INNOVATION
CENTER
STRATEGY
REFRESH

Contents
Driving Health System Transformation –
A Strategy for the CMS Innovation Center’s Second Decade . . . . . . . . . . . . .3
Lessons from the CMS Innovation Center’s First Decade –
Foundation for a Strategy Refresh . . . . . . . . . . . . . . . . . . . . . . . . . . . 4
A Roadmap for Achieving the Vision –
Strategic Objectives, Measuring Progress, and Next Steps . . . . . . . . . . . . .9
Innovation Center Strategic Objective 1:
Drive Accountable Care . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . 13
Innovation Center Strategic Objective 2:
Advance Health Equity . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . 18
Innovation Center Strategic Objective 3:
Support Care Innovations . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . 22
Innovation Center Strategic Objective 4:
Improve Access by Addressing Affordability . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . 24
Innovation Center Strategic Objective 5:
Partner to Achieve System Transformation . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . 27
Looking Forward . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . .32
3
Driving Health System Transformation - A Strategy for the CMS
Innovation Center’s Second Decade
The Center for Medicare and Medicaid Innovation
(CMS Innovation Center or “Innovation Center”)
is launching a bold new strategy with the goal of
achieving equitable outcomes through high-
quality, affordable, person-centered care. To
achieve this vision, the Innovation Center is
launching a strategic refresh organized around five
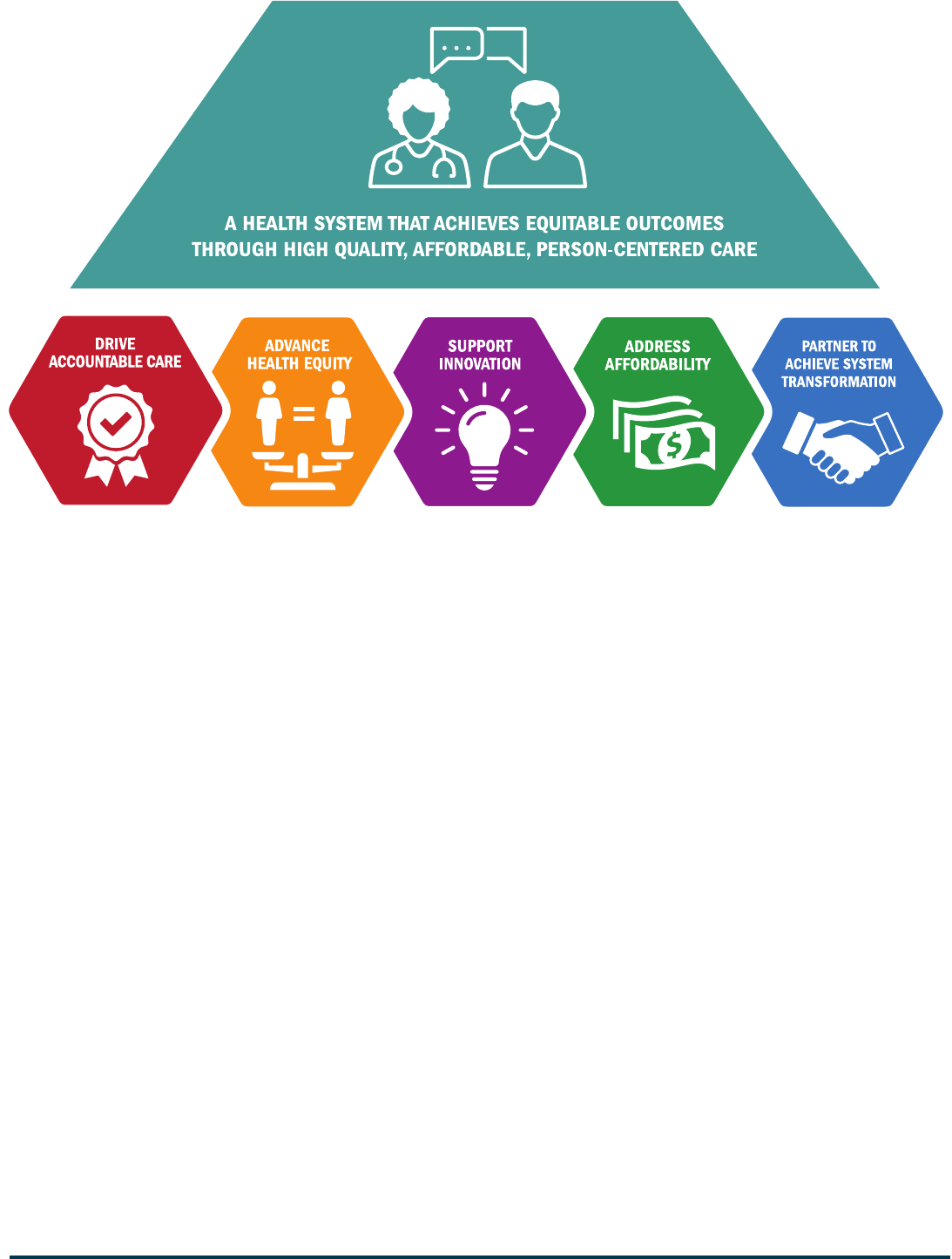
objectives [see Figure 1]. These strategic objectives
will guide the Innovation Center’s models and
priorities, and progress on achieving goals for each
will be to assess the CMS Innovation Center’s work
and impact.
INNOVATION CENTER STRATEGY REFRESH
The last ten years of testing and learning have laid
a strong foundation for the CMS Innovation Center
to lead the way towards broad and equitable
health system transformation. This white paper
describes the Innovation Center’s refreshed vision
and strategy and provides examples of approaches
and eorts under consideration to achieve the goals
of each strategic objective. The Innovation Center’s
overarching goal will continue to be expansion
of successful models that reduce program costs
and improve quality and outcomes for Medicare
and Medicaid beneciaries. In addition, the paper
emphasizes how measuring progress toward broader
health system transformation is also critical to
achieving these goals and vision.
Figure 1. CMS Innovation Center Vision and 5 Strategic Objectives for Advancing System
Transformation.

INNOVATION CENTER STRATEGY REFRESH 4
Lessons from the CMS Innovation Center’s First Decade –
Foundation for a Strategy Refresh
1 The Patient Protection and Aordable Care Act of 2010, Public Law 111-148, Section 1115A of the Social Security Act (the “Act”) (42 U.S.C.
1315a).
2 CMS Innovation Center. (2021).2020 Report to Congress: Center for Medicare and Medicaid Innovation.
3 Medicare Payment Advisory Commission (MedPAC). (2021) Report to the Congress: Medicare and the Health Care Delivery System.
4 National Academy of Medicine. (2021). Priorities in Advancing High-Quality Value-based Health and Health Care: CMMI catalyzing
innovative health system transformation.
The CMS Innovation Center was established in 2010
as part of the Aordable Care Act with the goal of
transitioning the health system to value-based care
by developing, testing, and evaluating new payment
and service delivery models in Medicare, Medicaid,
and the Children’s Health Insurance Program (CHIP).
1
In establishing the CMS Innovation Center, Congress
recognized the need for innovations in payment and
care delivery that addressed the two most pressing
problems facing the U.S. health system at the time
— lower than acceptable quality of care and ever
increasing spending that was (and continues to be)
a growing burden on households, states, and the
federal government.
In the last decade, the CMS Innovation Center has
launched over 50 model tests. From 2018-2020,
Innovation Center models have reached nearly
28 million patients and over 528,000 health care
providers and plans.
2
These models have generated
important lessons about how to transition the U.S.
health system to value-based care. Models have been
launched in advanced primary care, episode-based
care, accountable care, state-based transformation
eorts, and for specic populations, such as Medicare
beneciaries with end-stage renal disease (ESRD),
diabetes, heart disease, and in Medicaid for maternal
opioid-use disorders, and populations that experience
higher risk for premature births. Each model has
yielded important policy and operational insights
that will drive the next decade of health system
transformation, helping to address not only continued
challenges with health costs and quality of care, but
also the impacts of inequity and health disparities that
have become starkly apparent, particularly during the
COVID-19 pandemic.
The CMS Innovation Center has undertaken an
internal review of its portfolio of models and
consulted external research and experts to inform
this strategy refresh and chart its course for
the next decade. Leading health policy experts
and advisory bodies—including the Medicare
Payment and Advisory Commission (MedPAC) in
its June 2020 Report to Congress and the National
Academy of Medicine
3,4
— have recommended that
the Innovation Center reexamine its portfolio in
light of the need to accelerate the movement
to value-based care and drive broader system
transformation.
The CMS Innovation Center’s Statutory Authority and Expansion Potential
The CMS Innovation Center was created in Section 3021 of the Aordable Care Act (ACA) to test payment and delivery
models expected to reduce program costs and improve or maintain the quality of care for Medicare, Medicaid and
Children’s Health Insurance Program (CHIP) beneciaries. Congress gave the Innovation Center unique authorities
to test and expand models. Namely, the CMS Innovation Center can waive requirements in Medicare and, to a more
limited extent, Medicaid. This waiver authority allows the Center to test promising payment and service delivery
changes.
If models are deemed successful in that they reduce or do not increase federal health expenditures while maintaining
or improving quality for beneciaries, and certain other requirements are met, the ACA gave the Secretary of HHS the
authority to expand the duration and scope of the model test.

