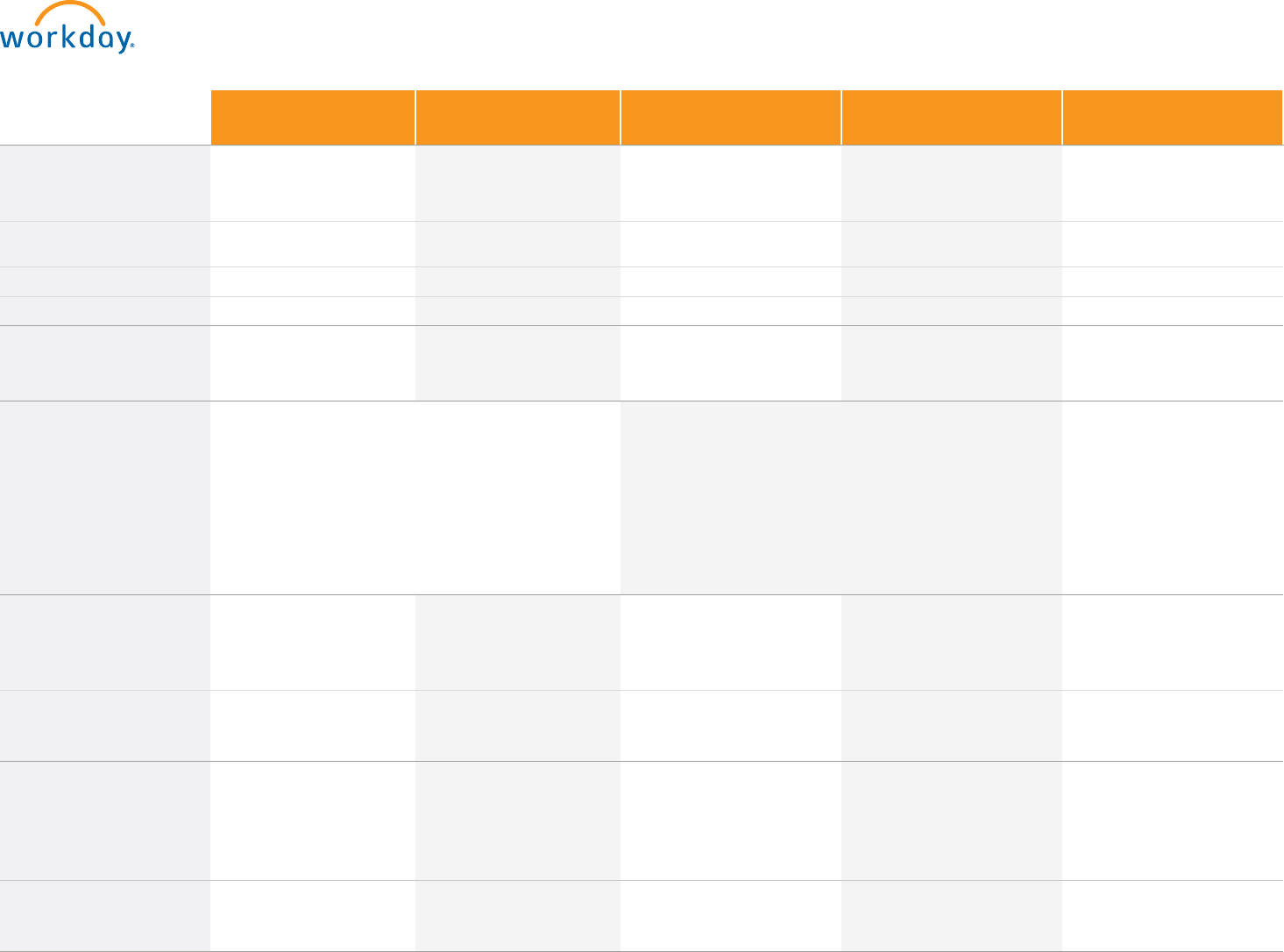
Cigna Smart Plan
With HSA
Cigna Core Plan
Kaiser Smart Plan With
HSA (CA, CO, & GA)
Kaiser HMO
(CA, CO, & GA)
SimplePay Health
Your Contributions
(24 pay periods)
EE Only $0.00 $12.50 $0.00 $12.50 $0
EE + Spouse / Domestic
Partner
$17.50 $112.50 $20.00 $100.00 $0
EE + Child(ren) $17.50 $97.50 $20.00 $85.00 $0
EE + Family $25.00 $210.00 $30.00 $155.00 $0
Workday Annual Funding
of HSA
1
• $1,000 Employee Only
• $2,000 Employee +
Dependent(s)
N/A • $1,000 Employee Only
• $2,000 Employee +
Dependent(s)
N/A N/A
Provider Choice You can go to any provider you like; however, you will benefit
from negotiated rates and higher benefit levels when you use
Cigna Open Access Plus (OAP) network providers.
