
Accessible and Affordable Health Care
COMPREHENSIVE, QUALITY HEALTH CARE SERVICES THAT ARE AVAILABLE AND
AFFORDABLE FOR ALL
Minnesota acknowledges that systemic racism and generational structural (social, economic, political
and environmental) inequities result in poor health outcomes. These inequities have a greater influence
on health outcomes than individual choices or one’s ability to access health care, and not all
communities are impacted the same way. All people living in Minnesota benefit when we reduce health
disparities and advance racial equity.
Current Landscape of Accessible and Affordable Health Care in Minnesota
Comprehensive, quality health care services are important for promoting and maintaining health
throughout the lifespan. Access to health care is impacted by household finances, insurance coverage,
geographic availability, and timeliness of entry into services. Poor access to health care services can
result in unmet health needs, lack of preventive services, hospitalization, and increased financial
burden.
2
Equally as important as access is the alarming rising costs of health care.
Around 264,000 Minnesotans (4.7%) lacked health insurance coverage in 2019, according to the most
recent Minnesota Health Access Survey. The maintained high rates of coverage in 2019 were consistent
with levels experienced after the full implementation of the Affordable Care Act in Minnesota in 2014 –
95.3 percent of Minnesotans had health insurance coverage that year. Compared to 2017, coverage in
the state was significantly higher, likely because of Minnesota’s the strong economy and job market, as
well as by provisions enacted by the Minnesota Legislature to help stabilize the individual health
insurance market. Despite relativity high levels of insurance coverage historical disparities in coverage
experienced by certain groups persisted in 2019. People of color and American Indians are around 2
times more likely to be uninsurance than White people living in Minnesota. Systemic racism creates
barriers to accessing health insurance.
As a result of an unfair and unjust health insurance system, the uninsured were more likely to be a
person of color or American Indian, a young adult (age 18 to 34), in a lower income bracket, or have a
high school education or less.
The highest proportion of Minnesotans without insurance live in rural areas in the northern regions of
the state. Minnesotans living in rural areas experience more barriers to accessing health care as a result
of decreased geographic access and health provider shortages. In 2017, there were 121 Health
Professional Shortage Areas (HPSA) in Minnesota and 97 Medically Underserved Areas (MUA).
1
Rural
residents are especially disadvantaged in terms of access to dental care with very few dental providers
practicing in Greater Minnesota counties.
Disparities in access to health care are also felt acutely among families of children and youth with special
health needs (CYSHN). In Minnesota, 7.8 percent of CYSHN did not received needed health care
compared to just 2 percent of children and youth without special health care needs.
2
The cost of health
care adversely affects families of CYSHN with 17.5 percent of these families struggling to pay for a child’s
medical bills compared to 10 percent of families without CYSHN.
2
The difference may seem small but
taken into consideration with the increased likelihood of parents of CYSHN to have to cut back their
work hours or stop working altogether to provide care for their child, the disparities in access to and
cost of health care can have a significant impact on families and their household income.
ACC E S S I B L E A N D A F F O R D A B L E H E A L T H C A R E
2
Data from the 2018-2019 National Survey of Children’s Health shows approximately 36 percent of
children in Minnesota had inadequate health insurance coverage or a gap in coverage in the previous 12
months. Of children in Minnesota without insurance, 9 percent needed health care services but did not
receive them compared to 2 percent of children with private insurance. Out of pocket health care costs
for the uninsured can be financially detrimental. Nearly 22 percent of Minnesota families paid $1,000 or
more in out of pocket health care costs for a child in the past 12 months.
