
AN EMPLOYER’S GUIDE TO
HEALTH AND DISABILITY
BENEFIT CIMS
EMPLOYEE BENEFITS SECURITY ADMINISTRATION
UNITED STATES DEPARTMENT OF LABOR

This publication has been developed by the U.S. Department of Labor,
Employee Benefits Security Administration (EBSA).
To view this and other publications, visit the agency’s Website at
dol.gov/agencies/ebsa.
To order publications, or to speak with a benefits advisor, contact EBSA
electronically at askebsa.dol.gov.
Or call toll free: 1-866-444-3272
This material will be made available in alternative format
to persons with disabilities upon request:
Voice phone: (202) 693-8664
TTY: (202) 501-3911
This booklet constitutes a small entity compliance guide for purposes of the
Small Business Regulatory Enforcement Fairness Act of 1996.

Introduction
If you’re an employer and you sponsor a group health or disability benet plan covered by the
Employee Retirement Income Security Act (ERISA), your plan must meet the minimum standards for
benet claims procedures set by rules issued by the Department of Labor.
Among other things, these standards include requirements for:
•
Processing benet claims;
•
The timeframes for deciding claims;
•
Notices of benet denials, reductions, or terminations; and
•
The standards for appeals.
If you are a duciary to an ERISA-covered group health or disability benet plan (including insured
and self-funded plans), you must maintain the plan’s claims procedures. Even if you hire benets
professionals or insurance companies to process claims, you need to understand the requirements
before selecting service providers who will be able to comply with the benet claims standards.
This booklet addresses ERISA’s claims procedures for private-sector group health and disability
plans (plans sponsored by government entities and churches are not covered by ERISA). It provides a
simplied explanation of the law and regulations. It is not a legal interpretation of ERISA, nor is it a
substitute for the advice of a legal professional.
Informing Participants and Beneficiaries about the Plan’s
Claims Procedures
Every employee benet plan must establish and maintain reasonable procedures for benets claims.
Plan administrators must provide these claims procedures to plan participants and beneciaries
when they enroll. Typically, this is done through the Summary Plan Description (SPD), a plain
language explanation of the plan. The SPD informs participants of how the plan works, the benets it
provides, and how they can le a claim for benets. Sometimes claims procedures are contained in a
separate booklet that is handed out with the SPD. The SPD or claims procedure booklet must include
information on where to le, what to le, and whom participants and beneciaries can contact with
questions about the plan.
If the plan is collectively bargained, the collective bargaining agreement may also include information
on claim ling, grievance, and appeal procedures.
What is a Claim?
A claim for benets is a request for a plan benet made in accordance with the plan’s procedures by a
claimant (participant or beneciary) or their authorized representative. If an authorized representative
les the claim, the plan can require the claimant to complete a form to name the representative.
However, in the case of a claim involving urgent care, the treating physician can automatically act as
the claimant’s authorized representative without having to complete a form.
AN EMPLOYER’S GUIDE TO HEALTH AND DISABILITY BENEFIT CLAIMS
1
Casual inquiries, including questions about plan benets, coverage, and eligibility, are generally not
considered claims for benets.
Plans generally cannot charge any ling fees or costs for ling claims and appeals.
Plans must decide all health and disability benet claims within a specic time limit, depending
on the type of claim led. The time limits are counted in calendar days, including weekends and
holidays. These limits do not govern when the benets must be paid or provided. Plans are required
to pay or provide benets within a reasonable time after a claim is approved. Below is a discussion
of how the claims procedure rules apply to health benets. For information on the rules that apply to
disability benets turn to page 7.
Health Benefit Claims
Types of Health Benefit Claims
There are three types of group health claims under the Department’s rule − urgent care, pre-service,
and post-service.
Urgent care claims are a special kind of pre-service claim that requires a quick decision because the
participant or beneciary’s health would be threatened if the plan took the normal time permitted to
decide a pre-service claim. If a physician with knowledge of the medical condition tells the plan that a
pre-service claim is urgent, the plan must treat it as an urgent care claim.