2
Some
services are not covered out-of-network.
You must use Kaiser Permanente providers,
except in case of urgent or emergency care.
You can go to any provider
you like; however, you will
benefit from lower Tier rates
when you use Aetna Choice
POS II Network providers.
3
ͥ Tier 1:
Meets all standards
4
ͥ Tier 2:
Meets most standards
4
ͥ Tier 3:
Meets minimum standards
4
Calendar-Year Deductible
In-Network • $1,600 Employee Only
• $3,200 Employee +
Dependent(s)
• $500 Individual
• $500 Individual in Family
• $1,000 Entire Family
• $1,600 Individual
• $3,200 Individual in Family
• $3,200 Entire Family
None None
Out-of-Network • $3,200 Employee Only
$6,400 Employee +
Dependent(s)
• $1,000 Individual
• $1,000 Individual in Family
• $2,000 Entire Family
N/A N/A None
Calendar-Year
Out-of-Pocket Maximum
In-Network • $3,200 Individual
• $3,200 Individual in Family
• $6,400 Entire Family
• $3,000 Individual
• $6,000 Family
• $4,000 Individual
• $4,000 Individual in Family
• $6,850 Entire Family
• $1,500 Individual
• $1,500 Individual in Family
• $3,000 Entire Family
• $2,000 Individual
• $2,000 Individual in Family
• $4,000 Family
Out-of-Network • $10,000 Individual
• $10,000 Individual in Family
• $20,000 Entire Family
• $8,000 Individual
• $16,000 Family
N/A N/A N/A
Comparing Your 2024 Medical Plan Options
January 2024
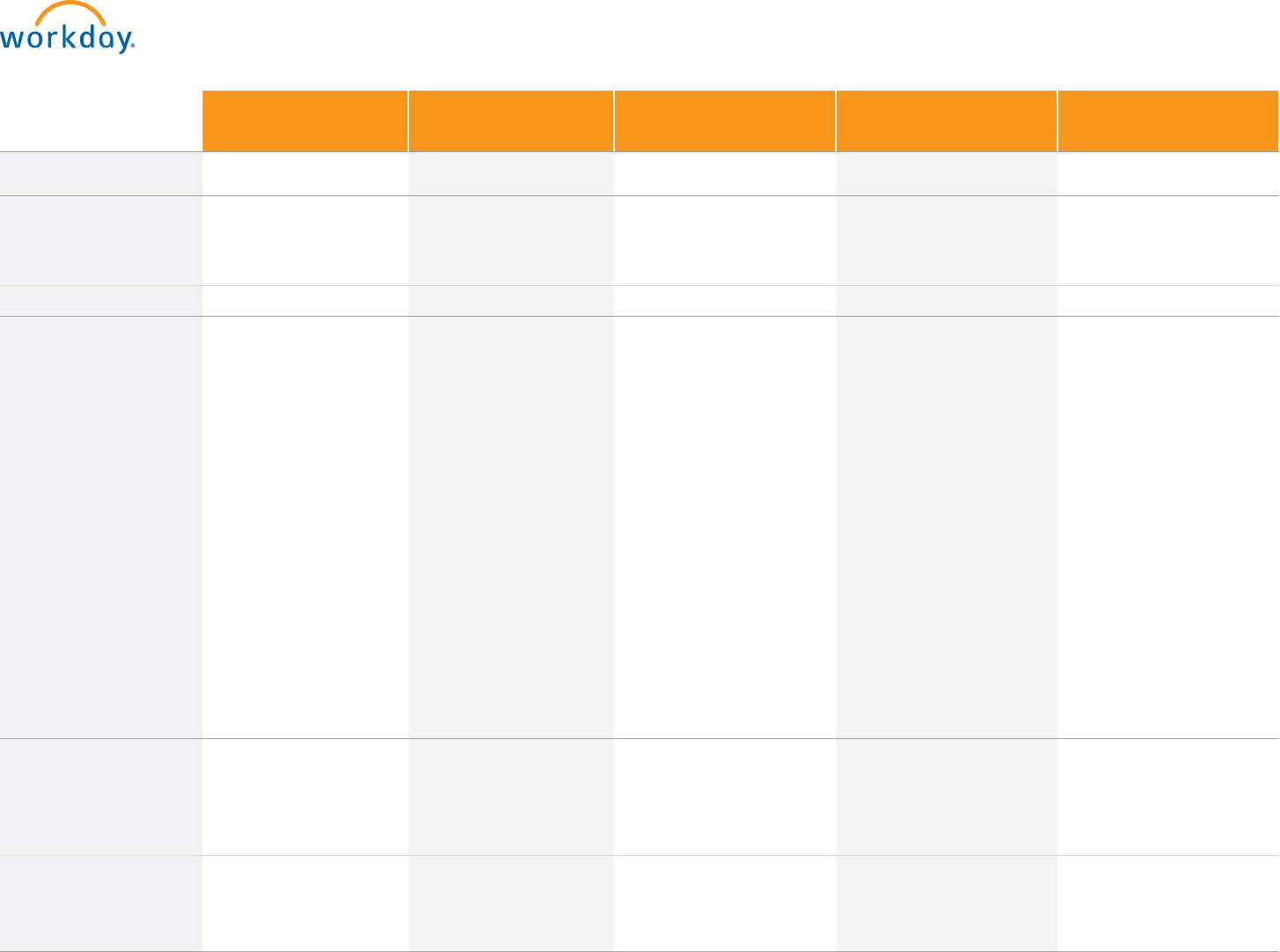
Cigna Smart Plan
With HSA
Cigna Core Plan
Kaiser Smart Plan With
HSA (CA, CO, & GA)
Kaiser HMO
(CA, CO, & GA)
SimplePay Health
Preventive Care $0 in-network $0 in-network $0 in-network $0 in-network $0 in-network
Office Visits You pay: You pay: You pay: You pay: You pay:
In-Network 20% after deductible $20 PCP / $30 Specialist 20% after deductible $20 PCP / $20 Specialist
ͥ $15 PCP / $30 Specialist
ͥ $20 PCP / $40 Specialist
ͥ $30 PCP / $65 Specialist
Out-of-Network 50% after deductible
5
40% after deductible
5
N/A N/A $35 PCP / $80 Specialist
3
Other Medical Expenses
See footnotes 3 and 5 for
more information about
limits on out-of-network
benefit payments.
