
Department of Health & Human Services
2014 ACTUARIAL REPORT
ON THE FINANCIAL OUTLOOK
FOR MEDICAID
Office of the Actuary
Centers for Medicare & Medicaid Services
United States Department of Health & Human Services
Report to Congress
2014 ACTUARIAL REPORT ON THE FINANCIAL OUTLOOK FOR
MEDICAID
Sylvia Mathews Burwell
Secretary of Health and Human Services
2014
2014 ACTUARIAL REPORT
ON THE FINANCIAL OUTLOOK
FOR MEDICAID
Prepared by:
Christopher J. Truffer, FSA, MAAA
Christian J. Wolfe, ASA, MAAA
Kathryn E. Rennie, ASA
Office of the Actuary
Centers for Medicare & Medicaid Services
United States Department of Health & Human Services
i
STATEMENT FROM THE CHIEF ACTUARY
The Medicaid program is of critical importance to American society. It is the largest
health program as measured by enrollment and represents one-sixth of the national
health economy. In 2013, its outlays of $457.8 billion accounted for a sizeable
portion of Federal and State budgets and were a significant source of revenue for
health care providers and insurers. As importantly, Medicaid serves as a safety net
for the Nation’s most vulnerable populations, covering about 59 million
beneficiaries in 2013. In this report, we analyze key historical Medicaid trends and
include projections of expenditures and enrollment with the goal to inform the
public and help policy makers gain insight into the future of the program.
Projections of health care costs are inherently uncertain. For Medicaid, such
projections present an even greater challenge as enrollment and costs are very
sensitive to economic conditions. The economic assumptions used to generate the
Medicaid projections in this report are the same as those used by the 2014 Social
Security and Medicare Boards of Trustees in their annual reports to Congress.
The projections in this report also include the expected significant effects of the
Affordable Care Act. This legislation has greatly reduced the number of uninsured
people in the U.S., largely as a result of expanded eligibility criteria for Medicaid.
We estimate that an average of 5.7 million newly eligible adults were covered in
calendar year 2014 and will increase to about 12.0 million in 2023. Medicaid costs,
particularly for the federal government, which pays a greater proportion of costs for
newly eligible individuals, will also grow significantly as a result of these changes.
The effects of the newly eligible population are presented throughout the report.
It is my opinion that (i) the techniques and methodology used herein to project the
future costs of the Medicaid program are based upon sound principles of actuarial
practice and are generally accepted within the actuarial profession, and (ii) the
principal assumptions and resulting actuarial estimates are, individually and in the
aggregate, reasonable for the purpose of projecting such costs under current law.
Considering the substantial uncertainties inherent in projecting future health care
costs, actual future Medicaid costs could differ significantly from these estimates.
I would like to thank team leader Chris Truffer and team members C.J. Wolfe and
Katie Rennie for their diligent efforts in preparing this report. We welcome
feedback from readers; comments may be sent to [email protected].
Paul Spitalnic, ASA, MAAA
Chief Actuary
Centers for Medicare & Medicaid Services
ii
EXECUTIVE SUMMARY
The joint Federal-State Medicaid program provides health care assistance to certain
low-income people and is one of the largest payers for health care in the United
States. This report presents an analysis of past Medicaid trends and 10-year
projections of expenditures and enrollment, including the impacts of the recent
eligibility changes under the Affordable Care Act. Like other projections of future
health care costs and coverage, these projections are subject to uncertainty.
HIGHLIGHTS AND FINDINGS
2013 Medicaid Information
• Total Medicaid outlays in Federal fiscal year (FY) 2013 were $457.8 billion;
$265.4 billion or 58 percent represented Federal spending, and $192.5 billion
or 42 percent represented State spending. Medicaid outlays increased by
6.1 percent between 2012 and 2013.
• Medicaid provided health care assistance for an estimated 58.9 million people
on average in 2013. An estimated total of 72.5 million people, or about one of
every five persons in the U.S., were enrolled in Medicaid for at least
one month in 2013. Enrollment is estimated to have grown by 1.6 percent
between 2012 and 2013.
• Per enrollee spending for health goods and services is estimated to have been
$6,897 in 2013. Estimated per enrollee spending for children ($2,807) and
adults ($4,391) was much lower than that for aged ($15,483) and disabled
($17,352) beneficiaries, reflecting the differing health statuses of, and use of
goods and services by, the members of these groups. Per enrollee spending is
estimated to have increased by 2.7 percent in 2013. (These figures exclude
expenditures for U.S. Territories, administration, collections and prior period
adjustments, and disproportionate share hospital payments. Per enrollee
spending including these expenditures increased 4.2 percent from 2012 to
2013.)
2014 Medicaid Estimates
• Medicaid expenditures are estimated to have increased 9.4 percent to
$498.9 billion in 2014, which includes the expenditures for newly eligible
enrollees. Because the Federal government paid for 100 percent of the costs of
newly eligible enrollees, the Federal share of all Medicaid expenditures is
estimated to have increased to 60 percent in 2014, and Federal expenditures
are estimated to have grown 13.9 percent to $299.7 billion.
• Average Medicaid enrollment is estimated to have increased 9.6 percent to
64.6 million people in 2014. Newly eligible adults are estimated to have
iii
accounted for 4.3 million of the 5.7-million enrollee increase from 2013 to
2014.
10-Year Medicaid Projections
• Over the next 10 years, expenditures are projected to increase at an average
annual rate of 6.2 percent and to reach $835.0 billion by 2023.
• Average enrollment is projected to increase at an average annual rate of
3.0 percent over the next 10 years and to reach 78.8 million in 2023.
Impacts of the Eligibility Changes under the Affordable Care Act
• Medicaid expenditures for adults newly eligible under the Affordable Care
Act are projected to amount to $457 billion from 2014 through 2023, or about
7 percent of total projected Medicaid spending over the 10-year period. Most
of this increase—$426 billion, or about 93 percent—is projected to be paid by
the Federal government. This amount would represent growth of about
11 percent in Federal Medicaid expenditures over 2014 through 2023.
• An average of 4.3 million newly eligible adults are projected to have been
enrolled in 2014, and newly eligible adult enrollment is projected to reach
12.0 million people by 2023—representing 7 percent and 15 percent,
respectively, of total projected program enrollment. These estimates are
based on preliminary 2014 data and the assumption that additional States
would expand eligibility, such that 50 percent of potentially newly eligible
enrollees reside in States that expanded Medicaid eligibility by 2015, and
60 percent reside in States that will expand eligibility by 2016 and later
years.
iv
CONTENTS
STATEMENT FROM THE CHIEF ACTUARY ............................. i
EXECUTIVE SUMMARY ............................................. ii
CONTENTS ........................................................ iv
I. INTRODUCTION .................................................. 1
II. OVERVIEW OF MEDICAID ........................................ 2
III. DATA AND ASSUMPTIONS ....................................... 5
IV. METHODOLOGY ............................................... 11
V. ACTUARIAL ANALYSIS .......................................... 15
A. FY 2013 MEDICAID OUTLAYS AND ENROLLMENT ................ 15
B. HISTORICAL MEDICAID TRENDS .............................. 20
C. MEDICAID EXPENDITURES AND ENROLLMENT PROJECTIONS,
FY 2014–FY 2023 ............................................. 23
D. IMPACTS OF THE MEDICAID ELIGIBILITY EXPANSION ........... 36
E. COMPARISON TO 2013 REPORT PROJECTIONS................... 40
F. MEDICAID IN CONTEXT ....................................... 42
VI. CONCLUSION ................................................. 47
VII. APPENDIX .................................................... 49
A. MEDICAID DATA SOURCES .................................... 49
B. DEMOGRAPHIC, ECONOMIC, AND HEALTH CARE ASSUMPTIONS .. 51
C. DATA POINTS FOR SELECTED FIGURES ........................ 60
1
I. INTRODUCTION
Medicaid is a cooperative program between the Federal and State governments to
pay for health care and medical services for certain low-income persons in the
United States and its Territories. The Federal and the State governments share
responsibilities in designing, administering, and funding the program. The Centers
for Medicare & Medicaid Services (CMS) is the agency charged with administering
Medicaid for the Federal government.
This is the sixth annual Medicaid report prepared by the Office of the Actuary
(OACT) at CMS. The purpose of this report is to describe the past and projected
trends for Medicaid expenditures and enrollment, including estimates for Federal
fiscal years (FYs) 2013 and 2014 and projections over the next 10 years. In addition,
this report discusses the impacts of the Affordable Care Act, which reflect the
expansion of Medicaid eligibility beginning in 2014. It also describes the data
available on Medicaid spending and enrollment, as well as the methodology and
assumptions used in the projections. Finally, this report places the Medicaid
program within the context of Federal and State government spending and the U.S.
health care system.

2
II. OVERVIEW OF MEDICAID
Authorized by Title XIX of the Social Security Act, Medicaid was signed into law in
1965 and is an optional program for the States. Currently all States, the District of
Columbia, and all of the Territories have Medicaid programs.
1
The Federal government establishes certain requirements for the States’ Medicaid
programs. The States then administer their own programs, determining the eligibility
of applicants, deciding which health services to cover, setting provider reimbursement
rates, paying for a portion of the total program, and processing claims.
Eligibility for enrollment in Medicaid is determined by both Federal and State law.
Title XIX of the Social Security Act specifies which groups of people must be
eligible, and States have the flexibility to extend coverage to additional groups. In
addition to income, eligibility is typically based on several other factors, including
age, disability status, other government assistance, other health or medical
conditions such as pregnancy, and in some cases financial resources (or assets).
Beginning January 2014, the Affordable Care Act provides the States the authority
under their State plan to expand Medicaid eligibility to almost all individuals under
age 65 who are living in families with income below 138 percent of the Federal
poverty level (FPL) (and who are citizens or eligible legal residents), with the
Federal government paying 100 percent of the costs for newly eligible adults.
2
Title XIX specifies that certain medical services must be covered under Medicaid,
while also granting the States flexibility to cover many other benefits. Services
usually covered include hospital care, physician services, laboratory and other
diagnostic tests, prescription drugs, dental care, and many long-term care services.
The States also have the options to use managed care plans to provide and
coordinate benefits and to apply for waivers that allow the States more flexibility in
developing specialized benefit packages for specific populations. With limited
exceptions, States must provide the same benefit package to all core Medicaid
enrollees. Exceptions to these requirements include the use of waivers,
demonstration projects, and alternative benefit plans. In addition, there may be
limited benefits provided for individuals who are eligible based only on medical
1
For more information on Medicaid, including information on eligibility and covered services, see
B. Klees, C. Wolfe, and C. Curtis, “Brief Summaries of Medicare & Medicaid,” November 2014:
http://www.cms.gov/Research-Statistics-Data-and-Systems/Statistics-Trends-and-Reports/
MedicareProgramRatesStats/Downloads/MedicareMedicaidSummaries2014.pdf .
2
The estimated impacts of the expansion of Medicaid eligibility on enrollment and expenditures are
presented in the Actuarial Analysis section of this report. The Affordable Care Act technically
specifies an upper income threshold of 133 percent of the FPL but also allows a 5-percent income
disregard, making the effective threshold 138 percent. California, Connecticut, the District of
Columbia, Minnesota, New Jersey, and Washington State elected to expand eligibility to higher
income levels prior to 2014 under the Affordable Care Act. In addition, some States continue to
maintain eligibility levels above 133 percent of the FPL.

3
need, through Medicare savings programs, or through special family planning
groups.
3
Additionally, States must extend eligibility to all mandatory populations
and cover all mandatory services defined by Title XIX in order to receive Federal
matching funds for their Medicaid programs.
4
The Federal government and the States share the responsibility for funding
Medicaid. States pay providers or managed care organizations for Medicaid costs
and then report these payments to CMS. The Federal government pays for a
percentage of the costs of medical services by reimbursing each State; this
percentage, known as the Federal Medical Assistance Percentage (FMAP), is
calculated annually for each State based on a statutory formula that takes into
account State per capita income with some adjustments prescribed by legislation.
5
Notably, the Affordable Care Act specifies FMAPs for adult beneficiaries who are
newly eligible as a result of the Medicaid expansion that began in 2014 (in States
that implement the expansion). Additionally, the Federal government pays for a
portion of each State’s administration costs. Beneficiary cost sharing, such as
deductibles or co-payments, and beneficiary premiums are very limited in Medicaid
and do not represent a significant share of the total cost of health care goods and
services for Medicaid enrollees.
In contrast to the Federal Medicare program, Medicaid’s financial operations are
not financed through trust funds. Other than a very small amount of premium
revenue from enrollees, as noted above, and some other sources of State revenue
(such as some provider taxes), there are no dedicated revenue sources comparable to
the Medicare Hospital Insurance payroll tax. Medicaid costs are met primarily by
Federal and State general revenues, on an as-needed basis; the States may also rely
on local government revenues to finance a portion of their share of Medicaid costs.
The Federal financing is authorized through an annual appropriation by Congress.
These funds are then spent through daily draws from the general fund of the
Treasury in the amounts required to pay that day’s Federal matching amounts on
the State program expenditures. As a result, Medicaid outlays and revenues are
automatically in financial balance, there is no need to maintain a contingency
3
The Medicare Savings Programs provide assistance to low-income aged persons and persons with
disabilities for their share of Medicare costs. Different programs cover a combination of the
beneficiary’s Part A premium, Part B premium, Part A deductible, and Part B cost-sharing
requirements.
4
One notable exception to this requirement is for newly eligible adults added by the Affordable Care
Act. While the new adult eligibility category is technically a mandatory population, the Supreme
Court ruled that the Federal government cannot withhold Federal funding for the rest of the
Medicaid program for States that do not expand eligibility to this group. See National Federation of
Independent Business v. Sebelius, 132 S. Ct. 2566 (2012).
5
In general, Title XIX specifies that the FMAP for each State cannot be lower than 50 percent or
higher than 83 percent; in FY 2014, FMAPs ranged from 50.00 percent to 73.05 percent. Also,
Title XIX provides for specific FMAP levels for certain States and, in some cases, for specific services
or populations.

4
reserve, and, unlike Medicare, the “financial status” of the program is not in
question from an actuarial perspective.
Medicaid coverage is extremely valuable to the low-income individuals and families
who qualify for the health care services provided by the program. By extension, the
program is also valuable to society at large, as it enables the least-fortunate
members of the population to obtain the health care they need in an orderly way. It
is also important, of course, to consider the costs to society of providing this
coverage and to anticipate likely future trends in such costs. The balance of this
report is intended to describe these trends.
6
6
This report does not cover expenditures and enrollment under the Children’s Health Insurance
Program (CHIP), whether operated under Title XIX or Title XXI of the Social Security Act. CHIP
provides health coverage to many children in households with income above Medicaid eligibility
levels. CHIP funding is only authorized through 2017. Should CHIP funding not be reauthorized,
children enrolled in Medicaid expansion CHIP would be eligible for coverage in Medicaid. For the
purpose of this report, CHIP is assumed to be fully funded through the entire projection period, and
there are no assumed increases in expenditures or enrollment from children enrolled in CHIP
becoming eligible for Medicaid as a result of the expiration of CHIP funding.

5
III. DATA AND ASSUMPTIONS
Projections of Medicaid expenditures and enrollment are highly dependent on both
demographic and economic assumptions. The most important such assumptions are
those regarding the growth of health care prices, growth in the use of health care
goods and services, overall economic growth, individual wage growth, and
population growth. In addition, there are various “programmatic” factors that have
historically influenced Medicaid expenditure and enrollment trends, including
decisions by the States regarding eligibility and payment rules for their Medicaid
plans, the coverage of and enrollment in other health insurance programs, including
Medicare and private health insurance, and changes in the participation rates of
eligible persons in Medicaid. The projections also depend on the nature and quality
of the available data on Medicaid operations. This section describes the sources and
limitations of data and assumptions that are used to generate the Medicaid
projections shown in this report.
The data and assumptions on which these Medicaid projections are based are
derived from four major sources. The first source is CMS data, which are submitted
by the States to CMS on a regular basis.
7
The States provide a quarterly report of
spending by type of service; this report, known as the CMS-64 or Financial
Management Report (FMR), includes the separate Federal and State expenditures
for all Medicaid fee-for-service programs and capitation arrangements. The CMS-64
is available on a separate “Net Services” basis, which includes all collections and
prior period adjustments. These adjustments reflect payments for services that
were reimbursed by the Federal government in a different quarter than the services
were covered by the State, and collections reflect negative adjustments to
expenditures, such as recoveries for overpayments made in previous accounting
periods. In addition, in 2014 the CMS-64 began reporting monthly enrollment data
by enrollment category and quarterly expenditures for newly eligible adults.
8
The
Medicaid Statistical Information System (MSIS) contains both service and
demographic data supplied by the States, including provider payments and
enrollment counts. MSIS expenditure data include only total Medicaid expenditures
and do not provide data separately for Federal or State expenditures. The MSIS
data used for the analysis presented in this report are derived from two sources: the
7
More information on these sources is available on the CMS website at
http://medicaid.gov/Medicaid-CHIP-Program-Information/By-Topics/Data-and-Systems/MBES/
medicaid-budget-and-expenditure-system-MBES.html and http://www.medicaid.gov/Medicaid-CHIP-
Program-Information/By-Topics/Data-and-Systems/MSIS/Medicaid-Statistical-Information-
System.html. Additional detail is provided in the Appendix.
8
The CMS-64 reports enrollment and expenditures for enrollees in the “VIII group,” which includes
those persons who are eligible under the criteria of section 1902(a)(10)(A)(i)(VIII) of the Social
Security Act. Most enrollees in this group are newly eligible adults, but some adults who may have
been eligible under pre-2014 criteria are in this group as well. The CMS-64 provides data on both
newly eligible adults and other enrollees in the VIII group separately for 2014.

6
Annual Person Summary (APS) files for the underlying expenditure breakdown and
the MSIS State Summary Datamarts for the enrollment. OACT makes several
adjustments to these data to merge them together for use in preparing projections.
The Boards of Trustees for Old-Age, Survivors, and Disability Insurance (OASDI, or
Social Security) and Medicare constitute the second source for the data and
assumptions.
9
The projections in this Medicaid report are based on the same
economic and demographic assumptions that were developed by the Trustees and
used to determine the intermediate estimates presented in their statutory
2014 annual reports to Congress on the financial status of the OASDI and Medicare
programs. The Trustees’ intermediate economic assumptions are also used to
develop the health care service price forecasts underlying the projections in this
report.
10
The third source from which data and assumptions are derived is the Office of the
Actuary Health Reform Model (OHRM), which is primarily based on the Medical
Expenditure Panel Survey (MEPS) Household Component, though OHRM has also
incorporated available enrollment and expenditure data for newly eligible adults
from the CMS-64.
11
OACT developed and used the OHRM to estimate the impact of
proposed health care reform legislation, including the Affordable Care Act as
enacted, and subsequently used the model to estimate the anticipated effects of
implementing this law. The estimates from the OHRM are used to develop the
projections presented in this report for the increases in Medicaid expenditures and
enrollment due to the expansion of Medicaid eligibility and other provisions of the
9
The 2014 Annual Report of the Boards of Trustees of the Federal Hospital Insurance and Federal
Supplementary Medical Insurance Trust Funds (http://www.cms.gov/Research-Statistics-Data-and-
Systems/Statistics-Trends-and-Reports/ReportsTrustFunds/Downloads/TR2014.pdf) and The 2014
Annual Report of the Board of Trustees of the Federal Old-Age and Survivors Insurance and Federal
Disability Insurance Trust Funds (http://www.ssa.gov/OACT/TR/2014/tr2014.pdf).
10
These assumptions are different from those used for projections in the President’s Fiscal Year 2016
Budget. Consequently, the projections presented in this report usually differ somewhat from the
President’s Budget projections. In addition, due to differences in the timing of this report and the
Budget, later data are generally available for use in this report. Finally, while the Trustees’
economic assumptions underlie the health care service price forecasts for both the Medicare Trustees
Report and the Medicaid actuarial report, the two sets of price growth forecasts are not the same.
The two programs have significantly different statutory mechanisms for setting provider price
updates, and these differences are reflected in the update assumptions for each program.
11
More information on MEPS can be found at http://meps.ahrq.gov/mepsweb/.