Pre-service claims are requests for approval required before medical care, such as preauthorization
or a decision on whether a treatment or procedure is medically necessary.
Post-service claims are all other claims for benets under a group health plan, including claims after
medical services have been provided, such as requests for reimbursement or payment for the provided
services. Most claims for group health benets are post-service claims.
UNITED STATES DEPARTMENT OF LABOR
2
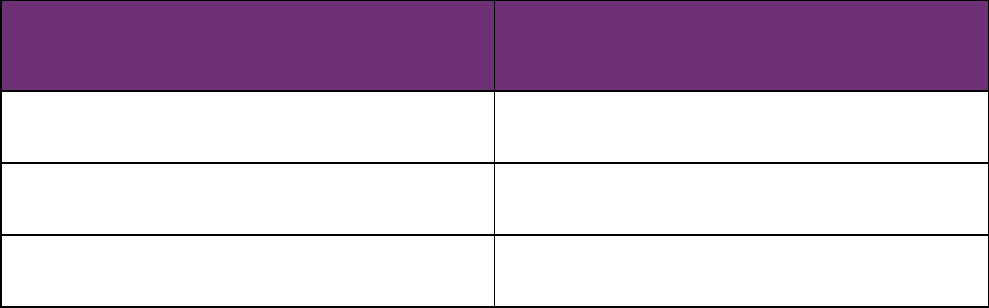
Deadline for Making an Initial Determination of a Health Benefit Claim
The timeframe for a plan to provide notice of a claim determination varies based on the type of claim
led.
CLAIM TYPE
DEADLINE FOR MAKING INITIAL
DETERMINATION
Urgent care
As soon as possible, and no later than 72 hours
after receiving the claim
Pre-service Within a reasonable time period, and no later than
15 days after receiving the claim*
Post-service Within a reasonable time period, and no later than
30 days after receiving the claim*
*Please note: A plan may extend the deadline for making a determination under specific circumstances.
Urgent care claims must be decided as soon as possible, taking into account the patient’s medical
needs, and no later than 72 hours after the plan receives the claim.
If the plan needs more information, it must tell the claimant within 24 hours and give the claimant
at least 48 hours to respond. Then the plan must decide the claim within 48 hours after receiving
the missing information or within 48 hours of the deadline for the claimant to supply the missing
information, whichever comes rst. The plan cannot extend the deadline to make the initial decision
without the claimant’s consent. The plan must notify the claimant that the claim has been granted
or denied before the end of the allotted time. The plan may notify the claimant orally as long as it
furnishes a written notication within three days after the oral notication.
Pre-service claims must be decided within a reasonable time period appropriate to the medical
circumstances, and no later than 15 days after the plan receives the claim.
The plan may extend the time period up to 15 days more if, for reasons beyond its control, the plan
cannot make the decision within the rst 15 days. The plan must notify the claimant before the rst 15-
day period ends:
•
Explaining the reason for the delay;
•
Requesting any additional information; and
•
Advising the claimant when it expects to make the decision.
If the plan requests more information, the claimant has at least 45 days to supply it. The plan then must
decide the claim within 15 days after receiving the additional information or within 15 days of the
deadline for the claimant to supply the additional information, whichever comes rst. The plan cannot
extend the deadline without the claimant’s consent. The plan must notify the claimant in writing that
the claim has been granted or denied before the deadline for the decision.
UNITED STATES DEPARTMENT OF LABOR
AN EMPLOYER’S GUIDE TO HEALTH AND DISABILITY BENEFIT CLAIMS
3
Post-service health claims must be decided within a reasonable time period, and no later than 30
days after the plan receives the claim.
The plan may extend the time period up to 15 days more if, for reasons beyond its control, the plan
cannot make the decision within the rst 30 days. However, the plan administrator must notify the
claimant before the rst 30-day period ends:
•
Explaining the reason for the delay;
•
Requesting any additional information needed; and
•
Advising the claimant when the plan expects to make a decision.