You pay a percentage of the
charge for most services,
after the deductible:
Inpatient Hospital:
• Network: 20%
• Non-Network: 50%
ER: 20%
Urgent Care:
• Network: 20%
• Non-Network: 20%
Outpatient Surgery:
• Network: 20%
• Non-Network: 50%
Lab and X-Ray (if done
outside a doctor’s office):
• Network: 20%
• Non-Network: 50%
You pay a copay for these
services:
ER: $150 (waived if admitted)
Urgent Care:
• Network: $50
(waived if admitted)
• Non-Network: $50
(waived if admitted)
You pay a percentage of the
charges for these services,
after the deductible:
Inpatient Hospital:
• Network: 20%
• Non-Network: 40%
Outpatient Surgery:
• Network: 20%
• Non-Network: 40%
Lab and X-Ray (if done
outside a doctor’s office):
• Network: 20%
• Non-Network: 40%
You pay a percentage of the
charges for most services,
after the deductible:
Inpatient Hospital: 20%
ER: 20%
Urgent Care: 20%
Outpatient Surgery: 20%
Lab and X-Ray: 20%
You pay a copay for most
services:
Inpatient Hospital:
$250 per admission
ER: $100
(waived if admitted)
Urgent Care: $20
Outpatient Surgery:
$100 per procedure
Lab and X-Ray:
No charge
You pay a set amount for
most services:
Inpatient Hospital:
ͥ $1,140
ͥ $1,520
ͥ $2,000
Non-Network: $2,640
3
ER: $115
Urgent Care:
ͥ $30
ͥ $40
ͥ $65
Non-Network: $80
3
Outpatient Surgery:
ͥ $465
ͥ $615
ͥ $1,030
Non-Network: $1,235
3
Routine Lab and X-Ray:
ͥ $10
ͥ $15
ͥ $20
Non-Network: $25
3
Behavioral Health
In-Network 20% after deductible Office Visits: $30 copay
Other Services: 20% after
deductible
20% after deductible $20 copay Office Visits
ͥ $15
ͥ $20
ͥ $30
Out-of-Network Office Visits: 20% after
in-network deductible
5
Other Services: 50% after
out-of-network deductible
5
Office Visits: 20% after
in-network deductible
5
Other Services: 40% after
out-of-network deductible
5
Not covered without prior
approval
Not covered without prior
approval
Office Visits: $35
3
Comparing Your 2024 Medical Plan Options
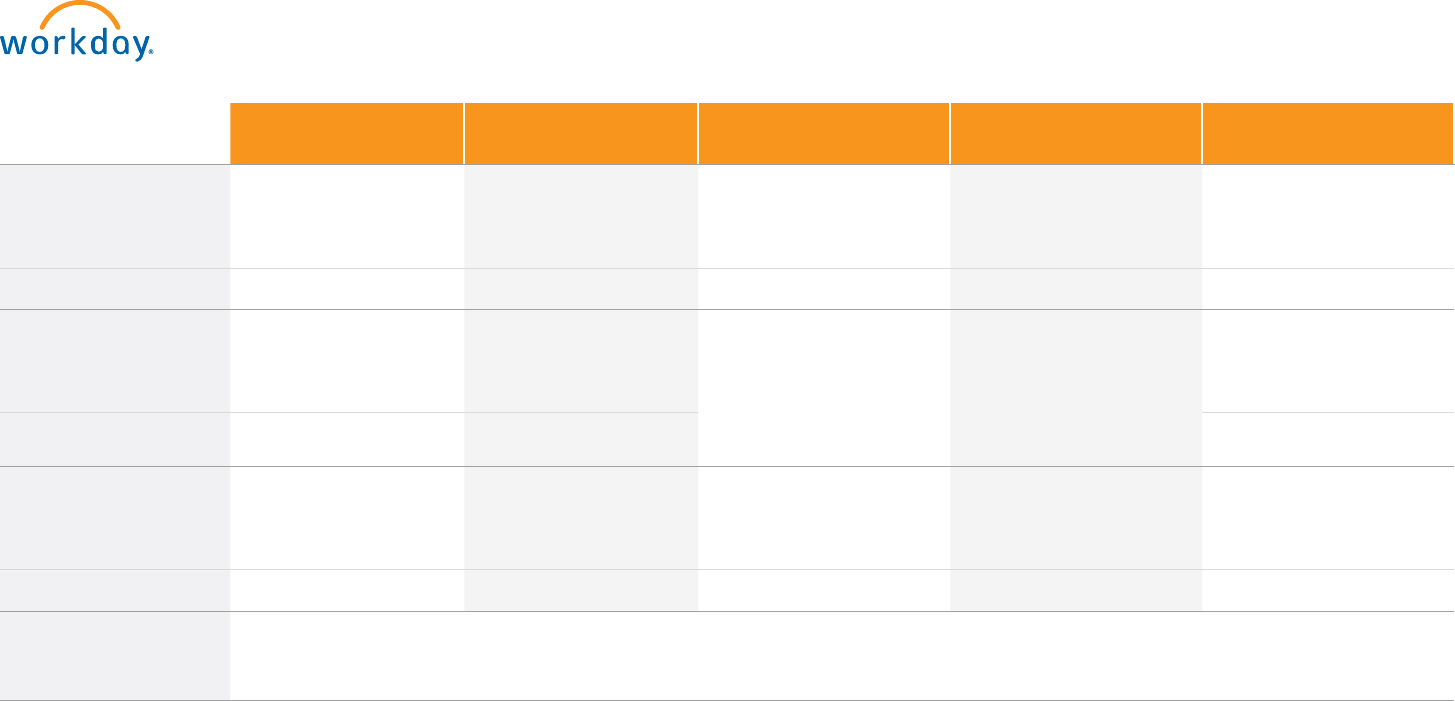
Comparing Your 2024 Medical Plan Options
Cigna Smart Plan
With HSA
Cigna Core Plan
Kaiser Smart Plan With
HSA (CA, CO, & GA)
Kaiser HMO
(CA, CO, & GA)
SimplePay Health
Chiropractic Care
In-Network 20% after deductible $30 copay $15 copay after deductible
(limit 30 visits per calendar year)
$15 copay
(limit 30 visits per calendar year)
ͥ $30
ͥ $40
ͥ $65
Out-of-Network 50% after deductible 40% after deductible N/A N/A $80
3
Acupuncture
In-Network 20% after deductible $30 copay Network Only: 20% after
deductible
(limited to treatment of nausea
or as part of comprehensive
