almost always
necessary to tie mental disorder symptoms to
specific periods of time in the client’s history, in
particular those times when an active SUD was
not present.
Most SUD assessment tools do not require
connection of mental disorder symptoms to
substance use or abstinence. Mental disorder
symptom information obtained from such tools
can confuse counselors and make them feel that
the whole process is not worth the effort. In fact,
when clinicians seek information about mental
disorder symptoms during periods of abstinence,
such information is almost never part of traditional
assessment forms. The mental disorder history
and substance use history have in the past been
collected separately and independently. As a result,
the opportunity to evaluate interaction, which is
the most important diagnostic information beyond
the history, has routinely been lost. Newer and
more detailed assessment tools overcome these
historical and potentially misleading divisions.
The M.I.N.I. Plus (a more detailed version of the
Mini-International Neuropsychiatric Interview
[Sheehan et al., 1998]) is structured to connect
any identified symptoms to periods of abstinence.
Clinicians can use this information to distinguish
substance-induced mental disorders from
Chapter 3 59

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
independent mental disorders. The Timeline Follow-
Back Method also is a valid and practical tool that
can be used with individuals with substance misuse
or CODs (Hjorthoj, Hjorthoj, & Nordentoft, 2012) to
gather a detailed and comprehensive assessment of
patterns of substance misuse beyond just quantity
and frequency.
Consequently, the SUD treatment counselor can
proceed in two ways:
•
Ask whether mental disorder symptoms or
treatments identified in screening were present
during periods of 30 days of abstinence
or longer, or were present before onset of
substance use. (“Did this symptom or episode
occur during a period when you were abstinent
for at least 30 days?”)
•
Define with the client specific time periods when
the SUD was in remission, and then get detailed
information about mental disorder symptoms,
diagnoses, impairments, and treatments during
those periods of time. (“Can you recall a time
when you were not using? Did these symptoms
[or whatever the client has reported] occur
during that period?”) This approach may yield
more reliable information.
During this latter process, the counselor can use
one of the medium-power symptom screening
tools as a guide. Alternatively, the counselor can
use the handy outlines of the DSM-5 criteria for
common disorders (provided in Chapter 4) and
inquire whether those criteria symptoms were met,
whether they were diagnosed and treated, and if
so, with what methods and how successfully. This
information can suggest or support the accuracy of
diagnoses. Documentation also can facilitate later
diagnostic assessment by a mental health–trained
clinician.
Assessment Step 7: Determine Disability
and Functional Impairment
Determination of both current and baseline
functional impairment contributes to identification
of the need for case management or higher
levels of support. This step also relates to the
determination of level of care requirements.
Assessment of current cognitive capacity, social
skills, and other functional abilities also is necessary
to determine whether there are deficits that may
require modification in the treatment protocols of
relapse prevention efforts or recovery programs.
For example, the counselor might inquire about
past participation in special education or related
testing.
Assessing Functional Capability
Current level of impairment is determined by
assessing functional capabilities and deficits
in each of the areas indicated in the following
list. Similarly, baseline level of impairment is
determined by identifying periods of extended
abstinence and mental health stability (greater than
30 days) according to the methods described in the
previous assessment step. The clinician determines:
•
Is the client capable of living independently (in
terms of independent living skills, not in terms
of maintaining abstinence)? If not, what types of
support are needed?
•
Is the client capable of supporting himself or
herself financially? If so, through what means?
If not, is the client disabled, or dependent on
others for financial support?
•
Can the client engage in reasonable social
relationships? Are there good social supports?
If not, what interferes with this ability, and what
supports would the client need?
•
What is the client’s level of cognitive
functioning? Is there a developmental or
learning disability? Are there cognitive or
memory impairments that impede learning?
Is the client limited in ability to read, write,
or understand? Is there difficulty focusing,
concentrating, and completing tasks?
Functional Assessment Tools
Several freely available, reliable, well-validated
tools measure functioning and impairment in
clients with mental illness, substance misuse, or
both (Gold, 2014; National Academies of Sciences,
Engineering, and Medicine, 2016; Sanchez-
Moreno, Martinez-Aran, & Vieta, 2017), including:
•
WHO Disability Assessment Schedule 2.0
([WHODAS 2.0] Üstün & WHO, 2010; www.
who.int/classifications/icf/whodasii/en/). When
DSM-5 removed the Global Assessment of
Functioning (Axis V in DSM-IV), APA proposed
Chapter 3 60

TIP 42
Chapter 3—Screening and Assessment of Co-Occurring Disorders
in its place the WHODAS 2.0 as a tool to rate
global impairment and functional capabilities
(APA, 2013). The WHODAS 2.0 assesses six
major domains, which are:
-
-
-
-
-
-
Understanding and communicating.
Getting around (mobility).
Self-care.
Getting along with people (social and
interpersonal functioning).
Life activities (home, academic, and
occupational functioning).
Participation in society (participation in family,
social, and community activities).
•
ASI (McLellan et al., 1992), a mental health
screening tool that provides information about
level of functioning for clients with SUDs. This
is valuable when supplemented by interview
information. (Note that the ASI also exists in an
expanded version specifically for women, ASI-F
[SAMHSA, 2009c].)
In a clinical interview, the counselor also should
inquire about any current or past difficulties
the client has had in learning or using relapse
prevention skills, participating in mutual-support
recovery programs, or obtaining medication
or following medication regimens. In the same
vein, the clinician may inquire about use of
transportation, budgeting, self-care, and other
related skills, and their effect on life functioning
and treatment participation.
For individuals with CODs, impairment may be
related to intellectual/cognitive ability or the
mental disorder, which may exist in addition to
the SUD. The clinician should establish level of
intellectual/cognitive functioning in childhood,
whether impairment persists, and if so, at what
level, during the periods when substance use is
in full or partial remission, just as in the previous
discussion of diagnosis.
Determining the Need for Capable or
Enhanced-Level Services
A specific tool to assess the need for capable- or
enhanced-level services for people with CODs
currently is not available. The consensus panel
recommends a process of “practical assessment”
that seeks to match the client’s assessment (mental
health, substance misuse, level of impairment)
to the type of services needed. The individual
may even be given trial tasks or assignments to
determine in concert with the counselor if his or
her performance meets the requirements of the
program being considered.
ASAM criteria for COD-capable and -eligible
programs are as follows (Mee-Lee, Shulman,
Fishman, Gastfriend, & Miller 2013):
•
Co-occurring–capable (COC) programs in
addiction treatment focus primarily on SUDs
but can treat patients with subthreshold or
diagnosable but stable mental disorders
(Mee-Lee et al., 2013). Mental health services
may be onsite or available by referral. COC
programs in mental health are those that
mainly focus on mental disorders but can treat
patients with subthreshold or diagnosable but
stable SUDs (Mee-Lee et al., 2013). Addiction
counselors are onsite or available through
referral.
•
Co-occurring–enhanced (COE) programs
have more integrated addiction and mental
health services and have staff who are trained
to recognize the signs and symptoms of both
disorders and are competent in providing
integrated treatment for both mental disorders
and SUDs at the same time.
•
Complexity-capable programs are designed
to meet the needs of individuals (and their
families) with multiple complex conditions
that extend beyond just CODs. Physical and
psychosocial conditions and treatment areas
of focus often include chronic medical illnesses
like HIV, trauma, legal matters, housing
difficulties, criminal justice system involvement,
unemployment, education concerns, childcare
or parenting difficulties, and cognitive
dysfunctions.
Assessment Step 8: Identify Strengths
and Supports
All assessment must include some specific
attention to the individual’s current strengths,
skills, and supports, both in relation to general
life functioning, and in relation to his or her ability
to manage either mental disorders or SUDs.
Chapter 3 61

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
This often provides a more positive approach to
treatment engagement than does focusing exclu-
sively on deficits that need to be corrected. This
is no less true for individuals with serious mental
disorders than it is for people with SUDs only.
Questions might focus on:
•
Talents and interests.
•
Areas of educational interest and literacy;
vocational skill, interest, and ability, such
as social skills or capacity for creative
self-expression.
•
Areas connected with high levels of motivation
to change, for either disorder or both.
•
Existing supportive relationships—treatment,
peer, or family—particularly ongoing mental
disorder treatment relationships.
•
Previous mental health services and SUD
treatment successes and exploration of what
worked.
•
Identification of current successes: What has the
client done right recently for either disorder?
•
Building treatment plans and interventions
based on utilizing and reinforcing strengths
and extending or supporting what has worked
previously.
ASSESSMENT STEP 8
APPLICATION TO CASE
EXAMPLES JANE B.
Jane B. expressed significant interest in
work once her paranoia subsided. She was
attempting to address her SUD on an outpatient
basis, as a residential treatment program was
unavailable. Her case management team
noted her interest and experience in caring
for animals. Via individualized placement and
support, they helped her obtain a part-time job
at a local pet shop two afternoons per week. She
was proud of her job and reported that it helped
maintain her motivation to stay away from
substances and to keep taking medication.
For individuals with SMI or substance misuse, the
Individualized Placement and Support model of
psychiatric rehabilitation has demonstrated that it is
a cost-effective way to generate positive vocational
and mental health outcomes compared with
other models of vocational rehabilitation for this
population, including improved rates of obtaining
competitive employment, greater number of hours
worked, increased wages, improvements in self-
esteem and quality of life, and reductions in mental
health service use (Drake, Bond, Goldman, Hogan,
& Karakus, 2016; LePage et al., 2016). In this
model, clients with disabilities who want to work
may be placed in sheltered work activities based
on strengths and preferences, even when actively
using substances and inconsistently complying
with medication regimens. In nonsheltered work
activities, it is critical to remember that many
employers have substance-free workplace policies.
Participating in ongoing jobs is valuable to self-
esteem in itself and can generate the motivation
to address mental disorders and substance misuse
problems, as they appear to interfere specifically
with work success. Taking advantage of educational
and volunteer opportunities also may enhance
self-esteem and is often a first step in securing
employment.
Assessment Step 9: Identify Cultural and
Linguistic Needs and Supports
Detailed cultural assessment is beyond the
scope of this publication. Cultural assessment of
individuals with CODs is not substantially different
from cultural assessment for those with SUDs or
mental disorders only, but some specific areas are
worth addressing, such as:
•
Problems with literacy.
•
Not fitting into the treatment culture (SUD or
mental health culture); conflict in treatment.
•
Cultural and linguistic service barriers.
Chapter 3 62
TIP 42
Chapter 3—Screening and Assessment of Co-Occurring Disorders
ASSESSMENT STEP 9APPLICATION TO CASE EXAMPLE GEORGE T.
The client is a 34-year-old married, employed African American man with cocaine use disorder, alcohol
misuse, and bipolar disorder (stabilized on lithium) mandated to cocaine treatment by his employer after
a failed drug test. George T. and his family realize he needs help not to use cocaine. He complains that his
mood swings intensify when he is using cocaine.
George T.’s counselor originally referred him to Cocaine Anonymous (CA). When George T. went, however,
he reported back to the counselor that he did not feel comfortable there. He felt that as a family man with
a responsible job, he had pulled himself out of the “street culture” that this specific meeting reflected. He
also noted that most participants were White. Unlike many people with CODs who feel more ashamed of
mental disorders than addiction, he felt more ashamed at the CA meeting than at his support group for
people with mental disorders. Therefore, for George T., it was culturally appropriate to address the shame
surrounding his substance use, encourage him to try other mutual-support program meetings, and
continue to provide positive feedback about his attendance at the support group for his mental disorder.
Not Fitting Into the Treatment Culture
To a certain degree, individuals with addiction
and SMI may have difficulty fitting into existing
treatment cultures. Many clients are aware of a
variety of different attitudes toward their disorders
that can affect relationships with others. Traditional
culture carriers (parents, grandparents) may have
different views of clients’ problems and the most
appropriate treatment compared with peers.
Individual clients may have positive or negative
allegiance to a variety of peer or treatment cultures
(e.g., mental health consumer movement, having
mild or moderate severity mental disorders vs. SMI,
12-Step or dual recovery mutual support) based on
past experience or on fears and concerns related to
the mental disorder. Specific questions to explore
with the client include:
•
“How are your substance use and mental health
concerns defined by your parents? Peers? Other
clients?”
•
“What do they think you should be doing to
remedy these problems?”
•
“How do you decide which suggestions to
follow?”
•
“In what kinds of treatment settings do you feel
most comfortable?”
•
“What do you think I (the counselor) should be
doing to help you improve your situation?”
Cultural and Linguistic Service Barriers
Cultural and linguistic barriers can compound
access to COD treatment. The assessment process
must address whether these barriers prevent
access to care (e.g., the client reads or speaks only
Spanish; the client is illiterate) and if so, determine
options for providing more individualized
intervention or for integrating intervention into
naturalistic culturally and linguistically appropriate
human service settings.
Chapter 5 describes components of culturally
responsive services. Chapter 6 offers information
about the needs of people of diverse racial/ethnic
backgrounds with CODs and how counselors
can help reduce treatment access and outcome
disparities experienced by marginalized racial/
ethnic groups.
Assessment Step 10: Identify Problem
Domains
Individuals with CODs may have difficulties
in multiple life domains (e.g., medical, legal,
vocational, family, social). The ASI can identify
and quantify substance use–related problems
across domains, to see which require attention.
It is used most effectively as a component of a
comprehensive assessment.
Chapter 3 63
TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
A comprehensive, biopsychosocial evaluation
for individuals with CODs requires clarifying how
each disorder interacts with the problems in each
domain, as well as identifying contingencies that
might promote treatment adherence for mental
health, SUD treatment, or both. Information about
others who might assist in the implementation
of such contingencies (e.g., probation officers,
family, friends) needs to be gathered, including
appropriate releases to obtain information.
Assessment Step 11: Determine Stage of
Change
A key evidence-based best practice for treatment
matching clients with CODs is to match
interventions not only to specific diagnoses but
also to stage of change and stage of treatment
for each disorder.
In SUD treatment settings, stage of change
assessment usually involves determination of
Prochaska and DiClemente Stages of Change:
precontemplation, contemplation, preparation
(or determination), action, maintenance, and
relapse (Prochaska & DiClemente, 1992). This
can involve using questionnaires such as the
University of Rhode Island Change Assessment
Scale (McConnaughy, Prochaska, & Velicer, 1983;
available at https://habitslab.umbc.edu/urica/) or
the Stages of Change Readiness and Treatment
Eagerness Scale (Miller & Tonigan, 1996; available
at https://casaa.unm.edu/inst/SOCRATESv8.pdf).
Stage of change can be determined clinically by
interviewing clients and evaluating their responses
in the context of change. For example, one
approach to stage of change identification is to ask
clients, for each problem, to select the statement
that most closely fits their view of that problem:
•
No problem, no interest in change, or both
(Precontemplation).
•
Might be a problem; might consider change
(Contemplation).
•
Definitely a problem; getting ready to change
(Preparation).
•
Actively working on changing, even if slowly
(Action).
•
Has achieved stability, and is trying to maintain
(Maintenance).
Stage of change assessment ideally will be applied
separately to each mental disorder and to each
SUD. For example, a client may be willing to take
medication for a depressive disorder but unwilling
to discuss trauma, or motivated to stop using
cocaine but unwilling to consider alcohol as a
problem.
For more indepth discussion of the stages of
change and motivational enhancement, see TIP 35,
Enhancing Motivation for Change in Substance Use
Disorder Treatment (SAMHSA, 2019c).
Assessment Step 12: Plan Treatment
A comprehensive assessment is the basis for
an individualized treatment plan. Appropriate
treatment plans and treatment interventions can
be quite complex, depending on what might be
discovered in each domain. No single, correct
intervention or program exists for individuals
with CODs. Rather, match appropriate
treatment to individual needs per these multiple
considerations.
The following case (Maria M.) illustrates how
the noted factors help generate an integrated
treatment plan that is appropriate to the needs and
situation of a particular client.
Chapter 3 64
TIP 42
Chapter 3—Screening and Assessment of Co-Occurring Disorders
ASSESSMENT STEP 12APPLICATION TO CASE EXAMPLE MARIA M.
The client is a 38-year-old Latina woman who is the mother of two teenagers. Maria M. presents with an
11-year history of cocaine dependence, a 2-year history of opioid dependence, and a history of trauma
related to a longstanding abusive relationship (now over for 6 years). She is not in an intimate relationship
at present and there is no current indication that she is at risk for either violence or self-harm. She also
has persistent major depression and panic treated with antidepressants. She is very motivated to receive
treatment.
Ideal Integrated Treatment Plan: The plan for Maria M. might include medication-assisted treatment
(e.g., methadone or buprenorphine), continued antidepressant medication, a mutual-support program,
and other recovery group support for cocaine dependence. She also could be referred to a group for both
SUD and trauma that is designed specifically to help reduce symptoms of trauma and resolve long-term
problems.
Individual, group, and family interventions could be coordinated by the primary counselor from opioid
maintenance treatment. The focus of these interventions might be on relapse prevention skills, taking
medication as prescribed, and identifying and managing trauma-related symptoms without using.
Considerations in Treatment
Matching
A major goal of the screening and assessment
process is to ensure the client is matched with
appropriate treatment. Acknowledging the
overriding importance of this goal, this discussion
of the process of clinical assessment for individuals
with CODs begins with a fundamental statement
of principle: Because clients with CODs are not
all the same, program placements and treatment
interventions should be matched individually to the
needs of each client.
The ultimate purpose of the assessment process is
to develop an appropriately individualized integrat-
ed treatment plan. In this model, the consensus
panel recommends the following approach:
•
Treatment planning for individuals with CODs
and associated problems should follow the
principle of mental disorder dual (or multiple)
primary treatment, in which a specific
intervention is matched to each problem or
diagnosis, as well as to stage of change and
external contingencies. Exhibit 3.9 shows
a sample treatment plan consisting of the
problem, intervention, and goal.
•
Integrated treatment planning involves helping
the client to make the best possible treatment
choices for each disorder and adhere to that
treatment consistently. At the same time, the
counselor needs to help the client adjust the
recommended treatment strategies for each
disorder as needed in order to take into account
problems related to the other disorder.
These principles are best illustrated by using a
case example to develop a sample treatment plan.
For this purpose, the case example for George T.
is used, incorporating the data gathered during
assessment (Exhibit 3.9). The problem description
presents various factors influencing the problem,
including stage of change and client strengths.
No specific person is recommended to carry out
interventions proposed in the second column,
as a range of professionals might carry out each
intervention appropriately.
The consensus panel has reviewed research
evidence and consensus clinical practice to identify
factors critical to the process of matching clients
to available treatment. Exhibit 3.10 lists these
considerations.
Chapter 3 65

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
EXHIBIT 3.9. Sample Treatment Plan for Case Example George T.
PROBLEM INTERVENTION GOAL
Cocaine use disorder
•
Work problem, primary reason
for referral
•
Family and work support
•
Resists mutual support
•
Mental symptoms trigger use
•
Action phase
Outpatient treatment
•
EAP monitoring
•
Family meetings
•
Address shame related to
disorder
•
Skill-building to manage
symptoms without using
•
Mutual-support meetings
Abstinence
•
Negative urinalysis results
•
Daily recovery plans
Rule out AUD
•
No clear problem
•
May trigger cocaine use
•
Precontemplation phase
•
Outpatient motivational
enhancement; thorough
evaluation of role of alcohol in
patient’s life, including family
education
•
Move into contemplation
•
Willing to consider the risk of
use or possible misuse
Bipolar disorder
•
Long history
•
On lithium
•
Some mood symptoms
•
Maintenance phase
•
Medication management
•
Help taking medication in
recovery programs
•
Bipolar Support Alliance
meetings
•
Advocate/collaborate with
prescribing health professional
•
Identify mood symptoms that
are triggers
•
Maintain stable mood
•
Able to manage fluctuating
mood symptoms that do occur
without using cocaine or other
substances to regulate his
bipolar disorder
EXHIBIT 3.10. Considerations in Treatment Matching
VARIABLE KEY DATA
Acute safety needs
Determines need
for immediate acute
stabilization to establish
safety prior to routine
assessment
•
Immediate risk of harm to self or others
•
Immediate risk of physical harm or abuse from others (Mee-Lee et al.,
2013)
•
Inability to provide for basic self-care
•
Medically dangerous intoxication or withdrawal
•
Potentially lethal medical condition
•
Acute severe mental disorder symptoms (e.g., mania, psychosis) leading to
inability to function or communicate effectively
Continued on next page
Chapter 3 66

TIP 42
Chapter 3—Screening and Assessment of Co-Occurring Disorders
Continued
Quadrant assignment
Guides the choice of the
most appropriate setting
for treatment
•
SPMI vs. non-SPMI
•
Severely acute or disabling mental disorder symptoms vs. mild-moderate
severity symptoms
•
High-severity SUD (e.g., active SUD) vs. lower severity SUD (e.g., hazardous
substance use)
•
Substance dependence in full vs. partial remission (Mee-Lee et al., 2013;
APA, 2013)
Level of care
Determines program
assignment
•
Dimensions of assessment for each disorder using criteria from the
LOCUS
Diagnosis
Determines the
recommended treatment
intervention
•
Specific diagnosis of each mental disorder and SUD, including distinction
of substance-induced symptoms
•
Information about past and present successful and unsuccessful
treatment efforts for each diagnosis
•
Identification of trauma-related disorders and culture-bound syndromes,
in addition to other mental disorders and substance-related problems
Disability
Determines case
management needs
and whether a standard
intervention is sufficient—
one at the capable or
intermediate level—or
whether an enhanced-level
intervention is essential
•
Cognitive deficits, functional deficits, and skill deficits that interfere with
ability to function independently or follow treatment recommendations
and which may require varying types and amounts of case management
or support
•
Specific functional deficits that may interfere with ability to participate in
SUD treatment in a particular program setting and may therefore require
a COE setting rather than a COC one
•
Specific deficits in learning or using basic recovery skills that require
modified or simplified learning strategies
Strengths and skills
Determines areas of prior
success around which to
organize future treatment
interventions
Determines skill-building
needs for management of
either disorder
•
Areas of particular capacity or motivation related to general life
functioning (e.g., capacity to socialize, work, or obtain housing)
•
Ability to manage treatment participation for any disorder (e.g., familiarity
and comfort with mutual-support programs, commitment to medication
adherence)
Availability and
continuity of recovery
support
Determines availability
of existing relationships
and whether to establish
continuing relationships
to provide contingencies
to promote learning
•
Presence or absence of continuing treatment relationships, particularly
mental disorder treatment relationships, beyond the single episode of
care
•
Presence or absence of an existing and ongoing supportive family,
peer support, or therapeutic community; quality and safety of recovery
environment (Mee-Lee et al., 2013)
Continued on next page
Chapter 3 67

TIP 42 Substance Use Disorder Treatment for People With Co-Occurring Disorders
Continued
Cultural context
Determines most
culturally appropriate
treatment interventions
and settings
•
Areas of cultural identification and support in relation to:
- Ethnic or linguistic culture identification (e.g., attachment to traditional
Native American cultural healing practices)
- Cultures that have evolved around treatment of mental disorders and
SUDs (e.g., identification with 12-Step and mutual recovery culture,
commitment to mental health empowerment movement)
•
Gender and gender identity
•
Sexual orientation
•
Rural vs. urban
Problem domains
Determines specific
problems to be solved
and opportunities for
contingencies to promote
treatment participation
Is there impairment, need, or strength in any of the following areas?
•
Financial
•
Legal
•
Employment
•
Housing
•
Social/family
•
Medical, parenting/child protective, abuse/victimization/victimizer
Phase of recovery/stage
of change (for each
problem)
Determines appropriate
phase-specific or stage-
specific treatment
intervention and
outcomes
•
Requirement for acute stabilization of symptoms, engagement, or
motivational enhancement
•
Active treatment to achieve prolonged stabilization
•
Relapse prevention/maintenance
•
Rehabilitation, recovery, and growth
•
Within the motivational enhancement sequence, precontemplation,
contemplation, preparation, action, maintenance, or relapse (Prochaska &
DiClemente, 1992)
•
Engagement, stabilization/persuasion, active treatment, or continuing
care/relapse prevention (Mueser & Gingerich, 2013; SAMHSA, 2009a)
Conclusion
Assessment is a systematic approach for behavioral
health service providers to gather information that
supports matched treatment plans for individuals
with CODs. It is a required competency and a key
component of the counselor–client relationship in
which providers learn to better understand their
clients; have opportunities to express genuine
concern, hope, and empathy for long-term
recovery; and help set the stage for effective
treatment. Most of these activities are already
a routine component of substance misuse-only
assessment; the key additional element is attention
to treatment requirements and stage of change
for mental disorders, and the possible interference
of mental disorder symptoms and disabilities
(including personality disorder symptoms) in SUD
treatment participation.
Chapter 3 68

Chapter 4—Mental and Substance-Related
Disorders: Diagnostic and Cross-Cutting Topics
KEY MESSAGES
TIP 42
SUBSTANCE USE DISORDER TREATMENT FOR
PEOPLE WITH CO-OCCURRING DISORDERS
• The co-occurrence of mental disorders with
substance use disorders (SUDs) is the rule, not
the exception. Addiction counselors should
expect and prepare to see clients with these
disorders in their settings.
• Addiction counselors generally do not
diagnose mental disorders. But to engage
in accurate treatment planning and to offer
comprehensive, efficacious, and responsive
services (or referral for such), clinicians must
be able to recognize the disorders most
likely to be seen in populations who misuse
substances.
• It is not always readily apparent whether a
co-occurring mental disorder is directly caused
by substance misuse or is an independent
disorder merely appearing alongside an SUD.
This differentiation can be difficult to make but
is critically important, as it informs treatment
decision making.
• Suicide and trauma are sadly common across
most combinations of co-occurring disorders
(CODs) and require special attention. Addiction
counselors have an ethical and professional
responsibility to keep clients safe and to provide
services that are supportive, empathic, and
person-centered, and that reduce suffering.
Disentangling symptoms of SUDs from those of
co-occurring mental disorders is a complex but
necessary step in correctly assessing, diagnosing,
determining level of service, selecting appropriate
and effective treatments, and planning follow-up
care. This chapter is designed to facilitate those
processes by ensuring addiction counselors and
other providers have a clear understanding of
mental disorder symptoms and diagnostic criteria,
their relationships with SUDs, and pertinent
management strategies.
This chapter provides an overview for working
with SUD treatment clients who also have mental
disorders. The audiences for this chapter are
counselors, other treatment/service providers,
Supervisors, and Administrators. It is presented
in concise form so that user can refer to this one
chapter to obtain basic information. The material
included is not a complete review of all mental
disorders and is not intended to be a primer on
diagnosis. Rather, it offers a summary of mental
disorders with special relevance to co-occurring
SUDs (see the section “Scope of the Chapter”).
Since the original publication of this Treatment
Improvement Protocol (TIP), updated mental
disorder criteria have been published in the
Diagnostic and Statistical Manual of Mental
Disorders (5th ed.; DSM-5; American Psychiatric
Association [APA], 2013). This chapter contains
these latest criteria and, where available, data from
prevalence studies and randomized controlled trials
in reflection of DSM-5.
Organization of the Chapter
The chapter begins with a brief description
of selected mental disorders and their DSM-5
diagnostic criteria. For each disorder, material
highlights some of the descriptive and diagnostic
features, prevalence statistics, and relationship
to SUDs. In general, the mental disorders in this
chapter are presented in the following descending
order by how commonly they co-occur with SUDs,
although this is not applied rigidly: Depressive
disorders, bipolar I disorder, posttraumatic stress
disorder (PTSD), personality disorders (PDs),
69

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
anxiety disorders, schizophrenia and psychosis,
attention deficit hyperactivity disorder (ADHD), and
feeding and eating disorders.
Because of the greater availability of case
histories from the mental health literature, the
illustrative material has more emphasis on the
mental disorders. Although not intended to offer
extensive guidance on treatment, this chapter’s
coverage of specific mental disorders does include
brief information about interventions for and
clinical approaches to managing CODs involving
each. (Chapter 7 focuses on treatment models for
people with CODs.) Case histories illustrate the
interaction between mental disorders and SUDs.
Each diagnostic topic contains an Advice to the
Counselor box containing key considerations
related to diagnosis, treatment, or both.
The next main section of this chapter addresses
substance-related disorders, including SUDs and
substance-induced mental disorders. (DSM-5
uses the term “substance/medication-induced
disorders”; this TIP focuses on nonmedication
substances and thus will exclude the term
“medication.”) Because the primary audience for
this chapter is addiction counselors, readers are
assumed to be highly familiar with SUDs and their
diagnostic criteria. Thus, the SUD section is briefer
than the mental disorders section. The overall focus
remains on substance-induced mental disorders,
their relationship to independent co-occurring
mental disorders, and what counselors need to
know in terms of assessment and treatment.
Licit and illicit drugs of misuse can cause
symptoms that are identical to the symptoms
of mental illness. Mental disorder diagnoses
should be provisional and reevaluated
constantly. Some mental disorders are
really substance-induced mental disorders,
meaning they are caused by substance use.
Treatment of the SUD and an abstinent period
of weeks or months may be required for a
definitive diagnosis of an independent, co-
occurring mental disorder. A fuller discussion of
substance-induced disorders is provided later
in this chapter.
The chapter ends with an overview of two concerns
that appear across nearly all COD populations:
suicidality and trauma. Although suicidality is
not strictly speaking a DSM-5-diagnosed mental
disorder, it is a high-risk behavior requiring serious
attention by providers. The discussion of suicidality
highlights key information addiction counselors
should know about risk of self-harm in combination
with substance misuse, mental disorders, or
both. The section offers factual information (e.g.,
prevalence data), commonly agreed-on clinical
practices, and other general information that may
be best characterized as “working formulations.”
Like suicide, trauma itself is not a mental disorder
but is extremely common in many psychiatric
conditions, frequently coincides with addiction, and
increases the odds of negative outcomes, including
suicide. Having at least a basic understanding
of suicide and trauma is a core competency for
addiction counselors working with clients who have
CODs and will help improve their ability to not only
offer effective services but keep clients safe.
Scope of the Chapter
The mental disorder section of this chapter does
not include all DSM-5 mental disorders. The
consensus panel acknowledges that people with
CODs may have multiple combinations of the
various mental disorders presented in this chapter
(e.g., a person could have an SUD, bipolar I
disorder, and borderline PD [BPD]). However, for
purposes of clarity and brevity, the panel chose to
focus the discussion on the main disorders primarily
seen in people with CODs and not explore the
multitude of possible combinations. This does not
mean that other mental disorders excluded from
this chapter cannot and do not co-occur with
substance misuse. But the scope of this chapter is
such that it focuses only on mental disorders most
likely to be seen by SUD treatment professionals.
The consensus panel recognizes that although
this chapter covers a broad range of mental
disorders and diagnostic material, it cannot and
should not replace the comprehensive training
necessary for diagnosing and treating clients with
specific mental disorders cooccurring with SUDs.
Readers of this TIP are assumed to already have
working knowledge of mental disorders and their
Chapter 4 70

TIP 42
Chapter 4—Diagnostic and Cross-Cutting Topics
symptoms. The “Advice to the Counselor” boxes
cannot fully address the complexity involved in
treating clients with CODs. These boxes distill for
counselors the main actions and approaches they
can take in working with clients in SUD treatment
who have the specific mental disorder being
discussed.
The consensus panel recognizes that this chapter
cannot cover each mental disorder exhaustively
and that addiction counselors are not expected
to diagnose mental disorders. The panel’s
limited goals for this chapter are to increase SUD
treatment counselors’ familiarity with mental
disorder terminology and criteria and to guide
them on how to proceed with clients who have
these disorders. The chapter also is meant to
stimulate further work in this area and to make this
research accessible to the addiction field.
Depressive Disorders
The depressive disorders category in DSM-5
comprises numerous conditions; addiction
counselors are most likely to encounter major
depressive disorder (MDD) and persistent
depressive disorder (PDD; also called dysthymia)
among their clients. Common features of all
depressive disorders are excessively sad, empty, or
irritable mood and somatic and cognitive changes
that significantly affect ability to function.
Major Depressive Disorder
MDD is not merely extreme sadness, although sad
mood is a defining characteristic. MDD is marked
by either depressed mood or loss of interest in
nearly all previously enjoyed activities. At least
one of those symptoms must be present and must
persist most of the day, almost every day over a
2-week period (Exhibit 4.1). Other core physical,
cognitive, and psychosocial features of MDD
also must be present nearly every day, with the
exception of weight change and suicidal ideation.
MDD is highly associated with suicide risk. A study
reported 39 percent of people with a lifetime MDD
diagnosis contemplated suicide; nearly 14 percent
had a lifetime history of suicide attempt (Hasin
et al., 2018). Yet suicide is not isolated to those
with depressed mood. Counselors always should
ask clients whether they have been thinking of
suicide, whether or not they have, or mention,
symptoms of depression.
Severe depressive episodes can include psychotic
features, such as an auditory hallucination of
a voice saying that the person is “horrible,” a
visual hallucination of a lost relative mocking the
person, or a delusion that one’s internal body
parts have rotted away. However, most people
who have an MDE do not exhibit psychotic
symptoms even when the depression is severe (for
more information on psychosis, see the section
“Schizophrenia and Other Psychotic Disorders”).
WARNING TO COUNSELORS: KNOW YOUR LIMITS OF PRACTICE
This TIP is for addiction counselors in direct clinical contact with clients who have SUDs. Legal titles, levels,
types of licenses, certifications, and scopes of practice for addiction counselors differ across all states and the
District of Columbia (University of Michigan Behavioral Health Workforce Research Center, 2018). For instance,
in certain states, addiction counselors can only conduct assessments and offer treatments for SUDs, limiting
their ability to reach clients with CODs. Certification requirements and authorized services also vary by state.
This TIP is intended to benefit all licensed or certified addiction counselors, regardless of their titles.
However, the diagnostic and counseling activities described in this TIP are not necessarily appropriate
for all addiction counselors to undertake, especially given that addiction counselors do not normally
possess the required training and clinical experience to diagnose mental disorders. Different SUD
treatment settings will have different policies and rules about what addiction counselors can and cannot
do. Whether certified/licensed or not, addiction counselors should use these methods only under the
supervision of an appropriately trained and certified or licensed SUD treatment provider or other
mental health clinician. Maintaining collaborative relationships with mental health service providers for
consultation and referral is recommended, either directly or through clinical supervision.
Chapter 4 71

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
EXHIBIT 4.1. Diagnostic Criteria for MDD
A. Five (or more) of the following symptoms have been present during the same 2-week period and
represent a change from previous functioning; at least one of the symptoms is either (1) depressed mood or
(2) loss of interest or pleasure.
Note: Do not include symptoms that are clearly attributable to another medical condition.
1. Depressed mood most of the day, nearly every day, as indicated by either subjective report (e.g., feels
sad, empty, hopeless) or observation made by others (e.g., appears tearful). Note: In children and
adolescents, can be irritable mood.
2. Markedly diminished interest or pleasure in all, or almost all, activities most of the day, nearly every day
(as indicated by either subjective account or observation).
3. Significant weight loss when not dieting or weight gain (e.g., a change of more than 5 percent of body
weight in a month), or decrease or increase in appetite nearly every day. Note: In children, consider
failure to make expected weight gain.
4. Insomnia or hypersomnia nearly every day.
5. Psychomotor agitation or retardation nearly every day (observable by others, not merely subjective
feelings of restlessness or being slowed down).
6. Fatigue or loss of energy nearly every day.
7. Feelings of worthlessness or excessive or inappropriate guilt (which may be delusional) nearly every day
(not merely self-reproach or guilt about being sick).
8. Diminished ability to think or concentrate, or indecisiveness, nearly every day (either by subjective
account or as observed by others).
9. Recurrent thoughts of death (not just fear of dying), recurrent suicidal ideation without a specific plan,
or a suicide attempt or a specific plan for committing suicide.
B. The symptoms cause clinically significant distress or impairment in social, occupational, or other
important areas of functioning.
C. The episode is not attributable to the physiological effects of a substance or to another medical
condition.
Note: Criteria A–C represent a major depressive episode (MDE).
Note: Responses to a significant loss (e.g., bereavement, financial ruin, losses from a natural disaster, a
serious medical illness or disability) may include the feelings of intense sadness, rumination about the loss,
insomnia, poor appetite, and weight loss noted in Criterion A, which may resemble a depressive episode.
Although such symptoms may be understandable or considered appropriate to the loss, the presence of
an MDE in addition to the normal response to a significant loss should also be carefully considered. This
decision inevitably requires the exercise of clinical judgment based on the individual’s history and the
cultural norms for the expression of distress in the context of loss.
*
D. The occurrence of the MDE is not better explained by schizoaffective disorder, schizophrenia,
schizophreniform disorder, delusional disorder, or other specified and unspecified schizophrenia spectrum
and other psychotic disorders.
E. There has never been a manic episode or a hypomanic episode.
Note: This exclusion does not apply if all of the manic-like or hypomanic-like episodes are substance-
induced or are attributable to the physiological effects of another medical condition.
Continued on next page
Chapter 4 72

TIP 42
Chapter 4—Diagnostic and Cross-Cutting Topics
Continued
Specify:
•
With anxious distress
•
With mixed features
•
With melancholic features
•
With atypical features
•
With mood-congruent psychotic features
•
With mood-incongruent psychotic features
•
With catatonia
•
With peripartum onset
•
With seasonal pattern (recurrent episode only)
Specify current severity/course:
•
Mild
•
Moderate
•
Severe
•
With psychotic features
•
In partial remission
•
In full remission
•
Unspecified
* In distinguishing grief from an MDE, it is useful to consider that in grief the predominant affect is feelings of emptiness
and loss, while in MDE it is persistent depressed mood and the inability to anticipate happiness or pleasure. The dysphoria
in grief is likely to decrease in intensity over days to weeks and occurs in waves, the so-called pangs of grief. These waves
tend to be associated with thoughts or reminders of the deceased. The depressed mood of MDE is more persistent
and not tied to specific thoughts or preoccupations. The pain of grief may be accompanied by positive emotions and
humor that are uncharacteristic of the pervasive unhappiness and misery characteristic of MDE. The thought content
associated with grief generally features a preoccupation with thoughts and memories of the deceased, rather than the
self-critical or pessimistic ruminations seen in MDE. In grief, self-esteem is generally preserved, whereas in MDE feelings
of worthlessness and self-loathing are common. If self-derogatory ideation is present in grief, it typically involves perceived
failings vis-à-vis the deceased (e.g., not visiting frequently enough, not telling the deceased how much he or she was
loved). If a bereaved individual thinks about death and dying, such thoughts are generally focused on the deceased and
possibly about “joining” the deceased, whereas in MDE such thoughts are focused on ending one’s own life because of
feeling worthless, undeserving of life, or unable to cope with the pain of depression.
Source: APA (2013, pp. 160–162). Reprinted with permission from the DSM-5 (Copyright ©2013). APA. All Rights Reserved.
MDE must be distinguished from grief or
bereavement, which are not mental disorders but
rather normal human responses to loss. However,
grief and MDD can be experienced at the same
time; that is, the presence of grief does not rule
out the presence of MDD. DSM-5 provides detailed
guidance on diagnosing MDD in people who are
bereaved.
Persistent Depressive Disorder
PDD presents as excessively sad or depressed
mood that lasts most of the day, more days than
not, for at least 2 years. PDD is somewhat of an
“umbrella” diagnosis in that it covers two different
types of people with depression: people with
chronic MDD (i.e., depression lasting at least 2
years) and people who do not meet criteria for an
MDD (see Criteria A through C in Exhibit 4.1) but
otherwise have had depressive symptoms for at
least 2 years. Thus, the criteria for PDD (Exhibit 4.2)
are similar to, but less severe than, those of MDD.
Prevalence
Data from a national epidemiological survey
indicate the 12-month and lifetime prevalence rates
of DSM-5 MDD are 10 percent and 21 percent,
respectively (Hasin et al., 2018). Prevalence of MDD
in emerging adults (ages 18 to 29 years) is 3 times
higher than the prevalence in older adults (ages 60
years and older). Women are 1.5 times as likely to
report depression as men (Hasin et al., 2018).
Twelve-month and lifetime prevalence rates
for DSM-5 PDD in U.S. samples have not been
reported at the time of this publication. Using
DSM-IV criteria, 12-month and lifetime prevalence
of PDD in U.S. adults are estimated at 1.5 percent
and 3 percent, respectively; DSM-IV dysthymia has
an estimated 12-month and lifetime prevalence of
0.5 percent and 1 percent, respectively (Blanco et
al., 2010).
Chapter 4 73

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
EXHIBIT 4.2. Diagnostic Criteria for PDD
This disorder represents a consolidation of DSM-IV-defined chronic MDD and dysthymic disorder.
A. Depressed mood for most of the day, for more days than not, as indicated by either subjective account
or observation by others, for at least 2 years. Note: In children and adolescents, mood can be irritable, and
duration must be at least 1 year.
B. Presence, while depressed, of two (or more) of the following:
1. Poor appetite or overeating
2. Insomnia or hypersomnia
3. Low energy or fatigue
4. Low self-esteem
5. Poor concentration or difficulty making decisions
6. Feelings of hopelessness
C. During the 2-year period (1 year for children or adolescents) of the disturbance, the individual has never
been without the symptoms in Criteria A and B for more than 2 months at a time.
D. Criteria for an MDD may be continuously present for 2 years.
E. There has never been a manic episode or a hypomanic episode, and criteria have never been met for
cyclothymic disorder.
F. The disturbance is not better explained by a persistent schizoaffective disorder, schizophrenia, delusional
disorder, or other specified or unspecified schizophrenia spectrum and other psychotic disorder.
G. The symptoms are not attributable to the physiological effects of a substance (e.g., a drug of misuse, a
medication) or another medical condition (e.g., hypothyroidism).
H. The symptoms cause clinically significant distress or impairment in social, occupational, or other
important areas of functioning.
Note: Because the criteria for an MDE include four symptoms that are absent from the symptom list
for persistent depressive disorder (dysthymia), a very limited number of individuals will have depressive
symptoms that have persisted longer than 2 years but will not meet criteria for PDD. If full criteria for an
MDE have been met at some point during the current episode of illness, they should be given a diagnosis
of MDD. Otherwise, a diagnosis of other specified depressive disorder or unspecified depressive disorder is
warranted.
Specify if:
•
With anxious distress
•
With mixed features
•
With melancholic features
•
With atypical features
•
With mood-congruent psychotic features
•
With mood-incongruent psychotic features
•
With peripartum onset
Specify if:
•
In partial remission
•
In full remission
Continued on next page
Chapter 4 74
TIP 42
Chapter 4—Diagnostic and Cross-Cutting Topics
Continued
Specify if:
•
Early onset: If onset is before age 21 years
•
Late onset: If onset is at age 21 years or older
Specify if (for most recent 2 years of persistent depressive disorder):
•
With pure dysthymic syndrome: Full criteria for MDE have not been met in at least the preceding 2 years
•
With persistent MDE: Full criteria for an MDE have not been met throughout the preceding 2-year period
•
With intermittent MDEs, with current episode: Full criteria for MDE are currently met, but there have
been periods of at least 8 weeks in at least the preceding 2 years with symptoms below the threshold for
a full MDE
•
With intermittent MDEs, without current episode: Full criteria for an MDE are not currently met, but
there has been one or more MDEs in at least the preceding 2 years
Specify current severity:
•
Mild
•
Moderate
•
Major
Source: APA (2013, pp. 168–169). Reprinted with permission from the DSM-5 (Copyright © 2013). APA. All Rights Reserved.
Depressive Disorders and SUDs
Depressive disorders are highly comorbid with
SUDs. For instance:
•
Presence of a 12-month or lifetime DSM-5
drug use disorder (i.e., a nonalcohol SUD) is
associated with a 1.5 to 1.9 increased odds of
having any mood disorder, a 1.3 to 1.5 increased
odds of having dysthymia, and a 1.2 to 1.3
increased odds of having MDD (Grant et al.,
2016).
•
Twelve-month alcohol use disorder (AUD) is also
associated with an increased risk of MDD and
lifetime AUD with persistent depression (Grant
et al., 2015).
•
A lifetime diagnosis of DSM-5 MDD is more
likely to occur in individuals with a history of
SUDs (58 percent; for AUD, 41 percent) than in
people with a history of any anxiety disorder (37
percent) or PD (32 percent) (Hasin et al., 2018).
People with depression and co-occurring SUDs
tend to have more severe mood symptoms (e.g.,
sleep disturbance, feelings of worthlessness),
higher risk of suicidal ideation and suicide
attempts, worse functioning, more psychiatric
comorbidities, and greater disease burden
(including increased mortality) than people with
MDD alone (Blanco et al., 2012; Gadermann,
Alonso, Vilagut, Zaslavsky, & Kessler, 2012).
They are less likely than people with MDD alone
to receive antidepressants—despite strong
evidence supporting the efficacy of antidepressant
medication in alleviating mood and even some
SUD symptoms (Blanco et al., 2012).
Addiction counselors may represent a way to
reduce lags in adequate depression care in
people with depressive disorders and SUDs.
Among 3.3 million people who reported both
MDEs and SUDs between 2008 to 2014, only 55
percent received services for depression in the
previous year (Han, Olfson, & Mojtabai, 2017).
However, people who had received SUD treatment
in the past year were 1.5 times more likely to have
received depression care than people who had
not engaged in SUD treatment (80 percent vs. 50
percent, respectively) and were 1.6 times more
likely to perceive their depressive care as being
helpful (48 percent vs. 32 percent) than people
who did not access SUD treatment in the previous
12 months (Han, Olfson, & Mojtabai, 2017).
Chapter 4 75

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
Other facts about depression and SUDs that
addiction counselors should know include the
following:
•
Both substance use and discontinuance can be
associated with depressive symptoms.
•
During the first months of sobriety, many people
with SUDs can exhibit symptoms of depression
that fade over time and that are related to acute
and protracted withdrawal.
•
People with co-occurring depressive disorders
and SUDs typically use a variety of drugs.
•
Recent evidence suggests there is increasing
cannabis use with depression, although
cannabinoids have not been shown to be
effective in self-management of depression. In
fact, cannabis may actually worsen the course of
MDD and reduce chances of treatment seeking
(Bahorik et al., 2018).
Treatment of MDD and SUD
Psychotherapy (e.g., integrated cognitive–
behavioral therapy [CBT], group CBT), with or
without adjunct antidepressant use, can effectively
reduce frequency of substance use and depressive
symptoms and improve functioning briefly and over
the long term (Paddock, Hunter, & Leininger, 2014;
Vujanovic et al., 2017). In a review examining MDD
and AUD specifically (Riper et al., 2014), treatment
as usual supplemented with CBT and motivational
interviewing had small but significant effects in
improving depression and decreasing alcohol
use versus treatment as usual alone or other brief
psychosocial interventions.
For more extensive guidance about counseling
clients with addiction and depression, see TIP 48,
Managing Depressive Symptoms in Substance
Abuse Clients During Early Recovery (Center for
Substance Abuse Treatment [CSAT], 2008).
Bipolar I Disorder
Bipolar I disorder, also sometimes termed manic-
depression, refers to a mental state wherein
a person’s mood fluctuates wildly between
depressive and manic episodes (Exhibit 4.3).
During depressive episodes, a person experiences
symptoms of MDD (e.g., excessive sadness, loss of
interest in normally pleasurably activities, physical
and cognitive symptoms). During manic episodes,
a person experiences the opposite—extreme
euphoria, energy, and activity. Manic episodes vary
with intensity and can be manifest in a variety of
ways, such as having little or no need for sleep,
very fast or “pressured” speech, impulsivity and
erratic decision making (especially decisions of
major consequence, like spending a large amount
of money), and racing thoughts. Some manic
episodes are milder in nature; these are known as
hypomanic episodes. People with bipolar I disorder
can experience both manic and hypomanic
episodes. Bipolar II disorder is a related disorder
in which the person only experiences hypomania
and not full-blown mania. For the purposes of
this chapter, only bipolar I disorder, which has
ample research strongly linking it to SUDs, will be
discussed.
Sometimes, manic episodes can produce symptoms
that conflict with reality and are delusional in nature
(e.g., a man believing he is going to marry the
Queen of England). Because of these delusional
and bizarre beliefs, bipolar disorder can sometimes
appear similar to schizophrenia and other psychotic
disorders (see the section “Schizophrenia and
Other Psychotic Disorders”). In fact, increasing
research supports a shared genetic risk between
the bipolar and psychotic disorders (Cardno &
Owen, 2014).
Suicidal thoughts and behaviors are common
among people with bipolar disorder (APA, 2013),
with some believing it could have the highest
suicide risk of all mental disorders (Schaffer et
Chapter 4 76

TIP 42
Chapter 4—Diagnostic and Cross-Cutting Topics
ADVICE TO THE COUNSELOR: COUNSELING A CLIENT WITH A DEPRESSIVE
DISORDER
•
Possibly as many as half of the clients an addiction counselor sees will have an MDE (Center for
Behavioral Health Statistics and Quality [CBHSQ], 2019). Counselors should expect to encounter
depressive symptoms and disorders in their work and proactively familiarize themselves with diagnostic
criteria and general treatment approaches.
• Differentiate among commonplace expressions of depression and depression associated with more
serious mental illness (SMI), medical conditions and medication side effects, and substance-induced
changes. Understand that it is possible to have depressive symptoms without meeting full criteria
for MDD or another depressive disorder. Distinguishing MDD from normal moods and depressive
symptoms is also important.
• Symptoms of depression can persist for 3 to 6 months following abstinence and need to be treated in
counseling. Educate clients about the relationship of depression to substance misuse so that they know
what to expect from treatment and the course of recovery.
• Sometimes substance use can mask depressive symptoms, and it may not become apparent that a
client has depression until after he or she has stopped using substances. Monitor symptoms continually
and respond immediately to any intensification of symptoms.
• Clients with depression often feel hopeless and unmotivated, which can hinder their participation and
retention in treatment. If clients seem reluctant to engage in SUD treatment, do not interpret that as
a sign of resistance or noncompliance. Alleviating their depressive symptoms could help with this to
an extent. But also work with clients on enhancing motivation and self-efficacy so they can develop
confidence and internalize the belief that recovery is possible.
• Gradually introduce and teach skills for participation in mutual-support programs.
• Consider CBT and motivational interviewing in place of or in addition to usual psychosocial treatment.
• Combine addiction counseling with medication and mental health services.
• Because antidepressants have such strong efficacy in reducing depressive symptoms, keep on hand the
names of local mental health professionals (if one isn’t available in the treatment setting) to refer clients
for complete assessment and medication review.
• Given that depressive symptoms can result from SUDs and not an underlying mental disorder, careful
and continual assessment is essential.
• Because of the increased risk of suicidality with MDD, continually assess and be vigilant for signs of
suicidal ideation, gestures/behaviors, and attempts. Use risk mitigation strategies (e.g., safety plans) to
protect clients from self-harm. (See the section “Cross-Cutting Topics: Suicide and Trauma” for more
guidance.)
al., 2015). An estimated 20 percent of people
with bipolar disorder try to commit suicide (Carra,
Bartoli, Crocamo, Brady, & Clerici, 2014), leading
to a standardized mortality ratio of suicide deaths
that is 10 to 30 times greater than that of the
general population (Schaffer et al., 2015). People
with bipolar disorder and SUD are significantly more
likely to try to commit suicide than people without
both conditions (Carra et al., 2014; Schaffer et al.,
2015). Interestingly, current or lifetime SUD is a
significant risk factor for suicide attempt in bipolar
disorder but not suicide death (Schaffer et al., 2015).
Chapter 4 77

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
EXHIBIT 4.3. Diagnostic Criteria for Bipolar I Disorder
For a diagnosis of bipolar I disorder, it is necessary to meet the following criteria for a manic episode. The
manic episode may have been preceded by and may be followed by hypomanic or MDEs.
Manic Episode
A. A distinct period of abnormally and persistently elevated, expansive, or irritable mood and abnormally
and persistently increased goal-directed activity or energy, lasting at least 1 week and present most of the
day, nearly every day (or any duration if hospitalization is necessary).
B. During the period of mood disturbance and increased energy or activity, three (or more) of the following
symptoms (four if the mood is only irritable) are present to a significant degree and represent a noticeable
change from usual behavior:
1. Inflated self-esteem or grandiosity
2. Decreased need for sleep (e.g., feels rested after only 3 hours of sleep)
3. More talkative than usual or pressure to keep talking
4. Flight of ideas or subjective experience that thoughts are racing
5. Distractibility (i.e., attention too easily drawn to unimportant or irrelevant external stimuli) as reported or
observed
6. Increase in goal-directed activity (either socially, at work or school, or sexually) or psychomotor agitation
(i.e., purposeless non-goal-directed activity)
7. Excessive involvement in pleasurable activities that have a high potential for painful consequences (e.g.,
engaging in unrestrained buying sprees, sexual indiscretions, or foolish business investments)
C. The mood disturbance is sufficiently severe to cause marked impairment in social or occupational
functioning or to necessitate hospitalization to prevent harm to self or others, or there are psychotic
features.
D. The episode is not attributable to the physiological effects of a substance (e.g., a drug of abuse, a
medication, other treatment) or to another medical condition.
Note: A full manic episode that emerges during antidepressant treatment (e.g., medication,
electroconvulsive therapy) but persists at a fully syndromal level beyond the physiological effect of that
treatment is sufficient evidence for a manic episode and, therefore, a bipolar I disorder.
Note: Criteria A–D constitute a manic episode. At least one lifetime manic episode is required for the
diagnosis of bipolar I disorder.
Hypomanic Episode
A. A distinct period of abnormally and persistently elevated, expansive, or irritable mood and abnormally
and persistently increased activity or energy, lasting at least 4 consecutive days and present most of the
day, nearly every day.
B. During the period of mood disturbance and increased energy and activity, three (or more) of the
following symptoms (four if the mood is only irritable) have persisted, represent a noticeable change from
usual behavior, and have been present to a significant degree:
1. Inflated self-esteem or grandiosity
2. Decreased need for sleep (e.g., feels rested after only 3 hours of sleep)
3. More talkative than usual or pressure to keep talking
4. Flight of ideas or subjective experience that thoughts are racing
5. Distractibility (i.e., attention too easily drawn to unimportant or irrelevant external stimuli) as reported or
observed.
Continued on next page
Chapter 4 78

TIP 42
Chapter 4—Diagnostic and Cross-Cutting Topics
Continued
6. Increase in goal-directed activity (either socially, at work or school, or sexually) or psychomotor
agitation.
7. Excessive involvement in activities that have a high potential for painful consequences (e.g., engaging
in unrestrained buying sprees, sexual indiscretions, or foolish business investments)
C. The episode is associated with an unequivocal change in functioning that is uncharacteristic of the
individual when not symptomatic.
D. The disturbance in mood and the change in functioning are observable by others.
E. The episode is not severe enough to cause marked impairment in social or occupational functioning or
to necessitate hospitalization. If there are psychotic features, the episode is, by definition, manic.
F. The episode is not attributable to the physiological effects of a substance (e.g., a drug of abuse, a
medication, other treatment).
Note: A full hypomanic episode that emerges during antidepressant treatment (e.g., medication,
electroconvulsive therapy) but persists at a fully syndromal level beyond the physiological effect of that
treatment is sufficient evidence for a hypomanic episode diagnosis. However, caution is indicated so that
one or two symptoms (particularly increased irritability, edginess, or agitation following antidepressant
use) are not taken as sufficient for diagnosis of a hypomanic episode, nor necessarily indicative of a bipolar
diathesis.
Note: Criteria A–F constitute a hypomanic episode. Hypomanic episodes are common in bipolar I disorder
but are not required for the diagnosis of bipolar I disorder.
MDE
A. Five (or more) of the following symptoms have been present during the same 2-week period and
represent a change from previous functioning; at least one of the symptoms is either (1) depressed mood
or (2) loss of interest or pleasure.
Note: Do not include symptoms that are clearly attributable to another medical condition.
1. Depressed mood most of the day, nearly every day, as indicated by either subjective report (e.g., feels
sad, empty, hopeless) or observation made by others (e.g., appears tearful). Note: In children and
adolescents, can be irritable mood.
2. Markedly diminished interest or pleasure in all, or almost all, activities most of the day, nearly every day
(as indicated by either subjective account or observation).
3. Significant weight loss when not dieting or weight gain (e.g., a change of more than 5 percent of body
weight in a month), or decrease or increase in appetite nearly every day. Note: In children, consider
failure to make expected weight gain.
4. Insomnia or hypersomnia nearly every day.
5. Psychomotor agitation or retardation nearly every day (observable by others, not merely subjective
feelings of restlessness or being slowed down).
6. Fatigue or loss of energy nearly every day.
7. Feelings of worthlessness or excessive or inappropriate guilt (which may be delusional) nearly every day
(not merely self-reproach or guilt about being sick).
8. Diminished ability to think or concentrate, or indecisiveness, nearly every day (either by subjective
account or as observed by others).
9. Recurrent thoughts of death (not just fear of dying), recurrent suicidal ideation without a specific plan,
or a suicide attempt or a specific plan for committing suicide.
Continued on next page
Chapter 4 79

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
B. The symptoms cause clinically significant distress or impairment in social, occupational, or other
important areas of functioning.
C. The episode is not attributable to the physiological effects of a substance or to another medical
condition.
Note: Criteria A–C constitute an MDE. MDEs are common in bipolar I disorder but are not required for the
diagnosis of bipolar I disorder.
Note: Responses to a significant loss (e.g., bereavement, financial ruin, losses from a natural disaster, a
serious medical illness or disability) may include the feelings of intense sadness, rumination about the
loss, insomnia, poor appetite, and weight loss noted in Criterion A, which may resemble a depressive
episode. Although such symptoms may be understandable or considered appropriate to the loss, the
presence of an MDE in addition to the normal response to a significant loss should also be carefully
considered. This decision inevitably requires the exercise of clinical judgment based on the individual’s
history and the cultural norms for the expression of distress in the context of loss.
*
Bipolar I Disorder
A. Criteria have been met for at least one manic episode (Criteria A—D under Manic Episode, above).
B. The occurrence of the manic episode and MDE is not better explained by schizoaffective disorder,
schizophrenia, schizophreniform disorder, delusional disorder, or other specified or unspecified
schizophrenia spectrum and other psychotic disorder.
Specify current severity:
•
Mild
•
Moderate
•
Severe
Specify:
•
With psychotic features
•
In partial remission
•
In full remission
•
Unspecified
Specify:
•
With anxious distress
•
With mixed features
•
With rapid cycling
•
With melancholic features
•
With atypical features
•
With mood-congruent psychotic features
•
With mood-incongruent psychotic features
•
With catatonia
•
With peripartum onset
•
With seasonal pattern
* In distinguishing grief from an MDE, it is useful to consider that in grief the predominant affect is feelings of
emptiness and loss, while in MDE it is persistent depressed mood and the inability to anticipate happiness or pleasure.
The dysphoria in grief is likely to decrease in intensity over days to weeks and occurs in waves, the so-called pangs of
grief. These waves tend to be associated with thoughts or reminders of the deceased. The depressed mood of MDE is
Continued on next page
Chapter 4 80
Continued
TIP 42Chapter 4—Diagnostic and Cross-Cutting Topics
Continued
more persistent and not tied to specific thoughts or preoccupations. The pain of grief may be accompanied by positive
emotions and humor that are uncharacteristic of the pervasive unhappiness and misery characteristic of MDE. The
thought content associated with grief generally features a preoccupation with thoughts and memories of the deceased,
rather than the self-critical or pessimistic ruminations seen in MDE. In grief, self-esteem is generally preserved, whereas
in MDE feelings of worthlessness and self-loathing are common. If self-derogatory ideation is present in grief, it typically
involves perceived failings vis-à-vis the deceased (e.g., not visiting frequently enough, not telling the deceased how
much he or she was loved). If a bereaved individual thinks about death and dying, such thoughts are generally focused
on the deceased and possibly about “joining” the deceased, whereas in MDE such thoughts are focused on ending one’s
own life because of feeling worthless, undeserving of life, or unable to cope with the pain of depression.
Source: APA (2013, pp. 123–127). Reprinted with permission from the DSM-5 (Copyright © 2013). APA. All Rights Reserved.
Prevalence
The 12-month and lifetime prevalence rates of
DSM-5 bipolar I disorder are 1.5 percent and 2
percent, respectively (Blanco et al., 2017). Rates
are nearly equivalent between men and women for
both 12-month and lifetime prevalence (Blanco et
al., 2017).
Bipolar I Disorder and SUDs
Individuals with bipolar I have high prevalence rates
(65 percent) of lifetime SUD, AUD (54 percent), and
drug use disorder (32 percent) (McDermid et al.,
2015). Presence of a 12-month or lifetime DSM-5
drug use disorder (i.e., an SUD excluding alcohol)
is associated with a 1.4 to 1.5 increased odds
in having bipolar I disorder (Grant et al., 2016).
Similarly, presence of past-year or lifetime bipolar I
disorder carries a 2 to 5.8 times greater risk of also
having any 12-month or lifetime SUD (Blanco et al.,
2017). A systematic review and meta-analysis found
strong associations between co-occurring SUDs
and bipolar illness in individuals in clinical settings,
with the highest prevalence (average: 30 percent)
for alcohol use, 20 percent (mean) for cannabis, and
17 percent (mean) for any drug use disorder (Hunt,
Malhi, Cleary, Lai, & Sitharthan, 2016b).
Co-occurring bipolar illness and substance misuse
are associated with numerous adverse clinical,
social, and economic consequences, including
increased symptom severity, poorer treatment
outcomes, and greater suicide risk (Ma, Coles, &
George, 2018). Presence of a co-occurring SUD
with bipolar disorder has been linked to lower SUD
treatment adherence and retention, protracted
mood episodes, poorer recovery of functional
abilities (even after abstaining from substances),
increased utilization of emergency services, greater
hospitalizations, more variable disease course,
greater affective instability, more impulsivity,
and poor response to lithium (the standard
pharmacotherapy of choice) (Swann, 2010; Tolliver
& Anton, 2015).
Treatment of Bipolar I Disorder and SUDs
Substance misuse by people with bipolar disorder
complicates diagnosis and treatment. Evidence
exists of a bidirectional relationship between
bipolar disorder and SUDs, yet the ways in which
these conditions influence one another is still
unclear (Tolliver & Anton, 2015). Little research
has examined nonpharmacological approaches
to managing comorbid bipolar I disorder and
SUDs. Group CBT, integrated therapy, and
relapse prevention techniques may help reduce
hospitalizations, increase abstinence, improve
medication adherence, reduce addiction
severity, and (to a lesser extent) improve mood
symptoms (Gold et al., 2018). However, results are
inconsistent across studies, underscoring the need
for more research.
Chapter 4 81

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
ADVICE TO THE COUNSELOR: COUNSELING A CLIENT WITH BIPOLAR I
DISORDER
•
Although true for most counseling situations, maintaining a calm demeanor and a reassuring presence
is especially important with these clients.
• Start low and go slow (that is, start “low” with general and nonprovocative topics and proceed gradually
as clients become more comfortable talking about problems).
• Monitor symptoms and respond immediately to any intensification.
• At every session, strongly emphasize and monitor medication compliance and promote medication
adherence. The cyclical nature of bipolar disorder is frequently punctuated by bouts of medication
noncompliance, and it is crucial to cultivate and convey an understanding of the allure of the manic
episode.
• Pay attention to signs of depression or mania, as medication might be able to ward off the worsening
of the client’s condition. For developing mania, which is virtually nonresponsive to psychosocial
interventions, a variety of mood stabilizers have demonstrated remarkable efficacy. Their timely use can
avert potentially life-altering, negative events. (See “Pharmacotherapy” in Chapter 7.)
• Although evidence on psychosocial treatments for bipolar I disorder and SUD is inconsistent, the
strongest support seems to come from the use of integrated group-based interventions that use
multiple treatment components to address both mood and substance-related symptoms. Techniques
include counseling, relapse prevention, psychoeducation, medication management, and regular phone
or in-person “check-in” sessions to monitor symptoms and treatment progress.
• Gradually introduce and teach skills for participation in mutual-support programs.
• Combine addiction counseling with medication and mental health services.
• Suicide and suicidal behaviors are major ongoing concerns for this client population, and the addiction
counselor should have a thorough understanding of her or his role in preventing suicide.
Case Study: Counseling an SUD treatment Client With Bipolar I Disorder
John W. is a 30-year-old man with bipolar I disorder and AUD. He has a history of hospitalizations, both
psychiatric and substance related; after the most recent extended psychiatric hospitalization, he was
referred for SUD treatment. He told the counselor he used alcohol to facilitate social contact, as well as
deal with boredom, because he had not been able to work for some time. The counselor learned that
during his early 20s, John W. achieved full-time employment and established an intimate relationship
with a nondrinking woman; however, his drinking led to the loss of both.
During one of his AUD treatments, he developed florid manic symptoms, believing himself to be
a prophet with the power to heal others. He was transferred to a closed psychiatric unit, where he
eventually stabilized on a combination of antipsychotic medications (risperidone) and lithium. Since that
time, he has had two episodes of worsening psychiatric symptoms leading to hospitalization; each of
these began with drinking, which then led to stopping his medications, then florid mania and psychiatric
commitment. However, when he is taking his medications and is sober, John W. has a normal mental
status and relates normally to others. Recently, following a series of stressors, John W. left his girlfriend,
quit his job, and began using alcohol heavily again. He rapidly relapsed to active mania, did not adhere to
a medication regimen, and was rehospitalized.
Continued on next page
Chapter 4 82

TIP 42
Chapter 4—Diagnostic and Cross-Cutting Topics
Continued
At the point John W. is introduced to the SUD treatment counselor, his mental status is fairly normal;
however, he warns the counselor that after manic episodes he tends to get somewhat depressed, even
when he is taking medications. The counselor takes an addiction history and finds that John W. has had
several periods of a year or two during which he was abstinent from alcohol and drugs of misuse, but he
has never had ongoing AUD treatment or attended Alcoholics Anonymous (AA) meetings. John W. replies
to the counselor’s questions about this with, “Well, if I just take my meds and don’t drink, I’m fine. So why
do I need those meetings?”
Using a motivational approach, the counselor helps John W. analyze what has worked best for him in
dealing with both addiction and mental problems, as well as what has not worked well for him. John W. is
tired of the merry-go-round of his life; he certainly acknowledges that he has a major mental disorder, but
thinks his drinking is only secondary to the mania. When the counselor gently points out that each of the
episodes in which his mental disorder led to hospitalization began with an alcohol relapse, John W. begins
to listen. In a group for clients with CODs at the SUD treatment agency, John W. is introduced to another
client in recovery with a bipolar disorder, who tells his personal story and how he discovered that both of his
problems need primary attention. This client agrees to be John W.’s temporary sponsor and calls John W.’s
case manager, who works at the mental health center where John W. gets his medication, and describes
the treatment plan. She then makes arrangements for a monthly meeting involving the counselor, case
manager, and John W.
Discussion: The SUD treatment counselor has taken the wise step of taking a detailed history and
attempting to establish the linkage between CODs. The counselor tries to appreciate the client’s own
understanding of the relationship between the two. She uses motivational approaches to analyze what
John W. did in his previous partially successful attempts to deal with the problem and helps develop
connections with other recovering clients to increase motivation. Lastly, she is working closely with the case
manager to ensure a coordinated approach to management of each disorder.
Posttraumatic Stress Disorder
PTSD is an exaggerated fear response that occurs
following exposure to one or more extremely
upsetting events. Such events can include, but are
not limited to, war, terrorist attacks, threatened
or actual physical or sexual violence, being
kidnapped, natural and man-made disasters, and
serious motor vehicle accidents. Events may be
experienced firsthand, witnessed, experienced
through repeated exposure as a part of one’s job
(e.g., police officers repeatedly hearing details
about child abuse, murder, and other violent and
upsetting crimes), or by learning about such events
occurring to a close loved one (e.g., learning of the
murder of one’s child). People with PTSD report
the most distressing trauma to be sexual abuse
before age 18 years (Goldstein et al., 2016).
Symptoms of PTSD are grouped into four categories:
•
Intrusive, persistent re-experiences of
the trauma, including recurrent dreams
or nightmares, flashbacks, and distressing
memories
•
Persistent avoidance of people, places, objects,
and events that remind the person of the trauma
or otherwise trigger distressing memories,
thoughts, feelings, and physiological reactions
•
Negative alterations in cognitions and mood,
such as memory loss (particularly regarding
details surrounding the event), self-blame, guilt,
hopelessness, social withdrawal, and an inability
to experience positive emotions
•
Marked alterations in arousal and reactivity,
such as experiencing sleeplessness or feeling
“jumpy,” “on edge,” easily started, irritable,
angry, or unable to concentrate
Exhibit 4.4 lists the DSM-5 criteria for PTSD in
adults and children older than age 6; separate
criteria are available for children ages 6 years and
younger and can be found in DSM-5.
Chapter 4 83

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
EXHIBIT 4.4. Diagnostic Criteria for PTSD
Note: The following criteria apply to adults, adolescents, and children older than 6 years.
A. Exposure to actual or threatened death, serious injury, or sexual violence in one (or more) of these ways:
1. Directly experiencing the traumatic event(s)
2. Witnessing, in person, the event(s) as it occurred to others
3. Learning that the traumatic event(s) occurred to a close family member or close friend. In cases of
actual or threatened death of a family member or friend, the event(s) must have been violent or
accidental.
4. Experiencing repeated or extreme exposure to aversive details of the traumatic event(s) (e.g., first
responders collecting human remains; police officers repeatedly exposed to details of child abuse)
Note: Criterion A4 does not apply to exposure through electronic media, television, movies, or pictures,
unless this exposure is work related.
B. Presence of one (or more) of the following intrusion symptoms associated with the traumatic events(s),
beginning after the traumatic event(s) occurred:
1. Recurrent, involuntary, and intrusive distressing memories of the traumatic event(s)
Note: In children older than 6 years, repetitive play may occur in which themes or aspects of the traumatic
event(s) are expressed.
2. Recurrent distressing dreams in which the content and/or affect of the dream are related to the
traumatic event(s)
Note: In children, there may be frightening dreams without recognizable content.
3. Dissociative reactions (e.g., flashbacks) in which the individual feels or acts as if the traumatic event(s)
were recurring. (Such reactions may occur on a continuum, with the most extreme expression being a
complete loss of awareness of present surroundings.)
Note: In children, trauma-specific reenactment may occur in play.
4. Intense or prolonged psychological distress at exposure to internal or external cues that symbolize or
resemble an aspect of the traumatic event(s)
5. Marked physiological reactions to internal or external cues that symbolize or resemble an aspect of the
traumatic event(s)
C. Persistent avoidance of stimuli associated with the traumatic event(s), beginning after the traumatic
event(s) occurred, as evidenced by one or both of the following:
1. Avoidance of or efforts to avoid distressing memories, thoughts, or feelings about or closely associated
with the traumatic event(s)
2. Avoidance of or efforts to avoid external reminders (people, places, conversations, activities, objects,
situations) that arouse distressing memories, thoughts, or feelings about or closely associated with the
traumatic event(s)
D. Negative alterations in cognitions and mood associated with the traumatic events(s), beginning or
worsening after the traumatic events(s) occurred, as evidenced by two (or more) of the following:
1. Inability to remember an important aspect of the traumatic events(s) (typically due to dissociative
amnesia and not to other factors such as head injury, alcohol, or drugs)
Continued on next page
Chapter 4 84

TIP 42
•
Chapter 4—Diagnostic and Cross-Cutting Topics
Continued
2. Persistent and exaggerated negative beliefs or expectations about oneself, others, or the world (e.g., “I
am bad,” “No one can be trusted,” “The world is completely dangerous,” “My whole nervous system is
permanently ruined”)
3. Persistent, distorted cognitions about the cause or consequences of the traumatic event(s) that lead the
individual to blame himself/herself or others
4. Persistent negative emotional state (e.g., fear, horror, anger, guilt, or shame)
5. Markedly diminished interest or participation in significant activities
6. Feelings of detachment or estrangement from others
7. Persistent inability to experience positive emotions (e.g., inability to experience happiness, satisfaction,
or loving feelings)
E. Marked alterations in arousal and reactivity associated with the traumatic events(s), beginning or
worsening after the traumatic events(s) occurred, as evidenced by two (or more) of the following:
1. Irritable behavior and angry outbursts (with little or no provocation) typically expressed as verbal or
physical aggression toward people or objects
2. Reckless or self-destructive behavior
3. Hypervigilance
4. Exaggerated startle response
5. Problems with concentration
6. Sleep disturbance (e.g., difficulty falling or staying asleep or restless sleep)
F. Duration of the disturbance (Criteria B, C, D, and E) is more than 1 month.
G. The disturbance causes clinically significant distress or impairment in social, occupational, or other
important areas of functioning.
H. The disturbance is not attributable to the physiological effects of a substance (e.g., medication, alcohol) or
another medical condition.
Specify whether:
With dissociative symptoms: The individual’s symptoms meet the criteria for PTSD, and in addition, in
response t
o the stressor, the individual experiences persistent or recurrent symptoms of either of the
following:
1. Depersonalization: Persistent or recurrent experiences of feeling detached from, and as if one were an
outside observer of, one’s mental processes or body (e.g., feeling as though one were in a dream; feeling
a sense of unreality of self or body or of time moving slowly)
2. Derealization: Persistent or recurrent experiences of unreality of surroundings (e.g., the world around the
individual is experienced as unreal, dreamlike, distant, or distorted)
Note: To use this subtype, the dissociative symptoms must not be attributable to the physiological effects
of a substance (e.g., blackouts, behavior during alcohol intoxication) or another medical condition (e.g.,
complex partial seizure).
Specify if:
With delayed expression: If the full diagnostic criteria are not met until at least 6 months after the event
(although the onset and expression of some symptoms may be immediate)
Source: APA (2013, pp. 271–272). Reprinted with permission from the DSM-5 (Copyright © 2013). APA. All Rights Reserved.
Chapter 4 85
TIP 42 Substance Use Disorder Treatment for People With Co-Occurring Disorders
Prevalence
Twelve-month and lifetime prevalence rates of
DSM-5 PTSD are 4.7 percent and 6.1 percent,
respectively (Goldstein et al., 2016). Rates are
markedly higher among women than men, about
6 percent and 8 percent for past-year and lifetime
PTSD, respectively (Goldstein et al., 2016). Lifetime
prevalence is even higher for female veterans (13.9
percent) and younger adults (ages 18 to 29 years,
15.3 percent) (Smith, Goldstein, & Grant, 2016). A
2016 study of veterans using DSM-5 criteria found
the lifetime prevalence of PTSD to be 6.9 percent,
with significantly higher prevalence rates noted
for women and younger age groups (Smith et al.,
2016).
Individuals in occupations at risk of exposure
to traumatic events (e.g., police, firefighters,
emergency medical personnel) have higher rates
of PTSD. Among high-risk individuals (those who
have survived rape, military combat, and captivity
or ethnically or politically motivated internment
and genocide), the proportion of those with PTSD
ranges from one-third to one-half (APA, 2013).
PTSD and SUDs
A strong association exists between PTSD and
substance misuse, including lifetime SUDs (Hasin &
Kilcoyne, 2012), lifetime drug use disorders (Grant
et al., 2016), and lifetime AUD (Grant et al., 2015).
Among people with SUDs, lifetime prevalence of
PTSD is thought to range between 26 percent and
52 percent and rates of current PTSD between 15
percent and 42 percent (Vujanovic, Bonn-Miller, &
Petry, 2016). Among people with PTSD, lifetime
rates of SUD are likely between 36 percent and
52 percent (Vujanovic et al., 2016). Presence of a
12-month or lifetime DSM-5 drug use disorder (i.e.,
an SUD excluding alcohol) is associated with a 1.5
to 1.6 increased odds of having PTSD (Grant et al.,
2016). Similarly, presence of 12-month or lifetime
PTSD is associated with a 1.3 to 1.5 increased odds
of having a past-year or lifetime SUD (Goldstein et
al., 2016).
Comorbid PTSD and addiction are highly complex
and associated with worse treatment outcomes
(including lower rates of remission and faster
relapse), poorer treatment response, more
cognitive difficulties, worse social functioning,
greater risk of suicide attempt, and heightened
mortality (Flanagan, Korte, Killeen, & Back, 2016;
Schumm & Gore, 2016). Compared with people
with PTSD or alcohol dependence alone, those
with both report more traumatic childhoods,
more psychiatric comorbidities, an increased risk
of suicide, more severe symptoms, and greater
disability (Blanco et al., 2013).
People with PTSD tend to misuse the most serious
substances (cocaine and opioids); however, misuse
of prescription medications, cannabis, and alcohol
also are common.
WARNING TO COUNSELORS:
PTSD OR DEPRESSION?
Many people with PTSD are mistakenly
diagnosed with depression, particularly in
SUD treatment settings where screening for
trauma is low. The two conditions are highly
comorbid. Symptoms can overlap to an extent,
and when occurring together, the combination
results in greater symptom severity than either
disorder alone (Post, Feeny, Zoellner, & Connell,
2016). Subclinical traumatic stress reactions are
commonly expressed as depressive symptoms.
However, PTSD has unique treatment needs
and a different disease course and treatment
response than depression. When working with
someone with a depressive disorder diagnosis
who also has a history of trauma, consider
screening for PTSD to gauge whether a referral
for diagnostic assessment might be warranted.
Treatment of PTSD and SUDs
Historically, there has been debate about whether
to treat PTSD and addiction concurrently or
sequentially, with most providers falling on the side
of treating the SUD separately and first (Schumm &
Gore, 2016). Some believe that substance misuse
among people with PTSD is a means of self-
medicating to help manage distressing mood and
anxiety symptoms, thus making PTSD the priority
target for treatment. Alternatively, others have
feared that treating PTSD first could exacerbate
SUD symptoms or cause clients to use substances
Chapter 4 86

TIP 42
Chapter 4—Diagnostic and Cross-Cutting Topics
as a means of coping with the hyperarousal and
negative mood that can occur while progressing
through PTSD treatment. However, integrated,
concurrent treatment that addresses both
conditions simultaneously has generated strong
empirical support, appears to be preferable to
clients, and is increasingly considered the current
standard of care, particularly when combining
psychosocial and pharmacologic approaches
(Flanagan et al., 2016; Schumm & Gore, 2016;
Simpson, Lehavot, & Petrakis, 2017).
Despite the evidence that concurrent
treatment can be effective, people with PTSD
and SUD are frequently only treated for
addiction; further, clients in SUD treatment
settings are often not even assessed for
PTSD (Vujanovic et al., 2016). Whereas treating
SUD alone rarely leads to improvement in
PTSD symptoms, reducing PTSD symptoms
can significantly decrease the odds of heavy
substance (Hien et al., 2010).
Exposure therapy can be safe and effective at
reducing trauma and SUD symptoms—although
more evidence is needed (Flanagan et al., 2016).
Nonexposure-based treatments have been
studied more widely for co-occurring PTSD
and SUD and may be moderately effective at
improving both PTSD and substance symptoms,
but the evidence is still premature (Flanagan et
al., 2016). A Cochrane Review found individual
trauma-focused psychotherapy with adjunctive
SUD treatment to be effective at reducing
posttreatment PTSD severity and substance use
at 5 to 7 months following treatment; however,
the authors deemed the current evidence base on
psychological treatments for PTSD-SUD to be weak
in terms of quality and methodology, underscoring
the need for more rigorous research in this area
(Roberts, Roberts, Jones, & Bisson, 2016). Studies
of pharmacologic treatments for SUD with PTSD,
and for AUD specifically, appear encouraging but,
again, are understudied, often inconclusive, and
require more data (Flanagan et al., 2016; Petrakis &
Simpson, 2017).
See the section “Cross-Cutting Topics: Suicide
and Trauma” at the end of this chapter for more
information about trauma-informed care for people
with CODs.
ADVICE TO THE COUNSELOR: COUNSELING A CLIENT WITH PTSD
•
As a counselor, it is important to recognize, and help clients understand, that becoming abstinent from
substances does not resolve PTSD; both disorders must be addressed in treatment.
• Treatment of PTSD with cooccurring SUDs requires careful planning and supervision.
− As the client faces painful trauma memories, the desire for intoxication can be overwhelming. By
exploring trauma memories, well-intentioned counselors inadvertently may drive a client back to
the substance by urging her to “tell her story” or “let out the abuse.” Even if a client wants to discuss
trauma and seems safe during the session, aftereffects may well ensue, including a flood of memories
the client is unprepared to handle, increased suicidality, and “retraumatization” (feeling like one is
reliving the event).
− Such treatment approaches should be undertaken only with adequate formal training in both PTSD
and substance misuse and only under careful clinical supervision.
• These clients need stability in their primary therapeutic relationship; hence, this work should not be
undertaken in settings with high staff turnover and never without training and supervision.
Continued on next page
Chapter 4 87

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
Continued
• Do not try to provide trauma exploration treatment in view of the potential for highly destabilizing
effects (including worsening of substance misuse).
• Provide present-focused psychoeducation about PSTD, such as teaching the client to recognize
symptoms of the disorder and how to cope with them.
• Clinicians are advised not to overlook the possibility of PTSD in men.
• People with PTSD and substance misuse are more likely to experience further trauma than people with
substance misuse alone.
• Repeated trauma is common in domestic violence, child abuse, and some substance-using lifestyles
(e.g., the drug trade), so helping the client protect against future trauma may be an important part of
treatment.
• Anticipate proceeding slowly with a client who is diagnosed with or has symptoms of PTSD. Consider
the effect of a trauma history on the client’s current emotional state, such as an increased level of fear,
depressed mood, or irritability.
• Trauma begets more trauma, as people with PTSD are at an increased risk of revictimization. Discuss
with clients this increased risk, how to recognize and avoid threatening situations, and how substance
use plays a role in increasing their vulnerability to revictimization.
• Develop a plan for increased safety if warranted.
• Respond more to the client’s behavior than his or her words.
• Limit questioning about details of trauma.
• Recognize that trauma injures an individual’s capacity for attachment. The establishment of a trusting
treatment relationship will be a goal of treatment, not a starting point.
• Recognize the importance of one’s own trauma history and countertransference.
• Help the client learn to deescalate intense emotions.
• Help the client understand the link between PTSD and substance use by providing psychoeducation.
• Teach coping skills to control PTSD symptoms.
• Recognize that PTSD/SUD treatment clients may have a more difficult time in treatment and that
treatment for PTSD may be long term, especially for those who have a history of serious trauma.
• Help the client access long-term PTSD treatment and refer to trauma experts for trauma exploratory
work.
• Given the high prevalence of self-harm in this population, counselors should screen for suicide risk
early on in treatment and throughout the course of care. Risk of suicide in people with PTSD is
correlated with a history of childhood maltreatment and more severe PTSD symptoms—especially ones
concerning negative mood and cognitions (Criterion D in DSM-5 diagnostic criteria).
Chapter 4 88
TIP 42Chapter 4—Diagnostic and Cross-Cutting Topics
CASE STUDY: COUNSELING AN SUD TREATMENT CLIENT WHO BINGE
DRINKS AND HAS PTSD
Caitlin P. is a 17-year-old Native American woman admitted to an inpatient SUD treatment program after
she tried to kill herself during a drunken episode. She has been binge drinking since age 12 and also has
tried a wide variety of pills without caring what she is taking. She has a history of depression and burning
her arms with cigarettes. She was the victim of a date rape at age 15 and did not tell anyone but a close
friend. She did not tell her family for fear that they would think less of her for not preventing or fighting
off the attack.
In treatment, she worked with staff to try to gain control over her repeated self-destructive behavior.
Together they worked on developing compassion for herself, created a safety plan to encourage her to
reach out for help when in distress, and began a log to help her identify her PTSD symptoms so that she
could recognize them more clearly. When she had the urge to drink, use drugs, or burn herself, she was
guided to try to “bring down” the feelings through grounding, rethink the situation, and reassure herself
that she could get through it. She began to see that her substance use had been a way to numb the pain.
Discussion: Counselors can help clients gain control over PTSD symptoms and self-destructive behavior
associated with trauma. Providing specific coping strategies and lots of encouragement typically appeals
to PTSD/SUD treatment clients, who may want to learn how to overcome the emotional rollercoaster of
their disorders. Notice that in such early-phase treatment, detailed exploration of the past is not generally
advised.
For more information about working with American Indian and Alaska Native clients who have SUDs or
CODs, see TIP 61, Behavioral Health Services for American Indians and Alaska Natives (SAMHSA, 2018a).
Personality Disorders
A PD refers to a person’s lifelong inability to form
healthy, functional relationships with others and
a failure to develop an adaptive sense of self.
These are manifest as (a) destructive or otherwise
problematic patterns of thinking and feeling about
oneself, one’s place in the world, and others and
(b) negative ways of behaving toward others.
People with PDs often lack insight into their
dysfunctional cognitive, emotional, and behavioral
patterns and often blame others or the world in
general for their difficulties. Many people with PDs
struggle to develop strong, positive relationships,
because they view reality from the perspective
of their own needs and therefore have a difficult
time understanding, empathizing with, and
connecting with others. PDs are lifelong conditions
that develop in adolescence or early adulthood.
They are frequently resistant to change and
result in significant impairments in interpersonal
functioning, work/school performance, and
self-concept.
Chapter 4 89

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
There are several types of PDs, and the precise
symptoms someone exhibits will depend on
which type of PD he or she has. For instance,
depending on the PD type, an individual might
think of himself/herself in overly negative ways or
in grandiose ways, might be overly attached to
others or completely indifferent to others, might
constantly try to be the center of attention or
might be socially reclusive. People with PDs must
first meet the diagnostic criteria for a general
PD (Exhibit 4.5) and then must meet additional
diagnostic criteria for whatever PD type is
most appropriate given their symptoms. Many
individuals with PDs have features of, or meet full
criteria for, other PDs.
This TIP provides details about the two PD types
that are commonly comorbid with addiction—BPD
and antisocial PD (ASPD). Before exploring BPD
and ASPD in detail, an overview of PDs in general
follows. Readers should be aware that the diagnostic
approach to PDs continues to undergo refinement,
as researchers in psychopathology have expressed
many concerns about the meaningfulness, gender
bias, accuracy, and utility of the current categorical
diagnostic system for PDs (see Section III of DSM-5
for more information on alternative PD classification
and diagnostic criteria).
PD Clusters
Once a person meets criteria for a general PD,
his or her diagnosis is further categorized based
on several specific PD types, including paranoid
PD, schizoid PD, schizotypal PD, histrionic
PD, narcissistic PD, ASPD, BPD, avoidant PD,
dependent PD, and obsessive-compulsive PD. If
the symptoms do not meet any of the types, he
or she can be diagnosed with either unspecified
PD or other specified PD. Detailed descriptions
and criteria for all 10 PD types can be found in
DSM-5. BPD and ASPD most frequently co-occur
with substance misuse (Köck & Walter, 2018). Thus,
they are included in this chapter and discussed in
respective subsections.
In DSM5, PD types are categorized into three
distinct clusters based on their common features:
•
Cluster A PDs describe people who may be
seen as odd or eccentric. This eccentricity can
express itself in many ways (e.g., paranoia and
suspicion, extreme social withdrawal/lack of
EXHIBIT 4.5. Diagnostic Criteria for General PD
A. An enduring pattern of inner experience and behavior that deviates markedly from the expectations of
the individual’s culture. This pattern is manifested in two (or more) of the following areas:
1. Cognition (i.e., ways of perceiving and interpreting self, other people, and events)
2. Affectivity (i.e., the range, intensity, lability, and appropriateness of emotional response)
3. Interpersonal functioning
4. Impulse control
B. The enduring pattern is inflexible and pervasive across a broad range of personal and social situations.
C. The enduring pattern leads to clinically significant distress or impairment in social, occupational, or other
important areas of functioning.
D. The pattern is stable and of long duration, and its onset can be traced back at least to adolescence or
early adulthood.
E. The enduring pattern is not better explained as a manifestation or consequence of another mental
disorder.
F. The enduring pattern is not attributable to the physiological effects of a substance (e.g., a drug of abuse, a
medication) or another medical condition (e.g., head trauma).
Source: APA (2013, pp. 646–647). Reprinted with permission from the DSM-5 (Copyright © 2013). APA. All Rights Reserved.
Chapter 4 90
TIP 42
-
-
-
-
-
-
-
-
-
-
Chapter 4—Diagnostic and Cross-Cutting Topics
WARNING TO COUNSELORS: PDS AND PROVIDER STIGMA
PDs are among the most stigmatized of all mental disorders (Sheehan, Nieweglowski, & Corrigan, 2016).
Primary care, mental health, and SUD treatment professionals sometimes have contemptuous attitudes
toward PDs and the people who live with them. They may think or say things such as:
•
“These people cannot be treated, so why bother?”
•
“I see PDs all the time, especially in women.”
•
“Most people with addiction also have a PD.”
•
“It is not worth the time to try to diagnose or treat someone with a PD because nothing can be done for
them anyway.”
•
“I don’t accept referrals for clients like that because they’re too much work and can’t be helped.”
•
“Most antisocial people are criminals and are just going to end up in prison.”
•
“People with ASPD are ‘psychopaths’ (or ‘sociopaths’).”
•
“These people are just manipulative liars; they don’t really want to get better or want my help.”
•
“That wasn’t a real suicide attempt. She’s borderline—she’s just seeking attention.”
It is true that PDs are lifelong disorders, can be challenging to work with, and may be more resistant
to change than other mental disorders or SUDs. But that does not mean that counselors cannot offer
people with these conditions any relief, and it does not mean that people with PDs cannot improve their
symptoms. Addiction professionals can help clients with PDs reduce substance misuse, which in turn can
indirectly help improve functioning and quality of life by reducing risky behavior and enhancing health.
Counselors can combat stigma and prejudice by:
•
Becoming familiar with the latest evidence in support of PD treatment. The notion that these disorders
are completely intractable is untrue. Even in the absence of validated treatments for the PD itself,
interventions can still help reduce disabling symptoms and CODs, including co-occurring addiction.
•
Engaging in honest self-reflection about their own views of and attitudes about PDs. Talking to a
clinical supervisor, or even engaging in brief counseling themselves, can foster self-awareness and
behavior change.
•
Remembering that stereotypes can be dangerous and affect how counselors serve (or do not serve) the
clients who need them. All people, regardless of symptoms or diagnoses, deserve health and happiness.
interest in interpersonal relationships, unusual
beliefs or behaviors). PD types included in this
cluster are:
Paranoid PD.
Schizoid PD.
Schizotypal PD.
•
Cluster B PDs are characterized by dramatic,
overly emotional, and erratic and unpredictable
behavior. PD types included in this cluster are:
Histrionic PD.
Narcissistic PD.
ASPD.
BPD.
•
Cluster C PDs are marked by anxious and fearful
behaviors. PD types included in this cluster are:
Obsessive-compulsive PD.
A
voidant PD.
Dependent PD.
Prevalence
Prevalence estimates for PDs among the general
population are difficult to ascertain, given lack
of research examining large samples from the
community (as opposed to clinical samples, in which
PDs are far more common and frequently studied).
Estimates are 9.1 percent for any PD, 5.7 percent for
any Cluster A PD, 1.5 percent for any Cluster B, and
6 percent for Cluster C (APA, 2013). In one analysis
of the National Epidemiologic Survey on Alcohol
Chapter 4 91

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
and Related Conditions (NESARC), the prevalence
of lifetime DSM-IV PDs varied from 0.5 percent to
7.9 percent, depending on the PD type (Hasin &
Grant, 2015). Prevalence rates for BPD and ASPD
are discussed in separate sections.
Diagnostic criteria for PDs have long been
debated among psychopathology researchers
and clinicians, given multiple problems with the
way PDs are classified and diagnosed (Paris,
2014; Sarkar & Duggan, 2010). Problems include
a lack of empirical evidence supporting PDs; the
extensive overlap between diagnostic criteria
among the specific types of PDs as well as
overlap with other mental disorders; the fact that
PD criteria are insufficiently discriminant, which
has resulted in many individuals who exhibit PD
pathology receiving a DSM-IV “personality disorder
not otherwise specified” diagnosis after failing
to “fit in” to any of the specified PD types; and
the difficulty mental health professionals have in
distinguishing PD traits from variants of normal
personality, which means that deciding whether
a person meets PD criteria is often a subjective
judgment. Thus, it is hard to know exactly how
many people have a PD, including how many
people with addiction have co-occurring PDs
(Paris, 2014).
PDs and SUDs
SUD counselors frequently see people with PD
diagnoses in their treatment settings. A review
found the prevalence of PDs among people
with SUDs to be wide ranging but nonetheless
extremely high, varying from about 35 percent
to 65 percent; rates of ASPD ranged from about
14 percent to almost 35 percent (Köck & Walter,
For most people with SUDs, drugs eventually
become more important than jobs, friends,
and family. These changes in priorities
often appear similar to a PD, but diagnostic
clarity for PDs in general is difficult. For
clients with substance-related disorders, the
true diagnostic picture might not emerge
for weeks or months. It is not unusual for
PD symptoms to clear with abstinence,
sometimes even fairly early in recovery.
2018). Similarly, among people undergoing
detoxification for AUD, rates of co-occurring PDs
vary widely from 5 percent to 87 percent (Newton-
Howes & Foulds, 2018). PDs may be present in
as much as 24 percent of people with AUD in the
general population (Newton-Howes & Foulds,
2018).
People with PDs and SUDs differ from those
with PDs only or SUDs only in important ways
(Köck & Walter, 2018), including more severe
mental and substance-related symptoms, longer
persisting substance use, a greater likelihood of
other co-occurring mental disorders (e.g., anxiety,
depressive, and eating disorders), increased
mortality, and higher SUD treatment dropout.
Treatment for PDs and SUDs
No evidence-based treatments exist for PDs
themselves (Bateman, Gunderson, & Mulder, 2015),
but effective treatments are available to address a
variety of PD symptoms, including risk of suicide
and self-harm, affective dysregulation, maladaptive
thought patterns, and poor interpersonal
functioning. Psychotherapy is the primary form of
intervention, as no medications have been approved
for the treatment of PDs. Pharmacotherapy may
be useful as an adjunctive treatment for certain
symptoms like affective lability, impulsivity,
and psychosis, but it is not useful as a primary
intervention. (See the section “Pharmacotherapy”
in Chapter 7 for more information.) Dialectical
behavioral therapy, dynamic deconstructive
psychotherapy, and dual-focused schema therapy
appear promising, particularly for BPD, and have
shown to positively affect psychiatric and addiction-
related outcomes, although, in general, the research
literature on effective treatments for PDs, with or
without co-occurring SUD, is sparse and requires
further evidence (Bateman et al., 2015; Köck &
Walter, 2018).
BPD
The essential feature of BPD is a pervasive pattern
of instability of interpersonal relationships, self-
image, and affects, along with marked impulsivity,
that begins by early adulthood and is present in
a variety of contexts (Exhibit 4.6). Relationships
with others are likely to be unstable—for instance,
people with BPD might remark how wonderful an
Chapter 4 92
TIP 42
Chapter 4—Diagnostic and Cross-Cutting Topics
ADVICE TO THE COUNSELOR: COUNSELING A CLIENT WITH A PD
•
Clients with PDs tend to be limited in their ability to receive, accept, or benefit from corrective feedback.
• A further difficulty is the strong countertransference providers can have in working with these clients,
who may be adept at igniting reactions in a variety of ways. Specific concerns will, however, vary
according to the specific PD and other individual circumstances.
• PDs may cause difficulty forming genuinely positive therapeutic alliances. Some clients tend to frame
reality in terms of their own needs and perceptions and not to understand the perspectives of others.
• The course and severity of PDs can be worsened by the presence of other mental disorders, such as
depressive, anxiety, and psychotic disorders. Be sure to offer empirical treatments for co-occurring
conditions as well as the primary PD and SUD.
• To get the best outcomes possible for clients with PDs and co-occurring SUDs, treatment should
address both conditions to the extent possible and should not neglect one disorder over the other.
EXHIBIT 4.6. Diagnostic Criteria for BPD
A pervasive pattern of instability of interpersonal relationships, self-image, and affects, and marked
impulsivity, beginning by early adulthood and present in various contexts, as indicated by five (or more) of
the following:
1. Frantic efforts to avoid real or imagined abandonment (Note: Do not include suicidal or self-mutilating
behavior covered in Criterion 5.)
2. A pattern of unstable and intense interpersonal relationships characterized by alternating between
extremes of idealization and devaluation
3. Identity disturbance: markedly and persistently unstable self-image or sense of self
4. Impulsivity in at least two areas that are potentially self-damaging (e.g., spending, sex, substance abuse,
reckless driving, binge eating) (Note: Do not include suicidal or self-mutilating behavior covered in
Criterion 5.)
5. Recurrent suicidal behavior, gestures, or threats, or self-mutilating behavior
6. Affective instability due to a marked reactivity of mood (e.g., intense episodic dysphoria, irritability, or
anxiety usually lasting a few hours and only rarely more than a few days)
7. Chronic feelings of emptiness
8. Inappropriate, intense anger or difficulty controlling anger (e.g., frequent displays of temper, constant
anger, recurrent physical fights)
9. Transient, stress-related paranoid ideation or severe dissociative symptoms
Source: APA (2013, p. 663). Reprinted with permission from the DSM-5 (Copyright © 2013). APA. All Rights Reserved.
individual is one day but express intense anger,
disapproval, condemnation, and even hate toward
that same individual a week later. The severe
instability people with BPD experience includes
fluctuating views and feelings about themselves.
Those with BPD often feel good about themselves
and their progress and optimistic about their future
for a few days or weeks, only to have a seemingly
minor experience turn their world upside down,
with concomitant plunging self-esteem and
depressing hopelessness. This instability often
extends to work and school.
When experiencing emotional states they cannot
handle, clients with BPD can be at high risk of
suicidal, self-mutilating, or brief psychotic states.
Chapter 4 93

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
About three-fourths of people with BPD have a
history of self-harm, and the disorder carries a
10-percent lifetime risk of completed suicide (Antai-
Otong, 2016).
Prevalence
BPD has a prevalence of 1.6 percent to 5.9 percent
in the general population but is more common
in mental health settings (about a 10-percent
prevalence rate for outpatient mental health clinics,
about 20 percent among psychiatric inpatients,
and 6 percent in primary care settings) (APA, 2013).
Lifetime prevalence of DSM-IV BPD is 5.9 percent
(Hasin & Grant, 2015).
Women are much more likely to be diagnosed with
BPD, generally at 3 times the rate of men (i.e.,
about 75 percent of cases are women) (APA, 2013).
However, the accuracy of this pattern is dubious
as epidemiologic surveys of the U.S. general
WARNING TO COUNSELORS:
THE MISDIAGNOSIS OF BPD
PDs can be difficult to diagnose. BPD is
especially prone to misdiagnosis, particularly
among women. Reasons for incorrect diagnosis
(or, alternatively, failure to diagnose) are
numerous and include (Fruzzetti, 2017):
•
Stigma surrounding the disorder may lead
providers to refuse to diagnose it or to be
overzealous in diagnosing it (the latter,
especially in women who are “emotional,”
unstable, argumentative, or in crisis).
•
Symptoms of BPD—including emotional
lability, suicidality, and impulsive behaviors—
that are also present in full or in part in many
other disorders, including MDD, bipolar
disorder, PTSD, SUDs, and more. This makes
it difficult to disentangle BPD from other
illnesses.
•
The incorrect belief that BPD is not treatable,
which may make clinicians less likely to give
the diagnosis, especially when they believe
that symptoms reflect a different disorder,
like depression or PTSD.
•
Women being significantly more likely to
receive a BPD diagnosis because of gender
bias.
population have found the lifetime prevalence of
BPD does not actually differ significantly between
men and women (Hasin & Grant, 2015).
BPD and SUDs
BPD is highly prevalent in SUD treatment settings
(and especially inpatient and residential treatment),
with rates averaging about 22 percent across
multiple studies but as high as 53 percent in some
research (Trull et al., 2018). Presence of a 12-month
or lifetime DSM-5 drug use disorder (i.e., an SUD
excluding alcohol) is associated with a 1.7 to 1.8
increased odds of having BPD (Grant et al., 2016).
Approximately 45 percent of individuals with BPD
also have a current SUD, and about 75 percent
have a lifetime SUD (Trull et al., 2018). Opioids,
cocaine, and alcohol are the substances with the
strongest associations with BPD (Trull et al., 2018).
Treatment of BPD and SUDs
People with BPD typically seek behavioral health
services based on their current life conditions and
emotional state. Those who seek mental health
services tend to be acutely emotionally distraught,
needing some relief from how they feel. Similarly,
those who choose (or are directed to choose) a
program are likely experiencing the SUD as the
immediate target for treatment. Consequently,
the average admission of a person with BPD to
a mental health program may be considerably
different from the average admission of a person
with BPD to an SUD treatment program.
In inpatient mental health service settings,
dialectical behavior therapy for BPD is
recommended to help reduce suicide risk, stabilize
behavior, and help clients regulate emotions (Ritter
& Platt, 2016). SUD treatment for people with BPD
can be complicated, and progress may be slow, but
effective interventions are available to help reduce
symptoms and improve functioning. A systematic
review of 10 studies on treatments for BPD and co-
occurring SUDs found good support for dialectical
behavior therapy, dynamic deconstructive therapy,
and dual-focused schema therapy in improving
outcomes of substance use, suicidal gestures and
self-harm, global and social functioning, treatment
utilization, and treatment retention (Lee, Cameron,
& Jenner, 2015).
Chapter 4 94

TIP 42
Chapter 4—Diagnostic and Cross-Cutting Topics
ADVICE TO THE COUNSELOR: COUNSELING A CLIENT WITH BPD
•
Anticipate that client progress will be slow and uneven.
• Assess the risk of self-harm by asking about what is wrong, why now, whether the client has specific
plans for suicide, past attempts, current feelings, and protective factors. (See the discussion of suicidality
at the end of this chapter.)
• Maintain a positive but neutral professional relationship, avoid overinvolvement in the client’s
perceptions, and monitor the counseling process frequently with supervisors and colleagues.
• Set clear boundaries and expectations regarding limits and requirements in roles and behavior.
• Understand that clients with BPD may be inconsistent in their attendance to sessions; anticipate and
discuss these interruptions with the client.
• Assist the client in developing skills (e.g., deep breathing, meditation, cognitive restructuring) to
manage negative memories and emotions.
• Help the client understand the connections between their feelings and their behaviors.
• Monitor newly abstinent individuals with BPD for compulsive sexual behavior, compulsive gambling,
compulsive spending/shopping, or other behaviors that result in negative or even dangerous
consequences.
• Medication management and monitoring should be included in the treatment plan. Individuals
with BPD often are skilled in seeking multiple sources of medication that they favor, such as
benzodiazepines. Once they are prescribed this medication in a mental health system, they may
demand to be continued on the medication to avoid dangerous withdrawal.
• Help clients manage their daily lives and responsibilities by focusing on work, family, and social
functioning.
• At the beginning of a crisis episode, a client with BPD may take a drink or use a different substance in
an attempt to quell the growing sense of tension or loss of control. The client must learn that at this
point, substance use increases harm and real loss of control. The client needs to develop positive coping
strategies to put into play immediately upon experiencing a desire to use substances.
• Educate clients about their SUDs and mental disorders. Clients should learn that treatment for
and recovery from their SUD may progress at a different rate than their treatment for and recovery
from BPD. In addition, although many clients appear to fully recover from their SUDs, the degree of
long-term recovery from BPD is less understood and characterized.
• Written and oral contracts that are simple, clear, direct, and time limited can be a useful part of the
treatment plan. Contracts can help clients create structure and safe environments for themselves,
prevent relapse, or promote appropriate behavior in therapy sessions and in mutual-support meetings.
• To treat people with BPD, pay attention to several areas, such as violence to self or others, transference
and countertransference, boundaries, treatment resistance, symptom substitution, and somatic
complaints.
• Therapists should be realistic in their expectations and know that clients might try to test them. To
respond to such tests, therapists should maintain a matter-of-fact, businesslike attitude, and remember
that people with PDs often display maladaptive behaviors that have helped them to survive in difficult
situations, sometimes called “survivor behaviors.” (See TIP 36, Substance Abuse Treatment for Persons
With Child Abuse and Neglect Issues [CSAT, 2000c]).
Chapter 4 95
TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
CASE STUDY: COUNSELING AN SUD TREATMENT CLIENT WITH BPD
Ming L., an Asian woman, was 32 years old when she was taken by ambulance to the local hospital’s
emergency department (ED). Ming L. had taken 80 Tylenol capsules and an unknown amount of Ativan in a
suicide attempt. Once medically stable, Ming L. was evaluated by the hospital’s social worker to determine
her clinical needs.
The social worker asked Ming L. about her family of origin. Ming L. gave a cold stare and said, “I don’t
talk about that.” Asked if she had ever been sexually abused, Ming L. replied, “I don’t remember.” Ming L.
acknowledged previous suicide attempts as well as a history of cutting her arm with a razor blade during
stressful episodes. She reported that the cutting “helps the pain.”
Ming L. denied having “a problem” with substances but admitted taking “medication” and “drinking
socially.” A review of Ming L.’s medications revealed the use of Ativan “when I need it.” It soon became clear
that Ming L. was using a variety of benzodiazepines (antianxiety medications) prescribed by several doctors
and probably was taking a daily dose indicative of severe SUD. She reported using alcohol “on weekends
with friends” but was vague about the amount. Ming L. did acknowledge that before her suicide attempts,
she drank alone in her apartment. This last suicide attempt was a response to a breakup with her boyfriend.
The counselor reads through notes from an evaluating psychiatrist and reviews the social worker’s report of
his interview with Ming. She notes that the psychiatrist describes the client as having a severe BPD, major
recurrent depression, and SUDs involving both benzodiazepines and alcohol.
Discussion: Knowing the limits of what an SUD treatment counselor or agency can and cannot realistically do
is important. A client with problems this serious is unlikely to do well in standard SUD treatment unless she
is also enrolled in a program qualified to provide treatment to clients with BPD, and preferably in a program
that offers treatment designed especially for this disorder, such as dialectical behavior therapy (Linehan et al.
1999) (although SUD treatment programs are increasingly developing their capacities to address specialized
mental disorders). She is likely to need detoxification either on an inpatient basis or in a long-term outpatient
program that knows how to address clients with PDs.
ASPD
The core features of ASPD are a pervasive
disregard for the rights, feelings, and needs of
others and a failure to form long-term, fulfilling,
adaptive relationships (Exhibit 4.7). Individuals
with ASPD often display a host of challenging
traits: deceitfulness, remorselessness, aggression,
disregard for rules and laws, low conscientiousness,
impulsivity, failure to adhere to social norms,
delinquency, and recklessness. As a result, these
individuals often lead unstable lives and are at high
risk of increased mortality, violence/aggression,
suicide and suicidal behavior, accidents, criminality,
incarceration, and chronic illnesses (e.g., cancer,
HIV) (Black, 2015; Black, 2017; Dykstra, Schumacher,
Mota & Coffey, 2015; Krasnova, Eaton, & Samuels,
2018; McCloskey & Ammerman, 2018). Many
people with ASPD have experienced traumatic or
disruptive childhoods (Sher et al., 2015).
Chapter 4 96
TIP 42
Chapter 4—Diagnostic and Cross-Cutting Topics
EXHIBIT 4.7. Diagnostic Criteria
for ASPD
A. A pervasive pattern of disregard for and
violation of the rights of others, occurring since
age 15 years, as indicated by three (or more) of
the following:
1. Failure to conform to social norms with
respect to lawful behaviors, as indicated by
repeatedly performing acts that are grounds
for arrest
2. Deceitfulness, indicated by repeated lying,
use of aliases, or conning others for personal
profit or pleasure
3. Impulsivity or failure to plan ahead
4. Irritability and aggressiveness, as indicated by
repeated physical fights or assaults
5. Reckless disregard for safety of self or others
6. Consistent irresponsibility, as indicated by
repeated failure to sustain consistent work
behavior or honor financial obligations
7. Lack of remorse, indicated by being indifferent
to or rationalizing having hurt, mistreated, or
stolen from another
B. The individual is at least age 18 years.
C. There is evidence of conduct disorder with
onset before age 15 years.
D. The occurrence of antisocial behavior is not
exclusively during the course of schizophrenia or
bipolar disorder.
Source: APA (2013, p. 659). Reprinted with permission
from the DSM-5 (Copyright © 2013). APA. All Rights
Reserved.
A particularly stigmatizing aspect of ASPD is its
history of being equated with derisive terms like
“sociopath” and “psychopath.” ASPD thus carries
extremely negative connotations that might well be
accurate in only a small percentage of those people
with the disorder. Psychopathy and sociopathy are
personality traits, not mental disorders. They are
related to ASPD but are usually manifest in more
extreme ways than ASPD (e.g., criminal behavior).
In short, psychopathy and sociopathy are not the
same as ASPD. (See the TIP 44, Substance Abuse
Treatment for Adults in the Criminal Justice System
[CSAT, 2005b] for a full discussion of psychopathy
and its relationship to ASPD.)
Prevalence
Twelve-month prevalence rates for DSM-IV ASPD
fall between 0.2 percent and 3.3 percent (APA,
2013). Lifetime DSM-IV ASPD is estimated at
3.6 percent (Hasin & Grant, 2015). Much higher
prevalence rates (up to 70 percent) have been
found in studies of men in treatment for AUD and
SUD treatment clinics, prisons, and other forensic
settings (APA, 2013).
Men are 2 to 8 times more likely to have an ASPD
diagnosis than women (Black, 2017). Lifetime
prevalence of DSM-IV ASPD is estimated at 1.9
percent in women and 5.5 percent in men (Hasin &
Grant, 2015).
ASPD and SUDs
Presence of a 12-month or lifetime DSM-5 drug use
disorder (i.e., an SUD excluding alcohol) is linked
with 1.4 to 2 increased odds of having ASPD (Grant
et al., 2016). Prevalence of ASPD is 7 percent to
40 percent in men with existing SUDs. ASPD is
significantly associated with persistent SUDs (Grant
et al., 2015; Grant et al., 2016).
An analysis of NESARC data (using DSM-IV
diagnoses) revealed gender differences in
comorbidities with ASPD (Alegria et al., 2013).
Men with ASPD were more likely to have AUD, any
drug use disorder, and narcissistic PD. Women with
ASPD were more likely to have any mood disorder,
MDD, dysthymia, any anxiety disorder, panic
disorder, specific phobia, PTSD, and generalized
anxiety disorder (GAD). Women were also more
likely to report childhood adverse events, such as
sexual abuse.
Another study of treatment-seeking individuals
assessing gender differences in individuals with an
ASPD diagnosis similarly found that women with
ASPD tended to be younger, had fewer episodes of
antisocial behavior and higher scores on measures
of trauma, including emotional and sexual abuse,
than men with an ASPD (Sher et al., 2015). Both
women and men with ASPD had comorbid alcohol
(43.6 percent for women and 50 percent for men)
and cannabis use disorders (21.8 percent and 29.7
Chapter 4 97

