
April 2022 REPORT 1
HP-2022-12
Addressing Social Determinants of Health:
Examples of Successful Evidence-Based Strategies
and Current Federal Efforts
Amelia Whitman, Nancy De Lew, Andre Chappel, Victoria Aysola, Rachael Zuckerman,
Benjamin D. Sommers
KEY POINTS
Long-standing health inequities and poor health outcomes remain a pressing policy challenge in
the U.S. Studies estimate that clinical care impacts only 20 percent of county-level variation in
health outcomes, while social determinants of health (SDOH) affect as much as 50 percent.
Within SDOH, socioeconomic factors such as poverty, employment, and education have the
largest impact on health outcomes.
SDOH include factors such as housing, food and nutrition, transportation, social and economic
mobility, education, and environmental conditions. Health-related social needs (HSRNs) refer to
an individual’s needs that might include affordable housing, healthy foods, or transportation. This
report provides select examples of the evidence in several of these areas.
Housing – Studies show strong evidence of the benefits for “housing first” interventions that
provide supportive housing to individuals with chronic health conditions (including behavioral
health conditions). Benefits include improved health outcomes and, in some cases, reduced
health care costs. In addition, interventions that reduce health and safety risks in homes, such as
lead paint or secondhand smoke, can also improve health outcomes and reduce costs.
Food and Nutrition – Efforts to improve food access through healthy food environments, public
benefit programs, health care systems, health insurers, and evidence-based nutrition standards
can lower health care costs and improve health outcomes.
Transportation – Enhanced built environment interventions including sidewalks, bicycle
infrastructure, and public transit infrastructure can make physical activity easier, safer, and more
accessible. Non-emergency medical transportation has been shown to be cost-effective by
increasing use of preventive and outpatient care and decreasing use of more expensive care.
Social and Economic Mobility – Multiple randomized trials show that cash payments to families
and income support for low-income individuals with disabilities are associated with better health
outcomes. Early childhood care and education are also associated with positive health outcomes.
Social Service Connections – Some studies of care management and coordination using multi-
disciplinary teams that support HRSNs show reduced total cost of care and improved health
outcomes, but the evidence overall on these effects is mixed.
Building on this evidence base, the U.S. Department of Health and Human Services is taking a
multifaceted approach to address SDOH across federal programs through timely and accessible
data, integration of public health, health care, and social services, and whole-of-government
collaborations, in order to advance health equity, improve health outcomes, and improve well-
being over the life course.
April
1, 2022

April 2022 REPORT 2
INTRODUCTION
Despite significant investments to improve access to high-quality health care, health inequities in the United
States persist by race, ethnicity, sexual orientation, gender identity, and disability, as well as by economic and
community level factors such as geographic location, poverty status, and employment. Black, Latino
*
,
American Indian and Alaska Native (AI/AN), Asian American, Native Hawaiian, and Pacific Islanders (AANHPI),
and LGBTQ+, individuals, people who live in rural areas, and people with disabilities fare worse than their
White, heterosexual, and urban counterparts and people without disabilities. These disparities exist for many
health outcomes, including infant and maternal mortality, heart disease, diabetes, hypertension, chronic
illness, disability, cancer, mental illness, substance use, and overall life expectancy.
1-10
While opportunities to advance health equity through clinical care continue to be important,
11
addressing the
ways in which social determinants of health (SDOH) increase or decrease the risk of poor health outcomes is
critical to improving the nation’s health and wellbeing. SDOH are the conditions where people are born, live,
learn, work, play, worship, and age that affect a wide range of health, functioning, and quality-of-life
outcomes.
12
When one or more of these conditions pose challenges, such conditions can become risk factors
for poor health outcomes. SDOH are fundamental social and structural factors that touch people’s lives and
impact their wellness and longevity. Health and wellness are shaped by and within overarching systems,
including structural racism, ableism, homophobia, and transphobia; and broad neighborhood and community
structures including physical safety, environmental quality, and occupation-related hazards. Educational
attainment, income, and the stress of financial hardship, along with discrimination due to nativity and racial or
ethnic origin, disability, sexual orientation, and gender identity, are key determinants that influence a variety
of more proximal factors (such as access to affordable housing) that impact the risk of morbidity, mortality,
and health throughout the life course.
Social and structural factors play a critical role in driving disparate health outcomes. One study estimated that,
on average, clinical care impacts only 20 percent of county-level variation in health outcomes, while SDOH
affect as much as 50 percent of health outcomes.
13
More specifically, socioeconomic factors alone may
account for 47 percent of health outcomes, while health behaviors, clinical care, and the physical environment
account for 34 percent, 16 percent, and 3 percent of health outcomes, respectively.
14
Moving from the county
level to the individual level, a given person’s physical health, behavioral health, and well-being are also
influenced by factors that are specific to the individual. At the individual level, we use the term health-related
social needs (HRSNs) to refer to an individual’s needs that might include affordable housing, healthy foods, or
transportation. An unequal distribution of SDOH is the root cause of HRSNs at the individual level. For
example, a particular community may lack abundant affordable housing, but local individuals may experience
housing needs differently. Distinguishing between SDOH and HRSNs is critical for developing measures,
evaluating data sources, assessing evidence and especially for formulating policy responses.
Figure 1, below, provides a pictorial representation of the SDOH and HRSNs ecosystem. The diagram includes
three segments depicting different points at which there are opportunities to address SDOH, with the river
representing the level of action and primary actors, and the banks representing the objectives and approaches
for each segment. Importantly, addressing structural racism and enhancing data infrastructure, noted in
boxes, are key factors for success. In the upstream segment are the underlying social and economic conditions
that create differences in SDOH. Interventions relevant to this segment apply at the community level and
attempt to address the root causes of socioeconomic and health inequities (such as poverty, employment, and
education). The midstream segment is human services (i.e., social service providers and community-based
organizations) that address individuals’ HRSNs in order to mitigate the effects of SDOH. The downstream
segment focuses on individual health care, which may refer or connect an individual to assistance for a social
_______________________
*
This brief uses the term “Latino” to refer to all individuals of Hispanic and Latino origin.
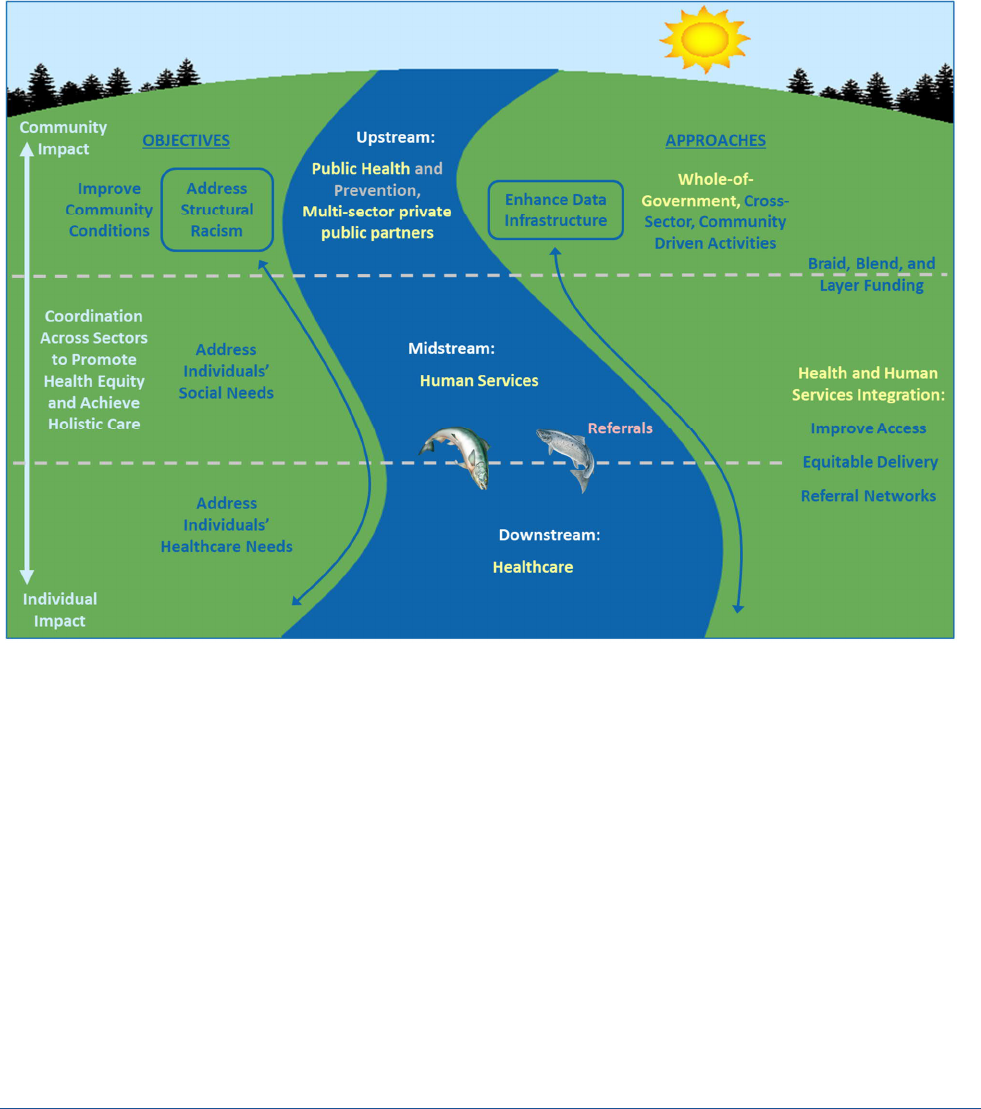
April 2022 REPORT 3
need. While the diagram indicates that human services and health care primarily address the needs of
individuals, the bi-directional arrows indicate the need for coordination across each of the three segments.
The Figure depicts the nation’s investment in health care spending as downstream of investments in
community conditions (including public health) and social services. While health care in the U.S. is by far the
most highly resourced sector of the three, improving health outcomes requires adequate support for all three
sectors. To develop comprehensive strategies and policies to address SDOH, it is important that those involved
in each of the three segments partner with each other to identify community-based approaches towards
addressing the underlying root causes of health disparities.
Figure 1. Social Determinants of Health Ecosystem
Note: Adapted from Castrucci B, Auerbach J. Meeting Individual Social Needs Falls Short of Addressing Social Determinants of Health.
Health Affairs Blog. January 16, 2019
This brief provides a high-level overview of select strategies to address SDOH and HRSNs that have
demonstrated success in reducing impediments to health and well-being, improving health outcomes, or
lowering health costs, as well as a discussion of some of the current HHS efforts to address SDOH and improve
the conditions that impact health and longevity among the American people. This brief surveys the evidence
on successful interventions designed to address SDOH and the HRSNs of people at various points in the
lifespan including infancy, childhood, adulthood, and older age; people who live in particular areas, such as
major cities or rural communities; and people with particular conditions such as asthma, HIV, and others. It
should be noted that interventions may improve health outcomes, utilization, or costs for one group but not
necessarily for other groups. In many cases, data on health outcomes are not available, so data on health care
utilization, costs, or healthy behaviors are presented as proxy measures. These may or may not represent
improved health and well-being and is therefore a critical limitation in evaluating impacts. As noted in the
conclusion, additional research is needed on the longer-term impacts of many of these interventions.
Conversely, even when interventions don’t improve utilization measures or lower health care costs, there may