pain management program for
the treatment of chronic pain)
Network Only: $20 copay
(limited to treatment of nausea
or as part of comprehensive
pain management program for
the treatment of chronic pain)
ͥ $30
ͥ $40
ͥ $65
Out-of-Network 50% after deductible 40% after deductible $80
3
Physical Therapy
In-Network 20% after deductible $20 PCP / $30 Specialist /
$30 Cardiac
20% after deductible $20 per outpatient visit
ͥ $30
ͥ $40
ͥ $65
Out-of-Network 50% after deductible 40% PCP / 40% Specialist N/A N/A $80
3
Family Planning
Services
All plans provide coverage for treatment of infertility. Please contact each carrier for coverage details.
Family planning benefits are administered for Workday by Maven Wallet and include a $25,000 lifetime reimbursement allowance for IVF or IUI, egg freezing, adoption,
or surrogacy.
NOTES
These charts provide a brief overview of benefits and coverage for the medical plans. You should also review the detailed disclosure and summary documents for each plan, available at
WorkdayBenefits.com. For questions about a specific procedure, service, or provider, please contact the medical plan directly. In the event of any inconsistency between this material, the Plan
Document, and the terms of the plans or programs, the terms of the plans or programs will control.
1
A portion of Workday’s contribution will be deposited into your HSA each pay period (24 pay periods). If you enroll midyear, the Workday contribution to your HSA will be reduced or prorated.
2
Workmates in Utah should select PPO (not Open Access Plus) from the list of options when looking for in-network providers on Cigna’s website. PPO is the network name. The name and network of
providers are different in Utah; however, the benefits and costs are the same as shown here.
3
When you use an in-network provider, you’ll know your copay in advance. Keep in mind that some services, like experimental treatments, aren’t covered. However, if you receive care from an out-of-
network provider, you’re responsible for a copay, PLUS any amount your provider may bill you above the usual and customary rate—an average of what providers usually charge insurance companies
for the service in that region. Since the cost of care varies among providers, you won’t always know ahead of time how much you’d pay out of pocket for out-of-network services. The SimplePay Health
plan does NOT have an annual out-of-pocket maximum for out-of-network services, therefore it’s strongly recommended that you stay in-network (except in emergencies).