7
Affordable Care Act. As a result, this report also relies on the data and assumptions
used by the OHRM.
12
In addition, OACT developed assumptions regarding States’ decisions to implement
the eligibility expansion. In National Federation of Independent Business v.
Sebelius, 132 S. Ct. 2566 (2012) (NFIB v. Sebelius), the Supreme Court ruled that a
State may not lose Federal funding for its existing program when it does not
implement the Medicaid eligibility expansion under the Affordable Care Act. OACT
estimated that 45 percent of all people who were potentially newly eligible Medicaid
enrollees resided in States that elected to expand Medicaid eligibility in 2014. To
develop an assumption about the effective national participation rate of the States
after 2014, OACT reviewed public information and statements for each State
regarding its intent to implement the expansion. Based on this information, OACT
assumed that 50 percent of all people who were potentially newly eligible Medicaid
enrollees in 2015 would reside in States that elected to expand Medicaid eligibility
and that, for 2016 and thereafter, 60 percent of such individuals would reside in
expansion States. OACT estimated that 45 percent of potentially newly eligible
enrollees resided in States that expanded eligibility in 2014.
In the future, the actual participation by States could differ from these
assumptions. A greater or lesser number of States could elect to expand eligibility
than has been assumed, and States’ decisions may change over time (either to
expand if they have not already done so or to end the expansion sometime in the
future). CMS policy guidance clarified that States would be required to expand
eligibility completely, as prescribed by the Affordable Care Act, to receive the
increased Federal matching rate; the assumptions used in this report are consistent
with this policy.
13
In addition, OACT estimated that the participation rate of persons eligible under
the pre-2014 criteria also increased in 2014 and that it would continue to increase
slightly thereafter. Even in States that did not expand eligibility, OACT estimated
that there would be increases in participation among eligible persons but that the
rate of increase would be about 20 percent less than in States that do expand
eligibility.
12
More information is contained in the memorandum titled “Estimated Financial Effects of the
Patient Protection and Affordable Care Act, as Amended,” which is available on the CMS website at
http://www.cms.gov/Research-Statistics-Data-and-Systems/Research/ActuarialStudies/Downloads/
PPACA_2010-04-22.pdf; however, the estimates of the Affordable Care Act’s impacts on Medicaid
have since been updated and are presented later in the report. A key assumption made in those
estimates and relied upon in these projections is that there would be a sufficient supply of health
care providers to meet the expected increases in demand for health care services, without
considering any market disruptions or price increases.
13
See “Frequently Asked Questions on Exchanges, Market Reforms and Medicaid,” December 10,
2012: http://medicaid.gov/State-Resource-Center/Frequently-Asked-Questions/.

8
The fourth source of underlying data and assumptions—national health
expenditure (NHE) historical data and projections—is used for comparing Medicaid
expenditures and enrollment with Medicare, private health insurance, and total
health care spending in the United States. OACT develops the NHE data and
projections.
14
It is important to note the limitations that are associated with the data described in
this section. First, the most recent complete APS data available are from 2010, and
2011 data were available for 45 States and the District of Columbia at the time
these projections were completed.
15
Additional enrollment data were obtainable from other MSIS reports. The latest
MSIS data available were from 2012 for 24 States and from 2011 for 48 States and
the District of Columbia. Accordingly, enrollment by eligibility group (children,
adults, aged, and disabled) was estimated for 2011, 2012 and 2013, incorporating
information from States with data available in those years (and for 2010 for those
States for which MSIS data were unavailable).
16
This is the only ready source of
complete enrollment data; consequently, to relate 2012 and 2013 actual
expenditures to the number of enrollees, OACT prepared estimates of Medicaid
enrollment for those 2 years (as well as for the States for which 2011 APS data were
not obtainable). MSIS also does not provide data on enrollment in Territory
programs, and thus enrollment figures for Territories are estimated from previous
data. As a result, the data have not been updated substantially from last year’s
report (2011 APS data were available for 29 States), and there is uncertainty
14
More information on the NHE historical accounts and projections is available on the CMS website
at http://www.cms.gov/Research-Statistics-Data-and-Systems/Statistics-Trends-and-Reports/
NationalHealthExpendData/index.html. Also, see M. Hartman, et al., “National Health Spending In
2013: Growth Slows, Remains In Step With The Overall Economy,” Health Affairs, January 2015;
34:150-160; and A. Sisko, et al., “National Health Expenditure Projections, 2013-23: Faster Growth
Expected With Expanded Coverage And Improving Economy,” Health Affairs, October 2014; 33:1841-
1850.
15
One additional State had 2011 enrollment data, but not expenditure data. The figures and
projections in this report include the 2011 enrollment data for that State and the 2010 expenditure
data by enrollment category.
16
In this report, child Medicaid enrollees include non-disabled children, children of unemployed
parents, and foster care children; adult Medicaid enrollees include non-disabled non-aged adults,
unemployed adults, and women covered under the Breast and Cervical Cancer Act expansion; and
disabled Medicaid enrollees include blind or disabled persons.

9
regarding the estimates of the number of enrollees and expenditures by enrollment
category in the most recent historical years.
17
Another qualification is that it was only in 2014 that the CMS-64 began providing
data on enrollment or spending by enrollment category (and, in the case of spending
by enrollment category, only for newly eligible adults or other adults in the “VIII
group”).
18
In addition, the definitions of medical service categories are not consistent
between the MSIS and the other CMS data sources. Adjustments are made to
develop a data set that contains not only service-level expenditures that match the
CMS-64 data but also expenditures by enrollment group; accordingly, the MSIS and
the CMS-64 are merged together to provide a more complete understanding of
Medicaid spending. Since the service definitions are different between these two
sources, MSIS data are used to estimate spending by enrollment group for each
Medicaid service reported in the CMS-64.
19
While every State that chose to expand
its program is reporting enrollment data in the CMS-64, regular updates to these
submissions indicate that the data are not yet final for 2014. OACT used data only
for the number of newly eligible adults enrolled and otherwise did not rely on the
enrollment data in the CMS-64 for this report.
Yet another limitation is the unavailability of comprehensive demographic,
macroeconomic, health care, and program assumptions specific to each State.
Because these State-specific assumptions are not available, it is not possible to
credibly project Medicaid spending or enrollment separately by State. In addition,
since the NHE data and projections use somewhat different definitions of Medicaid
spending and services than do the other Medicaid data sources, historical Medicaid
data and projections from the NHE accounts may not match the historical data and
projections presented here. A final caveat is that, although OACT reviewed the data
sources used in these projections for reasonableness, OACT relied on CMS program
components and the States to ensure the quality of the data.
The Medicaid expenditure and enrollment projections shown in this report are
based on current law; that is, they are consistent with current legislation and
17
CMS is in the process of transitioning Medicaid data from MSIS to the Transformed Medicaid
Statistical Information System (T-MSIS), but T-MSIS is not currently available. Until the system is
operational, it is unclear what data will be available and what form the data will take. CMS is
discontinuing the production of the APS files, and different approaches will likely be necessary to
incorporate data for 2012 and 2013 in future reports. More information about T-MSIS is available at
http://www.medicaid.gov/medicaid-chip-program-information/by-topics/data-and-systems/medicaid-
and-chip-operational-data.html.
18
The “VIII group” refers to enrollees who are eligible under section 1902(a)(10)(A)(i)(VIII) of the
Social Security Act, including newly eligible adults.
19
Certain services in the CMS-64 for which there is little to no history are combined with other
services assumed to have a matching underlying distribution of spending by eligibility category.

10
administrative policy regarding Medicaid as of January 1, 2015.
20,21
This analysis
does not attempt to forecast any future changes in policy or legislation that, if
realized, would affect the Medicaid program—including Federal Medicaid, State
Medicaid, or Medicare policy and legislation or other legislation that could affect
private health insurance plans. Thus, while changes in Federal or State Medicaid
policy have been a significant factor affecting the patterns of growth in expenditures
and enrollment over history, no future changes in policy are assumed (beyond those
already scheduled under current law).
Like any projection of future health care costs, the Medicaid projections presented
here are necessarily uncertain. Actual numbers of enrollees, the number of services
used, and the reimbursement levels per service will depend on all of the factors
described previously—none of which can be predicted with certainty. Past increases
in Medicaid and other health care costs have often been relatively volatile, adding
to the difficulty of correctly anticipating future trends. Moreover, the impacts of the
numerous sections of the Affordable Care Act that affect Medicaid, especially the
broadening of Medicaid eligibility in 2014, introduce additional uncertainty into
these projections. Finally, data sources that report the number of people who
became eligible for and enrolled in Medicaid in 2014 and their health care costs are
still incomplete; accordingly, while these estimates are more certain than those in
previous reports, they should still be considered uncertain due to the relative lack of
program data and experience to inform them and the uncertainty about which
States will expand their eligibility standards in the future.
For these reasons, the projections shown in this report should be regarded only as a
reasonable indication of future Medicaid costs under current law and from today’s
perspective. It is important to recognize that actual costs in the future could differ
significantly from these projections, as a result of (i) unanticipated developments in
demographic, economic, or health cost growth trends, (ii) effects of the Affordable
Care Act (such as the proportion of newly eligible individuals and families who
become enrolled) that differ from current estimates, or (iii) any further changes in
the legislation governing Medicaid.
20
The Medicare Access and CHIP Reauthorization Act of 2015 (Public Law 114-10) was signed into
law after the projections in this report were completed, and the effects of the legislation are not
reflected in the projections provided in the report.
21
Medicaid expenditures in this report include Part B premiums paid for dually eligible enrollees.
Consistent with the 2014 Medicare Trustees Report, the Part B estimates reflect a projected baseline
scenario, which includes an assumption of a legislative override of the scheduled Medicare physician
payment updates under the sustainable growth rate (SGR) system.

11
IV. METHODOLOGY
This section describes the methodology behind the projections of Medicaid spending
presented in this report.
Health actuaries typically base estimates of medical expenditures on three major
factors:
• C – the number of people enrolled in the program (“caseload”),
• U – the quantity of services each person uses (“utilization”), and
• P – the reimbursement (“price”) for each unit of service.
The product of these three factors yields an estimate of total expenditures for
medical services:
(1)
Direct application of equation (1) requires data on utilization and reimbursement
rates for Medicaid that are not currently available or practical to maintain.
22
An
alternative recursive approach is therefore used for the projections, as described
below.
Instead of using equation (1), the projection algorithm begins with development of
data on the current level of Medicaid expenditures, by eligibility category and by
type of medical service, to serve as a projection base. Changes in the three
determinants of expenditures in equation (1) are then projected for future years and
applied sequentially to the base year expenditures. Thus, if E
y
represents
expenditures in year y, then
(2)
where c
y+1
, u
y+1
, and p
y+1
are the assumed or projected rates of change in caseload,
utilization, and prices, respectively, between years y and y+1. Equation (2) is
applied separately to expenditures for each combination of the Medicaid eligibility
categories and categories for type of service.
With a few exceptions, caseload factors vary by eligibility category, price factors
vary by type of service, and utilization factors can vary by both eligibility category
and type of service. The projected caseload factors are determined by trend and
regression analysis of Medicaid enrollment data. Projections of future enrollment by
22
No comprehensive sources are available that track reimbursement rates and use by service for all
Medicaid programs. Because the expenditure data reported by the States in the CMS-64 are at an
aggregate service level, each category likely includes various services with different numbers of
claims and distinct reimbursement rates. Additionally, reimbursement rates and service use are
different for each State.

12
eligibility category are based on estimates of the change in the share of the U.S.
population enrolled in Medicaid, which has historically varied with the changes in
the unemployment rate. The relationship between Medicaid enrollment and
unemployment reflects (i) how many people are without other forms of insurance
and (ii) how many people might qualify for Medicaid based on its income
requirements. Historically, this relationship has varied by eligibility category, and,
in general, children and adult enrollment in Medicaid has been more sensitive to
changes in the unemployment rate, while enrollment of aged persons and persons
with disabilities has been relatively less sensitive.
Price changes are derived from economic forecasts produced for the 2014 Medicare
Trustees Report, including forecasts for economy-wide inflation, inflation for prices
of medical services, and wage growth. Utilization is treated as the residual between
total growth and the growth due to enrollment and price changes. The estimate of
utilization is determined by an analysis of the historical interrelationship of
expenditure, caseload, and price factor growth.
23
The residual factor, while termed
“utilization,” reflects not only the change in the average number of services per
enrollee but also changes in the “intensity” or average complexity of the services. In
addition, any errors in the measurement of the number of enrollees and price per
service are implicitly included in the residual.
The methodology used to calculate the utilization factor for the projections in this
year’s report has changed. Previously, the utilization factor was calculated across
all enrollees for each service. While this method was generally reliable, for some
services in which expenditures were disproportionately concentrated in one or two
enrollment categories, relative differences in enrollment growth among those
categories affected the calculation of the changes in utilization and in some cases
required adjustments to the projections. The new methodology calculates utilization
by service and by enrollment category, thereby producing a more reliable
calculation of utilization. For a number of services, historical utilization changes are
similar by enrollment category, and the same average utilization factor is used for
all enrollment categories in the projections. For other services, the utilization factor
may vary by enrollment category.
The results obtained from the “Caseload, Utilization, Price” (“CUP”) recursive
forecast, using equation (2), are frequently adjusted to be consistent with recent
expenditure data and outlay trends.
It is important to note that some of the reported expenditures in the financial data
are not projected using category- or service-specific growth rates with respect to
caseload, utilization, or price. Prior period adjustments and collections reported by
the States are combined from the financial reporting, and the net result is projected
23
More details on the trend residual methodology are included in the Appendix.

13
to increase at the underlying total Medicaid expenditure growth rate (which is
calculated net of all collections and prior period adjustments).
As noted previously, estimates of the impact of the Medicaid eligibility expansion of
the Affordable Care Act are derived from the results of the OHRM, as well as from
currently available data on Medicaid enrollment and expenditures from the CMS-
64.
24
This model is based on the MEPS, reweighted to match the spending and
insurance coverage estimates of the 2013-2023 NHE projections.
25
The OHRM
specifically estimates (i) the number of people who would become newly eligible for
Medicaid and would enroll as a result of the eligibility expansion; (ii) the number of
people who are already eligible for Medicaid, but are not enrolled, and who would
now enroll in the program as a result of the publicity and new assistance with the
application process that will result from the Affordable Care Act; and (iii) the
amount of the new enrollees’ per enrollee Medicaid expenditures once they enroll.
The results of the OHRM are adjusted using expenditure and enrollment data for
the newly eligible population on the CMS-64, which revises projected enrollment
and expenditures per enrollee in 2014 to reflect the most recent data.
The ultimate effective participation rate of persons who would have been uninsured
for a full year, but are newly eligible for Medicaid as a result of the Affordable Care
Act, is assumed to be 95 percent. For persons who would be eligible under current
Medicaid criteria and would otherwise be uninsured, about 70 percent of those in
States that expand Medicaid eligibility are assumed to enroll in Medicaid
ultimately; in States that do not expand Medicaid eligibility, about 56 percent of
non-newly eligible and otherwise uninsured persons are assumed to enroll
ultimately. These projections assume that some of the increase in participation in
Medicaid occurred prior to 2014 and is reflected in the growth in adult enrollment
between 2010 and 2013. In 2014 and 2015, the participation rates of those newly
eligible and non-newly eligible are assumed to be lower than the ultimate
participation rate (about 77 percent and 90 percent of the ultimate rates,
respectively).
These assumed rates are higher than actual Medicaid participation rates to date
and are based on the anticipated impacts of sections of the Affordable Care Act that
are intended to make the process of enrolling easier. In particular, simplified
eligibility determinations enable some individuals who have steady income and who
have applied for coverage to be enrolled through an expedited process using a prior
24
More information is contained in the memorandum titled “Estimated Financial Effects of the
Patient Protection and Affordable Care Act, as Amended,” which is available on the CMS website at
http://www.cms.gov/Research-Statistics-Data-and-Systems/Research/ActuarialStudies/Downloads/
PPACA_2010-04-22.pdf. These estimates have been updated to reflect more recent data and
information on the implementation of the many sections of the Affordable Care Act.
25
A. Sisko, et al., “National Health Expenditure Projections, 2013-23: Faster Growth Expected With
Expanded Coverage And Improving Economy.”
14
year’s income tax return as verification of eligibility for coverage. Moreover, the
legislation established State or federally facilitated Health Insurance Marketplaces,
which, among other responsibilities, facilitate the determination of individuals’ and
families’ eligibility for Federal financial assistance, either through Medicaid or
through the Federal premium and cost-sharing subsidies for private health
insurance plans. In addition, the more widespread availability of financial
assistance under the Affordable Care Act (for individuals and families with incomes
up to 400 percent of FPL) is anticipated to reduce any stigma associated with
receipt of such assistance through Medicaid. While final data for 2014 are not yet
available, preliminary data suggest that enrollment levels are generally consistent
with these assumptions.
In National Federation of Independent Business (NFIB) v. Sebelius, the Supreme
Court ruled that a State may not lose Federal funding for its existing program if it
does not implement the Medicaid eligibility expansion under the Affordable Care
Act. Based on the information currently available about the States’ intentions for
their Medicaid programs, it is estimated that (i) 50 percent of potentially newly
eligible persons lived in States that would expand eligibility in 2015, and (ii) in 2016
and later years, 60 percent of potentially newly eligible persons will reside in States
that would expand eligibility as additional States implement the eligibility
expansion.
It is possible that more or fewer States may expand Medicaid eligibility than have
been assumed for 2015 and later years. To the extent that the actual number of
States opting for expansion differs from the assumptions used in these projections,
future costs and enrollment would likely differ by a similar proportion, taking into
account the sizes of the potential newly eligible populations in those States.
To estimate expenditures by service category for newly eligible Medicaid enrollees,
OACT used currently available data from the CMS-64 on expenditures by service
category for newly eligible adults. More details on the estimates of Medicaid
impacts of the eligibility changes under the Affordable Care Act are available in the
Actuarial Analysis section of this report.

