
Preexposure Prophylaxis for the Prevention of HIV Infection in the United States – 2021 Update Clinical Practice Guideline
Page 1 of 108
US Public Health Service
PREEXPOSURE PROPHYLAXIS FOR
THE PREVENTION OF HIV
INFECTION IN THE UNITED STATES
– 2021 UPDATE
A CLINICAL PRACTICE GUIDELINE

Preexposure Prophylaxis for the Prevention of HIV Infection in the United States – 2021 Update Clinical Practice Guideline
Page 2 of 108
What’s New in the Preexposure Prophylaxis for the Prevention of HIV Infection in the
United States - 2021 Update – A Clinical Practice Guideline
The Preexposure Prophylaxis for the Prevention of HIV Infection in the United States – 2021
Update – A Clinical Practice Guideline includes revisions to several sections. These revisions are
intended to update existing guidance using the current evidence base, to incorporate recent FDA
PrEP medication approvals, and to clarify specific aspects of clinical care. Other revisions were
made to improve usability and increase implementation of the guideline based on comments
received from clinicians providing PrEP care. Minor revisions were also made to correct
typographical errors, add or update references, and update content from cited guidelines and
source materials.
What’s new…
In anticipation of likely FDA approval of a PrEP indication for cabotegravir (CAB) in late 2021,
we added a new section about prescribing PrEP with intramuscular injections of CAB every 2
months for sexually active men, women, and transgender persons with indications for PrEP use.
Summary (of graded recommendations)
• We added a recommendation to inform all sexually active adults and adolescents about
PrEP (IIIB).
• We added a recommendation: PrEP with intramuscular cabotegravir (CAB) injections
(conditional on FDA approval) is recommended for HIV prevention in adults reporting
sexual behaviors that place them at substantial ongoing risk of HIV exposure and
acquisition (IA).
Table Summarizing Clinical Guidance
• We added a table specific for CAB (as CAB has a different dosing and recommended
follow-up schedule than oral PrEP, and no renal or lipid monitoring is required) (Table
1b).
Identifying Indications for PrEP
• We simplified the determination of indications for PrEP use for sexually-active persons.
We replaced boxes with flow charts for assessing indications for sexually active persons
and persons who inject drugs.
Laboratory Tests and other Diagnostic Procedures
• We revised the HIV testing algorithm to provide two algorithms; one for assessing HIV
status in persons with no history of recent antiretroviral exposure starting (or restarting)
PrEP and, the other for assessing HIV status at follow-up visits while persons are taking,
or have recently taken, PrEP.
Providing PrEP
• We added F/TAF as an FDA-approved choice for sexually active men and transgender
women at risk of HIV acquisition; the FDA approval for F/TAF excluded persons at risk
through receptive vaginal sex including cisgender women (persons assigned female sex at
birth whose gender identity is female).
• We revised and reordered the sections on initiation and follow-up care to first describe
guidelines applicable to all PrEP patients and then describe guidelines applicable only to
selected patients.
• We revised frequency of assessing eCrCl to every 12 months for persons <50 years of age
or with eCrCL ≥90 ml/min at PrEP initiation and every 6 months for all other patients.
• We added medications to Table 4 of drug interactions for TAF.
• We outlined options for PrEP initiation and follow-up care by telehealth (“Tele-PrEP”).
• We outlined procedures for providing or prescribing PrEP medication to select patients on
the same day as initial evaluation for its use (“same-day PrEP”).
• We outlined procedures for the off-label prescription of TDF/FTC to men who have sex
with men on a non-daily regimen (“2-1-1”) and their follow-up care.
• We added a brief section on primary care considerations for PrEP patients (Table 6).
• We added a section on providing CAB for PrEP.
Evidence Review
• We updated the evidence review and moved it to Appendix 2.
• We added evidence reviews for CAB trials.
• We separated clinical trial results for transgender women and MSM into separate rows in
evidence tables.

Preexposure Prophylaxis for the Prevention of HIV Infection in the United States – 2021 Update Clinical Practice Guideline
Page 4 of 108
Revisions post FDA approval of cabotegravir injections for PrEP
It is anticipated that FDA will review and may approve cabotegravir injections for PrEP within
2-3 months after the publication of this guideline. We will then post a revised version of this
guideline that replaces references to pending FDA approval with statements indicating that
approval has been given.
Disclaimers:
All material in this publication is in the public domain and may be used and reprinted without
permission; citation as to source, however, is appreciated.
References to non-CDC sites on the internet are provided as a service to readers and do not
constitute or imply endorsement of these organizations or their programs by CDC or the U.S.
Department of Health and Human Services. CDC is not responsible for the content of these sites.
URL addresses listed were current as of the date of publication.
Use of trade names and commercial sources is for identification only and does not imply
endorsement by the U.S. Department of Health and Human Services.
Potential Conflicts of Interest:
CDC and individual employees involved in the guideline development process are named in US
government patents and patent applications related to methods for HIV prophylaxis.
Suggested Citation:
Centers for Disease Control and Prevention: US Public Health Service: Preexposure prophylaxis for
the prevention of HIV infection in the United States—2021 Update: a clinical practice guideline.
https://www.cdc.gov/hiv/pdf/risk/prep/cdc-hiv-prep-guidelines-2021.pdf. Published XXX 2021.
For More Clinical Advice About PrEP Guidelines:
• Call the National Clinicians Consultation Center PrEPline at 855-448-7737;
• Go to the National Clinicians Consultation Center PrEPline website at
http://nccc.ucsf.edu/clinician-consultation/prep-pre-exposure-prophylaxis/; and/or
• Go to the CDC HIV website for clinician resources at
https://www.cdc.gov/hiv/clinicians/index.html.

Preexposure Prophylaxis for the Prevention of HIV Infection in the United States – 2021 Update Clinical Practice Guideline
Page 5 of 108
Table of Contents
List of Tables, Figures, and Boxes ................................................................................................9
Abbreviations (In Guideline and Clinical Providers’ Supplement) ........................................11
Summary .......................................................................................................................................13
Introduction ..................................................................................................................................18
Evidence of Need for Additional HIV Prevention Methods.....................................................21
All Patients Being Assessed for PrEP Provision .......................................................................22
Identifying Indications for PrEP ..........................................................................................22
Assessing Risk of Sexual HIV Acquisition .................................................................................... 23
Assessing Risk of HIV Acquisition Through Injection Practices ................................................... 26
Laboratory Tests and Other Diagnostic Procedures ..........................................................28
HIV testing ..................................................................................................................................... 28
Acute HIV Infection ....................................................................................................................... 29
Testing for Sexually transmitted Infections.................................................................................... 31
Laboratory Tests for Patients Being Considered for Oral PrEP ......................................32
Renal function ................................................................................................................................ 33
Testing for Infection with Hepatitis B Virus (HBV) ...................................................................... 34
Lipid Profile (F/TAF) ..................................................................................................................... 34
Testing not Indicated Routinely for Oral PrEP Patients ................................................................. 34
Initial PrEP Prescription Visit for All Patients .........................................................................35
Goals of PrEP Therapy .........................................................................................................35
Same Day PrEP Prescribing .................................................................................................35
Nonoccupational Postexposure Prophylaxis........................................................................36
Prescribing Oral PrEP ..........................................................................................................37

Preexposure Prophylaxis for the Prevention of HIV Infection in the United States – 2021 Update Clinical Practice Guideline
Page 6 of 108
Recommended Oral Medication ..................................................................................................... 37
What Not to Use For Oral PrEP ..................................................................................................... 38
Providing PrEP by Telehealth ........................................................................................................ 40
Counseling to Support Oral Medication Adherence and Persistence in Care................................. 40
Managing side effects of oral PrEP ................................................................................................ 42
Time to achieving protection with daily oral PrEP ........................................................................ 42
Follow-up PrEP Care Visits for Oral PrEP Patients ..........................................................43
Clinical Follow-up and Monitoring For Oral PrEP ........................................................................ 43
Laboratory Testing Schedule for Oral PrEP Patients ..................................................................... 44
Optional Assessments for Patients Prescribed Oral PrEP .............................................................. 45
Bone Health ............................................................................................................................................ 45
Medication adherence drug monitoring ................................................................................................. 45
Discontinuing and Restarting Daily Oral PrEP .............................................................................. 46
Prescribing Cabotegravir PrEP Injections ..........................................................................47
Recommended Medication ............................................................................................................. 47
What Not to Use ............................................................................................................................. 47
CAB PrEP Initiation Visit .............................................................................................................. 48
Laboratory Testing For CAB PrEP Patients ................................................................................... 48
Testing Not Indicated Routinely for CAB PrEP Patients ............................................................... 51
Recommended CAB Injection ........................................................................................................ 51
Managing Injection site reactions ................................................................................................... 51
Patient Education/Counseling ........................................................................................................ 51
Clinical Follow-Up and Monitoring For CAB Injections ...................................................52
Discontinuing or Restarting CAB PrEP ......................................................................................... 52
Time to Protection With CAB PrEP ............................................................................................... 54
Managing PrEP Patients with Ambiguous HIV test Results ...................................................54

Preexposure Prophylaxis for the Prevention of HIV Infection in the United States – 2021 Update Clinical Practice Guideline
Page 7 of 108
Considerations and Options for Selected Patients ....................................................................55
Nondaily Oral PrEP Regimens for MSM ............................................................................55
Transgender Persons .............................................................................................................57
Persons Who Inject Drugs.....................................................................................................58
Patients with Renal Disease...................................................................................................59
HIV Discordant Partnerships ...............................................................................................59
Persons with Documented HIV Infection ............................................................................60
Women who Become Pregnant or Breastfeed While Taking PrEP ..................................60
Adolescent Minors .................................................................................................................62
Primary Care Considerations .....................................................................................................64
Financial Case-Management Issues for PrEP ...........................................................................65
Decision Support, Training and Technical Assistance .............................................................66
Related DHHS Guidelines ...........................................................................................................67
Appendices ....................................................................................................................................69
Appendix 1 Grading of Strength of Recommendations and Quality of Evidence ...........70
Appendix 2 Evidence of the Safety and Efficacy of Oral Antiretroviral Prophylaxis...72
Published Trials of Antiretroviral Preexposure Prophylaxis Among Men Who Have Sex with Men72
Published Observational and Open-Label Studies of Antiretroviral Preexposure Prophylaxis Among Men
Who Have Sex with Men ............................................................................................................... 75
Published Trials of Antiretroviral Preexposure Prophylaxis Among Heterosexual Men and Women77
Published Trial of Antiretroviral Preexposure Prophylaxis Among Persons Who Inject Drugs .... 80
Published Open-Label Study of Antiretroviral Preexposure Prophylaxis Among Person Who Inject Drugs
........................................................................................................................................................ 81
Trials of Injectable Antiretroviral Preexposure Prophylaxis .......................................................... 81
Trial Evidence Review Tables...............................................................................................86

Preexposure Prophylaxis for the Prevention of HIV Infection in the United States – 2021 Update Clinical Practice Guideline
Page 8 of 108
Table 12: Evidence Summary — Overall Evidence Quality of Randomized PrEP Clinical Trials (per
GRADE Criteria
186
) ........................................................................................................................ 86
Table 13: Evidence Summary of Randomized Clinical Trials — HIV Incidence Findings ........... 88
Table 14: Measures of Efficacy, by Medication Adherence, Percentage Reduction in HIV Incidence in
Randomized Clinical Trials ............................................................................................................ 91
Table 15: Evidence Summary of Randomized Clinical Trials — Safety and Toxicity .................. 92
Table 16: Evidence Summary of Randomized Clinical Trials — HIV Resistance Findings ......... 93
Table 17: Evidence Summary of Open-Label Studies ................................................................... 94
References .....................................................................................................................................95

List of Tables, Figures, and Boxes
Table 1a Summary of Clinician Guidance for Daily Oral PrEP Use .............................................................15
Table 1b Summary of Clinician Guidance for Cabotegravir Injection PrEP Use .......................................17
Table 2 Clinical Signs and Symptoms of Acute (Primary) HIV Infection ...................................................31
Table 3 Recommended Oral PrEP Medications .............................................................................................39
Table 4 Oral PrEP Medication Drug Interactions .........................................................................................40
Table 5 Timing of Oral PrEP-Associated Laboratory Tests .........................................................................44
Table 6 Cabotegravir PrEP Drug Interactions ................................................................................................48
Table 7 Timing of Cabotegravir PrEP-Associated Laboratory Tests.............................................................50
Table 8 Primary Care Health Measures ..........................................................................................................63
Table 9 NASTAD Table of State PrEP Financial Assistance Programs.......................................................66
Table 10 Rating Scheme for Recommendations ..............................................................................................70
Table 11 Criteria for Rating Quality of Scientific Evidence ..........................................................................71
Table 12 PrEP Evidence Summary—GRADE Overall Evidence Quality RCTs ............................................87
Table 13 PrEP Evidence Summary— HIV Incidence Findings RCTs ............................................................88
Table 14 PrEP Evidence Summary—Measures of Efficacy by Medication Adherence RCTs .......................92
Table 15 PrEP Evidence Summary— Safety and Toxicity RCTs .....................................................................93
Table 16 PrEP Evidence Summary— HIV Resistance Findings RCTs .............................................................94
Table 17 PrEP Evidence Summary— Open-Label Studies of Daily Oral F/TDF ............................................95
Figure 1 Populations and HIV Acquisition Risk ............................................................................................23
Figure 2 Assessing Indications for PrEP in Sexually-Active Persons ..........................................................24
Figure 3 Assessing Indications for PrEP in Persons Who Inject Drugs .......................................................29
Figure 4a Clinician Determination of HIV Status for PrEP Provision to Persons without Recent
Antiretroviral Prophylaxis Use ...........................................................................................................32
Figure 4b Clinician Determination of HIV Status for PrEP Provision to Persons with Recent or Ongoing
Antiretroviral Prophylaxis Use ...........................................................................................................33

Preexposure Prophylaxis for the Prevention of HIV Infection in the United States – 2021 Update Clinical Practice Guideline
Page 10 of 108
Figure 5 Adherence and F/TDF PrEP Efficacy in MSM ...............................................................................40
Figure 6 HIV Incidence in MSM Without, During, and After Discontinuing F/TDF PrEP Use................46
Figure 7 The Trade-off of PrEP Drug Levels and Risk of HIVInfection with Resistant Virus ................52
Figure 8 Schedule for “2-1-1-“ Dosing ............................................................................................................56
Box A Cockcroft-Gault Formulas ....................................................................................................................35
Box B Key Components of Medication Adherence Counseling.....................................................................42

Preexposure Prophylaxis for the Prevention of HIV Infection in the United States – 2021 Update Clinical Practice Guideline
Page 11 of 108
Abbreviations (In Guideline and Clinical Providers’ Supplement)
ACTG AIDS Clinical Trials Group
AHRQ Agency for Healthcare Research and Quality
AIDS acquired immunodeficiency syndrome
BMD bone mineral density
CAB cabotegravir
CDC Centers for Disease Control and Prevention
CPT common procedural terminology
DEXA dual-emission X-ray absorptiometry
DHAP Division of HIV/AIDS Prevention, CDC
DHHS Department of Health and Human Services
DP diphosphate
eCrCl estimated creatinine clearance rate (ml/min)
EIA enzyme-linked immunoassay
EPT expedited partner therapy
FDA Food and Drug Administration
FHI Family Health International
F emtricitabine (trade name Emtriva®), also called FTC
F/TAF emtricitabine coformulated with tenofovir alafenamide (trade name Descovy®)
F/TDF emtricitabine coformulated with tenofovir disoproxil fumarate (trade name Truvada®)
GEM Guidelines Elements Model
GLIA GuideLine Implementability Appraisal
GRADE Grading of Recommendations Assessment, Development and Evaluation
HBV hepatitis B virus
HCV hepatitis C virus
HIV human immunodeficiency virus
HRSA Health Resources and Services Administration
ICD International Classification of Diseases
IDU injection drug users (also referred to as PWID)
IFA indirect immunofluorescence assay
IHS Indian Health Service
INSTI integrase strand transfer inhibitor
IQR interquartile range
MSM men who have sex with men
MTN Microbicide Trials Network
NASTAD National Association of State and Territorial AIDS Directors
NCHHSTP National Center for HIV/AIDS, Viral Hepatitis, STD, and TB Prevention
NGC National Guidelines Clearinghouse
NIAID National Institute of Allergy and Infectious Diseases
NIH National Institutes of Health
nPEP nonoccupational postexposure prophylaxis
NSAID non-steroidal anti-inflammatory drug
NQMC National Quality Measures Clearinghouse

Preexposure Prophylaxis for the Prevention of HIV Infection in the United States – 2021 Update Clinical Practice Guideline
Page 12 of 108
OHAP Office of HIV/AIDS Policy, DHHS
ONAP Office of National AIDS Policy
ONDCP Office of National Drug Control Policy
OPA Office of Population Affairs, DHHS
PCR polymerase chain reaction
PEP postexposure prophylaxis
PHS (U.S.) Public Health Service
PWID persons who inject drugs
PrEP preexposure prophylaxis
SAMHSA Substance Abuse and Mental Health Services Administration
STD sexually transmitted disease
STI sexually transmitted infection
TB tuberculosis
TDF tenofovir disoproxil fumarate (trade name Viread®)
TAF tenofovir alafenamide
TGW transgender women
UNAIDS Joint United National Programme on HIV/AIDS
USPSTF United States Preventive Services Task Force
VA Veterans Administration
WHO World Health Organization

Preexposure Prophylaxis for the Prevention of HIV Infection in the United States – 2021 Update Clinical Practice Guideline
Page 13 of 108
Summary
Preexposure Prophylaxis for HIV Prevention in the United States – 2021 Update: A Clinical Practice Guideline
provides comprehensive information for the use of antiretroviral preexposure prophylaxis (PrEP) to reduce the
risk of acquiring HIV infection. The key messages of the guideline are as follows:
▪ Daily oral PrEP with emtricitabine (F) 200 mg in combination with 1) tenofovir disoproxil fumarate (TDF)
300 mg for men and women or 2) tenofovir alafenamide (TAF) 25 mg, for men and transgender women,
has been shown to be safe and effective in reducing the risk of sexual HIV acquisition
therefore,
o All sexually active adult and adolescent patients should receive information about PrEP. (IIIB)
o For both men and women, PrEP with daily F/TDF is recommended for HIV prevention for sexually-
active adults and adolescents weighing at least 35 kg (77 lb) who report sexual behaviors that place
them at substantial ongoing risk of HIV exposure and acquisition. (IA)
1
o For both men and women, PrEP with daily F/TDF is recommended for HIV prevention for adult and
adolescents weighing at least 35 kg (77 lb) who inject drugs (PWID) (also referred to as injection
drug users [IDU]) and report injection practices that place them at substantial ongoing risk of HIV
exposure and acquisition. (IA)
o For men only, daily oral PrEP with F/TAF is a recommended option for HIV prevention for sexually
active adults and adolescents weighing at least 35 kg (77 lb) who report sexual behaviors that place
them at substantial ongoing risk of HIV exposure and acquisition. PrEP with F/TAF has not yet been
studied in women (persons assigned female sex at birth whose gender identify is female) and so
F/TAF is not recommended for HIV prevention for women or other persons at risk through receptive
vaginal sex. (IA)
o For transgender women (persons assigned male sex at birth whose gender identity is female) who
have sex with men, and who report sexual behaviors that place them at substantial ongoing risk of
HIV exposure and acquisition, daily oral PrEP with F/TAF is a recommended option for HIV
prevention (IIB)
o The efficacy and safety of other daily oral antiretroviral medications for PrEP, either in place of, or
in addition to, F/TDF or F/TAF, have not been studied extensively and are not recommended. (IIIA)
▪ Renal function should be assessed by estimated creatinine clearance (eCrCl) at baseline for PrEP patients
taking daily oral F/TDF or F/TAF, and monitored periodically so that persons in whom clinically significant
renal dysfunction is developing do not continue to take it.
o Estimated creatinine clearance (eCrCl) should be assessed every 6 months for patients over age
50 or those who have an eCrCl <90 ml/min at initiation. (IIA)
o For all other daily oral PrEP patients, eCrCl should be assessed at least every 12 months. (IIA)
▪ Conditioned on a PrEP indication approved by FDA, PrEP with intramuscular cabotegravir (CAB)
injections is recommended for HIV prevention in adults and adolescents who report sexual behaviors that
place them at substantial ongoing risk of HIV exposure and acquisition. (IA)
▪ Acute and chronic HIV infection must be excluded by symptom history and HIV testing immediately before
any PrEP regimen is prescribed. (IA)
▪ HIV infection should be assessed at least every 3 months for patients taking daily oral PrEP, and every 4
months for patients receiving CAB injections for PrEP so that persons with incident infection do not
continue taking it. The 2-drug regimens of F/TDF or F/TAF and the single drug CAB are inadequate therapy
1
See Appendix 1, Grading of Strength of Recommendations and Quality of Evidence (Tables 12-13)

Preexposure Prophylaxis for the Prevention of HIV Infection in the United States – 2021 Update Clinical Practice Guideline
Page 14 of 108
for established HIV infection, and their use in persons with early HIV infection may engender resistance to
one or more of the PrEP medications. (IA)
▪ When PrEP is prescribed, clinicians should provide access, directly or by facilitated referral, to:
o Support for medication adherence and continuation in follow-up PrEP care, because high
medication adherence and persistent use are critical to PrEP effectiveness for prevention of HIV
acquisition. (IIA)
o Additional proven effective risk-reduction services, as indicated by reported HIV exposure-prone
behaviors, to enable the use of PrEP in combination with other effective prevention methods to
reduce risk for sexual acquisition of STIs or acquisition of bloodborne bacterial and viral
infections through injection drug use. (IIIA)

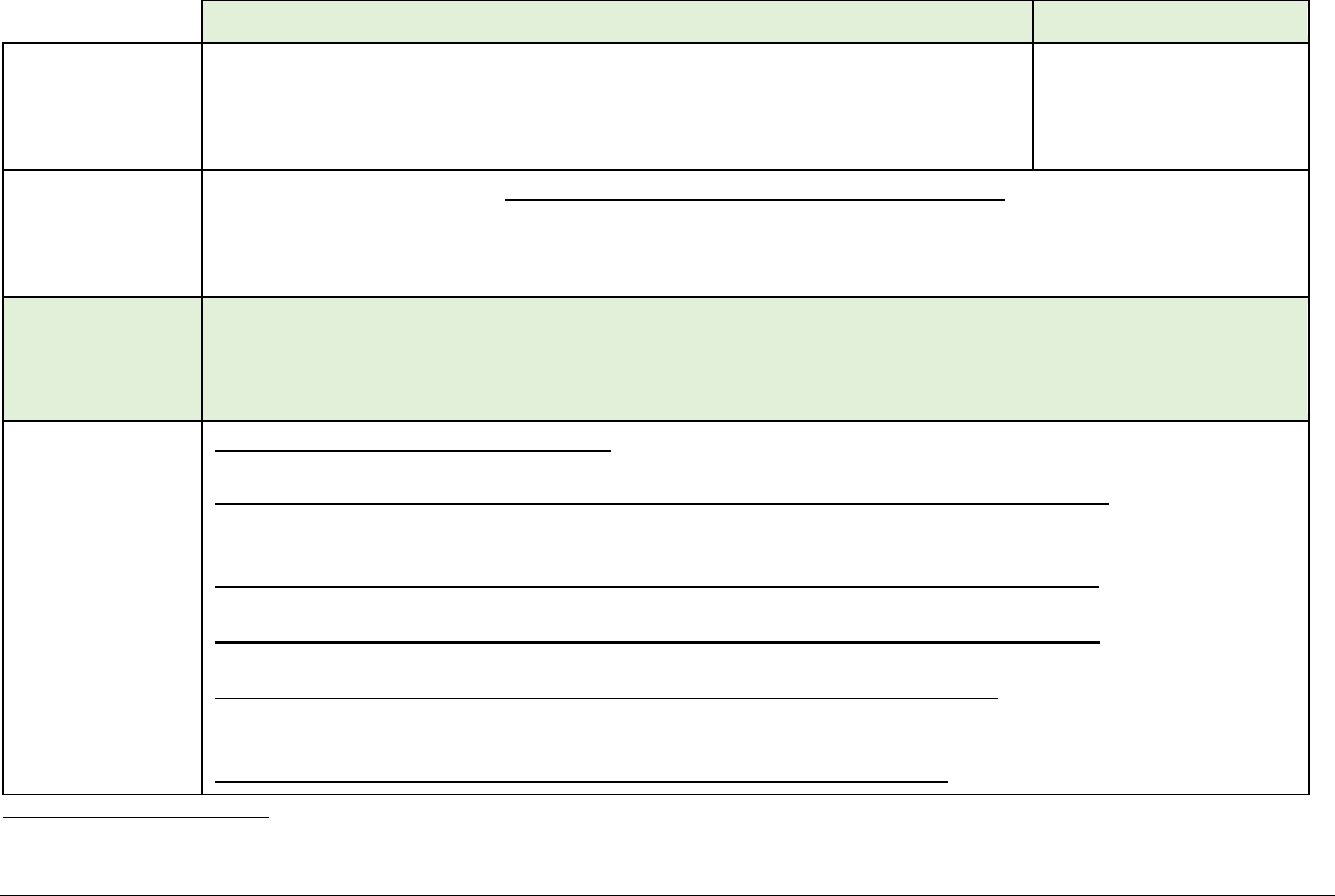
Table 1a: Summary of Clinician Guidance for Daily Oral PrEP Use
Sexually-Active Adults and Adolescents
1
Persons Who Inject Drug
2
Identifying
substantial
risk of acquiring HIV
infection
Anal or vaginal sex in past 6 months AND any of the following:
• HIV-positive sexual partner (especially if partner has an unknown or detectable viral load)
• Bacterial STI in past 6 months
3
• History of inconsistent or no condom use with sexual partner(s)
HIV-positive injecting partner
OR
Sharing injection equipment
Clinically eligible
ALL OF THE FOLLOWING CONDITIONS ARE MET:
• Documented negative HIV Ag/Ab test result within 1 week before initially prescribing PrEP
• No signs/symptoms of acute HIV infection
• Estimated creatinine clearance ≥30 ml/min
4
• No contraindicated medications
Dosage
• Daily, continuing, oral doses of F/TDF (Truvada®), ≤90-day supply
OR
• For men and transgender women at risk for sexual acquisition of HIV; daily, continuing, oral doses of F/TAF (Descovy®), ≤90-
day supply
Follow-up care
Follow-up visits at least every 3 months to provide the following:
• HIV Ag/Ab test and HIV-1 RNA assay, medication adherence and behavioral risk reduction support
• Bacterial STI screening for MSM and transgender women who have sex with men
3
– oral, rectal, urine, blood
• Access to clean needles/syringes and drug treatment services for PWID
Follow-up visits every 6 months to provide the following:
• Assess renal function for patients aged ≥50 years or who have an eCrCl <90 ml/min at PrEP initiation
• Bacterial STI screening for all sexually-active patients
3
– [vaginal, oral, rectal, urine- as indicated], blood
Follow-up visits every 12 months to provide the following:
• Assess renal function for all patients
• Chlamydia screening for heterosexually active women and men – vaginal, urine
• For patients on F/TAF, assess weight, triglyceride and cholesterol levels
1
adolescents weighing at least 35 kg (77 lb)
2
Because most PWID are also sexually active, they should be assessed for sexual risk and provided the option of CAB for PrEP when indicated
3
Sexually transmitted infection (STI): Gonorrhea, chlamydia, and syphilis for MSM and transgender women who have sex with men including those who inject drugs; Gonorrhea
and syphilis for heterosexual women and men including persons who inject drugs
4
estimated creatine clearance (eCrCl) by Cockcroft Gault formula ≥60 ml/min for F/TDF use, ≥30 ml/min for F/TAF use
Preexposure Prophylaxis for the Prevention of HIV Infection in the United States – 2021 Update Clinical Practice Guideline
Page 16 of 108
Table 1b: Summary of Clinician Guidance for Cabotegravir Injection PrEP Use
Sexually-Active Adults
Persons Who Inject Drugs
1
Identifying
substantial
risk of acquiring
HIV infection
Anal or vaginal sex in past 6 months AND any of the following:
• HIV-positive sexual partner (especially if partner has an unknown or detectable viral load)
• Bacterial STI in past 6 months
2
• History of inconsistent or no condom use with sexual partner(s)
HIV-positive injecting partner
OR
Sharing injection equipment
Clinically eligible
ALL OF THE FOLLOWING CONDITIONS ARE MET:
• Documented negative HIV Ag/Ab test result within 1 week before initial cabotegravir injection
• No signs/symptoms of acute HIV infection
• No contraindicated medications or conditions
Dosage
• 600 mg cabotegravir administered as one 3 ml intramuscular injection in the gluteal muscle
o Initial dose
o Second dose 4 weeks after first dose (month 1 follow-up visit)
o Every 8 weeks thereafter (month 3,5,7, follow-up visits etc)
Follow-up care
At follow-up visit 1 month after first injection
• HIV Ag/Ab test and HIV-1 RNA assay
At follow-up visits every 2 months (beginning with the third injection – month 3) provide the following:
• HIV Ag/Ab test and HIV-1 RNA assay
• Access to clean needles/syringes and drug treatment services for PWID
At follow-up visits every 4 months (beginning with the third injection- month 3) provide the following:
• Bacterial STI screening
2
for MSM and transgender women who have sex with men
2
– oral, rectal, urine, blood
At follow-up visits every 6 months (beginning with the fifth injection – month 7) provide the following:
• Bacterial STI screening
1
for all heterosexually-active women and men – [vaginal, rectal, urine - as indicated], blood
At follow-up visits at least every 12 months (after the first injection) provide the following:
• Assess desire to continue injections for PrEP
• Chlamydia screening for heterosexually active women and men – vaginal, urine
At follow-up visits when discontinuing cabotegravir injections provide the following:
1
Because most PWID are also sexually active, they should be assessed for sexual risk and provided the option of CAB for PrEP when indicated
2
Sexually transmitted infection (STI): Gonorrhea, chlamydia, and syphilis for MSM and transgender women who have sex with men including those who inject drugs; Gonorrhea
and syphilis for heterosexual women and men including persons who inject drugs