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
percent, respectively), and men had higher rates of
comorbid cocaine use disorder (22 percent) than
women (7.3 percent). Many people with ASPD use
substances in a polydrug pattern involving alcohol,
marijuana, heroin, cocaine, and methamphetamine.
People with ASPD and SUDs have higher rates
of aggression, impulsivity, and psychopathy than
people with SUDs alone (Alcorn et al., 2013).
Disregard for others’ rights is a key diagnostic
feature of ASPD. Yet most clients who are
actively using substances display behaviors
at some point that show such disregard, so
perceiving the distinction between SUD and
ASPD can be difficult for the mental health and
the SUD treatment fields.
Treatment of ASPD and SUDs
As with most PDs, no empirically supported
treatments exist for ASPD, much less ASPD
combined with SUDs (Bateman et al., 2015).
Various therapies for ASPD with addiction
(e.g., CBT, contingency management) may help
ameliorate substance-related outcomes, like
substance misuse and number of urine-negative
specimens over time, but studies are few and
sample sizes are small (Brazil, van Dongen, Maes,
Mars, & Baskin-Sommers, 2018).
Anxiety Disorders
The distinguishing feature of anxiety disorders is
excessive fear and worry along with behavioral
disturbances, usually out of attempts to avoid or
manage the anxiety. Anxiety disorders are highly
ADVICE TO THE COUNSELOR: COUNSELING A CLIENT WITH ASPD
•
As with CODs in general, clients with ASPD and those with both an SUD and ASPD may be seen as
particularly hard to treat, having poor prognoses, and warranting exclusion from treatment programs
or group counseling. Counselors should maintain a realistic but hopeful, optimistic attitude toward
helping clients improve symptoms and functioning.
• Be aware of the stigma that surrounds ASPD. Many mental health professionals have strongly negative
feelings about working with clients who have ASPD, or any PD. Some may even refuse to accept ASPD
referrals. Treating ASPD can be challenging, but people with ASPD have the same rights to quality,
ethical treatment as anyone else with any other mental disorder.
• Empirical support for interventions to effectively manage ASPD itself is lacking, but effective treatments
exist to address certain symptoms (e.g., risk of suicide or self-harm, affective instability), especially those
of co-occurring depression, anxiety, and SUDs. For instance, CBT can be useful in restructuring negative
thought patterns and reducing impulsivity, improving interpersonal functioning, and providing general
support.
• Heed the warning signs of countertransference and transference. Because many mental health
professionals have negative attitudes or misperceptions about ASPD, countertransference can occur
and prevent counselors from forming an empathic and effective therapeutic alliance with the client.
• Use a positive and empathetic attitude but remain firm in enforcing the structure, rules, and boundaries
of psychotherapy and therapeutic relationship.
• Differentiate true ASPD from substance-related antisocial behavior. This can best be done by looking at
how the person relates to others throughout the course of his or her life. People with this disorder will have
evidence of antisocial behavior preceding substance use and even during periods of enforced abstinence.
• It also is important to recognize that people with substance-related antisocial behavior may be more
likely to have MDD than other typical PDs. However, the type and character of depression that may be
experienced by those with true ASPD have been less well characterized, and their treatment is unclear.
Chapter 4 98

TIP 42
Chapter 4—Diagnostic and Cross-Cutting Topics
comorbid with each other but differ in the types
of situations that arouse fear and the content of
the anxiety-provoking thoughts and beliefs. Panic
attacks are a common fear response in anxiety
disorders but are not limited to these disorders.
Three of the more prevalent anxiety disorders in
the adult population that are likely to co-occur
with addiction are GAD, panic disorder, and social
anxiety disorder (SAD).
GAD
GAD is marked by excessive anxiety and worry
(apprehensive expectation) about a range of
topics or events, like everyday living, finances,
relationships, or work/school performance (Exhibit
4.8). Anxiety is intense, frequent, chronic (i.e.,
lasting at least 6 months), and disproportionate
to the actual threat posed by the subject of worry.
The worry is accompanied by additional cognitive/
physical symptoms.
Panic Disorder
Panic disorder is diagnosed in people who
experience repeated panic attacks that are
distressing and disabling (Exhibit 4.9). A panic
attack is an abrupt but very intense occurrence of
extreme fear. It often only lasts for a few minutes
but the symptoms can be extremely uncomfortable
and upsetting, such as hyperventilation,
palpitations, trembling, sweating, dizziness, hot
flashes or chills, numbness or tingling, and the
sensation or fear of nausea or choking. People
experiencing panic attacks also can experience
psychological symptoms, like feeling as though
they are going to die, as though they are “losing
their mind,” as though things are not real
(derealization), or as if they have left their body
EXHIBIT 4.8. Diagnostic Criteria for GAD
A. Excessive anxiety and worry (apprehensive expectation), occurring more days than not for at least 6
months, about a number of events or activities (such as work or school performance).
B. The individual finds it difficult to control the worry.
C. The anxiety and worry are associated with three (or more) of the following six symptoms (with at least
some symptoms having been present for more days than not for the past 6 months):
Note: Only one item is required in children.
1. Restlessness or feeling keyed up or on edge
2. Being easily fatigued
3. Difficulty concentrating or mind going blank
4. Irritability
5. Muscle tension
6. Sleep disturbance (difficulty falling or staying asleep, or restless, unsatisfying sleep)
D. The anxiety, worry, or physical symptoms cause clinically significant distress or impairment in social,
occupational, or other important areas of functioning.
E. The disturbance is not attributable to the physiological effects of a substance (e.g., a drug of abuse, a
medication) or another medical condition (e.g., hyperthyroidism).
F. The disturbance is not better explained by another mental disorder (e.g., anxiety or worry about having
panic attacks in panic disorder, negative evaluation in SAD [social phobia], contamination or other obsessions
in obsessive-compulsive disorder, separation from attachment figures in separation anxiety disorder,
reminders of traumatic events in PTSD, gaining weight in anorexia nervosa [AN], physical complaints in
somatic symptom disorder, perceived appearance flaws in body dysmorphic disorder, having a serious illness
in illness anxiety disorder, or the content of delusional beliefs in schizophrenia or delusional disorder).
Source: APA (2013, pp. 222). Reprinted with permission from the DSM-5 (Copyright © 2013). APA. All Rights Reserved
Chapter 4 99

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
(depersonalization). Because of the distressing
nature of panic attacks, people with panic disorder
may constantly worry about having subsequent
attacks or engage in behaviors in an attempt to
control the attacks (like avoiding places where they
have previously had a panic attack or fear they
might have one).
Panic disorder often is underdiagnosed at the
beginning of treatment or else is seen as secondary
to the more significant disorders, which are the
primary focus of treatment. However, panic
disorder can significantly impede a person’s ability
to take certain steps toward recovery, such as
getting on a bus to go to a meeting or sitting
in a 12-Step meeting. Sometimes counselors
can erroneously identify these behaviors as
manipulative or treatment-resistant behaviors.
EXHIBIT 4.9. Diagnostic Criteria for Panic Disorder
A. Recurrent unexpected panic attacks. A panic attack is an abrupt surge of intense fear or intense
discomfort that reaches a peak within minutes, and during which time four (or more) of the following
symptoms occur:
Note: The abrupt surge can occur from a calm state or an anxious state.
1. Palpitations, pounding heart, or accelerated heart rate
2. Sweating
3. Trembling or shaking
4. Sensations of shortness of breath or smothering
5. Feelings of choking
6. Chest pain or discomfort
7. Nausea or abdominal distress
8. Feeling dizzy, unsteady, lightheaded, or faint
9. Chills or heat sensations
10. Paresthesias (numbness or tingling sensations)
11. Derealization (feelings of unreality) or depersonalization (being detached from oneself)
12. Fear of losing control or “going crazy”
13. Fear of dying
Note: Culturespecific symptoms (e.g., tinnitus, neck soreness, headache, uncontrollable screaming or
crying) may be seen. Such symptoms should not count as one of the four required symptoms.
B. At least one of the attacks has been followed by 1 month (or more) of one or both of the following:
1. Persistent concern or worry about additional panic attacks or their consequences (e.g., losing control,
having a heart attack, “going crazy”).
2. A significant maladaptive change in behavior related to the attacks (e.g., behaviors designed to avoid
having panic attacks, such as avoidance of exercise or unfamiliar situations).
C. The disturbance is not attributable to the physiological effects of a substance (e.g. a drug of abuse, a
medication) or another medical condition (e.g., hyperthyroidism, cardiopulmonary disorders).
D. The disturbance is not better explained by another mental disorder (e.g., the panic attacks do not occur
only in response to feared social situations, as in SAD; in response to circumscribed phobic objects or
situations, as in specific phobia; in response to obsessions, as in obsessive-compulsive disorder; in response
to reminders of traumatic events, as in PTSD; or in response to separation from attachment figures, as in
separation anxiety disorder).
Source: APA (2013, pp. 208–209). Reprinted with permission from the DSM-5 (Copyright © 2013). APA. All Rights Reserved.
100 Chapter 4
TIP 42
Chapter 4—Diagnostic and Cross-Cutting Topics
Agoraphobia
One of the changes in DSM-5 concerns the
separation of agoraphobia from panic disorder.
Although now two distinct conditions, they are
closely related and many of their symptoms
overlap. In agoraphobia, people exhibit a strong
fear of being in certain places or situations where
escape could be difficult should the person
experience panic-like symptoms or otherwise feel
anxious or a loss of control. Situations typically
include being in crowds, on public transportation,
in open spaces (like bridges), in closed spaces (such
as the movie theater), or away from home. People
with agoraphobia avoid these situations for fear
of having panic attacks or similar incapacitating
or embarrassing symptoms (e.g., vomiting,
incontinence), or they tolerate them but with great
distress and discomfort.
Agoraphobia often occurs without panic disorder
in community settings but frequently occurs
with panic disorder in clinical settings; the two
conditions are distinct yet intertwined (APA, 2013;
Asmundson, Taylor, & Smits, 2014). SUDs can and
do co-occur with agoraphobia (Goodwin & Stein,
2013; Marmorstein, 2012), but literature on this
co-occurrence is relatively small compared with
other anxiety disorders or has been examined
as occurring with panic disorder (Cougle, Hakes,
Macatee, Chavarria, & Zvolensky, 2015) rather than
occurring alone. Furthermore, research is more
focused on its co-occurrence with nicotine than
other substances.
The linkage of agoraphobia with addiction may be
explained by its relationship with panic disorder
and not with SUD. Thus, agoraphobia is not a
subject of focus for this chapter but is mentioned
here because of its interrelationship with panic
disorder, which addiction counselors are likely to
see in their clients.
SAD
Social phobia describes the persistent and
recognizably irrational fear of embarrassment
and humiliation in social situations (Exhibit 4.10).
The social phobia may be quite specific (e.g.,
public speaking) or may become generalized to
all social situations. SAD, also called social phobia
in DSM-5, involves intense anxiety or fear in social
or performance situations. Individuals may fear
being judged by others (e.g., being perceived as
stupid, awkward, or boring); being embarrassed
or humiliated; accidentally offending someone;
or being the center of attention. As a result, the
individual will often avoid social or performance
situations; when a situation cannot be avoided, they
experience significant anxiety and distress. Many
people with SAD have strong physical symptoms
(e.g., rapid heart rate, nausea, sweating) and may
experience full-blown attacks when confronting a
feared situation. They recognize that their fear is
excessive and unreasonable, but people with SAD
often feel powerless against their anxiety.
EXHIBIT 4.10. Diagnostic Criteria for SAD
A. Marked fear or anxiety about one or more social situations in which the individual is exposed to possible
scrutiny by others. Examples include social interactions (e.g., having a conversation, meeting unfamiliar
people), being observed (e.g., eating or drinking), and performing in front of others (e.g., giving a speech).
Note: In children, the anxiety must occur in peer settings and not just during interactions with adults.
B. The individual fears that he or she will act in a way or show anxiety symptoms that will be negatively
evaluated (i.e., will be humiliating or embarrassing; will lead to rejection or offend others).
C. The social situations almost always provoke fear or anxiety.
Note: In children, the fear or anxiety may be expressed by crying, tantrums, freezing, clinging, shrinking, or
failing to speak in social situations.
D. The social situations are avoided or endured with intense fear or anxiety.
Continued on next page
Chapter 4 101
TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
Continued
E. The fear or anxiety is out of proportion to the actual threat posed by the social situation and to the
sociocultural context.
F. The fear, anxiety or avoidance is persistent, typically lasting for 6 months or more.
G. The fear, anxiety, or avoidance causes clinically significant distress or impairment in social, occupational,
or other important areas of functioning.
H. The fear, anxiety, or avoidance is not attributable to the physiological effects of a substance (e.g., a drug
of abuse, a medication) or another medical condition.
I. The fear, anxiety, or avoidance is not better explained by the symptoms of another mental disorder, such
as panic disorder, body dysmorphic disorder, or autism spectrum disorder.
J. If another medical condition (e.g., Parkinson’s disease, obesity, disfigurement from burns or injury) is
present, the fear, anxiety, or avoidance is clearly unrelated or is excessive.
Specify if:
•
Performance only: If the fear is restricted to speaking or performing in public
Source: APA (2013, pp. 202–203). Reprinted with permission from the DSM-5 (Copyright © 2013). APA. All Rights Reserved.
Prevalence
The lifetime prevalence of any anxiety disorder is
estimated at over 30 percent; 12-month prevalence
estimates are approximately 19 percent (Harvard
Medical School, 2005). A recent World Health
Organization (WHO) survey and analysis using
DSM-5 diagnostic criteria found the community
lifetime prevalence of GAD in the U.S. is 7.8
percent, and 12-month prevalence is 4 percent
(Ruscio et al., 2017). Women are twice as likely
as men to experience the disorder (APA, 2013).
Lifetime prevalence of panic attacks (ascertained
as part of an analysis of data collected worldwide
and defined per DSM-5 criteria) with or without
panic disorder is almost 28 percent (de Jonge
et al., 2016). The 12-month prevalence in the
general population for panic disorder is about 2.4
percent; lifetime prevalence is 6.8 percent (Kessler,
Petukhova, Sampson, Zaslavsky, & Wittchen, 2012).
The 12-month prevalence for SAD is approximately
7 percent; rates in the community trend higher in
women (1.5 times) than men, especially in young
adults (APA, 2013).
Anxiety Disorders and SUDs
The relationship between substance use and
anxiety disorders is complex and multifaceted, and
the two disorders commonly co-occur. Presence of
a 12-month or lifetime DSM-5 drug use disorder
(i.e., an SUD excluding alcohol) is associated with
a 1.2 to 1.3 increased odds of having any anxiety
disorder, a 1.0 to 1.3 increased odds of having
panic disorder, a 1.2 to 1.3 increased odds of
having GAD, and a 1.1 to 1.3 increased odds of
having SAD (Grant et al., 2016). Recent analyses
indicate lifetime (but not 12-month) diagnosis
of drug and alcohol use disorders is associated
with GAD (Grant et al., 2015; Grant et al., 2016).
Twelve-month prevalence of panic disorder with
co-occurring SUD is 11 percent, and lifetime co-
occurrence is 28 percent (de Jonge et al., 2016).
When anxiety and SUDs co-occur, the disorders
affect development and maintenance of
comorbidity, and each disorder modifies the
presentation and treatment outcomes for the
other (Brady, Haynes, Hartwell, & Killeen, 2013).
Consequently, people with anxiety disorders and
co-occurring SUDs experience worse outcomes
than those with either disorder alone, including
greater disability, more hospitalizations and
healthcare utilization, poorer functioning, more
difficulties in interpersonal relationships, more
severe symptoms, worse health-related quality
of life, and poorer treatment response (Buckner,
Heimberg, Ecker, & Vinci, 2013; Magidson, Liu,
Lejuez, & Blanco, 2012). GAD and addiction are
102 Chapter 4

TIP 42
Chapter 4—Diagnostic and Cross-Cutting Topics
ADVICE TO THE COUNSELOR: COUNSELING A CLIENT WITH AN ANXIETY
DISORDER
•
Treating only one disorder is usually insufficient, as is treating disorders in isolation (e.g., sequentially).
Clients with both anxiety and addictions need concurrent treatment that equally targets both conditions.
• Pharmacotherapies can effectively reduce anxiety symptoms (especially if combined with
psychotherapy) and may need to be a part of clients’ treatment plans. But prescribing psychotropic
medication in someone with an SUD can be tricky. As needed, refer the client to a mental health
professional for a full assessment to determine whether medication is warranted and how to safely
integrate it into the treatment plan.
• People in recovery from SUDs may have conflicting feelings about taking medication. Not all clients
with anxiety disorders will need pharmacotherapy, but in many cases it can help and, when combined
with psychotherapy, is frequently more effective at reducing anxiety symptoms and improving
functioning than either medication or psychotherapy alone. That said, do not “push” medications on
clients; instead, invite them to explore their feelings about taking medications and discuss advantages
and disadvantages of such.
• Selective serotonin reuptake inhibitors are commonly used to help manage GAD, panic disorder, and
SAD but should not be taken with alcohol. Addiction counselors must educate clients taking anxiolytics
(especially benzodiazepines) about the indications, contraindications, adverse effects, and dangers
of medication–alcohol interactions. For clients with anxiety and AUD specifically, referral to a mental
health professional to discuss medication management may be needed.
• Be mindful of the increased risk of dependence and abuse liability with benzodiazepines. This risk
might be heightened in people who misuse substances to self-medicate their anxiety symptoms or
in people with SUDs in general. Use CBT known to effectively treat anxiety disorders to minimize or
augment the use of medications.
• Educate clients on the dangers of using substances to self-medicate and control anxiety symptoms, and
make distress tolerance, self-regulation, and adaptive coping skills major focuses of treatment.
• Assess for (and advise against) over-the-counter substances that can cause or exacerbate anxiety
symptoms, like caffeine pills and weight loss supplements.
• Understand the special sensitivities of clients with SAD to social situations. Although group CBT can
help people with SAD learn to become more comfortable in social environments, individual CBT can be
equally effective and should be an option for clients who decline group treatment.
• When clients do not improve as expected, the cause is not necessarily treatment failure or client
noncompliance. Clients may be compliant and plans may be adequate, but disease processes remain
resistant.
• Expect a longer treatment duration compared with treatment for either anxiety or addiction alone.
• Clients with severe and persistent SUDs and anxiety disorders should not be seen as resistant,
manipulative, or unmotivated but in need of intensive support.
• Symptoms may result from SUDs, not underlying mental disorders; careful, continual assessment is key.
• Anxiety symptoms and disorders are risk factors for suicidal ideation and suicide attempt. Use suicide
risk mitigation (e.g., routine assessment, thorough documentation) and collaborate with clients to
implement safety plans.
Chapter 4 103

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
CASE STUDY: GAD AND PROTRACTED WITHDRAWAL
Ray Y., a 50-year-old husband and father of teenagers, is going through protracted alcohol withdrawal. He
appears “edgy” and irritable, sometimes sad, and complains to his SUD treatment counselor of insomnia,
headaches, and an upset stomach. He tells the counselor he can barely stand not to drink: “I’m jumping
out of my skin.” Although these symptoms are common during protracted withdrawal, because they have
persisted for over a month the counselor begins a more detailed exploration.
The counselor asks Ray Y. whether he had these symptoms before he used alcohol, and Ray Y. says he’s
“always been this way.” He worries about everything, even events that are weeks away. His family vacations
are nightmares because every aspect of vacation planning troubles him and keeps him awake. During
family therapy, it becomes apparent that his daughter deeply resents his controlling and distrustful
behavior, as well as his overprotective stance toward all her social commitments. The counselor refers
Ray Y. to a psychiatrist, who diagnoses GAD, begins a course of medication, and initiates mental health
counseling. The family receives help coping with Ray Y.’s disorder, and his daughter is referred for short-
term counseling to help her address the mental problems she is beginning to develop as a result of her
father’s excessive control.
Discussion: Anxiety symptoms are quite common during protracted withdrawal, but counselors should
consider the possibility that an anxiety disorder is indicated. Symptoms should be tracked to see whether
they persist beyond the normal time that might be expected for protracted withdrawal. Protracted
withdrawal can occur up to a few months to a year, particularly with antianxiety medication. It varies
according to severity, duration, and type of medication. Most protracted withdrawal is between 1 and 3
months. Counselors should also be aware of the effect of such disorders on close family members. Children
and adolescents may not understand that a parent has a mental disorder and may be relieved to have a
way of understanding and coping with difficult behavior.
associated with higher rates of heavy alcohol use,
hospitalizations, relapse, and leaving treatment
against medical advice compared with people with
SUDs but no GAD (Domenico, Lewis, Hazarika, &
Nixon, 2018).
Anxiety symptoms and anxiety disorders are
predictors of suicidal ideation and suicide attempt
(Bentley et al., 2016); given that SUDs also elevate
risk of suicide (Yuodelis-Flores & Ries, 2015), the
combination of the two suggests efforts to mitigate
suicide risk mitigation are warranted with these
clients.
Treatment of Anxiety Disorders and SUDs
SUD treatment for people with anxiety should
include interventions that address the anxiety
as well as the addiction. Clients may report a
reduction in some anxiety symptoms during
detoxification or early in recovery (McHugh, 2015).
That said, SUD treatment alone is not sufficient
to address the co-occurring anxiety. Further,
the presence of an anxiety disorder complicates
SUD treatment and can make achieving and
sustaining abstinence and preventing relapse more
problematic (McHugh, 2015).
Concurrent, integrated treatments that include CBT
or exposure therapy can safely, effectively reduce
psychiatric and SUD symptoms but in some studies
are no more effective than placebo (McHugh, 2015).
Schizophrenia and Other
Psychotic Disorders
Psychotic Disorders
Psychotic disorders are characterized by a severely
incapacitated mental and emotional state involving
a person’s thinking, perception, and emotional
control. Key features include distorted thoughts in
which an individual has false beliefs, sensations, or
perceptions that are imagined, are very extreme,
or both; and unusual emotional and behavioral
states with deterioration in thinking, judgment,
104 Chapter 4

TIP 42
Chapter 4—Diagnostic and Cross-Cutting Topics
self-control, or understanding. Psychotic disorders
are usually expressed clinically as a combination of:
•
Delusions: Beliefs that are fixed, resistant
to change, and are directly contradicted by
evidence or otherwise not grounded in reality
(e.g., the belief that one is being followed
by people from Mars, or that one is a very
important person to whom the President wants
to speak right away).
•
Hallucinations: Hearing, seeing, tasting, or
feeling things that are not there and being
unable to recognize that what is being
experienced is not real (such as hearing voices
that say self-condemning or other disturbing
things, or seeing a person who isn’t really there).
•
Disorganized thinking: This is reflected in
speech that is incoherent (“word salad”),
illogical, uses unconventional or made-up
words (neologisms and word approximations),
fluctuates from topic to topic (loose
associations), or is completely unrelated to
subject matter at hand (tangential speech).
•
Grossly disorganized or abnormal motor
behavior: This includes a wide range of
odd behaviors, such as laughing or smiling
inappropriately, grimacing, staring, talking to
oneself, purposeless or peculiar movements
and mannerisms, mimicking others’ speech or
movements (echolalia and echopraxia), and
random agitation. A specific psychomotor
disturbance called catatonia—which includes
immobility, stupor, and holding rigid body
positions against gravity over extended periods
of time (catalepsy)—can occur in schizophrenia
but is also present in other mental disorders (like
bipolar disorder) and some medical conditions.
•
Negative symptoms: A constellation of
symptoms reflecting diminished emotional
expression and self-motivated purposeful
activities (avolition). Negative symptoms also
may include diminished speech output (alogia)
or poverty of speech (e.g., one-word answers),
motivation, ability to experience pleasure
(anhedonia), or interest in social activities
(asociality).
Although schizophrenia is perhaps the most well
known psychotic disorder, people with bipolar
disorders may experience psychotic states
during periods of mania—the heightened state
of excitement, little or no sleep, impulsiveness,
and poor judgment (see the section “Bipolar
I Disorder”). Other conditions also can be
accompanied by a psychotic state, including toxic
poisoning, other metabolic difficulties (infections
[e.g., latestage AIDS]), and other mental disorders
(MDD, dementia, PTSD, alcohol withdrawal states,
brief reactive psychoses, and others).
SUD treatment counselors typically do not see
clients in the throes of an acute psychotic episode,
as such psychotic patients more likely present, or
are referred to, EDs and mental health services
facilities. Counselors are more likely to encounter
such clients in a “residual” or later and less active
phase of the illness, the time at which these
individuals may receive treatment for their SUDs
in an SUD treatment agency. Even if the SUD
treatment counselor never sees a client during an
actively psychotic period, knowing what the client
experiences as a psychotic episode will enable
the counselor to understand and assist the client
more effectively. On the other hand, counselors are
increasingly treating clients with methamphetamine
dependence who often have residual paranoid and
psychotic symptoms and may need antipsychotic
medications.
Schizophrenia
No single symptom specifically indicates or
characterizes schizophrenia. Symptoms include
a range of cognitive, behavioral, and emotional
dysfunctions (Exhibit 4.11). Thus, schizophrenia
is a heterogeneous clinical syndrome. Symptoms
of schizophrenia include delusions, hallucinations,
disorganized speech (e.g., frequent derailment
or incoherence), grossly disorganized or
catatonic behavior, and deficits in certain areas
of functioning—for example, the inability to
initiate and persist in goal-directed activities.
These symptoms regularly develop before the first
episode of a schizophrenic breakdown, sometimes
stretching back years and often intensifying prior
to reactivations of an active, acutely psychotic
state. Clinicians generally divide schizophrenia
symptoms into positive and negative symptoms.
Acute course schizophrenia is characterized by
positive symptoms like hallucinations, delusions,
excitement, motor manifestations (such as agitated
Chapter 4 105

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
EXHIBIT 4.11. Diagnostic Criteria for Schizophrenia
A. Two (or more) of the following, each present for a significant portion of time during a 1-month period (or
less if successfully treated). At least one of these must be 1, 2, or 3:
1. Delusions
2. Hallucinations
3. Disorganized speech (e.g., frequent derailment or incoherence)
4. Grossly disorganized or catatonic behavior
5. Negative symptoms, (i.e., diminished emotional expression or avolition)
B. For a significant portion of the time since the onset of the disturbance, level of functioning in one or
more major areas, such as work, interpersonal relations, or self-care, is markedly below the level achieved
prior to the onset (or when the onset is in childhood or adolescence, there is failure to achieve expected
level of interpersonal, academic, or occupational functioning).
C. Continuous signs of the disturbance persist for at least 6 months. This 6-month period must include at
least 1 month of symptoms (or less if successfully treated) that meet Criterion A (i.e., active-phase symptoms)
and may include periods of prodromal or residual symptoms. During these prodromal or residual periods, the
signs of the disturbance may be manifested by only negative symptoms or by two or more symptoms listed
in Criterion A present in an attenuated form (e.g., odd beliefs, unusual perceptual experiences).
D. Schizoaffective disorder and depressive or bipolar with psychotic features have been ruled out because
either (1) no major depressive or manic episodes have occurred concurrently with the active-phase
symptoms, or (2) if mood episodes have occurred during active-phase symptoms, they have been present
for a minority of the total duration of the active and residual periods of the illness.
E. The disturbance is not attributable to the physiological effects of a substance (e.g., a drug of abuse, a
medication) or another medical condition.
F. If there is a history of autism spectrum disorder or a communication disorder of childhood onset, the
additional diagnosis of schizophrenia is made only if prominent delusions or hallucinations, in addition to the
other required symptoms of schizophrenia, also are present for at least 1 month (or less if successfully treated).
Specify if:
The following course specifiers are only to be used after a 1-year duration of the disorder and if they are not
in contradiction to the diagnostic course criteria.
•
First episode, currently in acute episode: First manifestation of the disorder meeting the defining
diagnostic symptom and time criteria. An acute episode is a time period in which the symptom criteria
are fulfilled.
•
First episode, currently in partial remission: Partial remission is a period of time during which an
improvement after a previous episode is maintained and in which the defining criteria of the disorder are
only partially fulfilled.
•
First episode, currently in full remission: Full remission is a period of time after a previous episode during
which no disorder-specific symptoms are present.
•
Multiple episodes, currently in acute episode: Multiple episodes may be determined after a minimum of
two episodes (i.e., after a first episode, a remission and a minimum of one relapse).
•
Multiple episodes, currently in partial remission
•
Multiple episodes, currently in full remission
•
Continuous: Symptoms fulfilling the diagnostic symptom criteria of the disorder are remaining for the
majority of the illness course, with subthreshold symptom periods being very brief relative to the overall
course.
Continued on next page
106 Chapter 4
TIP 42
Chapter 4—Diagnostic and Cross-Cutting Topics
Continued
•
Unspecified
Specify if:
•
With catatonia
Specify current severity:
•
Severity is rated by a quantitative assessment of the primary symptoms of psychosis, including delusions,
hallucinations, disorganized speech, abnormal psychomotor behavior, and negative symptoms. Each of
these symptoms may be rated for its current severity (most severe in the last 7 days) on a 5-point scale
ranging from 0 (not present) to 4 (present and severe).
Note: Diagnosis of schizophrenia can be made without using this severity specifier.
Source: APA (2013, pp. 99–100). Reprinted with permission from the DSM-5 (Copyright © 2013). APA. All Rights Reserved.
behavior or catatonia), disorganized speech,
relatively minor thought disturbances, and positive
response to neuroleptic medication. Chronic
course schizophrenia is characterized by negative
symptoms, such as lack of enjoyment (anhedonia),
apathy, lack of emotional expressiveness (flat
affect), and social isolation. Some clients will live
their entire lives exhibiting only a single psychotic
episode; others may have repeated episodes
separated by varying durations of time.
Prevalence
Community prevalence rates for schizophrenia using
DSM-5 criteria are not available at the time of this
publication. The lifetime prevalence rate for adults
with DSM-IV schizophrenia is between 0.3 percent
and 0.7 percent (APA, 2013). The National Institute
of Mental Health (NIMH; 2018) reports similar but
slightly lower numbers, ranging between 0.25
percent and 0.64 percent. Although its prevalence
is very low, schizophrenia is very burdensome and
considered one of the top 15 leading causes of
global disability (GBD 2016 Disease and Injury
Incidence and Prevalence Collaborators, 2017).
Schizophrenia/Other Psychotic Disorders
and SUDs
Substance misuse often occurs in people with
schizophrenia and other psychotic disorders.
In a study of more than 1,200 people with
schizophrenia (Kerner, 2015), lifetime SUD
prevalence was 55 percent, including alcohol abuse
Individuals with SMI (including schizophrenia,
schizoaffective disorder, and bipolar disorder with
psychotic features) die approximately 10 to 25 years
earlier than the general population, mostly because
of the effects of physical illnesses caused at least
in part by SUDs (e.g., heart disease, lung disease,
infectious disease) (Hartz et al., 2014; WHO, n.d.).
at 17 percent, alcohol dependence at 26 percent,
illicit drug abuse at 13 percent, and illicit drug
dependence at 14 percent. The most commonly
used substances were alcohol (43 percent),
cannabis (35 percent), and other illegal substances
(27 percent). Compared with the general
population, people with severe psychotic disorders
have 4 times greater risk of heavy alcohol use, 3.5
times the risk of heavy cannabis use, and 4.6 times
the risk of recreational drug use (Hartz et al., 2014).
The combination of substance misuse in people
with schizophrenia or other psychotic disorders
contributes to shortened mortality and an
increased likelihood of deleterious health and
functional outcomes, including a higher risk for
self-destructive and violent behaviors, victimization,
suicide, housing instability, poor physical health,
cognitive impairment, employment problems,
legal difficulties, and unstable social relationships
(Bennett, Bradshaw, & Catalano, 2017; Trudeau
et al., 2018). Further, substance misuse in
schizophrenia can worsen disease course and may
reduce adherence to antipsychotic medication
(Werner & Covenas, 2017).
Chapter 4 107

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
CASE STUDY: COUNSELING AN SUD TREATMENT CLIENT WITH
SCHIZOPHRENIA
Adolfo M. is a 40-year-old Latino man who began using cannabis and alcohol at 15. He was diagnosed as
having schizophrenia when he was 18 and began using cocaine at 19. Sometimes, he lives with his sister
or with temporary girlfriends; sometimes, on the street. He has never had a sustained relationship, and he
has never held a steady job. He has few close friends. He has had periods of abstinence and freedom from
hallucinations and major delusions, but he generally has unusual views of the world that emerge quickly in
conversation.
Adolfo M. has been referred to an SUD treatment counselor, who was hired by the mental health center to
do most of the group and individual drug/alcohol work with clients. The first step the counselor takes is to
meet with Adolfo M. and his case manager together. This provides a clinical linkage and allows them to get
the best history. The clinical history reveals that Adolfo M. does best when he is sober and on medications,
but there are times when he will be sober and not adhere to a medical regimen, or when he is both taking
medications and drinking (although these periods are becoming shorter in duration and less frequent).
His case manager often is able to redirect him toward renewed sobriety and adherence to medications,
but Adolfo M. and the case manager agree that the cycle of relapse and the work of pulling things back
together is wearing them both out. After the meeting, the case manager, counselor, and Adolfo M. agree
to meet weekly for a while to see what they can do together to increase the stable periods and decrease
the relapse periods. After a month of these planning meetings, the following plan emerges. Adolfo M. will
attend SUD treatment groups for people with CODs (run by the counselor three times a week at the clinic),
see the team psychiatrist, and attend local dual disorder AA meetings. The SUD treatment group he will
be joining is one that addresses not only addiction problems but also difficulties with treatment follow-
through, life problems, ways of dealing with stress, and the need for social support for clients trying to get
sober. When and if relapse happens, Adolfo M. will be accepted back without prejudice and supported in
recovery and treatment of both his substance misuse and mental disorders; however, part of the plan is
to analyze relapses with the group. His goal is to have as many sober days as possible with as many days
adhering to a medical regimen as possible. Another aspect of the group is that monthly, 90-day, 6-month,
and yearly sobriety birthdays are celebrated. Part of the employment program at the center is that clients
need to have a minimum of 3 months of sobriety before they will be placed in a supported work situation,
so this becomes an incentive for sobriety as well.
Discussion: SUD treatment counselors working within mental health centers should be aware of the
need not only to work with the client but also to form solid working relationships with case managers,
the psychiatrist, and other personnel. Seeing clients with case managers and other team members is a
good way to establish important linkages and a united view of the treatment plan. In Adolfo M.’s case, the
counselor used his ties with the case manager to good effect and also is using relapse prevention and
contingency management strategies appropriately (see Chapter 5 for a discussion of relapse prevention).
ADVICE TO THE COUNSELOR: COUNSELING A CLIENT WITH
SCHIZOPHRENIA OR ANOTHER PSYCHOTIC DISORDER
•
Understand that what looks like resistance or denial may in reality be a manifestation of negative
symptoms of schizophrenia.
• Use a recovery perspective and a compassionate attitude toward the client. This can convey hope and
allow the clients to envision significant recovery and improvement in his or her life.
• Obtain a working knowledge of the signs and symptoms of the disorder.
Continued on next page
108 Chapter 4

TIP 42
Chapter 4—Diagnostic and Cross-Cutting Topics
Continued
• Be aware that an accurate understanding of the role of SUDs in the client’s psychotic disorder requires a
multiple-contact, longitudinal assessment.
• Work closely with a psychiatrist or mental health professional.
• Expect crises associated with the mental disorder and have available resources (e.g., crisis intervention,
psychiatric consultation) to facilitate stabilization.
• As appropriate, assist the client to obtain Medicare, Medicaid, Temporary Assistance to Needy Families,
disability payments, and other social services.
• Make available psychoeducation on the psychiatric condition and use of medication. The
psychoeducational component of treatment should include information about mental disorders and
SUDs, from causes and the natural histories of the disorders to the recovery process and how the
illnesses can interact.
• Understand that medication adherence is critical to control positive symptoms and maintain stability/
functionality. Yet nonadherence is common. Make medication monitoring and adherence a part of
treatment by:
− Providing psychoeducation about its importance.
− Checking in with clients about the status of their symptoms (given that nonresponsiveness to
medication may be a reason for nonadherence).
− Discussing with clients their reasons for not taking the medication (e.g., unpleasant side effects, high
cost, failing to remember to take them).
− Using motivational interviewing techniques to explore clients’ expectations and beliefs about taking
(and not taking) medication, which can help identify barriers to behavior change.
− Working with clients to develop helpful reminders, alerts, or other solutions to practical obstacles.
If cost is an issue, connect the client to a prescription assistance program (offered by numerous
nonprofit organizations, state/county/federal agencies, and pharmaceutical companies) or consult
with the client’s prescriber about the possibility of switching the client to a lower cost medication.
− Enlisting, when appropriate, the help of family or loved ones to aid in giving positive reinforcement
and supporting clients in adhering to their medication.
• Ensure that the treatment program philosophy is based on a multidisciplinary team approach. Ideally,
team members should be cross-trained, and there should be representatives from the medical, mental
health service, and addiction systems. The overall goals of long-term management should include:
− Providing comprehensive and integrated services for both the mental disorders and SUDs.
− Taking a long-term focus that addresses biopsychosocial matters in accord with a treatment plan with
goals specific to a client’s situation.
• Provide frequent breaks and shorter sessions or meetings.
• Use structure and support.
• Present material in simple, concrete terms with examples and use multimedia methods.
• Encourage participation in social clubs with recreational activities.
• Teach the client skills for detecting early signs of relapse for both mental illness and substance use.
• Consider including family members and community supports, when appropriate, in overall treatment.
Continued on next page
Chapter 4 109
TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
Continued
• Involve family in psychoeducational groups that specifically focus on education about SUDs and
psychotic disorders; establish support groups of families and significant others.
• Understand that psychotic disorders and SUDs tend to be chronic disorders with multiple relapses
and remissions, requiring long-term treatment. For clients with CODs involving psychotic disorders, a
long-term approach is imperative.
• Monitor clients for signs of substance misuse relapse and a return of psychotic symptoms.
• Remember that suicide is a significant risk in schizophrenia, more so when co-occurring with SUDs.
Ongoing monitoring/ assessment of suicidal ideation, gestures, plans, and attempts throughout
treatment is imperative. Work with clients to form safety plans/contracts; make positive coping skills
part of interventions.
Treatment of Schizophrenia/Other Psychotic
Disorders and SUDs
Antipsychotic medication is the standard of care
for reducing positive symptoms (e.g., delusions,
hallucinations) whereas various psychosocial inter-
ventions and approaches can help address addiction
recovery. Specifically, integrated CBT, group
behavioral therapy, contingency management,
12-Step facilitation, motivational enhancement,
motivational interviewing, assertive community
treatment, or (preferably) a combination thereof
may all help reduce substance use (quantity,
frequency, and severity), increase abstinence, reduce
number of drinking days, lower relapse rates,
reduce the number of positive urine samples, and
decrease negative consequences of substance use
in people with SUDs and schizophrenia or other SMI
(including psychotic disorders) (Bennett et al., 2017;
De Witte, Crunelle, Sabbe, Moggi, & Dom, 2014).
These approaches have also been associated with
improvements in psychiatric symptoms (including
negative symptoms), scores of global functioning,
hospitalizations, and achieving stable housing (De
Witte et al., 2014). Integrated treatments appear to
yield more positive results than single interventions
and are the recommended approach (De Witte et
al., 2014).
Attention Decit Hyperactivity
Disorder
ADHD is marked by a chronic inability to direct,
control, or sustain attention; hyperactivity; or
both (Exhibit 4.12). People with ADHD often have
difficulty concentrating for even short periods
of time. They may be disorganized and restless
or seem always “on the go,” constantly moving
and fidgeting. Some people with ADHD behave
impulsively.
Although ADHD is frequently associated with
children, the disorder can persist into adulthood
and for some individuals can begin in adulthood.
In adults, symptoms can include having a short
temper, difficulty being productive at work, and an
inability to sustain relationships.
The three types of ADHD are combined type
(person has difficulty paying attention and
hyperactivity); predominantly inattentive; and
predominantly hyperactiveimpulsive.
Prevalence
At the time of this publication, 12-month and
lifetime ADHD prevalence rates among all age
groups in the general population using DSM-5
criteria are not readily available. However, data
from the National Survey of Children’s Health show
that 6.1 million children and adolescents ages 2
to 17 years had ever been diagnosed with ADHD
(Danielson et al., 2018).
The prevalence of ADHD in adults is less studied
than in children. The overall current prevalence
of adult ADHD (using DSM-IV criteria) is around
2.5 percent (APA, 2013; Simon, Czobor, Balint,
Meszaros, & Bitter, 2009). Epidemiological
population-based survey data on U.S. adults with
ADHD (Kessler et al., 2005) suggest the estimated
110 Chapter 4

TIP 42
Chapter 4—Diagnostic and Cross-Cutting Topics
EXHIBIT 4.12. Diagnostic Criteria for ADHD
A. A persistent pattern of inattention and/or hyperactivity-impulsivity that interferes with functioning or
development, as characterized by (1) and/or (2):
1. Inattention: Six (or more) of the following symptoms have persisted for at least 6 months to a degree
that is inconsistent with developmental level and that negatively impacts directly on social and academic/
occupational activities. Note: The symptoms are not solely a manifestation of oppositional behavior,
defiance, hostility, or failure to understand tasks or instructions. For older adolescents and adults (age 17
and older), at least five symptoms are required.
a. Often fails to give close attention to details or makes careless mistakes in schoolwork, at work, or during
other activities (e.g., overlooks or misses details, work is inaccurate)
b. Often has difficulty sustaining attention in tasks or play activities (e.g., has difficulty remaining focused
during lectures, conversations, or lengthy reading)
c. Often does not seem to listen when spoken to directly (e.g., mind seems elsewhere, even in the absence
of any obvious distraction)
d. Often does not follow through on instructions and fails to finish schoolwork, chores, or duties in the
workplace (e.g., starts tasks but quickly loses focus and is easily sidetracked)
e. Often has difficulty organizing tasks and activities (e.g., difficulty managing sequential tasks; difficulty
keeping materials and belongings in order; messy, disorganized work; has poor time management; fails
to meet demands)
f. Often avoids, dislikes, or is reluctant to engage in tasks that require sustained mental effort (e.g.,
schoolwork or homework; for older adolescents and adults, preparing reports, completing forms,
reviewing lengthy papers)
g. Often loses things necessary for tasks or activities (e.g., school materials, pencils, books, tools, wallets,
keys, paperwork, eyeglasses, mobile phones)
h. Is often easily distracted by extraneous stimuli (for older adolescents and adults, may include unrelated
thoughts)
i. Is often forgetful in daily activities (e.g., doing chores, running errands; for older adolescents and adults,
returning calls, paying bills, keeping appointments)
2. Hyperactivity and impulsivity: Six (or more) of the following symptoms have persisted for at least 6
months to a degree that is inconsistent with developmental level and that negatively impacts directly
on social and academic/occupational activities. Note: The symptoms are not solely a manifestation
of oppositional behavior, defiance, hostility, or a failure to understand tasks or instructions. For older
adolescents and adults (ages 17 and older), at least five symptoms are required.
a. Often fidgets with or taps hands or feet or squirms in seat
b. Often leaves seat in situations in which remaining seated is expected (e.g., leaves his or her place in the
classroom, in the office or other workplace, or in other situations that require remaining in place)
c. Often runs about or climbs in situations in which it is inappropriate. (Note: In adolescents or adults, may
be limited to feeling restless.)
d. Often unable to play or engage in leisure activities quietly
e. Is often “on the go,” acting as if “driven by a motor” (e.g., is unable to be or uncomfortable being still for
extended time, as in restaurants, meetings; may be experienced by others as being restless or difficult
to keep up with)
f. Often talks excessively
g. Often blurts out an answer before a question has been completed (e.g., completes people’s sentences;
cannot wait for turn in conversation)
Continued on next page
Chapter 4 111
TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
Continued
h. Often has difficulty awaiting his or her turn (e.g., while waiting in line)
i. Often interrupts or intrudes on others (e.g., butts into conversations, games, or activities; may start
using other people’s things without asking or receiving permission; for adolescents and adults, may
intrude into or take over what others are doing)
B. Several inattentive or hyperactive-impulsive symptoms were present prior to age 12 years.
C. Several inattentive or hyperactive-impulsive symptoms are present in two or more settings (e.g., at
home, school, or work; with friends or relatives; in other activities).
D. There is clear evidence that the symptoms interfere with, or reduce the quality of, social, academic, or
occupational functioning.
E. The symptoms do not occur exclusively during the course of schizophrenia or another psychotic
disorder and are not better explained by another mental disorder (e.g., mood disorder, anxiety disorder,
dissociative disorder, PD, substance intoxication or withdrawal).
Specify whether:
•
Combined presentation: If both Criterion A1 (inattention) and Criterion A2 (hyperactivity-impulsivity) are
met for the past 6 months
•
Predominantly inattentive presentation: If Criterion A1 (inattention) is met but Criterion A2 (hyperactivity-
impulsivity) is not met for the past 6 months
•
Predominantly hyperactive/impulsive presentation: If Criterion A2 (hyperactivity-impulsivity) is met and
Criterion A1 (inattention) is not met for the past 6 months
Specify if:
•
In partial remission: When full criteria were previously met, fewer than the full criteria have been met
for the past 6 months, and the symptoms still result in impairment in social, academic, or occupational
functioning.
Specify current severity:
•
Mild: Few, if any, symptoms in excess of those required to make the diagnosis are present, and
symptoms result in no more than minor impairments in social or occupational functioning.
•
Moderate: Symptoms or functional impairment between “mild” and “severe” are present.
•
Severe: Many symptoms in excess of those required to make the diagnosis, or several symptoms that are
particularly severe, are present, or the symptoms result in marked impairment in social or occupational
functioning.
Source: APA (2013, pp. 59–61). Reprinted with permission from the DSM-5 (Copyright © 2013). APA. All Rights Reserved.
lifetime prevalence of DSM-IV ADHD in people
ages 18 to 44 years is 8.1 percent.
ADHD and SUDs
SUDs are among the most common comorbidities
of ADHD (Katzman, Bilkey, Chokka, Fallu, &
Klassen, 2017), and data from clinical and
epidemiological studies support this linkage
(Martinez-Raga, Szerman, Knecht, & de Alvaro,
2013). Among adults with substance misuse, the
prevalence of ADHD is approximately 23 percent,
although this estimate is dependent on substance
of misuse and assessment instrument used (van
Emmerik-van Oortmerssen et al., 2012). Among a
sample of more than 500 children with and without
ADHD who were followed throughout adolescence
and early adulthood (Molina et al., 2018), early
substance use in adolescence was greater and
escalated more quickly in the children with ADHD.
Further, weekly and daily cannabis use and daily
smoking in adulthood were significantly more
prevalent in the ADHD group than the non-ADHD
112 Chapter 4

TIP 42
Chapter 4—Diagnostic and Cross-Cutting Topics
group. Adults with ADHD have been found
primarily to use alcohol, nicotine, cannabis, and
cocaine (Lee, Humphreys, Flory, Liu, & Glass, 2011;
Luo & Levin, 2017).
People with addiction who have co-occurring
ADHD have a heightened risk for suicide attempts,
hospitalizations, earlier onset of addiction,
impulsivity, more severe disease course (for both
ADHD and the SUD) and polysubstance use as
well as lower rates of abstinence and treatment
adherence (Egan, Dawson, & Wymbs, 2017;
Katzman et al., 2017). ADHD and SUDs carry an
enhanced risk of comorbidity with depression,
conduct disorder, bipolar disorders, anxiety
disorders, and PDs (Luo & Levin, 2017; Martinez-
Raga et al., 2013; Regnart, Truter, & Meyer, 2017;
Young & Sedgwick, 2015; Zulauf, Sprich, Safren, &
Wilens, 2014). Symptoms of ADHD hyperactivity
and impulsivity are more strongly seen with
substance misuse and SUDs than ADHD symptoms
of inattention (De Alwis, Lynskey, Reiersen, &
Agrawal, 2014).
Although it is important to rule out other causes
of inattention or hyperactivity, including substance
misuse, misattribution of ADHD symptoms to
SUDs increases the likelihood of underdiagnosis
(Crunelle et al., 2018). People with SUDs who are
newly abstinent or those in active or protracted
withdrawal may experience some impairments
similar to ADHD. Many of the behavioral symptoms
of ADHD also appear during substance intoxication
and withdrawal, and functional consequences of
ADHD, such as poor job performance or job loss,
are also evident in people with addiction. Both
alcohol and cannabis can produce symptoms that
mimic ADHD. This underscores the importance of
conducting a thorough assessment (see Chapter 3)
to fully investigate symptoms in childhood, family
history of addiction and psychiatric illness, and other
biopsychosocial factors that can inform whether a
diagnosis of ADHD, SUD, or both are warranted.
Treatment of ADHD and SUDs
ADHD complicates SUD treatment because
clients with these CODs may have more difficulty
engaging in treatment and learning abstinence
skills, be at greater risk for relapse, and have
poorer substance use outcomes. The most
common attention problems in SUD treatment
populations are secondary to short-term toxic
effects of substances, and these should be
substantially better with each month of sobriety.
Only a limited number of studies explore treatment
of ADHD with comorbid SUDs (De Crescenzo,
Cortese, Adamo, & Janiri, 2017). Treatment of
adults with ADHD often involves use of stimulant
or nonstimulant medication; although efficacious in
reducing psychiatric symptoms, these medications
generally do not alleviate SUD symptoms (Cunill,
Castells, Tobias, & Capella, 2015; De Crescenzo
et al., 2017; Luo & Levin, 2017). Thus, ADHD
medication alone is an insufficient treatment
approach for clients with these CODs (Crunelle et
A consensus statement by an international panel of ADHD and addiction experts (including from the U.S.)
on the treatment of ADHD and SUDs recommends (Crunelle et al., 2018):
•
Using a combined treatment approach comprising psychoeducation, pharmacotherapy, individual or
group CBT, and peer support.
•
Integrating ADHD treatment into SUD treatment; integrating SUD treatment into mental health services.
•
Treating both disorders, but addressing the SUD first and then the ADHD shortly afterwards.
•
Considering residential treatment for cases of severe addiction.
•
Providing pharmacotherapy for ADHD (particularly with psychotherapy), but clinicians should be aware
that medication alone is usually not sufficient to treat the SUD.
•
Prescribing ADHD medication as needed but understand that this is a controversial topic because of
the misuse liability of stimulants. Clinicians should consider all risks and weigh them against potential
benefits when deciding whether to prescribe stimulant medications for people with ADHD-SUD.
Chapter 4 113

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
al., 2018; Zulauf et al., 2014). Stimulant medications
have misuse potential, and counselors should
be vigilant for signs of diversion. Use of long-
acting or extended-release medication or use of
antidepressants instead of stimulants can attenuate
diversion and misuse liability. The advised
approach to treatment involves a combination
of psychoeducation, behavioral coaching, CBT,
and nonstimulant or extended-release stimulant
medication (De Crescenzo et al., 2017).
Little research supports concurrent treatment of
these conditions. Some researchers recommend
first addressing whichever condition is most
debilitating to the client (Katzman et al., 2017;
Klassen, Bilkey, Katzman, & Chokka, 2012). Others
suggest that, to stabilize the client, treating the
SUD should be prioritized (Crunelle et al., 2018).
A systematic literature review and meta-analysis
of pharmacotherapy for ADHD and SUD (Cunill
et al., 2015) found no effect of timing of initiation
of treatment but warns that treatment of ADHD
symptoms may need to be delayed until after
abstinence is achieved, given possible harmful
interactions that can occur between ADHD
medications and substances of misuse.
Feeding and Eating Disorders
Feeding and eating disorders have as their
common core a persistent disturbance of eating
or eating-related behavior, resulting in changes
in consumption or absorption of food that
significantly impair physical health or psychosocial
functioning. The primary eating disorders linked to
SUD and discussed in this section are AN, bulimia
nervosa (BN), and binge eating disorder (BED).
Anorexia Nervosa
AN, the most visible eating disorder, is marked by a
refusal to maintain body weight above the minimally
normal weight for age and height because of an
intense fear of weight gain (Exhibit 4.13). The term
anorexia nervosa means “nervous loss of appetite,”
a misnomer; only in extreme stages of inanition
(i.e., exhaustion as a result of lack of nutrients in the
blood) is appetite actually lost.
Individuals with AN have a dogged determination
to lose weight and can achieve this in several ways.
Individuals with the restricting subtype of AN
severely limit their food intake, engage in excessive
exercise, and fast. Those with the binge-eating/
purging subtype engage in episodes of binge
eating or purging with self-induced vomiting,
CASE STUDY: COUNSELING AN SUD TREATMENT CLIENT WITH ADHD
John R., a 29-year-old White man, is seeking treatment. He has been in several treatment programs but
always dropped out after the first 4 weeks. He tells the counselor he dropped out because he would get
cravings and that he just could not concentrate in the treatment sessions. He mentions the difficulty of
staying focused during 3-hour intensive group sessions. A contributing factor in his quitting treatment was
that group leaders always seemed to scold him for talking to others. The clinician evaluating him asks how
John R. did in school and finds that he had difficulty in his classwork years before he started using alcohol
and drugs; he was restless and easily distracted. He had been evaluated for a learning disability and ADHD
and took Ritalin for about 2 years (in the 5th and 6th grades), then stopped. He was not sure why, but he did
terribly in school, eventually dropping out about the time he started using drugs regularly in the 8th grade.
Discussion: The SUD treatment provider reviewed John R.’s learning history and asked about anxiety or
depressive disorders. The provider referred him to the team’s psychiatrist, who uncovered more history
about the ADHD and also contacted John R.’s mother. When the provider reviewed a list of features
commonly associated with ADHD, she agreed that John R. had many of these features and that she had
noticed them in childhood. John R. was started on bupropion and moved to a less intensive level of care (1
hour of group therapy, 30 minutes of individual counseling, and AA meetings 3 times weekly). Over the next
2 months, John R.’s ability to tolerate a more intensive treatment improved. Although he was still somewhat
intrusive to others, he was able to benefit from more intensive group treatment.
114 Chapter 4

TIP 42
Chapter 4—Diagnostic and Cross-Cutting Topics
EXHIBIT 4.13. Diagnostic Criteria
for AN
A. Restriction of energy intake relative to
requirements, leading to a significantly low body
weight in the context of age, sex, developmental
trajectory, and physical health. Significantly
low weight is defined as a weight that is less
than minimally normal or, for children and
adolescents, less than minimally expected.
B. Intense fear of gaining weight or of becoming
fat, or persistent behavior that interferes with
weight gain, even though at a significantly low
weight.
C. Disturbance in the way in which one’s body
weight or shape is experienced, undue influence
of body weight or shape on self-evaluation, or
persistent lack of recognition of the seriousness
of the current low body weight.
Specify whether:
•
Restricting type: During the last 3 months,
the individual has not engaged in recurrent
episodes of binge eating or purging behavior
(i.e., self-induced vomiting or the misuse of
laxatives, diuretics, or enemas). This subtype
describes presentations in which weight loss
is accomplished primarily through dieting,
fasting, and/or excessive exercise.
•
Binge-eating/purging type: During the last
3 months, the individual has engaged in
recurrent episodes of binge eating or purging
behavior (i.e., self-induced vomiting or the
misuse of laxatives, diuretics, or enemas).
Specify if:
•
In partial remission: After full criteria for AN
were previously met, Criterion A (low body
weight) has not been met for a sustained
period, but either Criterion B (intense fear of
gaining weight or becoming fat or behavior
that interferes with weight gain) or Criterion C
(disturbances in self-perception of weight and
shape) is still met.
•
In full remission: After full criteria for AN were
previously met, none of the criteria have been
met for a sustained period of time.
Continued in next column
Continued
Specify current severity:
The minimum level of severity is based, for
adults, on current body mass index (BMI) (see
below) or, for children and adolescents, BMI
percentile. The ranges below are derived from
WHO categories for thinness in adults; for
children and adolescents, corresponding BMI
percentiles should be used. The level of severity
may be increased to reflect clinical symptoms,
the degree of functional disability, and the need
for supervision.
•
Mild: BMI ≥ 17 kg/m
2
•
Moderate: BMI 16–16.99 kg/m
2
•
Severe: BMI 15–15.99 kg/m
2
•
Extreme: BMI < 15 kg/m
2
Source: APA (2013, pp. 338–339). Reprinted with
permission from the DSM-5 (Copyright © 2013). APA.
All Rights Reserved.
laxatives, diuretics, or enemas. They engage in
these behaviors out of a marked fear of weight
gain, which is reinforced by distorted perceptions
of their body shape (e.g., believing oneself to be
“fat” even though bodyweight is extremely low).
Bulimia Nervosa
The core symptoms of BN are bingeing and
purging (Exhibit 4.14). A binge is a rapid
consumption of an unusually large amount of food,
by comparison with social norms, in a discrete
period of time (e.g., over 2 hours). Integral to the
notion of a binge is feeling out of control; thus, a
binge is not merely overeating. An individual with
BN may state that he or she is unable to postpone
the binge or stop eating willfully once the binge
has begun. The binge may only end when the
individual is interrupted, out of food, exhausted, or
physically unable to consume more.
The second feature of BN is purging. Individuals
with BN compensate in many different ways for
overeating. Ninety percent of people with BN
self-induce vomiting or misuse laxatives as their
form of purging (Westmoreland, Krantz, & Mehler,
2016). Other methods of purgation include the
Chapter 4 115
TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
EXHIBIT 4.14. Diagnostic Criteria for BN
A. Recurrent episodes of binge eating. An episode of binge eating is characterized by both of the following:
1. Eating, in a discrete period of time (e.g., within any 2-hour period), an amount of food that is definitely
larger than what most individuals would eat in a similar period of time under similar circumstances
2. A sense of lack of control over eating during the episode (e.g., a feeling that one cannot stop eating or
control what or how much one is eating)
B. Recurrent inappropriate compensatory behavior in order to prevent weight gain includes self-induced
vomiting; misuse of laxatives, diuretics, or other medications; fasting; or excessive exercise.
C. The binge eating and inappropriate compensatory behaviors both occur, on average, at least once a
week for 3 months.
D. Self-evaluation is unduly influenced by body shape and weight.
E. The disturbance does not occur exclusively during episodes of AN.
Specify if:
•
In partial remission: After full criteria for BN were previously met, some, but not all, of the criteria have been
met for a sustained period of time.
•
In full remission: After full criteria for BN were previously met, none of the criteria have been met for a
sustained period of time.
Specify current severity:
The minimum level of severity is based on the frequency of inappropriate compensatory behaviors (see
below). The level of severity may be increased to reflect other symptoms and the degree of functional
disability.
•
Mild: An average of 1–3 episodes of inappropriate compensatory behaviors per week
•
Moderate: An average of 4–7 episodes of inappropriate compensatory behaviors per week
•
Severe: An average of 8–13 episodes of inappropriate compensatory behaviors per week
•
Extreme: An average of 14 or more episodes of inappropriate compensatory behaviors per week
Source: APA (2013, p. 345). Reprinted with permission from the DSM-5 (Copyright © 2013). APA. All Rights Reserved.
misuse of diuretics and emetics; saunas; excessive
exercise; fasting; and other idiosyncratic methods
that people believe will lead to weight loss (such
as “mono” dieting, in which a person eats only
a single food for extended periods of time and
nothing else, like apples or eggs). Many of these
auxiliary methods are dangerous and ineffective
because they promote loss of water and valuable
electrolytes. As with AN, individuals with BN place
an undue emphasis on shape and weight in their
sense of identity. To meet criteria, bingeing and
purging must occur, on average, at least once per
week for 3 months.
Binge Eating Disorder
BED involves recurring episodes of eating
significantly more food in a short period of time than
most people would eat under similar circumstances,
with episodes marked by feelings of lack of control
(Exhibit 4.15). Someone with BED may eat too
quickly, even when he or she is not hungry. The
person may feel guilt, embarrassment, or disgust
and may binge eat alone to hide the behavior.
This disorder is linked with marked distress and
occurs, on average, at least once a week over 3
months. Unlike in BN, the binge is not followed by
compensatory behaviors to rid the body of food.
116 Chapter 4
TIP 42
Chapter 4—Diagnostic and Cross-Cutting Topics
EXHIBIT 4.15. Diagnostic Criteria for BED
A. Recurrent episodes of binge eating. An episode of binge eating is characterized by both of the following:
1. Eating, in a discrete period of time (e.g., within any 2-hour period), an amount of food that is definitely
larger than what most individuals would eat in a similar period of time under similar circumstances
2. A sense of lack of control over eating during the episode (e.g., a feeling that one cannot stop eating or
control what or how much one is eating)
B. The binge-eating episodes are associated with three (or more) of the following:
1. Eating much more rapidly than normal
2. Eating until feeling uncomfortably full
3. Eating large amounts of food when not feeling physically hungry
4. Eating alone because of feeling embarrassed by how much one is eating
5. Feeling disgusted with oneself, depressed, or very guilty afterward
C. Marked distress regarding binge eating is present.
D. The binge eating occurs, on average, at least once a week for 3 months.
E. The binge eating is not associated with the recurrent use of inappropriate compensatory behavior as in
BN and does not occur exclusively during the course of BN or AN.
Specify if:
•
In partial remission: After full criteria for binge-eating disorder were previously met, binge eating occurs
at an average frequency of less than one episode per week for a sustained period of time.
•
In full remission: After full criteria for binge-eating disorder were previously met, none of the criteria have
been met for a sustained period of time.
Specify current severity:
The minimum level of severity is based on the frequency of episodes of binge eating (see below). The level
of severity may be increased to reflect other symptoms and the degree of functional disability.
•
Mild: 1–3 binge-eating episodes per week
•
Moderate: 4–7 binge-eating episodes per week
•
Severe: 8–13 binge-eating episodes per week
•
Extreme: 14 or more binge-eating episodes per week
Source: APA (2013, p. 350). Reprinted with permission from the DSM-5 (Copyright © 2013). APA. All Rights Reserved.
Prevalence
Feeding and eating disorders in the general
population are rare. Twelve-month estimates of
DSM-5 AN, BN, and BED are 0.05 percent, 0.14
percent, and 0.44 percent, respectively; lifetime
prevalence rates are 0.80 percent, 0.28 percent,
and 0.85 percent, respectively (Udo & Grilo, 2018).
These rates are generally lower than previously
reported estimates using DSM-IV criteria (APA,
2013) but were drawn from a sample roughly 12
times larger than the samples used in other survey
studies (Udo & Grilo, 2018).
Eating disorders are far more prevalent in women
than men. Women have 12 times the odds of
having AN, 5.8 times the odds of having BN, and
about 3 times the odds of having BED (Udo &
Grilo, 2018).
Feeding and Eating Disorders and SUDs
Feeding and eating disorders are highly coincident
with substance misuse (SAMHSA, 2011a), likely
because the conditions share numerous physical,
mental, and social risk factors (Brewerton, 2014).
Most studies observe comorbidity rates that
Chapter 4 117

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
exceed the general population of women of similar
age. A meta-analysis (Bahji et al., 2019) found
lifetime prevalence of any SUD among people
with eating disorders to be 25 percent, including
20 percent for AUD, about 20 percent for any illicit
drug use disorder, almost 14 percent for cocaine
and cannabis use disorder (each), and 6 percent
for opioid use disorder (OUD). Even if not rising
to the level of addiction, licit and illicit substance
use is elevated in people with eating disorders,
especially individuals with bulimic features. In a
sample of almost 3,000 people, 80 percent of those
with BN reported using alcohol, and 50 percent
used other substances; 65 percent of those with
BED used alcohol, and nearly 24 percent used other
substances; and 60 percent of those with AN (binge/
purge subtype) used alcohol, and 44 percent used
other substances (Fouladi et al., 2015).
SUD treatment-seeking women have higher rates
of BN than any other feeding and eating disorder,
and SUDs are more common alongside BN or AN
with bulimic features than they are comorbid with
restrictive AN (APA, 2013; CSAT, 2009; Fouladi
et al., 2015). Some have suggested that the most
common comorbidity among feeding and eating
disorders and SUDs is BN (or AN with bulimic
features) and AUD (Gregorowski, Seedat, &
Jordaan, 2013; Munn-Chernoff et al., 2015).
Treatment outcomes of people with eating
disorders and SUDs are worse than those of people
without both conditions. They have higher odds of
early mortality, co-occurring physical and mental
illness, and delayed recovery (Root et al., 2010).
People in SUD treatment with feeding/eating
disorder symptoms have higher risk of treatment
dropout and discharge against medical advice
(Elmquist, Shorey, Anderson, & Stuart, 2015).
Alcohol misuse more than doubles mortality risk in
AN (Franko et al., 2013).
Treatment of Feeding and Eating Disorders
and SUDs
Feeding or eating disorders can make SUD
assessment and treatment more complex—such as
by raising risk of stopping SUD treatment against
medical advice (Elmquist et al., 2015). Heightened
mortality with feeding and eating disorders means
that multidisciplinary care should include primary
care providers and dietary/nutritional rehabilitation
professionals in addition to SUD treatment
professionals, mental health professionals (e.g.,
psychiatric and mental health nurses), and social
workers (SAMHSA, 2011a).
The literature does not currently describe
randomized controlled trials for treatment of
these CODs. In general, concurrent treatment
is recommended; sequential interventions can
increase likelihood of relapse or otherwise hinder
recovery from the untreated CODs (Gregorowski
et al., 2013). If integrated care is not possible,
SUD treatment should proceed first to halt
active substance use and allow the client to fully
participate in further care (SAMHSA, 2011a).
“DRUNKOREXIA”: A NEW AND DANGEROUS COMBINATION OF EATING
DISORDERS AND ALCOHOL MISUSE
Researchers are noticing a disturbing trend of college students (particularly women) engaging in
inappropriate compensatory behaviors prior to consuming alcohol in order to avoid or mitigate weight
gain from drinking. For instance, a woman might fast all day or drastically reduce her caloric intake prior
to going out to a party where she knows she will be drinking. This trend has been colloquially termed
“drunkorexia” (Barry & Piazza-Gardner, 2012; Bryant, Darkes, & Rahal, 2012; Burke, Cremeens, Vail-Smith, &
Woolsey, 2010; Hunt & Forbush, 2016; Wilkerson, Hackman, Rush, Usdan, & Smith, 2017) and is very serious
given that excess consumption of alcohol on an empty stomach raises the risk of alcohol poisoning and
damage to the brain and other organs. In light of high rates of binge and hazardous drinking in college-
aged populations, this makes the combination of disordered eating and alcohol misuse potentially very
dangerous.
118 Chapter 4

TIP 42
Chapter 4—Diagnostic and Cross-Cutting Topics
ADVICE TO THE COUNSELOR: COUNSELING A CLIENT WITH AN EATING
DISORDER
• When possible, work closely with a professional who specializes in eating disorders. Programs that
specialize in eating disorders and SUDs are rare, so parallel treatment by different providers may be
necessary.
• Screen for eating disorders both at intake and intermittently throughout SUD treatment (e.g., during
medical history, as a part of SUD assessment, as a part of daily or weekly meetings).
• Many symptoms and features of eating disorders overlap with those of SUDs as well as other mental
disorders, such as reduced food intake, low energy, depressed affect, difficulty concentrating, and sleep
disturbance. This underscores the importance of early screening and a thorough differential diagnosis.
• Addiction counselors may have a hard time detecting feeding and eating disorders because clients are
often adept at concealing their symptoms. Contrary to popular belief, many people with feeding and
eating disorders are not exceedingly thin. In fact, most people with BN are of normal weight or even
overweight. Learn the symptoms of AN, BN, and BED, and have screening tools and referral information
on hand for mental health professionals who can thoroughly assess clients for possible eating disorders
and symptoms. Do not merely look for clients who “look like” they have an eating disorder.
• The stereotypical picture of someone with an eating disorder is a young, heterosexual, White woman,
but these conditions occur in both genders, among diverse ethnic/racial groups, across cultures,
throughout the lifespan, and in people of all sexual orientations and gender identities.
• Co-occurring depression and anxiety are common in people with eating disorders and SUDs. Assess for
these (or their symptoms) and treat accordingly, because failure to do so can reduce overall treatment
success.
• Some clients may be hesitant to address their SUD out of fear that doing so will cause them to gain weight.
• Medical stabilization is critical, as people with feeding and eating disorders are at high risk for serious
health complications, including electrolyte imbalances, cardiovascular dysfunction (e.g., low blood
pressure, arrhythmias), withdrawal from laxative use, and dehydration. Treatment should include
continual collaboration with healthcare providers to ensure client safety and stability.
• People actively using substances need to be treated for their addiction before treatment for their eating
disorder can proceed. Ideally, both conditions would be managed concurrently using an integrated,
continuous care approach. But given that integrated programs for these CODs are uncommon, SUD
treatment may need to be the primary focus, assuming the client is already medically stable.
• Family dynamics often play a prominent role in the lives of people with eating disorders. As appropriate,
include family in the treatment process, including referral to a marriage and family therapist if needed.
• Document through a comprehensive assessment the individual’s full repertoire of weight loss
behaviors, as people with eating disorders will often go to dangerous extremes to lose weight.
• Conduct a behavioral analysis of foods and substances of choice; high-risk times and situations for
engaging in disordered eating and substance misuse; and the nature, pattern, and interrelationship of
disordered eating and substance use. Develop a treatment plan for both the eating disorder and the SUD.
• Use psychoeducation and CBT techniques.
Continued on next page
Chapter 4 119
TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
Continued
• Use adjunctive strategies such as nutritional consultation, the setting of a weight range goal, and
observations at and between mealtimes for disordered eating behaviors.
• Incorporate relapse prevention strategies for a long course of treatment and several treatment episodes.
• In addition to “traditional” drugs of misuse and alcohol, women with eating disorders are unique in their
misuse of pharmacological agents ingested for the purpose of weight loss, appetite suppression, and
purging. Among these drugs are prescription and over-the-counter diet pills, laxatives, diuretics, and
emetics. Nicotine and caffeine also must be considered when assessing substance use in women with
eating disorders.
• Drugs related to purging (e.g., diuretics, laxatives, emetics), are ineffective and potentially dangerous
methods of accomplishing weight loss or maintenance. The literature suggests that, like more common
drugs of misuse, tolerance and withdrawal occur with laxatives, diuretics, and possibly diet pills and
emetics.
• Alcohol and substances such as cannabis can disinhibit appetite (i.e., remove normal restraints on
eating) and increase the risk of binge eating as well as relapse in individuals with BN.
• Clients with feeding and eating disorders have craving, tolerance, and withdrawal from drugs linked
with purging (e.g., laxatives, diuretics) and urges (or cravings) for binge foods similar to urges for
substances.
• Feeding and eating disorders are quite serious and can be fatal. Treat them accordingly.
• Suicide risk in this population is perilously high. Regularly assess for suicidal thoughts, gestures, and
attempts and develop methods for safety monitoring and harm prevention (e.g., safety plans).
Only 51 percent of SUD treatment programs
report screening clients for feeding and eating
disorders (Kanbur & Harrison, 2016).
Regardless of treatment modality, providers must
first ensure medical and weight stabilization
so clients are healthy and able to physically and
cognitively participate in and benefit from therapy
(Harrop & Marlatt, 2010). Some clients with AN
or BN may require inpatient treatment or partial
hospitalization to stabilize weight. Depending on
the facility, staff may not be equipped to address
any co-occurring substance misuse simultaneously.
The primary treatment for these disorders is
psychosocial intervention, including individual,
group, family therapy, or a combination
thereof. CBT can be effective for feeding and
eating disorders but has not been researched
thoroughly in populations with co-occurring
addiction (Gregorowski et al., 2013). Dialectical
behavior therapy also can be useful in promoting
mindfulness, improving management of negative
emotions, and teaching affective and behavioral
self-regulation skills in feeding and eating disorders
and in SUDs separately (Ritschel, Lim, & Stewart,
2015) but, again, has not been studied extensively
in both concurrently. Pharmacotherapy may be
warranted for BN and BED (SAMHSA, 2011a) but
is not a first-line treatment. Further studies are
needed to clarify how the presence of a feeding
or eating disorder affects SUD treatment and how
best to integrate treatment for both conditions.
120 Chapter 4

TIP 42
Chapter 4—Diagnostic and Cross-Cutting Topics
Substance-Related Disorders
The primary aim of this section of the chapter is
to describe substance-induced mental disorders
and to clarify how to differentiate them from
mental disorders that co-occur with SUDs.
Substance-related disorders include two
subcategories: SUDs and substance-induced
disorders. SUDs identify the cluster of cognitive,
behavioral, and physical symptoms that occur as a
result of continued and frequent use of substances.
These consequences are not immediate. Rather,
they occur over time as addiction progresses.
Substance-induced mental disorders refer to the
immediate effects of substance use (intoxication),
the immediate effects of discontinuing a substance
(substance withdrawal), and other substance-
induced mental disorders (APA, 2013).
SUDs
The essential feature of an SUD is a cluster of
cognitive, behavioral, and physical symptoms
indicating that the individual continues using the
substance despite significant substance-related
problems. All DSM-5 SUDs have their own
diagnostic criteria, but criteria are largely the same
across substances. Addiction counselors should be
familiar with SUD diagnostic criteria and refer to
DSM-5 as needed.
Prevalence
Lifetime and 12-month prevalence rates of DSM-5
drug use disorders (i.e., non-alcohol-related SUDs)
are nearly 10 percent and 4 percent, respectively
(Grant et al., 2016). Lifetime and 12-month
prevalence rates of AUD are about 29 percent
and 14 percent, respectively (Grant et al., 2015).
Past-month prevalence rates of misuse of other
substances by adults ages 26 and older include
(CBHSQ, 2019):
•
8.6 percent for cannabis.
•
0.7 percent for cocaine.
•
1.0 percent for pain relievers.
•
0.5 for tranquilizers.
•
0.4 percent for stimulants.
•
0.1 percent for prescription sedatives.
•
0.4 percent for hallucinogens.
•
0.2 percent for heroin.
•
0.1 percent for inhalants.
Substance-Induced Mental Disorders
The toxic effects of substances can mimic
mental disorders in ways that can be difficult
to distinguish from mental illness. This section
focuses on a general description of symptoms of
mental illness that are the result of substances
or medications—a condition called substance-
induced mental disorders.
DSM-5 substance-induced mental disorders
include:
•
Substance-induced depressive disorders.
•
Substance-induced bipolar and related
disorders.
•
Substance-induced anxiety disorders.
•
Substance-induced psychotic disorders.
•
Substance-induced obsessive-compulsive and
related disorders.
•
Substance-induced sleep disorders.
•
Substance-induced sexual dysfunctions.
•
Substance-induced delirium.
•
Substance-induced neurocognitive disorder.
The first four of the listed substance-induced
mental disorders are the most common in
addiction, discussed further in the section,
“Specific Substance-Induced Mental Disorders.”
Exhibit 4.16 summarizes substances and the
substance-induced mental disorders associated
with each.
Chapter 4 121

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
EXHIBIT 4.16. Substances and Corresponding Substance-Induced
Mental Disorders
SUBSTANCE SUBSTANCEINDUCED MENTAL DISORDER
Alcohol
•
Psychotic disorders
•
Bipolar disorders
•
Depressive disorders
•
Anxiety disorders
•
Sleep disorders
Caffeine
•
Anxiety disorders
•
Sleep disorders
Cannabis
•
Psychotic disorders
•
Anxiety disorders
Hallucinogens
•
Psychotic disorders
•
Bipolar disorders
•
Depressive disorders
•
Anxiety disorders
Inhalants
•
Psychotic disorders
•
Depressive disorders
•
Anxiety disorders
Opioids
•
Depressive disorders
•
Anxiety disorders
•
Sleep disorders
Sedatives
•
Psychotic disorders
•
Bipolar disorders
•
Depressive disorders
•
Anxiety disorders
•
Sleep disorders
Stimulants (e.g., cocaine,
amphetamines)
•
Psychotic disorders
•
Bipolar disorders
•
Depressive disorders
•
Anxiety disorders
•
Sleep disorders
WARNING TO COUNSELORS: INDEPENDENT VERSUS SUBSTANCE
INDUCED MENTAL DISORDERS
The symptoms of substance-induced mental disorders may be identical to those of independent but co-
occurring mental disorders. Accurate assessment of a mental disorder cannot occur while an individual is
actively using substances. Knowing the difference between the two is key because they may (or may not)
need to be treated differently and will have different prognoses. Mental disorder symptoms resulting from
intoxication or withdrawal often need no formal treatment and will resolve on their own and quickly.
Also keep in mind the bidirectional and unstable temporal relationship between mental disorders and
SUDs. Whether a substance is causing psychiatric symptoms or vice versa is often unclear, and the answer
can change over time. Each disorder can affect the other reciprocally. Even when a substance clearly is
responsible for the emergence of a mental disorder/psychiatric symptoms, that does not preclude the
possibility of an independent mental disorder developing in the future. In fact, an individual can have
both a substance-induced and an independent mental disorder. For example, a client may present with
well-established independent and controlled bipolar I disorder and AUD in remission, but the same client
could be experiencing amphetamine-induced auditory hallucinations and paranoia from an amphetamine
misuse relapse over the last 3 weeks.
Even when the psychiatric diagnosis has not been established, the client’s co-occurring symptoms should
still be treated (with nonmedication). Counselors should not withhold treatment simply because a
determination about the origin of the mental disorder has not yet been made.
122 Chapter 4

TIP 42
Chapter 4—Diagnostic and Cross-Cutting Topics
General Considerations
Substance-induced mental disorders are distinct
from independent co-occurring mental disorders
in that all or most of the psychiatric symptoms
are the direct result of substance use. This
does not mean that substance-induced disorders
preclude co-occurring mental disorders, only
that the specific symptom cluster at a specific
point in time is more likely the result of substance
use, misuse, intoxication, or withdrawal than of
underlying mental illness.
Even when the psychiatric diagnosis has not
been established, the client’s co-occurring
symptoms should still be treated (with
nonmedication). Counselors should not withhold
treatment simply because a determination about
the origin of the mental disorder has not yet
been made.
Symptoms of substance-induced mental
disorders run the gamut from mild anxiety
and depression (these are the most common
across all substances) to full-blown manic and
other psychotic reactions (much less common).
For example, acute withdrawal symptoms from
physiological depressants such as alcohol and
benzodiazepines are hyperactivity, elevated blood
pressure, agitation, and anxiety (i.e., “the shakes”).
On the other hand, those who “crash” from
stimulants are tired, withdrawn, and depressed.
Because clients vary greatly in how they respond to
both intoxication and withdrawal given the same
exposure to the same substance, and also because
different substances may be taken at the same
time, prediction of any particular substance-related
syndrome has its limits. What is most important
is to continue to evaluate psychiatric symptoms
and their relationship to abstinence or ongoing
substance misuse over time. Most substance-
induced symptoms begin to improve within hours
or days after substance use has stopped. Notable
exceptions to this are psychotic symptoms caused
by heavy and longterm amphetamine misuse
and dementia (e.g., problems with memory,
concentration, problem solving) caused by using
substances directly toxic to the brain, which most
commonly include alcohol, inhalants like gasoline,
and amphetamines.
Exhibit 4.17 offers an overview of the most
common classes of misused substances and the
accompanying psychiatric symptoms seen in
intoxication and withdrawal.
EXHIBIT 4.17. Substance-Induced Mental Disorder Symptoms (by Substance)
ALCOHOL
Intoxication. In most people, moderate to heavy consumption is associated with euphoria, mood lability,
decreased impulse control, and increased social confidence (i.e., getting high). Symptoms may appear
hypomanic but are often followed by next-day mild fatigue, nausea, and dysphoria.
Withdrawal. Following acute withdrawal (a few days), some people will experience continued mood
instability, fatigue, insomnia, reduced sexual interest, and hostility for weeks or months, so-called
“protracted withdrawal.” Symptoms of alcohol withdrawal include agitation, anxiety, tremor, malaise,
hyperreflexia (exaggeration of reflexes), mild tachycardia (rapid heartbeat), increasing blood pressure,
sweating, insomnia, nausea or vomiting, and perceptual distortions. More severe withdrawal is
characterized by severe instability in vital signs, agitation, hallucinations, delusions, and often seizures.
Alcohol-induced deliriums after high-dose drinking are characterized by fluctuating mental status,
confusion, and disorientation and are reversible once both alcohol and its withdrawal symptoms are gone.
CANNABIS
Intoxication. Consumption typically results in a “high” feeling followed by symptoms including euphoria,
sedation, lethargy, impairment in short-term memory, difficulty carrying out complex mental processes,
impaired judgement, distorted sensory perceptions, impaired motor performance, and the sensation that
time is passing slowly. Occasionally, the individual experiences anxiety (which may be severe), dysphoria,
or social withdrawal.
Continued on next page
Chapter 4 123

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
Continued
Withdrawal. Cessation or substantial reduction in heavy or prolonged cannabis use may result in fatigue,
yawning, difficulty concentrating, and rebound periods of increased appetite and hypersomnia that
follow initial periods of loss of appetite and insomnia.
HALLUCINOGENS
Intoxication. Hallucinogens produce visual distortions and frank hallucinations. Some people who use
hallucinogens experience a marked distortion of their sense of time and feelings of depersonalization.
Hallucinogens may also be associated with drug-induced panic, paranoia, and even delusional states
in addition to the hallucinations. Hallucinogen hallucinations usually are more visual (e.g., enhanced
colors and shapes) as compared with schizophrenic-type hallucinations, which tend to be more auditory
(e.g., voices). Phencyclidine (PCP) causes dissociative and delusional symptoms and may lead to violent
behavior and amnesia of the intoxication.
OPIOIDS
Intoxication. Opioid intoxication is characterized by intense euphoria and feelings of well-being.
Withdrawal. Withdrawal can result in agitation, severe body aches, gastrointestinal symptoms, dysphoria,
and craving to use more opioids. Symptoms during withdrawal vary—some will become acutely anxious
and agitated, whereas others will experience depression and anhedonia. Even with abstinence, anxiety,
depression, and sleep disturbance can persist as a protracted withdrawal syndrome.
SEDATIVES
Intoxication. Acute intoxication with sedatives like diazepam is similar to what is experienced with alcohol.
Withdrawal. Withdrawal symptoms are also similar to alcohol and include mood instability with anxiety
or depression, sleep disturbance, autonomic hyperactivity, tremor, nausea or vomiting, and, in more
severe cases, transient hallucinations or illusions and grand mal seizures. There are reports of a protracted
withdrawal syndrome characterized by anxiety, depression, paresthesias, perceptual distortions, muscle
pain and twitching, tinnitus, dizziness, headache, derealization and depersonalization, and impaired
concentration. Most symptoms resolve in weeks, but some symptoms, such as anxiety, depression,
tinnitus, and paresthesias (sensations such as prickling, burning, etc.), have been reported to last a year or
more after withdrawal for some.
STIMULANTS INCLUDES COCAINE AND AMPHETAMINES
Intoxication. Mild to moderate intoxication from cocaine, methamphetamine, or other stimulants is
associated with euphoria, and a sense of internal well-being, and perceived increased powers of thought,
strength, and accomplishment. In fact, low to moderate doses of amphetamines may actually increase
certain test-taking skills temporarily in those with ADHD and even in people who do not have ADHD.
However, as more substance is used and intoxication increases, attention, ability to concentrate, and
function decrease.
With cocaine and methamphetamines, dosing is almost always beyond the functional window. As dosage
increases, the chances of impulsive dangerous behaviors, which may involve violence, promiscuous sexual
activity, and others, also increases.
Withdrawal. After intoxication comes a crash in which the person is desperately fatigued, depressed, and
often craves more stimulant to relieve these withdrawal symptoms. This dynamic is why it is thought that
people who misuse stimulants often go on week- or month-long binges and have a hard time stopping.
Even with several weeks of abstinence, many people who are addicted to stimulants report a dysphoric
state that is marked by anhedonia (absence of pleasure) or anxiety. Heavy, long-term amphetamine use
appears to cause long-term changes in the functional structure of the brain, and this is accompanied by
long-term problems with concentration, memory, and, at times, psychotic symptoms.
124 Chapter 4

TIP 42
Chapter 4—Diagnostic and Cross-Cutting Topics
INDUCED VERSUS INDEPENDENT
MENTAL DISORDERS: THE
IMPORTANCE OF TREATMENT
It will not always be clear whether a client’s
mental disorder or symptoms are independent
or caused by long-term substance use or
withdrawal. But withholding treatment until
this determination is made is inhumane and
unethical. Individuals should be engaged in
treatment that addresses their co-occurring
psychiatric symptoms, even if the origin of the
co-occurring mental disorder is unclear.
If counselors struggle to differentiate an
independent from a substance-induced mental
disorder, they should:
•
Observe the client and watch for changes in
symptoms (e.g., do symptoms abate once the
person is abstinent from the substance for a
length of time?).
•
Reevaluate the client to help discern
whether the symptoms/disorder is caused
by withdrawal, protracted withdrawal, or the
neurological effects of chronic substance use.
•
Offer nonmedication treatment (e.g., SUD
interventions or mental health services) for
all symptoms, regardless of whether a formal
diagnosis has been established.
Diagnoses of substance-induced mental
disorders will typically be provisional and will
require reevaluation—sometimes repeatedly.
Many apparent acute mental disorders may really
be substance-induced disorders, such as in those
clients who use substances and who are acutely
suicidal.
Some people who appear to have substance-
induced mental disorders turn out to have
a substance-induced mental disorder and
independent mental disorder. Consider
preexisting mood state, personal expectations,
drug dosage, and environmental surroundings
in understanding of how a particular client
might experience a substance-induced disorder.
Treatment of the SUD and an abstinent period of
weeks or months may be required for a definitive
diagnosis of an independent, co-occurring mental
disorder. As described in Chapter 3, SUD treatment
programs and clinical staff can concentrate on
screening for mental disorders and determining
the severity and acuity of symptoms, along with an
understanding of the client’s support network and
overall life situation.
Specic Substance-Induced Mental Disorders
This section briefly discusses the most common
substance-induced mental disorders in clinical
populations: substance-induced depressive, anxiety,
bipolar, and psychotic disorders. Diagnostic criteria
for all substance-induced mental disorders, including
the four mentioned, are nearly identical and
comprise five general characteristics (Exhibit 4.18).
EXHIBIT 4.18. Features of DSM-5 Substance-Induced Mental Disorders
A. The disorder represents a clinically significant symptomatic presentation of a relevant mental disorder.
B. There is evidence from the history, physical examination, or laboratory findings of both of the following:
1. The disorder developed during or within 1 month of a substance intoxication or withdrawal or taking a
medication; and
2. The involved substance/medication is capable of producing the mental disorder.
C. The disorder is not better explained by an independent mental disorder (i.e., one that is not substance-
or medication-induced). Such evidence of an independent mental disorder could include the following:
1. The disorder preceded the onset of severe intoxication or withdrawal or exposure to the medication; or
Continued on next page
Chapter 4 125

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
Continued
2. The full mental disorder persisted for a substantial period of time (e.g., at least 1 month) after the
cessation of acute withdrawal or severe intoxication or taking the medication. This criterion does not
apply to substance-induced neurocognitive disorders or hallucinogen persisting perception disorder,
which persist beyond the cessation of acute intoxication or withdrawal.
D. The disorder does not occur exclusively during the course of a delirium.
E. The disorder causes clinically significant distress or impairment in social, occupational, or other
important areas of functioning.
Source: APA (2013, p. 488). Reprinted with permission from the DSM-5 (Copyright © 2013). APA. All Rights Reserved.
EXHIBIT 4.19. Substances That Precipitate or Mimic Common Mental
Disorders
MENTAL DISORDER SUBSTANCES THAT
MIMIC MENTAL
DISORDERS DURING USE
INTOXICATION
SUBSTANCES THAT MIMIC MENTAL
DISORDERS AFTER USE WITHDRAWAL
Depression and dysthymia Alcohol, benzodiazepines,
opioids, barbiturates,
cannabis, steroids
(chronic), stimulants
(chronic)
Alcohol, benzodiazepines, barbiturates,
opioids, steroids (chronic), stimulants
(chronic)
Anxiety disorders Alcohol, amphetamine
and its derivatives,
cannabis, cocaine,
hallucinogens,
intoxicants and PCP,
inhalants, stimulants
Alcohol, cocaine, opioids, sedatives,
hypnotics, anxiolytics, stimulants
Bipolar disorders and mania Stimulants, alcohol,
hallucinogens, inhalants
(organic solvents),
steroids (chronic, acute)
Alcohol, benzodiazepines, barbiturates,
opioids, steroids (chronic)
Psychosis Alcohol, anxiolytics,
cannabis, hallucinogens
(e.g., PCP), inhalants,
sedatives, hypnotics,
stimulants
Alcohol, sedatives, hypnotics, anxiolytics
Exhibit 4.19 lists substances most likely to induce/
mimic depressive, anxiety, bipolar, and psychotic
disorders.
Substance-induced depressive disorders
The lifetime prevalence of substance-induced
depressive disorders in the general community is
0.26 percent (Blanco et al., 2012). Observed rates
among clinical populations are much higher. For
instance, in a study of people seeking treatment
for co-occurring depressive disorders and SUDs,
24 percent had substance-induced depression;
rates varied by substance. Among those with
12-month alcohol dependence, prevalence of
126 Chapter 4

TIP 42
Chapter 4—Diagnostic and Cross-Cutting Topics
substance-induced MDD was 22 percent; for
past-year cocaine dependence, 22 percent; and for
past-year heroin dependence, nearly 37 percent
(Samet et al., 2013). In another study of people
with SUDs, 60 percent of people with depression
had a substance-induced rather than independent
depressive disorder (Conner et al., 2014). DSM-5
notes that although about 40 percent of people
with AUD develop MDD, only about one-third to
one-half are cases of independent depression,
meaning as much as 75 percent of occurrences
of depressive disorders in the context of AUD
could be because of intoxication or withdrawal
(APA, 2013). Depressive disorders or their symptoms
could also be because of the long-term effects of
substance use.
Diagnosis of a substance-induced versus
independent depressive disorder can be difficult
given that many people with SUDs do have
mood symptoms, like depressed affect, and
intoxication and withdrawal from substances can
mirror symptoms of depression. During the first
months of abstinence, many people with SUDs
may exhibit symptoms of depression that fade
over time and are related to acute withdrawal.
Because depressive symptoms during withdrawal
and early recovery may result from SUDs and
not an underlying depression, a period of time
should elapse before depression is diagnosed. This
does not preclude the importance of addressing
depressive symptoms during the early stage of
recovery, before diagnosis. Further, even if an
episode of depression is substance induced, that
does not mean that it should not be treated.
Overall, the process of addiction can result in
biopsychosocial disintegration, leading to PDD or
depression often lasting from months to years.
Substance-induced mood alterations can result
from acute and chronic drug use as well as from
drug withdrawal. Substance-induced depressive
disorders, most notably acute depression lasting
from hours to days, can result from sedative–
hypnotic intoxication. Similarly, prolonged or
subacute withdrawal, lasting from weeks to months,
can cause episodes of depression, and sometimes is
accompanied by suicidal ideation or attempts.
Stimulant withdrawal may provoke episodes of
depression lasting from hours to days, especially
following high-dose, chronic use. Acute stimulant
withdrawal generally lasts from several hours to
1 week and is characterized by depressed mood,
agitation, fatigue, voracious appetite, and insomnia
or hypersomnia (oversleeping). Depression
resulting from stimulant withdrawal may be severe
and can be worsened by the individual’s awareness
of substance use–related adverse consequences.
Symptoms of craving for stimulants are likely and
suicide is possible. Protracted stimulant withdrawal
often includes sustained episodes of anhedonia
(absence of pleasure) and lethargy with frequent
ruminations and dreams about stimulant use.
Stimulant cessation may be followed for several
months by bursts of dysphoria, intense depression,
insomnia, and agitation. These symptoms may
be either worsened or lessened depending on
the provider’s treatment attitudes, beliefs, and
approaches. It is a delicate balance—between
allowing time to observe the direction of symptoms
to treating the client’s presenting symptoms
regardless of origin.
Substance-Induced Anxiety Disorders
The prevalence of substance-induced anxiety
disorders in the community is unreported and
thought to be quite low (less than 0.1 percent),
although likely higher in clinical samples (APA, 2013).
Licit and illicit substances can cause symptoms that
are identical to those in anxiety. In addition, many
medications, toxins, and medical procedures can
cause or are associated with an eruption of anxiety.
Moreover, these reactions vary greatly from mild
manifestations of shortlived symptoms to full-blown
manic and other psychotic reactions, which are not
necessarily short lived.
Symptoms that look like anxiety may appear
either during use or withdrawal. Alcohol, am-
phetamine and its derivatives, cannabis, cocaine,
hallucinogens, intoxicants and phencyclidine
and its relatives have been reported to cause
the symptoms of anxiety during intoxication.
Withdrawal from alcohol, cocaine, illicit opioids,
and also caffeine and nicotine can also cause
manifestations of anxiety. Similarly, withdrawal from
depressants, opioids, and stimulants invariably
includes potent anxiety symptoms.
Chapter 4 127

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
Substance-Induced Bipolar Disorders
Epidemiologic data on substance-induced mania or
bipolar disorders in the U.S. general population are
not readily available.
A number of substances of misuse (as well as
prescribed medications and several medical
conditions) are also associated with manic-
like phenomena. Acute manic symptoms may
be induced or mimicked by intoxication with
stimulants, steroids, hallucinogens, or polydrug
combinations. They may also be caused by
withdrawal from depressants such as alcohol.
Individuals experiencing acute mania with its
accompanying hyperactivity, psychosis, and often
aggressive and impulsive behavior should be
referred to emergency mental health professionals.
Stimulant-induced episodes of mania may include
symptoms of paranoia lasting from hours to days.
Stimulants such as cocaine and amphetamines
cause potent psychomotor stimulation. Stimulant
intoxication generally includes increased mental
and physical energy, feelings of well-being and
grandiosity, and rapid, pressured speech. Chronic,
high-dose stimulant intoxication, especially with
sleep deprivation, may prompt a manic episode.
Symptoms may include euphoric, expansive, or
irritable mood, often with flight of ideas, severe
social functioning impairment, and insomnia.
Substance-Induced Psychosis
This condition is very rare; exact prevalence
rates are unknown (APA, 2013). In first-episode
psychosis, 7 percent to 25 percent of cases are
substance induced (APA, 2013).
CASE STUDIES: IDENTIFYING DISORDERS
George M. is a 37-year-old divorced man who was brought to the ED intoxicated. His blood alcohol level
was 0.27, and the toxicology screen was positive for cocaine. He was also suicidal (“I’m going to do it right
this time!”). He has a history of three psychiatric hospitalizations and two inpatient SUD treatments. Each
psychiatric admission was preceded by substance use.
George M. never followed through with mental health services. He sometimes attended AA, but not
recently.
Teresa G. is a 37-year-old divorced woman who was brought into a detoxification unit 4 days ago with a
blood alcohol level of 0.21. She is observed to be depressed, withdrawn, with little energy, fleeting suicidal
thoughts, and poor concentration, but states she is just fine, not depressed, and life was good last week
before her relapse. She has never used substances (other than alcohol) and began drinking alcohol
only 3 years ago. However, she has had several alcohol-related problems since then. She has a history of
three psychiatric hospitalizations for depression, at ages 19, 23, and 32. She reports a positive response to
antidepressants. She is currently not receiving mental health services or SUD treatment. She is diagnosed
with AUD (relapse) and substance-induced depressive disorder, with a likely history of, but not active, major
depression.
Discussion: Many factors must be examined when making initial diagnostic and treatment decisions. For
example, if George M.’s psychiatric admissions were 2 or 3 days long, usually with discharges related to
leaving against medical advice, decisions about diagnosis and treatment would be different (i.e., this is likely
a substance-induced suicidal state and referral at discharge should be to an SUD treatment agency rather
than a mental health center) than if two of his psychiatric admissions were 2 or 3 weeks long with clearly
defined manic and psychotic symptoms continuing throughout the course, despite aggressive use of
mental health services and medication (this is more likely a person with both bipolar disorder and AUD who
requires integrated treatment for both his severe AUD and bipolar disorder).
Similarly, if Teresa G. became increasingly depressed/withdrawn in the past 3 months, and had for a month
experienced disordered sleep, poor concentration, and suicidal thoughts, she would be best diagnosed with
MDD with acute alcohol relapse, not substance-induced depressive disorder secondary to alcohol relapse.
128 Chapter 4

TIP 42
Chapter 4—Diagnostic and Cross-Cutting Topics
Heavy users of psychoactive substances, like
cannabis, amphetamines, and cocaine, are
vulnerable to substance-induced psychosis,
especially clients with cooccurring schizophrenia
and bipolar disorders. Antidepressants can also
precipitate psychotic episodes, as can medications
like prescribed steroids and nonsteroidal anti-
inflammatory drugs, antiviral agents, antibiotics,
anticholinergics, antihistamines, muscle relaxants,
and opioids. Any number of physical illnesses or
medication reactions, from brain tumors to steroid
side effects, can cause a psychotic episode or
psychotic behavior. Virtually any substance taken
in very large quantities over a long enough
period can lead to a psychotic state.
Differential diagnosis among psychotic disorders
can be challenging, even for experienced clinicians
and diagnosticians, especially when substances
are involved. When a client presents in a psychotic
state, any immediate or recent substance use is
difficult to determine, and it may be impossible to
discern whether the hallucinations or delusions are
caused by substance use. If the hallucinations or
delusions can be attributed to substance use but are
prominent and beyond what one might expect from
intoxication alone, the episode would be described
as a substance-induced psychotic disorder.
Hallucinations that the person knows are solely the
result of substance use are not considered indicative
of a psychotic episode; instead, they are diagnosed
as substance intoxication or substance withdrawal
with the specifier “with perceptual disturbances”
(APA, 2013).
Cross-Cutting Topics: Suicide and
Trauma
Suicide risk and trauma status are relevant to care
planning, client safety, and treatment outcomes
across many CODs. This section briefly addresses
each issue and offers guidance to help addiction
counselors understand why both need to be actively
considered as part of assessment and treatment.
Ample literature discusses suicide, mental
disorders, and addiction. This section is not
intended to thoroughly review all aspects of
suicide-related assessment, management, and
prevention techniques for COD populations;
readers instead are directed to TIP 50, Addressing
Suicidal Thoughts and Behaviors in Substance
Abuse Treatment (CSAT, 2009) for more
information. The aim of this text is to ensure that
readers have a broad and general understanding
of the high risk of suicidal thoughts and behaviors
in clients with CODs and feel confident in knowing
how to prevent and respond to such events.
Similarly, trauma has been a significant topic of
research in the behavioral health literature. What
follows is an abbreviated summary of the link
between trauma and mental disorders and SUDs
and how addiction counselors can offer trauma-
informed services. Readers should consult TIP
57, Trauma-Informed Care in Behavioral Health
Services (SAMHSA, 2014b) for more guidance in
this area.
For both suicide and trauma, readers are reminded
to review Chapter 3 for assessment techniques and
tools, Appendix B for links to suicide prevention
materials and other resources, and Appendix C for
counselor tools like trauma screeners.
Suicide
Suicide is a common risk factor that pertains
to nearly all CODs and particularly those
involving addiction and MDD, bipolar disorder,
schizophrenia, PTSD, or PDs (Yuodelis-Flores
& Ries, 2015). Suicidality itself is not a mental
disorder, but it is considered a high-risk behavior of
significant public health concern (Hogan & Grumet,
2016). Substance-induced or exacerbated suicidal
ideations, intentions, and behaviors are possible
complications of SUDs, especially for clients with
co-occurring mental disorders.
The topic of suicidality is critical for SUD treatment
counselors working with clients who have CODs.
SUDs alone increase suicidality (Yuodelis-Flores &
Ries, 2015), whereas the added presence of some
mental disorders doubles the already heightened
risk (O’Connor & Pirkis, 2016). The risk of suicide
is greatest when relapse occurs after a substantial
Chapter 4 129

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
These populations (Department of Health and Human Services, 2012) are vulnerable to suicide risk; many
are susceptible to addiction or CODs as well:
•
American Indians/Alaska Natives
•
Individuals who have lost a loved one to suicide
•
Clients involved in criminal justice/child welfare
systems
•
Clients who engage in nonsuicidal self-injury
•
Individuals with a history of previous suicide
attempt
•
Individuals with debilitating physical conditions
•
Clients with mental disorders, SUDs, or both
•
Individuals in the LGBTQ community
•
Members of the armed forces and veterans
•
Middle-aged and older men
period of abstinence—especially if there is
concurrent financial or psychosocial loss. Every
agency that offers SUD counseling must also
have a clear protocol in place that addresses the
recognition and treatment (or referral) of people
who may be suicidal.
Prevalence
Suicide is the 10th leading cause of death in the
United States among people ages 10 and older
(Stone et al., 2019). Suicide is the second leading
cause of death for people ages 10 to 34 and the
fourth leading cause of death for those ages 35
and 54 (NIMH, 2019). Per the Centers for Disease
Control and Prevention (CDC), from 1999 to 2018,
suicide rates in the United States increased 41
percent, from 10.5 to 14.8 per 100,000 people
(CDC, 2019). Suicide rates among men remain
more than 3 times higher (23.4 per 100,000 in
2018) than among women (6.4 per 100,000 in
2018) (CDC, 2020).
Almost half (46 percent) of all individuals in the
United States who died by suicide between
2014 and 2016 had a known mental health
condition, and 54 percent were in treatment at
the time of death (Stone et al., 2019). Depression
According to NSDUH data (CBHSQ, 2019), in 2018:
•
About 10.7 million U.S. adults ages 18 or older
thought seriously of dying by suicide (4.3
percent of adults).
•
3.3 million U.S. adults made suicide plans (1.3
percent).
•
1.4 million U.S. adults made nonfatal suicide
attempts (0.6 percent).
was the most common mental disorder diagnosis
among those who completed suicide (75 percent);
other major mental disorder diagnoses included
anxiety (17 percent), bipolar disorders (15 percent),
schizophrenia (5 percent), and PTSD (4 percent)
(Stone et al., 2019).
Suicide and SUDs
Substance misuse makes people susceptible
to self-harm; indeed, suicide is the leading
cause of death among people with addiction
(CSAT, 2009). From 2014 to 2016, 28 percent
of people who died by suicide had problematic
substance use, including 32 percent of people
with a known mental health disorder (Stone et al.,
2019). Of these individuals with known psychiatric
problems, 39 percent tested positive for alcohol,
39 percent for benzodiazepines, 29 percent for
opioids, 23 percent for cannabis, 10 percent for
amphetamines, and 6 percent for cocaine (Stone et
al., 2019).
Alcohol factors prominently into suicide (Darvishi,
Farhadi, Haghtalab, & Poorolajal, 2015). Acute
alcohol intoxication increases the risk of suicide
attempt by nearly 7 times and in some studies,
if use is heavy, by as much as 37 times (Borges
et al., 2017). This risk appears to increase with
corresponding increases in consumption; as such,
populations with AUD have higher rates of suicide
than people without problematic alcohol use
(Yuodelis-Flores & Ries, 2015).
Other substances also carry an increased risk of
self-harm, as suicidal behavior is prominent in
OUD, cocaine use disorder, and polysubstance
use (Yuodelis-Flores & Ries, 2015). Among
130 Chapter 4

TIP 42
Chapter 4—Diagnostic and Cross-Cutting Topics
individuals with a history of substance misuse
who died by suicide in 2014 (Fowler, Jack, Lyons,
Betz, & Petrosky, 2018), the most commonly
involved nonmedication substances were alcohol
(51 percent), opioids (23 percent), and cannabis
(almost 14 percent). Furthermore, among all suicide
cases that year, opioids were the direct cause of
death in 27 percent of people and alcohol in 13
percent (Fowler et al., 2018). The overall suicide
rate of U.S. veterans with an SUD is estimated
at 75.6 per 100,000 people and is highest
among those who misuse sedatives, followed by
amphetamines, opioids, cannabis, alcohol, and
cocaine (Bohnert, Ilgen, Louzon, McCarthy, & Katz,
2017). People who report misusing prescription
medication, and in particular pain relievers, also
appear to be vulnerable to suicidal ideation (Ford
& Perna, 2015).
The link between substance misuse and suicide
may relate to the capacity of substances, especially
alcohol, to quell inhibition, leading to poor
judgment, mood instability, and impulsiveness.
Depression, comorbid with suicide risk and
substance misuse, may moderate this relationship.
A population-based sample of people currently
using alcohol and with a history of depressed mood
(Sung et al., 2016) found that those with a positive
history of suicide attempt were significantly more
likely than those without such a history to have
problematic substance use, including 21 percent
with alcohol abuse or dependence and nearly 40
percent with illicit drug abuse or dependence. Yet
alcohol dependence in this sample significantly
increased the odds of suicidal ideation and suicide
attempt even among people without a history of
depressed mood. This suggests that depressed
mood alone cannot account for the relationship
between alcohol misuse and risk of suicide,
although it undoubtedly increases the odds.
Many psychiatric illnesses have a heightened
risk of suicidal thoughts and behaviors further
exacerbated in the presence of co-occurring
addiction. Risk factors for suicide that have been
identified in the general population, such as a
family history of suicide attempt or completion
and access to firearms, also apply to people
with CODs and make self-harm more likely.
Additionally, certain individuals with CODs may
be at even further risk based on the presence
of contributing factors that frequently appear
in populations with mental disorders and
SUDs. For instance, having a chronic physical
health condition (such as traumatic brain injury or
infectious disease), experiencing homelessness,
being a military veteran, and past involvement in
the criminal justice system are all associated with
suicide-related ideation, gestures, attempts, or
deaths (Ahmedani et al., 2017; Cook, 2013; Jahn
et al., 2018; Kang et al., 2015; Tsai & Cao, 2019)
and may further compromise the safety of people
with CODs. A history of adverse life experiences,
like childhood maltreatment or intimate partner
violence, also significantly increases risk of
self-harm (especially in people with CODs) and is
addressed in the section “Trauma.”
Prevention and Management of Suicidal
Behaviors
Although a rare event, suicide is often—but not
always—preventable. All SUD treatment clients
should receive at least a basic screening for
suicidality, and all SUD treatment professionals
should know how to conduct at least basic
screening and triage. (To learn more about suicide
screening, see Chapter 3 of this TIP.) SAMHSA’s
Five-Step Evaluation and Triage (SAMHSA, 2009b)
recommends using the following process for
identifying and responding to threat of self-harm:
1. Identify risk factors.
2. Identify protective factors.
3. Conduct a suicidal inquiry into the client’s
thoughts, plans, behaviors, and intents.
4. Determine the level of risk and appropriate
interventions.
5. Document risk, rationale, intervention, and
follow-up procedures.
Addiction counselors should regularly assess
and monitor all clients with CODs for suicidal
ideation, gestures, plans, and attempts and
especially clients with depressive disorders,
bipolar disorders, PTSD, schizophrenia, or PDs.
Routine assessment should be an integral part of
treatment but is especially critical during times of
high stress or increased substance use (including
relapse) as well as at intake, following any suicidal
behavior, following reports of suicidal ideation,
Chapter 4 131