15
V. ACTUARIAL ANALYSIS
A. FY 2013 MEDICAID OUTLAYS AND ENROLLMENT
The Federal government and the States collectively spent $457.8 billion for
Medicaid in 2013. Of this amount, the Federal government paid $265.4 billion,
representing about 58 percent of net program outlays, and the States paid
$192.5 billion, or about 42 percent of net outlays. Medicaid outlays increased by
6.1 percent between 2012 and 2013. Table 1 summarizes total Medicaid outlays for
2013.
Table 1—Medicaid Outlays for Fiscal Year 2013 by Type of Payment
(in billions)
Title XIX Outlays
1
Federal Share
State Share
Total
Medical Assistance Payments:
Acute Care Fee-For-Service Benefits
2
$81.1
$57.9
$138.9
Long-Term Care Fee-For-Service Benefits
2
65.4
49.8
115.2
Capitation Payments and Premiums
2
84.7
62.4
147.1
Disproportionate Share Hospital (DSH)
Payments
2
7.4
5.7
13.2
Adjustments
3
9.5
8.0
17.5
Subtotal, Medical Assistance Payments
248.1
183.8
431.9
Administration Payments
14.2
8.7
22.9
Vaccines for Children Program
3.6
—
3.6
Gross Outlays
265.9
192.5
458.4
Collections
4
−0.5
—
−0.6
Net Outlays
265.4
192.5
457.8
Totals may not add due to rounding.
1
Federal outlays are the funds drawn from the U.S. Treasury by the States. The State and total outlays reflect
spending as reported by the States for the purposes of drawing Federal funding from the U.S. Treasury.
Expenditures represent the spending as it was paid by the State to health care plans or providers. While
expenditures and outlays are generally similar, they are not equal mainly due to the timing differences between the
States paying for services and the States receiving Federal funds. Neither outlays nor expenditures include Title XIX
costs in support of the Children's Health Insurance Program.
2
Benefit expenditures as reported on the CMS-64 (base expenditures).
3
Adjustments include net adjustments of benefits from prior periods and the difference between expenditures and
outlays.
4
Collections from Medicare Part B for the Qualifying Individuals (QI) program and from other miscellaneous sources.
The great majority of Medicaid spending—94 percent of total outlays in 2013—was
for medical assistance payments. In table 1, these payments are divided into four
major categories: acute care, long-term care, capitation payments, and
disproportionate share hospital (DSH) payments.
Acute care includes fee-for-service (FFS) spending for inpatient and outpatient
hospital care, physician and other medical professional services, prescription drugs,
dental care, laboratory and imaging tests, mental hospital services, and case

16
management costs, as well as coinsurance payments for beneficiaries in managed
care plans. Long-term care includes FFS spending on nursing home services, home
health care, intermediate care facility services, and home and community-based
services. Capitation payments and premiums include amounts paid to Medicaid
managed care plans, pre-paid health plans, other health plan premiums, and
premiums for Medicare Part A and Part B. DSH payments are provided to certain
hospitals that have furnished care for a significant number of uninsured persons
and Medicaid beneficiaries and that have acquired, as a result, a substantial
amount of uncompensated care costs.
Of these four categories, capitation payments and other premiums represented the
largest portion of Medicaid spending in 2013, accounting for $147.1 billion or
34 percent of Medicaid benefit expenditures. Fee-for-service acute care expenditures
were nearly as large, constituting $138.9 billion or 32 percent of benefit
expenditures. In 2013, for the first time in the history of the Medicaid program,
spending on capitation payments and other premiums was greater than that for fee-
for-service acute care. Medicaid spending for fee-for-service long-term care
amounted to $115.2 billion, representing 27 percent of expenditures on benefits.
DSH payments accounted for $13.2 billion, or 3 percent, of Medicaid benefits in
2013.
Medicaid outlays for program administration totaled $23.2 billion in 2013—
$14.5 billion in Federal funds and $8.8 billion in State funds—and represented
5 percent of Medicaid outlays. Included in administration outlays were $3.9 billion
in health information technology incentive payments to providers.
26
Medicaid also
provided $3.6 billion in 2013 for the Vaccines for Children program.
27
Enrollment is measured in two ways: (i) “person-year equivalents” (PYE), or the
average enrollment over the course of a year, and (ii) “ever-enrolled” persons, or the
number of people covered by Medicaid for any period of time during the year. In
2013, Medicaid enrollment was estimated to be 58.9 million PYE (including
enrollment in the U.S. Territories). An estimated 72.5 million people, or slightly
more than one in five in the U.S. or U.S. Territories, were ever-enrolled.
Table 2 shows estimated enrollment by eligibility group for 2013 (excluding
Territory programs). Historically, children have been the largest group of Medicaid
enrollees. In 2013, this group is estimated to have represented 27.9 million PYE, or
26
Health information technology incentive payments were provided for by the American Recovery
and Reinvestment Act of 2009 and are paid entirely by the Federal government. This figure does not
include payments to States to administer the health information technology incentive payment
program.
27
The Vaccines for Children program is administered by the Centers for Disease Control and
Prevention and provides vaccines for children enrolled in Medicaid, as well as for other children who
might otherwise not be able to afford vaccines. All Vaccine for Children program costs are paid by
the Federal government.

17
47 percent of overall Medicaid enrollment. Adults made up an estimated
14.7 million PYE (25 percent), while disabled enrollees and aged enrollees are
estimated to have accounted for 10.1 million and 5.3 million PYE (17 percent and
9 percent, respectively). Another 1 million enrollees were estimated for the five U.S.
Territories (Puerto Rico, the U.S. Virgin Islands, Guam, American Samoa, and the
Northern Mariana Islands).
Table 2—2013 Estimated Enrollment, Expenditures,
and Estimated Per Enrollee Expenditures, by Enrollment Group
1
Eligibility Group
Enrollment
2
(in millions)
Expenditures
(in billions)
Per enrollee
spending
Children
27.9
$78.2
$2,807
Adults
14.7
64.5
4,391
Disabled
10.1
175.2
17,352
Aged
5.3
81.5
15,483
Total
57.9
399.3
6,897
Totals may not add due to rounding.
1
Does not include DSH expenditures, Territorial enrollees or payments, or adjustments.
2
Measured in person-year equivalents.
The average per enrollee cost for 2013 is estimated to have been $6,897 (based on
PYE enrollment and excluding DSH outlays, Territorial enrollees and costs,
adjustments, and administration costs). Children in Medicaid received an estimated
$2,807 in benefits on average in 2013, and adults received an estimated average of
$4,391 in benefits. In both instances, these average costs reflect the relatively
favorable health status of the enrollment groups; however, among adult enrollees, a
significant number are pregnant women, whose costs are on average relatively
greater. As would be expected, expenditures are substantially greater for the aged
and enrollees with disabilities; aged beneficiaries received an estimated $15,483 in
benefits on average, and disabled beneficiaries are estimated to have received an
average of $17,352 in benefits.
28
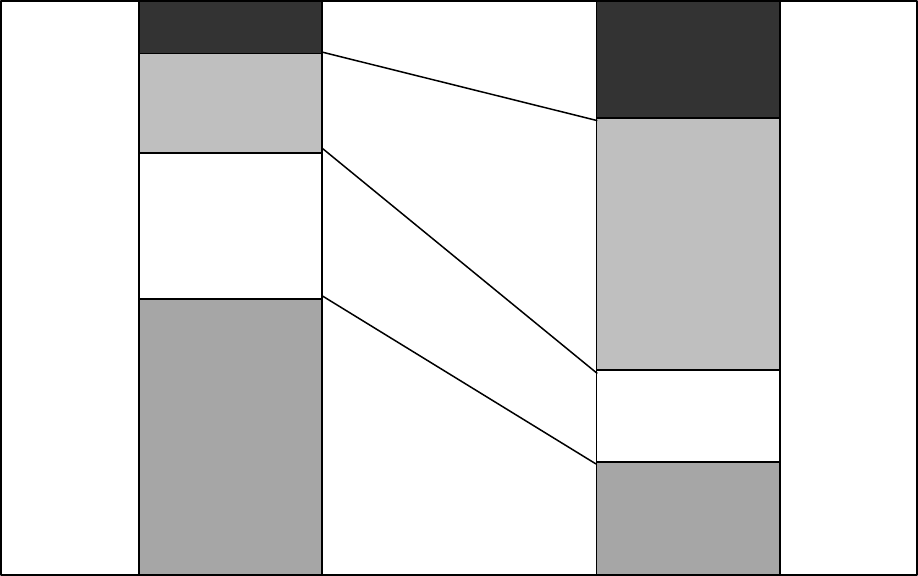
Figure 1 shows each enrollment group’s relative share of enrollment and
expenditures in Medicaid in 2013. While disabled enrollees and aged enrollees are
the smallest enrollment groups in Medicaid, they account for the majority of
spending. Conversely, children and adults are the largest enrollment groups in
Medicaid, but they receive a relatively smaller share of expenditures.
28
The average per enrollee costs may also vary substantially among States. These variations may
reflect differences in State Medicaid programs (for example, eligibility levels, benefits offered,
provider reimbursement rates, or program design) and differences in the overall health care market
across States.
18
Figure 1—Estimated Medicaid Enrollment and Expenditures by Enrollment Group,
as Share of Total, Fiscal Year 2013
Children
48%
Children
20%
Adults
25%
Adults
16%
Disabled
17%
Disabled
44%
Aged
9%
Aged
20%
Enrollment Expenditures
Note: Totals and components exclude DSH expenditures, Territorial enrollees and expenditures, and adjustments. Totals
may not add to 100 percent due to rounding.
Combined, spending on aged and disabled beneficiaries constituted 64 percent of
Medicaid benefit expenditures in 2013, but these groups accounted for only
27 percent of all enrollees. Children and adults represented 73 percent of all
enrollees in 2013, while only 36 percent of benefit expenditures were for enrollees in
these two groups.
These differences between the relative shares of enrollment and expenditures result
from per enrollee costs that vary dramatically among the enrollment groups. The
differences in average costs, while substantial, actually understate the impact of
differences in health status for these groups. In particular, Medicaid pays almost all
health care costs for enrolled children and adults. However, many aged or disabled
beneficiaries are also enrolled in Medicare, which is the primary payer of benefits

19
before Medicaid; thus, these per enrollee Medicaid estimates are less than the total
cost of such beneficiaries’ annual health care across all payers.
29
Expenditures for Medicaid increased 5.8 percent in 2013, while enrollment is
estimated to have grown 1.6 percent, resulting in an increase in the per enrollee
cost of 4.2 percent.
30
This was the highest rate of per enrollee growth and the lowest
rate of enrollment growth since 2007. Growth in Medicaid expenditures was driven
in part by an increase in the net of prior period adjustments and collections from
$10.4 billion in 2012 to $18.8 billion in 2013, a difference that accounted for about
one-third of the overall increase in Medicaid expenditures.
31
In addition, the effects
of the Affordable Care Act are estimated to have accounted for about $3 billion of
the growth (or 12 percent), reflecting the start of the temporary increases in
payments to primary care physicians and a decrease in prescription drug rebates
collected. (In 2012, a large amount of rebates were collected that were attributed to
2010 and 2011—an occurrence that otherwise reduced expenditures in 2012.) The
vast majority of the growth in Medicaid benefit expenditures was in capitated
payments and premiums, which accounted for 93 percent of the increase in benefit
expenditures (after excluding collections and prior period adjustments).
29
In 2010, Medicaid expenditures for persons eligible for Medicare and full Medicaid benefits (full-
benefit dual-eligible beneficiaries) amounted to $112.6 billion, and Medicare expenditures for these
persons were $134.7 billion, for a total of $247.3 billion in expenditures between both programs.
Medicaid accounted for about 46 percent of the total spending on dual-eligible beneficiaries. In
addition, for persons eligible for Medicare and limited Medicaid benefits (generally payments for
Medicare premiums or cost sharing), Medicaid benefits are typically an even smaller proportion of
their total benefits ($2.0 billion of $37.2 billion, or about 5 percent, in 2010). (These amounts
generally do not include lump-sum supplemental payments to providers that, in some states, account
for a significant amount of Medicaid expenditures. See Data Book: Beneficiaries Dually Eligible for
Medicare and Medicaid, Medicare Payment Advisory Commission and Medicaid and CHIP Payment
and Access Commission, 2015.
30
There are some differences between Medicaid outlays and Medicaid expenditures, mainly due to
timing differences between States paying for services and States receiving Federal funds. Thus, the
levels and trends in outlays and expenditures differ slightly.
31
California has historically reported some of the highest net prior period adjustments and
collections of any State, both in the amount reported and in the share of its total program (31 percent
of California’s expenditures in 2013). Of the $8.4 billion increase in the net of prior period
adjustments and collections nationally between 2012 and 2013, $7.1 billion of the increase was from
California.
20
B. HISTORICAL MEDICAID TRENDS
Since the start of the program, the year-to-year growth rates of total Medicaid
expenditures (Federal and State expenditures combined) and enrollment have
varied substantially, as can be seen in figure 2 and figure 3. The growth in
expenditures over time reflects growth in the number of enrollees in the program
and growth in the cost per enrollee. Enrollment growth is a result of a change in the
number of people eligible and electing to participate in the program, but it is also
strongly influenced by legislative changes to the eligibility criteria. Similarly, per
enrollee costs vary over time due to changes in the use of medical services and the
prices paid to providers of health care services and supplies, as well as legislative
and other policy changes to the benefits offered by State Medicaid programs.
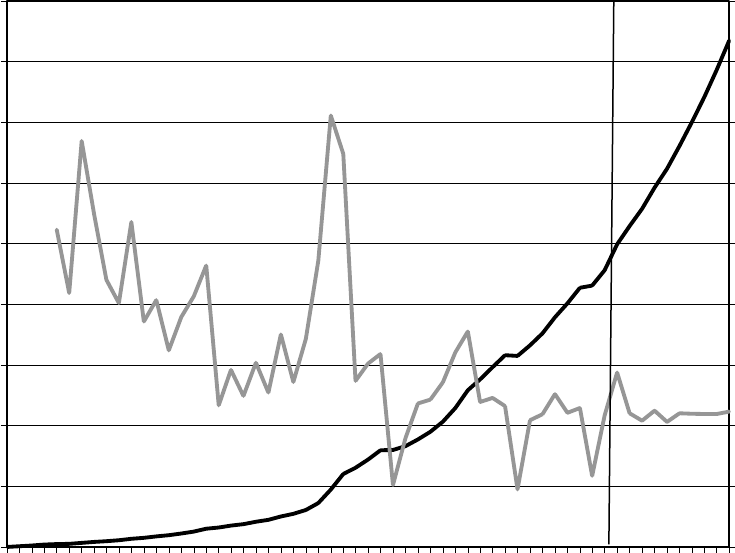
Figure 2—Historical and Projected Medicaid Expenditures and Annual Growth Rates,
FY 1966–FY 2023
-5%
0%
5%
10%
15%
20%
25%
30%
35%
40%
$0
$100
$200
$300
$400
$500
$600
$700
$800
$900
1965 1970 1975 1980 1985 1990 1995 2000 2005 2010 2015 2020
Annual Growth Rate
Expenditures (in billions)
Fiscal Year
Actual
Projected
Annual Growth
Rate (right axis)
Expenditures
(left axis)
21
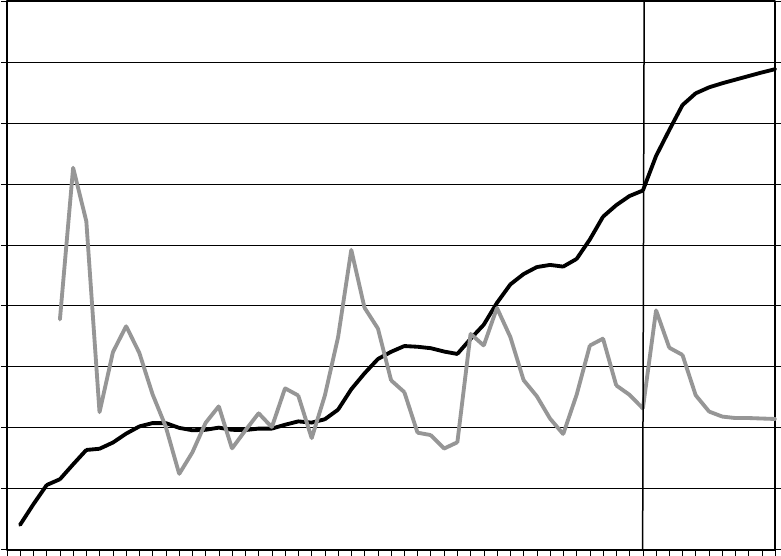
Figure 3—Historical and Projected Medicaid Enrollment and Annual Growth Rates,
FY 1966–FY 2023
-10%
-5%
0%
5%
10%
15%
20%
25%
30%
35%
0
10
20
30
40
50
60
70
80
90
1965 1970 1975 1980 1985 1990 1995 2000 2005 2010 2015 2020
Annual Growth Rate
Enrollment (in millions of person-year equivalents)
Fiscal Year
Actual
Projected
Annual Growth
Rate (right axis)
Enrollment
(left axis)
From 2004 to 2013, Medicaid expenditures grew at an average annual rate of
5.1 percent, but annual growth rates varied substantially over the last 10 years
(from −0.3 percent in 2006 to 7.6 percent in 2009). Growth in health care
expenditures is driven primarily by several key factors: growth in the population,
changes in the use of health care services, and changes in the prices of health care
services. In addition to these, there are several other factors that affected Medicaid
expenditure trends in recent history.
Federal legislation had a significant effect on historical expenditure trends. The
Medicare Modernization Act of 2003 created the Medicare Part D program, and in
2006 most prescription drug coverage for dual-eligible beneficiaries (those eligible
for both Medicaid and Medicare) shifted from Medicaid to Medicare Part D. All
dual-eligible beneficiaries were automatically enrolled in Part D, and Medicare
served as the primary source of their prescription drug coverage. As a result of this
shift in coverage, Medicaid drug spending (net of rebates) decreased 44 percent from
2005 to 2006, and aggregate Medicaid spending was 0.3 percent lower than in 2005,
decreasing for the first time in the program’s history.
The American Recovery and Reinvestment Act of 2009 provided for temporary
increases in the Federal share of Medicaid payments in 2009, 2010, and 2011, as

22
well as for health information technology incentive payments that were funded
entirely by the Federal government. While the increase in the Federal share of
Medicaid payments was significant, it is not estimated to have affected total
Medicaid expenditure growth in those years.
The Affordable Care Act also had a number of provisions that affected Medicaid
starting in 2010; however, most of the changes to the Medicaid program through
2013 are estimated to have had only minor effects on Medicaid expenditure growth
rates.
Medicaid expenditure growth is also affected by States’ decisions in operating their
programs. In the past, States took steps to control the costs of their Medicaid
programs, especially during periods of relatively faster growth, and many States
have taken such steps to slow the rate of expenditure growth in recent history.
32
Common methods have included provider reimbursement rate freezes or reductions
and limiting or curtailing optional health care benefits.
Medicaid enrollment grew at an average annual rate of 3.1 percent from 2004 to
2013. Annual growth rates varied substantially, from a low of −0.5 percent in 2007
to a high of 7.3 percent in 2010. Changes in Medicaid enrollment were generally
driven by population growth and by changes in economic growth and unemployment
rates. In general, Medicaid enrollment increases more quickly during economic
recessions, and growth slows as the economy expands. Faster Medicaid enrollment
growth in turn typically leads to increases in expenditure growth. Medicaid
enrollment and expenditure trends followed these historical patterns during the
2001 recession and the 2007-2009 recession and during the subsequent economic
recoveries.
32
These changes are described in detail in surveys of State Medicaid programs by the Kaiser Family
Foundation; see V. Smith, et al., “Medicaid in an Era of Health & Delivery System Reform: Results
from a 50-State Medicaid Budget Survey for State Fiscal Years 2014 and 2015,” Kaiser Family
Foundation, October 2014.