April 2022 REPORT 4
be value in the intervention in the form of improved health outcomes, well-being, or long-term impacts not
included in the studies’ time horizon. A key prerequisite for both addressing health disparities related to SDOH
and HRSNs and measuring progress after intervention implementation is a more robust and interconnected
data infrastructure to support evidence-based policies and better identify improved outcomes associated with
such policies.
This brief is not intended as a comprehensive review of all of the evidence on SDOH and HRSNs. It highlights
only a few of the many interventions that have been evaluated and largely focuses on selected domains where
there is at least some evidence to suggest potential health effects. There is a rich literature on SDOH and
HRSNs, some of which is referenced throughout this paper, and several systematic reviews and resource
libraries survey the full landscape of this evidence base.
15-21
Important methodological challenges exist in assessing the effects of interventions for SDOH and HRSNs. At
the community level, randomized designs are rare and the evidence is often not sufficient to make causal
conclusions. In addition, many interventions focus on individuals who have experienced adverse outcomes,
such as a hospitalization, high health care costs, or other negative health or social events. In such cases,
simple pre-post assessments, without a control or comparison group, will often suffer from regression to the
mean – the phenomenon in which people experiencing higher-than-expected outcomes in one period (e.g.,
total health care spending) will typically experience closer-to-average results in the subsequent period simply
by chance. Other challenges include lack of comprehensive data for both health and social outcomes; lack of
large sample sizes, particularly for subgroup analyses; and differences in unmeasured characteristics between
those who participate in HRSN interventions and those who do not. In addition, methods for evaluating SDOH
and HRSNs are not static and research innovation continues to evolve to enhance our understanding of the
effects of intervening on SDOH and HRSNs. For these reasons, this brief, which provides a broad view of the
current state of the research, attempts to highlight whenever possible the study design and the relative
strength of the evidence, preferentially reporting results from randomized trials and natural experiments with
defined comparison groups. This brief also references several systematic reviews that use consistent,
transparent, and scientifically rigorous methods, which provide the opportunity to look across many studies at
once in order to understand what interventions work and under what conditions.
EVIDENCE REGARDING SELECTED SOCIAL DETERMINANTS
Safe and Stable Housing
Safe and stable housing has been associated with improved health and well-being. For example, housing
instability among families has been associated with fair or poor caregiver and child health, maternal depressive
symptoms, child lifetime hospitalizations, and household material hardships, such as food insecurity and
foregone care.
22
The Community Preventive Services Task Force (CPSTF), which provides guidance on available
scientific evidence about community-based health promotion and disease prevention interventions,
recommends tenant-based housing voucher programs to improve health and health-related outcomes.
23
Permanent supportive housing (PSH), a model which pairs affordable housing assistance with voluntary
supportive services,
*
has been shown to be effective in improving housing stability.
24,25
Existing evidence
reviews have also found strong evidence of the benefits of providing supportive housing to individuals with
chronic health conditions, including behavioral health conditions, with studies demonstrating reduced
_______________________
*
Services provided as part of PSH are designed to build independent living and tenancy skills and connect individuals to needed
services. These supportive services can include case management, mental health services, primary health services, substance abuse
treatment, employment services, and parenting skills. National Alliance to End Homelessness. Permanent Supportive Housing.
https://endhomelessness.org/ending-homelessness/solutions/permanent-supportive-housing/ and Corporation for Supportive
Housing. Understanding Supportive Housing. https://www.csh.org/toolkit/understanding-supportive-housing/

April 2022 REPORT 5
inpatient, emergency department (ED), and long-term care utilization, and in some cases improved health
outcomes or reduced overall costs.
26,27,28
Housing interventions for adults experiencing homelessness who have chronic illnesses (such as heart disease,
diabetes, renal failure, cirrhosis, asthma, and HIV) have been shown to reduce hospitalizations, hospital days,
and ED visits.
29
Individuals with HIV experiencing homelessness who received permanent housing with
intensive case management had better outcomes than those receiving typical discharge planning, including
higher one-year rates of survival with intact immunity and a higher percentage with undetectable viral loads
than the usual care group.
30
The study also found reduced utilization among high cost individuals. A 2012
study looking at individuals with chronic medical illnesses experiencing homelessness in Chicago found that
those who received a housing and case management intervention experienced 2.6 fewer hospitalized days, 1.2
fewer ED visits, 7.5 fewer days in residential substance use disorder (SUD) treatment, 9.8 fewer nursing home
days, and 3.8 more outpatient visits each year, compared to individuals who received usual care.
31
Evidence is more mixed regarding the impact of housing on total cost of care. However, in a systematic
review, the CPSTF found that the economic benefits of PSH with Housing First programs in the United States
exceed the cost of intervention, with a substantial portion of savings attributable to health care.
32
In the 2012
study discussed earlier, among Chicago patients with chronic medical illnesses experiencing homelessness,
those receiving a housing and case management intervention had an estimated annual cost savings of $6,307
compared to the control group, accounting for health care, legal, housing, and case management costs.
Another study in Los Angeles compared the average monthly cost savings for persons in supportive housing
based on various characteristics and found the highest cost savings among individuals with HIV/AIDS, mental
illness and/or SUD, and those who were 45 to 65 years old. Conversely, costs increased among individuals who
worked in the last three years, as the average monthly cost savings for public services did not offset the cost of
providing supportive housing.
33
Ensuring housing is safe also has positive health impacts. There is evidence that improving individual’s existing
housing via home improvements or modifications improves outcomes.
34-39
A study comparing children with
public insurance living in redeveloped public housing (distressed and dilapidated urban public housing rebuilt
into lower density, townhome-style communities), non-redeveloped public housing, and nonpublic housing
found that children living in non-redeveloped public housing were 39 percent more likely to have repeat visits
within one year for acute care services unrelated to their initial visit, while there was no difference between
those in redeveloped and nonpublic housing.
40
Fixing housing issues related to health impacts can also
improve outcomes. An intervention that provided dust mite covers, a professional house cleaning, and roach
bait and trays to households of children with asthma found that the intervention group had lower dust mite
levels and better functional severity scores compared to a delayed intervention group, though overall asthma
severity scores did not change.
41
Healthy home environment assessments, which use home visitors to assess
and remediate environmental health risks within the home, have also been shown to decrease use of urgent
care and improve health outcomes.
42
A review by the CPSTF found such interventions resulted in a median
reduction of 21 symptoms days per year and 0.57 asthma acute care visits per year among children and
adolescents.
43
Smoke-free housing policies can also improve health outcomes through reduced exposure to
secondhand smoke.
44
Further, an 2014 analysis of national state cost savings associated with prohibiting
smoking in subsidized housing estimated that such prohibitions in all US subsidized housing would result in
$310 million in annual cost savings from reductions in secondhand smoke-related health care.
45
In some cases, housing modifications have also been associated with health care cost savings. Community
Aging in Place, Advancing Better Living for Elders (CAPABLE), which provides home repair and modifications
relevant to individuals’ functional goals along with other efforts to improve their self-care ability and functional
goals, resulted in $867 less Medicaid spending per month in 2018, on average, for dual-eligible beneficiaries
over age 65 who experienced difficulties with at least one activity of daily living (ADL).
46
Another study found

April 2022 REPORT 6
that the CAPABALE intervention reduced ADL disabilities by 30 percent in five months.
47
Modifications like
those done by CAPABLE can support individuals with a disability in living safely at home.
48
Reducing lead
exposure in homes by eradicating lead paint hazards from older homes and removing lead drinking water
service lines have also demonstrated health savings and benefits in health (measured via quality-adjusted life
years, QALYs). A 2019 analysis estimated that eradicating lead paint hazards from older homes of children
from low-income families would provide $3.5 billion in future benefits, including $60 million in health savings
and $110 million in health benefits, while removing lead service lines would result in $10 million in health
savings and $30 million in health benefits.
49
Nutrition and Food Access
Having healthy food available and affordable in food retail and food service settings allows people to make
healthier food choices. When healthy foods are not available, people may settle for foods that are higher in
calories and lower in nutritional value. Many strategies can contribute to healthy food environments,
including applying nutrition standards in childcare facilities, schools, hospitals, and worksites; providing
incentives for supermarkets or farmers’ markets to establish their businesses in underserved areas; and having
nutrition information and caloric content on restaurant and fast-food menus.
50,51
School-based interventions that combine meal or fruit and vegetable snack interventions with physical activity
interventions for elementary school students (through grade 6) increase students’ physical activity, modestly
increase their fruit and vegetable consumption, and decrease the prevalence of overweight and obesity.
52
Intervention approaches reviewed and recommended by the CPSTF to promote good nutrition include
community-based digital health and telephone interventions to increase healthy eating and physical activity;
digital health and telephone interventions to increase healthy eating and physical activity among students at
institutions of higher education; gardening interventions to increase vegetable consumption among children;
home-delivered and congregate meal services for older adults; and worksite digital health and telephone
interventions to increase healthy eating and physical activity.
53
For example, their review of community-based
digital health and telephone interventions to increase healthy eating and physical activity found that these
interventions resulted in a median 1.12 percent weight reduction, 10.25 milligrams/deciliter triglycerides
reduction, 4.00 milligrams/deciliter total cholesterol reduction, and 1.00 mmHg diastolic blood pressure
reduction.
54
Public benefit programs providing food assistance have been associated with lower health care costs, lower
health care utilization, and improve health outcomes.
55,56
However, it should be noted that most studies on
the impacts of such programs compare individuals who have enrolled in a given program versus those who
have not, and are subject to confounding due to differences between such individuals, which prevents drawing
any conclusions on cause and effect. A 2017 study of low-income adults participating in the Supplemental
Nutrition Assistance Program (SNAP) found an association between SNAP participation and lower health care
expenditures, with approximately $1,400 lower expenditures per year among SNAP participants.
57
A 2018
study found 5.8 percent lower expenses among older adult SNAP participants who were hospitalized as
compared to hospitalized older adults without SNAP, as well as 1 percent lower odds of hospitalization for
each $10 increase in SNAP monthly benefit amounts among individuals dually eligible for Medicare and
Medicaid.
58
The Special Supplemental Nutrition Program for Women, Infants, and Children (WIC) also has
been associated with improved maternal and child health outcomes, including reduced likelihood of preterm
births, lower odds of mortality within the first year, and reductions in disparities in low birthweight, extended
infant hospitalizations, and NICU outcomes, though with similar methodological limitations.
59,60,61
In addition,
an analysis of the National Health Interview Study found that respondents who participated in WIC were less
likely to forego or delay filling a prescription, skip medication doses, or take less medication than prescribed
due to costs.
62
The Older Americans Act (OAA) funded nutrition services is also associated with reduced health
care utilization and improved health outcomes for older adults. A study of OAA funded nutrition services

April 2022 REPORT 7
found that lower-income older adults who participated in the congregate meal program were significantly less
food insecure than nonparticipants, and 61 percent of home-delivered meal participants and 42 percent of
congregate meal participants indicated they would skip meals or eat less if the program was not available.
63
Individuals receiving home-delivered meals had greater improvements in anxiety and self-rated health, and
reduced rates of hospitalizations and falls compared with individuals on waiting lists.
64
Efforts to increase access to food via food pharmacies (pharmacies, health care clinics, or hospitals that store
and dispense healthy food
65
), food prescription programs (prescriptions from doctors for healthy foods that
can be used to subsidize the purchase of these items through community partners
66
), and home-delivered
meals, which are often funded through health care systems or health insurance, have been associated with
lowering health care costs and health care utilization.
67,68
Beginning in January 2016, a Geisinger Health
Systems hospital offered diabetic patients prescriptions for five days of breakfast and dinner ingredients per
week at their Fresh Food Farmacy, along with other supportive services. HbA1c levels (which indicate the level
of sugar in an individual’s blood) decreased by 20 percent among participants and Geisinger estimated that
every percentage point decline in HbA1c levels saved approximately $8,000 in health care costs, compared to
an annual investment in the program of $1,000 per patient per year; notably, however, this study did not
include a comparison group.
69,70
Similarly, health clinic produce prescription programs that provide funds to
purchase fresh produce from farmer’s markets have also found significant improvements in health outcomes,
including lower body mass indices (BMIs) among participants and improved glucose control among diabetic
participants, as well as improved patient-provider relationships.
71,72
Another intervention that has been shown
to improve outcomes is home-delivered meals. The provision of three free, nutritionally balanced meals,
seven days a week, to Medicaid beneficiaries in Philadelphia and southern New Jersey found a significant
decrease in total health care spending, fewer inpatient visits with shorter length of stays, and a greater
number of discharges home rather than to acute care facilities, compared to a similar group of Medicaid
beneficiaries who did not receive these services.
73
Another study found that, as compared to matched
nonparticipants, beneficiaries dually eligible for Medicare and Medicaid participating in a food delivery
program had fewer emergency department visits and lower medical spending.
74
Transportation
Transportation systems help ensure that people can reach everyday destinations, such as jobs, schools, healthy
food outlets and health care facilities, safely and reliably.
75
Transportation issues impact individuals’ ability to
obtain needed medical care, with 3.6 million people in the U.S. missing medical services due to transportation
issues annually.
76
Transportation barriers to accessing medical care are complex and include transportation
infrastructure, transportation costs, vehicle access, distance and time burden, and transportation policy.
77
Non-emergency medical transportation (NEMT) is one way to address some of these issues, including
transportation cost and vehicle access. NEMT has been shown to be cost-effective by increasing preventive
and outpatient care and decreasing more expensive care.
78
In a 2008 survey of Medicaid beneficiaries in New
Jersey, Louisiana, and Michigan receiving dialysis, SUD treatment, or diabetic wound care who used NEMT to
attend medical appointments, 58 percent of respondents indicated that they would make none of their
treatment appointments if NEMT were not provided.
79
Based on the results of this survey, study authors
estimated that per respondent, per month, Medicaid avoided $3,423 in costs for dialysis patients and $792 in
costs for wound care patients based on appointments that would likely be missed if not for NEMT, but did not
save on SUD treatments, as NEMT costs more than the additional medical costs from missed SUD treatments.
Another study comparing the costs and benefits of providing NEMT to individuals who lack access to
transportation found that for all 12 of the medical conditions analyzed, providing additional NEMT was cost-
effective, and it was cost-saving for four conditions (prenatal care, asthma, congestive heart failure, and
diabetes).
80
Cost-effectiveness was determined by establishing cost estimates for the provision of NEMT and
comparing the per capita cost of care for well-managed patients and poorly-managed patients for each
condition, accounting for additional factors such as QALYs. While NEMT is provided as a standard Medicaid

