
Main Menu Exit
United States
Office of Personnel Management
Medical Records
Technician Series
GS-0675
Nov 1991, TS-110
Workforce Compensation and Performance Service
Office of Performance and Compensation System Design
Classification Programs Division
July 1999, HRCD-7
Main Menu Exit
Medical Records Technician Series
GS-0675
CONTENTS
SERIES DEFINITION .......................................................1
EXCLUSIONS .............................................................1
OCCUPATIONAL INFORMATION ............................................2
TITLES ...................................................................5
EVALUATING POSITIONS ..................................................6
GRADE CONVERSION TABLE ...............................................6
FACTOR LEVEL DESCRIPTIONS .............................................7
FACTOR 1, KNOWLEDGE REQUIRED BY THE POSITION .....................7
FACTOR 2, SUPERVISORY CONTROLS ....................................9
FACTOR 3, GUIDELINES ................................................10
FACTOR 4, COMPLEXITY ...............................................11
FACTOR 5, SCOPE AND EFFECT .........................................12
FACTOR 6, PERSONAL CONTACTS
AND FACTOR 7, PURPOSE OF CONTACTS ..............................13
FACTOR 8, PHYSICAL DEMANDS ........................................14
FACTOR 9, WORK ENVIRONMENT .......................................14

Medical Records Technician, GS-0675 Page 1
Main Menu Exit
SERIES DEFINITION
This occupation includes positions involving technical work concerned with processing and
maintaining medical records for compliance with regulatory requirements. Included in this series
are positions that review, analyze, code, abstract, and compile or extract medical records data.
The work requires a practical knowledge of medical records procedures and references and the
organization and consistency of medical records. Positions also require a basic knowledge of
human anatomy, physiology, and medical terminology.
This standard replaces the Position Classification Standard for Medical Record Technician Series,
GS-675, issued in June 1971 (TS-6).
EXCLUSIONS
1. Classify positions that primarily involve application of statistical methods, procedures, and
techniques to the collection, processing, compilation, computation, analysis, editing, and
presentation of statistical data to the Statistical Assistant Series, GS-1531.
2. Classify positions the duties of which are primarily to compose or review correspondence for
the purpose of obtaining or supplying factual information when the work
requires skill in the composition of letters and memoranda to the Correspondence Clerk
Series, GS-0309.
3. Classify positions the duties of which are primarily to perform clerical work in support of the
care and treatment given to patients in a ward, in a clinic, or other such unit of a medical
facility to the Medical Clerk Series, GS-0679.
4. Classify positions the duties of which are primarily to advise on, administer, supervise, or
perform work involving the application of accepted theories and techniques of medical records
science in the development, maintenance, analysis, and use of diagnostic and therapeutic
medical records to the Medical Records Administration Series, GS-0669.
5. Classify positions that primarily involve operating or supervising the operation of keyboard
controlled machines to transcribe data or verify data in a form that can be used in automated
data processing systems to the Data Transcriber Series, GS-0356.
6. Classify positions that primarily involve supervising, verifying, or performing work coding
information from schedules, questionnaires, reports, documents, and other written source
material, according to codes involving numerical or alphabetical symbols to the Coding Series,
GS-0357.