2
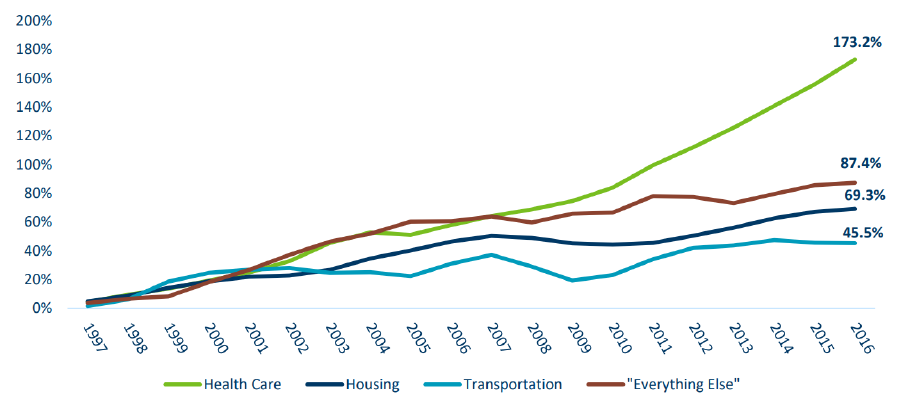
A study performed by the Minnesota Health Economics Program found that while household incomes
grew 80 percent between 1997 and 2016, family budgets devoted to health care spending rose more
than twice as fast. Figure 1 displays the disproportionate increase in health care spending compared to
housing, transportation and other expenses. There is no substantial evidence that increased health care
spending leads to similar positive gains in health.
3
Families who have private health insurance coverage
are paying a greater proportion of the cost of care than ever before. Families are seeing these rising
costs through higher cost-sharing, rising premiums, and re-configured benefits/plans (e.g. high
deductible health plans).
3
The increasing cost burden on families is causing many to delay or avoid care.
The 2019 Minnesota Health Access Survey found that 25 percent of Minnesotans did not receive some
kind of health care because of the cost. Additionally, even when an individual has access to health care
in their community, the financial burden experienced by seeing health care providers that are not within
an individual’s insurance network can greatly limit options for health care.
Figure 1. Cumulative Growth in Household Spending, Select Categories (1997-2016)
Source: MDH, Health Economics Program analysis of U.S. Bureau of Labor Statistics, Consumer Expenditure Survey for the
Midwest
Racial Justice and Accessible and Affordable Health Care
Systemic racism is pervasive within health care and has led to inequities in access to and affordability of
health care by race/ethnicity. It shows up in our health care system in many ways that impact Black,
Indigenous and People of Color (BIPOC) access to safe, affordable, and dignified health care.
4
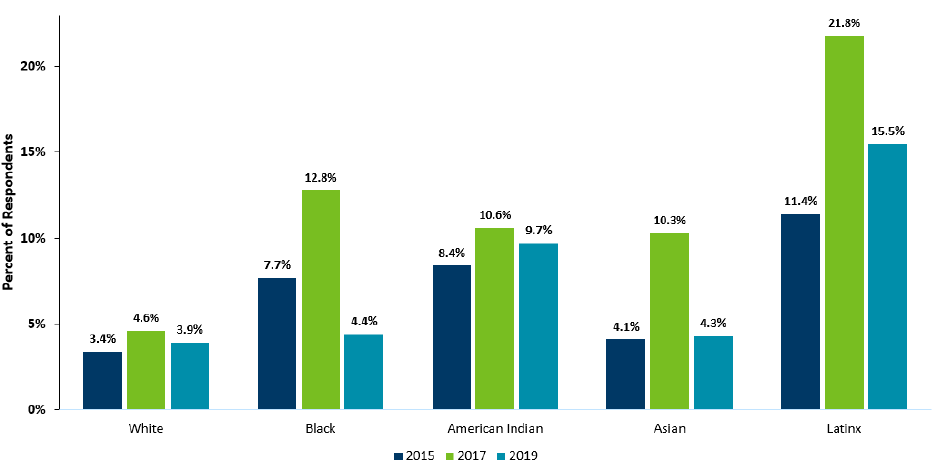
For
example, due to structural racism, which shapes things like who has opportunities for well-paying jobs
with benefits, uninsurance rates among BIPOC Minnesotans are significantly higher than those among
White Minnesotans (Figure 2).Error! Bookmark not defined.