If the plan requests more information, the claimant has at least 45 days to supply it. The plan must
then decide the claim within 15 days after receiving the additional information or within 15 days after
the deadline for the claimant to supply the additional information, whichever comes rst. The plan
cannot extend the deadline without the claimant’s consent.
The plan must notify the claimant that the claim has been denied in whole or in part (paying anything
less than 100 percent of a claim is a denial in part) before the deadline for the decision.
Health Benefit Claims Denial Notices
If a plan denies a claim, it must send a denial notice to the claimant, either in writing or electronically.
The notice must include:
•
Specic reasons for denial (for example, not medically necessary, not covered by the plan, or
reached maximum amount of treatment permitted under the plan);
•
A reference to any specic plan provisions relied upon for the denial;
•
If denied for a lack of information, a description of any additional material needed and an
explanation of why it’s necessary;
•
A description of the plan’s review procedures (for example, how appeals work and/or how to
initiate an appeal);
•
If denied based on rules, guidelines, or protocols, either a description of the rules, guidelines,
or protocols relied upon in denying the claim, or a statement that a free copy of such items will
be provided upon request;
•
If denied based on medical necessity or experimental treatment or similar exclusion or limit, an
explanation of the scientic or clinical judgment for the denial, applying the terms of the plan
to the claimant’s medical circumstances, or a statement that an explanation will be provided for
free upon request; and
•
A description of the claimant’s right to go to court to recover benets due under the plan.
Reviewing an Appeal of a Denied Health Benefit Claim
Plans must give claimants at least 180 days to le an appeal. Appeals must be reviewed by someone
new who looks at all of the information submitted and consults with qualied medical professionals
UNITED STATES DEPARTMENT OF LABOR
4
if a medical judgment is involved. This reviewer cannot be the same person who made the initial
decision or that person’s subordinate, and the reviewer must give no consideration to the initial
decision.
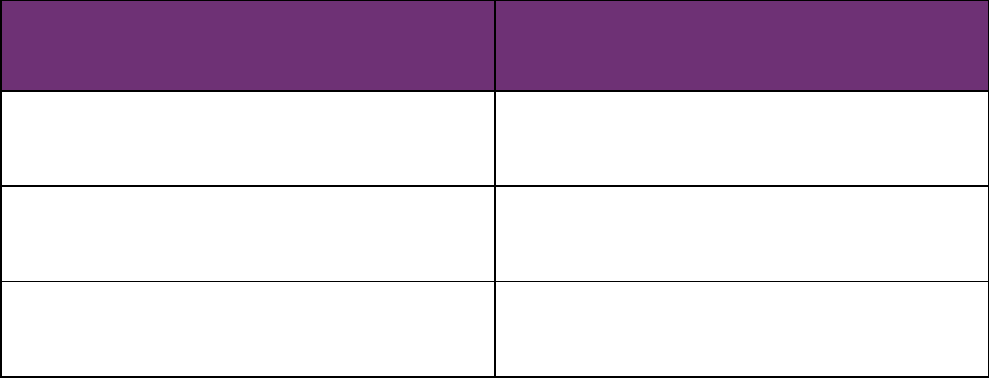
The timeframe for a plan to review appeals varies based on the type of claim led.
CLAIM TYPE DEADLINE FOR REVIEWING AN APPEAL
Urgent care As soon as possible, taking into account the
patient’s medical needs, and no later than 72 hours
after receiving the request to review a denied claim
Pre-service Within a reasonable time period appropriate to the
medical circumstances, and no later than 30 days
after receiving the request to review a denied claim*
Post-service Within a reasonable time period, and no later than
60 days after receiving the request to review a
denied claim*
*Please note: A plan may extend the timeline for reviewing an appeal with the claimant’s consent.
The plan cannot extend the deadline without the claimant’s consent. Also, there are two exceptions to
these deadlines:
•
Single-employer collectively bargained plans generally may use a collectively bargained
grievance process for their claims appeal procedure if it has provisions on ling, determination,
and review of benet claims.
•
Multiemployer collectively bargained plans have special timeframes to allow them to
schedule reviews on appeal of post-service claims for the regular quarterly board of trustee
meetings.