Preexposure Prophylaxis for the Prevention of HIV Infection in the United States – 2021 Update Clinical Practice Guideline
Page 17 of 108
• Re-educate patients about the “tail” and the risks during declining CAB levels
• Assess ongoing HIV risk and prevention plans
• If PrEP is indicated, prescribe daily oral F/TDF or F/TAF beginning within 8 weeks after last injection
• Continue follow-up visits with HIV testing quarterly for 12 months

Preexposure Prophylaxis for the Prevention of HIV Infection in the United States – 2021 Update Clinical Practice Guideline
Page 18 of 108
Introduction
Daily oral antiretroviral preexposure prophylaxis (PrEP) with a fixed-dose combination of either
tenofovir disoproxil fumarate (TDF) or tenofovir alafenamide (TAF) with emtricitabine (F).
has been found to be safe
1
and effective in substantially reducing HIV acquisition in gay,
bisexual, and other men who have sex with men (MSM)
2-4
, men and women in heterosexual
HIV-discordant couples
5
, and heterosexual men and women recruited as individuals.
6
In
addition, one clinical trial among persons who inject drugs (PWID) (also referred to as injection
drug users [IDU])
7
and one among men and women in heterosexual HIV-discordant couples
5
have demonstrated substantial efficacy and safety of daily oral PrEP with TDF alone. The
demonstrated efficacy of daily oral PrEP was in addition to the effects of repeated condom
provision, sexual risk-reduction counseling, and the diagnosis and treatment of sexually
transmitted infections (STI), all of which were provided to trial participants, including persons in
the drug treatment group and persons in the placebo group. In July 2012, after reviewing the
available trial results, the U.S. Food and Drug Administration (FDA) approved an indication for
the use of Truvada (F/TDF) “in combination with safer sex practices for pre-exposure
prophylaxis (PrEP) to reduce the risk of sexually acquired HIV-1 in adults at high risk”
8
. In May
2018, the approval for F/TDF was extended to adolescents weighing at least 35 kg (77 lb) based
on safety trials in adolescents
9
and young adults.
10
In June 2019, the US Preventive Services
Task Force recommended PrEP for adults and adolescents at risk of HIV acquisition with an “A”
rating (high certainty that the net benefit of the use of PrEP to reduce the risk of acquisition of
HIV infection in persons at high risk of HIV infection is substantial).
11
In 2021, based on this
recommendation, DHHS determined that most commercial insurers and some Medicaid
programs are required to provide oral PrEP medication, necessary laboratory tests, and clinic
visits with no out-of-pocket cost to patients., And in October 2019, based on a clinical trial
conducted with 5,387 MSM and 74 transgender women, the FDA approved a PrEP indication for
daily Descovy (F/TAF) for sexually active men and transgender women at risk of HIV
acquisition.
3, 4
Women (persons assigned female sex at birth) and other persons at risk through
receptive vaginal sex were specifically excluded from the F/TAF approval, because no women or
transgender men were included in the efficacy and safety PrEP trial. In 2020, results from a
clinical trial conducted with MSM and transgender women, and another conducted with women,
reported high efficacy and safety for injections of cabotegravir (CAB) every 2 months for
PrEP.
12, 13
Submission of data for review by the FDA for approval of a PrEP indication is
planned in 2021.
On the basis of these trial results and the FDA approvals, the U.S. Public Health Service
guidelines recommend that clinicians inform all sexually-active patients about PrEP and its role
in preventing HIV acquisition. Clinicians should evaluate all adult and adolescent patients who
are sexually active or who are injecting illicit drugs and offer to prescribe PrEP to persons whose
sexual or injection behaviors and epidemiologic context place them at substantial risk of
acquiring HIV infection.

Preexposure Prophylaxis for the Prevention of HIV Infection in the United States – 2021 Update Clinical Practice Guideline
Page 19 of 108
An estimated 1.2 million persons have indications for PrEP use.
14
Both the soon to be updated
HIV National Strategic Plan: A Roadmap to End the Epidemic for the United States - 2021–
2025. (https://files.hiv.gov/s3fs-public/HIV-National-Strategic-Plan-2021-2025.pdf) and the
federal initiative “Ending the HIV Epidemic in the United States”
(https://www.cdc.gov/endhiv/index.html) have called for rapid and large scale up of PrEP
provision by clinicians providing health care to HIV-uninfected persons at risk for HIV
acquisition. Since FDA approval, the minimum estimate of the number of persons receiving
PrEP prescriptions for F/TDF has risen from 8,800 in 2012 to nearly 220,000 in 2018.
15, 16
However, the geographic, sex, and racial/ethnic distribution of persons prescribed PrEP is not
equitable when compared to the distribution of new HIV diagnoses that could be prevented.
African Americans, Hispanics, women, and residents of southern states have disproportionately
low numbers of PrEP users.
17
The evidence base for this 2021 update of CDC’s PrEP guidelines was derived from a systematic
search and review of published literature. To identify all oral PrEP safety and efficacy trials and
observational studies pertaining to the prevention of sexual and injection acquisition of HIV, a
search was performed of the clinical trials registry (http://www.clinicaltrials.gov) by using
combinations of search terms (preexposure prophylaxis, pre-exposure prophylaxis, PrEP, HIV,
Truvada, Descovy, tenofovir, and antiretroviral). These search terms were used to search
PubMed, Web of Science, MEDLINE, Embase, CINAHL, and Cochrane Library databases for
January 2006-December 2020. Finally, a review of references from published PrEP trial data
confirmed that no additional trial results were available. For additional information about the
systematic review process, see the Clinical Providers’ Supplement, Section 12 at
https://www.cdc.gov/hiv/pdf/risk/prep-cdc-hiv-prep-provider-supplement-2021.pdf.
This publication provides a comprehensive clinical practice guideline for the use of PrEP for the
prevention of HIV infection in the United States. Currently, prescribing daily oral PrEP with
F/TDF is recommended for MSM, heterosexual men, heterosexual women, and PWID at
substantial risk of HIV acquisition; F/TAF is a recommended option for sexually active persons
except women and other persons at risk through receptive vaginal sex. FDA review of injections
of CAB every 2 months as PrEP is pending. As the results of additional PrEP clinical trials and
studies in these and other populations at risk of HIV acquisition become known, this guideline
will be updated.
Many of the studies that informed these guidelines included small numbers of transgender
women and none included transgender men, as a result, data specifically relevant for transgender
and non-binary people are often limited or not available. Most sections of these guidelines,
therefore, use the terminology, ‘women’ and ‘men’ unless specifically referring to transgender
women or men. Based on current data showing potentially high levels for protection with PrEP
for people exposed to HIV during rectal, vaginal, and /or oral sex we recommend gender-
inclusive models of PrEP care to ensure that services encompass and address the needs of all

Preexposure Prophylaxis for the Prevention of HIV Infection in the United States – 2021 Update Clinical Practice Guideline
Page 20 of 108
persons who would benefit from its use including cisgender and transgender adults and
adolescents as well as PWID.
The intended users of this guideline include:
▪ primary care clinicians who provide care to persons at risk of acquiring HIV infection;
▪ clinicians who provide substance abuse treatment or reproductive health care;
▪ infectious disease, HIV treatment, and STD treatment specialists who may provide PrEP
or serve as consultants to primary care clinicians about the use of antiretroviral
medications; and
▪ health program policymakers
▪ counselors and other adherence support providers

Preexposure Prophylaxis for the Prevention of HIV Infection in the United States – 2021 Update Clinical Practice Guideline
Page 21 of 108
Evidence of Need for Additional HIV Prevention Methods
Approximately 36,400 people in the United States acquired HIV in 2018. From 2014 through
2018, overall estimated annual HIV incidence remained stable. No decline or increase was
observed in the estimated number of annual HIV infections among persons of both sexes,
black/African American, Hispanic/Latino, or white persons, any transmission risk group, or any
region of the US. Estimated HIV incidence decreased from 2014 through 2018 among persons of
multiple races and among persons aged 13–24, and remained stable among all other age
groups.
18
In 2018, 67% of the 38,739 newly diagnosed HIV infections were attributed to male-male sexual
activity without injection drug use, 3% to male-male sexual activity with injection drug use, 24%
to male-female sexual contact without injection drug use, and 6% to injection drug use.
17
Among
all adults and adolescents, diagnoses of HIV infection among transgender persons accounted for
approximately 2% of diagnoses of HIV infections in the United States and 6 dependent areas; of
whom 92% of diagnoses of HIV infections were for transgender women. Among the 24% of
persons with newly diagnosed HIV infection attributed to heterosexual activity, 62% were
African-American women and men.
14
These data indicate a need for additional methods of HIV
prevention to further reduce new HIV infections, especially (but not exclusively) among young
adult and adolescent MSM of all races and Hispanic/Latino ethnicity and for African American
heterosexuals (populations with higher HIV prevalence and at higher risk of HIV infection
among persons without HIV infection).
Since 2012, when the FDA first approved a F/TDF indication for PrEP and clinical trial data
showed the efficacy and safety of daily, oral F/TDF for HIV prevention, the number of persons
prescribed PrEP has gradually increased each year
14
. In 2018, of the estimated 1.2 million adults
and adolescents with indication for PrEP use
12
, an estimated 220,000 persons received an oral
PrEP prescription, or about 18% of persons who would benefit from its use.
13
Equitable
provision of PrEP to populations at highest risk of HIV acquisition is not occurring. Black
persons constituted 42% of new HIV diagnoses in 2018 but only 6% of Black persons with
indications for its use were estimated to have received an oral PrEP prescription. Hispanic/Latino
persons constituted 27% of new HIV diagnoses but only 10% of Hispanic/Latino persons with
indications for its use had received an oral PrEP prescription. While women are 19% of persons
with new HIV diagnoses, they comprise only 7% of those prescribed oral PrEP.
17, 19
These guidelines are intended to inform clinicians and other partners to respond to both the soon
to be updated HIV National Strategic Plan: A Roadmap to End the Epidemic for the United
States - 2021–2025 (https://files.hiv.gov/s3fs-public/HIV-National-Strategic-Plan-2021-
2025.pdf) and the federal initiative Ending the HIV Epidemic in the United States
(https://www.cdc.gov/endhiv/index.html) through rapid expansion of PrEP delivery to all
persons who could benefit from its use as highly effective HIV prevention.

Preexposure Prophylaxis for the Prevention of HIV Infection in the United States – 2021 Update Clinical Practice Guideline
Page 22 of 108
All Patients Being Assessed for PrEP Provision
IDENTIFYING INDICATIONS FOR PREP
All sexually active adults and adolescents should be informed about PrEP for prevention of HIV
acquisition. This information will enable patients to both respond openly to risk assessment
questions and to discuss PrEP with persons in their social networks and family members who
might benefit from its use. Studies have shown that patients often do not disclose stigmatized
sexual or substance use behaviors to their health care providers (especially when not asked about
specific behaviors).
20-25
Taking a brief, targeted sexual history is recommended for all adult and adolescent patients as
part of ongoing primary care,
26
but the sexual history is often deferred because of urgent care
issues, provider discomfort, or anticipated patient discomfort. This deferral is common among
providers of primary care,
27
STI care,
28
and HIV care.
29-31
Routinely taking a sexual history is a necessary first step to identify which patients in a clinical
practice are having sex with same-sex partners, which are having sex with partners, and what
specific sexual behaviors may place them at risk for, or protect them from, HIV acquisition. To
identify the sexual health needs of all their patients, clinicians should not limit sexual history
assessments to only selected patients (e.g., young, unmarried persons, or women seeking
contraception), because new HIV infections and STIs are occurring in all adult and adolescent
age groups, both sexes, all genders, and both married and unmarried persons. The clinician can
introduce this topic by stating that taking a brief sexual history is routine practice for all patients,
go on to explain that the information is necessary to the provision of individually appropriate
sexual health care, and close by reaffirming the confidentiality of patient information.
Transgender persons are those whose sex at birth differs from their current self-identified gender.
Although the effectiveness of oral PrEP for transgender women has been more definitively
proven in some trials than in others
32
, cabotegravir injections for PrEP have been shown to
reduce the risk for HIV acquisition among transgender women and MSM during anal sex
13
and
women during vaginal sex
12
. Trials have not been conducted among transgender men.
Nonetheless, its use should be considered in all persons at risk of acquiring HIV sexually.
Patients may request PrEP because of concern about acquiring HIV but not feel comfortable
reporting sexual or injection behaviors to avoid anticipated stigmatizing responses in health care
settings.
33-36
For this reason, after attempts to assess patient sexual and injection behaviors,
patients who request PrEP should be offered it, even when no specific risk behaviors are elicited.
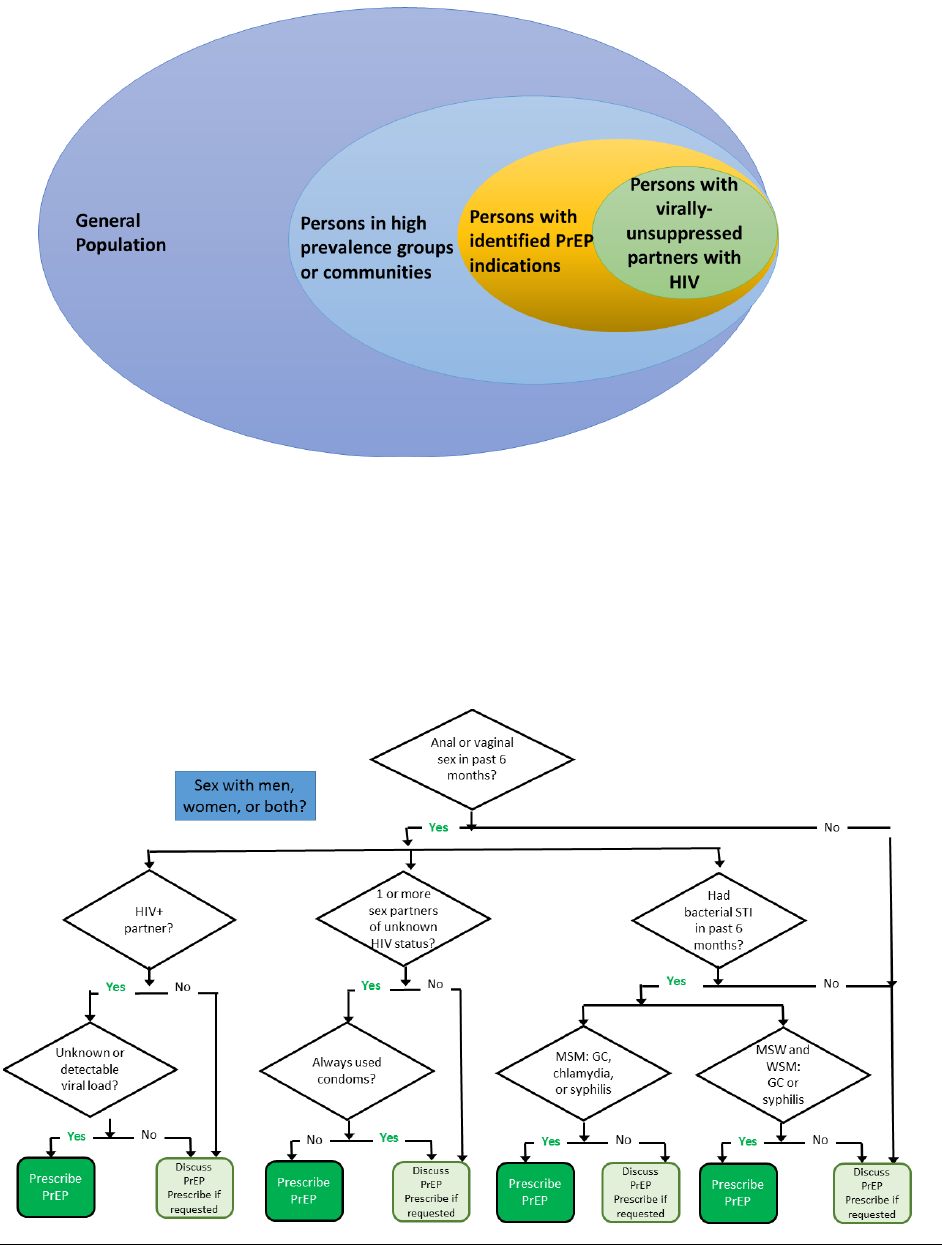
Preexposure Prophylaxis for the Prevention of HIV Infection in the United States – 2021 Update Clinical Practice Guideline
Page 23 of 108
Figure 1 Populations and HIV Acquisition Risk
ASSESSING RISK OF SEXUAL HIV ACQUISITION
PrEP should be offered to sexually active adults and adolescents at substantial risk of HIV
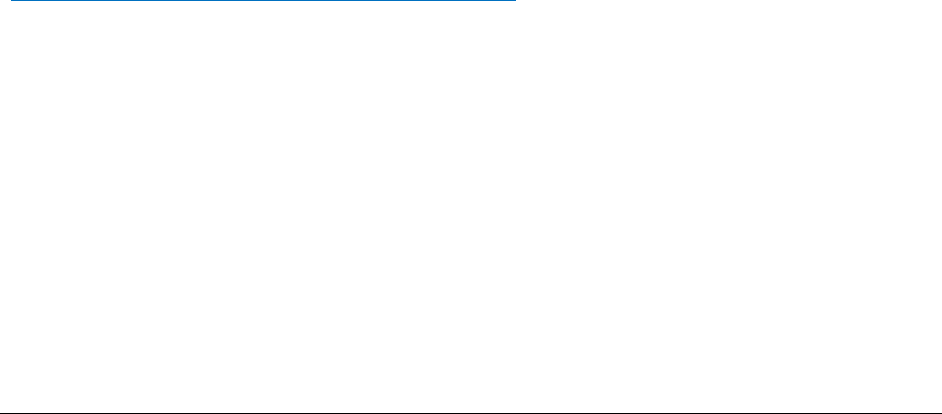
acquisition. Figure 2 outlines a set of brief questions designed to assess a key set of sexual
practices that are associated with the risk of HIV acquisition.
Figure 2 Assessing Indications for PrEP in Sexually Active Persons
Preexposure Prophylaxis for the Prevention of HIV Infection in the United States – 2021 Update Clinical Practice Guideline
Page 24 of 108
A patient who reports that one or more regular sex partners is of unknown HIV status should be
offered HIV testing for those partners, either in the clinician’s practice or at a confidential testing
site (see zip code lookup at https://www. gettested.cdc.gov/).
When a patient reports that one or more regular sex partners is known to have HIV, the clinician
should determine whether the patient being considered for PrEP use knows if the HIV-positive
partner is receiving antiretroviral therapy and has had an undetectable viral load (<200
copies/ml) for at least the prior 6 months.
37
Persons with HIV who have an undetectable viral
load pose effectively no risk for HIV transmission to sexual partners (see section below on
considerations for HIV discordant couples). PrEP for an HIV-uninfected patient may be
indicated if a sexual partner with HIV has been inconsistently virally suppressed or his/her viral
load status is unknown. In addition, PrEP may be indicated if the partner without HIV seeking
PrEP either has other sexual partners or wants the additional reassurance of protection that PrEP
can provide.
Clinicians should ask all sexually-active patients about any diagnoses of bacterial STIs
(chlamydia, syphilis, gonorrhea) during the past 6 months, because they provide evidence of
sexual activity that could result in HIV exposure. For heterosexual women and men, risk of HIV
exposure during condomless sex may also be indicated by recent pregnancy of a female patient
or a female sexual partner of a male patient considering PrEP. A scored risk index predictive of
incident HIV infection among MSM
38, 39
(see Clinical Providers’ Supplement, Section 5) is also
available.
Only a few questions are needed to establish whether indications for PrEP are present, However,
clinicians may want to ask additional questions to obtain a more complete sexual history that
includes information about a patient’s gender identity, partners, sexual practices, HIV/STI
protective practices, past history of STDs, and pregnancy intentions/preventive methods
(https://www.cdc.gov/std/treatment/sexualhistory.pdf). Clinicians should become familiar with
the evolving terminology referring to sex, gender identity, and sexual orientation.

Preexposure Prophylaxis for the Prevention of HIV Infection in the United States – 2021 Update Clinical Practice Guideline
Page 25 of 108
Clinicians should also briefly screen all patients for alcohol use disorder
40
(especially before
sexual activity), and the use of illicit non-injection drugs (e.g., amyl nitrite, stimulants).
41, 42
The
use of these substances may affect sexual risk behavior,
43
hepatic or renal health, or medication
adherence, any of which may affect decisions about the appropriateness of prescribing PrEP
medication. In addition, if a substance use disorder is identified, the clinician should provide
referral for appropriate treatment or harm-reduction services acceptable to the patient.
Sex The assignment of a person as male or female usually based on the appearance of their
external anatomy at birth. This is what is written on the birth certificate.
Gender Identity A person's internal, deeply held sense of their gender. Most people have a
gender identity of man or woman (or boy or girl). Gender identity is not visible to others.
Sexual Orientation A person's enduring physical, romantic, and/or emotional attraction to
another person. Gender identity and sexual orientation are not the same. Persons of varied
gender identities may be straight, lesbian, gay, bisexual, or queer
Transgender (adj.)
People whose gender identity differs from the sex they were assigned at birth. Many
transgender people are prescribed hormones by their doctors and some undergo surgery to
bring their bodies into alignment with their gender identity. A transgender identity is not
dependent upon physical appearance or medical procedures. Trans can be used as shorthand
for transgender
Cisgender (adj.) People whose gender identity is the same as the sex they were assigned at
birth Cis can be used as shorthand for cisgender.
Gender Expression External manifestations of gender, expressed through a person's name,
pronouns, clothing, haircut, behavior, voice, and/or body characteristics.
Gender Non-Conforming People whose gender expression is different from conventional
expectations of masculinity and femininity. Many people have gender expressions that are not
entirely conventional – that fact alone does not make them transgender. The term is not a
synonym for transgender or transsexual and should only be used if someone self-identifies as
gender non-conforming.
Non-binary and/or genderqueer Terms used by some people who experience their gender
identity and/or gender expression as falling outside or somewhere in between the categories
of man and woman. The term should only be used if someone self-identifies as non-binary
and/or genderqueer.
Adapted from GLAAD Media Reference Guide at
https://www.glaad.org/reference/transgender

Preexposure Prophylaxis for the Prevention of HIV Infection in the United States – 2021 Update Clinical Practice Guideline
Page 26 of 108
Lastly, clinicians should consider the epidemiologic context of the sexual practices reported by
the patient. The risk of HIV acquisition is determined by both the frequency of specific sexual
practices (e.g., condomless anal intercourse) and the likelihood that a sex partner has HIV. The
same behaviors when reported as occurring in communities and demographic populations with
high HIV prevalence or occurring with partners known to have HIV, are more likely to result in
exposure to HIV and so will indicate greater need for intensive risk-reduction methods (e.g.,
PrEP, multisession behavioral counseling) than when they occur in a community or population
with low HIV prevalence (for local prevalence estimates see http://www.AIDSvu.org or
http://www.cdc.gov/nchhstp/atlas/).
Reported consistent (“always”) condom use is associated with an 80% reduction in HIV
acquisition among heterosexual couples
44
and 70% among MSM.
45
Inconsistent condom use is
considerably less effective,
46, 47
and studies have reported low rates of recent consistent condom
use among MSM
48, 49
and other sexually active adults.
48
Especially low rates have been reported
when condom use was measured over several months rather than during most recent sex or the
past 30 days.
50
Therefore, unless the patient reports confidence that consistent condom use can
be achieved, PrEP should be prescribed while continuing to support condom use for prevention
of STIs and unplanned pregnancy (See Supplement Section 5).
ASSESSING RISK OF HIV ACQUISITION THROUGH INJECTION PRACTICES
Although the annual number of new HIV infections among PWID in the United States has
declined, a sizable number occur each year. In 2018, PWID (including MSM/PWID) accounted
for 7% of estimated incident HIV infections.
19
According to the National HIV Behavioral
Surveillance System (NHBS)
51
data collected in 2018, substantial proportions of HIV-negative
PWID report receptive sharing of syringes (33%) and receptive sharing of injection equipment
(55%), both of which may lead to HIV exposure. Few (1%) reported using PrEP in the previous
12 months. Data from NHBS also demonstrate that most PWID report sexual behaviors that
confer risk of HIV acquisition. Among HIV-negative PWID males, 69% reported having had
condomless vaginal sex in the prior 12 months, and 4% reported having had condomless anal sex
with a male partner. Among HIV-negative PWID females, 79% reported having had condomless
vaginal sex, and 27% reported having had condomless anal sex. 33% of HIV negative PWID
reported their most recent sex was condomless sex with a partner known to have HIV. Because
most PWID are sexually active, and many acquire HIV from sexual exposures,
52, 53
they should
be assessed for both sexual and injection behaviors that indicate HIV risk. The only randomized
clinical PrEP trial conducted with PWID found that TDF was effective in preventing HIV
acquisition but somewhat less effective than F/TDF in person with only sexual risk of HIV
acquisition.
7
In addition, antiretrovirals are effective as post-exposure prophylaxis against
needlestick exposures
54
and as treatment for HIV infection in PWID. Therefore, PWID are likely
to benefit from PrEP with any FDA-approved medication with or without an identified sexual
behavior risk of HIV acquisition.
Preexposure Prophylaxis for the Prevention of HIV Infection in the United States – 2021 Update Clinical Practice Guideline
Page 27 of 108
Lastly, non-sterile injection with shared syringes or other injection equipment sometimes occurs
among transgender persons while administering non-prescribed gender-affirming hormones or
among persons altering body shape with silicone or other “fillers.”
55-57
Providing PrEP to persons
who report non-sterile injection behaviors that can place them at substantial risk of acquiring
HIV will contribute to HIV prevention efforts.
Current evidence is sufficient to recommend that all adult patients be screened for injection
practices or other illicit drug use. The USPSTF
22
recommends that clinicians be alert to the signs
and symptoms of illicit drug use in patients. Clinicians should determine whether patients who
are currently using illicit drugs are in (or want to receive) medication-assisted therapy, in-patient
drug treatment, or behavioral therapy for substance use disorder. For persons with a history of
injecting illicit drugs but who are currently not injecting, clinicians should assess the risk of
relapse along with the patients’ use of relapse prevention services (e.g., a drug-related behavioral
support program, use of mental health services, medication-assisted therapy,12-step program).
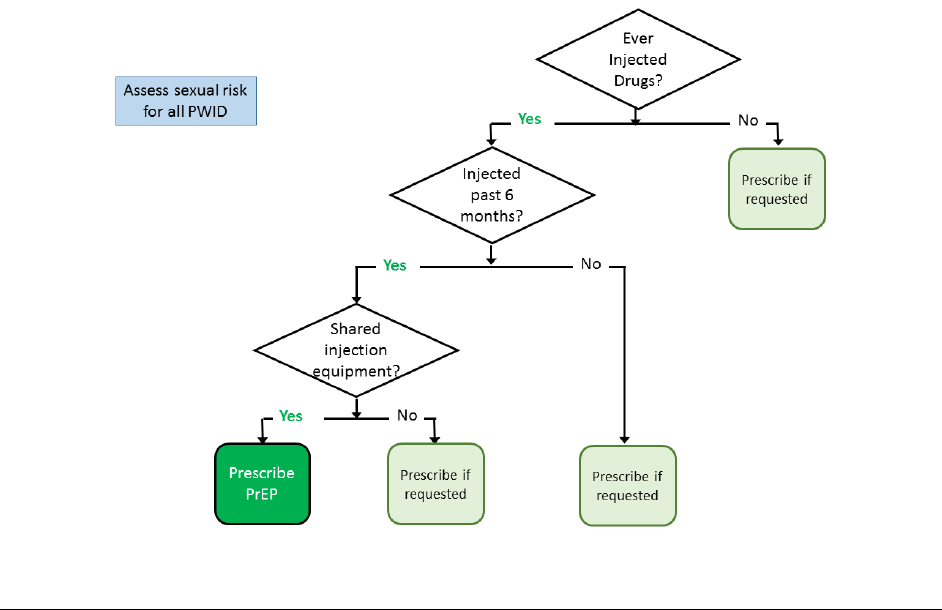
Figure 3 outlines a set of brief questions designed to assess a key set of injection practices that
are associated with the risk of HIV acquisition. For a scored risk index predictive of incident
HIV infection among PWID,
58
see the Clinical Providers’ Supplement, Section 7.
Figure 3 Assessing Indications for PrEP in Persons Who Inject Drugs