,
5
Not having health insurance makes
accessing and affording good health care more difficult. The 2019 Minnesota Health Access Survey
showed that people who were uninsured were more likely to: report being in only fair or poor health,
ACC E S S I B L E A N D A F F O R D A B L E H E A L T H C A R E
3
experience more unhealthy days related to their mental health, lack confidence in getting needed care,
and not receiving needed care due to cost with 54.6 percent of uninsured Minnesotans reporting
foregoing care due to cost.
Figure 2. Minnesota Uninsurance Rates by Race/Ethnicity, 2015-2019
Source: Minnesota Health Access Survey Data
Additionally, systemic racism has a detrimental effect on the quality of care that communities of color
receive. Data from the 2018-2019 National Survey of Children’s Health, reveals how structural racism
has affected whether or not children of color have access to and receive family-centered care – while
92.8 percent of White children received family-centered care in the last year, only 80.9 percent of
Hispanic children and 69.7 percent of Black children did.
2
Structural racism in rural communities also continues to negatively affect the health outcomes of people
of color.
6
In general, access to health care and health outcomes are worse among people living in rural
areas.
7
Systematic racism intersects with the rural context, creating additional barriers to health care
accessibility for people of color living in rural communities.
8
Additionally, providers within a community
may still not be accessible if they are not considered “in network” for insurance companies.
COVID-19 Pandemic: Impact on Accessible and Affordable Health Care
New research, based on an analysis using enrollment data supplied by insurance carriers, shows
Minnesota’s uninsured rate weathered the economic shock of the pandemic in the first half of 2020,
staying at a historically low rate of about 5% through July 2020.
9
Economic downturns often result in
higher rates of uninsurance in the U.S. due to the link between health insurance coverage and
employment. The state took a proactive approach to prevent as many Minnesotans as possible from
losing health care coverage during the pandemic. As a result of those efforts, Minnesota saw only a
modest impact on the uninsured rate during the pandemic.
Despite uninsurance rates staying stable the COVID-19 pandemic has exacerbated the accessibility and
affordability of health care in Minnesota and across the U.S. The COVID-19 pandemic has caused the
highest unemployment rates since the Great Depression, causing thousands of people living in
Minnesota to lose their employer-sponsored health insurance. There have also been large declines in

ACC E S S I B L E A N D A F F O R D A B L E H E A L T H C A R E
4
visits to primary care physicians and outpatient specialists, and many hospitals have postponed or
cancelled elective procedures multiple times throughout 2020 and 2021.
These trends have compounded the problems seen in our fragmented healthcare system with persistent
gaps in access to affordable coverage and care, especially for people of color. On top of the impact on
accessible and affordable care, people of color in Minnesota, due to medical racism and other forms of
structural oppression, have seen higher numbers of COVID-19 cases and hospitalizations during the
pandemic.
10
For example, as of April 2021, while African American and Black Minnesotans and Latinx
Minnesotans make up 7 and 6 percent of the overall state population, respectively. As of April 2021,
African American and Black Minnesotans also constitute 9 percent of confirmed COVID-19 cases and 12
percent of COVID-19 hospitalizations while Latinx Minnesotans constitute 9 percent of confirmed
COVID-19 cases and 8 percent of hospitalizations.
11
Furthermore, due to systemic racism and other
forms of oppression, BIPOC Minnesotans are already at increased risk for many of the underlying
medical conditions that can lead to worse outcomes from COVID-19. Systemic racism and other forms of
oppression have also affected vaccine distribution throughout the state, resulting in inequitable vaccine
access and delivery rates by race and ethnicity. For example, as of April 2021, while Latinx and African
American/Black Minnesotans make up 4.8 percent and 6 percent of the overall state population
respectively, they only represent 1.7 percent and 3.5 percent of Minnesotans aged 16 and older who
have received a COVID-19 vaccine.
12
Strategic Planning
The Division of Child and Family Health (CFH) in partnership with stakeholders conducted a
comprehensive assessment of the health and well-being of Minnesota's maternal and child health
populations – including women, mothers, fathers, caregivers, children and youth (including those with
special health needs), families, and communities. Following the prioritization of unmet needs, Accessible
and Affordable Health Care was selected as a top priority for Minnesota.