Medical Records Technician, GS-0675 Page 2
Main Menu Exit
OCCUPATIONAL INFORMATION
Health care facilities maintain a permanent medical record that contains health care
information to support the diagnosis and justify treatment rendered on each patient. This record
includes the patient's medical history, physical examination results, X-ray and laboratory reports,
diagnosis and treatment plans, and orders and notes from doctors, nurses, and other health care
professionals. Accurate medical records are essential for clinical, legal, and fiscal purposes, for
correct and prompt diagnosis and treatment of illnesses and injuries, and for continuity of care.
Medical records also serve as a source of information for other uses. They provide background
and documentation for insurance claims, legal actions, professional review of prescribed
treatments and medications, and training of health professionals. Medical records provide useful
information for research and resource management planning purposes. They contain data for
clinical studies, evaluation of costs of various medical procedures, and assessment of health needs,
and justify the management costs associated with treatment.
Medical records clerks and technicians assemble, analyze, code, abstract, report, and maintain
medical records information in manual and automated records systems. They organize and check
medical records for completeness, accuracy, and compliance with regulatory requirements. When
assembling a patient's medical record, they first ensure the medical record is complete. With a
paper medical record, this means that all documentation is present in appropriate format and
sequence, identified, and signed. Employees assure that all documents reach the record before
coding is done. In a growing number of medical centers, the medical staff use computers rather
than the traditional paper record to note patient care information. In these hospitals, technicians
use their own computer terminals to retrieve information from the patient's record in the hospital's
central computer. A few medical centers are developing larger patient care information systems
using optical disks and satellite transmission of data from one facility to another.
Coding
Employees must apply a thorough knowledge of various medical and clinical processes such
as disease, illness, or injury and conditions (e.g., pregnancy, psychological) and their
interrelationships to code the record correctly. They abstract all the necessary information and
assign codes which most accurately describe each documented diagnosis, surgical procedure, and
special therapy or procedure according to established guidelines and practices. Where multiple
diagnoses and procedures are listed, they must relate each surgical procedure to the proper
diagnosis. They select and assign a principal code along with other appropriate codes.
Technicians must assure that the diagnosis responsible for the length of stay is appropriately
identified and that the secondary diagnoses are sequenced properly in order to assure maximum
allocation under the Diagnostic Related Groups (DRG's) System. Because information in the
medical record is the basis for reimbursement as well as clinical decision making, coding entries
must be complete and accurate. A coding error can mean a financial loss for the hospital because
the amount of reimbursement depends on the correct coding of diagnoses and procedures to
ensure the appropriate DRG's assignment.

Medical Records Technician, GS-0675 Page 3
Main Menu Exit
Quality Control and Utilization Review
As part of quality control or utilization review, technicians compile, abstract, and analyze data
from medical records. For example, they develop information to find trends which show
differences in the average length of a hospital stay according to diagnosis, attending physician,
procedures performed, and health care provided. They also retrieve, analyze, and present
information for the institution's quality assurance studies and patient care evaluation activities.
Registries
Technicians serve as registrars maintaining special registries. These registries show
occurrences of disease by type, such as cancer, injury, or stroke, extent of illness, and survival.
Technicians maintain health record indexes and compile administrative and health statistics for
public health officials, medical center management, planners, and others.
Correspondence
In response to inquiries from patients, their authorized representative, and other third parties,
such as law firms and insurance companies, government agencies and researchers, medical records
technicians determine the validity of each request and provide medico-legal information from
medical records. They determine eligibility for release of information, abstract information from
the medical record, obtain supplemental reports, write factual summaries, and complete forms for
services. Technicians follow established procedures to ensure the confidentiality of health
information.
Research and Special Projects
Technicians perform data retrieval for medical center management and clinical staff for
research, diagnostic, and teaching purposes. Working with the researcher, they determine what
information is needed for a particular project and how to compile it.
The day-to-day tasks of medical records technicians vary with the complexity and
characteristics of the facility. Affiliated treatment facilities house many critically ill patients and
use the latest treatment methods resulting in comprehensive medical records with many diagnoses
and treatments. The time and knowledge needed to analyze and code a record increases in
proportion to the patient's length of stay and the complexity of the patient's diagnosis and
treatment. The scope of the work performed by the medical records technician is increased when
there are many health care providers involved in the care of a single patient. Several physicians
may provide care to one patient, all of whom write progress notes and determine diagnoses and
treatments. Medical records technicians in facilities offering a greater number of specialties,
health care providers, and diagnostic and therapeutic services must have increased knowledge and
understanding of many health care processes. They must stay abreast of new procedures and
therapies so they can analyze and code the record.

