
Table of contents
What are the differences between Original Medicare
and Medicare Advantage? . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . 2
What are Medicare Advantage Plans? . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . 5
How do Medicare Advantage Plans work? . . . . . . . . . . . . . . . . . . . . . . . . . . . . . 5
What do Medicare Advantage Plans cover? . . . . . . . . . . . . . . . . . . . . . . . . . . . 5
What are my costs? . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . 6
Who can join a Medicare Advantage Plan? . . . . . . . . . . . . . . . . . . . . . . . . . . . .8
When can I join, switch, or drop a Medicare Advantage Plan? . . . . . . . . . 9
How can I join a Medicare Advantage Plan? . . . . . . . . . . . . . . . . . . . . . . . . . . .11
Types of Medicare Advantage Plans. . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . 12
Compare Medicare Advantage Plans side-by-side . . . . . . . . . . . . . . . . . . . 20
What if I have a Medicare Supplement Insurance
(Medigap) policy? . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . 21
Where can I get more information? . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . .22

Introduction 1
Getting started:
Introduction
When you first sign up for Medicare and during certain times of the year, you can
choose how you get your Medicare coverage.
There are 2 main ways to get Medicare:
• Original Medicare is a fee-for-service health plan that has two parts:
Part A (Hospital Insurance) and Part B (Medical Insurance). After you pay a
deductible, Medicare pays its share of the Medicare-approved amount, and you pay
your share (coinsurance). If you want Medicare drug coverage
(Part D), you can join a separate Medicare drug plan.
• Medicare Advantage (also known as “Part C”) is a type of Medicare health plan
oered by a private company that contracts with Medicare. These plans include
Part A, Part B, and usually Part D. Plans may oer some extra benefits that Original
Medicare doesn’t cover.
Your decision about how to get Medicare aects how much you pay for coverage, what
services you get, and what doctors you can use.
Understanding Medicare Advantage Plans2
What are the differences between Original Medicare
and Medicare Advantage?
Original Medicare
• Includes Medicare Part A (Hospital
Insurance) and Part B (Medical Insurance).
• You can join a separate Medicare drug plan
to get Medicare drug coverage (Part D).
• You can use any doctor or hospital that
takes Medicare, anywhere in the U.S.
• To help pay your out-of-pocket costs
in Original Medicare (like your 20%
coinsurance), you can also shop for and
buy supplemental coverage.
Part A
Part B
You can add:
Part D
You can also add:
Supplemental
coverage
This includes Medicare Supplement
Insurance (Medigap). Or, you can use
coverage from a current or former
employer or union, or Medicaid.
Medicare Advantage
(also known as Part C)
• A Medicare-approved plan from a private
company that oers an alternative to
Original Medicare for your health and drug
coverage. These "bundled" plans include
Part A, Part B, and usually Part D.
• In many cases, you can only use doctors
who are in the plan’s network.
• In many cases, you may need to get
approval from your plan before it covers
certain drugs or services.
• Plans may have lower or higher
out-of-pocket costs than Original Medicar
You may also have an additional premium.
• Plans may oer some extra benefits that
Original Medicare doesn't cover - like
certain vision, hearing, and dental services
e.
.
Part A
Part B
Most plans include:
Part D
Some extra benefits
Some plans also include:
Lower out-of-pocket-costs
Understanding Medicare Advantage Plans 3
Original Medicare vs. Medicare Advantage
Doctor & hospital choice
Original Medicare Medicare Advantage (Part C)
You can go to any doctor or hospital that
takes Medicare, anywhere in the U.S.
In many cases, you can only use doctors
and other providers who are in the
plan’s network and service area (for
non-emergency care). Some plans
oer non-emergency coverage out of
network, but typically at a higher cost.
In most cases, you don’t need a referral
to use a specialist.
You may need to get a referral to use a
specialist.
Cost
Original Medicare Medicare Advantage (Part C)
For Part B-covered services, you usually
pay 20% of the Medicare-approved
amount after you meet your deductible.
This amount is called your coinsurance.
Out-of-pocket costs vary —plans may
have lower or higher out-of-pocket
costs for certain services.
You pay a premium (monthly payment)
for Part B. If you choose to join a
Medicare drug plan, you’ll pay a separate
premium for your Medicare drug
coverage (Part D).
You pay the monthly Part B premium
and may also have to pay the plan’s
premium. Some plans may have a $0
premium and may help pay all or part of
your Part B premium. Most plans include
Medicare drug coverage (Part D).
There’s no yearly limit on what you pay
out of pocket, unless you have
supplemental coverage—like Medicare
Supplement Insurance (Medigap).
Plans have a yearly limit on what you
pay out of pocket for services
Part A and Part B cover. Once you reach
your plan’s limit, you’ll pay nothing for
services Part A and Part B cover for the
rest of the year.
You can choose to buy Medigap to help
pay your remaining out-of-pocket costs
(like your 20% coinsurance). Or, you can
use coverage from a current or former
employer or union, or Medicaid.
You can’t buy Medigap.

Understanding Medicare Advantage Plans4
Original Medicare vs. Medicare Advantage
Coverage
Original Medicare Medicare Advantage (Part C)
Original Medicare covers most medically
necessary services and supplies in
hospitals, doctors’ oces, and other
health care facilities. Original Medicare
doesn’t cover some benefits like eye
exams, most dental care, and routine
exams.
Plans must cover all medically necessary
services that Original Medicare covers.
Plans may also oer some extra benefits
that Original Medicare doesn’t cover—
like certain vision, hearing, and dental
services.