In order to advance maternal and child health outcomes and health equity, CFH acknowledges that we
need to work together in authentic, collaborative, and innovative ways. CFH continued to engage
stakeholders by implementing a community-focused process to set and implement strategies to address
the priority needs using Strategy Teams. We have only begun this work and know there is still much
work to do. The outcome of this process helped form a statewide strategic plan that guides work on
improving maternal and child health systems going forward.
Vision for the Future
We strive for a Minnesota where all families, children, and communities have health care that is
affordable, accessible, and comprehensive. We envision a future where health care is transparent and
culturally responsive, where no one is excluded because of their background, geographic location, or
ability to pay. We aim for a Minnesota where systemic racism within health care is eliminated through
adequate funding and policies that prioritize health equity and community-driven approaches to health
care provision.
ACC E S S I B L E A N D A F F O R D A B L E H E A L T H C A R E
5
Strategies to Address Accessible and Affordable Health Care
A multidisciplinary Strategy Team was assembled to identify a set of strategies to address issues related
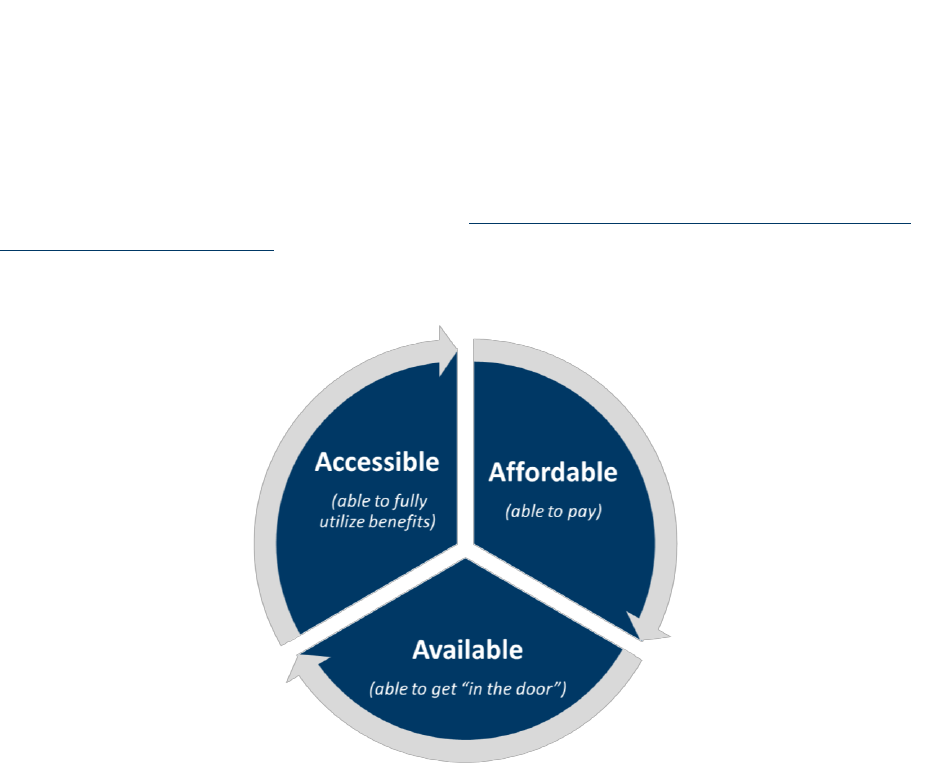
to Accessible and Affordable Health Care. During their discussion of the priority need, the Strategy Team
dissected the issue of Accessible and Affordable Health Care into three adjectives: Accessible (able to
fully utilize benefits), Available (able to reach location, i.e., “get in the door”), and Affordable (able to
pay). These features are intertwined with one another and embedded with issues of historic,
systematized discrimination and racism (Figure 3).
The discussion below is a brief summary of Minnesota’s strategies for improving accessible and
affordable health care. To learn more see the entire Minnesota Title V Maternal and Child Block Grant
Application and Annual Report.