Preexposure Prophylaxis for the Prevention of HIV Infection in the United States – 2021 Update Clinical Practice Guideline
Page 28 of 108
PrEP and other HIV prevention should be provided and integrated with prevention and clinical
care services for the other non-HIV health threats PWID may face (e.g., hepatitis B and C
infection, abscesses, septicemia, endocarditis, overdose).
59
In addition, referrals for treatment of
substance use disorder, mental health services, harm reduction programs, syringe service
programs (SSPs) where available or access to sterile injection equipment, and social services
may be indicated.
LABORATORY TESTS AND OTHER DIAGNOSTIC PROCEDURES
All patients whose sexual or drug injection history indicates consideration of PrEP and who are
interested in taking PrEP, as well as patients without indications who request PrEP, must
undergo laboratory testing to identify persons for whom this intervention could be harmful or for
whom it could present specific health risks that would require close monitoring.
HIV TESTING
HIV testing with confirmed results is required to document that patients do not have HIV when
they start taking PrEP medications (Figure 4a). For patient safety, HIV testing should be repeated
at least every 3 months after oral PrEP initiation (i.e., before prescriptions are refilled or
reissued) or every 2 months when CAB injections are being given. This requirement should be
explained to patients during the discussion about whether PrEP is appropriate for them.
The CDC and USPSTF recommend that MSM, PWID, patients with a sex partner who has HIV,
and others at substantial risk of HIV acquisition undergo an HIV test at least annually or for
those with additional risk factors, every 3-6 months.
60, 61
However, outside the context of PrEP
delivery, testing is often not done as frequently as recommended.
62-64
Clinicians should document a negative HIV test result within the week before initiating (or
reinitiating) PrEP medications, ideally with an antigen/antibody test conducted by a laboratory.
The required HIV testing before initiation can be accomplished by (1) drawing blood (serum)
and sending the specimen to a laboratory for an antigen/antibody test or (2) performing a rapid,
point-of-care, FDA-approved, fingerstick antigen/antibody blood test (see figure 4a). In the
context of PrEP, rapid tests that use oral fluid should not be used to screen for HIV infection
because they are less sensitive for the detection of acute or recent infection than blood tests.
65
Clinicians should not accept patient-reported test results or documented anonymous test results.
PrEP should not be prescribed in the event of a preliminary positive HIV antibody-only test
unless negative HIV status is confirmed according to the local laboratory standard practice.
66
If a
diagnosis of HIV infection is confirmed, HIV viral load, resistance testing, and CD4 lymphocyte
tests should be ordered to assist in future treatment decisions.
See http://www.cdc.gov/hiv/testing/laboratorytests.html for FDA-approved HIV tests, specimen
requirements, and time to detection of HIV infection.
Preexposure Prophylaxis for the Prevention of HIV Infection in the United States – 2021 Update Clinical Practice Guideline
Page 29 of 108
ACUTE HIV INFECTION
In clinical trials of oral tenofovir-based PrEP, drug-resistant virus has developed in a small
number of trial participants with unrecognized acute HIV infection and for whom PrEP had been
dispensed, including most often the M184V/I mutation associated with emtricitabine resistance
and less frequently the K65R mutation associated with tenofovir resistance.
67
In these trials, no
resistance mutations emerged among persons who acquired antiretroviral-sensitive HIV while
taking PrEP as prescribed. Therefore, identifying people with possible acute infection is critical
to ensure persons with HIV are not exposed to drug pressure from PrEP that might induce
antiretroviral resistance and limit future treatment options.
68
Among persons receiving CAB
injections for PrEP, integrase strand transfer inhibitor (INSTI) resistance mutations were found
in 4 of 9 patients with incident HIV infections and was not seen in patients who have stopped
injections (i.e., during the “tail” period when drug levels are slowly declining).
13
Clinicians should suspect acute HIV infection in persons who report having engaged in
exposure-prone behaviors in the 4 weeks prior to evaluation for PrEP (e.g., a condom broke
during sex with an HIV-infected partner, relapse to injection drug use with shared injection
equipment). For all PrEP candidates with a negative or an indeterminate result on an HIV
antigen/antibody, and those reporting a recent possible HIV exposure event, clinicians should
next solicit a history of nonspecific signs or symptoms of viral infection during the preceding
month or on the day of evaluation
69, 70
(Table 2).
Table 2: Clinical Signs and Symptoms of Acute (Primary) HIV Infection
71
Sex
Route of transmission
Features
Overall
(n = 375)
%
Male
(n = 355)
%
Female
(n = 23)
%
Sexual
(n = 324)
%
Injection Drug Use
(n = 34)
%
Fever
75
74
83
77
50
Fatigue
68
67
78
71
50
Myalgia
49
50
26
52
29
Skin rash
48
48
48
51
21
Headache
45
45
44
47
30
Pharyngitis
40
40
48
43
18
Cervical adenopathy
39
39
39
41
27
Arthralgia
30
30
26
28
26
Night sweats
28
28
22
30
27
Diarrhea
27
27
21
28
23
Figure 4a below illustrates the recommended clinical testing algorithm to establish HIV status
before the initiation of PrEP in persons without recent antiretroviral prophylaxis use. Laboratory
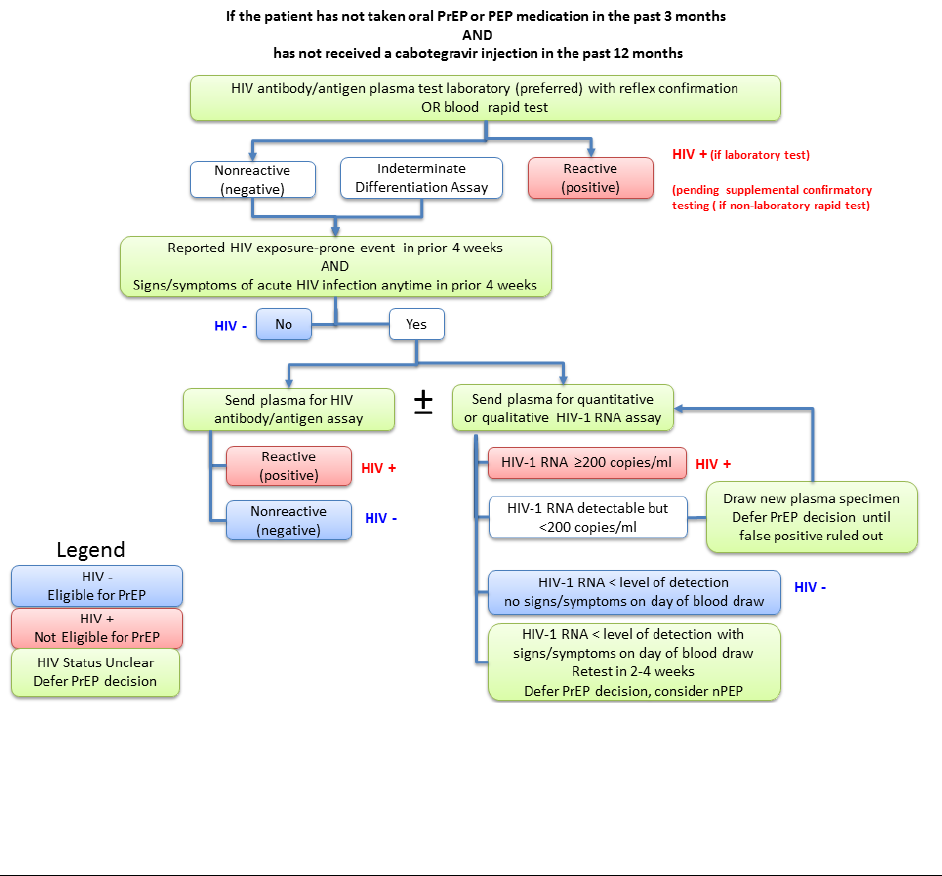
Preexposure Prophylaxis for the Prevention of HIV Infection in the United States – 2021 Update Clinical Practice Guideline
Page 30 of 108
antigen/antibody tests are preferred over rapid antigen/antibody tests (less preferred) because
they have the highest sensitivity for detecting acute HIV infection, which is associated with high
viral loads. While HIV-1 RNA testing is sensitive (a preferred option), healthcare providers
should be aware that available assays might yield false-positive low viral load results (e.g., <200
copies/ml) among persons without HIV.
72, 73
Without confirmatory tests, such false-positive
results can lead to misdiagnosis of HIV infection.
37, 74, 75
When clinicians prescribe PrEP based
solely on the results of point of care rapid tests, a laboratory antigen/antibody test should always
be ordered at the time baseline labs are drawn. This will increase the likelihood of detecting
unrecognized acute infection so that the patient can be transitioned from PrEP to antiretroviral
treatment in a timely manner.
Figure 4a Clinician Determination of HIV Status for PrEP Provision to Persons
without Recent Antiretroviral Prophylaxis Use
Recent data have shown that the performance of HIV tests in persons who acquire HIV infection
while taking antiretroviral medications for PrEP differs from test performance in persons not
exposed to antiretrovirals at or after the time of HIV acquisition
76, 77
. The antiretrovirals used for
PrEP can suppress early viral replication which can affect the timing of antibody development.
Preexposure Prophylaxis for the Prevention of HIV Infection in the United States – 2021 Update Clinical Practice Guideline
Page 31 of 108
In HPTN 083, detection among participants in the cabotegravir group with antigen/antibody
testing was delayed by a mean of 62 days compared to detection by qualitative HIV-1 RNA
assay for infections determined to have been present at baseline; the delay was 98 days for
incident infections. Among participants in the F/TDF group, detection by antigen/antibody
testing was delayed by a mean of 34 days from qualitative HIV-1 RNA detection for baseline
infections and 31 days for incident infections
78
. In retrospective testing of stored specimens,
reversion of Ag/Ab tests was seen for some specimens from persons who received cabotegravir
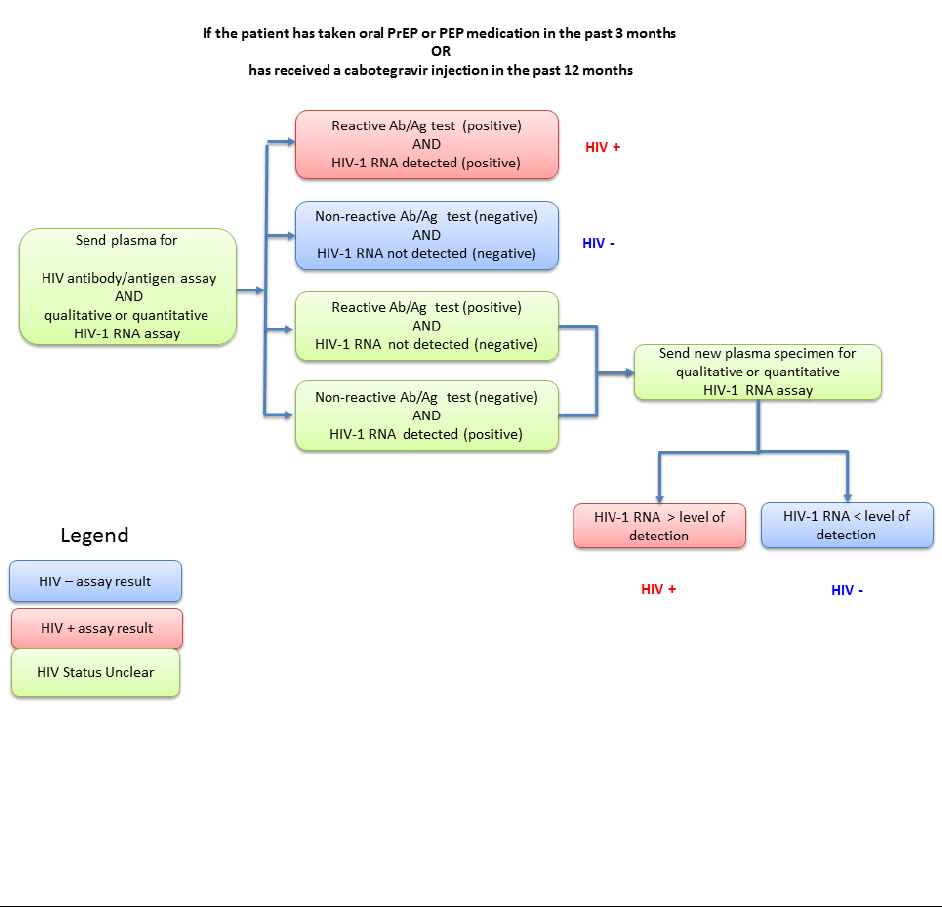
injections near the time of infection. For that reason, a different HIV testing algorithm is
recommended at follow-up visits for persons taking PrEP medication (Figure 4b).
Figure 4b Clinician Determination of HIV Status for PrEP Provision to Persons with
Recent or Ongoing Antiretroviral Prophylaxis Use
TESTING FOR SEXUALLY TRANSMITTED INFECTIONS
Tests to screen for syphilis are recommended for all adults prescribed PrEP, both at screening
and at semi-annual visits. See the 2021 STD guidelines for recommended assays.
79

Preexposure Prophylaxis for the Prevention of HIV Infection in the United States – 2021 Update Clinical Practice Guideline
Page 32 of 108
Tests to screen for gonorrhea are recommended for all sexually active adults prescribed PrEP,
both at screening, for MSM at quarterly visits, and for women at semi-annual visits. Tests to
screen for chlamydia are recommended for all sexually active MSM prescribed PrEP, both at
screening prior to initiation and at quarterly visits.
Chlamydia is very common, especially in young women
80
and does not correlate strongly with
risk of HIV acquisition
81, 82
so does not serve as an indication for initiating PrEP. However,
because it is a frequent infection among sexually active women at high risk, screening for
chlamydia is recommended at initiation and every 12 months for all sexually active women as a
component of PrEP care.
83
For MSM, gonorrhea and chlamydia screening using NAAT tests are preferred because of their
sensitivity. Pharyngeal, rectal, and urine specimens should be collected (“3-site testing”) to
maximize the identification of infection, which may occur at any of these sites of exposure
during sex. Patient self-collected samples have equivalent performance as clinician-obtained
samples
84-86
and can help streamline patient visit flow.
For women, both syphilis and gonorrhea correlate with risk of HIV acquisition.
81, 82, 87
Gonorrhea
screening of vaginal specimens by NAAT tests are preferred and may also be self-collected.
Although not indicated for all women who report anal sex, women being prescribed PrEP who
report engaging in anal sex are at higher risk
88
and so rectal specimens for gonorrhea and
chlamydia testing should be collected in addition to vaginal specimens.
88-91
Studies have
estimated that 29% of HIV infections in women are linked to sex with MSM (i.e., bisexual
men),
92, 93
a population with significantly higher prevalence of gonorrhea than men who have sex
only with women. More than one-third of women report having ever had anal sex,
94, 95
and 38%
of women at high risk of HIV acquisition in the HPTN 064 trial reported condomless anal sex in
the 6 months prior to enrollment.
96
Identifying asymptomatic rectal gonorrhea in women at
substantial risk for HIV acquisition and providing treatment can benefit the woman’s health and
help reduce the burden of infection in her sexual networks as well.
97, 98
Heterosexually-active adults and adolescents being evaluated for, or being prescribed PrEP, in
whom gonorrhea or chlamydia infection is detected, should be offered expedited partner therapy
(EPT),
99-101
especially for those patients whose partners are unlikely to access timely evaluation
and treatment. EPT is legal in most states but varies by chlamydia or gonorrhea infection.
Providers should visit http://www.cdc.gov/std/ept to obtain updated information for their state.
In light of limited data on the use of EPT for gonorrhea or chlamydial infection among MSM and
the potential for other bacterial STIs in MSM partners, shared clinical decision-making regarding
EPT is recommended. Patients with syphilis or HIV diagnosed should be referred for partner
services.
102, 103
LABORATORY TESTS FOR PATIENTS BEING CONSIDERED FOR ORAL PREP

Preexposure Prophylaxis for the Prevention of HIV Infection in the United States – 2021 Update Clinical Practice Guideline
Page 33 of 108
RENAL FUNCTION
In addition to confirming that any patient starting PrEP medication is not infected with HIV, a
clinician must assess renal function because decreased renal function is a potential safety issue
for the use of F/TDF or F/TAF as PrEP.
Both F/TDF and F/TAF are widely used in combination antiretroviral regimens for HIV
treatment.
37
Among persons with HIV prescribed TDF-containing regimens, mild decreases in
renal function (as measured by estimated creatinine clearance (eCrCl) have been documented,
and occasional cases of acute renal failure, including Fanconi’s syndrome, have occurred.
In observational studies and clinical trials of F/TDF PrEP use, small decreases in renal function
were likewise observed; these mostly reversed when PrEP was discontinued.
104, 105
In one
observational study with F/TDF, the development of decreased renal function was more likely in
patients >50 years of age or who had an eCrCl <90 ml/min when initiating PrEP with F/TDF.
106,
107
In the single clinical trial of F/TAF for PrEP among MSM (and a small number of TGW), no
decrease in renal function was observed.
4, 108
There was no difference in clinically important
renal health measures (e.g., grade 3 or 4 serious adverse renal events) between men taking
F/TDF or F/TAF in the DISCOVER trial. However, changes were seen in some biochemical
markers of proximal tubular function (e.g., ꞵ2-microlobulin:creatinine ratio, retinol binding
protein:creatinine ratio) that favored F/TAF.
4
This may indicate a longer-term safety benefit of
prescribing F/TAF for men with pre-existing risk factors for renal dysfunction (e.g.,
hypertension, diabetes).
Clinical trials and observational studies of F/TDF for PrEP have demonstrated safety when
prescribed to healthy, HIV-uninfected adults with an eCrCl≥60 ml/min. Safety data for F/TDF
prescribed for PrEP to patients with renal function <60 ml/min are not available. F/TAF is
approved for PrEP use in patients with an eCrCl ≥30 ml/min.
4
Therefore, for all persons
considered for PrEP with either F/TDF or F/TAF, a serum creatinine test should be done, and an
eCrCL should be calculated by using the Cockcroft-Gault formula (see Box A). Any person with
an eCrCl of ≥60 ml/min can safely be prescribed PrEP with F/TDF. PrEP with F/TAF can be
safely prescribed for persons with eCrCl of <60 ml/min but ≥30 ml/min.

Preexposure Prophylaxis for the Prevention of HIV Infection in the United States – 2021 Update Clinical Practice Guideline
Page 34 of 108
Box A: Cockcroft-Gault Formula
Basic Formula
109
eCrCl
CG
= [[(140 - age) × IBW × 0.85 for females] ÷ (serum creatinine × 72)]
IBW = ideal body weight Males: IBW = 50 kg + 2.3 kg for each inch over 5 feet
Females: IBW = 45.5 kg + 2.3 kg for each inch over 5 feet
Age in years, weight in kg, and serum creatinine in mg/100mL
TESTING FOR INFECTION WITH HEPATITIS B VIRUS (HBV)
Tenofovir and emtricitabine are also used to treat chronic HBV infection. When these drugs are
discontinued, patients with HBV infection may experience clinically significant hepatitis flares.
Ideally, prior to prescribing PrEP, patients should be screened for HBV
(https://www.cdc.gov/hepatitis/HBV/PDFs/SerologicChartv8.pdf) so that in the event they have
HBV infection, they can be informed of the danger of stopping PrEP medication without
appropriate monitoring for potential hepatitis flares. However, PrEP initiation should not be
withheld while waiting for HBV test results. Patients who are not immune and do not have HBV
infection should be vaccinated. Providers prescribing F/TDF or F/TAF as PrEP for patients who
have HBV infection (either known or first diagnosed as part of a PrEP evaluation) should do so
in consultation with a provider expert in HBV treatment.
LIPID PROFILE (F/TAF)
In the DISCOVER clinical trial comparing F/TDF and F/TAF for PrEP in MSM and transgender
women, higher rates of triglyceride elevation and of weight gain were seen among men taking
F/TAF than among men taking F/TDF. F/TDF has been associated with reductions in HDL and
LDL cholesterol that are not seen with F/TAF in the DISCOVER Trial.
4
This may indicate a
longer-term safety risk when prescribing F/TAF PrEP for men with pre-existing cardiovascular
health risk factors (e.g., obesity, age, lipid profiles). All persons prescribed F/TAF for PrEP
should have monitoring of triglyceride and cholesterol levels every 12 months. Lipid-lowering
medications should be prescribed when indicated.
TESTING NOT INDICATED ROUTINELY FOR ORAL PREP PATIENTS
In clinical trials for PrEP with F/TDF or F/TAF, additional testing was done to evaluate safety.
Findings in those trials indicated that DEXA scans to monitor bone mineral density (see section
on optional tests below), liver function tests, hematologic assays, and urinalysis are not indicated
for the routine care of all persons prescribed daily oral PrEP.

Preexposure Prophylaxis for the Prevention of HIV Infection in the United States – 2021 Update Clinical Practice Guideline
Page 35 of 108
Initial PrEP Prescription Visit for All Patients
GOALS OF PREP THERAPY
The ultimate goal of PrEP is to prevent the acquisition of HIV infection with its resulting
morbidity, mortality, and cost to individuals and society. Therefore, clinicians initiating the
provision of PrEP should:
• Prescribe medication regimens that are proven safe and effective for uninfected patients
who meet recommended criteria for PrEP initiation to reduce their risk of HIV
acquisition;
• Educate patients about the medications and the regimen to maximize their safe use;
• Provide support for medication-adherence to help patients achieve and maintain
protective levels of medication in their bodies;
• Provide HIV risk-reduction support and prevention services or service referrals to help
patients minimize their exposure to HIV and other STIs;
• Provide (or refer for) effective contraception to persons with childbearing potential who
are taking PrEP and who do not wish to become pregnant; and
Monitor patients to detect HIV infection, medication toxicities, and levels of risk
behavior in order to make indicated changes in strategies to support patients’ long-term
health.
SAME DAY PREP PRESCRIBING
For all patients, safely initiating PrEP requires determination of HIV status and assessment of
renal function. Safely shortening the time to initiation of PrEP may be useful for some patients.
For example, some patients may have time or work constraints that impose a significant burden
to return to the clinic a week or two after evaluation for a prescription visit. Other patients report
risk behaviors that put them at substantial risk of acquiring HIV infection in the time between
visits for evaluation and PrEP prescription. However, for all patients, safely initiating PrEP
requires determination of HIV status and assessment of renal function. Some sites have
developed protocols that allow them to safely initiate PrEP on the same day as the initial
evaluation for many patients.
110-112
To use a same-day PrEP initiation protocol, the clinic must be able to:
• Conduct point-of-care HIV testing, ideally with an antigen/antibody fingerstick or other
blood test
o Where same-day results can be obtained, laboratory-based antigen/antibody test
or an HIV-1 RNA test can be used (and is preferred)
o Oral fluid HIV testing should not be used in the context of PrEP initiation
• Draw blood for laboratory creatinine and HIV testing when same day HIV and creatinine
test results are not available

Preexposure Prophylaxis for the Prevention of HIV Infection in the United States – 2021 Update Clinical Practice Guideline
Page 36 of 108
o Where available, a point of care blood creatinine test may be used
• Provide assistance for eligible patients to enroll in health insurance, medication co-
payment assistance, or medication assistance programs for those who are uninsured or
underinsured
• Provide rapid follow-up contact for patients whose laboratory test results indicate HIV
infection or renal dysfunction
• Provide scheduled follow-up care appointments
• Have clinicians available to dispense or prescribe oral PrEP medication, to administer a
gluteal intramuscular injection of CAB, or optionally prescribe a daily oral CAB lead-in
for 4 weeks.
Optionally, clinics would be able to provide (on the first day):
• STI specimen collection for laboratory testing
Same-day PrEP initiation is not appropriate for:
• Patients who express ambivalence about starting PrEP (e.g., need more time to think)
• Patients for whom blood cannot be drawn for laboratory testing
• Patients with signs/symptoms and sexual history indicating possible acute HIV infection
• Patients with history of renal disease or associated conditions (e.g., hypertension,
diabetes)
• Patients without insurance or a means to pay when picking up the prescribed medication
that day
• Patients who do not have a confirmed means of contact should laboratory test indicate a
need to discontinue PrEP (e.g., HIV infection, unanticipated renal dysfunction)
Same-day PrEP initiation may not be appropriate for:
• Patients with a very recent possible HIV exposure but no signs and symptoms of acute
infection (should be evaluated for nPEP before PrEP)
• Patients who may not be easily contacted for return appointments
• Patients with mental health conditions that are severe enough to interfere with
understanding of PrEP requirements (adherence, follow-up visits)
NONOCCUPATIONAL POSTEXPOSURE PROPHYLAXIS
Patients not receiving PrEP who seek care within 72 hours after an isolated sexual or injection-
related HIV exposure should be evaluated for the potential need for nPEP.
113
If the exposure is
isolated (e.g., sexual assault, infrequent condom failure), nPEP should be prescribed, but PrEP or
other continued antiretroviral medication is not indicated after completion of the 28-day PEP
course.
Preexposure Prophylaxis for the Prevention of HIV Infection in the United States – 2021 Update Clinical Practice Guideline
Page 37 of 108
Patients who seek one or more courses of nPEP and who are at risk for ongoing HIV exposures
should be evaluated for possible PrEP use after confirming they have not acquired HIV
142
.
Because HIV infection has been reported in association with exposures soon after completing an
nPEP course,
114, 115
daily PrEP may be more protective than repeated intermittent episodes of
nPEP. Patients who engage in behaviors that result in frequent, recurrent exposures that would
require sequential or near-continuous courses of nPEP should be offered PrEP at the conclusion
of their 28-day nPEP medication course. Because nPEP is highly effective when taken as
prescribed, a gap is unnecessary between ending nPEP and beginning PrEP. Upon documenting
HIV-negative status, preferably by using a laboratory-based Ag/Ab test or plasma HIV-1 RNA
test (see figure 4), daily use of F/TDF OR F/TAF or CAB injections every 2 months can begin
immediately for patients for whom PrEP is indicated. See Clinical Providers’ Supplement
Section 8 for a recommended transition management strategy.
In contrast, patients fully adhering to a daily PrEP regimen or who have received CAB injections
on schedule do not need nPEP if they experience a potential HIV exposure while on PrEP. PrEP
is highly effective when taken daily or near daily. For patients who report taking their PrEP
medication sporadically, and those who did not take it within the week before the recent
exposure, initiating a 28-day course of nPEP might be indicated. In that instance, all nPEP
baseline and follow-up laboratory evaluations should be conducted
(https://www.cdc.gov/hiv/pdf/programresources/cdc-hiv-npep-guidelines.pdf). If, after the 28-
day nPEP regimen is completed, the patient is confirmed to be HIV uninfected, any previously
experienced barriers to PrEP adherence should be evaluated and if addressed, a PrEP regimen
can be reinitiated.
PRESCRIBING ORAL PREP
RECOMMENDED ORAL MEDICATION
The fixed-dose combination of F/TDF in a single daily dose (see Table 3), is approved by FDA
for PrEP in healthy adults and adolescents at risk of acquiring HIV. F/TDF continues to be most
commonly prescribed for PrEP (including PWID) who meet criteria for PrEP use. F/TDF is
available as a generic medication that is equivalent to the brand name medication (Truvada).
F/TAF has recently been approved for daily PrEP use by men and transgender women at sexual
risk. F/TAF is not approved for PrEP use by women at risk through receptive vaginal sex for
whom F/TDF should be prescribed instead. F/TAF and F/TDF have equivalent high efficacy and
safety as PrEP for men at sexual risk.
3, 116
Generic F/TAF is not available.
For most patients, there is no need to switch from F/TDF to F/TAF. While incremental
differences in laboratory markers of bone metabolism and renal function have been seen in some
studies, no differences in clinically meaningful adverse events have been seen
4
. However, F/TAF
is indicated for patients with eCrCl <60 ml/min but ≥30 ml/min. Either F/TDF or F/TAF can be