4
Standards are based on quality, relationship, experience, and efficiency criteria. Visit employers.simplepayhealth.com/workday for more information.
5
Member is responsible for any amount billed by their provider that exceeds the plan’s maximum reimbursable charges (MRC). Billed amounts in excess of MRC do not apply toward the deductible or
out-of-pocket maximum.
Your prescription drug coverage is included as part of the medical plan option you select.
• Cigna medical plan: Prescription drug benefits will be administered by CVS Caremark. To find cost information about your prescriptions, check the CVS Caremark formulary, available on
WorkdayBenefits.com. When you look up your prescriptions, check for prior-authorization requirements, quantity limits, and timing limits.
• Kaiser medical plan: Kaiser is also the administrator for the prescription drug coverage.
• SimplePay Health: Prescription drug benefits will be administered by CVS Caremark; however, you will pay SimplePay Health for any out-of-pocket costs. To find cost information about your
prescriptions, visit employers.simplepayhealth.com/workday. When you look up your prescriptions, check for prior-authorization requirements, quantity limits, and timing limits.
You should always consider using an in-network pharmacy to get the best price. You can access a list of pharmacies through your plan’s website or by calling the plan’s member services.
WHAT ARE PRESCRIPTION DRUG CLASSES?
Your cost for prescription drugs under the Cigna Core, Kaiser, and SimplePay Health plans differs based on the class or group of drugs your prescription drug belongs to. Generic medications are your
lowest-cost options, Preferred Brand drugs are midrange cost options, and Non-Preferred Brand are highest-cost options.
Specialty medications are used to treat complex medical conditions and are marked with an asterisk on the drug list. For the Cigna and SimplePay Health plans, specialty medications must be filled