Figure 3. Defining Accessible and Affordable Health Care
Strategy A. Recognize and Reduce Systemic Racism, Discrimination, and
Marginalization in Health Care
Minnesota ranks, on average, among the healthiest states in the nation. However, a closer look at the
data reveals that communities of color, American Indians, lesbian, gay, bisexual, transgender and queer
(LGBTQIA+) communities, the disability community, rural communities, and low-income communities
experience high inequities in the state. Minnesota's significant and long-lasting health inequities cannot
be explained by bio-genetic factors and personal choice. These health differences have in part resulted
from structural racism and discrimination, which refers to oppression that is built into systems and
policies, rather than solely individual prejudice.
13
Over the next five years, CFH will build off the work done at MDH, including work led by the Center for
Health Equity (CHE) and the Health Equity Advisory and Leadership (HEAL) Council. Our goal will be to
advance health equity focusing on reducing the discrimination and marginalization experienced by
women, mothers, fathers, caregivers, children and youth (including those with special health needs),
families, and communities in our healthcare system by:
▪ Monitoring and reporting data on racial and linguistic diversity of health care providers in
Minnesota, including partnering with the Office of Rural Health and Primary Care Healthcare

ACC E S S I B L E A N D A F F O R D A B L E H E A L T H C A R E
6
Workforce team at MDH and determine where and how to promote the needs of MCH
populations.
14
,
15
,
16
▪ Establishing promotion and training of accessibility in health care and other community settings for
children and adults with disabilities, including monitoring and influencing state legislation and
advocacy efforts as well as conducting a needs assessment related to community accessibility for
CYSHN and their families.
Strategy B. Expand Access to Health Care by Increasing Availability of Community-
Based and Remote Services
The second strategy aims to expand accessibility of community-based and remote services, such as
telemedicine. Over the next five years, CFH will focus on expanding community-based services and
remote services by:
▪ Providing road map/technical assistance to expand opportunities for collaboration between the
healthcare system and schools, for example surveying existing efforts in metro and Greater
Minnesota to improve health services in schools.
▪ Assessing and promoting accessible and barrier-free access to telehealth and other remote
methods of health care for MCH populations. This will include analyzing and reporting the use of
telehealth across the state and noting successes and barriers and understanding the landscape of
telehealth in state agencies and identifying areas for partnership.
Strategy C. Improve the Quality of Health Care by Promoting Person and Family-
Centered Practices
Many people have difficulty navigating the healthcare system in order to get the care they need. Specific
communities, such as people with disabilities and their families, people with limited English proficiency,
people living in rural areas, and communities that have been historically discriminated against, require
more unique approaches to accessing quality care. Understanding that some populations may need
different approaches in communication and outreach, it is important to leverage existing, trusted
networks (such as community health workers and other cultural brokers) in order to empower patients
and families with information and tools needed to be engaged in their health care. Over the next five
years, CFH will utilize these trusted health advocates as partners in Minnesota’s efforts to improve
quality of health care and person-centered practices in communities by:
▪ Increasing the availability and use of community health workers and other cultural brokers,
including by developing a partnership with Minnesota’s Community Health Worker Alliance.
17
,
18
▪ Working with the Birth Defects Unit within the CYSHN Section at MDH on a grant project to develop
community-based approaches for addressing the leading risk factors for birth defects in the state.
▪ Increasing access to family planning with special attention to youth, rural areas, and communities
of color and American Indians, by continuing the Family Planning Special Projects (FPSP) program
and developing interagency partnerships (e.g. Department of Human Services) within family
planning work.
▪ Training health care professionals on how to interact with and provide care to patients with
neurological differences and other disabilities and their families, with careful attention to the
context of COVID-19.
1
Minnesota Department of Health Office of Rural Health and Primary Care. (2017). Shortage designations. Retrieved from
https://www.health.state.mn.us/facilities/underserved/ designation.html.

ACC E S S I B L E A N D A F F O R D A B L E H E A L T H C A R E
7
2
Child and Adolescent Health Measurement Initiative. 2018-2019 National Survey of Children’s Health (NSCH) data query. Data
Resource Center for Child and Adolescent Health supported by Cooperative Agreement U59MC27866 from the U.S.