Preexposure Prophylaxis for the Prevention of HIV Infection in the United States – 2021 Update Clinical Practice Guideline
Page 38 of 108
used when eCrCl ≥60 ml/min.
117
Clinicians may prefer F/TAF for persons with previously
documented osteoporosis or related bone disease but routine screening for bone density is not
recommended for PrEP patients.
Table 3: Recommended Oral PrEP Medications
Generic
Name
Trade
Name
Dose
Frequency
Most Common Side
Effects
109,110
F/TDF
Truvada
200 mg/300 mg
Once a day
Headache, abdominal
pain, weight loss
F/TAF
Descovy
200 mg/25 mg
Once a day
Diarrhea
WHAT NOT TO USE FOR ORAL PREP
No antiretroviral regimens should be used for PrEP other than a daily oral dose of F/TDF or
F/TAF or injections of CAB every 2 months
No other medications or other dosing schedules are approved by FDA for PrEP to prevent HIV
acquisition among otherwise healthy adults and adolescents.
▪ Do not prescribe other antiretroviral medications either in place of, or in addition to
F/TDF or F/TAF.
▪ Do not prescribe other than continuous daily dosing of oral PrEP with the possible
exception of MSM (see section on clinical considerations for MSM).
▪ Do not provide oral PrEP as expedited partner therapy (i.e., do not prescribe for a person
not in your care).
Data on drug interactions and longer-term toxicities of TDF and TAF have been obtained mostly
from studies of their use in treatment of HIV-infected persons. Small studies have also been done
in HIV-uninfected, healthy adults (see Table 4).
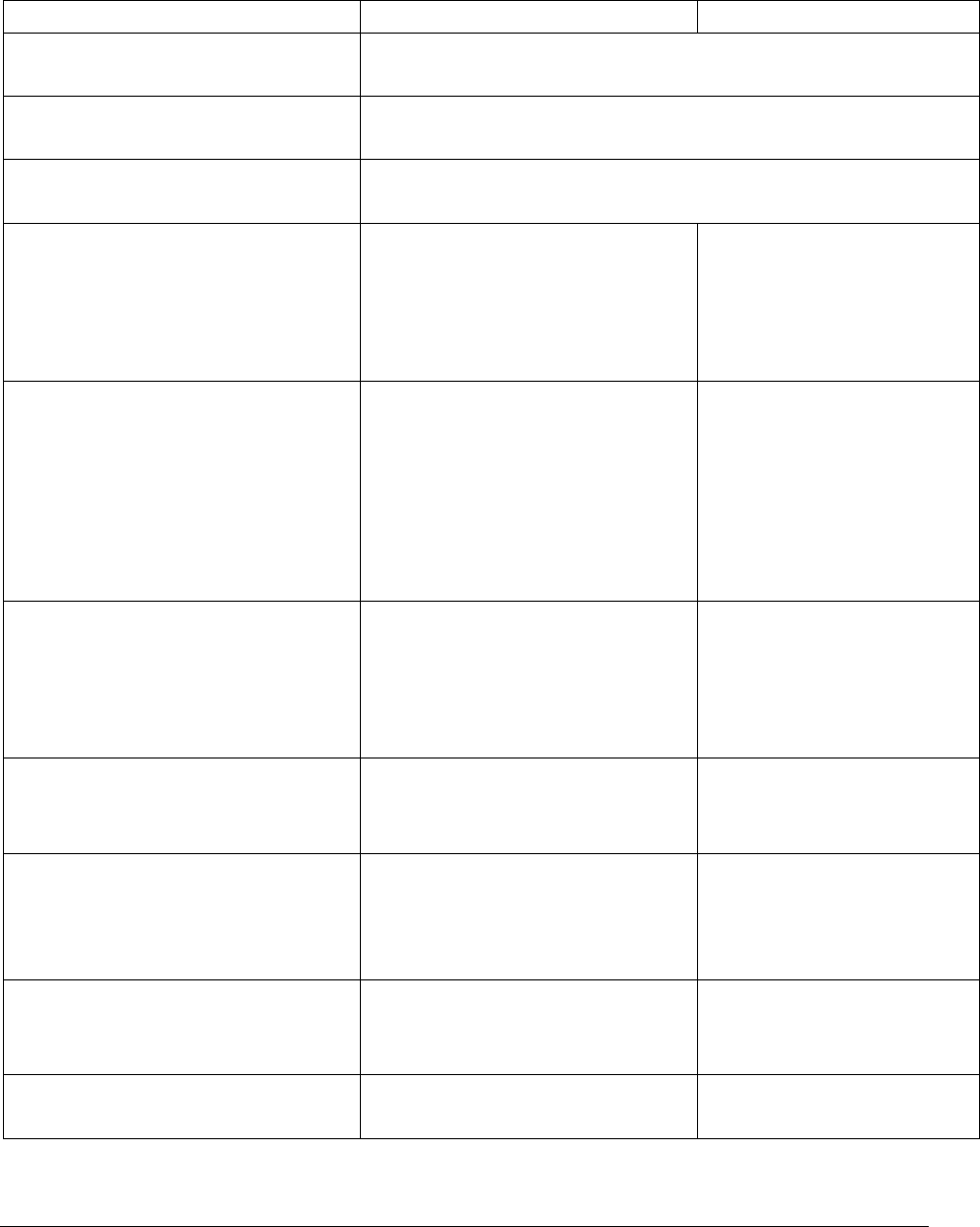
Preexposure Prophylaxis for the Prevention of HIV Infection in the United States – 2021 Update Clinical Practice Guideline
Page 39 of 108
Table 4: Oral PrEP Medication Drug Interactions
37, 118, 119
TDF
TAF
Buprenorphine
No significant effect
No dosage adjustment necessary
Methadone
No significant effect
No dosage adjustment necessary
Oral contraceptives
No significant effect
No dosage adjustment necessary
Feminizing hormones
(Spironolactone, estrogens)
Lower tenofovir-diphosphate
rectal tissue levels (unknown if it
affects PrEP effectiveness).
TDF does not affect hormone
levels
No data available
Acyclovir, valacyclovir, cidofovir,
ganciclovir, valganciclovir,
aminoglycosides, high-dose or
multiple NSAIDS or other drugs
that reduce renal function or
compete for active renal tubular
secretion
Serum concentrations of these
drugs and/or TDF may be
increased. Monitor for dose-
related renal toxicities
No data available
Adefovir
Do not co-administer with
TDF
Serum concentration of TDF
may be increased, monitor for
toxicities
No data available
Ledipasvir, sofosbuvir, velpatasvir,
voxilaprevir
Serum concentrations of TDF
may be increased. Monitor for
toxicities
No significant effect
St John’s Wort
No significant effect
Do not co-administer
with TAF
Decrease in TAF
concentration possible
Rifampin
No significant effect
Do not co-administer
with TAF unless benefits
outweigh risks
Rifabutin, Rifapentine
No significant effect
Do not co-administer
with TAF
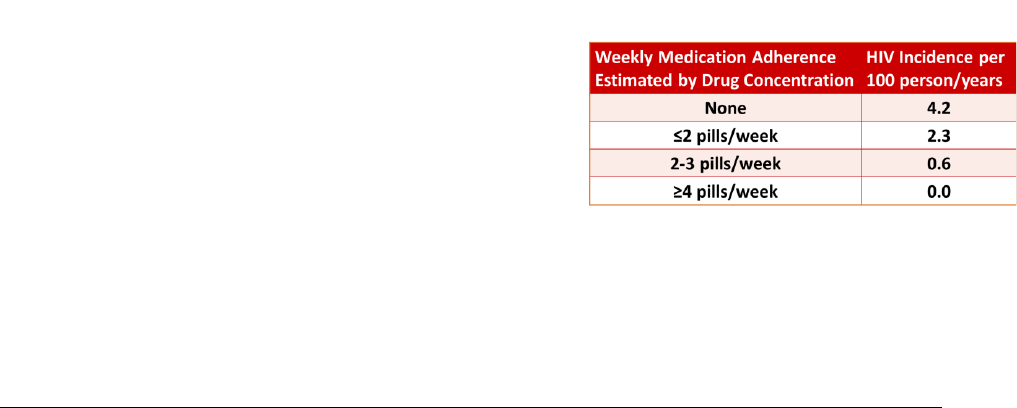
Preexposure Prophylaxis for the Prevention of HIV Infection in the United States – 2021 Update Clinical Practice Guideline
Page 40 of 108
PROVIDING PREP BY TELEHEALTH
Recent expansion of telehealth visits to replace some or all in-clinic visits have led to adaptations
for provision of PrEP.
120, 121
These adaptations can include the following procedures:
▪ Conduct PrEP screening, initiation, or follow-up visits by phone or web-based consult
with clinicians
▪ Obtain specimens for HIV, STI, or other PrEP-related laboratory tests by:
o Laboratory visits for specimen collection only
o Order home specimen collection kits for specified tests.
▪ Specimen kits are mailed to the patient’s home and contain supplies to
collect blood from a fingerstick or other appropriate method (e.g. self-
collected swabs and urine).
▪ The kit is then mailed back to the lab with test results returned to the
clinician who acts on results accordingly.
o For HIV testing, only if a patient has no possible access to a lab (in-person or by
mail), clinicians can provide an oral swab-based self-test that the patient can
conduct and report the result to the clinician (e.g., photo of the test result).
Because of the low sensitivity of oral Ab tests in detection of acute HIV infection,
this should only be used for PrEP patients as a last resort.
▪ When HIV-negative status is confirmed, provide a prescription for a 90-day supply of
PrEP medication (rather than a 30-day supply with two refills) to minimize trips to the
pharmacy and to facilitate PrEP adherence.
COUNSELING TO SUPPORT ORAL MEDICATION ADHERENCE AND PERSISTENCE IN
CARE
Data from the published clinical trials and observational studies of daily oral PrEP indicate that
medication adherence is critical to achieving the maximum prevention benefit (see Figure 5) and
reduce the risk of selecting for a drug-resistant virus if HIV infection occurs.
122-124
Data from a pharmacokinetics study with MSM given
directly observed TDF dosing were applied in a statistical
model to assess the relationship of dosing frequency to
protective efficacy. Based on the intracellular
concentrations of the active form of TDF (tenofovir
diphosphate), HIV risk reduction efficacy was estimated to
be of 99% for 7 doses per week, 96% for 4 doses per
week, and 76% for 2 doses per week.
125, 126
This finding suggests that although there is some
“forgiveness” for occasional missed doses of F/TDF PrEP for MSM, a high level of prevention
efficacy requires a high level of adherence to daily medication.
However, a laboratory study comparing vaginal and colorectal tissue levels of active metabolites
of TDF and FTC found that drug levels associated with significant protection against HIV
Figure 5: Adherence and F/TDF PrEP Efficacy in MSM

Preexposure Prophylaxis for the Prevention of HIV Infection in the United States – 2021 Update Clinical Practice Guideline
Page 41 of 108
infection required 6-7 doses per week (>85% adherence) for lower vaginal tract tissues but only
2 doses per week (28% adherence) for colorectal tissues.
127
This strongly suggests that there is
less “forgiveness” for missed doses among women than among MSM.
Approaches that can effectively support medication adherence include educating patients about
their medications; helping them anticipate and manage side effects; asking about adherence
successes and issues at follow-up visits (Box
B),
128
helping them establish dosing routines that
mesh with their work and social schedules;
providing reminder systems and tools; addressing
financial, substance use disorder, or mental
health needs that may impede adherence; and
facilitating social support. Data from PrEP trials
and observational studies have observed lower
adherence among younger MSM when seen
quarterly but higher adherence when visits were monthly.
9, 10
In terms of patient education, clinicians must ensure that patients understand clearly how to take
their medications (i.e., when to take them, how many pills to take at each dose) and what to do if
they experience problems (e.g., what constitutes a missed dose [number of hours after the failure
to take a scheduled dose], what to do if they miss a dose). Patients should be told to take a single
missed dose as soon as they remember it, unless it is almost time for the next dose. If it is almost
time for the next dose, patients should skip the missed dose and continue with the regular dosing
schedule.
Side effects can lead to non-adherence, so clinicians need a plan for addressing them. Clinicians
should tell patients about the most common side effects and should work with patients to develop
a specific plan for handling them, including the use of specific over-the-counter medications that
can mitigate symptoms. The importance of using condoms during sex for STI prevention, and for
HIV prevention in patients who decide to stop taking their PrEP medications, should be
reinforced.
Clinicians should reinforce patient understanding that the benefits of PrEP medication use
outweigh its reported risks and that the schedule of follow-up monitoring visits is designed to
address any potential medication-related harm in a timely manner. Clinician should review signs
and symptoms of active HIV infection and the need for rapid evaluation and HIV testing and
should review how to safely discontinue or restart PrEP use (e.g., get an HIV test).
A brief medication adherence question
“Many people find it difficult to take a
medicine every day.
Thinking about the last week; on how
many days have you not taken your
medicine?”

Preexposure Prophylaxis for the Prevention of HIV Infection in the United States – 2021 Update Clinical Practice Guideline
Page 42 of 108
Box B: Key Components of Oral Medication Adherence Counseling
Using a broad array of health care professionals (e.g., physicians, nurses, case-managers,
physician assistants, clinic-based and community pharmacists) that work together on a health
care team to influence and reinforce adherence instructions
129
significantly improves medication
adherence and may alleviate the time constraints of individual providers.
130, 131
This team-based
approach may also provide a larger number of providers to counsel patients about self-
management of behavioral risks.
MANAGING SIDE EFFECTS OF ORAL PREP
Patients taking PrEP should be informed of potential side effects. Some (<10%) of patients
prescribed F/TDF or F/TAF experience a “start-up syndrome” that usually resolves within the
first month of taking PrEP medication. This may include headache, nausea, or abdominal
discomfort. Clinicians should discuss the use of over-the-counter medications should these
temporary side effects occur. Patients should also be counseled about signs or symptoms that
indicate a need for urgent evaluation when they occur between scheduled follow-up visits (e.g.,
those suggesting possible acute renal injury or acute HIV infection). Weight gain is a reported
side effect of F/TAF for PrEP.
4, 119
TIME TO ACHIEVING PROTECTION WITH DAILY ORAL PREP
The time from initiation of daily PrEP use to maximal protection against HIV infection is
unknown. It has been shown that the pharmacokinetics of TDF and FTC vary by tissue,
127, 132
Establish trust and bidirectional communication
Provide simple explanations and education
▪ Medication dosage and schedule
▪ Management of common side effects
▪ Relationship of adherence to the efficacy of PrEP
▪ Signs and symptoms of acute HIV infection and recommended actions
Support adherence
▪ Tailor daily dose to patient’s daily routine
▪ Identify reminders and devices to minimize forgetting doses
▪ Identify and address barriers to adherence
▪ Reinforce benefit relative to uncommon harms
Monitor medication adherence in a non-judgmental manner
▪ Normalize occasional missed doses, while ensuring patient understands importance of
daily dosing for optimal protection
▪ Reinforce success
▪ Identify factors interfering with adherence and plan with patient to address them
▪ Assess side effects and plan how to manage them

Preexposure Prophylaxis for the Prevention of HIV Infection in the United States – 2021 Update Clinical Practice Guideline
Page 43 of 108
but there is not scientific consensus on what tissue-specific intracellular concentrations are
protective (see review of available data here:
https://www.youtube.com/watch?v=5WfNqJPIIH8).
Data from exploratory F/TDF pharmacokinetic studies suggest that maximum intracellular
concentrations of TFV-DP, the active form of tenofovir, are reached in blood PMBCs after
approximately 7 days of daily oral dosing, in rectal tissue at approximately 7 days, and in
cervicovaginal tissues at approximately 20 days.
F/TAF pharmacokinetic study data related to potential time to tissue-specific maximum
concentrations are not yet available, so the time from initiation of daily F/TAF for PrEP to
maximal tissue protection from HIV infection is not known.
Data is not available for either F/TDF or F/TAF PrEP in penile tissues susceptible to HIV
infection to inform considerations of time to protection for male insertive sex partners.
FOLLOW-UP PREP CARE VISITS FOR ORAL PREP PATIENTS
CLINICAL FOLLOW-UP AND MONITORING FOR ORAL PREP
Once daily oral PrEP is initiated, patients should return for follow-up approximately every 3
months by in-person, virtual, or phone visits. Clinicians may wish to schedule contact with
patients more frequently at the beginning of PrEP either by phone or clinic visit (e.g., 1 month
after initiation, to assess and confirm HIV-negative test status, assess for early side effects,
discuss any difficulties with medication adherence, and answer questions.
All patients receiving oral PrEP should be seen in follow-up:
▪ At least every 3 months to:
o Repeat HIV testing and assess for signs or symptoms of acute infection to document
that patients are still HIV negative (see Figure 4);
o Provide a prescription or refill authorization of daily PrEP medication for no more
than 90 days (until the next HIV test);
o Assess and provide support for medication adherence and risk-reduction behaviors;
o Conduct STI testing for sexually active persons with signs or symptoms of infection
and screening for asymptomatic MSM at high risk for recurrent bacterial STIs (e.g.,
those with syphilis, gonorrhea, or chlamydia at prior visits or multiple sex partners);
and
o Respond to new questions and provide any new information about PrEP use.
▪ At least every 6 months to:
o Monitor eCrCl for persons age ≥50 years or who have an eCrCl <90 ml/min at PrEP
initiation.
Preexposure Prophylaxis for the Prevention of HIV Infection in the United States – 2021 Update Clinical Practice Guideline
Page 44 of 108
• If other threats to renal safety are present (e.g., hypertension, diabetes), renal
function may require more frequent monitoring or may need to include additional
tests (e.g., urinalysis for proteinuria).
• A rise in serum creatinine is not a reason to withhold treatment if eCrCl remains
≥60 ml/min for F/TDF or ≥30 for F/TAF.
• If eCrCl is declining steadily (but still ≥60 ml/min for F/TDF or ≥30 ml/min for
F/TAF), ask if the patient is taking high doses of NSAID or using protein
powders; consultation with a nephrologist or other evaluation of possible threats
to renal health may be indicated.
o Conduct STI screening for sexually active persons (i.e., syphilis, gonorrhea, for all
PrEP patients and chlamydia for MSM and TGW even if asymptomatic.
o Assess interest in continuing or discontinuing PrEP.
▪ At least every 12 months to:
o Monitor eCrCl for all patients continuing on PrEP medication.
o Monitor triglyceride, cholesterol levels, and weight for patients prescribed F/TAF for
PrEP.
o Conduct chlamydia screening for heterosexual women and men even if asymptomatic
LABORATORY TESTING SCHEDULE FOR ORAL PREP PATIENTS
Table 5 Timing of Oral PrEP-associated Laboratory Tests
Test
Screening/Baseline
Visit
Q 3 months
Q 6 months
Q 12 months
When stopping
PrEP
HIV Test
X*
X
X*
eCrCl
X
If age ≥50 or
eCrCL <90
ml/min at
PrEP
initiation
If age <50 and
eCrCl ≥90
ml/min at
PrEP
initiation
X
Syphilis
X
MSM /TGW
X
MSM/TGW
Gonorrhea
X
MSM /TGW
X
MSM /TGW
Chlamydia
X
MSM /TGW
X
MSM /TGW
Lipid panel
(F/TAF)
X
X
Hep B serology
X
Hep C serology
MSM, TGW, and
PWID only
MSM,TGW,
and PWID
only
* Assess for acute HIV infection (see Figure 4)

Preexposure Prophylaxis for the Prevention of HIV Infection in the United States – 2021 Update Clinical Practice Guideline
Page 45 of 108
OPTIONAL ASSESSMENTS FOR PATIENTS PRESCRIBED ORAL PREP
Bone Health
Decreases in bone mineral density (BMD) have been observed in HIV-infected persons treated
with combination antiretroviral therapy (including TDF-containing regimes).
114,115
However, it is
unclear whether this 3%-4% decline would be seen in HIV-uninfected persons taking fewer
antiretroviral medications for PrEP. The iPrEx trial evaluating F/TDF and the CDC PrEP safety
trial in MSM evaluating TDF conducted serial dual-emission x-ray absorptiometry (DEXA)
scans on a subset of MSM in the trials and determined that a small (~1%) decline in BMD that
occurred during the first few months of PrEP either stabilized or returned to normal.
23,116
There
was no increase in fragility (atraumatic) fractures over the 1-2 years of observation in these
studies comparing those persons randomized to receive PrEP medication and those randomized
to receive placebo.
117
In the DEXA substudy of the DISCOVER trial, men randomized to F/TAF
showed slight mean percentage increases in BMD at the hip and spine through 96 weeks of
observation, while men randomized to F/TDF showed mild decreases at both anatomic sites.
However, there was no difference in the frequency of fractures between the treatment groups
with 91% of fractures related to trauma.
3,76
Therefore, DEXA scans or other assessments of bone health are not recommended before the
initiation of PrEP or for the monitoring of persons while taking PrEP. However, any person
being considered for PrEP who has a history of pathologic or fragility bone fractures or who has
significant risk factors for osteoporosis should be referred for appropriate consultation and
management.
Medication adherence drug monitoring
Several factors limit the utility of routine use of laboratory measures of medication adherence
during PrEP. These factors include: (1) a lack of established concentrations in blood associated
with robust efficacy of tenofovir (either TDF or TAF), or emtricitabine for the prevention of
HIV acquisition in adults after exposure during penile-rectal or penile-vaginal intercourse
133
and
(2) the limited but growing availability of clinical laboratories that can perform quantitation of
antiretroviral medicine concentrations under rigorous quality assurance and quality control
standards.
Several point-of-care tests are being used in research to assess adherence to daily oral PrEP.
None are yet FDA approved and CLIA waived for point-of-care use. These tests include: a urine
test that can assess adherence over the past few days,
134, 135
and a dried blood spot test that
measures red blood cell concentrations of tenofovir (from either TDF or TAF) and emtricitabine
active metabolites and can measure both short term (past few days) and longer term (past 6
weeks) adherence.
126, 136
A hair analysis test is being used in research to measure longer term
adherence (from past 1-6 months, depending on the length of hair available).
137
For any of these
measures, undetectable or low PrEP drug levels indicate the need to reinforce medication
adherence. Conversely, documented high drug levels may positively reinforce patients’
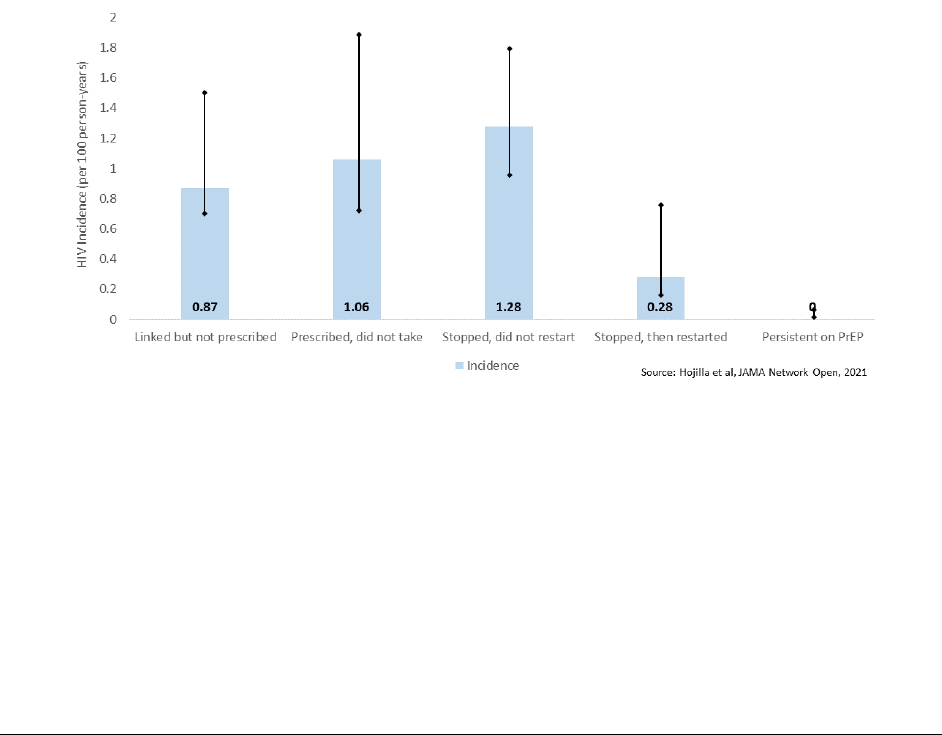
Preexposure Prophylaxis for the Prevention of HIV Infection in the United States – 2021 Update Clinical Practice Guideline
Page 46 of 108
adherence efforts. A home specimen-collection kit for a validated, CLIA-waived urine (very
recent adherence) or dried blood spot (longer term adherence) tenofovir assay is now available
from some laboratories.
121
DISCONTINUING AND RESTARTING DAILY ORAL PREP
PrEP medication may be discontinued for several reasons, including patient choice, changed life
situations resulting in lowered risk of HIV acquisition, intolerable toxicities, chronic
nonadherence to the prescribed dosing regimen or scheduled follow-up care visits, or acquisition
of HIV. How to safely discontinue and restart daily PrEP use should be discussed with patients
both when starting PrEP and when discontinuing PrEP. Protection from HIV infection will wane
over 7-10 days after ceasing daily PrEP use.
138, 139
Because some patients have acquired HIV
soon after stopping PrEP use,
140
alternative methods to reduce risk for HIV acquisition should be
discussed, including indications for nPEP and how to access it quickly if needed.
Figure 6 HIV Incidence in MSM Before, While Taking, and After Discontinuing
F/TDF PrEP Use
140, 141
Upon discontinuation of PrEP for any reason, the following should be documented in the health
record:
▪ HIV status at the time of discontinuation;
▪ Reason for discontinuation; and
▪ Recent medication adherence and reported sexual risk behavior.
For persons with incident HIV infection, see Persons with Documented HIV Infection. See also
Clinical Providers’ Supplement Section 8 for a suggested management protocol.