Medical Records Technician, GS-0675 Page 4
Main Menu Exit
In most facilities, medical records administrators manage medical records activities, but in
some facilities an experienced medical records technician may head the department. In other
medical records departments, a technician is usually responsible for supervising and training
medical records clerks. Also, in some medical facilities, technicians specialize in a certain area.
For example, a medical records technician may analyze the record to be sure that all correct
documents are in the record and ready to code. Another technician then codes the record. In
some cases, the technician is responsible for only those records needed for legal issues and
correspondence. In facilities that employ fewer people, a medical records technician may be
responsible for everything from analysis and coding to providing help on legal issues.
Knowledge Required
Medical records technicians must have a knowledge of:
-- Medical terminology and usages, covering the full range of general medical, surgical,
pharmaceutical, hospital terms, medical abstracts, and abbreviations.
-- Physiology, major anatomical systems, and related disease processes.
-- Medical records forms and formats.
-- Correlation of laboratory test results, procedures, and treatments with diagnosis.
-- Medical records classification systems and references such as the International Classification
of Diseases (ICD), Diagnostic Related Groups (DRG's), Physician's Desk Reference (PDR),
Current Procedural Terminology (CPT), medical dictionaries, manuals, textbooks, and
glossaries.
-- Legal and regulatory requirements of medical records to be sure the record is acceptable as a
legal document.
-- Laws and regulations on the confidentiality of medical records (Privacy Act and Freedom of
Information Act) and the procedures for informed consent for release of information from the
record.
-- Computerized data entry and information processing systems.
-- Data collection methods for basic health care and research information.
Technician Versus Administrator Positions
Medical records administrators use broad medical records management knowledges, concepts,
and principles in the administrative management of medical records systems, programs, or

Medical Records Technician, GS-0675 Page 5
Main Menu Exit
specialty areas. Medical records technicians work in support of the specialist to achieve program
goals.
Both medical records administrators and medical records technicians review and analyze
records. The administrator performs analyses that go beyond the contents of individual patient
records to assess the effectiveness of the medical records program. The administrator analyzes
the medical data requirements of the program and develops effective methods to collect and use
this information on an institution-wide basis. The technician analyzes individual records for
completeness, use of accepted terminology, and for compliance with regulatory requirements.
Medical records administrators are responsible for planning and developing the patient
information system, including developing operating methods and procedures covering all medical
records functions which require an understanding of the interrelationship of record services with
the rest of the facility's services. They must also apply administrative and management theories,
principles, and techniques to many situations and programs.
Medical records technicians follow established methods and procedures which have been
developed by medical records administrators. They are primarily concerned with the application
of these guidelines to specific medical records operations. Medical records technicians are
proficient in a number of medical records functions such as analyzing records, coding information,
and abstracting information from records to answer correspondence.
TITLES
Medical Records Clerk is the title for nonsupervisory positions in grades GS-3 and GS-4.
Medical Records Technician is the title for nonsupervisory positions in grades GS-5 and
above.
Supervisory Medical Records Technician is the title for supervisory positions which meet the
criteria in the appropriate supervisory guide.
Lead Medical Records Technician is the title for positions which meet the criteria in the Work
Leader Evaluation Guide.