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
and just before discharge. Information should be
collected on the client’s:
•
Personal and family history of suicidal thoughts
and behaviors.
•
Plan for suicide.
•
Reasons for not following through with past
plans for suicide.
•
Reasons for not following through with the
current plan for suicide.
•
Current support system.
•
Means and access to lethal methods (e.g.,
firearms).
•
History and current symptoms of impulsivity.
•
Depressed mood, feelings of hopelessness, or
both.
•
Protective factors (e.g., coping skills, spiritual/
religious beliefs).
Asking a client directly about his or her desire
to die by suicide does not make self-harm more
likely and in fact can yield helpful information.
Note that people may deny such thoughts or plans
despite having them. Thus, direct questioning
alone is an insufficient risk mitigation strategy.
Suicide risk assessment scales might be useful
in this regard (see Chapter 3 and Appendix C
for suicide risk and self-harm screening tools)
but often lack the specificity and sensitivity to
adequately detect impending suicidal behaviors
(Bolton, Gunnell, & Turecki, 2015). Providers
also should not rely solely on suicide measures.
Instead, suicide screening should include thorough
investigation of all major signs, symptoms, and risk
factors associated with self-harm in mental health,
addiction, or COD populations.
Safety planning is critical in suicide risk mitigation.
Suicide “contracts” are written statements in which
the person who is suicidal states that he or she
will not kill himself but rather call for help, go to
an ED, or other seek other assistance if he or she
becomes suicidal. These contracts are not effective
alone for a client who is suicidal. Such contracts
often help make clients and therapists less anxious
RESOURCE ALERT: SUICIDE PREVENTION RESOURCES FOR
COUNSELORS
•
American Counseling Association (ACA):
−
Suicide Prevention Tip Sheet (https://www.counseling.org/docs/default-source/Communications-/
suicide-prevention-final.pdf?sfvrsn=2)
−
Counselor Training in Suicide Assessment, Prevention, and Management (www.counseling.org/docs/
default-source/vistas/article_65d15528f16116603abcacff0000bee5e7.pdf?sfvrsn=4f43482c_6)
−
Developing Clinical Skills in Suicide Assessment, Prevention, and Treatment (www.counseling.org/
publications/frontmatter/72861-fm.pdf)
•
International Association for Suicide Prevention’s Guidelines for Suicide Prevention (www.iasp.info/
suicide_guidelines.php)
•
SAMHSA:
− Suicide Prevention Resource Center (www.sprc.org/)
− Suicide Assessment Five-Step Evaluation and Triage for Mental Health Professionals (https://store.
samhsa.gov/system/files/sma09-4432.pdf)
− TIP 50, Addressing Suicidal Thoughts and Behaviors in Substance Abuse Treatment (https://store.
samhsa.gov/product/TIP-50-Addressing-Suicidal-Thoughts-and-Behaviors-in-Substance-Abuse-
Treatment/SMA15-4381)
− Video companion to TIP 50, Addressing Suicidal Thoughts and Behaviors in Substance Abuse
Treatment (www.youtube.com/watch?v=1n2Qzlheuzc&feature=youtu.be)
132 Chapter 4

TIP 42
Chapter 4—Diagnostic and Cross-Cutting Topics
about a suicidal condition, but studies have never
shown these contracts to be effective at preventing
suicide. Rather, safety contracts help focus on the
key elements that are most likely to keep clients
safe, such as agreeing to remove the means a
client is most likely to use to commit suicide.
Counselors and other providers should know
their own skills and limitations in engaging,
screening, assessing, and intervening with
suicidal clients and work out these problems with
a supervisor before an emergency. Providers also
should know what immediate onsite and offsite
resources are available to help with someone
identified as suicidal. To learn more about
suicide prevention, see “Resource Alert: Suicide
Prevention Resources for Counselors.”
No empirical treatments for suicide exist. However,
interventions that reduce symptoms of SUDs and
mental illness can help mitigate suicide risk and
decrease self-harm behaviors by improving mood
and enhancing support and coping skills. Some
research supports the use of psychotherapies such
as CBT and dialectical behavior therapy in reducing
parasuicidal behavior and suicide attempts, but the
overall evidence base is small (Bolton et al., 2015).
Pharmacotherapy—particularly antidepressants—
can reduce suicidal behavior in people ages 25
years and older. Yet paradoxically, some studies
show that it actually increases suicide in people
ages 25 and younger (Bolton et al., 2015). Certain
mood stabilizers and antipsychotic medications
also may reduce self-harm in people with bipolar
disorder, schizophrenia, and other psychotic
disorders (Bolton et al., 2015).
The first steps in suicide intervention, and thus
crisis stabilization, are contained in the process
of a good engagement and evaluation. Asking
suicide-related questions, exploring the context
CASE STUDY: COUNSELING AN SUD TREATMENT CLIENT WHO IS SUICIDAL
Beth, a 44-year-old woman, comes to the SUD treatment center complaining that drinking too much
causes problems for her. She has tried to stop drinking before but always relapses. The counselor finds that
she has been sleeping and eating poorly and calling in sick to work. She spends much of the day crying and
thinking of how alcohol, which destroyed her latest significant relationship, has ruined her life. She takes
pain medication for a chronic back problem, which complicates her situation. The counselor tells her of a
therapy group that is a good fit, tells her how to register, and arranges some individual counseling to set
her on the right path. The counselor tells her she has done the right thing by coming in for help and offers
encouragement about her ability to stop drinking.
Beth misses her next appointment. The counselor calls her home and learns from her roommate that Beth
tried to commit suicide after leaving the SUD treatment center. She took an overdose of opioids and is
recovering in the hospital. The ED staff had found Beth under the influence of alcohol upon admission.
Discussion: Although Beth provided information that showed she was depressed, the counselor did not
explore the possibility of suicidal thinking. Counselors always should ask if the client has been thinking
of suicide, whether or not the client mentions depression. Clients, in general, may not answer a very
direct question or may hint at something darker without mentioning it directly. Interpreting the client’s
response requires sensitivity on the part of the counselor. It is important to realize that such questions
do not increase the likelihood of suicide. Clients who, in fact, are contemplating suicide are more likely to
feel relieved that the subject has now been brought into the light and can be addressed with help from
someone who cares.
The client reports taking alcohol and pain medications. Alcohol impairs judgment and, like pain
medications, depresses brain and body functions. The combination of substances increases the risk of
suicide or accidental overdose. Readers are encouraged to think through this case and apply the risk
assessment strategy included in Chapter 3 and use the tools in Appendix C, imagining what kind of
answers the counselor might have received. Readers could consider interventions and referrals that would
have been possible in their treatment settings.
Chapter 4 133

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
of those impulses, evaluating support systems,
considering the lethality of means, and assessing
the client’s motivation to seek help are in
themselves an intervention. Such an interview
will often elicit the client’s own insight and
problem solving and may result in a decrease in
suicidal impulses.
If, however, the client experiences little or no
relief after this process, psychiatric intervention is
required, especially if the client has a cooccurring
mental disorder or medical disorder in which
the risk of suicide is elevated or if the client has
a history of suicide attempts. If either or both is
true, arrangements should be made for transfer
to a facility that can provide more intensive
psychiatric evaluation and treatment. Emergency
ADVICE TO THE COUNSELOR: COUNSELING A CLIENT WHO IS SUICIDAL
•
All SUD treatment clients should receive at least a brief screening for suicide, such as: “In the past, have
you ever been suicidal or made a suicide attempt? Do you have any of those feelings now?”
• All SUD treatment staff should be able to screen for suicidality and basic mental disorders (e.g.,
depression, anxiety disorders, PTSD).
• Screen for suicidal thoughts or plans with anyone who makes suicidal references, appears seriously
depressed, or who has a history of suicide attempts. Treat all suicide threats with seriousness.
• Inquire directly about a client’s depressed mood or agitation. For example:
− “You know, you seem to be pretty down. How depressed are you?”
− The issue may arise via general questions. For example, a client may state, “I don’t use crack much
anymore. I get really down when I’m coming off it.” The counselor may then ask, “How down have you
gotten? Were you ever suicidal? How are you doing now?”
• The suicidal client is more likely to engage with the counselor and reveal suicidality if the counselor
responds to clues given by the client and inquires sensitively about them. Saying, “You seem pretty
uncomfortable and nervous—is there something I can do to help?” to an agitated client opens a door to
further assessment.
• If the client screens positive, use the risk assessment strategy described in Chapter 3 to more
thoroughly investigate suicide intent. Further screening/assessment should be documented to protect
both the client and the counselor. This means writing information on evaluation forms or making
additional notes, even if suicide-related items are not included on the form used.
• Assess the client’s risk of self-harm by asking about what is wrong, why now, whether specific plans
have been made to commit suicide, past attempts, current feelings, and protective factors. (See Chapter
3 and Appendix C for a risk assessment protocol and screening measures.)
• Develop a safety and risk management process with the client that involves a commitment on the
client’s part to follow advice, remove the means to commit suicide (e.g., a gun), and agree to seek help
and treatment. Avoid sole reliance on “no suicide contracts.”
• Assess the client’s risk of harm to others.
• Clients who are actively suicidal should be evaluated by a psychiatrist onsite immediately, or a case
manager or counselor should escort the client to emergency psychiatric services. Where available,
mobile crisis service, including a psychiatrist, is a quick-response resource for management of the client
who is suicidal.
Continued on next page
134 Chapter 4
TIP 42
Chapter 4—Diagnostic and Cross-Cutting Topics
Continued
• Be caring and supportive. The seriously suicidal client should have someone to contact 24 hours a day,
and frequent telephone contact between the client and the contact person usually is indicated.
• Provide availability of contact 24 hours per day until psychiatric referral is realized. Refer clients with
serious plans, previous attempts, or SMI for psychiatric intervention or obtain the assistance of a
psychiatric consultant for the management of these clients.
• Monitor and develop strategies to ensure medication adherence.
• Interventions should seek to increase support available to the client from family and community, and
should provide immediate interventions, including medication to stabilize the client’s mental state, if
needed.
• Families and individuals often benefit from education about depression and suicidality, including
warning signs, resources for help, and the importance of addressing this problem. Education often
provides individuals with a sense of hope and realistic expectations.
• Develop long-term recovery plans to treat substance misuse. Longer term treatment concerns for a
client who has been suicidal focus on long-term treatment strategies for CODs or on other risk factors
that have culminated in a suicidal event. In this case, treatment becomes long-term prevention.
• In people with serious and persistent mental disorders (e.g., bipolar disorder), long-term medication
compliance is key in preventing suicide. Just as essential as medication and medication compliance,
however, is the need to rebuild hope in the future and engender the belief that recovery from co-
occurring disorders is possible and that one has a sense of purpose, value, empowerment, and role in
one’s own recovery.
• Review all such situations with the supervisor or treatment team members.
• Document thoroughly all client reports and counselor suggestions.
procedures should be in place so the counselor
can accomplish this transfer even when a
psychiatrist or clinical supervisor/director is not
available. Once the client is stabilized and is safe
to return to a less restrictive setting, he or she
should return to the program.
Trauma
DSM-5 defines trauma as “as exposure to actual or
threatened death, serious injury, or sexual violence
in one or more of the following ways: (a) directly
experiencing the traumatic event; (b) witnessing,
in person, an event as it occurred to others; (c)
learning that the traumatic event occurred to
a close family member or close friend; and (d)
experiencing repeated or extreme exposure to
aversive details of the traumatic event(s)” (APA,
2013, p. 271).
For many people with mental disorders, SUDs,
or both, past or current trauma is a prominent
driver of negative outcomes such as psychiatric
hospitalizations; suicide attempts; self-harm
behaviors; arrest; aggression; and substance
use initiation, escalation (from occasional use,
to regular use, to misuse/heavy use/addiction),
treatment dropout, and relapse (Kumar, Stowe
Han, & Mancino, 2016; Lijffijt, Hu, & Swann, 2014;
Stinson, Quinn, & Levenson, 2016). Data from the
National Longitudinal Study of Adolescent to Adult
Health (Quinn et al., 2016) confirm that exposure to
childhood trauma (e.g., sexual/emotional/physical
abuse, neglect, witnessing violence) significantly
increases the risk of adulthood prescription pain
reliever misuse (PPRM) and injection drug use.
This risk only grows as the number of traumas
experienced increases; in the study, exposure
to one trauma increased the risk of PPRM by
Chapter 4 135

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
WARNING TO COUNSELORS: RETHINKING TRAUMA
When providers hear the term “trauma,” they probably get a specific picture in their mind of what a client
with trauma looks like—a woman who has been physically abused by her husband, a man who faced
combat as a Marine, a woman who was date raped while in college. These are indeed common examples of
trauma, but addiction counselors who only think of trauma in prototypical terms will overlook clients who
have faced adversities and are in need of help. When thinking about clients with trauma:
Do not think only of women. Men experience trauma, and although at lower rates than women, their
adversities are just as serious and potentially damaging.
Do not think only of military veterans or of people who served in combat. Rates of trauma and PTSD are
certainly high in military populations, but trauma happens to people from all walks of life. Among active
duty military personnel and veterans, people can experience trauma even if they were not directly involved
in combat. (See the section “Special Considerations: Trauma and Military Personnel.”)
Do not think only of physical violence. Emotional abuse and neglect are damaging and can have just as
serious an impact as physical or sexual abuse (Norman et al., 2012).
Do not think only of young people. PTSD is less prevalent in older adults, but up to 52 percent of people
ages 50 and older have had at least one traumatic event in their lives (Choi, DiNitto, Marti, & Choi, 2017).
Remember that someone may not have a PTSD diagnosis but still have PTSD symptoms, a history of
trauma, or both. These people may be just as much in need of treatment as someone with a full-blown
diagnosis. Also, PTSD and its symptoms are easily mistaken for other disorders, such as BPD and depressive
disorders (especially MDD). Although the person may not meet sufficient criteria for PTSD, he or she may
have traumatic stress reactions that need to be addressed. Subclinical traumatic stress reactions are more
commonly expressed through depressive symptoms. Do not assume that just because someone does
not have a PTSD diagnosis that he or she is not in need of trauma-informed care.
34 percent; two traumas, by 50 percent; three
traumas, by 70 percent; and four traumas, by 217
percent. Emotional and physical abuse nearly
doubled the risk of injection drug use.
Prevalence
Traumatic events are common in people with CODs
in part because they are so widely prevalent in the
general population. Almost 90 percent of people in
the United States have a lifetime history of exposure
to at least one traumatizing event, typically the
death of family/close friend because of violence/
accident/disaster; physical or sexual assault; disaster;
or accident/fire (Kilpatrick et al., 2013).
Trauma and CODs
As noted in the section “PTSD,” trauma in people
with addiction, mental illness, or both is the
norm rather than the exception (SAMHSA,
2014b). In more than 600 people receiving SUD
treatment, 49 percent reported a lifetime history of
physical or sexual abuse, and women were 5 times
more likely than men to report lifetime trauma
(Keyser-Marcus et al., 2015). In people with SMI,
trauma exposure is common, with prevalence rates
ranging from 25 percent to 72 percent for physical
abuse, 24 percent to 49 percent for sexual abuse,
and 20 percent to 47 percent for PTSD (Mauritz,
Goossens, Draijer, & van Achterberg, 2013).
Twelve-month or lifetime rates of DSM-5 drug use
disorder (i.e., an SUD excluding alcohol) carries
increased odds of having PTSD (Grant et al., 2016),
and 12-month or lifetime PTSD increases the odds
of having a past-year or lifetime SUD (Goldstein et
al., 2016).
Adverse life experiences are highly coincident
with SUDs and mental disorders, and vice versa:
•
Current PTSD prevalence in addiction
populations is likely 15 percent to 42 percent
(Vujanovic et al., 2016).
•
In active duty military personnel, prevalence
rates of various comorbid mental disorders and
SUDs in people with PTSD have been estimated
at 49 percent for depressive disorders, 36
136 Chapter 4

TIP 42
Chapter 4—Diagnostic and Cross-Cutting Topics
percent for GAD, and almost 27 percent for
AUD (Walter, Levine, Highfill-McRoy, Navarro, &
Thomsen, 2018).
•
Among a sample of U.S. adults with any lifetime
trauma, 47 percent screened positive for PTSD,
almost 47 percent for GAD, and 42 percent
for depression (Ghafoori, Barragan, & Palinkas,
2014).
•
Between 28 percent and 43 percent of people
with PTSD have an SMI (Lu et al., 2013).
•
People with past-year or lifetime PTSD are at
significant risk of developing any number of
comorbid mental disorders, including any mood
disorder (2.4 to 3 times the odds), bipolar I
disorder (2.1 to 2.2 times), any anxiety disorder
(2.6 to 2.8 times), GAD (2 to 2.2 times), panic
disorder (2.1 times), and BPD (2.8 to 3.3 times)
(Goldstein et al., 2016).
•
People with adverse childhood events (e.g.,
abuse, neglect) are more likely to report lifetime
drug use, past-year moderate-to-heavy alcohol
use, lifetime suicide attempt, and past-year
depressed mood than people without such a
history (Merrick et al., 2017). Emotional abuse in
childhood is linked with 6 times the odds for a
lifetime suicide attempt (Merrick et al., 2017).
Trauma-Informed Treatment of CODs
Historically, trauma has not been adequately
addressed in SUD treatment, given provider
fear that doing so would worsen mental and
addiction problems. However, research indicates
the opposite—that failing to address trauma
in people with SUDs leads to worse outcomes
(Brown, Harris, & Fallot, 2013).
Trauma-informed care means attending to trauma-
related symptoms and also creating a treatment
environment that is responsive to the unique needs
of individuals with histories of trauma. Treatment
is focused on reducing specific symptoms and
restoring functioning but also broader goals like
building resiliency, reestablishing trust, preventing
retraumatization, and offering hope for the future.
Creating a supportive, safe treatment environment
is crucial. Counselors must realize how the setting
and their interactions with clients who have trauma
can affect treatment adherence, retention, and
outcomes.
Trauma-informed care for people with mental
disorders, SUDs, or both often includes (SAMHSA,
2014b):
•
Psychoeducation, especially about the
relationship between trauma, mental health, and
addiction. Psychoeducation is also needed to
help normalize symptoms and reassure clients
that their experiences are not unusual, “wrong,”
or “bad.”
•
Teaching coping and problem-solving skills to
foster effective stress management.
•
Discussing retraumatization and developing
strategies to prevent further victimization.
•
Helping clients feel empowered and in control
of their lives.
•
Establishing a sense of safety in clients’ daily
lives and in treatment.
•
Promoting resilience and offering hope for
change and improvement.
•
Identifying and responding adaptatively to
triggers, like intrusive thoughts, feelings, and
sensations.
•
Building a therapeutic alliance, which fosters
trust, confidence, and self-worth—all keys to
healing.
•
Using trauma-specific interventions, like:
-
CBT.
-
Cognitive processing therapy.
-
Exposure therapy.
-
Eye movement desensitization/reprocessing.
-
Affective regulation.
-
Distress tolerance and stress inoculation.
-
Peer support services from other people who
have a trauma history and are thriving.
TIP 57, Trauma-Informed Care in Behavioral
Health Services (SAMHSA, 2014b) and SAMHSA’s
“Concept of Trauma and Guidance for a Trauma-
Informed Approach” (SAMHSA, 2014c) will help
addiction and mental health professionals tailor
their services in a way that is respectful of and
sensitive to clients’ trauma-related needs. Chapter
6 discusses adapting treatments for CODs to
female clients with trauma.
Chapter 4 137

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
ADVICE TO THE COUNSELOR: COUNSELING A CLIENT WITH TRAUMA
• Clients need not only to feel safe in the treatment environment, but also to feel safe from their trauma
symptoms, many of which are intrusive, overwhelming, and distressing.
• Ensure interventions/interactions do not distress or traumatize clients. Avoid:
− Being overly confrontational or argumentative with clients.
− Discounting and dismissing clients’ experiences and feelings.
− Minimizing or ignoring clients’ responses and needs.
− Pushing clients to talk in greater detail about their trauma.
− Violating clients’ physical boundaries.
• Educate clients about the link between trauma and mental disorders, SUDs, or both.
• Normalize clients’ reactions and feelings; this helps validate their experiences and offers a sense of relief.
• Help clients identify triggers and learn more adaptive ways to cope and respond to them. This reduces
maladaptive distress management strategies like substance use, self-injurious behaviors, and avoidance.
• Although trauma is an important focus of treatment, it does not need to be the sole focus. In fact,
constantly focusing on the trauma can be overwhelming and emotionally draining for clients.
• Include specific SUD treatment approaches and techniques to address addiction symptoms.
• Use an integrated trauma and SUD recovery model that fully addresses mental and substance-related
needs.
• Explore with clients their readiness for change using the Stages of Change Model. This aids treatment
matching, fosters better adherence/completion rates, and increases clients’ chances for long-term
recovery.
Special Considerations: Trauma and Military
Personnel
Active duty and veteran members of the military
are highly susceptible to trauma and all of its
deleterious aftereffects. PTSD prevalence is
significantly higher than that of the general
population and civilian clinical samples, including
9 percent among a sample of more than 4 million
veterans in primary care settings (Trivedi et al.,
2015), 23 percent among Operations Enduring
Freedom and Iraqi Freedom (OEF/OIF) veterans
(Fulton et al., 2015), 21 percent in Gulf War
veterans (Dursa, Barth, Schneiderman, & Bossarte,
2016), and 8.5 percent to 12.2 percent of Vietnam
War veterans (Marmar et al., 2015).
About 20 percent of veterans have CODs (Trivedi
et al., 2015); 16 percent have PTSD and SUDs
specifically (Mansfield, Greenbaum, Schaper,
Banducci, & Rosen, 2017). In a sample of (OEF/
OIF) veterans, 63 percent of people with SUD
also had PTSD (Seal et al., 2011). Other common
mental disorders in this population include SMI,
depression, and anxiety; all tend to co-occur
often (Exhibit 4.20). These illnesses are linked with
increased hospitalizations, ED use, and mortality,
with SMI and SUDs being particularly damaging
(Trivedi et al., 2015).
Many veterans seek treatment outside of the
Veterans Health Administration, so community
addiction counselors should prepare to work
with them. Counseling veteran or active duty
military populations requires a slightly different
knowledge base, clinical approach, and skillset
than civilian populations. SUD counselors should
note that (Briggs & Reneson, 2010; Teeters,
Lancaster, Brown, & Back, 2017):
•
War zone stress reactions often require
specialized care and an understanding of the
experiences faced by soldiers in combat.
138 Chapter 4

TIP 42
COMORBID
MENTAL
ILLNESSES
PRIMARY MENTAL ILLNESS
SUD 21.9 percent 23.2 percent 22.1 percent 29.0 percent —
SMI 8.8 percent 8.0 percent 10.2 percent — 12.8 percent
Anxiety 13.9 percent 19.4 percent — 13.3 percent 12.7 percent
Depression 48.1 percent — 55.0 percent 29.5 percent 37.8 percent
PTSD — 33.2 percent 27.1 percent 22.4 percent 24.6 percent
Specific
Disorder
PTSD Depression Anxiety SMI SUD
EXHIBIT 4.20. Veterans and CODs
Chapter 4—Diagnostic and Cross-Cutting Topics
Source: Trivedi et al. (2015).
•
Military-related trauma exposure does not
include only direct combat. For instance, people
working in intelligence gathering and medical
personnel are often deployed to war zones
where they witness horrific acts of violence and
are potential targets of violence themselves.
•
Female veterans often have specific service
needs, such as those to address military sexual
trauma (e.g., sexual assault, harassment),
intimate partner violence, and child care. (Note
that men also can be victims of military sexual
trauma, albeit at far lower rates than reported
by women. Do not assume that military sexual
trauma is solely a women’s issue.)
•
Many veterans are hesitant to seek SUD
treatment or mental health services because
of fear that doing so could negatively affect
their career advancement. Concerns about
confidentiality are thus understandably very high
in these clients.
•
Shame, embarrassment, and stigma over
mental health and addiction are prominent.
Military culture fosters some behaviors and
mindsets that can be adaptive in combat—like
independence, being “masculine,” and not
showing “weakness”—but make seeking
treatment much harder.
•
Suicide risk is high in veterans. It requires active
monitoring and management throughout
treatment, particularly for military personnel
with childhood trauma, PTSD, military sexual
trauma, or depression (Carroll, Currier,
McCormick, & Drescher, 2017; Cunningham
et al., 2017; Kimerling, Makin-Byrd, Louzon,
Ignacio, & McCarthy, 2016; McKinney, Hirsch, &
Britton, 2017; Pompili et al., 2013).
Indepth discussions about prevention programming
and treatment for military populations with
trauma, suicide risk, SUDs, mental disorders, or
a combination thereof is beyond the scope of
this TIP. However, ample information is available
elsewhere. The following resources offer helpful
guidance about working with military professionals
who engage in substance misuse or have mental
illness, including trauma, suicidality, and CODs:
•
ACA:
-
Suicide Among Veterans and the Implications
for Counselors (www.counseling.org/docs/
default-source/vistas/suicide-among-vet-
erans-and-the-implications-for-counselors.
pdf?sfvrsn=3803a659_11)
-
Comparison of Civilian Trauma and Combat
Trauma (https://pdfs.semanticscholar.org/
eff2/8af43d3feaac7bac3cc5bb789bd4d5f
100ec.pdf)
- Counseling Addicted Veterans: What
to Know and How to Help (https://
pdfs.semanticscholar.org/9742/967aac-
815ca02c4f599b36be996d0b10d3d9.pdf)
•
The Department of Veterans Affairs’ National
Center for PTSD (www.ptsd.va.gov/):
- Practice Recommendations for Treatment
of Veterans with Comorbid Substance Use
Disorder and Posttraumatic Stress Disorder
(www.mentalhealth.va.gov/providers/sud/
docs/SUD_PTSD_Practice_Recommendations.
pdf)
Chapter 4 139

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
- Veteran Outreach Toolkit: Preventing Veteran
Suicide Is Everyone’s Business (www.va.gov/
ve/docs/outreachToolkitPreventingVeteran-
SuicideIsEveryonesBusiness.pdf)
- National Strategy for Preventing Veteran
Suicide, 2018–2028 (www.mentalhealth.
va.gov/suicide_prevention/docs/
Office-of-Mental-Health-and-Suicide-
Prevention-National-Strategy-for-Preventing-
Veterans-Suicide.pdf)
•
SAMHSA’s Addressing the Substance Use
Disorder Service Needs of Returning Veterans
and Their Families (www.samhsa.gov/sites/
default/files/veterans_report.pdf)
•
Community Anti-Drug Coalitions of America’s
Strategies for Addressing Substance Abuse
in Veteran Populations (www.cadca.org/sites/
default/files/mckesson_toolkit_1.pdf)
Conclusion
The material in this chapter is intended to increase
SUD treatment counselors’ and other providers’
familiarity with mental disorders terminology
and criteria, as well as to provide advice on how
to proceed with clients who demonstrate these
disorders. The consensus panel encourages
counselors to continue to increase their
understanding of mental disorders by using the
resource material referenced in each section (and
in Appendix C), attending courses and conferences
in these areas, and engaging in dialog with mental
health professionals who are involved in treatment.
At the same time, the panel urges continued work
to develop improved treatment approaches that
address substance use in combination with specific
mental disorders, as well as better translation of
that work to make it more accessible to the SUD
treatment field.
140 Chapter 4

Chapter 5—Strategies for Working With
People Who Have Co-Occurring Disorders
KEY MESSAGES
TIP 42
SUBSTANCE USE DISORDER TREATMENT FOR
PEOPLE WITH CO-OCCURRING DISORDERS
• Building a positive therapeutic alliance is a
cornerstone of effective, high-quality, person-
centered care for all clients, especially those
with co-occurring disorders (CODs). Clients
with CODs often experience stigma, mistrust,
and low treatment engagement.
• CODs are complex and are associated with
certain clinical challenges that, if unaddressed,
can compromise the counselor–client
relationship and impinge on quality of care,
potentially leading to suboptimal outcomes.
• Strategies and approaches like empathic
support, motivational enhancement, relapse
prevention techniques, and skill building help
strengthen clients’ ability to succeed and
make long-term recovery more likely.
• Certain mental disorders are complex,
chronic, and difficult to treat, including major
depressive disorder (MDD), anxiety disorders,
posttraumatic stress disorder (PTSD), and
serious mental illness (SMI). Clients with these
disorders may have unique symptoms and
limitations in function.
• Empirically based substance use disorder
(SUD) treatment approaches can help
counselors address these unique symptoms
and functional limitations in ways that
will minimize their potential to disrupt the
therapeutic relationship and impede positive
treatment outcomes.
Establishing and maintaining a successful
therapeutic relationship with clients can enhance
treatment engagement, participation, and
outcomes. Building a good therapeutic relationship
with clients who have CODs is especially important,
yet doing so can be difficult. The first part of this
chapter reviews guidelines and techniques for
building rapport and optimizing outcomes when
providing SUD treatment to clients who have
CODs. The chapter also describes how to modify
general treatment principles to suit the needs of
clients with COD—particularly useful when working
with clients in Quadrants II and III. (Chapter 3
addresses the Four Quadrants Model of service
provision.) The second part describes evidence-
based techniques for building therapeutic rapport
and effectively counseling clients with CODs
involving specific mental disorders—MDD, anxiety
disorders, PTSD, and SMI.
The material in this chapter is consistent with
national or state consensus practice guidelines for
COD treatment and consonant with many recom-
mendations therein:
•
Counselors must be able to address common
clinical challenges, like managing feelings
and biases that could arise when working with
clients who have CODs (sometimes called
countertransference).
•
Together, providers and clients should monitor
clients’ disorders and symptoms by examining
the status of each disorder and alerting each
other to signs of relapse.
•
Counselors can help clients with functional
deficits in areas such as understanding
instructions by using repetition, skill-building
strategies, and other accommodations to aid
progress.
² SMI: A diagnosable mental, behavioral, or emotional disorder (other than developmental disorders or SUDs) that persists
long enough to meet diagnostic criteria and that causes functional impairment sufficient to substantially disrupt major life
activities (Substance Abuse and Mental Health Services Administration [SAMHSA], 2017).
141

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
•
The consensus panel recommends that
counselors primarily use a supportive,
empathic, and culturally responsive approach
when working with clients who have CODs.
Counselors need to distinguish behaviors and
beliefs of cultural origin from those that may
indicate a mental disorder.
•
Counselors and other service providers should
use motivational enhancement and relapse
prevention strategies consistent with each
client’s specific stage of recovery. These
strategies are helpful regardless of the severity of
a client’s mental disorder.
This chapter is intended for counselors and other
behavioral health service providers, supervisors,
and administrators. Throughout this chapter,
“Advice to the Counselor” boxes highlight
practical guidance for counselors.
Competencies for Working With
Clients Who Have CODs
Before establishing therapeutic rapport with clients
who have CODs, treatment providers first must
ensure that they possess integrated competencies
for working with the COD population. This means
having the specific attitudes, values, knowledge,
and skills needed to provide appropriate services
to individuals with CODs in the context of the
providers’ job and program setting.
Just as other types of integration exist on a
continuum, so too does integrated competency.
Some interventions or programs require only basic
competency in welcoming, screening, and assessing
individuals with CODs to identify their treatment
needs. Other interventions, programs, or job
functions (e.g., those of supervisory staff) may require
more advanced integrated competency. Clients with
more complex or unstable disorders require providers
with higher levels of integrated competency.
They also require more formal mechanisms within
programs to coordinate various staff members,
providing effective integrated treatment.
The mental health service and SUD treatment
systems are moving toward identification of a
basic, required level of integrated competency
for all providers. Many states are developing
curriculums for initial and ongoing training and
supervision to help providers achieve competency.
Other states have created career ladders and
certification pathways to encourage providers to
achieve greater competency and to reward them
for this achievement. (See Chapter 8 for further
discussion of counselor competencies.)
Guidelines for a Successful
Therapeutic Relationship
This section reviews 10 guidelines for forming a
good therapeutic relationship with clients who
have CODs, thereby increasing their chances of
successful long-term recovery.
Develop and Use a Therapeutic Alliance
To Engage Clients in Treatment
Research suggests that a therapeutic alliance is a
strong, if not essential, factor in supporting recovery
from mental disorders and SUDs (Kelly, Greene, &
Bergman, 2016; Shattock, Berry, Degnan, & Edge,
2018; Zugai, Stein-Parbury, & Roche, 2015). The
therapeutic alliance can foster desirable outcomes
by improving symptoms, functioning, treatment
engagement, treatment satisfaction, and quality
of life (Dixon, Holoshitz, & Nossel, 2016; Kidd,
10 GUIDELINES FOR
DEVELOPING SUCCESSFUL
THERAPEUTIC RELATIONSHIPS
WITH CLIENTS WHO HAVE CODS
1. Develop and use a therapeutic alliance to
engage clients in treatment.
2. Maintain a recovery perspective.
3. Ensure continuity of care.
4. Address common clinical challenges (e.g.,
countertransference, confidentiality).
5. Monitor psychiatric symptoms (including
symptoms of self-harm).
6. Use supportive and empathic counseling;
adopt a multiproblem viewpoint.
7. Use culturally responsive methods.
8. Use motivational enhancement.
9. Teach relapse prevention techniques.
10. Use repetition and skill building to address
deficits in functioning.
142 Chapter 5

TIP 42
Chapter 5—Strategies for Working With People Who Have Co-Occurring Disorders
Given the proliferation of research over the past few decades on technology-based interventions in
behavioral health services, some researchers have explored how technology can affect client–counselor
relationships in COD treatment. A pilot study from Ben-Zeev, Kaiser, and Krzos (2014) examined the use
of mobile phone technology to monitor clients with SMI and SUDs. Using daily text messages over 12
weeks, team members routinely texted clients (in what the study authors termed “hovering”) reminders
of upcoming appointments, inquiries about medication adherence, general suggestions about managing
symptoms, and, as needed, crisis management. At the end of the trial, participant ratings of therapeutic
alliance with providers who “hovered” were significantly higher than those for providers who did not use
the intervention. Most clients were satisfied with the technology, and 87 percent said it helped them feel
more in control of their lives.
Davidson, & McKenzie, 2017). For clients with
SMI (e.g., bipolar disorder, schizophrenia), better
therapeutic alliance has been linked to a reduction
in symptoms, fewer hospitalizations, greater
antipsychotic medication adherence, and improved
client self-esteem (Garcia et al., 2016; Shattock et
al., 2018). Studies of people with SUDs or CODs
also suggest that a strong therapeutic alliance is a
significant predictor of treatment retention, symptom
reduction, enhanced abstinence-related self-efficacy,
and more days of abstinence (Campbell, Guydish,
Le, Wells, & McCarty, 2015; Connors et al., 2016;
Maisto et al., 2015).
However, the personal beliefs of individuals with
CODs, such as mistrust of treatment providers
and fear of stigma, can be barriers to treatment
seeking, access, and engagement (Priester et
al., 2016) and can make establishing a close,
trusting client–provider relationship challenging.
Developing an effective relationship with clients who
have SMI and SUDs can be especially difficult. Some
individuals have little insight, lower motivation to
change, and less ability to seek/access care than
people without CODs (Pierre, 2018). Challenges
may be more apparent in clients with SUDs and co-
occurring psychosis, as they may have emotional/
cognitive dysfunctions inhibiting their ability to
participate in treatment (Priester et al., 2016). The
presence and level of clinical and functional deficits
varies widely from one person with CODs to the
next, and among all people with CODs over the
course of their illness and lifetime.
To foster treatment engagement for clients with
CODs, therapeutic relationships must build on
clients’ existing capacities. The therapeutic alliance
is the cornerstone of the COD recovery process.
Once established, the alliance is rewarding for
both client and provider and facilitates their joint
participation in a full range of therapeutic activities.
Counselors should document alliance-building
activities to help manage risk.
Maintain a Recovery Perspective
Varied Meanings of “Recovery”
The word “recovery” has different meanings in
different contexts. SUD treatment providers may
think of clients who have changed their substance
use behavior as being “in recovery” for the rest of
their lives (but not necessarily in formal treatment
forever). Mental health clinicians may think of
ADVICE TO THE COUNSELOR:
FORMING A THERAPEUTIC
ALLIANCE
The consensus panel recommends these
approaches to form a therapeutic alliance with
clients who have CODs:
• Demonstrate an understanding and
acceptance of clients.
• Help clients clarify the nature of their difficulties.
• Indicate that you will work together with clients.
• Communicate to clients that you will help
them help themselves.
• Express empathy and a willingness to listen to
clients’ understanding of their problems.
• Assist clients in solving external problems
directly and immediately.
Chapter 5 143

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
ADVICE TO THE COUNSELOR: MAINTAINING A RECOVERY PERSPECTIVE
The consensus panel recommends these approaches for maintaining a recovery perspective in treating CODs:
• Assess each client’s stage of change (see the section “Using Motivational Enhancement Consistent With
Clients’ Specific Stage of Change”).
• Ensure that treatment stage and expectations are consistent with each client’s stage of change.
• Use client empowerment to motivate change.
• Foster continuous support.
• Provide continuity of treatment.
• Acknowledge that recovery is a long-term process; support and applaud even small gains by clients.
recovery as a process in which the client moves
toward specific behavioral goals in stages; in this
conceptualization, recovery is assessed by whether
these goals are achieved. In mutual-support
programs, recovery implies not only abstinence
from substances but also a commitment to “working
the program,” which includes group members
changing the way they act with others and taking
responsibility for their actions. People with mental
disorders may see recovery as the process of
reclaiming a meaningful life beyond mental illness,
with symptom control and positive life activity.
Generally, it is recognized that recovery does
not refer solely to a change in substance use
but also to a change in an unhealthy way of
living. Markers such as improved health, better
ability to care for oneself and others, increased
independence, and enhanced self-worth indicate
progress in recovery.
Implications of the Recovery Perspective
The recovery perspective as developed in the SUD
treatment field has two main features:
1. It acknowledges that recovery is a long-term
process of internal change.
2. It recognizes that these internal changes proceed
through various stages (see De Leon [1996] and
Prochaska et al. [1992] for a detailed description).
The recovery perspective generates two main
principles for practice:
•
Develop a treatment plan that provides for
continuity of care over time. In preparing
this plan, the provider should recognize that
treatment may occur in different settings over
time (e.g., residential, outpatient). The plan
should reflect that much of the recovery process
is client driven and typically occurs outside of, or
following, professional treatment (e.g., through
participation in mutual support). Providers
should reinforce long-term participation in these
settings.
•
Use interventions that match the tasks and
challenges specific to each stage of the
COD recovery process. Doing so enables
providers to use sensible stepwise approaches
in developing and using treatment protocols.
Markers that are unique to individuals—such as
those related to their cultural, social, or spiritual
context—should be considered. Providers
should engage clients in defining markers of
progress that are meaningful to them in each
stage of recovery.
Stages of Change and Stages of Treatment
Working within the recovery perspective requires
a thorough understanding of the interrelationship
between stages of change (as originally defined by
Prochaska et al., 1992, and built upon by De Leon,
1996) and stages of treatment (see the section
“Using Motivational Enhancement Consistent
With Clients’ Specific Stage of Change”). De Leon
developed a measure of motivation for change
and readiness for treatment—Circumstances,
Motivation, and Readiness Scales—and provided
scores for samples of people with CODs (De
Leon, Sacks, Staines, & McKendrick, 2000). The
144 Chapter 5

TIP 42
Chapter 5—Strategies for Working With People Who Have Co-Occurring Disorders
scales have a demonstrated relationship with
retention in general SUD treatment populations
and programs (Ali, Green, Daughters, & Lejuez,
2017). A meta-analysis (Krebs, Norcross, Nicholson,
& Prochaska, 2018) found that client stage or
readiness level of change predicted psychotherapy
outcomes among people with SUDs, eating
disorders, anxiety disorders, depressive disorders,
borderline personality disorder, and CODs (e.g.,
PTSD and alcohol dependence). The authors
suggest tailoring goal setting, treatment processes,
and resources to each client’s stage of change
to optimize outcomes. Expectations for clients’
progress through treatment stages (e.g., outreach,
stabilization, early-middle-late primary treatment,
continuing care, long-term care) should be
consistent with clients’ stages of change.
Client Empowerment and Responsibility
The recovery perspective emphasizes clients'
empowerment and responsibility and their network
of family and significant others. Per Green,
Yarborough, Polen, Janoff, and Yarborough (2015),
achieving sobriety can be a major step in building
clients’ feelings of self-efficacy and confidence
to further achieve recovery in SMI and can be a
turning point in advancing their personal growth,
improving functioning, and meeting recovery goals.
Continuous Support
The recovery perspective highlights the need
for continuing recovery support. Providers
encourage clients to build a support network that
offers respect, acceptance, and appreciation.
For example, an important element of long-term
participation in Alcoholics Anonymous (AA) is
the sense of belonging or a “home.” AA offers
this supportive environment without producing
overdependence because members are expected
to contribute, as well as receive, support.
Ensure Continuity of Care
Continuity of treatment flows from a recovery
perspective and is a guiding principle in its own
right. Continuity of treatment implies that COD
services are constant. Treatment continuity for
clients with CODs begins with proper, thorough
identification, assessment, and diagnosis. Per a
review by McCallum et al. (2015), continuity of care
for people with CODs means providing:
•
Care that is regular and consistent over time.
•
Care that is continually adjusted to the client’s
needs.
•
Continuity in the counselor–client relationship,
such as through ongoing and reliable contact.
•
Continuity across services via case management,
coordination of care, and linkage to resources.
•
Continuity in the transfer of care, including
maintaining contact (as appropriate) even after
handoff.
On a program level (Padwa, Larkins, Crevecoeur-
MacPhail, & Grella, 2013), continuity of care for
clients with CODs can include having structures,
procedures, and training in place that enables
providers to:
•
Assess and monitor mental disorder and SUD
symptoms.
•
Develop discharge planning that continually
supports clients through community resources
(e.g., peer recovery support services, mutual
support).
•
Ensure medication needs are met (e.g.,
medication checks are scheduled, prescription
refill procedures are in place) for people on
pharmacotherapy.
More discussion of how counselors can ensure
continuity of care for clients with CODs across
different treatment settings can be found in
Chapters 2 and 7.
Address Common Clinical Challenges
Ease Discomfort and Reluctance
Providers’ ease in working toward a therapeutic
alliance is affected by their comfort level in working
with clients who have CODs. SUD counselors
may find some clients with SMI or severe SUDs
to be threatening or unsettling. This discomfort
may result from lack of experience, training, or
mentoring. Likewise, some mental health clinicians
may feel uncomfortable or intimidated by clients
with SUDs. Providers need to recognize certain
Chapter 5 145

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
ADVICE TO THE COUNSELOR: MITIGATING RELAPSE BY MANAGING THE
RECOVERY ENVIRONMENT
To guide clients through recovery and ensure delivery of comprehensive, recovery-oriented care,
counselors must help clients establish and maintain a supportive recovery environment. This environment
is more than where clients live; it compasses clients’ entire physical, emotional, social, educational, and
vocational world.
Understanding limitations in clients’ recovery environments is critical to helping them prevent relapse
and problem solve barriers. Environmental obstacles and lack of support can sabotage clients’ recovery
efforts and can be difficult to overcome without assistance from a mental health or addiction professional.
Counselors can help clients with CODs create a life conducive to recovery by assessing areas of
functioning and symptoms and offering services relevant to the American Society of Addiction Medicine’s
Patient Placement Criteria, Third Revision, Domain 6 (Mee-Lee et al., 2013). This means working with
clients to identify and explore:
• The client’s current living situation, including the physical living space, the people who co-occupy their
home, and the surrounding community (e.g., Is it safe? Is it disruptive to recovery? Does the client live in
an area where illicit substances are easily accessible?).
• The client’s available supports for all biopsychosocial needs, whether related to illness or broader
areas of living, like social life, work, and relationships. For instance, does the client have reliable
transportation? What about child care? Does the client have people in his or her life to rely on for
tangible and emotional support? Is the client able to maintain primary care and behavioral health
appointments?
• Threats to support in the client’s life, such as friends or loved ones who actively misuse substances or
family members who are unsupportive of SUD treatment?
• Whether the client engages in peer support, 12-Step support, or other mutual-support programs.
• Educational or occupational matters that facilitate or hinder recovery. For instance, is the client employed?
Does his or her supervisor know that the client is in recovery (and supportive of this)? Is the client working to
complete his or her degree, and does the client value degree completion as a recovery goal?
• Whether the client is engaged in meaningful activities with family, friends, partners, coworkers, classmates,
or peers. Also, does the client have hobbies or otherwise regularly engage in pleasant activities?
• Whether the client is involved in the criminal justice system, child welfare system, or both.
• Whether the client needs financial assistance (e.g., applying for Social Security Disability Insurance).
patterns that invite these feelings and not let them
interfere with clients’ treatment. Providers who find
it challenging to form a therapeutic alliance with
clients who have CODs should consider whether
their difficulty is related to:
•
The client’s difficulties.
•
A limitation in their own experience and skills.
•
Demographic differences between themselves
and their clients in areas such as age, gender,
education, socioeconomic status, race, or ethnicity.
•
Countertransference (see the section “Manage
Countertransference”).
A consultation with a supervisor or peer to discuss
this issue is important. Often these reactions can
be overcome with further experience, training,
supervision, and mentoring.
Individuals with CODs may also feel challenged
146 Chapter 5
TIP 42
Chapter 5—Strategies for Working With People Who Have Co-Occurring Disorders
in forming a therapeutic relationship with their
treatment providers. They often experience
demoralization and despair, given the complexity of
having multiple behavioral health concerns and the
difficulty of achieving treatment success. Inspiring
hope often is a necessary precursor that allows
clients to give up short-term relief for long-term
work, even when there is some uncertainty in
timeframe and benefit.
Manage Countertransference
Providers should understand difficulties related
to countertransference and be familiar with
strategies to manage it. Although the concept
of countertransference is somewhat dated
and infrequently used in the COD literature, it
can help providers understand how their past
experiences can influence current attitudes
toward certain clients. Transference describes the
process whereby clients project attitudes, feelings,
reactions, and images from the past onto their
providers. For example, the client may regard the
provider as an “authoritative father,” “know-it-all
older brother,” or “interfering mother.”
Countertransference is now understood to be a
normal part of providers’ treatment experience.
Particularly when working with clients who have
ADVICE TO THE COUNSELOR:
MANAGING
COUNTERTRANSFERENCE
The consensus panel recommends this
approach to manage countertransference with
clients who have CODs:
• Be aware of strong personal reactions and
biases toward clients.
• Get further supervision when
countertransference is suspected and may be
interfering with counseling.
• Receive formal and periodic clinical
supervision; counselors should have
opportunities to discuss countertransference
with their supervisors and with other staff at
clinical team meetings.
multiple, complicated problems, providers are
as vulnerable as clients to feelings of pessimism,
despair, and anger, as well as desires to abandon
treatment. Less experienced providers may find
it harder to identify countertransference, access
feelings evoked by interactions with clients, name
those feelings, and keep feelings from interfering
with the counseling relationship.
SUDs and mental disorders are stigmatized by
the general public. Stigma can also be present
among providers. Mental health clinicians who
usually do not treat people with SUDs may not
have worked out their own responses to substance
misuse, which can influence their interactions with
these clients. Providers working with clients who
have SMI may have more negative beliefs about
and express more negative attitudes toward clients
with SMI than those without such diagnoses (Smith,
Mittal, Chekuri, Han, & Sullivan, 2017; Stone et
al., 2019). Providers who treat clients with SMI can
benefit from working with supervisors to uncover
and correct underlying harmful thoughts and
attitudes.
Similarly, SUD treatment providers may be
unaware of their own reactions to people with
specific mental disorders and may have difficulty
preventing these reactions from influencing
treatment. Their negative attitudes or beliefs
may be communicated, directly or subtly, to the
client—for example, through thoughts like, “I was
depressed too, but I never took medications for
it—I just worked the Steps and got over it. So why
should this guy need medication?”
Negative feelings generated by countertrans-
ference can worsen over time. Some research
indicates that providers treating clients with CODs
may feel less satisfied with their jobs and increas-
ingly frustrated with their clients the longer they
stay in practice (Avery et al., 2016).
Providers’ negative attitudes toward clients with
CODs can have a significant impact on treatment
services and outcomes. For example, countertrans-
ference may result in providers failing to offer timely,
appropriate treatment and having poor communica-
tion with their clients (Avery et al., 2016). (For a full
discussion of countertransference in SUD treatment,
see Powell & Brodsky, 2004.) Countertransference
Chapter 5 147

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
Providers have a duty to be aware of federal
rules under the Health Insurance Portability and
Accountability Act and any additional regulations
in their states dictating what information they
can and cannot share with other providers (as
well as caregivers and family members) and
under which circumstances.
problems are particularly significant when working
with people who have CODs, because people with
SUDs and mental disorders may evoke strong
feelings in providers that could become barriers
to treatment if providers allow such feelings
to interfere. Providers may feel angry, used,
overwhelmed, confused, anxious, uncertain how to
proceed with a case, or just worn out.
Cultural concerns may cause strong yet unspoken
feelings, creating countertransference and trans-
ference. Counselors working with clients in their
area of expertise may be familiar with countertrans-
ference, but working with an unfamiliar population
will introduce different kinds and combinations of
feelings.
Protect Condentiality
Confidentiality and privacy are relevant to every
clinical situation and are especially important
for clients with SMI, SUDs, or both. These
conditions can be complex and debilitating, and
they are associated with an increased risk of harm
to self and others. Furthermore, people receiving
SUD treatment in federally funded programs are
protected by additional regulations that affect
information sharing, privacy, and consent. More
information about these regulations is available
online (www.samhsa.gov/about-us/who-we-are/
laws-regulations/confidentiality-regulations-faqs).
RESOURCE ALERT: FEDERAL
AND STATE MENTAL HEALTH
PRIVACY AND CONFIDENTIALITY
REGULATIONS
Mental health regulations regarding privacy,
confidentiality, and information sharing
(including duty to warn laws) vary by state.
Counselors can stay up-to-date on regulations in
the state(s) in which they practice by accessing
information and resources available online:
• SAMHSA’s Directory of Single State Agencies
for Substance Abuse Services (https://www.
samhsa.gov/sites/default/files/single-state-
agencies-directory-08232019.pdf)
• National Conference of State Legislatures’
Mental Health Professionals Duty to Warn
(www.ncsl.org/research/health/mental-health-
professionals-duty-to-warn.aspx)
General resources about the protection of
mental health clients’ and SUD treatment
clients’ rights include:
• Department of Health and Human Services’
Mental Health Information Privacy FAQs (www.
hhs.gov/hipaa/for-professionals/faq/mental-
health/index.html)
• SAMHSA’s Laws and Regulations (www.
samhsa.gov/about-us/who-we-are/
laws-regulations)
• SAMHSA’s Substance Abuse Confidentiality
Regulations FAQs (www.samhsa.gov/
about-us/who-we-are/laws-regulations/
confidentiality-regulations-faqs)
However, confidentiality is not absolute. Contexts
in which to be mindful of protections related
to client privacy and confidentiality—and the
limitations of those protections—include:
•
When collaborating with other providers,
especially those outside of the behavioral
health field. All clients have a right to privacy
and confidentiality. There are federal as well
as state regulations that dictate the type of
information providers can share with other
providers while upholding those rights for their
clients. Remember that counselors who practice
in more than one location must follow the
regulations in each of the states in which they
see clients. (See “Resource Alert: Federal and
State Mental Health Privacy and Confidentiality
Regulations.”)
148 Chapter 5

TIP 42
Chapter 5—Strategies for Working With People Who Have Co-Occurring Disorders
•
When working in a setting with electronic
health records (EHRs). The proliferation of EHRs
has helped foster easier record sharing between
mental health and general medical clinicians
but also poses a risk to confidentiality that, if
breached, could seriously damage client trust in
the counselor and in the psychotherapy process
in general (Shenoy & Appel, 2017).
•
When working with clients who verbalize
specific threats of harm to a third party. If
the counselor has reason to believe a violent
act is foreseeable and is directed at a specific
person, breach of confidentiality may be
appropriate or even required by the state’s
duty to warn mandate. Counselors should seek
consultation, as needed and as appropriate
given the volatility of the situation. If employed
by an agency, follow required treatment facility
policies/procedures as well.
•
When treating clients with trauma/PTSD.
Trauma survivors may be mistrustful and
concerned about privacy, posing barriers to
treatment (Kantor, Knefel, & Lueger-Schuster,
2017). Trauma in the context of ongoing
intimate partner violence, child maltreatment,
sexual assault, or elder abuse raises ethical and
legal concerns about breaching confidentiality
under duty to warn laws.
•
When working with clients ages 18 and
under, including students. Discussion of
pediatric and adolescent mental disorders
and substance misuse is beyond the scope of
this TIP. Information on laws affecting mental
health clinicians and addiction counselors is
available via American Academy of Pediatrics’
Confidentiality Laws Tip Sheet (www.aap.org/
en-us/advocacy-and-policy/aap-health-iniaves/
healthy-foster-care-america/Documents/
Condenality_Laws.pdf) and in the resource
alert about federal and state privacy and
confidentiality regulations.
Providers must understand how to involve
family members, when appropriate, without
jeopardizing client privacy and confidentiality.
Families often want to be involved in the care of a
loved one with CODs—especially if the individual
has a history of nonadherence to medication and
other treatment and does not have other support
systems in place. Sometimes, family members or
caregivers must be involved because the client
lacks capacity to make independent healthcare
decisions.
Recommended practices for involving families
(Rowe, 2012) in a client’s COD treatment include:
•
Involving family members in planning and
implementing treatments to the extent possible
(after discussing their involvement with the
client and obtaining his or her written consent).
•
Conveying the same respect and empathy
toward family members as toward clients to build
rapport.
•
Developing a contract that spells out what type
of information families will and will not receive
and what role they can play in their loved one’s
treatment.
Monitor Psychiatric Symptoms
Joint Treatment Planning
When SUD counselors work with clients who
have CODs, especially those who need medi-
cations or are receiving mental health services
separately from SUD treatment, it is especially
important that they participate in developing
client treatment plans and monitoring clients’
psychiatric symptoms. The SUD counselor should,
at minimum, be knowledgeable of the overall
treatment plan to permit reinforcement of the
plan’s mental health aspects as well as aspects
specific to recovery from SUDs. It is equally
important for clients to participate in developing
their COD treatment plans.
For example, for a client with bipolar disorder
and alcohol use disorder (AUD) who is receiving
treatment at both an SUD treatment agency and
a local mental health center, the treatment plan
might include individual SUD treatment counseling,
medication management, and group therapy. In
another example, for a client taking lithium, the
SUD treatment provider may assist in medication
monitoring by asking such questions as, “How are
your meds helping you? Are you remembering
to take them? Are you having any problems
with them? Do you need to check in with the
prescribing doctor?”
Chapter 5 149

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
Psychiatric Medications
Providers should ask clients with CODs to bring in
all medications to counseling sessions. Providers
can then ask clients in what manner, when, and
how they are taking medications. They can also ask
whether clients feel that the medication is helping
them, and how. Doing so presents an opportunity
for providers and their clients to review and discuss
attitudes toward medication and clients’ typical
patterns in taking medication. Some clients may
not disclose that they have discontinued their
medications, but when asked to bring in their
medications, they may bring medication bottles
that are completely full. Providers should help
educate clients about the effects of medication,
teach clients to monitor themselves (if possible),
and consult with clients’ physicians whenever
appropriate.
ADVICE TO THE COUNSELOR:
MONITORING PSYCHIATRIC
SYMPTOMS
The consensus panel recommends these
approaches to monitoring psychiatric symptoms
in clients with CODs:
• Obtain a mental status examination to
evaluate clients’ overall mental health and
danger profile. Ask about clients’ symptoms
and use of medication and look for signs of
mental disorders regularly.
• Keep track of changes in symptoms.
• Ask clients directly and regularly about the
extent of their depression and associated
suicidal thoughts.
Status of Psychiatric Symptoms
SUD counselors should monitor changes in severity
and number of psychiatric symptoms over time. For
example, most clients present for SUD treatment
with anxiety or depressive symptoms. Such
symptoms are substance induced (see Chapter
4) if they occur within 30 days of intoxication or
withdrawal.
Substance-induced symptoms tend to follow the
principle of “what goes up, must come down,”
and vice versa. Clients who have just ended a
binge on stimulants will seem tired and depressed
(clients using methamphetamines may present
with psychotic symptoms that require medication).
Conversely, those who recently stopped taking
depressants (e.g., alcohol, opioids) will likely seem
agitated and anxious. These substance-induced
symptoms result from substance withdrawal and
usually persist for days or weeks. Substance-related
depression may follow (which can be seen as a
neurotransmitter depletion state) and may begin to
improve within a few weeks. If depressive or other
symptoms persist, then a co-occurring (additional)
mental disorder is likely, and a differential
diagnostic process should ensue. Such symptoms
may be appropriate targets for establishing a
diagnosis or determining treatment choices.
SUD treatment providers can use various tools
to help monitor psychiatric symptoms. Some
tools consist only of questions and require no
formal instrument. For example, to gauge the
status of depression quickly, providers can ask a
client: “On a scale of 0 to 10, with 0 being your
best day and 10 your worst, how depressed are
you?” This simple scale, used from session to
session, can provide much useful information. SUD
treatment providers should also monitor adherence
to prescribed medication by asking clients
regularly for information about their use of these
medications and their effects.
To identify changes, providers should track psychiatric
symptoms clients mention at the outset of treatment
from week to week. For example, one may ask, “Last
week you mentioned low appetite, sleeplessness,
and feeling hopeless—are these symptoms better or
worse now?” Providers should also ascertain whether
clients follow their suggestions to alleviate symptoms,
and if so, with what result.
Chapter 3 and Appendix C also address screening
and assessment tools for mental disorders and SUDs.
Potential for Harm to Self or Others
According to the Centers for Disease Control
and Prevention (2018), 46 percent of people
who die by suicide have a known mental health
issue; 28 percent have problematic substance
150 Chapter 5

TIP 42
Chapter 5—Strategies for Working With People Who Have Co-Occurring Disorders
use. Individuals with CODs are at increased risk of
self-harm (e.g., cutting, suicide attempt) or harm
to others compared with people who do not have
CODs (Carra et al., 2014; Haviland, Banta, Sonne,
& Przekop, 2016; Tiet & Schutte, 2012).
Providers should always ask explicitly about
suicide or the intention to harm someone else
when client assessment indicates that either is
an issue. For clients who mention or seem to be
experiencing depression or sadness, explore the
extent to which suicidal thinking is present. (To
learn about duty to warn laws in each state, see
“Resource Alert: Federal and State Mental Health
Privacy and Confidentiality Regulations” in the
previous section of this chapter.)
Follow-up services for clients who screen positive
for suicide risk or have tried to commit suicide
or other self-injurious behaviors may effectively
prevent future harmful behaviors (including
completed suicides), but more research in this
area is needed (Brown & Green, 2014). Follow-up
services can include:
•
Conducting a full suicide risk assessment (see
Chapter 3).
•
Contacting the client (e.g., sending letters or
postcards) to express care and concern.
•
Scheduling follow-up appointments in person or
by phone to discuss the treatment plan.
•
Making home visits (as appropriate).
•
Administering follow-up psychiatric and suicide
risk assessments throughout the course of care.
Chapter 4 covers general approaches to prevent-
ing suicide and managing clients who have tried
to commit suicide or are at risk for self-harm.
Instructions on screening for risk of harm to self or
others appear in Chapter 3 and Appendix C.
Use Supportive and Empathic Counseling
A supportive and empathic counseling style
is one of the keys to establishing an effective
therapeutic alliance with clients who have CODs.
According to Lockwood, empathy is “the ability
to vicariously experience and to understand the
affect of other people”; it is the foundation adults
use for relating to and interacting with other adults
(Lockwood, 2016, p. 256).
ADVICE TO THE COUNSELOR:
USING AN EMPATHIC STYLE
Empathy is a key skill for the SUD counselor,
without which little could be accomplished. Bell
(2018, p. 111) notes that “it is the job of counselor
educators and supervisors to instill and nourish
the trait of empathy, while building skills that
relay empathy to the client.” An empathic style is
one that:
• Involves taking the client’s perspective and
trying to see life from his or her worldview.
• Tries to connect with clients who are difficult
or are engaging in behaviors the counselor
disagrees with or cannot otherwise relate to
(e.g., misusing substances, breaking the law).
• Is mindful, compassionate, and warm rather
than judgmental and accusatory.
• Is focused on listening to—rather than talking
at—the client.
• Includes nonverbal communication (e.g., open
body positioning, direct eye contact, nodding
along).
• Conveys reflective listening via techniques like
repetition and parroting, using verbal cues
like “I see” or “Tell me more about that,” and
paraphrasing content and feelings (“So, you’re
saying that he left, and then you decided to go
to the bar. Do I have that right?” or “I hear that
you were extremely angry about that”).
• Demonstrates comfort by expressing sympathy,
consolation, and reflexive reassurance (i.e.,
phrasing designed to alleviate anxiety and
worry without promising a certain outcome—
such as saying, “Just give it your best shot, and
let’s see how things play out” instead of saying,
“Everything will be just fine”).
See also Treatment Improvement Protocol (TIP)
35, Enhancing Motivation for Change in Substance
Use Disorder Treatment (SAMHSA, 2019c).
Sources: Bell (2018); Kelley & Kelley (2013).
Chapter 5 151

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
In empathic counseling, providers model
behaviors that can help clients build more pro-
ductive relationships. Providers’ empathy helps
clients begin to recognize and own their feelings,
which is an essential step toward managing them.
In learning to recognize and manage their own
feelings, clients will also learn to empathize with
the feelings of others.
Empathic counseling must be consistent over
time to keep the alliance intact, especially for
clients with CODs. Clients with CODs often have
lower motivation to address mental illness or
substance misuse, find it harder to understand
and relate to others, and need strong support and
understanding to make major lifestyle changes
such as adopting abstinence. Support and empathy
from providers can help maintain the therapeutic
alliance, increase client motivation, and assist with
medication adherence.
Confrontation and Empathy
Historically, addiction research defined
confrontation as an aggressive, argumentative
communication tactic to pressure people who
misused substances into treatment. Confrontation
has more recently come to be seen as a supportive,
honest approach to warning or advising at-risk
individuals about harmful behaviors (Polcin,
Galloway, Bond, Korcha, & Greenfield, 2010;
Polcin, Mulia, & Laura, 2012).
SUD treatment providers often feel tension
between offering clients empathic support and
addressing clients’ potential minimization, evasion,
dishonesty, and denial. However, providers can be
empathic and firm at once. Straightforward, factual
presentation of conflicting material or problematic
behavior in an inquisitive, caring manner can
be confrontational yet supportive. Achieving a
balance of empathy and firmness is critical for
providers to maintain therapeutic alliances with
clients who have CODs.
Structure and Support
Clients with CODs benefit from a careful balance
of structured versus free time. Free time is
both a trigger for substance use cravings and a
negative influence for many individuals with mental
disorders. Thus, management of free time is of
particular concern for clients with CODs. Clients
with CODs need strategies to better manage
their free time, such as by structuring one’s day to
include meaningful activities and to avoid activities
that are risky. Providers can help clients plan their
free time (especially weekends) to introduce new
pleasurable activities that may alleviate symptoms
and offer satisfaction through means other than
substance use. Other activities that can help
structure clients’ time are working on vocational
and relationship matters in treatment.
In addition to structure, clients’ daily activities
need to have opportunities for receiving support
and encouragement. Counselors should work
with clients to create a healthy support system of
friends, family, and activities.
Mutual support is a key tool providers can
introduce to clients with CODs. Dual recovery
mutual supports are increasingly available in most
large communities. Providers play an important
role in helping clients with CODs access and
benefit from such resources. (Chapter 7 has more
information on mutual-support approaches for
people with CODs.) If groups for clients who do
not speak English are unavailable locally, providers
can seek resources in nearby communities or, if
the number of clients in need warrants, organize a
group for those who speak the same non-English
language.
A provider can assist a client with CODs in
accessing mutual support by:
•
Helping the client locate an appropriate
group. The provider should be aware of
available local mutual-support programs
and dual recovery mutual-support groups,
especially those that are friendly to clients
with CODs, have other members with CODs,
or are designed specifically for people with
CODs. The provider can gain awareness by
visiting groups to see how they are conducted,
discussing groups with colleagues, updating
personal lists of groups periodically, and
gathering information from clients. The provider
should ensure that the group selected is a
good fit for the client in terms of its members’
ages, genders, and cultural characteristics.
Some communities offer alternatives to
152 Chapter 5
TIP 42
Chapter 5—Strategies for Working With People Who Have Co-Occurring Disorders
CASE STUDY: HELPING A CLIENT FIND A SPONSOR
Linda, a 24-year-old woman, had attended her mutual-support group for about 3 months. Although she
knew she should ask someone to sponsor her, she was shy and afraid of rejection. She had identified a few
women who might be good sponsors, but each week in counseling, she stated that she was afraid to reach
out. No one had approached her about sponsorship either, although the group members seemed “friendly
enough.” The counselor suggested that Linda share, in the next group meeting, that she’d like a sponsor
but has been feeling shy and hadn’t wanted to be rejected. The counselor and Linda role-played this act
of sharing during a counseling session. The counselor reminded Linda that it was okay to feel afraid and
reassured her that, if she couldn’t share at the next meeting, they would talk about what had stopped her.
After the next meeting, Linda related that she almost shared but got scared at the last minute. She felt bad
that she had missed an opportunity. She and the counselor talked about getting it over with, and Linda
resolved to reach out, starting her sharing statement with, “It’s hard for me to talk in public, but I want to
work this program, so I’m telling you all that I know it’s time to get a sponsor.” This counseling work helped
Linda convey her need to the group. The response from group members was helpful to Linda, as several
women offered to meet with her and talk about sponsorship. This experience also helped Linda become more
attached to the group and learn a new skill for seeking help. Although Linda was helped through counseling
strategies alone, others who are anxious in social settings may need medications in addition to counseling.
mutual-support groups, such as Secular
Organizations for Sobriety.
•
Helping the client prepare to participate
appropriately in the group. Some clients,
particularly those with SMI or anxiety about
group participation, benefit when providers
offer an explanation of the group process in
advance. The provider should inform the client
of the structure of a meeting, expectations
of sharing, and how to participate. The client
may need to rehearse the kinds of things that
are and are not appropriate to share at such
meetings. The provider should also teach the
client how to politely decline to participate and
when this would be appropriate. The counselor
should be familiar enough with group function
and dynamics to walk the client through the
meeting process before attending.
•
Helping overcome barriers to group
participation. The provider should be aware
of the genuine difficulties the client may have
in connecting with a group. Although clients
with CODs, like any clients, may have some
ambivalence about change, they also may have
legitimate barriers they cannot remove on
their own. For example, a client with cognitive
difficulties may need help working out how
he or she can physically get to the meeting.
The provider may need to write down detailed
instructions for this client that another would
not need (e.g., “Catch the number 9 bus on
the other side of the street from the treatment
center, get off at Main Street, and walk 3 blocks
to the left to the white church. Walk in at the
basement entrance and go to Room 5.”)
•
Debriefing the client after he or she has
attended a mutual-support group to help
process reactions and prepare for future
attendance. The provider’s work does not end
with referral to a mutual-support group. The
provider must be prepared to help the client
overcome any obstacles after attending the
first group to ensure engagement. Often, this
involves a discussion of the client’s reaction to
the group and a clarification of how he or she
can participate in future groups.
Use Culturally Appropriate Methods
Research is lacking on the ethnic/racial diversity of
populations with CODs. Limited published studies
suggest that although CODs are more frequently
observed among Whites, non-White Americans
also experience CODs. A report (Mericle, Ta Park,
Holck, & Arria, 2012) estimated lifetime prevalence
of CODs at 5.8 percent among Latinos, 5.4 percent
among African Americans, and 2.1 percent among
Asians. Whites, by comparison, had a lifetime
prevalence of 8.2 percent.
Chapter 5 153

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
Notable gaps exist in the rates of behavioral health
service access, utilization, and completion among
diverse racial and ethnic groups compared with
Whites (Cook, Trinh, Li, Hou, & Progovac, 2017;
Holden et al., 2014; Maura & Weisman de Mamani,
2017; Nam, Matejkowski, & Lee, 2017; Saloner & Le
Cook, 2013; Sanchez, Ybarra, Chapa, & Martinez,
2016). This is attributable to multiple factors such as
underassessment, underdiagnosis, and underreferral
(Priester et al., 2016) as well as cultural barriers like
language differences, fear of stigma, and shame
(Holden et al., 2014; Keen, Whitehead, Clifford,
Rose, & Latimer, 2014; Masson et al., 2013; Maura
& Weisman de Mamani, 2017; Pinedo, Zemore,
& Rogers, 2018). Culturally responsive care and
cultural competence training among behavioral
health staff are needed to help break down barriers
to service access and improve treatment outcomes
for diverse populations with CODs.
Understanding Clients’ Cultural Backgrounds
Population shifts are resulting in increasing
numbers of diverse racial and ethnic groups in
the United States (Colby & Ortman, 2014). Each
geographic area has its own cultural mix. To
provide effective COD treatment to people of
various cultural groups, providers should learn
as much as possible about characteristics of their
clients’ cultural groups.
Of particular importance are culturally based
conventions of social interaction, styles of
interpersonal communication, concepts of healing,
views of mental illness, and perceptions of
substance use. For example, some cultures may
tend to somaticize symptoms of mental disorders,
and clients from such groups may expect treatment
providers to offer relief for physical complaints.
These clients may be offended by too many
probing, personal questions early in treatment and
never return.
Similarly, COD treatment providers need to
understand culturally based concepts of and ex-
pectations surrounding families. Providers should
learn each client’s role in the family and its cultural
significance (e.g., expectations of the oldest son, a
daughter’s responsibilities to her parents, the role
of a grandmother as matriarch).
Providers should not make assumptions about
clients based on their perception of the clients’
culture. An individual client’s level of acculturation
and specific experiences may result in that person
identifying with the dominant culture or other
cultures. For example, a person from India adopted
by African American parents at an early age may
know little about the cultural practices in his birth
country. A provider working with this client would
need to acknowledge the birth country and explore
the client’s associations with it as well as what
those associations might mean. The client’s country
of origin may have little influence on his cultural
beliefs or practices.
Chapter 6 of this TIP further discusses culture-re-
lated topics in COD treatment, including how
counselors can reduce racial/ethnic disparities
and use culturally adapted services. For more
information about cultural competence in general
behavioral health services, see TIP 59, Improving
Cultural Competence (SAMHSA, 2014a), which
is available free of charge online (https://store.
samhsa.gov/system/files/sma14-4849.pdf).
Using Motivational Enhancement
Consistent With Clients’ Specic Stage
of Change
Motivational interviewing (MI) is a client-
centered approach that enhances clients’
internal motivation to change by exploring and
resolving ambivalence (Miller & Rollnick, 2013).
MI involves accepting a client’s level of motivation,
whatever it is, as the only possible starting point
for change. For example, if a client says she has no
interest in changing the amount or frequency of
her drinking, but is interested in complying with an
SUD assessment to be eligible for something else
(such as the right to return to work or a housing
voucher), the SUD treatment provider would
avoid arguing with or confronting her. Instead, the
provider would focus on establishing a positive
rapport with the client—even remarking on the
positive aspects of the client’s desire to return to
work or take care of herself by obtaining housing.
The provider would work with available openings
to probe the areas in which the client does have
motivation to change in hopes of eventually
affecting the client’s drinking or drug use.
154 Chapter 5

TIP 42
Chapter 5—Strategies for Working With People Who Have Co-Occurring Disorders
For an indepth discussion of MI and how to apply
its principles to stages of change in clients with
SUD, see TIP 35, Enhancing Motivation for Change
in Substance Use Disorder Treatment (SAMHSA,
2019c).
Guiding Processes of MI
Four overlapping processes guide the practice of
MI (Miller & Rollnick, 2013).
1. Engaging: The counselor uses strategies to
establish rapport and help build a trustful
relationship with the client. Techniques include
asking open- rather than close-ended questions,
using reflective listening, summarizing
statements from the client, and determining his
or her readiness to change.
2. Focusing: The counselor helps direct the
conversation and process as a whole through
agenda setting and identifying a target behavior
of change.
3. Evoking: The counselor helps clients express
their motivations or reasons for change. Use of
change talk (expressing a desire to change) is
core to this process and helps clients recognize
how their substance use is affecting their lives.
It helps clients recognize and respond to sustain
talk (expressing a desire not to change), which
creates ambivalence and should be minimized.
Use of open-ended questions and reflective
listening by the counselor will facilitate this
process.
4. Planning: The counselor collaborates with the
client to develop a plan for change. The plan is
critical for putting ideas about and reasons for
change into action. The counselor works with
clients to identify a specific change goal (like
reducing the number of drinks per day), explore
possible strategies that will lead to the change,
create steps to make the change, and problem-
solve possible obstacles to achieving lasting
behavior change.
The details of these strategies and techniques
are presented in TIP 35, Enhancing Motivation
for Change in Substance Use Disorder Treatment
(SAMHSA, 2019c) and in Miller and Rollnick’s
manual, Motivational Interviewing: Helping People
Change (2013).
Matching Motivational Strategies to Clients’
Stage of Change
The motivational strategies providers use should
be consistent with their clients’ stage of change
(i.e., precontemplation, contemplation, preparation,
action, maintenance, termination). A client with
CODs could be at one stage of recovery or change
for his or her mental disorder and another for his or
her SUD, which can complicate selection of strat-
egies. Furthermore, a client may be at one stage
of change for one substance and another stage
of change for another substance. For example, a
client who has combined alcohol and cocaine use
disorders with co-occurring panic disorder may
be in the contemplation stage (i.e., aware that a
problem exists and considering overcoming it, but
not committed to taking action) in regard to alcohol
use, precontemplation (i.e., unaware that a problem
exists, with no intention of changing behavior) in
regard to cocaine use, and action (i.e., actively
modifying behavior, experiences, or environment to
overcome the problem) for the panic disorder.
Evaluating clients’ motivational state is an
ongoing process. Court mandates, rules for clients
engaged in group therapy, the treatment agency’s
operating restrictions, and other factors may act as
barriers to implementing specific MI strategies in
particular situations.
MI and CODs
MI has been shown to be effective or effica-
cious in improving behavior change—such
as treatment engagement, attendance, and
resistance—as well as enhancing motivation and
confidence in people with mental or substance
misuse problems, including comorbid conditions
(Baker, Thornton, Hiles, Hides, & Lubman, 2012;
Keeley et al., 2016; Laakso, 2012; Romano &
Peters, 2015). MI also appears to be effective in
helping clients with SUD reduce substance misuse
and associated behaviors and consequences
(DiClemente, Corno, Graydon, Wiprovnick, &
Knoblach, 2017). For instance, a review of studies
on COD interventions for people involved in the
criminal justice system found MI helpful in reducing
self-reported substance misuse (Perry et al., 2015).
In a sample of people with PTSD seeking SUD
treatment (Coffey et al., 2016), trauma-focused
motivational enhancement therapy was associated
Chapter 5 155

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
with significantly greater reductions in PTSD
symptoms versus a control condition (12 sessions
of healthy lifestyle education). At 6 months after
treatment, just 6 percent of participants in the
motivational enhancement therapy group had a
positive urine drug screen for at least one illicit
substance, compared with almost 13 percent in the
healthy lifestyle control group.
Motivational strategies may be helpful with
people who have SMI, but more research
is needed. A 3-week MI intervention yielded
improvements in medication adherence, self-ef-
ficacy, and motivation to change among clients
receiving outpatient treatment for bipolar disorder
(McKenzie & Chang, 2015). Results concerning MI
and improved adherence to pharmacotherapy for
clients with schizophrenia are generally negative,
but some research suggests that MI reduces
psychotic symptoms and hospitalization rates
(Vanderwaal, 2015). A meta-analysis of MI plus
cognitive–behavioral therapy (CBT) as an adjunct to
or replacement for treatment as usual for co-occur-
ring AUD and depression (Riper et al., 2014) found
small but positive effects in decreasing alcohol
consumption and improving depressive symptoms.
Although more research is warranted, it appears
that MI strategies may be applied successfully to
the treatment of clients with CODs, especially in:
•
Assessing clients’ perceptions of their problems.
•
Exploring clients’ understanding of their disorders.
•
Examining clients’ desire for continued treatment.
•
Ensuring client attendance at initial sessions.
•
Expanding clients’ willingness to take
responsibility for change.
Teaching Relapse Prevention Techniques
SAMHSA (2011) considers relapse prevention a
critical component of integrated programming
for effective COD treatment. The long-term
course of comorbid mental illness and addiction is
often marked by (sometimes multiple) instances of
relapse and remission (Luciano, Bryan, et al., 2014;
Xie, Drake, McHugo, Xie, & Mohandas, 2010).
Per the National Institute on Drug Abuse (NIDA),
relapse is “a return to drug use after an attempt
to stop” (NIDA, 2018c). Others define relapse as
“a setback that occurs during the behavior change
In relapse prevention, providers recognize
that lapses (single episodes or brief returns
to substance use) are an expected part of
overcoming SUDs. Lapses do not signal failure or
loss of all treatment progress.
process, such that progress toward the initiation or
maintenance of a behavior change goal (e.g., absti-
nence from drug use) is interrupted by a reversion
to the target behavior” (Hendershot, Witkiewitz,
George, & Marlatt, 2011, p. 2).
A variety of SUD relapse prevention models are
described in the literature (Hendershot et al., 2011;
Melemis, 2015). However, all relapse prevention
approaches include anticipating problems likely to
arise in maintaining change, acknowledging them
as high-risk situations for resumed substance use,
and helping clients develop strategies to cope
with those situations without having a lapse.
To prevent relapse, providers and clients must
understand the types of triggers and cues that
precede it. These warning signs precede exposure
to events, environments, or internal processes
(high-risk situations) where or when resumed
substance use is likely. A lapse may occur in
response to these high-risk situations unless the
client is able to implement effective coping strate-
gies quickly and adequately.
For clients with CODs who require medication
to manage disruptive or disorganizing mental
disorder symptoms, providers must address
lapses in medication regimen adherence. In these
cases, a “lapse” is defined as not taking prescribed
medication. This type of lapse is different from
lapses that involve returns to substance misuse for
self-medication or pleasure seeking.
Counseling for relapse prevention can occur
individually or in small groups, and may include
practice or role-play to help clients learn how
to cope effectively with high-risk situations.
Relapse prevention approaches have many common
elements (Daley & Marlatt, 1992) that highlight the
need for clients to:
1. Have a range of cognitive and behavioral coping
strategies to handle high-risk situations and
relapse warning signs.
156 Chapter 5

TIP 42
Chapter 5—Strategies for Working With People Who Have Co-Occurring Disorders
2. Make lifestyle changes that decrease the need
for alcohol, drugs, or tobacco.
3. Increase healthy activities.
4. Be prepared to interrupt lapses so that they do
not end in full-blown relapse.
5. Resume or continue to practice relapse
prevention skills even when a full-blown relapse
does occur by renewing their commitment to
abstinence rather than giving up the goal of
living a drug-free life.
NIDA (2018) includes relapse prevention therapy
(RPT) in its list of effective SUD treatment
approaches. RPT helps people maintain health
behavior changes by teaching them to anticipate
and cope with relapse. RPT strategies fall into five
categories (Marlatt, 1985):
•
Assessment procedures help clients appreciate
the nature of their problems in objective terms,
to measure motivation for change, and to
identify risk factors that increase the probability
of relapse.
•
Insight/awareness-raising techniques help
clients adjust their beliefs about the behavior
change process (e.g., viewing it as a learning
process). Via self-monitoring, RPT also helps
clients identify patterns of emotion, thought,
and behavior related to SUDs and co-occurring
mental disorders.
•
Coping-skills training strategies teach clients
behavioral and cognitive strategies to avoid
relapse.
•
Cognitive strategies help clients manage urges
and craving, identify early warning signals of
relapse, and reframe reactions to an initial lapse.
•
Lifestyle modifications (e.g., meditation, exercise)
strengthen clients’ overall coping capacity.
The goal of RPT is to teach clients to recognize
increasing relapse risk and to intervene at earlier
points in the relapse process. Thus, RPT fosters
client progress toward maintaining abstinence and
living a life in which lapses occur less often and are
less severe. RPT frames a lapse as a “fork in the
road,” or a crisis. Each lapse has elements of danger
(progression to full-blown relapse) and opportunity
(reduced relapse risk in the future because of the
lessons learned from debriefing the lapse).
RPT encourages clients to create a balanced
lifestyle that will help them manage their CODs
more effectively and fulfill their needs without
using substances to cope with life’s demands and
opportunities. In delivering RPT, providers can:
•
Explore with clients the positive and negative
consequences of continued substance use
(“decisional balance,” as discussed in the
motivational interviewing section of this
chapter).
•
Help clients recognize high-risk situations for
returning to substance use.
•
Teach clients skills to avoid high-risk situations or
cope effectively with them.
•
Develop a relapse emergency plan for damage
control to limit lapse duration/severity.
•
Support clients in learning how to identify and
cope with substance-related urges and cravings.
Empirical Evidence Supporting Use of RPT in
COD Treatment
Much of the empirical literature on RPT addresses
its application in SUD treatment. In this context,
RPT has demonstrated strong and consistent
efficacy versus no treatment and similar efficacy to
other active treatments on outcomes like reduced
relapse risk and severity, increased treatment gains,
and greater use of treatment matching (Bowen
et al., 2014; Hendershot et al., 2011). Research
also supports RPT for enhancing substance use
outcomes among people with CODs.
In treating people with bipolar disorder and AUD
(Farren, Hill, & Weiss, 2012), integrated group
therapy focused on relapse prevention strategies
was associated with greater abstinence, fewer days
of substance misuse, and fewer days of alcohol use
to intoxication than controls/treatment as usual.
RPT with prolonged exposure therapy is linked
to marked improvement in client- and provider-
reported SUD and PTSD symptom severity and
past-week substance use (Ruglass et al., 2017).
RPT Adaptations for Clients With CODs
RPT adaptations for clients with CODs should
address their full range of symptoms and
circumstances. Adapted RPT should support
adherence to treatment (including medication
Chapter 5 157

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
adherence—particularly critical for people with
psychotic or bipolar disorders), improve social func-
tioning, and help clients meet basic living needs
(e.g., finding housing, gaining stable employment).
The aspects of RPT most useful for improving
recovery from CODs (Subodh, Sharma, & Shah,
2018; Weiss & Connery, 2011) include:
•
Encouraging abstinence.
•
Promoting adherence to mood-stabilizing
medication.
•
Supporting habits associated with stable mood,
like good sleep hygiene.
•
Promoting recovery by teaching clients
strategies for:
- Avoiding, recognizing, and responding
to high-risk situations that are likely to
exacerbate substance- or mood-related
symptoms and problems.
- Using substance-refusal skills.
•
Addressing multiple areas of functioning,
including interpersonal functioning.
•
Using family-focused interventions, especially
for clients who have demonstrated difficulty with
adhering to treatment/medication or who have
problems with cognition or insight.
•
Facilitating engagement in mutual-support
groups.
In a small qualitative analysis of men with CODs
(Luciano, Bryan, et al., 2014), client-reported
relapse prevention strategies deemed helpful for
maintaining at least 1 year of sobriety included:
•
Building a supportive community, including
peers in treatment.
•
Establishing a meaningful daily routine (e.g.,
going to work, attending school, exercising).
•
Adopting a healthy mindset that helped
individuals stay mindful of cravings and
other symptoms, develop insight about the
relationship between substance use and mental
illness, and maintain a sense of responsibility
(to themselves and to others) to live a life of
recovery.
RPT-based SUD interventions with integrated
components to address PTSD are supported by
a growing number of studies, reflecting the field’s
recognition that trauma commonly co-occurs with
addiction (Swopes, Davis, & Scholl, 2017; Vrana,
Killeen, Brant, Mastrogiovanni, & Baker, 2017;
Vujanovic, Smith, Green, Lane, & Schmitz, 2018). In
just one example of trauma-informed RPT adapta-
tions to address CODs, Vallejo and Amaro (2009)
adapted a mindfulness-based stress reduction
program for relapse prevention among women
with SUDs and trauma/PTSD to better address
trauma sensitivity and risk of relapse. Modifications
included:
•
Centrally focusing on stress management as a
key skill in preventing relapse.
•
Using shorter and more structured sessions.
•
Altering body scan activities during mindfulness
exercises to reduce anxiety and promote
feelings of safety (e.g., having participants
perform body scans with eyes open rather than
ADVICE TO THE COUNSELOR: USING RELAPSE PREVENTION METHODS IN
COD TREATMENT
The consensus panel recommends using the following relapse prevention methods with clients who have
CODs:
• Provide relapse prevention education on both mental disorders and SUDs and their interrelations.
• Teach clients skills to resist pressure to stop psychotropic medication and to increase medication adherence.
• Encourage attendance at dual recovery groups and teach social skills necessary for participation.
• Use daily inventory to monitor psychiatric symptoms and symptom changes.
If relapse occurs, use it as a learning experience to investigate triggers with the client. Reframe the
relapse as an opportunity for self-knowledge and a step toward ultimate success.
158 Chapter 5

TIP 42
Chapter 5—Strategies for Working With People Who Have Co-Occurring Disorders
closed; avoiding a detailed focus on scanning
parts of the body that could be triggering or
retraumatizing, like the pelvic area).
•
Using a more flexible curriculum that emphasized
early identification of warning signs of relapse.
•
Having counselors available to work with clients
on uncomfortable feelings that arose in sessions.
•
PTSD-related adaptations may be particularly
important when providing RPT for women, in
whom trauma-related symptoms have been
shown to predict returns to substance use
(Heffner, Blom, & Anthenelli, 2011).
Integrated Treatment
RPT and other CBT approaches to mental health
counseling and SUD treatment allow providers to
treat CODs in an integrated way by:
1. Conducting a detailed functional analysis of the
relationships between substance use, mental
disorder symptoms, and any reported criminal
conduct.
2. Evaluating unique and common high-risk factors for
each problem and gauging how they interrelate.
3. Assessing cognitive and behavioral coping skills
deficits.
4. Implementing cognitive and behavioral coping
skills training tailored to the specific needs
of each client with respect to substance use,
symptoms of mental disorder, and criminal
conduct.
Chapter 7 further discusses integrated treatments
and their outcomes for clients with CODs.
Use Repetition and Skill Building To
Address Decits in Functioning
In applying the approaches described previously,
providers should keep in mind that clients
with CODs often have cognitive limitations,
including difficulty concentrating. Sometimes,
these limitations are transient and improve during
the first several weeks of treatment. Other times,
symptoms persist for long periods. In some
cases, individuals with specific disorders (e.g.,
schizophrenia, attention deficit hyperactivity
disorder) may manifest these symptoms as part of
their disorder.
General treatment strategies to address cognitive
limitations in clients with CODs include:
•
Being more concrete and less abstract in
communicating ideas.
•
Using simpler concepts.
•
Having briefer discussions.
•
Repeating core concepts many times.
•
Presenting information in multiple formats
(verbally; visually; affectively through stories,
music, and experiential activities).
•
Using role-playing to practice real-life situations
with clients who have cognitive limitations (e.g.,
having a client practice “asking for help” by
phone using a prepared script individually with
the counselor, or in a group to obtain feedback
from the members).
Compared with individuals who have no ad-
ditional disorders or disabilities, people with
CODs and additional deficits require more SUD
treatment to attain and maintain abstinence.
Abstinence requires clients to develop and use a
set of SUD recovery skills. Clients with co-occurring
mental disorders face additional challenges that
require learning yet more diverse skills. They also
may require more support that provides treatment
in smaller steps with more practice, rehearsal, and
repetition. The challenge is not to provide more
intensive or complicated treatment for clients
CASE STUDY: USING REPETITION
AND SKILL BUILDING WITH A
CLIENT WHO HAS CODs
In individual counseling sessions with Susan, a
34-year-old White woman with bipolar disorder
and AUD, the counselor observes that she
frequently forgets details of her recent past,
including discussions and decisions made in
recent counseling sessions. Conclusions the
counselor thought were clear in one session
seem fuzzy by the next. The counselor adjusts
course, starting sessions with a brief review of the
last session. The counselor allows time at the end
of each session for a review. Susan has difficulty
remembering appointment times and other
responsibilities, so the counselor also helps her
devise a system of reminders.
Chapter 5 159

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
with CODs, but rather to tailor the skill acquisi-
tion process to the needs and abilities of each
client.
Guidance for Working With
Clients Who Have Specic
Co-Occurring Mental Disorders
Clients with certain mental disorders may have
specific treatment needs and do best with particular
counseling approaches tailored to their diagnosis
and levels of functioning. This is especially true for
mental disorders known to be highly disabling,
distressing, longstanding, or difficult to treat—such
as depression, anxiety, PTSD, and SMI. These
mental disorders are also the most likely to co-occur
with substance misuse. This section of Chapter 5
offers guidance for SUD treatment, mental health
service, and other providers on how best to deliver
SUD treatment and build rapport with clients who
have these disorders. Chapter 4 covers diagnosis
and management of the specific mental disorders
discussed.
MDD
Depression commonly co-occurs with SUDs (Lai et
al., 2015), and each can exacerbate the other. To
optimize treatment outcomes, counselors working
with clients who have an SUD and MDD should:
•
Use integrated CBT treatment approaches.
Review studies and meta-analyses confirm
CBT’s effectiveness in improving symptoms and
decreasing substance misuse among people
with depression and SUDs, particularly when
integrated with additional treatment strategies
such as RPT or MI (Baker et al., 2012; Riper et
al., 2014; Vujanovic et al., 2017). CBT treatment
elements most helpful for clients with depression
and SUDs include (Vujanovic et al., 2017):
- Functional analysis of situations in which
substance use is likely to occur and of
situations associated with depressive
symptoms.
- Cognitive training to identify and reframe
maladaptive thoughts associated with
increased substance use as well as with
negative mood.
- Behavioral skills to address craving, coping
with stressful situations, and improving mood.
•
Incorporate behavioral activation (BA)
techniques into CBT treatment. BA techniques
are often used in CBT to help clients improve
their mood by reengaging in pleasant and
rewarding behaviors. BA supports clients in
identifying rewarding activities and goals,
barriers to engaging in those activities (e.g.,
avoidance triggers), and solutions for reducing
avoidance. Research on BA for depression
and SUDs is still growing, but early evidence
suggests that CBT with BA is feasible and
efficacious in reducing negative mood,
increasing activation of pleasant behaviors,
and improving treatment retention (Daughters,
Magidson, Lejuez, & Chen, 2016; Martínez-
Vispo, Martínez, López-Durán, Fernández del
Río, & Becoña, 2018; Vujanovic et al., 2017).
•
Remain vigilant for double depression.
Not all clients with depression and SUDs will
meet criteria for MDD, but they may still have
distressing, impairing depressive symptoms that
would benefit from treatment. Counselors need
to look for clients with “double depression,” or
the occurrence of persistent depressive disorder
and intermittent major depressive episodes. In
a sample of clients seeking SUD treatment, 14
percent had double depression (Diaz, Horton,
& Weiner, 2012) and reported higher levels of
alcohol dependence and lower quality of life than
participants with dysthymia only or MDD only.
•
Perform (or give referrals for) medication
evaluations. Antidepressants can be highly
effective in treating MDD, but not all clients will
need medication. Evaluation by a psychiatrist
can help determine whether pharmacotherapy is
warranted.
•
Be mindful of the unclear temporal
relationship between depression and
substance misuse, as this can affect treatment
planning. Providers may be tempted to
assume that a client is misusing substances to
self-medicate for depression or that a client’s
depression is substance induced. But the
relationship between substance misuse and
depression is multifactorial, with more research
needed to clarify those factors. Although the
160 Chapter 5

TIP 42
Chapter 5—Strategies for Working With People Who Have Co-Occurring Disorders
self-medication hypothesis has some support,
several factors affect the temporal-causal
relationship between depression and substance
misuse, like sociocultural factors (e.g., income-
to-poverty ratio) and demographics (Lo, Cheng,
& de la Rosa, 2015). Counselors should not
make treatment decisions based on assumptions
that alleviating depressive symptoms will reduce
substance misuse or vice versa. CODs tend
to be intertwined in complex ways and often
require multiple trials of various approaches to
treatment.
Anxiety Disorders
Despite high rates of elevated anxiety among SUD
populations, research on the complex relationship
between substance misuse and anxiety is still
developing. The emerging picture suggests that
anxiety can be a risk for substance misuse (such as
through avoidance coping or self-medication) and
that substance use, craving, and withdrawal can
lead to increases in anxiety.
Counselors treating clients for anxiety disorders
and SUDs should be mindful that:
•
Anxiety needs to be assessed early in
treatment. Anxiety is related to more severe
substance dependence and is associated
with higher rates of treatment dropout and
posttreatment relapse (McHugh, 2015; Smith &
Randall, 2012; Vorspan, Mehtelli, Dupuy, Bloch,
& Lépine, 2015). Identifying clients with elevated
anxiety early in SUD treatment could help
providers better address risks for premature
treatment termination or posttreatment relapse.
Screening for elevated anxiety early in treatment
can also identify clients who may require
additional skills to help them manage elevated
distress related to stopping or decreasing their
substance use (e.g., distress associated with
withdrawal, worsening of anxiety symptoms
previously self-managed with drugs or alcohol).
•
The type of anxiety disorder can affect
treatment engagement, participation, and
retention. For instance, individuals with
elevated social anxiety may be reluctant to
speak during group treatment or to share their
social worries with their counselors for fear of
being judged or ridiculed. This can impede
their ability to participate in and benefit from
group or even individual SUD treatments.
Counselors should discuss with anxious clients
their reasons for treatment noncompliance
when relevant. Sometimes, anxious clients have
difficulty adhering to treatment because of their
symptoms or anxiety-related avoidance, not
because of low motivation.
•
Anxiety symptoms can mimic or occur as a
part of withdrawal from substances:
- Anxiety is a commonly reported withdrawal
symptom (Craske & Stein, 2016). When
clients reduce or stop using substances,
their anxiety may increase as a result of
withdrawal.
- Anxiety sensitivity (fear of anxiety-related
sensations) is related to premature treatment
termination (Belleau et al., 2017), in part
because clients with this sensitivity face
additional difficulty tolerating physical
symptoms of withdrawal. People may
misinterpret physical symptoms of withdrawal
(e.g., increased heart rate, sweating, sleep
problems, irritability) as signs of a medical
problem. Anxiety symptoms and anxiety
sensitivity can also evolve into full-blown
anxiety disorders if left untreated, making
clients vulnerable for returns to substance
use.
•
Integrated treatments are highly recommended:
- Given the worse outcomes associated with
treating anxiety and SUDs in isolation,
clients may benefit from an integrated
approach. Given the bidirectional relationship
between the two conditions, addressing
both simultaneously in integrated counseling
can mitigate relapse and provide a holistic
approach to treatment.
- Effective techniques include psychoeducation
about the nature of anxiety (e.g., the
relationship between thoughts, feelings,
and behaviors; normalizing anxiety), CBT
(including anxiety monitoring, thought
restructuring, clarifying cognitive distortions,
exposure therapy, and relaxation training),
medication, motivational enhancement,
mindfulness, and encouraging a healthy
lifestyle (e.g., good sleep hygiene, engaging
in physical activity).
Chapter 5 161

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
PTSD
People with PTSD or histories of trauma are
susceptible to substance misuse, often as a coping
mechanism. People with both PTSD and SUDs
tend to have worse clinical symptoms than people
with either disorder alone, including a higher risk
of suicide (SAMHSA, 2014b). Providers whose
clients have PTSD and SUDs can improve treatment
success if they:
•
Treat disorders concurrently. Integrated,
concurrent treatments are effective; clients may
prefer them over sequential treatment (Banerjee
& Spry, 2017; Flanagan et al., 2016; SAMHSA,
2014b). Additionally, some symptoms of PTSD
may worsen during abstinence. Do not make
the mistake of thinking that treating the SUD
will necessarily alleviate the PTSD. Both must be
treated jointly. In some instances, medication for
PTSD may also be needed.
•
Help clients increase their feelings of safety
at the outset of treatment through techniques
such as grounding exercises, establishing
routines in treatment, discussing safety-
promoting behaviors, and developing a safety
plan to help the client feel confident, prepared,
and in control (SAMHSA, 2014b).
•
Take steps to help prevent retraumatization
of clients. This includes being sensitive to
clients’ triggers (e.g., allowing a client to sit
facing the door instead of with his or her back
to it), sensitively addressing clients acting out
in response to triggering events, listening for
cues that cause reactions and behaviors, and
teaching clients to identify and manage trauma-
related triggers (SAMHSA, 2014b).
•
Adjust the pace, timing, and length of sessions
to the needs of clients. Do not rush clients
into talking about their trauma, and stay alert
for signs of clients feeling overwhelmed by the
intensity or speed of the intervention (SAMHSA,
2014b). Creating safety and enhancing coping
skills to manage traumatic stress reactions are
key aspects of helping clients heal from trauma.
•
Recognize the cyclical relationship between
trauma and substance use. Using substances
places people at greater risk for additional
traumatic events. These traumas increase
risks of substance misuse. Counselors need to
educate clients about this to help safeguard
them from harm.
Chapter 4 provides more information about
trauma-informed care for people with CODs.
SMI
People with SMI and SUDs often have complex
recovery trajectories with drastic shifts in symptoms
and functioning, employment, housing, family life,
social relationships, and physical health. Counselors
working with clients who have SMI and SUDs
should be aware that:
•
Although integrated treatments work for
many clients with SMI and SUDs, this approach
has different levels of success. Integrated
treatment for SMI and SUDs has demonstrated
mixed results in the empirical literature (Chow
et al., 2013; Hunt, Siegfried, Morley, Sitharthan,
& Cleary, 2013). It may help improve psychiatric
symptoms better than nonintegrated treatment
in outpatient and residential settings and may
be better at reducing alcohol consumption, but
not drug use, in residential settings compared
with outpatient settings. However, some
studies have found no significant effects of
integrated versus nonintegrated treatments.
For some clients with SMI and SUDs, parallel
treatment may be preferable and should not be
ruled out as an option after first trying to treat
concurrently.
•
Many SMI symptoms, like psychosis, apathy,
and cognitive dysfunction, can undermine
treatment participation and adherence.
Treatment should address (Horsfall, Cleary,
Hunt, & Walter, 2009):
- Managing positive and negative symptoms of
psychosis.
- Increasing coping skills.
- Improving social skills, including
communication with others.
- Enhancing problem-solving abilities.
- Building distress tolerance.
- Increasing motivation.
- Learning how to set and achieve goals.
- Expanding social support networks (including
peer supports).
162 Chapter 5

TIP 42
Chapter 5—Strategies for Working With People Who Have Co-Occurring Disorders
Given these potential cognitive, social, and
functional challenges, counselors may need to use
sessions that are shorter, more flexible, adapted to
client impairments, and lower in intensity.
•
SMI often requires medication for symptom
stabilization. Counselors should consider
referring clients not currently on medication
or not being followed by a psychiatrist for a
medication evaluation, especially for clients who
are unstable or experiencing positive psychiatric
symptoms (e.g., hallucinations, delusions).
•
Clients may need assistance with basic living
needs. Securing reliable housing and gainful
employment are often among the greatest
stressors people with SMI experience (Horsfall
et al., 2009). Vocational rehabilitation and
housing assistance should be provided as a part
of comprehensive COD care to help increase
the chances of long-term recovery. Certain
clients may also need help from counselors in
connecting with the criminal justice system.
•
Encouraging abstinence may indirectly help
improve psychiatric symptoms. Stopping
substance use can give clients a sense of
accomplishment and self-efficacy that can fuel
their confidence in being able to recover from
their mental illness as well (Green, Yarborough,
et al., 2015).
Conclusion
Therapeutic alliance is a critical component
of counseling essential to clients’ success and
long-term recovery. People with CODs often face
numerous difficulties in managing complex and
fluctuating symptoms as well as the effects of
symptoms on everyday living, including their ability
to function as a productive and healthy member
of society, hold down a job, maintain housing,
and have fulfilling relationships. Experiences of
stigma and feelings of hopelessness can contribute
to clients’ mistrust or low motivation to initiate,
engage in, and complete treatment.
Providers working with people who have CODs
should be aware of basic approaches that can
support the therapeutic relationship and make
interventions more effective. Although there is no
one-size-fits-all approach for treating CODs, the
techniques, skills, and interventions described in
this chapter should help counselors contribute
to the recovery process in a way that is evidence
based, person centered, and maximally beneficial
to clients.
Chapter 5 163
This page intentionally left blank.