Preexposure Prophylaxis for the Prevention of HIV Infection in the United States – 2021 Update Clinical Practice Guideline
Page 47 of 108
Patients with HBV infection who discontinue taking PrEP medication should be monitored
closely for hepatitis flares. Although documented to occur in some patients discontinuing
tenofovir-containing medication as part of their treatment regimens, such flares have not yet been
seen in HIV-uninfected patients with chronic active HBV infection who have stopped taking
TDF-containing PrEP regimens. Nonetheless, when such patients discontinue PrEP, they should
continue to receive care from a clinician experienced in the management of HBV infection so
that if flares occur, they can be detected promptly and treated appropriately.
Any person who wishes to resume taking PrEP medications after having stopped requires the
same pre-prescription evaluation as a person being newly prescribed PrEP, including an HIV test
to establish that they have not acquired HIV. In addition, discuss and document the changed
circumstances since discontinuing PrEP that indicate the need to restart medication and confirm
the commitment to take it as prescribed.
PRESCRIBING CABOTEGRAVIR PREP INJECTIONS
Patients considering PrEP should be informed of all FDA approved options. Cabotegravir
injections may be especially appropriate for patients with significant renal disease, those who
have had difficulty with adherent use of oral PrEP and those who prefer injections every 2
months to an oral PrEP dosing schedule. Cabotegravir should not be administered to persons
with a history of hypersensitivity reaction to cabotegravir.
RECOMMENDED MEDICATION
o 600 mg of cabotegravir injected into gluteal muscle every 2 months is recommended
(conditional on FDA approval) for PrEP in adults at risk of acquiring HIV.
o 30 mg daily oral cabotegravir is optional for a 4-week lead-in prior to injections.
WHAT NOT TO USE
Other than those recommended in this guideline, no other injectable antiretrovirals, injection
sites, or dosing schedules should be used as their efficacy is unknown.
o Do not administer or prescribe other antiretroviral medications in combination with CAB
for PrEP.
o Do not administer CAB injections at any site other than gluteal muscle because the
pharmacokinetics of drug absorption with injection at other sites is unknown
o Do not dispense CAB injections for use by patients for home administration (unless and
until self-administration is FDA approved).
o Do not prescribe ongoing daily oral CAB (other than for lead-in prior to initiating or
restarting injections).
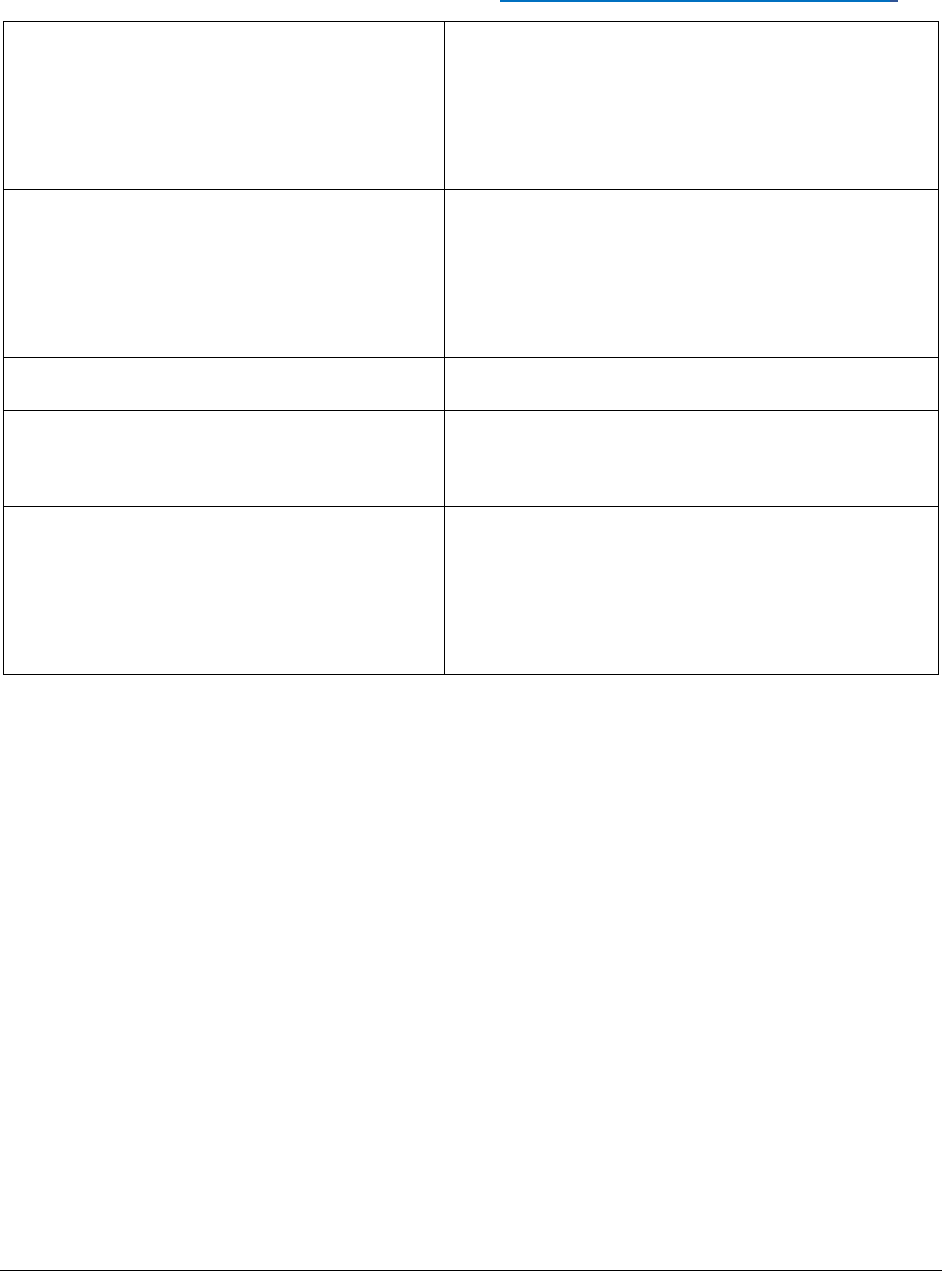
Preexposure Prophylaxis for the Prevention of HIV Infection in the United States – 2021 Update Clinical Practice Guideline
Page 48 of 108
Table 6 Cabotegravir PrEP Drug Interactions (https://www.hiv-druginteractions.org/)
Rifampicin, rifapentin
Do not co-administer with CAB
Rifampicin and rifapentine increase metabolism
of CAB and may result in significantly reduced
exposure to protective levels of CAB
142, 143
Rifabutin
Co-administer with caution
Rifabutin moderately increases metabolism of
CAB and may result in somewhat reduced
exposure to protective levels of CAB
144
Hormonal contraceptives
No significant effect
145
Feminizing hormones
(Spironolactone, estrogens)
No data yet available
146
Carbamazepine, oxcarbazepine, phenytoin,
phenobarbital
Do not co-administer with CAB
Concern that these anticonvulsants may result in
significantly reduced exposure to protective
levels of CAB but strength of evidence is weak
CAB PREP INITIATION VISIT
In the clinical trials of CAB injections for PrEP, patients were provided oral CAB 30 mg tablets
daily for 5 weeks prior to receiving the first injection.
147
Because there were no safety concerns
identified during this lead-in period or during the injection phase of the studies, an oral lead-in is
not required when initiating CAB PrEP. It may be optionally used for patients who are especially
worried about side effects to relieve anxiety about using the long-acting CAB injection.
However, continued daily oral CAB is not recommended or FDA-approved for PrEP.
Patients who have been taking daily oral PrEP, can initiate CAB injections as soon as HIV-1
RNA test results confirm that they remain HIV negative.
LABORATORY TESTING FOR CAB PREP PATIENTS
Patients whose HIV test results indicate that they do not have acute or chronic HIV infection can
be considered for initiation of cabotegravir injections (see Figure 4b). Because of the long
duration of drug exposure following injection, exclusion of acute HIV infection is necessary with
the most sensitive test available, an HIV-1 RNA assay. Ideally, this testing will be done within 1

Preexposure Prophylaxis for the Prevention of HIV Infection in the United States – 2021 Update Clinical Practice Guideline
Page 49 of 108
week prior to the initiation visit. If clinicians wish to provide the first injection at the first PrEP
evaluation visit based on the result of a rapid combined antigen/antibody assay, blood should
always be drawn for laboratory confirmatory testing that includes an HIV RNA assay.
All PrEP patients should have baseline STI tests (see Table 1b).
Preexposure Prophylaxis for the Prevention of HIV Infection in the United States – 2021 Update Clinical Practice Guideline
Page 50 of 108
Table 7 Timing of CAB PrEP-associated Laboratory Tests
Test
Initiation Visit
1 month
visit
Q2
months
Q4
months
Q6
months
Q12
months
When
Stopping
CAB
HIV*
X
X
X
X
X
X
X
Syphilis
X
MSM^/TGW
~
only
Heterosexually
active women
and men only
X
MSM/TGW
only
Gonorrhea
X
MSM/TGW
only
Heterosexually
active women
and men only
X
MSM/TGW
only
Chlamydia
X
MSM/TGW
only
MSM/TGW
only
Heterosexually
active women
and men only
MSM/TGW
only
* HIV-1 RNA assay
X all PrEP patients
^ men who have sex with men
~
persons assigned male sex at birth whose gender identification is female

Preexposure Prophylaxis for the Prevention of HIV Infection in the United States – 2021 Update Clinical Practice Guideline Page
51 of 108
TESTING NOT INDICATED ROUTINELY FOR CAB PREP PATIENTS
Based on the results of the CAB clinical trials,
12, 147, 148
the following laboratory tests are NOT
indicated before starting CAB injection or for monitoring patients during its use: creatinine,
eCrCl, hepatitis B serology, lipid panels, liver function tests.
Screening tests associated with routine primary care and not specific to the provision of CAB for
PrEP are discussed in the primary care section (see Table 8)
RECOMMENDED CAB INJECTION
o 3 ml suspension of CAB 600 mg IM in gluteal muscle (gluteus medius or gluteus
maximus)
o The use of a 2-inch needle is recommended for intramuscular injection for participants
with a body-mass index (BMI) of 30 or greater, and a 1.5-inch needle for participants
with a BMI of less than 30
MANAGING INJECTION SITE REACTIONS
In the clinical trials, injection site reactions (pain, tenderness, induration) were frequent
following CAB injections. These reactions were generally mild or moderate, lasted only a few
days, and occurred most frequently after the first 2-3 injections. Patients should be informed that
these reactions are common and transient. In addition, they should be provided with proactive
management advice
• for the first 2-3 injections
o take an over-the-counter pain medication within a couple of hours before or soon
after the injection and continue as needed for one to two days
o apply a warm compress or heating pad to the injection site for 15-20 minutes after the
injection (e.g., after arriving back at home)
• thereafter, as needed for subsequent injections
PATIENT EDUCATION/COUNSELING
Patients should be provided an appointment for the next injection 1 month after the initial one.
Patients should be educated about:
o the long “tail” of gradually declining drug levels when discontinuing CAB injections
and the risk of developing a drug-resistant strain if HIV infection is acquired during
that time
o the importance of keeping their follow-up appointments if they have decided not to
continue with CAB injections for PrEP

Preexposure Prophylaxis for the Prevention of HIV Infection in the United States – 2021 Update Clinical Practice Guideline Page
52 of 108
CLINICAL FOLLOW-UP AND MONITORING FOR CAB INJECTIONS
Once CAB injections are initiated, patients should return for follow-up visits 1 month after the
initial injection and then every 2 months.
• At visit 1 month after initial injection (month 1, second injection)
o Repeat HIV-1 RNA test and assess for signs or symptoms of acute infection
o Administer CAB injection
o Respond to new questions
• At each bimonthly visit (beginning with the third injection – month 3)
o Repeat HIV-1 RNA test and assess for signs or symptoms of acute infection
o Administer CAB injection
o Provide access to clean needles/syringes and drug treatment services for PWID
o Respond to new questions and provide any new information about CAB PrEP
o Discuss the benefits of persistent CAB PrEP use and adherence to scheduled injection
visits
• At least every 4 months (every other injection visit, beginning with the third injection-
month 3)
o Conduct bacterial STI screening for MSM and transgender women who have sex with
men – oral, rectal, urethral, blood (see Table 1b)
• At least every 6 months (beginning with the fifth injection – month 7)
o Conduct bacterial STI screening for all heterosexually active women and men–
[vaginal, rectal, urine - as indicated], blood (see Table 1b)
• At least every 12 months (after the first injection)
o Assess desire to continue injections for PrEP
o Conduct chlamydia screening for heterosexually active women and men even if
asymptomatic
DISCONTINUING OR RESTARTING CAB PREP
Patients without HIV on follow-up visit who wish to discontinue CAB injections for PrEP or
those who are a month or more late for an injection should be counseled about:
o How to safely discontinue or restart CAB injections for PrEP
o The risk of developing drug resistant HIV during the period of waning drug levels
(the “tail period”)
o Need for daily oral PrEP or other effective HIV prevention methods if ongoing risk of
HIV exposure is anticipated

Preexposure Prophylaxis for the Prevention of HIV Infection in the United States – 2021 Update Clinical Practice Guideline Page
53 of 108
CAB levels slowly wane over many months after injections are discontinued. In the HPTN 077
trial, the median time to undetectable CAB plasma levels was 44 weeks for men and 67 weeks
for women with a wide range for both sexes
149
. At some point during this “tail” phase, CAB
levels will fall below a protective threshold and persist for some time at nonprotective levels
exposing the patient to the risk of HIV acquisition. These lower levels of CAB may however be
sufficient to apply selective pressure that selects for existing or de-novo viral strains with
mutations that confer resistance to CAB or other INSTI medications. Infection with INSTI-
resistant virus may complicate HIV treatment
150, 151
.
Figure 7 The trade-off of PrEP drug levels and risk of HIV infection with resistant
virus
For these reasons, patients discontinuing CAB injections who may be at ongoing risk of sexual
and injection HIV exposure should be provided with another highly effective HIV prevention
method during the months following their last injection. As with daily oral PrEP, CAB PrEP has
been associated with delayed seroconversion and detection of HIV acquisition. CAB injections
can be restarted at any point after determining HIV status with HIV-1 RNA testing.
When helping patients discontinue CAB PrEP safely, clinicians should:
o Re-educate patients about the “tail” and the risks during declining CAB levels
o Assess ongoing risk/indications
o If PrEP is indicated, prescribe daily oral F/TDF or F/TAF beginning within 8 weeks
after last injection
o Educate about nPEP
o Continue follow-up visits quarterly for 12 months
o Conduct HIV-1 RNA tests at each quarterly follow-up visit after discontinuing CAB
injections

Preexposure Prophylaxis for the Prevention of HIV Infection in the United States – 2021 Update Clinical Practice Guideline Page
54 of 108
TIME TO PROTECTION WITH CAB PREP
No data are yet available from clinical trials in men or women to estimate the time from
initiation of CAB injections to maximal protection against HIV acquisition.
Managing PrEP Patients with Ambiguous HIV test Results
Acquiring HIV while taking daily PrEP as prescribed is very uncommon. While PrEP use has
steadily increased since 2012, with more than 220,000 persons prescribed PrEP in 2018,
152
only
a handful of incident HIV infections in PrEP-adherent patients have been documented in the US.
However, with quarterly HIV testing of persons prescribed PrEP, there is a small but increasing
number of PrEP patients with test results that are indeterminate (ambiguous) or that may be false
positive.
153, 154
Use of antiretroviral PrEP medications at the
time of infection can alter the dynamics of viremia and the
patient’s immune response and lead to ambiguous test
results using standard HIV testing algorithms. For example,
such patients may have positive point-of-care antibody
results but negative antigen results or may have a reactive
qualitative NAT test result but no virus detected by
quantitative NAT testing.
Clinicians who encounter ambiguous test results for a PrEP patient at a follow-up visit have
several options to confirm true HIV status:
• Carefully assess with the patient their medication adherence since the last negative HIV
test visit;
• Draw a new blood specimen after a few days for repeat laboratory HIV testing including
Ag/Ab and quantitative NAT testing; and
• If results are still ambiguous, contact the PrEPline (855-448-7737) for further testing
advice and identification of a laboratory that can do specialized testing.
While HIV status is being confirmed, clinicians have 3 antiretroviral management options for the
patient.
• Continue PrEP medication
o Because of the high effectiveness of PrEP, the pretest probability that adherent
patients are uninfected is high. If infected with HIV, continuing PrEP offers some
level of viral suppression but may select for drug resistance (particularly M184v).
However, if resistance occurs, well-tolerated and high effective treatment
regimens are available to the patient.
• Add a third drug to provide PEP for 28 days
o Adding a third drug to the PrEP regimen while HIV status is being confirmed
provides a fully suppressive treatment regimen while avoiding the need for an
CLINICIANS CAN CALL THE NATIONAL
CLINICIANS CONSULTATION CENTER
PREPLINE AT 855-448-7737 FOR
ADVICE ABOUT INTERPRETATION OF
HIV TEST RESULTS AND
MANAGEMENT OF PATIENTS WHO
ACQUIRE HIV INFECTION WHILE
TAKING PREP MEDICATION.
h
Preexposure Prophylaxis for the Prevention of HIV Infection in the United States – 2021 Update Clinical Practice Guideline Page
55 of 108
HIV diagnosis that may be difficult to undo if the patient is truly uninfected. If the
patient is confirmed to have acquired HIV, the three-drug regimen constitutes
early ART initiation and can be continued. This option is especially applicable
when a patient reports nonadherence to daily PrEP.
• Discontinue PrEP for 1-2 weeks
o Drawing blood for retesting after a patient has discontinued PrEP may facilitate
diagnosis by allowing viral replication resulting in a detectable viral load in a
patient who has acquired HIV. However, in persons who have not acquired HIV,
this leaves them without the protection of PrEP for a period of time.
• For patients receiving CAB injections for PrEP
o While HIV status is being confirmed, clinicians should not administer a new CAB
injection. During the 1-2 weeks needed for additional HIV testing to determine
HIV status, CAB is likely to remain at protective levels.
o If the final determination is that the patient has acquired HIV, treatment should be
immediately started. Follow guidance in section on “Persons with Documented
HIV Infection”
o If determined not to have acquired HIV, CAB injections every 2 months should
resume.
Considerations and Options for Selected Patients
The patient with certain clinical conditions may have indications for specific PrEP regimens or
may require special attention and follow-up by the clinician.
NONDAILY ORAL PREP REGIMENS FOR MSM
The “2-1-1” regimen (also called event-driven, intermittent, or “on-demand”) is a nondaily PrEP
regimen that times oral F/TDF doses in relation to sexual intercourse events. While not an FDA-
approved regimen, two clinical trials, IPERGAY
155
and the subsequent Prévenir open label study
in Paris,
156
have demonstrated the HIV prevention efficacy of 2-1-1 dosing only with F/TDF and
only for MSM. These trials were conducted with European and Canadian adult MSM.
Based on trial experience, MSM prescribed the 2-1-1 regimen should be instructed to take
F/TDF as follows:
• 2 pills in the 2-24 hours before sex (closer to 24 hours preferred)
• 1 pill 24 hours after the initial two-pill dose
• 1 pill 48 hours after the initial two-pill dose
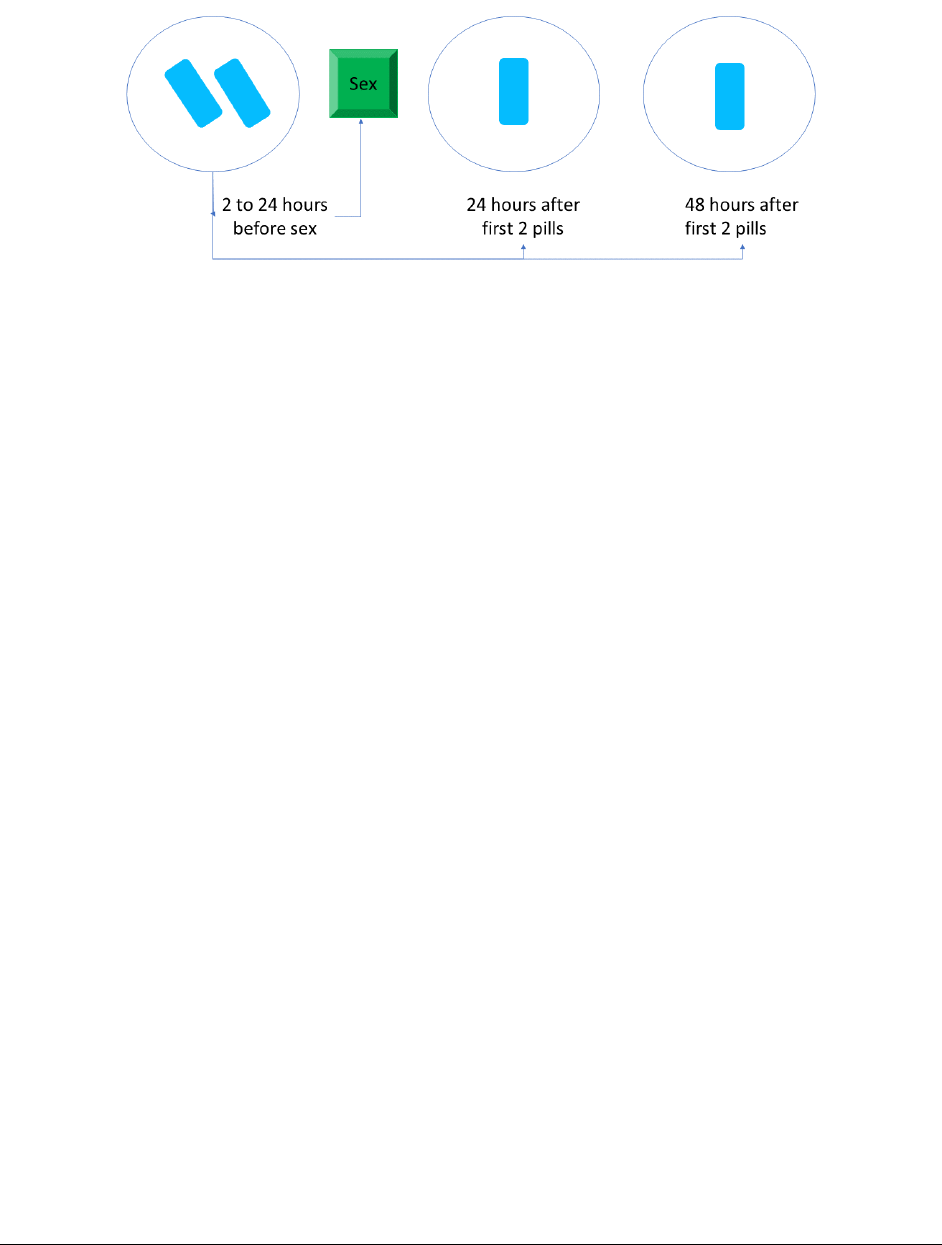
Preexposure Prophylaxis for the Prevention of HIV Infection in the United States – 2021 Update Clinical Practice Guideline Page
56 of 108
Figure 8 Schedule for “2-1-1” Dosing
Based on the timing of subsequent sexual events, MSM should be instructed to take additional
doses as follows:
• If sex occurs on the consecutive day after completing the 2-1-1 doses, take 1 pill per day
until 48 hours after the last sexual event.
• If a gap of <7 days occurs between the last pill and the next sexual event, resume 1 pill
daily.
• If a gap of ≥7 days occurs between the last pill and next sexual event, start again with 2
pills.
The dosing was designed and tested primarily to meet the needs of men who had infrequent sex
and thus for whom daily dosing might not be necessary. Yet in these trials, men took an average
3-4 doses per week which has been associated with high levels of protection in men prescribed
daily F/TDF. The IPERGAY and Prévenir trials showed high preventive efficacy of 86% or
more (see evidence review in Appendix 2). There are fewer data on the efficacy of “2-1-1”
dosing in MSM having less frequent sex.
157
The only U.S. data concerning nondaily dosing among MSM came from the ADAPT HPTN 067
study participants in Harlem, New York. Investigators estimated PrEP effectiveness among those
MSM prescribed a time-driven regimen (two doses per week 3-4 days apart) or an event-driven
regimen (one pill taken before and another after sex) compared to MSM who were prescribed
daily dosing. When assessing PrEP coverage of reported sex acts, predicted effectiveness was
significantly lower for the two nondaily dosing patterns (62% and 68%, respectively) compared
to daily dosing (80%).
158
No clinical trial or observational cohort data are yet available that assess the efficacy of the 2-1-1
regimen in US MSM and no submission of data has been made for FDA review and approval of
this dosing schedule. However, given the efficacy demonstrated in the IPERGAY and Prévenir
trials, the International AIDS Society-USA has recommended “2-1-1” dosing as an optional, off-
label, alternative to daily dosing for MSM,
159
and some local guidelines have also recommended
it for selected MSM.

Preexposure Prophylaxis for the Prevention of HIV Infection in the United States – 2021 Update Clinical Practice Guideline Page
57 of 108
Some clinicians may choose to prescribe F/TDF off-label using “2-1-1” dosing for adult MSM
who request non-daily dosing and who:
• have sex infrequently (e.g., less often than once a week) and
• can anticipate sex (or delay sex) to permit the doses at least 2 hours prior to sex.
Clinicians who elect to provide the 2-1-1 regimen off-label should prescribe no more than 30
pills without follow-up and documentation of another negative HIV test. Patients having sex less
than once weekly will have sufficient medication to cover up to 7 intermittent sexual events.
Clinicians who elect to provide the 2-1-1 regimen should also discuss with patients:
• the importance of taking both pre-sex and post-sex doses of F/TDF to achieve good
protection;
• the importance of using PrEP for all sexual encounters, not for only some partners or
events;
• the possibility of recurrent “start-up” symptoms with infrequent PrEP dosing;
• the possibility of inadvertent disclosure of same-sex behavior to peers or family members
since 2-1-1 dosing is only used by MSM;
• how to change between daily and 2-1-1 dosing;
• the continued need for follow-up visits for HIV and STI testing; and
• the possibility that this off-label use will not be covered by insurance.
2-1-1 dosing should not be prescribed:
• for populations other than adult MSM because it has been studied only in adult MSM;
• for MSM who it is anticipated will have difficulty adhering to a complex dosing regimen
(e.g., adolescents, patient with an active substance use disorder);
• with F/TAF because its use for pericoital dosing has not been studied; or
• for MSM with active hepatitis B infection because of the danger of hepatic flares with
episodic F/TDF exposure.
TRANSGENDER PERSONS
Transgender persons are those whose gender identity or expression differs from their sex at birth.
Among all adults and adolescents, diagnoses of HIV infection among transgender persons
accounted for approximately 2% of diagnoses of HIV infections in the United States and 6
dependent areas; of whom 92% of diagnoses of HIV infections were for transgender women.
19
The effectiveness of PrEP with either F/TDF or F/TAF for transgender women has not yet been
definitively proven in trials
that were underpowered because of the small number of transgender
women included.
3, 4, 32
All studies conducted to date have shown no effect of F/TDF on hormone
levels. Some studies have shown that the high-doses of feminizing hormones prescribed to

Preexposure Prophylaxis for the Prevention of HIV Infection in the United States – 2021 Update Clinical Practice Guideline Page
58 of 108
transgender women result in lowering of activated tenofovir diphosphate levels in rectal
tissue.
160, 161
However, other studies do not show significantly lower levels of tenofovir
diphosphate among TGW taking PrEP with a feminizing hormone regimen.
162
. It is unclear
whether the extent of any possible reduction at the site of exposure affects PrEP effectiveness but
the observed decrease in some studies suggests that daily adherence is especially important for
transgender women taking feminizing hormones. Other studies have shown that medication
adherence and persistence is low in some cohorts of transgender women.
163, 164
Transgender women were not specifically included in the FDA approval for F/TDF for PrEP.
However, FDA approved F/TAF for PrEP was based on an analysis that combined 5,387 MSM
(2,694 given F/TAF) and 74 transgender women (45 given F/TAF). Only 24 transgender women
remained in the study and on PrEP through the period of analysis. There were too few
transgender women remaining in the study for a separate analysis, leaving unresolved questions
about the level of proof of effectiveness for them.
3
No data are available about the prevention
effectiveness of either F/TDF or F/TAF for PrEP in transgender men.
In HPTN 083, there were a sufficient number of transgender women analyzed separately from
MSM. Transgender women in the F/TDF group had similar HIV incidence (1.8 per 100 py) as
MSM (1.14 per 100 py) and similar hazard ratios compared to the cabotegravir MSM groups
(0.34 for TGW, 0.35 for MSM). F/TDF PrEP has been shown to reduce the risk for HIV
acquisition during both anal sex and penile-vaginal sex. F/TAF has been proven effective in
persons exposed to HIV through non-vaginal sex, and efficacy has been shown for cabotegravir
injection, therefore PrEP is recommended for transgender women at risk for HIV acquisition
165
.
When prescribed, clinicians should discuss the need for high medication adherence and reassure
patients that PrEP medications do not impact the effects of feminizing hormones.
PERSONS WHO INJECT DRUGS
Persons who inject drugs not prescribed to them should be offered PrEP. In addition, reducing or
eliminating injection risk practices can be achieved by providing access to drug treatment and
relapse prevention services
59
. Persons who inject opioids can be offered medication-assisted
treatment, either within the PrEP clinical setting (e.g., provision of daily oral buprenorphine or
naltrexone) or by referral to a drug treatment clinic (e.g., methadone program). Local substance
use disorder treatment resources can be found at https://findtreatment.samhsa.gov/locator.
For persons not able (e.g., on a waiting list or lacking insurance) or not motivated to engage in
drug treatment, providing access to sterile injection equipment through syringe service programs
(where legal and available), and through prescriptions of syringes or purchase of syringes from
pharmacies without a prescription (where legal), can reduce exposure to HIV and other
infectious agents (e.g., HCV). In addition, providing or referring PWID for cognitive or
behavioral counseling and any indicated mental health or social services may help reduce risky
injection practices.

Preexposure Prophylaxis for the Prevention of HIV Infection in the United States – 2021 Update Clinical Practice Guideline Page
59 of 108
PATIENTS WITH RENAL DISEASE
Patients with eCrCl ≥ 60 ml/min may be prescribed daily F/TDF for PrEP; those with an eCrCl
between 30 and 60 ml/min may be prescribed daily F/TAF (but not F/TDF) for PrEP.
119
Persons
with an eCrCl of <30 ml/min, should not be prescribed F/TDF or F/TAF for PrEP, because the
safety of tenofovir-containing regimens for such persons was not evaluated in the clinical trials.
Dose reduction of either F/TDF or F/TAF is not recommended for PrEP prescribed to patients
with significant renal disease.
CAB for PrEP can be especially considered for patients with significant renal disease (e.g.,
eCrCl <30 ml/min) in whom tenofovir-containing regimens are not recommended.
HIV DISCORDANT PARTNERSHIPS
When assessing indications for PrEP use in an HIV discordant couple, clinicians should ask
about the treatment and viral load status of the partner with HIV (if the negative partner knows
it). Persons with HIV who achieve and maintain a plasma HIV RNA viral load <200 copies/ml
with antiretroviral therapy have effectively no risk of sexually transmitting HIV.
166
This is
sometimes referred to as “undetectable equals untransmittable” (“U=U”) or “treatment as
prevention” (TASP).
167
However, some partners who know they have HIV may not be in care, may not be receiving
antiretroviral therapy, may not be receiving highly effective regimens, may not be adherent to
their medications, or for other reasons may not consistently have viral loads that are associated
with the least risk of transmission to an uninfected sex partner. In addition, studies have shown
that patient-reported viral load status may not be accurate,
168, 169
but clinicians providing care to
the HIV-negative patient may not have access to the medical records of the HIV-positive partner
to document their recent viral load status and the consistency of their viral suppression over time.
In the HIV discordant couples studies, reported sex with outside partners was not uncommon and
HIV infections occurred that were genetically unlinked to the partner in the couple with HIV.
170-
172
PrEP may be indicated if the partner with HIV has been inconsistently virally suppressed or their
viral load status is unknown, if the partner without HIV has other sexual partners (especially if of
unknown HIV status), or if the partner without HIV wants the additional reassurance of
protection that PrEP can provide. PrEP should not be withheld from HIV-uninfected patients
who request it even if their sexual partner with HIV is reported to have achieved and maintained
a suppressed viral load. Several studies, using viral genotyping, have documented HIV infection
in a previously uninfected patient that was acquired from a partner outside the relationship with
the partner known to have HIV
173
.