through CVS Specialty pharmacy; otherwise, you pay the entire cost of the prescription drugs after one retail fill.
Step therapy: Certain classes of medications aren’t covered until you try one or more alternatives first. These medications have “ST” next to them on the drug list.
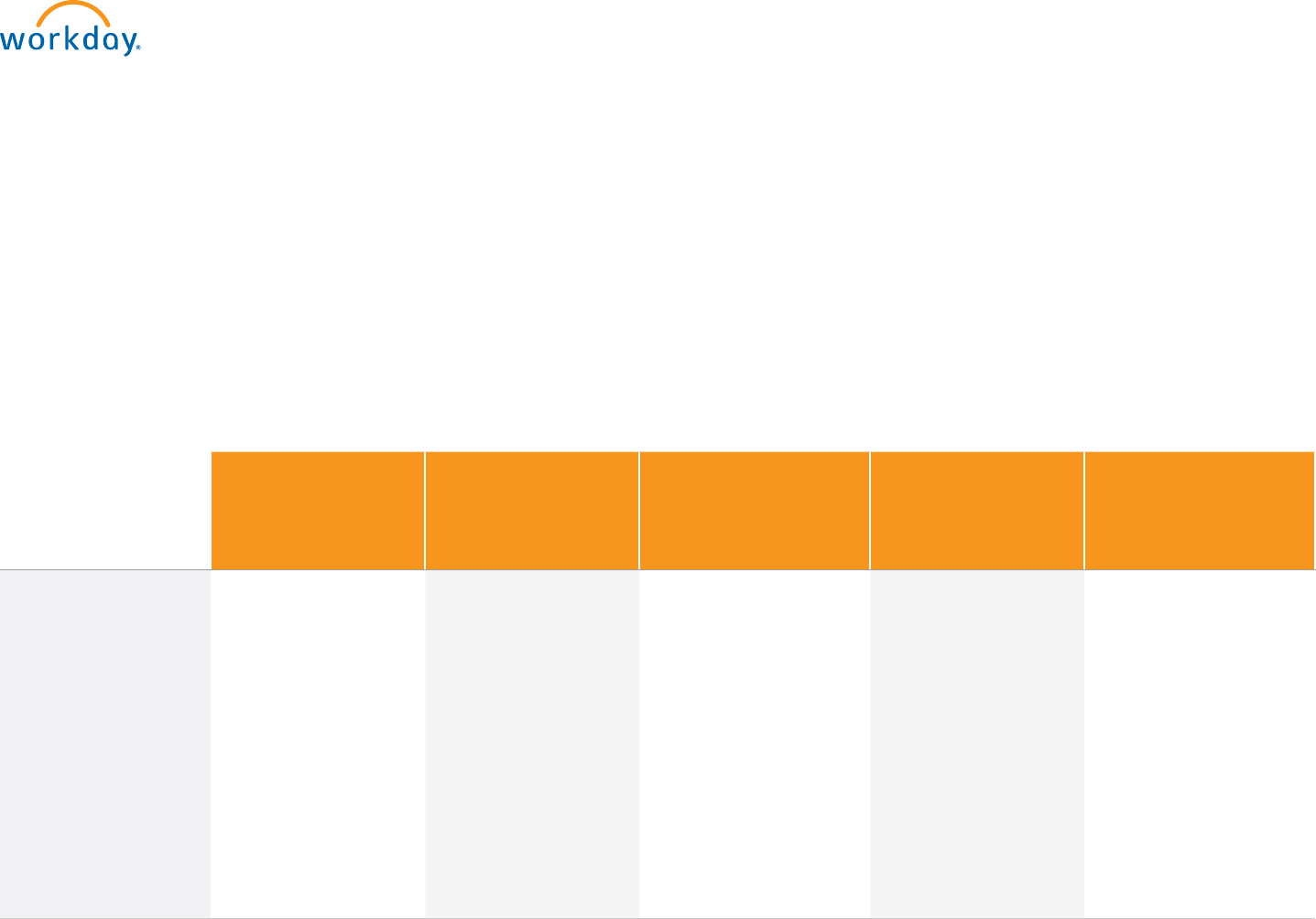
Cigna Smart Plan
With HSA
Formularies:
Performance Drug List and
Advanced Control Specialty
Cigna Core Plan
Formularies:
Performance Drug List and
Advanced Control Specialty
Kaiser Smart Plan With
HSA (CA, CO, & GA)
Kaiser HMO
(CA, CO, & GA)
SimplePay Health
Formulary:
Standard Formulary
Prescription Drugs Retail:
You pay:
• 20% after deductible for
most drugs (deductible
waived for eligible
preventive medications)
30-day supply (up to 90-day
supply available through
Mail Order or participating
retail pharmacies)
Mail Order:
You pay:
• 20% after deductible
90-day supply
Retail:
You pay:
• $10 Generic
• $30 Preferred Brand
• $60 Non-Preferred
Brand
30-day supply (up to 90-day
supply available through
Mail Order or participating
retail pharmacies)
Mail Order:
You pay:
• $25 Generic
• $75 Preferred Brand
• $150 Non-Preferred
Brand
90-day supply
Retail:
You pay:
• $10 Generic after
deductible
• $30 Brand after deductible
30-day supply
Mail Order:
You pay:
• $20 Generic after
deductible
• $60 Brand after deductible
100-day supply (CA)
90-day supply (CO & GA)
Retail:
You pay:
• $10 Generic
• $30 Brand
30-day supply
Mail Order:
You pay:
• $20 Generic
• $60 Brand
100-day supply (CA)
90-day supply (CO & GA)
30-Day Supply:
You pay:
• Generic
– $5 in-network
– $10 out-of-network
• Preferred Brand
– $15 in-network
– $20 out-of-network
• Non-Preferred Brand
– $20 in-network
– $25 out-of-network
• $15 Specialty
(mail order only)
90-Day Supply:
You pay:
• $10 Generic
• $30 Preferred Brand
• $40 Non-Preferred Brand
Prescription Drugs