April 2022 REPORT 8
benefit, as of February 2022, four states have demonstration programs that waive provision of these
benefits.
81
Increasing access to safe, equitable public transportation infrastructure can also help address some of the
transportation barriers to accessing medical care and is also associated with positive health behaviors and
other positive health impacts. Public transportation is safer than travel in passenger vehicles, with motor
vehicle crashes being the leading cause of death for people ages 1-34.
82,83
In addition, air pollution from motor
vehicles contributes to adverse respiratory and cardiovascular health effects.
84
Public transportation is also
associated with increased access to health care and healthy food as well as improvements in mental health
and physical activity levels.
85,86
A study comparing train commuters to car commuters found that train
computers walked an average of 30 percent more steps per day and were four times more likely to walk
10,000 steps per day.
87
Similarly, a systematic review found an additional 8-33 minutes of walking per day
attributable to public transportation use.
88
However, given the disparities in traffic-related pedestrian death
rates, it is important that safe walking routes are included in efforts to support public transportation
infrastructure.
89
Further, a review from the CPSTF found that built environment strategies that combined one
or more interventions to improve pedestrian or bicycle transportation systems with one or more land use and
environmental design interventions increased physical activity.
90
Social and Economic Mobility
Social and economic factors such as socioeconomic status, income levels, poverty, and educational attainment
are fundamental drivers of poor health outcomes because they facilitate or impede access to important
resources that affect health outcomes directly and through multiple mechanisms.
91
In a study of societal
health burden and life expectancy, social and economic factors accounted for two of the three largest impacts
on health and life expectancy. Experiencing poverty or near poverty (living at incomes below 200 percent of
the federal poverty level) imposed the greatest burden and lowered quality-adjusted life expectancy more
than any other risk factor, with 8.2 QALYs lost per person exposed over his or her lifetime.
92
Poverty limits
opportunities and access to resources conducive to healthy behaviors, affects the physical “built”
environment, and limits service availability within communities, all of which have independent effects on
health outcomes.
93,94
Further, the cumulative effect of poverty over the life course also matters. For example,
the greater the number of years a child spends living in poverty, the more elevated the child’s cortisol levels
and the more dysregulated the child’s cardiovascular response to acute stressors.
95
These changes may impact
children’s cognitive development and chronic disease development, with larger exposures increasing the risk
of adverse outcomes later in life.
96
Cash transfers aimed at increasing income and reducing poverty can be particularly impactful for improving
health outcomes.
97
A recent meta-analysis examining health effects of randomized social experiments in the
United States identified seven cash-transfer interventions and found that they were associated with
improvement in self-rated health, though not with smoking status or obesity.
98
For example, the Stockton
Economic Empowerment Demonstration, a universal basic income experiment in Stockton, CA, gave randomly
selected residents $500 per month for two years with no strings attached, which measurably improved
participants' overall well-being and physical and emotional health.
99
Another income maintenance experiment
in Gary, IN, found that supplemental income provided to mothers was associated with higher birth weights for
their children in the absence of any health intervention, with the supplemental income linked to greater
changes in birth weight than tobacco use or race.
100
In addition, a study of low-income American Indian
children in families that received an annually increasing supplemental case income benefit found that by the
fourth year of the program, formerly poorly resourced children’s level of psychiatric symptoms was
comparable to those of children who were never poor.
101

April 2022 REPORT 9
Tax credits and supplemental income support for low-income individuals with disabilities also reduce poverty
and are associated with better health, including improved birth outcomes, maternal mental health, and
perceptions of health.
102,103
By reducing poverty and increasing income for working families, the Earned
Income Tax Credit (EITC) has been linked to positive health outcomes, particularly for infants and
mothers.
104,105
The EITC has led to improvements in infant health, including overall increases in birth weight
and reductions in low birth weight rates.
106,107
A study of the association between the EITC and health
outcomes found that compared to similar households that were not eligible for the credit, families eligible for
the credit were more likely to have all of their children covered by health insurance.
108
The same study also
found that infant mortality was lower in states with greater EITC penetration. The magnitude of this
relationship was strong: each 10-percentage point increase in EITC penetration (within or between states) was
associated with a 23.2 per 100 000 reduction in infant mortality rate (P = 0.013). Studies also show greater
health improvements when larger, more generous EITC benefits are available.
109
Supplemental Social Security
Income has also been associated with health improvements. A quasi-experimental study on Supplemental
Social Security Income (SSI) that examined within-state changes to maximum SSI benefits found that an
increase of $100 per month in the maximum benefit reduced mobility limitations among older adults.
110
In addition to programs providing economic support, educational supports such as high-quality preschool
programs also have been shown in studies to improve health outcomes.
111
Early childhood education is
associated with improved child development and can serve as a protective factor against future disease and
disability.
112
A review of research on early childhood education programs found that model programs, such as
Abecedarian, the Perry Preschool Project, and the Infant Health and Development Program, improved health
and health behaviors, including reduced smoking, improved cardiovascular health, and improved metabolic
health among participants in adulthood, compared to controls.
113
The review also found that such programs,
as well as Head Start, a federally-funded nationwide preschool program for low-income families, were
associated with reductions in depression and disabilities in adolescence and early adulthood.
Social Service Connections
In studies of programs that use multiple types of providers, such as social workers, nurses, physicians, and case
managers, to offer services that coordinate care across provider types and assist individuals with managing
their health care conditions and HRSNs some studies have found reductions in total health care spending and
health care utilization, and improved health outcomes, while in other cases results have been mixed.
114,115
Health Homes, which provide comprehensive care management, care coordination, health promotion, patient
and family support, and referral to community and social support services to individuals with multiple chronic
conditions or a serious mental illness, have been associated with improvements in linkages to SDOH-related
services, reduced ED utilization and inpatient admissions, and improvements in performance on process of
care measures among the first 11 states to launch the program.
116
Other models that provide linkages to social services and supports have been successful as well. However,
several evaluations have noted the need to do more than refer individuals to social services and supports. For
example, an evaluation of the Centers for Medicare & Medicaid Services Accountable Health Communities
model, which connects beneficiaries to community resources, found that only 14 percent of beneficiaries
referred to social service navigation had their needs resolved, while 33 percent were lost to follow up, 4
percent were connected to resources but their needs were unmet, 10 percent opted out after accepting
navigation, and 8 percent of needs could not be met.
117
Evidence suggests when partnerships are coordinated and well-funded, they are more likely to be successful.
WellCare Health Plans, Inc., a national managed care health plan that primarily serves patients in Medicaid,
Medicare, or dually eligible for both programs, in 2011 launched WellCare “CommUnity” Health Investment
Program, which included grants to social service providers and referred members and non-members to the

April 2022 REPORT 10
funded partners. Patients for whom a social barrier had been removed as a result of a referral to WellCare
CommUnity partners were more likely to have a better BMI, a better medication assessment score, and to
schedule and go to their annual primary care visit than patients without an intervention or referral.
118
Further,
as of 2017, these services provided through WellCare CommUnity partners generated $3,200 in per member
per year savings, including $3.47 health care savings for every $1 invested in the program. In addition, studies
have found improved outcomes when health systems partner with community-based organizations (CBOs) to
provide social services. For example, one study concluded that Accountable Care Organizations (ACOs) were
more likely to succeed in integrating SDOH when they implemented networking initiatives that connect them
to CBOs.
119
Another study found that hospitals in Hospital Service Areas that performed well on ambulatory
care-related hospitalizations, readmission rates, and average reimbursements per Medicare beneficiary had
deeper and more consistent collaboration with CBOs that provided social services.
120
Similarly, partnerships
between hospitals and Area Agencies on Aging (AAA), which coordinate and offer services such as case
management, home-delivered meals, and transportation that help older adults who desire to remain in their
homes were associated with a $136 reduction in average annual Medicare spending per beneficiary between
2008 and 2013, as well as a significant reduction in hospital readmissions within a year.
121,122
Studies looking at the use of Community Health Workers (CHWs, frontline public health workers who are
trusted members of a community and have a close understanding of the community in which they are
serving
123
) to connect individuals to health or social supports have found reductions in Medicaid spending and
utilization of ED visits and an increase in use of ambulatory care.
124
For example, a randomized trial of adults
participating in ACOs found that individuals with contact with a CHW were less likely to experience a hospital
readmission within 30 days of discharge.
125
Among women with depression, women enrolled in a CHW
intervention had a reduction in the frequency of high-cost encounters and lower average total charge
amounts, compared to women enrolled in an enhanced screening and referral control group.
126
ILLUSTRATIVE EXAMPLES OF ACTIONS HHS IS TAKING TO ADDRESS SDOH
There are many efforts underway across HHS to address SDOH and HRSNs, several of which are highlighted
below. Table 1 shows illustrative examples of the relationship between the HHS agency initiatives described
below and the evidence base described in the preceding section. While many of these initiatives are in
progress and do not yet have completed evaluations at this time, in many cases, agencies are planning to
conduct evaluations of the programs discussed in order to document the programs’ successes, challenges, and
opportunities for improvement.
Table 1: Selected Evidence-Based Interventions Used In HHS Agencies: Illustrative Examples
*
AGENCY CMS HRSA CDC ACL ACF SAMHSA
Housing Related Services X X X X X
Home Modifications and
Improvements
X X X X
Food Access X X X X
Non-Emergency Medical
Transportation
X X X
Public Transportation X X
Case Management & Social
Service Connection
X X X X
Community Health Workers
X
X
X
X
Social and
Economic Mobility
X
X
Note: This table is not an exhaustive list of HHS activities in these areas and also does not necessarily reflect specific
funding or designated programs in each area.
_______________________
*
Agencies included may have additional programs that support evidence-based interventions listed on this table.

April 2022 REPORT 11
Centers for Medicare & Medicaid Services
Medicaid: Though Medicaid rules limit spending on non-medical services, nearly all states have implemented
at least some policies or initiatives to address HRSNs through their Medicaid programs for various populations.
In January 2021, the Centers for Medicare & Medicaid Services (CMS) issued a State Health Official letter
identifying opportunities for states to better address SDOH under Medicaid and CHIP and to support states
with improving outcomes and lowering costs by addressing SDOH. Using a variety of mechanisms, including
using section 1905(a) State Plan Authority, Home and Community Based Services (HCBS), section 1115
demonstrations, section 1945 Health, and managed care contract requirements, among others, states are
addressing HRSNs, including housing-related services and supports, non-medical transportation, home-
delivered meals, educational services, employment, community integration and social supports, and case
management.
127
Section 1905(a) State Plan Authority: States have used Section 1905(a) to establish peer supports and
case management services, which are then used to link beneficiaries to HRSN supports. As of 2018, 19
states indicated that case management is a covered benefit in their program, and 36 indicated that
targeted case management is a covered benefit (though this benefit may be provided under section
1915(g)
*
).
128,129
Home and Community Based Services (HCBS): Several states have utilized HCBS to implement
housing-related services, including 46 states with section 1915(c) waivers;
†
four states with section
1915(i) benefits; and eight states with section 1915(k) benefits as of 2021.
130,131
For example,
Minnesota is using section1915(i) state plan authority to provide housing stabilization services to
certain individuals that are experiencing homelessness or are at risk of becoming homeless.
132
In their
first year, the state reported that they served 7,203 individuals.
Section 1115 Demonstrations: As of 2021, 25 states have utilized the flexibility provided by section
1115 demonstrations
‡
to address HRSNs, such as housing-related services, nutrition, transportation,
and interpersonal violence.
133
For example, CMS recently approved an 1115 waiver for California’s
Medicaid program (Medi-Cal) to launch California Advancing and Innovating Medi-Cal (CalAIM), which
seeks to integrate the Medi-Cal program with other social services through a “no wrong door”
approach that couples clinical care with Medicaid reimbursable nonmedical services, including housing
supports, medical respite, personal care, medically tailored meals, and peer supports.
134
However, as
of February 2022, four states have also used section 1115 demonstrations to waive NEMT, a benefit
that is typically required.
135
Section 1945 Health Homes: As of April 2021, there are 37 Health Home models across 21 states and
the District of Columbia, all of which must include comprehensive case management, individual and
family support, and referrals to community and social services, among other required services.
136
Managed Care Programs: As of 2018, 37 states have implemented requirements in their managed care
contracts related to HRSN and SDOH.
137
These requirements include:
o Relationships with social service providers (31 states);
_______________________
*
Section 1915(g) enables plans to provide case management services under Medicaid.
†
Section 1915(c) waivers allow states to pay for housing transition and tenancy services for beneficiaries to individuals meeting an
institutional level of care; Section 1915(i) benefits allow states to offer housing-related services for individuals who do not necessarily
meet an institutional level of care; Section 1915(k) benefits allow states to pay for services and supports identified as part of a person-
centered care plan, which can include home modifications or transition costs for moving an individual from an institution to a home or
community-based setting.
‡
Section 1115 demonstrations allow states to implement experimental, pilot, or demonstration projects that are likely to assist in
promoting the objectives of the Medicaid program.