INNOVATION CENTER STRATEGY REFRESH 5
Over the last ten years, only six out of more than 50
models launched generated statistically significant
savings to Medicare and to taxpayers
5
and four of
these met the requirements to be expanded in
duration and scope.
6
CMS Innovation Center sta
also: examined policy and operational lessons from
other model tests and used these to directly inform
5 As of September 2021, the models that showed statistically significant savings include the Maryland All-Payer Model (MDAPM); Repetitive,
Scheduled Non-Emergent Ambulance Transport (RSNAT) Prior Authorization Model; the Home Health Value-Based Purchasing (HHVBP) Model;
the ACO Investment Model (AIM); the Pioneer ACO Model; and the Medicare Care Choices Model (MCCM).
6 As of September 2021, the Pioneer ACO, Medicare Diabetes Prevention Program (MDPP), RSNAT, and HHVBP model met the requirements
under Section 1115A(c) of the Social Security Act (the Act) to be expanded in duration and scope.
development of subsequent models; performed an
extensive literature review; conducted interviews
with experts and other stakeholders; and convened
focus groups with agency leaders. Based on this
internal and external review, the Innovation Center
identied key lessons learned, as well as next steps
for addressing issues and challenges (see Table 1).
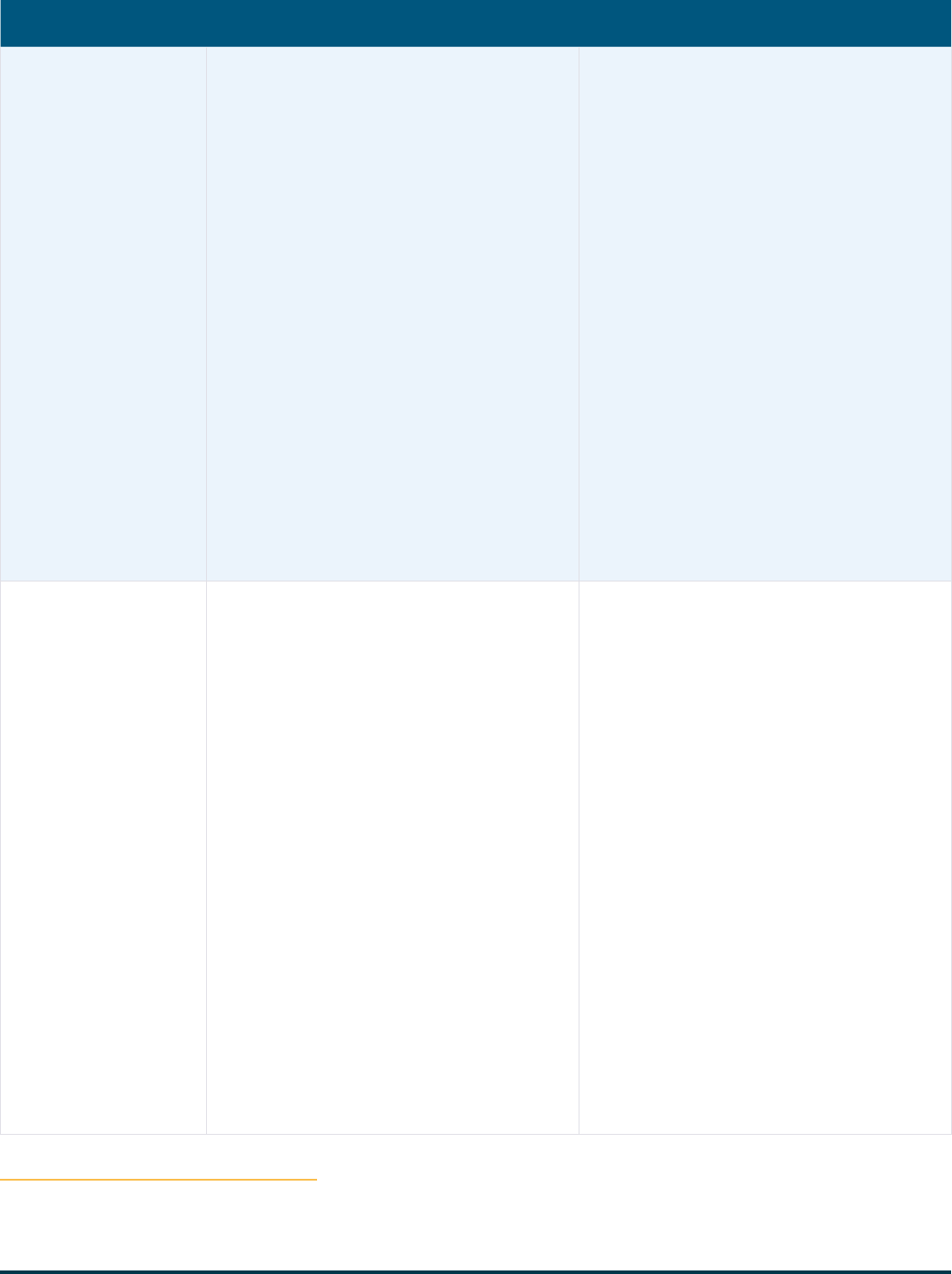
Table 1. Informing the CMS Innovation Center’s Future Direction - Key Learnings
Lesson Learned Issues and Challenges Next Steps
Ensure health
equity is
embedded in
every model.
• The full diversity of beneficiaries in
Medicare and Medicaid is not reflected in
many models to date.
• Medicare-focused models have limited
reach to Medicaid beneficiaries and safety
net providers.
• Models have not been systematically
evaluated impacts across beneficiaries
with
different demographic
characteristics.
• Better understand facilitators and
barriers to participation in value-based
payment models so that future models
are designed to target and increase
participation among providers that care
for underserved populations.
• Ensure all beneficiaries have access to
providers engaged in care transformation
to deliver high-quality care by addressing
issues such as implicit bias in model
design, implementation and evaluation.
• Launch more Medicaid-focused models
and/or modify existing models to include
additional Medicaid beneficiaries.
• Require a more deliberate and consistent
approach within the Innovation Center,
as well as across CMS, in quality
measurement and evaluations to assess
the impact of models on underserved
populations and to close disparities in
care and outcomes.

INNOVATION CENTER STRATEGY REFRESH 6
Lesson Learned Issues and Challenges Next Steps
Streamline the
model portfolio
and reduce
complexity
and overlap to
help scale what
works.
• Complex payment policies and model
overlap rules in CMS Innovation Center
models can sometimes result in
conflicting or opposing incentives for
health care providers (e.g., multiple
shared savings models operating in the
same health system).
• Participants face difficulty in joining or
continuing in models due to investments
required for care transformation,
complexity of model payment and/or
participation parameters, administrative
burden, and lack of clarity on long-term
strategy for models.
• Complexity of model design impedes
scalable transformation.
• Create a cohesive strategy that drives
model development and evolution.
• Ensure the hierarchy of models in the
case of overlap is rational and incents
distribution of financial incentives to
achieve model objectives and is also
clear on elements such as beneficiary
attribution and allocation of savings.
• Build on successful integration of CMS
Innovation Center model policies and
efforts in Medicare programs—such as
the Medicare Shared Savings Program—to
more systematically align with the overall
direction of CMS programs.
• Make model parameters, requirements,
and other critical details as transparent
and easily understandable as possible
for participants and to make scaling and
integration into broader CMS operations
easier.
• Assess current participation requirements
with an aim to reduce administrative
burden.
Tools to support
transformation in
care delivery can
assist providers
in assuming
financial risk.
• Accepting downside risk
7
is challenging
if providers lack: care management tools,
sufficient protection against the financial
impact of beneficiaries with unpredictably
high-costs, and appropriate payment and
regulatory flexibilities.
• Significant infrastructure investments are
often needed to participate in models,
including electronic health record (EHR)
enhancements, new staff, and data
analytic support especially for safety net
providers and those serving Medicaid
beneficiaries.
• Make available and increase uptake of
actionable data, learning collaboratives,
and payment and regulatory flexibilities
to participants, especially those caring for
the underserved, to enable them
to transform delivery at the point of care,
assume greater levels of financial risk,
and use model evaluation to drive
dissemination of best practices.
• Send strong and consistent signals
and expectations about Medicare and
Medicaid’s commitment to value-based
care so that participants can more
predictably make the necessary
investments.
• Improve sharing of more timely and
actionable data with providers to support
decision-making at point of care and to
identify successful care delivery practices
for dissemination.
• Encourage and support use of
interoperability standards for the
exchange of health data.
7 Note that downside risk is the term for the nancial risk model participants bear when actual spending exceeds nancial targets or capitation rates.

INNOVATION CENTER STRATEGY REFRESH 7
Lesson Learned Issues and Challenges Next Steps
Design of
models may not
consistently
ensure broad
provider
participation.
• Certain model design features, including
in some cases voluntary participation,
can limit potential savings and impede
evaluation due to selection bias, as
participants may opt in if they project that
the financial incentives in the model (e.g.,
benchmarking) are in their favor and drop
out when potential losses are projected.
• Multi-payer models designed for Medicare
providers have not consistently led to
high levels of participation from Medicaid
and commercial payers.
• Reduce selection bias by improving
model design (e.g., benchmarking, risk
adjustment, and care transformation
supports) to ensure participation from
a diverse group of providers—including
those that care for underserved
communities—in order to stabilize
participation across the life cycle of model
tests, and to help meet the requirements
for model expansion and potential scaling
by other providers and payers.
• To avoid risk selection associated with
voluntary models, examine whether
mandatory models can increase quality
and access for beneficiaries, as well as
increase provider participation, without
negatively impacting those who care for
underserved populations.
• Consider multi-payer alignment
opportunities earlier in model design
process.
Complexity
of financial
benchmarks
have undermined
model
effectiveness.
• Many financial benchmarks and risk
adjustment methodologies have created
opportunities for potential gaming and
upcoding among participants — and
reduced savings for Medicare.
• Set benchmarks to balance achieving
the following goals: maximizing
provider participation, while sustainably
generating savings, limiting spending
growth, and motivating continuous
improvement.
• Improve testing and analysis of
benchmarks and risk adjustment
methodologies prior to model launch.
• Test risk adjustment methodologies
that incent appropriate coding of patient
conditions and needs.
• Continue to refine benchmark
methodologies that leverage lessons
learned from models and incorporate
input from and consideration of the future
needs of CMS programs.
• Share lessons learned with Medicaid and
other payers to inform