23
C. MEDICAID EXPENDITURES AND ENROLLMENT PROJECTIONS,
FY 2014–FY 2023
The projections presented in this report focus on Medicaid medical assistance
payments (or “benefit” expenditures) and Medicaid enrollment; administration costs
are also included and are based on the projections from the President’s Fiscal Year
2016 Budget.
33
Other Title XIX expenditures (such as the Vaccines for Children
program) are not included. Historical and projected Medicaid enrollment and
expenditures for medical assistance payments and administration are shown in
table 3.
34,35
33
The projections of administration expenditures are based on the projected trends for Medicaid
administration outlays in the President’s Budget, but are adjusted to be consistent with the
expenditures reported in the CMS-64; in addition, total expenditures are also projected for
administration, whereas the President’s Budget only projects Federal outlays.
34
In table 3, enrollment and expenditure data for the period 1966–1976 have been revised to be
consistent with the current definition of the Federal fiscal year (October-September).
35
There are some differences between Medicaid outlays and Medicaid expenditures, mainly due to
timing differences between States paying for services and States receiving Federal funds. Thus, the
levels and trends in outlays and expenditures differ slightly, and the amounts shown in table 3 differ
from those shown in table 1.

24
Table 3—Historical and Projected Medicaid Enrollment and Expenditures
and Average Federal Share of Expenditures, Selected Years
(Enrollment in millions of person-year equivalents, expenditures in billions of dollars)
Fiscal
Year
Total Expenditures
Benefit Expenditures
Administration
Expenditures
Avg.
Federal
Share
Enrollment
Total
Federal
State
Total
Federal
State
Total
Federal
State
Historical:
1966
4.0
$0.9
$0.5
$0.4
$0.9
$0.4
$0.4
$0.0
$0.0
$0.0
50%
1970
14.0
5.1
2.8
2.3
4.9
2.6
2.2
0.2
0.1
0.1
54%
1975
20.2
13.1
7.3
5.9
12.6
6.9
5.6
0.6
0.3
0.3
55%
1980
19.6
25.2
14.0
11.2
24.0
13.3
10.7
1.2
0.7
0.5
55%
1985
19.8
41.3
22.8
18.4
39.3
21.7
17.6
2.0
1.2
0.8
57%
1990
22.9
72.2
40.9
31.3
68.7
38.9
29.8
3.5
2.0
1.5
57%
1995
33.4
159.5
90.7
68.8
151.8
86.5
65.3
7.7
4.2
3.4
57%
2000
34.5
206.2
117.0
89.2
195.7
111.1
84.6
10.6
5.9
4.7
57%
2005
46.3
315.9
180.4
135.5
300.7
172.1
128.7
15.1
8.3
6.8
57%
2006
46.7
315.1
179.3
135.8
299.0
170.6
128.5
16.0
8.7
7.3
57%
2007
46.4
332.2
189.0
143.2
315.8
180.0
135.8
16.4
9.0
7.5
57%
2008
47.7
351.9
200.2
151.7
334.2
190.6
143.6
17.7
9.6
8.1
57%
2009
50.9
378.6
246.3
132.3
360.3
236.3
124.0
18.3
10.0
8.3
65%
2010
54.6
401.5
269.8
131.7
383.6
260.0
123.6
17.9
9.8
8.1
67%
2011
56.5
427.4
270.7
156.7
407.9
259.8
148.1
19.5
10.9
8.6
63%
2012
58.0
431.0
248.8
182.2
408.8
235.1
173.7
22.2
13.7
8.4
58%
2013
58.9
456.1
263.1
193.0
433.2
248.9
184.3
22.9
14.2
8.7
58%
Projections:
2014
64.6
498.9
299.7
199.2
474.5
284.5
190.0
24.4
15.2
9.2
60%
2015
68.9
529.0
320.0
209.0
503.1
303.7
199.4
25.9
16.3
9.6
60%
2016
72.9
557.6
336.4
221.2
532.4
320.8
211.5
25.2
15.5
9.7
60%
2017
74.8
592.3
356.8
235.5
567.2
341.8
225.4
25.1
15.1
10.0
60%
2018
75.8
623.6
375.3
248.3
597.9
360.1
237.8
25.8
15.2
10.5
60%
2019
76.5
661.1
397.5
263.6
634.4
381.8
252.5
26.7
15.7
11.1
60%
2020
77.1
700.6
418.4
282.2
672.7
402.1
270.6
27.9
16.3
11.6
60%
2021
77.7
742.3
442.7
299.6
713.1
425.7
287.5
29.2
17.0
12.2
60%
2022
78.2
786.6
468.8
317.7
756.0
451.1
304.9
30.6
17.8
12.8
60%
2023
78.8
835.0
497.4
337.5
802.9
478.8
324.1
32.1
18.6
13.4
60%
Note: Enrollment is projected for 2011, 2012, and 2013.

25
Expenditures
Total Medicaid expenditures (Federal and State combined) for medical assistance
payments and administration are estimated to have grown 9.4 percent in 2014 to
$498.9 billion and are projected to reach $835.0 billion by 2023, increasing at an
average rate of 6.2 percent per year over the next 10 years. Federal government
spending on Medicaid medical assistance payments and administration costs is
estimated to have increased by 13.9 percent to $299.7 billion in 2014, representing
about 60 percent of total Medicaid benefit expenditures. Federal spending on
Medicaid is projected to reach $497.4 billion by 2023, or about 60 percent of total
spending. Total State Medicaid expenditures for benefits and administration are
estimated to have increased to $199.2 billion in 2014, a growth rate of 3.2 percent,
and are projected to reach $337.5 billion by 2023.
The Affordable Care Act contains many Medicaid provisions, most of which were
implemented by 2014 and are expected to have a significant influence on future
Medicaid expenditure trends. Included in these provisions is a substantial increase
in Medicaid eligibility that began in 2014. The impacts of this increase are
presented in more detail in the next section.
In recent history, the average annual Federal share of Medicaid expenditures has
been about 57 percent of total expenditures, with several years of greater Federal
shares due to changes specified in legislation. The average Federal share was
57.7 percent in 2013. It is estimated to have risen in 2014 due mainly to the higher
FMAP for newly eligible Medicaid beneficiaries as required in the Affordable Care
Act. The average Federal share is estimated to have increased to about 60 percent
in 2014 and is projected to remain at that level through 2023.
Total Medicaid expenditures (Federal and State combined) for medical assistance
payments (excluding administration) are estimated to have grown 9.5 percent in
2014 to $474.5 billion. This would be a significant acceleration in expenditure
growth, increasing from 6.0 percent in 2013 and from only 0.2 percent in 2012.
Medicaid expenditures on such payments are projected to reach $802.9 billion by
2023, growing at an average rate of 6.4 percent per year over the next 10 years.
Federal government spending on these Medicaid payments is estimated to have
amounted to $284.5 billion in 2014 and is projected to grow to $478.8 billion by
2023.
Growth in Medicaid benefit expenditures in 2014 is largely attributable to the start
of the Medicaid eligibility expansion that occurred on January 1, 2014 under the
Affordable Care Act. The majority of the projected acceleration was driven by new
expenditures for newly eligible enrollees, but the projected increase in the growth
rate also reflects additional enrollment among non-newly eligible persons.
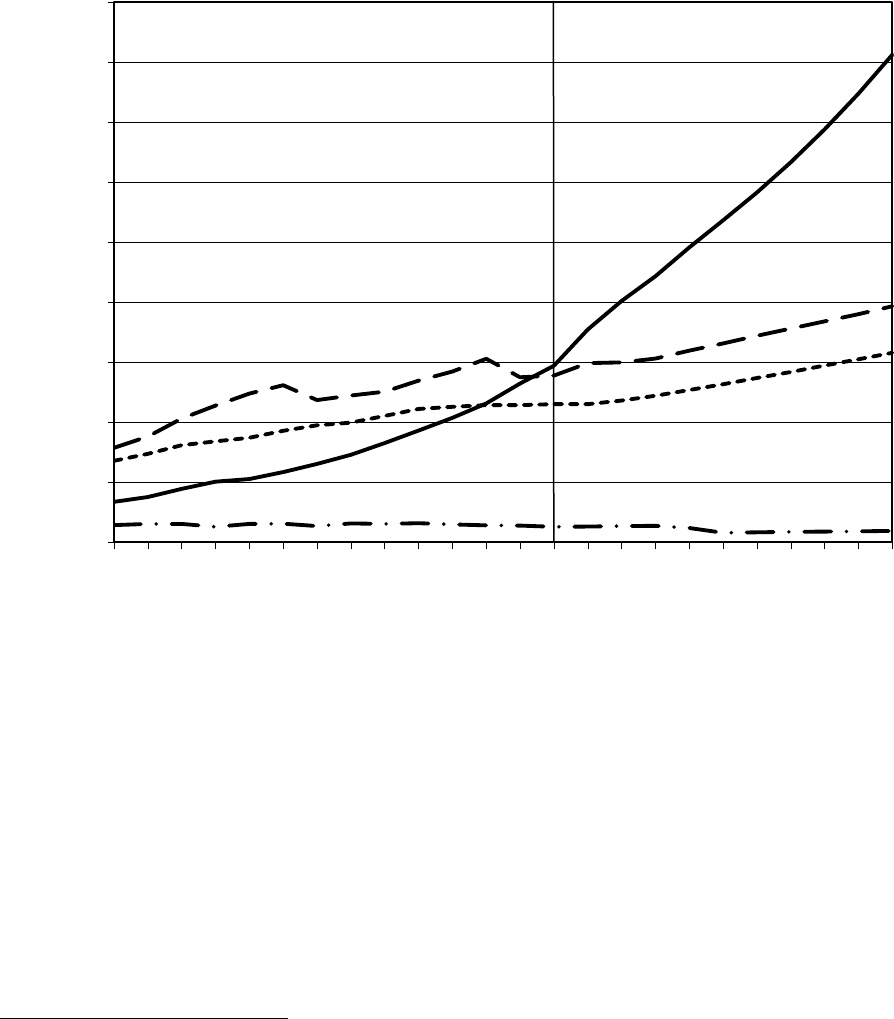
26
Figure 4 shows historical and projected Medicaid benefit expenditures by four major
categories of services: acute care fee-for-service, long-term care, capitation
payments and premiums, and DSH.
Figure 4—Past and Projected Medicaid Expenditures for Medical Assistance Payments,
by Type of Payment, FY 2000–FY 2023
36
(in billions)
$0
$50
$100
$150
$200
$250
$300
$350
$400
$450
2000 2002 2004 2006 2008 2010 2012 2014 2016 2018 2020 2022
Expenditures
Fiscal Year
Actual
Projected
DSH
Capitation Payments
and Premiums
Long-Term Care (FFS)
Acute Care (FFS)
Over the next 10 years, expenditures for capitation payments and premiums are
expected to grow the fastest of the major Medicaid service categories, as shown in
figure 4. These expenditures are projected to grow 10.7 percent per year on average
from 2014 to 2023, which would be 4.3 percentage points faster than overall
Medicaid benefit growth. Relatively faster projected growth in these payments is in
part the result of the Medicaid eligibility expansion under the Affordable Care Act,
since most of the new enrollees are expected to be enrolled in managed care plans.
Moreover, expenditures for capitation payments and premiums have grown
substantially more quickly than other service expenditures in recent history.
37
From
2001 to 2013, Medicaid payments for managed care plans and other premiums grew
on average 11.9 percent per year, faster than overall Medicaid benefit expenditures
(6.0 percent).
36
The data for this graph can be found in table 14 of Appendix E.
37
Centers for Medicare & Medicaid Services, 2011 Medicaid Managed Care Enrollment Report.

27
Acute care fee-for-service Medicaid expenditures are projected to grow at an average
rate of 3.5 percent per year over the next decade. In 2014, these expenditures are
estimated to have grown by 7.4 percent—a sharp increase that was partly due to
the increase in adult enrollees related to the eligibility expansion, as some of their
costs were covered through fee-for-service programs (although the majority of the
expenditures are expected to be paid under managed care). In addition, the 2014
growth rate reflects the temporarily increased primary care physician payment
rates provided by the Affordable Care Act.
38
Medicaid spending on fee-for-service long-term care is projected to grow by
3.2 percent on average for 2014 through 2023. Aged and disabled enrollees receive
the vast majority of long-term care services, and growth in these expenditures is
driven in part by growth in enrollment among these beneficiaries. Newly eligible
adults, along with other adults and children, are expected to need very few long-
term care services. In recent history, Medicaid expenditures on these services have
increased very slowly; from 2009 to 2013, long-term care expenditures grew at an
average rate of only 1.8 percent per year. This limited growth reflects relatively
slower growth in reimbursement rates and utilization of long-term care services.
Additionally, there has been increased use of managed care for long-term care in
Medicaid over the last several years, which has slowed fee-for-service expenditure
growth in the program. As a result, the projected growth rate of long-term care
expenditures through fee-for-service programs is notably slower than in last year’s
report.
39
Medicaid DSH expenditures are typically expected to grow at the same rate as the
Medicaid Federal DSH allotments, which are based on the Consumer Price Index
(CPI). The Affordable Care Act, however, prescribes reductions in Medicaid DSH
allotments, and subsequent legislation has extended those reductions through
38
Based on a review of the most recently available data, it appears that most of the payments related
to the primary care physician payment rate increases that were incurred in 2013 were paid and
reported in 2014.
39
Use of home and community-based services can substantially reduce expenditures for enrollees
who would otherwise have had to enter a nursing home or who transition from institutional to
community settings. Conversely, the expanding use of these services, by those who would not
otherwise have had nursing home care, adds to overall program costs. Growth in the use of home and
community long-term care reflects the increase in the number of home and community-based
waivers in Medicaid. In addition, in Olmstead v. L.C., 119 S. Ct. 2176 (1999), the Supreme Court
ruled that under the Americans with Disabilities Act of 1990, States must provide community-based
placement for persons with mental disabilities when appropriate and consistent with consumer
wishes. This ruling is also expected to have led to an increase in non-institutional long-term care
expenditures in Medicaid.

28
2025.
40
Thus, the average growth rate for DSH spending is projected to be
−1.9 percent over the next 10 years.
Administration costs are estimated to have amounted to $24.4 billion in 2014,
reflecting an increase of 6.5 percent. This growth follows a smaller increase in 2013
of 3.5 percent. The projected growth is expected to have been driven by additional
administration costs associated with the increase in enrollment and expenditures in
2014, while health information technology incentive payments are expected to have
decreased slightly. Administration costs are projected to reach $32.1 billion by 2023,
growing at an average annual rate of 3.4 percent. These projected costs include
additional administration expenditures related to the Medicaid eligibility expansion
under the Affordable Care Act.
Enrollment
Increasing levels of Medicaid enrollment are expected to contribute to expenditure
growth over the next 10 years. Historical and projected Medicaid enrollments are
shown by category in figure 5.
40
Reductions to DSH allotments were prescribed for 2017 through 2024 under prior law. The
Medicare Access and CHIP Reauthorization Act of 2015 (Public Law 114-10) delayed the first year of
the reductions until 2018, made changes to the annual reduction amounts, and extended the
reductions through 2025. The effects of this legislation are not included in the projections shown in
this report.
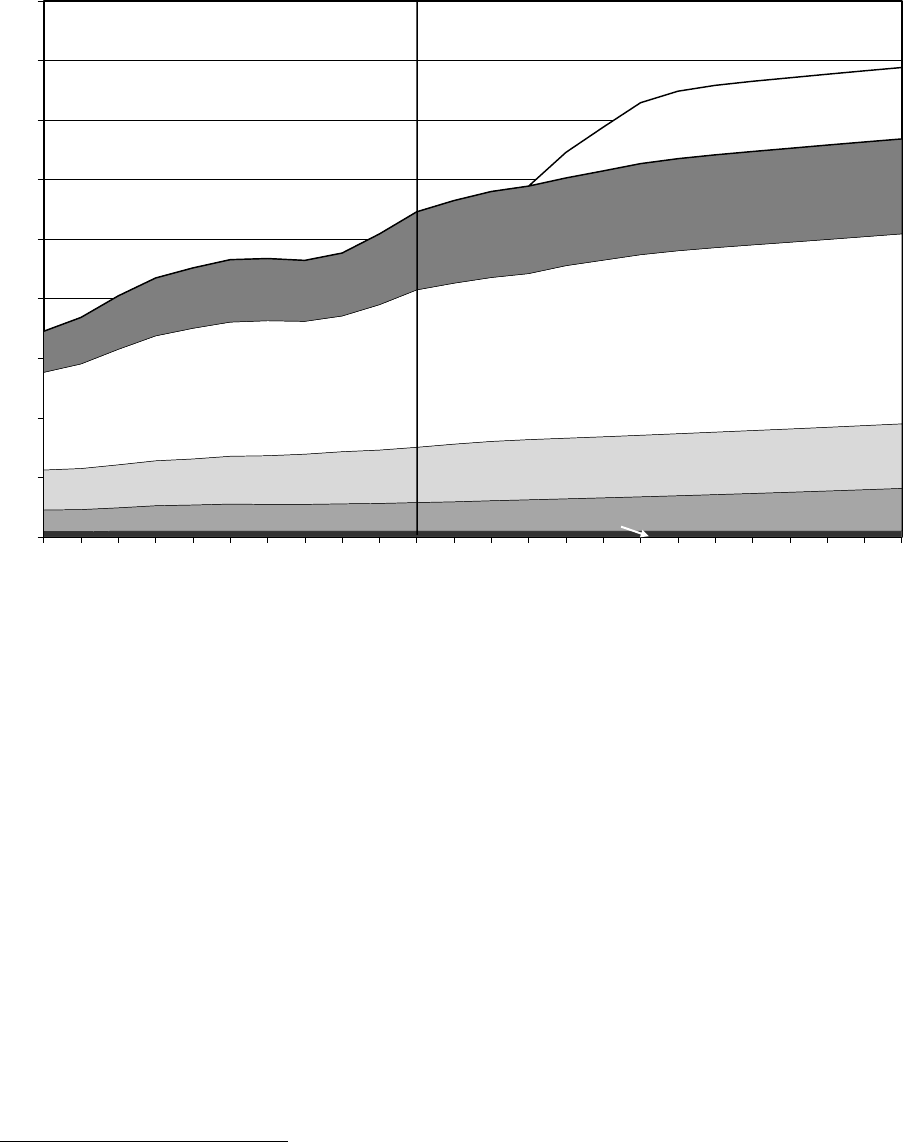
29
Figure 5—Past and Projected Numbers of Medicaid Enrollees, by Category,
FY 2000–FY 2023
41
(in millions of person-year equivalents)
Territories
Aged
Disabled
Children
Adults
0
10
20
30
40
50
60
70
80
90
2000 2002 2004 2006 2008 2010 2012 2014 2016 2018 2020 2022
Fiscal Year
Actual
Projected
Newly Eligible Adults
Total enrollment is estimated to have increased from 58.9 million PYE in 2013
(including 1.0 million enrollees in the U.S. Territories) to 64.6 million PYE in 2014,
and it is projected to increase to 78.8 million PYE by 2023.
Enrollment in 2014 is estimated to have increased by 9.6 percent, primarily due to
the start of the Medicaid eligibility expansion. Excluding the newly eligible adults,
enrollment in 2014 is estimated to have increased by 2.3 percent (faster than the
rate of 1.6 percent estimated in 2013) and is driven in part by expected increases in
participation in Medicaid due to outreach efforts and enrollment simplifications.
The majority of the increase in Medicaid enrollees attributable to the eligibility
expansion is assumed to occur during the period 2014–2016, with most of the
increase taking place in 2014. Enrollment growth in 2015 and 2016 is estimated to
average 6.3 percent per year, reflecting increased enrollee participation and
assumed increases in the number of States expanding Medicaid eligibility after
2014.
41
The data for this graph can be found in table 15 of Appendix E.
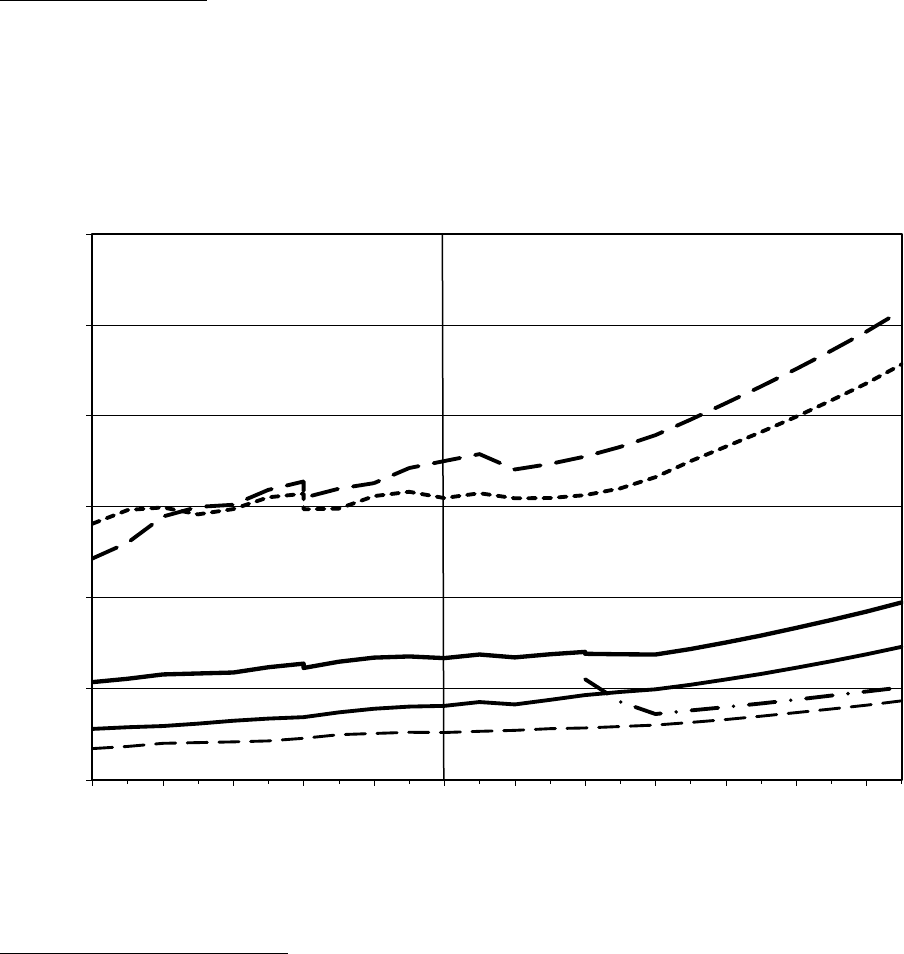
30
The total number of Medicaid enrollees is projected to increase during 2017 through
2023 at about 1.1 percent per year, reflecting population growth, stable economic
assumptions, and an increase in the number of aged enrollees as baby boomers
continue to reach age 65. Excluding the newly eligible enrollment groups, growth in
the number of aged adults is expected to be faster than for the other categories of
enrollment; the average annual increase for aged adults is estimated to be
3.2 percent over the next 10 years, as compared to 1.1 percent for other non-newly
eligible enrollment groups.
Per Enrollee Costs
In addition to increases in Medicaid enrollment, the average costs of benefits for all
enrollees are projected to increase over the next 10 years. Figure 6 displays
historical and projected average Medicaid benefit expenditures per enrollee for all
enrollees collectively and by eligibility group.
Figure 6—Past and Projected Medicaid Expenditures on Medical Assistance Payments
Per Enrollee, by Enrollment Category, FY 2000–FY 2023
42
$0
$5,000
$10,000
$15,000
$20,000
$25,000
$30,000
2000 2002 2004 2006 2008 2010 2012 2014 2016 2018 2020 2022
Fiscal Year
Actual
Projected
Disabled
Aged
Children
Adults
Average of All Enrollees
Newly eligible adults
Note: Per enrollee amounts for 2011, 2012, and 2013 are based on actual expenditures and estimated enrollment.
42
The data for this graph can be found in table 16 of Appendix E.