You can join a separate Medicare drug
plan to get Medicare drug coverage
(Part D).
Medicare drug coverage (Part D) is
included in most plans. In most types
of Medicare Advantage Plans, you can’t
join a separate Medicare drug plan.
In most cases, you don’t need approval
for Original Medicare to cover your
services or supplies.
In many cases, you may need to get
approval from your plan before it covers
certain services or supplies.
Foreign Travel
Original Medicare Medicare Advantage (Part C)
Original Medicare generally doesn’t
cover medical care outside the U.S.
You may be able to buy a Medicare
Supplement Insurance (Medigap) policy
that covers emergency care outside the
U.S.
Plans generally don’t cover medical
care outside the U.S. Some plans
may oer a supplemental benefit that
covers emergency and urgently needed
services when traveling outside the U.S.

Understanding Medicare Advantage Plans 5
What are Medicare Advantage Plans?
A Medicare Advantage Plan is another way to get your Medicare Part A and
Part B coverage. Medicare Advantage Plans, sometimes called “Part C” or “MA” Plans,
are oered by Medicare-approved private companies that must follow rules set by
Medicare. Most Medicare Advantage Plans include drug coverage (Part D). There are
several types of Medicare Advantage Plans (go to page 12 for more information).
Each of these Medicare Advantage Plan types have special rules about how you get
your Medicare-covered Part A and B services and any supplemental benefits your
plan covers.
If you join a Medicare Advantage Plan you’ll still have Medicare, but you’ll get most
of your Part A and Part B coverage from your Medicare Advantage Plan, not Original
Medicare. You’ll have the same rights and protections you would have under Original
Medicare.
You must use the card from your Medicare Advantage Plan to get your Medicare-
covered services. Keep your red, white, and blue Medicare card in a safe place
because you may need to show your Medicare card for some services. Also, you’ll
need it if you ever switch back to Original Medicare.
How do Medicare Advantage Plans work?
When you join a Medicare Advantage Plan, Medicare pays a fixed amount for your
coverage each month to the company oering your Medicare Advantage Plan.
Companies that oer Medicare Advantage Plans must follow rules that Medicare sets.
However, each Medicare Advantage Plan can charge dierent out-of-pocket costs
and have dierent rules for how you get services (like whether you need a referral
to use a specialist or whether you have to go to doctors, facilities, or suppliers that
belong to the plan’s network for non-emergency or non-urgent care). These rules can
change each year. The plan must notify you about any changes before the start of the
next enrollment year through the Annual Notice of Change, typically mailed to you
before September 30.
What do Medicare Advantage Plans cover?
Medicare Advantage Plans provide all your Part A and Part B benefits, except for
certain costs of clinical trials (clinical research studies), hospice care, the cost of
getting a kidney for transplant, and, for a temporary time, some new benefits that
come from legislation or national coverage determinations.
With a Medicare Advantage Plan, you may have coverage for things Original Medicare
doesn’t cover, like fitness programs (gym memberships or discounts) and some
vision, hearing, and dental services (like routine checkups or cleanings). Plans also
have a yearly limit on your out-of-pocket costs for all Part A and Part B services.
Once you reach this limit, you’ll pay nothing for services Part A and Part B cover.

Understanding Medicare Advantage Plans6
What do Medicare Advantage Plans cover? (continued)
Medicare drug coverage (Part D)
Most Medicare Advantage Plans include Medicare drug coverage (Part D). In certain
types of plans that don’t include Medicare drug coverage (like Medical Savings
Account Plans and some Private Fee-for-Service Plans), you can join a separate
Medicare drug plan.
However, if you join a Health Maintenance Organization or Preferred Provider
Organization Plan that doesn’t cover drugs, you can’t join a separate Medicare drug
plan. Go to pages 12–13 for more information.
Note: If you’re in a plan that doesn’t oer drug coverage, and you don’t have a
Medicare drug plan or other creditable prescription drug coverage, you may have to
pay a late enrollment penalty if you decide to join a Medicare drug plan later. Visit
Medicare.gov/basics/costs/medicare-costs/avoid-penalties to learn more about the
Part D late enrollment penalty.
What are my costs?
Each year, plans set the amounts they charge for premiums, deductibles, and services.
The plan (rather than Medicare) decides how much you pay for the covered services
you get. The plan can only change what you pay once a year, on January 1. You still
have to pay the Part B premium. Most people pay the standard Part B premium
amount every month. To get this year’s standard Part B premium, visit Medicare.gov/
basics/costs/medicare-costs.
When calculating your out-of-pocket costs in a Medicare Advantage Plan, in addition
to your premium, deductible, copayments, and coinsurance, you should also consider:
• The type of health care services you need and how often you get them.
• Whether you go to a doctor or supplier who accepts assignment. Assignment
means that your doctor, provider, or supplier agrees (or is required by law) to
accept the Medicare-approved amount as full payment for services Medicare
covers.
• Whether the plan oers extra benefits (in addition to Original Medicare benefits)
and if you need to pay extra to get them.
• Whether you have Medicaid or get help from your state through a Medicare
Savings Program to pay your Medicare costs. Each type of coverage is called a
“payer.” When there’s more than one payer, “coordination of benefits” rules decide
who pays first.
• The maximum out-of-pocket limit set by your plan.

Understanding Medicare Advantage Plans 7
What are my costs? (continued)
What’s the difference between a deductible, coinsurance,
copayment, and a maximum out-of-pocket limit?
Deductible—The amount you must pay for health care or prescriptions before
Original Medicare, your Medicare Advantage Plan, your Medicare drug plan, or your
other insurance begins to pay.