INNOVATION CENTER STRATEGY REFRESH 8
Lesson Learned Issues and Challenges Next Steps
Models should
encourage
lasting care
delivery
transformation.
• Model testing has been focused on
meeting the statutory standards for
certification and expansion.
• Transformation can be limited to the
duration of model test.
• In addition to statutory criteria for model
expansion, consider a model’s impact on
dimensions of system transformation,
such as equity, care delivery
transformation, patient outcomes, and/or
market characteristics.
• Align models and lessons learned across
CMS, including Medicare FFS, Medicare
Advantage, and Medicaid.
• Facilitate multi-payer alignment with
Medicaid, states, and private payers
on service delivery and operational
model elements to accelerate system
transformation.
The CMS Innovation Center will continue to
develop and test models that can meet the
statutory criteria for expansion to reduce federal
health expenditures and improve care delivery for
beneciaries. However, the renewed vision also
calls for a more streamlined portfolio of models
that can deliver high-quality, person-centered
care, and drive health system transformation.
Broad transformation of health systems and
markets should support the delivery of care
that is consistent with people’s goals and values,
is culturally and linguistically responsive, and
focuses on what matters to them, such as their
health outcomes and functional status. The CMS
Innovation Center believes meaningful partnership
with providers, health plans, employers, and
states, among others, will be critical to achieve this
vision for all people.

9
A Roadmap for Achieving the Vision – Strategic Objectives,
Measuring Progress, and Next Steps
CMS Innovation Center’s Strategic Refresh:
Beneficiary and Provider Goals
The health system must recognize and meet
people’s medical needs by considering their
preferences, values, and circumstances, should
strive to keep people healthy and independent, and
help providers coordinate care seamlessly and
holistically across settings in a manner that puts
people at the center of their own care. This must
include a more intentional focus on addressing
health disparities and on ensuring equitable access,
quality, and outcomes. For models to drive system
transformation in this way, the CMS Innovation
Center must work more closely with external
stakeholders, especially beneficiaries and
caregivers, primary care, specialty, and other
providers that are most directly affected by models.
This includes collaborating across the life cycle of
models – from design to evaluation and potentially
expansion – and in the implementation of each of
the five objectives of the strategic refresh.
In particular, beneficiaries, patient groups, and
providers will see a deeper partnership with
the CMS Innovation Center in which their needs and
perspectives inform model development,
evaluation, and the definition of success, and in
which beneficiaries see improvements in quality of
care and providers receive clear signals and a more
transparent movement to value-based care (see
Table 2).
As part of its strategy refresh, the CMS Innovation
Center set out to articulate a vision of the health
system of the future for Medicare and Medicaid
beneciaries — and to reinvigorate the national
push toward value with a clear path and strategy
for the Innovation Center’s role in achieving
these goals. The new strategy lays out how the
vision will be advanced in partnership with other
components within CMS, including the Center for
Medicare (CM), the Center for Medicaid and CHIP
Services (CMCS), the Center for Clinical Standards
and Quality (CCSQ), the Medicare-Medicaid
Coordination Oce (MMCO), the Oce of
Minority Health (OMH), and other Department of
Health and Human Services (HHS) partners, such
as the Centers for Disease Control and Prevention
(CDC), the Food and Drug Administration (FDA),
the Health Resources and Services Administration
(HRSA), the Indian Health Service (IHS), and the
Administration for Community Living (ACL),
among others. It will be just as critical, however,
for the CMS Innovation Center to work more
synergistically with external stakeholders —
especially beneciaries, caregivers, and providers
that are most directly impacted by our models
as well as other payers, both public and private.
The implementation of the strategic refresh is
described in greater detail below, starting with
how the CMS Innovation Center will more closely
collaborate with beneciaries and providers in
particular. This is followed by sections on the
strategic objectives, which includes an aim for
each and long-term approaches to measuring
progress. The CMS Innovation Center will
also be setting interim targets to regularly
assess progress and to inform changes to the
implementation of the new strategy as needed.
CMS Innovation Center Vision
A health system that achieves equitable
outcomes through high-quality,
aordable, and person-centered care.
INNOVATION CENTER STRATEGY REFRESH

INNOVATION CENTER STRATEGY REFRESH 10
Table 2. CMS Innovation Center Strategy Refresh - Beneficiary and Provider Impact Goals
Accountable Care
Beneficiary Goals
• Medicare FFS beneficiaries will be in an accountable care relationship with
providers and will have the opportunity to select who will be responsible for
assessing and coordinating their care needs and the cost and quality of their
care.
• Medicare FFS beneficiaries will continue to have the choice to seek care from
any FFS provider.
• Medicaid beneficiaries in FFS and managed care organizations (MCOs) will be
in accountable care relationships that drive improved quality and outcomes
for beneficiaries.
• Dual eligible beneficiaries will be in
accountable care relationships that help
manage the quality and cost of their care and improve their care across the
Medicare and Medicaid programs.
Provider Goals
• Transformation supports, such as data-sharing, learning opportunities, and
regulatory flexibilities, as well as varying levels of options to assume risk will
be
available for primary care practices to transition to population-based
payments and to sustain accountable care relationships.
• Increase the capability of primary care providers, as well as specialists and
other providers, to engage in accountable care relationships with beneficiaries
through incentives and flexibilities to manage quality and total cost of care.
Health Equity
Beneficiary Goals
• Underserved beneficiaries will have increased access to accountable, value-
based care as the CMS Innovation Center focuses on increasing
participation among safety net providers in its models.
• Underserved beneficiaries will experience improved quality and outcomes
due to CMS Innovation Center efforts to design models that are simpler
and responsive to the needs of these beneficiaries and communities.
Provider Goals
• The CMS Innovation Center will address barriers to participation for providers
that serve a high proportion of underserved and rural beneficiaries, such as
those in Health Professional Shortage Areas (HPSAs) and Medically
Underserved Areas (MUAs), and designated provider types such as Federally
Qualified Health Centers (FQHCs), rural health clinics (RHCs), and other
safety net providers and create more opportunities for them to join models
with supports needed to be successful.
• The CMS Innovation Center will offer targeted learning opportunities for
model participants to advance health equity, including collaborating with
community
partners to address social needs.
• The CMS Innovation Center will require and consider incentives and supports
for model participants to collect data on race, ethnicity, geography, disability,
and other demographics and results will be reported to the Innovation Center
to help providers address health disparities (in a manner that protected health
information (PHI) complies with HIPAA-and other applicable laws).

INNOVATION CENTER STRATEGY REFRESH 11
Care Innovations
Beneficiary Goals
• Drawing on more diverse beneficiary, caregiver, and patient perspectives will
systematically inform development of models that test care delivery changes
and innovations that are meaningful and understandable to them.
• Beneficiaries in accountable care relationships will receive more person-
centered, integrated care, which could include support with social determinants
of health (SDoH) and greater access to care in the home and community.
• Beneficiaries in accountable care relationships and their caregivers may have
access to benefit enhancements and beneficiary engagement incentives that
support engagement and care management.
Provider Goals
• Providers will receive support to leverage actionable, practice-specific data,
detailed case studies, and other data to implement practice changes that
deliver integrated, person-centered, and community-based care.
• Providers participating in models, particularly total cost of care models, will
have access to more payment flexibilities that support accountable care,
such as telehealth, remote patient monitoring, and home-based care.
Address Affordability
Beneficiary Goals
• Beneficiaries in CMS Innovation Center models may have lower out-of-pocket
costs through changes in cost-sharing or through reductions in avoidable
utilization of duplicative or wasteful services.
• Beneficiaries may experience reduced out-of-pocket costs on drugs by lowering
program spending, and by increasing biosimilar and generic drug utilization.
• Beneficiaries may experience reduced barriers to accessing high-value care
using tools such as value-based insurance design that can help improve
outcomes and lower overall costs.
Provider Goals
• Better align provider and beneficiary incentives to increase use of high-value
services that efficiently deliver and coordinate care, achieve the best outcomes
for patients, and reduce utilization of duplicative or wasteful services –
especially in total cost of care models.
• Create payment and performance incentives in models, especially in total cost
of care models, for specialty and primary care providers to coordinate delivery
of high-value care and to reduce duplicative or wasteful care.

INNOVATION CENTER STRATEGY REFRESH 12
Partner to Achieve Health System Transformation
Beneficiary Goals
• Beneficiaries in accountable care relationships will experience more person-
centered, seamless care that supports their health and independence.
• The perspectives of all Medicare and Medicaid beneficiaries, including
underserved populations, caregivers, and
patient groups will help shape models
from conceptualization and design to evaluation and potential expansion.
Provider Goals
• Providers will be able to deliver more integrated care across settings and
engage in more comprehensive and longitudinal care as a result of accountable
care relationships and participation in total cost of care models.
• Providers will benefit from burden reduction as a result of alignment across
payers on value-based care initiatives.
• Aligning and partnering with other payers on key design features such as clinical
tools and outcome measures will enable improved evaluation and scaling of
transformation.