Preexposure Prophylaxis for the Prevention of HIV Infection in the United States – 2021 Update Clinical Practice Guideline Page
60 of 108
For patients in an HIV discordant partnership for whom PrEP is being considered, especially
where the partner with HIV is not virally suppressed, either CAB injections or daily oral PrEP
are recommended options.
PERSONS WITH DOCUMENTED HIV INFECTION
All persons with an HIV-positive test result whether at screening or while taking F/TDF or
F/TAF or receiving CAB injections as PrEP should be provided the following services:
37
▪ Laboratory confirmation of HIV status (see Figure 4).
▪ Determination of CD4 lymphocyte count and plasma HIV RNA viral load to guide
therapeutic decisions.
▪ Documentation of results of genotypic HIV viral resistance testing to guide future
treatment decisions.
▪ If on PrEP, conversion of the PrEP regimen to an HIV treatment
regimen recommended by the DHHS Panel on Antiretroviral
Guidelines for Adults and Adolescents
37
without waiting for
additional laboratory test results. See Clinical Providers’
Supplement Section 8.
▪ Provision of, or referral to, an experienced provider for the
ongoing medical management of HIV infection.
▪ Counseling about their HIV status and steps they should take to
prevent HIV transmission to others and to improve their own
health.
▪ Assistance with, or referral to, the local health department for the identification of sex
partners who may have been recently exposed to HIV so that they can be tested for HIV
infection, considered for nonoccupational postexposure prophylaxis (nPEP),
113
and
counseled about their risk-reduction practices.
In addition, a confidential report of new HIV infection should be provided to the local health
department.
WOMEN WHO BECOME PREGNANT OR BREASTFEED WHILE TAKING PREP
The guidance in this section focuses on the use of PrEP during periconception, pregnancy, and
breastfeeding. All research on PrEP cited here was conducted with cisgender women. There are
no data yet about transgender men, genderqueer, or non-binary individuals who have become
pregnant and given birth while taking PrEP medication. Therefore, this section uses the
terminology, ‘women’.
An increased risk of HIV acquisition has been documented for women during periods of
conception, pregnancy, and breastfeeding.
174, 175
Providers should offer PrEP with F/TDF to
CLINICIANS CAN CALL THE NATIONAL
CLINICIANS CONSULTATION CENTER
PREPLINE AT 855-448-7737 FOR
ADVICE ABOUT INTERPRETATION OF
HIV TEST RESULTS AND
MANAGEMENT OF PATIENTS WHO
ACQUIRE HIV INFECTION WHILE
TAKING PREP MEDICATION.
h

Preexposure Prophylaxis for the Prevention of HIV Infection in the United States – 2021 Update Clinical Practice Guideline Page
61 of 108
women seeking to conceive (i.e., sex without a condom) and pregnant or breastfeeding women
whose sexual partner has HIV, especially when their current partner’s viral load is unknown, is
detectable, or cannot be documented as undetectable.
176
Women whose sexual partner with HIV
achieves and maintains an HIV-1 viral load <200 copies/ml are at effectively no risk of sexual
acquisition of HIV.
177
The extent to which PrEP use further decreases risk of HIV acquisition
when the male partner has a documented recent undetectable viral load is unknown but there
may be benefit when viral suppression is not durable or the woman has other partners. F/TAF is
not approved for PrEP for women.
Clinicians providing pre-conception and pregnancy care to women often do not provide care to
their male partners. When partner’s HIV status is unknown or not recently assessed, clinicians
should offer HIV testing for the partner. When a woman’s sexual partner is reported to be HIV-
positive, but his recent viral load status is not known, documentation of the recent viral load
status can be requested.
The FDA labeling information
6
is permissive of use of F/TDF for PrEP in pregnant and
breastfeeding women. The perinatal antiretroviral treatment guidelines
178
recommend PrEP with
F/TDF. Data directly related to the safety of PrEP use for a developing fetus were initially
limited.
179
In the F/TDF PrEP trials with heterosexual women, medication was promptly
discontinued for women who became pregnant, so the safety for exposed fetuses could not be
adequately assessed. However a recent analysis of 206 Kenyan women with prenatal PrEP use
and 1,324 without found no difference in pregnancy outcomes (preterm birth of low birthweight)
and similar infant growth at 6 weeks postpartum.
180
In the parent Kenyan study, of 193 pregnant
or postpartum women with partners living with HIV, 153 initiated PrEP and none acquired
HIV.
181
Additionally, TDF and FTC (also TAF) are widely used for the treatment of HIV infection and
are continued during pregnancies that occur.
182-184.
Data on pregnancy outcomes in the
Antiretroviral Pregnancy Registry provide no evidence of adverse effects among fetuses exposed
to these medications when used for either HIV treatment or prevention of HIV acquisition during
pregnancy.
185
Providers should discuss the potential risks and benefits of all available alternatives for safer
conception
186
and if indicated make referrals for assisted reproduction therapies. Providers
should include discussion of the potential risks and benefits of beginning or continuing PrEP
during pregnancy and breastfeeding so that an informed decision can be made. Whether or not
PrEP is elected, the partner with HIV should be taking maximally effective antiretroviral therapy
before conception attempts.
5
Health care providers are strongly encouraged to prospectively and anonymously submit
information about any pregnancies in which PrEP is used to the Antiretroviral Pregnancy
Registry at: http://www.apregistry.com/.

Preexposure Prophylaxis for the Prevention of HIV Infection in the United States – 2021 Update Clinical Practice Guideline Page
62 of 108
The safety of PrEP with F/TDF or F/TAF for infants exposed during lactation has not been
adequately studied. However, data from studies of infants born to HIV-infected mothers and
exposed to TDF or FTC through breast milk suggest limited drug exposure.
187-189
The World
Health Organization recommends the use of F/TDF (or 3TC/efavirenz) for all pregnant and
breastfeeding women with HIV to prevent perinatal and postpartum mother-to-child HIV
transmission.
190
Therefore, providers should discuss current evidence about the potential risks
and benefits of beginning or continuing PrEP during breastfeeding so that an informed decision
can be made.
§
Conditioned on FDA approval, CAB for PrEP may be initiated or continued in women who may
become pregnant while receiving injections when it is determined that the anticipated benefits
outweigh the risks.
Health care providers should prospectively and anonymously submit information about any
pregnancies in which F/TDF or cabotegravir for PrEP is used to the Antiretroviral Pregnancy
Registry at: http://www.apregistry.com/.
The published data on cabotegravir-exposed pregnancies among women without HIV are sparse,
with only 4 pregnancies documented in HPTN 077
148
. Data from additional pregnancies that
occurred among participants in HPTN 084 will be available in the near term.
The known increased risk of HIV acquisition during pregnancy and subsequent risk of HIV
transmission to the infant during pregnancy and breastfeeding exceed any theoretical risk to
maternal or infant health yet identified or observed in cabotegravir PrEP trials or in pregnancies
occurring during treatment trials with cabotegravir-containing regimens.
ADOLESCENT MINORS
PrEP is recommended for adolescents (weighing at least 35 kg or 77 lb) who report sexual or
injection behaviors that indicate a risk of HIV acquisition. As a part of primary health care, HIV
screening should be discussed with all adolescents who are sexually active or have a history of
injection drug use. USPSTF recommends (grade “A”) that all adolescents (age ≥15 years) be
screened for HIV.
61
Parental/guardian involvement in an adolescent’s health care is often
desirable but is sometimes contraindicated for the safety of the adolescent. Laws and regulations
that may be relevant for PrEP-related services provided to adolescent minors (including HIV
§
The DHHS Perinatal HIV Guidelines state that “Health care providers should offer and promote oral combination
tenofovir disoproxil fumarate/emtricitabine (TDF/FTC) pre-exposure prophylaxis (PrEP) to individuals who are at
risk for HIV and are trying to conceive or arepregnant, postpartum, or breastfeeding:”
9
The FDA-approved package
insert for F/TDF
6
says “In HIV-uninfected women, the developmental and health benefits of breastfeeding and the
mother’s clinical need for TRUVADA for HIV-1 PrEP should be considered along with any potential adverse
effects on the breastfed child from TRUVADA and the risk of HIV-1 acquisition due to nonadherence and
subsequent mother to child transmission.”

Preexposure Prophylaxis for the Prevention of HIV Infection in the United States – 2021 Update Clinical Practice Guideline Page
63 of 108
testing), such as those concerning consent, confidentiality,
191
parental disclosure, and
circumstances requiring reporting to local agencies, differ by jurisdiction. Clinicians considering
providing PrEP to a person under the age of legal adulthood (a minor) should be aware of local
laws, regulations, and policies that may apply
192
(see
(https://www.cdc.gov/hiv/policies/law/states/minors.html). Clinicians should explicitly discuss
any limits of confidentiality based on these local laws, regulations and policies and what
methods will be used to assure confidentiality is maintained to the extent permitted.
Nearly all trials and observational studies have shown lower adherence and persistence rates in
adolescents and young adults prescribed daily F/TDF for PrEP, particularly African American
young MSM.
193
This is not unexpected as adolescents have low adherence to many medications
they are prescribed.
194, 195
Therefore, to help adolescents achieve adequate protection from
acquiring HIV, it will be critical to provide supportive counseling and interventions (e.g., phone
apps) when they have been proven effective.
In the ATN 110 (ages 18-22 years) and 113 studies (ages 15-17 years), bone density changes in
young MSM were measured during PrEP use and after completing the PrEP trial period (48
weeks). They reported decreased bone mineral density during the period of F/TDF PrEP use with
larger declines in those ages 15-19 years than in those ages 20-22 years. While men ages 18-22
years had full improvement during the 48 weeks after PrEP use stopped, declines were persistent
in younger men.
196
The bone changes were more frequently seen in young men with greatest
adherence (i.e., higher drug exposure).
197
Likelihood of adherence problems and effects on long-term bone health should be weighed
against the potential benefit of providing PrEP for an individual adolescent at substantial risk of
HIV acquisition. Because differences in pharmacodynamics suggest less bone effect with F/TAF
than with F/TDF, clinicians may want to preferentially prescribe F/TAF to adolescent males
initiating PrEP.
CAB for PrEP has not been studied in men or women < 18 years of age. These studies are
underway but until safety is determined for this population, and reviewed by FDA, CAB is not
recommended for adolescents <18 years old.
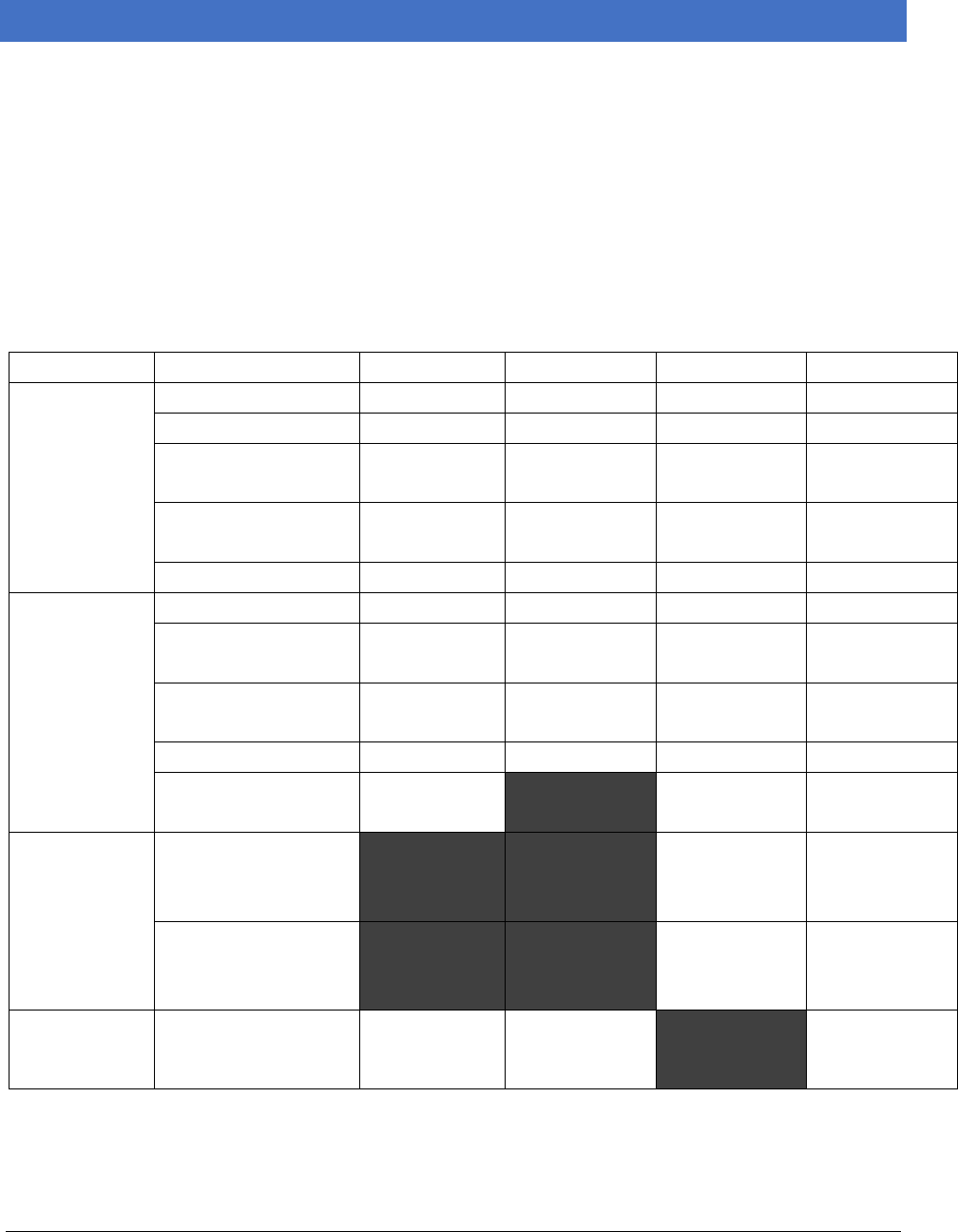
Preexposure Prophylaxis for the Prevention of HIV Infection in the United States – 2021 Update Clinical Practice Guideline Page
64 of 108
Primary Care Considerations
Provision of PrEP affords the opportunity to manage other preventive health measures during
both initial and follow-up visits, especially for persons who may not otherwise be engaged in
primary care. These health measures include: vaccinations, screening for sex-specific
conditions, and screening for mental health, tobacco/nicotine use, and alcohol use disorder.
When providing sex-specific health care for transgender persons, the principle of “screen what
you have” should be applied. For example, all persons with a cervix should be screened for
cervical cancer and all persons with a prostate should be considered for prostate cancer
screening, regardless of gender identification.
Table 8 Primary Care Health Measures
MSM
MSW*
Women*
PWID
Vaccines#
(if not
previously
vaccinated)
Hepatitis A vaccine
Yes
Yes
Yes
Yes
Hepatitis B vaccine
Yes
Yes
Yes
Yes
HPV vaccine
Through age
26
Through age
26
Through age
26
Through age
26
Meningococcal B
vaccine
Ages 16-18
Ages 16-18
Ages 16-18
Ages 16-18
Influenza vaccine
Yes
Yes
Yes
Yes
General
Health
Hepatitis C infection^
Ages 18-79
Ages 18-79
Ages 18-79
Ages 18-79
Screen for
depression^
Yes
Yes
Yes
Yes
Screen for unhealthy
alcohol use^
Ages 18 and
older
Ages 18 and
older
Ages 18 and
older
Ages 18 and
older
Screen for smoking^
Yes
Yes
Yes
Yes
Screen for Intimate
Partner Violence^
Yes
Yes
If female, Yes
Women’s
Health
Mammography^
Ages 50-74
every two
years
If female, Ages
50-74 every
two years
Screen for cervical
cancer^~
Ages 21-65
every three
years
If female, Ages
21-65 every
three years
Men’s Health
Screen for prostate
cancer^
Ages 55-69
Ages 55-69
If male, Ages
55-69
*”screen what you have” principle for transgender persons
# per ACIP recommendations
^per USPSTF recommendations
~per ASCCP (American Society of Colposcopy and Cervical Pathology} guidelines
198

Preexposure Prophylaxis for the Prevention of HIV Infection in the United States – 2021 Update Clinical Practice Guideline Page
65 of 108
Financial Case-Management Issues for PrEP
A means to pay for PrEP medications and recommended clinical and counseling services is
required for successful PrEP use. Nearly all public and private insurers cover PrEP, but co-pay,
co-insurance, and prior authorization policies differ.
Clinicians should provide benefits counseling to assist eligible patients to obtain insurance (e.g.,
Medicaid, Medicare, ACA plans) either by in-clinic benefits counseling or by referral to
community resources.
The USPSTF recommends that PrEP be provided to “persons who are at high risk of HIV
acquisition” with an A grade indicating that there is high certainty that the net benefit is
substantial.
11
This rating requires most commercial
insurers and some Medicaid programs to provide oral
PrEP with no out-of-pocket cost to patients. In
addition to PrEP medication, DHHS has determined
that laboratory tests necessary for PrEP are included in
this provision as well as clinic visits when the primary
purpose of the office visit is the delivery of PrEP
care
199
.
For patients residing in the US without health insurance or whose insurance does not cover PrEP
medication, there are two programs that can provide free F/TDF or F/TAF for PrEP.
For patients who lack outpatient prescription drug coverage, the HHS “Ready, Set, PrEP”
program makes prescribed PrEP medication (either F/TDF or F/TAF) available at no cost. With a
clinician’s prescription, patients can enroll on the website at https://www.getyourprep.com/ or by
calling toll-free 855-447-8410.
For patients without health insurance or whose insurance does not cover PrEP medication, and
whose household income is <500% of the federal poverty level, Gilead Sciences has established
a PrEP medication assistance program (includes both F/TDF and F/TAF). In addition to
providing medication at no cost for eligible patients, this program also provides access to free
HIV testing. For commercially insured patients whose personal resources are insufficient to pay
out-of-pocket costs for medication co-pay or co-insurance, the Gilead co-pay assistance program
provides assistance and other co-pay programs are also available.
165
Providers may obtain,
complete, and sign applications for their patients to receive free PrEP medication or co-pay
assistance at www.gileadadvancingaccess.com or by calling toll-free 855-330-5479.
In addition, some states have PrEP-specific financial assistance programs that cover medication,
clinical care, or both. (see Table 9). These change over time and a current list can be found at
https://www.nastad.org/prepcost-resources/prep-assistance-programs.
A guide to billing codes for PrEP
coverage is available at
https://www.nastad.org/resource/bi
lling-coding-guide-hiv-prevention
(see Clinical Providers’
Supplement Section 10)
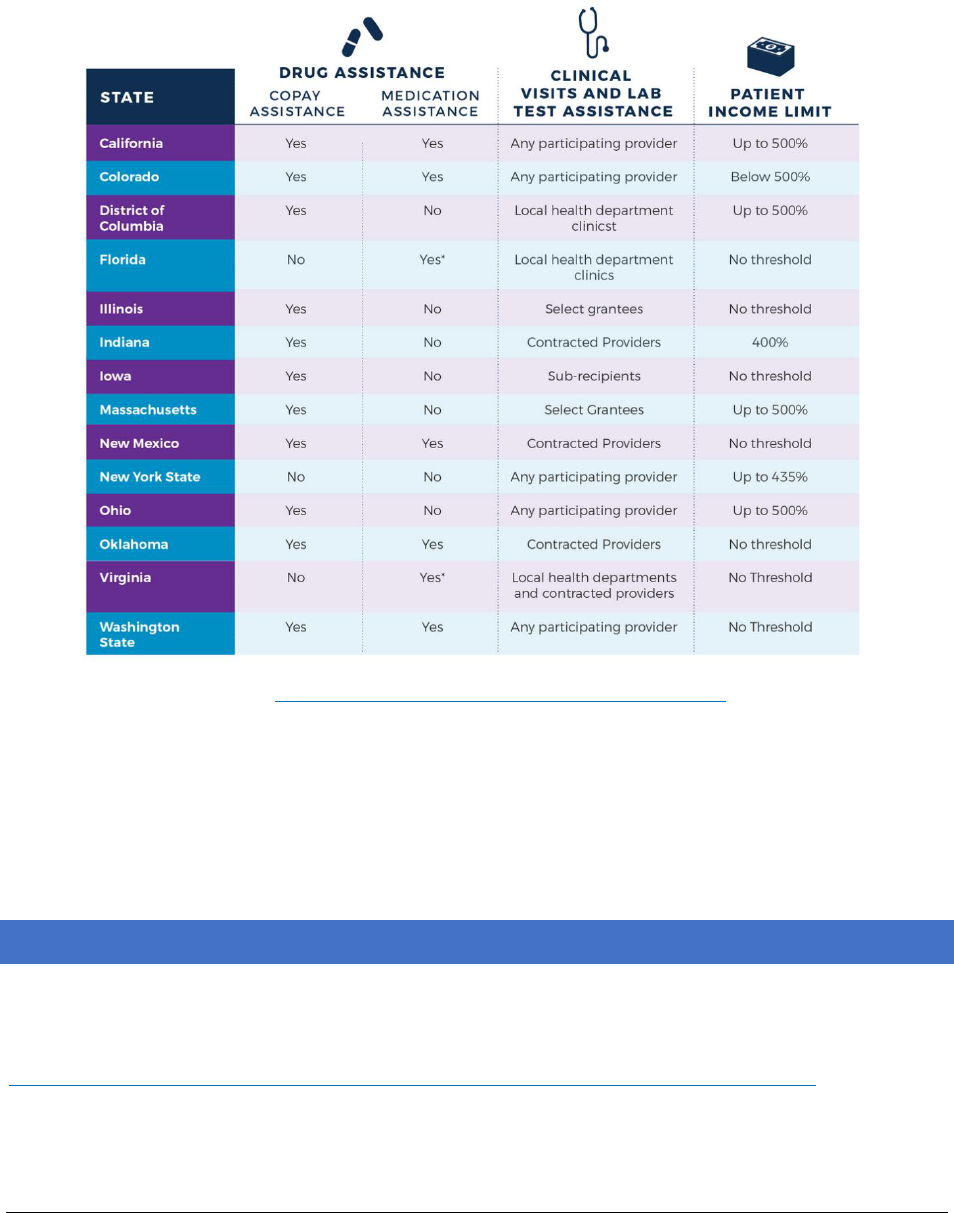
Preexposure Prophylaxis for the Prevention of HIV Infection in the United States – 2021 Update Clinical Practice Guideline Page
66 of 108
Table 9 NASTAD Table of State PrEP Financial Assistance Programs (as of August
2022)
** Table provided by NASTAD (source: https://www.nastad.org/prepcost-resources/prep-assistance-programs )
At the time of this guideline update, FDA approval of CAB has not yet occurred. So no
medication assistance programs are yet available. It is anticipated that when FDA approves a
CAB indication for PrEP, one or more assistance programs will become available for uninsured
and underinsured patients with low income. A USPSTF determination about CAB for PrEP has
not yet been made.
Decision Support, Training and Technical Assistance
Decision support systems (electronic and paper), flow sheets, checklists (see Clinical Providers’
Supplement, Section 1 for a PrEP provider/patient checklist at
https://www.cdc.gov/hiv/pdf/risk/prep/cdc-hiv-prep-provider-supplement-2021.pdf), feedback
reminders, and involvement of nurse clinicians and pharmacists can help manage the many steps
indicated for the safe use of PrEP and increase the likelihood that patients will follow them.
Often these systems are locally developed but may become available from various sources

Preexposure Prophylaxis for the Prevention of HIV Infection in the United States – 2021 Update Clinical Practice Guideline Page
67 of 108
including training centers and Websites funded by government agencies, professional
associations, or interested private companies. Examples include downloadable applications
(widgets) to support the delivery of nPEP or locate nearby sites for confidential HIV tests
(http://www.hivtest.org); and confidential commercial services to electronically monitor
medication-taking, send text message reminders, or provide telephone assistance to help patients
with problems concerning medication adherence.
Training and technical assistance in providing components of PrEP-related services, medications,
and counseling are available at the following Web sites:
▪ PrEPline: National Clinician’s Consultation Center (http://nccc.ucsf.edu/clinical-
resources/prep-guidelines-and-resources/)
▪ Integrating HIV Care, Treatment & Prevention Services into Primary Care – A Toolkit
for Health Centers (https://bphc.hrsa.gov/media/p4c-toolkit-2018.pdf)
▪ National PrEP Clinician Locator (https://preplocator.org/)
▪ Decision-Making Guide for the Provision of PrEP Services in Title X-Funded Family
Planning Service Sites (https://opa.hhs.gov/sites/default/files/2020-07/OPA-PrEP-
Decision-Guide_0.pdf)
▪ HIV Nexus Clinician Resources (https://www.cdc.gov/hiv/clinicians/index.html)
▪ The AIDS Education Training Centers National Resource Center (http://www.aids-
ed.org)
▪ The Addiction Technology Transfer Center Network (http://www.attcnetwork.org)
▪ AIDS Info (http://www.aidsinfo.nih.gov, http://www.aids.gov)
▪ The National Network of STD Clinical Prevention Training Centers (http://nnptc.org/)
Related DHHS Guidelines
This document is consistent with several other guidelines from several organizations related to
sexual health, HIV prevention, and the use of antiretroviral medications. Clinicians should refer
to these other documents for detailed guidance in their respective areas of care.
▪ Prevention of Human Immunodeficiency Virus (HIV) Infection: Preexposure Prophylaxis
Final Recommendation USPSTF, 2019
11
▪ Screening For HIV Infection: Current Recommendations USPSTF, 2019
61
▪ Revised Recommendations for HIV Testing of Adults, Adolescents, and Pregnant
Women in Health-Care Settings
200
▪ Recommendations for HIV Screening of Gay, Bisexual, and Other Men Who Have Sex
with Men — United States, 2017
60
▪ Guidelines for the Use of Antiretroviral Agents in HIV-1-Infected Adults and
Adolescents
201
▪ Recommendations for Use of Antiretroviral Drugs in Pregnant Women with HIV
Infection and Interventions to Reduce Perinatal HIV Transmission in the United States
158

Preexposure Prophylaxis for the Prevention of HIV Infection in the United States – 2021 Update Clinical Practice Guideline Page
68 of 108
▪ Updated Guidelines for Antiretroviral Postexposure Prophylaxis After Sexual, Injection
Drug Use, or Other Non-occupational Exposure to HIV -United States, 2017
202
▪ Sexually Transmitted Diseases Treatment Guidelines, 2021
79
▪ Recommendations for Partner Services Programs for HIV Infection, Syphilis, Gonorrhea,
and Chlamydial Infection
102
▪ Expedited Partner Therapy in the Management of Sexually Transmitted Diseases, 2006
101
▪ Guidance on the Use of Expedited Partner Therapy in the Treatment of Gonorrhea,
2016
100
▪ Behavioral counseling interventions to prevent sexually transmitted infections: U.S.
Preventive Services Task Force recommendation statement
203
▪ CDC Recommendations for Hepatitis C Screening Among Adults — United States,
2020
204
▪ Hepatitis C guidance: AASLD-I DSA recommendations for testing, managing, and
treating adults infected with hepatitis C virus
205
▪ Integrated prevention services for HIV infection, viral hepatitis, sexually transmitted
diseases, and tuberculosis for persons who use drugs illicitly: summary guidance from
CDC and the U.S. Department of Health and Human Services
185

Preexposure Prophylaxis for the Prevention of HIV Infection in the United States – 2021 Update Clinical Practice Guideline Page
69 of 108
Appendices

Preexposure Prophylaxis for the Prevention of HIV Infection in the United States – 2021 Update Clinical Practice Guideline Page
70 of 108
APPENDIX 1 GRADING OF STRENGTH OF RECOMMENDATIONS AND QUALITY OF
EVIDENCE
Key recommendations in this guideline are based on the review of published scientific evidence
and expert opinions. For details on the guidelines development process used, see the Clinical
Providers’ Supplement, Section 11 at https://www.cdc.gov/hiv/pdf/risk/prep-cdc-hiv-prep-
provider-supplement-2021.pdf.
Using the same grading system as the DHHS antiretroviral treatment guidelines,
201
these key
recommendations are rated with a letter to indicate the strength of the recommendation and with
a numeral to indicate the quality of the combined evidence supporting each recommendation.
Table 10: Rating Scheme for Recommendations
Strength of Recommendation
Quality of Evidence Supporting a
Recommendation
A. Strong recommendation for the
statement
I. One or more well-executed
randomized, controlled trials with
clinical outcomes, validated
laboratory endpoints, or both
B. Moderate recommendation for the
statement
II. One or more well-executed,
nonrandomized trials or
observational cohort studies with
clinical outcomes
C. Optional recommendation for the
statement
III. Expert opinion
Preexposure Prophylaxis for the Prevention of HIV Infection in the United States – 2021 Update Clinical Practice Guideline Page
71 of 108
The quality of scientific evidence ratings in Table 11 are based on the GRADE rating system
206
.
Table 11: Criteria for rating quality of scientific evidence
Type of
evidence
Randomized trial = high
Observational study = low
Any other evidence = very low
Decrease
grade if
**
▪ Serious or very serious limitation to study quality
▪ Important inconsistency
▪ Some or major uncertainty about directness
▪ Imprecise or sparse data
▪ High probability of reporting bias
Increase
grade if
▪ Strong evidence of association – significant relative risk >2 based on
consistent evidence from 2 or more observational studies, with no
plausible confounders (+1)
▪ Very strong evidence of association – significant relative risk of >5
based on direct evidence with no major threats to validity (+2)
▪ Evidence of a dose-response gradient (+1)
▪ All plausible confounders would have reduced the effect (+1)
Range
High-quality evidence
Moderate-quality evidence
Low-quality evidence
Very-low quality evidence
**
Each quality criterion can reduce or increase the quality by 1 or, if very significant, by 2 levels.