Coinsurance—An amount you may be required to pay as your share of the cost for
benefits after you pay any deductibles. Coinsurance is usually a percentage (for
example, 20%).
Copayment—An amount you may be required to pay as your share of the cost for
benefits after you pay any deductibles. A copayment is a fixed amount, like $30.
Maximum Out-of-Pocket Limit—Plans have a yearly limit on what you pay out of
pocket for services Part A and Part B cover. Once you reach your plan’s limit, you’ll
pay nothing for Part A and Part B services the plan covers for the rest of the year.
More cost details from each plan
If you join a Medicare Advantage Plan, review these notices you get from your plan
each year:
• Annual Notice of Change: Includes any changes in coverage, costs, provider
networks, service area, and more that will be eective in January. Your plan will
mail a copy to you, typically before September 30.
• Evidence of Coverage: Gives you details about what the plan covers, how much
you pay, and more. Your plan will send you a notice (or printed copy) by October
15, which will include information on how to access the Evidence of Coverage
electronically or request a printed copy.
Organization determinations
You or your provider can get a decision, either verbally or in writing, from your plan
in advance to find out if it covers a service, drug, or supply. You can also find out how
much you’ll have to pay. This is called an “organization determination.” Sometimes
you have to do this as prior authorization for your plan to cover the service, drug, or
supply.
You, your representative, or your doctor can request an organization determination. A
representative is someone you can appoint to help you. Your representative can be a
family member, friend, advocate, attorney, financial advisor, doctor, or someone else
who will act on your behalf. Based on your health needs, you, your representative, or
your doctor can ask for a fast decision on your organization determination request. If
your plan denies coverage, the plan must tell you in writing, and you have the right to
appeal.
Understanding Medicare Advantage Plans8
What are my costs? (continued)
Plan Directed Care
If a plan provider refers you for a service or to a provider outside the network, but
doesn’t get an organization determination in advance, this is called “plan directed
care.” In most cases, you won’t have to pay more than the plan’s usual cost sharing.
Check with your plan for more information about this protection.
Who can join a Medicare Advantage Plan?
To join a Medicare Advantage Plan, you must:
• Have Part A and Part B.
• Live in the plan’s service area.
• Be a U.S. citizen or lawfully present in the U.S.
What if I have a pre-existing condition?
You can join a Medicare Advantage Plan even if you have a pre-existing condition.
What if I have End-Stage Renal Disease (ESRD)?
You can join a Medicare Advantage Plan even if you have ESRD. In many Medicare
Advantage Plans, you can only use health care providers who are in the plan’s
network and service area. Before you join, you may want to check with your providers
and the plan you’re considering to make sure the providers you currently use (like
your dialysis facility or kidney doctor), or want to use in the future (like a transplant
specialist), are in the plan’s network. If you’re already in a Medicare Advantage Plan,
check with your providers to make sure they’ll still be part of the new plan’s network.
Read the plan materials or contact the plan you’re considering for more information.
What if I have other coverage?
Talk to your employer, union, or other benefits administrator about their rules before
you join a Medicare Advantage Plan. In some cases, joining a Medicare Advantage
Plan might cause you to lose your employer or union coverage for yourself, your
spouse, and your dependents and you may not be able to get it back. In other cases,
if you join a Medicare Advantage Plan, you may still be able to use your employer or
union coverage along with the Medicare Advantage Plan you join. Your employer or
union may also oer a Medicare Advantage retiree health plan that they sponsor.
Understanding Medicare Advantage Plans 9
When can I join, switch, or drop a Medicare Advantage
Plan?
You can only join, switch, or drop a Medicare Advantage Plan during these enrollment
periods:
Open Enrollment Period—Between October 15 and December 7 each year, anyone
with Medicare can join, switch, or drop a Medicare Advantage Plan. Your coverage will
begin on January 1 (as long as the plan gets your request by December 7).
Medicare Advantage Open Enrollment Period—Between January 1 and
March 31 of each year, you can make these changes:
• If you’re in a Medicare Advantage Plan (with or without drug coverage), you can
switch to another Medicare Advantage Plan (with or without drug coverage).
• You can drop your Medicare Advantage Plan and return to Original Medicare. You’ll
also be able to join a separate Medicare drug plan.
During the Medicare Advantage Open Enrollment Period, if you have Original
Medicare you can’t:
• Switch to a Medicare Advantage Plan.
• Join a Medicare drug plan.
• Switch from one Medicare drug plan to another.
You can only make one change during the Medicare Advantage Open Enrollment
Period, and any change you make will be eective the first of the month after the
plan gets your request. If you’re returning to Original Medicare and joining a separate
Medicare drug plan, you don’t need to contact your Medicare Advantage Plan to
disenroll. The disenrollment will happen automatically when you join the drug plan.
Understanding Medicare Advantage Plans10
When can I join, switch, or drop a Medicare Advantage Plan?
(continued)
Initial Enrollment Period—When you first become eligible for Medicare, you can join
a Medicare Advantage Plan during your Initial Enrollment Period. For many, this is
the 7-month period that begins 3 months before the month you turn 65, includes the
month you turn 65, and ends 3 months after the month you turn 65.
If you’re under 65 and have a disability, you’ll automatically get Part A and
Part B after you get disability benefits from Social Security or certain disability
benefits from the Railroad Retirement Board for 24 months.
If you sign up during the first 3 months of your Initial Enrollment Period, in most
cases, your coverage starts the first day of your birthday month. However, if your
birthday is on the first day of the month, your coverage will start the first day of the
prior month.
If you join a Medicare Advantage Plan the month you turn 65, your coverage will start
the first day of the following month.