INNOVATION CENTER STRATEGY REFRESH 13
Innovation Center Strategic Objective 1:
Drive Accountable Care
Aim:
Increase the number of people in a care relationship with
accountability for quality and total cost of care.
Measuring Progress:
• All Medicare beneficiaries with Parts A and B will be in a care
relationship with accountability for quality and total cost of care by
2030.
• The vast majority of Medicaid beneficiaries will be in a care relationship with accountability for
quality and total cost of care by 2030.
The key feature of accountable care is to give all
participating providers the incentives and tools
to deliver high-quality, coordinated, team-based
care that promotes health, thereby reducing
fragmentation and costs for people and the health
system. Depending on the model or program
and their respective requirements, accountable
entities could include physician group practices,
++A ++8+A
Part A and B Traditional Medicare &
Medicare Advantage Beneficiaries
Traditional Medicare (Part A & B) Medicare FFS benes not in an ACO
Medicare Advantage and Other Health Plan Enrollment
Medicare FFS benes in other ACOs and ACO-like models
Medicare FFS benes in a MSSP ACO*
Accountable Care in Traditional Medicare
53%
(30.5M benes)
57%
(17.5M benes)
35%
(10.7M benes)
7%
(2.3M benes)
47%
(27.2M benes)
8 Medicare Payment Advisory Commission (MedPAC). (2020). “A Data Book: Health Care Spending and the Medicare Program.”
9 Medicare Payment Advisory Commission (MedPAC). (2020). “A Data Book: Health Care Spending and the Medicare Program.”
hospitals, and other health care providers, Medicare
Advantage (MA) plans, Programs of All-Inclusive Care
for the Elderly (PACE), or even Medicaid managed
care plans. In 2020, 67% of Medicare beneciaries
enrolled in Part A and Part B were in MA plans or
were attributed to an accountable care organization
(ACO) through either a CMS Innovation Center model
or the Shared Savings Program (See Figure 2).
8, 9
++A ++8+A
Figure 2. Medicare Beneficiaries in Accountable Care Relationships (2021).
INNOVATION CENTER STRATEGY REFRESH 14
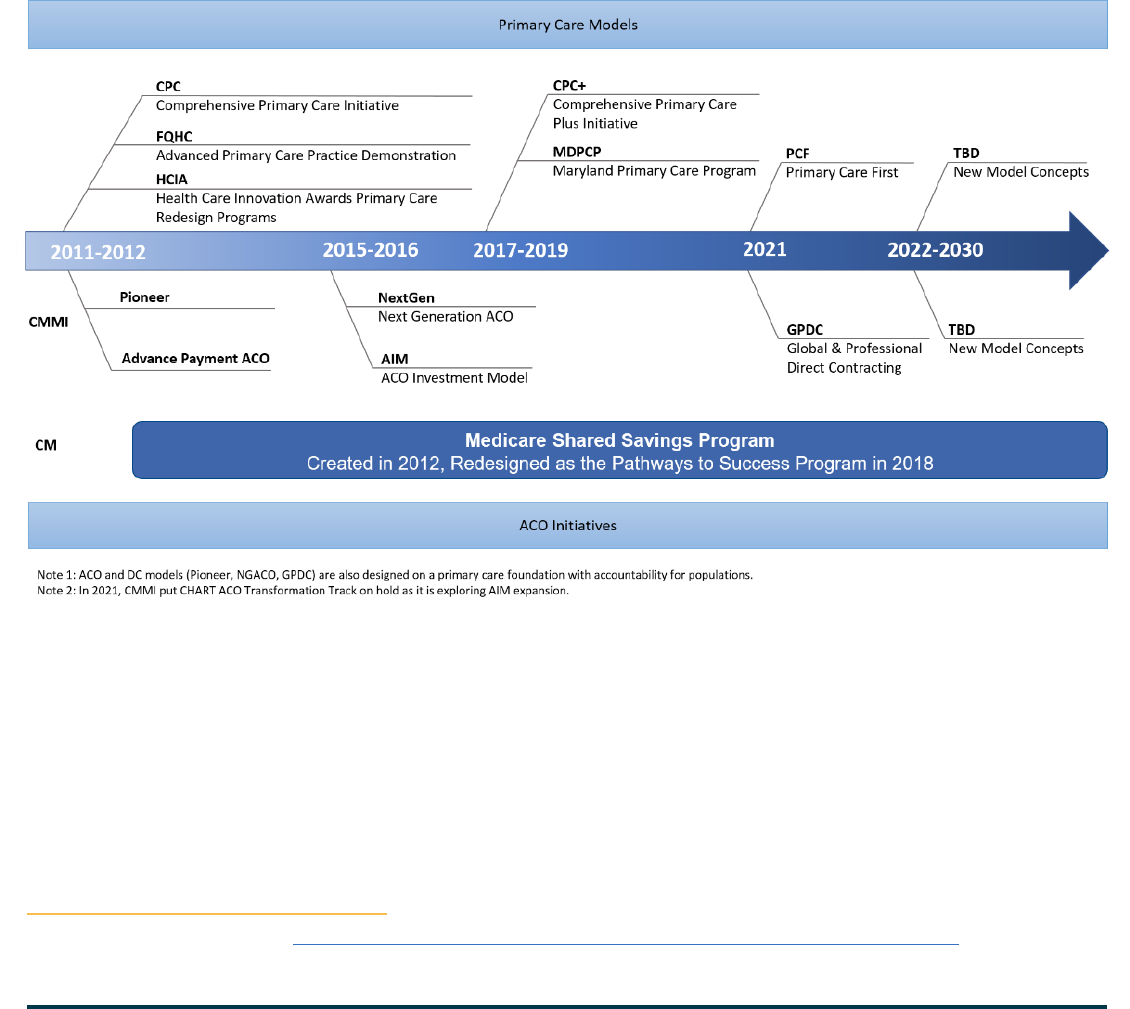
Advanced primary care and accountable care models
are central to driving growth in the number of
beneciaries in accountable care relationships. The
CMS Innovation Center has set the goal of having
every Medicare FFS beneciary in an accountable
care relationship by 2030 and will set interim targets
to measure progress towards that goal. This goal
would not only aim to have all beneciaries in
value-based care arrangements, but for them to
be in care arrangements where their needs are
holistically assessed and their care is coordinated
within a broader total cost of care system. CMS
anticipates that this could lead to an additional 30
million beneciaries (adjusted for growth in the
Medicare population) attributed to organizations
such as an advanced primary care practice, an ACO,
or similar entity that is responsible for the cost
and quality of care. The CMS Innovation Center is
also committed to working with CMCS to dene
accountable care that achieves equitable, high-
quality, person-centered care for Medicaid and
dually eligible beneficiaries. Lessons learned and the
considerations for future work in these two areas,
which will include coordinating with the Medicare
and Medicaid programs, are outlined below (see
Figure 3).
Figure 3. Primary Care and ACO Model Evolution
Advanced Primary Care – Lessons Learned and
Model Considerations
The National Academy of Medicine recently
published a report on rebuilding primary care,
which noted that high-quality primary care forms
the foundation of a high-functioning health system
and is key to improving the experience of patients
and care teams, as well as population health,
and reducing costs.
10
Given the foundational
10 National Academy of Medicine, Implementing High-Quality Primary Care: Rebuilding the Foundation of Health Care (2021).
role of primary care in transforming the health
system, the CMS Innovation Center has devoted
signicant time and resources to develop and
test primary care models. Models have tested
advanced primary care across the country to
improve and enhance how practices deliver
care. The Comprehensive Primary Care (CPC)
and Comprehensive Primary Care Plus (CPC+)
multi-payer models, for example, gave practices

INNOVATION CENTER STRATEGY REFRESH 15
CPC+ practices. These models have also oered
lessons for future model testing: there was limited
participation among independent practices;
beneciaries in advanced primary care models
were more likely to be white and less likely to be
dually eligible; and further, these primary care
models have not generated net savings for the
Medicare program. In the context of the strategy
refresh, the CMS Innovation Center can make
improvements to broaden participation among
practices, to include a broader population of
beneciaries, and to consider primary care’s role
in generating savings.
CMS Innovation Center models have also tested
bundled payment models to drive improved
quality and lower costs for episodic care. Future
models must test incentives for advanced primary
and specialty, episodic care to generate greater
value under total cost of care approaches. Such
models may need to include tracks that dier by
readiness to take on risk, targeted populations,
and payment schedules.
the opportunity to deepen their capabilities to
deliver comprehensive and coordinated primary
care. In CPC+, participating practices were able
to gain experience in assuming limited risk
for performance. In turn, these models gave
the Innovation Center a chance to build an
infrastructure to deliver more timely data to
participants, to provide learning resources to
engage practices in continuous improvement, and
to gain experience in working with other payers to
align care goals. The CPC and CPC+ models directly
informed the design of the Primary Care First (PCF)
model, which was launched earlier this year.
Previous primary care models illustrated that
practices can be eectively incentivized to broaden
their care delivery capabilities, including making
medical record and facilities more accessible after
hours for patients in need. Practices have also
eectively increased usage of care managers,
integrated behavioral health, and incorporated
screening for social service needs at rates much
higher than non-participating practices. These
results have begun translating into favorable
outcomes – the latest CPC+ evaluation report
indicates there have been slight decreases in
emergency department and hospital utilization
among beneciaries attributed to participating