31
Per enrollee benefits costs are projected to grow somewhat faster over 2014 to 2023
than they did in the previous 10-year period. Aged Medicaid enrollee benefit costs
(which grew at an average annual rate of 0.6 percent from 2004 to 2013 and are
projected to grow at an average annual rate of 4.0 percent from 2014 to 2023) and
disabled Medicaid enrollee benefit costs (with average annual growth of 1.5 percent
over 2004 to 2013 and 4.0 percent over 2014 to 2023) are projected to exhibit the
largest differences between the prior 10-year period and the next 10 years.
These differences are in part due to historical events that led to slower increases in
expenditure growth. The largest change was the start of the Medicare prescription
drug benefit in 2006, which shifted prescription drug coverage from Medicaid to
Medicare for persons enrolled in both programs (dual-eligible beneficiaries). This
change significantly reduced per enrollee costs in 2006 for aged and disabled
enrollees, as many were dually eligible. In addition, the slow rate of growth of long-
term care expenditures in recent history contributed to limited growth in the benefit
costs for aged and disabled enrollees, as these individuals receive the vast majority
of long-term care services. Expenditures for institutional long-term care (primarily
nursing facility services) grew very slowly, while costs for community long-term
care (including home and community-based waiver services) grew relatively quickly,
although the growth rate has decelerated more recently. Slow cost growth for long-
term care through fee-for-service programs was partially offset by increasing
managed care expenditures, especially for managed long-term care services. During
and immediately after the 2007-2009 recession, States took stronger actions to limit
Medicaid expenditure growth, including freezing or reducing provider
reimbursement rates.
43
Aged and disabled enrollees are projected to experience the lowest average benefit
cost growth over the next 10 years compared to other enrollee groups due in large
part to projected relatively slower growth in the cost of long-term care services.
States are expected to continue to use more home and community-based long-term
care to postpone enrollees’ need for long-term care facilities as long as possible. In
addition, States are projected to shift long-term care expenditures from fee-for-
service programs into managed care. As a result, managed care expenditures are
expected to grow more quickly and to constitute a larger share of benefits for aged
and disabled enrollees.
While average benefit cost growth is expected to be slower for aged and disabled
enrollees over the next 10 years compared to other populations in Medicaid, it is
nevertheless expected to be faster than in recent history. In addition to the
deceleration of historical growth by legislative changes that affected Medicaid,
States have instituted fewer provider reimbursement rate freezes and reductions
43
V. Smith, et al., “Medicaid in an Era of Health & Delivery System Reform: Results from a 50-State
Medicaid Budget Survey for State Fiscal Years 2014 and 2015,” Kaiser Family Foundation,
October 2014.

32
and have allowed for more rate increases, and it is expected that these increases
will continue in the future.
44
Benefit costs per enrollee for adults (excluding newly eligible adults) are projected
to grow somewhat faster over the next 10 years (from 3.6 percent on average during
the period 2004 to 2013 to 5.2 percent on average during 2014 to 2023), as are
benefit costs per enrollee for children (from 3.3 percent on average over 2004 to
2013 to 4.4 percent on average over 2014 to 2023). Similar to the experience for
aged and disabled enrollees, in the past several years States have taken steps to
control the Medicaid expenditure growth that occurred during and after the 2007-
2009 recession, especially in limiting or reducing provider reimbursement rates.
45
Spending for managed care represented over half of Medicaid expenditures for
adults and children in 2013, and, for these enrollees, this type of care is expected to
be the fastest growing service category over the next 10 years. More recently, States
have made fewer provider reimbursement rate reductions and are instituting more
rate increases, and together these factors are anticipated to contribute to somewhat
faster expenditure growth.
46
Although the estimated average benefit costs for newly eligible adults are expected
to be greater than those for other adults in 2014, such expenditures are projected to
ultimately be lower over the next several years. More detail on these projections is
provided in the next section of this report.
Enrollment Mix
The growth in average Medicaid benefit expenditures per enrollee for all enrollment
categories is significantly affected by the relative proportion of enrollment across
these categories. In this report, the “enrollment mix” is defined as the contribution
of the change in these relative proportions to the growth in Medicaid benefit
expenditures per enrollee. This concept is similar to “age-gender mix” effects in
other health care plans or programs (which measure the contribution to health care
expenditures of changes in the relative proportion of enrollees by age and by gender
in a plan). The enrollment mix differs in that it does not specifically consider gender
and considers age in only broad ranges, but does take into account the disability
status of enrollees.
The enrollment mix is an important consideration in analyzing and projecting
Medicaid benefit expenditures. While the effects of age-gender mix on other
programs are usually relatively small and do not change significantly from year to
year, the effect of enrollment mix on Medicaid expenditures can be substantially
44
Ibid.
45
Ibid.
46
Ibid.

33
larger or smaller and may vary greatly each year. This variation can occur because
Medicaid enrollment categories experience substantially different average costs—
aged and disabled enrollees’ average Medicaid costs are much greater than those of
child and adult enrollees—and because the enrollment growth for these groups may
vary among categories and may fluctuate annually.
For this report, the enrollment mix is measured as the difference between the
increase in Medicaid benefit expenditures per enrollee and the increase in Medicaid
benefit expenditures per enrollee if enrollment were held constant each year. To
calculate this difference, enrollment was set at 2010 levels for each enrollment
category.
47
From 2004 to 2013, Medicaid benefit expenditures per enrollee grew at an average
annual rate of 1.7 percent. The effects of changes in enrollment mix over this time
period reduced spending by an average of 0.2 percentage point per year; that is,
excluding the impacts of changes in enrollment, Medicaid benefit expenditures per
enrollee would have grown 1.9 percent per year. The effects of the changes in
enrollment mix on spending ranged from −2.4 percent to 1.4 percent over these
10 years. The negative effects of the changes in enrollment mix were the result of
relatively faster enrollment growth for children and adults than for aged and
disabled enrollees, especially from 2008 to 2010.
Medicaid benefit expenditures per enrollee are estimated to have increased
0.3 percent in 2014. Excluding the impact of the change in the enrollment mix,
Medicaid benefit expenditures per enrollee are estimated to have increased
3.1 percent, which would be faster than any single-year growth rate since 2009. As
described previously in this section, this relatively faster rate of growth is expected
to have been driven by States’ actions to increase provider payment rates and
program benefits, following years in which States took more actions to limit the rate
of program expenditure growth. In addition, the increase in benefit expenditures
per enrollee (excluding the impact of changes in the enrollment mix) is attributable
to sections of the Affordable Care Act other than the eligibility expansion (notably
greater expenditures for the temporary increase in primary care physician
payments).
While Medicaid benefit expenditures per enrollee are projected to grow more rapidly
over the next 10 years at an average annual rate of 3.5 percent, changes in
enrollment mix are projected to decrease per enrollee Medicaid expenditure growth
by an average of 0.5 percentage point per year over this time period; thus, excluding
the effect of changes in the enrollment mix, Medicaid benefit expenditures per
47
2010 was selected as the base year for enrollment because it was the latest year for which complete
Medicaid enrollment data were available. A review of the measurement of enrollment mix using
other years as the base year showed no significant differences in results.

34
enrollee are projected to grow at an average annual rate of 4.1 percent.
48
This
difference in the per enrollee growth rate is largely the result of the addition of
newly eligible adult enrollees and increases in the enrollment of non-newly eligible
adult and child enrollees that began in 2014 under the Affordable Care Act. As the
benefit costs for these enrollees are projected to be less than the average benefit
costs of all Medicaid enrollees (substantially less than the costs of aged and disabled
enrollees and, on average, somewhat less than the costs of current adult enrollees
after 2015), the addition of these new enrollees is expected to slow growth in
expenditures per enrollee in the next several years. The effect of the new enrollees
due to the Affordable Care Act is partially offset by relatively faster growth in the
number of aged Medicaid enrollees, as the oldest members of the baby boom
generation reach age 65.
Excluding the effects of changes in the enrollment mix, Medicaid benefit
expenditures per enrollee grew at an average annual rate of 1.9 percent per year
from 2004 through 2013. From 2014 to 2023, Medicaid benefit expenditures per
enrollee, minus the effects of estimated changes in the enrollment mix, are
projected to increase 4.1 percent per year on average. This difference is driven in
part by several recent legislative acts (the most significant of which was the
Medicare Modernization Act of 2003) that generally provided for one-time
reductions to the rate of Medicaid expenditures per enrollee. Moreover, efforts by
States to limit Medicaid expenditure growth (most notably, in 2011 and 2012) are
not projected to continue with the same intensity into the future. Finally, medical
price inflation is also projected to be modestly faster in the next 10 years than in
recent history.
Impacts of Recent Legislation
In addition to the effects of the Affordable Care Act, the impacts of the following
legislative actions are also reflected in these projections:
The American Taxpayer Relief Act (Public Law 112-240) extended the
qualifying individuals (QI) program and transitional medical assistance
(TMA) into 2014;
The Bipartisan Budget Act (Public Law 113-67) provided additional
extensions for the QI program and TMA and strengthened Medicaid’s third-
party liability enforcement;
The Protecting Access to Medicare Act of 2014 (Public Law 113-93) further
extended the QI program and TMA and adjusted future DSH allotments by
decreasing reductions to the allotments through 2019 and then increasing the
reductions in 2024; and
48
These figures do not sum due to rounding.

35
The Veterans Access, Choice, and Accountability Act (Public Law 113-146)
provided for additional Veterans Administration (VA) funding, which is
expected to reduce Medicaid expenditures in 2015 and 2016, and made
changes to VA pension rules, which are expected to increase Medicaid
enrollment and expenditures in the future.
The net impact of these laws on Medicaid expenditures from 2014 through 2023 is
projected to be an increase of $3.5 billion, with costs attributed to the extensions of
the QI program and TMA and changes to VA pensions, offset in part by savings
related to adjustments to DSH allotments. These changes to the program are
projected to have a negligible effect on Medicaid enrollment.
49
49
The effects of the Medicare Access and CHIP Reauthorization Act of 2015 (Public Law 114-10) are
not included in the projections in this report.

36
D. IMPACTS OF THE MEDICAID ELIGIBILITY EXPANSION
With respect to Medicaid, the most significant provision of the Affordable Care Act
is the expansion of Medicaid eligibility, beginning in 2014, to almost all persons
under age 65 who are living in families with incomes below 138 percent of the FPL
(and who are citizens or eligible legal residents).
50
This expansion is estimated to
have added 4.3 million PYE to enrollment during the 9 months that the new
eligibility rules were in effect for FY 2014 and is expected to add 12.0 million PYE
by 2023 (represented by adults who have met the definition of “newly eligible” in
section 1905(y)(2) of the Social Security Act).
51
Expenditures for newly eligible adults are estimated to have amounted to
$23.7 billion in 2014 and are projected to total $460 billion over 2014 through 2023.
Of these costs, the majority are expected to be paid by the Federal government—
$430 billion, or about 93 percent—and the States are anticipated to spend an
additional $30 billion. The Affordable Care Act specifies a much higher Federal
matching rate for newly eligible beneficiaries, decreasing from 100 percent in 2014,
2015, and 2016 to 90 percent by 2020 and beyond.
In 2014, the average benefit costs of newly eligible adult enrollees are expected to
have been substantially greater than those for non-newly eligible adult enrollees in
the program. Newly eligible adults are estimated to have had average benefit costs
of $5,517 in 2014, 19 percent greater than non-newly eligible adults’ average benefit
costs of $4,650. These estimates are significantly different from those in previous
50
While previous reports presented estimates of Medicaid expenditures and enrollment for all
sections of the Affordable Care Act, this report presents estimates for only the eligibility expansion
sections of the legislation. Moreover, these estimates do not include costs for persons who were
eligible under previous eligibility criteria and would not have been enrolled (and thus are not newly
eligible).
51
In addition to the higher level of allowable income, the Affordable Care Act expands eligibility to
people under age 65 who have no other qualifying factors that would have made them eligible for
Medicaid under prior law, such as being under age 18, disabled, pregnant, or parents of eligible
children. As noted previously, the category of “Adults” is expected to have the greatest increase in
enrollment in Medicaid under the Affordable Care Act, since the law does not require individuals to
be parents of eligible children. “Newly eligible” individuals are persons between the ages of 19 and
64 who, beginning in 2014, are enrolled in the new adult group and who would not have been eligible
for full Medicaid benefits, benchmark coverage (described in subparagraph (A), (B), or (C) of section
1937(b)(1) of the Social Security Act), or benchmark-equivalent coverage (described in section
1937(b)(2) of the Social Security Act) as of December 1, 2009. An individual may also be newly
eligible if he or she would have been eligible but could not have been enrolled for such benefits or
coverage because the applicable Medicaid waiver or demonstration had limited or capped enrollment
as of December 1, 2009. The estimates of Medicaid enrollment and expenditures due to the eligibility
expansion also include State programs that have received waivers to cover newly eligible enrollees in
qualified health plans on the Health Insurance Marketplaces.

37
reports, in which average benefit costs for newly eligible adults in 2014 were
estimated to be 1 percent lower than those of non-newly eligible adults.
52
There are several explanations for the difference between the estimates in this
year’s report and those in previous reports. First, most of the States that
implemented the eligibility expansion are covering newly eligible adults in Medicaid
managed care programs, and on average the capitation rates for the newly eligible
adult enrollees were significantly greater than the projected average costs
previously calculated. In particular, two assumptions varied significantly. In many
States, the capitation rates for managed care plans included significant
adjustments to reflect a higher level of acuity or morbidity among newly eligible
adults compared to non-newly eligible adults. In most States, this adjustment was
positive (in other words, that newly eligible adults had a higher level of acuity than
non-newly eligible adults), and in some cases the adjustment was substantial. In
last year’s report, the level of acuity for newly eligible adults was estimated to be
less than the acuity level of non-newly eligible adults; for persons who were
previously uninsured and are newly eligible for Medicaid, the costs were projected
ultimately to be about 30 percent less than those for non-newly eligible adults. A
significant amount of the per-enrollee cost difference estimated in last year’s report
is likely due to many pregnant women being included with non-newly eligible
adults, as the health care costs of pregnant women are typically greater than those
of other non-disabled non-aged adults in Medicaid. However, the modeling results
suggest that the acuity level of newly eligible adults would on average be lower than
that of non-newly eligible adults, even after adjusting for the health care costs for
pregnant women.
53
Second, the capitation rates for newly eligible adults also included other
adjustments. A number of States projected increased costs due to pent-up demand,
anticipating that many enrollees would have been previously uninsured and would
use additional services in the first several months of coverage. The rates in some
States also included adjustments for adverse selection with the expectation that the
52
2013 Actuarial Report on the Financial Outlook for Medicaid: http://www.medicaid.gov/medicaid-
chip-program-information/by-topics/financing-and-reimbursement/downloads/medicaid-actuarial-
report-2013.pdf.
53
It is difficult to generalize about the adjustments that the States have estimated for several
reasons. States may have defined differently the non-newly eligible adult population that served as
the basis for comparison for the newly eligible adults. (For example, States may have compared the
newly eligible adults to only non-newly eligible childless adults or to childless adults and parents or
caretaker adults, or States may have compared the newly eligible adults to only non-disabled adults
or to non-disabled adults and some adults with disabilities.) Most States also removed from the
comparison pregnant women who are non-newly eligible for Medicaid, but the projections in this
report include pregnant women among non-newly eligible adults; thus, it is difficult to compare the
assumptions the States made with the projections and analysis in this report directly. In addition,
States used various methodologies to develop this adjustment and in some cases combined it with
other adjustments (for example, for adverse selection or pent-up demand).