April 2022 REPORT 12
o Inclusion of SDOH in care coordination (24 states);
o Social determinant screening (24 states);
o Dedicated staff for SDOH (17 states);
o SDOH quality performance measures (11 states);
o Provider training on SDOH (10 states);
o Collection and reporting on SDOH information (7 states);
o Value-added services related to SDOH (7 states);
o Member education on SDOH (5 states); and
o Social determinant expenditure requirements or incentives (3 states).
138
In addition to state flexibilities to address SDOH and HRSNs, CMS is partnering with the U.S. Department of
Agriculture to connect people enrolled in food assistance programs, such as SNAP, with Medicaid and vice
versa.
139
This partnership aims to improve participation rates and drive progress on both health and food
security.
Center for Medicare and Medicaid Innovation (CMMI): CMMI established the Accountable Health
Communities (AHC) Model in 28 locations to promote clinical-community collaboration to address HRSNs of
Medicare and Medicaid beneficiaries through screening, referral, and community navigation services.
140
The
model, which focuses on five core HRSNs of housing instability, food insecurity, transportation problems, utility
difficulties, and interpersonal violence, found that 15 percent of the nearly 483,000 beneficiaries screened
were eligible for navigation services, and more than half of these navigation-eligible beneficiaries reported
more than one core HRSN.
141
CMMI is working to incorporate learnings from the AHC model into future
models. As part of their Strategy Refresh, CMMI will require all new models to collect and report on data on
HRSNs and SDOH, as appropriate.
142
In addition, CMS will consider models that aim to address upstream,
community-level SDOH.
Medicare: CMS is also working to address HRSNs and SDOH in the Medicare program. As of 2019, CMS
expanded the definition of supplemental benefits in Medicare Advantage (MA) plans to better address
SDOH.
143
As of 2019, MA plans can offer a broader array of benefits that are primarily health-related, such as
transportation, meal delivery, and adult day care, and as of 2020, plans can offer non-primarily health-related
benefits to the chronically ill, such as pest control.
144
In addition, Medicare ACOs provide high-quality care to
Medicare beneficiaries to ensure that patients get the right care at the right time through care coordination.
In FY22, CMS also included a request for information in the final Hospital Inpatient Prospective Payment
System (IPPS) and Long-Term Care Hospital (LTCH) rule that sought ideas to make reporting of health
disparities based on social risk factors and race and ethnicity more comprehensive and actionable. Inclusion of
such measures in future payment rules would also build on the work of the CMMI AHC model.
145
Health Resources & Services Administration
Health Resources & Services Administration (HRSA) provides cooperative agreement funding for a number of
initiatives to support training and technical assistance for community health centers on topics related to SDOH
and HRSNs, including the Corporation for Supportive Housing (CSH) and the National Center for Medical-Legal
Partnerships.
146,147
CSH provides no-cost training and technical assistance to health centers that serve
individuals experiencing homelessness and/or operate Health Care for the Homeless programs. This assistance
provides health centers with strategies for improving health care access, housing stability, and health
outcomes for these patients.
148
The National Center for Medical-Legal Partnerships provides training and

April 2022 REPORT 13
technical assistance to health centers on implementing medical-legal partnerships. These partnerships bring
together legal professionals and health care teams to detect, address, and prevent social conditions negatively
impacting individual and community health. HRSA-funded health centers also play an important role in
improving HRSNs through the provision of enabling services, such as transportation, community health
workers, and other nonclinical services that enable people’s access to health care.
149
An important part of HHS’s strategic approach to addressing SDOH and HRSNs is to enhance data
infrastructure and how data is used. Aligned with this goal, as part of their Uniform Data System (UDS)
Modernization Initiative, HRSA began collecting SDOH data in 2020 and will gather patient-level data starting
in 2023, which will permit a better understanding of the impact of SDOH on clinical outcomes in health center
populations.
Centers for Disease Control and Prevention
The Centers for Disease Control and Prevention (CDC) seeks to protect public health through preparedness,
disease prevention, and health promotion. The focus of public health is on the health, safety, and well-being
of entire populations, and strives to provide the maximum benefit for the largest number of people.
150
Through their focus on public health, CDC’s data, research and programs address SDOH and HRSNs in a
number of ways.
Within the National Center for Chronic Disease Prevention and Health Promotion, numerous programs focus
on SDOH and HRSNs. For example, for over 20 years, CDC’s Racial and Ethnic Approaches to Community
Health (REACH) grants have funded locally-based, culturally-tailored solutions to addressing health inequities,
many of which are focused on SDOH.
151
Between 2014 and 2018, REACH provided better access to healthy
foods and beverages to over 2.9 million people, more opportunities to be physically active to approximately
1.4 million people, and access to local chronic disease programs linked to clinics for over 830,000 people.
152
In
2021, CDC also launched the Closing the Gap with Social Determinants of Health Accelerator Plans pilot project
that funds 20 state, local, tribal, or territorial jurisdictions to develop action plans including evidence-based
strategies to prevent and reduce chronic diseases among people experiencing health disparities.
153
In addition,
the Good Health and Wellness in Indian Country (GHWIC), CDC’s largest investment to improve American
Indian/Alaskan Native tribal health, focuses on improving nutrition, physical activity, and breastfeeding,
reducing commercial tobacco use and exposure, and strengthening links between community programs and
access to clinical services in order to promote health and prevent chronic disease.
Safe, stable, nurturing relationships and environments are essential to children’s health and wellbeing. In
addition to reductions in chronic health conditions, preventing adverse childhood experiences (ACEs) may also
lead to reductions in socioeconomic challenges.
154
CDC’s comprehensive approach to preventing ACEs uses
multiple strategies derived from the best available evidence.
CDC’s Stopping Elderly Accidents, Deaths & Injuries (STEADI) initiative, offers tools for health care providers to
screen older patients for fall risk.
155
Components of STEADI include home modifications such as mounting grab
bars near toilets and installing carpet on all surfaces that may get wet, coupled with referral to effective
community-based fall prevention programs.
In August 2021, CDC launched the Community Health Workers for COVID Response and Resilient Communities
initiative to put additional trained CHWs in communities with high rates of COVID-19 and long-standing health
disparities related to race, income, geographic location, or other sociodemographic characteristics.
156
These
CHWs will help build and strengthen community resilience to fight COVID-19 by addressing health disparities.

April 2022 REPORT 14
The Health Impact in 5 Years (HI-5) initiative highlights non-clinical, community-wide approaches that have
evidence for reporting positive health impacts within five years.
157
The 14 evidence-based community-wide
population health interventions included in this initiative fall into two categories – those that “change the
context to make healthy choices easier,” and those that address the SDOH. The six interventions aimed at
addressing SDOH are:
Early Childhood Education
Clean Diesel Bus Fleets
Public Transportation System
Home Improvement Loans and Grants
Earned Income Tax Credits
Water Fluoridation
CDC has also established cross-departmental relationships aimed at addressing SDOH. CDC and the
Department of Housing and Urban Development (HUD) have established an interagency agreement to build a
sustainable, collaborative partnership to intentionally advance shared priorities related to health and housing.
The first step is to provide evidence informed approaches for affordable senior housing programs. CDC and
HUD are also working to develop a strategic framework or blueprint outlining goals to support state and local
public health agencies and housing agencies to partner and achieve shared priorities locally. In addition, the
Federal Transit Administration (FTA) in the Department of Transportation (DOT) has partnered with HHS,
including CDC, on the Interagency Coordinating Council on Access and Mobility (CCAM), which is charged with
increasing transportation access for low- income populations, older adults, and people with disabilities. The
CCAM is jointly working across 11 federal departments to develop a 2023-2026 Strategic Plan for Human
Services Transportation.
In addition to implementing and funding interventions aimed at impacting SDOH, CDC is also working to build
the evidence base around effective interventions. The Guide to Community Preventive Services (The
Community Guide), a collection of evidence-based findings of the Community Preventive Services Task Force
(CPSTF), is a resource to help jurisdictions select interventions to improve health and prevent disease in states,
communities, community organizations, businesses, health care organizations, or schools.
158
In 2020, CPSTF
selected SDOH as one of nine priority topics to guide their systematic reviews on population health
interventions for 2020-2025, and they formed a Health Equity Committee to assess and advance their work in
this area. In 2020, CDC also awarded funds to the Association of State and Territorial Health Officials (ASTHO)
and National Association of City and County Health Officials (NACCHO) to complete a retrospective evaluation
of multi-sector coalitions to advance health equity by addressing SDOH. Year one findings of the 42
community multi-sector partnerships from across the country selected as a part of the Improving Social
Determinants of Health–Getting Further Faster (GFF) pilot project showed that GFF partnerships built
community capacity to address SDOH through new or strengthened partnerships, data and data systems, or
strategic plans; leveraged resources; or engaged residents.
159
Ninety percent of GFF partnerships contributed
to community changes that promote healthy living, such as building new walking trails, bike lanes, and
playgrounds; creating new community and school gardens; and adopting tobacco-free policies. More than half
of GFF partnerships reported positive health outcomes data for their SDOH initiatives, including improved
health behaviors, clinical outcomes, and overall health and wellness, and decreased health care use and costs.
Administration for Community Living
The Administration for Community Living (ACL), in partnership with CMS, the Substance Abuse and Mental
Health Services Administration (SAMHSA), ASPE, and HUD, recently launched the Housing Services Resource
Center, which fosters collaboration and cross-sector partnerships to streamline services, better leverage
resources, and make community living possible for more people.
160
This initiative offers innovative models and
strategies to people who work at the organizations and systems that provide housing resources and

April 2022 REPORT 15
homelessness services, behavioral health services, independent living services and other supportive services,
and others who are working to help people live successfully and stably in the community. It provides
resources on how to develop and expand partnerships, tools for community collaborations, and information
on supporting people with disabilities, older adults, and people experiencing homelessness to get and/or keep
affordable and accessible housing and voluntary supportive services.
ACL also funds a nationwide network of aging and disability organizations that provide access to a variety of
local community-based services that address social needs. Through this network, ACL provides 150 million
home-delivered meals to over 883,000 individuals and 73.6 million congregate meals to more than 1.5 million
seniors, funded through the OAA Nutrition Program.
161
Nutrition services help older Americans remain healthy
and independent in their communities by providing meals and related services in a variety of community
settings and via home-delivery to older adults who are homebound due to illness, disability, or geographic
isolation. As compared to the U.S. population age 60 and older, participants in the OAA Nutrition Program are
more likely to be in poor or fair health, have difficulties with three or more ADLs, live alone, and live in rural
communities.
162
In addition to meals, the program provides nutrition screening, assessment, education, and
counseling, and provides connections to other in-home and community supports. ACL also provides
transportation services through their network, providing more than 20.4 million rides to doctor’s offices,
grocery stores, pharmacies, senior centers, meal sites, and other critical daily activities.
163
Forty-six percent of
passengers on OAA-funded transportation are mobility impaired, meaning they do not own a car, or if they do
own a car, they do not drive, and are not near public transportation.
164
Of the transportation participants, 71
percent have at least one chronic condition that could impair their ability to navigate safely, and 96 percent
take daily medications, with over 16 percent taking 10 to 25 medications daily. In addition, ACL’s network
provided 3.3 million hours of case management services in Fiscal Year 2019 to assess needs, develop care
plans, and arrange services for older persons or their caregivers. Over 82 percent of clients receiving case
management reported that, as a result of the services arranged by the case manager, they were better able to
care for themselves.
165
In addition, ACL’s Social Care Referrals Challenge is working to support health care systems and community-
based organizations through health IT solutions.
166
The challenge seeks to cultivate care coordination,
including the sharing of standardized data on SDOH, by developing or optimizing interoperable, scalable
technology solutions that foster connections between community-based organizations and health care
systems. Twelve proposals were selected for phase two of the competition, which will give the teams $30,000
and will allow teams to continue develop their solutions as they compete for a second award of $60,000 and a
grand prize of $140,000.
Through grant awards made in September 2021, ACL is also supporting the infrastructure of 12 Network Lead
Entities, or community hubs, that coordinate the activities of a broader network to efficiently contract with
health plans and providers to address social needs. Increasingly, CBOs are organizing to form networks,
allowing them to deliver a broad scope of services, expand populations served and geographic coverage, build
stronger administrative functions, and offer a single point of contracting for payers.
167
As part of their support for their disability network, ACL also offers several grants to enhance the cultural and
linguistic competency of the disability network to ensure that all people with disabilities can access ACL-funded
programs and services.
168
These include grants to build cultural competency within University Centers for
Excellence in Developmental Disabilities, increase the diversity of leadership and staff in the development
disability network, establish a diversity community of practice to create and share policies, practices, and
systems in cultural and linguistic competence in disability programs, and conduct a gap analysis of cultural
competency in the developmental disability network programs, among others.
Administration for Children and Families