INNOVATION CENTER STRATEGY REFRESH 16
critical component of the CMS Innovation Center’s
strategic refresh and its goal of engaging all
beneciaries in an accountable care relationship.
Next Steps to Advance Accountable Care
• Educate and engage beneciaries on what
an accountable care relationship is and the
potential value and benets associated with
these arrangements for them.
• Test voluntary beneciary alignment and
attribution methodologies, benet enhancements,
and beneciary engagement incentives to
facilitate accountable care relationships between
beneciaries and care teams.
• Include outcome measures that are meaningful
to people, such as functional status, out-of-
pocket costs, and patient-reported outcomes
measures (PROMs) to ensure meaningful
accountability for quality improvement.
• Create and test combinations of risk levels,
per beneciary per month payments, and
population-based and advanced payment
options to increase the number of health
care providers and organizations—including
primary care practices and safety net
providers—that can participate in accountable
and total cost of care models.
• Test incentives to drive coordination between
providers responsible for accountable
care relationships and specialty providers
accountable for delivering high-cost episodic
and/or complex care.
• Test approaches that enable ACOs to manage
more high-cost specialty and episodic care
using lessons learned from bundled payments
and other models.
• Provide time-limited upfront funds to smaller
primary care practices or those with more
limited experience in value-based payment
models to help them prepare for the transition
to population-based payments and total cost of
care approaches.
Accountable Care Organizations (ACOs) –
Lessons Learned and Model Considerations
CMS has learned signicant lessons from its
portfolio of ACO initiatives as it has grown and
evolved over the last ten years. The CMS Innovation
Center designed and led rst-generation models
including the Pioneer ACO Model and Advanced
Payment ACO Model, and second-generation
models including the Next Generation ACO Model
(NGACO) and the ACO Investment Model (AIM).
While only the Pioneer ACO Model, as tested in
the rst two years of the model, was certied for
expansion the Innovation Center has learned
much from the other ACO models, both in terms
of successes and challenges, which are informing
future ACO model development. For instance,
the CMS Innovation Center is examining its
benchmarking and risk adjustment approaches
to provide incentives to encourage participation,
especially among providers caring for underserved
beneciaries. It is important to ensure that
benchmarks and risk adjustors are appropriate
for ACOs at varying levels of experience and that
models are not resulting in inaccurate payments
and potential upcoding among participants, both of
which can reduce savings for Medicare.
The Innovation Center is also examining how
beneciaries can be better engaged in accountable
care relationships through benet enhancements
and beneciary engagement incentives, as well as
voluntary alignment, which supports beneciaries
actively choosing a provider either on Medicare.
gov or via paper forms. The experience of the ACO
Investment Model (AIM), which demonstrated the
value of advancing payments to support new ACOs
in rural and underserved areas, is informing current
and future ACO model design concepts. Last, ACOs
must manage high-cost episodic and specialty care
more eectively. Future ACO eorts will incorporate
lessons learned from other models, including
bundled payment models, to drive coordinated and
ecient care.
These rst two generations of ACO models have
informed the development of new ACO models,
such as the Global and Professional Direct
Contracting (GPDC) Model. ACO models are a

INNOVATION CENTER STRATEGY REFRESH 17
• Pursue changes to risk adjustment and
benchmarking methodologies to drive
accountability and improve accuracy of
payments in CMS programs and Innovation
Center models.
• Work with the Medicare and Medicaid
programs, including the Medicare Shared
Savings Program and the Quality Payment
Programs, to better incentivize the transition
towards value-based care and encourage
alternative payment model (APM) participation.
• Ensure that Medicaid beneciaries – in
managed care and FFS programs – are not
only attributed to a provider but also in
arrangements that drive accountability for
quality, outcomes, and costs

INNOVATION CENTER STRATEGY REFRESH 18
Innovation Center Strategic Objective 2:
Advance Health Equity
Aim:
Embed health equity in every aspect of CMS Innovation Center
models and increase focus on underserved populations.
Measuring Progress:
• All new models will require participants to collect and report the
demographic data of their beneficiaries and, as appropriate, data on
social needs and social determinants of health. *
• All new models will include patients from historically underserved populations and safety net
providers, such as community health centers and disproportionate share hospitals.
• Identify areas for reducing inequities at the population level, such as avoidable admissions, and
set targets for reducing those inequities.
The CMS Innovation Center is committed to
developing a health system that advances health
equity, a goal that is integral to its mission to
improve health care quality. Healthy People 2030
defined health equlity as “the attainment of the
highest level of health for all people.”
11
Achieving this goal requires considering equity
12
in all stages of model development, including
ideation, development, recruitment,
implementation, and evaluation, and
harmonizing this approach across model tests.
The CMS Innovation Center will build on early
efforts to address health equity, which have laid
the groundwork for increasing and accelerating
efforts to ensure equity is embedded in the
design, testing, and evaluation of all models. The
Community Health Access and Rural
Transformation (CHART) and Pennsylvania
11 U.S. Department of Health and Human Services. (2021). Healthy People 2030 Questions & Answers.
12 As dened in the Racial Equity and Support for Underserved Communities Through the Federal Government Executive Order 13985,
the term “equity” means “The consistent and systematic fair, just, and impartial treatment of all individuals, including individuals who belong
to underserved communities that have been denied such treatment, such as Black, Latino, and Indigenous and Native American persons,
Asian Americans and Pacic Islanders and other persons of color; members of religious minorities; lesbian, gay, bisexual, transgender,
and queer (LGBTQ+) persons; persons with disabilities; persons who live in rural areas; and persons otherwise adversely aected by
persistent poverty or inequality. The term “underserved communities” refers to populations sharing a particular characteristic, as well as
geographic communities, that have been systematically denied a full opportunity to participate in aspects of economic, social, and civic life, as
exemplied by [the aforementioned list.]
Rural Health Models, for example, focus on
rural health access and outcomes, the Maternal
Opioid Misuse (MOM) model connects current
and expecting mothers enrolled in Medicaid to
substance use disorder treatment and wrap-
around services, and the Integrated Care for
Kids (InCK) model aims to improve prevention,
early identication, and treatment of children’s
behavioral and physical health needs. In addition,
the Accountable Health Communities (AHC)
Model is examining whether identifying and
addressing the health-related social needs of
Medicare and Medicaid beneciaries improves
health outcomes and reduces costs.
Recent evaluation results from the Next
Generation ACO model showed that aligned
Medicare beneciaries were more likely to
*Data would be collected in a manner in which PHI complies with HIPAA and other applicable laws.

INNOVATION CENTER STRATEGY REFRESH 19
be white and less likely to be either dually
eligible or to live in rural areas relative to other
FFS beneciaries in the same market areas.
13
Internal Innovation Center analysis of Medicare
beneciaries aligned to participants in other
models, including CPC+, PCF, and Global and
Professional Direct Contracting yielded similar
ndings. Recognizing this, the CMS Innovation
Center is committed to broadening the reach of
all models to underserved populations.
The CMS Innovation Center’s focused eorts to
advance equity encompass actions across the
following domains:
1. Develop new models and modify existing
models to address health equity and social
determinants of health (SDoH);
2. Increase the number of beneciaries from
underserved communities that receive care
through value-based payment models by
increasing the participation of Medicare and
Medicaid providers who serve them;
3. Evaluate models specically for their impact
on health equity and share data and “lessons
learned” to inform future work; and
4. Strengthen data collection and intersectional
analyses for populations dened by
demographic factors such as race, ethnicity,
language, geography, and disability—in
order to identify gaps in care and develop
interventions to address them (in a manner
that PHI complies with HIPAA and other
applicable laws).
Success will require partnerships with stakeholders
with deep expertise and experience in providing
equitable care for underserved populations,
including organizations that may not have
historically engaged with the Innovation Center.
13 NORC. (2020). Next Generation Accountable Care Organization Model Evaluation. See Exhibit 2.10.
Developing new models and modifying existing
models to address equity
The CMS Innovation Center has tested several
models that have had the potential to advance
equity – especially through advanced primary care
and ACO models; however, equity has not been
systematically addressed across the Innovation
Center’s portfolio of interventions. Eorts will now
include identication of opportunities to embed
equity across the life cycle of models, including
design, testing, and evaluation.
The Innovation Center has also supported model
tests that tackle beneciaries’ social needs and
will broaden its eorts to incorporate screening
tools and/or facilitate coordination with social
service providers, as in the AHC and MOM
models. In addition, the CMS Innovation Center
will also consider model tests that address issues
of specic concern to underserved populations,
which could include certain diseases, health
conditions, or care settings, as well as models that
seek to remedy upstream, community-level SDoH.
Increasing participation of underserved
beneficiaries and safety net providers
Health care providers participating in models
such as ACOs continue to have fewer Medicare
beneciaries from underserved populations
and generally include beneciaries who are less
likely to live in rural areas. To broaden the reach
of model tests to underserved beneciaries, the
Innovation Center will emphasize engagement
with local communities and public health leaders
in order to reach providers who may not have
previously participated in value-based care,
including those that disproportionately care for
uninsured, Medicaid, rural, and other underserved
populations. Examples of these providers include
community health centers, rural health clinics,
community-based providers, and public and
critical access hospitals.
Beyond outreach, the CMS Innovation Center is
reviewing its application and selection processes
to ensure such providers are not disadvantaged