38
persons who were most likely to enroll in the first year would be those with the
greatest health care needs. In previous reports, the projections were adjusted in
2014 to account for these effects, increasing the projected expenditures per enrollee
by about 12 percent. In many cases, the capitated rates included adjustments for
these factors that were substantially greater than this percentage.
Data for newly eligible adults are still limited. While CMS has reported some
enrollment and expenditure data for this group, data on claims and managed care
encounters, along with data on the health status and demographics of these
enrollees, are not yet available. Thus, there is still considerable uncertainty about
the health care costs of newly eligible adults in 2014, as well as for future years.
Given the uncertainty inherent in covering a large new population in Medicaid
(many of whom were expected to have been previously uninsured), most States that
implemented the eligibility expansion included risk-sharing arrangements in their
contracts with managed care plans for newly eligible adults in 2014.
54
The most
common approaches were to use a risk corridor or to use a minimum medical loss
ratio. Under a risk corridor, the managed care plans would return some payments
to the State and the Federal government if the average benefits per enrollee or loss
ratio fell below a certain level or ratio, and the plans would receive additional
payments from the State and the Federal government if the average benefits per
enrollee or loss ratio exceeded a certain level or ratio. In States requiring a
minimum medical loss ratio, the managed care plans would return some payments
to the State and the Federal government if the loss ratio fell below a certain level,
but the plans would not receive additional funding if the loss ratio was higher than
expected. Most of these arrangements are expected to continue into 2015 as well.
As a result of these arrangements, there is the potential that the ultimate payments
for newly eligible adults in 2014 could be notably greater than or less than those
currently reported. The settlement of these provisions will not be completed until
later in 2015. Based on the comparison to the projections in prior reports, there is a
greater likelihood that funds would be returned to the States and the Federal
government than that the States and Federal government would be required to
provide additional funds to the plans. It is also possible that the amount returned to
the States and the Federal government could represent a significant portion of the
payments made in 2014; however, since data are not yet available, the projections
in this report assume that there will be no net payments due to these
arrangements.
For 2015, the total projected expenditures were adjusted to reflect about 50 percent
of the relative difference between the model projections and the preliminary actual
54
Of the States that did not use a risk-sharing arrangement, several covered newly eligible adults
under fee-for-service arrangements, and one covered enrollees through private health insurance
plans using premium assistance. Several other States chose not to use risk-sharing arrangements.

39
expenditures from the CMS-64 reports in 2014. This adjustment is based on two
assumptions: (i) that the effects of pent-up demand and adverse selection are
substantially less in the second year of the eligibility expansion and (ii) that
preliminary data and additional analysis would be incorporated into the
development of capitation rates for Medicaid managed care plans. As capitation
rates for 2015 plans are not yet available for all States, it is not known what
amounts States have projected for these costs in 2015, and the actual costs per
enrollee could differ significantly with these projections and assumptions. The
projected per enrollee costs for newly eligible adults in 2015 are about 11 percent
less than those for other adults in 2015.
For 2016 through 2023, the projected expenditures from the OHRM are used in this
report. Based on those projections, per enrollee costs for newly eligible adults are
between 27 percent and 30 percent less than per enrollee costs for other adults.
The estimates for newly eligible adult enrollees in 2014 have also increased since
the 2013 report. In this year’s report, enrollment for this group is estimated to have
been 4.3 million PYE in fiscal year 2014, which is equivalent to about 5.7 million
enrollees over the calendar year. Preliminary enrollment data suggest that monthly
enrollment increased substantially over the course of the year and that enrollment
reached about 7 million by September 2014.
55
In the 2013 report, the estimate for
newly eligible adult enrollment in 2014 was lower: 3.7 million PYE, or the
equivalent of about 4.9 million enrollees over the calendar year.
There are several reasons for the differences between the projections in the
2013 report and this year’s projections, which are based on preliminary enrollment
data. For example, there may have been more people eligible under the new criteria
than estimated previously, or there may have been a greater participation rate
among newly eligible persons than previously assumed. In addition, there may have
been more persons enrolled in Medicaid through 2013 who were technically newly
eligible in 2014 (either persons who were covered as part of a limited-benefit waiver
but were considered newly eligible under the 2014 criteria, or persons who were
covered in States that expanded eligibility after the Affordable Care Act was
enacted but prior to 2014).
Due to the limited data on newly eligible enrollees in 2014 and the uncertainties
regarding both their health care costs and enrollment in the program, the estimates
and projections regarding this population may differ significantly from the
projections shown in this report, as they depend on a number of factors that are
unknown at this point in time.
55
These figures are based on preliminary 2014 data available from the CMS-64.
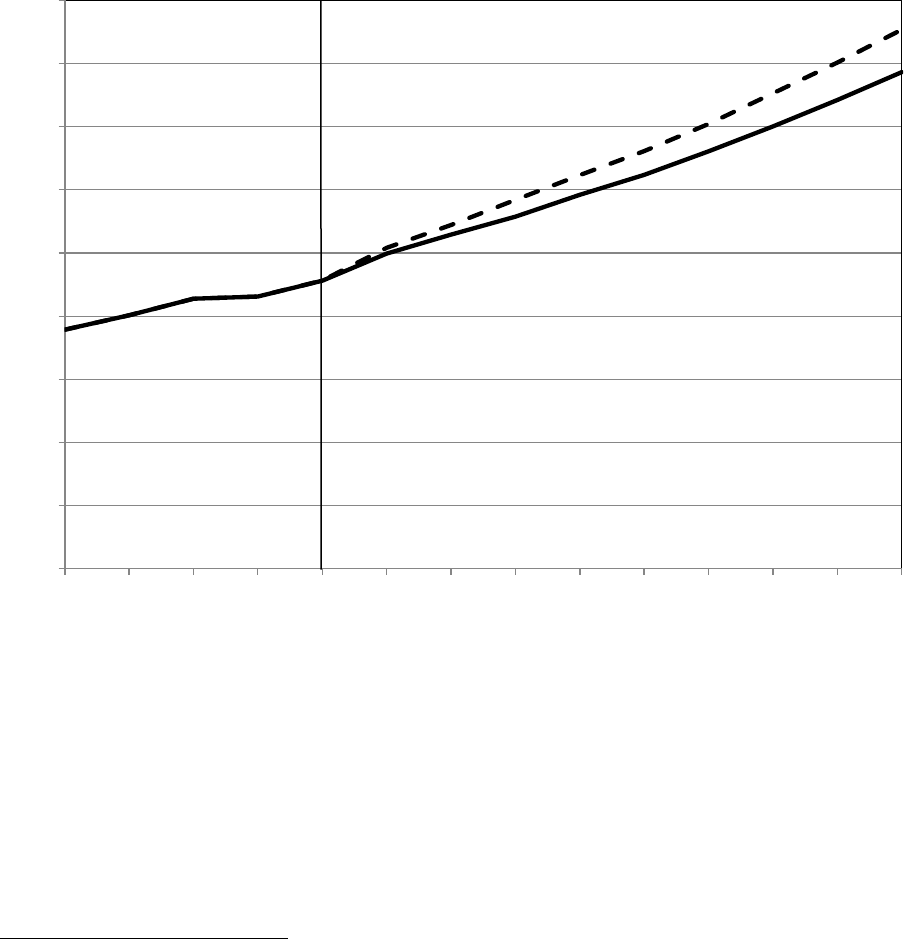
40
E. COMPARISON TO 2013 REPORT PROJECTIONS
The projections of Medicaid expenditures in this report are slightly lower than in
the 2013 Actuarial Report on the Financial Outlook for Medicaid. Figure 7 compares
the 2014 projections of total Medicaid expenditures (including Federal and State) to
those in last year’s report.
Figure 7—Projected Medicaid Expenditures: Comparison of 2013 versus 2014
Actuarial Reports on the Financial Outlook for Medicaid,
FY 2009–FY 2022
56
(in billions)
$0
$100
$200
$300
$400
$500
$600
$700
$800
$900
2009 2010 2011 2012 2013 2014 2015 2016 2017 2018 2019 2020 2021 2022
Fiscal Year
2014 Report
2013 Report
Actual
Projected
Projected spending of $786.6 billion in 2022 is 7.9 percent lower than the
corresponding amount in last year’s report ($853.6 billion). In total, the 10-year
projections from 2013 through 2022 are $341.6 billion, or 5.3 percent, lower.
This reduction is the result of several factors. First, 2014 expenditures in this year’s
report ($498.9 billion) were estimated to be lower than in last year’s report
($508.0 billion), representing a 1.8-percent difference. Most of the difference is
attributable to slower per enrollee expenditure growth for the non-newly eligible
56
The data for this graph can be found in table 17 of Appendix E.
41
enrollees in 2014 than projected last year, with States continuing to try to control
cost growth. This decrease is partly offset by greater expenditures for newly eligible
adults than previously projected. Lower expenditures in 2014 for non-newly eligible
Medicaid populations, along with a decrease in estimated costs for newly eligible
adults after 2014, result in lower projected expenditures in each year through 2022.
The projected increases in utilization (or the residual factors) were slower in this
year’s report than in last year’s. As recent historical expenditures have grown more
slowly, the outlook for future utilization growth in the program has become more
negative. In addition, the assumption regarding how many States would expand
Medicaid in the future has been reduced (from States covering 65 percent of
potentially newly eligible adults to 60 percent), and this modification also
contributes to lower projected expenditures by 2022.
Medicaid enrollment is expected to be somewhat lower by 2022 than projected in
the 2013 report for the same year. Enrollment is projected to reach 78.2 million
PYE by 2022, whereas enrollment was projected to be 80.9 million by 2022 in last
year’s report (a difference of 3.3 percent). This difference is due to updated partial
enrollment data for 2011, partial enrollment data for 2012, and the assumption that
fewer States would elect to implement the eligibility expansion than assumed last
year. Medicaid enrollment from 2013 to 2022 is projected to grow at an average rate
of 3.0 percent, which is lower than last year’s projection of 3.3 percent over the same
period.

42
F. MEDICAID IN CONTEXT
From the estimates and analysis of health spending in the U.S. provided by the
NHE accounts, additional insight can be obtained into the role of Medicaid within
the total U.S. health care system.
57
Medicaid spending in the 2013 NHE accounts
represented 15.4 percent of total NHE. Private health insurance was the largest
source of spending on health care in 2013, accounting for 32.9 percent of total NHE,
while Medicare paid for 20.1 percent.
58
The historical NHE also presents health care spending by the original source of
financing (or sponsor). In calendar year (CY) 2013, Medicaid represented
35.3 percent of Federal government expenditures on health services and supplies
and 38.6 percent of such spending by State and local governments. Medicaid is
slightly smaller than Medicare as a share of Federal government expenditures on
health services and supplies (Medicare accounted for 36.2 of Federal expenditures
in 2013). Medicaid is the largest source of Federal general revenue-based spending
on health services. A sizeable portion of Medicare spending is funded by income
from dedicated revenue sources—which include Medicare Part A payroll taxes and
Part B and Part D beneficiary premiums—with the balance mostly from Federal
general revenues. In contrast, Medicaid does not have any dedicated Federal
revenue source; all Federal spending on Medicaid comes from general revenue. For
State governments, Medicaid is the largest source of general revenue-based
spending on health services, although spending on all other health programs in
2009 exceeded spending on Medicaid, largely because of the temporary increases to
the FMAP.
59
Medicaid has a greater number of enrollees than Medicare. In FY 2013, Medicaid
was estimated to have covered 58.9 million PYE (including persons residing in U.S.
Territories), and 72.5 million people were enrolled in the program at some point
during the year. In comparison, Medicare covered an average of 52.3 million people
57
The historical Medicaid spending data and projections presented in this report differ slightly from
the NHE estimates and projections in several ways. Some of the differences are as follows: (i) the
data and projections featured in this report are shown on a fiscal year basis, whereas the NHE
amounts are on a calendar year basis; (ii) the NHE accounts make several adjustments to Medicaid,
such as classifying Medicaid spending for Medicare premiums as Medicare spending; and (iii) the
NHE accounts use somewhat different definitions of services than do the data presented in this
report.
58
Hartman, et al., “National Health Spending In 2013: Growth Slows, Remains In Step With The
Overall Economy.”
59
Ibid. There are some State dedicated revenues for Medicaid. For more detail on this analysis of
health care spending by sponsor, see the methodology paper at http://www.cms.gov/Research-
Statistics-Data-and-Systems/Statistics-Trends-and-Reports/NationalHealthExpendData/Downloads/
dsm-11.pdf.