Department of Health and Human Services, Health Resources and Services Administration’s Maternal and Child Health Bureau
(HRSA MCHB).
3
Minnesota Department of Health, Health Economics Program. (2019). Minnesota Health Care Spending: 2015 and 2016
Estimates and Ten-Year Projections. Retrieved from
https://www.health.state.mn.us/data/economics/docs/costs/healthspending2019.pdf.
4
Hardeman, R. R., Medina, E. M., & Kozhimannil, K. B. (2016). Structural Racism and Supporting Black Lives—The Role of Health
Professionals. New England Journal of Medicine, 375(22), 2113–2115. https://doi.org/10.1056/NEJMp1609535
5
Davis, A., & Moritz, K. (2020). Structural racism and health care. https://www.mprnews.org/episode/2020/06/09/davis-
structural-racism-and-health-care
6
Henning-Smith, C. E., Hernandez, A. M., Hardeman, R. R., Ramirez, M. R., & Kozhimannil, K. B. (2019). Rural Counties With
Majority Black Or Indigenous Populations Suffer The Highest Rates Of Premature Death In The US. Health Affairs, 38(12), 2019–
2026. https://doi.org/10.1377/hlthaff.2019.00847
7
James CV, Moonesinghe R, Wilson-Frederick SM, Hall JE, Penman-Aguilar A, Bouye K. Racial/Ethnic Health Disparities Among
Rural Adults — United States, 2012–2015. MMWR Surveill Summ 2017;66(No. SS-23):1–9. DOI:
http://dx.doi.org/10.15585/mmwr.ss6623a1
8
Kozhimannil, K.B., & Henning-Smith, C. (2018). Racism and Health in Rural America. Journal of Health Care for the Poor and
Underserved 29(1), 35-43. doi:10.1353/hpu.2018.0004.
9
Minnesota Department of Health, Health Economics Program. (2020). Pandemic’s Impact on Health Insurance
Coverage in Minnesota Was Modest by Summer 2020.
https://www.health.state.mn.us/data/economics/docs/inscoverage2020.pdf
10
Carlson, J. (2021). COVID widens racial gap in Minnesota's health care system. Retrieved March, 2021.
https://www.startribune.com/covid-widens-racial-gap-in-minnesota-s-health-care-system/572402602/
11
Minnesota COVID-19 Response. (2021). COVID-19 Data by Race/Ethnicity. Retrieved March 2021.
https://mn.gov/covid19/data/data-by-race-ethnicity/index.jsp
12
Minnesota COVID-19 Response. (2021). Vaccine Data. Retrieved March 2021. https://mn.gov/covid19/vaccine/data/index.jsp
13
Jackson C.S. & Gracia J.N. (2014). Addressing health and health care disparities: The role of a diverse workforce and the social
determinants of health.
14
Cohen, J.J., Gabriel, B.A., Terrell, C. (2002). The case for diversity in the health care workforce. Health Affairs, 21(5), 90-102.
15
Nair L, Adetayo OA (2019). Cultural competence and ethnic diversity in healthcare. International Open Access Journal of the
American Society of Plastic Surgeons, 7(5), e2219.
16
St. George’s University Medical School (2018). The Importance of Diversity in Health Care: Medical Professionals Weigh In.
Retrieved from https://www.sgu.edu/blog/medical/pros-discuss-the-importance-of-diversity-in-health-care/.
17
Minnesota Community Health Worker Alliance. Definition of CHW. Retrieved from http://mnchwalliance.org/who-are-
chws/definition/.
18
Minnesota Community Health Worker Alliance Mission Statement. Retrieved from http://mnchwalliance.org/about-
us/vision/.
Child and Family Health Division
Minnesota Department of Health
PO Box 64975
St. Paul, MN 55164-0975
651-201-3589
www.health.state.mn.us
5/3/2021
To obtain this information in a different format, call: 651-201-3589. Printed on recycled paper.