Plans can require no more than two levels of review. If a plan requires two levels of review, the
maximum time period for each review generally is half of the time period permitted for one review.
For example, a group health plan with one appeal level must review a pre-service claim within a
reasonable period of time appropriate to the medical circumstances and no later than 30 days after
the plan receives the appeal. If the plan requires two appeals, each review must be completed within
15 days for pre-service claims. If a claim on appeal is still denied after the rst review, the plan must
allow the claimant a reasonable period of time (but not a full 180 days) to le for the second review.
UNITED STATES DEPARTMENT OF LABOR
AN EMPLOYER’S GUIDE TO HEALTH AND DISABILITY BENEFIT CLAIMS
5
Notice of Denial of a Health Benefit Claim on Appeal
Once a plan makes a nal denial of a claim on appeal, the plan must send the claimant a written notice
of the decision. The notice must include:
•
The specic reasons the claim was denied on appeal;
•
A reference to the plan provisions on which the decision is based;
•
A description of any voluntary processes the plan offers to resolve claims disputes;
•
An explanation of the claimant’s right to receive documents relevant to the benet claim
(documents and records upon which the decision is based and other documents prepared or
used during the process), free of charge; and
•
A description of the claimant’s rights to seek judicial review of the plan’s decision.
The plan’s claims procedure must provide for a full and fair review of a benet claim if a claimant
les an appeal of the denial. In addition to following the standards outlined above, the reviewer must
consult with a qualied health professional (and others as needed) when the denial is based on a
determination of whether a particular treatment, drug, or other item is experimental, investigational,
or not “medically necessary”. In addition, mandatory binding arbitration of claims is generally
prohibited. However, non-binding arbitration is permissible if done within the required timelines.
Additional Rules for Plans Not Grandfathered Under the Affordable
Care Act
Plans that are not grandfathered under the Affordable Care Act (those established, or that have
made certain signicant changes, after March 23, 2010) must comply with additional internal
claims procedure requirements. The claims and appeal process must cover rescissions (retroactive
cancellations) of coverage, as well as other denials of benets. They, or their insurers, also must:
•
Provide claimants with new or additional evidence or rationale, and a reasonable opportunity
to respond to it, before making a nal decision on the claim;
•
Ensure that claims and appeals are adjudicated in an independent and impartial manner;
•
Provide detail in all claims denial notices on the claim involved, the reason for denial
(including the denial code and meaning), any available internal and external appeals processes,
and consumer assistance information;
•
Provide, on request, diagnosis and treatment codes (and their meanings) for any denied claim;
•
Provide notices in a culturally and linguistically appropriate manner;
•
Allow claimants to begin the external review process if the plan fails to follow the internal
claims requirements (unless the plan’s violation is minimal); and
•
Allow claimants to resubmit a claim through the internal claims process if a request for
immediate external review is rejected by the external reviewer under specic circumstances.
More information on the Affordable Care Act requirements of the claims and appeal process, including
model notices, can be found in Appendix A and Appendix C of the Department’s publication,
Compliance Assistance Guide – Health Benets Coverage Under Federal Law.
UNITED STATES DEPARTMENT OF LABOR
6
If a Claimant’s Health Benefit Appeal Is Denied
Claimants normally must complete the plan’s internal claim process before ling an action in court to
challenge the denial of a claim for benets. However, a claimant who believes that the plan failed to
establish or follow a claims procedure consistent with the Department’s rules described in this booklet
may have the right to ask a court to review the benet claim without waiting for a decision from the
plan.
In addition, plans not grandfathered under the Affordable Care Act must provide for external review
of claim denials by an independent party. The external review process used by the plan depends on
whether the plan is self-funded or provides benets through an insurance company.
Self-funded plans generally must comply with the procedures set by the Department of Labor. A plan
may choose to refer requests for external review to an accredited Independent Review Organization,
or may voluntarily comply with a state external review process if the state allows access. For more
information, visit the Department of Labor’s page on internal claims and appeals and external review
at
dol.gov/agencies/ebsa/laws-and-regulations/laws/aordable-care-act/for-employers-
and-advisers/internal-claims-and-appeals
.