Medical Records Technician, GS-0675 Page 6
Main Menu Exit
EVALUATING POSITIONS
Evaluate positions using factor level descriptions and assigned point values in this standard.
For those few positions that may warrant factor levels above and below the levels provided in this
standard, refer to the FES Primary Standard or other related standards.
Evaluate positions which perform supervisory and program management work with the
criteria in this standard and the appropriate supervisory guide. When this approach produces two
different results, the proper grade is the higher of the two.
Evaluate work leader positions using the Work Leader Grade Evaluation Guide.
GRADE CONVERSION TABLE
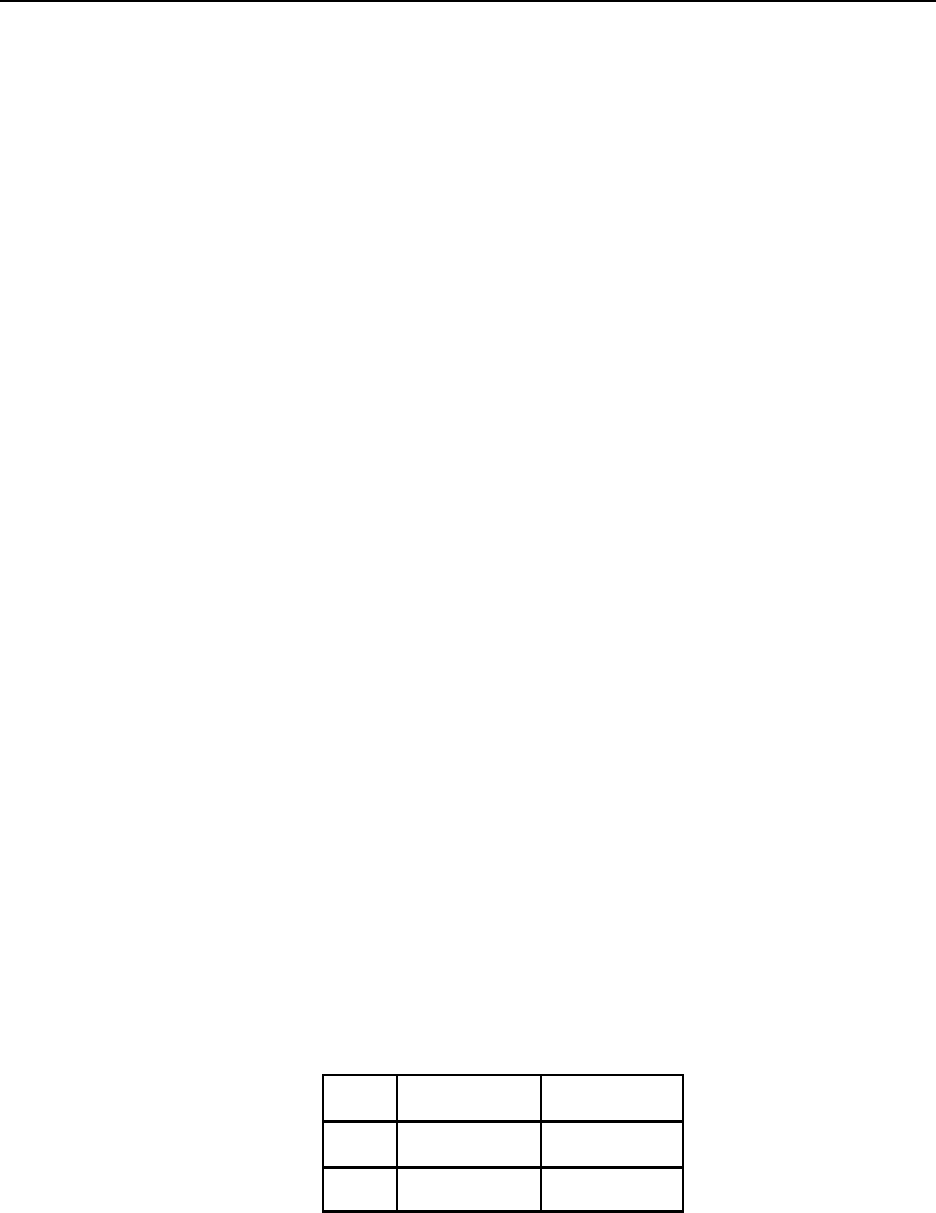
Total points on all evaluation factors are converted to GS grade as follows:
GS Grade Point Range
3
4
5
6
7
8
455-650
655-850
855-1100
1105-1350
1355-1600
1605-1850