43
during CY 2013.
60
Within these totals, there are substantial differences between the
programs in the number and nature of people covered. For example, Medicare
automatically covers nearly all people over age 65 (43.5 million beneficiaries in
2013), but only those aged individuals with very low incomes—and who apply for
the coverage—become Medicaid enrollees (estimated at 5.3 million PYE).
Enrollment for persons with disabilities was more similar between the two
programs; Medicaid covered an estimated PYE average of 10.1 million blind or
disabled persons in 2013, while Medicare covered 8.8 million disabled beneficiaries.
Although the definition of disability is essentially the same for the two programs,
the other eligibility criteria are entirely different.
61
Finally, as noted earlier, a
majority of Medicaid enrollees are either children or certain adults in families with
low incomes. Medicare does not have comparable categories of beneficiaries. Dual-
eligible individuals accounted for an estimated $146.1 billion of total Medicaid
expenditures in 2013, or 34 percent of benefits.
62
Among the different types of health care services, Medicaid plays the largest role in
the funding of long-term care. According to the 2013 NHE, Medicaid is estimated to
have paid for 36.5 percent of all freestanding home health care and 30.1 percent of
all freestanding nursing home care in the U.S. In addition, Medicaid covered an
estimated 55.7 percent of other health, personal, and residential care in 2013,
including payments for intermediate care facilities and for home and community-
based waivers.
63
Medicaid has a major responsibility for providing long-term care
because the program covers some aged and many persons with disabilities, who
tend to be the most frequent and most costly users of such care, and because private
health insurance and Medicare often furnish only limited coverage for these
benefits, particularly for nursing homes. Many people who pay for nursing home
care privately become impoverished due to the expense; as a result, these people
eventually become eligible for Medicaid. Figure 8 shows the percentage of total
spending for the major health care services that Medicaid covers.
60
The 2014 Annual Report of the Boards of Trustees of the Federal Hospital Insurance and Federal
Supplementary Medical Insurance Trust Funds. http://www.cms.gov/Research-Statistics-Data-and-
Systems/Statistics-Trends-and-Reports/ReportsTrustFunds/downloads/tr2014.pdf.
61
Medicaid eligibility for individuals with disabilities is based on income and asset criteria (among
other measures). Medicare eligibility generally depends on an individual’s sufficient participation in
the paid work force prior to disability. Despite these different requirements, a significant number of
persons with disabilities qualify for coverage under both Medicaid and Medicare.
62
These figures reflect actual 2013 reported expenditures from the CMS-64 and projected
2013 enrollment and expenditure information that are based on 2010 and 2011 APS data.
63
Hartman, et al., “National Health Spending In 2013: Growth Slows, Remains In Step With The
Overall Economy.”
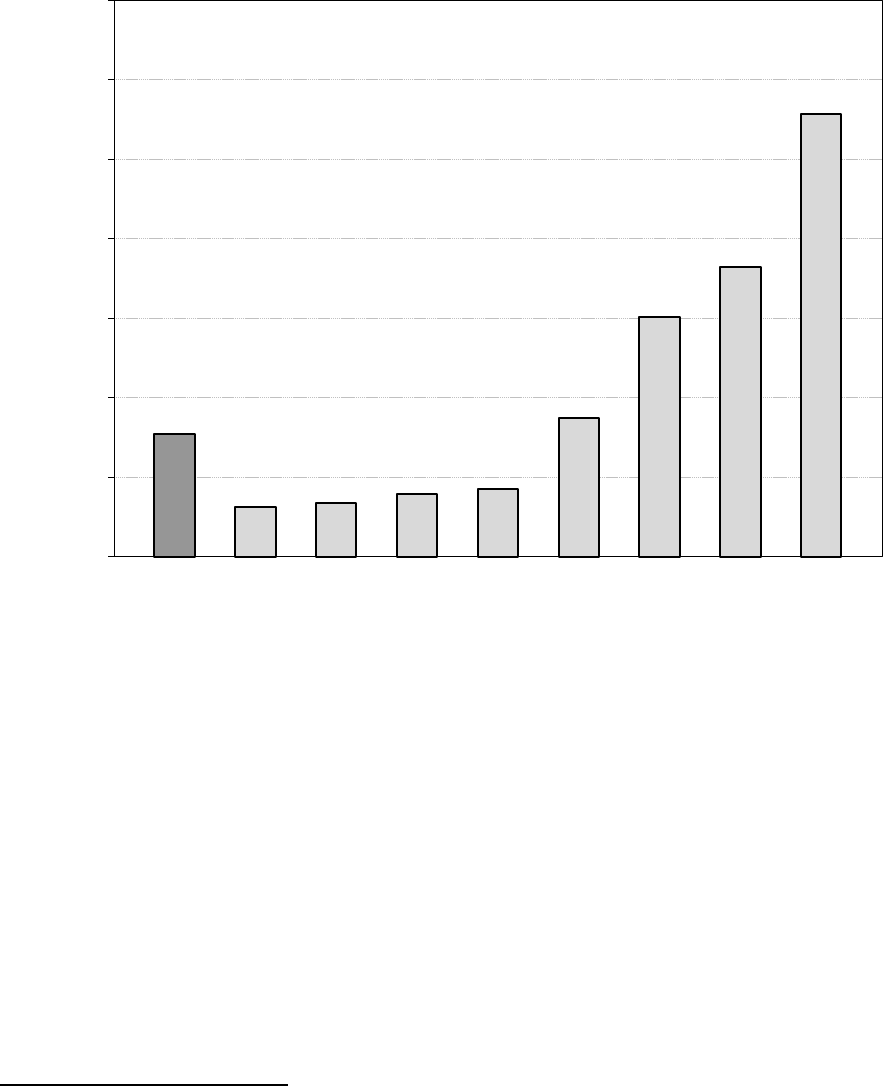
44
Figure 8—Medicaid Expenditures as Percentage of Total U.S. Health Expenditures,
by Service Category, CY 2013
Total
15.4%
Other Prof.
6.2%
Dental
6.8%
Drugs
7.8%
Physicians
and Clinics
8.5%
Hospital
17.5%
Nursing Home
30.1%
Home Health
36.5%
Oth Hlth, Resid.
& Pers. Care
55.7%
0%
10%
20%
30%
40%
50%
60%
70%
Medicaid Share
Service
Medicaid represents a significant share of the Federal and State budgets. In
FY 2014, out of a total of $3,506 billion spent by the Federal government for all
purposes, $301 billion (or 8.6 percent) can be attributed to Medicaid. Under the
President’s Fiscal Year 2016 Budget, Federal outlays on Medicaid are projected to
account for 8.9 percent of all Federal outlays by 2023.
64
According to the National Association of State Budget Officers (NASBO), Medicaid
represented an estimated 24.5 percent of all State government spending in State
fiscal year 2013.
65
This amount, however, includes all Federal contributions to State
Medicaid spending, as well as expenditures from State general revenue funds and
other State funds (which for Medicaid may include provider taxes, fees, donations,
assessments, and local funds). According to NASBO, Medicaid was the largest
program in 2013. When only State general revenues are considered, however,
Medicaid spending constituted an estimated 18.9 percent of State expenditures in
2013, placing it well behind elementary and secondary education. The share of
64
More information on the Federal budget is available in Analytical Perspectives, Budget of the
United States Government, Fiscal Year 2016.
65
State Expenditure Report: Examining Fiscal 2012–2014 State Spending, National Association of
State Budget Officers, 2014.
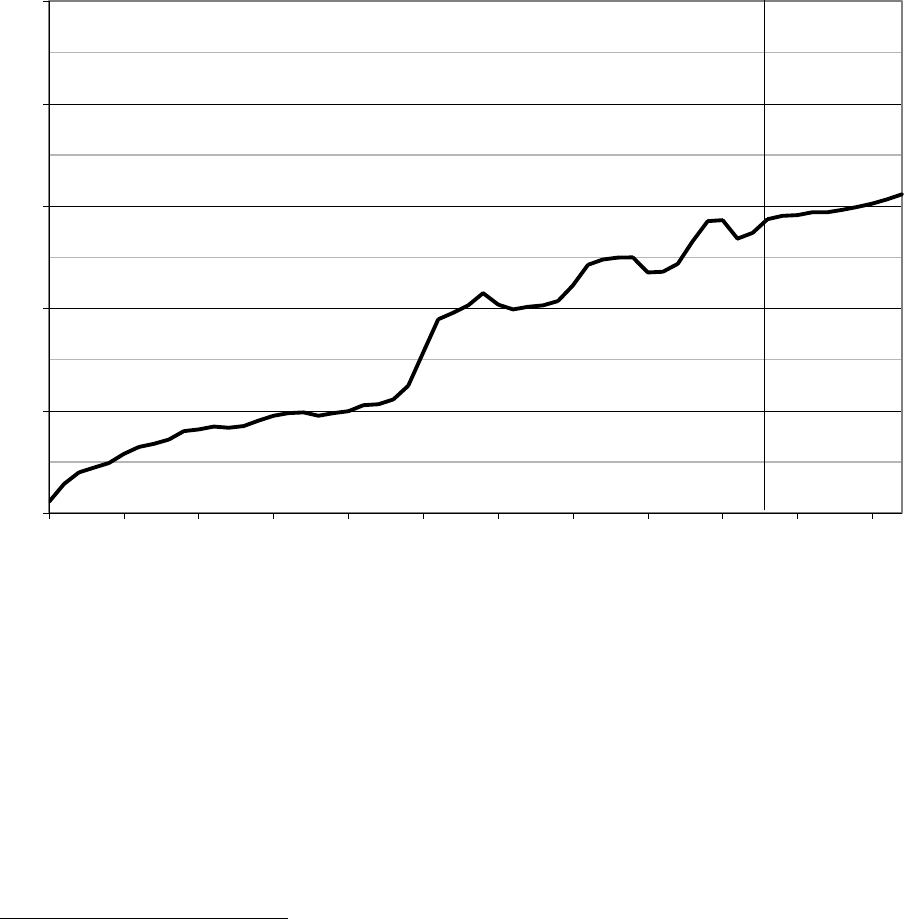
45
State general revenues devoted to Medicaid decreased from 2012 to 2013 (from
19.2 percent to 18.9 percent). Overall in 2013, State general revenue expenditures
for Medicaid increased by 2.8 percent, which was slower than the overall State
general revenue growth rate of 4.3 percent.
As shown in figure 9, Medicaid represented about 2.7 percent of GDP in 2013—the
same as the share in 2012. This increase corresponds with the typical historical
trend in Medicaid growth as a share of GDP.
Figure 9—Past and Projected Medicaid Expenditures as Share of GDP,
FY 1966–FY 2023
0%
1%
2%
3%
4%
5%
1966 1971 1976 1981 1986 1991 1996 2001 2006 2011 2016 2021
Fiscal Year
Actual
Projected
66
In 2014, GDP is estimated to have grown at a rate of 4.3 percent, while Medicaid
spending is expected to have increased by 9.4 percent due to the coverage expansion
under the Affordable Care Act. While GDP is anticipated to grow more rapidly in
2015 and 2016, the continuing effects of the eligibility expansion are expected to
contribute to faster Medicaid growth and further increases in Medicaid’s share of
GDP. By 2016, Medicaid spending is projected to reach 2.9 percent of GDP.
As seen in figure 9, the program’s expenditures are projected to continue to grow to
3.1 percent of GDP by 2023. From 2014 through 2023, Medicaid expenditures are
projected to increase about 1.4 percentage points faster than GDP on average per
66
The data for this graph can be found in table 18 of Appendix E.
46
year. Much of this difference is expected to be due to the eligibility expansion, which
accounts for 0.8 percentage point, or about two-thirds, of the difference between
projected Medicaid expenditure and GDP growth rates over the 10 years.
This projection of Medicaid spending as a share of GDP is less than the projection
included in last year’s report. The share of GDP devoted to Medicaid in 2022 is
projected to be 3.1 percent, about 0.2 percentage point lower than in the
2013 projection. Medicaid expenditures are projected to grow more slowly than
previously projected, driven primarily by lower 2014 per enrollee expenditure
growth and a reduction in the assumption about the number of States that would
expand eligibility.
47
VI. CONCLUSION
Medicaid expenditures are estimated to have grown 9.4 percent in 2014 and to have
reached $498.9 billion. Faster growth is estimated to have been strongly driven by
the eligibility expansion that started on January 1, 2014 under the Affordable Care
Act. Growth is expected to slow after 2014, but the expansion of eligibility by
additional States is projected to contribute to some additional increases in
expenditures and enrollment of newly eligible adults. Total Medicaid expenditures
are projected to grow to $835.0 billion by 2023. The projected annual average
growth rate of Medicaid expenditures from 2014 to 2023 is 6.2 percent—notably
faster than the projection of average annual GDP growth of 4.9 percent. Should
these trends continue as projected under current law, Medicaid’s share of both
Federal and State budgets would continue to expand.
The expansion of Medicaid eligibility under the Affordable Care Act will likely
broaden Medicaid’s role as part of the U.S. health care system. This growing role,
however, also increases the likelihood that health care-related issues and concerns
will necessarily involve Medicaid to a greater extent than in the past.
While some data are available on the number of newly eligible adults enrolled in
Medicaid and their health care costs, there is still a considerable amount of
uncertainty regarding the projections of the eligibility expansion impacts. Along
with the expansion of Medicaid eligibility, other significant changes occurred in
2014, including the conversion of the income eligibility criteria to a modified
adjusted gross income (MAGI) basis and the start of the Health Insurance
Marketplaces. Accordingly, the actual expenditures, enrollment, and effects of the
Affordable Care Act may differ significantly from the estimates and projections
presented in this report.
The proportion of Medicaid expenditures for capitation payments and premiums has
been increasing, as are the number of enrollees that receive all or some of their
Medicaid benefits through a managed care plan. This trend is expected to accelerate
due to the coverage by many States of newly eligible enrollees through managed
care plans in 2014. In addition, States have expanded the use of managed care to
cover aged and disabled enrollees and long-term care services. Thus, understanding
how the use of managed care in Medicaid will affect future expenditure growth—
and how fee-for-service expenditures for acute care and long-term care will also be
affected—will be an important consideration for Medicaid programs in the future.
Because Medicaid does not have any dedicated revenue source at the Federal level
or a trust fund approach to financing, the solvency of the program is not an issue;
the expenditures of each State (or Territory) program are covered by the State’s
revenues plus Federal matching general revenues. However, even without solvency
as a concern, Medicaid constitutes a significant portion of spending by both Federal
and State governments and thus is important to evaluate as part of the budget.
48
Typically the cost growth rates of different payers and programs, such as Medicare,
Medicaid, and private health insurance plans, are related. Attempts by one payer or
program to affect costs can have a direct or indirect impact on other payers and
programs. Whether such efforts are focused on the payment or management of
health care specific to certain programs, or on the delivery or practice of health care
generally, it will be important to consider the potential effects not just on Medicaid
but across all health care payers. Programs and demonstrations that focus on
health care provided for persons enrolled in both Medicare and Medicaid (dual-
eligible beneficiaries), or that focus on Medicare but also include some dual-eligible
beneficiaries, may have some effects on the costs and quality of care paid for by
Medicaid.
This report includes projections of the current-law Medicaid program. As policy
makers consider changes or reforms to the program, for Medicaid specifically or for
the broader health care system, particular attention may need to be paid to the
ways in which Medicaid differs from other types of health care coverage—for
example, in its administration, the benefits offered, the populations covered, and
the ways in which it pays for health care. Other important issues for consideration,
as Medicaid’s role continues to evolve, are provider participation, Medicaid payment
rates, and beneficiary access to services.

49
VII. APPENDIX
A. MEDICAID DATA SOURCES
The primary sources for Medicaid statistical data used in the projections of
Medicaid expenditures and enrollment are the Medicaid Statistical Information
System (MSIS) and the CMS-64 and CMS-37 reports.
Medicaid Statistical Information System (MSIS)
MSIS is the basic source of State-submitted eligibility and claims data on the
Medicaid population, its demographic characteristics, utilization of health care
services, and payments. The purpose of MSIS is to collect, manage, analyze, and
disseminate information on eligible individuals, beneficiaries, utilization, and
payment for services that are covered. States provide CMS with quarterly files
consisting of specified data elements for persons covered by Medicaid and
adjudicated claims for medical services reimbursed with Title XIX funds. Four types
of claims files representing inpatient, long-term care, prescription drugs, and non-
institutional services are submitted. Claims records contain information on the
types of services used, providers, service dates, costs, and types of reimbursements.
Eligibility characteristics, such as basis-of-eligibility and maintenance assistance
status, are the foundation of OACT’s demographic projections; specifically, the
primary basis-of-eligibility categories include aged persons, blind or disabled
persons, non-disabled children (including foster care children), and non-aged non-
disabled adults (including women eligible under the Breast and Cervical Cancer Act
eligibility expansion). MSIS data are made available in several different files;
generally, the analysis presented in this report has relied on the Annual Person
Summary (APS) files.
CMS-64 and CMS-37 Reports
The CMS-64 and CMS-37 reports are products of the Medicaid and CHIP Budget
and Expenditure Systems (MBES/CBES). These reports are submitted by the States
quarterly. The CMS-64 provides current fiscal year spending, while the CMS-37
provides State budgeted amounts for the next 2 fiscal years. The expenditure
amount shown on the CMS-64 report is a summary of expenditures for the various
mandatory and optional services covered by the Medicaid State programs.
The mandatory services contained in the CMS-64 and CMS-37 reports include
inpatient and outpatient hospital care, physician services, nursing facility care for
individuals aged 21 or older, family planning services, rural health clinic services,
home health care, laboratory and x-ray tests, other practitioner services, federally
qualified health centers, and early and periodic screening, diagnostic, and
treatment services for children under age 21 (EPSDT). Among the many reported
optional services that States may provide are clinic services, prescription drugs,
50
intermediate care facilities for the intellectually disabled, hospice care, home and
community-based care to certain persons with chronic impairments, and targeted
case management services. Additionally, these reports capture expenditures for
DSH payments, offsets to drug spending through rebates, Medicare Parts A and B
premiums paid for those dually eligible for both Medicare and Medicaid, premiums
paid for Medicaid-only capitated arrangements, and expenditures for home and
community-based waiver programs.
Users of Medicaid data may note discrepancies between the expenditure
information captured in MSIS and the CMS-64. For example, DSH payments and
Medicare premiums do not appear in MSIS. Whereas actual payments are reflected
in the CMS-64, in MSIS adjudicated claims data are used. Service definitions vary
in these two sources, as well. Territorial data for American Samoa, Guam, the
Northern Mariana Islands, Puerto Rico, and the Virgin Islands appear in the
CMS-64, but not in MSIS. Each State has a different system for capturing
statistical (MSIS) and financial (CMS-64) data.

51
B. DEMOGRAPHIC, ECONOMIC, AND HEALTH CARE ASSUMPTIONS
The primary demographic, economic, and health cost inflation assumptions
underlying the Medicaid projections shown in this report are the same as those used
by the Social Security and Medicare Boards of Trustees in their 2014 report to
Congress.
67
Price Assumptions
The price assumptions used to develop the Medicaid expenditure projections are
derived from the Social Security and Medicare Trustees Report assumptions. While
these price assumptions are specifically meant to measure the changes in the prices
that Medicare would pay providers, they also generally reflect the projected growth
in the prices of health care services.
As noted in section IV of this report, there is no single data source available that
tracks all Medicaid prices or price changes. In addition, there are no specific or
consistent forecasts of the changes in the prices for health care services that can be
used across all Medicaid programs since States do not have a prescribed
methodology for updating provider reimbursement rates. Accordingly, we rely on
other forecasts from Medicare, which we believe are reasonable projections of the
underlying growth in health care prices that States would consider when changing
provider reimbursement rates within their Medicaid programs.
The principal economic assumptions include growth in average wages and the CPI.
These and other assumptions are used to generate health care service input price
indices (or “market baskets”) for inpatient hospital and home health care services.
These indices serve as indicators of increases in Medicaid payments per service.
It is important to note that these price assumptions may not accurately measure
the underlying changes in the prices paid by Medicaid programs year to year. States
have significant discretion in setting reimbursement rates, and in any given year
the changes in rates paid to providers may differ from the changes in the price
assumptions that are used to project future price changes for Medicaid
expenditures. Thus, while these price forecasts are expected to reasonably estimate
the changes in prices over time, they may not be precise measures of the actual
changes in prices in any State Medicaid program. Moreover, to the extent that any
specific price assumption is not an accurate assessment of the change in the price
paid for any particular service, the difference between the actual change in price
and the change in the price assumption would be reflected in the residual factor.
67
Further information on the Trustees’ population projections and economic assumptions is available
in the 2014 Social Security and Medicare Trustees Reports: http://www.cms.gov/Research-Statistics-
Data-and-Systems/Statistics-Trends-and-Reports/ReportsTrustFunds/downloads/tr2014.pdf.

52
While in general the residual factor is meant to represent changes in utilization, it
would also incorporate errors in the measurement of prices.
Enrollment Projections and Demographic Assumptions
Medicaid enrollment is projected by eligibility category: aged, disabled, children,
and adults. Enrollment for newly eligible adults is projected separately as part of
the OHRM. The model measures enrollment by eligibility category as a percentage
of the U.S. population by relevant age group (aged—U.S. population aged 65 and
over; disabled—U.S. population aged 0-64; children—U.S. population aged 0-19; and
adults—U.S. population aged 20-64). Historical enrollment is measured for 1992
through 2010—the period for which reliable enrollment data exist in the MSIS.
68
The relationship between the change in the share of the U.S. population enrolled in
Medicaid by eligibility category and the change in the national U.S. unemployment
rate is measured using a regression model. Analysis conducted in developing this
enrollment model has shown that the unemployment rate is the most meaningful
factor in analyzing changes in historical Medicaid enrollment. Other economic
variables are either not statistically significant or do not improve the accuracy of
the model. In addition, changes in the unemployment rate have a strong theoretical
relationship with Medicaid enrollment. As the unemployment rate increases, fewer
people have jobs, leading in turn to a greater number of people with lower incomes
and more individuals likely eligible for Medicaid. In addition, a decrease in the
number of people with jobs is likely to lead to fewer people with private health
insurance, and as a result more people may enroll in Medicaid for health care
coverage. Conversely, as the unemployment rate decreases, an increase in the
number of people with jobs is likely to lead to increases in income and more people
with private health insurance, and as a result enrollment growth in Medicaid may
be slower.
The change in the share of the U.S. enrolled population is projected forward using
the results of the regression model and forecasts of the unemployment rate from the
2014 Social Security Trustees Report for each eligibility category. Enrollment is
projected using those results and the forecasts of the U.S. population from the 2014
Trustees Report. The projections from the model may be adjusted, in particular for
estimates of enrollment in recent years (in this report, enrollment is estimated for
68
Medicaid enrollment data have lagged by as much as 2 years in recent history, and this lag has
increased substantially during the transition to the new Medicaid data system. CMS is in the
process of transitioning Medicaid data from MSIS to the Transformed Medicaid Statistical
Information System (T-MSIS), but T-MSIS is not currently available. Until the system is
operational, it is unclear what data will be available and what form the data will take. CMS is
discontinuing the production of the APS files, and different approaches will likely be necessary to
incorporate data for 2012 and 2013 in future reports. More information about T-MSIS is available at
http://www.medicaid.gov/medicaid-chip-program-information/by-topics/data-and-systems/medicaid-
and-chip-operational-data.html.

53
2011, 2012, and 2013); in estimating historical enrollment, other information or
data is often used to adjust the results from the Medicaid enrollment models.
Typically, other sources do not provide enrollment at the same level of detail as
shown in MSIS or in this report, but such sources may inform the overall level of
enrollment or the growth rate of total enrollment in those historical years.
Residual Analysis and Utilization Assumptions
Changes in the utilization of services and other changes in expenditures not
reflected in changes in enrollment or prices are reflected in the “residual” factors in
the model. The trend residual approach to projecting Medicaid expenditures begins
with an analysis of historical Medicaid expenditures per enrollee on a service-by-
service basis. The annual percent change in these per enrollee expenditures is
compared to the change in the applicable price indicator (listed below), and the
differential, or residual, is calculated. This residual measures the collective impact
of changes in utilization and “intensity” (average complexity) of services, case mix
effects, and other factors, and it is calculated by service and by eligibility category.
For the purpose of developing projected expenditures, the residual may be
calculated as the average across all eligibility categories (typically when the
residuals across eligibility categories have similar values, or when the amount of
spending for one or more eligibility categories is relatively small and there are
potential concerns about the credibility of the residual factor). The basis of the
projected residual is the historical average of the residual value (either as a
weighted average or an unweighted average over the previous several years), but
the residual may be adjusted by gradually increasing or decreasing the residual
toward the average residual for a broader category of services (such as all acute
care, all long-term care, or all medical services).
The residuals are adjusted to limit the value of any particular service from
significantly increasing or decreasing more than the value of all services (or broader
categories of services). In general, the residual of all services (or broader categories
of services) tends to be more stable, but it is necessary to use residuals by service to
account for changes in the Medicaid program as well. Often, these adjustments are
made to reflect areas where there has likely been a shift between services or
categories of services in recent history, but projecting those changes to continue at
the same rate over 10 years would not necessarily be the best estimate of future
expenditures.
One key example concerns the historical shifts of Medicaid expenditures from fee-
for-service programs (especially acute care services, such as hospital services,
physician and other professional services, and prescription drugs) to managed care.
As part of the adjustment, managed care expenditures as a share of total
expenditures were reviewed by State and by eligibility category. This review
provided more detailed information on the use of managed care across States, as
well as some evidence regarding the extent to which recent expenditure growth in
54
managed care programs was driven by the States’ expansion of their use of these
programs. The analysis suggested that managed care expenditures were likely to
continue to grow relatively quickly but, over time, were more likely to slow, as the
rate at which States shift expenditures to managed care programs slows. Similarly,
the analysis suggested that the residuals for acute care services in general would
increase over the same period as the shift from fee-for-service programs decelerates.
The table below displays the price indicators currently used to produce Medicaid
expenditure projections.
Type of Service
Price Indicator
Inpatient and outpatient hospital
Medicare hospital input price index (market basket),
before the application of productivity adjustment
Physician, clinic, and related services
Medical CPI increase
Institutional long-term care
Maximum of CPI increase and average wage increase
Community long-term care and home
and community-based waiver services
Medicare home health input price index, before the
application of productivity adjustment
Prescription drugs
CPI increase
Managed care
Medical CPI increase
One exception to the trend residual methodology occurs in the case of some
premiums. Costs for other premiums for Medicare are based on the Trustees’
projected premium rates for Medicare Parts A and B. The proportions of aged and
blind or disabled enrollees who are “bought into” Medicare by the States or the
Federal government through premium payments are assumed to remain at
historical levels.