If you sign up during the last 3 months of your Initial Enrollment Period, your
coverage will start the first day of the month after you sign up.
If you join a Medicare Advantage Plan during your Initial Enrollment Period, you can
change to another Medicare Advantage Plan (with or without drug coverage) or go
back to Original Medicare (with or without a separate Medicare drug plan) within the
first 3 months you have Medicare.
If you have Part A coverage and you get Part B for the first time between January 1
and March 31, you can also join a Medicare Advantage Plan. Your coverage will start
the first day of the month after you sign up.
Special Enrollment Period—In most cases, if you join a Medicare Advantage Plan, you
must keep it for the calendar year starting the date your coverage begins. However, in
certain situations, like if you move or you lose other insurance coverage, you may be
able to join, switch, or drop a Medicare Advantage Plan during a Special Enrollment
Period.
You may also qualify for a Special Enrollment Period to sign up for Medicare (and
join a Medicare Advantage Plan) if you miss an enrollment period because of
certain exceptional circumstances, like if you’re impacted by a natural disaster or an
emergency. Visit Medicare.gov or check with your plan for more information.
Understanding Medicare Advantage Plans 11
How can I join a Medicare Advantage Plan?
Not all Medicare Advantage Plans work the same way. Before you join, you can find
and compare Medicare plans in your area by visiting Medicare.gov/plan-compare or
calling 1-800-MEDICARE (1-800-633-4227). TTY users can call 1-877-486-2048. Once
you understand the plan’s rules and costs, you can join by:
• Visiting Medicare.gov/plan-compare and searching by ZIP code to find a plan and
join. You can also log in to your secure Medicare account for personalized results.
If you have questions about a plan, select “Plan Details” on the search results page
to get the plan’s contact information.
• Calling the plan you want to join, or visiting the plan’s website to find out if you can
join online.
• Filling out a paper enrollment form. Contact the plan to get an enrollment form, fill
it out, and return it to the plan. All plans must oer this option.
• Calling 1-800-MEDICARE.
When you’re ready to join a Medicare Advantage Plan, you’ll need this information
from your Medicare card:
• Your Medicare Number
• The date your Medicare Part A and/or Part B coverage started
Remember, when you join a Medicare Advantage Plan, in most cases, you must use
the card from your Medicare Advantage Plan to get your Medicare-covered services.
For some services (like hospice care), you may need to show your red, white, and
blue Medicare card.

Understanding Medicare Advantage Plans12
Types of Medicare Advantage Plans
There are different types of Medicare Advantage Plans:
• Health Maintenance Organization (HMO) Plan: Go to page 12.
• Preferred Provider Organization (PPO) Plan: Go to page 13.
• Private Fee-for-Service (PFFS) Plan: Go to page 14.
• Special Needs Plan (SNPs): Go to page 15.
• Medical Savings Account (MSA) Plan: Go to page 17.
The area where you live might have all, some, or none of these plan types available.
In addition, multiple plans of the same type might be available in your area, if private
companies choose to oer them. To find available Medicare Advantage Plans,
visit Medicare.gov/plan-compare, read your “Medicare & You” handbook, or call
1-800-MEDICARE (1-800-633-4227). TTY users can call 1-877-486-2048.
Health Maintenance Organization (HMO) Plan
An HMO Plan is a type of Medicare Advantage Plan that generally provides health
care coverage exclusively from doctors, other health care providers, or hospitals in the
plan’s network (except emergency care, out-of-area urgent care, or temporary out-
of-area dialysis). A network is a group of doctors, hospitals, and medical facilities that
contract with a plan to provide services. Most HMOs also require you to get a referral
from your primary care doctor for specialist care, so that your care is coordinated.
Can I get my health care from any doctor, other health care provider, or
hospital?
No. You generally must get your care and services from doctors, other health care
providers, or hospitals in the plan’s network (except for emergency care, out-of-
area urgent care, or temporary out-of-area dialysis, which is covered whether it’s
provided in the plan’s network or outside the plan’s network). However, some HMO
plans, known as HMO Point-of-Service (HMOPOS) plans, oer an out-of-network
benefit for some or all covered benefits, but you’ll usually pay a higher copayment
or coinsurance.
If you get non-emergency health care outside the plan’s network without
authorization, you may have to pay the full cost. It’s important that you follow
the plan’s rules, like getting prior approval for a certain service when needed. In
most cases, you need to choose a primary care doctor. Certain services, like yearly
screening mammograms, don’t require a referral. If your doctor or other health
care provider leaves the plan’s network, your plan will notify you. You may choose
another doctor in the plan’s network.
Understanding Medicare Advantage Plans 13
Types of Medicare Advantage Plans (continued)
Health Maintenance Organization (HMO) Plan (continued)
Do these plans cover prescription drugs?
In most cases, yes. If you’re planning to enroll in an HMO and you want Medicare
drug coverage (Part D), you must join an HMO Plan that oers Medicare drug
coverage. If you join an HMO Plan without drug coverage, you can’t join a separate
Medicare drug plan.
Preferred Provider Organization (PPO) Plan
A Preferred Provider Organization (PPO) Plan is a Medicare Advantage Plan that has a
network of doctors, specialists, hospitals, and other health care providers you can use.
Can I get my health care from any doctor, other health care provider, or hospital?
Yes. You can also use out-of-network providers for covered services, usually for a
higher cost, if the provider agrees to treat you and hasn’t opted out of Medicare
(for Medicare Part A and Part B items and services). You’re always covered for
emergency and urgent care.