April 2022 REPORT 16
The Administration for Children and Families (ACF) promotes the economic and social well-being of families,
children, youth, individuals, and communities. Although not specifically designed to influence health, these
anti-poverty and family support programs provide cash assistance, in-kind family support, and other individual,
family and child services that can profoundly affect traditional health outcomes. All ACF programs, including
childcare, Head Start, Child Support Enforcement, Child Welfare, Runaway and Homeless Youth, Temporary
Assistance for Needy Families, healthy marriage and responsible fatherhood programs, community services,
refugee resettlement, Low Income Home Energy Assistance, adolescent pregnancy prevention, and family
violence prevention, address social determinants that can affect health and quality of life outcomes.
The Temporary Assistance for Needy Families (TANF) cash assistance benefits, which supported more than one
million families in 2019 experiencing poverty, reduced poverty by 11.3 percentage points among
recipients.
169,170
TANF funds are used to supplement income and for employment, education, and training that
can promote economic mobility; to provide transportation assistance; to provide subsidies for utility payments
to prevent utility shut offs; and to provide subsidies for food assistance. Case management provided through
TANF can also screen for and identify health-related barriers such as mental health concerns or substance use
disorder. During the COVID-19 pandemic, TANF programs across the country also used TANF funds to serve
and support families experiencing or at risk of homelessness.
171
HHS oversees the national Child Support program, partnering with state, tribal and local child support
agencies, and others to encourage parental responsibility so that children receive financial, emotional, and
medical support from both parents, even when they live in separate households. Child support payments help
to increase income and reduce poverty among low-income custodial parents and their children. In fiscal year
2020, preliminary data shows the national program collected $34.9 billion and served 13.8 million children and
their families.
172
Additional analyses shows that child support reduced poverty by 6.3 percentage points
among individuals in families who received payments.
173
ACF also provides grant funding and oversight to the programs that provide Head Start services across the
country. Head Start promotes school readiness by offering educational, nutritional, health, social, and other
services to children in low-income families.
174
In 2019, Head Start was funded to serve nearly one million
children and pregnant women, and since its inception it has served more than 37 million children and their
families.
Substance Abuse and Mental Health Services Administration
The Substance Abuse and Mental Health Services Administration (SAMHSA) provides programs and resources
to help address social determinants of behavioral health, SDOH, and HRSNs for individuals with behavioral
health conditions. For example, services provided through SAMHSA’s grant programs help people with mental
and substance use issues find housing and supportive services, increase access to disability income benefits for
eligible adults who are experiencing or at risk for homelessness, and provide case management and other
supports that assist in preventing or ending homelessness.
175
The Office of the National Coordinator for Health Information Technology
The Office of the National Coordinator for Health Information Technology (ONC) seeks to improve the health
and well-being of individuals and communities through the use of technology and health information,
including SDOH information, that is accessible when and where it matters most. Advancing the use and
interoperability of SDOH data is important to improving the health and well-being of all individuals and
communities. Though not discussed in the evidence-based interventions above, accessible data is
fundamental to the success of SDOH interventions. ONC is focused on ensuring that both patients and
providers understand what capabilities are possible and required by the 21st Century Cures Act to ensure that
with increased adoption of health information technology (IT), we can also more effectively capture

April 2022 REPORT 17
information about the conditions in which people live, learn, work, and play to improve health outcomes.
Standardization of the way in which the data is obtained and exchanged will help providers more easily
address non-clinical factors, such as food, housing, and transportation insecurities, which can have a profound
impact on a person’s overall health. For example, as of March 2022, almost all hospitals and roughly 75
percent of physicians use electronic health records (EHRs) certified through the ONC Health IT Certification
Program, helping to enable widespread capabilities for the capture, reporting, exchange, and use of granular
race and ethnicity data. This functionality will soon extend to the widespread use of interoperable SDOH data
that can be electronically captured, used, and exchanged.
ONC works collaboratively with federal partners and the stakeholder community to advance the electronic
exchange and use of SDOH data to help improve individual and population health by guiding the development,
dissemination, and adoption of health IT standards; informing the development of policies to overcome SDOH
data interoperability challenges and data use; supporting states and local governments as they build the
infrastructures for SDOH data; and driving innovation in care delivery by using health IT tools and standards to
integrate SDOH data into workflows.
CONCLUSION
Studies indicate that some SDOH and HRSN interventions, provided in the right settings and depending on the
population, can improve health outcomes and well-being. In addition, some interventions may also decrease
health care costs, though successful interventions can be cost-effective and worth undertaking even if they do
not ultimately save money overall. Much of the research to date has focused on shorter-term outcomes and
medically complex populations or those with high health care utilization. Research on community
interventions has also demonstrated health improvements with long-term impact. However, as we focus our
efforts on SDOH and HRSNs, more work to assess the impact of various interventions on multiple populations
is warranted. Additional research can help us better understand how interventions to address risks related to
SDOH and HRSNs in less medically complex individuals impact health and well-being over the life course, as
well as the longer-term impacts of interventions; the impact on a wider range of populations, including rural
communities and individuals without chronic illnesses; and the most appropriate “dose” of various
interventions. Further, as discussed in the introduction, additional research is needed that focuses on health
outcomes, in addition to health utilization, health costs, and healthy behaviors.
In addition to efforts to improve SDOH and HRSNs, HHS is committed to building the evidence base and
measuring success related to these efforts. The Healthy People initiative identifies data-driven national
objectives to improve the health of the nation. One of Healthy People 2030’s five overarching goals is
specifically related to SDOH: “Create social, physical, and economic environments that promote attaining the
full potential for health and well-being for all.”
176
The benchmarks set by Healthy People 2030 include targets
to monitor progress and motivate and focus action and will help HHS in its efforts to track progress on
improving SDOH.
Through a whole-of-government, multi-sector strategy, HHS is working to improve health and well-being of the
U.S. population by investing in efforts to identify and address the underlying systemic and environmental
factors that affect health status. As discussed further in “HHS’s Strategic Approach to Addressing Social
Determinants of Health to Advance Health Equity – At a Glance,
*
” HHS will drive progress through coordinated
strategies and activities to better integrate health and human services and to advance public health initiatives
involving cross-sector partnerships and community engagement to address specific SDOH drivers. These
strategies and activities include strengthening data and data infrastructure, which can be used to improve
evaluation and support other objectives moving forward; improving connections between health and social
_______________________
*
https://aspe.hhs.gov/sites/default/files/documents/aabf48cbd391be21e5186eeae728ccd7/SDOH-Action-Plan-At-a-Glance.pdf

April 2022 REPORT 18
services, including community partners, to address HRSNs; and adopting whole-of-government collaborations
to address SDOH and enhance population health and well-being. HHS is not only supporting and implementing
initiatives that are based on existing evidence but is also working to evaluate current efforts to contribute to
our understanding of effective SDOH and HRSN interventions, refine existing efforts, and identify future
initiatives to address HRSNs and SDOH that may also have a beneficial effect on health and well-being.

April 2022 REPORT 19
REFERENCES
1. Ely DM, Driscoll AK. Infant Mortality in the United States, 2018: Data from the Period Linked
Birth/Infant Death File. National Vital Statistics Report; vol 69 no 7. Hyattsville, MD: National Center
for Health Statistics. July 2020.
2. Ely DM, Driscoll AK, Matthews TJ. Infant Mortality Rates in Rural and Urban Areas in the United
States, 2014. NCHS Data Brief; no 285. Hyattsville, MD: National Center for Health Statistics.
September 2017.
3. National Cancer Institute. Cancer Disparities. November 17, 2020. https://www.cancer.gov/about-
cancer/understanding/disparities
4. National Center for Health Statistics. Health, United States Spotlight: Racial and Ethnic Disparities in
Heart Disease. April 2019.
https://www.cdc.gov/nchs/hus/spotlight/HeartDiseaseSpotlight_2019_0404.pdf
5. Schopfer DW. Rural health disparities in chronic heart disease. Prev Med. 2021 Nov;152(Pt 2):106782.
doi: 10.1016/j.ypmed.2021.106782. Epub 2021 Sep 7. PMID: 34499971.
6. Arias E, Tejada-Vera B, Ahmad F, Kochanek KD. Provisional life expectancy estimates for 2020. Vital
Statistics Rapid Release; no 15. Hyattsville, MD: National Center for Health Statistics. July 2021.
7. Henning Smith, C., A.M. Hernandez, M. Ramirez, R. Hardeman, K. Kozhimannil. March 2019. “Dying
Too Soon: County-Level Disparities in Premature Death by Rurality, Race, and Ethnicity.” University of
Minnesota Rural Health Research Center https://3pea7g1qp8f3t9ooe3z3npx1-wpengine.netdna-
ssl.com/wp-content/uploads/2019/03/1552267547UMNpolicybriefPrematureDeath.pdf
8. Krehely J. How to Close the LGBT Health Disparities Gap. Center for American Progress. December
2009. https://www.americanprogress.org/article/how-to-close-the-lgbt-health-disparities-gap/
9. Centers for Disease Control and Prevention. Human Development and Disability, Health Equity.
January 2022. https://www.cdc.gov/ncbddd/humandevelopment/health-equity.html
10. Muenning, Peter, Kevin Fiscella, Daniel Tancredi, and Peter Franks. The Relative Health Burden of
Selected Social and Behavioral Risk Factors in the United States: Implications of Policy. American
Journal of Public Health. 2010; 100 (9): 1758–64. doi: 10.2105/AJPH.2009.165019
11. World Health Organization. Health Equity. https://www.who.int/health-topics/health-equity
12. U.S. Department of Health and Human Services. Healthy People 2030, Social Determinants of Health.
https://health.gov/healthypeople/objectives-and-data/social-determinants-health
13. Hood CM, Gennuso KP, Swain GR, et al. County Health Rankings: Relationships Between Determinant
Factors and Health Outcomes. American Journal of Preventive Medicine. February 2016; 50(2):129-
135. doi:10.1016/j.amepre.2015.08.024
14. Hood, CM, Gennuso KP, Swain GR, et al. County Health Rankings: Relationships Between Determinant
Factors and Health Outcomes in 45 States. American Journal of Preventive Medicine. February 2016;
50(2): 129-35. doi: 10.1016/j.amepre.2015.08.024
15. Tsega M, Lewis C, McCarthy D, Shah T, Coutts K. Review of Evidence for Health-Related Social Needs
Interventions. July 2019. The Commonwealth Fund.
https://www.commonwealthfund.org/sites/default/files/2019-07/ROI-EVIDENCE-REVIEW-FINAL-
VERSION.pdf
16. Taylor LA, Coyle CE, Ndumele C, et al. Leveraging the Social Determinants of Health: What Works?
June 2015. Blue Cross Blue Shield of Massachusetts Foundation.
https://www.bluecrossmafoundation.org/sites/g/files/csphws2101/files/2020-
10/Social_Equity_Report_Final.pdf
17. Williams MV, Perez L, Siddiqi S, et al. Building the Evidence Base for Social Determinants of Health
Interventions. September 2021. U.S. Department of Health and Human Services, Office of the