55
Utilization Factors for Selected Services by Medicaid Population
This section provides the results of the residual analysis used to calculate the
utilization factors for the projections. The following tables show the historical
utilization factors and the projected values by eligibility category and by service for
the largest five services by eligibility category (as measured by total
2013 expenditures).
Table 5—Historical and Projected Utilization Factors for Aged Enrollees, Selected Services,
FY 2006–FY 2023
Fiscal
Year
Nursing
facility
Managed
care
Home and community-
based waivers
Personal
care
Inpatient
hospital
Historical data:
2006
−3.2%
−23.8%
3.7%
8.0%
-5.8%
2007
−6.4%
13.1%
6.2%
9.0%
1.4%
2008
−2.5%
38.8%
7.1%
−7.5%
0.4%
2009
0.2%
8.4%
−1.2%
0.0%
−2.0%
2010
−5.7%
22.8%
−9.7%
−8.2%
−4.3%
2011
−4.9%
19.1%
−1.1%
−12.7%
19.4%
2012
−5.7%
19.2%
−1.8%
−5.0%
−11.5%
2013
−3.2%
9.7%
−0.2%
−15.5%
1.0%
Projections:
2014
−4.1%
16.0%
0.3%
−7.8%
−0.1%
2015
−3.8%
14.1%
0.3%
−7.2%
−0.1%
2016
−3.6%
12.2%
0.3%
−6.6%
−0.2%
2017
−3.3%
10.3%
0.3%
−5.9%
−0.2%
2018
−3.0%
8.4%
0.3%
−5.3%
−0.3%
2019
−2.8%
6.5%
0.3%
−4.7%
−0.4%
2020
−2.8%
6.5%
0.3%
−4.7%
−0.4%
2021
−2.8%
6.5%
0.3%
−4.7%
−0.4%
2022
−2.8%
6.5%
0.3%
−4.7%
−0.4%
2023
−2.8%
6.5%
0.3%
−4.7%
−0.4%
These are the largest six services for aged enrollees based on estimates of
2013 expenditures, and they constituted 82 percent of total estimated Medicaid
expenditures for aged enrollees, as shown in table 6. (Medicare Part B premiums
are shown below, but utilization factors are not calculated for Medicare premiums.)
Table 6—FY 2013 Selected Service Expenditures for Aged Enrollees
(in billions)
Service
2013 Expenditures
Nursing Facility
$38.3
Managed Care
10.7
Home and Community-Based Waivers
5.5
Medicare Part B Premiums
5.0
Personal Care
3.5
Inpatient Hospital
3.4
Total Aged Enrollees Expenditures
81.5

56
Table 7—Historical and Projected Utilization Factors for Disabled Enrollees, Selected Services,
FY 2006–FY 2023
Fiscal Year
Home and
community-
based waivers
Managed
care
Inpatient
hospital
Nursing
facility
Prescription
drugs
Historical data:
2006
9.0%
−4.7%
−2.2%
−2.3%
−34.9%
2007
1.2%
17.4%
−0.1%
−6.5%
−23.1%
2008
1.9%
12.2%
−3.4%
−2.3%
−2.9%
2009
4.2%
7.5%
−1.5%
3.0%
1.7%
2010
3.0%
2.9%
3.2%
−4.6%
−2.4%
2011
−4.6%
11.6%
3.4%
−3.8%
2.1%
2012
−1.9%
9.1%
−10.5%
−6.1%
−15.2%
2013
1.1%
11.6%
−1.3%
−2.6%
−16.3%
Projections:
2014
0.3%
9.3%
−2.0%
−3.3%
−4.7%
2015
0.3%
8.3%
−1.8%
−3.2%
−4.3%
2016
0.3%
7.3%
−1.7%
−3.0%
−3.9%
2017
0.3%
6.3%
−1.6%
−2.8%
−3.5%
2018
0.3%
5.3%
−1.4%
−2.6%
−3.1%
2019
0.3%
4.3%
−1.3%
−2.4%
−2.7%
2020
0.3%
4.3%
−1.3%
−2.4%
−2.7%
2021
0.3%
4.3%
−1.3%
−2.4%
−2.7%
2022
0.3%
4.3%
−1.3%
−2.4%
−2.7%
2023
0.3%
4.3%
−1.3%
−2.4%
−2.7%
This is the list of residuals for the top five services for persons with disabilities
based on estimates of 2013 expenditures, and these services constituted 66 percent
of total estimated Medicaid expenditures for disabled enrollees, as shown in table 8.
(Prescription drug expenditures do not include Medicaid prescription drug rebates.)
Table 8—FY 2013 Selected Service Expenditures for Disabled Enrollees
(in billions)
Service
2013 Expenditures
Home and Community-Based Waivers
$32.6
Managed Care Organizations
31.6
Inpatient Hospital
28.0
Nursing Facility
12.6
Prescription Drugs
11.4
Total Disabled Enrollees Expenditures
175.2

57
Table 9—Historical and Projected Utilization Factors for Child Enrollees, Selected Services,
FY 2006–FY 2023
Fiscal Year
Managed
care
Inpatient
hospital
Prescription
drugs
Physician
Outpatient
hospital
Historical data:
2006
17.9%
−4.5%
−0.3%
−2.8%
−10.6%
2007
11.2%
5.4%
0.5%
−7.0%
7.7%
2008
−2.4%
1.0%
1.2%
0.2%
−10.8%
2009
2.1%
−4.7%
−0.2%
−1.9%
6.8%
2010
−0.9%
−9.5%
0.8%
−5.7%
−4.9%
2011
5.0%
−1.5%
7.6%
−0.2%
6.6%
2012
14.4%
−11.4%
−15.9%
−13.9%
−19.9%
2013
10.5%
−1.0%
−19.4%
−10.4%
3.9%
Projections:
2014
6.8%
−4.4%
−4.7%
−5.3%
−3.2%
2015
5.0%
−3.4%
−3.7%
−4.2%
−2.6%
2016
3.1%
−2.5%
−2.7%
−3.0%
−1.9%
2017
3.1%
−2.5%
−2.7%
−3.0%
−1.9%
2018
3.1%
−2.5%
−2.7%
−3.0%
−1.9%
2019
3.1%
−2.5%
−2.7%
−3.0%
−1.9%
2020
3.1%
−2.5%
−2.7%
−3.0%
−1.9%
2021
3.1%
−2.5%
−2.7%
−3.0%
−1.9%
2022
3.1%
−2.5%
−2.7%
−3.0%
−1.9%
2023
3.1%
−2.5%
−2.7%
−3.0%
−1.9%
This is the list of residuals for the top five services for the child population based on
estimates of 2013 expenditures, and these services constituted 80 percent of total
estimated Medicaid expenditures for children, as shown in table 10. (Prescription
drug expenditures do not include Medicaid prescription drug rebates.)
Table 10—FY 2013 Selected Service Expenditures for Child Enrollees
(in billions)
Service
2013 Expenditures
Managed Care Organizations
$41.1
Inpatient Hospital
10.9
Prescription Drugs
4.1
Physician Services
3.3
Outpatient Hospital
2.9
Total Children Expenditures
78.2

58
Table 11—Historical and Projected Utilization Factors for Adult Enrollees, Selected Services,
FY 2006–FY 2023
Fiscal Year
Managed
care
Inpatient
hospital
Outpatient
hospital
Prescription
drugs
Physician
Historical data:
2006
13.4%
−5.1%
−10.6%
−17.1%
−2.9%
2007
11.5%
0.6%
7.7%
−8.6%
−7.8%
2008
5.4%
−3.6%
−10.8%
−0.4%
−3.8%
2009
1.5%
−7.4%
6.8%
4.8%
−5.9%
2010
4.4%
−8.6%
−4.9%
9.9%
−6.8%
2011
6.7%
7.5%
6.6%
15.0%
−2.4%
2012
10.9%
−15.5%
−19.9%
−16.7%
−14.5%
2013
8.5%
1.8%
3.9%
−12.7%
−8.4%
Projections:
2014
7.3%
−4.1%
−3.2%
−4.7%
−6.6%
2015
5.3%
−3.2%
−2.6%
−3.7%
−5.1%
2016
3.4%
−2.4%
−1.9%
−2.7%
−3.6%
2017
3.4%
−2.4%
−1.9%
−2.7%
−3.6%
2018
3.4%
−2.4%
−1.9%
−2.7%
−3.6%
2019
3.4%
−2.4%
−1.9%
−2.7%
−3.6%
2020
3.4%
−2.4%
−1.9%
−2.7%
−3.6%
2021
3.4%
−2.4%
−1.9%
−2.7%
−3.6%
2022
3.4%
−2.4%
−1.9%
−2.7%
−3.6%
2023
3.4%
−2.4%
−1.9%
−2.7%
−3.6%
This is the list of residuals for the top five services for the adult population based on
estimates of 2013 expenditures, and these services constituted 90 percent of total
estimated Medicaid expenditures for adults, as shown in table 10. (Prescription
drug expenditures do not include Medicaid prescription drug rebates.)
Table 12—FY 2013 Selected Service Expenditures for Adult Enrollees
(in billions)
Service
2013 Expenditures
Managed Care Organizations
$34.9
Inpatient Hospital
11.9
Outpatient Hospital
4.3
Prescription Drugs
3.8
Physician Services
3.1
Total Adults Expenditures
64.5

59
Table 13—Historical and Projected Price Factors and Unemployment Rates,
FY 2006–FY 2023
Fiscal
Year
Medical
consumer price
index
Consumer
price index
Home health
input price
index
Inpatient
price index
Wages
Unemployment
rate (CY)
Historical data:
2006
3.3%
3.7%
3.5%
3.7%
4.4%
4.6%
2007
3.5%
2.3%
3.4%
3.4%
4.6%
4.6%
2008
3.7%
4.4%
3.1%
3.3%
2.9%
5.8%
2009
3.3%
−0.3%
2.9%
3.6%
−0.4%
9.3%
2010
3.4%
1.7%
2.2%
2.1%
1.6%
9.6%
2011
3.1%
2.7%
2.1%
2.6%
2.9%
8.9%
2012
3.5%
2.0%
2.3%
3.0%
2.7%
8.1%
2013
2.8%
1.6%
2.3%
2.6%
1.9%
7.4%
Projections:
2014
2.4%
1.6%
2.3%
2.5%
3.2%
6.9%
2015
3.4%
1.9%
2.8%
2.7%
4.0%
6.7%
2016
3.8%
2.2%
3.3%
3.3%
4.2%
6.5%
2017
4.0%
2.4%
3.4%
3.7%
4.3%
6.2%
2018
4.2%
2.6%
3.5%
3.9%
4.3%
5.9%
2019
4.3%
2.7%
3.6%
4.0%
4.2%
5.8%
2020
4.3%
2.7%
3.5%
3.8%
4.0%
5.6%
2021
4.3%
2.7%
3.5%
3.8%
3.8%
5.6%
2022
4.3%
2.7%
3.4%
3.8%
3.6%
5.6%
2023
4.3%
2.7%
3.4%
3.8%
3.6%
5.6%

60
C. DATA POINTS FOR SELECTED FIGURES
The following tables provide the data points underlying selected figures in the
report.
Table 14—Past and Projected Medicaid Expenditures for Medical Assistance Payments,
by Type of Payment, FY 2000–FY 2023
(in billions)
Fiscal Year
Acute care
FFS
Long-term
care FFS
Capitation
payments &
premiums
Disproportionate
share hospital
payments
Historical data:
2000
$78.8
$67.9
$33.9
$14.4
2001
88.2
73.9
37.8
15.5
2002
103.2
81.1
44.7
15.4
2003
114.0
84.2
50.7
13.0
2004
124.0
87.3
52.7
15.4
2005
131.0
93.0
58.5
15.6
2006
118.5
97.6
65.4
13.7
2007
122.4
99.9
73.1
15.8
2008
125.6
105.5
82.8
15.4
2009
134.7
111.2
93.3
16.1
2010
142.4
113.0
103.9
15.1
2011
152.9
114.3
115.8
14.3
2012
137.5
114.4
132.4
14.1
2013
138.9
115.2
147.1
13.2
Projections:
2014
149.3
115.3
177.3
13.4
2015
149.9
118.1
201.1
13.6
2016
153.2
122.2
221.7
13.8
2017
159.7
127.0
245.7
12.1
2018
165.8
131.8
268.3
8.1
2019
172.2
136.9
291.5
8.4
2020
178.2
142.0
316.7
8.9
2021
184.0
147.3
344.1
9.2
2022
190.1
152.6
373.7
9.3
2023
196.6
158.0
406.2
9.8

61
Table 15—Past and Projected Numbers of Medicaid Enrollees, by Category,
FY 2000–FY 2023
(in millions of person-year equivalents)
Fiscal Year
Aged
Disabled
Children
Adults
Newly
eligible
adults
Territories
Historical data:
2000
3.6
6.7
16.4
6.9
n/a
0.9
2001
3.7
6.9
17.5
7.8
n/a
0.9
2002
3.9
7.2
19.4
9.0
n/a
1.0
2003
4.3
7.5
21.0
9.7
n/a
1.0
2004
4.4
7.7
21.9
10.1
n/a
1.0
2005
4.5
8.0
22.5
10.5
n/a
1.0
2006
4.5
8.2
22.6
10.4
n/a
1.0
2007
4.5
8.4
22.3
10.2
n/a
1.0
2008
4.6
8.8
22.8
10.6
n/a
1.0
2009
4.7
9.0
24.4
11.9
n/a
1.0
2010
4.8
9.3
26.4
13.1
n/a
1.0
2011
4.9
9.7
27.0
13.9
n/a
1.0
Projections:
2012
5.1
10.0
27.5
14.4
n/a
1.0
2013
5.3
10.1
27.9
14.7
n/a
1.0
2014
5.4
10.2
28.9
14.7
4.3
1.0
2015
5.6
10.2
29.6
15.0
7.4
1.0
2016
5.8
10.3
30.3
15.3
10.2
1.0
2017
5.9
10.4
30.7
15.5
11.3
1.0
2018
6.1
10.5
30.9
15.6
11.7
1.0
2019
6.3
10.6
31.1
15.7
11.8
1.0
2020
6.5
10.6
31.3
15.8
11.8
1.0
2021
6.7
10.7
31.5
15.8
11.9
1.0
2022
7.0
10.8
31.7
15.9
11.9
1.0
2023
7.2
10.8
31.9
15.9
12.0
1.0

62
Table 16—Past and Projected Medicaid Expenditures on Medical Assistance Payments
Per Enrollee, by Enrollment Category, FY 2000–FY 2023
(in dollars per person-year equivalent enrollee)
Fiscal Year
Aged
Disabled
Children
Adults
Newly
eligible
adults
Average
of all
enrollees
Historical data:
2000
$14,068
$12,156
$1,714
$2,797
n/a
$5,359
2001
14,817
13,022
1,831
2,879
n/a
5,545
2002
14,960
14,466
1,997
2,954
n/a
5,779
2003
14,585
14,982
2,036
3,081
n/a
5,833
2004
14,872
15,108
2,073
3,237
n/a
5,893
2005
15,513
15,921
2,137
3,356
n/a
5359
2006
14,863
15,490
2,276
3,436
n/a
6,136
2007
14,903
15,989
2,471
3,694
n/a
6,483
2008
15,576
16,290
2,537
3,893
n/a
6,703
2009
15,821
17,126
2,604
4,011
n/a
6,779
2010
15,481
17,504
2,593
4,054
n/a
6,684
2011
15,737
17,886
2,665
4,269
n/a
6,882
Projections:
2012
15,461
17,042
2,707
4,140
n/a
6,716
2013
15,483
17,352
2,807
4,391
n/a
6,897
2014
15,630
17,755
2,844
4,650
$5,517
6,921
2015
15,999
18,285
2,926
4,817
4,281
6,890
2016
16,626
18,927
3,002
4,964
3,606
6,885
2017
17,505
19,790
3,144
5,220
3,806
7,184
2018
18,296
20,682
3,307
5,504
3,989
7,535
2019
19,098
21,609
3,492
5,816
4,189
7,925
2020
19,946
22,573
3,685
6,152
4,403
8,340
2021
20,838
23,577
3,884
6,509
4,620
8,776
2022
21,784
24,630
4,099
6,889
4,843
9,240
2023
22,827
25,771
4,334
7,299
5,076
9,745

63
Table 17—Projected Medicaid Expenditures: Comparison of 2013 versus 2014 Actuarial Reports
on the Financial Outlook for Medicaid, FY 2000–2023
(in billions of dollars)
Fiscal Year
2014 Report
2013 Report
Historical data:
2000
$206.2
$206.2
2001
229.0
229.0
2002
258.2
258.2
2003
276.2
276.2
2004
296.3
296.3
2005
315.9
315.9
2006
315.1
315.1
2007
332.2
332.2
2008
351.9
351.9
2009
378.6
378.6
2010
401.5
401.5
2011
427.4
427.4
2012
431.0
431.0
2013
456.1
456.4
Projections:
2014
498.9
508.0
2015
529.0
544.4
2016
557.6
584.0
2017
592.3
623.2
2018
623.6
661.2
2019
661.1
704.2
2020
700.6
752.8
2021
742.3
801.8
2022
786.6
853.6
2023
835.0
n/a

64
Table 18—Past and Projected Medicaid Expenditures as Share of GDP, FY 1966–FY 2023,
Selected Years
(in billions of dollars)
Fiscal Year
Total
expenditures
Expenditures as
share of GDP
Historical data:
1966
$0.9
0.1%
1970
5.1
0.5%
1975
13.1
0.8%
1980
25.2
0.9%
1985
41.3
1.0%
1990
72.2
1.2%
1995
159.5
2.2%
2000
206.2
2.1%
2001
229.0
2.2%
2002
258.2
2.4%
2003
276.2
2.5%
2004
296.3
2.5%
2005
315.9
2.5%
2006
315.1
2.4%
2007
332.2
2.4%
2008
351.9
2.4%
2009
378.6
2.7%
2010
401.5
2.9%
2011
427.4
2.9%
2012
431.0
2.7%
2013
456.1
2.7%
Projections:
2014
498.9
2.9%
2015
529.0
2.9%
2016
557.6
2.9%
2017
592.3
2.9%
2018
623.6
2.9%
2019
661.1
3.0%
2020
700.6
3.0%
2021
742.3
3.0%
2022
786.6
3.1%
2023
835.0
3.1%