INNOVATION CENTER STRATEGY REFRESH 20
or disincentivized from participating. Examining
the barriers and challenges safety net and
rural providers have faced in participating in
previous models can inform changes. Once in
models, safety net providers need dedicated—
and sometimes greater—nancial and technical
assistance to provide equitable care, given
that upfront infrastructure investments may
be needed for them to succeed in value-based
care arrangements. The Innovation Center is
considering a variety of incentives to encourage
and sustain participation, such as upfront
payments, social risk adjustment, benchmark
considerations, and payment incentives for
reducing disparities or screening for SDoH and
coordinating with community-based organizations
to address social needs. Technical assistance
may include application support, sharing of best
practices for caring for underserved populations,
and assistance with screening tools and data
collection workows.
Evaluating health equity impact
A critical component of the Innovation Center’s
health equity strategy is assessing the individual
and collective impact of models on underserved
populations, and eorts to do so will be aligned
with eorts across CMS. Standardized, hypothesis-
driven evaluation requirements and measures
for health impact assessment will be developed
early during the model design process. In addition,
the CMS Innovation Center will consider how to
measure health equity impact across its portfolio
of models, which will include retrospective review
as feasible. Finally, the Innovation Center will
determine how to share site-specic data and
evaluation ndings with participants and partners
during and at completion of models as feasible.
Increasing collection and analysis of
demographic data
Across model design, testing, and evaluation, the
availability of demographic data is fundamental
to the success of the Innovation Center’s strategic
objective focused on equity. The CMS Innovation
14 CDC/ATSDR Social Vulnerability Index. (2021)
15 University of Wisconsin, School of Medicine and Public Health, Department of Medicine. Neighborhood Atlas
®
.
Center will require participants in all new models
to collect and report data to identify and monitor
impacts on health and the reduction of disparities.
For existing models, requirements, incentives, or
other mechanisms to collect data from
participants will be considered, and CMS will
potentially examine the use of other federal data
sources such as T-MSIS to gain a greater
understanding of those being served. In addition,
the Innovation Center will continue to review and
curate its data repositories and will work with
federal partners to obtain additional demographic
data when appropriate and feasible. Common and
validated area-level indices, such as the Social
Vulnerability Index (SVI) and the Area Deprivation
Index (ADI), might be used to augment patient and
provider data.
14, 15
Data will be used to support
participants, including through the use of data
dashboards or other mechanisms for sharing.
Next Steps to Advance Equity
• Conduct and release analyses of characteristics
of participating providers and Medicare and
Medicaid beneciaries attributed to model
participants to help ensure equitable reach of
models.
• Develop approaches to model design and
the model application process to improve
participation of applicants that provide care for
underserved communities.
• Require and consider incentives or supports for
the collection of beneciary-level demographic
data (in a manner that PHI complies with HIPAA
and other applicable laws) to identify and
monitor impacts on underserved beneciaries
in CMS Innovation Center models.
• Incorporate screening and referral for social
needs, coordination with community-based
organizations, and processes to collect social
needs data in standardized formats.

INNOVATION CENTER STRATEGY REFRESH 21
• Incorporate equity in model quality strategies,
including quality measurement and monitoring
performance to incentivize the reduction of
health disparities.
• Provide learning supports to model
participants on equity (e.g., support
for participants caring for underserved
populations and best practices for partnering
with community-based organizations) and data
and model design support to states seeking to
align with Innovation Center models.

INNOVATION CENTER STRATEGY REFRESH 22
Innovation Center Strategic Objective 3:
Support Care Innovations
Aim:
Leverage a range of supports that enable integrated, person-
centered care such as actionable, practice-specific data,
technology, dissemination of best practices, peer-to-peer learning
collaboratives, and payment flexibilities.
Measuring Progress:
• Set targets to im
prove performance
of models on patient
experience measures, such as health and functional status, or a subset of
Consumer Assessme
nt of
Healthcare Providers and Systems (CAHPS®)
* measures that
assess health promotion and education,
shared decision-m
aking, and care coordination.
• All models will consider or include patient-reported outcomes as part of the
performance
measurement strategy.
Accountable care models, especially those that
include total cost of care approaches, will need
payment incentives to support the delivery of
integrated, equitable person-centered care. This
could include testing supports for providers
to deliver care that is more accessible and
convenient for beneciaries and to integrate
care across providers and settings. Driving care
innovations that facilitate person-centered care
should increase the proportion of people who
receive care that is aligned to their goals, values,
and preferences – and increase provider and
participant success in Innovation Center models.
Integrating Whole-Person Care
Person-centered care integrates individuals’ clinical
needs across providers and settings, as well as
addressing their social needs. For instance, areas
that can be explored for greater integration with
primary care include behavioral health, palliative care,
and care for beneciaries with complex needs and
serious illness, where there is signicant opportunity
to improve care and outcomes while reducing overall
costs.
16 HHS, Assistant Secretary for Planning and Evaluation. (2021). Overview of Social Determinants of Health (SDoH) and Equity in the
Context of Alternative Payment Models (APMs) and Physician-Focused Payment Models (PFPMs).
The CMS Innovation Center is examining how to
enhance addressing SDoH in models.
16
This includes
cross-model eorts to support providers’ ability to
address SDoH, including improving the collection and
precision of SDoH data, addressing evidence gaps
on what works, understanding beneciary needs
and the costs of services, improving coordination
between community-based organizations and health
care entities, better coordinating federal funding, and
identifying incentives to address SDoH in health care
settings.
Providing Payment and Regulatory Flexibilities
The Innovation Center has also tested a number
of payment and regulatory waivers and exibilities
in models to support the delivery of more person-
centered care including waivers of conditions
of payment for post-acute care rules, such as
requirement that the beneciary be determined
as homebound to receive home health care,
beneciary engagement incentives, such as oering
transportation, and other provider payment
arrangements that are otherwise not allowed in
Medicare FFS. For instance, a number of models use
telehealth waivers of originating site requirements in
* CAHPS® is a registered trademark of the Agency for Healthcare Research and Quality.

23
nancial measures. The goal is to help guide
participant decision making at the beginning of
the model, rather than providing this information
later in the performance period. These tools
are key to giving providers access to more user-
friendly information that also reduces their
administrative burden of participation. Finally,
the CMS Innovation Center will continue to work
across CMS and HHS to support adoption and
implementation of interoperability standards
that allow for the exchange of health data that
will enhance care delivery, support patient
engagement, and improve research on and
evaluation of models.
Next Steps to Provide Tools to Drive Care
Innovations
• Deepen and sustain outreach and solicitation
of input from beneciary and caregiver groups,
and providers on gaps in care and their impact,
preferences for home- and community-based
treatment choices, and supports to facilitate
provider-patient communication.
• Develop and test models or care delivery
innovations across models that address gaps
in care, such as behavioral health, SDoH, and
palliative care.
• Test payment waivers and regulatory
exibilities as participants move to total cost
of care models that can support home- and
community-based care that meets patient and
caregiver needs and preferences.
• Support providers in the delivery of person-
centered care through actionable, practice-
specic data, technology, dissemination of
best practices, and peer-to-peer learning
collaboratives to make more timely, actionable
data available to model participants in order
to both facilitate care that is responsive to
changing patient needs and that reduces
administrative burden.
• Accelerate sharing of best practices and tools
across participants to facilitate successful
model implementation and participation.
order to furnish care in new settings that are more
person-centric, such as home or community centers.
Moving forward, payment and regulatory exibilities
for model participants will be examined that can
support the provision of home or community-based
care, especially in models that are moving towards or
that encompass total cost of care. Last, it will be critical
to coordinate within CMS to identify opportunities for
program alignment and to share learnings.
Sharing Actionable Practice-Specific Data
Access to more actionable, close to real-time
data are needed to support providers in value-
based care arrangements. The CMS Innovation
Center is committed to making practice-specic
data on performance available and is considering
options for a more interactive value-based care
management system. As part of the PCF Model,
the Innovation Center is currently piloting a
tool that would provide model participants with
an interactive platform to assist in managing
patient-care. Such platforms are intended to
help providers better understand and forecast
their performance through interactive data
visualizations and dashboards that highlight
factors driving quality performance and can be
important tools to help facilitate person-centered
care at the practice level.
These eorts will also aim to simplify CMS
Innovation Center operations by helping to
automate beneciary attribution, risk adjustment,
and model payment calculations and tracking
quality measure performance. In addition,
CMS is exploring eorts to accelerate data
sharing, including the use of Fast Healthcare
Interoperability Resources-based (FHIR)
application program interfaces (APIs) such as the
Beneficiary Claims Data (BCD) API for sharing
claims data with participants. This BCD API option
is currently offered in the Global and Professional
Direct Contracting Model, a Medicare payment
model, with other models to follow. Further,
the Innovation Center is continuing to build
and share actionable dashboards such as in the
CHART Model in which participants will receive
a dashboard of their community’s baseline
performance on access to care, quality, and other
INNOVATION CENTER STRATEGY REFRESH

INNOVATION CENTER STRATEGY REFRESH 24
Innovation Center Strategic Objective 4:
Improve Access by Addressing Affordability
Aim:
Pursue strategies to address health care prices, affordability, and
reduce unnecessary or duplicative care.
Measuring Progress:
• Set targets to reduce the percentage of beneficiaries that forgo care
due to cost by 2030.
• All models will consider and include opportunities to improve affordability of high-value care by
beneficiaries.
The statutory provisions establishing the CMS
Innovation Center called for the testing of
models that are expected to reduce costs while
maintaining or improving the quality of care for
beneciaries of the Medicare, Medicaid, and CHIP
programs. Although national health spending
growth slowed between 2010-2019 compared to
the previous decade, costs are continuing to rise
at unsustainable rates, not just for the federal and
state governments, but also for households.
17
As a
result, aordability is an important consideration
in achieving the Innovation Center’s vision of
driving broad system transformation.
Reducing Program Expenditures to Lower Out-
of-pocket Costs for Beneficiaries
As cost pressures mount on individuals and families,
CMS Innovation Center models will focus not only on
reducing federal health expenditures, but also how
they can help lower out-of-pocket costs for Medicare
and Medicaid beneciaries and maintain access to
quality care. An example of this focus is the Part D
Senior Savings Model, which the CMS Innovation
Center launched to test the impact of oering
beneciaries Part D prescription drug plan options
that oer lower out-of-pocket costs and maintain
access to insulin. The Innovation Center will prioritize
models that test ways to lower beneciary and
program spending on drugs and incentivize the use
17 Center for Medicare and Medicaid Services (2020). National Health Expenditure Data.
of biosimilar and generic drug utilization to improve
quality and beneciary health. This could include
models that test innovative payment approaches
for Medicare Part B drugs, such as shared savings
and bundled payment models for episodes of care,
models that build on the Part D Senior Savings
Model or lower cost-sharing for Low-income Subsidy
(LIS) beneciaries utilizing biosimilar and generic
drugs, or future total cost of care models that could
include both Part B and Part D drugs. While Medicaid
beneciaries’ exposure to out-of-pocket costs is
more limited, they can still face co-pays and other
indirect nancial barriers to access care, such as lack
of access to transportation, child care, or taking time
from work to attend to medical issues.
Medicare beneciaries can also be subject to
dierential out-of-pocket costs for the same services
depending on where they are delivered (e.g., in a
hospital outpatient department or a physician’s
oce). The Radiation Oncology Model is one
example of Medicare testing an innovative payment
where the amount paid does not vary by care setting
or how much care is delivered over time. Given
the potential to reduce Medicare spending and
beneciary out-of-pocket costs, the CMS Innovation
Center could consider models that include site-
neutral payments for services oered in dierent
settings.