APPENDIX 2 EVIDENCE OF THE SAFETY AND EFFICACY OF ORAL ANTIRETROVIRAL
PROPHYLAXIS
Clinical trials were conducted to evaluate the safety and efficacy of oral PrEP in populations at risk of
HIV acquisition through several routes of exposure. The results of completed trials and open label or
observational studies published as of January 2020 are summarized below. See also Tables 12-17 that
follow. The quality of evidence in each study was assessed using GRADE criteria
(https://bestpractice.bmj.com/info/us/toolkit/learn-ebm/what-is-grade/) and the strength of evidence for
all studies relevant to a specific recommendation was assessed by the method used in the DHHS
antiretroviral treatment guidelines (See Appendix 1).
PUBLISHED TRIALS OF ANTIRETROVIRAL PREEXPOSURE PROPHYLAXIS AMONG MEN WHO
HAVE SEX WITH MEN
iPrEx (Preexposure Prophylaxis Initiative) Trial
The iPrEx study
2
was a phase 3, randomized, double-blind, placebo-controlled trial conducted in Peru,
Ecuador, Brazil, Thailand, South Africa, and the United States among men and male-to-female
transgender adults who reported sex with a man during the 6 months preceding enrollment. Participants
were randomly assigned to receive a daily oral dose of either the fixed-dose combination of TDF and
FTC or a placebo. All participants (drug and placebo groups) were seen every 4 weeks for an interview,
HIV testing, counseling about risk- reduction and adherence to PrEP medication doses, verifying
returned pill count, and dispensing of pills and condoms.
Analysis of data through May 1, 2010, revealed that after the exclusion of 58 participants (10 later
determined to be HIV- infected at enrollment and 48 who did not have an HIV test after enrollment), 36
of 1,224 participants in the F/TDF group and 64 of 1,217 in the placebo group had acquired HIV.
Enrollment in the F/TDF group was associated with a 44% reduction in the risk of HIV acquisition (95%
CI, 15-63). The reduction was greater in the as-treated analysis: at the visits at which adherence was
≥50% (by self-report and pill count/dispensing), the reduction in HIV acquisition was 50% (95% CI, 18-
70). The reduction in the risk of HIV acquisition was 73% at visits at which self-reported adherence was
≥90% (95% CI, 41-88) during the preceding 30 days. Among participants randomly assigned to the
F/TDF group, plasma and intracellular drug-level testing was performed for all persons who acquired
HIV during the trial and for a matched subset who remained HIV- uninfected: a 92% reduction in the
risk of HIV acquisition (95% CI, 40-99) was found in participants with detectable levels of F/TDF
versus those with no drug detected.
Generally, F/TDF was well tolerated, although nausea in the first month was more common among
participants taking medication than among those taking placebo (9% versus 5%). No differences in
severe (grade 3) or life-threatening (grade 4) adverse laboratory events were observed between the
active and placebo group, and no drug-resistant virus was found in the 100 participants infected after
enrollment. Among 10 participants who were HIV-negative at enrollment but later found to have been
infected before enrollment, FTC-resistant virus was detected in 2 of 2 men in the active group and 1 of 8
men in the placebo group. Compared to participant reports at baseline, over the course of the study,
participants in both the F/TDF and placebo groups reported fewer total numbers of sex partners with

Preexposure Prophylaxis for the Prevention of HIV Infection in the United States – 2021 Update Clinical Practice Guideline
Page 73 of 108
whom the participants had receptive anal intercourse and higher percentages of partners who used
condoms.
In the original iPrEx publication,
2, 125
of 2,499 MSM, 29 identified as female (i.e., transgender women).
In a subsequent subgroup analysis,
19
men were categorized as transgender women (n=339) if they were
born male and either identified as women (n=29), identified as transgender (n=296), or identified as
male and used feminizing hormones (n=14). Using this expanded definition, among transgender women,
no efficacy of F/TDF for PrEP was demonstrated.
207
There were 11 infections among the PrEP group
and 10 in the placebo group (HR 1.1, 95% CI: 0.5-2.7). By drug level testing (always versus less than
always), compared with MSM, transgender women had less consistent PrEP use OR 0.39 (95% CI:
0.16-0.96). In the subsequent open-label extension study (see below), one transgender woman
seroconverted while receiving PrEP and one seroconversion occurred in a woman who elected not to use
PrEP.
US MSM Safety Trial
The US MSM Safety Trial
1
was a phase 2 randomized, double-blind, placebo-controlled study of the
clinical safety and behavioral effects of TDF for HIV prevention among 400 MSM in San Francisco,
Boston, and Atlanta. Participants were randomly assigned 1:1:1:1 to receive daily oral TDF or placebo
immediately or after a 9- month delay. Participants were seen for follow-up visits 1 month after
enrollment and quarterly thereafter. Among MSM without directed drug interruptions, medication
adherence was high: 92% by pill count and 77% by pill bottle openings recorded by Medication Event
Monitoring System (MEMS) caps. Temporary drug interruptions and the overall frequency of adverse
events did not differ significantly between TDF and placebo groups. In multivariable analyses, back pain
was the only adverse event associated with receipt of TDF. In a subset of men at the San Francisco site
(n=184) for whom bone mineral density (BMD) was assessed, receipt of TDF was associated with small
decrease in BMD (1% decrease at the femoral neck, 0.8% decrease for total hip). TDF was not
associated with reported bone fractures at any anatomical site. Among 7 seroconversions, no HIV with
mutations associated with TDF resistance was detected. No HIV infections occurred while participants
were being given TDF; 3 occurred in men while taking placebo; 3 occurred among men in the delayed
TDF group who had not started receiving drug; 1 occurred in a man who had been randomly assigned to
receive placebo and who was later determined to have had acute HIV infection at the enrollment visit.
Adolescent Trials Network (ATN) 082
ATN 082
208
was a randomized, blinded, pilot feasibility study comparing daily PrEP with F/TDF with
and without a behavioral intervention (Many Men, Many Voices) to a third group with no pill and no
behavioral intervention. Participants had study visits every 4 weeks with audio-computer assisted
interviews (ACASI), blood draws, and risk-reduction counseling. The outcomes of interest were
acceptability of study procedures, adherence to pill-taking, safety of F/TDF, and levels of sexual risk
behaviors among a population of young (ages 18-22 years) MSM in Chicago. One hundred participants

Preexposure Prophylaxis for the Prevention of HIV Infection in the United States – 2021 Update Clinical Practice Guideline
Page 74 of 108
were to be followed for 24 weeks, but enrollment was stopped, and the study was unblinded early when
the iPrEx study published its efficacy result. Sixty-eight participants were enrolled. By drug level
detection, adherence was modest at week 4 (62%), and declined to 20% by week 24. No HIV
seroconversions were observed.
IPERGAY (Intervention Préventive de l’Exposition aux Risques avec et pour les Gays)
The results of a randomized, blinded, trial of non-daily dosing of F/TDF or placebo for HIV preexposure
prophylaxis has also been published
155
and is included here for completeness, although non-daily dosing
is not currently recommended by the FDA or CDC.
Four-hundred MSM in France and Canada were randomized to a complex peri-coital dosing regimen
that involved taking: 1) 2 pills (F/TDF or placebo) between 2 and 24 hours before sex, 2) 1 pill 24 hours
after the first dose, 3) 1 pill 48 hours after the first dose, 4) continuing daily pills if sexual activity
continues until 48 hours after the last sex. If more than a 1week break occurred since the last pill,
retreatment initiation was with 2 pills before sex or if less than a 1 week break occurred since the last
pill, retreatment initiation was with 1 pill before sex. Each pre-sex dose was then followed by the 2 post-
sex doses. Study visits were scheduled at 4 and 8 weeks after enrollment, and then every 8 weeks. At
study visits, participants completed a computer-assisted interview, had blood drawn, received adherence
and risk reduction counseling, received diagnosis and treatment of STIs as indicated, and had a pill
count and a medication refill. Following an interim analysis by the data and safety monitoring board at
which efficacy was determined, the placebo group was discontinued and all study participants were
offered F/TDF. In the blinded phase of the trial, efficacy was 86% (95% CI: 40-98). By self-report,
patients took a median of 15 pills per month. By measured plasma drug levels in a subset of those
randomized to F/TDF, 86% had TDF levels consistent with having taken the drug during the previous
week.
Because of the high frequency of sex and therefore of pill-taking among MSM in this study, it is not yet
known whether the regimen will work if taken only a few hours or days before sex, without any buildup
of the drug in rectal tissue from prior use. Studies suggest that it may take days, depending on the site of
sexual exposure, for the active drug in PrEP to build up to an optimal level for preventing HIV infection.
No data yet exist on how effective this regimen would be for heterosexual persons or those who inject
drugs, or on adherence to this relatively complex PrEP regimen outside a trial setting. IPERGAY
findings, combined with other recent research, suggest that even with less than perfect daily adherence,
PrEP may still offer substantial protection for MSM if taken consistently.
DISCOVER Trial
The DISCOVER Trial
3, 4
was a phase 3, randomized, double-blind, active-controlled, non-inferiority
trial conducted in 11 European and North American countries among men and male-to-female
transgender persons ≥ 18 years of age who reported: 1) two or more condomless anal sex episodes with
a man during the 12 weeks preceding enrollment or 2) a diagnosis of syphilis, rectal gonorrhea or rectal
chlamydia in the 24 weeks prior to enrollment. Participants were randomly assigned to receive a daily
oral dose of either F/TDF or F/TAF. All participants were seen at 4 weeks, 12 weeks, and every 12
weeks thereafter for an interview, HIV testing, focused physical exam, specimen collection for clinical

Preexposure Prophylaxis for the Prevention of HIV Infection in the United States – 2021 Update Clinical Practice Guideline
Page 75 of 108
laboratory tests, counseling about risk- reduction and adherence to PrEP medication doses, pill count,
and dispensing of pills and condoms. 200 persons in each study group (F/TDF or F/TAF) were enrolled
in a substudy to assess BMD by DEXA scans at the hip and spine.
Analysis of data through 96 weeks of follow-up, revealed that after 8,756 person-years of follow-up, 15
HIV infections occurred in the F/TDF group and 7 infections occurred in the F/TAF group. The
incidence rate ratio (0.47, 95% CI=0.19-1.15) was below the upper bound of the value (1.62) needed to
demonstrate non-inferiority of F/TAF compared to F/TDF. Five participants (4 in the F/TDF arm and 1
in the F/TAF arm) were suspected to have acquired HIV before baseline; M184V or M184I mutations
were found in the 4 participants in the F/TDF arm who may have acquired HIV before initiating PrEP at
baseline. No resistance was detected among persons in either arm with incident infections that occurred
after baseline.
Generally, F/TDF and F/TAF were equally well tolerated and low rates of side-effects (≤6% of
participants) were observed with no difference between treatment groups. No differences were observed
between the treatment groups in severe (grade 3) or life-threatening (grade 4) adverse laboratory or
clinical events. No clinically significant declines in median eGFR were seen in either treatment group
between baseline and 48 weeks: +1.8 ml/min for F/TAF (from baseline median 123 ml/min) and -2.3
ml/min for F/TDF (from baseline median 121 ml/min). Compared to participants randomized to F/TAF,
participants randomized to F/TDF had greater decreases from baseline in serum fasting lipid levels.
Conversely, participants randomized to F/TAF had increases in fasting triglycerides while participants
receiving F/TDF had declines. The number and percentage of subjects who initiated lipid-lowering
agents was two-fold higher in the F/TAF group (43 [1.6%]) compared to the F/TDF group (21 [0.8%];
p=0.008). BMD declines of >3% were more common in participants taking F/TDF than participants
taking F/TAF with larger differences in younger men.
Daily oral PrEP with F/TDF or F/TAF is recommended for sexually-active MSM at substantial risk of
HIV acquisition, because the iPrEx and DISCOVER trials present evidence of safety and efficacy in this
population, especially when medication adherence is high. (IA).
Daily oral PrEP with F/TDF or F/TAF is recommended for sexually-active TGW at substantial risk of
HIV acquisition although the evidence of efficacy in this population is limited (IIIB).
PUBLISHED OBSERVATIONAL AND OPEN-LABEL STUDIES OF ANTIRETROVIRAL
PREEXPOSURE PROPHYLAXIS AMONG MEN WHO HAVE SEX WITH MEN
iPrEx Open-Label Extension (OLE) Study
Persons previously enrolled in the iPrEx, ATN 082, and CDC safety PrEP clinical trials were enrolled in
a 72-week open-label study and were offered PrEP free of charge.
125
Seventy-six percent of 1,603
persons (1,428 MSM and 175 transgender women) enrolled received PrEP. HIV incidence among
participants receiving PrEP was 1.8 per 100 person-years (py) versus 2.6 per 100 py in participants
concurrently not choosing PrEP (HR 0.51, 95% CI: 0.26-1.01), adjusted for baseline sexual behaviors.
Among participants receiving PrEP, by dried blood spot drug levels, there were no infections in persons

Preexposure Prophylaxis for the Prevention of HIV Infection in the United States – 2021 Update Clinical Practice Guideline
Page 76 of 108
with drug levels associated with having taken 4 or more doses per week (p<0.0001) compared with
participants taking < 2 doses per week.
PROUD Open-Label Extension (OLE) Study
PROUD was an open-label, randomized, wait-list controlled trial designed for MSM attending sexual
health clinics in England.
209
A pilot was initiated to enroll 500 MSM, in which 275 men were
randomized to receive daily oral F/TDF immediately, and 269 were deferred to start after 1 year. At an
interim analysis, the data monitoring committee stopped the trial early for efficacy at an interim analysis
and recommended that all deferred participants be offered PrEP. Follow-up was completed for 94% of
those in the immediate PrEP arm and 90% of participants in the deferred arm. PrEP efficacy was 86%
(90% CI: 64-96).
Kaiser Permanente Observational Study
An evaluation of a specialized PrEP program provided at the Kaiser Permanente San Francisco Medical
Center
210
reported on a cohort of 653 MSM, 3 heterosexual women, and 1 transgender man (with male
sexual partners) who initiated F/TDF for PrEP between July 2012 and February 2015. Of these
participants, 20 restarted PrEP after discontinuing it during the study period. The mean duration of use
was 7.2 months. No HIV diagnoses were made during 388 py of follow-up on PrEP. No medication
adherence measures were reported. After 12 months of use, 50% of PrEP users had received a diagnosis
of one or more STI (95% CI: 26-35). In a subsequent report on PrEP patients seen at this center, as of
February 2017, there were no HIV infections during 5,104 py of PrEP use while they were being
prescribed medication.
26
Demo Project Open-Label Study
In this demonstration project, conducted at 3 community-based clinics in the United States,
211
MSM (n =
430) and transgender women (n=5) were offered daily oral F/TDF free of charge for 48 weeks. All
patients received HIV testing, brief counseling, clinical monitoring, and STI diagnosis and treatment at
quarterly follow-up visits. A subset of men underwent drug level monitoring with dried-blood spot
testing and protective levels (associated with ≥4 doses per week) were high (80.0%-85.6%) at follow-up
visits across the sites. STI incidence remained high but did not increase over time. Two men became
infected (HIV incidence 0.43 infections per 100 py, 95% CI: 0.05-1.54), both of whom had drug levels
consistent with having taken fewer than 2 doses per week at the visit when seroconversion was detected.
IPERGAY Open-Label Extension (OLE) Study
Findings have been reported from the open-label phase of the IPERGAY trial that enrolled 361 of the
original trial participants.
212
All of the open-label study participants were provided peri-coital PrEP as in
the original trial. After a mean follow-up time of 18.4 months (IQR: 17.7-19.1), the HIV incidence
observed was 0.19 per 100 py which, compared to the incidence in the placebo group of the original trial
(6.60 per 100 py), represented a 97% (95% CI: 81-100) relative reduction in HIV incidence. The one
participant who acquired HIV had not taken any PrEP in the 30 days before his reactive HIV test and
was in an ongoing relationship with an HIV positive partner. Of 336 participants with plasma drug
levels obtained at the 6-month visit, 71% had tenofovir detected. By self-report, PrEP was used at the

Preexposure Prophylaxis for the Prevention of HIV Infection in the United States – 2021 Update Clinical Practice Guideline
Page 77 of 108
prescribed dosing for the most recent sexual intercourse by 50% of participants, with suboptimal dosing
by 24%, and not used by 26%. Reported condomless receptive anal sex at most recent sexual intercourse
increased from 77% at baseline to 86% at the 18-month follow-up visit (p=0.0004). The incidence of a
first bacterial STI in the observational study (59.0 per 100 py) was not higher than that seen in the
randomized trial (49.1 per 100 py) (p=0.11).
The frequency of pill-taking in the open label study population was higher (median 18 pills per month)
than that in the original trial (median 15 pills per month). Therefore, it remains unclear whether the
regimen will be highly protective if taken only a few hours or days before sex, without any buildup of
the drug from prior use.
PUBLISHED TRIALS OF ANTIRETROVIRAL PREEXPOSURE PROPHYLAXIS AMONG
HETEROSEXUAL MEN AND WOMEN
Partners PrEP Trial
The Partners PrEP trial
5
was a phase 3 randomized, double-blind, placebo-controlled study of daily oral
F/TDF or TDF for the prevention of acquisition of HIV by the uninfected partner in 4,758 HIV-
discordant heterosexual couples in Uganda and Kenya. The trial was stopped after an interim analysis in
mid-2011 showed statistically significant efficacy in the medication groups (F/TDF or TDF) compared
with the placebo group. In 48% of couples, the infected partner was male. HIV-positive partners had a
median CD4 count of 495 cells/µL and were not being prescribed antiretroviral therapy, because they
were not eligible by local treatment guidelines. Participants had monthly follow-up visits, and the study
drug was discontinued among women who became pregnant during the trial.
Adherence to medication was very high: 98% by pills dispensed, 92% by pill count, and 82% by plasma
drug-level testing among randomly selected participants in the TDF and F/TDF study groups. Rates of
serious adverse events and serum creatinine or phosphorus abnormalities did not differ by study group.
Modest increases in gastrointestinal symptoms and fatigue were reported in the antiretroviral medication
groups compared with the placebo group, primarily in the first month of use. Among participants of both
sexes combined, efficacy estimates for each of the 2 antiretroviral regimens compared with placebo
were 67% (95% CI, 44-81) for TDF and 75% (95% CI, 55-87) for F/TDF. Among women, the estimated
efficacy was 71% for TDF and 66% for F/TDF. Among men, the estimated efficacy was 63% for TDF
and 84% for F/TDF. Efficacy estimates by drug regimen were not statistically different among men,
women, men and women combined, or between men and women. In a Partners PrEP substudy that
measured plasma TFV levels among participants randomly assigned to receive F/TDF, detectable drug
was associated with a 90% reduction in the risk of HIV acquisition. TDF- or FTC- resistant virus was
detected in 3 of 14 persons determined to have been infected when enrolled (2 of 5 in the TDF group; 1
of 3 in the F/TDF group).
213
No TDF or FTC resistant virus was detected among those infected after
enrollment. Among women, the pregnancy rate was high (10.3 per 100 py), and rates did not differ
significantly between the study groups.
TDF2 Trial

Preexposure Prophylaxis for the Prevention of HIV Infection in the United States – 2021 Update Clinical Practice Guideline
Page 78 of 108
The Botswana TDF2 Trial
6
, a phase 2 randomized, double-blind, placebo-controlled study of the safety
and efficacy of daily oral F/TDF, enrolled 1,219 heterosexual men and women in Botswana, and follow-
up has been completed. Participants were seen for monthly follow-up visits, and study drug was
discontinued in women who became pregnant during the trial.
Among participants of both sexes combined, the efficacy of F/TDF was 62% (95% CI 22%-83%).
Efficacy estimates by sex did not statistically differ from each other or from the overall estimate,
although the small number of endpoints in the subsets of men and women limited the statistical power to
detect a difference. Compliance with study visits was low: 33.1% of participants did not complete the
study per protocol. However, many were re-engaged for an exit visit, and 89.3% of enrolled participants
had a final HIV test.
Among 3 participants later found to have been infected at enrollment, F/TDF -resistant virus was
detected in 1 participant in the F/TDF group and a low level of F/TDF -resistant virus was transiently
detected in 1 participant in the placebo group. No resistant virus was detected in the 33 participants who
seroconverted after enrollment.
Medication adherence by pill count was 84% in both groups. Nausea, vomiting, and dizziness occurred
more commonly, primarily during the first month of use, among those randomly assigned to F/TDF than
among those assigned to placebo. The groups did not differ in rates of serious clinical or laboratory
adverse events. Pregnancy rates and rates of fetal loss did not differ by study group.
FEM-PrEP Trial
The FEM-PrEP trial
214
was a phase 3 randomized, double-blind, placebo-controlled study of the HIV
prevention efficacy and clinical safety of daily F/TDF among heterosexual women in South Africa,
Kenya, and Tanzania. Participants were seen at monthly follow-up visits, and study drug was
discontinued among women who became pregnant during the trial. The trial was stopped in 2011, when
an interim analysis determined that the trial would be unlikely to detect a statistically significant
difference in efficacy between the two study groups.
Adherence was low in this trial: study drug was detected in plasma samples of <50% of women
randomly assigned to F/TDF. Among adverse events, only nausea and vomiting (in the first month) and
transient, modest elevations in liver function test values were more common among those assigned to
F/TDF than those assigned to placebo. No changes in renal function were seen in either group. Initial
analyses of efficacy results showed 4.7 infections per 100/ person-years in the F/TDF group and 5.0
infections per 100 person-years in the placebo group. The hazard ratio 0.94 (95% CI, 0.59-1.52)
indicated no reduction in HIV incidence associated with F/TDF use. Of the 68 women who acquired
HIV during the trial, TDF or FTC resistant virus was detected in 5 women: 1 in the placebo group and 4
in the F/TDF group. In multivariate analyses, there was no association between pregnancy rate and study
group.
Phase 2 Trial of Preexposure Prophylaxis with Tenofovir Among Women in Ghana, Cameroon,
and Nigeria

Preexposure Prophylaxis for the Prevention of HIV Infection in the United States – 2021 Update Clinical Practice Guideline
Page 79 of 108
A randomized, double-blind, placebo-controlled trial of oral tenofovir TDF was conducted among
heterosexual women in West Africa - Ghana (n = 200), Cameroon (n = 200), and Nigeria (n = 136).
215
The study was designed to assess the safety of TDF use and the efficacy of daily TDF in reducing the
rate of HIV infection. The Cameroon and Nigeria study sites were closed prematurely because
operational obstacles developed, so participant follow-up data were insufficient for the planned efficacy
analysis. Analysis of trial safety data from Ghana and Cameroon found no statistically significant
differences in grade 3 or 4 hepatic or renal events or in reports of clinical adverse events. Eight HIV
seroconversions occurred among women in the trial: 2 among women in the TDF group (rate=0.86 per
100 person-years) and 6 among women receiving placebo (rate= 2.48 per 100 person-years), yielding a
rate ratio of 0.35 (95% CI, 0.03-1.93; p=0.24). Blood specimens were available from 1 of the 2
participants who seroconverted while taking TDF; standard genotypic analysis revealed no evidence of
drug-resistance mutations.
VOICE (Vaginal and Oral Interventions to Control the Epidemic) Trial
VOICE (MTN-003)
216
was a phase 2B randomized, double-blind study comparing oral (TDF or F/TDF)
and topical vaginal (tenofovir) antiretroviral regimens against corresponding oral and topical placebos
among 5,029 heterosexual women enrolled in eastern and southern Africa. Of these women, 3,019 were
randomly assigned to daily oral medication (F/TDF, 1,003; TDF, 1,007; oral placebo, 1,009). In 2011,
the trial group receiving oral TDF and the group receiving topical tenofovir were stopped after interim
analyses determined futility. The group receiving oral F/TDF continued to the planned trial conclusion.
After the exclusion of 15 women later determined to have had acute HIV infection when enrolled in an
oral medication group and 27 with no follow-up visit after baseline, 52 incident HIV infections occurred
in the oral TDF group, 61 in the F/TDF group, and 60 in the oral placebo group. Effectiveness was not
significant for either oral PrEP medication group; −49%% for TDF (hazard ratio [HR] 1.49; 95% CI,
0.97-2.29) and −4.4% for F/TDF (HR, 1.04; 95% CI, 0.73-1.49) in the modified-intent-to-treat (mITT)
analysis.
Face-to-face interview, audio computer-assisted self-interview, and pill-count medication adherence
were high in all 3 groups (84%-91%). However, among 315 participants in the random cohort of the
case-cohort subset for whom quarterly plasma samples were available, tenofovir was detected, on
average, in 30% of samples from women randomly assigned to TDF and in 29% of samples from
women randomly assigned to F/TDF. No drug was detected at any quarterly visit during study
participation for 58% of women in the TDF group and 50% of women in the F/TDF group. The
percentage of samples with detectable drug was less than 40% in all study drug groups and declined
throughout the study. In a multivariate analysis that adjusted for baseline confounding variables
(including age, marital status), the detection of study drug was not associated with reduced risk of HIV
acquisition.
The number of confirmed creatinine elevations (grade not specified) observed was higher in the oral
F/TDF group than in the oral placebo group. However, there were no significant differences between
active product and placebo groups for other safety outcomes. Of women determined after enrollment to
have had acute HIV infection at baseline, two women from the F/TDF group had virus with the
M184I/V mutation associated with FTC resistance. One woman in the F/TDF group who acquired HIV

Preexposure Prophylaxis for the Prevention of HIV Infection in the United States – 2021 Update Clinical Practice Guideline
Page 80 of 108
after enrollment had virus with the M184I/V mutation; no participants with HIV had virus with a
mutation associated with tenofovir resistance.
In summary, although low adherence and operational issues precluded reliable conclusions regarding
efficacy in 3 trials (VOICE, FEM-PrEP and the West African trial),
217
2 trials (Partners PrEP and TDF2)
with high medication adherence have provided substantial evidence of efficacy among heterosexual men
and women. All 5 trials have found PrEP to be safe for these populations.
Daily oral PrEP with F/TDF is recommended for heterosexually-active men and women at substantial
risk of HIV acquisition, because these trials present evidence of its safety and 2 present evidence of
efficacy in these populations, especially when medication adherence is high. Daily oral PrEP with
F/TAF is recommended for heterosexually active men based on the results of the DISCOVER trial but is
not yet recommended for women (assigned female sex at birth) who may be exposed to HIV through
vaginal sex, because no trial data for women are available (IA).
PUBLISHED TRIAL OF ANTIRETROVIRAL PREEXPOSURE PROPHYLAXIS AMONG PERSONS
WHO INJECT DRUGS
Bangkok Tenofovir Study (BTS)
BTS was a phase 3 randomized, double-blind, placebo-controlled study of the safety and efficacy of
daily oral TDF for HIV prevention among 2,413 PWID (also called IDU) in Bangkok, Thailand
7
.
The
study was conducted at drug treatment clinics; 22% of participants were receiving methadone treatment
at baseline. At each monthly visit, participants could choose to receive either a 28-day supply of pills or
to receive medication daily by directly-observed therapy. Study clinics (n=17) provided condoms,
bleach (for cleaning injection equipment), methadone, primary medical care, and social services free of
charge. Participants were followed for 4.6 years (mean) and received directly- observed therapy 87% of
the time.
In the modified intent- to-treat analysis (excluding 2 participants with evidence of HIV infection at
enrollment), efficacy of TDF was 48.9% (95% CI, 9.6-72.2; P = .01). A post-hoc modified intent-to-
treat analysis was done, removing 2 additional participants in whom HIV infection was identified within
28 days of enrollment, including only participants on directly observed therapy who met pre-established
criteria for high adherence (taking a pill at least 71% of days and missing no more than two consecutive
doses), and had detectable levels of tenofovir in their blood. Among this set of participants, the efficacy
of TDF in plasma was associated with a 73.5% reduction in the risk for HIV acquisition (95% CI, 16.6-
94.0; P = .03). Among participants in an unmatched case-control study that included the 50 persons with
incident HIV infection and 282 participants at 4 clinics who remained HIV uninfected, detection of TDF
in plasma was associated with a 70.0% reduction in the risk for acquiring HIV (95% CI, 2.3-90.6; P =
.04).
Rates of nausea and vomiting were higher among TDF than among placebo recipients in the first 2
months of medication but not thereafter. The rates of adverse events, deaths, or elevated creatinine did
not differ significantly between the TDF and the placebo groups. Among the 49 HIV infections for