Chapter 6—Co-Occurring Disorders Among
Special Populations
KEY MESSAGES
TIP 42
SUBSTANCE USE DISORDER TREATMENT FOR
PEOPLE WITH CO-OCCURRING DISORDERS
• The recovery community is diverse. Assessment,
diagnosis, and treatment of substance use
disorders (SUDs), mental disorders, or both (co-
occurring disorders [CODs]) should be inclusive
of all people who need services.
• People experiencing homelessness, those
involved in the criminal justice system,
women, and people who identify with diverse
racial/ethnic groups have historically been
underserved, often have unique needs and
presenting symptoms, and face certain
barriers to care (and thus to recovery) that
counselors can help address.
• Counselors may need to adapt treatment
approaches to clients with CODs to ensure
the most beneficial outcomes for these
groups. Adaptations are possible across a
wide spectrum, involving basic to increasingly
complex modifications. Regardless of
complexity, all population-specific adaptations
should aim to improve the therapeutic
alliance, increase clients’ engagement in
services, and give people with CODs the best
chances for long-term recovery.
• Ample resources are available to help counselors
tailor SUD treatment and mental health services
to the needs of special populations with CODs.
Some people with CODs are especially vulnerable
to treatment challenges and poor outcomes—
namely, women, people from diverse racial/ethnic
backgrounds, people experiencing homelessness,
and people involved in the criminal justice system.
This chapter describes proven and emerging
COD treatment strategies that can effectively
address substance misuse in these populations
and is intended for counselors, other treatment/
service providers, supervisors, and administrators.
It describes unique aspects of CODs among
specific populations and offers recommendations
to SUD treatment providers, other behavioral
health service providers, program supervisors/
administrators, and primary care providers who
may encounter clients with CODs in their practice.
A complete description of the demographic, socio-
cultural, and other aspects of the noted populations
and related treatment programs and models is
beyond the scope of this Treatment Improvement
Protocol (TIP). However, readers can find more
detailed information about population-specific
behavioral health services in other TIPs, including:
•
TIP 44, Substance Abuse Treatment for Adults
in the Criminal Justice System (Center for
Substance Abuse Treatment, 2005b).
•
TIP 51, Substance Abuse Treatment: Addressing
the Specific Needs of Women (Substance Abuse
and Mental Health Services Administration
[SAMHSA], 2009b).
MILITARY PERSONNEL
Active duty military members and veterans are
a unique, complex population at risk for CODs,
trauma, posttraumatic stress disorder (PTSD),
and suicidal ideation. They often lack access to
sufficient behavioral health services. Providers
will need to make special considerations
regarding military culture (especially surrounding
stigma toward mental illness) and circumstances,
such as deployments and family stress, to provide
behavioral health services that are responsive
to this population’s needs. See the “Trauma”
section in Chapter 4 for more information on
military personnel. Chapter 4 also lists resources
that address some of the specific behavioral
health needs of the military population and how
counselors can best meet those needs.
165

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
•
TIP 55, Behavioral Health Services for People
Who Are Homeless (SAMHSA, 2013).
•
TIP 57, Trauma-Informed Care in Behavioral
Health Services (SAMHSA, 2014b).
•
TIP 59, Improving Cultural Competence
(SAMHSA, 2014a).
People Experiencing Homelessness
Homelessness continues to be one of the United
States’ most intractable and complex social
problems, although homelessness affects only
about 0.2 percent of the U.S. population (Willison,
2017). The Department of Housing and Urban
Development (Henry et al., 2020) reported that
approximately 568,000 people experienced
homelessness in the United States on any given
night in 2019. Moreover, the prevalence of
homelessness is rising. From 2018 to 2019, the
number of individuals experiencing homelessness
rose by 3 percent and the number living in
unsheltered locations increased by 9 percent;
the number experiencing chronic homelessness
increased by 9 percent (Henry et al., 2020).
Among more than 36,000 U.S. adults who
participated in the 2012–2013 Wave 3 of the
National Epidemiologic Survey on Alcohol
and Related Conditions (Tsai, 2018), lifetime
homelessness was about 4 percent and
past-year homelessness was 1.5 percent. Risk of
homelessness was associated with a history of
mental illness (including serious mental illness
[SMI]), lifetime tobacco use, and lifetime suicide
attempt, among other demographic and social
variables (Tsai, 2018).
Homelessness, Mental Health, and
Substance Misuse
The prevalence of substance misuse and mental
illness among people experiencing homelessness
is high. Solari and colleagues (2017) found that
about 37 percent of adults in permanent support-
ive housing programs had a mental disorder; 10
percent, substance abuse; and 29 percent, CODs.
Further statistics paint a similar picture:
•
Stringfellow et al. (2016) reported that 3-month
substance use among individuals experiencing
homelessness was 50 percent for alcohol, 19
percent for cannabis, 16 percent for cocaine,
7.5 percent for opioids, and 6.5 percent
for sedatives. Furthermore, 59 percent of
individuals who took the Alcohol, Smoking,
and Substance Involvement Screening Test had
moderate or high risk for substance misuse.
•
In a study of more than 870,000 veterans with
SMI, 7 percent experienced homelessness
(Hermes & Rosenheck, 2016).
•
Among a sample of women experiencing
homelessness who were seeking treatment in
primary care settings (Upshur, Jenkins, Weinreb,
Gelberg, & Orvek, 2017), self-reported rates
of SUDs or mental disorders greatly exceeded
those in the general population. Specifically,
women reported rates higher than the general
population for:
- SMI (4 times higher).
- Major depressive disorder (MDD; 5 times
higher).
- Alcohol use disorder (AUD; 4 times higher).
- Any drug use disorder (12 times higher).
•
A study of people 50 and older experiencing
homelessness (Spinelli et al., 2017) found that:
- 38 percent had current symptoms of MDD.
- 33 percent had current symptoms of PTSD.
- 19 percent had at least one lifetime
hospitalization for psychiatric symptoms.
- 33 percent reported experiencing childhood
physical abuse, and 13 percent experienced
childhood sexual abuse.
- 63 percent had used an illicit substance in the
previous 6 months; the most commonly used
illicit substances were cannabis (48 percent),
cocaine (38 percent), opioids (7 percent), and
amphetamines (7 percent).
- 49 percent drank alcohol in the past 6
months, including 26 percent whose alcohol
use was of moderate or greater severity and
15 percent whose use was of high severity.
- 10 percent reported binge drinking.
166 Chapter 6

TIP 42
Chapter 6—Co-Occurring Disorders Among Special Populations
People experiencing homelessness often have
CODs. In 2010, about 17 percent of adults enrolled
in permanent supportive housing programs had
CODs; this increased to 22 percent in 2014, 25
percent in 2015, and 29 percent in 2016 (Solari
et al., 2016; Solari et al., 2017). Among women
experiencing homelessness and seeking primary
health care, 26 percent reported at least one
mental disorder and one SUD (Upshur et al., 2017).
In a sample of veterans experiencing homeless-
ness, 77 percent had at least one previous mental
disorder diagnosis; 47 percent, a substance-related
diagnosis; and 37 percent, a COD diagnosis (Ding,
Slate, & Yang, 2017).
The Importance of Housing
Housing is more than just physical shelter. It is
a social determinant of health and is essential
for individual physical, emotional, and socioeco-
nomic wellbeing. Housing affects communities,
governments, and nations through its impact on
the economy, healthcare system, workforce, and
more.
Housing for veterans and civilians with mental
disorders, SUDs, or CODs is particularly important.
Homelessness in these populations is associated
with negative treatment-system factors, including
•
Increased emergency department (ED) usage
(Cox, Malte, & Saxon, 2017; Moulin, Evans,
Xing, & Melnikow, 2018).
•
Higher ED costs (Mitchell, Leon, Byrne, Lin, &
Bharel, 2017).
•
Greater usage of inpatient services (Cox et al.,
2017).
•
Higher risk of incarceration/criminal justice
involvement (Cusack & Montgomery, 2017;
Polcin, 2016).
People experiencing homelessness who screened
at highest risk for an SUD had lower scores of
social support and higher scores of psychological
distress compared with those who screened at low
or moderate risk (Stringfellow et al., 2016). Those
with highest SUD risk also reported more difficulty
paying for food, shelter, and utilities; were less
likely to have medical insurance; and experienced
more episodic health conditions.
Service Models for People With CODs
Who Are Experiencing Homelessness
To address substance misuse, mental illness, or
both in clients who lack housing, providers can
choose among several service models, including:
•
Supportive housing—housing combined with
access to services and supports to address the
needs of individuals without housing so that
they may live independently in the community.
This model is an option for individuals and
families who have lived on the street for longer
periods of time or whose needs can best be met
by services accessed through their housing.
•
Linear housing—housing that is contingent on
completion of treatment for SUDs or mental
disorders. Subsidized housing programs
participating in this model typically require
abstinence as a condition of housing, often
through completion of residential treatment.
•
Integrated treatment—receipt of housing
concurrently with addiction/mental health
services.
To help clients with CODs address housing
needs, treatment programs need to establish
ongoing relationships with housing authorities,
landlords, and other housing providers. Groups
and seminars that discuss housing difficulties may
be necessary to help clients with CODs transition
from residential treatment to supportive or inde-
pendent housing. To ease clients’ transition, an
effective strategy COD treatment programs can
use is to coordinate housing tours with supportive
housing programs.
Relapse prevention efforts are essential to help
clients with CODs maintain housing. Substance
misuse may disqualify clients from public housing in
the community (Curtis, Garlington, & Schottenfield,
2013).
TIP 55, Behavioral Health Services for People
Who Are Homeless (SAMHSA, 2013) offers more
information on treatment and recovery support
approaches specific to people experiencing or at
risk for homelessness.
Chapter 6 167

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
Supportive Housing Model
A systematic literature review (Benston, 2015)
found that permanent supportive housing
programs for people experiencing homelessness
and mental illness often led to better housing
stability (e.g., percentage of participants housed
versus not housed at the end of the study,
proportion of time spent in stable housing versus
experiencing homelessness, number of days
housed versus homeless) compared with control
conditions. Although the studies reported mixed
results because of variations in design, results,
and definitions of “housing,” some, but not all,
found that supportive housing was associated
with improvement in psychiatric symptoms and
reduced substance use.
Similarly, an earlier literature review of treatments
for people with CODs who were experiencing
homelessness recommended use of supportive
housing rather than treatment only or linear
models (Sun, 2012). Another review (Rog et al.,
2014) found that, among people with CODs,
supportive housing was associated with reduced
homelessness and improvements in housing
tenure, less ED use, fewer hospitalizations, and
better client satisfaction (compared with linear
housing models).
Housing First
The Housing First (HF) model provides housing no
matter where a person is in recovery from SUDs
or mental disorders. HF is one of the best-known
and well-researched approaches to supportive
housing. SAMHSA supports the HF model as a
preferred approach for addressing homelessness
in individuals with mental illness, SUDs, or
both, as does the U.S. Interagency Council on
Homelessness (2014). (See “Resource Alert:
Implementing Supportive Housing Programs.”)
HF helps people with CODs (including SMI)
establish stable housing and is associated with
good housing retention rates (Collins, Malone, &
Clifasefi, 2013; Pringle et al., 2017; Watson, Orwat,
Wagner, Shuman, & Tolliver, 2013). In some studies,
HF is associated with better SUD outcomes than
treatment only (Padgett, Stanhope, Henwood,
& Stefancic, 2011). However, research on SUD
outcomes in HF has generally had mixed results
(Paquette & Pannella Winn, 2016). Compared with
linear housing models, Kertesz, Crouch, Milby,
Cusimano, and Schumacher (2009) found that HF
showed better housing stability and retention and,
in some cases, favorable reductions in substance
misuse severity—but both models benefitted
people experiencing homelessness with SMI, SUDs,
or both.
The following examples of supportive housing
models have successfully reduced homelessness
and enhanced outcomes among people with SUDs,
mental disorders, or both.
RESOURCE ALERT: IMPLEMENTING SUPPORTIVE HOUSING PROGRAMS
For guidance on implementation of supportive housing programs, see the following resources:
• The National Alliance to End Homelessness’s toolkit for adopting an HF approach (https://
endhomelessness.org/wp-content/uploads/2009/08/adopting-a-housing-first-approach.pdf)
• Pathways to Housing training and consultation (www.pathwayshousingfirst.org/training)
• SAMHSA’s Permanent Supportive Housing Evidence-Based Practices toolkit (https://store.samhsa.gov/
product/Permanent-Supportive-Housing-Evidence-Based-Practices-EBP-KIT/SMA10-4510)
• United States Interagency Council on Homelessness’s Implementing Housing First in Permanent
Supportive Housing fact sheet (www.usich.gov/resources/uploads/asset_library/Implementing_Housing_
First_in_Permanent_Supportive_Housing.pdf)
168 Chapter 6

TIP 42
Chapter 6—Co-Occurring Disorders Among Special Populations
Pathways to Housing
The well-known and heavily researched Pathways
to Housing program is an example of HF-based
supportive housing. The program was originally
designed (Tsemberis & Eisenberg, 2000;
Tsemberis, Moran, Shinn, Asmussen, & Shern,
2003) to serve a highly visible and vulnerable
segment of New York’s population experiencing
homelessness: people with CODs who were
living in the streets, parks, subway tunnels, and
similar places. It has since been expanded to
other areas, including Washington, DC, Vermont,
Pennsylvania, and Canada. Pathways to Housing
reflects a client-centered perspective and offers
clients experiencing homelessness the option
of moving directly into a furnished apartment of
their own. However, clients must agree to receive
case management and work with a representative
payee to ensure that rent and utilities are paid
and resources are well managed (Tsemberis &
Eisenberg, 2000). Pathways to Housing uses
assertive community treatment (ACT) teams to
offer clients an array of support services in twice-
monthly sessions. Vocational, medical, behavioral
health, and other services are among the options.
Highlights of outcomes reported from Pathways to
Housing programs include the following:
•
Pathways to Housing DC (2017) reported a
91-percent housing success rate.
•
Pathways to Housing PA (2018) supplied 2,992
hours of medical, mental, and SUD treatment
services and 2,996 hours of paid transitional
employment. Additionally, 100 percent of clients
retained housing through the first year, and 65
percent were in SUD treatment after 6 months.
•
Over about 3 years, Pathways to Housing VT
achieved an 85-percent housing retention rate,
and mean number of days spent homeless
decreased significantly over the course of a
year (11 days at baseline vs. 2 days at 12-month
follow-up) (Stefancic et al., 2013).
Linear Housing Model
The linear model provides housing contingent
on abstinence from substances. It was once the
preferred approach for aiding people with SUDs,
mental disorders, or CODs who were experiencing
homelessness. Research has since shown this
approach to produce less favorable housing retention
outcomes than supportive housing (Kertesz et al.,
2009; Polcin, 2016). Linear models often require
completion of an SUD treatment program (typically
residential treatment) in addition to abstinence
before housing is provided, yet SUD treatment
completion rates are frequently low. Often, linear
programs also lack access to and control of stable,
permanent housing, which contributes to low rates
of housing stability compared with permanent
supportive housing programs such as HF (Kertesz et
al., 2009; Polcin, 2016).
Linear programs do appear effective in helping
clients improve substance use outcomes.
Therapeutic communities (TCs), an example of the
linear model, have been shown to reduce substance
use and psychiatric symptoms, but according to some
research, may not produce robust improvements
in housing status (Kertesz et al., 2009). Compared
with usual care (e.g., receiving day treatment only),
the Birmingham approach to the linear housing
model can improve both housing and substance use
outcomes. This approach offers referrals for private
or public housing only upon completion of a compre-
hensive, community-based SUD treatment program
that includes behavioral interventions, employment
training, and community reinforcement and supports
(e.g., relapse prevention, goal setting, rewards for
achieving objectively defined recovery goals). The
Birmingham approach has significantly improved
abstinence, housing stability (especially among clients
THE ROLE OF RECOVERY
HOUSING FOR PEOPLE WITH
CODs
Recovery housing is a critical issue for all
clients with CODs—not just those experiencing
homelessness. Without stable supportive
housing, achieving and maintaining long-term
recovery is less likely. The National Alliance for
Recovery Residences maintains a resource library
on recovery housing to help providers learn
about the various types of recovery residences,
how recovery housing affects client outcomes,
and how to support clients in identifying and
obtaining housing that best meets their recovery
needs (https://narronline.org/resources/).
Chapter 6 169
TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
who achieve longer term abstinence), and employ-
ment; program retention has been moderate to high
(Kertesz et al., 2009).
Integrated Housing and Treatment Models
People experiencing homelessness often have
diverse, complex treatment and support needs.
Thus, a multifactorial, flexible, integrated
approach to addressing clients’ behavioral
health and housing needs may be preferable, in
some cases, to the more structured housing service
models described previously (Polcin, 2016). The
Comprehensive, Continuous, Integrated System of
Care is an integrated COD treatment approach that
has been adapted to include housing and employ-
ment supports. In one program using this approach
(Harrison, Moore, Young, Flink, & Ochshorn, 2008),
homelessness decreased by 90 percent, permanent
housing increased by 202 percent, unemployment
decreased by 16 percent, and employment increased
by 1,215 percent. The program also showed decreases
in number of days of past-month illicit substance use,
and past-month substance use declined over the
course of 6 months. Other significant improvements
included (Moore, Young, Barrett, & Ochshorn, 2009):
•
Decreased need for SUD treatment and
psychological/emotional services.
ADVICE TO THE COUNSELOR:
WORKING WITH CLIENTS
WHO HAVE CODs AND ARE
EXPERIENCING HOMELESSNESS
The consensus panel recommends that providers:
• Address the housing needs of clients.
• Help clients obtain housing.
• Teach clients skills for maintaining housing.
• Collaborate with shelter workers and other
providers of services to people experiencing
homelessness.
• Address real-life concerns in addition to
housing, such as SUD treatment, legal/
criminal justice matters, Supplemental Security
Insurance/entitlement applications, problems
related to children, and health care.
•
Increased receipt of needed SUD treatment and
psychological/emotional services.
•
Reductions in unmet medical needs.
•
Decreased self-reported mental disorder
symptoms.
People Involved in the Criminal
Justice System
Estimated rates of mental disorders and SUDs in
prison populations vary but are consistently high,
often exceeding general population rates (Fazel,
Yoon, & Hayes, 2017; Reingle Gonzalez & Connell,
2014; Marotta, 2017). Among those incarcerated in
U.S. state prisons (Prins, 2014), mental disorders of
highest prevalence include:
•
9 percent to 29 percent for current MDD.
•
5.5 percent to 16 percent for bipolar disorder.
•
1 percent (women), 5.5 percent (men and
women), and 7 percent (men) for panic disorder.
•
2 percent to 6.5 percent for schizophrenia.
In a sample of more than 8,000 U.S. inmates
(Al-Rousan et al., 2017), nearly 48 percent had a
history of mental illness, 29 percent had an SMI,
and 26 percent had an SUD. About 48 percent of
those with a mental illness also misused substances.
People on probation or parole from 2002 to 2014
had significantly higher rates of Diagnostic and
Statistical Manual of Mental Disorders, Fourth
Edition (DSM-IV) SUDs than U.S. adults not on
probation or parole (Fearn et al., 2016); 13 percent
had alcohol abuse (vs. 4 percent), 15 percent had
alcohol dependence (vs. 3 percent), 2 percent had
illicit drug abuse (vs. 0.3 percent), and 8 percent
had illicit drug dependence (vs. 1 percent).
Rationale for Treatment
Inmates with a history of mental illness or CODs
are at higher risk of violence (Peters et al., 2017).
They are more likely to be charged with violent
crimes before incarceration and to experience
or perpetrate prison-related assaults during
incarceration (Wood, 2013).
The rationale for providing SUD treatment
in the criminal justice system is based on the
well-established link between substance misuse
and criminal behavior. The overall goal of SUD
170 Chapter 6

TIP 42
Chapter 6—Co-Occurring Disorders Among Special Populations
Among individuals in the criminal justice system,
comorbid SMI and SUDs substantially increase
the risk of multiple reincarcerations compared
with having either disorder alone (Baillargeon et
al., 2010). However, the odds of incarceration are
reduced when people engage in SUD treatment
(Luciano, Belstock, et al., 2014).
treatment for criminal offenders, especially those
who have engaged in violence, is to reduce
criminality.
Evidence suggests that people with CODs can be
effectively treated while incarcerated (Peters et
al., 2017). Unfortunately, despite the high need for
services, lifetime treatment rates among offenders
with CODs are low: approximately 38 percent have
received any type of previous behavioral health
services; 27 percent, inpatient or outpatient SUD
treatment; 4 percent, inpatient mental health
services; 7 percent, both SUD treatment and
mental health services; and 16 percent, any type of
behavioral health service during the past year (Hunt,
Peters, & Kremling, 2015).
Treatment Features, Approaches, and
Empirical Evidence
Several features distinguish COD treatment
programs currently available in the criminal justice
system from other treatment programs:
•
Staff are trained and experienced in treating
both mental disorders and SUDs.
•
Both disorders are treated as “primary.”
•
Treatment services are integrated if possible.
•
Treatment is comprehensive, flexible, and
individualized.
•
The focus of the treatment is long term.
Treatment frameworks that yield positive results
for incarcerated people with CODs include
integrated dual disorder treatment (IDDT), risk-
need-responsivity (RNR) models, and CBT (Peters
et al., 2017):
•
IDDT models integrate SUD treatment and
mental health services in a single setting;
professionals with training in both sets of
disorders address all symptoms concurrently.
IDDT treatments can be adapted for
incarcerated populations to address criminal
thinking and reduce risk of recidivism.
•
RNR models match service intensity to clients’
risk of recriminalization after release, which
tends to be high in people with CODs. RNR
programs are often highly focused on reducing
substance misuse, which is strongly linked
to reincarceration. Additional recidivism risk
factors addressed through this framework
include reducing antisocial attitudes and beliefs,
addressing family and relationship problems,
enhancing education and employment skills, and
encouraging prosocial activities.
•
CBT can be tailored to offenders with CODs by
addressing antisocial thoughts and maladaptive
behaviors, increasing coping skills to reduce
substance use (e.g., urges, cravings) and
criminal behavior, and cognitive restructuring to
decrease criminal thinking.
These and other COD treatment approaches
can be implemented across a range of criminal
justice settings and services, including as part of
prebooking diversion programs, drug and mental
health courts, reentry programs, and probation
supervision. Many prison- and jail-based treat-
ments for offenders with CODs have generated
positive results for reincarceration (especially for
TCs). Certain interventions, including case manage-
ment via mental health drug courts, motivational
interviewing combined with cognitive training, and
interpersonal psychotherapy, often show no effect
RESOURCE ALERT: SAMHSA
PUBLICATIONS ON SCREENING,
ASSESSMENT, AND TREATMENT
FOR CRIMINAL JUSTICE
POPULATIONS
• TIP 44, Substance Abuse Treatment for Adults
in the Criminal Justice System (https://store.
samhsa.gov/system/files/sma13-4056.pdf)
• SAMHSA’s Screening and Assessment of
Co-Occurring Disorders in the Justice System
(https://store.samhsa.gov/system/files/sma15-
4930.pdf)
Chapter 6 171

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
on criminal activity and drug use—possibly because
of small sample sizes and the low quality of studies
(Perry et al., 2015; Peters et al., 2017). However,
some research does report positive outcomes,
suggesting that COD treatment should not be
dismissed outright. For instance, a COD wraparound
intervention for drug courts resulted in significant
reductions in the average number of nights spent
in jail, alcohol use, and drug use, and increases in
full-time employment (Smelson et al., 2018).
Evidence in Support of Postrelease
Treatment and Follow-Up
In the past decade, several studies have
established the importance of linking institutional
services to community services (of various kinds).
Postrelease programs often include reentry courts,
ACT, and integrated case management services,
all of which should offer comprehensive services
to address mental health, SUDs, and housing and
employment needs.
Forensic adaptations to continuous care for CODs
via ACT can be leveraged to improve criminal
justice–related, substance-related, and functional
outcomes. Integrated, comprehensive approaches
to postrelease treatment and follow-up may help
reduce rearrest and reconvictions when adapted
for criminal justice populations. Adaptations may
include modifications like inclusion of a reentry
plan, transportation to and supervision for
treatment visits, and acquisition/reinstatement of
financial assistance (e.g., Social Security income,
Medicaid; Peters et al., 2017).
Smith, Jennings, and Cimino (2010) used a stage
progressive recovery model of ACT to help
offenders with CODs transition from incarceration
on an inpatient forensic unit to community living.
Participants were provided stage-specific skills and
interventions (e.g., support to improve self-care,
medication management, relapse prevention,
enhanced socialization). Stages of treatments were
tied to behavioral rewards and increased privileges
(such as less supervision) and included assessment
and orientation, a CBT program, a prerelease
stage, and conditional release and community
continuing care programming. Ninety percent
of individuals who completed the program had
“overall success” (e.g., no psychiatric state hospital
readmissions and no rearrests following release), 75
percent maintained substance abstinence, and 82
percent maintained steady housing (i.e., keeping
a consistent home without being evicted, ejected,
or changing residences more than three times
in any year). Interestingly, of the five individuals
who were rearrested following release, all had
maintained substance abstinence, stable housing,
and employment.
Meanwhile, Cusack, Morrissey, Cuddeback, Prins,
and Williams (2010) compared forensic adaptations
of ACT for criminal justice–involved individuals
who had mental illness, SUDs, or CODs with usual
treatment. They found reductions in jail bookings
and psychiatric hospitalizations, increases in the
use of outpatient mental health services, increases
in the odds of staying out of jail after release, and
decreases in inpatient psychiatric service costs and
per-person jail costs.
Women
Women with CODs can be served in mixed-
gender COD programs using the same strategies
mentioned elsewhere in this TIP. However,
specialized COD programs do exist that address
In 2002, the National Institute on Drug Abuse
(NIDA) established the Criminal Justice Drug
Abuse Treatment Studies Series to fund regional
research centers meant to forge partnerships
between SUD treatment providers and the
criminal justice system. The goal is to foster
the design and testing of approaches to better
integrate in-prison treatment and postprison
services. In 2008, NIDA launched the second
wave of studies; these focused specifically on
testing interventions in prison settings, including
provision of medication-assisted treatment (MAT)
and screening and assessment to identify SUDs
and co-occurring health conditions and mental
disorders.
An archive of related studies and publications is
available online (www.icpsr.umich.edu/icpsrweb/
NAHDAP/series/244/studies).
Other NIDA justice system research initiatives
are also available online (www.drugabuse.gov/
researchers/research-resources/criminal-justice-
drug-abuse-treatment-studies-cj-dats).
172 Chapter 6

TIP 42
Chapter 6—Co-Occurring Disorders Among Special Populations
pregnancy and childcare difficulties as well as
certain kinds of trauma, violence, and victimization.
These issues are sometimes best dealt with in
women-only programs.
Substance Misuse and Mental Illness in
Women
Although women exhibit lower rates of SUDs than
men do, prevalence rates are still high. According
to 2018 National Survey on Drug Use and Health
(NSDUH) data, about 17 percent of women ages
18 and older reported past-year use of illicit
drugs, about 4 percent reported past-month
heavy alcohol use, and about 22 percent engaged
in past-month binge alcohol use (Center for
Behavioral Health Statistics and Quality [CBHSQ],
2019).
In the United States, mental illness prevalence
estimates are higher for women than men. The
2018 NSDUH showed that approximately 15
percent of men ages 18 and older reported
a past-year mental illness compared with
approximately 23 percent of women. However,
rates for men and women are very similar for SMI
(3.4 percent for men and 5.7 percent for women),
CODs (4.0 percent for men and 3.4 for women),
and combined SUDs with SMI (1.1 percent for men
and 1.4 percent for women). More women than
men with any mental illness received mental health
services in 2018, whether including or excluding
SMI (CBHSQ, 2019).
Treatment Approaches for Women
SUD treatment
Women disproportionately face barriers to
treatment related to children and child care.
Responsibility for care of dependent children is
one of the most significant barriers women face in
entering treatment, because many programs will
not enroll women who lack child care (Taylor, 2010).
Women who enter treatment sometimes risk losing
public financial assistance and custody of their
children, making the decision to begin treatment
a difficult one (Taylor, 2010). However, women
accompanied by their children into treatment can
achieve successful outcomes. The Iowa Pregnant
and Postpartum Women’s Residential Treatment
Program (https://idph.iowa.gov/substance-abuse/
programs/ppw), funded through a SAMHSA grant,
reported a 76-percent treatment completion rate
and 90.5-percent abstinence rate from drugs and
alcohol at 5 to 8 months after admission (Jones &
Arndt, 2017).
Other barriers to SUD treatment women face
include (McHugh, Votaw, Sugarman, & Greenfield,
2018; Taylor, 2010):
•
Fear of stigma, shame, and embarrassment,
especially among women with a history of sex
work.
•
Lack of support from partners, family, or friends.
•
Inability to afford the high cost of treatment;
women are less likely than men to have health
insurance or sufficient funds to cover costs.
•
Lack of programs that serve women and
children.
•
Denial or tendency to attribute substance-
related problems to sources other than the
addiction itself (like stress or physical health).
•
Avoidance of programs including men,
particularly if there is a history of physical or
sexual abuse.
•
Presence of a co-occurring mental illness,
especially PTSD, depression, anxiety, or an
eating disorder. CODs in women may lead to
difficulty initiating, engaging in, and completing
treatment.
Women differ from men in their SUD treatment
initiation and participation behaviors and needs
(Grella, 2008; McHugh et al., 2018; NIDA, 2018d):
•
Women are more likely to be referred to
or enter treatment via community-based
social services, like welfare and child welfare
programs, and are less likely to enter via the
criminal justice system.
•
Women are more likely to require public
assistance to pay for treatment.
•
Women may be more likely to initiate treatment
after fewer years of substance misuse than men,
but their clinical profiles are often more severe
(e.g., greater psychosocial distress, greater odds
of trauma experience, higher childcare burden,
worse functional impairment). They also tend to
start substance use at a later age but progress
from first use to addiction faster than men do.
Chapter 6 173

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
•
Women with SUDs have a higher reported
prevalence of mental disorders, particularly
internalizing conditions (e.g., depression,
anxiety, eating disorders, PTSD) and lower
self-esteem, whereas men with SUDs are more
likely to exhibit externalizing conditions (e.g.,
antisocial personality disorder [PD]).
•
Whereas women with SUDs report having more
difficulty with emotional problems, their male
counterparts report having more trouble with
functioning (e.g., work, money, legal problems).
Regarding treatment outcomes, large-scale
randomized clinical trials have been mixed in their
findings but generally find no gender differences.
Over the past two decades, there has been
an increase in policy and research supporting
the need for gender-sensitive SUD treatments.
Compared with mixed-gender approaches (Grella,
2008; McHugh et al., 2018), some women-specific
programs have been linked to:
•
Better treatment retention and substance use
outcomes (including abstinence).
•
Better client satisfaction, comfort, and self-
reported feelings of safety.
•
Reduced risk of criminal activity and
incarceration.
•
Higher rates of receiving continuity of care.
Positive outcomes are especially likely in
programs that include residential treatment
with in-house accommodations for children,
outpatient treatments that incorporate
family therapy, and comprehensive services
that address women-specific needs (e.g.,
case management, pregnancy-related services,
parenting training/classes, child care, job training,
and continuing care). Gender-specific treatments
are effective in several subpopulations of women,
including those with children, CODs, trauma
history, or criminal justice system involvement
(McHugh et al., 2018).
Programs offering COD treatment have a re-
sponsibility to address women’s specific needs.
Mixed-gender programs need to be responsive
to women’s needs. Women in mixed-gender
outpatient programs require careful, appro-
priate counselor matching and the availability
of specialized women-only groups to address
sensitive topics such as trauma, parenting, stigma,
and self-esteem. Strong administrative policies
pertaining to sexual harassment, safety, and
language must be clearly stated and upheld. The
same responsibility exists for residential programs
designed for women who have multiple and
complex needs and require a safe environment for
stabilization, intensive treatment, and an intensive
recovery support structure. Residential treatment
for pregnant women with CODs should provide
integrated SUD and mental disorder treatment and
primary medical care, as well as attention to related
problems and disorders. The needs of women in
residential care depend in part on the severity and
complexity of their co-occurring mental disorders.
Other areas meriting attention include past or
present history of domestic violence or sexual
abuse, physical health, and pregnancy or parental
status.
Exhibit 6.1 lists suggestions for gender-responsive
SUD treatment. TIP 51, Substance Abuse Treatment:
Addressing the Specific Needs of Women (SAMHSA,
2009c) offers more information on adapting
behavioral health services to the needs of women.
COD Treatment
The treatment barriers and socioeconomic
burdens facing women with either SUDs or
mental illness alone are multiplied for women
with both conditions, leading to substantial
challenges that make recovery more difficult and
relapse more likely. Women with SUDs frequently
have comorbid mental disorders, including SMI
(Evans, Padwa, Li, Lin, & Hser, 2015). This leads to
more severe symptoms, worse functioning, lower
quality of life, and more complex treatment needs
than for women who only have SUDs. Specifically,
women with CODs (particularly involving SMI, like
bipolar disorder or psychosis) are more likely than
women with only SUDs to (Evans et al., 2015):
•
Experience homelessness.
•
Be unmarried.
•
Have a past history of physical or sexual abuse.
•
Receive public assistance.
•
Have a longer substance use history.
•
Have more severe alcohol use–related problems.
174 Chapter 6
TIP 42
Chapter 6—Co-Occurring Disorders Among Special Populations
EXHIBIT 6.1. Adapting Treatment Services to Women’s Needs
•
Use nonconfrontational, strengths-based, trauma-informed treatment approaches.
•
Offer evidence-based interventions that have been researched specifically in female populations.
•
Ensure staff training and competencies regarding women-specific problems in substance misuse.
•
Provide:
- Prenatal/postnatal services.
- Women-only groups.
- Parenting training/counseling.
- Trauma/abuse counseling and other services.
- Education about and referral to women’s health services.
•
Use gender-specific assessments (including assessment of intimate partner violence and trauma).
•
Offer services related to child care and children’s needs, including:
- Onsite child care or, for residential settings, live-in accommodations for children.
- Screening and assessments for children.
- Child and family counseling (or referral for those services).
- Coordinated care with child welfare/children’s protective services.
•
Ensure the physical treatment environment is safe and secure. Being in close proximity to schools,
child care, and public transportation is also desirable.
Sources: Grella (2008); Tang, Claus, Orwin, Kissin, & Arieira (2012).
•
Have more severe problems related to
employment.
•
Have more severe medical conditions.
•
Have greater family dysfunctions.
•
Be on psychiatric medication.
Services for women with CODs should address
these disparities. Women with CODs may also lack
social support compared with women who have
only SUDs; counselors should help women with
CODs locate and use supportive services (Brown,
Harris, & Fallot, 2013).
Women receiving treatment for SUDs or CODs
often benefit from trauma-informed approaches.
Trauma is present in an overwhelming majority of
women with CODs (SAMHSA, 2015c), regardless
of their age. Most women have a history of at least
one adverse childhood experience, often abuse
(Choi et al., 2017). However, women with CODs
are less likely than women with SUDs only to enter
treatment and to receive ongoing care (Bernstein et
al., 2015), despite mental disorders and SUDs both
being disabling in women and a common cause of
inpatient hospitalization (Bennett, Gibson, Rohan,
Howland, & Rankin, 2018).
Women with CODs—and particularly with
SMI and SUDs—often do not receive services
for their conditions. Of women who entered
SUD treatment with a co-occurring mental
illness (Evans et al., 2015), almost 30 percent
with a comorbid mental disorder received no
mental health services over the course of 8 years,
including 7 percent with co-occurring psychosis,
13 percent with bipolar disorder, and 20 percent
with depressive disorder.
Pregnancy and CODs
Pregnancy can both aggravate and diminish the
symptoms of co-occurring mental illness. Women
with schizophrenia may experience a worsening
of symptoms, whereas women with bipolar
disorder have exhibited lower rates of new onset
or recurrence of symptoms (Jones, Chandra,
Dazzan, & Howard, 2014). Ample research has
examined MDD during the prenatal, perinatal, and
postnatal periods. Antidepressant discontinuation
or untreated depression during pregnancy can
exacerbate symptoms, including those related
to risk of suicide, and worsen outcomes for both
Chapter 6 175

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
mother and child (Gentile, 2017; Vigod, Wilson,
& Howard, 2016). However, pregnancy has been
linked to lower substance use in women, even
if abstinence is temporary (Muhuri & Gfroerer,
2009; SAMHSA, 2009c). Compared with women
who have a single disorder or no disorder,
pregnant women with CODs are at elevated
risk for negative perinatal outcomes, including
birth complications, premature birth, low infant
birthweight, nonadherence to prenatal care, child
developmental delays, and poorer psychosocial
functioning (Benningfield et al., 2010; Lee King,
Duan, & Amaro, 2015).
Topics To Address With Co-Occurring Mental
Illness
Careful treatment plans are essential for
pregnant women with mental disorders. Plans
should address childbirth and infant care. Women
often are concerned about the effects of their
medication on their fetuses. Treatment programs
should aim to maintain medical and mental stability
during clients’ pregnancies and collaborate with
other healthcare providers to ensure coordination
of treatment.
Experts recommend a multidisciplinary
approach to perinatal COD treatment, including
consultation with providers in obstetrics, addiction,
mental health, and pediatrics on pharmacotherapy
(e.g., selective serotonin-reuptake inhibitors
[SSRIs], MAT for opioid use disorder [OUD]),
individual counseling (e.g., CBT, exposure, other
trauma-based therapies), SUD treatment, prenatal
care, maternal education, health promotion, and
linkage to social services (Goodman, Milliken,
Theiler, Nordstrom, & Akerman, 2015).
Pregnant women with CODs report desiring SUD
treatment that includes (Kuo et al., 2013):
•
More flexible treatment schedules.
•
Longer sessions.
•
Assistance with transportation to and from
sessions.
•
Group treatments.
•
Interpersonal support (from partners, friends,
family, and counselors).
•
Linkage to community resources (like mutual-
support programs).
•
Treatment environments that convey a sense of
safety and comfort.
When women are parenting, it can often
retrigger their own childhood traumas. Therefore,
providers need to balance growth and healing with
coping and safety. Focusing on women’s desire to
be good mothers, the sensitive counselor will be
alert to guilt, shame, denial, and resistance related
to dealing with these problems, as recovering
women gain awareness of effective parenting skills.
Providers should allow for evaluation over time
for women with CODs. Reassessments should
occur as mothers progress through treatment.
Pharmacological Considerations
Prescribers should be aware that pregnant
women must understand the risks and benefits
of taking medications and sign informed consent
forms verifying receipt and understanding
of the information provided to them. Certain
psychoactive medications are associated with
birth defects, especially in the first trimester of
pregnancy; weighing potential risk/benefit is
important. In most cases, a sensible direction can
be found through consultation with physicians
and pharmacists who have expertise in treating
pregnant women with mental disorders. Screen
women for dependence on substances that can
produce life-threatening withdrawal for the mother:
alcohol, benzodiazepines, and barbiturates. These
substances, as well as opioids, can also cause a
withdrawal syndrome in babies, who may need
treatment. Make pregnant women aware of
wraparound services to assist them in managing
newborns, such as food, shelter, and medical
clinics for inoculations. Also ensure that women
are informed of programs that can help with
developmental or physical problems the infant may
experience as a result of alcohol or drug exposure.
Postpartum Depression and Psychosis
The term “postpartum depression” (PPD) in
Diagnostic and Statistical Manual of Mental
Disorders (5th ed.; DSM-5; American Psychiatric
Association [APA], 2013) refers to MDD in which
the most recent depressive episode has an onset
either during pregnancy or within 4 weeks after
delivery. DSM-5 designates such cases through
176 Chapter 6
TIP 42
Chapter 6—Co-Occurring Disorders Among Special Populations
PREGNANCY AND MAT FOR OUD
The approval of three medications by the Food and Drug Administration to treat OUD—methadone,
buprenorphine, and naltrexone—has given the primary care and behavioral health fields powerful new
tools to fight the opioid epidemic and save lives.
Considerations for MAT to address OUD in pregnant women include the following:
•
MAT is possible for women with OUD who are pregnant and should be actively considered, given the
wealth of evidence showing its effectiveness in reducing opioid use and preventing overdose.
•
Pregnant women should be considered for methadone or transmucosal buprenorphine treatment.
•
Pregnant women treated with methadone or sublingual or buccal buprenorphine have better outcomes
than pregnant women not in treatment who continue to misuse opioids.
•
Little research has examined the use of naltrexone during pregnancy. It should not be used with women
who are pregnant. Instead, they should be referred for an evaluation for methadone or buprenorphine.
•
Neonatal abstinence syndrome may occur in newborns of pregnant women who take buprenorphine.
Women receiving opioid agonist therapy while pregnant should talk with their healthcare provider about
neonatal abstinence syndrome and how to reduce it.
•
An obstetrician and an SUD treatment provider should deliver collaborative treatment, and the woman
should be offered counseling and other behavioral health services as needed.
Source: SAMHSA (2018c).
the MDD specifier “with peripartum onset.” (See
Chapter 4 for DSM-5 diagnostic criteria for MDD.)
PPD prevalence estimates vary, given differences
in timeframes researchers use to define the
postpartum period. According to DSM-5 (APA,
2013), 3 percent to 6 percent of women will
experience a major depressive episode either
during pregnancy or in the weeks and months
following childbirth. In a sample of 10,000 mothers
screened for depression 4 to 6 weeks following
delivery, 14 percent were positive for depression
(Wisner et al., 2013). Forty percent had postpartum
onset, 33 percent had onset during pregnancy, and
27 percent had onset prior to pregnancy. Thoughts
of self-harm occurred in 19 percent.
PPD is considered distinct from postpartum
“blues,” which is a mild, transient depression
occurring most commonly within 3 to 5 days after
delivery in about 30 percent to 80 percent of
women after childbirth (Buttner, O’Hara, & Watson,
2012; Jones & Shakespeare, 2014). Prominent in its
causes are a woman’s emotional letdown following
the excitement and fears of pregnancy and
delivery, the discomforts of the period immediately
after giving birth, hormonal changes, fatigue from
loss of sleep during labor and while hospitalized,
energy expenditure at labor, and anxieties about
caring for the newborn at home. Symptoms
include weepiness, insomnia, depression, anxiety,
poor concentration, moodiness, and irritability.
These symptoms tend to be mild and transient,
and women usually recover completely with rest
and reassurance. Anticipation and preventive
reassurance throughout pregnancy can prevent
postpartum blues from becoming a problem.
Women with sleep deprivation should be assisted
in getting proper rest. Follow-up care should
ensure that the woman is making sufficient
progress and not heading toward a relapse to
substance use.
Moderate-to-strong risk factors for PPD include
prior history of depression, anxiety, or other
mental distress during pregnancy; prepregnancy
mental disorder diagnosis (especially depression);
presence of postpartum blues; psychosocial stress
(e.g., poor marital relationships, lack of social
support, child care-related distress); and certain
personality traits and features (i.e., neuroticism, low
self-esteem) (O’Hara & McCabe, 2013).
Prospects for recovery from PPD are good with
supportive mental health counseling (especially
for acute cases) accompanied as needed by
pharmacotherapy, particularly in severe PPD
(Thomson & Sharma, 2017). Various forms of
Chapter 6 177

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
counseling (e.g., CBT, behavioral activation,
interpersonal therapy), pharmacotherapy
(e.g., SSRIs, selective norepinephrine reuptake
inhibitors), and brain stimulation (e.g.,
electroconvulsive therapy, repetitive transcranial
magnetic stimulation) have all been successful
in treating PPD (Guille, Newman, Fryml, Lifton,
& Epperson, 2013; O’Hara & Engeldinger, 2018;
Thomson & Sharma, 2017). Additionally, the
drug brexanolone received FDA approval for
treating PDD in 2019. Because some medications
pass into breastmilk and can cause infant
sedation, women should consult an experienced
psychiatrist or pharmacist for details on
pharmacotherapy.
Patients with PPD need to be monitored for
thoughts of suicide, infanticide, and progression
of psychosis in addition to their response to
treatment. Postpartum psychosis is a serious
but rare mental disorder, with first lifetime onset
occurring in 0.25 to 0.6 per 1,000 births (Bergink,
Rasgon, & Wisner, 2016). Women with this disorder
may lose touch with reality and experience
delusions, hallucinations, and disorganized speech
or behavior. Women most likely to be diagnosed
with postpartum psychosis have a previous
diagnosis or family history of bipolar disorder or
other psychotic disorders (e.g., schizophrenia,
schizoaffective disorder) (Davies, 2017). Other
studies reviewed by Bergink and colleagues
(2016) indicate that physiological factors, such as
hormonal, immunological, and circadian rhythm
disturbances, can increase the risk of postpartum
psychosis in women who are already genetically
vulnerable (e.g., those with a personal or family
history of bipolar disorder, those with certain
variants of the serotonin transporter gene). Typical
onset is 3 to 10 days after delivery (Bergink et al.,
2016).
Postpartum psychosis is associated with an
increased risk of suicide and infanticide (Bergink
et al., 2016; Brockington, 2017). As such, the
severity of the symptoms mandates immediate
evaluation (for diagnosis and for safety), which
often needs to be performed in an inpatient
setting, and treatment with benzodiazepines,
lithium, antipsychotics, electroconvulsive therapy,
or a combination thereof (Bergink et al., 2016;
Doucet, Jones, Letourneau, Dennis, & Blackmore,
2011). The risk of self-harm or harm to the baby
needs to be assessed. Monitoring of mother–infant
pairs by trained personnel can limit risks.
PPD and Substance Misuse
Little research has examined the relationship
between PPD and substance use. One review
of substance use in postpartum women found
that problematic alcohol use occurred in 1.5
percent to 8 percent and drug use (cocaine and
prescription psychoactive drugs) occurred in 2.5
percent (Chapman & Wu, 2013). Among women
who reported using substances postpartum or who
had a positive history of substance misuse, PPD
was highly prevalent (20 percent to 46 percent).
However, the women participating in these studies
were likely to have had higher rates of depression
than the general population to begin with because
of low income and socially marginalized status
(e.g., teenage mothers). The review also found
that alcohol or illicit drug use was associated with
higher scores of depression in postpartum women.
These findings are consistent with an earlier review
(Ross & Dennis, 2009) that similarly observed
an association between substance use and an
increased risk of PPD.
Women, Trauma, and Violence
Up to 80 percent of women seeking SUD
treatment have a lifetime history of physical
or sexual victimization, often traced back to
childhood (Cohen, Field, Campbell, & Hien,
2013). Intimate partner violence is also strongly
connected to women’s substance misuse and
mental illness (Macy, Renz, & Pelino, 2013; Mason
& Dumont, 2015). In addition to SUDs, trauma-
exposed individuals in the community who have
PTSD are at an increased risk for MDD, dysthymic
disorder, bipolar I and II disorders, generalized
anxiety disorder, panic disorder, agoraphobia
without panic disorder, social and specific phobias,
and lifetime suicide attempt (Pietrzak, Goldstein,
Southwick, & Grant, 2011).
People seeking SUD treatment who have PTSD
are 14 times more likely to have an SUD than
people without PTSD (McCauley, Killeen, Gros,
Brady, & Back, 2012). In the general public,
178 Chapter 6
TIP 42
Chapter 6—Co-Occurring Disorders Among Special Populations
lifetime prevalence rates of PTSD (full or partial)
are two times higher in women than in men, with
46 percent of people with full PTSD also meeting
criteria for an SUD (Pietrzak et al., 2011). Women
who are incarcerated have even higher rates of
each disorder—88 percent with full or partial PTSD
and 87 percent with an SUD (Wolff et al., 2011).
Women with trauma/PTSD may misuse substances
to avoid intrusive, distressing symptoms (e.g.,
flashbacks, nightmares) or to numb themselves to
emotional pain (Dass-Brailsford & Safilian, 2017).
Few SUD treatment programs assess for, treat,
or educate clients about trauma and instead
focus on managing the addiction (Macy et al.,
2013). This is a serious deficiency, given the many
interrelated consequences of failing to address
trauma. Greater violence leads to more serious
substance misuse and other addictions (e.g., eating
disorders, sexual addiction, compulsive exercise),
along with higher rates of depression, self-harm,
and suicidal impulses. People with PTSD and
AUD, for example, are vulnerable to more severe
symptoms, greater risk of comorbid mood and
PDs, worse physical functioning, and higher risk
of suicide attempt than those with either disorder
alone (Blanco et al., 2013). SUDs place women at
higher risk of future trauma through associations
with dangerous people and lowered self-protection
when using substances (e.g., going home with a
stranger after drinking).
Integrated trauma-informed treatment programs
and approaches may be equally or more effi-
cacious or effective than usual care in reducing
substance misuse and psychiatric symptoms.
Examples include integrated CBT, Seeking Safety,
the Treatment Affect Regulation: Guide for
Education and Therapy program, the Addictions
and Trauma Recovery Integration program, the
Concurrent Treatment of PTSD and Substance Use
Disorders Using Prolonged Exposure program, and
the Trauma Recovery and Empowerment Model
(Dass-Brailsford & Safilian, 2017; Killeen, Back, &
Brady, 2015).
For more information about trauma and for
guidance on offering trauma-informed care, see
Chapter 4.
For more detailed information, including
individual and other models of trauma healing,
see:
•
TIP 51, Substance Abuse Treatment: Addressing
the Specific Needs of Women (https://store.
samhsa.gov/system/files/sma15-4426.pdf).
•
TIP 57, Trauma-Informed Care in Behavioral
Health Services (https://store.samhsa.gov/
system/files/sma14-4816.pdf).
People of Diverse Racial/Ethnic
Backgrounds
As racial and ethnic diversity in the United States
increases, the need to address cultural differences
in mental health and SUD treatment access,
provision, and outcomes is becoming more urgent.
Per NSDUH data (CBHSQ, 2019), 2.9 percent of
Whites had a past-year illicit drug use disorder
in 2018 versus about 3.4 percent of African
Americans, 4.0 percent of American Indians and
Alaskan Natives, 3 percent of Latinos, and 1.6
percent of Asian Americans. AUD, prevalence was
5.7 percent among Whites, 4.5 percent among
African Americans, 7.1 percent among American
Indians or Alaskan Natives, 5.3 percent among
Latinos, and 3.8 percent among Asian Americans.
Approximately 16 percent of African American
adults ages 18 and older had any past-year mental
illness in 2018; similar rates occurred in other
groups, including Latinos (16.9 percent) and Asian
Americans (14.7 percent). By comparison, 20.4
percent of Whites and 22.1 percent of American
Indians and Alaska Natives reported any past-year
mental illness.
Cultural Perceptions of Substance Misuse,
Mental Disorders, and Healing
Clients may have culturally determined concepts
of what it means to misuse substances or to have
a mental disorder, what causes these disorders,
and how they may be “cured.” Providers are
encouraged to explore these concepts with
people who are familiar with the cultures
represented in their client population and with
the clients themselves. Counselors should be
Chapter 6 179

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
alert to differences in how their role and the
healing process are perceived by people who
are of cultures other than their own. Whenever
appropriate, familiar healing practices meaningful
to clients should be integrated into treatment. An
example would be the use of acupuncture to calm
a Chinese client or help control cravings.
Cultural Perceptions and Diagnosis
Being aware of cultural and ethnic bias in
diagnosis is important. For example, in the
past some African Americans were stereotyped
as having paranoid PDs, whereas women have
been diagnosed frequently as being histrionic or
borderline. American Indians with spiritual visions
have been misdiagnosed as delusional or as having
borderline or schizotypal PDs. Diagnostic criteria
should be tempered by sensitivity to cultural
differences in behavior and emotional expression
and by an awareness of the provider’s own
biases and stereotyping.
Treatment Access and Utilization
Compared with Whites, other racial/ethnic
populations make up a smaller percentage of
the U.S. population with mental disorders, SUDs,
or both. Yet concerns remain about treatment
access and use, as people of diverse ethnic/racial
backgrounds are disproportionately uninsured
(Kaiser Family Foundation, 2017; Sohn, 2017). Racial
and ethnic populations have historically faced more
financial and nonfinancial barriers to health care in
general than Whites, including low cultural compe-
tency in their treatment providers (Mitchell, 2015).
These barriers lead to worse health outcomes (e.g.,
increased morbidity, worse quality of care) as well
as higher healthcare costs. Similarly, marginalized
groups face systemic, organizational, cultural, and
attitudinal obstacles to SUD treatment and mental
health services (Holden et al., 2014; Keen et al.,
2014; Masson et al., 2013; Maura & Weisman de
Mamani, 2017; Pinedo, Zemore, & Rogers, 2018),
including:
•
Fear of stigma and feelings of shame.
•
Mistrust of providers.
•
Language barriers.
•
Logistical obstacles (e.g., lack of transportation,
lengthy wait times).
•
Fearing the provider will not understand the
client’s culture, religion, or circumstances (e.g.,
immigration) or that the services won’t be
culturally responsive.
•
Lack of insurance.
•
Not knowing where to go for treatment.
•
Not believing treatment is needed.
•
Lacking confidence in treatment effectiveness.
•
Family factors (e.g., lack of support, pressure
RACIALETHNIC DISPARITIES AND SMI
Findings from a 2017 review of ethnic/racial disparities in the diagnosis and treatment of SMI suggest that:
•
African Americans, Asian Americans, and Latinos offered mental health services in medical settings are
more likely than Whites to receive a schizophrenia spectrum diagnosis.
•
African Americans are more likely than Whites to be diagnosed with schizophrenia (and in one study
were more than four times likely).
•
African Americans are more likely than Whites to get higher doses of antipsychotics and are less likely to
be prescribed newer generation antipsychotics (which have fewer side effects).
•
Mental health service retention is lower for African Americans than for Whites.
•
African Americans have worse mental health outcomes following inpatient treatment than Whites.
•
Minorities are more likely to drop out of treatment by psychologists, psychiatrists, and general
practitioners.
•
African Americans are less likely than Whites to receive continuing care (e.g., medication management,
outpatient visits/follow-up services) following hospital discharge.
•
Diverse racial and ethnic populations in medical settings are more likely to use emergency rather than
community services and thus are more likely to be hospitalized than Whites.
Source: Maura & Weisman de Mamani (2017).
180 Chapter 6

TIP 42
Chapter 6—Co-Occurring Disorders Among Special Populations
to not enter treatment, withdrawal of financial
help, not including family in treatment).
The effects of these barriers are reflected in
lagging rates of treatment access, utilization,
and completion for mental illnesses, SUDs,
or CODs by diverse ethnic/racial populations
compared with Whites (Cook et al., 2017; Holden
et al., 2014; Maura & Weisman de Mamani, 2017;
Nam et al., 2017; Saloner & Le Cook, 2013;
Sanchez et al., 2016). This inequity may result
from underassessment, underdiagnosis, and
underreferral (Priester et al., 2016) as well as from
cultural barriers.
Rates of SUD treatment provided in criminal
justice facilities, in which racial/ethnic populations
are overrepresented compared with Whites
(Pew Research Center, 2018), also reveal cultural
disparities (Nicosia, Macdonald, & Arkes, 2013).
Whites who are incarcerated and have an SUD are
more likely than African Americans and Latinos
to receive SUD treatment and more likely to have
SUD treatment and mental health services as a part
of their sentencing requirements (Nowotny, 2015).
Reducing Racial/Ethnic Disparities
Recommended approaches to improving
disparities in treatment access, utilization, and
completion center on implementing healthcare
and funding policy changes (e.g., legislation to
increase awareness about disparities, expanding
state Medicaid funding for treatment programs)
and improving workforce cultural responsiveness
(Morgan, Kuramoto, Emmet, Stange, & Nobunaga,
2014; Saloner & Le Cook, 2013; Wile & Goodwin,
2018). For instance, culturally responsive
organizational practices (e.g., diverse hiring, staff
training, linkage with surrounding community) and
acceptance of public insurance have reduced gaps
in service access and provision for low-income
minority racial/ethnic populations by reducing
wait time and improving SUD treatment retention
(Guerrero, 2013).
Integrated and person-centered care also may
help reduce healthcare disparities through strate-
gies such as (Maura & Weisman de Mamani, 2017;
Sanchez et al., 2016):
•
Using bilingual case managers.
•
Maintaining a diverse workforce.
•
Ensuring staff are trained in culturally responsive
care.
•
Using multilingual mutual-support programs.
•
Using patient navigators to help clients access
community resources and overcome logistical
barriers (e.g., keeping appointments).
•
Performing assessments that address clients’
cultural concepts/understanding of their
symptoms.
•
Using culturally relevant interpretations and
frameworks to describe mental disorders
(e.g., depression) rather than solely relying on
Western definitions.
•
Eliciting client preferences about treatment
decisions, including giving the option to forego
medication in favor of psychotherapy.
•
When appropriate, including family in the
treatment process and in education about
mental illness.
•
Using patient-centered communication to
improve client education and reduce stigma,
shame, and misunderstanding.
•
Using sensitive, empathic, person-centered
communication to build trust and enhance
rapport.
•
Providing culturally adapted evidence-based
treatments when possible.
For more information about developing
and implementing culturally responsive and
competent services, see TIP 59, Improving Cultural
Competence (SAMHSA, 2014a).
Cultural Dierences and Treatment:
Empirical Evidence on Eectiveness
Studies of cultural differences in COD treatment
are scarce. However, culturally adapted mental
health services have been linked to small-to-mod-
erate benefits compared with nonadapted
treatments, placebo, waitlists, and usual care
(Cabassa & Baumann, 2013). For example, a review
of culturally responsive mental health services for
people with SUDs (Gainsbury, 2017) reported that:
•
Culturally tailored psychosocial interventions
increase treatment engagement and
Chapter 6 181

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
ADVICE TO THE COUNSELOR: USING CULTURALLY APPROPRIATE
METHODS
The consensus panel recommends these modifications to provide culturally appropriate COD treatment:
• Adapting interventions by altering the content of materials or communications to reflect racial/ethnic or
cultural facts, values, imagery, beliefs, and norms. Engage members of the community (such as through
focus groups) to ensure content adaptations are appropriate, accurate, and relevant.
• Use translated materials to meet the needs of clients for whom English is not a primary language.
Simplified materials (such as those using illustrations, which can be more universally understood) are
also desirable.
• Tailor services by culturally matching counselors to clients (if possible) and via culture-specific
resources.
• When able, implement programs directly in the community where clients reside.
• Take into account the client’s cultural beliefs about mental health, substance use, help-seeking
behavior, causes of problems, and approaches to treatment. Similarly, in some cultures, there may be
strong beliefs about the role of the family in the treatment of mental illness, substance misuse, or both;
those beliefs may need to be accounted for when treatment planning.
Source: Healey et al. (2017).
participation, enhance client–provider alliance,
reduce early treatment discontinuation, and
improve symptoms.
•
Cultural competence training for staff is
associated with improved communication,
more accurate diagnosis, a positive therapeutic
alliance, and greater client satisfaction.
•
Providing treatment in a client’s native language
or dialect can lead to better treatment
outcomes and may be more influential than
matching the provider’s race/ethnicity to that of
the client.
•
Providers who show greater comfort with openly
discussing cultural identities and values with
clients may have better client retention rates
than those who are uneasy talking about such
topics.
Cultural competence should be a goal for
programs as well as providers. In a study of more
than 350 nationally representative outpatient SUD
treatment programs (Guerrero & Andrews, 2011),
program cultural competence—namely, managers’
culturally sensitive beliefs—predicted reduced
client wait time and increased retention among
Latinos and African Americans. Program leadership
can influence staff uptake of culturally responsive
care, translating to potentially better outcomes for
clients.
Conclusion
To effectively fill practice gaps and more
comprehensively address the widespread problem
of unmet COD treatment needs, behavioral health
service providers and programs need to recognize
groups who have been historically underserved.
The recovery community is diverse, and counselors
may need to think outside of the box in adapting
traditional techniques and perspectives to better
meet the individual needs of all clients. Using a
cookie-cutter approach for all clients in all settings
increases the likelihood of improper diagnosis and
treatment and is inconsistent with expert guidance
on providing comprehensive, person-centered,
recovery-oriented care.
182 Chapter 6

Chapter 7—Treatment Models and Settings
for People With Co-Occurring Disorders
KEY MESSAGES
TIP 42
SUBSTANCE USE DISORDER TREATMENT FOR
PEOPLE WITH CO-OCCURRING DISORDERS
• Co-occurring disorders (CODs) are
undertreated conditions that exact a serious
toll on both the individuals living with them as
well as on their families, caregivers, and society
as a whole. Early and effective treatments
offer people the opportunity to live fulfilling,
healthy, productive lives.
• Available treatment models work by
leveraging education, support, resources, and
other services drawn from multiple sources,
such as healthcare professionals collaborating
across primary care service, mental health
services, and substance use disorder (SUD)
treatment; mutual-support programs;
professionals in the recovery community; and
peer recovery support specialists.
• Treatment providers should not operate in silos
nor should they use treatments in isolation.
The best way to serve people with CODs is to
offer services and programs that are integrated,
comprehensive, person centered, and recovery
oriented in their structure, milieu, and practice.
• Counselors and programs need to provide
effective interventions across multiple settings
because people with mental disorders and
SUDs often move among across levels of care,
and this should not be a barrier to receiving
needed evidence-based services.
• Although psychosocial services are often
a cornerstone of interventions for CODs,
counselors working with this population
should be familiar with medication treatment,
as many effective pharmacotherapies are
available to help people reduce at least some
of their symptoms and make appreciable gains
in functioning.
Of the 9.2 million adults who had CODs in 2018,
approximately half received no treatment at all, and
only 8 percent received care for both conditions
(Center for Behavioral Health Statistics and Quality,
2019). What happens to people with CODs who
enter traditional SUD treatment settings? What
can counselors, other providers, supervisors, and
administrators do to help people with CODs more
successfully access needed services? How can
programs provide the best possible services to
clients? What treatment options are available, and
to what extent are they supported by science? This
chapter is addressed to counselors, other treatment/
service providers, supervisors, and administrators
and seeks to answer these and other important
questions about the management of co-occurring
mental illness and addiction.
This chapter examines treatment models (e.g.,
integrated care, assertive community treatment
[ACT], intensive case management [ICM], mutual-
support and peer-based programs) and treatment
settings (e.g., therapeutic communities [TCs],
outpatient and residential care, acute care and
other medical settings) for clients with CODs. It
opens with an overview of general COD treatment
considerations, including types of programs, levels
of service (and matching clients to appropriate
levels), episodes of treatment, integrated versus
nonintegrated treatment, culturally competent
services, and barriers to care. The bulk of the
material then focuses on three areas: treatment
models, treatment settings, and pharmacotherapy.
Specific interventions, like cognitive–behavioral
therapy (CBT), behavioral therapy, multidimensional
family therapy, and dialectical behavior therapy, are
beyond the scope of this Treatment Improvement
Protocol (TIP). Readers should already possess a
basic understanding of and working familiarity with
these commonly used SUD treatments. Rather, the
material is focused on describing the models and
settings in which such interventions are provided.
183

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
Regarding pharmacotherapy, the chapter is
not intended to offer exhaustive guidance on
medication for CODs, and prescribers are not
the intended primary audience of this chapter.
However, counselors and other providers working
with people who have CODs will encounter people
taking medication and thus need to become
familiar with medication names, side effects, and
warnings about harmful interactions (especially with
alcohol) and other adverse consequences.
Several examples of program models designed to
serve COD populations are included throughout
this chapter, as are “Advice to the Counselor”
boxes to provide readers who have basic
backgrounds with the most immediate practical
guidance for implementing various program
models in different treatment settings. To an
extent, this chapter works hand in hand with
the programmatic perspectives of Chapter 8 by
discussing how to design and implement programs
in various settings. Administrators will benefit from
reviewing this information but should also be sure
to read Chapter 8 for additional information about
workforce hiring, training, and retention.
Treatment Overview
Treatment Programs
A mental health program offers an organized array
of services and interventions focused on treating
mental disorders, providing acute stabilization
or ongoing treatment. These programs exist in
various settings, like traditional outpatient mental
health centers (e.g., psychosocial rehabilitation
programs, outpatient clinics) or more intensive
inpatient treatment units. Many such programs
treat significant numbers of individuals with CODs.
Programs more advanced in treating people with
CODs may offer various interventions for SUDs
(e.g., motivational interviewing, SUD counseling,
skills training) in the context of the ongoing mental
health services.
An SUD treatment program offers an organized
array of services and interventions focused on
treating SUDs, providing both stabilization and
ongoing treatment. SUD treatment programs
more advanced in treating people with CODs
may offer a variety of interventions for mental
disorders (e.g., symptom management training,
psychopharmacology,) in the context of the
ongoing SUD treatment.
Program Types
The American Society of Addiction Medicine
(ASAM; Mee-Lee et al., 2013) describes three
types of service programs for people with CODs:
•
Co-occurring–capable (COC) programs are SUD
treatment programs that mainly focus on SUDs
but can also treat patients with subthreshold
or diagnosable but stable mental disorders
(Mee-Lee et al., 2013). These programs may
offer mental health services onsite or by referral.
COC programs in mental health focus mainly
on mental disorders but can treat patients with
subthreshold or diagnosable but stable SUDs
(Mee-Lee et al., 2013). COC programs have
addiction counselors onsite or available through
referral.
•
Co-occurring–enhanced programs have a higher
level of integration of SUD treatment and
mental health services, staff trained to recognize
the signs and symptoms of both disorders, and
competence in providing integrated treatment
for mental disorders and SUDs at the same time.
•
Complexity-capable programs are designed to
meet the needs of individuals (and their families)
with multiple complex conditions that extend
beyond just CODs. Physical and psychosocial
conditions and treatment areas of focus often
include chronic medical illnesses (e.g., HIV
and other infectious diseases), trauma, legal
matters, housing difficulties, criminal justice
system involvement, unemployment, education
difficulties, childcare or parenting difficulties,
and cognitive dysfunctions.
Levels of Service
Because mental disorders and SUDs are complex
and vary in their severity and consequences, a
wide range of levels of service are needed, from
high-intensity inpatient medical service to periodic
outpatient treatment. Not all people with CODs
will require the full continuum of services, and
not all clients will move through levels of care
in a linear fashion. Clients can transition to and
from greater and lower intensity services and
184 Chapter 7
TIP 42
high
severity
Category III
Mental disorders less severe
SUDs more severe Locus of care
SUD Treatment System
Category I
Mental disorders less severe
SUDs less severe Locus of care
Primary healthcare settings
Alcohol and Drug Use Disorders
low
severity
Category IV
Mental disorders more severe
SUDs more severe Locus of care
State hospitals, jails/prisons,
emergency rooms, etc.
Category II
Mental disorders more severe
SUDs less severe Locus of care
Mental health system
high
severity
Mental Illness
Chapter 7—Treatment Models and Settings for People With Co-Occurring Disorders
should be offered services based on clinical need
(e.g., symptom severity, functional ability, person’s
overall level of stability) and stage of change.
The Level of Care Utilization System (LOCUS;
American Association of Community
Psychiatrists, 2016) describes six major domains
of service levels for people with CODs:
1. Recovery Maintenance/Health Management
2. Low Intensity Community Based Services
3. High Intensity Community Based Services
4. Medically Monitored Non-Residential Services
5. Medically Monitored Residential Services
6. Medically Managed Residential Services
Chapter 3 further addresses levels of care, including
services/populations associated with each.
Treatment Matching to Levels of Service
Using the Quadrants of Care
Effective treatment matching is an essential
component of quality care for people with CODs
that benefits the healthcare system as a whole.
Treatment matching not only ensures clients
receive the appropriate type and dose of service
needed, it can help reduce unnecessary lengths
of stay for residential treatment and helps reserve
use of costly healthcare resources for those who
truly require complex interventions. The widely
used Four Quadrant Model (Ries, 1993; Exhibit
7.1) provides a framework for treatment decision
making and prioritizing service needs for clients
with CODs based on symptom/disorder severity.
It has good concurrent and predictive validity
(McDonell et al., 2012).
Under this conceptualization, clients are catego-
rized accordingly:
•
Category I: Less severe mental disorder/less
severe SUD
•
Category II: More severe mental disorder/less
severe SUD
•
Category III: Less severe mental disorder/more
severe SUD
•
Category IV: More severe mental disorder/more
severe SUD
For a more detailed description of each quadrant
and how to integrate treatment matching into
the assessment process using the Four Quadrant
Model, see Chapter 3.
EXHIBIT 7.1. The Four Quadrants of Care
Chapter 7 185

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
Episodes of Treatment
An individual with CODs can participate in
recurrent episodes of treatment involving acute
stabilization (e.g., crisis intervention, detoxification,
psychiatric hospitalization) and specific ongoing
treatment (e.g., mental health–supported housing,
day treatment for mental illness, or residential
treatment for SUDs). Counselors should recognize
the reality that clients engage in a series of
treatment episodes, as many individuals with CODs
progress gradually through repeated involvement
in treatment.
Integrated Versus Nonintegrated
Treatment
Providers generally treat CODs in one of three
ways (Morisano, Babor, & Robaina, 2014):
1. Sequential or serial treatment, in which the
client is treated for one disorder at a time.
This has been the historic approach, but its
effectiveness is dubious and may lead to worse
outcomes given that, in some conditions,
treatment of one disorder can worsen symptoms
of the other (e.g., exposure therapy for a client
with posttraumatic stress disorder [PTSD] might
lead to anxiety and distress and subsequent
alcohol use as a form of coping).
2. Simultaneous or parallel treatment, wherein
the client is treated for both disorders but by
separate providers and in separate systems.
Although an improvement over sequential
treatment, this approach does not lead to
collaborative, comprehensive care.
3. Integrated treatment, which is the preferred
method because it addresses all of a client’s
diagnoses and symptoms within one service
system/agency/program and through a single
team of providers working closely together.
Integrated treatment is a means of actively
combining interventions intended to address
SUDs and mental disorders in order to treat
both disorders, related problems, and the whole
person more effectively.
Integrated treatments for people with CODs
have demonstrated superiority to nonintegrated
approaches and help improve substance use,
mental illness symptoms, treatment retention,
cost effectiveness, and client satisfaction (Kelly &
Daley, 2013; Morisano et al., 2014). For an indepth
discussion, see the section “Integrated Care” later
in this chapter.
Culturally Responsive Treatment
One definition of cultural competence refers
to “effective, equitable, understandable, and
respectful quality care and services that are
responsive to diverse cultural health beliefs and
practices, preferred languages, health literacy and
other communication needs” (Office of Minority
Health, 2018). Treatment providers should view
clients with CODs and their treatment in the
context of their language, culture, ethnicity,
geographic area, socioeconomic status, gender,
age, sexual orientation, religion, spirituality, and
physical/cognitive disabilities.
Cultural factors that may have an impact on
treatment include heritage, history and experience,
beliefs, traditions, values, customs, behaviors,
institutions, and ways of communicating. The
client’s culture may include distinctive ways of
understanding disease or disorder, including
mental disorders and SUDs, which the provider
needs to understand. Referencing a model of
disease that is familiar to the client can help
communication and enhance treatment. Counselors
should educate themselves about the cultural
factors that are important to racial/ethnic groups
that their clients represent.
Clients, not counselors, define what is cultur-
ally relevant to them. Making assumptions,
however well intentioned, about the client’s
cultural identity can damage the relationship
with a client. For example, a client of Hispanic
origin may be a third-generation U.S. citizen, fully
acculturated, who feels little or no connection with
her Hispanic heritage. A counselor who assumes
this client shares the beliefs and values of many
Hispanic cultures would be making an erroneous
generalization. Similarly, it is helpful to remember
that all of us represent multiple cultures. Clients are
more than their racial/ethnic identities. A 20-year-
old African-American man from the rural south may
identify, to some extent, with youth, rural south,
or African-American cultural elements—or might,
instead, identify more strongly with another cultural
186 Chapter 7

TIP 42
Chapter 7—Treatment Models and Settings for People With Co-Occurring Disorders
element that is not readily apparent, such as his
faith. Counselors are advised to open a respectful
dialog with clients around the cultural elements
that have significance to them.
For discussion of cultural competence in SUD
treatment, see TIP 59, Improving Cultural
Competence (SAMHSA, 2014a). Chapter 6
addresses cultural competency for counselors
whose clients have CODs.
Barriers to Treatment
People with CODs usually have extensive
treatment needs, which unfortunately often go
unmet. Among the approximately 8.5 million
U.S. adults ages 18 and older with a past-year
SUD and any mental illness in 2018, less than 10
percent received treatment for both disorders
(Center for Behavioral Health Statistics and Quality,
2019). Similarly, from 2008 to 2014, 52 percent of
people with CODs received neither mental health
REDUCING BARRIERS TO CARE: WHAT CAN COUNSELORS AND
ADMINISTRATORS DO?
•
Use person-centered approaches in assessing and treating clients with CODs. Consider factors such as:
- The client’s gender, age, race/ethnicity, or other demographic characteristic that could affect how the
client experiences his or her illnesses and treatment.
- The client’s cultural background, including birth status (i.e., native born vs. immigrant).
- The client’s degree of acculturation and acculturation stress.
- The client’s history of trauma.
- The client’s current functional status (including housing and educational/vocational status).
- Whether the client is experiencing any cognitive disabilities because of her or her diagnoses
(particularly if the person has a psychotic disorder).
- The interaction style to which the person best responds (e.g., Direct? Nonconfrontational?).
•
Consider offering harm-reduction treatments in addition to abstinence-based services. Programs that
limit themselves to abstinence-only treatments may fail to engage and retain clients who are not ready to
stop substance use altogether but are otherwise amenable to treatment.
•
Offer informal pretreatment services for people who are awaiting intake/appointments.
•
Adapt services to the logistical demands facing clients. For instance:
- When possible, offer appointments throughout the week and at various times (including before and
after normal business hours to accommodate people who work or attend school full time).
- Use remote services (e.g., telehealth) to reach and engage clients who are immobile or live at a distance.
•
Make integrated care a priority. Programs that offer comprehensive services that work to
simultaneously address all of a client’s needs, using the same set of providers, are more likely to keep
clients engaged and participating in treatment than ones that are fragmented. Treating substance
use and mental disorders in isolation hinders counselors’ ability to help clients address all aspects of
functioning and disability, including their housing status, medication needs, and family relationships.
These factors require attention because they can become reasons for clients to drop out.
•
Use a staged approach to interventions (i.e., engagement, persuasion, active treatment, relapse
prevention) that is tailored to clients’ readiness to change and is flexible, as clients often move through
stages in a nonlinear fashion. Motivational interviewing can help determine clients’ readiness for
interventions and aids in the creation of personally meaningful and realistic treatment goals.
•
Use assertive community outreach, such as ICM and ACT services, as these foster therapeutic alliance
and reduce practical/logistical barriers to treatment access and adherence (e.g., providing in-home
services).
•
Emphasize COD leadership within programs. Programs need to have a director on staff whose primary
job is to oversee COD programming, services, fidelity, and staff competency/training.
Sources: Priester et al. (2016); SAMHSA (2009a).
Chapter 7 187

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
RESOURCE ALERT: FINDING QUALITY TREATMENT FOR SUBSTANCE USE
DISORDERS
SAMHSA’s fact sheet helps people with SUDs make decisions about quality services and learn where to locate
SUD treatment facilities and providers (https://store.samhsa.gov/system/files/pep18-treatment-loc.pdf).
services nor SUD treatment in the prior year (Han,
Compton, Blanco, & Colpe, 2017). People might
avoid pursuing treatment given lack of afford-
ability, lack of knowledge about where to access
treatment, and low perceived treatment need (e.g.,
not feeling ready to stop using substances, feeling
like they could handle mental illness on their own)
(Han, Compton, et al., 2017). Other common
obstacles to accessing and benefiting from COD
treatment include (Priester et al., 2016):
•
Attitudinal and motivational barriers.
•
Personal beliefs about and cultural conceptions
of mental illness, addiction, and treatment.
•
A lack of culturally sensitive/responsive
assessments and treatments.
•
Gender-specific factors. (e.g., a history of
violence/abuse/trauma among women).
•
Racial/ethnic factors. (e.g., lower rates of
diagnosis and treatment referral for minorities
than for Whites.)
•
Stigma.
•
Impaired cognition and insight (particularly
among people with serious mental illness [SMI]).
•
Logistical barriers (e.g., lack of transportation,
childcare needs, limited access to resources).
•
Limited social support.
•
High levels of distress.
•
Providers’ inability to identify CODs because
of inadequate training, lack of comprehensive
screening and assessment procedures, or both.
•
A dearth of COD-specialized services across
inpatient and outpatient settings.
•
Social, political, systemic, and legal barriers
(e.g., poor service availability, insurance
barriers).
•
Socioeconomic factors, like low income,
relying on public assistance, being uninsured,
or Medicaid restrictions affecting program
reimbursement.
•
Organizational “red tape” leading to delays in
care and lack of service provision.
Some populations, such as women, diverse racial/
ethnic groups , people involved in the criminal
justice system, and individuals experiencing
homelessness, are especially vulnerable to
treatment access challenges and poor outcomes.
Learn more about these groups and how to adapt
services to meet their needs in Chapter 6.
Treatment Models
Integrated Care
Integrated interventions are specific treatment
strategies or techniques in which interventions for
CODs are combined in a single session/interaction
or in a series of interactions/multiple sessions.
Integrated interventions can include a wide range
of techniques. Some examples include:
•
Integrated screening and assessment processes.
•
Dual recovery mutual-support group meetings.
•
Dual recovery groups (in which recovery skills for
both disorders are discussed).
•
Motivational enhancement interventions
(individual or group) that address both mental
and substance use problems.
•
Group interventions for people with the triple
diagnosis of mental disorder, SUD, and another
problem, such as a chronic medical condition
(e.g., HIV), trauma, homelessness, or criminality.
•
Combined psychopharmacological
interventions, in which a person receives
medication designed to reduce addiction to or
cravings for substances as well as medication for
a mental disorder.
Integrated interventions can be part of a single
program or can be used in multiple program
settings.
188 Chapter 7
TIP 42
Chapter 7—Treatment Models and Settings for People With Co-Occurring Disorders
INTEGRATED CARE: PARTNERSHIPS FOR PHARMACOTHERAPY
Recovery-oriented systems of care foster both integrated care for the simultaneous treatment of mental
illness and SUDs but also foster critical processes, like active linkages, warm handoffs, and ongoing follow-
up from one stage or environment of care to the next. This is particularly important for people with SMI
because these diagnoses tend to require lifelong monitoring and management of potentially debilitating
symptoms. If a client is not responding to a nonpharmacological treatment, consider whether:
•
An alternative treatment or service (e.g., a different psychotherapeutic approach, medication, mutual
support) is needed.
•
The treatment is a good match the client’s level of service need.
•
The treatment is a good match for the client’s readiness for change.
Given that medication often plays a role in helping people with SMI achieve and sustain recovery, it may
be worth considering whether referral of clients with CODs (and especially SMI) to a provider qualified to
assess for pharmacologic options is needed.
Behavioral health programs should encourage the provider making that referral to do a warm handoff and
follow up with the client in 2 to 4 weeks to determine how well the medication is working and whether
the client has any concerns. If pharmacotherapy is being provided offsite (e.g., to a methadone clinic), the
provider will need to obtain the client’s written consent to discuss with the prescribing provider how the
client is faring, whether medication seems to be effective, and whether any nonpharmacologic treatments
or services need to be tailored in any way as a result of the client taking medication.
For more guidance about medication treatments for CODs, see the section “Pharmacotherapy” at the end of
this chapter. Also see the text box “Knowing When To Refer for Medication Management” within that section.
Empirical Evidence of Integrated Care for
CODs
The integrated model of care is considered a
best practice for serving people with CODs. (See
“Resource Alert: Implementing Integrated Care for
People With CODs.”) It has been linked to many
desirable substance-, psychiatric-, functional-, and
service-related outcomes, including decreased
substance use and abstinence (Drake, Bond, et
al., 2016; Flanagan et al., 2016; Kelly & Daley,
2013; McGovern et al., 2015; Ruglass et al., 2017;
Schumm & Gore, 2016; Sterling, Chi, & Hinman,
2011); improved mental functioning (Alterman, Xie,
& Meier, 2011; Drake, Bond, et al., 2016; Flanagan
et al., 2016; Kelly & Daley, 2013; McGovern,
Lambert-Harris, Ruglass, et al., 2017); decreased
emergency department (ED) visits, inpatient hos-
pitalizations, and healthcare costs (Morse & Bride,
2017); gains in independent housing and com-
petitive employment (Drake, Bond, et al., 2016);
improved life satisfaction or quality of life (Drake,
Bond, et al., 2016); and greater client satisfaction
(Schulte, Meier, & Stirling, 2011).
Integrated COD care can be effective across different
settings and in diverse populations, including:
•
In residential facilities (McKee, Harris, &
Cormier, 2013). Here, integrated care has been
associated with significant reductions in mental
illness symptoms, improvements in COD-related
knowledge and skills, increased self-esteem,
and good client satisfaction—even among
clients with complex, challenging clinical and
psychosocial histories (e.g., presence of PTSD,
polysubstance misuse, childhood maltreatment,
adolescent substance misuse, unstable housing,
reliance on public assistance, being unemployed
or out of school).
•
In a variety of criminal justice–related settings,
such as prebooking diversion programs, drug
or mental health courts, in jails or prisons, and
as a part of community release (Peters et al.,
2017; Rojas & Peters, 2015). Integrated COD
care has been linked to desirable outcomes
such as improved psychiatric symptoms,
reduced substance use, and decreased rates of
reoffending and recidivism.
Chapter 7 189
TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
RESOURCE ALERT: IMPLEMENTING INTEGRATED CARE FOR PEOPLE WITH
CODs
•
SAMHSA’s Integrated Treatment for Co-Occurring Disorders Evidence-Based Practices KIT
(https://store.samhsa.gov/product/Integrated-Treatment-for-Co-Occurring-Disorders-Evidence-Based-
Practices-EBP-KIT/SMA08-4366)
• Case Western Reserve’s Center for Evidence-Based Practices. Integrated Dual Disorder Treatment
Clinical Guide (www.centerforebp.case.edu/client-files/pdf/iddtclinicalguide.pdf)
•
With people experiencing homelessness
(Polcin, 2016; Smelson et al., 2016). In these
populations, integrated COD treatment can
help reduce substance use and mental illness
symptoms while, depending on the housing
service model used, also increasing housing
stability and retention.
Assertive Community Treatment
Developed in the 1970s by Stein and Test (Stein &
Test, 1980; Test, 1992) for clients with SMI, the ACT
model was designed as an intensive, long-term
approach to providing services for those who
were reluctant to engage in traditional treatment
approaches and who required significant outreach
and engagement activities. ACT has evolved and
been modified to address the needs of individuals
with mental disorders (especially SMI) and co-
occurring SUDs (De Witte et al., 2014; Fries &
Rosen, 2011; Manuel, Covell, Jackson, & Essock,
2011; Young, Barrett, Engelhardt, & Moore, 2014).
Program Model
ACT programs typically use intensive outreach
activities, active and continued engagement
with clients, and a high intensity of services.
Multidisciplinary teams, including specialists in key
areas of treatment, provide a range of services to
clients. Members typically include mental health
and SUD treatment counselors, case managers,
nursing staff, and psychiatric consultants. The ACT
team provides the client with practical assistance in
life management as well as direct treatment, often
within the client’s home environment, and remains
responsible and available 24 hours a day (SAMHSA,
2008). The team has the capacity to intensify
services as needed and may make several visits
each week (or even per day) to a client. Caseloads
are kept smaller than other community-based
treatment models to accommodate the intensity
of service provision (a 1:10 staff-to-client ratio is
typical).
ACT Activities and Interventions
Examples of ACT interventions include (Bond &
Drake, 2015; SAMHSA, 2008):
•
Outreach/engagement. To involve and
sustain clients in treatment, counselors and
administrators must develop multiple ways
to attract, engage, and reengage clients.
Expectations for clients are often minimal to
nonexistent, especially in programs serving very
resistant or hard-to-reach clients.
•
Practical assistance in life management. This
feature incorporates case management activities
that facilitate linkages with support services in
the community, including employment services.
Whereas the role of a counselor in the ACT
approach includes standard counseling, in many
instances substantial time also is spent on life
management and behavioral management
matters.
•
Tangible support. For some clients, especially
with SMI, help with logistical and everyday
functional needs is critical to ensuring treatment
access, engagement, participation, and
retention. Supportive care can include assistance
with housing, benefits/insurance, transportation,
and child care.
•
Counseling. The nature of the counseling
activity is matched to the client’s motivation and
readiness for treatment. Interventions may also
involve family and other support networks as
appropriate.
190 Chapter 7

TIP 42
Chapter 7—Treatment Models and Settings for People With Co-Occurring Disorders
NINE ESSENTIAL FEATURES OF
ACT
1. Services that are provided in the community
rather than in clinic offices
2. Assertive engagement with active outreach
3. Holistic approaches that address clients’
symptoms, medication needs, housing
difficulties, financial needs, and other areas of
daily living (e.g., transportation)
4. A multidisciplinary team of mental health
service and SUD treatment professionals
(e.g., counselors, psychiatrists, social workers,
psychiatric and mental health nurses
[specialty practice registered nurses], case
managers)
5. Providing clients with services directly rather
than utilizing referrals to other professionals
6. Integrated services that are tailored to
comprehensively and simultaneously address
a client’s full range of clinical, functional,
vocational, social, and everyday living needs
7. A low client–provider ratio (usually about 10
clients per provider)
8. Continuous care, including 24/7 emergency
services
9. Focus on helping to support long-term rather
than acute recovery
Source: Bond & Drake (2015).
•
Crisis assessment and intervention. This is
provided during extended service hours (24
hours a day, ideally through a system of on-call
rotation).
Key Modications for Integrating COD
Treatment
As applied to CODs, the goals of the ACT model
are to engage the client in a helping relationship,
to assist in meeting basic needs (e.g., housing),
to stabilize the client in the community, and to
provide direct and integrated SUD treatment and
mental health services. The standard ACT model
as developed by Test (1992) has been modified
to include treatment for people who have SUD as
well as SMI (Bond & Drake, 2015) and to address
common needs within the COD community (e.g.,
housing needs, criminal justice–related needs). Key
elements in this evolution have been (Neumiller et
al., 2009):
•
Offering direct SUD interventions for clients
with CODs (often through the inclusion of an
addiction counselor on the multidisciplinary
team) or, if not possible, referral to SUD
treatment.
•
Using a COD-based model of care that focuses
on specialized services, a nonconfrontational
and supportive milieu, and recovery-oriented
stages of care.
•
Providing higher intensity of services via “mini-
teams” of case managers, mental health service
and SUD treatment providers, and consumer
advocates.
•
Adapting ACT to support housing placement,
such as:
- Integrating a Housing First (HF) model of
supportive permanent housing.
- Including outreach workers and assistants to
give providers more time with clients.
- Placing time limits on services to encourage
client engagement in interventions that
support independent living (like employment
and vocational training).
- Monitoring psychiatric symptoms and
medication response.
- Offering SUD treatment/education.
- Adding residential housing as a temporary
solution for clients in the process of obtaining
independent stable housing.
•
Modifying for criminal justice settings/
populations (Lamberti et al., 2017; Landess &
Holoyda, 2017; Marquant, Sabbe, Van Nuffel,
& Goethals, 2016) by collaborating with
and including criminal justice agencies and
professionals (e.g., probation officers) in the
ACT team; using court sanctions or other legal
leverage to increase motivation and treatment
participation/retention; applying forensic
rehabilitation strategies to target factors
associated with reoffending and recidivism;
and educating and training providers in unique
aspects of criminal justice–mental health
collaboration.
Chapter 7 191

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
SUD treatment strategies are related to the client’s
motivation and readiness for treatment and include:
•
Enhancing motivation (for example, through use
of motivational interviewing).
•
Cognitive–behavioral skills for relapse prevention.
•
Mutual-support programming, including peer
recovery supports to strengthen recovery.
•
Psychoeducational instruction about addictive
disorders.
For clients uninterested in abstinence, motivational
approaches to ACT can highlight the detrimental
effects of substance use on their lives and those of
the people around them. Therapeutic interventions
are then modified to meet the client’s current stage
of change and receptivity. Learn more in Chapter
5 and in TIP 35, Enhancing Motivation for Change
in Substance Use Disorder Treatment (SAMHSA,
2019c).
Populations Served
When modified as described previously for CODs,
the ACT model is capable of including clients with
greater mental and functional disabilities who
do not fit well into many traditional treatment
approaches. The characteristics of those served
by ACT programs for CODs include people with
an SUD and mental illness, SMI (e.g., intractable
depression, bipolar disorder, schizophrenia and
other psychotic disorders), serious functional
impairments, avoidance of or poor response to
traditional outpatient mental health services and
SUD treatment, homelessness, criminal justice
involvement, or some combination thereof.
Consequently, clients targeted for ACT often are
high users of expensive service delivery systems
(EDs and hospitals) as immediate resources for
mental health and SUD services.
Empirical Evidence for ACT
The ACT model has been researched widely as
a means of providing community-based services
to people with chronic mental illness. The low
caseload ratio and delivery of community-based
services, combined with intensive attention,
structure, monitoring, and outreach, are beneficial
for people with SMI, because SMI is typically
unstable and highly disabling. For instance,
a randomized trial of integrated ACT versus
standard case management found ACT significantly
improved medication adherence among people
with psychotic disorders and SUDs over a 3-year
period (Manuel et al., 2011).
Research on ACT for individuals with CODs has
been somewhat limited compared with research
on ACT for mental illness alone, and findings
to date have been mixed. ACT demonstrated
superiority to standard clinical case management
in reducing alcohol use and incarcerations among
people with CODs plus antisocial personality
disorder (PD) but not people with CODs without
antisocial PD (ASPD; Frisman et al., 2009).
However, this study used a small sample size
and lacks generalizability. ACT combined with
integrated dual disorder treatment (including from
an addiction specialist) for people with SMI and
SUD (Morse, York, Dell, Blanco, & Birchmier, 2017)
improved symptoms of SUDs and mental illness,
including decreasing alcohol use but not drug
use or overall substance use. In a SAMHSA grant-
funded program that provided ACT and integrated
COD treatment services to people experiencing
chronic homelessness (Young et al., 2014), ACT
was associated with improved housing stability,
global mental health, past-month depression and
anxiety, client self-esteem and decision-making
abilities, treatment satisfaction, and treatment
RESOURCE ALERT: IMPLEMENTING ACT FOR PEOPLE WITH CODs
•
SAMHSA’s ACT for Co-Occurring Disorders Evidence-Based Practices KIT
(https://store.samhsa.gov/product/Assertive-Community-Treatment-ACT-Evidence-Based-Practices-EBP-
KIT/sma08-4344)
• Georgia Department of Behavioral Health & Developmental Disabilities Program Tool Kit for ACT
(https://dbhdd.georgia.gov/sites/dbhdd.georgia.gov/files/related_files/document/Georgia%20Toolkit%20
for%20ACT%20Teams%20docxfinal%202015.pdf)
192 Chapter 7

TIP 42
Chapter 7—Treatment Models and Settings for People With Co-Occurring Disorders
engagement but not self-reported alcohol or illicit
drug use. In a review of outpatient treatments for
schizophrenia and SUD (De Witte et al., 2014),
integrated ACT outperformed treatment as usual
in terms of substance use, hospitalizations, stable
housing, and negative and disorganized symptoms
of psychosis but was no better than integrated
case management at reducing substance use and
improving psychiatric symptom severity.
These mixed findings are likely due in part to ACT’s
unproven ability to ameliorate SUDs. A review of
randomized clinical trials of ACT for substance
misuse (Fries & Rosen, 2011) found that it helped
reduce alcohol and drug use over time when
supplemented with SUD treatment. But effects
were small, and reductions in substance use were
typically no better than those from other treatment
approaches (e.g., case management). This suggests
that traditional ACT is likely not an effective
addiction management tool on its own but when
used with adjunctive SUD treatment (e.g., inclusion
of addiction counselors, use of contingency
management for abstinence) may be as effective as
case management at improving substance-related
outcomes. Nevertheless, based on the weight
of evidence, ACT is a recommended treatment
model for clients with CODs, especially when
used as an integrated treatment with adjunct
substance use services.
Examples of ACT Programs
The University of Washington Program for ACT
The University of Washington’s Program for ACT
(PACT) was established to provide outreach-based
services to clients with mental and addiction needs,
particularly people with SMI and SUDs. Washington
PACT teams carry a low caseload (1:10 provider–
client ratio) and use high-intensity, multidisciplinary
services (e.g., 24/7 care, treatments predominantly
offered in the community), including CBT, SUD
treatment, family psychoeducation, motivational
interviewing, pharmacotherapy, relapse prevention,
crisis management, psychiatric rehabilitation,
community outreach, social skills training, and
supported education/employment services. The
program currently has 15 teams located throughout
Washington State. Program reports indicate up to
60 percent of Washington PACT team clients have
CODs.
RESOURCE ALERT: UNIVERSITY
OF WASHINGTON PACT
IMPLEMENTATION AND
ENGAGEMENT TOOLS
The PACT program website lists resources to
help programs implement ACT and improve
client engagement (https://depts.washington.
edu/ebpa/projects/revised_comprehensive_
assessment_r-ca). Resources include:
• A blank weekly client schedule form.
• A sample daily staff schedule.
• A sample client contact log.
• An ACT Transition Assessment Scale to assess
client readiness to step down to less intensive
services.
• The PACT Comprehensive Assessment Scale,
used to help programs assess the client/family
needs and determine which program services
would best serve the client.
• A sample case study.
• Putting It Together Worksheet, used to
summarize content from assessment and
develop a treatment plan.
• Checklist of areas for further assessment and
tools for follow-up assessment.
• Links to specific assessment tools for:
− PTSD.
− Suicide risk.
− Alcohol use disorder (AUD).
− SUD.
− Client ambivalence to change.
− Recovery assessment.
− Strengths assessment.
− Nicotine use.
− Psychiatric rehabilitation.
Mercy Maricopa ACT Program
Mercy Maricopa, an integrated physical and
behavioral health Medicaid managed care
plan, offers an ACT program of 23 ACT teams
Chapter 7 193

TIP 42 Substance Use Disorder Treatment for People With Co-Occurring Disorders
(including 3 forensic ACT programs) specifically
focused on people with SMI. ACT teams provide
comprehensive, multidisciplinary wraparound
care including psychiatric and SUD treatment,
medication management, case management, social
services, vocational rehabilitation, housing and
vocational assistance, and peer support.
A healthcare analysis from 2018 (NORC, 2018)
found that, pre–post enrollment in the ACT
program, clients incurred significantly lower
overall facility costs ($608 less per member per
quarter), overall professional service costs ($485
less), behavioral health service costs ($410 less),
and total behavioral health costs ($808 less). Total
spending from pre- to postprogram participation
decreased by $734 but was not significant.
Pharmacy expenditures were significantly higher
following ACT program participation ($246 more).
ACT clients had significantly less ED utilization and
fewer psychiatric hospitalizations from baseline
to postprogram participation. Compared to a
matched comparison group not participating in the
ACT program, ACT clients had significantly lower
rates of ED utilization.
Integrated Case Management
The earliest model of case management was
primarily a brokerage model. Linkages to services
were based on clients’ individual needs, but case
managers provided no formal clinical services.
Over time, it became apparent that providers
could provide more effective case management
services. Thus, clinical case management largely
supplanted the brokerage model. ICM emerged as
a strategy in the late 1980s and early 1990s. It was
designed as a thorough, long-term service to assist
clients with SMI (particularly those with mental and
functional disabilities and a history of not adhering
to prescribed outpatient treatment) by establishing
and maintaining linkages with community-based
service providers.
ICM is not a precisely defined term but rather is
used in the literature to describe an alternative to
both traditional case management and ACT. The
goals of the ICM model are to engage individuals
in a trusting relationship, assist in meeting their
basic needs (e.g., housing), and help them access
and use brokered services in the community. The
fundamental element of ICM is a low caseload
per case manager, which translates into more
intensive and consistent services for each client.
TIP 27, Comprehensive Case Management for
Substance Abuse Treatment (Center for Substance
Abuse Treatment [CSAT], 2000b), contains more
information on the history of case management,
both how it has developed to meet the needs of
clients in SUD treatment (including clients with
CODs) and specific guidelines about how to
implement case management services.
Program Model
ICM programs typically involve outreach and
engagement activities, brokering of community-
based services, direct provision of some support/
counseling services, and a higher intensity of
services than standard case management. The
integrated case manager assists the client in
selecting services, facilitates access to these
services, and monitors the client’s progress through
services provided by others (inside or outside the
program structure or by a team). Client roles in
this model include serving as a partner in selecting
treatment components.
In some instances, the ICM model uses
multidisciplinary teams similar to ACT. The
composition of the ICM team is determined by the
resources available in the agency implementing
the programs. The team often includes a
cluster-set of case managers rather than the
specialists prescribed as standard components
of the treatment model. The ICM team may
offer services provided by ACT teams, including
practical assistance in life management (e.g.,
housing) and some direct counseling or other
forms of treatment. Caseloads are kept smaller
than those in other community-based treatment
models (typically, the client–counselor ratio
ranges from 15:1 to 25:1) but larger than those in
the ACT model. Because the case management
responsibilities are so wide ranging and require a
broad knowledge of local treatment services and
systems, a typically trained counselor may require
some retraining or close, instructive supervision in
order to serve effectively as a case manager.
194 Chapter 7

TIP 42
Chapter 7—Treatment Models and Settings for People With Co-Occurring Disorders
ADVICE TO ADMINISTRATORS:
TREATMENT PRINCIPLES FROM
ICM
•
Select clients with more mental/functional
disabilities who are resistant to traditional
outpatient treatment.
• Use a low caseload per case manager to
accommodate more intensive services.
• Assist in meeting basic needs (e.g., housing).
• Facilitate access to and utilization of brokered
community-based services.
• Provide long-term support, such as counseling
services.
• Monitor the client’s progress through services
provided by others.
• Use multidisciplinary teams.
Treatment Activities and Interventions
Examples of ICM activities and interventions
include:
•
Engaging the client in an alliance to facilitate
the process and connecting the client with
community-based treatment programs.
•
Assessing needs, identifying barriers to
treatment, and facilitating access to treatment.
•
Offering practical help with life management;
facilitating linkages with community support
services.
•
Making referrals to treatment programs offered
by others in the community; see also TIP 27
(CSAT, 2000b) for guidance on establishing
linkages for service provision and interagency
cooperation.
•
Advocating for the client with treatment
providers and service delivery systems.
•
Monitoring progress.
•
Providing counseling and support to help the
client maintain stability in the community.
•
Crisis intervention.
•
Assisting in integrating treatment services by
facilitating communication between service
providers.
Key Modications of ICM for CODs
Key ICM modifications from basic case manage-
ment for clients with CODs include:
•
Using direct interventions for clients with CODs,
such as enhancing motivation for treatment
and discussing the interactive effects of mental
disorders and SUDs.
•
Making referrals to providers of integrated
SUD treatment and mental health services
or, if integrated services are not available or
accessible, facilitating communication between
separate brokered mental health service and
SUD treatment providers.
•
Coordinating with community-based services
to support the client’s involvement in mutual-
support groups and outpatient treatment
activities.
Empirical Evidence
Most published literature on ICM has focused on
mental illness, with fewer U.S. studies examining
SUD or CODs. ICM may help people with SMI
reduce hospitalizations, stay in treatment longer,
and improve social functioning. But many of these
studies are considered to be of low quality (e.g.,
small sample sizes, flawed methodology or study
design), and findings are not consistently better
than those from standard care or other non-ICM
approaches (Dieterich et al., 2017). Some research-
ers have reported positive effects of ICM for SMI in
terms of:
•
Increasing social integration among people in
supported housing and acquisition of Section 8
housing vouchers (Tsai & Rosenheck, 2012).
•
Improving physical health (e.g., weight, blood
pressure) among veterans (Harrold et al., 2018).
•
Reducing mental illness hospitalizations (by 70
percent); average number of days hospitalized for
mental illness (by 75 percent); and average 30-day
inpatient psychiatric service costs, outpatient
psychiatric service costs, and outpatient medical
service costs (Kolbasovsky, 2009).
Studies of ICM and substance use in U.S.
populations are tentatively positive, but the
research is limited in number and generalizability. In
women with substance misuse receiving Temporary
Assistance for Needy Families (Morgenstern et al.,
Chapter 7 195

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
2009), ICM was associated with greater rates of
short-term and long-term abstinence and a greater
likelihood of being employed full time than was
usual care (i.e., screening and referral). In a related
study, Kuerbis, Neighbors, and Morgenstern
(2011) observed paradoxical moderating effects of
depression on ICM substance use outcomes such
that women with substance misuse and higher
scores of depression who participated in the ICM
program had better SUD treatment engagement
and fewer drinks per drinking days than women
in the program with lower scores of depression.
Women with higher depression also exhibited
higher or equal rates of SUD treatment attendance
and percentage of days abstinent than less-
depressed women. Hence, the ICM program was
effective at improving addiction outcomes and may
be especially so among women with comorbid high
depression.
Regarding CODs, ICM appears effective in
specific populations (e.g., veterans, people with
housing needs, individuals in the criminal justice
system), although the magnitude of effect of these
programs is unclear, as is whether they are superior
to ACT or other approaches. A rural-based ICM for
people with and without CODs (Mohamed, 2013)
helped more military veterans with CODs engage
in rehabilitation, housing, vocational, and addiction
services than it did veterans without CODs. The
ICM program was associated with improvements
in mental disorder symptoms, distress, quality
of life, treatment satisfaction, income, and days
employed; however, there were no differences in
any of these variables between veterans with and
without CODs.
Malte, Cox, and Saxon (2017) also examined
veterans receiving ICM but with a focus on
promoting housing stability and addiction recovery.
Almost 60 percent of program participants had a
comorbid depressive disorder, 43 percent PTSD, 31
percent an anxiety disorder, 21 percent a psychotic
disorder, and 19 percent a bipolar disorder. Over
time, participants increased their percentage of
days spent in their own home or in transitional
housing; decreased days spent homeless or living
with others; increased rates of 30-day abstinence;
and improved their Addiction Severity Index (ASI)
scores (legal, drug, and psychiatric composite
scales). However, none of these improvements
were significantly different from those observed in
the control condition (a housing support group).
Nevertheless, the addiction/housing ICM program
was associated with more days spent in SUD
treatment (almost 53 days longer than controls),
greater treatment participation, and higher
treatment satisfaction.
The Northern Kentucky Female Offender Reentry
Project (McDonald & Arlinghaus, 2014) examined
ICM among incarcerated women with SMI, SUDs,
or both (78 percent had a COD). Compared with
women who only participated in the program while
incarcerated, women who participated during
imprisonment and after release demonstrated
better outcomes in educational attainment (e.g.,
obtaining a General Equivalency Degree, enrolling
in college after release), obtaining part- or full-time
work, SUD treatment and mental health service
engagement, and recidivism.
Examples of ICM Programs
SAMHSA’s Cooperative Agreement to Benet
Homeless Individuals
SAMHSA’s Cooperative Agreement to Benefit
Homeless Individuals (CABHI) programs use
integrated approaches, including ICM, to address
addiction, mental illness, and medical, housing, and
employment needs. Funding is administered as part
of SAMHSA’s Recovery Support Strategic Initiative,
with the overarching goal of helping people with
SUDs, SMI, or CODs reduce the experience of
homelessness (e.g., via subsidized and supportive
housing). The program was initiated in 2011 to
provide funding to public and nonprofit entities
and was expanded in 2013 to offer funds to help
establish or enhance statewide service infrastructure
and planning. It again expanded in 2016 to include
more communities (including tribal communities)
and nonprofit organizations. Integrated services
offered by CABHI programs include community
outreach; screening, assessment, and treatment for
addictions, mental illness, or both; peer recovery
support services; and ICM.
The Extended Hope Project in Yolo County,
California, is a CABHI recipient (2016–2019)
offering integrated treatments to improve housing
stability, behavioral and physical health, and
criminal justice status for people in Yolo County
with CODs who are experiencing homelessness.
196 Chapter 7

TIP 42
Chapter 7—Treatment Models and Settings for People With Co-Occurring Disorders
The program includes:
•
A screening, assessment, and triage service
to link clients with outreach workers to assess
clients for needed services and enroll them in
case management.
•
An ICM and treatment team, including case
managers, who responded to crisis needs,
worked with clients on shared treatment
decision making, and helped develop tailored
treatment plans; peer recovery support
specialists, who provided mentorship, support,
and education; and an employment specialist to
aid with job placement.
•
Collaboration with a housing navigator to
help connect clients with permanent housing
placement and teach eviction prevention
strategies.
Pathways to Housing, Inc.’s HF Programs
The HF program uses the supportive permanent
housing model (see Chapter 6) to help people with
CODs obtain stable housing and prevent future
homelessness (Tsemberis, 2010). Originally launched
in New York City in 1992, programs now also exist
in Washington, DC, Vermont, Pennsylvania, and
Canada. HF programs do not require clients to
achieve abstinence before enrolling and instead
integrate SUD and mental disorder treatment with
housing support services (e.g., ACT or ICM).
The Tulsa Housing and Recovery Program, a
recipient of the SAMHSA Services in Supportive
Housing 5-year grant in 2009, is a collaboration
between community mental health centers and
housing providers that offers SUD treatment,
mental health services, and supportive housing (via
the HF model) to individuals with CODs who are
experiencing homelessness. Integrated services
and ICM are key components of the program. From
2009 to 2013, the program reported numerous
improved outcomes (Shinn & Brose, 2017),
including the following:
•
94 percent of clients retained in housing (i.e.,
continuously housed for 12 months or longer)
•
72 percent of clients reduced their substance
use at 6 months
•
70 percent scored at minimal or no risk for
substance misuse at 6 months
•
69 percent reported at least 3 months of
abstinence
•
79 percent had a reduction in self-reported
trauma symptoms at 6 months
•
81 percent achieved trauma-related treatment
gains in 6 months
•
100 percent of clients were successfully linked
to healthcare services through peer support and
nurse-led assessment and triage
Comparison of ACT and ICM
Both ACT and ICM share the following key activi-
ties and interventions:
•
Focus on increased treatment participation
•
Client management
•
Abstinence as a long-term goal, with short-term
supports
•
Stagewise motivational interventions
•
Psychoeducational instruction
•
Cognitive–behavioral relapse prevention
•
Encouraging participation in mutual-support
programs
•
Supportive services
•
Skills training
•
Crisis intervention
•
Individual counseling
Dierences Between ACT and ICM
ACT is more intensive than most ICM approaches.
The ACT emphasis is on developing a therapeutic
alliance with the client and delivery of service
components in the client’s home, on the street, or in
program offices (based on the client’s preference).
ACT services are provided predominantly by the
multidisciplinary staff of the ACT team, and the
program often is located in the community (Bond &
Drake, 2015; Ellenhorn, 2015). Most ACT programs
provide services 16 hours a day on weekdays,
8 hours a day on weekends, plus on-call crisis
intervention, including visits to the client’s home
at any time, day or night, with the capacity to
make multiple visits to a client on any given day.
Caseloads usually are 10:1. ICM programs typically
include fewer hours of direct treatment, but they
may include 24-hour crisis intervention; the focus of
ICM is on brokering community-based services for
the client. ICM caseloads range up to 25:1.
Chapter 7 197

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
The ACT multidisciplinary team shares responsibility
for the entire defined caseload of clients and meets
frequently (ideally, teams meet daily) to ensure that
all members are fully up-to-date on clinical matters.
Although team members may play different roles,
all are familiar with every client on the caseload.
The nature of ICM team functioning is not as
defined, and cohesion is not necessarily a focus of
team functioning; the ICM team can operate as a
loose organization of independent case managers
or as a cohesive unit in a manner similar to ACT.
Also, the ACT model can include the clients’ family
within treatment services (White, McGrew, Salyers,
& Firmin, 2014), which is not always true for ICM
models.
ICM most frequently involves the coordination of
services across different systems over extended
periods of time, whereas ACT integrates and
provides treatment for CODs within the team. As
a consequence, advocacy with other providers
is a major component of ICM, but advocacy
in ACT focuses on ancillary services. The ACT
multidisciplinary team approach to treatment
emphasizes providing integrated treatment for
clients with CODs directly, assuming that the team
members include both mental health and SUD
treatment counselors and are fully trained in both
approaches.
Recommendations for Extending ACT and
ICM in SUD Treatment Settings
ACT and ICM models translate easily to SUD
treatment. The consensus panel offers five recom-
mendations for successful use of ACT and ICM in
SUD treatment with clients who have CODs:
1. Use ACT and ICM for clients who require
considerable supervision and support. ACT
is a treatment alternative for those clients
with CODs who have a history of sporadic
adherence with continuing care or outpatient
services and who require extended monitoring
and supervision (e.g., medication monitoring
or dispensing) and intensive onsite treatment
supports to sustain their tenure in the
community (e.g., criminal justice clients). For this
subset of the COD population, ACT provides
accessible treatment supports without requiring
return to a residential setting. The typical ICM
program is capable of providing less intense
levels of monitoring and supports, but can still
provide these services in the client’s home on a
more limited basis.
2. Develop ACT programs, ICM programs, or
both selectively to address the needs of
clients with SMI who have difficulty adhering
to treatment regimens most effectively.
ACT, which is a more complex and expensive
treatment model to implement than ICM,
has been used for clients with SMI who have
difficulty adhering to a treatment regimen.
Typically, these are among the highest users
of expensive (e.g., ED, hospital) services. ICM
programs can be used with treatment-resistant
clients who are clinically and functionally
capable of progressing with much less intensive
onsite counseling and less extensive monitoring.
3. Extend and modify ACT and ICM for other
clients with CODs in SUD treatment. With
their strong tradition in the mental health field,
particularly for clients with SMI, ACT and ICM
are attractive, accessible, and flexible treatment
approaches that can be adapted for individuals
with CODs. Components of these programs can
be integrated into SUD treatment programs.
4. Add SUD treatment components to existing
ACT and ICM programs. Incorporating
methods from the SUD treatment field, such as
substance use education, peer mutual support,
and greater personal responsibility, can continue
to strengthen the ACT approach as applied to
clients with CODs. The degree of integration of
substance use and mental health components
within ACT and ICM depends on the ability of
the individual case manager/counselor or the
team to provide both services directly or with
coordination.
5. Extend the empirical base of ACT and ICM
to further establish their effectiveness for
clients with CODs in SUD treatment settings.
The empirical base for ACT derives largely from
application among people with SMI and needs
to be extended to establish firm support for the
use of ACT across the entire COD population.
In particular, adding an evaluation component
to new ACT programs in SUD treatment can
provide documentation currently lacking in
198 Chapter 7

TIP 42
Chapter 7—Treatment Models and Settings for People With Co-Occurring Disorders
VOCATIONAL SERVICES AND TREATMENT MODELS
Vocational rehabilitation has long been one of the services offered to clients recovering from mental
disorders and, to some degree, to those recovering from SUDs. The fact is that many individuals with CODs
are not working, including 9 percent who are unemployed and 23 percent not in the labor force for other
reasons (e.g., disabled, retired, in school) (Center for Behavioral Health Statistics and Quality, 2019). However,
it is unreasonable to expect employers to tolerate employees who are actively using alcohol on the job or
who violate their drug-free workplace policies.
Vocational support is vital because steady and unsteady work among people with CODs has been linked
to improvement in symptoms, achieving independent housing, and enhanced quality of life (McHugo,
Drake, Xie, & Bond, 2012). Vocational programs and supported employment can help clients with CODs
gain competitive employment, more work hours, and increased earnings (Frounfelker, Wilkniss, Bond,
Devitt, & Drake, 2011; Luciano & Carpenter-Song, 2014; Marshall et al., 2014; Mueser, Campbell, & Drake, 2011).
Therefore, if work is to become an achievable goal for individuals with CODs, vocational rehabilitation and
supported employment should be integrated into comprehensive COD recovery services.
Vocational services can be incorporated into many treatment models, including ACT and ICM. For more
information about incorporating vocational rehabilitation into treatment, see TIP 38, Integrating Substance
Abuse Treatment and Vocational Services (SAMHSA, 2000).
the field concerning the effectiveness and cost
benefit of ACT in treating the person who
misuses substances with co-occurring mental
disorders in SUD treatment settings. The
limitations of ICM have been listed in previous
sections. Providers should use ACT or ICM to
meet clients’ needs as indicated by assessment.
Dual Recovery Mutual-Support Programs
The dual recovery mutual-support movement is
emerging from two cultures: the 12-Step recovery
movement and, more recently, the culture of the
mental health consumer movement. This section
describes both, as well as other, consumer-driven
psychoeducational efforts.
In the past decade, mutual-support approaches
have emerged for people with CODs. Mutual-
support programs apply a broad spectrum
of personal responsibility and peer support
principles, usually including 12-Step programs.
These programs are gaining recognition as more
meetings are being held in both agency and
community settings throughout the United States,
Canada, and abroad.
In recent years, dual recovery mutual-support
organizations have emerged as a source of support
for people in recovery from CODs (Bogenschutz
et al., 2014b; Monica, Nikkel, & Drake, 2010;
Zweben & Ashbrook, 2012). Mental health
advocacy organizations—including the National
Alliance for the Mentally Ill and the National
Mental Health Association—offer resources to help
locate dual recovery mutual-support organizations
(see “Resource Alert: Locating Mutual-Support
Groups for People With CODs” and Appendix B).
At the federal level, SAMHSA also has produced
documents identifying dual recovery mutual-
support organizations (Center for Mental Health
Services, 1998; CSAT, 1994).
Several areas inform the rationale for establishing
dual recovery programs as additions to mutual-sup-
port programs (Bogenschutz et al., 2014b; Timko,
Sutkowi, & Moos, 2010; Zweben & Ashbrook,
2012):
•
Stigma and prejudice: Stigma related to
both SUDs and mental illness continues to
be problematic, despite the efforts of many
advocacy organizations. Unfortunately, these
negative attitudes may surface within a meeting.
When this occurs, people in dual recovery may
find it difficult to maintain a level of trust and
safety in the group setting.
•
Inappropriate or controversial advice
(confused bias): Many members of addiction
Chapter 7 199

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
recovery groups recognize the real problem of
cross-addiction and are aware that people use
certain prescription medications as intoxicating
drugs. Confusion about the appropriate role of
psychiatric medication exists, and as a result,
some members may offer well-intended, but
inappropriate, advice by cautioning newcomers
against using medications. Clearly, confused bias
against medications may create either of two
problems. First, newcomers may follow inappro-
priate advice and stop taking their medications,
causing a recurrence of symptoms. Second,
newcomers quickly may recognize confused
bias against medications within a meeting, feel
uncomfortable, and keep a significant aspect of
their recovery a secret.
•
Interpersonal connectedness: Individuals with
CODs often experience difficulty establishing
and maintaining close personal relationships.
The presence of a mental disorder could make
establishing rapport and developing an alliance
with mutual-support program members and
sponsors more difficult, subsequently hindering
participation and causing clients to feel reluctant
about sharing their stories and struggles with
others who are only facing addiction rather than
both illnesses.
•
Direction for recovery: A strength of traditional
mutual-support program fellowships is their
ability to offer direction for recovery that is
based on years of collective experience. The
new dual recovery programs offer an oppor-
tunity to begin drawing on the experiences
that members have encountered during both
the progression of their CODs and the process
of their dual recovery. In turn, that body of
experience can be shared with fellow members
and newcomers to provide direction into the
pathways to dual recovery.
•
Acceptance: Mutual-support program fellow-
ships provide meetings that offer settings for
recovery. Dual recovery meetings may offer
members and newcomers a setting of emotional
acceptance, support, and empowerment. This
condition provides opportunities to develop
a level of group trust in which people can feel
safe and able to share their ideas and feelings
honestly while focusing on recovery from both
illnesses.
Although a dual-focused mutual-support program
is clearly preferable, people with CODs can still
derive benefit from attending traditional mutual-
support groups, such as Alcoholics Anonymous
(AA). A meta-analysis of 22 studies examining AA
attendance by people with CODs (Tonigan, Pearson,
Magill, & Hagler, 2018) found a significant effect of
increased alcohol abstinence compared with people
with CODs who did not attend AA. Attending and
being involved in AA and other non-COD-based
mutual-support groups appears to help young
adults with CODs improve abstinence, although
rates of abstinence may not improve as significantly
as in young adults with SUDs alone (Bergman,
Greene, Hoeppner, Slaymaker, & Kelly, 2014).
Dual Recovery Mutual-Support Approaches
Dual recovery mutual-support program fellowship
groups recognize the unique value of people
in recovery sharing their personal experiences,
strengths, and hope to help other people in
recovery. This section provides an overview
of emerging mutual-support fellowships
and describes a model mutual-support
psychoeducational group.
Mutual-Support Groups
Four dual recovery mutual-support organizations
have gained recognition in the field. Each
fellowship is an independent and autonomous
membership organization with its own principles,
steps, and traditions. Dual recovery fellowship
members are free to interpret, use, or follow the
program in a way that meets their own needs.
Members use the program to learn how to manage
their addiction and mental disorders together. The
following section provides additional information
on the mutual-support model. (See also “Resource
Alert: Locating Mutual-Support Groups for People
With CODs.”)
1. Double Trouble in Recovery (DTR). This
organization provides 12 Steps that are based
on a traditional adaptation of the original 12
Steps. For example, the identified problem in
Step 1 is changed to CODs, and the population
to be assisted is changed in Step 12 accordingly.
The organization provides a format for meetings
that are chaired by members of the fellowship.
200 Chapter 7