Before you get services from an out-of-network provider, you may want to ask
for an organization determination of coverage from your plan to ensure that the
services are medically necessary and that your plan covers them. Go to page 7 for
more information on organization determinations.
Do these plans cover prescription drugs?
In most cases, yes. If you’re planning to join a PPO and you want Medicare drug
coverage (Part D), you must join a PPO Plan that oers Medicare drug coverage. If
you join a PPO Plan without drug coverage, you can’t join a separate Medicare drug
plan.
Understanding Medicare Advantage Plans14
Types of Medicare Advantage Plans (continued)
Private Fee-for-Service (PFFS) Plans
A Private Fee-for-Service (PFFS) Plan is another kind of Medicare Advantage Plan
oered by a private health insurance company. The plan determines how much it will
pay doctors, other health care providers, and hospitals, and how much you must pay
when you get care.
Can I get my health care from any doctor, other health care provider, or
hospital?
You can go to any Medicare-approved doctor, other health care provider, or
hospital that accepts the plan’s payment terms, agrees to treat you, and hasn’t
opted out of Medicare (for Medicare Part A and Part B items and services). If you
join a PFFS Plan that has a network, you can also use any of the network providers
who have agreed to treat plan members. You can also choose an out-of-network
doctor, hospital, or other provider who accepts the plan’s terms, but you may pay
more. Typically, your plan ID card tells your provider that you belong to a PFFS
Plan.
If your provider doesn’t agree to the plan’s terms and conditions of payment, the
plan is only required to pay them for emergency services, urgently needed services,
and out-of-area dialysis. For other covered services, you’ll need to find another
provider that will accept your PFFS Plan.
Note: A PFFS Plan may also allow “balance billing,” which means that a provider
can charge up to 15% more than the amount Medicare pays, and bill you for that
amount.
If your plan allows balance billing, you may have to pay both the plan’s copayment
or coinsurance and the dierence between what the provider charged and the
amount Medicare pays.
Do these plans cover prescription drugs?
Sometimes. If your PFFS Plan doesn’t oer Medicare drug coverage, you can join a
separate Medicare drug plan to get Medicare drug coverage
(Part D).
Understanding Medicare Advantage Plans 15
Types of Medicare Advantage Plans (continued)
Special Needs Plans (SNP)
Special Needs Plans provide benefits and services to people with specific diseases,
certain health care needs, or who also have Medicaid coverage. SNPs tailor their
benefits, provider choices, and what drugs they cover to best meet the specific needs
of the groups they serve.
Each SNP limits its membership to people in one of the groups listed below, or a subset
of one of these groups. You can only stay enrolled in an SNP if you continue to meet
the special eligibility rules for the SNP.
You may qualify for an SNP if you live in the plan’s service area and meet the
requirements for one of the 3 SNP types:
1. Chronic condition SNP (or C-SNP): You have one or more specific
severe or disabling chronic conditions like:
• Chronic alcohol and other drug dependence
• Certain autoimmune disorders
• Cancer (excluding pre-cancer conditions)
• Certain cardiovascular disorders
• Chronic heart failure
• Dementia
• Diabetes mellitus
• End-stage liver disease
• End-Stage Renal Disease (ESRD) requiring any mode of dialysis
• Certain severe hematologic disorders
• HIV/AIDS
• Certain chronic lung disorders
• Certain chronic and disabling mental health conditions
• Certain neurologic disorders
• Stroke
Understanding Medicare Advantage Plans16
Types of Medicare Advantage Plans (continued)
2. Institutional SNP (or I-SNP): You live in the community but need the level of care
a facility oers, or if you live (or are expected to live) for at least 90 days straight
in a facility like a:
• Nursing facility
• Intermediate care facility
• Skilled nursing facility
• Rehabilitation hospital
• Long-term care hospital
• Swing-bed hospital
• Psychiatric hospital
• Other facility that oers similar long-term health care services, and whose
residents have similar needs and health care status as residents of the facilities
listed above
3. Dual Eligible SNP (or D-SNP): You’re eligible for both Medicare and
Medicaid. D-SNPs also contract with your state Medicaid program to help
coordinate your Medicare and Medicaid benefits.
SNPs are either PPO, HMO, or HMOPOS plan types, and cover the same Medicare Part
A and Part B services that all Medicare Advantage Plans cover. However, SNPs might
also cover extra services tailored to the special groups they serve. For example, if
you have a severe or chronic condition, like cancer or chronic heart failure, and you
require a hospital stay, an SNP may cover extra days in the hospital.
Understanding Medicare Advantage Plans 17
Types of Medicare Advantage Plans (continued)
Can I get my health care from any doctor, other health care provider, or
hospital?
If your SNP is also an HMO, you generally must get your care and services from
doctors, other health care providers, or hospitals in the plan’s network (except
for emergency care, out-of-area urgent care, or out-of-area dialysis). You may be
required to have a primary care doctor.
However, if your SNP is also a PPO, then you may get services from any qualified
provider or hospital, but usually at a higher cost than you would pay for services
from a network provider.
SNPs typically have specialists in the diseases or conditions that aect their
members. Both an HMO and PPO SNP may require you to have a care coordinator
to help with your health care. A care coordinator is someone who helps make
sure people get the right care and information. For example, an SNP for people
with diabetes might provide the services of a care coordinator to help members
monitor their blood sugar and follow their diet.
Do these plans cover prescription drugs?
Yes. All SNPs must provide Medicare drug coverage (Part D).