INNOVATION CENTER STRATEGY REFRESH 25
enable model participants to provide home visits
following a hospital discharge or for beneciaries
at high risk of hospitalization. In designing new
models and modifying existing models, payment
waivers such as these can be tested to enable
model participants to provide enhanced Medicare
services under the model.
Innovation Center models have also involved
additional exibilities, including beneciary
engagement incentives, many of which involve
incentivizing choices to use high-value services.
For instance, in certain FFS models, the
Innovation Center has permitted participating
providers to reduce or eliminate beneciary
co-pays for high-value care such as primary
care services and certain other Part B services.
Other beneciary incentives include preventive
care items and services that advance a clinical
goal, such as vouchers for over-the-counter
medications recommended by their providers. In
designing new and modifying existing models, the
Innovation Center may explore the use of these
and other exibilities.
Increasing Utilization of High-Value Care –
Regulatory, Beneficiary, and Plan Flexibilities
Duplicative or wasteful care is dened as
services that are not needed, increase costs,
and may cause harm. These can be harmful
to and inecient for patients and ultimately
cause signicant waste of valuable health care
resources and dollars, including out-of-pocket
costs. The Innovation Center has also used
and is exploring the use of other model design
features and incentives to increase the delivery
of higher value care. For instance, accountable
care models with total cost of care approaches
could be used to reduce waste and encourage
high-value care.
Payment Waiver and Other Flexibilities.
Payment waivers and other flexibilities can enable
providers and suppliers to encourage beneficiaries
to use more high-value services. For instance, the
Innovation Center has tested a number
of payment waivers to support the delivery of
high-value care in dierent models, including
waivers of physician supervision requirements to

26
In addition, the Innovation Center establishes
quality metrics for each model that frequently
aect payment. For example, many models are
structured such that participating providers may
share in savings with CMS, but these savings may
be adjusted or contingent based on achieving
specic quality performance thresholds. The CMS
Innovation Center is exploring how quality metrics
may also be used in models to promote greater
beneciary use of high-value services.
Next Steps to Provide Tools to Improve Access
by Addressing Affordability
• Identify ways to align or integrate episode
payment models with accountable care and
other total cost of care models to ensure
delivery of accountable and aordable
specialty care in addition to robust advanced
primary care.
• Identify areas where Innovation Center
models can test eorts to reduce program
expenditures, which may also lower out-of-
pocket costs for beneciaries.
• Explore model tests that make changes to
payment structures for specialty care that
results in the delivery of high-value person-
centered care.
• Include payment waivers and other exibilities
in total cost of care models to incentivize use
of high-value services across Innovation Center
models and benet designs.
Value-based Insurance Design (VBID). Under
VBID, health plans modify the incentives that they
offer to enrollees to encourage high-value care. The
Innovation Center is testing VBID in the Medicare
Advantage program, allowing plans exibility to
provide supplemental benets for beneciaries
based on health conditions and/or socioeconomic
factors. These benets include reduced cost-sharing
for high value care, access to new and existing
technologies and FDA-approved medical devices,
vouchers for transportation to health care visits and
for over-the-counter medications recommended
by their providers, as well as items and services
that have a reasonable expectation of improving
or maintaining the health or overall function of an
enrollee with regard to the chronic condition or
socioeconomic status, which may include food and
housing supports. The model also requires plans to
engage with their enrollees in wellness and advance
care planning, and some plans are also testing
access to concurrent hospice care. Lessons learned
from these eorts could be tested more broadly to
increase utilization of high-value care in future CMS
Innovation Center eorts.
Increasing Utilization of High-Value Care –
Provider efforts
The strategic refresh includes a focus on
creating nancial incentives and support for
providers to deliver high-value care while
eliminating duplicative or wasteful services.
Model strategies may include testing payment
targets and implementing payment structures
that foster greater accountability by reducing
the delivery of duplicative or wasteful services
and for overall spending and outcomes. Through
episodic payments for all care furnished during
an episode of intense treatment, the CMS
Innovation Center tests ways to foster greater
appropriateness in the choice of high-value
care, as well as ways of generating eciency in
operations and administration. For example,
skilled nursing facility use after an acute care
hospitalization has declined significantly under
BPCI Advanced episodes without compromising
quality and outcomes for beneficiaries.
INNOVATION CENTER STRATEGY REFRESH

27
Innovation Center Strategic Objective 5:
Partner to Achieve System Transformation
Aim:
Align priorities and policies across CMS and aggressively engage
payers, purchasers, providers,
states and beneficiaries to
improve quality, to achieve equitable outcomes, and to reduce
health care costs.
Measuring Progress:
• Where applicable, all new models will make multi-payer
alignment available by 2030.
• All new models will collect and integrate patient perspectives across the life cycle.
•
The CMS Innovation Center’s vision for broad
health system transformation is ambitious and
requires
collaboration with and actions by a wide
range of stakeholders. In particular, alignment with
private payers, purchasers, and states is needed
to increase the number of providers participating
in value-based payment models and to make their
participation sustainable across payers. Achieving
this vision requires working across CMS and
beyond, taking a whole-of-government approach
– and collaborating with employers, health plans,
and states, as well as with patients, caregivers,
providers, and community organizations.
CMS Health Care Payment Learning and Action
Network (LAN) and Private Purchasers and
Payers
The
CMS Innovation Center has historically engaged
with external partners in dierent ways. The
Health Care Payment Learning and Action Network
(LAN), a public-private collaboration funded by
HHS through the Innovation Center, is the most
public, structured, and signicant mechanism for
engagement and partnerships centered on shared
goals with external stakeholders. The LAN and its
participants will be critical partners in ensuring
INNOVA
TION CENTER STRATEGY REFRESH
successful implementation of the refreshed
strategy, particularly in achieving the goals of
multi-payer alignment by increasing the number of
providers that are sustainably participating in value-
based payment models and to advance system
transformation nationally.
State and Medicaid partners
In a number of CMS Innovation Center models,
such as the State Innovation Model (SIM), CPC+,
the Maryland Total Cost of Care Model, the
Vermont All Payer ACO Model, CHART, OCM, the
Pennsylvania Rural Health Model, and PCF, CMS
is partnering with other payers and/or states to
amplify the model’s impact across Medicare and
Medicaid, as well as commercial payers, in some
cases. Providers have found that multi-payer
alignment can make it easier to transition to
value-based care. Recognizing that payers are in
dierent stages of the value-based care journey
with their own operational considerations, the
Innovation Center will build on lessons learned
from these eorts to work more closely with
CMCS to drive alignment on critical payment and
operational design components such as clinical
tools, outcome measures, and payment.

INNOVATION CENTER STRATEGY REFRESH 28
initiatives. Federal collaboration can also help
examine ways that federal investments to address
social needs can be used more eectively with
Medicare and Medicaid payments to achieve
improved and more sustainable outcomes. To
start, partnerships will be formed in areas of
shared interest, such as health equity, accountable
care, SDoH, state-based transformation, measure
alignment, and health information technology and
interoperability.
Next Steps to Partner to Achieve Health System
Transformation
• Focus on opportunities to drive multi-payer
alignment, especially with Medicaid programs,
during development of new models.
• Strengthen partnerships with beneciary,
caregiver, and patient groups, as well as
providers, and solicit input and feedback to
understand care needs and challenges that can
be addressed across the life cycle of models.
• Make model data more easily available to
stakeholders to advance transparency on
model performance and to support external
research and learnings.
• Focus the collaboration with the LAN and
its members on achieving the vision of the
Innovation Center’s strategic refresh, especially
in terms of advancing health equity and
advancing multi-payer alignment.
Beneficiary collaborations
Closer collaborations with beneciaries, caregivers,
and patient groups across the lifecycle of models
from conceptualization to evaluation and potential
model expansion will help ensure that existing
and new models are meeting people’s needs –
and not just the needs of providers. Public input
is also critical to developing and testing tools
that support person-centered care. However,
patient and caregiver perspectives are not often
brought to the process early enough to inuence
the development of care management tools and
programs, payment incentives for providers, and
payment waivers and other exibilities. Across all
of the strategic objectives in the CMS Innovation
Center’s refreshed vision, beneciary and patient
engagement and collaboration is a key mechanism
for driving broad system transformation.
Health equity partnerships
Working with groups with deep expertise and
experience in providing equitable care for
underserved populations, including community-
based organizations and other entities that have
historically not engaged with the Innovation
Center, will be critical to increasing the reach of
value-based models to underrepresented and
underserved populations. Such collaborations
will benet model design, implementation, and
evaluations.
CMS, HHS, and other federal partnerships
Achieving broad health system transformation
requires working across CMS, HHS, and the
federal government. Every part of the Innovation
Center’s strategy and work moving forward could
be strengthened by successfully engaging federal
partners for their insights and support in testing
new approaches to payment and care delivery
and incorporating lessons learned from other
programs into CMS Innovation Center models.
These enhanced federal partnerships will assist
in facilitating the adoption of the CMS Innovation
Center’s lessons learned into the Medicare and
Medicaid programs, improving care and reducing
costs and improving and automating the collection
and analysis of data that can support decision
making on models, program changes, and new