TIP 42
Chapter 7—Treatment Models and Settings for People With Co-Occurring Disorders
2. Dual Disorders Anonymous. This organization
follows a similar format to DTR. It provides a
meeting format that is used by group members
who chair the meetings.
3. Dual Recovery Anonymous. This organization
provides 12 Steps adapted and expanded
from the traditional 12 Steps, similar to DTR
and Dual Disorders Anonymous. The terms
“assets” and “liabilities” are used instead of the
traditional term “character defects.” In addition,
it incorporates affirmations into 3 of the 12
Steps. Similar to other dual recovery fellowships,
this organization provides a suggested meeting
format that is used by group members who chair
the meetings.
4. Dual Diagnosis Anonymous. This organization
provides a hybrid approach that uses 5 addi-
tional steps in conjunction with the traditional
12 Steps. The five steps differ from those of
other dual recovery groups in underscoring the
potential need for medical management, clinical
interventions, and therapies. Similar to other
dual recovery fellowships, this organization
provides a meeting format that is used by group
members who chair the meetings.
The dual recovery fellowships are membership
organizations rather than consumer service delivery
programs. The fellowships function as autonomous
networks, providing a system of support parallel
to traditional clinical or psychosocial services.
Meetings are facilitated by members, who
are responsible, and take turns “chairing” or
“leading” the meetings for fellow members and
newcomers. Meetings are not led by professional
counselors (unless a member is a professional
counselor and takes a turn at leading a meeting),
nor are members paid to lead meetings. However,
the fellowships may develop informal working
relationships or linkages with professional providers
and consumer organizations.
Dual recovery mutual-support program fellowships
do not provide specific clinical or counseling
interventions, classes on psychiatric symptoms,
or any services similar to case management. Dual
recovery fellowships maintain a primary purpose of
members helping one another achieve and maintain
dual recovery, prevent relapse, and carry the
message of recovery to others who experience dual
disorders. Dual recovery mutual-support program
members who take turns chairing their meetings are
members of their fellowship as a whole. Anonymity
of meeting attendees is preserved because group
facilitators do not record the names of their fellow
members or newcomers. Fellowship members carry
out the primary purpose through the service work of
their groups and meetings.
Groups provide various types of meetings, such
as step study meetings, in which the discussion
revolves around ways to use the fellowship’s 12
Steps for personal recovery. Another type of
meeting is a topic discussion meeting, in which
members present topics related to dual recovery
and discuss how they cope with situations by
applying the recovery principles and steps of their
fellowship. Hospital and institutional meetings
may be provided by fellowship members to
individuals currently in hospitals, treatment
programs, or criminal justice settings.
Fellowship members who are experienced in
recovery may sponsor newer members. Newcomers
may ask a member they view as experienced to help
them learn fellowship recovery principles and steps.
Outreach by fellowship members may provide
information about their organization to agencies
and institutions through inservice programs,
workshops, or other types of presentations.
Access and Linkage
The fellowships are independent organizations
based on 12-Step principles and traditions that
generally develop cooperative and informal
relationships with service providers and other
organizations. The fellowships can be seen as
providing a source of support that is parallel to
formal services, that is, participation while receiving
treatment and continuing care services.
Referral to dual recovery fellowships is informal:
•
An agency may provide a “host setting” for
one of the fellowships to hold its meetings. The
agency may arrange for its clients to attend the
scheduled meeting.
•
An agency may provide transportation for its
clients to attend a community meeting provided
by one of the fellowships.
Chapter 7 201
TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
RESOURCE ALERT: LOCATING MUTUALSUPPORT GROUPS FOR PEOPLE
WITH CODs
•
Dual Recovery Anonymous. Index of Registered Dual Recovery Anonymous 12-Step Meetings
(www.draonline.org/meetings.html)
• Faces & Voices of Recovery. Mutual Aid Groups for Co-Occurring Health Conditions, including groups
specifically for co-occurring mental disorders and SUDs (https://facesandvoicesofrecovery.org/resources/
mutual-aid-resources/)
• SAMHSA. Behavioral Health Treatment Services Locator. Self-Help, Peer Support, and Consumer Groups
(https://findtreatment.gov/)
•
An agency may offer a schedule of community
meetings provided by one of the fellowships as
a support to referral for clients.
Common Features of Dual Recovery Mutual-
Support Fellowships
Dual recovery fellowships tend to have the
following in common:
•
A perspective describing CODs and dual
recovery
•
A series of steps providing a plan to achieve and
maintain dual recovery
•
Literature describing the program for members
and the public
•
A structure for conducting meetings in a way
that provides a setting of acceptance and
support
•
Plans for establishing an organizational
structure to guide growth of membership,
that is, a central office, fellowship network of
area intergroups, groups, and meetings. An
“intergroup” is an assembly of people made up
of delegates from several groups in an area. It
functions as a communications link upward to
the central office or offices and outward to all
the area groups it serves.
Empirical Evidence
Empirical evidence suggests that participation in
mutual-support programs contributes substantially
to members’ progress in dual recovery and should
be encouraged. Specifically, studies have found the
following positive outcomes:
•
Among veterans with an SUD and depression,
lower scores of depression and lower future
alcohol use (Worley, Tate, & Brown, 2012)
•
Fewer days of alcohol and other substance
use, better scores of mental health, and fewer
self-reported substance-related problems
(Rosenblum et al., 2014; Woodhead, Cowden
Hindash, & Timko, 2013)
•
Greater treatment attendance and possibly
increased alcohol abstinence and decreased
drinks per drinking day over time (but not
necessarily better than usual care) (Bogenschutz
et al., 2014b)
Qualitative studies (Hagler et al., 2015; Matusow
et al., 2013; Penn, Brooke, Brooks, Gallagher, &
Barnard, 2016; Roush, Monica, Carpenter-Song,
& Drake, 2015) exploring perspectives of clients
with CODs who engage in mutual-support services
(e.g., 12-Step and SMART Recovery) also detail
numerous perceived benefits from these programs,
such as:
•
Fellowship building (e.g., meeting others with
similar problems).
•
Addressing spiritual needs/topics (this may be
considered a negative aspect by some clients).
•
Building camaraderie, affiliation, and a sense of
community.
Dual recovery mutual-support programs recognize the unique value of people in recovery sharing their
personal experiences, strengths, and hope to help other people in recovery.
202 Chapter 7

TIP 42
Chapter 7—Treatment Models and Settings for People With Co-Occurring Disorders
•
Having a “safe space” to share experiences
without fear of judgment or rejection.
•
Increased knowledge/insight about mental
illness and SUDs (especially how they
interrelate).
•
Learning skills and tools that facilitate recovery.
•
Feeling empowered.
•
Developing a sense of hope for recovery.
•
Access to therapy/therapeutic services that would
otherwise be inaccessible, given lack of insurance.
Peer Recovery Support Services
The inclusion of peer supports—people who have
experienced addiction, mental illness, or both
and are in recovery—in SUD and mental illness
recovery processes has increased substantially in
the past decade. Peer recovery support services
can help improve long-term recovery by increasing
abstinence, decreasing inpatient services and
hospitalization, and improving functioning (Bassuk,
Hanson, Greene, Richard, & Laudet, 2016; Chinman
et al., 2014; Davidson, Bellamy, Guy, & Miller, 2012;
Reif, Braude, et al., 2014).
Research suggests that peer-based services help
people with mental disorders and SUDs improve
clinical and functional outcomes (Acri, Hooley,
Richardson, & Moaba, 2017; Bassuk et al., 2016;
Chapman, Blash, Mayer, & Spetz, 2018; Chinman
et al., 2014; Reif, Braude, et al., 2014; SAMHSA,
2017). These include:
•
Rates of abstinence.
•
Number of days abstinent.
•
Relapse rates.
•
Treatment engagement.
•
Treatment retention.
•
Residential treatment use.
•
Rehospitalization.
•
Adherence to treatment plan.
•
Treatment completion.
•
Treatment satisfaction.
•
Relationships with treatment providers.
•
Housing stability.
•
Probation/parole status.
•
Number of criminal justice charges.
•
Recovery capital.
•
Mental disorder symptoms.
•
Knowledge about mental illness and SUDs.
•
Family functioning, including parenting abilities.
•
Access to social supports.
Little research has examined the use of peer
supports for CODs. Given the success of peer
services in promoting recovery and wellness in
people with either mental illness or addiction, it
is reasonable to hypothesize that peer support
could also be effective for individuals with both.
O’Connell, Flanagan, Delphin-Rittmon, & Davidson
(2017) found inclusion of peer supports for
people with co-occurring psychosis and substance
misuse significantly improved positive (but not
negative) symptoms of psychosis, number of
days of alcohol use, number of days experiencing
alcohol-related problems, self-rated importance
of getting treatment for alcohol misuse, feelings
of relatedness, social functioning, and inpatient
readmissions relative to a treatment as usual
condition. Evidence-based interventions for CODs,
such as ACT and integrated therapies, were not
originally designed to include peer support, but
more and more, peer providers are becoming a
formal part of COD treatment teams (Harrison,
Cousins, Spybrook, & Curtis, 2017). Including peers
in COD services might improve staff treatment
fidelity, which is critical for ensuring that evidence-
based services produce intended outcomes
(Harrison et al., 2017).
Treatment Settings
Therapeutic Communities
The goals of TCs are to promote abstinence from
alcohol and illicit drug use, and to effect a global
change in lifestyle, including attitudes and values.
The TC views substance misuse as a disorder
of the whole person, reflecting problems in
conduct, attitudes, moods, values, and emotional
management. Treatment focuses on abstinence,
coupled with social and psychological change
that requires a multidimensional effort, involving
intensive mutual support, typically in a residential
setting. Residential TC treatment duration is
typically 6 to 12 months, although treatment
duration has been decreasing under the influence
of managed care and other factors.
Chapter 7 203
TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
In a definitive book titled The Therapeutic
Community: Theory, Model, and Method, De Leon
(2000) provided a full description of the TC for
SUD treatment to advance research and guide
training, practice, and program development.
Descriptions of TCs also appear in the National
Institute on Drug Abuse (NIDA, 2015) Research
Report titled Therapeutic Communities (https://
d14rmgtrwzf5a.cloudfront.net/sites/default/files/
therapueticcomm_rrs_0723.pdf).
TCs have demonstrated positive outcomes in
substance misuse and SUD treatment retention (De
Leon, 2015; NIDA, 2015). A review of randomized
and nonrandomized trials of TCs (Vanderplasschen
et al., 2013) found that, compared with control
conditions, TCs gave advantages in employment,
psychological symptoms, and family/social
relationships. SUD outcomes were variable but
generally favored the TC condition. Relapse rates
among TC clients also varied widely but were
relatively high (25 percent to 55 percent returned
to substance use within 12 to 18 months), although
time to relapse was typically longer in TCs than in
control conditions. This is consistent with earlier
research from Malivert, Fatséas, Denis, Langlois,
& Auriacombe (2012) that associated TCs with
decreased substance use but high relapse rates.
Clients in TCs with lower relapse rates tended
to stay longer in treatment and continuing care
than people who relapsed more quickly. Forensic
outcomes were consistently positive for recidivism,
rearrests, and reincarceration, even over time (3
years and 5 years). Again, TCs plus continuing care
were associated with even greater improvements in
abstinence and rearrests than TCs only.
Modied TCs for Clients With CODs
The modified TC (MTC) approach adapts
the principles and methods of the TC to the
circumstances of the client with CODs. The
illustrative work in this area has been done
with people with CODs, both men and women,
providing treatment based on community-as-
method—that is, the community is the healing
agent. This section focuses on MTCs as a potent
residential model for SUD treatment; most of this
section applies to both TCs and other residential
SUD treatment programs.
WHAT MAKES TCs WORK?
It remains unclear how and why TCs are
effective at improving outcomes for people
recovering from addiction. Pearce and Pickard
(2013) suggest that TCs are effective because
of their ability to promote in clients a sense of
belongingness, which is associated with better
self-esteem and feelings of acceptance and
happiness. TCs promote belongingness through
high frequency of client contacts that are positive
in nature, that exhibit mutual concern for the
client’s wellbeing, and that occur over a long
period of time.
The other key mechanism is the ability of TCs
to promote in clients a sense of responsible
agency. This includes the ability to: (1) “reflect on
one’s behavior, make decisions about how one
wants to do things differently, form resolutions,
and commit to change” as well as (2) “to see this
resolution or commitment through: not to waver
from the chosen course, or, if one wavers, to find
a way to get back on track rather than sink into
despair” (Pearce & Pickard, 2013, p. 7). Responsible
agency has been linked to greater self-efficacy
and ability to change behaviors (and sustain
those new behaviors over time). TCs promote
responsible agency through motivational
interviewing; cognitive interventions like CBT
or dialectical behavior therapy; and by helping
clients understand the relationships between
thoughts, emotions, and behaviors.
Treatment Activities/Interventions
All program activities and interactions, singly and
in combination, are designed to produce change.
Interventions are grouped into four categories—
community enhancement (to promote affiliation
with the TC community), therapeutic/educative (to
promote expression and instruction), community/
clinical management (to maintain personal and
physical safety), and vocational (to operate the
facility and prepare clients for employment).
Implementation of the groups and activities listed
in Exhibit 7.2 establishes the TC community.
Although each intervention has specific individual
functions, all share community, therapeutic, and
educational purposes.
204 Chapter 7
TIP 42
Chapter 7—Treatment Models and Settings for People With Co-Occurring Disorders
EXHIBIT 7.2. TC Activities and
Components
•
Maintaining highly structured daily regimens
that include:
- Morning and evening house meetings
- Daily jobs/tasks
- Individual therapy sessions
- Group therapy sessions
- Seminars and education meetings
•
Adhering to clearly articulated expectations
(accompanied by rewards and punishments to
help shape adaptive behaviors)
•
Vocation or educational activities, or both
•
Social activities to increase bonding among
housemates and help client establish healthy,
supportive networks, such as:
- Group discussions, including group therapy,
to help change behaviors and cognitions and
build new skills
- Community meetings to review the rules,
goals, and procedures of the TC
- Education meetings (e.g., seminars)
- Role-playing activities
- Games and recreational activities
Source: NIDA (2015).
Key Modications
The MTC alters the traditional TC approach in
response to the client’s psychiatric and addic-
tion-related symptoms, cognitive impairments,
reduced level of functioning, short attention span,
and poor urge control. A noteworthy alteration
is the change from encounter group to conflict
resolution group. Conflict resolution groups have
the following features:
•
Staff led and staff guided throughout
•
Three highly structured and often formalized
phases:
- Feedback on behavior from one participant
to another
- Opportunity for both participants to explain
their position
- Resolution between participants with plans
for behavior change
•
Substantially reduced emotional intensity;
emphasis on instruction and learning of new
behaviors
•
Persuasive appeal for personal honesty,
truthfulness in dealing with others, and
responsible behavior to self and others
To create an MTC program for clients with CODs,
three fundamental alterations can be applied:
•
Increased flexibility
•
Decreased intensity
•
Greater individualization
More recent adaptations also can include:
•
Accepting clients on medication-assisted
treatment (MAT) for opioid use disorder (OUD)
and, in some cases, incorporating medication
into treatment plans (NIDA, 2015).
•
Placing greater limits on long-term residential
treatment, given rising healthcare costs (NIDA,
2015).
•
Teaming with a medical facility that provides
integrated healthcare services so that the TC
can be considered a federally qualified health
center and thus help increase treatment access
for vulnerable populations, including people
with CODs (NIDA, 2015; Smith, 2012).
Nevertheless, the central TC feature remains;
the MTC, like all TC programs, seeks to develop
a culture in which clients learn through mutual
support and affiliation with the community to
foster change in themselves and others. Respect
for ethnic, racial, and gender differences is a basic
tenet of all TC programs and is part of teaching
the general lesson of respect for self and others.
Exhibit 7.3 summarizes the key modifications
necessary to address the unique needs of clients
with CODs.
Role of the Family
Many MTC clients come from highly impaired,
disrupted family situations. MTC programs offer
them a new frame of reference and support group.
Some clients do have available intact families or
family members who are supportive. For these
clients, MTC programs offer various family-
centered activities like special family weekend
Chapter 7 205
TIP 42 Substance Use Disorder Treatment for People With Co-Occurring Disorders
EXHIBIT 7.3. TC Modifications for People With CODs
STRUCTURAL
MODIFICATIONS
PROCESS
MODIFICATIONS
INTERVENTION MODIFICATIONS
There is increased flexibility in
program activities.
Sanctions are fewer with
greater opportunity
Orientation and instruction are emphasized
in programming/planning.
Meetings and activities are
shorter.
for corrective learning
experiences.
Individual counseling is provided more
frequently to enable clients to absorb the TC
experience.
There is greatly reduced
intensity of interpersonal
interaction.
Engagement and
stabilization receive more
time and effort.
Task assignments are individualized.
More explicit affirmation is
given for achievements.
Breaks are offered frequently during work
tasks.
Greater sensitivity is shown to
individual differences.
Progression through
the program is paced
individually, according
Individual counseling and instruction are
more immediately provided in work-related
activities.
Greater responsiveness to the
special developmental needs
of the individual.
to the client’s rate of
learning.
Engagement is emphasized throughout
treatment.
More staff guidance is given
in the implementation of
activities; many activities
remain staff assisted for a
considerable period of time.
Criteria for moving to the
next phase are flexible to
allow lower functioning
clients to move through
the program phase
Activities are designed to overlap.
There is greater staff
responsibility to act as role
models and guides.
system.
Activities proceed at a slower pace.
Smaller units of information
are presented gradually and
are fully discussed.
Live-out reentry
(continuing care) is an
essential component of
Individual counseling is used to assist in the
effective use of the community.
Greater emphasis is placed on
assisting individuals.
the treatment process.
The conflict resolution group replaces the
encounter group.
Increased emphasis is placed
on providing instruction,
practice, and assistance.
Clients can return to
earlier phases to solidify
gains as necessary.
Source: Sacks & Sacks (2011).
206 Chapter 7

TIP 42
Chapter 7—Treatment Models and Settings for People With Co-Occurring Disorders
ADVICE TO ADMINISTRATORS: RECOMMENDED TREATMENT AND
SERVICES FROM THE MTC MODEL
In addition to the general guidelines for working with people who have CODs described in Chapter 5, the
following treatment recommendations are derived from MTC work and are applicable across all models:
• Treat the whole person.
• Provide a highly structured daily regimen.
• Use peers to help one another.
• Rely on a network or community for both support and healing.
• Regard all interactions as opportunities for change.
• Foster positive growth and development.
• Promote change in behavior, attitudes, values, and lifestyle.
• Teach, honor, and respect cultural values, beliefs, and differences.
visiting, family education and counseling sessions,
and, if children are involved, classes focused
on prevention. All such activities occur later in
treatment to facilitate client reintegration into the
family and into mainstream living.
Empirical Evidence
A series of studies has established that:
•
MTCs affect a wide range of clinical and
functional variables, including substance use,
mental disorder symptoms, criminal behavior,
employment, and housing (Sacks, McKendrick,
Sacks, & Cleland, 2010). For instance, a review
of TCs and MTCs (Magor-Blatch, Bhullar,
Thomson, & Thorsteinsson, 2014) reported
reduced substance use (including increased
abstinence and reduced risk of relapse),
decreased criminal behavior (including
rearrests and reincarcerations), and improved
psychological functioning among diverse
populations, including people with CODs.
However, benefits were more consistent from
pre–post treatment than when comparing TCs/
MTCs with control groups (e.g., no treatment,
other treatment).
•
Among people involved in the criminal justice
system who have CODs, MTCs can effectively
reduce SUD and mental illness symptoms,
delay relapse, improve social functioning,
reduce criminal activity, and decrease recidivism
compared with traditional TCs (Magor-Blatch et
al., 2014; Peters et al., 2017). MTCs also appear
to reduce reincarceration better than parole
supervision (Sacks, Chaple, Sacks, McKendrick,
& Cleland, 2012).
•
People with CODs and HIV receiving MTC
continuing care had a greater decrease in SUD
and mental illness symptoms at 6 months than
people receiving standard continuing care
(Sacks, McKendrick, Vazan, Sacks, & Cleland,
2011). Larger improvements were observed
in MTC clients who had higher levels of
psychosocial functioning and health at the start
of treatment.
•
MTCs can meet the various needs of pregnant
and parenting women with SUDs—many of
whom have co-occurring mental disorders,
experiences with homelessness, criminal justice
involvement, or a combination thereof. One
such program (Bromberg, Backman, Krow, &
Frankel, 2010) reduced recidivism, promoted
long-term abstinence (about 90 percent of
clients remained abstinent for 2 years after
program completion), and facilitated drug-free
births and healthy infant development.
Outpatient SUD Treatment
Treatment for SUDs occurs most frequently in
outpatient settings—a term that encompasses a
variety of disparate programs (Cohen, Freeborn, &
McManus, 2013; NIDA, 2018b; SAMHSA, 2019a).
Chapter 7 207
TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
RESOURCE ALERT: HOW TO IMPLEMENT TCMTC PROGRAMMING
Guidance on designing and implementing TCs/MTCs is available online through various manuals, reports,
and other documentation. Some of the publications in the following list are specific to a particular
organization or state. However, they can still serve as useful tools for informing the types of services,
structures, and processes needed to make TC/MTC programming successful:
• NIDA’s Therapeutic Communities Research Report (https://d14rmgtrwzf5a.cloudfront.net/sites/default/
files/therapueticcomm_rrs_0723.pdf)
• The Arkansas Department of Human Services’ Therapeutic Communities Certification Manual (https://
humanservices.arkansas.gov/images/uploads/dpsqa/DBHS_Therapuetic_Communities_Certification_-_
FINAL.pdf)
• Missouri Department of Corrections and Maryville Treatment Center’s Therapeutic Community Program
Handbook (www.law.umich.edu/special/policyclearinghouse/Documents/MO%20-%20Maryville%20
Treatment%20Center%20Therapeutic%20Community%20Program%20Handbook.pdf)
• National Institute of Justice’s Program Profile: Modified Therapeutic Community for Offenders With
Mental Illness and Chemical Abuse Disorders (www.crimesolutions.gov/ProgramDetails.aspx?ID=90)
• University of Delaware Center for Drug and Alcohol Studies. Therapeutic Community Treatment
Methodology: Treating Chemically Dependent Criminal Offenders in Corrections (www.cdhs.udel.edu/
content-sub-site/Documents/CDHS/CTC/Treating%20Chemically%20Dependent%20Criminal%20
Offenders%20in%20Corrections.pdf)
Some offer high-intensity services, like several
hours of treatment each week, which can include
mental health and other support services as well
as individual and group counseling for substance
misuse; others provide minimal services, such
as only one or two brief sessions to give clients
information and refer them elsewhere (NIDA,
2018b). Some agencies offer outpatient programs
that provide services several hours per day and
several days per week, thus meeting the LOCUS
criteria for High Intensity Community Based
Services.
Typically, treatment includes individual and
group counseling, with referrals to appropriate
community services. Until recently, there were few
specialized approaches for people with CODs in
outpatient SUD treatment settings.
Many individuals with CODs have multiple
health and social problems that complicate their
treatment. Evidence from prior studies indicates
that a mental disorder often makes effective
SUD treatment harder because of cognitive,
psychosocial, and economic barriers that hinder
engagement and retention (Priester et al., 2016).
Outpatient treatment programs are available
widely and serve the most clients (Cohen et al.,
2013; SAMHSA, 2019a), so using current best
practices from the SUD treatment and mental
health fields is vital. Doing so enables these
programs to use the best available treatment
models to reach the greatest possible number of
people with CODs.
Prevalence
Outpatient SUD treatment programs are the most
common form of SUD treatment setting in this
country. In 2018, 83 percent of SUD treatment
facilities in the United States offered outpatient
services (SAMHSA, 2019a). Specifically, 77 percent
offered regular outpatient services, 46 percent
intensive outpatient, 14 percent day treatment
or partial hospitalization, 10 percent outpatient
detoxification, and 28 percent outpatient
methadone/buprenorphine maintenance or
naltrexone treatment.
CODs are commonly found in clients who enter
SUD treatment. In 2018, 50.2 percent of individuals
208 Chapter 7

TIP 42Chapter 7—Treatment Models and Settings for People With Co-Occurring Disorders
in SUD treatment had a COD, and 99.8 percent
of SUD treatment facilities reported having
clients with CODs (SAMHSA, 2019a). Despite the
complexity of CODs, outpatient programs have
good capacity (e.g., organization structures and
policies) to meet the treatment needs of these
populations, perhaps even more so than intensive
outpatient programs and residential programs
(Lambert-Harris, Saunders, McGovern, & Xie,
2013).
Empirical Evidence of Eectiveness
Outpatient settings can be paired with a variety
of treatment approaches to help clients with
CODs successfully improve substance-related
mental health outcomes and functional outcomes,
including frequency of substance use, abstinence,
relapse risk, mental illness symptom remission,
psychiatric hospitalizations, social functioning,
having independent housing, gaining competitive
employment, and life satisfaction (Drake, Bond, et
al., 2016; Haller, Norman, et al., 2016; McDonell
et al., 2013). Most integrated treatments—such as
those combining CBT, motivational interviewing,
and family services—are offered in outpatient, not
residential, settings and have a strong evidence
base supporting their effectiveness for CODs (Kelly
& Daley, 2013), including SMI with SUDs (Cleary,
Hunt, Matheson, & Walter, 2009; De Witte et al.,
2014).
Outpatient COD treatment can yield positive
outcomes even when treatment is not tailored
specifically to CODs. Tiet and Schutte (2012)
reviewed the differential benefits of COD
treatment at either addiction, mental illness, or
COD outpatient treatment programs. All clients
improved in 6-month abstinence and suicide
attempts compared with baseline, although people
attending COD outpatient settings did not fare any
better on these outcomes than clients completing
outpatient treatment from SUD clinics or mental
health service clinics.
Outpatient treatment can also be leveraged
as a form of continuing care, such as following
discharge from hospitalization or release from
jail/prison, to help clients maintain long-term
recovery and wellness (Grella & Shi, 2011).
Six-month outpatient ACT for men with SMI and
SUD (Noel, Woods, Routhier, & Drake, 2016)
was effective in sustaining improvements clients
experienced during the previous 6 months in
residential treatment, including improvements in
mental health, substance use, housing, education,
employment, family functioning, spirituality, and
sleep hygiene. Outpatient mental health services
focused on supporting community reintegration
following release from jail were associated with
12-month declines in number of arrests and
number of days in jail among people with CODs
and people with mental disorders only (Alarid &
Rubin, 2018).
Evidence suggests that intensive outpatient
treatment for people with CODs can improve
substance misuse and increase abstinence among
a range of populations, including civilians and
veterans, women, people from diverse racial/ethnic
backgrounds, uninsured individuals, and people
experiencing homelessness (McCarty et al., 2014).
Intensive outpatient treatment has been associated
with decreases in psychological symptoms and
distress, decreases in the average number of
days per week of substance use, improvements in
Global Assessment of Functioning scores, and high
client satisfaction (Wise, 2010).
Designing Outpatient Programs for Clients
With CODs
People with CODs vary in their motivation for
treatment, nature and severity of their SUD (e.g.,
drug of choice, polysubstance misuse), and nature
and severity of their mental disorder. However,
most clients with CODs in outpatient treatment
have less serious and more stabilized mental and
SUD symptoms than those in residential treatment
(Mee-Lee et al., 2013).
Outpatient treatment can be the primary
treatment or provide continuing care for clients
after residential treatment, offering flexibility in
activities/interventions and intensity of treatment.
Treatment failures occur for people with SMI
and those with less serious mental disorders for
several reasons, among the most important being
that programs lack resources to provide time for
mental health services and medications that would
likely improve recovery rates and recovery time
significantly.
Chapter 7 209
TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
RESOURCE ALERT: OUTPATIENT SUD TREATMENT
•
SAMHSA’s TIP 47, Substance Abuse: Clinical Issues in Intensive Outpatient Treatment
(https://store.samhsa.gov/system/files/sma13-4182.pdf)
• SAMHSA’s TIP 46, Substance Abuse: Administrative Issues in Outpatient Treatment
(https://store.samhsa.gov/system/files/toc.pdf)
If lack of funding prevents the full integration of
mental health assessment and medication services
within an SUD treatment agency that provides
outpatient services, establishing a collaborative
relationship with a mental health agency (through
a memorandum of agreement) would ensure that
the services for the clients with CODs are adequate
and comprehensive. In addition, modifications are
needed to both treatment design interventions
and staff training to ensure implementation of
interventions appropriate to the needs of the client
with CODs.
To meet the needs of specific populations
among people with CODs, the consensus panel
encourages outpatient treatment programs to
develop special services for populations that
are represented in significant numbers in their
programs. Examples include women, women
with dependent children, individuals and families
experiencing homelessness, and racial/ethnic
populations. (Information on how programs can
adapt services to these and other vulnerable
populations can be found in Chapter 6.) Types of
CODs will vary depending on the subpopulation
targeted; each program must deal with CODs in a
different manner, often by adding other treatment
components for CODs to existing program models.
Referral and Placement
Careful assessment will help identify those clients
who require more secure inpatient treatment
settings (e.g., clients who are actively suicidal
or homicidal), as well as those who require
24-hour medical monitoring, those who need
detoxification, and those with serious SUDs who
may require a period of abstinence or reduced use
before they can engage actively in all treatment
components. Information about the full screening
and assessment process, which includes referral, is
in Chapter 3.
Counselors should view clients’ placement in
outpatient care in the context of continuity of
care and the network of available providers and
programs. Outpatient treatment programs may
serve a variety of functions, including outreach/
engagement, primary treatment, and continuing
care. Ideally, a full range of outpatient SUD
treatment programs would include interventions
for unmotivated, disaffiliated clients with CODs,
as well as for those seeking abstinence-based
primary treatments and those requiring continuity
of supports to sustain recovery.
Likewise, ideal outpatient programs will facilitate
access to services through rapid response to
all agency and self-referral contacts, imposing
few exclusionary criteria, and using some client/
treatment matching criteria to ensure that all
referrals can be engaged in some level of treatment.
Additional criteria for admission may be imposed
on the treatment agency by individual states,
insurance companies, or other funding sources. Per
the consensus panel, treatment providers should
not place clients in a higher level of care (i.e., more
intense) than necessary. A client who may remain
engaged in a less intense treatment environment
may drop out in response to the demands of a more
intense treatment program.
Engagement and Retention
Because clients with CODs often have lower
treatment engagement, every effort should be
made to use treatment methods with the best
prospects for increasing engagement. Clients with
CODs, especially those opposed to traditional
treatment approaches and those who do not accept
that they have CODs, can have difficulty committing
to and maintaining treatment. By providing
continuous outreach, engagement, direct assistance
with immediate life problems (e.g., housing),
advocacy, and close monitoring of individual needs,
210 Chapter 7

TIP 42
Chapter 7—Treatment Models and Settings for People With Co-Occurring Disorders
IMPROVING ENGAGEMENT AND
ADHERENCE OF CLIENTS WITH
CODS IN OUTPATIENT SETTINGS
•
Implement behavioral continuing care
contracts for clients transitioning from
residential treatment into outpatient care.
•
Use reminders (e.g., mailed appointment cards,
telephone calls); offer feedback before sessions
to promote attendance.
•
Follow up by phone with clients who miss
appointments.
•
Reinforce attendance to appointments with
praise and other rewards (e.g., earning a
completion certificate after attending a certain
number of sessions, earning a medal or other
recognition for completing all required sessions).
•
Offer peer recovery support services.
•
Use incentives to increase clients’ buy-in to
the need for and importance of treatment.
Incentives related to assistance with housing
and employment may be particularly
meaningful and effective.
•
Rather than solely creating treatment goals
focused centrally around abstinence, work with
clients to develop treatment goals focused
on reducing the harmful effects of substance
use (e.g., reducing homelessness by gaining
independent housing).
•
People with CODs who have positive family
relationships are more likely to stay engaged
in treatment. Encourage clients lacking family
support to reach out to relatives and try to
gain their support. With permission from the
client, include family in treatment and educate
them on the importance of being a source of
emotional and tangible support for the client.
•
Helping clients understand the connection
between substance use and negative
outcomes (e.g., legal problems, housing and
employment instability, exacerbating mental
disorder symptoms) can help them understand
the need for treatment. This is vital because
perceived need for treatment is a common
barrier to entering and staying engaged in SUD
treatment.
Sources: Brown, Bennett, Li, & Bellack (2011); Demarce,
Lash, Stephens, Grambow, & Burden (2008); Mangrum
(2009).
the ACT and ICM models provide techniques that
enable clients to access services and foster the
development of treatment relationships.
Discharge Planning
Discharge planning is important to maintain
gains achieved through outpatient care. Clients
with CODs leaving an outpatient SUD treatment
program have a number of continuing care options.
These options include mutual-support programs,
relapse prevention groups, continued individual
counseling, mental health services (especially
important for clients who will continue to require
medication), as well as ICM monitoring and
supports. A carefully developed discharge plan,
produced in collaboration with the client, will
identify and match client needs with community
resources, providing supports to sustain progress
achieved in outpatient treatment. The provider
seeks to develop a support network for the client
that involves family, community, recovery groups,
friends, and significant others.
Clients with CODs often need a range of services
besides SUD treatment and mental health services.
Generally, prominent needs include housing and
case management services to establish access to
community health and social services. In fact, these
two services should not be considered “ancillary,”
but key ingredients for clients’ successful recovery.
Without a place to live and some degree of
economic stability, clients with CODs are likely to
return to substance use or experience a return of
symptoms of mental disorder. Every SUD treatment
provider should keep strong and current linkages
with community resources to help address these
and other client needs. Clients with CODs often
will require a wide variety of services that cannot be
provided by a single program.
Discharge planning for clients with CODs
must ensure continuity of services, medication
management, and support, without which client
stability and recovery are severely compromised.
Relapse prevention interventions after outpatient
treatment need to be modified so clients can
recognize symptoms of SUD or mental disorder
relapse on their own, use symptom management
techniques (e.g., self-monitoring, reporting
to a “buddy,” group monitoring), and access
Chapter 7 211

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
assessment services rapidly, as the return of
psychiatric symptoms can often trigger substance
use relapse.
Developing positive peer networks is another
important facet of discharge planning for
continuing care. The provider seeks to develop a
support network for the client that involves family,
community, recovery groups, friends, and significant
others. If a client’s family of origin is not healthy
and supportive, other networks can be accessed
or developed for support. Programs also should
encourage client participation in mutual-support
programs, particularly those that focus on CODs
(e.g., dual recovery mutual-support groups).
These groups can provide a continuing supportive
network for the clients, who usually can continue to
participate in such programs even if they move to a
different community. Therefore, these groups are an
important method of providing continuity of care.
The consensus panel also recommends that
programs working with clients who have CODs try
to involve advocacy groups in program activities.
These groups can help clients become advocates
themselves, furthering the development and
responsiveness of the treatment program while
enhancing clients’ sense of self-esteem and
providing a source of affiliation.
Residential SUD Treatment
Residential treatment for SUDs comes in a variety
of forms, including long-term residential treatment
facilities, criminal justice-based programs, halfway
houses, and short-term residential programs. The
long-term residential SUD treatment facility is the
primary treatment site and the focus of this section
of the TIP. Historically, residential SUD treatment
facilities have provided treatment to clients with
more serious and active SUDs but with less severe
mental disorders. Most providers now agree
that the prevalence of people with SMI entering
residential SUD treatment facilities has risen.
Prevalence
In 2018, 24 percent of SUD treatment facilities in
the United States offered any residential treatment
(SAMHSA, 2019a). Specifically, 14 percent offered
short-term residential care; 19 percent, long-term
care; and 8 percent, residential detoxification.
Clients admitted to long-term residential care
tend to have more severe substance misuse and
psychiatric problems. Veterans with SUDs and
PTSD admitted to residential treatment reported
worse PTSD symptoms, more frequent substance
use, more time spent around high-risk people or
places, and fewer days spent at work or school
than veterans with SUDs and PTSD who entered
outpatient care (Haller, Colvonen, et al., 2016).
Other studies have found an increased rate of
suicide attempt and violence (as a victim and as a
perpetrator) among people with CODs entering
residential treatment (Havassy & Mericle, 2013;
Watkins, Sippel, Pietrzak, Hoff, & Harpaz-Rotem,
2017) as well as lower treatment retention rates,
particularly in people with ASPD and SUD (Meier &
Barrowclough, 2009).
Empirical Evidence of Eectiveness
Evidence from large-scale, longitudinal, multisite
treatment studies supports the effectiveness
of residential SUD treatment (Reif, George, et
al., 2014; Weinstein, Wakeman, & Nolan, 2018).
Residential SUD treatment generally results
in significant improvements in substance use,
mental health, employment, and physical and
social functioning. Residential treatment for
CODs is linked to improved SUD outcomes (e.g.,
illicit drug and alcohol use), mental disorder
symptoms, quality of life, and social/community
functioning, even if treatment is not integrated
(Reif, George, et al., 2014). A multisite study of
residential COD treatment programs in Tennessee
and California (Schoenthaler et al., 2017) found
significant reductions in illicit substance use per
month, intoxication per month, alcohol use days
per month, and ASI drug and alcohol composite
scores from 1 month before treatment admission to
12-month postdischarge.
Designing Residential Programs for Clients
With CODs
To design and develop services for clients with
CODs, providers and administrators can undertake a
series of interrelated program activities. The specific
MTC model that appeared previously in this chapter
serves as a frame of reference in the following
sections, but it is not a prescriptive model.
212 Chapter 7

TIP 42
Chapter 7—Treatment Models and Settings for People With Co-Occurring Disorders
Intake
Chapter 3 further addresses screening and
assessment. This section addresses intake procedures
for people with CODs in residential SUD treatment
settings. The four interrelated intake steps are:
1. Written referral. Referral information from
other programs or services can include the
client’s psychiatric diagnosis, history, current
level of mental functioning, medical status
(including results of screening for tuberculosis,
HIV, sexually transmitted disease, hepatitis),
and assessment of functional level. Referrals
also may include a psychosocial history and a
physical examination.
2. Intake interview. An intake interview is
conducted at the program site by a counselor or
clinical team. At this time, the referral material
is reviewed for accuracy and completeness, and
each client is interviewed to determine if the
referral is appropriate in terms of the history of
mental and substance use problems. The client’s
residential and treatment history is reviewed
to assess the adequacy of past treatment
attempts. Furthermore, each client’s motivation
and readiness for change are assessed, and
the client’s willingness to accept the current
placement as part of the recovery process is
evaluated. Screening instruments, such as those
described in Chapter 3 and located in Appendix
C, can be used in conjunction with this intake
interview.
3. Program review. Each client should receive a
complete description of the program and a tour
of the facility to ensure that both are acceptable.
This review includes a description of the daily
operation of the program in terms of groups,
activities, and responsibilities; a tour of the
physical site (including sleeping arrangements
and communal areas); and an introduction to
some of the clients who are already enrolled in
the program.
4. Team meeting. At the end of the intake
interview and program review, the team meets
with the client to decide whether to proceed
with admission to the program. The client’s
receptivity to the program is considered, and
additional information (e.g., involvement with
the justice system, suicide attempts) is obtained
as needed. It should be noted that the decision-
making process is inclusive; that is, a program
accepts referrals as long as the clients meet the
eligibility criteria, are not currently a danger to
self or others, do not refuse medication, express
a readiness and motivation for treatment, and
accept the placement and the program as part
of their recovery process.
Engagement and Retention
Clients with CODs need to be engaged in
treatment so they can fully use available services.
Successful engagement helps clients view the
treatment program as an important resource. To
accomplish this, the program must meet essential
needs and ensure psychiatric stabilization.
Residential treatment programs can accomplish this
by offering a wide range of services that include
both targeted services for mental disorders and
SUDs and other wraparound services, including
medical, social, and work-related activities. The
extensiveness of residential services has been well
documented (Reif, George, et al., 2014).
Clients in residential settings for SUDs are three
times more likely to complete treatment than
those in outpatient settings (Stahler, Mennis, &
DuCette, 2016). Retention in treatment is associated
with positive outcomes, and identifying factors
that predict length of stay can inform practices
to improve engagement and adherence. Shorter
stays in residential care are linked to older age,
male gender, and low readiness for change
(Morse, Watson, MacMaster, & Bride, 2015). Better
retention in residential SUD treatment settings is
linked to younger age, White race/ethnicity (vs.
African Americans and Latinos), type of SUD (i.e.,
non-OUD), more severe ASI medical-, employment-,
and psychiatric-related scale scores, and greater
readiness for change (Choi, Adams, MacMaster, &
Seiters, 2013).
Discharge Planning
Discharge planning follows many of the same
procedures discussed in the section on outpatient
treatment. However, several other important points
apply to residential programs:
•
Discharge planning begins upon entry into the
program.
Chapter 7 213

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
•
The latter phases of residential placement
should be devoted to developing with the client
a specific discharge plan and beginning to
follow some of its features.
•
Discharge planning often involves continuing in
treatment as part of continuity of care.
•
Obtaining housing, when needed, is an integral
part of discharge planning.
Given the chronic and cyclical nature of SUDs
and mental disorders, continuing care following
residential services (such as the provision of lower
intensity outpatient treatment postdischarge)
can help optimize client stability and functioning.
Individuals with SUDs who receive continuing care
are retained in treatment and maintain abstinence
more so than clients who do not participate in
continuing care (McKay, 2009).
Acute Care and Other Medical Settings
Although not strictly speaking SUD treatment
settings, acute care and other medical settings are
included here because important SUD treatment
and mental health services occur in medical units.
Acute care refers to short-term care provided in
intensive care units, brief hospital stays, and EDs.
Individuals with substance misuse or mental illness
often access care from primary care clinics as
opposed to specialty care settings. People going
to EDs for treatment for mental disorders and
SUDs is also on the rise.
The integration of SUD treatment with primary
medical care can be effective in reducing both
medical problems and levels of substance use.
Clients can be more readily engaged and retained
in SUD treatment if that treatment is integrated
with medical care than if clients are referred to
a separate SUD treatment program—especially
individuals with SUDs who have chronic medical
needs (Drainoni et al., 2014; Hunter, Schwartz,
& Friedmann, 2016). Extensive treatment for
SUDs and co-occurring mental disorders may be
unavailable in acute care settings given constraints
on time and resources; however, brief assessments,
referrals, and interventions can help move clients
to the next level of treatment.
More information on particular topics relating to
SUD screening and treatment in acute and medical
care settings can be found in TIP 45, Detoxification
From Alcohol and Other Drugs (CSAT, 2006b).
More information on the use and value of brief
interventions can be found in TIP 34, Brief
Interventions and Brief Therapies for Substance
Abuse (CSAT, 1999a).
RECOMMENDATIONS FOR CONTINUING CARE FOLLOWING DISCHARGE
FROM RESIDENTIAL TREATMENT
•
Clients should be engaged in continuing care services for a minimum of 3 to 6 months following discharge.
•
Scheduling of continuing care appointments should occur prior to discharge so that appointments are
already in place by the time a client leaves inpatient care.
•
To facilitate monitoring, programs should implement formal follow-up procedures to ensure staff maintain
contact with clients regularly at set time points (e.g., 30 days, 6 months), ideally for at least 12 months.
•
Clients should be educated about the importance of continuing care and the availability of treatment
options following residential treatment, including the use of pharmacotherapy with outpatient services.
•
Residential staff should introduce clients to outpatient providers before discharge so as to provide a
“warm handoff” and foster rapport-building between clients and their continuing care providers.
•
Programs should be flexible in offering a wide range of continuing care services to meet clients’
scheduling and daily living needs (e.g., offer outpatient therapy groups 5 days per week, use telehealth
services so clients who live at a distance and are unable to travel to outpatient services regularly can still
access treatment).
•
Counselors should link clients to mutual-support programs and other community-based supports and
resources available.
Sources: Proctor & Herschman (2014); Rubinsky et al. (2017).
214 Chapter 7

TIP 42
Chapter 7—Treatment Models and Settings for People With Co-Occurring Disorders
HOW COMMON ARE MENTAL DISORDERS AND SUDS IN ACUTE CARE
AND OTHER MEDICAL SETTINGS?
•
More than 70 percent of primary care visits are related to psychosocial needs (National Association of
State Mental Health Program Directors, 2012).
- In a sample of 2,000 adults in primary care clinics in four states, 36 percent met Diagnostic and
Statistical Manual of Mental Disorders (5th ed.; American Psychiatric Association, 2013) criteria for an
SUD in the last year, including almost 22 percent with a moderate/severe SUD (Wu et al., 2017). About 28
percent endorsed past-year illicit drug or nonmedical medication use.
- From 2012 to 2014 (Cherry, Albert, & McCaig, 2018), 26 percent of mental health office visits in large
metropolitan areas, 44 percent of visits in small-to-medium metropolitan areas, and 54 percent of visits
in rural areas were to primary care.
•
Of the 1.18 billion ambulatory medical visits that occurred between 2009 and 2011 (Lagisetty, Maust,
Heisler, & Bohnert, 2017), 17.6 million involved an SUD diagnosis.
- This included 8.6 percent for AUD, 64.2 percent for tobacco use disorder, and 9.6 percent for OUD.
- Among the people with an SUD, 13.4 percent also had anxiety, 5.7 percent had depression, and 2.3
percent had bipolar disorder.
•
Data from the National Hospital Ambulatory Medical Care Survey indicate that from 2005 to 2011, mental
and substance use–related ED visits increased from 27.9 per 1,000 visits to 35.1 per 1,000 visits, with
the greatest increases observed in people ages 25 to 44 (Ayangbayi, Okunade, Karakus, & Nianogo, 2017).
Odds of visits were higher in people who were uninsured or on public health insurance, or had been
discharged from a hospital in the previous week.
•
Individuals with CODs are more likely than people without CODs to use EDs for mental disorder
and SUD-related needs (Moulin et al., 2018), as are individuals experiencing homelessness (Lam, Arora,
& Menchine, 2016).
Prevalence
In 2018, 5 percent of SUD treatment facilities in
the United States were hospital-based inpatient
services (SAMHSA, 2019a). Specifically, 4 percent
of facilities offered hospital-based treatment and
5 percent offered hospital-based detoxification. In
2018, 40 percent of general hospitals offered COD
programming (SAMHSA, 2019b).
Empirical Evidence of Eectiveness
Over the past two decades, significant research
has emerged in support of team-based, integrated
behavioral health services in acute medical
care settings (e.g., EDs, primary care clinics).
Collaborative behavioral health service models
are feasible and can be as effective as (and in
some cases even more effective than) usual care
in identifying and managing SMI, SUDs, or CODs
(Chan, Huang, Bradley, & Unutzer, 2014; Chan,
Huang, Sieu, & Unutzer, 2013; Kumar & Klein,
2013; Park, Cheng, Samet, Winter, & Saitz, 2015;
Walley et al., 2015). Integrated, collaborative
behavioral health services can improve mental
disorder symptoms (including remission and
recovery), treatment adherence, treatment
satisfaction, quality of life (mental and physical),
medication adherence, and social functioning
and are cost-effective and valued by clients
(Epstein, Barry, Fiellin, & Busch, 2015; Goodrich,
Kilbourne, Nord, & Bauer, 2013). Most of these
studies are focused on mental health services,
with comparatively fewer examining integrated
SUD treatment, but research suggests addiction
models also are feasible and can produce positive
outcomes (Goodrich et al., 2013), including
long-term abstinence (Savic, Best, Manning, &
Lubman, 2017). Primary care–based SUD treatment
may also help reduce length of inpatient stay and
ED utilization while also increasing recovery coach
contacts and use of addiction pharmacotherapy
(i.e., buprenorphine and naltrexone) (Wakeman et
al., 2019).
Primary care–based SUD treatment can reduce
gaps in service use by offering treatment in a
setting that clients prefer. More than 42,000
U.S. adults were screened for SUDs to assess
Chapter 7 215

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
willingness to enter SUD treatment based on
service setting (Barry, Epstein, Fiellin, Fraenkel, &
Busch, 2016). Those who screened positive but
were not currently enrolled in SUD treatment were
randomized to one of three hypothetical treatment
setting vignettes: treatment in a specialty drug
treatment center (i.e., usual care), primary care, or
collaborative care in a primary care setting. About
a quarter (24.6 percent) of people with an SUD
and 18 percent with AUD who were randomized
to specialty care were willing to enter treatment,
whereas more people randomized to the primary
care setting were willing to enter treatment (37
percent with an SUD; 20 percent with AUD).
Similarly, more people randomized to the primary/
collaborative care setting were willing to enter
treatment than people in the specialty care setting
(34 percent with an SUD; almost 21 percent with
AUD). Nonspecialty settings like primary care
clinics may be desirable for individuals needing
SUD treatment because of a perceived lack of
stigma attached to medical facilities (compared
with, for instance, methadone clinics) and the
ability of medical settings to address both SUD
treatment and physical healthcare needs in one
location (Barry et al., 2016).
Designing Acute Medical and Primary Care
Programs for Clients With CODs
Programs that rely on identification (i.e., screening
and assessment) and referral occupy a service niche
in the treatment system. To succeed, they need
a clear view of treatment goals and limitations.
Effective linkages with various community-based
SUD treatment facilities are essential to ensure an
appropriate response to client needs and to facilitate
access to additional services when clients are ready.
The discussion that follows highlights the essential
features of providing treatment to clients with
CODs in acute care and other medical settings.
Screening and Assessment in Acute and Other
Medical Settings
Clients entering acute care or other medical facilities
generally are not seeking SUD treatment. Often,
providers (primary care and mental health) are not
familiar with SUDs. Their lack of expertise can lead
THE INTEGRATION OF CARE FOR MENTAL HEALTH, SUBSTANCE ABUSE
AND OTHER BEHAVIORAL HEALTH CONDITIONS INTO PRIMARY CARE:
AMERICAN COLLEGE OF PHYSICIANS ACP POSITION PAPER
1. The ACP supports the integration of behavioral health care into primary care and encourages its
members to address SUDs and mental disorders within the limits of their competencies and resources.
2. The ACP recommends that public and private health insurance payers, policymakers, and primary
care and behavioral health care professionals work toward removing payment barriers that impede
behavioral health and primary care integration. Stakeholders should also ensure the availability of
adequate financial resources to support the practice infrastructure required to effectively provide such
care.
3. The ACP recommends that federal and state governments, insurance regulators, payers, and other
stakeholders address behavioral health insurance coverage gaps that are barriers to integrated care.
This includes strengthening and enforcing relevant nondiscrimination laws.
4. The ACP supports increased research to define the most effective and efficient approaches to integrate
behavioral health care in the primary care setting.
5. The ACP encourages efforts by federal/state governments and training and continuing education
programs to ensure an adequate workforce to provide for integrated behavioral health care in primary
care settings.
6. The ACP recommends that all relevant stakeholders initiate programs to reduce the stigma associated
with behavioral health. These programs need to address negative perceptions held by the general
population and by many physicians and other providers.
Source: Crowley & Kirschner (2015).
216 Chapter 7

TIP 42
Chapter 7—Treatment Models and Settings for People With Co-Occurring Disorders
to unrealistic expectations or frustrations, which may
be directed inappropriately toward the client.
Even in the absence of indepth training in
addiction medicine, primary care and mental
health service providers can quickly and easily
screen clients for SUDs using brief, validated
instruments—leading to better detection of SUDs,
more client–provider discussions about substance
misuse, and overall improvements in care (Jones,
Johnston, Biola, Gomez, & Crowder, 2018; Savic
et al., 2017). (Chapter 3 contains a full description
of screening and assessment procedures and
instruments applicable to CODs, including those
that can be used in primary care settings; select
instruments are also located in Appendix C.)
Although addiction screening can and should be
offered in both nonurgent and urgent medical
care settings, approaches may need to be im-
plemented differently for each. O’Grady, Kapoor,
and colleagues (2019) describe use of a screening,
brief intervention, and referral for treatment (often
referred to as SBIRT) program for people with or
at risk for addiction that was implemented at EDs
and primary care clinics. Compared with people
screened as high risk for substance misuse in the
primary care clinics, those screened as high risk in
the EDs were significantly more likely to also have
unstable housing, be unemployed, have self-re-
ported “extreme” stress, have “serious” depres-
sion or anxiety, and have poor current health. They
also reported higher addiction screening scores
and more frequent substance use than people in
the primary care clinics. Prescreening in the EDs
was less likely to be completed than in primary
care because clients were more likely to be in acute
states, actively intoxicated, or have altered mental
status. Further, more than one-third of people who
prescreened positive for substance misuse did not
receive full screening and intervention. This finding
is consistent with results from two longitudinal
surveys of 1,500 ED physicians that found only 15
percent to 20 percent of clients were screened
for substance misuse and only 19 percent to 26
percent of ED physicians reported using a formal
addiction screening tool (Broderick Kaplan, Martini,
& Caruso, 2015).
These data are worrisome, given feedback from the
American College of Emergency Physicians (2017)
that ED professionals are, “positioned and qualified
to mitigate the consequences of alcohol misuse
through screening programs, brief intervention,
and referral to treatment” and that EDs should
maintain “wide availability of resources necessary
to address the needs of patients with alcohol-
related problems and those at-risk for them.” ED
staff may therefore require additional training
to better recognize and respond to clients with
addiction, particularly those with severe disorders.
Formal procedures may also be needed to foster
successful referral and implementation of brief
interventions (e.g., education, harm reduction).
Interventions
Several differences exist in behavioral health
service provision (including addiction services)
in medical settings versus traditional mental
health service settings (Exhibit 7.4). Acute medical
settings may be less likely than mental health clinics
to have SUD treatment providers on staff, unless
the setting offers integrated care. For this reason,
acute care and other medical settings should have
formal procedures in place so providers know
when clients require referral for specialty addition
treatment versus in-office brief interventions (e.g.,
education about substance use, harm reduction
tips) (Shapiro, Coffa, & McCance-Katz, 2013).
Pharmacologic treatment is likely easier for clients
to access in medical settings than in mental health
centers because of the widespread availability
of onsite prescribers. Pharmacologic treatment
should be offered based on the latest evidence-
based best practices (e.g., TIP 63, Medications for
Opioid Use Disorder [SAMHSA, 2018c]; Veterans
Administration (VA)/Department of Defense (DoD)
Clinical Practice Guidelines for the Management of
Substance Use Disorders [VA/DoD, 2015]). See the
section “Pharmacotherapy” for a full discussion of
medication treatment of people with CODs.
In integrated settings, treatment planning will
often need to occur in collaboration with the other
team providers (Savic et al., 2017). To this end,
providers likely will need to engage in greater
sharing of confidential client information than in
nonintegrated, traditional settings to foster case
management and coordination of services (Savic et
al., 2017). Clients need to be briefed about these
Chapter 7 217

TIP 42 Substance Use Disorder Treatment for People With Co-Occurring Disorders
limits to confidentiality at intake and their consent
documented.
Exhibit 7.5 offers a sample (not exhaustive)
listing of questions that addiction providers
and administrators should consider if they
wish to integrate their services with primary
care settings. (Also see “Resource Alert: How
To Integrate Primary Care and Behavioral Health
Services for People With SMI.”)
Historically, providers in acute care settings have
not been concerned with treating SUDs beyond
detoxification, stabilization, and referral. However,
as the uptake of brief interventions increases and
as the healthcare field’s awareness grows about the
importance of detecting and treating SUDs and
mental disorders, treatment options are expanding
beyond just stabilization and referral. In EDs, case
managers help triage “high users” (who often
include people with SUDs, mental disorders, or
both [Minassian, Vilke, & Wilson, 2013; Moulin et
EXHIBIT 7.4. Traditional Mental Health Settings Versus Integrated
Mental Health–Primary Care Settings
FACTOR TRADITIONAL MENTAL
HEALTH SETTING
INTEGRATED MENTAL HEALTHPRIMARY
CARE SETTING
Service Provision Individualized/case based Population based (e.g., services are for all of
those attending the primary care clinic, the
community served by the clinic)
Service Target(s) The client/family The client/family, other colleagues in the
integrated system with whom the mental
health provider collaborates (e.g., the primary
care provider), community at large
Intensity and Length of Care Comprehensive and
long-term (as needed)
Comprehensive but briefer, more episodic,
and with larger caseload turnover
Client Motivation Usually high (unless
treatment is compulsory,
such as in forensic cases)
Often ambivalent, hesitant; clients may be
less amenable to advice or referral for services
Client Confidentiality High; other providers
may or may not be
involved in the client’s
care
Moderate; client information is regularly
shared with other integrated care team
members
Focus of Treatment Skill oriented and
symptom focused but
also exploratory (e.g.,
interpersonal therapy,
psychodynamic therapy)
Tends to be more concrete, skills oriented, and
symptom based
Source: Joseph, Kester, O’Brien, & Huang (2017).
218 Chapter 7

TIP 42
Chapter 7—Treatment Models and Settings for People With Co-Occurring Disorders
EXHIBIT 7.5. Redesigning Addiction Services for Integration With Primary
Care: Questions for Addiction Providers and Administrators To Consider
Administrative Questions
•
Is integration a part of your organization’s vision and mission?
•
What type of integration do you want to implement? Different options include:
- Addressing substance use problems only.
- Addressing substance use in primary care.
- Addressing all substance use and mental disorder needs without primary care.
- Addressing all substance use and mental disorder needs with primary care.
•
Have you developed a strategic plan related to integration?
•
Do you/your staff understand the primary care and SUD needs of the population you are serving?
•
Do you have administrative policies in place to support integration (e.g., confidentiality, billing and
reimbursement, ethics)?
•
What clinical and business practices in your organization need to change to facilitate integration?
Capacity/Resource Questions
•
Do you have existing relationships (formal or informal) with other service providers in mental health and
primary care? If not, what needs to be done to establish those relationships?
•
What existing community resources can you draw on (e.g., community coalitions, prevention programs)?
•
Do you have relationships with medical providers at various levels of care (e.g., inpatient, outpatient) so
you can refer clients seamlessly across the entire continuum of care?
•
Do you have staff and other resources to treat primary care- and substance-related disorders? Is your
organization licensed to provide these services? If not, what licensing regulations need to be met?
•
Does your program have staff with a range of expertise and competencies in providing integrated care
(e.g., case management, care coordination, wellness programming)?
•
Does your program currently offer any integrated components, even if on an informal basis and not part
of a defined program structure (e.g., as-needed use of case management to coordinate services)?
Financing Questions
•
Do you have professional staff capable of providing billable primary care or mental health services?
•
What expenditures—such as hiring staff or investing in training or other resources—might be required?
•
What profit does your organization need to make to support your integrated care vision (key elements:
number of consumers seen; how often they are seen per year; payer mix; reimbursement per visit)?
•
Can you organization accept all types of payment (i.e., Medicaid, Medicare, private insurance)?
•
What do you need to learn about joining provider networks of major payers?
Clinical Supports Questions
•
Does your organization use a certified electronic medical records system?
•
Can your records system create patient data registries (or link to existing registries) to support
integration?
•
Does your records system have a formal way of documenting coordination of care?
•
Does your records system have a formal way of documenting physical health-related services?
Source: SAMHSA-Health Resources and Services Administration Center for Integrated Health Solutions (2013).
Chapter 7 219

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
RESOURCE ALERT: HOW TO INTEGRATE PRIMARY CARE AND
BEHAVIORAL HEALTH SERVICES FOR PEOPLE WITH SMI
Milbank Memorial Fund’s Integrating Primary Care into Behavioral Health Settings: What Works for
Individuals with Serious Mental Illness (www.milbank.org/wp-content/uploads/2016/04/Integrating-
Primary-Care-Report.pdf)
al., 2018; Smith, Stocks, & Santora, 2015]) to ap-
propriate levels of care (e.g., admission, outpatient
referral) (Turner & Stanton, 2015). Aspects of case
management interventions—which are typically
delivered not solely by case managers but collab-
oratively with other ED team members like nurses,
physicians, and social workers—that can reduce ED
visits, and in some cases reduce ED costs (Kumar &
Klein, 2013) include:
•
Educating clients about and linking them to
community resources to address symptoms/
problems.
•
Offering referral to mental health services and
SUD treatment.
•
Assisting clients with transportation needs.
•
Assisting clients with financial benefits/public
assistance.
•
Performing crisis intervention.
•
Helping clients acquire stable housing.
•
Working with clients to create an ED treatment
plan or other individualized care plan.
•
Following up with clients after discharge,
including when providing referrals to specialty
care.
Interview-based interventions, like motivational
interviewing and brief negotiated interviews,
decrease alcohol and illicit drug use in some
studies, but other studies have reported
inconsistent results (Hawk & D’Onofrio, 2018).
Some research suggests that brief ED interventions
affect substance use no more than minimal
screening alone (Bogenschutz et al., 2014a),
possibly because people presenting to the ED
with substance-related problems tend to have
higher levels of severity. Overdose education and
distribution of naloxone kits are also being used
increasingly in EDs, given the surge of evidence
demonstrating the effectiveness of MAT for
OUD; however, evidence for their effectiveness in
preventing overdose and substance use over time
has yet to be borne out (Hawk & D’Onofrio, 2018).
Research on the placement of peer recovery
support specialists in EDs also appears to be
promising but is still in its early stages (Ashford,
Meeks, Curtis, & Brown, 2018; Samuels et
al., 2018). The AnchorED Program in Rhode
Island found that, during its first year, use of
certified recovery coaches in the ED for people
experiencing opioid overdose resulted in high
engagement of recovery support services after
discharge (83 percent), including enrollment at
a local recovery community organization (Joyce
& Bailey, 2015). Only 5 percent of people who
engaged with the recovery coach experienced
repeat ED visits. From 2016 to 2017, 87 percent of
people engaged with AnchorED recovery coaches
after ED discharge, and 51 percent accepted
service referrals (e.g., inpatient treatment program,
outpatient treatment program, MAT program)
(Waye et al., 2019). However, more evidence is
needed to elucidate the efficacy and effectiveness
of peer-based approaches for ED populations.
Pharmacotherapy
This TIP does not comprehensively discuss
pharmacotherapies for SUDs and mental illness.
This section is an overview of medications for
certain SUDs (i.e., OUD, AUD) and for mental
disorders likely to co-occur with SUDs. The aim
of this section is to foster appropriate monitoring
and treatment planning by educating counselors
about common medications that clients with
CODs may be taking and side effects they may
experience. For indepth discussion of medication
for opioid addiction, see TIP 63, Medications for
Opioid Use Disorder (SAMHSA, 2018c). “Resource
Alert: Learning More About Pharmacotherapy and
CODs” offers more information about medication
treatment for CODs.
220 Chapter 7

TIP 42
Chapter 7—Treatment Models and Settings for People With Co-Occurring Disorders
Medication for Mental Illness
Mental disorders are diseases of the brain or
central nervous system. They affect a person’s
thinking, emotions, and mood. Medications
can relieve distressing symptoms and improve
functioning for people with mental illness, and
they work in a variety of ways. Medications may
be effective for more than one disorder but be
referred to by the condition they are most often
used to treat. For example, a medication may be
referred to as an “antidepressant” but also help
with anxiety or an eating disorder. Antipsychotic
medications are typically associated with diseases
like schizophrenia but may also be used for bipolar
disorder or severe depression. Because the
same medication can be used to treat various
disorders, always ask clients for which condition
they take a medication.
A person may have a history of taking different
medications in the past or may report a change
in his or her medications while working with a
counselor. People need different medications
depending on how their illness is expressing itself
(e.g., which symptoms are most severe or most
disabling). Medications used to treat the first
episode of a mental illness may be different from
those used later in disease course. Age may affect
medication selection and dosage; aging affects
metabolism and the bioavailability of some drugs.
Sometimes a medication becomes less effective
over time and will have to be changed or another
medication added. There may also be periods
when no medication is used at all.
Medication Management
A person with a mental illness should be cared
for by a team of providers, which may include
a primary care provider, a psychiatrist, and
a behavioral health professional, such as a
psychologist, social worker, or counselor. Different
members of the care team may serve as primary
contact over time. Medications will typically
be prescribed by the primary care provider or
psychiatrist. The team should work together
to monitor the effects and side effects of the
medication. Monitoring may include blood tests
and checking blood pressure and weight.
KNOWING WHEN TO REFER FOR
MEDICATION MANAGEMENT
Sometimes a nonprescribing professional
in behavioral health (e.g., licensed clinical
social workers, addiction counselors, most
psychologists) will need to refer a client for an
evaluation to explore pharmacotherapy options
and appropriateness. Such situations include
when a client:
•
Has not had success improving symptoms
or functioning after trying multiple
psychotherapies.
•
Has had limited success improving symptoms
or functioning with psychotherapy but is still
experiencing symptoms that are distressing or
interfere with the person’s functioning.
•
Wants to be abstinent but has had difficulty
stopping substance use (especially use of
opioids or alcohol).
•
Reports having previous success with a
medication and expresses an interest in trying
the medication again.
•
Has (or is suspected to have):
- Psychotic symptoms (e.g., hallucinations,
delusions).
- Schizophrenia.
- Severe depression (especially with suicidal
thoughts, behaviors, or attempts).
- Bipolar disorder or mania.
Equally important is knowing to whom you
should refer clients for medication evaluation.
You should refer to primary care or behavioral
health professionals with prescribing privileges,
such as:
•
A physician.
•
A psychiatrist.
•
An advanced practice registered nurse (especially
a psychiatric/mental health specialty nurse).
Considerations for the SUD Treatment
Provider
A patient who appears sedated, agitated, or
intoxicated may be experiencing a medication side
effect or other medical illness. Medications that
work in the brain are considered “psychotropic,"
meaning they affect a person’s mental state. Drugs
of misuse are psychotropic, too. The benefits, side
Chapter 7 221

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
effects, and drug interactions of medications for
mental illness can affect clients similarly to, or look
like some of the effects of, illicit substances. This
may be triggering for the client or those around him
or her or lead to misuse of prescribed medication.
Illicit substances and prescribed medications may
interact with one another, potentially reducing the
beneficial effects of the prescribed medication
(Lindsey, Stewart, & Childress, 2012).
Medication for Depression
Medication can be used to treat major depression
at all levels of severity; it should be started early
and combined with psychotherapy (American
Psychiatric Association [APA], 2010; Schulz &
Arora, 2015). The goal of medication is to relieve
distressing symptoms and help restore function.
Several classes of medications have been approved
for treating depression (FDA, 2017), including
selective serotonin reuptake inhibitors (SSRIs),
serotonin norepinephrine reuptake inhibitors
(SNRIs), tricyclic antidepressants (TCAs), and
monoamine oxidase inhibitors (MAOIs). Each
works in different ways but ultimately treats
depression by changing the balance of chemicals
(neurotransmitters) in the brain that regulate mood,
such as serotonin, norepinephrine, and dopamine.
Sometimes medication not specifically approved
for depression, such as mood stabilizers or anti-
psychotics, will be added to the antidepressant to
address specific symptoms (FDA, 2017).
In 2019, FDA approved the first ever nasal spray
antidepressant (FDA, 2019), derived from a pain
reliever called ketamine. The spray (esketamine)
is specifically for treatment-resistant major
depression and is designed to begin relieving
symptoms, in a matter of hours. Its release
represents the first time FDA has approved a
new antidepressant since the medication Prozac
entered the market in 1988.
Side Eects
Common side effects when antidepressants are
started or when the dose is increased are nausea,
vomiting, and diarrhea (Exhibit 7.6). These usually
improve in a few weeks. Side effects such as weight
gain, sleep disturbances, and sexual dysfunction
can be longer lasting. Some medication side effects
may mimic signs of intoxication or withdrawal
or may be triggering for clients. Medication for
depression might increase suicidal thoughts in
young adults (i.e., people ages 18 through 24).
Some antidepressants are associated with birth
defects or cause the newborn to experience a
withdrawal syndrome.
Medication for Anxiety Disorders
Anxiety disorders are best treated with combined
psychotherapy and medication (Benich, Bragg,
& Freedy, 2016). Medication can help relieve
distressing symptoms. Antidepressants and
benzodiazepines are the most common classes
EXHIBIT 7.6. Side Effects of Antidepressants
MEDICATION CLASS SIDE EFFECTS
SSRI High blood pressure, headache, sexual dysfunction, hyperalertness, restlessness,
teeth grinding, sweating, internal bleeding, insomnia, nausea/vomiting,
osteopenia
SNRI Dry mouth, sexual dysfunction, hyperalertness, restlessness, sweating, insomnia,
nausea/vomiting, weight gain
TCA Irregular heart rhythm, low blood pressure with risk of falls, constipation, dry
mouth, sweating, sedation, weight gain
MAOI High blood pressure, low blood pressure with risk of falls, weight gain
Other Seizure, insomnia, nausea/vomiting, sedation, weight gain
222 Chapter 7

TIP 42Chapter 7—Treatment Models and Settings for People With Co-Occurring Disorders
A NOTE ABOUT SEROTONIN SYNDROME
Serotonin syndrome is a potentially fatal condition caused by too much serotonin (Bartlett, 2017). It can
occur if a person takes too much of a prescribed SSRI or SNRI or when multiple prescribed medications
interact. Over-the-counter cold and allergy medications and certain illicit substances (e.g., cocaine, other
stimulants, opioids) can also cause serotonin syndrome.
Mild serotonin syndrome can look like opioid withdrawal. More serious serotonin syndrome can look like
intoxication with a stimulant or hallucinogen or withdrawal from a benzodiazepine. Fever, dangerously
high blood pressure, and seizure can lead to organ failure and death if the syndrome is not recognized and
treated. Counselors should remain vigilant for and seek medical evaluation for possible serotonin syndrome
when clients with CODs present with unexpected withdrawal or intoxication symptoms.
of FDA-approved medication for anxiety.
Antidepressants in the SSRI and SNRI classes are
considered first-line therapy. Benzodiazepines
should generally be used only for short periods,
taken per a schedule rather than as needed (Benich
et al., 2016). Taking benzodiazepines with opioids
markedly increases the risk of overdose (NIDA,
Revised March 2018).
Benzodiazepines can cause dependence after
relatively brief periods of regular use. People
dependent on benzodiazepines will experience
withdrawal if they stop taking them abruptly.
Side effects of antidepressants prescribed for
anxiety are the same as those for depression
(Exhibit 7.6). Benzodiazepines carry an increased
risk of central nervous system depression, which
can lead to sedation, fatigue, dizziness, and
impaired driving ability (Bandelow, Michaelis, &
Wedekind, 2017). Older adults taking benzodiaze-
pines can have negative changes in cognition, such
as memory, learning, and attention. Older adults
taking benzodiazepines are thus at an increased
risk of falls and fracture (Markota, Rummans,
Bostwick, & Lapid, 2016).
Medication for PTSD
Medication combined with psychotherapy can be
effective in relieving symptoms of PTSD (VA/DoD,
2017). The FDA has approved two SSRIs for the
The pharmacist from whom a client gets his
or her prescriptions may be a helpful source
of information if counselors have concerns or
questions about side effects or drug interactions.
treatment of PTSD. Studies are also underway to
explore the benefit of using certain antipsychotics
in PTSD.
Medication for Bipolar Disorder
Bipolar disorder is typically managed with both
medication and psychotherapy, given its lifelong
course and need for continuous treatment
(SAMHSA, 2016). The goal of medication in
bipolar disorder is to prevent or suppress mania
while relieving depression (Fountoulakis et al.,
2017). Sometimes people will have already
begun treatment for depression when mania
presents for the first time. When this happens,
the antidepressant may be stopped and restarted
later. Medications used to treat bipolar disorder
are often referred to as “mood stabilizers.” This
is not a single class of medication but a group of
different types of medications that reduce the
abnormal brain activity that causes mania and
rapidly changing mood states. Mood stabilizers,
antiseizure medications, and antipsychotic
medications may be used to treat bipolar
disorder; sometimes these medications are used in
combination.
Mood Stabilizers
Medication to prevent severe mood fluctuations
can be effective at treating mania, particularly the
first-line medication lithium (Fountoulakis et al.,
2017). Mood stabilizers treat and prevent mania
by decreasing abnormal activity in the brain.
People taking lithium need to see a physician
regularly for monitoring of blood levels and kidney
and thyroid functioning. Side effects that may
improve with time are nausea, diarrhea, dizziness,
muscle weakness, fatigue, and feeling “dazed.”
Chapter 7 223
TIP 42 Substance Use Disorder Treatment for People With Co-Occurring Disorders
Other symptoms are likely to continue, such as
fine tremor, frequent urination, and thirst. Lithium
can cause skin disorders like acne, psoriasis, and
rashes. Serious side effects include irregular heart
rhythm and serotonin syndrome. Anesthesia and
antidepressants are associated with serotonin
syndrome when taken with lithium. Elevated
blood levels of lithium can cause uncontrollable
shaking, clumsiness, ringing in the ears, slurred
speech, and blurred vision. Salt, caffeine, alcohol,
other medications, and dosing mistakes can
cause lithium toxicity, which can be a medical
emergency.
Antiseizure Medication
Antiepileptic medications can be used to treat
bipolar disorder (Fountoulakis et al., 2017; National
Institute of Mental Health [NIMH], 2016). These
medications may have both benign and life-
threatening side effects, including rash, damage to
internal organs, and a decrease in blood cells (e.g.,
platelets, white blood cells). These medications
can interact negatively with medications used to
treat common medical concerns, such as diabetes
and high blood pressure. They also can make
hormonal contraceptives less effective. Other
serious side effects include peeling or blistering of
the skin, bruising, bleeding, weakness, headache,
stiff neck, chest pain, nausea/vomiting, vision
changes, swelling of the face/eyes/lips, dark urine,
yellowing of the skin or eyes, abnormal heartbeat,
loss of appetite, and abdominal pain. Common but
less-serious side effects include blurred or double
vision; dizziness; uncontrollable movements;
sleepiness; weight change; ringing in the ears; hair
loss; back, stomach, or joint pain; painful menstrual
periods; confusion; difficulty speaking; and dry
mouth.
Antipsychotic Medication
Antipsychotic medication may be used to treat
mania with psychosis. See the section “Medication
for Schizophrenia and Other Psychotic Disorders”
for detailed information about the medications.
Tobacco smoke affects how medications
are absorbed, spread through the body, are
metabolized, and eliminated by the body; how
medications work can also be affected (Lucas &
Martin, 2013). Changing the amount of tobacco
smoked, including stopping or starting, can
interfere with medication effectiveness or risk of
side effects.
Medication for Schizophrenia and Other
Psychotic Disorders
Antipsychotics are the most common medications
for schizophrenia and other psychotic disorders
(Lally & MacCabe, 2015; Patel, Cherian, Gohil, &
Atkinson, 2014). They have many side effects and
require careful monitoring. Most are taken daily,
but a few long-lasting forms can be administered
once or twice a month.
Antipsychotics are divided into two categories:
“first-generation” or “typical” antipsychotics and
“second-generation” or “atypical” antipsychotics.
Both types can be used to help treat schizophrenia
and mania related to bipolar disorder. Some
antipsychotics have a wider range of uses,
including severe depression, generalized anxiety
disorder, obsessive-compulsive disorder, PTSD,
dementia, and delirium. Symptoms such as
agitation and hallucinations may remit within a
few days of starting the medication, whereas
delusions may take a few weeks to resolve. The
full effect of an antipsychotic may not be seen for
up to 6 weeks. A person may need to stay on the
antipsychotic for months or years to stay well.
Side Eects
All antipsychotics have the potential to cause side
effects such as drowsiness, dizziness, restlessness,
dry mouth, constipation, nausea, vomiting, blurred
vision, low blood pressure, and uncontrollable
muscle movements (NIMH, 2016). People who
take antipsychotics need to have their blood cell
counts, blood glucose, and cholesterol monitored
by a healthcare provider. Care should be taken
when starting or stopping other medications,
given the many potential drug interactions,
not all of which are known. The typical or first-
generation antipsychotics may cause rigidity and
224 Chapter 7

TIP 42
Chapter 7—Treatment Models and Settings for People With Co-Occurring Disorders
muscle spasms, tremors, and restlessness. They
may also cause a condition of abnormal muscle
movements called tardive dyskinesia, which can
persist even when the medication is discontinued.
Some antipsychotics cause electrocardiogram
abnormalities, such as QT prolongation, a
condition in which the heart takes longer to
recharge between beats. An individual can
overdose on antipsychotics, especially if they are
combined with alcohol or other sedating drugs.
Medication for Attention Decit
Hyperactivity Disorder
Attention deficit hyperactivity disorder (ADHD)
in adults may be treated with short- or long-
acting stimulants, nonstimulant medications,
and behavioral therapy (NIMH, 2016). Typically,
a nonstimulant medication is prescribed first;
a stimulant is prescribed only if nonstimulant
response is insufficient. Stimulant medications help
people with ADHD focus and feel calmer but can
cause euphoria (SAMHSA, 2015a).
Stimulants may be misused by people who have
no prescription. Typically, people who misuse
stimulants are motivated to improve academic/
work performance and hope to experience
enhanced concentration and alertness rather than
euphoria. Many people who consistently misuse
prescription stimulants exhibit symptoms of ADHD.
Adults who are prescribed stimulants for ADHD
may misuse them by taking larger doses than
prescribed. Some evidence exists that adults who
misuse stimulants prescribed to them are more
likely to report misuse of other substances as well
(Wilens et al., 2016).
No specific guidelines exist on whether stimulants
should be prescribed for co-occurring ADHD in
people with SUDs. Available research is unclear as
to whether stimulants are effective for ADHD in
the presence of an SUD. Although efficacious in
reducing ADHD symptoms, stimulant medications
generally do not alleviate SUD symptoms (Cunill
et al., 2015; De Crescenzo et al., 2017; Luo &
Levin, 2017). Thus, ADHD medication alone, if
used at all, is an insufficient treatment approach
for ADHD-SUD (Crunelle et al., 2018; Zulauf et
al., 2014). Stimulants do have misuse potential,
but current evidence suggests that most people
with ADHD and SUD generally do not divert or
misuse stimulant medication for ADHD (e.g., to
experience euphoria) (Luo & Levin, 2017). However,
diversion can and does occur in some people. Use
of long-acting or extended-release medication or
of antidepressants instead of stimulants can help
reduce the chances of diversion and misuse.
Medications for ADHD can have potentially life-
threatening cardiovascular side effects (Sinha,
Lewis, Kumar, Yeruva, & Curry, 2016). Changes in
heart rhythm and blood pressure can occur that raise
risk of stroke and heart attack, especially in adults
with preexisting heart conditions (Zukkoor, 2015).
These medications should be prescribed cautiously
and with consideration of the client’s personal and
family history of cardiovascular problems. Combined
medication and psychotherapy may provide the
best long-term relief of ADHD symptoms (Arnold,
Hodgkins, Caci, Kahle, & Young, 2015).
Medication for PDs
No medications are FDA approved to treat any PD.
Antidepressants, mood stabilizers, antipsychotics,
and antianxiety medications can be prescribed to
target symptoms/improve function.
Medication for Feeding and Eating Disorders
Medication is generally not a first-line or standalone
treatment approach for eating disorders, and only
one medication—the SSRI fluoxetine (Prozac)—is
approved by the FDA to treat these conditions
(specifically, bulimia nervosa [BN]) (Davis & Attia,
2017). Other antidepressants may be effective for
the management of BN and binge eating disorder
(BED) but have been relatively less successful with
anorexia nervosa (AN; Davis & Attia, 2017). Second-
generation antipsychotics (notably olanzapine) may
offer a promising pharmacotherapy option for AN,
but more research is needed (Davis & Attia, 2017).
Certain stimulants known to suppress appetite have
shown some success with reducing symptoms of
BED (Davis & Attia, 2017).
Medication for SUDs
Because SUDs are brain-based diseases,
pharmacologic research has explored the
development of agents that can effectively
target disruptions in neurotransmitters and
Chapter 7 225

TIP 42 Substance Use Disorder Treatment for People With Co-Occurring Disorders
neuromodulators that occur as a part of addiction.
These medications often help reduce withdrawal
symptoms or craving, which in turn can make
abstinence easier to achieve and sustain. In
general, pharmacotherapy for SUDs is considered
supportive rather than curative and is typically
combined with psychotherapy, behavioral
counseling, psychoeducation, mutual support,
other recovery services, or a combination of these.
The sections that follow briefly discuss
medications for AUD and OUD. Currently no
FDA-approved pharmacotherapies exist for
cocaine, methamphetamine, or cannabis use
disorders. Clinicians often use FDA-approved
nicotine replacement therapy and nonnicotine
medications to manage tobacco use disorder.
Tobacco use is outside the scope of this TIP, so
these pharmacotherapies are not discussed.
Readers interested in learning more can review
FDA’s guidance about medication to support
tobacco cessation (www.fda.gov/ForConsumers/
ConsumerUpdates/ucm198176.htm).
Medication use by people battling addiction
has been controversial given attitudes by some
providers and mutual-support programs, like AA
and Narcotics Anonymous, that view medication
use as incompatible with abstinence and
therefore not a valid part of recovery. Counselors
should be sensitive to this and educate clients
about the potential value of medication as well as
possible negative reactions they might face from
some mutual-support programs and addiction
professionals.
Medication is not a cure for addiction and
is not right for everyone. But the science
is clear: in certain instances (e.g., for OUD),
pharmacotherapy can not only help improve
lives, it can help save them as well.
Medication for AUD
Three medications are FDA approved for AUD
(disulfiram, naltrexone, and acamprosate), and
each has a different mechanism of action. These
include disincentivizing use by causing unpleasant
side effects (e.g., nausea, headache, vomiting)
when alcohol is consumed (disulfiram); blocking
the euphoric effects of intoxication (naltrexone);
and normalizing neurotransmitter activity
that is dysregulated in addiction and during
withdrawal (acamprosate). Other medications,
including anticonvulsants, antipsychotics, and
antidepressants, can help reduce consumption and
craving and potentially help support abstinence
(Akbar, Egli, Cho, Song, & Noronha, 2018).
Medication for OUD
Unlike AUD and other SUDs, pharmacotherapy
(with or without adjunctive psychosocial
treatment) is the recommended approach
to managing OUD. Ample research strongly
supports the effectiveness of MAT` for OUD in
increasing abstinence, preventing or reversing
overdose, reducing risk of relapse, and mitigating
negative outcomes associated with opioid
addiction, like infectious diseases and incarceration
(SAMHSA, 2018c). FDA-approved medications
for OUD include methadone, buprenorphine,
and naltrexone. In addition, the FDA-approved
rescue medication naloxone can rapidly reverse
opioid overdose and prevent fatality. Readers
should consult TIP 63, Medications for Opioid
Use Disorder (SAMHSA, 2018c), for extensive
information about opioid pharmacotherapy and
its role in helping clients manage symptoms and
achieve long-term recovery.
226 Chapter 7

TIP 42
Chapter 7—Treatment Models and Settings for People With Co-Occurring Disorders
RESOURCE ALERT: LEARNING MORE ABOUT PHARMACOTHERAPY AND CODs
Pharmacology interventions can be safe and effective for many individuals with CODs. Although
prescribing is outside the practice of addiction counselors, licensed clinical social workers, and most
psychologists, all providers should become familiar with common psychotropic medications, their side
effects, and their potential risks. Following are several resources to help nonprescribing behavioral health
service providers learn more about pharmacotherapy for mental disorders and SUDs:
• SAMHSA’s TIP 63, Medications for Opioid Use Disorder (https://store.samhsa.gov/product/
TIP-63-Medications-for-Opioid-Use-Disorder)
• SAMHSA’s Medication for the Treatment of Alcohol Use Disorder: A Brief Guide (https://store.samhsa.gov/
system/files/sma15-4907.pdf)
• APA’s Practice Guideline for the Pharmacological Treatment of Patients With Alcohol Use Disorder
(https://psychiatryonline.org/doi/pdf/10.1176/appi.books.9781615371969)
• National Library of Medicine’s Drug Information Portal (https://druginfo.nlm.nih.gov/drugportal/)
• FDA’s Medication Guides (www.fda.gov/drugs/drugsafety/ucm085729.htm)
• NIMH’s Mental Health Medications (www.nimh.nih.gov/health/topics/mental-health-medications/index.
shtml)
• University of Washington’s Commonly Prescribed Psychotropic Medications (https://aims.uw.edu/
resource-library/commonly-prescribed-psychotropic-medications)
Conclusion
CODs are exceedingly common in both the SUD
population and the mental illness population, and
addiction counselors should expect to see both
conditions in their work. A wide range of treatment
approaches are available and can be adapted to
the specific needs of people with CODs, including
their symptoms as well as their stages of change
and readiness to engage in services. Because the
disease course of SUDs and mental disorders is
often unstable and unpredictable, counselors must
be ready to offer COD-appropriate interventions
across all settings, including nontraditional settings
like jails and prisons. Continuous, integrated
treatment modalities that link clients with resources
and supports in the community give people with
addiction the best chances at achieving lasting
recovery.
Chapter 7 227
This page intentionally left blank.

Chapter 8—Workforce and Administrative
Concerns in Working With People Who Have
Co-Occurring Disorders
KEY MESSAGES
TIP 42
SUBSTANCE USE DISORDER TREATMENT FOR
PEOPLE WITH CO-OCCURRING DISORDERS
• Mental health and addiction labor force
problems directly affect treatment access,
quality, and cost. Without addressing gaps in
personnel and training, the behavioral health
field will struggle to meet the needs of the
growing numbers of people living with co-
occurring disorders (CODs).
• Although current workforce challenges may
seem daunting, substance use disorder (SUD)
treatment supervisors and administrators can
help confront and overcome these difficulties
by creating, implementing, and sustaining
professional development and training
opportunities within their organizations.
This in turn will help support the uptake and
utilization of best practices.
• Recruitment and retention priorities are
urgently needed because of the challenging
nature of the addiction and mental health
service professions, which leads to high rates
of staff burnout and turnover.
• Professional education and accreditation,
combined with mentoring and supervision,
can help increase adoption of core and
advanced clinical competencies, increase
providers’ comfort with working with people
who have CODs, reduce stigma surrounding
the profession/field, and provide structured
career development.
Availability, quality, and cost of SUD treatment and
mental health services are intricately tied to the
current state of the behavioral health workforce.
Without a robust, sizeable labor force, how will
people with mental disorders and addiction
problems have their needs met? Without enough
trainees entering the field or staff willing to stay in
their jobs long term, how will addiction and mental
health service organizations keep their doors open?
What sort of ripple effects might an understaffed
or ill-prepared workforce have on our healthcare
system, economy, and society as a whole?
Rather than serve as a primer on labor difficulties
in the mental health and addiction fields, this
chapter—addressed primarily to supervisors and
administrators—provides an informative update on
the current state of mental health and addictions
professions. The goal is to help supervisors,
administrators, and other organizational leadership
understand aspects of the workforce relevant to
their organization’s ability to provide high-quality,
cost-effective, evidence-based services for CODs
and help them feel better prepared to address
workforce gaps in their own agency.
This chapter is divided into two main sections:
•
The first half addresses recruitment, hiring, and
retention in the behavioral health workforce.
Finding, getting, and keeping the right
employees is critical to ensuring the long-term
sustainability, viability, and effectiveness of the
field. Toward that end, the chapter contains links
to practical, web-based resources for programs
and administrators, including toolkits and
manuals.
•
The second half of this chapter focuses on
ensuring the competency and professional
development of program staff. This section
includes detailed discussions about the role of
training, supervision, and credentialing, all of
which are necessary components of preparing
the field to deliver evidence-based care and
fostering increased service provision.
229

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
Note that general guidelines aimed at supervisors
and administrators serving people with CODs are
in Chapter 2 and information about implementing
various treatment models and settings is in
Chapter 7.
This chapter discusses training needs for
addiction counselors working with clients who
have CODs. However, any behavioral health
service provider in any setting (e.g., primary
care, a social worker’s office, SUD treatment, a
psychologist’s/psychiatrist’s office) should have
the skills and competencies to recognize CODs
and provide at least a basic screening that
encompasses CODs, with enough knowledge
of community resources to refer for integrated
COD treatment if the provider can’t provide such
treatment himself/herself.
Recruitment, Hiring, and
Retention
As of March 2020, the Health Resources and
Services Administration (HRSA) has identified
approximately 5,537 mental health professional
shortage areas in the United States, requiring 6,387
mental health practitioners to fill the shortage
(HRSA, 2020). The behavioral health workforce
is fraught with profession gaps and similar
challenges that serve as barriers to treatment
access for people with mental disorders and
SUDs. For instance (Olfson, 2016; Weil, 2015):
•
Formal education in psychology and psychiatry
is time consuming and costly, making it harder
to recruit and retain trainees.
•
The number of medical trainees specializing in
psychiatry is shrinking.
•
Within psychiatry, types of services provided are
variable (e.g., medication management only vs.
psychotherapy and pharmacotherapy).
•
Psychiatrists are less likely to accept Medicaid
than other medical specialties, which is
particularly damaging to individuals with serious
mental illness (SMI), like schizophrenia, who
often require public assistance. Psychologists
also are unlikely to accept Medicaid given low
reimbursement rates.
•
Psychologists and psychiatrists tend to
be disproportionately clustered in certain
geographic regions, leaving shortages in rural
areas (vs. more affluent urban and suburban
areas) and particular regions of the United
States (e.g., Midwest, Deep South).
•
People with SMI are grossly underserved due
in part to factors like lack of formal training
opportunities in SMI and low provider comfort
with working with these populations.
•
Social workers and primary care providers can
help fill critical workforce and service gaps
A focus group of mental health and SUD treat-
ment providers identified organizational and sys-
tem-related factors they believed hindered their
ability to adequately care for clients with CODs
(Padwa, Guerrero, Braslow, & Fenwick, 2015):
•
Lack of support for COD services, such as
low allocation of resources, discontinuing
consultations with outside COD experts,
discontinuing onsite drug testing of clients, and
not implementing integrated care procedures
even when already developed by staff
•
Lack of COD training opportunities
•
An inability to bill for CODs (e.g., certain
organizations would only permit billing for
mental health services and not SUD treatment)
•
Lack of local addiction services, which make
coordinating care, referring clients to specialty
services, and linking clients to needed
resources more difficult. Even when these
services are present, available slots are limited
and wait-times are often long.
•
Large caseloads and limited time to work with
clients
•
Difficulty initiating and maintaining contact
with outside SUD treatment providers,
especially with providers in residential
treatment settings
•
Fragmented, nonintegrated care that results
in different providers using different (and
sometimes opposing) treatment approaches
with the same client. This is particularly
problematic when clients on pharmacotherapy
attend mutual-support groups or treatment
programs that strongly discourage
psychotropic medication.
230 Chapter 8

TIP 42
Chapter 8—Workforce and Administrative Concerns
left by psychiatry and psychology (particularly
in treating clients with SMI), but this will
require additional training in behavioral health
assessment, diagnosis, and treatment and better
compensation.
Recruitment and Retention
The documented workforce shortage in SUD
treatment and mental health services underscores
the need for aggressive, effective, and even
creative recruitment and hiring strategies and
policies. Extended vacancies in behavioral health
service positions leave programs—and the clients
they serve—vulnerable to negative outcomes
like further turnover, high stress, low morale, and
fragmented, ineffective care.
The ability to recruit and hire quality, long-term
employees first requires attracting the right
candidates. Job postings and advertisements
in multiple outlets, such as websites, on social
media, at job fairs, in newspapers, and within the
community, can increase exposure and widen the
potential pool of applications. Less traditional but
nonetheless effective places to advertise include
churches, synagogues, and other faith-based
organizations; community welfare agencies and
housing offices; shopping centers; and health
clinics and senior centers. Staff referral incentives
encourage current employees to act as recruiters
and also help increase retention.
Exhibit 8.1 outlines steps from the Substance
Abuse and Mental Health Services Administration’s
(SAMHSA) Recruitment and Retention Toolkit,
designed to aid behavioral health service
organizations in building more effective
recruitment, hiring, and retention practices. The
toolkit offers a six-step approach and includes
numerous resources (e.g., templates, samples,
worksheets) to guide programs at each step
(see “Resource Alert: Recruitment and Retention
Resources for the Behavioral Health Workforce”).
EXHIBIT 8.1. Building an Effective Recruitment and Retention Plan for
Behavioral Health Service Providers
•
Step 1. Gather organizational baseline information. Before programs can effectively recruit and hire
the right personnel, they first need to assess the landscape: What are the current retention rates for
healthcare providers? What previously used recruitment and hiring strategies have proved effective and
ineffective for the field? What can be learned about job satisfaction from exit interviews?
•
Step 2. Decide on a priority recruitment and retention focus (job position). Programs should gather
and analyze data to identify their most pressing hiring needs and challenges. This should result in
programs selecting the most urgent priority position to fill.
•
Step 3. Analyze the selected job position. Once a priority position is selected from Step 2, programs
need to identify the benefits and challenges of the position to develop a clear and accurate position
description.
•
Step 4. Write an accurate job description. The position description needs to be articulate, direct, and
thorough to attract the best fitting, most qualified candidates possible.
•
Step 5. Identify the strategy and intervention. Programs can choose from among several options the
best recruitment or retention strategy that fits their needs and that they feel will be most effective at
helping them overcome their specific challenges.
•
Step 6. Develop an action plan. At this step, the strategy and intervention are implemented. In
preparation, programs should develop and assign specific tasks; appoint managers to oversee the
process; define outcomes for their intervention; determine steps for monitoring, communicating about,
and assessing the intervention’s effectiveness; and finalize the implementation plan.
Source: SAMHSA (n.d.).
Chapter 8 231
TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
RESOURCE ALERT: RECRUITMENT AND RETENTION RESOURCES FOR THE
BEHAVIORAL HEALTH WORKFORCE
•
Addiction Technology Transfer Center (ATTC) Network’s National Workforce Report 2017: Strategies for
Recruitment, Retention, and Development of the Substance Use Disorder Treatment and Recovery
Services Workforce (https://attcnetwork.org/centers/global-attc/national-workforce-study)
•
Behavioral Health Education Center of Nebraska’s Retention Toolkit (www.naadac.org/assets/2416/
samhsa-naadac_workforce_bhecn_retention_toolkit2.pdf)
•
National Association for Alcoholism and Drug Abuse Counselors (NAADAC) and SAMHSA webinar, Focus
on the Addiction and Mental Health Workforce: Increasing Retention For Today and Tomorrow (www.
naadac.org/assets/2416/2016-09-12_wf_retention_webinarslides.pdf)
•
SAMHSA Recruitment and Retention Toolkit (http://toolkit.ahpnet.com/Home.aspx)
Reducing Sta Turnover
Behavioral health service provider turnover and
burnout can strain organizational infrastructure,
prevent clients from receiving much-needed
services, and weaken the field as a whole. The
Department of Labor’s Bureau of Labor Statistics
estimates a national turnover rate across all
professions of around 3.7 percent (Bureau of Labor
Statistics, February 11, 2020). By comparison,
turnover in the behavioral health field is quite
high. Among addiction counselors and supervisors,
average annual turnover has been estimated to
range between 23 percent and 33 percent (Eby,
Burk, & Maher, 2010; Knight, Broome, Edwards,
& Flynn, 2011; Laschober & Eby, 2013) and
between approximately 17 percent and 26 percent
among mental health therapists and supervisors
(Beidas et al., 2016; Bukach, Ejaz, Dawson, &
Gitter, 2017). In both sectors, turnover is usually
voluntary—an additional cause for concern.
Reasons for behavioral health service providers to
leave their jobs voluntarily include burnout (driven
by factors like high workload and not having a clear
understanding of job roles and duties), low levels
of support from supervisors and coworkers, and job
dissatisfaction (related to high workload and poor
supervisory relationships) (Garner & Hunter, 2014;
Yanchus, Periard, & Osatuke, 2017; Young, 2015).
(Also see the section “Avoiding Burnout.”)
Turnover is destabilizing to an agency for
numerous reasons (Young, 2015). Turnover often
negatively affects an organization’s capacity to
serve clients, efficiency, profit-earning potential,
operational spending, and staff morale and stress
levels. The issue of staff turnover is especially
important for professionals working with clients
who have CODs because of the limited workforce
pool and the high investment of time and effort
involved in developing a trained workforce. It
matters, too, because of the crucial importance of
the treatment relationship to successful outcomes.
Rapid turnover disrupts the context in which
recovery occurs. Clients in such agencies may
become discouraged about the possibility of being
helped by others.
Turnover sometimes results from the unique
professional and emotional demands of working
with clients who have CODs. On the other hand,
most providers in this area are very dedicated
and find the work to be rewarding. Evidence
suggests that turnover may be connected to
providers’ feelings of preparedness to serve clients
with CODs. SUD treatment providers who leave
an organization but stay in the field (program
turnover) are more likely to have formal education,
training, and experience in SUDs than addiction
counselors who leave an organization and withdraw
from the field entirely (profession turnover)
(Eby, Laschober, & Curtis, 2014). This suggests
that programmatic training and professional
development could help strengthen not only the
individual agency but the workforce as a whole.
Turnover in the addiction field is linked to
attitudinal and organizational predictors, including
lower job satisfaction, lower job involvement,
less support from supervisors or coworkers, and
poor role manageability (Garner & Hunter, 2014).
These factors are largely modifiable and are
232 Chapter 8

TIP 42
Chapter 8—Workforce and Administrative Concerns
EXHIBIT 8.2. Reducing Staff Turnover in Programs for Clients With CODs
To decrease staff turnover, whenever possible, programs should:
•
Hire staff members who have familiarity with both SUDs and mental disorders and have a positive regard
for clients with either disorder.
•
Hire staff members who are critically minded and can think independently, but who are also willing to
ask questions and listen, remain open to new ideas, maintain flexibility, work cooperatively, and engage in
creative problem-solving.
•
Provide staff with a framework of realistic expectations for the progress of clients with CODs.
•
Establish reasonable client caseloads and scheduled time during work hours to follow-up with case
management matters and paperwork.
•
Provide opportunities for consultation among staff members who share the same client (including
medication providers).
•
Ensure that supervisory staff are supportive and knowledgeable about areas specific to clients with CODs.
•
Provide and support opportunities for further education and training.
•
Provide structured opportunities for staff feedback in the areas of program design and implementation.
•
Solicit feedback from staff about their perceptions of the work environment, including levels of support,
civility, resource needs, and relationships with supervisors.
•
Conduct exit interviews with departing employees to gather perspectives on areas for improvement.
•
Promote knowledge of, and advocacy for, CODs among administrative staff, including those in decision-
making positions (e.g., directors) and others (e.g., financial officers, billing personnel, state reporting monitors).
•
Provide a desirable work environment through adequate compensation, salary incentives for COD
expertise, opportunities for training and for career advancement, involvement in quality improvement or
clinical research activities, and efforts to adjust workloads.
important targets for monitoring and implementing
programmatic changes to help providers feel
satisfied, supported, and competent on the job
(Yanchus et al., 2017). Exhibit 8.2 offers methods
for reducing staff turnover.
Avoiding Burnout
A logical approach to reducing turnover is to
prevent the occurrence of burnout. Burnout
has been reported in as much as 67 percent of
professionals in the mental health field (Morse,
Salyers, Rollins, Monroe-DeVita, & Pfahler, 2012).
Reasons mirror those for turnover, including, but
not limited to, demanding workloads and not
feeling rewarded by one’s work (Young, 2015).
Often, mental health service and SUD treatment
providers are expected to manage growing and
more complex caseloads. “Compassion fatigue”
may occur when the pressures of work erode
a counselor’s spirit and outlook and begin to
interfere with the counselor’s personal life; see
also Treatment Improvement Protocol (TIP) 36,
Substance Abuse Treatment for Persons With Child
Abuse and Neglect Issues (Center for Substance
Abuse Treatment [CSAT], 2000c, p. 64). Assisting
clients who have CODs is difficult and emotionally
taxing; the danger of burnout is considerable.
Program administrators must maintain awareness
of the problem of burnout and the benefits of
reducing turnover. Program administrators must
demonstrate interest in staff well-being to sustain
morale and team cohesion.
To lessen burnout among counselors working with
a demanding caseload that includes clients with
CODs, behavioral health service organizations
should (Atkinson, Rodman, Thuras, Shiroma, &
Chapter 8 233
TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
RESOURCE ALERT: DEALING WITH
STRESS IN BEHAVIORAL HEALTH
SERVICE SETTINGS
SAMHSA’s Recruitment and Retention Toolkit
chapter, Dealing With Stress in the Workplace:
Frustration, Stress, and Compassion Fatigue/
Burnout (http://toolkit.ahpnet.com/Dealing-with-
Stress-in-the-Workplace.aspx)
Lime, 2017; Oser, Biebel, Pullen, & Harp, 2013;
Morse et al., 2012):
•
Create a collegial environment for staff,
particularly by encouraging support between
coworkers.
•
Increase the amount of supervision given to
staff, not only for skill building but because
supervision can serve as another outlet for
emotional support and encouragement much
needed by providers.
•
Advocate for and help staff cultivate self-care
and self-compassion. For instance, provide
staff with cognitive–behavioral interventions
to improve their coping skills, foster positive
attitudes, and increase relaxation, and promote
mindfulness.
•
Decrease workloads, increase provider
autonomy, and clarify roles and expectations.
Competency and Professional
Development
This section focuses on some key areas programs
face in developing a workforce able to meet the
needs of clients with CODs. These include:
•
The attitudes and values providers must have to
work successfully with these clients.
•
Essential competencies for providers (basic,
intermediate, and advanced).
•
Opportunities for continuing professional
development as well as professional licensure.
Areas of weakness exist in many COD programs’
services, staff training/supervision, and staff com-
petencies (Petrakis, Robinson, Myers, Kroes, &
O’Connor, 2018). Of 256 U.S. addiction treatment
and mental health service programs surveyed
(McGovern et al., 2014), only 18 percent of SUD
programs and 9 percent of mental disorder
programs were COD capable. In a survey of 30
publicly funded COD programs (Padwa et al., 2013):
•
About 43 percent met or exceeded criteria for
COD-capable programming.
•
About half had mission statements, organizational
certification and licensure, service coordination,
and financial incentives focused on treating either
mental illness or SUDs but not both.
•
24 of 30 programs could only bill for mental
health services or SUD treatment but not both.
•
18 programs routinely used clinical interview
assessment techniques adapted to CODs,
but only 6 of those programs had formal
standardized screening tools for CODs. Only
five programs had formal procedures in place to
conduct comprehensive assessments of clients
who screen positive for CODs.
•
Most programs lacked stagewise treatments
specifically for CODs, including a lack of
psychoeducation about and recovery support
for both mental disorders and SUDs.
•
18 programs had onsite prescribers.
•
23 programs used supervision and consultation
to address mental conditions and substance
use. However, most programs did not have
licensed or otherwise competently trained
staff to provide COD services other than
pharmacotherapy management.
•
Over 80 percent of the sites offered direct staff
training in basic competencies (e.g., prevalence,
signs and symptoms, assessment procedures),
but only about 57 percent of programs had
staff with at least some advanced competency
training in treating CODs.
The consensus panel underscores the importance
of an investment in creating a supportive
environment for staff that encourages professional
development to include skill acquisition, values
clarification, training, and competency attainment
equal to an investment in new COD program
development. An organizational commitment to
both is necessary for successful implementation
of programs. Examples of staff support may
include standards of practice related to consistent
234 Chapter 8
TIP 42
Chapter 8—Workforce and Administrative Concerns
high-quality supervision, favorable tuition
reimbursement and release-time policies, helpful
personnel policies related to bolstering staff
wellness practices, and incentives or rewards
for work-related achievement. Together these
elements help create an environment in which
high-quality service can thrive.
In support of all behavioral health service providers
embodying the “no wrong door” policy for service
readiness, the consensus panel strongly suggests
all administrators consider providing COD
training as part of their workforce development
for staff, even if their program is not a specialty
COD program.
Attitudes and Values
Attitudes and values guide the way providers
meet client needs and affect the overall treatment
climate. They not only determine how the client
is viewed by the provider (thereby generating
assumptions that could either facilitate or deter
achievement of the highest standard of care), but
also profoundly influence how the client feels as
he or she experiences a program. Attitudes and
values are particularly important in working with
clients who have CODs because the counselor is
confronted with two disorders that require complex
interventions.
Attitudes and values are important targets of
professional development and training. Some
research indicates that behavioral health service
providers and trainees have more negative attitudes
toward people with SMI and with SUDs—either
separately or in combination—than they do toward
people with medical or other mental disorders, and
that attitudes toward individuals with comorbid
SUDs and psychotic disorders in particular are
among the most negative and worsen over time
(Avery et al., 2016; Avery et al., 2017; Avery &
Zerbo, 2015; Mundon, Anderson, & Najavits, 2015).
Education-focused training and increased exposure
to SMI, SUD, and COD populations could potentially
help increase provider comfort, competency, and
confidence while diluting personal biases that
directly affect clinical care.
The essential attitudes and values for working with
clients who have CODs shown in Exhibit 8.3 are
adapted from Technical Assistance Publication
21, Addiction Counseling Competencies: The
Knowledge, Skills, and Attitudes of Professional
Practice (CSAT, 2006a). The consensus panel
believes these attitudes and values also are
consistent with the attitudes and values of the vast
majority of those who commit themselves to the
challenging fields of SUD treatment and mental
health services.
EXHIBIT 8.3. Essential Attitudes and Values for Providers Serving
Clients With CODs
•
Desire and willingness to work with people who have CODs
•
Appreciation of the complexity of CODs
•
Openness to new information
•
Awareness of personal reactions and feelings
•
Recognition of the limitations of one’s own personal knowledge and expertise
•
Recognition of the value of client input into treatment goals and receptivity to client feedback
•
Patience, perseverance, and therapeutic optimism
•
Ability to use diverse theories, concepts, models, and methods
•
Flexibility of approach
•
Cultural competence
•
Belief that all people have strengths and are capable of growth and development
•
Recognition of the rights of clients with CODs, including the right and need to understand assessment
results and the treatment plan
Chapter 8 235