Insured plans and insurance companies generally must comply with their state’s external review
process, if the state process includes minimum consumer standards set by the Department of Health
and Human Services (HHS). If the state process does not meet these standards, group health plans
and insurers may use either the accredited Independent Review Organization process or an HHS-
administered Federal external review process. For the status of your state’s external process, see
cms.gov/CCIIO/Resources/Files/external_appeals.html.
Disability Benefit Claims
Disability benet claims are requests for benets where the plan must make a determination of
disability to decide the claim. If benets under a plan are conditioned on someone other than the plan
making a disability determination, then the special rules for disability claims discussed below do not
apply. For example, if a pension plan provides that pension benets will be paid to a person who has
been determined to be disabled by the Social Security Administration or under the employer’s long-
term disability plan, then a claim for such pension benets is covered by the ERISA rules for pension
claims, not the rules for disability claims.
UNITED STATES DEPARTMENT OF LABOR
AN EMPLOYER’S GUIDE TO HEALTH AND DISABILITY BENEFIT CLAIMS
7
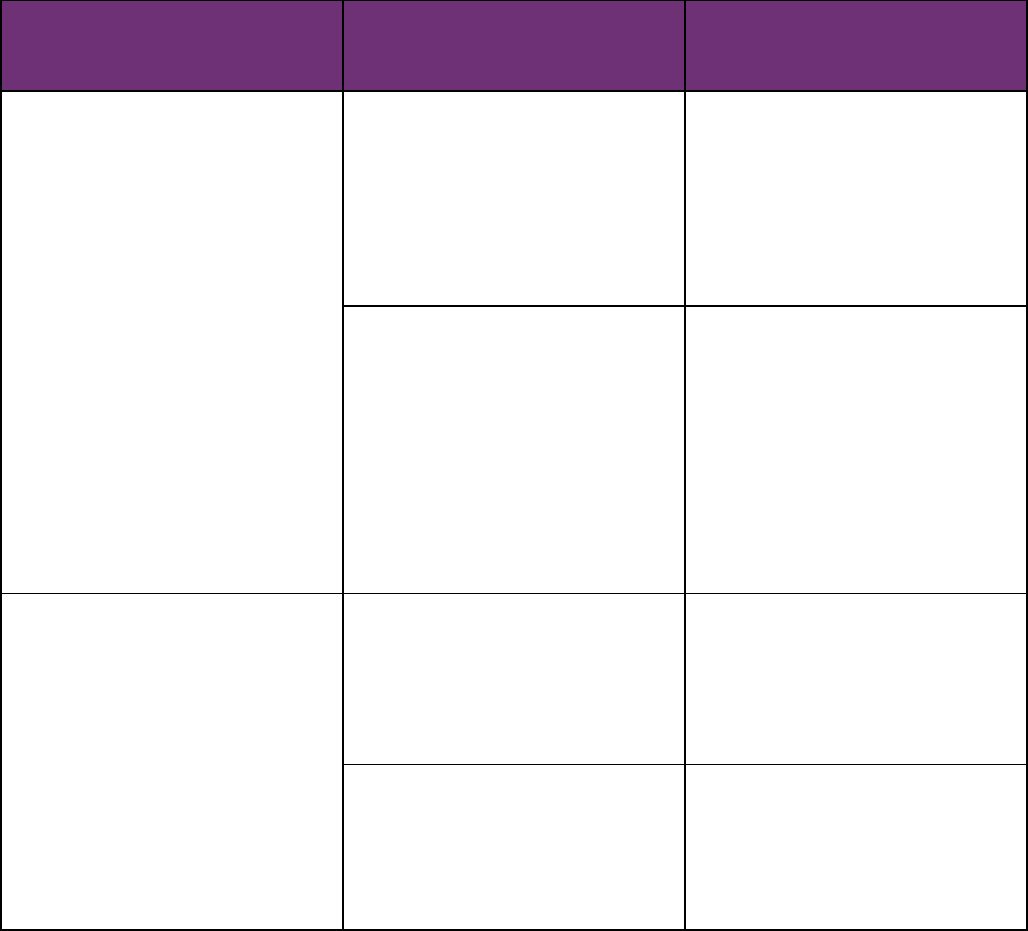
Deadline for Deciding a Disability Claim
Disability claims must be decided within a reasonable time period, but no later than 45 days after the
plan receives the claim. There are some circumstances that could extend the timeline:
IF… AND THE PLAN…
THEN THE PLAN CAN
EXTEND THE DEADLINE
FOR MAKING A DECISION…
The plan needs more time to review,
for reasons beyond its control
• Tells the claimant, within the
initial 45-day period, that it
needs more time,
• Explains why,
• Does not request any additional
information needed, and
• Tells the claimant when it plans
tomakeanaldecision
Up to 30 days
• Tells the claimant, within the
initial 45-day period, that it
needs more time,
• Explains why,
• Requests additional
information (in which case the
plan must give the claimant
at least 45 days to supply the
information), and
• Tells the claimant when it plans
tomakeanaldecision
Up to 30 days after receiving the
information OR when the time
period to provide the information
ends,whichevercomesrst
The plan still needs more time to
reviewaftertherstextension
• Notiestheclaimantbeforethe
rstextensionexpires
Up to 30 days more
• Notiestheclaimantbeforethe
rstextensionexpires
• Requests additional
information (giving the claimant
at least 45 days to supply the
information)
Up to 30 days after receiving the
information OR when the time
period to provide the information
ends,whichevercomesrst
For any additional extensions, the plan needs the claimant’s consent. The plan must notify the claimant