INNOVATION CENTER STRATEGY REFRESH 29
We anticipate this will assist researchers in
generating valuable insights on the impacts of
models and design features on quality,
outcomes, and costs. We also note that many
models engage in data collection for clinical
information not submitted on claims and
through various surveys. The CMS Innovation
Center is also actively working to identify and
prepare additional data les from these model
specic data collections in order to further
supplement and enrich the data available
for analysis in the VRDC. Making additional
supplemental summary-level, de-identied data
on model performance available on the website
would allow those stakeholders who do not
work in the VRDC additional insights into the
models.
3. Dening Success. The CMS Innovation Center’s
overarching goal will continue to be expansion of
successful models that reduce program costs and
improve quality and outcomes for Medicare and
Medicaid beneciaries. The statutory language
creating the Innovation Center stipulated that a
model that reduces costs or improves quality can
be expanded in duration and scope only if the CMS
Chief Actuary certies that it would not increase net
program spending in addition to meeting certain
other requirements outlined in the ACA. However,
only a handful of models have met the certication
standard. In addition to reducing costs or improving
quality, model success will also be considered for
impacts on health equity, person-centered care,
and health system transformation–eorts which
are aligned with CMS-wide goals.
This would entail eorts such as tracking
progress on the metrics oered in this white
paper for each of the strategic objectives, using
qualitative research ndings to understand
model impacts on beneciaries, providers,
and health care markets (see Table 3). A
more systematic and structured approach
to understanding model impacts on these
broader factors could help inform not only the
CMS Innovation Center’s future models, but
also other payers and providers in their move
to value-based payment and care.
CMS Innovation Center Commitment to
Transparency and Communication
In order for implementation of the strategy outlined
here to be successful, the Innovation Center
must improve the transparency of its work and
communication with key stakeholders. As part of
the strategy refresh, the following issues have been
identied as critical to implementation of each of
the ve objectives:
1. Stakeholder Outreach. The CMS Innovation
Center is committed to strengthening
communication with stakeholders. This work
starts with beneficiaries and patient advocates to
help ensure that their perspectives and needs are
a key driver to designing and deploying care
innovations that facilitate integrated, high-value,
and affordable care. New and more consistent
mechanisms for outreach will include regular
listening sessions with existing and new partners,
private purchasers and payers, providers, and
other model participants, and broad Innovation
Center participation in stakeholder events. It will
also be critical to speak with non-participants to
understand barriers to participating in prior or
current models – and how future models can be
designed for them to participate.
2. Data Transparency. Transforming the health
system will require generating insights and
learnings from models with leaders and experts
outside of the CMS Innovation Center, making
sharing data on models an imperative. As a first
step, the Innovation Center is piloting efforts to
share research identifiable files via the CMS
Virtual Research Data Center (VRDC) so that
researchers may link claims data with model
participant lists (in a manner that safeguards PHI
and is consistent with HIPAA and other
applicable laws) to identify model claims data
sets for analysis. Lessons are also being
examined from the Medicare Shared Savings
Program, which provides research identifiable
files on beneficiaries assigned to and providers
participating in ACOs and that are updated on a
regular basis and available to researchers.
INNOVATION CENTER STRATEGY REFRESH 30
Table 3. Approaches to Assessing CMS Innovation Center Impact.
Categories for Assessing CMS
Innovation Center Model Impact
Examples of Metrics
Beneficiary Impacts
• Patient experience
• Functional status improvements
• Population level metrics, such as avoidable admissions
• Quality of care transitions across settings
• Access to follow-up care
• Coordination across providers
• Access to home- and community-based care
• Access to telehealth services and other forms of virtual care
• Disparities in outcomes by demographic characteristics
• Beneficiary costs
Provider Impacts
• Care transformation
• Impact on administrative burden
• Level of alignment on models across payers
• Sustainability of participation in models
• Access to actionable, more real-time data to inform care
management
Market Impacts
• Level of consolidation
• New linkages or relationships between providers
• Spread of model elements to other payers
• Scalability of model to other regions or payers
• Generalizability of impacts to other populations
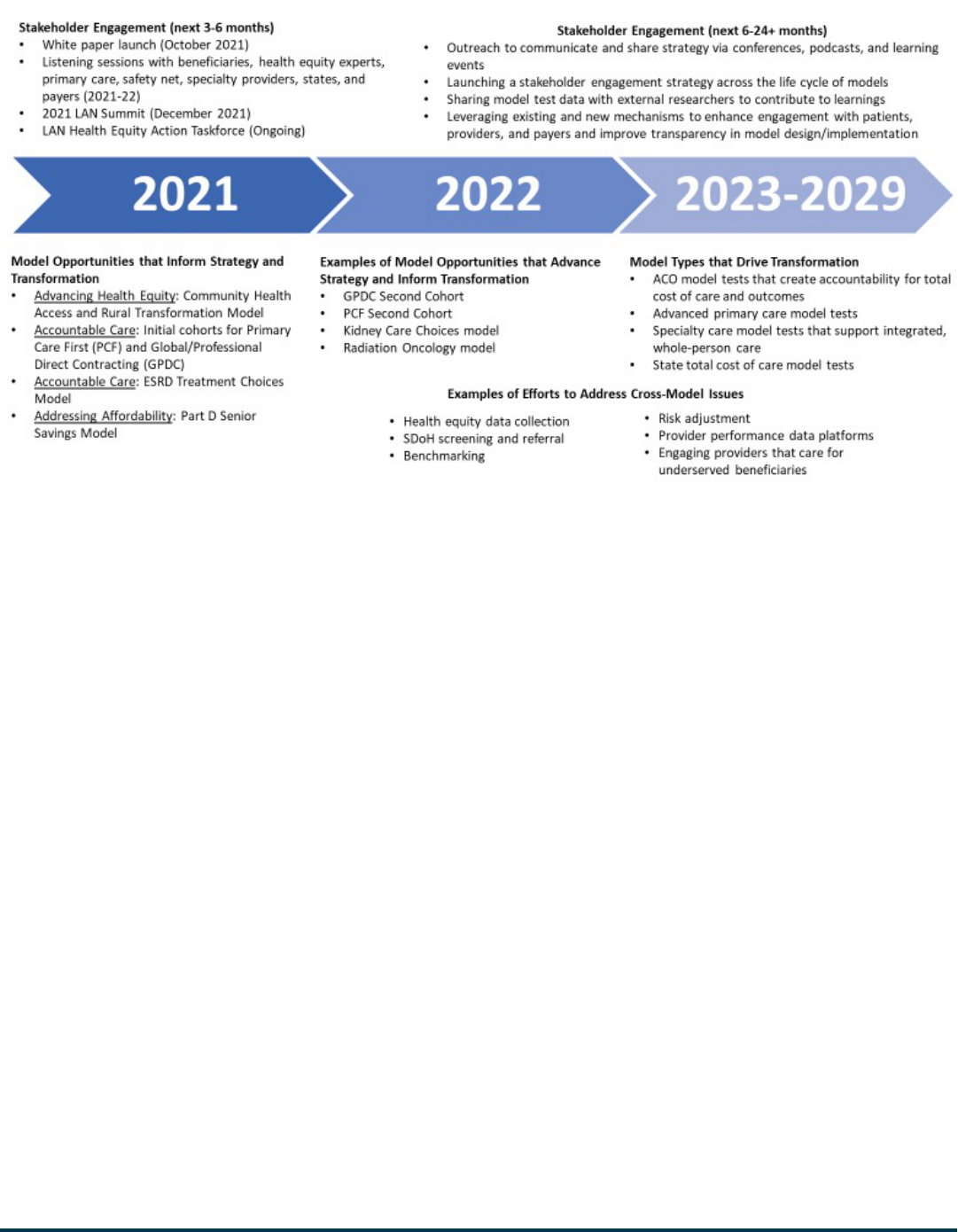
INNOVATION CENTER STRATEGY REFRESH 31
A commitment to transparency and improved and regular communication with stakeholders and the
research community, including providing more information about forthcoming models, will accelerate
the Innovation Center’s mission to drive value-based payment across the health system – and ability to
achieve its renewed vision.
Figure 4. CMS Innovation Center Strategy – Moving to Implementation.

INNOVATION CENTER STRATEGY REFRESH 32
Looking Forward
The CMS Innovation Center enters its second
decade with a solid foundation of models,
results, and lessons learned that can be
leveraged to achieve a bold, renewed vision
by 2030. A commitment to the ve strategic
objectives and to measuring progress against
dened metrics will guide revisions to existing
models and the development of a more
streamlined portfolio that can drive broad
system transformation. Cross-cutting issues
identied in this white paper will be critical
to success, including engaging in deeper
collaborations with beneciaries and patient
advocates, advancing access to value-based
care for underserved populations, and sharing
data with external researchers and experts
to accelerate learning. As part of achieving
the Innovation Center’s renewed vision, its
contribution to building a health system of the
future that achieves equitable outcomes through
high-quality, affordable, person-centered care
will need to be assessed. Beyond reducing costs
and improving quality, success must also be
measured by how its models impact CMS
programs, patients and families, providers,
payers, states, and the broader health care
system to ensure all benet from and participate
in this vision.
Streamlining and Harmonizing
CMS Innovation Center Models
To build a more harmonized and streamlined
portfolio of models, the CMS Innovation
Center will consider a number of issues to
guide model development and renement
moving forward.
• How would a model support or advance one
or more of the five strategic objectives?
• What are the potential impacts of a model on
health system transformation for
beneficiaries and patients, providers, payers,
states, and the Medicare and Medicaid
programs?
• What is the likelihood of successful execution
of a model?
• What is the potential for adoption and scaling
by other payers and providers?
• What is the potential for a model to support
innovation in the Medicare and Medicaid
programs more broadly?