Medicare Medical Savings Account (MSA) Plans
Medicare Medical Savings Account (MSA) plans combine a high-deductible insurance
plan with a medical savings account:
1. High-deductible health plan: The first part of an MSA Plan is a special type of
high-deductible Medicare Advantage Plan. The plan will only begin to cover your
costs once you meet a high yearly deductible, which varies by plan.
2. Medical savings account: The second part of an MSA is a special type of savings
account. The MSA Plan deposits money into your account that you can use to pay
for your health care costs.
Understanding Medicare Advantage Plans18
Types of Medicare Advantage Plans (continued)
Medicare Medical Savings Account (MSA) Plans (continued)
Who can’t join an MSA Plan?
You can’t join an MSA Plan if:
• You have health coverage that would cover the Medicare MSA Plan deductible.
• You joined another Medicare Advantage Plan.
• You get benefits from the U.S. Department of Defense (TRICARE) or the U.S.
Department of Veterans Aairs (VA).
• You’re a retired Federal government employee and part of the Federal Health
Benefits Program (FEHBP).
• You’re eligible for Medicaid.
• You’re currently getting hospice care.
• You live outside the U.S. more than 183 (total) days a year.
Once you decide which MSA Plan you want, you’ll need to contact the plan for
enrollment information and to join. The plan will tell you how to set up your medical
savings account with a bank that the plan selects. You must set up this account
before the plan can process your enrollment. After you join, you’ll get a letter from
the plan telling you when your coverage begins. Once you join and have MSA
coverage:
• Medicare gives the plan an amount of money each year for your health care.
• The plan deposits money into your account on your behalf. You can’t deposit your
own money.
• You can use the money in your account to pay for health care costs, including
health care costs that aren’t covered by Medicare.
• If you use all the money in your account and you have additional health care costs,
you’ll have to pay for your Medicare-covered services out of pocket until you reach
your plan’s deductible.
• During the time you’re paying out of pocket for services before the deductible
is met, doctors and other providers can’t charge you more than the Medicare-
approved amount.
• Your payments for Medicare-covered Part A and Part B services count toward your
plan’s deductible. After you reach your deductible, your plan will cover your Medicare-
covered services.
• Money left in your account at the end of the year stays in the account and may be
used for health care costs in future years. If you stay with the same MSA Plan the
following year, the new deposit will be added to any leftover amount.

Understanding Medicare Advantage Plans 19
Types of Medicare Advantage Plans (continued)
MSA plans and your taxes
If you use funds from your account, when you file your income taxes you must include
IRS Form 8853 with information on how you used your account money.
Each year, you should get a 1099-SA form from your bank that includes all of the
withdrawals from your account. You’ll need to show that you’ve had Qualified Medical
Expenses equal to at least this amount, or you may have to pay taxes and additional
penalties.
Visit irs.gov/forms-pubs/about-publication-969 to get more tax information related
to MSA plans, like a list of Qualified Medical Expenses.
If you have one, talk to your personal financial advisor about how choosing an MSA
Plan could aect your financial situation.
Can I get my health care from any doctor, other health care provider, or
hospital?
MSA plans generally don’t have a network of health care providers. You can get
Medicare Part A and Part B services from any Medicare-eligible provider in the
U.S. or U.S. territories.
Do these plans cover prescription drugs?
No. If you join a Medicare MSA Plan and want Medicare drug coverage (Part D),
you’ll have to join a separate Medicare drug plan.
Understanding Medicare Advantage Plans20