April 2022 REPORT 20
Assistant Secretary for Planning and Evaluation. https://aspe.hhs.gov/reports/building-evidence-
base-social-determinants-health-interventions
18. Patient-Centered Outcomes Research Institute. PCORI Scoping Review and Evidence Map Report:
Social Needs Interventions to Improve Health Outcomes. February 2021.
https://www.pcori.org/research-results/2020/evidence-map-social-needs-interventions-and-health-
outcomes
19. National Academies of Sciences, Engineering, and Medicine. Systems Practices for the Care of Socially
At-Risk Populations. The National Academies Press. 2016. doi:10.17226/21914
20. University of San Francisco California. Social Interventions Research and Evaluation Network (SIREN)
Evidence & Resource Library. https://sirenetwork.ucsf.edu/tools/evidence-library
21. U.S. Department of Health and Human Services. The Guide to Community Preventive Services (The
Community Guide). Community Preventive Services Task Force.
https://www.thecommunityguide.org/
22. Sandel M, Sheward R, Ettinger de Cuba S, et al. Unstable Housing and Caregiver and Child Health in
Renter Families. Pediatrics. 2018; 141(2): e2017-2199. doi:10.1542/peds.2017-2199
23. Community Preventive Services Task Force. Health Equity: Tenant-Based Housing Voucher Programs.
The Community Guide. https://www.thecommunityguide.org/findings/health-equity-tenant-based-
housing-voucher-programs
24. Dohler E, Bailey P, Rice D, et al. Supportive Housing Helps Vulnerable People Live and Thrive in the
Community. May 2016. Center for Budget and Policy Priorities.
https://www.cbpp.org/research/housing/supportive-housing-helps-vulnerable-people-live-and-
thrive-in-the-community
25. Community Preventive Services Task Force. Health Equity: Permanent Supportive Housing with
Housing First (Housing First Programs). The Community Guide.
https://www.thecommunityguide.org/findings/health-equity-housing-first-programs
26. Tsega M, Lewis C, McCarthy D, Shah T, Coutts K. Review of Evidence for Health-Related Social Needs
Interventions. July 2019. The Commonwealth Fund.
https://www.commonwealthfund.org/sites/default/files/2019-07/ROI-EVIDENCE-REVIEW-FINAL-
VERSION.pdf
27. Taylor LA, Coyle CE, Ndumele C, et al. Leveraging the Social Determinants of Health: What Works?
June 2015. Blue Cross Blue Shield of Massachusetts Foundation.
https://www.bluecrossmafoundation.org/sites/g/files/csphws2101/files/2020-
10/Social_Equity_Report_Final.pdf
28. U.S. Department of Health and Human Services, Office of the Assistant Secretary for Planning and
Evaluation. Building the Evidence Base for Social Determinants of Health Interventions. May 2021.
https://aspe.hhs.gov/sites/default/files/documents/e400d2ae6a6790287c5176e36fe47040/PR-
A1010-1_final.pdf
29. Sadowski LS, Kee RA, VanderWeele TJ, Buchanan D. Effect of a housing and case management
program on emergency department visits and hospitalizations among chronically ill homeless adults:
a randomized trial. JAMA. 2009;301(17):1771-1778. doi:10.1001/jama.2009.561
30. Buchanan D, Kee R, Sadowski LS, Garcia D. The health impact of supportive housing for HIV-positive
homeless patients: a randomized controlled trial. Am J Public Health. 2009;99 Suppl 3(Suppl 3):S675-
S680. doi:10.2105/AJPH.2008.137810
31. Basu A, Kee R, Buchanan D, et al. Comparative Cost Analysis of Housing and Case Management
Program for Chronically Ill Homeless Adults Compared to Usual Care. Health Services Research.
November 2011; 47(1 pt 2): 523-543. doi: 10.1111/j.1475-6773.2011.01350.x

April 2022 REPORT 21
32. Jacob V, Chattopadhyay SK, Attipoe-Dorcoo, S, et al. Permanent Supportive Housing With Housing
First: Findings From a Community Guide Systematic Economic Review. American Journal of Preventive
Medicine. 2022;62(3):e188-e201. doi:10.1016/j.amepre.2021.08.009
33. Flaming D, Burns P, Matsunaga M, et al. Where We Sleep: Costs when Homeless and Housed in Los
Angeles. Economic Roundtable. 2009. https://shnny.org/uploads/Where_We_Sleep.pdf
34. Tsega M, Lewis C, McCarthy D, Shah T, Coutts K. Review of Evidence for Health-Related Social Needs
Interventions. July 2019. The Commonwealth Fund.
https://www.commonwealthfund.org/sites/default/files/2019-07/ROI-EVIDENCE-REVIEW-FINAL-
VERSION.pdf
35. U.S. Department of Health and Human Services, Office of the Assistant Secretary for Planning and
Evaluation. Building the Evidence Base for Social Determinants of Health Interventions. May 2021.
https://aspe.hhs.gov/sites/default/files/documents/e400d2ae6a6790287c5176e36fe47040/PR-
A1010-1_final.pdf
36. KPMG Government Institute. Investing in social services as a core strategy for healthcare
organizations: Developing the business case. 2018.
https://institutes.kpmg.us/content/dam/institutes/en/government/pdfs/2018/investing-social-
services.pdf
37. Centers for Disease Control and Prevention. Home Improvement Loans and Grants. Health Impact in 5
Years Interventions. https://www.cdc.gov/policy/hst/hi5/homeimprovement/index.html
38. Stark S, Keglovits M, Arbesman M, et al. Effect of Home Modification Interventions on the
Participation of Community-Dwelling Adults With Health Conditions: A Systematic Review. American
Journal of Occupational Therapy. 2017;71(2): 7102290010p1-7102290010p11. doi:
10.5014/ajot.2017.018887.
39. Carnemolla P, Bridge C. A scoping review of home modification interventions – Mapping the evidence
base. Indoor and Built Environment. 2020;29(3):299-310. doi:10.1177/1420326X18761112
40. Kersten EE, LeWinn KZ, Gottlieb L, Jutte DP, Adler NE. San Francisco Children Living In Redeveloped
Public Housing Used Acute Services Less Than Children In Older Public Housing. Health Affairs. 2014;
33(12): 2230-2237. doi: 10.1377/hlthaff.2014.1021
41. Williams, SG, Brown CM, Falter KH, et al. Does a Multifaceted Environmental Intervention Alter the
Impact of Asthma on Inner-City Children? Journal of the National Medical Association. February 2006;
98(3): 249-260. PMCID: PMC2595052
42. County Health Rankins & Roadmaps. Healthy home environment assessments. April 2019.
https://www.countyhealthrankings.org/take-action-to-improve-health/what-works-for-
health/strategies/healthy-home-environment-assessments
43. Community Preventive Services Task Force. Asthma Control: Home-Based Multi-Trigger,
Multicomponent Environmental Interventions for Children and Adolescents with Asthma. Task Force
Finding and Rationale Statement. September 2013.
https://www.thecommunityguide.org/sites/default/files/assets/Asthma-Home-Based-Children.pdf
44. Centers for Disease Control and Prevention. Smokefree Policies Reduce Secondhand Smoke Exposure.
August 2020.
https://www.cdc.gov/tobacco/data_statistics/fact_sheets/secondhand_smoke/protection/shs_expos
ure/index.htm
45. King BA, Peck RM, Babb SD. National and State Cost Savings Associated With Prohibiting Smoking in
Subsidized and Public Housing in the United States. Preventing Chronic Disease. 2014; 11:140222. doi:
10.5888/pcd11.140222

April 2022 REPORT 22
46. Szanton SL, Alfonso YN, Leff B, et al. Medicaid Cost Savings of a Preventive Home Visit Program for
Disabled Older Adults. Journal of the American Geriatrics Society. 2018; 66(3):614-620. doi:
10.1111/jgs.15143
47. Szanton SL, Xue Q, Leff B, et al. Effect of a Biobehavioral Environmental Approach on Disability Among
Low-Income Older. JAMA Intern Med. 2019;179(2):204-211. doi:10.1001/jamainternmed.2018.6026
48. Aliberti MJR, Covinsky KE. Home Modifications to Reduce Disability in Older Adults With Functional
Disability. JAMA Intern Med. 2019;179(2):211-212. doi:10.1001/jamainternmed.2018.6414
49. Health Impact Project. 10 Policies to Prevent and Respond to Childhood Lead Exposure. August 2017.
Robert Wood Johnson Foundation and The Pew Charitable Trusts. https://www.pewtrusts.org/-
/media/assets/2017/08/hip_childhood_lead_poisoning_report.pdf
50. Centers for Disease Control and Prevention. Healthy Food Environments. February 2021.
https://www.cdc.gov/nutrition/healthy-food-environments/index.html
51. Centers for Disease Control and Prevention. Guidelines & Recommendations. April 2021.
https://www.cdc.gov/nutrition/strategies-guidelines/index.html
52. Community Preventive Services Task Force. Obesity Prevention and Control: Meal or Fruit and
Vegetable Snack Interventions Combined with Physical Activity Interventions in Schools. The
Community Guide. https://www.thecommunityguide.org/findings/obesity-prevention-control-meal-
fruit-vegetable-snack-interventions-combined-physical-activity-interventions-schools
53. Community Preventive Services Task Force. CPSTF Findings for Nutrition. The Community Guide.
https://www.thecommunityguide.org/content/task-force-findings-nutrition
54. Community Preventive Services Task Force. TFFRS - Nutrition and Physical Activity: Community-based
Digital Health and Telephone Interventions to Increase Healthy Eating and Physical Activity, The
Community Guide. https://www.thecommunityguide.org/content/tffrs-nutrition-and-physical-
activity-community-based-digital-health-and-telephone-interventions-increase-healthy-eating-and-
physical-activity
55. Tsega M, Lewis C, McCarthy D, Shah T, Coutts K. Review of Evidence for Health-Related Social Needs
Interventions. July 2019. The Commonwealth Fund.
https://www.commonwealthfund.org/sites/default/files/2019-07/ROI-EVIDENCE-REVIEW-FINAL-
VERSION.pdf
56. Taylor LA, Coyle CE, Ndumele C, et al. Leveraging the Social Determinants of Health: What Works?
June 2015. Blue Cross Blue Shield of Massachusetts Foundation.
https://www.bluecrossmafoundation.org/sites/g/files/csphws2101/files/2020-
10/Social_Equity_Report_Final.pdf
57. Berkowitz SA, Seligman HK, Rigdon J, et al. Supplemental Nutrition Assistance Program (SNAP)
Participation and Health Care Expenditures Among Low-Income Adults. JAMA Internal Medicine.
2017; 177(11):1642-1649. doi:10.1001/jamainternmed.2017.4841
58. Samuel LJ, Szanton SL, Cahill R, et al. Does the Supplemental Nutrition Assistance Program Affect
Hospital Utilization Among Older Adults? The Case of Maryland. Population Health Management.
2018;21(2): 88-95. doi: 10.1089/pop.2017.0055.
59. Soneji, S, Beltran-Sanchez H. Association of Special Supplemental Nutrition Program for Women,
Infants, and Children With Preterm Birth and Infant Mortality. JAMA Network Open.
2019;2(12):e1916722. doi:10.1001/jamanetworkopen.2019.16722
60. Testa A, Jackson DB. Race, ethnicity, WIC participation, and infant health disparities in the United
States. Annals of Epidemiology. June 2021; 58:22-28. doi: 10.1016/j.annepidem.2021.02.005
61. Taylor LA, Coyle CE, Ndumele C, et al. Leveraging the Social Determinants of Health: What Works?
June 2015. Blue Cross Blue Shield of Massachusetts Foundation.

April 2022 REPORT 23
https://www.bluecrossmafoundation.org/sites/g/files/csphws2101/files/2020-
10/Social_Equity_Report_Final.pdf
62. Berkowitz SA, Seligman HK, Choudhry NK. Treat or Eat: Food Insecurity, Cost-related Medication
Underuse, and Unmet Needs. The American Journal of Medicine. 2014;127(4):P303-310.E3. doi:
10.1016/j.amjmed.2014.01.002
63. Mabli J, Gearan E, Cohen R, Niland K, et al. Evaluation of the Effect of the Older Americans Act Title III-
C Nutrition Services Program on Participants’ Food Security, Socialization, and Diet Quality. April
2017. Mathematica Policy Research. https://acl.gov/sites/default/files/programs/2017-
07/AoA_outcomesevaluation_final.pdf
64. Kowlessar N, Robinson K, Schur C. Older Americans Benefit from Older Americans Act Nutrition
Programs. September 2015. Administration for Community Living.
https://acl.gov/sites/default/files/programs/2016-11/AoA-Research-Brief-8-2015.pdf
65. White, N. Produce Prescriptions, Food Pharmacies, and the Potential Effect on Food Choice. Am J
Lifestyle Med. 2020;14(4): 335-268. doi: 10.1177/1559827620915425
66. Ibid.
67. Tsega M, Lewis C, McCarthy D, Shah T, Coutts K. Review of Evidence for Health-Related Social Needs
Interventions. July 2019. The Commonwealth Fund.
https://www.commonwealthfund.org/sites/default/files/2019-07/ROI-EVIDENCE-REVIEW-FINAL-
VERSION.pdf
68. Harvard Law School. Food is Medicine: Peer-Reviewed Research in the U.S. December 2020. Center
for Health Law and Policy Innovation. https://chlpi.org/wp-content/uploads/2013/12/Food-is-
Medicine_Peer-Reviewed-Research-in-the-U.S.1.pdf
69. KPMG Government Institute. Investing in social services as a core strategy for healthcare
organizations: Developing the business case. 2018.
https://institutes.kpmg.us/content/dam/institutes/en/government/pdfs/2018/investing-social-
services.pdf
70. Hess, A, Passaretti M, Coolbaugh S. Fresh Food Farmacy (Editorial). American Journal of Health
Promotion. May 2019; 33(5):830-832. doi: 10.1177/0890117119845711d
71. Trust for America’s Health. Produce Rx: Using Prescriptions to Improve Affordability of Healthy Foods.
n.d. https://www.tfah.org/story/produce-rx-using-prescriptions-to-improve-affordability-of-healthy-
foods/
72. Bryce R, Guajardo C, Ilarraza D, et al. Participation in a farmers' market fruit and vegetable
prescription program at a federally qualified health center improves hemoglobin A1C in low income
uncontrolled diabetics. Prev Med Rep. 2017;7:176-179. doi:10.1016/j.pmedr.2017.06.006
73. Gurvey J, Rand K, Daughtery S, et al. Examining Health Care Costs Among MANNA Clients and a
Comparison Group. Journal of Primary Care & Community Health. 2013; 4(4):311-317. DOI:
10.1177/2150131913490737
74. Berkowitz SA, Terranova J, Hill C, et al. Meal Delivery Programs Reduce The Use Of Costly Health Care
In Dually Eligible Medicare And Medicaid Beneficiaries. Health Affairs. 2018;37(4): 535-542. doi:
10.1377/hlthaff.2017.0999.
75. U.S. Department of Transportation. Connectivity. August 2015.
https://www.transportation.gov/mission/health/connectivity
76. Wallace R, Hughes-Cromwick P, Mull H, et al. Access to health care and nonemergency medical
transportation: Two missing links. Transportation Research Record: Journal of the Transportation
Research Board. 2005;1924(1):76-84. doi:10.1177/0361198105192400110