Medical Records Technician, GS-0675 Page 7
Main Menu Exit
FACTOR LEVEL DESCRIPTIONS
FACTOR 1, KNOWLEDGE REQUIRED BY THE POSITION
Level 1-3 -- 350 Points
Knowledge of standardized medical records procedures, methods, and requirements to
perform a full range of routine medical records clerical assignments. Employees use a general
knowledge of the procedures, rules, operations, sequence of steps, documentation requirements,
time requirements, functions, and workflow to process medical records, to review records for
accuracy and completeness, and to keep track of processing deadlines. Employees use an
elementary understanding of human anatomy and physiology and a knowledge of medical
terminology to code records. This level requires basic knowledge of regulations on the
confidentiality of medical records.
Illustrations:
- Employees assemble medical records in proper sequence ensuring all necessary forms and
documents are present, accurate, and complete. They perform coding of diseases, surgical
procedures, and causes of injury using standard medical records references, i.e., DRG's.
- Employees compose responses to routine requests for release of patient information. They
select and compile information from medical records and prepare correspondence to insurance
companies and physicians concerning information from the medical record.
- Employees assemble and issue data collected by the tumor registry. They answer requests for
data and prepare routine and special reports which summarize cancer patient treatment
records. They collect core data from patients records, including demographic characteristics,
diagnostic procedures, diagnoses, stage and extent of disease, and treatment, as documented
by medical staff members. They code stage of disease using the International Classification of
Diseases for Oncology and carry out follow-up programs to gather information about the
quality and length of survival.
Level 1-4 -- 550 Points
In addition to the knowledges and skills at Level 1-3, positions require a practical knowledge
of well-established medical records procedures, regulations, and principles to carry out a variety
of medical records functions such as analysis, coding, quality assurance, and compiling data. In
addition, employees use--
-- elementary practical knowledge of the structure and physiology of major anatomical systems
and the major disease processes of each;

Medical Records Technician, GS-0675 Page 8
Main Menu Exit
-- knowledge of a broad range of medical records references and regulatory requirements for
medical records;
-- knowledge of classification systems to code diagnostic and operative/procedural information
using various classification methods; and
-- skill to collect and organize data for statistical reports.
Illustrations:
- Employees analyze the consistency of records that include references to several diseases, and
various medical, diagnostic, therapeutic, and surgical procedures. They identify
inconsistencies or discrepancies among medical documentation and discuss with appropriate
staff member. They code medical records by determining and sequencing codes to reflect the
resources used in the care of patients. They relate an operation to the proper diagnosis when
there are multiple diagnoses and select the most descriptive code when more than one
anatomical location is involved.
- Employees prepare correspondence and summaries of medical records in response to a variety
of requests. They review and screen requests to release medical information from records by
interpreting and applying the Privacy Act and corresponding local policies governing the
release of medical information or health records to individuals other than the patient.
- Employees assist in the technical evaluation of medical records for compliance with regulatory
requirements. They review patient medical records to gather information on the reasons for
admission and length of stay using special screening criteria. They refer utilization data to
quality assurance specialists for review and resolution and identify and code the stage and
extent of disease by using the ICD.
Level 1-5 -- 750 Points
Employees apply knowledge and skill as described in Level 1-4 and in addition, a thorough
knowledge of medical records activities, operations, and regulations to carry out limited
specialized assignments such as setting up special registries. Technicians aid in a wide range of
quality assurance studies, code complicated medical records, or make recommendations to
improve procedures for compiling and retrieving medical record information. Technicians apply
an extensive knowledge of regulatory requirements governing medical record operations to
provide problem-solving services in specific medical record functions and in research activities.
Illustrations:
- Employees assist in the performance of a variety of quality assurance studies. They --
-- review a specific area of a medical record department as part of a quality assurance team;