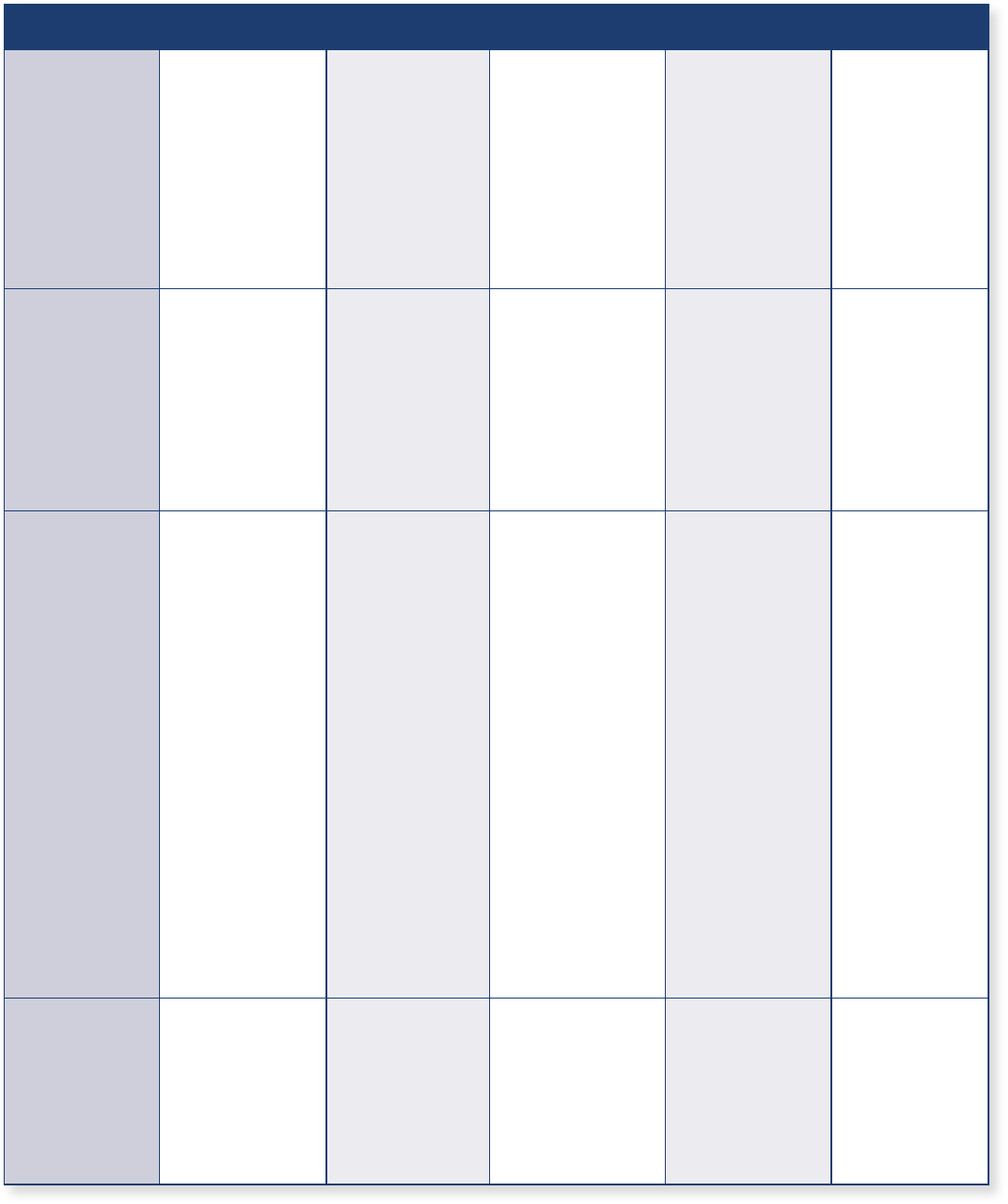
Compare Medicare Advantage Plans side-by-side
The chart below shows basic information about each type of Medicare Advantage Plan.
HMO PPO PFFS SNP MSA
Premium
Do most
plans charge
a monthly
premium?
Yes
Many charge
a premium in
addition to the
monthly Part B
premium.
Yes
Many charge
a premium in
addition to the
monthly Part B
premium.
Yes
Many charge
a premium in
addition to the
monthly Part B
premium.
Yes
Many charge
a premium in
addition to the
monthly Part B
premium.
No
You won’t
have to pay
a separate
monthly
premium, but
you’ll continue
to pay the
monthly Part B
premium.
Drugs
Does the plan
oer Medicare
drug coverage
(Part D)?
Usually
If you join an
HMO Plan that
doesn’t oer
drug coverage,
you can’t get a
separate Medicare
drug plan.
Usually
If you join a
PPO Plan that
doesn’t oer
drug coverage,
you can’t get
a separate
Medicare drug
plan.
Usually
If you join a
PFFS Plan that
doesn’t oer drug
coverage, you can
get a separate
Medicare drug
plan.
Yes
All SNPs must
provide Medicare
drug coverage
(Part D).
No
You may join
a separate
Medicare drug
plan.
Providers
Can I use
any doctor
or hospital
that accepts
Medicare
for covered
services?
Sometimes
You generally
must get your
care and services
from doctors,
other health
care providers,
or hospitals
in the plan’s
network (except
emergency or
urgent care
or out-of-area
dialysis).
In an HMOPOS
Plan, you may be
able to get some
services out of
network for a
higher copayment
or coinsurance.
Yes
Each plan has
a network
of doctors,
hospitals, and
other providers
that you may go
to. You may also
go out of the
plan’s provider
network, but your
costs may be
higher.
Yes
You can go to
any Medicare-
approved doctor,
other health
care provider,
or hospital that
accepts the plan’s
payment terms
and agrees to treat
you. If the plan
has a network, you
can use any of the
network providers
(if you go to an
out-of-network
provider that
accepts the plan’s
terms, you may
pay more).
Sometimes
If your SNP is an
HMO, you must
get your care
and services
from doctors
or hospitals
in the SNP’s
network (except
emergency or
urgent care
or out-of-area
dialysis). However,
if your SNP is
a PPO, you can
get Medicare-
covered services
out of network.
Yes
MSA Plans
generally don’t
have network
providers. You
may go to
any Medicare-
approved
provider for
services Original
Medicare covers.
Referral
Do I need a
referral from my
doctor to use a
specialist?
Yes No No Maybe
If the SNP is an
HMO, you need
a referral. If the
SNP is a PPO,
you don’t need a
referral.
No
Understanding Medicare Advantage Plans 21
What if I have a Medicare Supplement Insurance (Medigap)
policy?
If you’re in a Medicare Advantage Plan, it’s illegal for anyone to sell you a Medigap
policy unless you’re switching back to Original Medicare. If you aren’t planning
to drop your Medicare Advantage Plan, and someone tries to sell you a Medigap
policy, report it to your State Insurance Department. If you have Medigap and join a
Medicare Advantage Plan, you may want to drop Medigap. You can’t use Medigap to
pay your Medicare Advantage Plan copayments, deductibles, and premiums.
If you want to cancel your Medigap policy, contact your insurance company.
In most cases, if you drop your Medigap policy to join a Medicare Advantage Plan,
you may not be able to get the same policy back.
If you join a Medicare Advantage Plan for the first time and you aren’t happy with the
plan, you have a “trial right” under federal law to buy a Medigap policy and a separate
Medicare drug plan if you return to Original Medicare within 12 months of joining the
Medicare Advantage Plan.
• If you had Medigap before you joined a Medicare Advantage Plan, you may be able
to get the same policy back if the company still sells it. If it isn’t available, you can
buy another policy.
• If you joined a Medicare Advantage Plan when you were first eligible for Medicare
(and you aren’t happy with the plan), you can choose any Medigap policy if you
switch to Original Medicare within the first year of joining.