April 2022 REPORT 24
77. American Hospital Association. Social Determinants of Health Series: Transportation and the Role of
Hospitals. November 2017. https://www.aha.org/ahahret-guides/2017-11-15-social-determinants-
health-series-transportation-and-role-hospitals
78. Tsega M, Lewis C, McCarthy D, Shah T, Coutts K. Review of Evidence for Health-Related Social Needs
Interventions. July 2019. The Commonwealth Fund.
https://www.commonwealthfund.org/sites/default/files/2019-07/ROI-EVIDENCE-REVIEW-FINAL-
VERSION.pdf
79. Adelberg M, Salber P, Pruisner T, et al.Non-Emergency Medical Transportation: Findings from a
Return on Investment Study. Medical Transportation Access Coalition. 2008.
https://mtaccoalition.org/wp-content/uploads/2018/07/NEMT-ROI-Methodology-Paper.pdf
80. Hughes-Cromwick P, Wallace R, Mull H, et al. Cost Benefit Analysis of Providing Non-Emergency
Medical Transportation. Transportation Research Board of the National Academies. October 2005.
https://altarum.org/sites/default/files/uploaded-publication-
files/05_project_report_hsd_cost_benefit_analysis.pdf
81. Kaiser Family Foundation. Medicaid Waiver Tracker: Approved and Pending Section 1115 Waivers by
State. February 2022. https://www.kff.org/medicaid/issue-brief/medicaid-waiver-tracker-approved-
and-pending-section-1115-waivers-by-state/
82. Centers for Disease Control and Prevention. Public Transportation System: Introduction or Expansion.
October 2018. https://www.cdc.gov/policy/hst/hi5/publictransportation/index.html
83. Centers for Disease Control and Prevention. CDC Recommendations for Improving Health through
Transportation Policy. April 2010. https://www.cdc.gov/transportation/docs/FINAL-CDC-
Transportation-Recommendations-4-28-2010.pdf
84. Centers for Disease Control and Prevention. Public Transportation System: Introduction or Expansion.
October 2018. https://www.cdc.gov/policy/hst/hi5/publictransportation/index.html
85. Litman, T. Evaluating Public Transportation Health Benefits. Victoria Transport Policy Institute. 2020.
https://www.vtpi.org/tran_health.pdf
86. Rissel C, Curac N, Greenaway M, Bauman A. Physical activity associated with public transport use--a
review and modelling of potential benefits. Int J Environ Res Public Health. 2012;9(7):2454-2478.
doi:10.3390/ijerph9072454
87. Wener RE, Evans GW. A Morning Stroll: Levels of Physical Activity in Car and Mass Transit Commuting.
Environment and Behavior. 2007;39(1):62-74. doi:10.1177/0013916506295571
88. Rissel C, Curac N, Greenaway M, Bauman A. Physical activity associated with public transport use--a
review and modelling of potential benefits. Int J Environ Res Public Health. 2012;9(7):2454-2478.
doi:10.3390/ijerph9072454
89. Centers for Disease Control and Prevention. Motor Vehicle Traffic-Related Pedestrian Deaths —
United States, 2001–2010. Morbidity and Mortality Weekly Report. April 2013.
https://www.cdc.gov/mmwr/preview/mmwrhtml/mm6215a1.htm
90. Community Preventive Services Task Force. Physical Activity: Built Environment Approaches
Combining Transportation System Interventions with Land Use and Environmental Design. The
Community Guide. https://www.thecommunityguide.org/findings/physical-activity-built-
environment-approaches
91. Chetty R, Friedman JN, Hendren N, et al. The Economic Impacts of COVID-19: Evidence from a New
Public Database Built Using Private Sector Data. November 2020. https://opportunityinsights.org/
92. Muenning, Peter, Kevin Fiscella, Daniel Tancredi, and Peter Franks. The Relative Health Burden of
Selected Social and Behavioral Risk Factors in the United States: Implications of Policy. American
Journal of Public Health. 2010; 100 (9): 1758–64. doi: 10.2105/AJPH.2009.165019

April 2022 REPORT 25
93. Phelan JC, Link BG, Tehranifar P. Social conditions as fundamental causes of health inequalities:
theory, evidence, and policy implications. Journal of Health and Social Behavior. 2010;51 Suppl:S28-
S40. doi: 10.1177/0022146510383498
94. Macintyre S, Ellaway A, Cummins S. Place effects on health: how can we conceptualise, operationalise
and measure them? Social Science Medicine. 2002;55(1):125-139. doi:10.1016/S0277-
9536(01)00214-3
95. American Academy of Family Physicians. Poverty and Health - The Family Medicine Perspective
(Position Paper). April 2021. https://www.aafp.org/about/policies/all/poverty-health.html
96. Evans GW, Kim P. Childhood poverty and health: cumulative risk exposure and stress dysregulation.
Psychol Sci. 2007;18(11):953-957. doi: 10.1111/j.1467-9280.2007.02008.x.
97. Sun S, Huang S, Hudson DL, et al. Cash Transfers and Health. Annual Review of Public Health. April
2021; 42:363-380. doi: 10.1146/annurev-publhealth-090419-102442
98. Olshansky SJ, Antonucci T, Berkman L, et al. Differences in life expectancy due to race and educational
differences are widening, and many may not catch up. Health Affairs. 2012;31(8):1803-1813. doi:
10.1377/hlthaff.2011.0746
99. West S, Castro Baker A, Samra S, et al. Preliminary Analysis: SEED’s First Year. 2021.
https://static1.squarespace.com/static/6039d612b17d055cac14070f/t/603ef1194c474b329f33c329/
1614737690661/SEED_Preliminary+Analysis-SEEDs+First+Year_Final+Report_Individual+Pages+-2.pdf
100. Kehrer BH, Wolin CM. Impact of income maintenance on low birth weight: Evidence form the Gary
experiment. Journal of Human Resources. 1979;14:434–462. doi: 10.2307/145316
101. Costello EJ, Compton SN, Keeler G, et al. Relationships Between Poverty and Psychopathology: A
Natural Experiment. JAMA. 2003;290(15):2023-2029. doi:10.1001/jama.290.15.2023
102. Chaudry A, Wilmer C, Macartney S, et al. Poverty in the United States: 50-Year Trends and Safety Net
Impacts. Office of the Assistant Secretary for Planning and Evaluation. March 2016.
https://aspe.hhs.gov/sites/default/files/migrated_legacy_files//142581/50YearTrends.pdf
103. Taylor LA, Coyle CE, Ndumele C, et al. Leveraging the Social Determinants of Health: What Works?
June 2015. Blue Cross Blue Shield of Massachusetts Foundation.
https://www.bluecrossmafoundation.org/sites/g/files/csphws2101/files/2020-
10/Social_Equity_Report_Final.pdf
104. Arno PS, Sohler N, Viola D, et al. Bringing health and social policy together: The case of the earned
income tax credit. J Public Health Policy. 2009; 30(2): 198-207. doi: 10.1057/jphp.2009.3
105. Hoynes H, Miller D, Simon D. Income, the Earned Income Tax Credit, and Infant Health. American
Economic Journal: Economic Policy 2015, 7(1):172-211. doi: 10.1257/pol.20120179
106. Strully KW, Rehkopf DH, Xuan Z. Effects of Prenatal Poverty on Infant Health: State Earned Income Tax
Credits and Birth Weight. Am Sociol Rev. 2010 Aug 11; 75(4): 534–562. doi:
10.1177/0003122410374086
107. Hoynes H, Miller D, Simon D. Income, the Earned Income Tax Credit, and Infant Health. American
Economic Journal: Economic Policy 2015, 7(1):172-211. doi: 10.1257/pol.20120179
108. Arno PS, Sohler N, Viola D, et al. Bringing health and social policy together: The case of the earned
income tax credit. J Public Health Policy. 2009; 30(2): 198-207. doi: 10.1057/jphp.2009.3
109. Wicks-Lim J, Arno PS. Improving population health by reducing poverty: New York’s Earned Income
Tax Credit. SSM – Population Health. December 2017; 3: 373-381. doi: 10.1016/j.ssmph.2017.03.006
110. Herd P, Schoeni RF, House JS. Upstream Solutions: Does the Supplemental Security Income Program
Reduce Disability in the Elderly? University of Wisconsin Madison; University of Michigan, Ann Arbor.
https://deepblue.lib.umich.edu/bitstream/handle/2027.42/72843/j.1468-
0009.2007.00512.x.pdf?sequence=1&isAllowed=y

April 2022 REPORT 26
111. Bauer, L, Whitmore Schanzenbach D. The Long-Term Impact of the Head Start Program. The Hamilton
Project. August 2016.
https://www.hamiltonproject.org/assets/files/long_term_impact_of_head_start_program.pdf
112. Centers for Disease Control and Prevention. Early Childhood Education.
https://www.cdc.gov/policy/hst/hi5/earlychildhoodeducation/index.html#:~:text=Preschool%2Daged
%20children%20experience%20profound,emotional%20regulation%2C%20and%20motor%20skills.
113. Morrissey, T. The Effects of Early Care and Education on Children’s Health. Health Affairs. April 2019.
https://www.healthaffairs.org/do/10.1377/hpb20190325.519221/full/
114. Tsega M, Lewis C, McCarthy D, Shah T, Coutts K. Review of Evidence for Health-Related Social Needs
Interventions. July 2019. The Commonwealth Fund.
https://www.commonwealthfund.org/sites/default/files/2019-07/ROI-EVIDENCE-REVIEW-FINAL-
VERSION.pdf
115. Taylor LA, Coyle CE, Ndumele C, et al. Leveraging the Social Determinants of Health: What Works?
June 2015. Blue Cross Blue Shield of Massachusetts Foundation.
https://www.bluecrossmafoundation.org/sites/g/files/csphws2101/files/2020-
10/Social_Equity_Report_Final.pdf
116. Office of the Assistant Secretary for Planning and Evaluation, U.S. Department of Health & Human
Services. Report To Congress on the Medicaid Health Home State Plan Option. May 2018.
https://www.medicaid.gov/state-resource-center/medicaid-state-technical-assistance/health-home-
information-resource-center/downloads/medicaidhomehealthstateplanoptionrtc.pdf
117. Centers for Medicare & Medicaid Services. Accountable Health Communities Evaluation of
Performance Years 1-3 (2017-2019). https://innovation.cms.gov/data-and-reports/2020/ahc-first-
eval-rpt-fg
118. KPMG Government Institute. Investing in social services as a core strategy for healthcare
organizations: Developing the business case. 2018.
https://institutes.kpmg.us/content/dam/institutes/en/government/pdfs/2018/investing-social-
services.pdf
119. Murray, G. F., Rodriguez, H. P., & Lewis, V. A. Upstream with a small paddle: How ACOs are working
against the current to meet patients' social needs. Health Affairs. 2020; 39(2):199-206.
doi:10.1377/hlthaff.2019.01266
120. Brewster, A. L., Kunkel, S., Straker, J., & Curry, L. A. Cross-sectoral partnerships by area agencies on
aging: Associations with health care use and spending. Health Affairs,. 2018;37(1):15-21.
doi:10.1377/hlthaff.2017.1346
121. Brewster AL, Wilson TL, Frehn J, et al. Linking Health And Social Services Through Area Agencies On
Aging Is Associated With Lower Health Care Use And Spending. Health Affairs. 2020;39(4):587-594.
doi:10.1377/hlthaff.2019.01515
122. Li F, Guo J, Suga-Nakagawa A, et al. The Impact of Kaua'i Care Transition Intervention on Hospital
Readmission Rates. The American Journal of Managed Care. 2015;21(10): e560-e566.
123. American Public Health Association, Community Health Workers, https://www.apha.org/apha-
communities/member-sections/community-health-workers
124. Tsega M, Lewis C, McCarthy D, Shah T, Coutts K. Review of Evidence for Health-Related Social Needs
Interventions. July 2019. The Commonwealth Fund.
https://www.commonwealthfund.org/sites/default/files/2019-07/ROI-EVIDENCE-REVIEW-FINAL-
VERSION.pdf