whether the claim has been denied before the deadline for the decision.
UNITED STATES DEPARTMENT OF LABOR
8
Disability Claims Denial Notices
If a plan denies a claim, it must send a denial notice to the claimant, either in writing or electronically.
The notice must include:
•
A detailed explanation of why the claim was denied. If applicable, the notice must explain
why the plan disagreed with the views of a medical professional or vocational expert
(including those who treated the claimant and those whose advice was obtained by the plan),
or a disability determination made by the Social Security Administration;
•
A reference to the specic plan provisions on which the denial is based;
•
A statement that the claimant is entitled to receive, upon request and at no cost, reasonable
access to all documents relevant to the claim, and copies of them;
•
The plan rules, guidelines, protocols, standards, or other similar criteria relied upon in
denying the claim, or a statement that none exist; and
•
A description of the plan’s appeal process, including the time limits involved, and a statement
of the claimant’s right to pursue the claim in court if it is denied on appeal.
Reviewing an Appeal of a Denied Disability Claim
Claimants have at least 180 days to le an appeal. Appeals must be reviewed by someone new
who looks at all of the information submitted and consults with qualied medical professionals if a
medical judgment is involved. This reviewer cannot be the same person who made the initial decision
or that person’s subordinate, and the reviewer must give no consideration to the initial decision.
Disability appeals must be reviewed within a reasonable period of time, but not later than 45
days after the plan receives the request to review a denied claim. If the plan determines special
circumstances justify an extension, the plan may take up to an additional 45 days to decide the
appeal. However, the plan rst must notify the claimant in writing during the rst 45-day period,
explaining the special circumstances and the date by which the plan expects to make the decision.
There are two exceptions to these time limits:
•
Single-employer collectively bargained plans generally may use a collectively bargained
grievance process for their claims appeal procedure if it has provisions on ling,
determination, and review of benet claims.
•
Multiemployer collectively bargained plans have special timeframes to allow them to
schedule reviews on appeal for the regular quarterly board of trustee meetings.
A plan cannot deny a claimant’s appeal based on new or additional evidence or rationales that were
not included when the benet was rst denied, unless the plan noties the claimant and gives them a
reasonable opportunity to respond before the date the plan’s decision is due.