Medical Records Technician, GS-0675 Page 9
Main Menu Exit
-- identify problems and potential problems in record documentation; and
-- provide evidence that various functions within the section are in compliance with
requirements of regulatory agencies.
- Employees perform a wide range of technical duties involved in the development and analysis
of diagnostic and therapeutic cancer data. They coordinate activities for a facility's tumor
registry by --
-- setting up procedures within the framework established by higher level authority;
-- devising administrative procedures or processes to use in identifying diagnosed cases of
malignant disease through audits of medical record disease indices;
-- organizing and maintaining a data system which conforms to the standards of tumor
registry operations and meets the needs of the users of the registry data; and
-- maintaining quality control of case-finding, abstracting, coding, and follow-up procedures.
- Employees code complicated medical records having diagnostic, surgical, and therapeutic
procedures on specific DRG's that are identified as difficult to classify. They also use
specialized procedures and methods to correct and amend records.
- Employees assist clinical services staff in retrieving data for research, diagnostic, and teaching
purposes. They advise researchers of the data available and retrieve and compile specified
reports. They aid staff in research activities by offering guidance on the best approach to
gather data, and they compile requested data for special studies and research projects that
directly relate to the problem.
FACTOR 2, SUPERVISORY CONTROLS
Level 2-1 -- 25 Points
The supervisor or higher grade technician makes assignments and gives specific and detailed
instructions about tasks. The supervisor is readily available to provide additional guidance.
The employee performs the work as instructed, referring to the supervisor all problems not
specifically covered by instruction.
The supervisor maintains close control over the work by checking it in progress and reviewing
completed work for accuracy, adequacy, and adherence to instructions.
Level 2-2 -- 125 Points

Medical Records Technician, GS-0675 Page 10
Main Menu Exit
The supervisor provides continuing assignments showing generally what is to be done,
limitations, quality and quantity expected, deadlines, and priority of assignments. The supervisor
provides additional, specific instructions for new or difficult assignments including work methods
or advice on source materials available.
The employee carries out recurring assignments and refers deviations from established
procedures, unanticipated problems, or unfamiliar situations not covered by instructions to the
supervisor for a decision. The employee uses initiative in choosing the best method for carrying
out the work according to instructions, policies, or previous cases.
The supervisor assures that finished work and methods used are technically accurate and in
compliance with instructions or established procedures.
Level 2-3 -- 275 Points
The supervisor makes assignments by defining the overall goals and priorities of the work and
helps the technician with unusual situations which do not have clear precedents.
At this level, the technician plans and carries out assignments, and handles problems and
deviations in the work assignment using established policies, instructions, and accepted practices
in medical records management. The supervisor places considerable reliance upon the technician's
knowledge of medical records.
The supervisor reviews the work for results achieved, technical soundness, and conformity to
medical record policy and requirements.
FACTOR 3, GUIDELINES
Level 3-1 -- 25 Points
Specific and detailed guidelines and procedures such as procedural manuals, coding
references, operating guides, verbal instructions, and medical dictionaries cover the assignments.
The employee works in strict adherence to the guidelines referring deviations to the supervisor
for direction.
Level 3-2 -- 125 Points
There are well-established procedures for doing the work and other specific guidelines are
available including a variety of written medical record references and regulatory requirements.
The number and similarity of guidelines and work situations require the employee to use
judgment to identify and select the most appropriate guidelines, references, and procedures for

Medical Records Technician, GS-0675 Page 11
Main Menu Exit
application in making minor deviations to adapt the guidelines to specific cases. Employee refers
situations to which existing guidelines are not applicable to the supervisor.
Level 3-3 -- 275 Points
Guidelines are a variety of technical instructions, technical manuals, hospital regulations,
regulatory requirements, and established procedures governing medical records. These guides are
general in nature and do not cover all areas of the work performed by the medical record
technician, such as cases involving new diseases or treatments or experimental drugs.
The employee uses judgment to adapt and interpret guidelines for application to specific cases
or problems, using discretion and initiative in deciding on the appropriate course of action to
correct deficiencies and improve reliability of information in the records. This may require
developing approaches and work methods within the framework established by higher level
authority, devising procedures to use when applying new regulatory requirements, or adapting to
new computer technology.
FACTOR 4, COMPLEXITY
Level 4-1 -- 25 Points
Employee performs clear-cut, repetitive, and interrelated tasks, such as assembling the medical
record in proper sequence and checking the medical record to insure all necessary forms are
present.
The nature of the work provides little opportunity for employees to decide what is to be done.
The employee performs assignments with few variations and with little likelihood of
complications. Standard operating procedures and instructions directly apply.
Level 4-2 -- 75 Points
Assignments are to solve routine problems of limited complexity. The work consists of duties
involving related steps, processes, or methods such as compiling, recording, and reviewing
medical record data. There are established procedures for performing the work.
Decisions about what needs to be done involve various choices requiring the technician to
recognize the existence of and differences among a few easily recognizable alternatives. The
work includes such tasks as determining which code, from several choices, most accurately
describes the diagnosis and the surgery performed; relating the operation to the proper diagnosis
when multiple diagnoses are listed; determining the final diagnosis rather than an initial or
consultative diagnosis; and assigning the DRG's while staying within the regulatory framework.