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
How To Improve Providers’ Attitudes Toward
Clients With CODs
Several strategies can help reduce stigma and
negative attitudes and opinions among behavioral
health service providers about people with CODs.
These include (Avery et al., 2016):
•
Increasing didactic and clinical exposure to
clients with these disorders to improve provider
knowledge and experience.
•
Providing education about commonly held
negative attitudes and misperceptions about
CODs, and encouraging trainees to reflect on
and discuss their own experiences and beliefs
(e.g., via journaling, writing reflection papers).
•
Offering supervision and mentorship by senior
providers trained in addiction medicine with
experience working with CODs.
Provider Competencies
Provider competencies are the specific and
measurable skills providers must possess. Several
states, university programs, and expert committees
have defined the key competencies for working
with clients who have CODs. Typically, these
competencies are developed by training mental
health and SUD treatment counselors together,
often using a case-based approach that allows
trainees to experience the insights each field
affords the other.
One challenge of training is to include culturally
sensitive methods and materials that reflect
consideration for the varying levels of expertise
and background of participants. The consensus
panel recommends viewing competencies as basic,
intermediate, and advanced to foster continuing
professional development of all counselors and
clinicians in the field of CODs. Clearly, the sample
competencies listed within each category cannot
be completely separated from each other (e.g.,
competencies in the “basic” category may require
some competency in the “intermediate” category).
Still, the groupings within each category reflect, on
the whole, different levels of provider competency.
Providers in the field face unusual challenges and
often provide effective treatment while working
within their established frameworks. In fact,
research studies previously cited have established
the effectiveness of SUD treatment approaches in
working with people who have low- to moderate-
severity mental disorders. Still, the classification
of competencies supports continued professional
development and promotes training opportunities.
Basic, intermediate, and advanced competencies
are discussed further in the following sections. See
also “Resource Alert: Oregon Health Authority’s
Competency Checklists for COD Providers”
and Technical Assistance Publication (TAP) 21,
Addiction Counseling Competencies (CSAT, 2006a)
for more examples of provider skills within these
competency categories.
Basic Competencies
Every SUD treatment and mental health service
program should require counselors to have certain
basic skills. Basic COD competencies include
having a perfunctory understanding and working
knowledge of the prevalence of CODs, screening
and assessment procedures, common signs and
symptoms, how to triage clients appropriately (e.g.,
referring for specialty care, engaging in treatment),
how to provide brief interventions, and how to
engage clients in treatment decision making
(SAMHSA, 2011b). In keeping with the principle
that there is “no wrong door,” the consensus
panel recommends that clinicians working in SUD
treatment settings be able to carry out the mental
health–related activities shown in Exhibit 8.4.
Intermediate Competencies
Intermediate competencies encompass skills
in engaging SUD treatment clients with CODs,
screening, obtaining and using mental health
assessment data, treatment planning, discharge
planning, mental health system linkage, supporting
medication, running basic mental disorder
education groups, and implementing routine and
emergent mental disorder referral procedures.
In a mental health unit, mental health providers
would exhibit similar competencies related to
SUDs. The consensus panel recommends the
intermediate level competencies shown in Exhibit
8.5, developed jointly by the New York State Office
of Mental Health and the New York State Office of
Alcohol and Substance Abuse Services.
236 Chapter 8
TIP 42
Chapter 8—Workforce and Administrative Concerns
RESOURCE ALERT: OREGON HEALTH AUTHORITY’S COMPETENCY
CHECKLISTS FOR COD PROVIDERS
The Oregon Health Authority maintains a resource webpage (www.oregon.gov/oha/HSD/AMH/Pages/Co-
occurring.aspx) that includes checklists for ensuring that behavioral health service providers working with
clients who have CODs meet basic, intermediate, and advanced competencies:
•
Basic Competencies (www.oregon.gov/oha/HSD/AMH/CoOccurring%20Resources/Basic%20
Compentencies%20Checklist.pdf)
•
Intermediate Competencies (www.oregon.gov/oha/HSD/AMH/CoOccurring%20Resources/
Intermediate%20Compentencies%20CheckList.pdf)
•
Advanced Competencies
•
(www.oregon.gov/oha/HSD/AMH/CoOccurring%20Resources/Advanced%20Competencies%20Checklist.pdf)
EXHIBIT 8.4. Examples of Basic Competencies Needed To Treat People
With CODs
•
Perform a basic screening to determine whether CODs might exist and be able to refer the client for a
formal diagnostic assessment by someone trained to do this.
•
Form a preliminary impression of the nature of the disorder a client may have, which can be verified by
someone formally trained and licensed in mental disorder diagnosis.
•
Conduct a preliminary screening to determine whether a client poses an immediate danger to self or
others and coordinate any subsequent assessment with appropriate staff and consultants.
•
Be able to engage the client in such a way as to enhance and facilitate future interaction.
•
Deescalate the emotional state of a client who is agitated, anxious, angry, or in another vulnerable
emotional state.
•
Manage a crisis involving a client with CODs, including a threat of suicide or harm to others. This may
involve seeking out assistance by others trained to handle certain aspects of such crises—for example,
processing commitment papers and related matters.
•
Refer a client to the appropriate mental health service or SUD treatment facility and follow up to ensure
the client receives needed care.
•
Coordinate care with a mental health counselor serving the same client to ensure that the interaction of
the client’s disorders is well understood and that treatment plans are coordinated.
Chapter 8 237

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
EXHIBIT 8.5. Six Intermediate
Competencies for Treating
People With CODs
•
Competency I: Integrated Diagnosis of
Substance Abuse and Mental Disorders.
Differential diagnosis, terminology (definitions),
pharmacology, laboratory tests and physical
examination, withdrawal symptoms, cultural
factors, effects of trauma on symptoms, staff
self-awareness
•
Competency II: Integrated Assessment of
Treatment Needs. Severity assessment, lethality/
risk, assessment of motivation/readiness for
treatment, appropriateness/treatment selection
•
Competency III: Integrated Treatment Planning.
Goal setting/problem solving, treatment
planning, documentation, confidentiality,
legal/reporting standards, documenting clinical
concerns for managed care providers
•
Competency IV: Engagement and Education.
Staff self-awareness, engagement, motivating,
educating
•
Competency V: Early Integrated Treatment
Methods. Emergency/crisis intervention,
knowledge of and access to treatment services,
when and how to refer or communicate
•
Competency VI: Longer Term Integrated
Treatment Methods. Group treatment,
relapse prevention, case management,
pharmacotherapy, alternatives/risk education,
ethics, confidentiality, mental health, reporting
requirements, family interventions
Confidentiality is governed by the federal
“Confidentiality of Alcohol and Drug Abuse Patient
Records” regulations (42 C.F.R. Part 2) and the federal
“Standards for Privacy of Individually Identifiable Health
Information” (45 C.F.R. Parts 160 and 164).
Advanced Competencies
At the advanced level, the practitioner goes beyond
an awareness of the addiction and mental health
fields as individual disciplines to a more sophisticated
appreciation for how CODs interact. This enhanced
awareness leads to an improved ability to provide
appropriate integrated treatment. At a minimum,
advanced competencies in CODs should include
possessing an indepth knowledge of specific
EXHIBIT 8.6. Examples of
Advanced Competencies for
Treatment of People With CODs
•
Understand the transtheoretical model and
how client motivation and readiness to change
affect behavior.
•
Learn to enhance motivation via motivational
interviewing and motivational enhancement
therapy skills.
•
Be aware of the relapse prevention model
and integrating relapse prevention skills into
treatments.
•
Use criteria from Diagnostic and Statistical
Manual of Mental Disorders (5th ed.; American
Psychiatric Association [APA], 2013) to assess
substance-related and other mental disorders.
•
Understand the effects of level of functioning
and degree of disability related to both
substance-related and mental disorders,
separately and combined.
•
Apply knowledge of psychotropic medications,
their actions, medical risks, side effects, and
possible interactions with other substances.
•
Use integrated models of assessment,
intervention, and recovery for people having
both substance-related and mental disorders,
as opposed to sequential treatment efforts that
resist integration.
•
Collaboratively develop and implement an
integrated treatment plan based on thorough
assessment that addresses both/all disorders
and establishes sequenced goals based on
urgent needs, considering the stage of recovery,
stage of change, and level of engagement.
•
Involve the person, family members, and other
supports and service providers (including peer
supports and those in the natural support
system) in establishing, monitoring, and
refining the current treatment plan.
•
Help clients expand their social networks and
systems of support.
therapies and treatment interventions, assessment
and diagnosis procedures, and basic knowledge of
pharmacotherapies (SAMHSA, 2011b). Exhibit 8.6
gives examples of advanced skills.
238 Chapter 8

TIP 42
Chapter 8—Workforce and Administrative Concerns
Supervision
Staff working in COD programs need relational
skills (Petrakis et al., 2018), skills that are best
learned through clinical supervision. A lack of
high-quality supervision can hinder the ability of
individual providers and programs as a whole to
provide effective, evidence-based treatments
for clients with COD (Petrakis et al., 2018; Sacks
et al., 2013). To feel capable and confident in
delivering appropriate treatments, providers
need regular, ongoing, structured supervision
that not only addresses specific aspects of
individual caseloads but broad didactics about
COD populations as a whole. Active listening,
interviewing techniques, the ability to summarize,
and the capacity to provide feedback are all
skills that can be best modeled by a supervisor.
Strong, active supervision of ongoing cases
is a key element in assisting staff to develop,
maintain, and enhance relational skills. (See also
“Resource Alert: Competencies and Training for
SUD Treatment Supervisors.”) Leadership efforts
among supervisors, administrators, management,
and senior staff help improve the uptake and
provision of evidence-based COD services by
providers and help processes for treating clients
with CODs become part of the culture of the
organization, leading to better outcomes for
clients. Such efforts include actively championing
and encouraging COD-specific clinical training
and supervision practices and securing resources
to support integrated care (Guerrero, Padwa,
Lengnick-Hall, Kong, & Perrigo, 2015).
To achieve COD capability, SAMHSA (2011b)
recommends that programs ideally offer supervi-
sion that:
•
Is provided by professionals with licensure/
certification in the addiction field, such as
licensed/certified addiction counselors, clinical
psychologists, psychiatrists, clinical social
workers, psychological counselors, marriage and
family therapists, and specialty practice nurse
practitioners (psychiatric and mental health
nurses).
•
Is provided formally and routinely, preferably
onsite. Otherwise, supervision should at least
be available as needed and offered on a
semistructured basis.
•
Includes a focus on assessment and treatment
skill development and, at the very least, should
cover topics of case disposition and crisis
management.
•
Is performed individually, in groups, or both.
•
Uses multiple methods of oversight, such as
reviewing provider–supervisor rating forms,
reviewing audio/video recordings of client
sessions, direct observation, or a combination
thereof.
Continuing Professional Development
The consensus panel is aware that many providers
in the SUD treatment and mental health services
fields have effectively performed the difficult task
of providing services for clients with CODs, often
without much guidance from established research
and knowledge or systematized approaches. The
landscape has changed, and a solid knowledge
base is now available to the counselor. However,
that knowledge typically is scattered through many
journals and reports. This TIP makes an effort to
integrate the available information. Counselors
reading this TIP can review their own knowledge
RESOURCE ALERT: COMPETENCIES AND TRAINING FOR SUD TREATMENT
SUPERVISORS
•
Family Health International 360’s Training Curriculum on Drug Addiction Counseling Trainer Manual.
Chapter 9: Clinical Supervision and Support (www.fhi360.org/sites/default/files/media/documents/
Training%20Curriculum%20on%20Drug%20Addiction%20Counseling%20-%20Chapter%209.pdf)
•
SAMHSA’s TAP 21-A: Competencies for Substance Abuse Treatment Clinical Supervisors (https://store.
samhsa.gov/system/files/sma12-4243.pdf)
•
SAMHSA’s Recruitment and Retention Toolkit chapter on Supervision Intervention Strategies (http://
toolkit.ahpnet.com/Supervision-Intervention-Strategies.aspx)
Chapter 8 239

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
and determine what they need to continue their
professional development.
Counselors should check with their states’
certification bodies to determine whether training
leading to formal credentials in counseling people
with CODs is available (also see the Section “COD/
Addiction Certification in Health Disciplines” for
links to websites that offer such information).
Appendix B also lists some resources counselors
can use to enhance their professional knowledge
and development.
Education and Training
Although many program staff who treat clients with
CODs possess basic skills, advanced provider skills
and specialized training in CODs are frequently
lacking (Padwa et al., 2013; Petrakis et al., 2018;
Sacks et al., 2013). Training (along with supervision)
in mental health service and SUD treatment can
be effective in improving providers’ competence
and treatment fidelity, which in turn have been
associated with reductions in the severity of clients’
mental illness symptoms and substance use (Meier
et al., 2015). Inadequate staff training is a barrier
to people with CODs receiving needed treatment
(Padwa et al., 2015). Rather than focusing on staff
performance, like managing large caseloads and
increasing billable hours, providers may benefit
more from COD-specific training to enhance their
knowledge of and comfort with treating clients
who have co-occurring SUDs (Padwa et al., 2015).
Staff in integrated primary care and behavioral
health service settings report desiring more
education, training, and support related to SUD
treatment services (Zubkoff, Shiner, & Watts, 2016),
including:
•
Hiring more staff, especially professionals with
previous knowledge and experience in SUDs.
•
Additional tangible resources (e.g., more
therapy rooms).
•
More guidance in providing brief addiction
interventions, such as motivational interviewing.
•
Training on how to address clients with complex
SUD-related needs.
•
Education about the availability of different SUD
treatment options.
•
Quick and easy access to as-needed
The scope of practice that addiction counselors
must follow legally and under which they can be
reimbursed varies from state to state (University
of Michigan Behavioral Health Workforce
Research Center, 2018). In some states, practice
privileges are broad, and in others they are
quite restrictive. For instance, certain states
mandate that addiction counselors can only
conduct assessments and provide treatments
for SUDs, limiting their ability to serve clients
with CODs. Certification requirements and
authorized services also are inconsistent. The
lack of standardized training, credentialing, and
practices makes it difficult for the behavioral
health field as a whole to effectively respond to
gaps in COD treatment access and provision.
consultations (e.g., phone-based consultations
with peers with experience in treating SUDs).
Discipline-Specic Education
Staff education and training are fundamental
to all SUD treatment programs. Few university-
based programs offer a formal curriculum on
CODs, despite some improvement during the
past decade. Many professional organizations are
promoting the development of competencies and
practice standards for intervening with substance
use problems, including the American Psychiatric
Association, American Psychological Association,
American Society of Addiction Medicine, National
Association of Social Workers, and American
Counseling Association. They are also specifically
encouraging faculty members to enhance their
knowledge in this area so they can better prepare
their students to meet the needs of clients with
CODs. The consensus panel encourages all
such organizations to identify standards and
competencies for their membership related to
CODs and to encourage the development of
training for specific disciplines.
Because the consequences of both addiction
and mental disorders can present with physical
or psychiatric manifestations, medical students,
internal medicine and general practice residents,
and general psychiatry residents all need to be
educated in the problems of CODs. Too few hours
of medical education are devoted to the problems
240 Chapter 8

TIP 42
Chapter 8—Workforce and Administrative Concerns
MEETING THE GROWING DEMAND FOR ADDICTION COUNSELORS IN
THE FUTURE: FARING WELL OR FALLING SHORT?
HRSA (2018) projects the number of addiction counselors will increase by 6 percent from 2016 to 2030.
However, during that same time period, they calculate a 21-percent increase in the demand for addiction
counselors, leaving a deficit of 13,600 full-time addiction counselor positions in the labor force. When
calculating the supply and demand while also accounting for the millions of Americans who will have
unmet behavioral health service needs, demand will exceed supply by 38 percent. Under this scenario,
there would be a deficit of nearly 35,000 addiction counselors.
of addiction and mental disorders. Medication
can play a critical role in the treatment of CODs,
so having adequately trained physicians who can
manage medication therapies for clients with CODs
is important.
Continuing Education and Training
Many SUD treatment counselors learn through
continuing education and facility-sponsored
training. Continuing education and training involves
participation in a variety of courses and workshops
from basic to advanced level offered by a number
of training entities. The strength of continuing
education and training courses and workshops is
that they provide the counselor with the opportunity
to review and process written material with a
qualified instructor and other practitioners.
Continuing education is useful because it can
respond rapidly to the needs of a workforce
that has diverse educational backgrounds and
experience. To have practical utility, competency
training must address the day-to-day concerns
that counselors face in working with clients who
have CODs. The educational context must be rich
with information, culturally sensitive, designed for
adult students, and must include examples and
role models. Ideally, the instructors have extensive
A recent survey (SAMHSA, 2018e) that asked
approximately 13,600 SUD treatment facilities
nationwide about their quality assurance
practices found that almost 98 percent included
continuing education among their standard
operating procedures. Nearly all facilities (almost
94 percent) regularly conducted case reviews
between providers and supervisors. About 92
percent conducted client satisfaction surveys.
experience as practitioners in the field.
Continuing education is essential for effective
provision of services to people with CODs, but it is
not sufficient in and of itself. Counselors must have
ongoing support, supervision, and opportunity
to practice new skills if they are to truly integrate
COD content into their practice.
Cross-Training
Cross-training is the simultaneous provision of
material and training to more than one discipline at
a time (e.g., addiction and social work counselors;
addiction counselors and corrections officers).
Counselors who have primary expertise in either
addiction or mental health will be able to work
far more effectively with clients who have CODs
if they have some degree of cross-training in the
other field. The consensus panel recommends that
counselors of either field receive at least basic level
cross-training in the other field to better assess,
refer, understand, and work effectively with the
large number of clients with CODs. Cross-trained
individuals who know their primary field of training
well and also have an appreciation for the other
field, provide a richness of capacity that cannot
be attained using any combination of personnel
familiar with one system alone.
Cross-training facilitates interaction and
communication between the counselors from
each discipline. This helps to remove barriers,
increase understanding, and promote integrated
work. Cross-training is particularly valuable for
staff members who will work together in the
same program. Consensus panel members have
found cross-training very valuable in mental health
services, SUD treatment, and criminal justice work.
Chapter 8 241

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
EXHIBIT 8.7. Certification for Health Professions
PROFESSION CERTIFICATION IN SUDS OR CODS
Physicians
Physicians from any specialty, including primary care, psychiatry, and internal
medicine can become certified by the American Society of Addiction Medicine
(ASAM). Psychiatrists can receive added qualifications in Addiction Psychiatry
through the formal American College of Graduate Medical Education Board
Certification process or through the American Academy of Addiction Psychiatry
(AAAP). Osteopathic physicians from any specialty can receive addiction
qualifications through the American Osteopathic Association:
•
ASAM Addiction Medicine Certification (www.asam.org/education/certification-
MOC)
•
AAAP (www.aaap.org/clinicians/)
•
American Osteopathic Academy of Addiction Medicine (https://aoaam.org/
PCSS-waiver-eligibility-training)
•
American Board of Preventive Medicine Addiction Medicine Certification
(www.theabpm.org/become-certified/subspecialties/addiction-medicine/)
Nurses
Registered nurses can gain licensure in addiction medicine through a partnership
between the Addictions Nursing Certification Board and the Center for Nursing
Education and Testing, Inc.
•
Certified Addictions Registered Nurse (www.cnetnurse.com/carn-exam)
•
Certified Addictions Registered Nurse–Advanced Practice (www.cnetnurse.com/
ap-carn-exam)
Psychologists
•
The Society of Addiction Psychology (Division 50 of the American
Psychological Association) offers credentialing in addiction psychology (https://
addictionpsychology.org/education-training/certification).
•
Psychologists can also obtain Master Addiction Counselor With Co-Occurring
Disorders Component credentials from NAADAC (www.naadac.org/mac).
Social Workers
The National Association of Social Workers offers a Certified Clinical Alcohol,
Tobacco & Other Drugs Social Worker credential (www.socialworkers.org/Careers/
Credentials-Certifications/Apply-for-NASW-Social-Work-Credentials/Certified-
Clinical-Alcohol-Tobacco-Other-Drugs-Social-Worker).
Counselors
NAADAC offers several certifications in addiction and COD specialties:
•
National Certified Addiction Counselor, Level I (www.naadac.org/ncac-i)
•
National Certified Addiction Counselor, Level II (www.naadac.org/ncac-ii)
•
Master Addiction Counselor With Co-Occurring Disorders Component
(www.naadac.org/mac)
The International Certification & Reciprocity Consortium also offers counselor
certifications in CODs: Advanced Alcohol and Drug Counselor (certification for
CODs) (https://internationalcredentialing.org/creds/aadc)
Other
•
Adler Graduate School offers in-person and online training leading to a
Certificate in Co-Occurring Disorders and Addiction Counseling; providers may
need to meet additional state-specific licensure requirements (http://alfredadler.
edu/programs/certificate/certificate-in-COD).
•
Breining Institute offers credentialing as a Certified Co-Occurring Disorders
Specialist (www.breining.edu/index.php/professional-certification/certified-co-
occurring-disorders-specialist-ccds/).
242 Chapter 8
TIP 42Chapter 8—Workforce and Administrative Concerns
National Training Resources
Curriculums and other educational materials are
available through ATTCs, universities, state entities,
and private consultants. These materials can help
enhance the ability of SUD treatment counselors
to work with clients who have mental disorders,
as well as to enable mental health personnel to
improve their efforts with people who have SUDs.
ATTCs offer workshops, courses, and online remote
location courses. (See Appendix B for training
sources.)
COD/Addiction Certication in Health
Disciplines
The disciplines of medicine and psychology
have recognized subspecialties in CODs with a
defined process for achieving a certificate in this
area. Exhibit 8.7 summarizes current information
on certification by discipline. Drug and alcohol
certification requirements vary by state (review
at https://addictionstraininginstitute.com/
certifications-in-florida/) as do addiction counselor
requirements (www.addiction-counselors.com/).
Conclusion
The consensus panel strongly encourages
counselors to acquire competencies specific to
working effectively with clients who have CODs.
Juggling a high-stress, demanding workload
with continuing professional development is
difficult. The panel urges agency and program
administrators, including line-level and clinical
supervisors, to develop COD competencies
themselves and to support and encourage
continuing workforce education and training.
To the extent possible, they should customize
education and training efforts—in content,
schedule, and location—to meet the needs of
counselors in the field. That is, bring the training
to the counselor. Rewards can include salary and
advancement tied to counselors’ efforts to increase
effectiveness in serving clients with CODs, shown
via job performance. Clinicians in primary care
settings, community mental health centers, or
private mental health offices also should enhance
their knowledge of alcohol and drug use in clients
with mental difficulties.
Chapter 8 243
This page intentionally left blank.

TIP 42
SUBSTANCE USE DISORDER TREATMENT FOR
PEOPLE WITH CO-OCCURRING DISORDERS
Appendix A—Bibliography
Abroms, M., & Sher, L. (2016). Dual disorders and suicide.
Journal of Dual Diagnosis, 12(2), 148–149. doi:10.1080/15
504263.2016.1172898
Acri, M., Hooley, C. D., Richardson, N., & Moaba, L. B.
(2017). Peer models in mental health for caregivers
and families. Community Mental Health Journal, 53(2),
241–249. doi:10.1007/s10597-016-0040-4
Afful, S. E., Strickland, J. R., Cottler, L., & Bierut, L. J. (2010).
Exposure to trauma: A comparison of cocaine-dependent
cases and a community-matched sample. Drug and
Alcohol Dependence, 112(1–2), 46–53. doi:10.1016/j.
drugalcdep.2010.05.012
Ahmedani, B. K., Peterson, E. L., Hu, Y., Rossom, R. C.,
Lynch, F., Lu, C. Y., . . . Simon, G. E. (2017). Major physical
health conditions and risk of suicide. American Journal
of Preventive Medicine, 53(3), 308–315. doi:10.1016/j.
amepre.2017.04.001
Ait-Daoud, N., Blevins, D., Khanna, S., Sharma, S., &
Holstege, C. P. (2017). Women and addiction. Psychiatric
Clinics of North America, 40(2), 285–297. doi:10.1016/j.
psc.2017.01.005
Akbar, M., Egli, M., Cho, Y., Song, B., & Noronha, A. (2018).
Medications for alcohol use disorders: An overview.
Pharmacology & Therapeutics, 185, 64–85. doi: 10.1016/j.
pharmthera.2017.11.007.
Alam, D. A., & Martorana, A. (2011). Addiction treatment:
Level of care determination. Primary Care, 38(1),
125–136. doi:10.1016/j.pop.2010.11.009
Alarid, L. F., & Rubin, M. (2018). Misdemeanor
arrestees with mental health needs: Diversion
and outpatient services as a recidivism reduction
strategy. International Journal of Offender Therapy
and Comparative Criminology, 62(3), 575–590.
doi:10.1177/0306624x16652892
Alcorn, J. L., 3rd, Gowin, J. L., Green, C. E., Swann, A.
C., Moeller, F. G., & Lane, S. D. (2013). Aggression,
impulsivity, and psychopathic traits in combined antisocial
personality disorder and substance use disorder. Journal
of Neuropsychiatry and Clinical Neurosciences, 25(3),
229–232. doi:10.1176/appi.neuropsych.12030060
Alegria, A. A., Blanco, C., Petry, N. M., Skodol, A. E., Liu,
S. M., Grant, B., & Hasin, D. (2013). Sex differences in
antisocial personality disorder: Results from the National
Epidemiologic Survey on Alcohol and Related Conditions.
Personality Disorders, 4(3), 214–222. doi:10.1037/
a0031681
Alexander, M., Layman, D., & Haugland, G. (2013).
Validating the Modified Mini Screen (MMS) as a mental
health referral screen for public assistance recipients in
New York State. Annual Meeting of the American Public
Health Association, Boston, MA.
Alexander, M. J., Haugland, G., Lin, S. P., Bertollo, D.
N., & McCorry, F. A. (2008). Mental health screening
in addiction, corrections and social service settings:
Validating the MMS. International Journal of Mental
Health and Addiction, 6(1), 105–119.
Ali, B., Green, K. M., Daughters, S. B., & Lejuez, C. W.
(2017). Distress tolerance interacts with circumstances,
motivation, and readiness to predict substance abuse
treatment retention. Addictive Behaviors, 73, 99–104.
doi:10.1016/j.addbeh.2017.04.016
Al-Rousan, T., Rubenstein, L., Sieleni, B., Deol, H., &
Wallace, R. B. (2017). Inside the nation’s largest mental
health institution: A prevalence study in a state prison
system. BMC Public Health, 17(1), 342. doi:10.1186/
s12889-017-4257-0
American Association of Community Psychiatrists.
(2016). LOCUS: Level of Care Utilization System for
Psychiatric and Addiction Services: Adult version
20. Retrieved from https://drive.google.com/
file/d/0B89glzXJnn4cV1dESWI2eFEzc3M/view
American College of Emergency Physicians. (January 2017).
Alcohol screening in the emergency department. Policy
statement. Retrieved from www.acep.org/globalassets/
new-pdfs/policy-statements/alcohol-screening-in-the-
emergency-department.pdf
American Psychiatric Association. (2010). Practice guideline
for the treatment of patients with major depressive
disorder. Retrieved from https://psychiatryonline.org/pb/
assets/raw/sitewide/practice_guidelines/guidelines/mdd.
pdf
American Psychiatric Association. (2013). Diagnostic and
statistical manual of mental disorders (5th ed.). Arlington,
VA: American Psychiatric Association.
Antai-Otong, D. (2016). Evidence-based care of the
patient with borderline personality disorder. Nursing
Clinics of North America, 51(2), 299–308. doi:10.1016/j.
cnur.2016.01.012
Arkins, B., Begley, C., & Higgins, A. (2016). Measures for
screening for intimate partner violence: A systematic
review. Journal of Psychiatric Mental Health Nursing,
23(3–4), 217–235. doi:10.1111/jpm.12289
Arnold, L. E., Hodgkins, P., Caci, H., Kahle, J., & Young,
S. (2015). Effect of treatment modality on long-term
outcomes in attention-deficit/hyperactivity disorder:
A systematic review. PLoS ONE, 10(2), e0116407.
doi:10.1371/journal.pone.0116407
Arunogiri, S., & Lubman, D. I. (2015). Anxiety and
substance use disorders: A worrying combination.
Australasian Psychiatry, 23(4), 382–387.
doi:10.1177/1039856215590053
245

TIP 42 Substance Use Disorder Treatment for People With Co-Occurring Disorders
Ashford, R. D., Meeks, M., Curtis, B., & Brown, A. M. (2018).
Utilization of peer-based substance use disorder and
recovery interventions in rural emergency departments:
Patient characteristics and exploratory analysis. Journal
of Rural Mental Health, 43(1), 17–29. doi:10.1037/
rmh0000106
Asmundson, G. J., Taylor, S., & Smits, J. A. (2014). Panic
disorder and agoraphobia: An overview and commentary
on DSM-5 changes. Depression and Anxiety, 31(6),
480–486. doi:10.1002/da.22277
Atkinson, D. M., Rodman, J. L., Thuras, P. D., Shiroma, P. R.,
& Lim, K. O. (2017). Examining burnout, depression, and
self-compassion in Veterans Affairs mental health staff.
Journal of Alternative and Complementary Medicine,
23(7), 551–557. doi:10.1089/acm.2017.0087
Avery, J., Han, B. H., Zerbo, E., Wu, G., Mauer, E., Avery, J.,
… Penzner, J. B. (2017). Changes in psychiatry residents’
attitudes towards individuals with substance use disorders
over the course of residency training. American Journal
on Addictions, 26(1), 75–79. doi: 10.1111/ajad.12406
Avery, J., & Zerbo, E. (2015). Improving psychiatry residents’
attitudes toward individuals diagnosed with substance
use disorders. Harvard Review of Psychiatry, 23(4),
296–300. doi:10.1097/hrp.0000000000000047
Avery, J., Zerbo, E., & Ross, S. (2016). Improving
psychiatrists’ attitudes towards individuals with psychotic
disorders and co-occurring substance use disorders.
Academic Psychiatry, 40(3), 520–522. doi:10.1007/
s40596-015-0361-6
Ayangbayi, T., Okunade, A., Karakus, M., & Nianogo, T.
(2017). Characteristics of hospital emergency room visits
for mental and substance use disorders. Psychiatric
Services, 68(4), 408–410. doi:10.1176/appi.ps.201600125
Babor, T. F., Higgins-Biddle, J. C., Saunders, J. B., &
Monteiro, M. G. (2001). AUDIT: The alcohol use disorders
identification test: Guidelines for use in primary care
(2nd ed.). Retrieved from https://apps.who.int/iris/
bitstream/handle/10665/67205/WHO_MSD_MSB_01.6a.
pdf?sequence=1&isAllowed=y
Bahji, A., Mazhar, M. N., Hudson, C. C., Nadkarni, P.,
MacNeil, B. A., & Hawken, E. (2019). Prevalence of
substance use disorder comorbidity among individuals
with eating disorders: A systematic review and meta-
analysis. Psychiatry Research, 273, 58–66. doi:10.1016/j.
psychres.2019.01.007
Bahorik, A. L., Sterling, S. A., Campbell, C. I., Weisner,
C., Ramo, D., & Satre, D. D. (2018). Medical and non-
medical marijuana use in depression: Longitudinal
associations with suicidal ideation, everyday functioning,
and psychiatry service utilization. Journal of Affective
Disorders, 241, 8–14. doi:10.1016/j.jad.2018.05.065
Baillargeon, J., Penn, J. V., Knight, K., Harzke, A.
J., Baillargeon, G., & Becker, E. A. (2010). Risk of
reincarceration among prisoners with co-occurring
severe mental illness and substance use disorders.
Administration and Policy in Mental Health, 37(4),
367–374. doi:10.1007/s10488-009-0252-9
Baker, A. L., Thornton, L. K., Hiles, S., Hides, L., & Lubman,
D. I. (2012). Psychological interventions for alcohol misuse
among people with co-occurring depression or anxiety
disorders: A systematic review. Journal of Affective
Disorders, 139(3), 217–229. doi:10.1016/j.jad.2011.08.004
Baker, J. H., Mitchell, K. S., Neale, M. C., & Kendler, K. S.
(2010). Eating disorder symptomatology and substance
use disorders: Prevalence and shared risk in a population
based twin sample. International Journal of Eating
Disorders, 43(7), 648–658. doi:10.1002/eat.20856
Bandelow, B., & Michaelis, S. (2015). Epidemiology of
anxiety disorders in the 21st century. Dialogues in Clinical
Neuroscience, 17(3), 327–335.
Bandelow, B., Michaelis, S., & Wedekind, D. (2017).
Treatment of anxiety disorders. Dialogues in Clinical
Neuroscience, 19(2), 93–107.
Banerjee, S., & Spry, C. (2017). CADTH Rapid Response
Reports. In Concurrent treatment for substance use
disorder and trauma-related comorbidities: A review
of clinical effectiveness and guidelines. Ottawa (ON):
Canadian Agency for Drugs and Technologies in Health.
Barry, A. E., & Piazza-Gardner, A. K. (2012). Drunkorexia:
Understanding the co-occurrence of alcohol consumption
and eating/exercise weight management behaviors.
Journal of American College Health, 60(3), 236–243. doi:
10.1080/07448481.2011.587487
Barry, C. L., Epstein, A. J., Fiellin, D. A., Fraenkel, L., &
Busch, S. H. (2016). Estimating demand for primary care-
based treatment for substance and alcohol use disorders.
Addiction, 111(8), 1376–1384. doi:10.1111/add.13364
Bartlett, D. (2017). Drug-induced serotonin syndrome.
Critical Care Nurse, 37(1), 49–54. doi:10.4037/
ccn2017.169
Bassuk, E. L., Hanson, J., Greene, R. N., Richard, M., &
Laudet, A. (2016). Peer-delivered recovery support
services for addictions in the United States: A systematic
review. Journal of Substance Abuse Treatment, 63, 1–9.
Bateman, A. W., Gunderson, J., & Mulder, R. (2015).
Treatment of personality disorder. Lancet, 385(9969),
735–743. doi:10.1016/s0140-6736(14)61394-5
Batterham, P. J., Ftanou, M., Pirkis, J., Brewer, J. L.,
Mackinnon, A. J., Beautrais, A., . . . Christensen, H.
(2015). A systematic review and evaluation of measures
for suicidal ideation and behaviors in population-based
research. Psychological Assessment, 27(2), 501–512.
doi:10.1037/pas0000053
246 Appendix A

TIP 42
Appendix A—Bibliography
Baum, N. (2016). Secondary traumatization in mental
health professionals: A systematic review of gender
findings. Trauma, Violence, & Abuse,17(2), 221–235. doi:
10.1177/1524838015584357
Beck, A. T., & Steer, R. A. (1987). Beck Depression Inventory
manual. San Antonio, TX: The Psychological Corporation,
Harcourt Brace Jovanovich.
Beck, A. T., Steer, R. A., & Brown, G. K. (1996). Beck
Depression Inventory-II manual. San Antonio, TX:
Psychological Corporation.
Becker, M. A., Boaz, T. L., Andel, R., & Hafner, S. (2017).
Risk of early rehospitalization for non-behavioral health
conditions among adult Medicaid beneficiaries with
severe mental illness or substance use disorders. Journal
of Behavioral Health Services & Research, 44(1), 113–121.
doi:10.1007/s11414-016-9516-9
Beidas, R. S., Marcus, S., Wolk, C. B., Powell, B., Aarons, G.
A., Evans, A. C., . . . Mandell, D. S. (2016). A prospective
examination of clinician and supervisor turnover within
the context of implementation of evidence-based
practices in a publicly-funded mental health system.
Administration and Policy in Mental Health and Mental
Health Services Research, 43(5), 640–649.
Bell, H. (2018). Creative interventions for teaching empathy
in the counseling classroom. Journal of Creativity in
Mental Health, 13(1), 106–120. doi:10.1080/15401383.20
17.1328295
Belleau, E. L., Chin, E. G., Wanklyn, S. G., Zambrano-
Vazquez, L., Schumacher, J. A., & Coffey, S. F. (2017).
Pre-treatment predictors of dropout from prolonged
exposure therapy in patients with chronic posttraumatic
stress disorder and comorbid substance use disorders.
Behaviour Research and Therapy, 91, 43–50.
Benich, J. J., 3rd, Bragg, S. W., & Freedy, J. R. (2016).
Psychopharmacology in primary care settings. Primary
Care, 43(2), 327–340. doi:10.1016/j.pop.2016.01.002
Bennett, A. C., Gibson, C., Rohan, A. M., Howland, J. F., &
Rankin, K. M. (2018). Mental health and substance use-
related hospitalizations among women of reproductive
age in Illinois and Wisconsin. Public Health Reports,
134(1), 17–26.
Bennett, M. E., Bradshaw, K. R., & Catalano, L. T. (2017).
Treatment of substance use disorders in schizophrenia.
American Journal of Drug and Alcohol Abuse, 43(4),
377–390. doi:10.1080/00952990.2016.1200592
Benningfield, M. M., Arria, A. M., Kaltenbach, K., Heil, S.
H., Stine, S. M., Coyle, M. G., . . . Martin, P. R. (2010).
Co-occurring psychiatric symptoms are associated
with increased psychological, social, and medical
impairment in opioid dependent pregnant women.
American Journal on Addictions, 19(5), 416–421.
doi:10.1111/j.1521-0391.2010.00064.x
Benston, E. A. (2015). Housing programs for homeless
individuals with mental illness: Effects on housing and
mental health outcomes. Psychiatric Services, 66(8),
806–816. doi:10.1176/appi.ps.201400294
Bentley, K. H., Franklin, J. C., Ribeiro, J. D., Kleiman, E. M.,
Fox, K. R., & Nock, M. K. (2016). Anxiety and its disorders
as risk factors for suicidal thoughts and behaviors: A meta-
analytic review. Clinical Psychology Review, 43, 30–46.
doi:10.1016/j.cpr.2015.11.008
Ben-Zeev, D., Kaiser, S. M., & Krzos, I. M. (2014). Remote
“hovering” with individuals with psychotic disorders and
substance use: Feasibility, engagement, and therapeutic
alliance with a text-messaging mobile interventionist.
Journal of Dual Diagnosis, 10(4), 197–203.
Berenz, E. C., & Coffey, S. F. (2012). Treatment of co-
occurring posttraumatic stress disorder and substance
use disorders. Current Psychiatry Reports, 14(5), 469–477.
doi:10.1007/s11920-012-0300-0
Bergink, V., Rasgon, N., & Wisner, K. L. (2016). Postpartum
psychosis: Madness, mania, and melancholia in
motherhood. American Journal of Psychiatry, 173(12),
1179–1188. doi:10.1176/appi.ajp.2016.16040454
Bergman, B. G., Greene, M. C., Hoeppner, B. B., Slaymaker,
V., & Kelly, J. F. (2014). Psychiatric comorbidity and
12-step participation: A longitudinal investigation
of treated young adults. Alcoholism: Clinical and
Experimental Research, 38(2), 501–510. doi:10.1111/
acer.12249
Bernert, R. A., Hom, M. A., & Roberts, L. W. (2014). A
review of multidisciplinary clinical practice guidelines
in suicide prevention: Toward an emerging standard
in suicide risk assessment and management, training
and practice. Academic Psychiatry, 38(5), 585–592.
doi:10.1007/s40596-014-0180-1
Bernstein, J., Derrington, T. M., Belanoff, C., Cabral, H.
J., Babakhanlou-Chase, H., Diop, H., … Kotelchuck, M.
(2015). Treatment outcomes for substance use disorder
among women of reproductive age in Massachusetts:
A population-based approach. Drug and Alcohol
Dependence, 147, 151–159. doi:10.1016/j.drugalcdep
Bhugra, D. (2005). The global prevalence of schizophrenia.
PLoS Medicine, 2(5), e151. doi:10.1371/journal.
pmed.0020151
Black, D. W. (2015). The natural history of antisocial
personality disorder. Canadian Journal of Psychiatry,
60(7), 309–314. doi:10.1177/070674371506000703
Black, D. W. (2017). The treatment of antisocial personality
disorder. Current Treatment Options in Psychiatry, 4(4),
295–302.
Appendix A 247

TIP 42 Substance Use Disorder Treatment for People With Co-Occurring Disorders
Blanco, C., Alegria, A. A., Liu, S. M., Secades-Villa,
R., Sugaya, L., Davies, C., & Nunes, E. V. (2012).
Differences among major depressive disorder with
and without co-occurring substance use disorders and
substance-induced depressive disorder: Results from the
National Epidemiologic Survey on Alcohol and Related
Conditions. Journal of Clinical Psychiatry, 73(6), 865–873.
doi:10.4088/JCP.10m06673
Blanco, C., Compton, W. M., Saha, T. D., Goldstein,
B. I., Ruan, W. J., Huang, B., & Grant, B. F. (2017).
Epidemiology of DSM-5 bipolar I disorder: Results from
the National Epidemiologic Survey on Alcohol and
Related Conditions – III. Journal of Psychiatric Research,
84, 310–317. doi:10.1016/j.jpsychires.2016.10.003
Blanco, C., Okuda, M., Markowitz, J. C., Liu, S. M.,
Grant, B. F., & Hasin, D. S. (2010). The epidemiology
of chronic major depressive disorder and dysthymic
disorder: Results from the National Epidemiologic
Survey on Alcohol and Related Conditions. Journal of
Clinical Psychiatry, 71(12), 1645–1656. doi:10.4088/
JCP.09m05663gry
Blanco, C., Xu, Y., Brady, K., Perez-Fuentes, G., Okuda,
M., & Wang, S. (2013). Comorbidity of posttraumatic
stress disorder with alcohol dependence among US
adults: Results from National Epidemiological Survey
on Alcohol and Related Conditions. Drug and Alcohol
Dependence, 132(3), 630–638. doi:S0376-8716(13)00145-
2 [pii];10.1016/j.drugalcdep.2013.04.016 [doi]
Blodgett, J. C., Maisel, N. C., Fuh, I. L., Wilbourne, P. L.,
& Finney, J. W. (2014). How effective is continuing care
for substance use disorders? A meta-analytic review.
Journal of Substance Abuse Treatment, 46(2), 87–97.
doi:10.1016/j.jsat.2013.08.022
Boden, M. T., & Hoggatt, K. J. (2018). Substance use
disorders among veterans in a nationally representative
sample: Prevalence and associated functioning and
treatment utilization. Journal of Studies on Alcohol and
Drugs, 79(6), 853–861.
Bogenschutz, M. P., Donovan, D. M., Mandler, R.
N., Perl, H. I., Forcehimes, A. A., Crandall, C., . . .
Douaihy, A. (2014a). Brief intervention for patients
with problematic drug use presenting in emergency
departments: A randomized clinical trial. JAMA
Internal Medicine, 174(11), 1736–1745. doi:10.1001/
jamainternmed.2014.4052
Bogenschutz, M. P., Rice, S. L., Tonigan, J. S., Vogel, H. S.,
Nowinski, J., Hume, D., & Arenella, P. B. (2014b). 12-step
facilitation for the dually diagnosed: A randomized
clinical trial. Journal of Substance Abuse Treatment, 46(4),
403–411. doi:10.1016/j.jsat.2013.12.009
Boggs, J. M., Beck, A., Hubley, S., Peterson, E. L., Hu,
Y., Williams, L. K., . . . Ahmedani, B. K. (2018). General
medical, mental health, and demographic risk factors
associated with suicide by firearm compared with other
means. Psychiatric Services, 69(6), 677–684. doi:10.1176/
appi.ps.201700237
Bohnert, K. M., Ilgen, M. A., Louzon, S., McCarthy, J. F.,
& Katz, I. R. (2017). Substance use disorders and the
risk of suicide mortality among men and women in the
US Veterans Health Administration. Addiction, 112(7),
1193–1201. doi:10.1111/add.13774
Bolton, J. M., Gunnell, D., & Turecki, G. (2015). Suicide risk
assessment and intervention in people with mental illness.
BMJ, 351, h4978. doi:10.1136/bmj.h4978
Bond, G. R., & Drake, R. E. (2015). The critical ingredients of
assertive community treatment. World Psychiatry, 14(2),
240–242. doi:10.1002/wps.20234
Bonsack, C., Gibellini Manetti, S., Favrod, J., Montagrin,
Y., Besson, J., Bovet, P., & Conus, P. (2011). Motivational
intervention to reduce cannabis use in young people
with psychosis: A randomized controlled trial.
Psychotherapy and Psychosomatics, 80(5), 287–297.
doi:10.1159/000323466
Boothroyd, R. A., Peters, R. H., Armstrong, M. I., Rynearson-
Moody, S., & Caudy, M. (2015). The psychometric
properties of the simple screening instrument for
substance abuse. Evaluation and the Health Professions,
38(4), 538–562. doi:10.1177/0163278713490165
Borges, G., Bagge, C. L., Cherpitel, C. J., Conner, K. R.,
Orozco, R., & Rossow, I. (2017). A meta-analysis of
acute use of alcohol and the risk of suicide attempt.
Psychological Medicine, 47(5), 949–957. doi:10.1017/
s0033291716002841
Bowen, S., Witkiewitz, K., Clifasefi, S. L., Grow, J., Chawla,
N., Hsu, S. H., . . . Larimer, M. E. (2014). Relative
efficacy of mindfulness-based relapse prevention,
standard relapse prevention, and treatment as usual
for substance use disorders: A randomized clinical
trial. JAMA Psychiatry, 71(5), 547–556. doi:10.1001/
jamapsychiatry.2013.4546
Bradizza, C. M., Stasiewicz, P. R., & Dermen, K. H. (2014).
Behavioral interventions for individuals dually-diagnosed
with a severe mental illness and a substance use disorder.
Current Addiction Reports, 1(4), 243–250. doi:10.1007/
s40429-014-0032-9
Brady, K. T., Back, S. E., & Coffey, S. F. (2004). Substance
abuse and posttraumatic stress disorder. Current
Directions in Psychological Science, 13(5), 206–209.
doi:10.1111/j.0963-7214.2004.00309.x
Brady, K. T., Haynes, L. F., Hartwell, K. J., & Killeen, T. K.
(2013). Substance use disorders and anxiety: A treatment
challenge for social workers. Social Work in Public Health,
28(3–4), 407–423. doi:10.1080/19371918.2013.774675
Brazil, I. A., van Dongen, J. D. M., Maes, J. H. R., Mars, R.
B., & Baskin-Sommers, A. R. (2018). Classification and
treatment of antisocial individuals: From behavior to
biocognition. Neuroscience and Biobehavioral Reviews,
91, 259–277. doi:10.1016/j.neubiorev.2016.10.010
248 Appendix A
TIP 42
Appendix A—Bibliography
Brewerton, T. D. (2014). Are eating disorders addictions? In
T. Brewerton& A. Baker Dennis (Eds.), Eating disorders,
addictions and substance use disorders: Research, clinical
and treatment perspectives (pp. 267–299). New York:
Springer-Verlag Publishing.
Briggs, C. A., & Reneson, S. (2010). Counseling
addicted veterans: What to know and how to
help. Retrieved from https://pdfs.semanticscholar.
org/9742/967aac815ca02c4f599b36be996d0b10d3d9.pdf
Brockington, I. (2017). Suicide and filicide in postpartum
psychosis. Archives of Women’s Mental Health, 20(1),
63–69. doi:10.1007/s00737-016-0675-8
Broderick, K. B., Kaplan, B., Martini, D., & Caruso, E. (2015).
Emergency physician utilization of alcohol/substance
screening, brief advice and discharge: A 10-year
comparison. Journal of Emergency Medicine, 49(4),
400–407. doi:10.1016/j.jemermed.2015.05.014
Bromberg, S. R., Backman, T. L., Krow, J., & Frankel, K. A.
(2010). The Haven Mother’s House Modified Therapeutic
Community: Meeting the gap in infant mental health
services for pregnant and parenting mothers with drug
addiction. Infant Mental Health Journal, 31(3), 255–276.
doi:10.1002/imhj.20255
Brook, J. S., Zhang, C., Rubenstone, E., Primack, B. A., &
Brook, D. W. (2016). Comorbid trajectories of substance
use as predictors of antisocial personality disorder, major
depressive episode, and generalized anxiety disorder.
Addictive Behaviors, 62, 114–121. doi:10.1016/j.
addbeh.2016.06.003
Brooner, R. K., Kidorf, M. S., King, V. L., Peirce, J., Neufeld,
K., Stoller, K., & Kolodner, K. (2013). Managing psychiatric
comorbidity within versus outside of methadone
treatment settings: A randomized and controlled
evaluation. Addiction, 108(11), 1942–1951.
Brown, C. H., Bennett, M. E., Li, L., & Bellack, A. S. (2011).
Predictors of initiation and engagement in substance
abuse treatment among individuals with co-occurring
serious mental illness and substance use disorders.
Addictive Behaviors, 36(5), 439–447. doi:10.1016/j.
addbeh.2010.12.001
Brown, G. K., & Green, K. L. (2014). A review of evidence-
based follow-up care for suicide prevention: Where
do we go from here? American Journal of Preventive
Medicine, 47(3)(Suppl. 2), S209–S215. doi:10.1016/j.
amepre.2014.06.006
Brown, V. B., Harris, M., & Fallot, R. (2013). Moving toward
trauma-informed practice in addiction treatment: A
collaborative model of agency assessment. Journal of
Psychoactive Drugs, 45(5), 386–393. doi:10.1080/027910
72.2013.844381
Bryant, J. B., Darkes, J., & Rahal, C. (2012). College students’
compensatory eating and behaviors in response to alcohol
consumption. Journal of American College Health, 60(5),
350–356. doi:10.1080/07448481.2011.630702
Buck, K. D., & Lysaker, P. H. (2010). Clinical supervision
for the treatment of adults with severe mental illness:
Pertinent issues when assisting graduate nursing
students. Perspectives in Psychiatric Care, 46(3), 234–243.
doi:10.1111/j.1744-6163.2010.00258.x
Buckner, J. D., Heimberg, R. G., Ecker, A. H., & Vinci, C.
(2013). A biopsychosocial model of social anxiety and
substance use. Depression and Anxiety, 30(3), 276–284.
doi:10.1002/da.22032
Bukach, A. M., Ejaz, F. K., Dawson, N., & Gitter, R. J. (2017).
Turnover among community mental health workers
in Ohio. Administration and Policy in Mental Health
and Mental Health Services Research, 44(1), 115–122.
doi:10.1007/s10488-015-0706-1
Bureau of Labor Statistics. (2019, March 7). Labor force
statistics from the Current Population Survey. Databases,
tables & calculators by subject. Retrieved from https://
data.bls.gov/timeseries/lns14000000
Bureau of Labor Statistics (BLS). (2020, February 11). Job
openings and labor turnover—August 2019. Retrieved
from www.bls.gov/news.release/pdf/jolts.pdf
Bureau of Labor Statistics. (2020, March 3). Databases,
tables & calculators by subject. Labor force statistics from
the Current Population Survey. Retrieved from https://
data.bls.gov/timeseries/LNS14000000
Burke, S. C., Cremeens, J., Vail-Smith, K., & Woolsey, C.
(2010). Drunkorexia: Calorie restriction prior to alcohol
consumption among college freshman. Journal of Alcohol
and Drug Education, 54(2), 17–34.
Bush, K., Kivlahan, D. R., McDonell, M. B., Fihn, S. D., &
Bradley, K. A. (1998). The AUDIT alcohol consumption
questions (AUDIT-C): An effective brief screening test for
problem drinking. Archives of Internal Medicine, 158(16),
1789–1795.
Buttner, M., O’Hara, M. W., & Watson, D. (2012). The
structure of women’s mood in the early postpartum.
Assessment, 19, 247–256.
Cabassa, L. J., & Baumann, A. A. (2013). A two-way street:
Bridging implementation science and cultural adaptations
of mental health treatments. Implementation Science: IS,
8, 90. doi:10.1186/1748-5908-8-90
Campbell, B. K., Guydish, J., Le, T., Wells, E. A., & McCarty,
D. (2015). The relationship of therapeutic alliance and
treatment delivery fidelity with treatment retention in
a multisite trial of twelve-step facilitation. Psychology
of Addictive Behaviors, 29(1), 106–113. doi:10.1037/
adb0000008
Cardno, A. G., & Owen, M. J. (2014). Genetic relationships
between schizophrenia, bipolar disorder, and
schizoaffective disorder. Schizophrenia Bulletin, 40(3),
504–515. doi:10.1093/schbul/sbu016
Appendix A 249
TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
Carpenter, R. W., Wood, P. K., & Trull, T. J. (2016).
Comorbidity of borderline personality disorder
and lifetime substance use disorders in a nationally
representative sample. Journal of Personality Disorders,
30(3), 336–350. doi:10.1521/pedi_2015_29_197
Carra, G., Bartoli, F., Crocamo, C., Brady, K. T., & Clerici, M.
(2014). Attempted suicide in people with co-occurring
bipolar and substance use disorders: Systematic review
and meta-analysis. Journal of Affective Disorders, 167,
125–135. doi:10.1016/j.jad.2014.05.066
Carroll, J. F. X., & McGinley, J. J. (2000). Mental health
screening form-iii (MHSF-III). Unpublished screening
instrument, Project Return Foundation, Inc., New York,
NY.
Carroll, J. F. X., & McGinley, J. J. (2001). A screening
form for identifying mental health problems in alcohol/
other drug dependent persons. Alcoholism Treatment
Quarterly, 19(4), 33–47. doi:10.1300/J020v19n04_02
Carroll, T. D., Currier, J. M., McCormick, W. H., & Drescher,
K. D. (2017). Adverse childhood experiences and risk for
suicidal behavior in male Iraq and Afghanistan veterans
seeking PTSD treatment. Psychological Trauma, 9(5),
583–586. doi:10.1037/tra0000250
Carter, A. C., Capone, C., & Short, E. E. (2011). Co-
occurring posttraumatic stress disorder and alcohol
use disorders in veteran populations. Journal of Dual
Diagnosis, 7(4), 285–299. doi:10.1080/15504263.2011.6
20453
Center for Behavioral Health Statistics and Quality (CBHSQ).
(2019). 2018 National Survey on Drug Use and Health:
Detailed tables. Rockville, MD: Substance Abuse and
Mental Health Services Administration. Retrieved from
https://www.samhsa.gov/data/
Center for Mental Health Services. (1998). Cooccurring
psychiatric and substance disorders in managed
care systems: Standards of care, practice guidelines,
workforce competencies, and training curricula.
Retrieved from http://citeseerx.ist.psu.edu/viewdoc/
download?doi=10.1.1.493.5621&rep=rep1&type=pdf
Center for Quality Assessment and Improvement in Mental
Health. (2007). The Suicide Behaviors Questionnaire-
Revised (SBQ-R) – Overview. Retrieved from http://www.
cqaimh.org/pdf/tool_sbq-r.pdf
Center for Substance Abuse Treatment. (1994). Simple
screening instruments for outreach for alcohol and
other drug abuse and infectious diseases. Treatment
Improvement Protocol (TIP) Series 11 (DHHS Publication
No. (SMA) 94-2094). Rockville, MD: Substance Abuse and
Mental Health Services Administration.
Center for Substance Abuse Treatment. (1995). Alcohol and
other drug screening of hospitalized trauma patients.
Treatment Improvement Protocol (TIP) Series 16 (DHHS
Publication No. (SMA) 95-3041). Rockville, MD: Substance
Abuse and Mental Health Services Administration.
Center for Substance Abuse Treatment. (1997). A guide
to substance abuse services for primary care clinicians.
Treatment Improvement Protocol (TIP) Series 24 (DHHS
Publication No. (SMA) 97-3139). Rockville, MD: Center for
Substance Abuse Treatment.
Center for Substance Abuse Treatment. (1998a).
Comprehensive case management for substance abuse
treatment. Treatment Improvement Protocol (TIP) Series
27 (DHHS Publication No. (SMA) 15-4215). Rockville, MD:
Center for Substance Abuse Treatment.
Center for Substance Abuse Treatment. (1998b). Substance
use disorder treatment for people with physical and
cognitive disabilities. Treatment Improvement Protocol
(TIP) Series 29 (DHHS Publication No. (SMA) 98-3249).
Rockville, MD: Center for Substance Abuse Treatment.
Center for Substance Abuse Treatment. (1999a). Brief
interventions and brief therapies for substance abuse.
Treatment Improvement Protocol (TIP) Series 34 (DHHS
Publication No. (SMA) 99-3353). Rockville, MD: Center for
Substance Abuse Treatment.
Center for Substance Abuse Treatment. (1999b). Enhancing
motivation for change in substance abuse treatment.
Treatment Improvement Protocol (TIP) Series 35 (DHHS
Publication No. (SMA) 99-3354). Rockville, MD: Center for
Substance Abuse Treatment.
Center for Substance Abuse Treatment. (2000a). Changing
the conversation: Improving substance abuse treatment.
The National Treatment Improvement Plan. Panel reports,
public hearings, and participant acknowledgements. HHS
Publication No. (SMA) 003479. Rockville, MD: Center for
Substance Abuse Treatment.
Center for Substance Abuse Treatment. (2000b).
Comprehensive case management for substance abuse
treatment. Treatment Improvement Protocol (TIP) Series
27 (DHHS Publication No. (SMA) 15-4215). Rockville, MD:
Center for Substance Abuse Treatment.
Center for Substance Abuse Treatment. (2000c). Substance
abuse treatment for persons with child abuse and neglect
issues. Treatment Improvement Protocol (TIP) Series 36
(DHHS Publication No. (SMA) 00-3357). Rockville, MD:
Center for Substance Abuse Treatment.
Center for Substance Abuse Treatment. (2005a). 9
substance-induced disorders. In Substance abuse
treatment for persons with co-occurring disorders.
Treatment Improvement Protocol (TIP) Series, No. 42.
Rockville, MD: Center for Substance Abuse Treatment.
Center for Substance Abuse Treatment. (2005b). Substance
abuse treatment for adults in the criminal justice system.
Treatment Improvement Protocol (TIP) Series 44 (DHHS
Publication No. (SMA) 05-4056). Rockville, MD: Center for
Substance Abuse Treatment.
250 Appendix A

TIP 42Appendix A—Bibliography
Center for Substance Abuse Treatment. (2006a). Addiction
counseling competencies: The knowledge, skills, and
attitudes of professional practice. Technical Assistance
Publication (TAP) Series 21 (DHHS Publication No. (SMA)
06-4171). Rockville, MD: Center for Substance Abuse
Treatment.
Center for Substance Abuse Treatment. (2006b).
Detoxification from alcohol and other drugs. Treatment
Improvement Protocol (TIP) Series 45 (DHHS Publication
No. (SMA) 06-4131). Rockville, MD: Substance Abuse and
Mental Health Services Administration.
Center for Substance Abuse Treatment. (2008). Managing
depressive symptoms in substance abuse clients during
early recovery. Treatment Improvement Protocol (TIP)
Series 48. (DHHS Publication No. (SMA) 08-4353).
Rockville, MD: Center for Substance Abuse Treatment.
Center for Substance Abuse Treatment. (2009). Addressing
suicidal thoughts and behaviors in substance abuse
treatment. Treatment Improvement Protocol (TIP) Series
50 (HHS Publication No. (SMA) 09-4381). Rockville, MD:
Center for Substance Abuse Treatment.
Centers for Disease Control and Prevention (CDC). (2014).
Healthy People 2020. Retrieved from www.cdc.gov/
dhdsp/hp2020.htm
Centers for Disease Control and Prevention. (2018). Suicide
rising across the US. Retrieved from www.cdc.gov/
vitalsigns/suicide/index.html
Centers for Disease Control and Prevention. (2020).
Underlying Cause of Death 1999–2018 on CDC WONDER
Online Database. Retrieved from https://wonder.cdc.gov/
ucd-icd10.html
Chan, Y. F., Huang, H., Bradley, K., & Unutzer, J. (2014).
Referral for substance abuse treatment and depression
improvement among patients with co-occurring disorders
seeking behavioral health services in primary care.
Journal of Substance Abuse Treatment, 46(2), 106–112.
doi:10.1016/j.jsat.2013.08.016
Chan, Y. F., Huang, H., Sieu, N., & Unutzer, J. (2013).
Substance screening and referral for substance abuse
treatment in an integrated mental health care program.
Psychiatric Services, 64(1), 88–90. doi:10.1176/appi.
ps.201200082
Chaple, M., Sacks, S., Randell, J., & Kang, B. (2016).
A technical assistance framework to facilitate the
delivery of integrated behavioral health services in
Federally Qualified Health Centers (FQHCs). Journal of
Substance Abuse Treatment, 60, 62–69. doi:10.1016/j.
jsat.2015.08.006
Chapman, S. A., Blash, L. K., Mayer, K., & Spetz, J. (2018).
Emerging roles for peer providers in mental health
and substance use disorders. American Journal of
Preventive Medicine, 54(6S3), S267–S274. doi:10.1016/j.
amepre.2018.02.019
Chapman, S. L., & Wu, L. T. (2013). Postpartum substance
use and depressive symptoms: A review. Women and
Health, 53(5), 479–503. doi:10.1080/03630242.2013.804
025
Charzynska, K., Kucharska, K., & Mortimer, A. (2015).
Does employment promote the process of recovery
from schizophrenia? A review of the existing evidence.
International Journal of Occupational Medicine and
Environmental Health 28(3), 407–418. doi:10.13075/
ijomeh.1896.00341
Cherry, D., Albert, M., & McCaig, L. F. (2018). Mental
health-related physician office visits by adults aged 18
and over: United States, 2012–2014. NCHS Data Brief,
June (311), 1–8.
Chhatre, S., Cook, R., Mallik, E., & Jayadevappa, R. (2017).
Trends in substance use admissions among older adults.
BMC Health Services Research, 17(1), 584. doi:10.1186/
s12913-017-2538-z
Chinman, M., George, P., Dougherty, R. H., Daniels, A. S.,
Ghose, S. S., Swift, A., & Delphin-Rittmon, M. E. (2014).
Peer support services for individuals with serious mental
illnesses: Assessing the evidence. Psychiatric Services,
65(4), 429–441.
Choi, N. G., DiNitto, D. M., Marti, C. N., & Choi, B. Y.
(2017). Association of adverse childhood experiences
with lifetime mental and substance use disorders
among men and women aged 50+ years. International
Psychogeriatrics, 29(3), 359–372. doi:10.1017/
s1041610216001800
Choi, S., Adams, S. M., MacMaster, S. A., & Seiters, J.
(2013). Predictors of residential treatment retention
among individuals with co-occurring substance abuse and
mental health disorders. Journal of Psychoactive Drugs,
45(2), 122–131. doi:10.1080/02791072.2013.785817
Chow, C. M., Wieman, D., Cichocki, B., Qvicklund, H.,
& Hiersteiner, D. (2013). Mission impossible: Treating
serious mental illness and substance use co-occurring
disorder with integrated treatment: A meta-analysis.
Mental Health and Substance Use: Dual Diagnosis, 6(2),
150–168. doi:10.1080/17523281.2012.693130
Clark, C., Guenther, C. C., & Mitchell, J. N. (2016). Case
management models in permanent supported housing
programs for people with complex behavioral issues who
are homeless. Journal of Dual Diagnosis, 12(2), 185–192.
doi:10.1080/15504263.2016.1176852
Clark, R. E., Samnaliev, M., & McGovern, M. P. (2007).
Treatment for co-occurring mental and substance use
disorders in five state Medicaid programs. Psychiatric
Services, 58(7), 942–948. doi:10.1176/ps.2007.58.7.942
Cleary, M., Hunt, G. E., Matheson, S., & Walter, G. (2009).
Psychosocial treatments for people with co-occurring
severe mental illness and substance misuse: Systematic
review. Journal of Advanced Nursing, 65(2), 238–258.
doi:10.1111/j.1365-2648.2008.04879.x
Appendix A 251

TIP 42 Substance Use Disorder Treatment for People With Co-Occurring Disorders
Coffey, S. F., Schumacher, J. A., Nosen, E., Littlefield,
A. K., Henslee, A. M., Lappen, A., & Stasiewicz, P. R.
(2016). Trauma-focused exposure therapy for chronic
posttraumatic stress disorder in alcohol and drug
dependent patients: A randomized controlled trial.
Psychology of Addictive Behaviors, 30(7), 778–790.
doi:10.1037/adb0000201
Cohen, A., Freeborn, B., & McManus, B. (2013).
Competition and crowding out in the market
for outpatient substance abuse treatment.
International Economic Review, 54(1), 159–184.
doi:10.1111/j.1468-2354.2012.00729.x
Cohen, L. R., Field, C., Campbell, A. N., & Hien, D. A.
(2013). Intimate partner violence outcomes in women
with PTSD and substance use: A secondary analysis
of NIDA Clinical Trials Network “Women and Trauma”
multi-site study. Addictive Behaviors, 38(7), 2325–2332.
doi:10.1016/j.addbeh.2013.03.006
Colby, S. L., & Ortman, J. M. (2014). Projections of the size
and composition of the U.S. population: 2014 to 2060.
Current Population Reports, P25-1143, Washington, DC:
U.S. Census Bureau.
Collins, S. E., Malone, D. K., & Clifasefi, S. L. (2013).
Housing retention in single-site housing first for
chronically homeless individuals with severe alcohol
problems. American Journal of Public Health, 103(Suppl.
2), S269–S274. doi:10.2105/ajph.2013.301312
Conner, K. R., Gamble, S. A., Bagge, C. L., He, H., Swogger,
M. T., Watts, A., & Houston, R. J. (2014). Substance-
induced depression and independent depression in
proximal risk for suicidal behavior. Journal of Studies on
Alcohol and Drugs, 75(4), 567–572.
Connors, G. J., Maisto, S. A., Schlauch, R. C., Dearing, R. L.,
Prince, M. A., & Duerr, M. R. (2016). Therapeutic alliances
predict session by session drinking behavior in the
treatment of alcohol use disorders. Journal of Consulting
and Clinical Psychology, 84(11), 972–982. doi:10.1037/
ccp0000130
Cook, B. L., Trinh, N. H., Li, Z., Hou, S. S., & Progovac, A.
M. (2017). Trends in racial-ethnic disparities in access
to mental health care, 2004–2012. Psychiatric Services,
68(1), 9–16. doi:10.1176/appi.ps.201500453
Cook, T. B. (2013). Recent criminal offending and suicide
attempts: A national sample. Social Psychiatry and
Psychiatric Epidemiology, 48(5), 767–774. doi:10.1007/
s00127-012-0567-9
Cougle, J. R., Hakes, J. K., Macatee, R. J., Chavarria, J.,
& Zvolensky, M. J. (2015). Quality of life and risk of
psychiatric disorders among regular users of alcohol,
nicotine, and cannabis: An analysis of the National
Epidemiological Survey on Alcohol and Related
Conditions (NESARC). Journal of Psychiatric Research,
66–67, 135–141. doi: 10.1016/j.jpsychires.(2015). .05.004
Cox, K. B., Malte, C. A., & Saxon, A. J. (2017).
Characteristics and service utilization of homeless
veterans entering VA substance use treatment.
Psychological Services, 14(2), 208–213. doi:10.1037/
ser0000133
Craske, M. G., & Stein, M. B. (2016). Anxiety.
Lancet, 388(10063), 3048–3059. doi:10.1016/
s0140-6736(16)30381-6
Creswell, K. G., Bachrach, R. L., Wright, A. G., Pinto, A., &
Ansell, E. (2016). Predicting problematic alcohol use with
the DSM-5 alternative model of personality pathology.
Personality Disorders, 7(1), 103–111. doi:10.1037/
per0000131
Crisanti, A. S., Duran, D., Greene, R. N., Reno, J., Luna-
Anderson, C., & Altschul, D. B. (2017). A longitudinal
analysis of peer-delivered permanent supportive housing:
Impact of housing on mental and overall health in an
ethnically diverse population. Psychological Services,
14(2), 141–153. doi:10.1037/ser0000135
Crits-Christoph, P., Hamilton, J. L., Ring-Kurtz, S., Gallop, R.,
McClure, B., Kulaga, A., & Rotrosen, J. (2011). Program,
counselor, and patient variability in the alliance: A
multilevel study of the alliance in relation to substance
use outcomes. Journal of Substance Abuse Treatment,
40(4), 405–413. doi:10.1016/j.jsat.2011.01.003
Crowley, R. A., & Kirschner, N. (2015). The integration
of care for mental health, substance abuse, and other
behavioral health conditions into primary care: Executive
summary of an American College of Physicians position
paper. Annals of Internal Medicine, 163(4), 298–299.
doi:10.7326/m15-0510
Crunelle, C. L., van den Brink, W., Moggi, F., Konstenius,
M., Franck, J., Levin, F. R., . . . Matthys, F. (2018).
International consensus statement on screening,
diagnosis and treatment of substance use disorder
patients with comorbid attention deficit/hyperactivity
disorder. European Addiction Research, 24(1), 43–51.
doi:10.1159/000487767
Cunill, R., Castells, X., Tobias, A., & Capella, D. (2015).
Pharmacological treatment of attention deficit
hyperactivity disorder with co-morbid drug dependence.
Journal of Psychopharmacology, 29(1), 15–23.
doi:10.1177/0269881114544777
Cunningham, K. C., Farmer, C., LoSavio, S. T., Dennis, P. A.,
Clancy, C. P., Hertzberg, M. A., . . . Beckham, J. C. (2017).
A model comparison approach to trauma-related guilt as
a mediator of the relationship between PTSD symptoms
and suicidal ideation among veterans. Journal of Affective
Disorders, 221, 227–231. doi:10.1016/j.jad.2017.06.046
Curtis, M. A., Garlington, S., & Schottenfield, L. S. (2013).
Alcohol, drug, and criminal history restrictions in public
housing. Cityscape, 15, 37–52.
252 Appendix A

TIP 42Appendix A—Bibliography
Cusack, K. J., Morrissey, J. P., Cuddeback, G. S., Prins, A.,
& Williams, D. M. (2010). Criminal justice involvement,
behavioral health service use, and costs of forensic
assertive community treatment: A randomized trial.
Community Mental Health Journal, 46(4), 356–363.
doi:10.1007/s10597-010-9299-z
Cusack, M., & Montgomery, A. E. (2017). Examining the
bidirectional association between veteran homelessness
and incarceration within the context of permanent
supportive housing. Psychological Services, 14(2),
250–256. doi:10.1037/ser0000110
Cutcliffe, J. R., Travale, R., Richmond, M. M., & Green,
T. (2016). Considering the contemporary issues and
unresolved challenges facing therapeutic communities for
clients with alcohol and substance abuse. Issues in Mental
Health Nursing, 37(9), 642–650. doi:10.3109/01612840.2
016.1169465
Daley, D. C., & Marlatt, G. A. (1992). Relapse prevention:
Cognitive and behavioral interventions. In J. G. Lowinson,
P. Ruiz, R. B. Millman, & J. G. Langrod (Eds.), Substance
abuse: A comprehensive textbook (pp. 533–542).
Baltimore, MD: Williams and Wilkins.
Danielson, M. L., Bitsko, R. H., Ghandour, R. M., Holbrook,
J. R., Kogan, M. D., & Blumberg, S. J. (2018). Prevalence
of parent-reported ADHD diagnosis and associated
treatment among US children and adolescents, 2016.
Journal of Clinical Child & Adolescent Psychology, 47(2),
199–212.
Darvishi, N., Farhadi, M., Haghtalab, T., & Poorolajal, J.
(2015). Alcohol-related risk of suicidal ideation, suicide
attempt, and completed suicide: A meta-analysis.
PLoS ONE, 10(5), e0126870. doi:10.1371/journal.
pone.0126870
Dass-Brailsford, P., & Safilian, C. M. (2017). Integrated
approaches to treating psychological trauma and
substance abuse in women: An update. Trauma & Acute
Care, 2(2), 41.
Daughters, S. B., Magidson, J. F., Lejuez, C. W., & Chen,
Y. (2016). LETS ACT: A behavioral activation treatment
for substance use and depression. Advances in Dual
Diagnosis, 9(2–3), 74–84. doi:10.1108/ADD-02-2016-0006
Davidson, L., Bellamy, C., Guy, K., & Miller, R. (2012). Peer
support among persons with severe mental illnesses: A
review of evidence and experience. World Psychiatry,
11(2), 123–128.
Davies, W. (2017). Understanding the pathophysiology of
postpartum psychosis: Challenges and new approaches.
World Journal of Psychiatry, 7(2), 77–88. doi:10.5498/wjp.
v7.i2.77
Davis, H., & Attia, E. (2017). Pharmacotherapy of eating
disorders. Current Opinion in Psychiatry, 30(6), 452–457.
doi:10.1097/YCO.0000000000000358
Dawson, D. A., Smith, S. M., Saha, T. D., Rubinsky, A. D.,
& Grant, B. F. (2012). Comparative performance of the
AUDIT-C in screening for DSM-IV and DSM-5 alcohol
use disorders. Drug and Alcohol Dependence, 126(3),
384–388. doi:10.1016/j.drugalcdep.2012.05.029
De Alwis, D., Lynskey, M. T., Reiersen, A. M., & Agrawal, A.
(2014). Attention-deficit/hyperactivity disorder subtypes
and substance use and use disorders in NESARC.
Addictive Behaviors, 39(8), 1278–1285. doi:10.1016/j.
addbeh.2014.04.003
De Crescenzo, F., Cortese, S., Adamo, N., & Janiri, L. (2017).
Pharmacological and non-pharmacological treatment
of adults with ADHD: A meta-review. Evidence Based
Mental Health, 20(1), 4–11. doi:10.1136/eb-2016-102415
De Hert, M., Cohen, D., Bobes, J., Cetkovich-Bakmas,
M., Leucht, S., Ndetei, D. M., . . . Correll, C. U. (2011).
Physical illness in patients with severe mental disorders.
II. Barriers to care, monitoring and treatment guidelines,
plus recommendations at the system and individual level.
World Psychiatry, 10(2), 138–151.
de Jonge, P., Roest, A. M., Lim, C. C., Florescu, S. E.,
Bromet, E. J., Stein, D. J., . . . Scott, K. M. (2016). Cross-
national epidemiology of panic disorder and panic attacks
in the world mental health surveys. Depression and
Anxiety, 33(12), 1155–1177. doi:10.1002/da.22572
de la Sierra, L. R. (2002). Countertransference: Our
difficulties in the treatment of substance abuse. In The
psychodynamics of addiction (pp. 141–152). Philadelphia,
PA: Whurr Publishers.
De Leon, G. (1996). Integrative recovery: A stage
paradigm. Substance Abuse, 17(1), 51–63.
doi:10.1080/08897079609444728
De Leon, G. (2000). Modified therapeutic community
for homeless mentally ill chemical abusers: Treatment
outcomes. American Journal of Drug and Alcohol Abuse
26(3), 461–480.
De Leon, G. (2015). “The gold standard” and related
considerations for a maturing science of substance abuse
treatment. Therapeutic communities; a case in point.
Substance Use and Misuse, 50(8–9), 1106–1109. doi:10.3
109/10826084.2015.1012846
De Leon, G., Sacks, S., Staines, G., & McKendrick, K. (2000).
Modified therapeutic community for homeless mentally ill
chemical abusers: Treatment outcomes. American Journal
of Drug and Alcohol Abuse, 26(3), 461–480.
DeMarce, J. M., Lash, S. J., Stephens, R. S., Grambow, S.
C., & Burden, J. L. (2008). Promoting continuing care
adherence among substance abusers with co-occurring
psychiatric disorders following residential treatment.
Addictive Behaviors, 33(9), 1104–1112. doi:10.1016/j.
addbeh.2008.02.008
Appendix A 253

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
Department of Veterans Affairs & Department of Defense.
(2015). VA/DoD clinical practice guideline for the
management of substance use disorders. Version 3. 0.
Retrieved from www.healthquality.va.gov/guidelines/MH/
sud/VADODSUDCPGRevised22216.pdf
Department of Veterans Affairs & Department of
Defense. (2017). VA/DoD clinical practice guideline
for the management of posttraumatic stress disorder
and acute stress disorder. Version 3.0. Retrieved
from www.healthquality.va.gov/guidelines/MH/ptsd/
VADoDPTSDCPGFinal012418.pdf
Detweiler, M. B., Pagadala, B., Candelario, J., Boyle, J. S.,
Detweiler, J. G., & Lutgens, B. W. (2016). Treatment of
post-traumatic stress disorder nightmares at a Veterans
Affairs medical center. Journal of Clinical Medicine, 5(12).
pii: E117. doi:10.3390/jcm5120117
De Witte, N. A., Crunelle, C. L., Sabbe, B., Moggi, F.,
& Dom, G. (2014). Treatment for outpatients with
comorbid schizophrenia and substance use disorders: A
review. European Addiction Research, 20(3), 105–114.
doi:10.1159/000355267
Diaz, N., Horton, E. G., & Weiner, M. (2012). Dysthymia,
major depression, and double depression among
individuals receiving substance abuse treatment. Health,
4(12), 1–9. doi:10.4236/health.2012.412181
Dickey, B., & Ware, N. C. (2008). Therapeutic
communities and mental health system reform.
Psychiatric Rehabilitation Journal, 32(2), 105–109.
doi:10.2975/32.2.2008.105.109
DiClemente, C. C., Corno, C. M., Graydon, M. M.,
Wiprovnick, A. E., & Knoblach, D. J. (2017). Motivational
interviewing, enhancement, and brief interventions over
the last decade: A review of reviews of efficacy and
effectiveness. Psychology of Addictive Behaviors, 31(8),
862–887. doi:10.1037/adb0000318
Dieterich, M., Irving, C. B., Bergman, H., Khokhar, M.
A., Park, B., & Marshall, M. (2017). Intensive case
management for severe mental illness. Schizophrenia
Bulletin, 43(4), 698–700. doi:10.1093/schbul/sbx061
Ding, K., Slate, M., & Yang, J. (2017). History of co-
occurring disorders and current mental health status
among homeless veterans. BMC Public Health, 18, 751.
Ding, K., Yang, J., Cheng, G., Schiltz, T., Summers, K. M.,
& Skinstad, A. H. (2011). Hospitalizations and hospital
charges for co-occurring substance use and mental
disorders. Journal of Substance Abuse Treatment, 40(4),
366–375. doi:10.1016/j.jsat.2010.12.005
Dixon, L. B., Holoshitz, Y., & Nossel, I. (2016). Treatment
engagement of individuals experiencing mental illness:
Review and update. World Psychiatry, 15(1), 13–20.
doi:doi:10.1002/wps.20306
Domenico, L. H., Lewis, B., Hazarika, M., & Nixon, S. J.
(2018). Characterizing anxiety among individuals receiving
treatment for alcohol and substance use disorders.
Journal of the American Psychiatric Nurses Association,
24(4), 343–351. doi:10.1177/1078390317739106
Doucet, S., Jones, I., Letourneau, N., Dennis, C. L., &
Blackmore, E. R. (2011). Interventions for the prevention
and treatment of postpartum psychosis: A systematic
review. Archives of Women’s Mental Health, 14(2), 89–98.
doi:10.1007/s00737-010-0199-6
Drainoni, M. L., Farrell, C., Sorensen-Alawad, A., Palmisano,
J. N., Chaisson, C., & Walley, A. Y. (2014). Patient
perspectives of an integrated program of medical care
and substance use treatment. AIDS Patient Care and
STDs, 28(2), 71–81. doi:10.1089/apc.2013.0179
Drake, R. E., Bond, G. R., Goldman, H. H., Hogan, M.
F., & Karakus, M. (2016). Individual placement and
support services boost employment for people with
serious mental illnesses, but funding is lacking. Health
Affairs (Millwood), 35(6), 1098–1105. doi:10.1377/
hlthaff.2016.0001
Drake, R. E., Luciano, A. E., Mueser, K. T., Covell, N.
H., Essock, S. M., Xie, H., & McHugo, G. J. (2016).
Longitudinal course of clients with co-occurring
schizophrenia-spectrum and substance use disorders in
urban mental health centers: A 7-year prospective study.
Schizophrenia Bulletin, 42(1), 202–211. doi:10.1093/
schbul/sbv110
Drymalski, W. M., & Campbell, T. C. (2009). A review of
Motivational Interviewing to enhance adherence to
antipsychotic medication in patients with schizophrenia:
Evidence and recommendations. Journal of Mental
Health, 18(1), 6–15. doi:10.1080/09638230802052161
Drymalski, W. M., & Nunley, M. R. (2016). The use of the
Addiction Severity Index psychiatric composite scores
to predict psychiatric inpatient admissions. Journal
of Addictions Nursing, 27(3), 190–196. doi:10.1097/
jan.0000000000000134
Drymalski, W. M., & Nunley, M. R. (2018). Sensitivity of
the ASAM criteria to psychiatric need. International
Journal of Mental Health and Addiction, 16(3), 617–629.
doi:10.1007/s11469-017-9801-8
Duijkers, J. C., Vissers, C. T., & Egger, J. I. (2016).
Unraveling executive functioning in dual diagnosis.
Frontiers in Psychology, 7, 979.
Dundon, W. D., Pettinati, H. M., Lynch, K. G., Xie, H.,
Varillo, K. M., Makadon, C., & Oslin, D. W. (2008). The
therapeutic alliance in medical-based interventions
impacts outcome in treating alcohol dependence. Drug
and Alcohol Dependence, 95(3), 230–236. doi:10.1016/j.
drugalcdep.2008.01.010
254 Appendix A

TIP 42Appendix A—Bibliography
Dunne, E. M., Burrell, L. E., 2nd, Diggins, A. D., Whitehead,
N. E., & Latimer, W. W. (2015). Increased risk for
substance use and health-related problems among
homeless veterans. American Journal of Addictions, 24(7),
676–680. doi:10.1111/ajad.12289
Dursa, E. K., Barth, S. K., Schneiderman, A. I., & Bossarte, R.
M. (2016). Physical and mental health status of Gulf War
and Gulf Era veterans: Results from a large population-
based epidemiological study. Journal of Occupational
and Environmental Medicine, 58(1), 41–46. doi:10.1097/
jom.0000000000000627
Dye, M. H., Roman, P. M., Knudsen, H. K., & Johnson, J. A.
(2012). The availability of integrated care in a national
sample of therapeutic communities. Journal of Behavioral
Health Services & Research, 39(1), 17–27. doi:10.1007/
s11414-011-9251-1
Dykstra, R. E., Schumacher, J. A., Mota, N., & Coffey, S.
F. (2015). Examining the role of antisocial personality
disorder in intimate partner violence among substance
use disorder treatment seekers with clinically significant
trauma histories. Violence Against Women, 21(8),
958–974. doi:10.1177/1077801215589377
Eby, L. T., Burk, H., & Maher, C. P. (2010). How serious
of a problem is staff turnover in substance abuse
treatment? A longitudinal study of actual turnover.
Journal of Substance Abuse Treatment, 39(3), 264–271.
doi:10.1016/j.jsat.2010.06.009
Eby, L. T., Laschober, T. C., & Curtis, S. L. (2014). Substance
abuse-specific knowledge transfer or loss? Treatment
program turnover versus professional turnover among
substance abuse clinicians. Journal of Addictive Diseases,
33(3), 243–252. doi:10.1080/10550887.2014.950022
Edwards, R. (2006). The role and competencies of staff in
the treatment of coexisting problems of mental health
and substance misuse. In R. G. Hussein (Ed.), Dual
diagnosis nursing (pp. 285–295). Hoboken, NJ: Blackwell
Publishing.
Egan, T. E., Dawson, A. E., & Wymbs, B. T. (2017).
Substance use in undergraduate students with histories
of attention-deficit/hyperactivity disorder (ADHD): The
role of impulsivity. Substance Use and Misuse, 52(10),
1375–1386. doi:10.1080/10826084.2017.1281309
Ellenhorn, R. (2015). Assertive community treatment:
A “living-systems” alternative to hospital and
residential care. Psychiatric Annals, 45(3), 120–125.
doi:10.3928/00485713-20150304-06
Elmquist, J., Shorey, R. C., Anderson, S., & Stuart, G. L.
(2015). Eating disorder symptoms and length of stay in
residential treatment for substance use: A brief report.
Journal of Dual Diagnosis, 11(3–4), 233–237. doi:10.1080/
15504263.2015.1104480
Epstein, A. J., Barry, C. L., Fiellin, D. A., & Busch, S.
H. (2015). Consumers’ valuation of primary care-
based treatment options for mental and substance
use disorders. Psychiatric Services, 66(8), 772–774.
doi:10.1176/appi.ps.201500077
Evans, E., Padwa, H., Li, L., Lin, V., & Hser, Y. I. (2015).
Heterogeneity of mental health service utilization and
high mental health service use among women eight years
after initiating substance use disorder treatment. Journal
of Substance Abuse Treatment, 59, 10–19. doi:10.1016/j.
jsat.2015.06.021
Ewing, G., Austin, L., Diffin, J., & Grande, G. (2015).
Developing a person-centred approach to career
assessment and support. British Journal of
Community Nursing, 20(12), 580–584. doi:10.12968/
bjcn.2015.20.12.580
Farren, C. K., Hill, K. P., & Weiss, R. D. (2012). Bipolar
disorder and alcohol use disorder: A review. Current
Psychiatry Reports, 14(6), 659–666. doi:10.1007/
s11920-012-0320-9
Fazel, S., Yoon, I. A., & Hayes, A. J. (2017). Substance use
disorders in prisoners: An updated systematic review and
meta-regression analysis in recently incarcerated men
and women. Addiction, 112(10), 1725–1739. doi:10.1111/
add.13877
Fearn, N. E., Vaughn, M. G., Nelson, E. J., Salas-Wright, C.
P., DeLisi, M., & Qian, Z. (2016). Trends and correlates
of substance use disorders among probationers and
parolees in the United States 2002–2014. Drug and
Alcohol Dependence, 167, 128–139. doi:10.1016/j.
drugalcdep.2016.08.003
Fisher, W. H., Geller, J. L., & Pandiani, J. A. (2009). The
changing role of the state psychiatric hospital. Health
Affairs, 28(3), 676–684. doi:10.1377/hlthaff.28.3.676
Flanagan, J. C., Korte, K. J., Killeen, T. K., & Back, S. E.
(2016). Concurrent treatment of substance use and
PTSD. Current Psychiatry Reports, 18(8). doi:10.1007/
s11920-016-0709-y
Food and Drug Administration (FDA). (March
2007). Strattera. Patient information. www.
accessdata.fda.gov/drugsatfda_docs/
label/2007/021411s004s012s013s015s021lbl.pdf
Food and Drug Administration. (2010). Kapvay. Prescribing
information. www.accessdata.fda.gov/drugsatfda_docs/
label/2010/022331s001s002lbl.pdf
Food and Drug Administration. (2013). Intuniv. Prescribing
information. www.accessdata.fda.gov/drugsatfda_docs/
label/2013/022037s009lbl.pdf
Food and Drug Administration. (April 28, 2017). Depression:
FDA-approved medications may help. Consumer
updates. Retrieved from www.fda.gov/forconsumers/
consumerupdates/ucm095980.htm
Appendix A 255

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
Food and Drug Administration. (March 5, 2019). FDA
approves new nasal spray medication for treatment-
resistant depression; available only at a certified doctor’s
office or clinic. Retrieved from www.fda.gov/NewsEvents/
Newsroom/PressAnnouncements/ucm632761.htm
Ford, J. A., & Perna, D. (2015). Prescription drug misuse
and suicidal ideation: Findings from the National Survey
on Drug Use and Health. Drug and Alcohol Dependence,
157, 192–196. doi:10.1016/j.drugalcdep.2015.10.010
Fouladi, F., Mitchell, J. E., Crosby, R. D., Engel, S. G., Crow,
S., Hill, L., . . . Steffen, K. J. (2015). Prevalence of alcohol
and other substance use in patients with eating disorders.
European Eating Disorders Review, 23(6), 531–536.
doi:10.1002/erv.2410
Fountoulakis, K. N., Grunze, H., Vieta, E., Young, A.,
Yatham, L., Blier, P., … Moeller, H. J. (2017). The
International College of Neuro-Psychopharmacology
(CINP) treatment guidelines for bipolar disorder in
adults (CINP-BD-2017), Part 3: The clinical guidelines.
International Journal of Neuropsychopharmacology,
20(2), 180–195. doi:10.1093/ijnp/pyw109
Fowler, K. A., Jack, S. P. D., Lyons, B. H., Betz, C. J., &
Petrosky, E. (2018). Surveillance for violent deaths—
National Violent Death Reporting System, 18 states,
2014. MMWR Surveillance Summaries, 67(2), 1–36.
doi:10.15585/mmwr.ss6702a1
Franko, D. L., Keshaviah, A., Eddy, K. T., Krishna, M., Davis,
M. C., Keel, P. K., & Herzog, D. B. (2013). A longitudinal
investigation of mortality in anorexia nervosa and bulimia
nervosa. American Journal of Psychiatry, 170(8), 917–925.
doi:10.1176/appi.ajp.2013.12070868
Fries, H. P., & Rosen, M. I. (2011). The efficacy of assertive
community treatment to treat substance use. Journal
of the American Psychiatric Nurses Association, 17(1),
45–50. doi:10.1177/1078390310393509
Frisman, L. K., Mueser, K. T., Covell, N. H., Lin, H. J.,
Crocker, A., Drake, R. E., & Essock, S. M. (2009).
Use of integrated dual disorder treatment via
assertive community treatment versus clinical case
management for persons with co-occurring disorders
and antisocial personality disorder. Journal of Nervous
and Mental Disease, 197(11), 822–828. doi:10.1097/
NMD.0b013e3181beac52
Frounfelker, R. L., Wilkniss, S. M., Bond, G. R., Devitt,
T. S., & Drake, R. E. (2011). Enrollment in supported
employment services for clients with a co-occurring
disorder. Psychiatric Services, 62(5), 545–547.
doi:10.1176/ps.62.5.pss6205_0545
Fruzzetti, A. E. (October 03, 2017). Why borderline
personality disorder is misdiagnosed. Retrieved from
www.nami.org/Blogs/NAMI-Blog/October-2017/
Why-Borderline-Personality-Disorder-is-Misdiagnose
Fulton, J. J., Calhoun, P. S., Wagner, H. R., Schry, A. R.,
Hair, L. P., Feeling, N., . . . Beckham, J. C. (2015). The
prevalence of posttraumatic stress disorder in Operation
Enduring Freedom/Operation Iraqi Freedom (OEF/OIF)
veterans: A meta-analysis. Journal of Anxiety Disorders,
31, 98–107. doi:10.1016/j.janxdis.2015.02.003
Gadermann, A. M., Alonso, J., Vilagut, G., Zaslavsky, A. M.,
& Kessler, R. C. (2012). Comorbidity and disease burden
in the National Comorbidity Survey Replication (NCS-R).
Depression and Anxiety, 29(9), 797–806. doi:10.1002/
da.21924
Gainsbury, S. M. (2017). Cultural competence in the
treatment of addictions: Theory, practice and evidence.
Clinical Psychology & Psychotherapy, 24(4), 987–1001.
doi:10.1002/cpp.2062
Galán, C. A., & Humphreys, K. L. (Aug 2, 2017). ADHD
and substance use: Current evidence and treatment
considerations. Psychiatric Times, 34(8), 1–3.
Garcia, S., Martinez-Cengotitabengoa, M., Lopez-Zurbano,
S., Zorrilla, I., Lopez, P., Vieta, E., & Gonzalez-Pinto, A.
(2016). Adherence to antipsychotic medication in bipolar
disorder and schizophrenic patients: A systematic review.
Journal of Clinical Psychopharmacology, 36(4), 355–371.
doi:10.1097/jcp.0000000000000523
Garner, B. R., & Hunter, B. D. (2014). Predictors of staff
turnover and turnover intentions within addiction
treatment settings: Change over time matters. Substance
Abuse, 8, 63–71. doi:10.4137/SART.S17133
GBD 2016 Disease and Injury Incidence and Prevalence
Collaborators. (2017). Global, regional, and national
incidence, prevalence, and years lived with disability for
328 diseases and injuries for 195 countries, 1990–2016:
A systematic analysis for the Global Burden of Disease
Study 2016. Lancet, 390(10100), 1211–1259. doi:10.1016/
s0140-6736(17)32154-2
Gentile, S. (2017). Untreated depression during pregnancy:
Short- and long-term effects in offspring. A systematic
review. Neuroscience, 342, 154–166. doi:10.1016/j.
neuroscience.2015.09.001
Ghafoori, B., Barragan, B., & Palinkas, L. (2014). Mental
health service use among trauma-exposed adults:
A mixed-methods study. Journal of Nervous and
Mental Disease, 202(3), 239–246. doi:10.1097/
nmd.0000000000000108
Gibbon, S., Duggan, C., Stoffers, J., Huband, N., Vollm,
B. A., Ferriter, M., & Lieb, K. (2010). Psychological
interventions for antisocial personality disorder.
Cochrane Database of Systematic Reviews, 6, CD007668.
doi:10.1002/14651858.CD007668.pub2
Gilmer, T. P., Manning, W. G., & Ettner, S. L. (2009). A cost
analysis of San Diego County’s REACH program for
homeless persons. Psychiatric Services, 60(4), 445–450.
doi:10.1176/appi.ps.60.4.445
256 Appendix A

TIP 42Appendix A—Bibliography
Gilmore, A. K., Brignone, E., Painter, J. M., Lehavot, K.,
Fargo, J., Suo, Y., . . . Gundlapalli, A. V. (2016). Military
sexual trauma and co-occurring posttraumatic stress
disorder, depressive disorders, and substance use
disorders among returning Afghanistan and Iraq veterans.
Women’s Health Issues, 26(5), 546–554. doi:10.1016/j.
whi.2016.07.001
Glenn, A. L., Johnson, A. K., & Raine, A. (2013). Antisocial
personality disorder: A current review. Current Psychiatry
Reports, 15(12), 427. doi:10.1007/s11920-013-0427-7
Gold, A. K., Otto, M. W., Deckersbach, T., Sylvia, L. G.,
Nierenberg, A. A., & Kinrys, G. (2018). Substance use
comorbidity in bipolar disorder: A qualitative review of
treatment strategies and outcomes. American Journal of
Addictions, 27(3), 188–201. doi:10.1111/ajad.12713
Gold, L. H. (2014). DSM-5 and the assessment of
functioning: The World Health Organization disability
assessment schedule 2.0 (WHODAS 2.0). Journal of the
American Academy of Psychiatry and the Law, 42(2),
173–181.
Goldstein, R. B., Smith, S. M., Chou, S. P., Saha, T. D., Jung,
J., Zhang, H., . . . Grant, B. F. (2016). The epidemiology of
DSM-5 posttraumatic stress disorder in the United States:
Results from the National Epidemiologic Survey on
Alcohol and Related Conditions-III. Social Psychiatry and
Psychiatric Epidemiology, 51(8), 1137–1148. doi:10.1007/
s00127-016-1208-5
Goodman, D. J., Milliken, C. U., Theiler, R. N., Nordstrom,
B. R., & Akerman, S. C. (2015). A multidisciplinary
approach to the treatment of co-occurring opioid use
disorder and posttraumatic stress disorder in pregnancy:
A case report. Journal of Dual Diagnosis, 11(3–4),
248–257. doi:10.1080/15504263.2015.1104484
Goodrich, D. E., Kilbourne, A. M., Nord, K. M., & Bauer, M.
S. (2013). Mental health collaborative care and its role in
primary care settings. Current Psychiatry Reports, 15(8),
383. doi:10.1007/s11920-013-0383-2
Goodwin, R. D., & Stein, D. J. (2013). Anxiety disorders and
drug dependence: Evidence on sequence and specificity
among adults. Psychiatry and Clinical Neurosciences,
67(3), 167–173. doi:10.1111/pcn.12030
Grant, B. F., Chou, S. P., Goldstein, R. B., Huang, B., Stinson,
F. S., Saha, T. D., . . . Ruan, W. J. (2008). Prevalence,
correlates, disability, and comorbidity of DSM-IV
borderline personality disorder: Results from the Wave 2
National Epidemiologic Survey on Alcohol and Related
Conditions. Journal of Clinical Psychiatry, 69(4), 533–545.
doi:ej07m03916
Grant, B. F., Goldstein, R. B., Saha, T. D., Chou, S. P., Jung,
J., Zhang, H., . . . Hasin, D. S. (2015). Epidemiology of
DSM-5 alcohol use disorder: Results from the National
Epidemiologic Survey on Alcohol and Related Conditions
III. JAMA Psychiatry, 72(8), 757–766. doi:10.1001/
jamapsychiatry.2015.0584
Grant, B. F., Hasin, D. S., Stinson, F. S., Dawson, D. A.,
Chou, S. P., Ruan, W. J., & Pickering, R. P. (2004).
Prevalence, correlates, and disability of personality
disorders in the United States: Results from the National
Epidemiologic Survey on Alcohol and Related Conditions.
Journal of Clinical Psychiatry, 65(7), 948–958.
Grant, B. F., Saha, T. D., Ruan, W. J., Goldstein, R. B., Chou,
S. P., Jung, J., . . . Hasin, D. S. (2016). Epidemiology of
DSM-5 drug use disorder: Results from the National
Epidemiologic Survey on Alcohol and Related Conditions-
III. JAMA Psychiatry, 73(1), 39–47. doi:10.1001/
jamapsychiatry.2015.2132
Grattan, A., Sullivan, M. D., Saunders, K. W., Campbell, C.
I., & Von Korff, M. R. (2012). Depression and prescription
opioid misuse among chronic opioid therapy recipients
with no history of substance abuse. Annals of Family
Medicine, 10(4), 304–311. doi:10.1370/afm.1371
Green, C. A., Yarborough, M. T., Polen, M. R., Janoff, S. L.,
& Yarborough, B. J. (2015). Dual recovery among people
with serious mental illnesses and substance problems:
A qualitative analysis. Journal of Dual Diagnosis, 11(1),
33–41. doi:10.1080/15504263.2014.975004
Green, K. L., Brown, G. K., Jager-Hyman, S., Cha, J., Steer,
R. A., & Beck, A. T. (2015). The predictive validity of
the Beck Depression Inventory suicide item. Journal
of Clinical Psychiatry, 76(12), 1683–1686. doi:10.4088/
JCP.14m09391
Gregorowski, C., Seedat, S., & Jordaan, G. P. (2013). A
clinical approach to the assessment and management of
co-morbid eating disorders and substance use disorders.
BMC Psychiatry, 13, 289. doi:10.1186/1471-244x-13-289
Grella, C. E. (2008). From generic to gender-responsive
treatment: Changes in social policies, treatment services,
and outcomes of women in substance abuse treatment.
Journal of Psychoactive Drugs, 40(Suppl. 5), 327–343.
Grella, C. E., & Shi, Y. (2011). Stability of outcomes following
residential drug treatment for patients with co-occurring
disorders. Journal of Dual Diagnosis, 7(1–2), 103–112. doi
:10.1080/15504263.2011.566067
Grewal, R. S., & George, T. P. (July 14, 2017). Cannabis-
induced psychosis: A review. Psychiatric Times, 34(7), 1–5.
Group, W. A. W. (2002). The Alcohol, Smoking and
Substance Involvement Screening Test (ASSIST):
Development, reliability and feasibility. Addiction, 97(9),
1183–1194.
Guerrero, E., & Andrews, C. M. (2011). Cultural competence
in outpatient substance abuse treatment: Measurement
and relationship to wait time and retention. Drug and
Alcohol Dependence, 119(1–2), e13–e22. doi:10.1016/j.
drugalcdep.2011.05.020
Guerrero, E. G. (2013). Enhancing access and retention
in substance abuse treatment: The role of Medicaid
payment acceptance and cultural competence. Drug and
Alcohol Dependence, 132(3), 555–561. doi:10.1016/j.
drugalcdep.2013.04.005
Appendix A 257

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
Guerrero, E. G., Padwa, H., Lengnick-Hall, R., Kong, Y., &
Perrigo, J. L. (2015). Leadership and licensure for drug
treatment and the implementation of co-occurring
disorder treatment in community mental health centers.
Community Mental Health Journal, 51(5), 554–566.
doi:10.1007/s10597-015-9886-0
Guille, C., Newman, R., Fryml, L. D., Lifton, C. K., &
Epperson, C. N. (2013). Management of postpartum
depression. Journal of Midwifery & Women’s Health,
58(6), 643–653. doi:10.1111/jmwh.12104
Habel, L. A., Cooper, W. O., Sox, C. M., Chan, K. A.,
Fireman, B. H., Arbogast, P. G., . . . Selby, J. V. (2011).
ADHD medications and risk of serious cardiovascular
events in young and middle-aged adults. JAMA, 306(24),
2673–2683. doi:10.1001/jama.2011.1830
Hagler, K. J., Rice, S. L., Munoz, R. E., Salvador, J. G.,
Forcehimes, A. A., & Bogenschutz, M. P. (2015). “It
Might Actually Work This Time”: Benefits and barriers
to adapted 12-step facilitation therapy and mutual-
help group attendance from the perspective of dually
diagnosed individuals. Journal of Addictions Nursing,
26(3), 120–128. doi:10.1097/jan.0000000000000083
Haller, M., Colvonen, P. J., Davis, B. C., Trim, R. S., Bogner,
R., Sevcik, J., & Norman, S. B. (2016). Examining
pretreatment differences between veterans in residential
versus outpatient treatment for alcohol use disorder
and comorbid combat-related PTSD. Journal of Dual
Diagnosis, 12(3–4), 282–289. doi:10.1080/15504263.201
6.1256516
Haller, M., Norman, S. B., Cummins, K., Trim, R. S., Xu,
X., Cui, R., . . . Tate, S. R. (2016). Integrated cognitive
behavioral therapy versus cognitive processing therapy
for adults with depression, substance use disorder, and
trauma. Journal of Substance Abuse Treatment, 62,
38–48. doi:10.1016/j.jsat.2015.11.005
Halloran, L. (2013). Substance abuse in primary care. Journal
for Nurse Practitioners, 9(7), 475–476.
Hamdi, N. R., & Iacono, W. G. (2014). Lifetime
prevalence and co-morbidity of externalizing
disorders and depression in prospective assessment.
Psychological Medicine, 44(2), 315–324. doi:10.1017/
s0033291713000627
Han, B., Compton, W. M., Blanco, C., & Colpe, L. J. (2017).
Prevalence, treatment, and unmet treatment needs of US
adults with mental health and substance use disorders.
Health Affairs (Millwood), 36(10), 1739–1747.
Han, B., Olfson, M., & Mojtabai, R. (2017). Depression
care among adults with co-occurring major depressive
episodes and substance use disorders in the United
States. Journal of Psychiatric Research, 91, 47–56.
doi:10.1016/j.jpsychires.2017.02.026
Harrison, J., Cousins, L., Spybrook, J., & Curtis, A. (2017).
Peers and co-occurring research-supported interventions.
Journal of Evidence-Informed Social Work, 14(3),
201–215. doi:10.1080/23761407.2017.1316220
Harrison, M. L., Moore, K. A., Young, S., Flink, D., &
Ochshorn, E. (2008). Implementing the comprehensive,
continuous, integrated system of care model for
individuals with co-occurring disorders: Preliminary
findings from a residential facility serving homeless
individuals. Journal of Dual Diagnosis, 4(3), 238–259.
Harrold, S. A., Libet, J., Pope, C., Lauerer, J. A., Johnson,
E., & Edlund, B. J. (2018). Increasing physical activity
for veterans in the Mental Health Intensive Case
Management Program: A community-based intervention.
Perspectives in Psychiatric Care, 54(2), 266–273.
doi:10.1111/ppc.12233
Harrop, E. N., & Marlatt, G. A. (2010). The comorbidity of
substance use disorders and eating disorders in women:
Prevalence, etiology, and treatment. Addictive Behaviors,
35(5), 392–398. doi:10.1016/j.addbeh.2009.12.016
Hartz, S. M., Pato, C. N., Medeiros, H., Cavazos-Rehg,
P., Sobell, J. L., Knowles, J. A., . . . Pato, M. T. (2014).
Comorbidity of severe psychotic disorders with measures
of substance use. JAMA Psychiatry, 71(3), 248–254.
doi:10.1001/jamapsychiatry.2013.3726
Harvard Medical School. (2005). National Comorbidity
Survey (NCS). Retrieved from https://www.hcp.med.
harvard.edu/ncs/
Hasin, D., Fenton, M. C., Skodol, A., Krueger, R., Keyes,
K., Geier, T., . . . Grant, B. (2011). Personality disorders
and the 3-year course of alcohol, drug, and nicotine
use disorders. Archives of General Psychiatry, 68(11),
1158–1167. doi:10.1001/archgenpsychiatry.2011.78
Hasin, D., & Kilcoyne, B. (2012). Comorbidity of psychiatric
and substance use disorders in the United States:
Current issues and findings from the NESARC. Current
Opinion in Psychiatry, 25(3), 165–171. doi:10.1097/
YCO.0b013e3283523dcc
Hasin, D. S., & Grant, B. F. (2015). The National
Epidemiologic Survey on Alcohol and Related Conditions
(NESARC) Waves 1 and 2: Review and summary of
findings. Social Psychiatry and Psychiatric Epidemiology,
50(11), 1609–1640. doi:10.1007/s00127-015-1088-0
Hasin, D. S., Kerridge, B. T., Saha, T. D., Huang, B.,
Pickering, R., Smith, S. M., . . . Grant, B. F. (2016).
Prevalence and correlates of DSM-5 cannabis use
disorder, 2012–2013: Findings from the National
Epidemiologic Survey on Alcohol and Related Conditions-
III. American Journal of Psychiatry, 173(6), 588–599.
doi:10.1176/appi.ajp.2015.15070907
Hasin, D. S., O’Brien, C. P., Auriacombe, M., Borges, G.,
Bucholz, K., Budney, A., . . . Grant, B. F. (2013). DSM-5
criteria for substance use disorders: Recommendations
and rationale. American Journal of Psychiatry, 170(8),
834–851. doi:10.1176/appi.ajp.2013.12060782
258 Appendix A