Plans can require no more than two levels of review. If a plan requires two levels of review, the
maximum time period for each review generally is half of the time period permitted for one review.
UNITED STATES DEPARTMENT OF LABOR
AN EMPLOYER’S GUIDE TO HEALTH AND DISABILITY BENEFIT CLAIMS
9
For example, a plan with one appeal level must review a disability claim within a reasonable period of
time and no later than 45 days after receiving the appeal. If the plan requires two appeals, both reviews
must be completed within 45 days. If a claim on appeal is still denied after the rst review, the plan
must allow the claimant a reasonable period of time (but not a full 180 days) to le for the second
review.
Notice of Denial of a Disability Claim on Appeal
Once the plan makes a nal decision on the claim, it must send the claimant a written notice of the
decision. The notice must include:
•
A detailed explanation of why the claim was denied. If applicable, the notice must explain
why the plan disagreed with the views of a medical professional or vocational expert (including
those who treated the claimant and those whose advice was obtained by the plan), or a disability
determination made by the Social Security Administration;
•
A reference to the specic plan provisions on which the decision is based;
•
Information on any additional voluntary levels of appeal;
•
An explanation of the claimant’s right to receive documents that are relevant to the benet
claim, free of charge;
•
The plan rules, guidelines, protocols, standards, or other similar criteria relied upon in denying
the claim, or a statement that none exist; and
•
A description of the claimant’s rights to seek judicial review of the plan’s decision, including a
description of any contractual limitations period that applies to the right to bring an action, and
the calendar date on which the claim’s contractual limitations period expires.
If a Claimant’s Disability Appeal Is Denied
Normally, the claimant must complete the plan’s claim process before ling an action in court to
challenge the denial of a claim for benets. However, the claimant can immediately pursue the claim
in court if the plan failed to establish or does not follow the claims processing rules (unless the plan’s
violation is minimal). If a court rejects the request for immediate review of a denied claim, the plan
must treat the claim as re-led on appeal.
Additional Requirements for Disability Claims and Appeals
The plan must ensure that both claims and appeals are adjudicated in an independent and impartial
manner. For example, a person deciding a claim, or any medical or vocational expert involved in the
decision, cannot be hired, promoted, terminated or compensated based on the likelihood that person
will support the denial of benets.
If a claimant lives in a county where 10 percent or more of the population is literate only in the same
non-English language, the plan must provide oral language assistance in that language and provide
written notices in that language upon request. In such counties, benet denial notices must include a
prominent statement in the relevant non-English language about the availability of language assistance.
UNITED STATES DEPARTMENT OF LABOR
10

Claimants are permitted to pursue their claim in court if the plan fails to follow the claims procedure
requirements (unless the plan’s violation is minimal).
These rules apply also to certain rescissions (meaning a retroactive cancellation or discontinuance) of
disability coverage. Rescissions for non-payment of premiums are not covered by these rules.
Resources
Employer Publications
UNITED STATES DEPARTMENT OF LABOR
AN EMPLOYER’S GUIDE TO HEALTH AND DISABILITY BENEFIT CLAIMS
11
•
Compliance Assistance - Group Health and Disability Plans Benet Claims Procedure
Regulation
•
Understanding Your Fiduciary Responsibilities Under a Group Health Plan
•
Compliance Assistance Guide – Health Benets Coverage Under Federal Law
•
Reporting and Disclosure Guide For Employee Benet Plans
Employee Publications
•
Filing a Claim for Your Health Benets
•
Filing a Claim for Your Disability Benets
•
Top 10 Ways to Make Your Health Benets Work for You
•
Life Changes Require Health Choices...Know Your Benet Options
•
Work Changes Require Health Choices...Protect Your Rights
Order publications, ask questions, or request assistance from a benefits advisor:
Main site: dol.gov/agencies/ebsa
Ask EBSA: askebsa.dol.gov
Toll-free: 1-866-444-3272
TTY: 202-501-3911

EMPLOYEE BENEFITS SECURITY ADMINISTRATION
UNITED STATES DEPARTMENT OF LABOR
September 2018