Medical Records Technician, GS-0675 Page 12
Main Menu Exit
The technician corrects technical errors using prescribed methods and performs other checks
to be sure of the validity of information.
Level 4-3 -- 150 Points
The work includes the performance of different and varied medical record processes and
methods. The technician performs periodic reviews of the work and that of other employees in
compliance with the regulatory requirements.
Decisions about what needs to be done require the employee to determine the relevance of
many facts and conditions such as information within the record, legal and regulatory
requirements, and other variables. The chosen course of action may have to be selected from
many alternatives, for example, when standardized procedures are silent on an issue.
The work involves analyzing and interpreting conditions and elements to correct complicated
inconsistencies or discrepancies in the records.
FACTOR 5, SCOPE AND EFFECT
Level 5-1 -- 25 Points
The work involves performance of specific and routine duties that include a few separate tasks
or procedures such as compiling data, answering specific questions for which information is
readily available, filing, or retrieving records.
The work facilitates the work of others in the immediate work unit or aids medical records
personnel in the same organization.
Level 5-2 -- 75 Points
The work involves performance of assignments according to specific rules or procedures
which represent a significant segment of the medical record function. For example, the employee
analyzes medical records information to ensure compliance with procedural requirements, codes
diseases and operations, and compiles other medical information.
The work affects the accuracy, timeliness, reliability, and acceptability of information in the
medical record.
Level 5-3 -- 150 Points
Medical Records Technician, GS-0675 Page 13
Main Menu Exit
P
E
R
S
o
N
S
The work involves performance of a variety of specialized medical records tasks and resolving
problems according to established criteria. For example, the employee processes medical records
and data that involve inconsistencies, discrepancies, and other nonroutine problems.
The work typically has a direct effect on medical recordkeeping and a direct impact on the
accuracy, timeliness, and reliability of some medical record services.
FACTOR 6, PERSONAL CONTACTS
AND
FACTOR 7, PURPOSE OF CONTACTS
Match the level of assigned, recurring personal contacts with their purpose and credit the
appropriate point value using the chart below.
Persons Contacted
1. Contacts are with employees within the immediate organization or work unit and in related or
support units. Contacts with members of the general public take place in highly structured
situations where, for example, the purpose of the contact and the question of with whom to
deal are relatively clear.
2. Contacts are with employees in the same agency, but outside the immediate organization.
Contacts with members of the general public take place in a moderately structured setting.
For example, the contacts are generally established on a routine basis, usually at the
employee's work place; the exact purpose of the contact may be unclear at first to one or more
of the parties; and one or more of the parties may be uninformed concerning the role and
authority of other participant. Examples of contacts include representatives of state agencies,
court officials, and insurance companies.
Purpose
a. To exchange factual information.
b. To coordinate work efforts and solve technical problems.
P U R P O S E
a b
1 30 60
2 45 75

Medical Records Technician, GS-0675 Page 14
Main Menu Exit
FACTOR 8, PHYSICAL DEMANDS
Level 8-1 -- 5 Points
The work is primarily sedentary. The employee sits comfortably to do the work. However, there
may be some walking, standing, or carrying of light items such as manuals and files. The work
does not require special physical demands.
Level 8-2 -- 20 Points
The work requires physical exertion such as prolonged periods of standing, bending, reaching,
and lifting moderately heavy items such as record boxes.
FACTOR 9, WORK ENVIRONMENT
Level 9-1 -- 5 Points
The work environment involves everyday risks or discomforts which require normal safety
precautions typical of such places as medical facility offices. There is adequate light, heat, and
ventilation in the work area.