• Some states provide additional special rights to buy a Medigap policy. Check with
your State Insurance Department for more information.
Medigap plans sold to people who are newly eligible for Medicare aren’t allowed
to cover the Part B deductible. For more information about Medigap plans, visit
Medicare.gov/health-drug-plans/medigap or read or download the booklet,
“Choosing a Medigap Policy: A Guide to Health Insurance for People with Medicare”
at Medicare.gov/publications.
Accessible Communications22
Where can I get more information?
Find a Medicare plan
Visit Medicare.gov/plan-compare to shop and compare plans that meet your needs.
You can also enter your drugs and pharmacies to get more accurate costs for plans in
your area.
1-800-MEDICARE
Call 1-800-MEDICARE (1-800-633-4227) to get help with specific questions about
billing, claims, medical records, expenses, and more. TTY users can call
1-877-486-2048.
SHIPs (State Health Insurance Assistance Programs)
SHIPs are state programs that get money from the federal government to give
local health insurance counseling to people with Medicare at no cost. SHIPs aren’t
connected to any insurance company or health plan. SHIP volunteers can help you
with these Medicare questions or concerns:
• Your Medicare rights
• Billing problems
• Complaints about your medical care or treatment
• Plan choices
• How Medicare works with other insurance
• Finding help paying for health care costs
You can find the phone number for your state’s SHIP by visiting shiphelp.org or
calling 1-800-MEDICARE.
Medicare Advantage Plans
Contact the plans you’re interested in for detailed information about costs and
coverage.

Accessible Communications 23
Accessible communications
Medicare provides free auxiliary aids and services, including information in
accessible formats like braille, large print, data or audio files, relay services and
TTY communications. If you request information in an accessible format, you
won’t be disadvantaged by any additional time necessary to provide it. This
means you’ll get extra time to take any action if there’s a delay in fulfilling your
request.
To request Medicare or Marketplace information in an accessible format you
can:
1. Call us:
For Medicare: 1-800-MEDICARE (1-800-633-4227)
TTY: 1-877-486-2048
For Marketplace: 1-800-318-2596
TTY: 1-855-889-4325
2. Email us: altformatreques[email protected]v
3. Send us a fax: 1-844-530-3676
4. Send us a letter:
Centers for Medicare & Medicaid Services
Oces of Hearings and Inquiries (OHI)
7500 Security Boulevard, Mail Stop DO-01-20
Baltimore, MD 21244-1850
Attn: Customer Accessibility Resource Sta (CARS)
Your request should include your name, phone number, type of information
you need (if known), and the mailing address where we should send the
materials. We may contact you for additional information.
Note: If you’re enrolled in a Medicare Advantage Plan or Medicare drug plan,
contact your plan to request its information in an accessible format. For
Medicaid, contact your State Medical Assistance (Medicaid) oce.

Nondiscrimination Notice24
Nondiscrimination Notice
The Centers for Medicare & Medicaid Services (CMS) doesn’t exclude, deny
benefits to, or otherwise discriminate against any person on the basis of race,
color, national origin, disability, sex (including sexual orientation and gender
identity), or age in admission to, participation in, or receipt of the services and
benefits under any of its programs and activities, whether carried out by CMS
directly or through a contractor or any other entity with which CMS arranges
to carry out its programs and activities.
You can contact CMS in any of the ways included in this notice if you have any
concerns about getting information in a format that you can use.
You may also file a complaint if you think you’ve been subjected to
discrimination in a CMS program or activity, including experiencing issues with
getting information in an accessible format from any Medicare Advantage Plan,
Medicare drug plan, state or local Medicaid oce, or Marketplace Qualified
Health Plans. There are 3 ways to file a complaint with the U.S. Department of
Health & Human Services, Oce for Civil Rights:
1. Online:
HHS.gov/civil-rights/filing-a-complaint/complaint-process/index.html
2. By phone:
Call 1-800-368-1019.
TTY users can call 1-800-537-7697.
3. In writing: Send information about your complaint to:
Oce for Civil Rights
U.S. Department of Health & Human Services
200 Independence Avenue, SW
Room 509F, HHH Building
Washington, D.C. 20201


Need a copy of this booklet in Spanish?
To get a free copy of this booklet in Spanish, visit
Medicare.gov or call 1-800-MEDICARE
(1-800-633-4227). TTY users can call 1-877-486-2048.
Esta publicación está disponible en Español. Para
obtener una copia gratis, visite Medicare.gov o llame al
1-800-MEDICARE.
U.S. Department of Health & Human Services
Centers for Medicare & Medicaid Services
7500 Security Blvd.
Baltimore, MD 21244-1850
Ocial Business
Penalty for Private Use, $300
CMS Product No. 12026 • 12/2023
The information in this booklet describes the Medicare Program at the time this booklet was printed.
Changes may occur after printing. Visit Medicare.gov, or call 1-800-MEDICARE (1-800-633-4227) to get the
most current information. TTY users can call 1-877-486-2048.
“Medicare Rights & Protections” isn’t a legal document. Ocial Medicare Program legal guidance is
contained in the relevant statutes, regulations, and rulings.
You have the right to get Medicare information in an accessible format, like large print, braille, or audio.
You also have the right to file a complaint if you feel you’ve been discriminated against. Visit
Medicare.gov/about-us/accessibility-nondiscrimination-notice, or call 1-800-MEDICARE
(1-800-633-4227) for more information. TTY users can call 1-877-486-2048.
This product was produced at U.S. taxpayer expense.