TIP 42
Appendix A—Bibliography
Hasin, D. S., Sarvet, A. L., Meyers, J. L., Saha, T. D., Ruan,
W. J., Stohl, M., & Grant, B. F. (2018). Epidemiology of
Adult DSM-5 major depressive disorder and its specifiers
in the United States. JAMA Psychiatry, 75(4), 336–346.
doi:10.1001/jamapsychiatry.2017.4602
Haug, N. A., Duffy, M., & McCaul, M. E. (2014). Substance
abuse treatment services for pregnant women:
Psychosocial and behavioral approaches. Obstetrics and
Gynecology Clinics of North America, 41(2), 267–296.
doi:10.1016/j.ogc.2014.03.001
Havassy, B. E., & Mericle, A. A. (2013). Recent violence
among persons entering short-term residential mental
health and substance abuse treatment. Journal of Dual
Diagnosis, 9(3). doi:10.1080/15504263.2013.804773
Haviland, M. G., Banta, J. E., Sonne, J. L., & Przekop,
P. (2016). Posttraumatic stress disorder-related
hospitalizations in the United States (2002–2011): Rates,
co-occurring illnesses, suicidal ideation/self-harm, and
hospital charges. Journal of Nervous and Mental Disease,
204(2), 78–86. doi:10.1097/NMD.0000000000000432
Hawk, K., & D’Onofrio, G. (2018). Emergency department
screening and interventions for substance use disorders.
Addiction Science & Clinical Practice, 13(1), 18.
doi:10.1186/s13722-018-0117-1
Healey, P., Stager, M. L., Woodmass, K., Dettlaff, A. J.,
Vergara, A., Janke, R., & Wells, S. J. (2017). Cultural
adaptations to augment health and mental health
services: A systematic review. BMC Health Services
Research, 17(1), 8. doi:10.1186/s12913-016-1953-x
Health Resources and Services Administration (HRSA).
(2018). Behavioral health workforce projections,
2016–2030: Addiction counselors. Retrieved from https://
bhw.hrsa.gov/sites/default/files/bhw/nchwa/projections/
addiction-counselors-2018.pdf
Health Resources and Services Administration. (2020, March
1). Shortage areas. Retrieved from https://data.hrsa.gov/
topics/health-workforce/shortage-areas
Heffner, J. L., Blom, T. J., & Anthenelli, R. M. (2011).
Gender differences in trauma history and symptoms
as predictors of relapse to alcohol and drug use.
American Journal of Addictions, 20(4), 307–311.
doi:10.1111/j.1521-0391.2011.00141.x
Heimberg, R. G., Hofmann, S. G., Liebowitz, M. R., Schneier,
F. R., Smits, J. A. J., Stein, M. B., . . . Craske, M. G. (2014).
Social anxiety disorder in DSM-5. Depression and Anxiety,
31(6), 472–479. doi:10.1002/da.22231
Hendershot, C. S., Witkiewitz, K., George, W. H., & Marlatt,
G. A. (2011). Relapse prevention for addictive behaviors.
Substance Abuse Treatment, Prevention, and Policy, 6,
17. doi:10.1186/1747-597x-6-17
Henry, M., Shivji, A., de Sousa, T., and Cohen, R. (2015).
The 2015 Annual Homeless Assessment Report
(AHAR) to Congress. Part 1 – Point in time estimates of
homelessness. Retrieved from https://files.hudexchange.
info/resources/documents/2015-AHAR-Part-1.pdf
Henry, M., Watt, R., Rosenthal, L., & Shivji, A. (2016,
November). The 2016 Annual Homeless Assessment
Report (AHAR) to Congress. Part 1: Point-in-time
estimates of homelessness. Retrieved from https://files.
hudexchange.info/resources/documents/2016-AHAR-
Part-1.pdf
Henry, M., Watt, R., Mahathey, A., Ouellette, J., Sitler, A,
& Abt Associates. (2020, January). The 2019 Annual
Homeless Assessment Report (AHAR) to Congress.
Part 1: Point-in-time estimates of homelessness.
Retrieved from https://files.hudexchange.info/resources/
documents/2019-AHAR-Part-1.pdf
Hermes, E., & Rosenheck, R. (2016). Psychopharmacologic
services for homeless veterans: Comparing psychotropic
prescription fills among homeless and non-homeless
veterans with serious mental illness. Community
Mental Health Journal, 52(2), 142–147. doi:10.1007/
s10597-015-9904-2
Heslin, K. C., Elixhauser, A., & Steiner, C. A. (2015, June).
Hospitalizations involving mental and substance use
disorders among adults, 2012. HCUP Statistical Brief
#191. Agency for Healthcare Research and Quality,
Rockville, MD. Retrieved from www.hcup-us.ahrq.
gov/reports/statbriefs/sb191-Hospitalization-Mental-
Substance-Use-Disorders-2012.pdf
Hien, D. A., Jiang, H., Campbell, A. N. C., Hu, M.-C., Miele,
G. M., Cohen, L. R., . . . Nunes, E. V. (2010). Do treatment
improvements in PTSD severity affect substance use
outcomes? A secondary analysis from a randomized
clinical trial in NIDA’s Clinical Trials Network. American
Journal of Psychiatry, 167(1), 95–101. doi:10.1176/appi.
ajp.2009.09091261
Hjorthoj, C. R., Hjorthoj, A. R., & Nordentoft, M. (2012).
Validity of Timeline Follow-Back for self-reported use of
cannabis and other illicit substances—Systematic review
and meta-analysis. Addictive Behaviors, 37(3), 225–233.
doi:10.1016/j.addbeh.2011.11.025
Hogan, M. F., & Grumet, J. G. (2016). Suicide prevention:
An emerging priority for health care. Health Affairs, 35(6),
1084–1090. doi:10.1377/hlthaff.2015.1672
Holden, K., McGregor, B., Thandi, P., Fresh, E., Sheats,
K., Belton, A., . . . Satcher, D. (2014). Toward culturally
centered integrative care for addressing mental health
disparities among ethnic minorities. Psychological
Services, 11(4), 357–368. doi:10.1037/a0038122
Horsfall, J., Cleary, M., Hunt, G. E., & Walter, G.
(2009). Psychosocial treatments for people with
co-occurring severe mental illnesses and substance
use disorders (dual diagnosis): A review of empirical
evidence. Harvard Review of Psychiatry, 17(1), 24–34.
doi:10.1080/10673220902724599
Appendix A 259
TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
Hudson, J. I., Hiripi, E., Pope, H. G., Jr., & Kessler, R.
C. (2007). The prevalence and correlates of eating
disorders in the National Comorbidity Survey Replication.
Biological Psychiatry, 61(3), 348–358. doi:10.1016/j.
biopsych.2006.03.040
Huggard, P., Law, J., & Newcombe, D. (2017). A systematic
review exploring the presence of vicarious trauma,
compassion fatigue, and secondary traumatic stress in
alcohol and other drug clinicians. Australasian Journal of
Disaster and Trauma Studies, 21(2), 65–72.
Hunt, E., Peters, R. H., & Kremling, J. (2015). Behavioral
health treatment history among persons in the justice
system: Findings from the Arrestee Drug Abuse
Monitoring II Program. Psychiatric Rehabilitation Journal,
38(1), 7–15. doi:10.1037/prj0000132
Hunt, G. E., Malhi, G. S., Cleary, M., Lai, H. M. X., &
Sitharthan, T. (2016a). Comorbidity of bipolar and
substance use disorders in national surveys of general
populations, 1990–2015: Systematic review and meta-
analysis. Journal of Affective Disorders, 206, 321–330.
doi:10.1016/j.jad.2016.06.051
Hunt, G. E., Malhi, G. S., Cleary, M., Lai, H. M. X., &
Sitharthan, T. (2016b). Prevalence of comorbid bipolar
and substance use disorders in clinical settings,
1990–2015: Systematic review and meta-analysis. Journal
of Affective Disorders, 206, 331–349. doi:10.1016/j.
jad.2016.07.011
Hunt, G. E., Siegfried, N., Morley, K., Sitharthan, T.,
& Cleary, M. (2013). Psychosocial interventions for
people with both severe mental illness and substance
misuse. Cochrane Database of Systematic Reviews, 10,
CD001088. doi:10.1002/14651858.CD001088.pub3
Hunt, G. E., Siegfried, N., Morley, K., Sitharthan, T., &
Cleary, M. (2014). Psychosocial interventions for people
with both severe mental illness and substance misuse.
Schizophrenia Bulletin, 40(1), 18–20.
Hunt, T. K., & Forbush, K. T. (2016). Is “drunkorexia” an
eating disorder, substance use disorder, or both? Eating
Behaviors, 22, 40–45. doi:10.1016/j.eatbeh.2016.03.034
Hunter, S. B., Schwartz, R. P., & Friedmann, P. D. (2016).
Introduction to the Special Issue on the Studies on
the Implementation of Integrated Models of Alcohol,
Tobacco, and/or Drug Use Interventions and Medical
Care. Journal of Substance Abuse Treatment, 60, 1–5.
doi:10.1016/j.jsat.2015.10.001
Ilgen, M. A., Bohnert, A. S., Ignacio, R. V., McCarthy, J.
F., Valenstein, M. M., Kim, H. M., & Blow, F. C. (2010).
Psychiatric diagnoses and risk of suicide in veterans.
Archives of General Psychiatry, 67(11), 1152–1158.
doi:10.1001/archgenpsychiatry.2010.129
Jaffe, D. J. (2017). What is “serious mental illness” and what
is not? Retrieved from https://mentalillnesspolicy.org/
serious-mental-illness-not/
Jahn, D. R., Muralidharan, A., Drapalski, A. L., Brown, C. H.,
Fang, L. J., & Lucksted, A. (2018). Differences in suicide
and death ideation among veterans and nonveterans
with serious mental illness. Psychological Services, 15(1),
31–39. doi:10.1037/ser0000127
Johnson, J. A., Lee, A., Vinson, D., & Seale, J. P. (2013).
Use of AUDIT-based measures to identify unhealthy
alcohol use and alcohol dependence in primary
care: A validation study. Alcoholism: Clinical and
Experimental Research, 37(Suppl. 1), e253–e259.
doi:10.1111/j.1530-0277.2012.01898.x
Jones, C. M., & McCance-Katz, E. F. (2019). Co-occurring
substance use and mental disorders among adults with
opioid use disorder. Drug and Alcohol Dependence, 197,
78–82. doi:10.1016/j.drugalcdep.2018.12.030
Jones, D., & Arndt, S. (2017, October). The Iowa Pregnant
and Postpartum Women’s Residential Treatment Program:
Annual report. Retrieved from https://idph.iowa.gov/
Portals/1/userfiles/148/PPW%20Year%202%20Eval.pdf
Jones, I., Chandra, P. S., Dazzan, P., & Howard, L. M.
(2014). Bipolar disorder, affective psychosis, and
schizophrenia in pregnancy and the post-partum
period. Lancet, 384(9956), 1789–1799. doi:10.1016/
s0140-6736(14)61278-2
Jones, I., & Shakespeare, J. (2014). Postnatal depression.
BMJ, 349, g4500. doi:10.1136/bmj.g4500
Jones, Q., Johnston, B., Biola, H., Gomez, S., & Crowder,
C. (2018). Implementing standardized substance use
disorder screening in primary care. Journal of the
American Academy of Physician Assistants, 31(10), 42–45.
doi:10.1097/01.Jaa.0000511792.75301.73
Joseph, R., Kester, R., O’Brien, C., & Huang, H. (2017). The
evolving practice of psychiatry in the era of integrated
care. Psychosomatics, 58(5), 466–473. doi:10.1016/j.
psym.2017.04.003
Joyce, T. F., & Bailey, B. (2015). Supporting recovery in
acute care and emergency settings [PowerPoint slides].
Retrieved from www.samhsa.gov/sites/default/files/
programs_campaigns/recovery_to_practice/supporting-
recovery-in-acute-care-emergency-settings.pdf
Kaiser Family Foundation. (2017). Uninsured rates for the
nonelderly by race/ethnicity. Retrieved from www.kff.org/
uninsured/state-indicator/rate-by-raceethnicity/?currentT
imeframe=0&sortModel=%7B%22colId%22:%22Location
%22,%22sort%22:%22asc%22%7D
Kaiser Permanente. (2019). Alcohol use in older adults.
Retrieved from https://wa.kaiserpermanente.org/
healthAndWellness/index.jhtml?item=%2Fcommon%2Fh
ealthAndWellness%2FhealthyLiving%2Flifestyle%2Falcoh
ol-seniors.html
Kanbur, N., & Harrison, A. (2016). Co-occurrence of
substance use and eating disorders: An approach to the
adolescent patient in the context of family centered care.
A literature review. Substance Use and Misuse, 51(7),
853–860. doi:10.3109/10826084.2016.1155614
260 Appendix A

TIP 42Appendix A—Bibliography
Kang, H. K., Bullman, T. A., Smolenski, D. J., Skopp, N. A.,
Gahm, G. A., & Reger, M. A. (2015). Suicide risk among
1.3 million veterans who were on active duty during the
Iraq and Afghanistan wars. Annals of Epidemiology, 25(2),
96–100. doi:10.1016/j.annepidem.2014.11.020
Kantor, V., Knefel, M., & Lueger-Schuster, B. (2017).
Perceived barriers and facilitators of mental health service
utilization in adult trauma survivors: A systematic review.
Clinical Psychology Review, 52, 52–68. doi:10.1016/j.
cpr.2016.12.001
Katzman, M. A., Bilkey, T. S., Chokka, P. R., Fallu, A.,
& Klassen, L. J. (2017). Adult ADHD and comorbid
disorders: Clinical implications of a dimensional
approach. BMC Psychiatry, 17(1), 302. doi:10.1186/
s12888-017-1463-3
Keeley, R. D., Brody, D. S., Engel, M., Burke, B. L.,
Nordstrom, K., Moralez, E., . . . Emsermann, C. (2016).
Motivational interviewing improves depression outcome
in primary care: A cluster randomized trial. Journal of
Consulting and Clinical Psychology, 84(11), 993–1007.
doi:10.1037/ccp0000124
Keen, I. L., Whitehead, N. E., Clifford, L., Rose, J., &
Latimer, W. (2014). Perceived barriers to treatment in
a community-based sample of illicit-drug-using African
American men and women. Journal of Psychoactive
Drugs, 46(5), 444–449. doi:10.1080/02791072.2014.964
382
Kelley, K. J., & Kelley, M. F. (2013). Teaching empathy and
other compassion-based communication skills. Journal
for Nurses in Professional Development, 29(6), 321–324.
doi:10.1097/01.nnd.0000436794.24434.90
Kelly, J. F., Greene, M. C., & Bergman, B. G. (2016).
Recovery benefits of the “therapeutic alliance” among
12-step mutual-help organization attendees and their
sponsors. Drug and Alcohol Dependence, 162, 64–71.
doi.10.1016/j.drugalcdep.2016.02.028
Kelly, T. M., & Daley, D. C. (2013). Integrated treatment of
substance use and psychiatric disorders. Social Work in
Public Health, 28(3–4), 388–406. doi:10.1080/19371918.2
013.774673
Kerfoot, K. E., Rosenheck, R. A., Petrakis, I. L., Swartz, M.
S., Keefe, R. S., McEvoy, J. P., & Stroup, T. S. (2011).
Substance use and schizophrenia: Adverse correlates
in the CATIE study sample. Schizophrenia Research,
132(2–3), 177–182. doi:10.1016/j.schres.2011.07.032
Kerner, B. (2015). Comorbid substance use disorders
in schizophrenia: A latent class approach. Psychiatry
Research, 225(3), 395–401. doi:10.1016/j.
psychres.2014.12.006
Kertesz, S. G., Crouch, K., Milby, J. B., Cusimano, R.
E., & Schumacher, J. E. (2009). Housing first for
homeless persons with active addiction: Are we
overreaching? Milbank Quarterly, 87(2), 495–534.
doi:10.1111/j.1468-0009.2009.00565.x
Kessler, R. C. (2005). National Comorbidity Survey.
Retrieved from www.hcp.med.harvard.edu/ncs/
Kessler, R. C., Adler, L., Barkley, R., Biederman, J., Conners,
C. K., Demler, O., . . . Zaslavsky, A. M. (2006). The
prevalence and correlates of adult ADHD in the United
States: Results from the National Comorbidity Survey
Replication. American Journal of Psychiatry, 163(4),
716–723. doi:10.1176/appi.ajp.163.4.716
Kessler, R. C., Andrews, G., Colpe, L. J., Hiripi, E., Mroczek,
D. K., Normand, S. L., . . . Zaslavsky, A. M. (2002). Short
screening scales to monitor population prevalences
and trends in non-specific psychological distress.
Psychological Medicine, 32(6), 959–976.
Kessler, R. C., Barker, P. R., Colpe, L. J., Epstein, J. F.,
Gfroerer, J. C., Hiripi, E., . . . Zaslavsky, A. M. (2003).
Screening for serious mental illness in the general
population. Archives of General Psychiatry, 60(2),
184–189.
Kessler, R. C., Berglund, P., Demler, O., Jin, R., Merikangas,
K. R., & Walters, E. E. (2005). Lifetime prevalence and
age-of-onset distributions of DSM-IV disorders in the
National Comorbidity Survey Replication.Archives Of
General Psychiatry,62(6), 593–602.
Kessler, R. C., Green, J. G., Gruber, M. J., Sampson, N.
A., Bromet, E., Cuitan, M., . . . Zaslavsky, A. M. (2010).
Screening for serious mental illness in the general
population with the K6 screening scale: Results from
the WHO World Mental Health (WMH) survey initiative.
International Journal of Methods in Psychiatric Research,
19(Suppl. 1), 4–22. doi:10.1002/mpr.310
Kessler, R. C., Petukhova, M., Sampson, N. A., Zaslavsky, A.
M., & Wittchen, H. U. (2012). Twelve-month and lifetime
prevalence and lifetime morbid risk of anxiety and mood
disorders in the United States. International Journal
of Methods in Psychiatric Research, 21(3), 169–184.
doi:10.1002/mpr.1359
Keyser, D. J., Watkins, K. E., Vilamovska, A. M., & Pincus,
H. A. (2008). Focus on alcohol & drug abuse: Improving
service delivery for individuals with co-occurring
disorders: New perspectives on the quadrant model.
Psychiatric Services, 59(11), 1251–1253. doi:10.1176/appi.
ps.59.11.1251
Keyser-Marcus, L., Alvanzo, A., Rieckmann, T., Thacker, L.,
Sepulveda, A., Forcehimes, A., Islam, L. Z., … Svikis, D.
S. (2015). Trauma, gender, and mental health symptoms
in individuals with substance use disorders. Interpersonal
Violence, 30(1), 3–24. doi:10.1177/0886260514532523
Khalid, M. M., & Hamilton, R. J. (2020). Beta-blocker
toxicity. StatPearls [Internet]. Retrieved from www.ncbi.
nlm.nih.gov/books/NBK448097/?report=printable
Kidd, S. A., Davidson, L., & McKenzie, K. (2017). Common
factors in community mental health intervention: A
scoping review. Community Mental Health Journal, 53(6),
627–637. doi:10.1007/s10597-017-0117-8
Appendix A 261

TIP 42 Substance Use Disorder Treatment for People With Co-Occurring Disorders
Kidorf, M., Brooner, R. K., Gandotra, N., Antoine, D.,
King, V. L., Peirce, J., & Ghazarian, S. (2013). Reinforcing
integrated psychiatric service attendance in an opioid-
agonist program: A randomized and controlled trial. Drug
and Alcohol Dependence, 133(1), 30–36.
Killeen, T. K., Back, S. E., & Brady, K. T. (2015).
Implementation of integrated therapies for comorbid
post-traumatic stress disorder and substance use
disorders in community substance abuse treatment
programs. Drug and Alcohol Review, 34(3), 234–241.
doi:10.1111/dar.12229
Kills Small, N. J., Simons, J. S., & Stricherz, M. (2007).
Assessing criterion validity of the Simple Screening
Instrument for Alcohol and Other Drug Abuse (SSI-AOD)
in a college population. Addictive Behaviors, 32(10),
2425–2431. doi:10.1016/j.addbeh.2007.04.003
Kilpatrick, D. G., Resnick, H. S., Milanak, M. E., Miller, M.
W., Keyes, K. M., & Friedman, M. J. (2013). National
estimates of exposure to traumatic events and PTSD
prevalence using DSM-IV and DSM-5 criteria. Journal of
Traumatic Stress, 26(5), 537–547. doi:10.1002/jts.21848
Kim, G., DeCoster, J., Bryant, A. N., & Ford, K. L. (2016).
Measurement equivalence of the K6 Scale: The effects of
race/ethnicity and language. Assessment, 23(6), 758–768.
doi:10.1177/1073191115599639
Kimerling, R., Makin-Byrd, K., Louzon, S., Ignacio, R. V., &
McCarthy, J. F. (2016). Military sexual trauma and suicide
mortality. American Journal of Preventive Medicine, 50(6),
684–691. doi:10.1016/j.amepre.2015.10.019
Klassen, L. J., Bilkey, T. S., Katzman, M. A., & Chokka, P.
(2012). Comorbid attention deficit/hyperactivity disorder
and substance use disorder: Treatment considerations.
Current Drug Abuse Reviews, 5(3), 190–198.
Kline, A., Weiner, M. D., Ciccone, D. S., Interian, A., St.
Hill, L., & Losonczy, M. (2014). Increased risk of alcohol
dependency in a cohort of National Guard troops
with PTSD: A longitudinal study. Journal of Psychiatric
Research, 50, 18–25. doi:10.1016/j.jpsychires.2013.11.007
Knight, D. K., Broome, K. M., Edwards, J. R., & Flynn, P.
M. (2011). Supervisory turnover in outpatient substance
abuse treatment. Journal of Behavioral Health Services &
Research, 38(1), 80–90. doi:10.1007/s11414-009-9198-7
Köck, P., & Walter, M. (2018). Personality disorder and
substance use disorder—An update. Mental Health and
Prevention, 12, 82–89. doi:10.1016/j.mhp.2018.10.003
Kolbasovsky, A. (2009). Reducing 30-day inpatient
psychiatric recidivism and associated costs
through intensive case management. Professional
Case Management, 14(2), 96–105. doi:10.1097/
NCM.0b013e31819e026a
Kondo, K., Low, A., Jindai, K., Mendelson, A., Motu’apuaka,
M., Mansoor, D., . . . Hartung, D. (2015). Interventions
to improve pharmacological adherence among adults
with psychotic spectrum disorders, bipolar disorder,
and posttraumatic stress disorder (Vol. VA ESP Project
#05-225). Washington, DC: U.S. Department of Veterans
Affairs.
Konkoly Thege, B., Horwood, L., Slater, L., Tan, M. C.,
Hodgins, D. C., & Wild, T. C. (2017). Relationship
between interpersonal trauma exposure and addictive
behaviors: A systematic review. BMC Psychiatry, 17(1),
164. doi:10.1186/s12888-017-1323-1
Krasnova, A., Eaton, W. W., & Samuels, J. F. (2019).
Antisocial personality and risks of cause-specific
mortality: Results from the Epidemiologic Catchment
Area study with 27 years of follow-up. Social Psychiatry
Psychiatric Epidemiology, 54(5), 617–625. doi: 10.1007/
s00127-018-1628-5
Krawczyk, N., Feder, K. A., Saloner, B., Crum, R. M.,
Kealhofer, M., & Mojtabai, R. (2017). The association of
psychiatric comorbidity with treatment completion among
clients admitted to substance use treatment programs in
a U.S. national sample. Drug and Alcohol Dependence,
175, 157–163. doi:10.1016/j.drugalcdep.2017.02.006
Krebs, P., Norcross, J. C., Nicholson, J. M., & Prochaska,
J. O. (2018). Stages of change and psychotherapy
outcomes: A review and meta-analysis. Journal of Clinical
Psychology, 74(11), 1964–1979. doi:10.1002/jclp.22683
Kuerbis, A. N., Neighbors, C. J., & Morgenstern, J.
(2011). Depression’s moderation of the effectiveness of
intensive case management with substance-dependent
women on temporary assistance for needy families:
Outpatient substance use disorder treatment utilization
and outcomes. Journal of Studies on Alcohol and Drugs,
72(2), 297–307.
Kumar, G. S., & Klein, R. (2013). Effectiveness of case
management strategies in reducing emergency
department visits in frequent user patient populations: A
systematic review. Journal of Emergency Medicine, 44(3),
717–729. doi:10.1016/j.jemermed.2012.08.035
Kumar, N., Stowe, Z. N., Han, X., & Mancino, M. J. (2016).
Impact of early childhood trauma on retention and phase
advancement in an outpatient buprenorphine treatment
program. American Journal on Addictions, 25(7),
542–548. doi: 10.1111/ajad.12437.
Kuo, C., Schonbrun, Y. C., Zlotnick, C., Bates, N., Todorova,
R., Kao, J. C., & Johnson, J. (2013). A qualitative study
of treatment needs among pregnant and postpartum
women with substance use and depression. Substance
Use and Misuse, 48(14), 1498–1508. doi:10.3109/108260
84.2013.800116
Kupfer, D. J. (2015). Anxiety and DSM-5. Dialogues in
Clinical Neuroscience, 17(3), 245–246.
262 Appendix A

TIP 42Appendix A—Bibliography
Laakso, L. J. (2012). Motivational interviewing: Addressing
ambivalence to improve medication adherence in patients
with bipolar disorder. Issues in Mental Health Nursing,
33(1), 8–14. doi:10.3109/01612840.2011.618238
Lagisetty, P. A., Maust, D., Heisler, M., & Bohnert, A. (2017).
Physical and mental health comorbidities associated with
primary care visits for substance use disorders. Journal
of Addiction Medicine, 11(2), 161–162. doi:10.1097/
adm.0000000000000280
Lai, H. M., Cleary, M., Sitharthan, T., & Hunt, G. E. (2015).
Prevalence of comorbid substance use, anxiety and
mood disorders in epidemiological surveys, 1990–2014:
A systematic review and meta-analysis. Drug and
Alcohol Dependence, 154, 1–13. doi:10.1016/j.
drugalcdep.2015.05.031
Lally, J., & MacCabe, J. H. (2015). Antipsychotic medication
in schizophrenia: A review. British Medical Bulletin, 114(1),
169–179. doi:10.1093/bmb/ldv017
Lam, C. N., Arora, S., & Menchine, M. (2016). Increased
30-day emergency department revisits among homeless
patients with mental health conditions. Western Journal
of Emergency Medicine, 17(5), 607–612. doi:10.5811/
westjem.2016.6.30690
Lambert, M. J., & Simon, W. (2008). The therapeutic
relationship: Central and essential in psychotherapy
outcome. In S. F. Hick & T. Bien (Eds.), Mindfulness and
the therapeutic relationship (pp.19–33). New York, NY:
Guilford Press.
Lambert-Harris, C., Saunders, E. C., McGovern, M. P., & Xie,
H. (2013). Organizational capacity to address co-occurring
substance use and psychiatric disorders: Assessing
variation by level of care. Journal of Addiction Medicine,
7(1), 25–32. doi:10.1097/ADM.0b013e318276e7a4
Lamberti, J. S., Weisman, R. L., Cerulli, C., Williams, G.
C., Jacobowitz, D. B., Mueser, K. T., . . . Caine, E. D.
(2017). A randomized controlled trial of the Rochester
Forensic Assertive Community Treatment Model.
Psychiatric Services, 68(10), 1016–1024. doi:10.1176/appi.
ps.201600329
Landess, J., & Holoyda, B. (2017). Mental health courts
and forensic assertive community treatment teams as
correctional diversion programs. Behavioral Sciences and
the Law, 35(5–6), 501–511. doi:10.1002/bsl.2307
Lanier, D., & Ko, S. (2008). Screening in primary care
settings for illicit drug use: Assessment of screening
instruments—A supplemental evidence update for the
U.S. Preventive Services Task Force. Evidence Synthesis
No. 58, Part 2. AHRQ Publication No. 08-05108-EF-2.
Rockville, MD: Agency for Healthcare Research and
Quality.
Laschober, T. C., & Eby, L. T. (2013). Substance use disorder
counselors’ job performance and turnover after 1 year:
Linear or curvilinear relationship? Administration and
Policy in Mental Health and Mental Health Services
Research, 40(4), 300–310.
Lawson, K. M., Back, S. E., Hartwell, K. J., Moran-Santa
Maria, M., & Brady, K. T. (2013). A comparison of
trauma profiles among individuals with prescription
opioid, nicotine, or cocaine dependence.
American Journal of Addictions, 22(2), 127–131.
doi:10.1111/j.1521-0391.2013.00319.x
Lee King, P. A., Duan, L, & Amaro, H. (2015). Clinical needs
of in-treatment pregnant women with co-occurring
disorders: Implications for primary care. Maternal and
Child Health Journal, 19(1), 180–187. doi:10.1007/
s10995-014-1508-x
Lee, M. T., Acevedo, A., Garnick, D. W., Horgan, C. M.,
Panas, L., Ritter, G. A., & Campbell, K. M. (2018).
Impact of agency receipt of incentives and reminders on
engagement and continuity of care for clients with co-
occurring disorders. Psychiatric Services, 69(7), 804–811.
doi:10.1176/appi.ps.201700465
Lee, M. T., Horgan, C. M., Garnick, D. W., Acevedo,
A., Panas, L., Ritter, G. A., … Reynolds, M. (2014).
A performance measure for continuity of care after
detoxification: Relationship with outcomes. Journal of
Substance Abuse Treatment, 47(2), 130–139.
Lee, N. K., Cameron, J., & Jenner, L. (2015). A systematic
review of interventions for co-occurring substance use
and borderline personality disorders. Drug and Alcohol
Review, 34(6), 663–672. doi:10.1111/dar.12267
Lee, S. S., Humphreys, K. L., Flory, K., Liu, R., & Glass, K.
(2011). Prospective association of childhood attention-
deficit/hyperactivity disorder (ADHD) and substance
use and abuse/dependence: A meta-analytic review.
Clinical Psychology Review, 31(3), 328–341. doi:10.1016/j.
cpr.2011.01.006
LePage, J. P., Lewis, A. A., Crawford, A. M., Parish, J. A.,
Ottomanelli, L., Washington, E. L., & Cipher, D. J. (2016).
Incorporating individualized placement and support
principles into vocational rehabilitation for formerly
incarcerated veterans. Psychiatric Services, 67(7),
735–742. doi:10.1176/appi.ps.201500058
Lijffijt, M., Hu, K., & Swann, A. C. (2014). Stress modulates
illness-course of substance use disorders: A translational
review. Frontiers in Psychiatry, 5, 83. doi:10.3389/
fpsyt.2014.00083.
Lindsey, W. T., Stewart, D., & Childress, D. (2012).
Drug interactions between common illicit drugs and
prescription therapies. American Journal of Drug and
Alcohol Abuse, 38(4), 334–343. doi:10.3109/00952990.2
011.643997
Lo, C. C., Cheng, T. C., & de la Rosa, I. A. (2015).
Depression and substance use: A temporal-ordered
model. Substance Use & Misuse, 50(10), 1274–1283.
Lockwood, P. L. (2016). The anatomy of empathy:
Vicarious experience and disorders of social cognition.
Behavioural Brain Research, 311, 255–266. doi:10.1016/j.
bbr.2016.05.048
Appendix A 263

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
Lotito, M., & Cook, E. (2015). A review of suicide risk
assessment instruments and approaches. Mental Health
Clinician, 5(5), 216–223.
Lu, W., Yanos, P. T., Silverstein, S. M., Mueser, K. T.,
Rosenberg, S. D., Gottlieb, J. D., . . . Giacobbe, G. (2013).
Public mental health clients with severe mental illness and
probable posttraumatic stress disorder: Trauma exposure
and correlates of symptom severity. Journal of Traumatic
Stress, 26(2), 266–273. doi:10.1002/jts.21791
Lucas, C., & Martin, J. (2013). Smoking and drug
interactions. Australian Prescriber, 36, 102–104.
Luciano, A., Belstock, J., Malmberg, P., McHugo, G. J.,
Drake, R. E., Xie, H., . . . Covell, N. H. (2014). Predictors
of incarceration among urban adults with co-occurring
severe mental illness and a substance use disorder.
Psychiatric Services, 65(11), 1325–1331. doi:10.1176/appi.
ps.201300408
Luciano, A., Bryan, E. L., Carpenter-Song, E. A., Woods, M.,
Armstrong, K., & Drake, R. E. (2014). Long-term sobriety
strategies for men with co-occurring disorders. Journal of
Dual Diagnosis, 10(4), 212–219. doi:10.1080/15504263.2
014.961884
Luciano, A., & Carpenter-Song, E. A. (2014). A qualitative
study of career exploration among young adult
men with psychosis and co-occurring substance use
disorder. Journal of Dual Diagnosis, 10(4), 220–225.
doi:10.1080/15504263
Lugoboni, F., Levin, F. R., Pieri, M. C., Manfredini,
M., Zamboni, L., Somaini, L., . . . Gruppo InterSert
Collaborazione, S. (2017). Co-occurring attention deficit
hyperactivity disorder symptoms in adults affected
by heroin dependence: Patients characteristics and
treatment needs. Psychiatry Research, 250, 210–216.
doi:10.1016/j.psychres.2017.01.052
Luo, S. X., & Levin, F. R. (2017). Towards precision addiction
treatment: New findings in co-morbid substance
use and attention-deficit hyperactivity disorders.
Current Psychiatry Reports, 19(3), 14. doi:10.1007/
s11920-017-0769-7
Lusk, S. L., Koch, L. C., & Paul, T. M. (2016). Recovery-
oriented vocational rehabilitation services for individuals
with co-occurring psychiatric disabilities and substance
use disorders. Rehabilitation Research, Policy, and
Education, 30(3), 243–258.
Lutterman, T., Shaw, R., Fisher, W., & Manderscheid, R.
(2017, August). Trend in psychiatric inpatient capacity,
United States and each state, 1970 to 2014. Retrieved
from www.nri-inc.org/media/1319/tac-paper-10-
psychiatric-inpatient-capacity-final-09-05-2017.pdf
Lydecker, K. P., Tate, S. R., Cummins, K. M., McQuaid, J.,
Granholm, E., & Brown, S. A. (2010). Clinical outcomes
of an integrated treatment for depression and substance
use disorders. Psychology of Addictive Behaviors, 24(3),
453–465. doi:10.1037/a0019943
Ma, M., Coles, A. S., & George, T. P. (2018, September 27).
Understanding and treating co-occurring bipolar disorder
and substance use disorders. Psychiatric Times. Retrieved
from www.psychiatrictimes.com/bipolar-disorder/
understanding-and-treating-co-occurring-bipolar-
disorder-and-substance-use-disorders
Macy, R. J., Renz, C., & Pelino, E. (2013). Partner
violence and substance abuse are intertwined:
Women’s perceptions of violence-substance
connections. Violence Against Women, 19(7), 881–902.
doi:10.1177/1077801213498208
Magidson, J. F., Liu, S.-M., Lejuez, C. W., & Blanco, C.
(2012). Comparison of the course of substance use
disorders among individuals with and without generalized
anxiety disorder in a nationally representative sample.
Journal of Psychiatric Research, 46(5), 659–666.
doi:10.1016/j.jpsychires.2012.02.011
Magor-Blatch, L., Bhullar, N., Thomson, B., & Thorsteinsson,
E. (2014). A systematic review of studies examining
effectiveness of therapeutic communities. Therapeutic
Communities, 35(4), 168–184. doi:10.1108/
TC-07-2013-0024
Maisto, S. A., Roos, C. R., O’Sickey, A. J., Kirouac, M.,
Connors, G. J., Tonigan, J. S., & Witkiewitz, K. (2015).
The indirect effect of the therapeutic alliance and alcohol
abstinence self-efficacy on alcohol use and alcohol-
related problems in Project MATCH. Alcoholism: Clinical
and Experimental Research, 39(3), 504–513. doi:10.1111/
acer.12649
Malivert, M., Fatséas, M., Denis, C., Langlois, E., &
Auriacombe, M. (2012). Effectiveness of therapeutic
communities: A systematic review. European Addiction
Research, 18(1), 1–11. doi:10.1159/000331007
Malte, C. A., Cox, K., & Saxon, A. J. (2017). Providing
intensive addiction/housing case management to
homeless veterans enrolled in addictions treatment: A
randomized controlled trial. Psychology of Addictive
Behaviors, 31(3), 231–241. doi:10.1037/adb0000273
Mandavia, A., Robinson, G. G., Bradley, B., Ressler, K. J., &
Powers, A. (2016). Exposure to childhood abuse and later
substance use: Indirect effects of emotion dysregulation
and exposure to trauma. Journal of Traumatic Stress,
29(5), 422–429. doi:10.1002/jts.22131
Mangrum, L. F. (2009). Client and service characteristics
associated with addiction treatment completion of clients
with co-occurring disorders. Addictive Behaviors, 34(10),
898–904. doi:10.1016/j.addbeh.2009.03.006
Mansfield, A. J., Greenbaum, M. A., Schaper, K. M.,
Banducci, A. N., & Rosen, C. S. (2017). PTSD care among
veterans with and without co-occurring substance
use disorders. Psychiatric Services, 68(6), 632–635.
doi:10.1176/appi.ps.201600128
264 Appendix A

TIP 42
Appendix A—Bibliography
Manuel, J. I., Covell, N. H., Jackson, C. T., & Essock, S. M.
(2011). Does assertive community treatment increase
medication adherence for people with co-occurring
psychotic and substance use disorders? Journal of the
American Psychiatric Nurses Association, 17(1), 51–56.
doi:10.1177/1078390310395586
Markota, M., Rummans, T. A., Bostwick, J. M., & Lapid,
M. I. (2016). Benzodiazepine use in older adults:
Dangers, management, and alternative therapies. Mayo
Clinic Proceedings, 91(11), 1632–1639. doi:10.1016/j.
mayocp.2016.07.024
Marlatt, G. A. (1985). Relapse prevention: Theoretical
rationale and overview of the model. In G. A. Marlatt &
J. R. Gordon (Eds.), Relapse prevention: Maintenance
strategies in the treatment of addictive behaviors (1st ed.,
pp. 3–70). New York: Guilford Press.
Marlatt, G. A., & Gordon, J. R. (Eds.). (1985). Relapse
prevention: Maintenance strategies in the treatment of
addictive behaviors. New York: Guilford Press.
Marmar, C. R., Schlenger, W., Henn-Haase, C., Qian, M.,
Purchia, E., Li, M., . . . Kulka, R. A. (2015). Course of
posttraumatic stress disorder 40 years after the Vietnam
War: Findings from the National Vietnam Veterans
Longitudinal Study. JAMA Psychiatry, 72(9), 875–881.
doi:10.1001/jamapsychiatry.2015.0803
Marmorstein, N. R. (2012). Anxiety disorders and substance
use disorders: Different associations by anxiety disorder.
Journal of Anxiety Disorders, 26(1), 88–94. doi:10.1016/j.
janxdis.2011.09.005
Marotta, P. L. (2017). Childhood adversities and substance
misuse among the incarcerated: Implications for
treatment and practice in correctional settings. Substance
Use and Misuse, 52(6), 717–733. doi:10.1080/10826084.2
016.1261899
Marquant, T., Sabbe, B., Van Nuffel, M., & Goethals, K.
(2016). Forensic assertive community treatment: A review
of the literature. Community Mental Health Journal, 52(8),
873–881.
Marshall, T., Goldberg, R. W., Braude, L., Dougherty, R. H.,
Daniels, A. S., Ghose, S. S., … Delphin-Rittmon, M. E.
(2014). Supported employment: Assessing the evidence.
Psychiatric Services, 65(1), 16–23. doi:10.1176/appi.
ps.2013.00262
Martinez-Raga, J., Szerman, N., Knecht, C., & de Alvaro, R.
(2013). Attention deficit hyperactivity disorder and dual
disorders. Educational needs for an underdiagnosed
condition. International Journal of Adolescent Medicine
and Health, 25(3), 231–243. doi:10.1515/ijamh-2013-0057
Martínez-Vispo, C., Martínez, López-Durán, A., Fernández
del Río, E., & Becoña, E. (2018). Effects of behavioural
activation on substance use and depression: A systematic
review. Substance Abuse: Treatment, Prevention, and
Policy, 13(1), 36. doi:10.1186/s13011-018-0173-2
Martino, S., Carroll, K. M., Nich, C., & Rounsaville, B.
J. (2006). A randomized controlled pilot study of
motivational interviewing for patients with psychotic
and drug use disorders. Addiction, 101(10), 1479–1492.
doi:10.1111/j.1360-0443.2006.01554.x
Martins, S. S., & Gorelick, D. A. (2011). Conditional
substance abuse and dependence by diagnosis of
mood or anxiety disorder or schizophrenia in the U.S.
population. Drug and Alcohol Dependence, 119(1–2),
28–36. doi:10.1016/j.drugalcdep.2011.05.010
Mason, R., & Du Mont, J. (2015). Advancing our knowledge
of the complexity and management of intimate partner
violence and co-occurring mental health and substance
abuse problems in women. F1000 Prime Reports, 7, 65.
doi:10.12703/P7-65
Masson, C. L., Shopshire, M. S., Sen, S., Hoffman, K. A.,
Hengl, N. S., Bartolome, J., . . . Iguchi, M. Y. (2013).
Possible barriers to enrollment in substance abuse
treatment among a diverse sample of Asian Americans
and Pacific Islanders: Opinions of treatment clients.
Journal of Substance Abuse Treatment, 44(3), 309–315.
doi:10.1016/j.jsat.2012.08.005
Matusow, H., Guarino, H., Rosenblum, A., Vogel, H.,
Uttaro, T., Khabir, S., . . . Magura, S. (2013). Consumers’
experiences in dual focus mutual aid for co-occurring
substance use and mental health disorders. Substance
Abuse: Research and Treatment, 7, 39–47. doi:10.4137/
SART.S11006
Maura, J., & Weisman de Mamani, A. (2017). Mental health
disparities, treatment engagement, and attrition among
racial/ethnic minorities with severe mental illness: A
review. Journal of Clinical Psychology in Medical Settings,
24(3–4), 187–210. doi:10.1007/s10880-017-9510-2
Mauritz, M. W., Goossens, P. J., Draijer, N., & van
Achterberg, T. (2013). Prevalence of interpersonal trauma
exposure and trauma-related disorders in severe mental
illness. European Journal of Psychotraumatology, 4.
Published online. doi:10.3402/ejpt.v4i0.19985
McCabe, S. E., West, B. T., Jutkiewicz, E. M., & Boyd, C.
J. (2017). Multiple DSM-5 substance use disorders: A
national study of US adults. Human Psychopharmacology,
32(5). doi:10.1002/hup.2625
McCallum, S., Mikocka-Walus, A., Turnbull, D., & Andrews,
J. M. (2015). Continuity of care in dual diagnosis
treatment: Definitions, applications, and implications.
Journal of Dual Diagnosis, 11(3–4), 217–232. doi:10.1080/
15504263.2015.1104930
McCance-Katz, E. F. (2019). The National Survey on Drug
Use and Health: 2018. Slide Presentation. Retrieved from
https://www.samhsa.gov/data/sites/default/files/cbhsq-
reports/Assistant-Secretary-nsduh2018_presentation.pdf
Appendix A 265

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
McCarty, D., Braude, L., Lyman, D. R., Dougherty, R. H.,
Daniels, A. S., Ghose, S. S., & Delphin-Rittmon, M. E.
(2014). Substance abuse intensive outpatient programs:
Assessing the evidence. Psychiatric Services, 65(6),
718–726.
McCauley, J. L., Killeen, T., Gros, D. F., Brady, K. T., &
Back, S. E. (2012). Posttraumatic stress disorder and
co-occurring substance use disorders: Advances in
assessment and treatment. Clinical Psychology: Science
and Practice, 19(3), 283–304. doi:10.1111/cpsp.12006
McCloskey, M. S., & Ammerman, B. A. (2018). Suicidal
behavior and aggression-related disorders. Current
Opinion in Psychology, 22, 54–58. doi:10.1016/j.
copsyc.2017.08.010
McConnaughy, E. A., Prochaska, J., & Velicer, W. F. (1983).
Stages of change in psychotherapy: Measurement and
sample profiles. Psychotherapy: Theory, Research, and
Practice, 20(3), 368–375.
McDermid, J., Sareen, J., El-Gabalawy, R., Pagura, J.,
Spiwak, R., & Enns, M. W. (2015). Co-morbidity of bipolar
disorder and borderline personality disorder: Findings
from the National Epidemiologic Survey on Alcohol
and Related Conditions. Comprehensive Psychiatry, 58,
18–28. doi:10.1016/j.comppsych.2015.01.004
McDermott, K. W., Elixhauser, A., & Sun, R. (2017, June).
Trends in hospital inpatient stays in the United States,
2005–2014. HCUP Statistical Brief #225. Agency
for Healthcare Research and Quality, Rockville, MD.
Retrieved from www.hcup-us.ahrq.gov/reports/statbriefs/
sb225-Inpatient-US-Stays-Trends.pdf
McDonald, D., & Arlinghaus, S. L. (2014). The role of
intensive case management services in reentry: The
northern Kentucky female offender reentry project.
Women and Criminal Justice, 24(3), 229–251. doi:10.1080
/08974454.2014.909759
McDonell, M. G., Kerbrat, A. H., Comtois, K. A., Russo,
J., Lowe, J. M., & Ries, R. K. (2012). Validation of the
co-occurring disorder quadrant model. Journal of
Psychoactive Drugs, 44(3), 266–273. doi:10.1080/027910
72.2012.705065
McDonell, M. G., Srebnik, D., Angelo, F., McPherson, S.,
Lowe, J. M., Sugar, A., . . . Ries, R. K. (2013). Randomized
controlled trial of contingency management for stimulant
use in community mental health patients with serious
mental illness. American Journal of Psychiatry, 170(1),
94–101. doi:10.1176/appi.ajp.2012.11121831
McGovern, M. P., Clark, R. E., & Samnaliev, M. (2007).
Co-occurring psychiatric and substance use disorders:
A multistate feasibility study of the quadrant model.
Psychiatric Services, 58(7), 949–954. doi:10.1176/
ps.2007.58.7.949
McGovern, M. P., Lambert-Harris C., Alterman A. I., Xie,
H., & Meier, A. (2011). A randomized controlled trial
comparing integrated cognitive behavioral therapy
versus individual addiction counseling for co-occurring
substance use and posttraumatic stress disorders. Journal
of Dual Diagnosis, 7(4), 207–227.
McGovern, M. P., Lambert-Harris, C., Gotham, H. J., Claus,
R. E., & Xie, H. (2014). Dual diagnosis capability in mental
health and addiction treatment services: An assessment
of programs across multiple state systems. Administration
and Policy in Mental Health, 41(2), 205–214. doi:10.1007/
s10488-012-0449-1
McGovern, M. P., Lambert-Harris, C., Xie, H., Meier, A.,
McLeman, B., & Saunders, E. (2015). A randomized
controlled trial of treatments for co-occurring substance
use disorders and post-traumatic stress disorder.
Addiction, 110(7), 1194–1204. doi:10.1111/add.12943
McGovern, M. P., Saunders, E. C., & Kim, E. (2013).
Substance abuse treatment implementation research.
Journal of Substance Abuse Treatment, 44(1), 1–3.
doi:10.1016/j.jsat.2012.09.006
McGrath, J., Saha, S., Welham, J., El Saadi, O., MacCauley,
C., & Chant, D. (2004). A systematic review of the
incidence of schizophrenia: The distribution of
rates and the influence of sex, urbanicity, migrant
status and methodology. BMC Medicine, 2, 13.
doi:10.1186/1741-7015-2-13
McHugh, R. K. (2015). Treatment of co-occurring anxiety
disorders and substance use disorders. Harvard
Review of Psychiatry, 23(2), 99–111. doi:10.1097/
HRP.0000000000000058
McHugh, R. K., Gratz, K. L., & Tull, M. T. (2017). The role
of anxiety sensitivity in reactivity to trauma cues in
treatment-seeking adults with substance use disorders.
Comprehensive Psychiatry, 78, 107–114. doi:10.1016/j.
comppsych.2017.07.011
McHugh, R. K., Votaw, V. R., Sugarman, D. E., & Greenfield,
S. F. (2018). Sex and gender differences in substance
use disorders. Clinical Psychology Review, 12–23.
doi:10.1016/j.cpr.2017.10.012
McHugo, G. J., Drake, R. E., Burton, H. L., & Ackerson, T. H.
(1995). A scale for assessing the stage of substance abuse
treatment in persons with severe mental illness. Journal of
Nervous and Mental Disease, 183(12), 762–767.
McHugo, G. J., Drake, R. E., Xie, H., & Bond, G. R. (2012). A
10-year study of steady employment and non-vocational
outcomes among people with serious mental illness and
co-occurring substance use disorders. Schizophrenia
Research, 138(2–3), 233–239. doi:10.1016/j.
schres.2012.04.007
McKay J. R. (2009). Continuing care research: What we have
learned and where we are going. Journal of Substance
Abuse Treatment, 36(2), 131–145.
McKay, J. R., Knepper, C., Deneke, E., O’Reilly, C.,
& DuPont, R. L. (2016). An initial evaluation of a
comprehensive continuing care intervention for clients
with substance use disorders: My first year of recovery
(MyFYR). Journal of Substance Abuse Treatment, 67,
50–54. doi:10.1016/j.jsat.2016.04.003
266 Appendix A

TIP 42Appendix A—Bibliography
McKee, S. A., Harris, G. T., & Cormier, C. A. (2013).
Implementing residential integrated treatment for
co-occurring disorders. Journal of Dual Diagnosis, 9(3),
249–259.
McKenzie, K., & Chang, Y. P. (2015). The effect of nurse-led
motivational interviewing on medication adherence in
patients with bipolar disorder. Perspectives in Psychiatric
Care, 51(1), 36–44. doi:10.1111/ppc.12060
McKeown, R. E., Holbrook, J. R., Danielson, M. L., Cuffe,
S. P., Wolraich, M. L., & Visser, S. N. (2015). The impact
of case definition on attention-deficit/hyperactivity
disorder prevalence estimates in community-based
samples of school-aged children. Journal of the American
Academy of Child Adolescent Psychiatry, 54(1), 53–61.
doi:10.1016/j.jaac.2014.10.014
McKetin, R., Voce, A., Burns, R., Ali, R., Lubman, D. I., Baker,
A. L., & Castle, D. J. (2018). Latent psychotic symptom
profiles amongst people who use methamphetamine:
What do they tell us about existing diagnostic
categories? Frontiers in Psychiatry, 9, 578. doi:10.3389/
fpsyt.2018.00578
McKinney, J. M., Hirsch, J. K., & Britton, P. C. (2017). PTSD
symptoms and suicide risk in veterans: Serial indirect
effects via depression and anger. Journal of Affective
Disorders, 214, 100–107. doi:10.1016/j.jad.2017.03.008
McLellan, A. T., Kushner, H., Metzger, D., Peters, R., Smith,
I., Grissom, G., . . . Argeriou, M. (1992). The fifth edition
of the Addiction Severity Index. Journal of Substance
Abuse Treatment, 9(3), 199–213.
Mdege, N. D., & Lang, J. (2011). Screening instruments
for detecting illicit drug use/abuse that could be
useful in general hospital wards: A systematic review.
Addictive Behaviors, 36(12), 1111–1119. doi:10.1016/j.
addbeh.2011.07.007
Mee-Lee, D., Shulman, G. D., Fishman, M. J., Gastfriend,
D. R., & Miller, M. M. (Eds.). (2013).The ASAM criteria:
Treatment for addictive, substance-related, and co-
occurring conditions(3rd ed.). Carson City, NV: The
Change Companies.
Meier, A., McGovern, M. P., Lambert-Harris, C.,
McLeman, B., Franklin, A., Saunders, E. C., & Xie, H.
(2015). Adherence and competence in two manual-
guided therapies for co-occurring substance use and
posttraumatic stress disorders: Clinician factors and
patient outcomes. American Journal of Drug and Alcohol
Abuse, 41(6), 527–534. doi:10.3109/00952990.2015.106
2894
Meier, P. S., & Barrowclough, C. (2009). Mental health
problems: Are they or are they not a risk factor for
dropout from drug treatment? A systematic review of the
evidence. Drugs: Education, Prevention and Policy, 16(1),
7–38. doi:10.1080/09687630701741030
Melemis, S. M. (2015). Relapse prevention and the five rules
of recovery. Yale Journal of Biology and Medicine, 88(3),
325–332.
Mentalhelp.Net. (2019a). Mental Health,
Dual-Diagnosis, & Behavioral Addictions.
Retrieved from www.mentalhelp.net/articles/
behavioral-addictions-mental-health-dual-diagnosis/
MentalHelp.Net. (2019b). Schizophrenia. Retrieved from
www.mentalhelp.net/articles/schizophrenia/
Mericle, A. A., Ta Park, V. M., Holck, P., & Arria, A.
M. (2012). Prevalence, patterns, and correlates of
co-occurring substance use and mental disorders
in the United States: Variations by race/ethnicity.
Comprehensive Psychiatry, 53(6), 657–665. doi:10.1016/j.
comppsych.2011.10.002
Merrick, M. T., Ports, K. A., Ford, D. C., Afifi, T. O., Gershoff,
E. T., & Grogan-Kaylor, A. (2017). Unpacking the impact
of adverse childhood experiences on adult mental health.
Child Abuse and Neglect, 69, 10–19. doi:10.1016/j.
chiabu.2017.03.016
Meyer, R. E., Salzman, C., Youngstrom, E. A., Clayton, P. J.,
Goodwin, F. K., Mann, J. J., . . . Sheehan, D. V. (2010).
Suicidality and risk of suicide—Definition, drug safety
concerns, and a necessary target for drug development:
A consensus statement. Journal of Clinical Psychiatry,
71(8), e1–e21. doi:10.4088/JCP.10cs06070blu
Miller, J. M., & Khey, D. N. (2016). An implementation and
process evaluation of the Louisiana 22nd judicial district’s
behavioral health court. American Journal of Criminal
Justice, 41(1). doi:10.1007/s12103-015-9326-2
Miller, W. R., & Rollnick, S. (2013). Motivational interviewing:
Helping people change (3rd ed.). New York: Guilford
Press.
Miller, W. R., & Tonigan, J. S. (1996). Assessing drinkers’
motivation for change: The Stages of Change
Readiness and Treatment Eagerness Scale (SOCRATES).
Psychology of Addictive Behaviors, 10(2), 81–89.
doi:10.1037/0893-164X.10.2.81
Minassian, A., Vilke, G. M., & Wilson, M. P. (2013). Frequent
emergency department visits are more prevalent in
psychiatric, alcohol abuse, and dual diagnosis conditions
than in chronic viral illnesses such as hepatitis and human
immunodeficiency virus. Journal of Emergency Medicine,
45(4), 520–525. doi:10.1016/j.jemermed.2013.05.007
Minkoff, K. (1989). An integrated treatment model for
dual diagnosis of psychosis and addiction. Hospital and
Community Psychiatry, 40(10), 1031–1036.
Minnich, A., Erford, B. T., Bardhoshi, G., & Atalay, Z. (2018).
Systematic review of the Michigan Alcoholism Screening
Test. Journal of Counseling and Development, 96(3),
335–344. doi:10.1002/jcad.12207
Mitchell, F. M. (2015). Racial and ethnic health disparities
in an era of health care reform. Health and Social Work,
40(3), e66–e74. doi:10.1093/hsw/hlv038
Appendix A 267

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
Mitchell, M. S., Leon, C. L. K., Byrne, T. H., Lin, W. C., &
Bharel, M. (2017). Cost of health care utilization among
homeless frequent emergency department users.
Psychological Services, 14(2), 193–202. doi:10.1037/
ser0000113
Mohamed, S. (2013). Dual diagnosis among intensive
case management participants in the Veterans Health
Administration: Correlates and outcomes. Journal of Dual
Diagnosis, 9(4), 311–321. doi:10.1080/15504263.2013.8
35162
Molina, B. S. G., Howard, A. L., Swanson, J. M., Stehli,
A., Mitchell, J. T., Kennedy, T. M., … Hoza, B. (2018).
Substance use through adolescence into early adulthood
after childhood-diagnosed ADHD: Findings from the
MTA longitudinal study. Journal of Child Psychology and
Psychiatry, 59(6), 692–702. doi:10.1111/jcpp.12855
Monica, C., Nikkel, R. E., & Drake, R. E. (2010). Dual
Diagnosis Anonymous of Oregon. Psychiatric Services,
61, 738–740.
Moore, K. A., Young, M. S., Barrett, B., & Ochshorn, E.
(2009). A 12-month follow-up evaluation of integrated
treatment for homeless individuals with co-occurring
disorders. Journal of Social Service Research, 35(4),
322–335. doi:10.1080/01488370903110829
Morgan, O., Kuramoto, F., Emmet, W., Stange, J. L., &
Nobunaga, E. (2014). The impact of the Affordable
Care Act on behavioral health care for individuals from
racial and ethnic communities. Journal of Social Work in
Disability and Rehabilitation, 13(1–2), 139–161. doi:10.10
80/1536710X.2013.870518
Morgenstern, J., Neighbors, C. J., Kuerbis, A., Riordan,
A., Blanchard, K. A., McVeigh, K. H., . . . McCrady, B.
(2009). Improving 24-month abstinence and employment
outcomes for substance-dependent women receiving
temporary assistance for needy families with intensive
case management. American Journal of Public Health,
99(2), 328–333. doi:10.2105/ajph.2007.133553
Morisano, D., Babor, T. F., & Robaina, K. A. (2014).
Co-occurrence of substance use disorders with other
psychiatric disorders: Implications for treatment services.
Nordic Studies on Alcohol and Drugs, 31(1), 5–25.
Morrens, M., Dewilde, B., Sabbe, B., Dom, G., De
Cuyper, R., & Moggi, F. (2011). Treatment outcomes
of an integrated residential programme for patients
with schizophrenia and substance use disorder.
European Addiction Research, 17(3), 154–163.
doi:10.1159/000324480
Morse, G., Salyers, M. P., Rollins, A. L., Monroe-DeVita, M.,
& Pfahler, C. (2012). Burnout in mental health services: A
review of the problem and its remediation. Administration
and Policy in Mental Health, 39(5), 341–352. doi:10.1007/
s10488-011-0352-1
Morse, G. A., York, M. M., Dell, N., Blanco, J., & Birchmier,
C. (2017). Improving outcomes for homeless people with
alcohol disorders: A multi-program community-based
approach. Journal of Mental Health, 1–8. doi:10.1080/096
38237.2017.1340617
Morse, S., & Bride, B. E. (2017). Decrease in healthcare
utilization and costs for opioid users following
residential integrated treatment for co-occurring
disorders. Healthcare (Basel), 5(3), 54. doi:10.3390/
healthcare5030054
Morse, S. A., Watson, C., MacMaster, S. A., & Bride, B. E.
(2015). Differences between older and younger adults in
residential treatment for co-occurring disorders. Journal
of Dual Diagnosis, 11(1), 75–82. doi:10.1080/15504263.2
014.993263
Moulin, A., Evans, E. J., Xing, G., & Melnikow, J.
(2018). Substance use, homelessness, mental
illness and Medicaid coverage: A set-up for high
emergency department utilization. Western Journal
of Emergency Medicine, 19(6), 902–906. doi:10.5811/
westjem.2018.9.38954
Mueser, K. T., Campbell, K., & Drake, R. E. (2011). The
effectiveness of supported employment in people with
dual disorders. Journal of Dual Diagnosis, 7(1–2), 90–102.
Mueser, K. T., & Gingerich, S. (2013). Treatment of co-
occurring psychotic and substance use disorders. Social
Work in Public Health, 28(3–4), 424–439. doi:10.1080/193
71918.2013.774676
Muhuri, P. K., & Gfroerer, J. C. (2009). Substance use among
women: Associations with pregnancy, parenting, and
race/ethnicity. Maternal and Child Health Journal, 13(3),
376–385. doi:10.1007/s10995-008-0375-8
Mundon, C. R., Anderson, M. L., & Najavits, L. M. (2015).
Attitudes toward substance abuse clients: An empirical
study of clinical psychology trainees. Journal of
Psychoactive Drugs, 47(4), 293–300. doi:10.1080/027910
72.2015.1076090
Munn-Chernoff, M. A., & Baker, J. H. (2016). A primer on
the genetics of comorbid eating disorders and substance
use disorders. European Eating Disorders Review, 24(2),
91–100. doi:10.1002/erv.2424
Munn-Chernoff, M. A., Grant, J. D., Agrawal, A., Sartor,
C. E., Werner, K. B., Bucholz, K. K., . . . Duncan, A. E.
(2015). Genetic overlap between alcohol use disorder
and bulimic behaviors in European American and African
American women. Drug and Alcohol Dependence, 153,
335–340. doi:10.1016/j.drugalcdep.2015.05.043
Nam, E., Matejkowski, J., & Lee, S. (2017). Racial/ethnic
differences in contemporaneous use of mental health and
substance use treatment among individuals experiencing
both mental illness and substance use disorders.
Psychiatric Quarterly, 88(1), 185–198. doi:10.1007/
s11126-016-9444-0
268 Appendix A

TIP 42Appendix A—Bibliography
Nanni, V., Uher, R., & Danese, A. (2012). Childhood
maltreatment predicts unfavorable course of illness
and treatment outcome in depression: A meta-analysis.
American Journal of Psychiatry, 169(2), 141–151.
National Academies of Sciences, Engineering, and
Medicine. (2016). Part 3: Instruments available for
measuring specific mental illness diagnoses with
functional impairment. In Measuring specific mental
illness diagnoses with functional impairment: Workshop
summary. Washington, DC: National Academies Press.
National Association of State Mental Health Program
Directors (NASMHPD). (June 2012). Fact sheet on
accelerating integration of primary care, behavioral
health and prevention: The SBHA role. Retrieved from
www.nasmhpd.org/sites/default/files/Behavioral%20
Health%20Primary_Fact%20Sheet%20Accelerating%20
Integration%20of%20Primary%20Care.pdf
National Association of State Mental Health Program
Directors, & National Association of State Alcohol
and Drug Abuse Directors (NASADAD). (March 1999).
National dialogue on co-occurring mental health and
substance abuse disorders. Retrieved fromhttp://
nasadad.org/2015/03/national-dialogue-on-co-occurring-
mental-health-and-substance-abuse-disorders/
National Institute of Mental Health (NIMH). (n.d.). Ask
Suicide-Screening Questions (ASQ) Toolkit. Retrieved
from https://www.nimh.nih.gov/research/research-
conducted-at-nimh/asq-toolkit-materials/index.shtml
National Institute of Mental Health. (2016, February).
Schizophrenia. Retrieved from www.nimh.nih.gov/health/
topics/schizophrenia/index.shtml
National Institute of Mental Health. (2016, October). Mental
health medications: Overview. Retrieved from www.nimh.
nih.gov/health/topics/mental-health-medications/index.
shtml
National Institute of Mental Health. (2017, November).
Attention-deficit/hyperactivity disorder (ADHD). Retrieved
from www.nimh.nih.gov/health/statistics/attention-deficit-
hyperactivity-disorder-adhd.shtml - part_154905
National Institute of Mental Health. (2019). Suicide.
Retrieved from www.nimh.nih.gov/health/statistics/
suicide.shtml
National Institute on Alcohol Abuse and Alcoholism.
(n.d.). Drinking levels defined. Retrieved from
https://www.niaaa.nih.gov/alcohol-health/
overview-alcohol-consumption/moderate-binge-drinking
National Institute on Drug Abuse. (2012a). Adoption
of NIDA’s evidence-based treatments in real world
settings—A National Advisory Council on Drug Abuse
Workgroup report. Retrieved from www.drugabuse.gov/
sites/default/files/files/evidence-based_treatments_in_
real_world_settings_workgroup_report.pdf
National Institute on Drug Abuse. (2012b).
Resource guide: Screening for drug use in
general medical settings. Retrieved from www.
drugabuse.gov/publications/resource-guide-
screening-drug-use-in-general-medical-settings/
nida-quick-screen
National Institute on Drug Abuse. (2015, July). How
are therapeutic communities adapting to the current
environment? Retrieved from www.drugabuse.gov/
publications/research-reports/therapeutic-communities/
how-are-therapeutic-communities-adapting-to-current-
environment
National Institute on Drug Abuse. (2018a). Common
comorbidities with substance use disorders. Retrieved
from https://d14rmgtrwzf5a.cloudfront.net/sites/default/
files/1155-common-comorbidities-with-substance-use-
disorders.pdf
National Institute on Drug Abuse. (2018b). Principles of
drug addiction treatment: A research-based guide (3rd
ed.). Rockville, MD: National Institute on Drug Abuse,
National Institutes of Health, U.S. Department of Health
and Human Services.
National Institute on Drug Abuse. (2018c). Treatment and
recovery. In Drugs, brains, and behavior: The science of
addiction (pp. 22–25). Bethesda, MD: National Institute
on Drug Abuse.
National Institute on Drug Abuse. (2018d, July). Sex and
gender differences in substance use disorder treatment.
Retrieved fromwww.drugabuse.gov/publications/
research-reports/substance-use-in-women/sex-gender-
differences-in-substance-use-disorder-treatment
National Institute on Drug Abuse. (Revised March
2018). Benzodiazepines and opioids. Retrieved
from www.drugabuse.gov/drugs-abuse/opioids/
benzodiazepines-opioids
Neumiller, S., Bennett-Clark, F., Young, M. S., Dates,
B., Broner, N., Leddy, J., . . . De Jong, F. (2009).
Implementing assertive community treatment in diverse
settings for people who are homeless with co-occurring
mental and addictive disorders: A series of case
studies. Journal of Dual Diagnosis, 5(3–4), 239–263.
doi:10.1080/15504260903175973
Newell, J. M., Nelson-Gardell, D., & MacNeil, G. (2016).
Clinician responses to client traumas: A chronological
review of constructs and terminology. Trauma, Violence,
& Abuse, 17(3), 306–13. doi: 10.1177/1524838015584365
Newton-Howes, G., & Foulds, J. (2018). Personality
disorder and treatment outcome in alcohol use disorder.
Current Opinion in Psychiatry, 31(1), 50–56. doi:10.1097/
YCO.0000000000000375
Nicosia, N., Macdonald, J. M., & Arkes, J. (2013). Disparities
in criminal court referrals to drug treatment and prison for
minority men. American Journal of Public Health, 103(6),
e77–e84. doi:10.2105/ajph.2013.301222
Appendix A 269

TIP 42 Substance Use Disorder Treatment for People With Co-Occurring Disorders
Noel, V., Woods, M., Routhier, J., & Drake, R. (2016).
Planning treatment and assessing recovery in participants
with dual diagnosis: Preliminary evaluation of a new
clinical tool. Journal of Dual Diagnosis, 12(1), 55–62. doi:1
0.1080/15504263.2016.1146555
Norman, R. E., Byambaa, M., De, R., Butchart, A., Scott,
J., & Vos, T. (2012). The long-term health consequences
of child physical abuse, emotional abuse, and neglect:
A systematic review and meta-analysis. PLoS Medicine,
9(11), e1001349. doi:10.1371/journal.pmed.1001349
Nowotny, K. M. (2015). Race/ethnic disparities in the
utilization of treatment for drug dependent inmates in
U.S. state correctional facilities. Addictive Behaviors, 40,
148–153. doi:10.1016/j.addbeh.2014.09.005
O’Connell, M., Kasprow, W., & Rosenheck, R. A. (2010).
National dissemination of supported housing in the
VA: Model adherence versus model modification.
Psychiatric Rehabilitation Journal, 33(4), 308–319.
doi:10.2975/33.4.2010.308.319
O’Connell, M. J., Flanagan, E. H., Delphin-Rittmon, M. E., &
Davidson, L. (2017). Enhancing outcomes for persons with
co-occurring disorders through skills training and peer
recovery support. Journal of Mental Health, 1–6. doi:10.1
080/09638237.2017.1294733
O’Connor, R., & Pirkis, J. (2016). The international
handbook of suicide prevention (2nd ed.). Chichester, UK:
Wiley Blackwell.
O’Grady, M. A., Kapoor, S., Kwon, N., Morley, J.,
Auerbach, M., Neighbors, C. J., . . . Morgenstern, J.
(2019). Substance use screening and brief intervention:
Evaluation of patient and implementation differences
between primary care and emergency department
settings. Journal of Evaluation in Clinical Practice 25(3),
441–447. doi:10.1111/jep.13060
O’Grady, M. A., Neighbors, C. J., Lincourt, P., Burke, C.,
& Maldonado, A. (2019). Development and testing of
an addiction treatment level of care determination tool.
Journal of Behavioral Health Services & Research, 46,
487–496. doi:10.1007/s11414-018-9623-x
O’Hara, M. W., & Engeldinger, J. (2018). Treatment of
postpartum depression: Recommendations for the
clinician. Clinical Obstetrics and Gynecology, 61(3),
604–614. doi:10.1097/grf.0000000000000353
O’Hara, M. W., & McCabe, J. E. (2013). Postpartum
depression: Current status and future directions. Annual
Review of Clinical Psychology, 9, 379–407. doi:10.1146/
annurev-clinpsy-050212-185612
Office of Disease Prevention and Health Promotion. (2019).
Topics & objectives A–Z. Healthy People 2020. Retrieved
from www.healthypeople.gov/2020/topics-objectives
Office of Minority Health. (October 2018). The national
CLAS standards. Retrieved from https://minorityhealth.
hhs.gov/omh/browse.aspx?lvl=2&lvlid=53
Oldham, J. M. (March 2005). Guideline watch: Practice
guideline for the treatment of patients with borderline
personality disorder. Arlington, VA: American Psychiatric
Association. Retrieved from https://psychiatryonline.org/
pb/assets/raw/sitewide/practice_guidelines/guidelines/
bpd-watch.pdf
Olfson, M. (2016). Building the mental health workforce
capacity needed to treat adults with serious mental
illnesses. Health Affairs, 35(6), 983–990. doi:10.1377/
hlthaff.2015.1619
Oquendo, M. A., Currier, D., Liu, S. M., Hasin, D. S.,
Grant, B. F., & Blanco, C. (2010). Increased risk for
suicidal behavior in comorbid bipolar disorder and
alcohol use disorders: Results from the National
Epidemiologic Survey on Alcohol and Related Conditions
(NESARC). Journal of Clinical Psychiatry, 71(7), 902–909.
doi:10.4088/JCP.09m05198gry
Oser, C. B., Biebel, E. P., Pullen, E., & Harp, K. L. (2013).
Causes, consequences, and prevention of burnout among
substance abuse treatment counselors: A rural versus
urban comparison. Journal of Psychoactive Drugs, 45(1),
17–27. doi:10.1080/02791072.2013.763558
Osman, A., Bagge, C. L., Gutierrez, P. M., Konick, L.
C., Kopper, B. A., & Barrios, F. X. (2001). The Suicidal
Behaviors Questionnaire-Revised (SBQ-R): Validation
with clinical and nonclinical samples. Assessment, 8(4),
443–454. doi:10.1177/107319110100800409
Paddock, S. M., Hunter, S. B., & Leininger, T. J. (2014).
Does group cognitive-behavioral therapy module type
moderate depression symptom changes in substance
abuse treatment clients? Journal of Substance Abuse
Treatment, 47(1), 78–85. doi:10.1016/j.jsat.2014.02.005
Padgett, D. K., Stanhope, V., Henwood, B. F., & Stefancic, A.
(2011). Substance use outcomes among homeless clients
with serious mental illness: Comparing Housing First with
Treatment First programs. Community Mental Health
Journal, 47(2), 227–232. doi:10.1007/s10597-009-9283-7
Padwa, H., Guerrero, E. G., Braslow, J. T., & Fenwick, K.
M. (2015). Barriers to serving clients with co-occurring
disorders in a transformed mental health system.
Psychiatric Services, 66(5), 547–550. doi:10.1176/appi.
ps.201400190
Padwa, H., Larkins, S., Crevecoeur-MacPhail, D. A., & Grella,
C. E. (2013). Dual diagnosis capability in mental health
and substance use disorder treatment programs. Journal
of Dual Diagnosis, 9(2), 179–186. doi:10.1080/15504263.
2013.778441
Palmer, R. H., Nugent, N. R., Brick, L. A., Bidwell, C. L.,
McGeary, J. E., Keller, M. C., & Knopik, V. S. (2016).
Evidence of shared genome-wide additive genetic effects
on interpersonal trauma exposure and generalized
vulnerability to drug dependence in a population of
substance users. Journal of Traumatic Stress, 29(3),
197–204. doi:10.1002/jts.22103
270 Appendix A

TIP 42
Appendix A—Bibliography
Paquette, K., & Pannella Winn, L. A. (2016). The role of
recovery housing: Prioritizing choice in homeless services.
Journal of Dual Diagnosis, 12(2), 153–162. doi:10.1080/15
504263.2016.1175262
Paris, J. (2014). After DSM-5: Where does personality
disorder research go from here? Harvard Review
of Psychiatry, 22(4), 216–221. doi:10.1097/
HRP.0000000000000041
Park, T. W., Cheng, D. M., Samet, J. H., Winter, M. R., &
Saitz, R. (2015). Chronic care management for substance
dependence in primary care among patients with
co-occurring disorders. Psychiatric Services, 66(1), 72–79.
doi:10.1176/appi.ps.201300414
Parks, J., & Radke, A. Q. (Eds.) (July 2014). The vital role of
state psychiatric hospitals. Retrieved from https://www.
nasmhpd.org/sites/default/files/The%20Vital%20Role%20
of%20State%20Psychiatric%20HospitalsTechnical%20
Report_July_2014.pdf
Pasche, S. (2012). Exploring the comorbidity of anxiety
and substance use disorders. Current Psychiatry Reports,
14(3), 176–181. doi:10.1007/s11920-012-0264-0
Patel, K. R., Cherian, J., Gohil, K., & Atkinson, D. (2014).
Schizophrenia: Overview and treatment options.
Pharmacy & Therapeutics, 39(9), 638–645.
Pathways to Housing DC. (2017). Program updates.
Retrieved from https://pathwaystohousingdc.org/wp-
content/uploads/financials/Annual%20Highlights%20
2016-2017.pdf
Pathways to Housing PA. (2018). Reclaiming lives.
Triennial Report 2018. Retrieved from https://
pathwaystohousingpa.org/sites/pathwaystohousingpa.
org/files/PTH%20Trienniel_11.1.18.pdf
Peachey, J. E., & Lei, H. (1988). Assessment of opioid
dependence with naloxone. British Journal of Addiction,
83(2), 193–201.
Pearce, S., & Autrique, M. (2010). On the need for
randomised trials of therapeutic community approaches.
Therapeutic Communities, 31(4), 338–355.
Pearce, S., & Pickard, H. (2013). How therapeutic
communities work: Specific factors related to positive
outcome. International Journal of Social Psychiatry, 59(7),
636–645. doi:10.1177/0020764012450992
Pearson, C., Montgomery, A. E., & Locke, G. (2009).
Housing stability among homeless individuals with serious
mental illness participating in Housing First programs.
Journal of Community Psychology, 37(3), 404–417.
doi:10.1002/jcop.20303
Penn, P. E., Brooke, D., Brooks, A. J., Gallagher, S. M., &
Barnard, A. D. (2016). Co-occurring conditions clients and
counselors compare 12-step and smart recovery mutual
help. Journal of Groups in Addiction and Recovery, 11(2),
76–92. doi:10.1080/1556035X.2015.1104643
Perry, A. E., Neilson, M., Martyn-St. James, M., Glanville,
J. M., McCool, R., Duffy, S., . . . Hewitt, C. (2015).
Interventions for drug-using offenders with co-occurring
mental illness. Cochrane Database of Systematic Reviews,
1, CD010901. doi:10.1002/14651858.cd010901
Peters, R. H., Young, M. S., Rojas, E. C., & Gorey, C. M.
(2017). Evidence-based treatment and supervision
practices for co-occurring mental and substance use
disorders in the criminal justice system. American Journal
of Drug and Alcohol Abuse, 43(4), 475–488. doi:10.1080/
00952990.2017.1303838
Petrakis, I. L., & Simpson, T. L. (2017). Posttraumatic stress
disorder and alcohol use disorder: A critical review of
pharmacologic treatments. Alcoholism: Clinical and
Experimental Research, 41(2), 226–237. doi:10.1111/
acer.13297
Petrakis, M., Robinson, R., Myers, K., Kroes, S., & O’Connor,
S. (2018). Dual diagnosis competencies: A systematic
review of staff training literature. Addictive Behaviors
Reports, 7, 53–57. doi:10.1016/j.abrep.2018.01.003
Pew Research Center. (2018, January 12). Blacks
and Hispanics are overrepresented in U.S.
prisons. Retrieved from http://www.pewresearch.
org/fact-tank/2018/01/12/shrinking-gap-
between-number-of-blacks-and-whites-in-prison/
ft_18-01-10_prisonracegaps_2/
Pierre, J. M. (2018). Real world challenges in managing dual
diagnosis patients. Current Psychiatry, 17(9), 24–30.
Pietrzak, R. H., Goldstein, R. B., Southwick, S. M., & Grant,
B. F. (2011). Prevalence and Axis I comorbidity of full and
partial posttraumatic stress disorder in the United States:
Results from Wave 2 of the National Epidemiologic
Survey on Alcohol and Related Conditions. Journal
of Anxiety Disorders, 25(3), 456–465. doi:10.1016/j.
janxdis.2010.11.010
Pinedo, M., Zemore, S., & Rogers, S. (2018). Understanding
barriers to specialty substance abuse treatment among
Latinos. Journal of Substance Abuse Treatment, 94, 1–8.
doi:10.1016/j.jsat.2018.08.004
Plakun, E. M. (2018). Clinical and insurance perspectives
on intermediate levels of care in psychiatry. Journal
of Psychiatric Practice, 24(2), 111–116. doi:10.1097/
pra.0000000000000291
Polcin, D. L. (2016). Co-occurring substance abuse and
mental health problems among homeless persons:
Suggestions for research and practice. Journal of Social
Distress and the Homeless, 26(1), 1–10. doi:10.1179/1573
658X15Y.0000000004
Polcin, D. L., Galloway, G. P., Bond, J., Korcha, R., &
Greenfield, T. K. (2010). How do residents of recovery
houses experience confrontation between entry and
12-month follow-up? Journal of Psychoactive Drugs,
42(1), 49–62. doi:10.1080/02791072.2010.10399785
Appendix A 271

TIP 42 Substance Use Disorder Treatment for People With Co-Occurring Disorders
Polcin, D. L., Mulia, N., & Laura, J. M. A. (2012).
Substance users’ perspectives on helpful and unhelpful
confrontation: Implications for recovery. Journal of
Psychoactive Drugs, 44(2), 144–152. doi:10.1080/027910
72.2012.684626
Pompili, M., Serafini, G., Innamorati, M., Dominici, G.,
Ferracuti, S., Kotzalidis, G. D., . . . Lester, D. (2010).
Suicidal behavior and alcohol abuse. International Journal
of Environmental Research and Public Health, 7(4),
1392–1431. doi:10.3390/ijerph7041392
Pompili, M., Sher, L., Serafini, G., Forte, A., Innamorati, M.,
Dominici, G., . . . Girardi, P. (2013). Posttraumatic stress
disorder and suicide risk among veterans: A literature
review. Journal of Nervous and Mental Disease, 201(9),
802–812. doi:10.1097/NMD.0b013e3182a21458
Posner, K., Brown, G. K., Stanley, B., Brent, D. A., Yershova,
K. V., Oquendo, M. A., . . . Mann, J. J. (2011). The
Columbia-Suicide Severity Rating Scale: Initial validity
and internal consistency findings from three multisite
studies with adolescents and adults. American Journal
of Psychiatry, 168(12), 1266–1277. doi:10.1176/appi.
ajp.2011.10111704
Post, L. M., Feeny, N. C., Zoellner, L. A., & Connell, A. M.
(2016). Post-traumatic stress disorder and depression
co-occurrence: Structural relations among disorder
constructs and trait and symptom dimensions. Psychology
and Psychotherapy, 89(4), 418–434. doi:10.1111/
papt.12087
Powell, D. J., & Brodsky, A. (2004). Clinical supervision in
alcohol and drug abuse counseling: Principles, models,
methods (Revised ed.). San Francisco: Jossey-Bass.
Priester, M. A., Browne, T., Iachini, A., Clone, S., DeHart,
D., & Seay, K. D. (2016). Treatment access barriers and
disparities among individuals with co-occurring mental
health and substance use disorders: An integrative
literature review. Journal of Substance Abuse Treatment,
61, 47–59. doi:10.1016/j.jsat.2015.09.006
Pringle, J., Grasso, K., & Lederer, L. (2017). Integrating the
integrated: Merging Integrated Dual Diagnosis Treatment
(IDDT) with Housing First. Community Mental Health
Journal, 53(6), 672–678. doi:10.1007/s10597-017-0107-x
Pringsheim, T., & Gardner, D. M. (2014). Dispensed
prescriptions for quetiapine and other second-
generation antipsychotics in Canada from 2005 to 2012:
A descriptive study. CMAJ Open, 2(4), e225–e232.
doi:10.9778/cmajo.20140009
Prins, A., Bovin, M. J., Kimerling, R., Kaloupek, D. G, Marx,
B. P., Pless Kaiser, A., & Schnurr, P. P. (2015). Primary
Care PTSD Screen for DSM-5 (PC-PTSD-5) [Measurement
instrument]. Retrieved from www.ptsd.va.gov/
professional/assessment/documents/pc-ptsd5-screen.pdf
Prins, A., Bovin, M. J., Smolenski, D. J., Marx, B. P.,
Kimerling, R., Jenkins-Guarnieri, M. A., . . . Tiet, Q.
Q. (2016). The Primary Care PTSD Screen for DSM-5
(PC-PTSD-5): Development and evaluation within
a veteran primary care sample. Journal of General
Internal Medicine, 31(10), 1206–1211. doi:10.1007/
s11606-016-3703-5
Prins, S. J. (2014). Prevalence of mental illnesses in US state
prisons: A systematic review. Psychiatric Services, 65(7),
862–872. doi:10.1176/appi.ps.201300166
Prochaska, J. J., Sung, H. Y., Max, W., Shi, Y., & Ong,
M. (2012). Validity study of the K6 scale as a measure
of moderate mental distress based on mental health
treatment need and utilization. International Journal
of Methods in Psychiatric Research, 21(2), 88–97.
doi:10.1002/mpr.1349
Prochaska, J. O., & DiClemente, C. C. (1992). Stages
of change in the modification of problem behaviors.
Progress in Behavior Modification, 28, 183–218.
Prochaska, J. O., DiClemente, C. C., & Norcross, J. C.
(1992). In search of how people change: Applications
to addictive behaviors. American Psychologist, 47(9),
1102–1114.
Proctor, S. L., & Herschman, P. L. (2014). The continuing
care model of substance use treatment: What works,
and when is “enough,” “enough?” Psychiatry Journal,
692423. doi:10.1155/2014/692423
Puntis, S., Rugkåsa, J., Forrest, A., Mitchell, A., & Burns,
T. (2015). Associations between continuity of care and
patient outcomes in mental health care: A systematic
review. Psychiatric Services, 66(4), 354–363.
Quinn, K., Boone, L., Scheidell, J. D., Mateu-Gelabert,
P., McGorray, S. P., Beharie, N., … Khan, M. R. (2016).
The relationships of childhood trauma and adulthood
prescription pain reliever misuse and injection drug
use. Drug and Alcohol Dependence, 169, 190–198.
doi:10.1016/j.drugalcdep.2016.09.021
Raza, G. T., DeMarce, J. M., Lash, S. J., & Parker, J. D.
(2014). Paranoid personality disorder in the United States:
The role of race, illicit drug use, and income. Journal of
Ethnic Substance Abuse, 13(3), 247–257. doi:10.1080/153
32640.2013.850463
Regnart, J., Truter, I., & Meyer, A. (2017). Critical
exploration of co-occurring attention-deficit/hyperactivity
disorder, mood disorder and substance use disorder.
Expert Review of Pharmacoeconomics & Outcomes
Research, 17(3), 275–282. doi:10.1080/14737167.2017.1
351878
Reif, S., Braude, L., Lyman, D. R., Dougherty, R. H., Daniels,
A. S., Ghose, S. S., . . . Delphin-Rittmon, M. E. (2014).
Peer recovery support for individuals with substance use
disorders: Assessing the evidence. Psychiatric Services,
65(7), 853–861. doi:10.1176/appi.ps.201400047
272 Appendix A

TIP 42Appendix A—Bibliography
Reif, S., George, P., Braude, L., Dougherty, R. H., Daniels,
A. S., Ghose, S. S., & Delphin-Rittmon, M. E. (2014).
Residential treatment for individuals with substance use
disorders: assessing the evidence. Psychiatric Services,
65(3), 301–312. doi:10.1176/appi.ps.201300242
Reingle Gonzalez, J. M., & Connell, N. M. (2014). Mental
health of prisoners: Identifying barriers to mental health
treatment and medication continuity. American Journal
of Public Health, 104(12), 2328–2333. doi:10.2105/
AJPH.2014.302043
Ries, R. K. (1993). The dually diagnosed patient with
psychotic symptoms. Journal of Addictive Diseases, 12(3),
103–122. doi:10.1300/J069v12n03_09
Riper, H., Andersson, G., Hunter, S. B., de Wit, J., Berking,
M., & Cuijpers, P. (2014). Treatment of comorbid alcohol
use disorders and depression with cognitive-behavioural
therapy and motivational interviewing: A meta-analysis.
Addiction, 109(3), 394–406. doi:10.1111/add.12441
Ritschel, L. A., Lim, N. E., & Stewart, L. M. (2015).
Transdiagnostic applications of DBT for adolescents
and adults. American Journal of Psychotherapy, 69(2),
111–128. doi:10.1176/appi.psychotherapy.2015.69.2.111
Ritter, S., & Platt, L. M. (2016). What’s new in treating
inpatients with personality disorders?: Dialectical behavior
therapy and old-fashioned, good communication. Journal
of Psychosocial Nursing and Mental Health Services,
54(1), 38–45. doi:10.3928/02793695-20151216-03
Roberts, N. P., Roberts, P. A., Jones, N., & Bisson, J. I.
(2016). Psychological therapies for post-traumatic
stress disorder and comorbid substance use disorder.
Cochrane Database of Systematic Reviews, 4, CD010204.
doi:10.1002/14651858.CD010204.pub2
Rog, D. J., Marshall, T., Dougherty, R. H., George, P.,
Daniels, A. S., Ghose, S. S., & Delphin-Rittmon, M.
E. (2014). Permanent supportive housing: Assessing
the evidence. Psychiatric Services, 65(3), 287–294.
doi:10.1176/appi.ps.201300261
Rojas, E. C., & Peters, R. H. (2015). Evidence-based
practices for co-occurring disorders in offenders.
Addiction Research & Theory, 24(3), 223–235.
Romano, M., & Peters, L. (2015). Evaluating the mechanisms
of change in motivational interviewing in the treatment
of mental health problems: A review and meta-analysis.
Clinical Psychology Review, 38, 1–12. doi:10.1016/j.
cpr.2015.02.008
Root, T. L., Pinheiro, A. P., Thornton, L., Strober, M.,
Fernandez-Aranda, F., Brandt, H., . . . Bulik, C. M. (2010).
Substance use disorders in women with anorexia nervosa.
International Journal of Eating Disorders, 43(1), 14–21.
doi:10.1002/eat.20670
Rosenblum, A., Matusow, H., Fong, C., Vogel, H., Uttaro, T.,
Moore, T. L., & Magura, S. (2014). Efficacy of dual focus
mutual aid for persons with mental illness and substance
misuse. Drug and Alcohol Dependence, 135, 78–87.
doi:10.1016/j.drugalcdep.2013.11.012
Rosenthal, R. J. (1992). Pathological
gambling. Psychiatric Annals, 22(2), 72–78.
doi:10.3928/0048-5713-19920201-09
Ross, L. E., & Dennis, C. L. (2009). The prevalence of
postpartum depression among women with substance
use, an abuse history, or chronic illness: A systematic
review. Journal of Women’s Health, 18(4), 475–486.
doi:10.1089/jwh.2008.0953
Roush, S., Monica, C., Carpenter-Song, E., & Drake, R.
E. (2015). First-person perspectives on Dual Diagnosis
Anonymous (DDA): A qualitative study. Journal of Dual
Diagnosis, 11(2), 136–141. doi:10.1080/15504263.2015.1
025215
Rowe, J. (2012). Great expectations: A systematic
review of the literature on the role of family carers
in severe mental illness, and their relationships
and engagement with professionals. Journal of
Psychiatric and Mental Health Nursing, 19(1), 70–82.
doi:10.1111/j.1365-2850.2011.01756.x
Rubinsky, A. D., Ellerbe, L. S., Gupta, S., Phelps, T. E., Bowe,
T., Burden, J. L., & Harris, A. H. S. (2017). Outpatient
continuing care after residential substance use disorder
treatment in the US Veterans Health Administration:
Facilitators and challenges. Substance Abuse, 39(3),
322–330. doi:10.1080/08897077.2017.1391923
Ruglass, L. M., Lopez-Castro, T., Papini, S., Killeen, T., Back,
S. E., & Hien, D. A. (2017). Concurrent treatment with
prolonged exposure for co-occurring full or subthreshold
posttraumatic stress disorder and substance use
disorders: A randomized clinical trial. Psychotherapy and
Psychosomatics, 86(3), 150–161. doi:10.1159/000462977
Ruglass, L. M., Miele, G. M., Hien, D. A., Campbell, A. N.,
Hu, M. C., Caldeira, N., . . . Nunes, E. V. (2012). Helping
alliance, retention, and treatment outcomes: A secondary
analysis from the NIDA Clinical Trials Network Women
and Trauma Study. Substance Use & Misuse, 47(6),
695–707. doi:10.3109/10826084.2012.659789
Ruiz, M. A., Douglas, K. S., Edens, J. F., Nikolova, N. L., &
Lilienfeld, S. O. (2012). Co-occurring mental health and
substance use problems in offenders: Implications for
risk assessment. Psychological Assessment, 24(1), 77–87.
doi:10.1037/a0024623
Ruiz, M. A., Peters, R. H., Sanchez, G. M., & Bates,
J. P. (2009). Psychometric properties of the Mental
Health Screening Form III within a metropolitan
jail. Criminal Justice and Behavior, 36(6), 607–619.
doi:10.1177/0093854809334013
Ruscio, A. M., Hallion, L. S., Lim, C. C. W., Aguilar-Gaxiola,
S., Al-Hamzawi, A., Alonso, J., . . . Scott, K. M. (2017).
Cross-sectional comparison of the epidemiology
of DSM-5 Generalized Anxiety Disorder across the
globe. JAMA Psychiatry, 74(5), 465–475. doi:10.1001/
jamapsychiatry.2017.0056
Appendix A 273

TIP 42 Substance Use Disorder Treatment for People With Co-Occurring Disorders
Sacks, S., Chaple, M., Sacks, J. Y., McKendrick, K., &
Cleland, C. M. (2012). Randomized trial of a reentry
modified therapeutic community for offenders with
co-occurring disorders: Crime outcomes. Journal
of Substance Abuse Treatment, 42(3), 247–259.
doi:10.1016/j.jsat.2011.07.011
Sacks, S., Chaple, M., Sirikantraporn, J., Sacks, J. Y.,
Knickman, J., & Martinez, J. (2013). Improving the
capability to provide integrated mental health and
substance abuse services in a state system of outpatient
care. Journal of Substance Abuse Treatment, 44(5),
488–493. doi:10.1016/j.jsat.2012.11.001
Sacks, S., McKendrick, K., Sacks, J. Y., & Cleland, C. M.
(2010). Modified therapeutic community for co-occurring
disorders: Single investigator meta analysis. Substance
Abuse, 31(3), 146–161. doi:10.1080/08897077.2010.495
662
Sacks, S., McKendrick, K., Vazan, P., Sacks, J. Y., & Cleland,
C. M. (2011). Modified therapeutic community aftercare
for clients triply diagnosed with HIV/AIDS and co-
occurring mental and substance use disorders. AIDS
Care, 23(12), 1676–1686. doi:10.1080/09540121.2011.58
2075
Sacks, S., & Sacks, J. Y. (2011, February 10). Modified
therapeutic community and specialized housing programs
for justice-involved individuals with co-occurring mental
and substance use disorders illnesses. A presentation at
the JMHCP National Training and Technical Assistance
Event: Achieving and Communicating Public Health and
Safety Outcomes for our Communities. Baltimore, MD.
Saha, S., Chant, D., Welham, J., & McGrath, J. (2005). A
systematic review of the prevalence of schizophrenia.
PLoS Medicine, 2(5). doi:10.1371/journal.pmed.0020141
Saloner, B., & Le Cook, B. (2013). Blacks and Hispanics are
less likely than whites to complete addiction treatment,
largely due to socioeconomic factors. Health Affairs,
32(1), 135–145. doi:10.1377/hlthaff.2011.0983
Samet, S., Fenton, M. C., Nunes, E., Greenstein,
E., Aharonovich, E., & Hasin, D. (2013). Effects of
independent and substance-induced major depressive
disorder on remission and relapse of alcohol, cocaine
and heroin dependence. Addiction, 108(1), 115–123.
doi:10.1111/j.1360-0443.2012.04010.x
Samuels, E. A., Bernstein, S. L., Marshall, B. D. L., Krieger,
M., Baird, J., & Mello, M. J. (2018). Peer navigation and
take-home naloxone for opioid overdose emergency
department patients: Preliminary patient outcomes.
Journal of Substance Abuse Treatment, 94, 29–34.
doi:10.1016/j.jsat.2018.07.013
Sanchez, K., Ybarra, R., Chapa, T., & Martinez, O. N. (2016).
Eliminating behavioral health disparities and improving
outcomes for racial and ethnic minority populations.
Psychiatric Services, 67(1), 13–15. doi:10.1176/appi.
ps.201400581
Sanchez-Moreno, J., Martinez-Aran, A., & Vieta, E. (2017).
Treatment of functional impairment in patients with
bipolar disorder. Current Psychiatry Reports, 19(1), 3.
doi:10.1007/s11920-017-0752-3
Sansone, R. A., & Sansone, L. A. (2011a). Gender patterns
in borderline personality disorder. Innovations in Clinical
Neuroscience, 8(5), 16–20.
Sansone, R. A., & Sansone, L. A. (2011b). Substance use
disorders and borderline personality. Innovations in
Clinical Neuroscience, 8(9), 10–13.
Sansone, R. A., & Sansone, L. A. (2015). Borderline
personality in the medical setting. Primary Care
Companion for CNS Disorders, 17(3). doi:10.4088/
PCC.14r01743
Sarkar, J., & Duggan, C. (2010). Diagnosis and classification
of personality disorder: Difficulties, their resolution
and implications for practice. Advances in Psychiatric
Treatment, 16(5), 388–396. doi:10.1192/apt.16.6.476a
Sarvet, A. L., Wall, M. M., Keyes, K. M., Olfson, M., Cerdá,
M., & Hasin, D. S. (2018). Self-medication of mood and
anxiety disorders with marijuana: Higher in states with
medical marijuana laws. Drug and Alcohol Dependence,
186, 10–15. doi:10.1016/j.drugalcdep.2018.01.009
Savic, M., Best, D., Manning, V., & Lubman, D. I. (2017).
Strategies to facilitate integrated care for people with
alcohol and other drug problems: A systematic review.
Substance Abuse: Treatment, Prevention, and Policy,
12(1). doi:10.1186/s13011-017-0104-7
Schaffer, A., Isometsa, E. T., Tondo, L., H. Moreno,
D., Turecki, G., Reis, C., . . . Yatham, L. N. (2015).
International Society for Bipolar Disorders Task Force on
Suicide: Meta-analyses and meta-regression of correlates
of suicide attempts and suicide deaths in bipolar disorder.
Bipolar Disorders, 17(1), 1–16. doi:10.1111/bdi.12271
Schaumberg, K., Welch, E., Breithaupt, L., Hubel, C., Baker,
J. H., Munn-Chernoff, M. A., . . . Bulik, C. M. (2017). The
science behind the Academy for Eating Disorders’ nine
truths about eating disorders. European Eating Disorders
Review, 25(6), 432–450. doi:10.1002/erv.2553
Schneier, F. R., Foose, T. E., Hasin, D. S., Heimberg, R. G.,
Liu, S. M., Grant, B. F., & Blanco, C. (2010). Social anxiety
disorder and alcohol use disorder co-morbidity in the
National Epidemiologic Survey on Alcohol and Related
Conditions. Psychological Medicine, 40(6), 977–988.
doi:S0033291709991231
Schoenthaler, S. J., Blum, K., Fried, L., Oscar-Berman, M.,
Giordano, J., Modestino, E. J., & Badgaiyan, R. (2017).
The effects of residential dual diagnosis treatment
on alcohol abuse. Journal of Systems and Integrative
Neuroscience, 3(4). doi:10.15761/jsin.1000169
Schulte, S. J., Meier, P. S., & Stirling, J. (2011). Dual
diagnosis clients’ treatment satisfaction – A systematic
review. BMC Psychiatry, 11, 64.
274 Appendix A

TIP 42
Appendix A—Bibliography
Schulz, P. E., & Arora, G. (2015). Depression. Behavioral
Neurology and Neuropsychiatry, 21(3), 756–771.
doi:10.1212/01.CON.0000466664.35650.b4
Schumm, J. A., & Gore, W. L. (2016). Simultaneous
treatment of co-occurring posttraumatic stress disorder
and substance use disorder. Current Treatment Options in
Psychiatry, 3(1), 28–36. doi:10.1007/s40501-016-0071-z
Scott, E. L., & Hulvershorn, L. (2011, September 7). Anxiety
disorders with comorbid substance abuse. Psychiatric
Times, 28(9), 1–2.
Seal, K. H., Cohen, G., Waldrop, A., Cohen, B. E., Maguen,
S., & Ren, L. (2011). Substance use disorders in Iraq
and Afghanistan veterans in VA healthcare, 2001–2010:
Implications for screening, diagnosis and treatment.
Drug and Alcohol Dependence, 116(1–3), 93–101.
doi:10.1016/j.drugalcdep.2010.11.027
Selzer, M. L. (1971). The Michigan Alcoholism Screening
Test: The quest for a new diagnostic instrument.
American Journal of Psychiatry, 127(12), 1653–1658.
doi:10.1176/ajp.127.12.1653
Shapiro, B., Coffa, D., & McCance-Katz, E. F. (2013). A
primary care approach to substance misuse. American
Family Physician, 88(2), 113–121.
Shattock, L., Berry, K., Degnan, A., & Edge, D. (2018).
Therapeutic alliance in psychological therapy for people
with schizophrenia and related psychoses: A systematic
review. Clinical Psychology & Psychotherapy, 25(1), e60–
e85. doi:10.1002/cpp.2135
Sheehan, D. V., Harnett-Sheehan, K., & Raj, B. A. (1996).
The measurement of disability. International Clinical
Psychopharmacology, 11(Suppl. 3), 89–95.
Sheehan, D. V., Lecrubier, Y., Sheehan, K. H., Amorim, P.,
Janavs, J., Weiller, E., . . . Dunbar, G. C. (1998). The Mini-
International Neuropsychiatric Interview (M.I.N.I.): The
development and validation of a structured diagnostic
psychiatric interview for DSM-IV and ICD-10. Journal of
Clinical Psychiatry, 59(Suppl. 20), 22–33; quiz 34–57.
Sheehan, L., Nieweglowski, K., & Corrigan, P. (2016). The
stigma of personality disorders. Current Psychiatry
Reports, 18(1), 1–7. doi:10.1007/s11920-015-0654-1
Shenoy, A., & Appel, J. M. (2017). Safeguarding
confidentiality in electronic health records. Cambridge
Quarterly of Healthcare Ethics, 26(2), 337–341.
doi:10.1017/s0963180116000931
Sher, L., Siever, L. J., Goodman, M., McNamara, M., Hazlett,
E. A., Koenigsberg, H. W., & New, A. S. (2015). Gender
differences in the clinical characteristics and psychiatric
comorbidity in patients with antisocial personality
disorder. Psychiatry Research, 229(3), 685–689.
doi:10.1016/j.psychres.2015.08.022
Sherman, L. J., Lynch, S. E., Greeno, C. G., & Hoeffel, E.
M. (2017, July 11). Behavioral health workforce: Quality
assurance practices in substance abuse treatment
facilities. SAMHSA CBHSQ report. Retrieved from
www.samhsa.gov/data/sites/default/files/report_3059/
ShortReport-3059.html
Shinn, G., & Brose, M. (2017). Building partnerships
and collaboration between housing providers and
behavioral health practitioners. Mental Health Association
Oklahoma. Retrieved from www.samhsa.gov/sites/
default/files/programs_campaigns/recovery_to_practice/
homelessness-3-building-partnerships.pdf
Shionogi Pharma Inc. (2010). KAPVAY (clonidine
hydrochloride) extended-release tablets, oral Initial
U.S. approval: 1974. Prescribing information. Retrieved
from www.accessdata.fda.gov/drugsatfda_docs/
label/2010/022331s001s002lbl.pdf
Shire US Inc. (Revised February 2013). INTUNIV®
(guanfacine) extended-release tablets, for oral use. Initial
U.S. approval: 1986 Retrieved from www.accessdata.fda.
gov/drugsatfda_docs/label/2013/022037s009lbl.pdf
Simon, R. I., Hales, R. E., & American Psychiatric Publishing.
(2012).The American Psychiatric Publishing textbook
of suicide assessment and management(2nd ed.).
Washington, DC: American Psychiatric Publishing.
Simon, V., Czobor, P., Balint, S., Meszaros, A., & Bitter, I.
(2009). Prevalence and correlates of adult attention-
deficit hyperactivity disorder: Meta-analysis. British
Journal of Psychiatry, 194(3), 204–211. doi:10.1192/bjp.
bp.107.048827
Simpson, T. L., Lehavot, K., & Petrakis, I. L. (2017). No
wrong doors: Findings from a critical review of behavioral
randomized clinical trials for individuals with co-occurring
alcohol/drug problems and posttraumatic stress disorder.
Alcoholism: Clinical and Experimental Research, 41(4),
681–702. doi:10.1111/acer.13325
Simpson, T. L., Stappenbeck, C. A., Luterek, J. A., Lehavot,
K., & Kaysen, D. L. (2014). Drinking motives moderate
daily relationships between PTSD symptoms and alcohol
use. Journal of Abnormal Psychology, 123(1), 237–247.
doi:10.1037/a0035193
Sinha, A., Lewis, O., Kumar, R., Yeruva, S. L. H., & Curry,
B. H. (2016). Adult ADHD medications and their
cardiovascular implications.Case Reports in Cardiology,
2016, 2343691. doi: 10.1155/2016/2343691
Skinner, H. A. (1982). The Drug Abuse Screening
Test. Addictive Behaviors, 7(4), 363–371.
doi:10.1016/0306-4603(82)90005-3
Smelson, D., Farquhar, I., Fisher, W., Pressman, K., Pinals,
D. A., Samek, B., . . . Sawh, L. (2018). Integrating a
co-occurring disorders intervention in drug courts: An
open pilot trial. Community Mental Health Journal, 55(2),
222–231. doi:10.1007/s10597-018-0255-7
Appendix A 275
TIP 42 Substance Use Disorder Treatment for People With Co-Occurring Disorders
Smelson, D. A., Zaykowski, H., Guevermont, N., Siegfriedt,
J., Sawh, L., Modzelewski, D., … Kane, V. (2016).
Integrating permanent supportive housing and co-
occurring disorders treatment for individuals who are
homeless. Journal of Dual Diagnosis, 12(2), 193–201. doi:
10.1080/15504263.2016.1174010
Smink, F. R. E., van Hoeken, D., & Hoek, H. W. (2013).
Epidemiology, course, and outcome of eating disorders.
Current Opinion in Psychiatry, 26(6), 543–548.
doi:10.1097/YCO.0b013e328365a24f
Smith, D. E. (2012). Editor’s note: The medicalization of
therapeutic communities in the era of health care reform.
Journal of Psychoactive Drugs, 44(2), 93–95. doi:10.1080/
02791072.2012.684608
Smith, J. D., Mittal, D., Chekuri, L., Han, X., & Sullivan, G.
(2017). A comparison of provider attitudes toward serious
mental illness across different health care disciplines.
Stigma and Health, 2(4), 327–337.
Smith, J. P., & Book, S. W. (2008). Anxiety and substance
use disorders: A review. Psychiatric Times, 25(10), 19–23.
Smith, J. P., & Randall, C. L. (2012). Anxiety and alcohol use
disorders: Comorbidity and treatment considerations.
Alcohol Research, 34(4), 414–431.
Smith, M. W., Stocks, C., & Santora, P. B. (2015). Hospital
readmission rates and emergency department visits
for mental health and substance abuse conditions.
Community Mental Health Journal, 51(2), 190–197.
doi:10.1007/s10597-014-9784-x
Smith, R. J., Jennings, J. L., & Cimino, A. (2010).
Forensic continuum of care with Assertive Community
Treatment (ACT) for persons recovering from co-
occurring disabilities: Long-term outcomes. Psychiatric
Rehabilitation Journal, 33(3), 207–218.
Smith, S. M., Goldstein, R. B., & Grant, B. F. (2016). The
association between post-traumatic stress disorder and
lifetime DSM-5 psychiatric disorders among veterans:
Data from the National Epidemiologic Survey on
Alcohol and Related Conditions-III (NESARC-III). Journal
of Psychiatric Research, 82, 16–22. doi:10.1016/j.
jpsychires.2016.06.022
Sohal, H., Eldridge, S., & Feder, G. (2007). The sensitivity
and specificity of four questions (HARK) to identify
intimate partner violence: A diagnostic accuracy
study in general practice. BMC Family Practice, 8, 49.
doi:10.1186/1471-2296-8-49
Sohn, H. (2017). Racial and ethnic disparities in health
insurance coverage: Dynamics of gaining and losing
coverage over the life-course. Population Research
and Policy Review, 36(2), 181–201. doi:10.1007/
s11113-016-9416-y
Solari, C. D., Morris, S., Shivji, A., & Souza, T. D. (2016,
October). The 2015 Annual Homeless Assessment
Report (AHAR) to Congress. Part 1 - PIT estimates of
homelessness in the U.S. Retrieved from https://files.
hudexchange.info/resources/documents/2015-AHAR-
Part-1.pdf
Sowers, W. (2016). Level of Care Utilization System for
psychiatric and addiction services (LOCUS), Adult version
20. Task Force on Level of Care Determinations of the
American Association of Community Psychiatrists (AACP).
Dallas, TX: AACP. Retrieved from https://drive.google.
com/file/d/0B89glzXJnn4cV1dESWI2eFEzc3M/view
Spinelli, M. A., Ponath, C., Tieu, L., Hurstak, E. E., Guzman,
D., & Kushel, M. (2017). Factors associated with
substance use in older homeless adults: Results from the
HOPE HOME study. Substance Abuse, 38(1), 88–94. doi:1
0.1080/08897077.2016.1264534
Stahler, G. J., Mennis, J., & DuCette, J. P. (2016). Residential
and outpatient treatment completion for substance
use disorders in the U.S.: Moderation analysis by
demographics and drug of choice. Addictive Behaviors,
58, 129–135. doi:10.1016/j.addbeh.2016.02.030
Stefancic, A., Henwood, B. F., Melton, H., Shin, S.
M., Lawrence-Gomez, R., & Tsemberis, S. (2013).
Implementing housing first in rural areas: Pathways
Vermont. American Journal of Public Health, 103(Suppl.
2), S206–S209. doi:10.2105/ajph.2013.301606
Stein, L. I., & Test, M. A. (1980). Alternative to mental
hospital treatment: I. Conceptual model, treatment
program, and clinical evaluation. Archives of General
Psychiatry, 37(4), 392–397.
Sterling, S., Chi, F., & Hinman, A. (2011). Integrating care
for people with co-occurring alcohol and other drug,
medical, and mental health conditions. Alcohol Research
& Health, 33(4), 338–349.
Stice, E., Marti, C. N., & Rohde, P. (2013). Prevalence,
incidence, impairment, and course of the proposed
DSM-5 eating disorder diagnoses in an 8-year prospective
community study of young women. Journal of Abnormal
Psychology, 122(2), 445–457. doi:10.1037/a0030679
Stinson, J. D., Quinn, M. A., & Levenson, J. S. (2016).
The impact of trauma on the onset of mental health
symptoms, aggression, and criminal behavior in an
inpatient psychiatric sample. Child Abuse and Neglect,
61, 13–22. doi:10.1016/j.chiabu.2016.09.005
Stirman, S. W., Gutner, C. A., Langdon, K., & Graham,
J. R. (2016). Bridging the gap between research and
practice in mental health service settings: An overview
of developments in implementation theory and research.
Behavior Therapy, 47(6), 920–936. doi:10.1016/j.
beth.2015.12.001
276 Appendix A