April 2022 REPORT 27
125. Carter J, Hassan S, Walton A, et al. Effect of Community Health Workers on 30-Day Hospital
Readmissions in an Accountable Care Organization Population. JAMA Network Open.
2021;4(5):e2110936. doi:10.1001/jamanetworkopen.2021.10936
126. Embick ER, Maeng DD, Juskiewicz I, et al. Demonstrated health care cost savings for women: findings
from a community health worker intervention designed to address depression and unmet social
needs. Archives of Womens Mental Health. 2021; 24:85-92. doi: 10.1007/s00737-020-01045-9
127. Centers for Medicare & Medicaid Services. Re: Opportunities in Medicaid and CHIP to Address Social
Determinants of Health (SDOH) (SHO #21-001). January 7, 2021. https://www.medicaid.gov/federal-
policy-guidance/downloads/sho21001.pdf
128. Kaiser Family Foundation. State Health Facts, Medicaid Benefits: Case Management. 2018.
https://www.kff.org/other/state-indicator/medicaid-benefits-case-
management/?currentTimeframe=0&sortModel=%7B%22colId%22:%22Location%22,%22sort%22:%2
2asc%22%7D
129. Kaiser Family Foundation. State Health Facts, Medicaid Benefits: Targeted Case Management. 2018.
https://www.kff.org/medicaid/state-indicator/targeted-case-
management/?currentTimeframe=0&sortModel=%7B%22colId%22:%22Location%22,%22sort%22:%2
2asc%22%7D
130. Medicaid and CHIP Payment and Access Commission. Medicaid’s Role in Housing. June 2021.
https://www.macpac.gov/wp-content/uploads/2021/06/Medicaids-Role-in-Housing-1.pdf
131. Atkeson A. How States Use Federal Medicaid Authorities to Finance Housing-Related Services.
National Academy for State Health Policy. March 2021. https://www.nashp.org/wp-
content/uploads/2021/03/housing-medicaid-waiver-report-3-4-2021.pdf
132. Corporation for Supportive Housing. Summary of State Actions, Medicaid & Housing Services. August
2021. https://www.csh.org/wp-content/uploads/2021/08/Summary-of-State-Action_-Medicaid-and-
Supportive-Housing-Services-2021-08.pdf
133. Medicaid and CHIP Payment and Access Commission. Medicaid’s Role in Housing. June 2021.
https://www.macpac.gov/wp-content/uploads/2021/06/Medicaids-Role-in-Housing-1.pdf
134. California Health Care Foundation. CalAIM Explained: A Five-Year Plan to Transform Medi-Cal.
October 2021. https://www.chcf.org/wp-content/uploads/2021/07/CalAIMExplainedFiveYearPlan.pdf
135. Kaiser Family Foundation. Medicaid Waiver Tracker: Approved and Pending Section 1115 Waivers by
State. February 2022. https://www.kff.org/medicaid/issue-brief/medicaid-waiver-tracker-approved-
and-pending-section-1115-waivers-by-state/
136. Centers for Medicare & Medicaid Services. Medicaid Health Homes: An Overview. April 2021.
https://www.medicaid.gov/state-resource-center/medicaid-state-technical-assistance/health-home-
information-resource-center/downloads/hh-overview-fact-sheet.pdf
137. https://www.communityplans.net/wp-content/uploads/2018/12/Addressing-Social-Determinants-of-
Health-via-Contracts-and-1115-Demonstrations.pdf
138. Rosenbaum S, Casoni M, Somodevilla A, et al. How States Are Using Comprehensive Medicaid
Managed Care to Strengthen and Improve Primary Health Care. Commonwealth Fund. July 2020.
https://www.commonwealthfund.org/publications/issue-briefs/2020/jul/how-states-are-using-
comprehensive-medicaid-managed-care
139. Centers for Medicare & Medicaid Services. : United States Department of Agriculture (USDA)
Demonstration Project to Evaluate Using Medicaid Eligibility Data to Directly Certify Children for Free
and Reduced Price School Meals. September 2021. CMCS Informational Bulletin. https://fns-
prod.azureedge.net/sites/default/files/resource-files/cmcs-demonstration-eligibility-using-
medicaid%20data.pdf

April 2022 REPORT 28
140. Centers for Medicare & Medicaid Services. Accountable Health Communities Model. October 2021.
https://innovation.cms.gov/innovation-models/ahcm
141. Centers for Medicare & Medicaid Services. Accountable Health Communities Evaluation of
Performance Years 1-3 (2017-2020). https://innovation.cms.gov/data-and-reports/2020/ahc-first-
eval-rpt-fg
142. Centers for Medicare & Medicaid Services, Innovation Center Strategy Refresh.
https://innovation.cms.gov/strategic-direction-whitepaper
143. Centers for Medicare & Medicaid Services. CMS finalizes Medicare Advantage and Part D payment
and policy updates to maximize competition and coverage. April 2019.
https://www.cms.gov/newsroom/press-releases/cms-finalizes-medicare-advantage-and-part-d-
payment-and-policy-updates-maximize-competition-and
144. Kornfield T, Kazan M, Frieder M, et al. Medicare Advantage Plans Offering Expanded Supplemental
Benefits: A Look at Availability and Enrollment. The Commonwealth Fund. February 2021.
https://www.commonwealthfund.org/publications/issue-briefs/2021/feb/medicare-advantage-plans-
supplemental-benefits
145. Centers for Medicare & Medicaid Services. Fiscal Year (FY) 2022 Medicare Hospital Inpatient
Prospective Payment System (IPPS) and Long Term Care Hospital (LTCH) Rates Final Rule (CMS-1752-
F). April 2021. https://www.cms.gov/newsroom/fact-sheets/fiscal-year-fy-2022-medicare-hospital-
inpatient-prospective-payment-system-ipps-and-long-term-care-0
146. Health Resources & Services Administration. Corporation for Supportive Housing.
https://www.hrsa.gov/library/corporation-supportive-housing
147. Health Resources & Services Administration. National Center for Medical-Legal Partnership.
https://www.hrsa.gov/library/national-center-medical-legal-partnership
148. Health Center Resource Clearinghouse. Corporation for Supportive Housing (CSH).
https://www.healthcenterinfo.org/our-partners/corporation-for-supportive-housing-csh/
149. Yue D, Pourat N, Chen X, et al. Enabling Services Improve Access to Care, Preventative Services, and
Satisfaction Among Health Center Patients. Health Affairs. September 2019; 38(9). doi:
10.1377/hlthaff.2018.05228
150. Centers for Disease Control and Prevention The Public Health Approach to Violence Prevention.
January 2022. https://www.cdc.gov/violenceprevention/about/publichealthapproach.html
151. Centers for Disease Control and Prevention. Racial and Ethnic Approaches to Community Health
(REACH). February 2022. https://www.cdc.gov/nccdphp/dnpao/state-local-
programs/reach/index.htm
152. Centers for Disease Control and Prevention. Program Impact. March 2020.
https://www.cdc.gov/nccdphp/dnpao/state-local-programs/reach/program_impact/index.htm
153. Centers for Disease Control and Prevention. Accelerator Plans. October 2021.
https://www.cdc.gov/chronicdisease/programs-impact/sdoh/accelerator-plans.htm
154. Merrick MT, Ford DC, Ports KA, e tal. Vital Signs: Estimated proportion of adult health problems
attributable to Adverse Childhood Experiences and implications for prevention – 25 states, 2015-
2017. November 2019. MMWR Morbidity and Mortality Weekly Report, 68, 99-
1005.https://www.cdc.gov/mmwr/volumes/68/wr/mm6844e1.htm
155. Centers for Disease Control and Prevention. STEADI—Older Adult Fall Prevention. July 2021.
https://www.cdc.gov/steadi/index.html
156. Centers for Disease Control and Prevention. Community Health Workers for COVID Response and
Resilient Communities (CCR). December 2021. https://www.cdc.gov/covid-community-health-
workers/index.html

April 2022 REPORT 29
157. Centers for Disease Control and Prevention. Health Impact in 5 Years. February 2022.
https://www.cdc.gov/policy/hst/hi5/index.html
158. U.S. Department of Health and Human Services. The Guide to Community Preventive Services (The
Community Guide). Community Preventive Services Task Force.
https://www.thecommunityguide.org/
159. Centers for Disease Control and Prevention. Improving Social Determinants of Health—Getting
Further Faster. https://www.cdc.gov/chronicdisease/programs-impact/sdoh/pdf/GFF-eval-brief-
508.pdf
160. Administration for Community Living. Housing and Services Resource Center. December 2021.
https://acl.gov/HousingAndServices
161. Administration for Community Living. Nutrition Services. February 2022.
https://acl.gov/programs/health-wellness/nutrition-services
162. Kowlessar N, Robinson K, Schur C. Older Americans Benefit from Older Americans Act Nutrition
Programs. September 2015. Administration for Community Living.
https://acl.gov/sites/default/files/programs/2016-11/AoA-Research-Brief-8-2015.pdf
163. Administrative for Community Living. Title III Older Americans Act (OAA) State Performance Report
(SPR) and Older Americans Act Performance System (OAAPS). October 2021. https://acl.gov/news-
and-events/announcements/older-americans-act-oaa-state-program-performance-report-spr-
redesign
164. Administration for Community Living. National Survey of OAA Participants, 2019.
https://agid.acl.gov/datafiles/NPS/
165. Ibid.
166. Administration for Community Living. ACL Announces Social Care Referrals Challenge Phase 1
Awardees. November 2021. https://acl.gov/programs/acl-announces-social-care-referrals-challenge-
phase-1-awardees
167. Administration for Community Living. ACL Awards 2021 No Wrong Door Community Infrastructure
Grants. September 2021. https://acl.gov/news-and-events/announcements/acl-awards-2021-no-
wrong-door-community-infrastructure-grants
168. Administration for Community Living. ACL Grants Promote Inclusion and Cultural Competency Across
Disability Programs. October 2016. https://acl.gov/news-and-events/announcements/acl-grants-
promote-inclusion-and-cultural-competency-across
169. Administration for Children and Families, Office of Family Assistance. TANF Caseload Data 2019: Total
Recipients TANF and SSP-MOE Combined. August 2020. https://www.acf.hhs.gov/ofa/resource/tanf-
caseload-data-2019
170. Chaudry A, Wilmer C, Macartney S, et al. Poverty in the United States: 50-Year Trends and Safety Net
Impacts. Office of the Assistant Secretary for Planning and Evaluation. March 2016.
https://aspe.hhs.gov/sites/default/files/migrated_legacy_files//142581/50YearTrends.pdf
171. Administration for Children and Families, Office of Planning, Research & Evaluation. Using TANF
Funding to Provide Housing Assistance During the COVID-19 Pandemic. February 2022.
https://www.acf.hhs.gov/opre/report/using-tanf-funding-provide-housing-assistance-during-covid-
19-pandemic
172. Administration for Children and Families, Office of Child Support Enforcement. About the Office of
Child Support Enforcement. December 2021. https://www.acf.hhs.gov/css/about
173. Chaudry A, Wilmer C, Macartney S, et al. Poverty in the United States: 50-Year Trends and Safety Net
Impacts. Office of the Assistant Secretary for Planning and Evaluation. March 2016.
https://aspe.hhs.gov/sites/default/files/migrated_legacy_files//142581/50YearTrends.pdf

April 2022 REPORT 30
174. Administration for Children and Families. Head Start Program Facts: Fiscal Year 2019. April 2021.
https://eclkc.ohs.acf.hhs.gov/about-us/article/head-start-program-facts-fiscal-year-2019
175. Substance Abuse and Mental Health Services Administration. Homelessness Programs and Resources.
March 2019. https://www.samhsa.gov/homelessness-programs-resources
176. U.S. Department of Health and Human Services, Office of Disease Prevention and Promotion. Social
Determinants of Health. Healthy People 2030. https://health.gov/healthypeople/objectives-and-
data/social-determinants-health