TIP 42Appendix A—Bibliography
Stone, D. M., Simon, T. R., Fowler, K. A., Kegler, S. R., Yuan,
K., Holland, K. M., . . . Crosby, A. E. (2018). Vital signs:
Trends in state suicide rates — United States, 1999–2016
and circumstances contributing to suicide — 27 states,
2015. Morbidity and Mortality Weekly Report, 67(22),
617–624. doi:10.15585/mmwr.mm6722a1
Stone, E. M., Chen, L. N., Daumit, G. L., Linden, S., &
McGinty, E. E. (2019). General medical clinicians’ attitudes
toward people with serious mental illness: A scoping
review. Journal of Behavioral Health Services & Research,
18. doi:10.1007/s11414-019-09652-w
Stringfellow, E. J., Kim, T. W., Gordon, A. J., Pollio, D. E.,
Grucza, R. A., Austin, E. L., . . . Kertesz, S. G. (2016).
Substance use among persons with homeless experience
in primary care. Substance Abuse, 37(4), 534–541. doi:10.
1080/08897077.2016.1145616
Strom, J. B., Kramer, D. B., Wang, Y., Shen, C., Wasfy,
J. H., Landon, B. E., . . . Yeh, R. W. (2017). Short-term
rehospitalization across the spectrum of age and
insurance types in the United States. PLoS ONE, 12(7),
e0180767. doi:10.1371/journal.pone.0180767
Subodh, B. N., Sharma, N., & Shah, R. (2018). Psychosocial
interventions in patients with dual diagnosis. Indian
Journal of Psychiatry, 60(Suppl. 4), S494–S500.
doi:10.4103/psychiatry.IndianJPsychiatry_18_18
Substance Abuse and Mental Health Services
Administration. (n.d.) Recruitment and Retention Toolkit.
Substance Abuse and Mental Health Services
Administration. (2000). Integrating substance
abuse treatment and vocational services. Treatment
Improvement Protocol (TIP) Series, No. 38. HHS
Publication No. (SMA) 12-4216. Rockville, MD: Substance
Abuse and Mental Health Services Administration.
Substance Abuse and Mental Health Services
Administration. (2008). Assertive Community Treatment
(ACT) Evidence-Based Practices (EBP) KIT. Retrieved from
https://store.samhsa.gov/product/Assertive-Community-
Treatment-ACT-Evidence-Based-Practices-EBP-KIT/
sma08-4344
Substance Abuse and Mental Health Services
Administration. (2009a). Integrated treatment for co-
occurring disorders: training frontline staff. DHHS Pub.
No. SMA-08-4366. Rockville, MD: Center for Mental
Health Services, Substance Abuse and Mental Health
Services Administration, U.S. Department of Health and
Human Services.
Substance Abuse and Mental Health Services
Administration. (2009b). SAFE-T – Suicide assessment
five-step evaluation and triage. Pocket card. Retrieved
from https://store.samhsa.gov/system/files/sma09-4432.
pdf
Substance Abuse and Mental Health Services
Administration. (2009c). Substance abuse treatment:
Addressing the specific needs of women. Revised 2013.
Treatment Improvement Protocol (TIP) Series 51 (HHS
Publication No. (SMA)13-4426). Rockville, MD: Substance
Abuse and Mental Health Services Administration.
Substance Abuse and Mental Health Services
Administration. (2011a). Clients with substance
use and eating disorders. Advisory, 10(1), 1–11.
Retrieved from https://store.samhsa.gov/product/
clients-with-substance-use-and-eating-disorders/
SMA10-4617
Substance Abuse and Mental Health Services
Administration. (2011b). Dual diagnosis capability
in mental health treatment toolkit version 4.0. (HHS
Publication No. SMA-XX-XXXX). Rockville, MD: Substance
Abuse and Mental Health Services Administration.
Substance Abuse and Mental Health Services
Administration. (2012). SAMHSA’s working definition
of recovery. Retrieved from https://store.samhsa.gov/
system/files/pep12-recdef.pdf
Substance Abuse and Mental Health Services
Administration. (2013). Behavioral health services for
people who are homeless. (HHS Publication No. (SMA)
13-4734). Rockville, MD: Substance Abuse and Mental
Health Services Administration.
Substance Abuse and Mental Health Services
Administration. (2014a). Improving cultural competence.
Treatment Improvement Protocol (TIP) Series No. 59 (HHS
Publication No. (SMA) 14-4849). Rockville, MD: Substance
Abuse and Mental Health Services Administration.
Substance Abuse and Mental Health Services
Administration. (2014b). Trauma-informed care in
behavioral health services. Treatment Improvement
Protocol (TIP) Series 57. (HHS Publication No. (SMA)
14-4816.). Rockville, MD: Substance Abuse and Mental
Health Services Administration.
Substance Abuse and Mental Health Services
Administration (2014c). SAMHSA’s concept of trauma
and guidance for a trauma-informed approach. HHS
Publication No. (SMA) 14-4884. Rockville, MD: Substance
Abuse and Mental Health Services Administration, 2014.
Substance Abuse and Mental Health Services
Administration. (2015a). Adults with attention deficit
hyperactivity disorder and substance use disorders.
Advisory 14(3). Retrieved from https://store.samhsa.
gov/product/Advisory-Adults-With-Attention-Deficit-
Hyperactivity-Disorder-and-Substance-Use-Disorders/
SMA15-4925
Substance Abuse and Mental Health Services
Administration. (2015b). Screening and assessment of co-
occurring disorders in the justice system. (HHS Publication
No. (SMA)-15-4930). Rockville, MD: Substance Abuse and
Mental Health Services Administration.
Appendix A 277
TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
Substance Abuse and Mental Health Services
Administration. (2015c, March). Women in the mirror:
Addressing co-occurring mental health issues and trauma
in women with substance use disorders. Retrieved from
https://www.samhsa.gov/sites/default/files/programs_
campaigns/women_children_families/women-in-mirror.pdf
Substance Abuse and Mental Health Services
Administration. (2016). An introduction to bipolar
disorder and co-occurring substance use disorders.
Advisory, 15(2). Retrieved from https://store.samhsa.gov/
system/files/sma16-4960.pdf
Substance Abuse and Mental Health Services
Administration. (2017). Suicide prevention. Retrieved
from https://www.samhsa.gov/suicide-prevention
Substance Abuse and Mental Health Services
Administration. (2018a). Behavioral health services
for American Indians and Alaska Natives. Treatment
Improvement Protocol (TIP) Series 61 (HHS Publication
No. (SMA) 18-5070). Rockville, MD: Substance Abuse and
Mental Health Services Administration.
Substance Abuse and Mental Health Services
Administration. (2018b). Key substance use and mental
health indicators in the United States: Results from the
2017 National Survey on Drug Use and Health (HHS
Publication No. SMA 18-5068, NSDUH Series H-53).
Rockville, MD: Center for Behavioral Health Statistics and
Quality, Substance Abuse and Mental Health Services
Administration.
Substance Abuse and Mental Health Services
Administration. (2018c). Medications for opioid use
disorder. Treatment Improvement Protocol (TIP) Series 63
(HHS Publication No. (SMA) 18-5063FULLDOC). Rockville,
MD: Substance Abuse and Mental Health Services
Administration.
Substance Abuse and Mental Health Services
Administration. (2018d). National Mental Health Services
Survey (N-MHSS): 2017. Data on mental health treatment
facilities. Rockville, MD: Substance Abuse and Mental
Health Services Administration.
Substance Abuse and Mental Health Services
Administration. (2018e). National Survey of Substance
Abuse Treatment Services (N-SSATS): 2017. Data
on substance abuse treatment facilities. Rockville,
MD: Substance Abuse and Mental Health Services
Administration.
Substance Abuse and Mental Health Services
Administration. (2019a). National Survey of Substance
Abuse Treatment Services (N-SSATS): 2018. Data
on substance abuse treatment facilities. Rockville,
MD: Substance Abuse and Mental Health Services
Administration.
Substance Abuse and Mental Health Services
Administration. (2019b). National Mental Health Services
Survey (N-MHSS): 2018. Data on mental health treatment
facilities. Rockville, MD: Substance Abuse and Mental
Health Services Administration.
Substance Abuse and Mental Health Services
Administration. (2019c). Enhancing motivation for
change in substance use disorder treatment. Treatment
Improvement Protocol (TIP) Series 35. (SAMHSA
Publication No. PEP19-02-01-003). Rockville, MD: Center
for Substance Abuse Treatment.
Substance Abuse and Mental Health Services
Administration. (2019d). Mental health annual report:
2017. Use of mental health services: National client
level data. Rockville, MD: Center for Behavioral Health
Statistics and Quality.
Substance Abuse and Mental Health Services
Administration, Center for Behavioral Health Statistics
and Quality. (2017). Treatment Episode Data Set (TEDS):
2005–2015. National admissions to substance abuse
treatment services. BHSIS Series S-91, HHS Publication
No. (SMA) 17-5037. Rockville, MD: Substance Abuse and
Mental Health Services Administration.
Substance Abuse and Mental Health Services
Administration, Center for Behavioral Health Statistics
and Quality. (2019). Treatment Episode Data Set (TEDS):
2017. Admissions to and discharges from publicly-funded
substance use treatment. Rockville, MD: Substance Abuse
and Mental Health Services Administration.
Sullivan, J. T., Sykora, K., Schneiderman, J., Naranjo, C. A.,
& Sellers, E. M. (1989). Assessment of alcohol withdrawal:
The revised Clinical Institute Withdrawal Assessment for
Alcohol scale (CIWA-Ar). British Journal of Addiction,
84(11), 1353–1357.
Sun, A. P. (2012). Helping homeless individuals with co-
occurring disorders: The four components. Social Work,
57(1), 23–37.
Sung, Y. K., La Flair, L. N., Mojtabai, R., Lee, L. C., Spivak,
S., & Crum, R. M. (2016). The association of alcohol use
disorders with suicidal ideation and suicide attempts in a
population-based sample with mood symptoms. Archives
of Suicide Research, 20(2), 219–232. doi:10.1080/138111
18.2015.1004489
Swann, A. C. (2010). The strong relationship between
bipolar and substance-use disorder. Annals of the
New York Academy of Sciences, 1187, 276–293.
doi:10.1111/j.1749-6632.2009.05146.x
Swopes, R. M., Davis, J. L., & Scholl, J. A. (2017).
Treating substance abuse and trauma symptoms
in incarcerated women: An effectiveness study.
Journal of Interpersonal Violence, 32(7), 1143–1165.
doi:10.1177/0886260515587668
278 Appendix A

TIP 42Appendix A—Bibliography
Szaflarski, M., Bauldry, S., Cubbins, L. A., & Meganathan, K.
(2017). Nativity, race-ethnicity, and dual diagnosis among
US adults. Research in the Sociology of Health Care, 35,
171–191.
Tang, Z., Claus, R. E., Orwin, R. G., Kissin, W. B., & Arieira,
C. (2012). Measurement of gender-sensitive treatment
for women in mixed-gender substance abuse treatment
programs. Drug and Alcohol Dependence, 123(1–3),
160–166. doi:10.1016/j.drugalcdep.2011.11.003
Taylor, O. D. (2010). Barriers to treatment for women
with substance use disorders. Journal of Human
Behavior in the Social Environment, 20(3), 393–409.
doi:10.1080/10911351003673310
Teeters, J. B., Lancaster, C. L., Brown, D. G., & Back, S.
E. (2017). Substance use disorders in military veterans:
Prevalence and treatment challenges. Substance Abuse
and Rehabilitation, 8, 69–77. doi:10.2147/sar.S116720
Test, M. A. (1992). Training in community living. In R. P.
Lieberman (Ed.), Handbook of psychiatric rehabilitation
(pp. 153–170). New York, NY: MacMillan Publishing.
Thiel, N., Hertenstein, E., Nissen, C., Herbst, N.,
Külz, A. K., & Voderholzer, U. (2013). The effect of
personality disorders on treatment outcomes in
patients with obsessive-compulsive disorders. Journal
of Personality Disorders, 27(6), 697–715. doi:10.1521/
pedi_2013_27_104
Thomson, M., & Sharma, V. (2017). Therapeutics
of postpartum depression. Expert Review of
Neurotherapeutics, 17(5), 495–507. doi:10.1080/1473717
5.2017.1265888
Thronson, L. R., & Pagalilauan, G. L. (2014).
Psychopharmacology. Medical Clinics of North America,
98(5), 927–958. doi:10.1016/j.mcna.2014.06.001
Thurber, S., Wilson, A., Realmuto, G., & Specker, S. (2018).
The relationship between the INTERMED patient
complexity instrument and Level of Care Utilisation
System (LOCUS). International Journal of Psychiatry in
Clinical Practice, 22(1), 80–82. doi:10.1080/13651501.20
17.1353635
Tiet, Q. Q., & Schutte, K. K. (2012). Treatment setting and
outcomes of patients with co-occurring disorders. Journal
of Groups in Addiction & Recovery, 7(1), 53–76. doi:10.10
80/1556035X.2012.632330
Timko, C., Sutkowi, A., & Moos, R. (2010). Patients with dual
diagnoses or substance use disorders only: 12-step group
participation and 1-year outcomes. Substance Use &
Misuse, 45(4), 613–627. doi:10.3109/10826080903452421
Tolliver, B. K., & Anton, R. F. (2015). Assessment and
treatment of mood disorders in the context of substance
abuse. Dialogues in Clinical Neuroscience, 17(2),
181–190.
Tonigan, J. S., Pearson, M. R., Magill, M., & Hagler, K.
J. (2018). AA attendance and abstinence for dually
diagnosed patients: A meta-analytic review. Addiction,
113(11), 1970–1981. doi:10.1111/add.14268
Trivedi, R. B., Post, E. P., Sun, H., Pomerantz, A., Saxon,
A. J., Piette, J. D., . . . Nelson, K. (2015). Prevalence,
comorbidity, and prognosis of mental health among US
veterans. American Journal of Public Health, 105(12),
2564–2569. doi:10.2105/ajph.2015.302836
Trudeau, K. J., Burtner, J., Villapiano, A. J., Jones, M.,
Butler, S. F., & Joshi, K. (2018). Burden of schizophrenia
or psychosis-related symptoms in adults undergoing
substance abuse evaluation. Journal of Nervous
and Mental Disease, 206(7), 528–536. doi:10.1097/
NMD.0000000000000835
Trull, T. J., Freeman, L. K., Vebares, T. J., Choate, A.
M., Helle, A. C., & Wycoff, A. M. (2018). Borderline
personality disorder and substance use disorders:
An updated review. Borderline Personality Disorder
and Emotion Dysregulation, 5, 15. doi:10.1186/
s40479-018-0093-9
Trull, T. J., Jahng, S., Tomko, R. L., Wood, P. K., & Sher, K. J.
(2010). Revised NESARC personality disorder diagnoses:
Gender, prevalence, and comorbidity with substance
dependence disorders. Journal of Personality Disorders,
24(4), 412–426. doi:10.1521/pedi.2010.24.4.412
Tsai, J. (2018). Lifetime and 1-year prevalence of
homelessness in the US population: Results from the
National Epidemiologic Survey on Alcohol and Related
Conditions-III. Journal of Public Health (Oxford, England),
40(1), 65–74. doi:10.1093/pubmed/fdx034
Tsai, J., & Cao, X. (2019). Association between suicide
attempts and homelessness in a population-based
sample of US veterans and non-veterans. Journal of
Epidemiology and Community Health, 73(4), 346-352.
doi:10.1136/jech-2018-211065
Tsai, J., Kasprow, W. J., & Rosenheck, R. A. (2014). Alcohol
and drug use disorders among homeless veterans:
Prevalence and association with supported housing
outcomes. Addictive Behaviors, 39(2), 455–460.
doi:10.1016/j.addbeh.2013.02.002
Tsai, J., Lee, C. Y. S., Byrne, T., Pietrzak, R. H., & Southwick,
S. M. (2017). Changes in public attitudes and perceptions
about homelessness between 1990 and 2016. American
Journal of Community Psychology, 60(3–4), 599–606.
doi:10.1002/ajcp.12198
Tsai, J., & Rosenheck, R. A. (2012). Outcomes of a group
intensive peer-support model of case management
for supported housing. Psychiatric Services, 63(12),
1186–1194.
Tsemberis, S., & Eisenberg, R. F. (2000). Pathways to
housing: Supported housing for street-dwelling homeless
individuals with psychiatric disabilities. Psychiatric
Services, 51(4), 487–493. doi:10.1176/appi.ps.51.4.487
Appendix A 279

TIP 42 Substance Use Disorder Treatment for People With Co-Occurring Disorders
Tsemberis, S. J. (2010) Housing First: The Pathways model
to end homelessness for people with mental health
and substance use disorders. Center City, Minnesota:
Hazelden Publishing.
Tsemberis, S. J., Moran, L., Shinn, M., Asmussen, S. M.,
& Shern, D. L. (2003). Consumer preference programs
for individuals who are homeless and have psychiatric
disabilities: A drop-in center and a supported housing
program. American Journal of Community Psychology,
32(3–4), 305–317.
Turner, S. B., & Stanton, M. P. (2015). Psychiatric case
management in the emergency department. Professional
Case Management, 20(5), 217–227; quiz 228–219.
doi:10.1097/ncm.0000000000000106
Tyrer, P., Sharfstein, S., O’Reilly, R., Allison, S., &
Bastiampillai, T. (2017). Psychiatric hospital beds: An
Orwellian crisis. Lancet, 389(10067), 363. doi:10.1016/
s0140-6736(17)30149-6
U.S. Department of Health and Human Services (HHS)
Office of the Surgeon General and National Action
Alliance for Suicide Prevention. (2012, September). 2012
National Strategy for Suicide Prevention: Goals and
objectives for action. Washington, DC: HHS.
U.S. Department of Health and Human Services, Office
of the Surgeon General. (2016, November). Facing
Addiction in America: The Sur geon General’s Report on
Alcohol, Drugs, and Health. Washington, DC: HHS.
U.S. Department of Housing and Urban Development.
(2018). 2018 Continuum of Care Homeless Populations
and Subpopulations Report - All states, territories, Puerto
Rico, and DC. Washington, DC: Author. Retrieved May
29, 2018, from https://files.hudexchange.info/reports/
published/CoC_PopSub_NatlTerrDC_2018.pdf
U.S. Interagency Council on Homelessness. (2014, June).
Implementing Housing First in Permanent Supportive
Housing. Fact Sheet from USICH with assistance from
the Substance Abuse and Mental Health Services
Administration. Retrieved from www.usich.gov/resources/
uploads/asset_library/Implementing_Housing_First_in_
Permanent_Supportive_Housing.pdf
U.S. Preventive Services Task Force (USPTSF). (2013).
Archived: Intimate partner violence and abuse of elderly
and vulnerable adults: Screening. Retrieved from www.
uspreventiveservicestaskforce.org/Page/Document/
UpdateSummaryFinal/intimate-partner-violence-and-
abuse-of-elderly-and-vulnerable-adults-screening
Udo, T., & Grilo, C. M. (2018). Prevalence and
correlates of DSM-5-defined eating disorders in
a nationally representative sample of U.S. adults.
Biological Psychiatry, 84(5), 345–354. doi:10.1016/j.
biopsych.2018.03.014
Ullman, S. E., Relyea, M., Peter-Hagene, L., & Vasquez, A.
L. (2013). Trauma histories, substance use coping, PTSD,
and problem substance use among sexual assault victims.
Addictive Behaviors, 38(6), 2219–2223. doi:10.1016/j.
addbeh.2013.01.027
University of Michigan Behavioral Health Workforce
Research Center. (2018). Scopes of practice and
reimbursement patterns of addiction counselors,
community health workers, and peer recovery specialists
in the behavioral health workforce. Ann Arbor, MI:
University of Michigan School of Public Health.
Upshur, C. C., Jenkins, D., Weinreb, L., Gelberg, L., &
Orvek, E. A. (2017). Prevalence and predictors of
substance use disorders among homeless women seeking
primary care: An 11 site survey. American Journal of
Addictions, 26(7), 680–688. doi:10.1111/ajad.12582
Üstün, T. B., & World Health Organization. (2010).
Measuring health and disability: Manual for WHO
Disability Assessment Schedule WHODAS 2.0. Geneva:
World Health Organization.
Vallejo, Z., & Amaro, H. (2009). Adaptation of mindfulness-
based stress reduction program for addiction relapse
prevention. The Humanistic Psychologist, 37(2), 192–206.
doi:10.1080/08873260902892287
van de Glind, G., Van Emmerik-van Oortmerssen, K.,
Carpentier, P. J., Levin, F. R., Koeter, M. W. J., Barta, C.,
. . . van den Brink, W. (2013). The International ADHD
in Substance Use Disorders Prevalence (IASP) study:
Background, methods and study population. International
Journal of Methods in Psychiatric Research, 22(3),
232–244.
Vanderplasschen, W., Colpaert, K., Autrique, M., Rapp,
R. C., Pearce, S., Broekaert, E., & Vandevelde, S.
(2013). Therapeutic communities for addictions: A
review of their effectiveness from a recovery-oriented
perspective. Scientific World Journal, 13, 427817.
doi:10.1155/2013/427817
Vanderwaal, F. M. (2015). Impact of motivational
interviewing on medication adherence in schizophrenia.
Issues in Mental Health Nursing, 36(11), 900–904. doi:10.
3109/01612840.2015.1058445
van Emmerik-van Oortmerssen, K., van de Glind, G., van
den Brink, W., Smit, F., Crunelle, C. L., Swets, M., &
Schoevers, R. A. (2012). Prevalence of attention-deficit
hyperactivity disorder in substance use disorder patients:
A meta-analysis and meta-regression analysis. Drug and
Alcohol Dependence, 122(1–2), 11–19. doi:10.1016/j.
drugalcdep.2011.12.007
Vega, W. A., Canino, G., Cao, Z., & Alegria, M. (2009).
Prevalence and correlates of dual diagnoses in U.S.
Latinos. Drug and Alcohol Dependence, 100(1–2), 32–38.
doi:10.1016/j.drugalcdep.2008.08.018
280 Appendix A
TIP 42
Appendix A—Bibliography
Verges, A., Jackson, K. M., Bucholz, K. K., Trull, T. J., Lane,
S. P., & Sher, K. J. (2014). Personality disorders and the
persistence of substance use disorders: A reanalysis
of published NESARC findings. Journal of Abnormal
Psychology, 123(4), 809–820. doi:10.1037/abn0000011
Vest, B. M., Hoopsick, R. A., Homish, D. L., Daws, R. C., &
Homish, G. G. (2018). Childhood trauma, combat trauma,
and substance use in National Guard and reserve soldiers.
Substance Abuse, 39(4), 452–460. doi:10.1080/08897077
.2018.1443315
Veterans Administration/Department of Defense (VA/
DoD). (2015). VA/DoD clinical practice guideline for the
management of substance use disorders. Version 3.0.
Retrieved from www.healthquality.va.gov/guidelines/MH/
sud/VADoDSUDCPGRevised22216.pdf
Veterans Administration/Department of Defense. (2017).
VA/DoD clinical practice guideline for the management
of posttraumatic stress disorder and acute stress disorder.
Version 3.0. Retrieved from www.healthquality.va.gov/
guidelines/MH/ptsd/VADoDPTSDCPGFinal012418.pdf
Vigod, S. N., Wilson, C. A., & Howard, L. M. (2016).
Depression in pregnancy. BMJ (Online), 352. doi:10.1136/
bmj.i1547
Volkert, J., Gablonski, T.-C., & Rabung, S. (2018). Prevalence
of personality disorders in the general adult population
in Western countries: Systematic review and meta-
analysis. British Journal of Psychiatry, 213(6), 709–715.
doi:10.1192/bjp.2018.202
Volpi-Abadie, J., Kaye, A. M., & Kaye, A. D. (2013).
Serotonin syndrome. Ochsner Journal, 13(4), 533–540.
Vorspan, F., Mehtelli, W., Dupuy, G., Bloch, V., & Lépine,
J. P. (2015). Anxiety and substance use disorders: Co-
occurrence and clinical issues. Current Psychiatry Reports,
17(2). doi:10.1007/s11920-014-0544-y
Vrana, C., Killeen, T., Brant, V., Mastrogiovanni, J., & Baker,
N. L. (2017). Rationale, design, and implementation of a
clinical trial of a mindfulness-based relapse prevention
protocol for the treatment of women with comorbid post
traumatic stress disorder and substance use disorder.
Contemporary Clinical Trials, 61, 108–114. doi:10.1016/j.
cct.2017.07.024
Vujanovic, A. A., Bonn-Miller, M. O., & Petry, N. M. (2016).
Co-occurring posttraumatic stress and substance use:
Emerging research on correlates, mechanisms, and
treatments—Introduction to the special issue. Psychology
of Addictive Behaviors, 30(7), 713–719. doi:10.1037/
adb0000222
Vujanovic, A. A., Meyer, T. D., Heads, A. M., Stotts, A.
L., Villarreal, Y. R., & Schmitz, J. M. (2017). Cognitive-
behavioral therapies for depression and substance use
disorders: An overview of traditional, third-wave, and
transdiagnostic approaches. American Journal of Drug
and Alcohol Abuse, 43(4), 402–415. doi:10.1080/0095299
0.2016.1199697
Vujanovic, A. A., Smith, L. J., Green, C. E., Lane, S. D.,
& Schmitz, J. M. (2018). Development of a novel,
integrated cognitive-behavioral therapy for co-occurring
posttraumatic stress and substance use disorders: A pilot
randomized clinical trial. Contemporary Clinical Trials, 65,
123–129. doi:10.1016/j.cct.2017.12.013
Wakeman, S. E., Rigotti, N. A., Chang, Y., Herman, G. E.,
Erwin, A., Regan, S., & Metlay, J. P. (2019). Effect of
integrating substance use disorder treatment into primary
care on inpatient and emergency department utilization.
Journal of General Internal Medicine. 34(6), 871–877.
doi:10.1007/s11606-018-4807-x
Walley, A. Y., Palmisano, J., Sorensen-Alawad, A.,
Chaisson, C., Raj, A., Samet, J. H., & Drainoni, M. L.
(2015). Engagement and substance dependence in a
primary care-based addiction treatment program for
people infected with HIV and people at high-risk for HIV
infection. Journal of Substance Abuse Treatment, 59,
59–66. doi:10.1016/j.jsat.2015.07.007
Walsh, F. P. & Tickle, A. C. (2013). Working towards
recovery: The role of employment in recovery from
serious mental health problems: A qualitative meta-
synthesis. International Journal of Psychosocial
Rehabilitation, 17(2) 35–49.
Walsh, K., McLaughlin, K. A., Hamilton, A., & Keyes, K. M.
(2017). Trauma exposure, incident psychiatric disorders,
and disorder transitions in a longitudinal population
representative sample. Journal of Psychiatric Research,
92, 212–218. doi:10.1016/j.jpsychires.2017.05.001
Walter, K. H., Levine, J. A., Highfill-McRoy, R. M., Navarro,
M., & Thomsen, C. J. (2018). Prevalence of posttraumatic
stress disorder and psychological comorbidities among
U.S. active duty service members, 2006–2013. Journal of
Traumatic Stress, 31(6), 837–844. doi:10.1002/jts.22337
Walton, M. T., & Hall, M. T. (2016).). The effects of
employment interventions on addiction treatment
outcomes: A review of the literature. Journal of Social
Work Practice in the Addictions, 16(4), 358–384.
Watkins, K. E., Hunter, S., Hepner, K., Paddock, S., Zhou,
A., & de la Cruz, E. (2012). Group cognitive-behavioral
therapy for clients with major depression in residential
substance abuse treatment. Psychiatric Services, 63(6),
608–611. doi:10.1176/appi.ps.201100201
Watkins, L. E., Sippel, L. M., Pietrzak, R. H., Hoff, R., &
Harpaz-Rotem, I. (2017). Co-occurring aggression and
suicide attempt among veterans entering residential
treatment for PTSD: The role of PTSD symptom clusters
and alcohol misuse. Journal of Psychiatric Research, 87,
8–14. doi:10.1016/j.jpsychires.2016.12.009
Watson, D. P., Orwat, J., Wagner, D. E., Shuman, V., &
Tolliver, R. (2013). The Housing First Model (HFM) fidelity
index: Designing and testing a tool for measuring
integrity of housing programs that serve active substance
users. Substance Abuse Treatment, Prevention, and
Policy, 8, 16. doi:10.1186/1747-597x-8-16
Appendix A 281

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
Waye, K. M., Goyer, J., Dettor, D., Mahoney, L., Samuels,
E. A., Yedinak, J. L., & Marshall, B. D. L. (2019).
Implementing peer recovery services for overdose
prevention in Rhode Island: An examination of two
outreach-based approaches. Addictive Behaviors, 89,
85–91. doi:10.1016/j.addbeh.2018.09.027
Weathers, F. W., Litz, B. T., Keane, T. M., Palmieri, P. A.,
Marx, B. P., & Schnurr, P. P. (2013). The PTSD Checklist
for DSM-5 (PCL-5) – Standard. Retrieved October 15,
2019, from www.ptsd.va.gov/professional/assessment/
documents/PCL5_Standard_form.PDF
Weaver, N., Coffey, M., & Hewitt, J. (2017). Concepts,
models and measurement of continuity of care in mental
health services: A systematic appraisal of the literature.
Journal of Psychiatric and Mental Health Nursing, 24(6),
431–450. doi:10.1111/jpm.12387
Weil, T. P. (2015). Insufficient dollars and qualified personnel
to meet United States mental health needs. Journal of
Nervous and Mental Disease, 203(4), 233–240.
Weinstein, Z. M., Wakeman, S. E., & Nolan, S. (2018).
Inpatient addiction consult service: Expertise for
hospitalized patients with complex addiction problems.
Medical Clinics of North America, 102(4), 587–601.
doi:10.1016/j.mcna.2018.03.001
Weiss, R. D., & Connery, H. S. (2001). Integrated group
therapy for bipolar disorder and substance abuse. New
York, NY: Guilford Press.
Werner, F. M., & Covenas, R. (2017). Long-term
administration of antipsychotic drugs in schizophrenia and
influence of substance and drug abuse on the disease
outcome. Current Drug Abuse Reviews, 10(1), 19–24. doi:
10.2174/1874473710666171020104524
Westmoreland, P., Krantz, M. J., & Mehler, P. S. (2016).
Medical complications of anorexia nervosa and
bulimia. American Journal of Medicine, 129(1), 30–37.
doi:10.1016/j.amjmed.2015.06.031
White, A. R. (2011). Characteristics of three consumer
cohorts in vocational rehabilitation: A comparison of
consumers with dual-diagnosis, psychiatric, or substance
use related disorders. Journal of Applied Rehabilitation
Counseling, 42(1), 15–24.
White, L. M., McGrew, J. H., Salyers, M. P., & Firmin, R.
L. (2014). Assertive community treatment for parents
with serious mental illnesses: A comparison of “parent-
sensitive” assertive community treatment teams versus
other teams. Psychiatric Rehabilitation Journal, 37(3),
251–260. doi:10.1037/prj0000050
WHO ASSIST Working Group. (2002). The Alcohol, Smoking
and Substance Involvement Screening Test (ASSIST):
Development, reliability and feasibility. Addiction, 97(9),
1183–1194.
Wile, M., & Goodwin, K. (2018, February). The costs and
consequences of disparities in behavioral health care.
National Conference of State Legislatures. Retrieved
from http://www.ncsl.org/research/health/the-costs-and-
consequences-of-disparities-in-behavioral-health-care.
aspx
Wilens, T., Zulauf, C., Martelon, M., Morrison, N. R., Simon,
A., Carrellas, N. W., . . . Anselmo, R. (2016). Nonmedical
stimulant use in college students: Association with
attention-deficit/hyperactivity disorder and other
disorders. Journal of Clinical Psychiatry, 77(7), 940–947.
doi:10.4088/JCP.14m09559
Wilens, T. E., Adler, L. A., Tanaka, Y., Xiao, F., D’Souza, D.
N., Gutkin, S. W., & Upadhyaya, H. P. (2011). Correlates
of alcohol use in adults with ADHD and comorbid
alcohol use disorders: Exploratory analysis of a placebo-
controlled trial of atomoxetine. Current Medical Research
and Opinion, 27(12), 2309–2320. doi:10.1185/03007995.
2011.628648
Wilens, T. E., & Morrison, N. R. (2011). The intersection of
attention-deficit/hyperactivity disorder and substance
abuse. Current Opinion in Psychiatry, 24(4), 280–285.
doi:10.1097/YCO.0b013e328345c956
Wilkerson, A. H., Hackman, C. L., Rush, S. E., Usdan, S.
L., & Smith, C. S. (2017). “Drunkorexia”: Understanding
eating and physical activity behaviors of weight conscious
drinkers in a sample of college students. Journal of
American College Health, 65(7), 492–501. doi:10.1080/07
448481.2017.1344848
Willison, C. (2017). Shelter from the storm: Roles,
responsibilities, and challenges in United States housing
policy governance. Health Policy, 121, 1113–1123.
Wise, E. A. (2010). Evidence-based effectiveness of a
private practice intensive outpatient program with dual
diagnosis patients. Journal of Dual Diagnosis, 6(1), 25–45.
doi:10.1080/15504260903498862
Wisner, K. L., Sit, D. K. Y., McShea, M. C., Rizzo, D. M.,
Zoretich, R. A., Hughes, C. L., … Hanusa, B. H. (2013).
Onset timing, thoughts of self-harm, and diagnoses in
postpartum women with screen-positive depression
findings. JAMA Psychiatry, 70, 490–498.
Wittchen, H. U. (2010). Screening for serious mental illness:
Methodological studies of the K6 screening scale.
International Journal of Methods in Psychiatric Research,
19(Suppl. 1), 1–3. doi:10.1002/mpr.316
Wittchen, H. U., Gloster, A. T., Beesdo-Baum, K., Fava, G.
A., & Craske, M. G. (2010). Agoraphobia: A review of the
diagnostic classificatory position and criteria. Depression
and Anxiety, 27(2), 113–133. doi:10.1002/da.20646
Wolff, N., Frueh, B., Shi, J., Gerardi, D., Fabrikant, N., &
Schumann, B. (2011). Trauma exposure and mental health
characteristics of incarcerated females self–referred
to specialty PTSD treatment. Psychiatric Services, 62,
954–958.
282 Appendix A

TIP 42
Appendix A—Bibliography
Wolff, N., Huening, J., Shi, J., & Frueh, B. C. (2014).
Trauma exposure and posttraumatic stress disorder
among incarcerated men. Journal of Urban Health, 91(4),
707–719. doi:10.1007/s11524-014-9871-x
Wood, S. R. (2013). Dual severe mental and substance use
disorders as predictors of federal inmate assaults. Prison
Journal, 93(1), 34–56. doi:10.1177/0032885512467312
Woodhead, E. L., Cowden Hindash, A., & Timko, C. (2013).
Dual diagnosis, mutual-help use, and outcomes: A
naturalistic follow-up. Journal of Dual Diagnosis, 9(2),
158–164. doi:10.1080/15504263.2013.777986
World Health Organization. (WHO). (n.d.). Constitution.
Retrieved from www.who.int/about/who-we-are/
constitution
World Health Organization. (2019). Premature death
among people with severe mental disorders. Information
Sheet. Retrieved from www.who.int/mental_health/
management/info_sheet.pdf
Worley, M. J., Tate, S. R., & Brown, S. A. (2012). Mediational
relations between 12-Step attendance, depression and
substance use in patients with comorbid substance
dependence and major depression. Addiction, 107(11),
1974–1983. doi:10.1111/j.1360-0443.2012.03943.x
Worley, M. J., Trim, R. S., Tate, S. R., Hall, J. E., & Brown, S.
A. (2010). Service utilization during and after outpatient
treatment for comorbid substance use disorder and
depression. Journal of Substance Abuse Treatment, 39(2),
124–131. doi:10.1016/j.jsat.2010.05.009
Wu, L. T., McNeely, J., Subramaniam, G. A., Brady, K. T.,
Sharma, G., VanVeldhuisen, P., . . . Schwartz, R. P. (2017).
DSM-5 substance use disorders among adult primary
care patients: Results from a multisite study. Drug
and Alcohol Dependence, 179, 42–46. doi:10.1016/j.
drugalcdep.2017.05.048
Xie, H., Drake, R. E., McHugo, G. J., Xie, L., & Mohandas, A.
(2010). The 10-year course of remission, abstinence, and
recovery in dual diagnosis. Journal of Substance Abuse
Treatment, 39(2), 132–140. doi:10.1016/j.jsat.2010.05.011
Yager, J., Devlin, M. J., Halmi, K. A., Herzog, D. B.,
Mitchell, J. E., Powers, P., & Zerbe, K. J. (June 2006).
Practice guideline for the treatment of patients with
eating disorders (3rd ed.). Retrieved from https://
psychiatryonline.org/pb/assets/raw/sitewide/practice_
guidelines/guidelines/eatingdisorders.pdf
Yager, J., & Feinstein, R. E. (2017). General psychiatric
management for suicidal patients, with remarks on
chronicity: Contending with the angel of death. Journal
of Nervous and Mental Disease, 205(6), 419–426.
doi:10.1097/nmd.0000000000000701
Yanchus, N. J., Periard, D., & Osatuke, K. (2017). Further
examination of predictors of turnover intention among
mental health professionals. Journal of Psychiatric and
Mental Health Nursing, 24(1), 41–56. doi:10.1111/
jpm.12354
Young, M. S., Barrett, B., Engelhardt, M. A., & Moore, K. A.
(2014). Six-month outcomes of an integrated assertive
community treatment team serving adults with complex
behavioral health and housing needs. Community
Mental Health Journal, 50(4), 474–479. doi:10.1007/
s10597-013-9692-5
Young, S. (2015). Understanding substance abuse counselor
turnover due to burnout: A theoretical perspective.
Journal of Human Behavior in the Social Environment,
25(6), 675–686. doi:10.1080/10911359.2015.1013658
Young, S., & Sedgwick, O. (2015). Attention deficit
hyperactivity disorder and substance misuse: An
evaluation of causal hypotheses and treatment
considerations. Expert Review of Neurotherapeutics,
15(9), 1005–1014. doi:10.1586/14737175.2015.1059756
Yu, R., Geddes, J. R., & Fazel, S. (2012). Personality
disorders, violence, and antisocial behavior: A systematic
review and meta-regression analysis. Journal of
Personality Disorders, 26(5), 775–792. doi:10.1521/
pedi.2012.26.5.775
Yudko, E., Lozhkina, O., & Fouts, A. (2007). A
comprehensive review of the psychometric properties
of the Drug Abuse Screening Test. Journal of Substance
Abuse Treatment, 32(2), 189–198. doi:10.1016/j.
jsat.2006.08.002
Yuodelis-Flores, C., & Ries, R. K. (2015). Addiction and
suicide: A review. American Journal on Addictions, 24(2),
98–104. doi:10.1111/ajad.12185
Zetterqvist, M. (2015). The DSM-5 diagnosis of nonsuicidal
self-injury disorder: A review of the empirical literature.
Child and Adolescent Psychiatry and Mental Health, 9,
31. doi:10.1186/s13034-015-0062-7
Zgierska, A., Amaza, I. P., Brown, R. L., Mundt, M., &
Fleming, M. F. (2014). Unhealthy drug use: How to screen,
when to intervene. Journal of Family Practice, 63(9),
524–530.
Zhu, H., & Wu, L. T. (2018). National trends and
characteristics of inpatient detoxification for drug use
disorders in the United States. BMC Public Health, 18(1),
1073. doi:10.1186/s12889-018-5982-8
Zilm, D. H., & Sellers, E. M. (1978). The quantitative
assessment of physical dependence on opiates. Drug and
Alcohol Dependence, 3(6), 419–428.
Zubkoff, L., Shiner, B., & Watts, B. V. (2016). Staff
perceptions of substance use disorder treatment in VA
primary care-mental health integrated clinics. Journal of
Substance Abuse Treatment, 70, 44–49. doi:10.1016/j.
jsat.2016.07.011
Zugai, J. S., Stein-Parbury, J., & Roche, M. (2015).
Therapeutic alliance in mental health nursing: An
evolutionary concept analysis. Issues in Mental Health
Nursing, 36(4), 249–257. doi:10.3109/01612840.2014.96
9795
Appendix A 283

TIP 42 Substance Use Disorder Treatment for People With Co-Occurring Disorders
Zukkoor, S. (2015). The safety of stimulant medication use
in cardiovascular and arrhythmia patients. Retrieved
from https://www.acc.org/latest-in-cardiology/
articles/2015/04/28/10/06/the-safety-of-stimulant-
medication-use-in-cardiovascular-and-arrhythmia-patients
Zulauf, C. A., Sprich, S. E., Safren, S. A., & Wilens, T.
E. (2014). The complicated relationship between
attention deficit/hyperactivity disorder and substance
use disorders. Current Psychiatry Reports, 16(3), 436.
doi:10.1007/s11920-013-0436-6
Zur, J., & Mojtabai, R. (2013). Medicaid expansion initiative
in Massachusetts: Enrollment among substance-abusing
homeless adults. American Journal of Public Health,
103(11), 2007–2013. doi:10.2105/ajph.2013.301283
Zweben, J. E., & Ashbrook, S. (2012). Mutual-help groups
for people with co-occurring disorders. Journal of Groups
in Addiction and Recovery, 7(2–4), 202–222. doi:10.1080/
1556035X.2012.705700
284 Appendix A

TIP 42
SUBSTANCE USE DISORDER TREATMENT FOR
PEOPLE WITH CO-OCCURRING DISORDERS
Appendix B—Resources
Training for Providers and
Administrators
Sources of Training in Substance Use
Disorders
Addiction-Counselors.com (www.addiction-coun-
selors.com/): A website to help professionals
and trainees find state-by-state information
about substance use disorder (SUD) counseling
requirements.
Addictions Nursing Certification Board and the
Center for Nursing Education and Testing, Inc.
Offers certification in addiction nursing.
•
Certified Addictions Registered Nurse: www.
cnetnurse.com/carn-exam
•
Certified Addictions Registered Nurse-Advanced
Practice: www.theabpm.org/become-certified/
subspecialties/addiction-medicine/
Addiction Technology Transfer Center (ATTC)
Network (https://attcnetwork.org/centers/global-
attc/products-resources-catalog): Find local ATTC.
Course offerings vary.
•
Curricula, lectures, videos, and printed
training materials available through ATTCs:
https://attcnetwork.org/centers/global-attc/
products-resources-catalog
•
Directory of ATTC trainers: https://attcnetwork.
org/trainers
Addictions Training Institute (https://
addictionstraininginstitute.com/certifications-
in-florida/): Florida-based organization offering
national certification in addiction counseling.
Maintains a listing of drug and alcohol counseling
certificates offered by state.
American Academy of Addiction Psychiatry (www.
aaap.org/clinicians/): Offers professional education
and trainee resources for psychiatrists.
American Board of Preventive Medicine
Addiction Medicine Certification (www.theabpm.
org/become-certified/subspecialties/addiction-
medicine/): Offers physicians subspecialty
certification in addiction medicine.
American Osteopathic Academy of Addiction
Medicine (www.aoaam.org/Essentials-and-
Advanced): Offers physicians basic and advanced
courses for in addiction medicine.
Hazelden Betty Ford Foundation (www.
hazeldenbettyford.org/education): Hazelden offers
training opportunities at many levels and locations,
including graduate degree and certification
programs, medical and professional education
programs, and addiction psychology training
(a clinical practicum, doctoral internships, and
postdoctoral psychology residency training).
International Certification & Reciprocity
Consortium (IC&RC) (https://
internationalcredentialing.org/): IR&RC is the
largest credentialing body in addiction prevention,
treatment, and recovery. They offer six credential
in addiction counseling, prevention, supervision,
and peer recovery. The Advanced Alcohol & Drug
Counselor certificate provides credentialing for
co-occurring disorder (CODs) services: https://
internationalcredentialing.org/creds/aadc.
NAADAC, the Association for Addiction
Professionals (www.naadac.org/): Oversees the
National Certification Commission for Addiction
Professionals, through which NAADAC is a leading
provider of national credentialing in addiction
counseling.
•
National Certified Addiction Counselor, Level I:
www.naadac.org/ncac-i
•
National Certified Addiction Counselor, Level II:
www.naadac.org/ncac-ii
•
International and State Certification
Boards: www.naadac.org/
state-international-certification-boards
285

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
National Association of Social Workers’ (NASW)
Certified Clinical Alcohol, Tobacco & Other Drugs
Social Worker (www.socialworkers.org/Careers/
Credentials-Certifications/Apply-for-NASW-Social-
Work-Credentials/Certified-Clinical-Alcohol-
Tobacco-Other-Drugs-Social-Worker): Offers social
workers certification in addiction services.
Society of Addiction Psychology (Division 50 of
the American Psychological Association (https://
addictionpsychology.org/education-training/
certification): Offers psychologists credentialing in
addiction care.
Rutgers Center of Alcohol & Substance Use
Studies (https://alcoholstudies.rutgers.edu/):
Offers professional development opportunities for
addiction counselors and professionals in related
fields, including the criminal justice system. Their
programs are accredited by multiple state and
national organizations, including the National Board
for Certified Counselors, NAADAC, and NASW.
SAMHSA
•
Technical Assistance Publication (TAP) 21,
Addiction Counseling Competencies: The
Knowledge, Skills, and Attitudes of Professional
Practice: https://store.samhsa.gov/system/files/
sma12-4171.pdf
•
TAP 21-A: Competencies for Substance Abuse
Treatment Clinical Supervisors https://store.
samhsa.gov/system/files/sma12-4243.pdf
Sources of Training in Mental Health
American Counseling Association (ACA; www.
counseling.org/continuing-education/overview):
Home study courses, learning institutes, and onsite
training.
American Psychological Association (www.
apa.org/education/ce): Home study and other
approved courses, including some COD-specific
offerings (see Continuing Education programs
under the topic “addiction”).
American Psychiatric Association (APA) (https://
education.psychiatry.org/): The organization’s
Learning Center provides online courses and
Continuing Education programs, including some
in CODs (search the catalog of courses at https://
education.psychiatry.org/Users/ProductList.aspx.
SAMHSA: Offers online mental health training in
numerous areas:
•
Disaster Technical Assistance Training: www.
samhsa.gov/dtac/education-training
•
Mental Health First Aid Training: www.samhsa.
gov/homelessness-programs-resources/
hpr-resources/mental-health-first-aid-training
Sources of Training in CODs
Addiction Technology Transfer Center (ATTC)
Network (https://attcnetwork.org/centers/global-
attc/products-resources-catalog): Find local ATTC.
Course offerings vary.
•
Curricula, lectures, videos, and printed
training materials available through ATTCs:
https://attcnetwork.org/centers/global-attc/
products-resources-catalog
•
Directory of ATTC trainers: hps://acnetwork.
org/trainers
Adler Graduate School (https://alfredadler.
edu/programs/certificate/certificate-in-COD): A
nonprofit educational institute based in Minnesota
that offers online training toward a Certificate in
Co-Occurring Substance Use and Mental Health
Disorders.
Breining Institute’s Certified Co-Occurring
Disorders Specialist (www.breining.edu/index.php/
professional-certification/certified-co-occurring-
disorders-specialist-ccds/): This higher education
institution is specifically for addiction professionals
and offers numerous courses and certifications,
including in CODs.
IC&RC (https://internationalcredentialing.
org/): IR&RC is the largest credentialing body in
addiction prevention, treatment, and recovery.
They offer six credential in addiction counseling,
prevention, supervision, and peer recovery. The
Advanced Alcohol & Drug Counselor certificate
provides credentialing for COD services: https://
internationalcredentialing.org/creds/aadc.
NAADAC, the Association for Addiction
Professionals (www.naadac.org/): Oversees the
National Certification Commission for Addiction
Professionals, through which NAADAC is a leading
286 Appendix B

TIP 42
Appendix B—Resources
provider of national credentialing in addiction
counseling. They offer two credentials in CODs:
•
Master Addiction Counselor With Co-Occurring
Disorders Component: www.naadac.org/mac
•
The Oregon Health Authority: Provides a
directory of resources on CODs to assist
counselors, administrators, and programs with
implementation and training.
•
Checklists for counselor competencies: www.
oregon.gov/oha/HSD/AMH/Pages/Co-
occurring.aspx
•
Basic Competencies: www.oregon.gov/oha/
HSD/AMH/CoOccurring%20Resources/
Basic%20Compentencies%20Checklist.pdf
•
Intermediate Competencies: www.oregon.gov/
oha/HSD/AMH/CoOccurring%20Resources/
Intermediate%20Compentencies%20CheckList.
pdf
•
Advanced Competencies: www.oregon.gov/
oha/HSD/AMH/CoOccurring%20Resources/
Advanced%20Competencies%20Checklist.pdf
Other Resources for Counselors,
Providers, and Programs
Publications
National Institute on Alcohol Abuse and
Alcoholism (NIAAA; www.niaaa.nih.gov/
publications): Offers resources, including
fact sheets, educator resources, videos, and
professional education materials.
National Institute on Drug Abuse (NIDA; www.
drugabuse.gov/publications): NIDA publishes a
wide variety of treatmentrelated materials.
•
Comorbidity: Substance Use Disorders and
Other Mental Illness: www.drugabuse.gov/
publications/drugfacts/comorbidity-substance-
use-disorders-other-mental-illnesses
•
Common Comorbidities With Substance
Use Disorders: www.drugabuse.gov/
publications/research-reports/common-
comorbidities-substance-use-disorders/
introduction
•
Criminal Justice Drug Abuse Treatment Studies
Series archive of publications and research:
www.icpsr.umich.edu/icpsrweb/NAHDAP/
series/244/studies
•
Other NIDA justice system-related research
initiatives: www.drugabuse.gov/researchers/
research-resources/criminal-justice-drug-abuse-
treatment-studies-cj-dats
National Institute of Mental Health (NIMH; www.
nimh.nih.gov/health/publications/index.shtml):
NIMH provides manuals and research reports,
including texts on disorders and conditions that
commonly co-occur with SUDs, such as depression,
anxiety, posttraumatic stress disorder (PTSD),
schizophrenia, trauma, and suicide risk.
SAMHSA (https://store.samhsa.gov/profession-
al-research-topics): Offers numerous publications
on a range of evidence-based topics in prevention,
treatment, workforce development, and more.
•
TAP 21-A, Competencies for Substance Abuse
Treatment Clinical Supervisors: https://store.
samhsa.gov/system/files/sma12-4243.pdf
•
TIP 27, Comprehensive Case Management
for Substance Abuse Treatment: https://store.
samhsa.gov/system/files/sma15-4215.pdf
•
TIP 34, Brief Interventions and Brief Therapies
for Substance Abuse: https://store.samhsa.gov/
system/files/sma12-3952.pdf
•
TIP 35, Enhancing Motivation for Change
in Substance Use Disorder Treatment:
https://store.samhsa.gov/product/
TIP-35-Enhancing-Motivation-for-Change-
in-Substance-Use-Disorder-Treatment/
PEP19-02-01-003
•
TIP 38, Integrating Substance Abuse Treatment
and Vocational Services: https://store.samhsa.
gov/system/files/sma12-4216.pdf
•
TIP 44, Substance Abuse Treatment for Adults
in the Criminal Justice System: https://store.
samhsa.gov/system/files/sma13-4056.pdf
•
TIP 45, Detoxification and Substance Abuse
Treatment: https://store.samhsa.gov/system/
files/sma15-4131.pdf
•
TIP 46, Substance Abuse: Administrative Issues
in Outpatient Treatment: https://store.samhsa.
gov/system/files/toc.pdf
Appendix B 287

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
•
TIP 47, Substance Abuse: Clinical Issues in
Intensive Outpatient Treatment: https://store.
samhsa.gov/system/files/sma13-4182.pdf
•
TIP 48, Managing Depressive Symptoms in
Substance Abuse Clients During Early Recovery:
https://www.ncbi.nlm.nih.gov/books/NBK64057/
•
TIP 50, Addressing Suicidal Thoughts and
Behaviors in Substance Abuse Treatment:
https://store.samhsa.gov/product/
TIP-50-Addressing-Suicidal-Thoughts-and-
Behaviors-in-Substance-Abuse-Treatment/
SMA15-4381
•
TIP 51, Substance Abuse Treatment: Addressing
the Specific Needs of Women: https://store.
samhsa.gov/system/files/sma15-4426.pdf
•
TIP 52, Clinical Supervision and Professional
Development of the Substance Abuse
Counselor: https://store.samhsa.gov/system/
files/sma14-4435.pdf
•
TIP 55, Behavioral Health Services for People
Who Are Homeless: https://store.samhsa.
gov/product/TIP-55-Behavioral-Health-
Services-for-People-Who-Are-Homeless/
SMA15-4734
•
TIP 57, Trauma-Informed Care in Behavioral
Health Services: https://store.samhsa.gov/
system/files/sma14-4816.pdf
•
TIP 59, Improving Cultural Competence: https://
store.samhsa.gov/system/files/sma14-4849.pdf
•
TIP 63, Medications for Opioid Use
Disorder: https://store.samhsa.gov/product/
TIP-63-Medications-for-Opioid-Use-Disorder
•
SAMHSA’s Concept of Trauma and Guidance
for a Trauma-Informed Approach: https://store.
samhsa.gov/system/files/sma14-4884.pdf
•
Screening and Assessment of Co-occurring
Disorders in the Justice System: https://store.
samhsa.gov/system/files/sma15-4930.pdf
Treatment Locators
Addiction Recovery Guide’s Treatment Locators
(www.addictionrecoveryguide.org/treatment/
treatment_locators): A listing of treatment locators,
including methadone providers.
Department of Veterans Affairs Veterans Affairs
Substance Use Disorder Program Locator (www.
va.gov/directory/guide/SUD.asp): This website
provides an interactive treatment locator for
Veterans Affairs SUD treatment programs.
Faces & Voices of Recovery Guide to
Mutual Aid Support Resources (http://
facesandvoicesofrecovery.org/resources/mutual-
aid-resources/): Offers a comprehensive listing of
12-Step and non-12-Step recovery support groups
throughout the United States and online.
Foundations Recovery Network Finding
Treatment for Drug Addiction (www.
dualdiagnosis.org/addiction-treatment/): Includes a
listing of resources to find treatment for CODs.
National Alliance of Advocates for Buprenorphine
Treatment (www.treatmentmatch.org/TM_index.
php): Offers a free, 24/7, anonymous treatment
matching service for patients and providers.
SAMHSA
•
SAMHSA’s Behavioral Health Treatment Services
Locator is a confidential and anonymous source
of information for patients and providers about
treatment facilities in the United States or
U.S. Territories for SUDs and mental disorders
(https://findtreatment.gov/).
•
Finding Quality Treatment for Substance Use
Disorders indicates how and where to locate
addiction treatment facilities and providers
(https://store.samhsa.gov/system/files/pep18-
treatment-loc.pdf).
288 Appendix B

TIP 42
Appendix B—Resources
General Resources
Condentiality
Health and Human Services’ Mental Health
Information Privacy FAQs: (www.hhs.gov/hipaa/
for-professionals/faq/mental-health/index.html):
A listing of mental health-related privacy and
confidentiality questions by topic areas (e.g.,
disclosures for coordinated care, group therapy,
disclosures to law enforcement).
National Conference of State Legislatures’
Mental Health Professionals Duty to Warn
(www.ncsl.org/research/health/mental-health-
professionals-duty-to-warn.aspx): A searchable
database of duty to warn laws for mental health
professionals by state.
SAMHSA
•
Directory of Single State Agencies for Substance
Abuse Services: https://www.samhsa.gov/
sites/default/files/single-state-agencies-
directory-08232019.pdf
•
SAMHSA’s Laws and Regulations (https://
www.samhsa.gov/about-us/who-we-are/
laws-regulations)
Supervision
Family Health International 360’s Training
Curriculum on Drug Addiction Counseling
Trainer Manual. Chapter 9: Clinical Supervision
and Support (www.fhi360.org/sites/default/files/
media/documents/Training%20Curriculum%20
on%20Drug%20Addiction%20Counseling%20
-%20Chapter%209.pdf): This training manual
offers basic guidance for addiction counseling
supervision, including case conferencing and
helping supervisees avoid burnout.
SAMHSA
•
Supervision Intervention Strategies (http://
toolkit.ahpnet.com/Supervision-Intervention-
Strategies.aspx): This section of SAMHSA’s
Recruitment and Retention Toolkit provides
indepth information about effective supervision,
including communication and motivation
strategies, conflict negotiation, and performance
appraisal.
•
TIP 52, Clinical Supervision and Professional
Development of the Substance Abuse
Counselor (https://store.samhsa.gov/system/
files/sma14-4435.pdf): This TIP provides
guidance on teaching, coaching, consulting, and
mentoring functions of clinical supervisors in
addiction treatment.
Workforce Recruitment and Retention
ATTC Network’s National Workforce Report
2017: Strategies for Recruitment, Retention, and
Development of the Substance Use Disorder
Treatment and Recovery Services Workforce
(https://attcnetwork.org/centers/network-
coordinating-office/product/national-workforce-
report-national-qualitative-report):This nationwide
survey summarizes findings on recruitment and
retention challenges facing the addiction recovery
labor force.
Behavioral Health Education Center of
Nebraska’s Retention Toolkit (www.naadac.org/
assets/2416/samhsa-naadac_workforce_bhecn_
retention_toolkit2.pdf): This toolkit was developed
to help behavioral health employers improve
retention. Although developed out of Nebraska,
the toolkit offers suggestions and resources that
can be used by any behavioral health service
organization.
SAMHSA
•
Focus on the Addiction and Mental Health
Workforce: Increasing Retention For Today and
Tomorrow: www.naadac.org/assets/2416/2016-
09-12_wf_retention_webinarslides.pdf
•
Recruitment and Retention Toolkit: http://
toolkit.ahpnet.com/Home.aspx
•
Dealing With Stress in the Workplace:
Frustration, Stress, and Compassion Fatigue/
Burnout: http://toolkit.ahpnet.com/Dealing-
with-Stress-in-the-Workplace.aspx
•
Dual Diagnosis Capability in Addiction
Treatment (DDCAT) Toolkit (version 4.0): www.
centerforebp.case.edu/client-files/pdf/ddcat-
toolkit.pdf
Appendix B 289

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
Criminal Justice System Military Populations
NIDA
American Counseling Association (ACA)
•
Criminal Justice Drug Abuse Treatment Studies
Series archive of publications and research:
www.icpsr.umich.edu/icpsrweb/NAHDAP/
series/244/studies
•
Other NIDA justice system-related research
initiatives: www.drugabuse.gov/researchers/
research-resources/criminal-justice-drug-abuse-
treatment-studies-cj-dats
SAMHSA
•
GAINS Center for Behavioral Health and Justice
Transformation: www.samhsa.gov/gains-center
•
TIP 44, Substance Abuse Treatment for Adults
in the Criminal Justice System: https://store.
samhsa.gov/system/files/sma13-4056.pdf
•
Screening and Assessment of Co-occurring
Disorders in the Justice System: https://store.
samhsa.gov/system/files/sma15-4930.pdf
Homelessness
Housing First
•
The National Alliance to End Homelessness’s
toolkit for adopting a Housing First approach:
https://endhomelessness.org/wp-content/
uploads/2009/08/adopting-a-housing-first-
approach.pdf
•
United States Interagency Council on
Homelessness’s Implementing Housing First
in Permanent Supportive Housing fact sheet:
www.usich.gov/resources/uploads/asset_library/
Implementing_Housing_First_in_Permanent_
Supportive_Housing.pdf
Pathways to Housing
•
Resources: https://pathwaystohousingpa.org/
housing-first-university/HFU-resources#
•
PA Training Institute’s training and technical
assistance: https://pathwaystohousingpa.org/
Training
SAMHSA’s Permanent Supportive Housing
Evidence-Based Practices Toolkit (https://store.
samhsa.gov/product/Permanent-Supportive-Housing-
Evidence-Based-Practices-EBP-KIT/SMA10-4510):
This toolkit describes key aspects of supportive
housing for people with mental disorders.
•
Suicide Among Veterans and the Implications
for Counselors: www.counseling.org/
docs/default-source/vistas/suicide-among-
veterans-and-the-implications-for-counselors.
pdf?sfvrsn=3803a659_11
•
Comparison of Civilian Trauma and Combat
Trauma: https://pdfs.semanticscholar.org/
eff2/8af43d3feaac7bac3cc5bb789bd4d5f100ec.
pdf
•
Counseling Addicted Veterans: What
to Know and How to Help: https://
pdfs.semanticscholar.org/9742/967aac-
815ca02c4f599b36be996d0b10d3d9.pdf
Community Anti-Drug Coalitions of America’s
Strategies for Addressing Substance Abuse
in Veteran Populations (www.cadca.org/sites/
default/files/mckesson_toolkit_1.pdf): This toolkit
was created to help programs implement addiction
prevention strategies targeting veterans in their
communities.
Department of Veterans Affairs national Center
for PTSD (www.ptsd.va.gov/):
•
Practice Recommendations for Treatment
of Veterans with Comorbid Substance Use
Disorder and Posttraumatic Stress Disorder:
www.mentalhealth.va.gov/providers/sud/docs/
SUD_PTSD_Practice_Recommendations.pdf
•
Veteran Outreach Toolkit: Preventing Veteran
Suicide is Everyone’s Business: www.va.gov/ve/
docs/outreachToolkitPreventingVeteranSuicideI-
sEveryonesBusiness.pdf
•
National Strategy for Preventing Veteran
Suicide 2018–2028: www.mentalhealth.va.gov/
suicide_prevention/docs/Office-of-Mental-
Health-and-Suicide-Prevention-National-
Strategy-for-Preventing-Veterans-Suicide.pdf
SAMHSA’s Addressing the Substance Use Disorder
Service Needs of Returning Veterans and Their
Families (www.samhsa.gov/sites/default/files/
veterans_report.pdf): This report summarizes
findings from case studies in nine states that
implemented addiction prevention and treatment
services for returning veterans and their families.
290 Appendix B

TIP 42
Appendix B—Resources
Women
The Iowa Pregnant and Postpartum Women’s
Residential Treatment Program (https://idph.
iowa.gov/substance-abuse/programs/ppw): Offers
provider resources for treating pregnant and
postpartum women with addiction, including an
intake form, follow-up strategies, a client satisfaction
survey, and documentation requirements.
SAMHSA
•
TIP 51, Substance Abuse Treatment: Addressing
the Specific Needs of Women: https://store.
samhsa.gov/system/files/sma15-4426.pdf
•
TIP 57, Trauma-Informed Care in Behavioral
Health Services: https://store.samhsa.gov/
system/files/sma14-4816.pdf
Integrated Care
Case Western Reserve’s Center for Evidence-
Based Practices. Integrated Dual Disorder
Treatment Clinical Guide (www.centerforebp.case.
edu/client-files/pdf/iddtclinicalguide.pdf): This
manual offer guidance on developing an Integrated
Dual Disorder Treatment (IDDT) program.
Milbank Memorial Fund’s Integrating Primary
Care into Behavioral Health Settings: What
Works for Individuals with Serious Mental
Illness (SMI) (www.milbank.org/wp-content/
uploads/2016/04/Integrating-Primary-Care-
Report.pdf): This report offers guidance on key
implementation techniques to help programs
treating clients with SMI learn how to integrate
their services into primary care settings.
SAMHSA’s Integrated Treatment for Co-
Occurring Disorders Evidence-Based Practices
KIT (https://store.samhsa.gov/product/Integrated-
Treatment-for-Co-Occurring-Disorders-Evidence-
Based-Practices-EBP-KIT/SMA08-4366): This toolkit
reviews the principles of integrated care for CODs
and includes video and written materials.
Assertive Community Treatment (ACT)
Case Western Reserve’s Center for Evidence-
Based Practices. Integrated Dual Disorder
Treatment Clinical Guide (www.centerforebp.case.
edu/client-files/pdf/iddtclinicalguide.pdf): This
manual offers guidance on developing an IDDT
program.
Georgia Department of Behavioral Health
& Developmental Disabilities Program Tool
Kit for ACT (https://dbhdd.georgia.gov/sites/
dbhdd.georgia.gov/files/related_files/document/
Georgia%20Toolkit%20for%20ACT%20Teams%20
docxfinal%202015.pdf): This toolkit is designed
to support programs launching ACT services and
covers such areas as staff requirements, critical
services, treatment intensity, and program capacity.
SAMHSA’s ACT for Co-Occurring Disorders
Evidence-Based Practices KIT (https://store.
samhsa.gov/product/Assertive-Community-
Treatment-ACT-Evidence-Based-Practices-EBP-KIT/
sma08-4344): This toolkit reviews the principles
of assertive community outreach for clients with
CODs and includes video and written materials.
University of Washington Program for ACT
(https://depts.washington.edu/ebpa/projects/
pact): Program resources offered here are wide
ranging and include addiction and mental
disorder assessment scales, sample staff and client
schedules, a case study, a transition assessment
tool, and other relevant client measures (e.g., stage
of change, recovery beliefs, violence risk).
Therapeutic Communities
Arkansas Department of Human Services
Therapeutic Communities Certification Manual
(https://humanservices.arkansas.gov/images/
uploads/dpsqa/DBHS_Therapuetic_Communities_
Certification_-_FINAL.pdf): Summarizes the
standards and certification requirements for
therapeutic communities (TCs) under the Arkansas
Department of Human Services, Division of
Behavioral Health Services.
Missouri Department of Corrections and
Maryville Treatment Center Therapeutic
Community Program Handbook (www.law.umich.
edu/special/policyclearinghouse/Documents/
MO%20-%20Maryville%20Treatment%20
Center%20Therapeutic%20Community%20
Program%20Handbook.pdf): Describes therapeutic
community (TC) structure, roles, procedures, and
guidelines.
Appendix B 291

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
National Institute of Justice’s Program
Profile: Modified Therapeutic Community for
Offenders With Mental Illness and Chemical
Abuse Disorders (www.crimesolutions.gov/
ProgramDetails.aspx?ID=90): Offers guidance on
adapting the TC model to people with CODs who
are involved in the criminal justice system.
NIDA Research Report, Therapeutic Communities
(https://d14rmgtrwzf5a.cloudfront.net/sites/default/
files/therapueticcomm_rrs_0723.pdf): This research
report describes the purpose of TCs, evidence of
their effectiveness, fundamental components, and
adaptations to special populations, including people
experiencing homelessness, women, and people in
the criminal justice system.
University of Delaware Center for Drug and
Alcohol Studies. Therapeutic Community
Treatment Methodology: Treating Chemically
Dependent Criminal Offenders in Corrections
(www.cdhs.udel.edu/content-sub-site/Documents/
CDHS/CTC/Treating%20Chemically%20
Dependent%20Criminal%20Offenders%20in%20
Corrections.pdf): This slide deck offers material on
the use of TCs in criminal justice settings, including
relapse prevention, use and misuse of therapeutic
tools, and staff roles and functions.
Suicide Prevention
ACA
•
Suicide Prevention Tip Sheet: www.counseling.
org/docs/default-source/Communications-/
suicide-prevention-final.pdf?sfvrsn=2
•
Counselor Training in Suicide Assessment,
Prevention, and Management: www.
counseling.org/docs/default-source/vistas/
article_65d15528f16116603abcacff0000bee5e7.
pdf?sfvrsn=4f43482c_6
•
Developing Clinical Skills in Suicide Assessment,
Prevention, and Treatment: www.counseling.org/
publicaons/frontmaer/72861-fm.pdf
APA’s Practice Guidelines (2016)
Recommendations Regarding Assessment
of Suicide As Part of the Initial Psychiatric
Assessment (https://stopasuicide.org/assets/docs/
APAPracticeGuidelines.pdf): A checklist of items
to assess in determining suicide risk and history
during an initial psychiatric assessment.
International Association for Suicide Prevention’s
Guidelines for Suicide Prevention (www.iasp.info/
suicide_guidelines.php): A summary of prevention
and risk-reduction strategies for behavioral health
service providers.
National Suicide Prevention Lifeline (https://
suicidepreventionlifeline.org/ or 1-800-273-8255):
Funded by SAMHSA, this national network of local
crisis centers offer free and confidential support
to people in suicidal crisis or emotional distress 24
hours a day, 7 days a week. Professional initiatives
to promote public knowledge of suicide prevention
are also provided: https://suicidepreventionlifeline.
org/professional-initiatives/
SAMHSA
•
Suicide Prevention Resource Center: www.sprc.
org/
•
Suicide Assessment Five-Step Evaluation and
Triage for Mental Health Professionals: https://
store.samhsa.gov/system/files/sma09-4432.pdf
•
TIP 50, Addressing Suicidal Thoughts and
Behaviors in Substance Abuse Treatment:
https://store.samhsa.gov/product/
TIP-50-Addressing-Suicidal-Thoughts-and-
Behaviors-in-Substance-Abuse-Treatment/
SMA15-4381
•
Video companion to TIP 50, Addressing
Suicidal Thoughts and Behaviors in Substance
Abuse Treatment: www.youtube.com/
watch?v=1n2QZlheuzc&feature=youtu.be
Trauma
SAMHSA’s TIP 57, Trauma-Informed Care in
Behavioral Health Services (https://store.samhsa.
gov/system/files/sma14-4816.pdf): Includes
guidance for working with behavioral health clients
with trauma and for implementing trauma-informed
programming.
Veterans Affairs National Center for PTSD (www.
ptsd.va.gov/): The National Center for PTSD is one
of the world’s largest repositories of PTSD-related
education and resources, designed to improve
patient care, increase provider knowledge, and
help clients and families better understand this
condition. Many of the Center’s publications, tools,
292 Appendix B

TIP 42
Appendix B—Resources
and resources are aimed at military personnel (e.g.,
deployment measures) but many are useful for and
applicable to civilian populations as well.
Veterans Affairs/Department of Defense Clinical
Practice Guideline for the Management of
Posttraumatic Stress Disorder and Acute Stress
Disorder (www.healthquality.va.gov/guidelines/
MH/ptsd/VADoDPTSDCPGFinal012418.pdf):
Evidence-based guidelines for treating trauma and
extreme stress in military populations, including
treatment recommendations and algorithms.
Medication Management
SAMHSA
•
TIP 63, Medications for Opioid Use Disorder
(https://store.samhsa.gov/product/TIP-63-
Medications-for-Opioid-Use-Disorder): A
compendium of the latest evidence in support
of Food and Drug Administration (FDA)-
approved pharmacotherapy for opioid use
disorder (OUD).
•
Medication for the Treatment of Alcohol Use
Disorder: A Brief Guide (https://store.samhsa.
gov/system/files/sma15-4907.pdf): Offers a
succinct summary of medications for AUD,
including how to discuss them with clients,
integrating medication into treatment, and
medications for people with CODs.
APA’s Practice Guideline for the Pharmacological
Treatment of Patients With Alcohol Use Disorder
(https://psychiatryonline.org/doi/pdf/10.1176/appi.
books.9781615371969): Clinical practice guideline
to inform the use of mediation for AUD.
National Library of Medicine’s Drug Information
Portal (https://druginfo.nlm.nih.gov/drugportal/):
A searchable database organized by medication
name and category.
FDA’s Medication Guides Database (www.
accessdata.fda.gov/scripts/cder/daf/index.
cfm?event=medguide.page): A searchable index of
FDA-approved medications.
NIMH’s Mental Health Medications (www.nimh.
nih.gov/health/topics/mental-health-medications/
index.shtml): A brief summary of psychotropic
medication, their uses, and their side effects.
University of Washington’s Commonly Prescribed
Psychotropic Medications (https://aims.
uw.edu/resource-library/commonly-prescribed-
psychotropic-medications): A printable factsheet of
common antidepressant, antianxiety, antipsychotic,
and mood stabilizing medication.
Client and Family Resources
Organizations
Hazelden Betty Ford Foundation (www.
hazeldenbettyford.org/recovery/families-friends):
Includes support and tools for clients, families, and
friends.
Learn to Cope (www.learn2cope.org/): A secular
mutual-support group that offers education,
resources, and peer support for families of people
with SUDs (although primarily focused on OUD).
They also maintain an online forum, but groups are
only available in a few states.
Legal Action Center (www.lac.org): Offers
information about the rights of people with
criminal records, HIV/AIDS, and SUDs.
Mental Health America (www.
mentalhealthamerica.net/): A nonprofit community-
based organization that aims to improve public
knowledge of mental disorders and enhance
prevention and treatment strategies. It includes
over 200 affiliates in 41 states, 6,500 affiliate staff,
and over 10,000 volunteers.
National Alliance on Mental Illness (NAMI; www.
nami.org): The largest grassroots educational, peer
support, and mental health advocacy organization
in the United States. Founded in 1979 by a
group of family members of people with mental
disorders, NAMI has developed into an association
of hundreds of local affiliates, state organizations,
and volunteers.
National Empowerment Center (https://power2u.
org/): The Center has an extensive resource
listing including a directory of consumer-run
organizations, peer support, and webinars.
Appendix B 293

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
National Suicide Prevention Lifeline (https://
suicidepreventionlifeline.org/ or 1-800-273-8255):
Funded by SAMHSA, this national network of local
crisis centers offer free and confidential support
to people in suicidal crisis or emotional distress 24
hours a day, 7 days a week.
Parents of Addicted Loved Ones (https://
palgroup.org/): A secular support group for parents
who have a child with an SUD. They only have
meetings in some state
s but also host telephone
meetings.
Mutual-Support Programs
Alcoholics Anonymous (AA; www.aa.org): Offers
group meetings for people who have problems
relating to drinking and wish to stop. AA sponsors
offer members personal support from experienced
individuals.
Al-Anon Family Groups (www.al-anon.org):
Group meetings in which friends and families
of people with substance use problems share
experiences and learn to apply Al-Anon principles
to their situations. Sponsorship helps members
get personal support from more experienced
individuals in the program.
Cocaine Anonymous (https://ca.org/): A mutual-
support program for people with cocaine use
disorder. Cocaine Anonymous follows the 12-Step
tradition and offers meetings worldwide.
Dual Disorders Anonymous ([847] 781-1553): A
mutual-support program with 48 groups in several
states (more than half in Illinois). This program is
modeled after AA.
Dual Diagnosis Anonymous of Oregon (www.
ddaoforegon.com/). This mutual-support program
uses AA’s 12 Step plus five more focused on CODs.
The organization has chapters in several states and
in Canada.
Dual Recovery Anonymous (www.draonline.org/):
This mutual-support program follows 12-Step
principles to support people in recovery from
addiction and emotional/mental illness. It focuses
on preventing relapse and actively improving
quality of members’ lives via a mutual-support
community.
Dual Diagnosis Recovery Network (www.
dualdiagnosis.org/resource/ddrn/): Part of
Foundations Recovery Network, the Dual Diagnosis
Recovery Network is an advocacy group for people
with CODs. They offer information on mutual-
support programs, outreach, and education.
Emotions Anonymous (http://emotionsanonymous.
org/): A 12-Step fellowship based on AA for people
with any emotional difficulties (not only clinical
mental disorders). Groups are located in more than
30 countries, with more than 600 active groups,
including Skype and phone meetings.
Faces and Voices of Recovery (http://
facesandvoicesofrecovery.org/): Offers recovery
stories, news and events information, publications,
and webinars.
Heroin Anonymous (www.heroinanonymous.org):
A nonprofit fellowship of individuals in recovery
from heroin addiction and committed to helping
each other stay sober. This organization holds local
support meetings, a directory of which can be
found on their website.
Narcotics Anonymous (NA; www.na.org/): A
global, community-based organization with
a multilingual, multicultural membership that
supports recovery from addiction through a
12-Step program, including regular attendance
at group meetings. The group offers an ongoing
support network for maintaining a drug-free
lifestyle. NA does not focus on any particular
addictive substance.
Nar-Anon Family Groups (www.nar-anon.org/):
Group meetings in which friends and family of
people with drug use problems can share their
experiences and learn to apply the 12-Steps
Nar-Anon program to their lives. Nar-Anon offers
individualized support from experienced members
acting as sponsors.
National Mental Health Consumers’ Self-Help
Clearinghouse (www.mhselfhelp.org/): The
organization has developed and offers a resource
kit providing the names and contacts for resources
and information on substance addictions, co-
occurring disorders, services, and mutual help
support.
294 Appendix B

TIP 42
Appendix B—Resources
Pills Anonymous (www.pillsanonymous.org): A
12-Step mutual-support fellowship that holds
regular meetings in which individuals in recovery
from addiction to medication can share their
experiences, build their strengths, and offer hope
for recovery to one another.
Recoveries Anonymous (www.r-a.org/): A 12-Step
mutual fellowship that welcomes people with
a broad range of problems, from addictions,
to mental disorders, to “problem behaviors”
(e.g., compulsive spending, risk-taking, suicidal
behaviors).
Schizophrenia Alliance (https://sardaa.org/
schizophrenia-alliance/sa-group-locations/):
Operating under the auspices of the Schizophrenia
and Related Disorders Alliance of America, this
12-Step mutual-support program offers information
and fellowship for people with schizophrenia
or other psychotic disorders, including bipolar
disorder. They hold meetings among 150 groups
throughout 31 states.
Secular Organizations for Sobriety (www.
sossobriety.org/): A nonprofit, nonreligious network
of autonomous, nonprofessional local groups that
help people achieve and maintain abstinence from
alcohol and drug addiction.
Self-Management and Recovery Training (SMART
Recovery; www.smartrecovery.org/): SMART
Recovery a self-empowering addiction recovery
support group that teaches science-based tools
for addiction recovery and grants access to an
international recovery community of mutual-
support groups.
Women for Sobriety (https://womenforsobriety.
org/): An abstinence-based mutual-support
program that helps women find individual paths
to recovery by acknowledging their unique needs
in recovery. It is not affiliated with other recovery
organizations. It offers tools to help women
in recovery develop coping skills focused on
emotional growth, spiritual growth, self-esteem,
and a healthy lifestyle.
Publications and Other Resources
American Society of Addiction Medicine (www.
asam.org/resources/patient-resources): Includes
a treatment locator, listing of client and family
support group, and a treatment guideline about
opioid addiction.
Foundations Recovery Network Articles and
Publications (www.dualdiagnosis.org/resource/):
Offers material on COD treatment, gender-specific
concerns, family functions, mutual support, advocacy,
and success stories.
National Institute on Alcohol Abuse and
Alcoholism (www.rethinkingdrinking.niaaa.nih.gov/
help-links/): Provides links to patient and family
education, help lines, and other recovery resources
NIDA (www.drugabuse.gov/nidamed-medical-
health-professionals/tool-resources-your-practice/
patient-materials): Patient materials include online
tools, booklets, and fact sheets about substance
misuse, prevention, and treatment.
SAMHSA (https://store.samhsa.gov/): Provides
patient and family educational tools about SUD
and co-occurring mental illness.
•
No Longer Alone. A Story About Alcohol,
Drugs, Depression, and Trauma: https://store.
samhsa.gov/system/files/sma13-4781eng.pdf
•
People Recover. An Educational Comic Book on
Co-Occurring Disorders: https://store.samhsa.
gov/product/people-recover/sma13-4712
•
Should You Talk to Someone About a Drug,
Alcohol, or Mental Health Problem? (https://
store.samhsa.gov/product/Should-You-Talk-to-
Someone-About-a-Drug-Alcohol-or-Mental-
Health-Problem-/sma15-4585). This publication
is available in English, Cambodian, Chinese,
Russian, and Vietnamese.
•
Steve’s Path to a Better Life: Alcohol and
Depression: https://store.samhsa.gov/system/
files/sma16-5013.pdf
Appendix B 295

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
Online Boards and Chat Rooms
12-Step forums: Some AA meetings are available
online, each with their own view of medication.
•
The AA online intergroup directory lists
numerous online AA meetings: www.aa-
intergroup.org/
Bipolar World Online (https://bipolarworld.org/):
This online community includes support chat, an
online forum, online journals, and articles about
bipolar disorder.
Facebook forums and groups: A handful of COD
and addiction recovery organizations maintain
a presence on Facebook because of the ease of
creating online mutual-support and chat groups.
•
Dual Diagnosis Co-Occurring Mental
Illness and Substance Disorders
Treatment Programs: www.facebook.com/
FirstDualDiagnosisTreatmentandPrograms1984/
•
Recovery Group for Dual Diagnosis: www.
facebook.com/events/139669280229645/
•
Secular Organizations for Sobriety: www.
facebook.com/groups/251215211975/
LifeRing Secular Recovery Dual Diagnosis
Recovery Online Support Groups (https://www.
lifering.org/post/lifering-offers-dual-diagnosis-
recovery-support-group-online).
Mental Health America Online Support
Groups (https://www.inspire.com/groups/
mental-health-america/).
SMART Recovery Online Forum (www.
smartrecovery.org/community/forum.php).
Mobile Apps
Foundations Recovery Network (www.dualdiag-
nosis.org/apps-for-addiction-recovery-and-mental-
health/): maintains a listing of COD, SUD, and
mental illness-related mobile apps.
296 Appendix B
Appendix C—Provider Forms, Measures,
and Tools
Biopsychosocial Intake Forms
A sample assessment form is included in a
PDF that is linked to the Providers Clinical
Support System (PCSS) website. Go to
https://30qkon2g8eif8wrj03zeh041-wpengine.
netdna-ssl.com/wp-content/uploads/2017/09/
Intake-Assessment-3.pdf and see pages 23–32 of
the PDF.
Suicide and Safety Screening and
Assessment Tools
Columbia-Suicide Severity Rating Scale (http://
cssrs.columbia.edu/the-columbia-scale-c-ssrs/
cssrs-for-communities-and-healthcare/#filter=.
general-use.english): Numerous versions of this
screener are available for different populations,
including adults, adolescents, and people with
cognitive difficulties. Versions are also available for
certain settings, including general care settings,
military settings, schools, and military settings.
Furthermore, this screener can be downloaded in
both English and Spanish.
HUMILIATION, AFRAID, RAPE,
AND KICK
TIP 42
SUBSTANCE USE DISORDER TREATMENT FOR
PEOPLE WITH CO-OCCURRING DISORDERS
• H: Humiliation-Within the last year, have you
been humiliated or emotionally abused in
other ways by your partner or your ex-partner?
• A: Afraid-Within the last year, have you been
afraid of your partner or ex-partner?
• R: Rape-Within the last year, have you been
raped or forced to have any kind of sexual
activity by your partner or ex-partner?
• K: Kick-Within the last year, have you been
kicked, hit, slapped, or otherwise physically
hurt by your partner or ex-partner?
Source: Sohal, Eldridge, & Feder (2007). Adapted
from material distributed under the terms of the
Creative Commons Attribution License (https://
creativecommons.org/licenses/by/2.0/).
Mental Disorder Screening and
Assessment Tools
Addiction Severity Index: This is a semistructured
interview that takes approximately an hour to
administer. Information on administration and
scoring can be found at https://pubs.niaaa.nih.gov/
publications/assessingalcohol/InstrumentPDFs/04_
ASI.pdf. The interview is available for free
online, including here: (http://adai.washington.
edu/instruments/pdf/addiction_severity_index_
baseline_followup_4.pdf).
297

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
MENTAL HEALTH SCREENING FORMIII
Please circle “yes” or “no” for each question.
1. Have you ever talked to a psychiatrist, psychologist, therapist, social worker, or counselor
about an emotional problem?
Yes No
2. Have you ever felt you needed help with your emotional problems, or have you had
people tell you that you should get help for your emotional problems?
Yes No
3. Have you ever been advised to take medication for anxiety, depression, hearing voices, or
for any other emotional problem?
Yes No
4. Have you ever been seen in a psychiatric emergency room or been hospitalized for
psychiatric reasons?
Yes No
5. Have you ever heard voices no one else could hear or seen objects or things which others
could not see?
Yes No
6. (a) Have you ever been depressed for weeks at a time, lost interest or pleasure in most
activities, had trouble concentrating and making decisions, or thought about killing
Yes No
yourself?
(b) Did you ever attempt to kill yourself?
Yes No
7. Have you ever had nightmares or flashbacks as a result of being involved in some
traumatic/terrible event? For example, warfare, gang fights, fire, domestic violence, rape,
incest, car accident, being shot or stabbed?
Yes No
8. Have you ever experienced any strong fears? For example, of heights, insects, animals, dirt,
attending social events, being in a crowd, being alone, being in places where it may be
hard to escape or get help?
Yes No
9. Have you ever given in to an aggressive urge or impulse, on more than one occasion, that
resulted in serious harm to others or led to the destruction of property?
Yes No
10. Have you ever felt that people had something against you, without them necessarily
saying so, or that someone or some group may be trying to influence your thoughts or
behavior?
Yes No
11. Have you ever experienced any emotional problems associated with your sexual interests,
your sexual activities, or your choice of sexual partner?
Yes No
12. Was there ever a period in your life when you spent a lot of time thinking and worrying
about gaining weight, becoming fat, or controlling your eating? For example, by
repeatedly dieting or fasting, engaging in much exercise to compensate binge eating,
taking enemas, or forcing yourself to throw up?
Yes No
13. Have you ever had a period of time when you were so full of energy and your ideas came
very rapidly, when you talked nearly nonstop, when you moved quickly from one activity
to another, when you needed little sleep, and when you believed you could do almost
anything?
Yes No
14. Have you ever had spells or attacks when you suddenly felt anxious, frightened, or
uneasy to the extent that you began sweating, your heart began to beat rapidly, you
were shaking or trembling, your stomach was upset, or you felt dizzy or unsteady, as if
you would faint?
Yes No
Continued on next page
298 Appendix C

TIP 42
Appendix C—Provider Forms, Measures, and Tools
Continued
15. Have you ever had a persistent, lasting thought or impulse to do something over and over
that caused you considerable distress and interfered with normal routines, work, or social
relations? Examples would include repeatedly counting things, checking and rechecking
on things you had done, washing and rewashing your hands, praying, or maintaining a
very rigid schedule of daily activities from which you could not deviate.
Yes No
16. Have you ever lost considerable sums of money through gambling or had problems at
work, in school, or with your family and friends as a result of your gambling?
Yes No
17. Have you ever been told by teachers, guidance counselors, or others that you have a
special learning problem?
Yes No
Instructions and scoring information are available online. (https://idph.iowa.gov/Portals/1/Files/SubstanceAbuse/jackson_
mentalhealth_screeningtool.pdf).
Source: Carroll & McGinley (2000). Reprinted with permission.
Substance Use/Misuse Screening
and Assessment Tools
National Institute on Drug Abuse (NIDA)-
Modified Alcohol, Smoking, and Substance
Involvement Screening Test (ASSIST) (www.
drugabuse.gov/nmassist/): NIDA developed
an abbreviated version of the World Health
Organization’s (WHO) ASSIST tool called the NIDA-
Modified ASSIST that can be completed online.
PCSS – Clinical Tools: https://pcssnow.org/
resources/clinical-tools
ALCOHOL USE DISORDERS IDENTIFICATION TEST
PATIENT: Because alcohol use can affect your health and can interfere with certain medications and
treatments, it is important that we ask some questions about your use of alcohol. Your answers will remain
confidential, so please be honest.
For each question in the chart below, place an X in one box that best describes your answer.
NOTE: In the U.S., a single drink serving contains about 14 grams of ethanol or “pure” alcohol. Although
the drinks below are different sizes, each one contains the same amount of pure alcohol and counts as a
single drink:
12 fl oz. of
beer
(about 5%
alcohol)
8-9 fl oz. of
malt liquor
(about 7%
alcohol)
5 fl oz. of
wine
(about 12%
alcohol)
1.5 fl oz. of
hard liquor
(about 40%
alcohol)
= = =
QUESTIONS 0 1 2
1. How often do you have a
drink containing alcohol?
Never Monthly or
less
2 to 4 times
a month
2 to 3 times
a week
4 or more
times a
week
Continued on next page
3 4
Appendix C 299

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
Continued
2. How many drinks
containing alcohol do
you have on a typical day
when you are drinking?
1 or 2 3 or 4 5 or 6 7 to 9 10 or more
3. How often do you have
5 or more drinks on one
occasion?
Never Less than
monthly
Monthly Weekly Daily or
almost
daily
4. How often during the last
year have you found that
you were not able to stop
drinking once you had
started?
Never Less than
monthly
Monthly Weekly Daily or
almost
daily
5. How often during the
last year have you failed
to do what was normally
expected of you because
of drinking?
Never Less than
monthly
Monthly Weekly Daily or
almost
daily
6. How often during the last
year have you needed a
first drink in the morning
to get yourself going after
a heavy drinking session?
Never Less than
monthly
Monthly Weekly Daily or
almost
daily
7. How often during the
last year have you had a
feeling of guilt or remorse
after drinking?
Never Less than
monthly
Monthly Weekly Daily or
almost
daily
8. How often during the
last year have you been
unable to remember
what happened the night
before because of your
drinking?
Never Less than
monthly
Monthly Weekly Daily or
almost
daily
9. Have you or someone
else been injured
because of your
drinking?
No Yes, but not
in the last
year
Yes, during
the last
year
10. Has a relative, friend,
doctor, or other health
care worker been
concerned about your
drinking or suggested
you cut down?
No Yes, but not
in the last
year
Yes, during
the last
year
Total
Source: Babor et al. (2001).
300 Appendix C

TIP 42
□ □
Appendix C—Provider Forms, Measures, and Tools
THE ALCOHOL USE DISORDERS IDENTIFICATION TEST CONCISE
How often do you have a drink containing alcohol?
□ Never □ 2-3 times a week
□ Monthly or less □ 4 or more times a week
□ 2-4 times a month
How many standard drinks containing alcohol do you have on a typical day?
□ 1 or 2 □ 7 to 9
□ 3 to 4 □
10 or more
□ 5 to 6
How often do you have six or more drinks on one occassion?
□ Daily or almost daily Less than monthly
□ Weekly
□
□
Never
□ Monthly
The AUDIT-C tool, along with scoring instructions and further information, is available online at https://www.queri.
research.va.gov/tools/alcohol-misuse/alcohol-faqs.cfm#3.
Source: Bush, Kivlahan, McDonell, Fihn, & Bradley (1998). Reprinted from material in the public domain.
MICHIGAN ALCOHOLISM SCREENING TEST
Yes No Points
0. Do you enjoy drinking now and then?
1. * Do y
ou feel you are a normal drinker? (“normal” - drink as much or less than most
people)
□ □ (2)
2. Have you ever awakened the morning after some drinking the night before and
found that you could not remember a part of the evening?
□ □ (2)
□ □ (1)
□ □ (2)
□ □ (1)
□ □ (2)
□ □ (2)
□ □ (5)
□ □ (1)
3. Does your wife, husb
and, a parent, or other near relative ever worry or complain
about your drinking?
4. * Can y
ou stop drinking without a struggle after one or two drinks?
5. Do you ev
er feel guilty about your drinking?
6. * Do fr
iends or relatives think you are a normal drinker?
7. * Are you able t
o stop drinking when you want to?
8. Hav
e you ever attended a meeting of Alcoholics Anonymous (AA)?
9. Have y
ou gotten into physical fights when drinking?
Continued on next page
Appendix C 301

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
Continued
10. Has your drinking ever created problems between you and your wife, husband, a
parent, or other relative?
□ □ (2)
□ □ (2)
□ □ (2)
□ □ (2)
□ □ (2)
11. Has your wif
e, husband (or other family members) ever gone to anyone for help
about your drinking?
12. Ha
ve you ever lost friends because of your drinking?
13. Hav
e you ever gotten into trouble at work or school because of drinking?
14. Ha
ve you ever lost a job because of drinking?
15. Hav
e you ever neglected your obligations, your family, or your work for two or more
days in a row because you were drinking?
□ □ (2)
□ □ (1)
□ □ (2)
□ □ (2)
□ □ (5)
□ □ (5)
□ □ (2)
□ □ (2)
□ □ (2)
□ □ (2)
16. Do y
ou drink before noon fairly often?
17. Ha
ve you ever been told you have liver trouble? Cirrhosis?
18. *
* After heavy drinking have you ever had Delirium Tremens (D.T.s) or severe
shaking, or heard voices, or seen things that are really not there?
19. Ha
ve you ever gone to anyone for help about your drinking?
20. Ha
ve you ever been in a hospital because of drinking?
21. Hav
e you ever been a patient in a psychiatric hospital or on a psychiatric ward
of a general hospital where drinking was part of the problem that resulted in
hospitalization?
22. Ha
ve you ever been seen at a psychiatric or mental health clinic or gone to any
doctor, social worker, or clergyman for help with any emotional problem, where
drinking was part of the problem?
23. **
* Have you ever been arrested for drunk driving, driving while intoxicated, or
driving under the influence of alcoholic beverages? (if YES, How many times?__)
24. *
** Have you ever been arrested, or taken into custody even for a few hours,
because of other drunk behavior? (if YES, How many times?__)
* Alc
oholic response is negative
** 5 points for Delirium Tremens
*** 2 points for each arrest
SCORING
Add up the points for every question you answered with YES, for Q23 and Q24 multiply
the number of times by points
0 - 3 No apparent problem
4 Early or middle problem drinker
5 or more Problem drinker (Alcoholic)
This instrument is available online at www.ncbi.nlm.nih.gov/books/NBK64829.
Source: Adapted from Selzer (1971).
302 Appendix C

TIP 42
Yes No
Yes No
Yes No
Yes No
Yes No
Yes No
Yes No
Yes No
Yes No
Yes No
Yes No
Yes No
Appendix C—Provider Forms, Measures, and Tools
SIMPLE SCREENING INSTRUMENT FOR SUBSTANCE ABUSE
During the past 6 months:
1. Have you used alcohol or other drugs? (such as wine, beer, hard liquor, pot, coke, heroin
or other opiates, uppers, downers, hallucinogens, or inhalants) Yes No
Yes No
Yes No
Yes No
2. Have you felt that you use too much alcohol or other drugs?
3. Have you tried to cut down or quit drinking or using drugs?
4. Have you gone to anyone for help because of your drinking or drug use?
(such as Alcoholics Anonymous, Narcotics Anonymous, Cocaine Anonymous,
counselors, or a treatment program)
5. Have you had any of the following?
Put a check mark next to any problems you have experienced.
□ Blackouts or other periods of memory loss?
□ Injury to your head after drinking or using drugs?
□ Convulsions or delirium tremens (DTs)?
□ Hepatitis or other liver problems?
□ Felt sick, shaky, or depressed when you stopped drinking or using drugs?
□ Felt “coke bugs” or a crawling feeling under the skin after you stopped
using drugs?
□ Injury after drinking or using?
□ Used needles to shoot drugs?
Circle “yes” if at least one of the eight items above is checked
6. Has your drinking or other drug use caused problems between you and your family
or friends?
7. Has your drinking or other drug use caused problems at school or at work?
8. Have you been arrested or had other legal problems? (such as bouncing bad checks,
driving while intoxicated, theft, or drug possession)
9. Have you lost your temper or gotten into arguments or fights while drinking or
using drugs?
10. Do you need to drink or use drugs more and more to get the effect you want?
11. Do you spend a lot of time thinking about or trying to get alcohol or other drugs?
12. When drinking or using drugs, are you more likely to do something you wouldn’t
normally do, such as break rules, break the law, sell things that are important to you, or
have unprotected sex with someone?
13. Do you feel bad or guilty about your drinking or drug use?
The next questions are about lifetime experiences.
14. Have you ever had a drinking or other drug problem?
15. Have any of your family members ever had a drinking or drug problem?
16. Do you feel that you have a drinking or drug problem now?
Source: Center for Substance Abuse Treatment (CSAT; 1994). Reprinted from material in the public domain.
Appendix C 303

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
Substance Withdrawal Screening Tools
CLINICAL INSTITUTE NARCOTIC ASSESSMENT SCALE FOR WITHDRAWAL
SYMPTOMS
Parameters Based on Questions
and Observation
Findings Points
1. Abdominal changes:
Do you have any pains in your
abdomen? Crampy abdominal
pain, diarrhea, active bowel
sounds.
No abdominal complaints, normal
bowel sound. Reports waves of
crampy abdominal pain.
0 1 2
2. Changes in temperature: Do
you feel hot or cold? Clammy to
touch. Uncontrolled shivering.
None reported. Reports feeling
cold, hands cold and clammy to
touch. Uncontrolled shivering.
0 1 2
3. Nausea and vomiting:
Do you feel sick in your stomach?
Have you vomited?
No nausea or vomiting. Mild
nausea; no retching or vomiting.
Intermittent nausea with dry
heaves. Constant nausea;
frequent dry heaves and/or
vomiting.
0 2 4 6
4. Muscle aches: Do you have any
muscle cramps?
No muscle aching reported, arm
and neck muscles soft at rest.
Mild muscle pains. Reports severe
muscle pains, muscles in legs,
arms or neck in constant state of
contraction.
0 1 3
Parameters Based on
Observation Alone
Findings Points
5. Goose flesh None visible. Occasional goose
flesh but not elicited by touch;
not permanent. Prominent goose
flesh in waves and elicited by
touch. Constant goose flesh over
face and arms.
0 1 2 3
6. Nasal congestion No nasal congestion or sniffling.
Frequent sniffling. Constant
sniffling, watery discharge.
0 1 2
7. Restlessness Normal activity. Somewhat more
than normal activity; moves legs
up and down; shifts position
occasionally. Moderately fidgety
and restless; shifting position
frequently. Gross movement
most of the time or constantly
thrashes about.
0 1 2 3
Continued on next page
304 Appendix C

TIP 42Appendix C—Provider Forms, Measures, and Tools
Continued
8. Tremor None. Not visible but can be felt
fingertip to fingertip. Moderate
with patient’s arm extended.
Severe even if arms not extended.
0 1 2 3
9. Lacrimation None. Eyes watering; tears at
corners of eyes. Profuse tearing
from eyes over face.
0 1 2
10. Sweating No sweat visible. Barely
perceptible sweating; palms
moist. Beads of sweat obvious on
forehead. Drenching sweats over
face and chest.
0 1 2 3
11. Yawning None. Frequent yawning.
Constant uncontrolled yawning.
0 1 2
TOTAL SCORE Sum of points for all 11 parameters
Minimum score = 0, Maximum score = 31. The higher the score, the more severe the withdrawal syndrome. Percent of
maximal withdrawal symptoms = total score/31 x 100%.
Source: Peachey & Lei (1988). Adapted with permission of John Wiley and Sons Inc.; permission conveyed through
Copyright Clearance Center, Inc.
CLINICAL INSTITUTE WITHDRAWAL ASSESSMENT OF ALCOHOL SCALE, REVISED
Patient: _________ Date: ______ Time: ________ (24 hour clock, midnight = 00:00)
Pulse or heart rate, taken for one minute: _______ Blood pressure: ______
NAUSEA AND VOMITING – Ask “Do you feel
sick to your stomach? Have you vomited?”
Observation.
0 no nausea and no vomiting
1 mild nausea with no vomiting
2
3
4 intermittent nausea with dry heaves
5
6
7 constant nausea, frequent dry heaves
and vomiting
TACTILE DISTURBANCES – Ask “Have you any
itching, pins and needles sensations, any burning, any
numbness, or do you feel bugs crawling on or under
your skin?” Observation.
0 none
1 very mild itching, pins and needles, burning
or numbness
2 mild itching, pins and needles, burning or numbness
3 moderate itching, pins and needles, burning
or numbness
4 moderately severe hallucinations
5 severe hallucinations
6 extremely severe hallucinations
7 continuous hallucinations
Continued on next page
Appendix C 305

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
Continued
TREMOR – Arms extended and fingers
spread apart. Observation.
0 no tremor
1 not visible, but can be felt fingertip
to fingertip
2
3
4 moderate, with patient’s arms extended
5
6
7 severe, even with arms not extended
AUDITORY DISTURBANCES – Ask “Are you more aware
of sounds around you? Are they harsh? Do they frighten
you? Are you hearing anything that is disturbing to
you? Are you hearing things you know are not there?”
Observation.
0 not present
1 very mild harshness or ability to frighten
2 mild harshness or ability to frighten
3 moderate harshness or ability to frighten
4 moderately severe hallucinations
5 severe hallucinations
6 extremely severe hallucinations
7 continuous hallucinations
PAROXYSMAL SWEATS – Observation.
0 no sweat visible
1 barely perceptible seating, palms moist
2
3
4 beads of sweat obvious on forehead
5
6
7 drenching sweats
VISUAL DISTURBANCES – Ask “Does the light appear
to be too bright? Is its color different? Does it hurt your
eyes? Are you seeing anything that is disturbing to
you? Are you seeing things you know are not there?”
Observation.
0 not present
1 very mild sensitivity
2 mild sensitivity
3 moderate sensitivity
4 moderately severe hallucinations
5 severe hallucinations
6 extremely severe hallucinations
7 continuous hallucinations
ANXIETY – Ask “Do you feel nervous?”
Observation.
0 no anxiety, at ease
1 mild anxious
3
4
moderately anxious, or guarded, so
anxiety is inferred
5
6
7
equivalent to acute panic states as seen
in severe delirium or acute schizophrenic
reactions
HEADACHE, FULLNESS IN HEAD – Ask "Does your
head feel different? Does it feel like there is a band
around your head?" Do not rate for dizziness or
lightheadedness. Otherwise, rate severity.
0 not present
1 very mild
2 mild
3 moderate
4 moderately severe
5 severe
6 very severe
7 extremely severe
Continued on next page
306 Appendix C
TIP 42
Appendix C—Provider Forms, Measures, and Tools
Continued
AGITATION – Observation.
0 normal activity
1 somewhat more than normal activity
2
3
4 moderately fidgety and restless
5
6
7
paces back and forth during most of the
interview, or constantly thrashes about
ORIENTATION AND CLOUDING OF SENSORIUM – Ask
“What day is this? Where are you? Who am I?”
0 oriented and can do serial additions
1 cannot do serial additions or is uncertain about date
2 disoriented for date by no more than 2 calendar days
3 disoriented for date by more than 2 calendar days
4 disoriented for place/or person
Total CIWA-Ar Score______
Rater’s initials ______
Maximum Possible Score 67
Source: Sullivan, Sykora, Schneiderman, Naranjo, & Sellers (1989).
Appendix C 307
TIP 42
YES NO
YES NO
YES NO
YES NO
YES NO
YES NO
Substance Use Disorder Treatment for People With Co-Occurring Disorders
Trauma Screening and Assessment Tools
PRIMARY CARE PTSD SCREEN FOR DSM5
Sometimes things happen to people that are unusually or especially frightening, horrible, or traumatic.
For example:
•
A serious accident or fire
•
A physical or sexual assault or abuse
•
An earthquake or flood
•
A war
•
Seeing someone be killed or seriously injured
•
Having a loved one die through homicide or suicide
Have you ever experienced this kind of event?
If no, screen total = 0. Please stop here.
If yes, please answer the questions below.
In the past month, have you…
1. Had nightmares about the event(s) or thought about the event(s) when you did not want to?
2. Tried hard not to think about the event(s) or went out of your way to avoid situations that reminded you
of the event(s)?
3. Been constantly on guard, watchful, or easily startled?
4. Felt numb or detached from people, activities, or your surroundings?
5. Felt guilty or unable to stop blaming yourself or others for the event(s) or any problems the event(s)
may have caused?
Information about administration and scoring is available online (www.ptsd.va.gov/professional/assessment/documents/
pc-ptsd5-screen.pdf).
Source: Prins et al. (2015). Reprinted from material in the public domain.
308 Appendix C

TIP 42
Appendix C—Provider Forms, Measures, and Tools
PTSD CHECKLIST FOR DSM5
Instructions: Below is a list of problems that people sometimes have in response to a very stressful
experience. Please read each problem carefully and then circle one of the numbers to the right to indicate
how much you have been bothered by that problem in the past month.
In the past month, how much were you bothered by:
Not
at all
A
little
bit Moderately
Quite
a bit Extremely
1 Repeated, disturbing, and unwanted memories of the
stressful experience?
0 1 2 3 4
2 Repeated, disturbing dreams of the stressful
experience?
0 1 2 3 4
3 Suddently feeling or acting as if the stressful
experience were actually happening again (as if you
were actually back there reliving it)?
0 1 2 3 4
4 Feeling very upset when someone reminded you of
the stressful experience?
0 1 2 3 4
5 Having strong physical reactions when something
reminded you of the stressful experience (for example,
heart pounding, trouble breathing, sweating)?
0 1 2 3 4
6 Avoiding memories, thoughts, or feelings related to
the stressful experience?
0 1 2 3 4
7 Avoiding external reminders of the stressful
experience (for example, people, places,
conversations, activities, objects, or situations)?
0 1 2 3 4
8 Trouble remembering important parts of the stressful
experience?
0 1 2 3 4
9 Having strong negative beliefs about yourself, other
people, or the world (for example, having thoughts
such as: I am bad, there is something seriously
wrong with me, no one can be trusted, the world is
completely dangerous)?
0 1 2 3 4
10 Blaming yourself or someone else for the stressful
experience or what happened after it?
0 1 2 3 4
11 Having strong negative feelings such as fear, horror,
anger, guilt, or shame?
0 1 2 3 4
12 Loss of interest in actitivies that you used to enjoy? 0 1 2 3 4
13 Feeling distant or cut off from other people? 0 1 2 3 4
14 Trouble experiencing positive feelings (for example,
being unable to feel happiness or have loving feelings
for people close to you)?
0 1 2 3 4
15 Irritable behavior, angry outbursts, or acting
aggressively?
0 1 2 3 4
Continued on next page
Appendix C 309

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
Continued
16 Taking too many risks or doing things that could
cause you harm?
0 1 2 3 4
17 Being "superalert" or watchful or on guard? 0 1 2 3 4
18 Feeling jumpy or easily startled? 0 1 2 3 4
19 Having difficulty concentrating? 0 1 2 3 4
20 Trouble falling or staying asleep?
0 1 2 3 4
Information about administration and scoring is available online (www.ptsd.va.gov/professional/assessment/adult-sr/ptsd-
checklist.asp).
Source: Weathers et al. (2013). Reprinted from material in the public domain.
Levels of Care Tool
Level of Care Utilization System for
Psychiatric and Addiction Services
(LOCUS; https://drive.google.com/file/
d/0B89glzXJnn4cV1dESWI2eFEzc3M/view): The
LOCUS Adult Version 20 is a lengthy measure that
assesses many areas of symptoms and functioning
to determine level of care.
Functioning and Disability Tools
WHO’s Disability Assessment Schedule 2.0
(WHODAS 2.0; www.who.int/classifications/icf/
whodasii/en/): Various versions are available in the
following locations:
•
WHODAS 2.0 36-item version, self-
administered: www.who.int/classifications/icf/
WHODAS2.0_36itemsSELF.pdf
•
WHODAS 2.0 36-item, interviewer-
administered: www.who.int/classifications/icf/
WHODAS2.0_36itemsINTERVIEW.pdf
•
WHODAS 2.0 12-item, self-administered:
www.who.int/classifications/icf/
WHODAS2.0_12itemsSELF.pdf?ua=1
•
WHODAS 2.0 12-item, interviewer-
administered: www.who.int/classifications/icf/
WHODAS2.0_12itemsINTERVIEW.pdf
Stage of Change Tools
The Stages of Change Readiness and Treatment
Eagerness Scale (https://casaa.unm.edu/inst/
socratesv8.pdf): This scale is available in two
formats: one for alcohol use and one for drug use.
The University of Rhode Island Change
Assessment Scale (https://habitslab.umbc.edu/
urica/): Multiple short- and long-form versions of
this measure are available, including for alcohol
use, drug use, and initiating psychotherapy.
310 Appendix C

TIP 42
Appendix C—Provider Forms, Measures, and Tools
SAMPLE TREATMENT PLAN FOR CASE EXAMPLE GEORGE T. CHAPTER 3
Problem Intervention Goal
Cocaine use disorder Outpatient treatment Abstinence
•
Work problem primary
•
EAP monitoring
•
Negative urinalysis results
reason for referral
•
Family meetings
•
Daily recovery plans
•
Family and work support
•
Work support group
•
Resists 12-Step
•
Teach skills to manage symptoms
•
Mental symptoms trigger without using
use
•
12-Step meetings
•
Action phase
Rule out AUD
•
No clear problem
•
May trigger cocaine use
•
Precontemplation phase
•
Outpatient motivational
enhancement; thorough
evaluation of role of alcohol in
patient’s life, including family
education
•
Move into contemplation phase of
readiness to change
•
Willing to consider the risk of use
or possible abuse
Bipolar disorder
•
Medication management
•
Maintain stable mood
•
Long history
•
Help take medication while in
•
Able to manage fluctuating mood
•
On lithium
•
Some mood symptoms
•
Maintenance phase
recovery programs
•
Bipolar Support Alliance
meetings
•
Advocate/collaborate with
prescribing health professional
•
Identify mood symptoms as
triggers
symptoms that do occur without
using cocaine or other substances
to regulate his bipolar disorder
CONSIDERATIONS IN TREATMENT MATCHING
Variable Key Data
Acute safety needs
Determines need
for immediate acute
stabilization to establish
safety prior to routine
assessment
•
Immediate risk of harm to self or others
•
Immediate risk of physical harm or abuse from others (Mee-Lee et al., 2013)
•
Inability to provide for basic self-care
•
Medically dangerous intoxication or withdrawal
•
Potentially lethal medical condition
•
Acute severe mental symptoms (e.g., mania, psychosis) leading to inability
to function or communicate effectively
Quadrant assignment
Guides the choice of the
most appropriate setting
for treatment
•
Serious, persistent mental illness (SPMI) vs. non-SPMI
•
Severely acute or disabling mental symptoms vs. mild to moderate severity
symptoms
•
High (e.g., active SUD) vs. low (e.g., hazardous substance use) severity SUD
•
Substance dependence in full vs. partial remission (Mee-Lee et al., 2013;
American Psychiatric Association, 2013)
Continued on next page
Appendix C 311

TIP 42
Substance Use Disorder Treatment for People With Co-Occurring Disorders
Continued
Variable Key Data
Level of care
Determines client’s
program assignment
•
Dimensions of assessment for each disorder using criteria from the LOCUS
Diagnosis
•
Specific diagnosis of each mental disorder and SUD, including distinction
Determines the
between and SUD and substance-induced symptoms
recommended treatment
•
Information about past and present successful and unsuccessful treatment
intervention efforts for each diagnosis
•
Identification of trauma-related disorders and culture-bound syndromes, in
addition to other mental disorders and substance-related problems
Disability
•
Cognitive deficits, functional deficits, and skill deficits that interfere with
Determines case
management needs
ability to function independently or follow treatment recommendations
and that may require varying types and amounts of case management or
and whether a
support
standard intervention is
•
Specific functional deficits that may interfere with ability to participate in
sufficient—at capable SUD treatment in a particular program setting and may therefore require a
or intermediate level— co-occurring–enhanced setting rather than a co-occurring–capable one
or whether a more
advanced “enhanced”
level intervention is
•
Specific deficits in learning or using basic recovery skills that require
modified or simplified learning strategies
essential
Strengths and skills
Determines areas of prior
success around which to
organize future treatment
interventions and areas of
skill building to manage
either disorder
•
Areas of particular capacity or motivation in relation to general life
functioning (e.g., capacity to socialize, work, or obtain housing)
•
Ability to manage treatment participation for any disorder (e.g., familiarity
and comfort with 12-Step programs, commitment to medication
adherence)
Availability and
continuity of recovery
support
Determines whether
to establish continuing
relationships and existing
relationship availability to
provide contingencies to
promote learning
•
Presence or absence of continuing treatment relationships, particularly
mental disorder treatment relationships, beyond the single episode of care
•
Presence or absence of an existing and ongoing supportive family,
peer support, or therapeutic community; quality and safety of recovery
environment (Mee-Lee et al., 2013)
Continued on next page
312 Appendix C

TIP 42
Appendix C—Provider Forms, Measures, and Tools
Continued
Variable Key Data
Cultural context
•
Areas of cultural identification and support in relation to each of the
Determines most
following
culturally appropriate
•
Ethnic or linguistic culture identification (e.g., attachment to traditional
treatment interventions American-Indian cultural healing practices)
and settings
•
Cultures that have evolved around treatment of mental disorders and SUDs
(e.g., identification with 12-Step recovery culture; commitment to mental
health empowerment movement)
•
Gender and gender identity
•
Sexual orientation
•
Rural vs. urban
Problem domains
•
Is there impairment, need, or (conversely) strength in any of the following
Determines problems
areas
to be solved specifically,
•
Financial
and opportunities for
contingencies to promote
treatment participation
•
Legal
•
Employment
•
Housing
•
Social/family
•
Medical, parenting/child protective, abuse/victimization/victimizer
Phase of recovery/stage
•
Requirement for acute stabilization of symptoms, engagement, or
of change (for each motivational enhancement
problem)
•
Active treatment to achieve prolonged stabilization
Determines appropriate
phase-specific or stage-
specific treatment
•
Relapse prevention/maintenance
•
Rehabilitation, recovery, and growth
intervention and
•
In the motivational enhancement sequence, precontemplation,
outcomes
contemplation, preparation, action, maintenance, or relapse (Prochaska &
DiClemente, 1992)
•
Engagement, stabilization/persuasion, active treatment, or continuing care/
relapse prevention (Mueser & Gingerich, 2013; SAMHSA, 2009a)
Additional Screening Tools for
Common Mental Disorders
Depression. Patient Health Questionnaire
(PHQ-9): https://www.hiv.uw.edu/page/
mental-health-screening/phq-9
Anxiety. General Anxiety Disorder 7-item
(GAD-7) Scale: https://www.hiv.uw.edu/page/
mental-health-screening/gad-7
Appendix C 313
This page intentionally left blank.