Preexposure Prophylaxis for the Prevention of HIV Infection in the United States – 2021 Update Clinical Practice Guideline
Page 81 of 108
which viral RNA could be amplified (of 50 incident infections and 2 infections later determined to have
been present at enrollment), no viruses with mutations associated with TDF resistance were identified.
Among participants with HIV followed up for a maximum of 24 months, HIV plasma viral load was
lower in the TDF than in the placebo group at the visit when HIV infection was detected (P =0.01) but
not thereafter (P =0.10).
PUBLISHED OPEN-LABEL STUDY OF ANTIRETROVIRAL PREEXPOSURE PROPHYLAXIS
AMONG PERSON WHO INJECT DRUGS
Bangkok Tenofovir Study (BTS) Open-Label Extension (OLE) Study
All 1,315 participants in the randomized trial (BTS) who were HIV-negative and had no renal
contraindication were offered daily oral TDF for 1 year in an open label extension study.
218
Sixty-one
percent (n=798) elected to take PrEP. Participants who were older (≥30 years, p<0.0001), injected
heroin (p=0.007) or had been in prison (p=0.0007) were more likely to start PrEP than participants
without these characteristics. Twenty-eight percent (n=220) did not return for any follow-up visits.
Participants who had injected heroin (p=0.01) or had been in prison (p=0.0007) during the 3 months
before the open label study returned for a follow-up visit. Overall, by diary, adherence was lower in the
open label study (38.5 % of days) than in the randomized clinical trial (83.8% of days). Participants who
injected midazolam (p=0.02) or were in prison (p<0.0001) during the open label study were more likely
to be more than 90% adherent than those without these characteristics. During a median 335 days of
follow-up, one HIV infection occurred in a participant who reported not taking any doses during the 60
days before the positive test, yielding an HIV incidence of 2.1 per 1000 py (95% CI: 0.05-11.7). Among
the 339 (42%) who completed a 12-month follow-up visit, injection and needle sharing did not increase
during the open-label study.
Daily oral PrEP with F/TDF is recommended for PWID at substantial risk of HIV acquisition, because
this trial presents evidence of the safety and efficacy of TDF as PrEP in this population, especially when
medication adherence is high. (IA)
TRIALS OF INJECTABLE ANTIRETROVIRAL PREEXPOSURE PROPHYLAXIS
HPTN 077
HPTN 077
219
was a double-blind, placebo-controlled phase 2a trial conducted in Brazil, Malawi, South
Africa, and the US. Healthy men and women (sex at birth) age 18-65 years at low HIV risk were
randomized (3:1) to receive cabotegravir or placebo injections. For the initial 4 weeks, trial participants
received 1 daily oral tablet containing either CAB or placebo to monitor for short term adverse events.
Participants without safety concerns in the oral phase then received injections in one of two cohorts that
were enrolled sequentially. Cohort 1 enrolled 110 participants to receive 3 intramuscular (IM) injections
of CAB 800 mg or 0.9% saline as placebo every 12 weeks for 3 injection cycles. Cohort 2 enrolled 89
participants to receive IM injections of CAB 600 mg or placebo for 5 injection cycles with the first 2

Preexposure Prophylaxis for the Prevention of HIV Infection in the United States – 2021 Update Clinical Practice Guideline
Page 82 of 108
injections separated by 4 weeks and the remaining 3 injections separated by 8 weeks. Primary analyses
assessed safety tolerability, and pharmacokinetics during the injection phase (weeks 5-41) and adverse
events during both the oral and injection phases. After the last CAB injection at 41 weeks had been
completed for all participants, the study was unblinded. Consenting participants were then seen for
quarterly follow-up visits through 52-76 weeks to assess adverse events and pharmacokinetics during
the “tail” (post-injection) period. HPTN 077 followed the ÉCLAIR trial that showed safety,
acceptability, and tolerability of CAB 800 mg injections in US men without HIV.
220
In the primary analysis through 41 weeks of observation, the only statistically significant difference in
clinical adverse events between those receiving CAB and those receiving placebo was for injection site
pain. A grade 2 (moderate) or higher injection site reaction (ISR) occurred in 38% of participants
receiving CAB and 2% of participants receiving placebo injections (p<0.001). Approximately 90% of
participants in both CAB cohorts experienced any ISRs but most were mild or moderate, and led to
discontinuation of injections for only 1 participant.
Analysis of the pharmacokinetic data through 41 weeks of follow-up showed that the 600 mg every 8
weeks dose used in cohort 2 consistently met prespecified pharmacokinetic targets (e.g., trough
concentrations). All participants met the targets of 80% and 95% of participants with trough
concentrations above 4× and 1× PA-IC90 (protein-adjusted 90% maximum inhibitory concentration),
respectively. Participants with lower body mass index were found to generally exhibit higher
pharmacokinetic peak concentrations after injection, as well as increased AUC (area under the curve)
concentrations. However, the 800 mg every 12 weeks dose used in cohort 1 did not consistently achieve
target concentrations with some differences between male and female participants.
Among 85 women (46 in cohort 1, 39 in cohort 2), 79 reported using hormonal contraception at baseline
and 6 reported that they did not
221
. Reported oral contraception use was associated with lower peak CAB
concentration but was not associated with significant differences in other pharmacokinetic parameters
(including trough levels, AUC, and time to LLOQ) when compared to reported non-use of hormonal
contraception. No other hormonal contraceptive type (injectable, implants, and other) was associated
with significant differences in CAB pharmacokinetic parameters.
The tail-phase analyses
149
included 177 participants, including 43 placebo recipients and 134 persons
who had at least one CAB injection and had at least three cabotegravir measurements higher than the
LLOQ after the final injection at 41 weeks. 117 women and 60 men were followed, 74 participants in
CAB cohort 1 and in CAB cohort 2, 25 in placebo cohort 1 and 18 in placebo cohort 2.
The incidence of grade 2 or worse adverse events was significantly lower during the tail phase than the
injection phase (p<0·0001). The pharmacokinetic analysis found that the median time from the last
injection to the time when cabotegravir concentration decreased below the LLOQ was approximately
33% longer for women (67.3 weeks [IQR 29.1–89.6; range 17.7–225.5] (p=0·0003)) than for men (43.7
weeks [IQR 31·1–66·6; range 20.4–152.5] (geometric mean by sex at birth found a fold-change 1.33,
95% CI 1·06–1.68; p=0.014)). The median time to LLOQ was 31% longer 65.4 weeks (IQR 49.8–95.3;
range 19.7–198.2) for participants with a high body-mass index (BMI) than for those with a low BMI

Preexposure Prophylaxis for the Prevention of HIV Infection in the United States – 2021 Update Clinical Practice Guideline
Page 83 of 108
57.7 weeks (IQR 36.2–76.3; range 17.7–225.5) (geometric mean fold-change 1.31, 95% CI 1.06–1.63;
p=0·015). However, sex at birth and BMI accounted for, less than 10% of the variability observed in the
duration of the pharmacologic tail.
In these low-risk cohorts, one female participant in cohort 1 acquired HIV. The seroconversion occurred
48 weeks after the final injection of CAB. Her plasma CAB concentrations were below the level of
quantitation at both the visit when HIV infection was first detected and at her visit 12 weeks earlier
when she had undetectable HIV RNA. No integrase resistance mutations were detected with next
generation sequencing.
Four pregnancies occurred, two among women receiving placebo (one full-term healthy infant, 1one
miscarriage likely due to Zika virus infection) and 2 among women receiving CAB. Both CAB
pregnancies occurred during the tail phase one 32 weeks after her final CAB injection (early term,
healthy infant) cohort 2) and one 108 weeks after her final injection (full-term, healthy infant, cohort 1).
No birth defects were identified in newborns.
A post-hoc analysis
222
found no significant changes in weight or fasting glucose or lipid parameters
when comparing participants receiving CAB injections to those receiving placebo.
The low number of transgender men (n=6) and transgender women (n=1) in this low-risk cohort did not
allow the investigation of the effects of gender affirming hormone therapy.
HPTN 083
HPTN 083 is a phase 3, randomized, double-blind, active control trial conducted in Argentina, Peru,
Brazil, Thailand, Vietnam, South Africa, and the United States among adult men and transgender
women who reported sex with a man during the 6 months preceding enrollment. Participants were
randomly assigned to receive cabotegravir
13
or oral F/TDF. During a 5-week lead-in phase, 2282
persons in the cabotegravir group received daily oral cabotegravir tablets (30 mg) and 2284 persons in
the F/TDF arm received placebo tablets for daily use. Following completion of the lead-in period, those
randomized to the cabotegravir group received daily oral placebo tablets and intramuscular injections of
600 mg cabotegravir at weeks 5 and 9 and every 8 weeks thereafter. Those randomized to the F/TDF
group received F/TDF tablets for daily use and placebo intramuscular injections at weeks 5 and 9 and
every 8 weeks thereafter. All participants (cabotegravir and F/TDF groups) had regularly scheduled
interviews, HIV testing, counseling about risk-reduction and adherence to oral pills prescribed.
A scheduled interim analysis review by the Data Safety and Monitoring Board in May 2020 determined
that CAB was non-inferior to F/TDF, the study was unblinded, and CAB was offered to all study
participants and study follow-up visits were continued. The final prespecified primary analysis
determined that the statistical criteria for superiority of CAB compared to F/TDF was met. After the
exclusion of participants later determined to have been HIV- infected at enrollment and those who did
not have an HIV test after enrollment, 39 of 2247 participants in the F/TDF group and 13 of 2243 in the

Preexposure Prophylaxis for the Prevention of HIV Infection in the United States – 2021 Update Clinical Practice Guideline
Page 84 of 108
CAB group had acquired HIV. HIV incidence was low in both groups; 1.22/100 person-years in the
F/TDF group and 0.41/100 person-years in the CAB group. Participation in the CAB group was
associated with a 66% reduction in the risk of HIV acquisition (95% CI, 38%-82%) compared to the
F/TDF group. Post-hoc centralized testing of stored plasma specimens led to readjudication of the
timing identification of the first HIV-positive test from incident to baseline infection for 2 participants in
the CAB group and none in the F/TDF group. Based on this post-hoc readjudication, incidence in the
CAB group was revised to 0.37/100 person-years with a 68% reduction in the risk of HIV acquisition
(95% CI, 35%-81%) compared to the F/TDF group.
In the group randomized to CAB, 1 in 4 baseline infections and 4 of 9 incident infections with a
resistance test result had one or more INSTI resistance mutations detected
78
. No resistance mutations
were detected among 4 infections that occurred after the last CAB injection (i.e., during the tail phase).
Among the 5 participants with INSTI resistance mutations detected, phenotyping results for 3
participants found low replication capacity and susceptibility to dolutegravir. Some showed partial or
significant resistance to one or more INSTI medications.
CAB was well tolerated. ISRs (e.g., pain, tenderness, induration at the site) occurred in 81% of
participants in the CAB group and 31% of those in the F/TDF group who received normal saline placebo
injections. These were most common after the first, second, or third injection. Nearly all were mild or
moderate severity and resolved within 1 week of injection. Only 2.4% of CAB participants discontinued
receiving injections because of the discomfort of injection site reactions. 33% of participants had grade 3
or higher laboratory adverse events with no statistically significant differences between the CAB and
F/TDF groups. In the first 40 weeks of the study, participants in the CAB group had a median weight
gain from enrollment of 1.54 kg (95% CI 1.0-2.0). but from week 40-105, median weight gain was only
1.07 kg (95% CI 0.61-1.5).
Additional trials to assess the safety of PrEP with CAB injections for adolescent men and transgender
women who have sex with men are planned.
HPTN 084
HPTN 084
13
is a phase 3, randomized, double-blind, active control trial conducted in Botswana,
Eswatini, Kenya, Malawi, South Africa, Uganda, and Zimbabwe among adult women who reported sex
with a man during the 6 months preceding enrollment. Participants were randomly assigned to receive
cabotegravir or oral F/TDF. During a 5-week lead-in phase, 2282 women in the cabotegravir group
received daily oral cabotegravir tablets and 2284 women in the F/TDF arm received placebo tablets for
daily use. Following completion of the lead-in period, those randomized to the cabotegravir group
received daily oral placebo tablets and intramuscular injections of cabotegravir at weeks 5 and 9 and
every 8 weeks thereafter. Those randomized to the F/TDF group received F/TDF tablets for daily use
and placebo intramuscular injections at weeks 5 and 9 and every 8 weeks thereafter. All participants
(cabotegravir and F/TDF groups) had regularly scheduled interviews, HIV testing, counseling about
risk-reduction and adherence to oral pills prescribed.
Preexposure Prophylaxis for the Prevention of HIV Infection in the United States – 2021 Update Clinical Practice Guideline
Page 85 of 108
A scheduled interim analysis review by the Data Safety and Monitoring Board in November 2020
determined that CAB was superior to F/TDF, the study was unblinded, CAB was offered to all study
participants, and study follow-up visits were continued. After the exclusion of participants later
determined to have been HIV-infected at enrollment and those who did not have an HIV test after
enrollment, 38 HIV infections occurred during follow-up, with 4 infections in the CAB group (incidence
rate 0.21/100 person/years) and 34 infections in the F/TDF group (incidence rate 1.79/100 person/years).
The hazard ratio comparing the CAB and F/TDF groups was 0.11 (95% CI 0.04-0.32). HIV incidence
was lower than expected in both groups demonstrating that both drugs offered high levels of protection
but participation in the CAB group was associated with an 89% reduction in the risk of HIV acquisition
compared to the F/TDF group.
CAB was well tolerated with ISRs (e.g., pain, tenderness, induration at the site) the most commonly
occurring adverse event. Nearly all were mild or moderate severity.
Additional studies to determine the safety of PrEP with CAB injections for adolescent women and
confirm safety for pregnant women and their newborns are planned.
PrEP with cabotegravir intramuscular injections is recommended for adults at substantial risk of HIV
acquisition, because clinical trials present evidence of its safety and efficacy in these populations (IA).
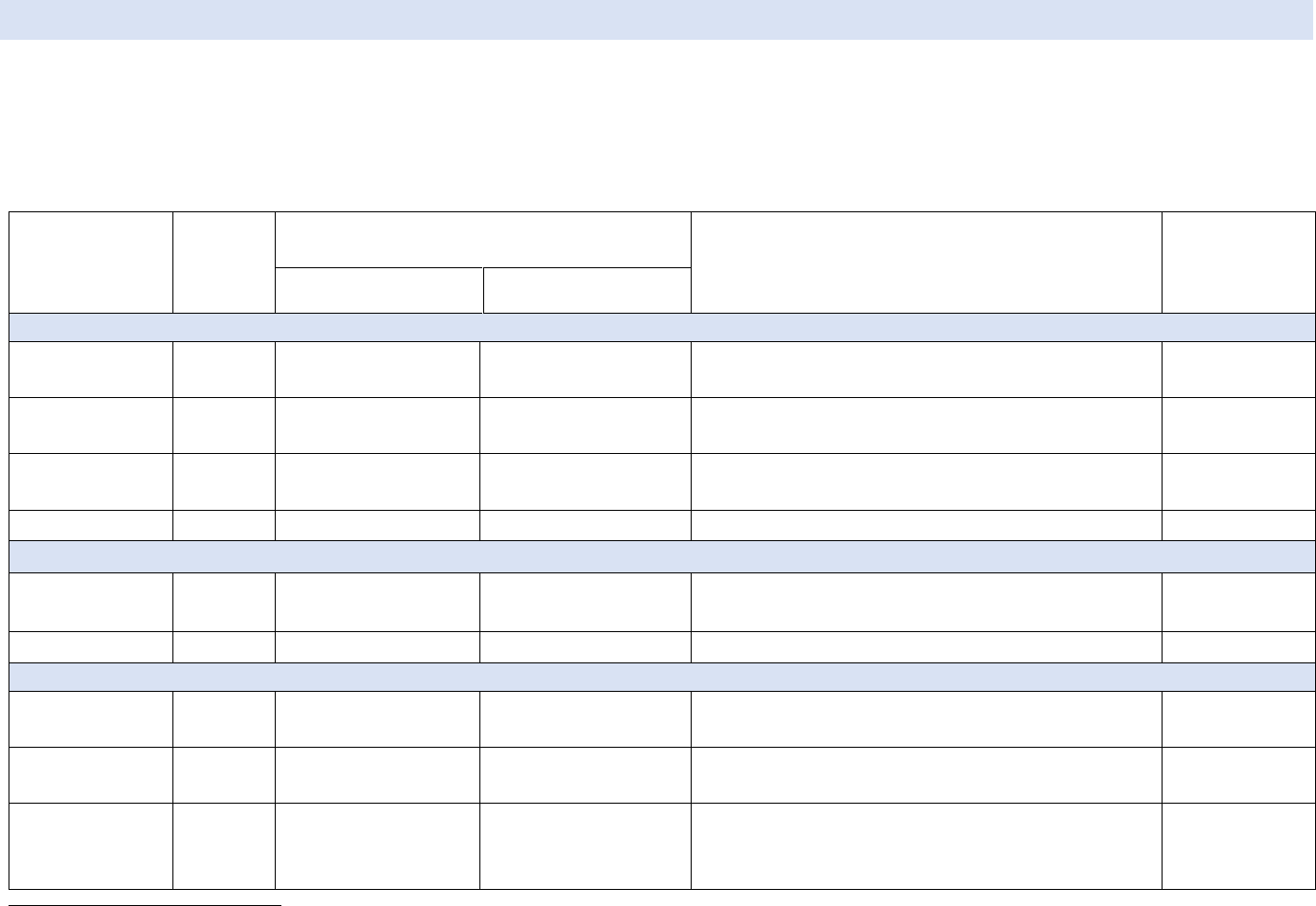
TRIAL EVIDENCE REVIEW TABLES
TABLE 12: EVIDENCE SUMMARY — OVERALL EVIDENCE QUALITY OF RANDOMIZED PREP CLINICAL TRIALS (PER
GRADE CRITERIA
186
)
Oral Tenofovir-based PrEP Trials
Study
Design
a
Participants
Limitations
Quality of
Evidence
(See Table 11,
Appendix 1)
Agent
Control
Among Men Who have Sex with Men
iPrEx Trial
Phase 3
F/TDF (n = 1251)
Placebo (n = 1248)
Adherence
High
US MSM Safety
Trial
Phase 2
TDF (n = 201)
Placebo (n = 199)
Minimal
High
ATN 082
Pilot
F/TDF (n=20)
Placebo (n=19)
No pill (n=19)
Small size, stopped early, limited follow-up time, low
medication adherence
Low
DISCOVER
Phase 3
F/TAF (n=2694)
F/TDF (n=2693)
Minimal
High
Among Heterosexual Men and Women
Partners PrEP
Phase 3
TDF (n = 1589)
F/TDF (n = 1583)
Placebo (n = 1586)
Minimal
High
TDF2
Phase 2
F/TDF (n = 611)
Placebo (n = 608)
High loss to follow-up; modest sample size
Moderate
Among Heterosexual Women
FEM-PrEP
Phase 3
F/TDF (n = 1062)
Placebo (n = 1058)
Stopped at interim analysis, limited follow-up time;
very low adherence to drug regimen
Low
West African
Trial
Phase 2
TDF (n = 469)
Placebo (n = 467)
Stopped early for operational concerns; small sample
size; limited follow-up time on assigned drug
Low
VOICE
Phase 2B
TDF (n = 1007)
F/TDF (n = 1003)
Placebo (n = 1009)
TDF arm stopped at interim analysis (futility); very
low adherence to drug regimen in both TDF and
F/TDF arms
Low
a
All trials in this table were randomized, double-blind, prospective clinical trials of daily oral PrEP
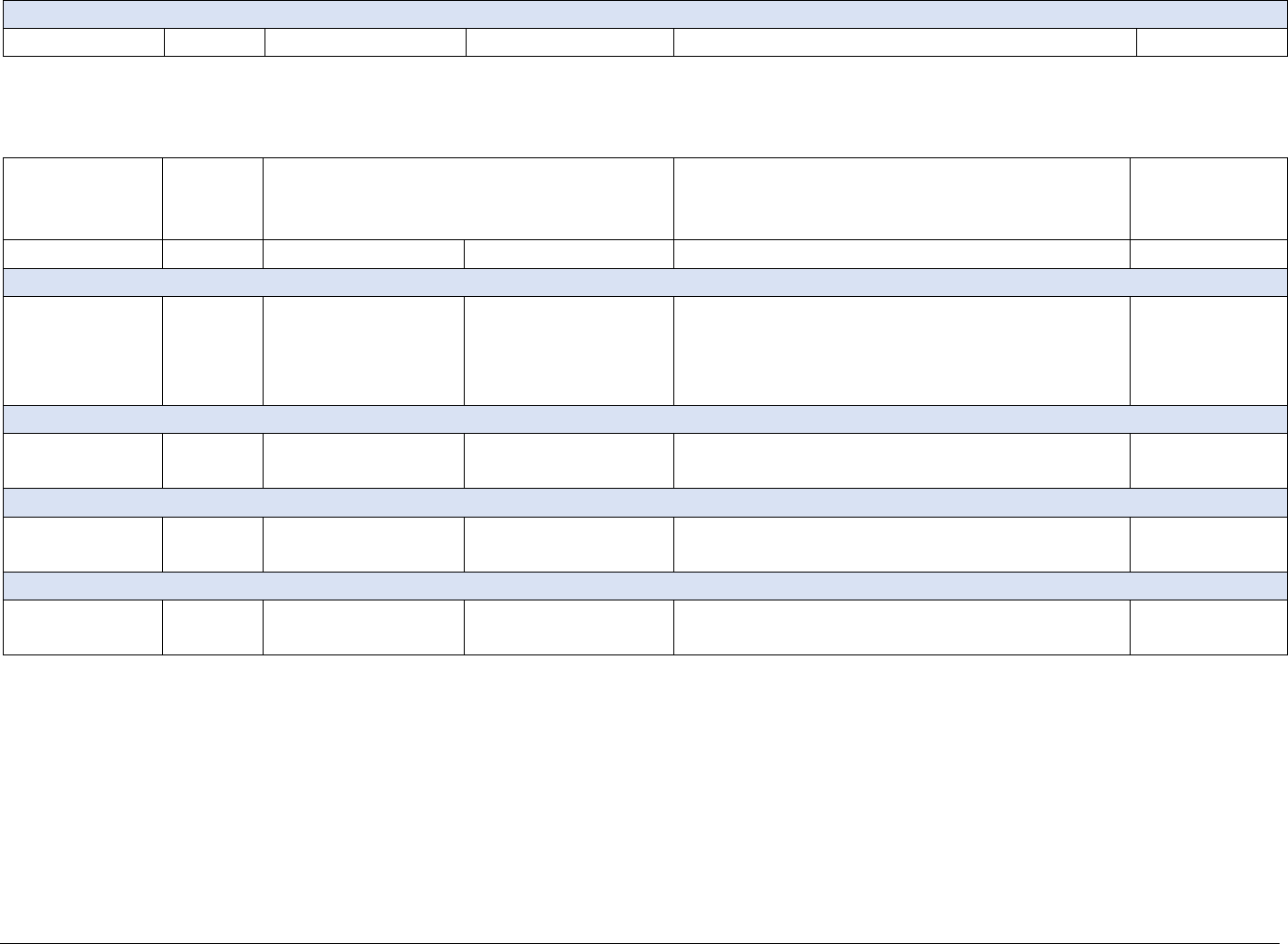
Preexposure Prophylaxis for the Prevention of HIV Infection in the United States – 2021 Update Clinical Practice Guideline
Page 87 of 108
Among Injection Drug Users
BTS
Phase 3
TDF (n = 1204)
Placebo (n = 1207)
Minimal
High
Injectable Cabotegravir PrEP Trials
Study
Design
Participants
Limitations
Quality of
Evidence
Agent
Control
Among Men and Women
HPTN 077
Phase 2a
Cabotegravir 800 mg
injection (n=82)
Cabotegravir 600 mg
injection(n=69)
Placebo (n=28)
Placebo (n=20)
High follow-up discontinuation rates
Limited sample size
Moderate
Among Men Who have Sex with Men and Transgender Women
HPTN 083
Phase
2b/3
Cabotegravir 600 mg
injection (n=2282)
F/TDF daily oral
(n=2284)
Minimal
High
Among Transgender Women
HPTN 083
Phase
2b/3
Cabotegravir 600 mg
injection (n=)
F/TDF daily oral (n=)
Minimal
High
Among Heterosexual Women
HPTN 084
Phase 3
Cabotegravir 600 mg
injection (n=1613)
F/TDF daily oral
(n=1610)
Minimal
High
Note: GRADE quality ratings:
high = further research is very unlikely to change our confidence in the estimate of effect;
moderate = further research is likely to have an important impact on our confidence in the estimate of effect and may change the estimate;
low = further research is very likely to have an important impact on our confidence in the estimate of effect and is likely to change the estimate;
very low = any estimate of effect is very uncertain.
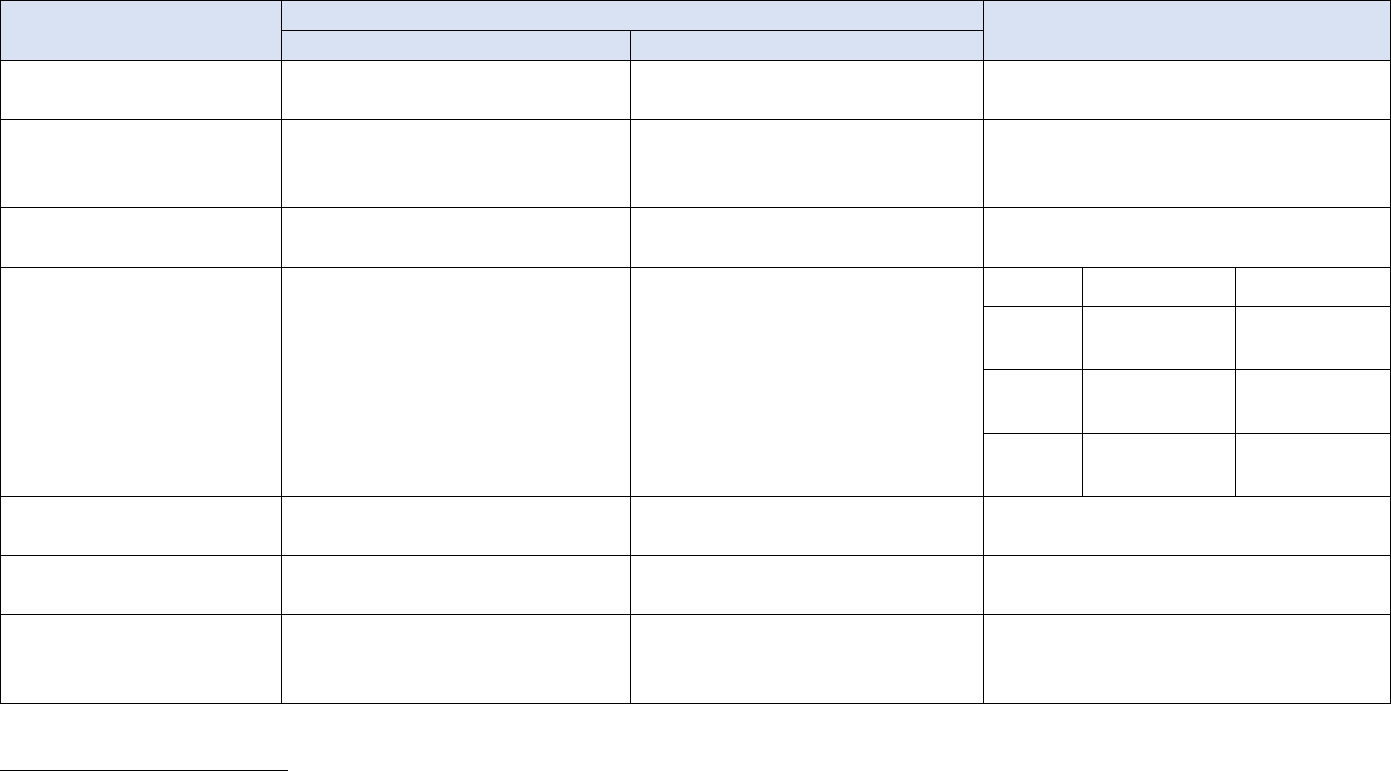
TABLE 13: EVIDENCE SUMMARY OF RANDOMIZED CLINICAL TRIALS — HIV INCIDENCE FINDINGS
Study
Outcome Analyses— HIV incidence (mITT)
Effect — HR [Efficacy Estimate]
(95% CI)
Agent
Control
iPrEx (MSM and TGW)
36 infections among 1,224 persons
64 infections among 1,217 persons
0.56 [44%]
(0.37–0.85)
iPrEx (TGW)
expanded TGW definition
11 infections (# on F/TDF not
reported)
10 infections (# on placebo not
reported)
1.1 (0.5-2.7)
US MSM Safety Trial
3 infections among 201 persons
(all 3 in delayed arm, not on TDF)
4 infections among 199 persons
(1 acute infection at enrollment)
Not Reported
Partners PrEP (heterosexual
men and women)
TDF
17 infections among 1572 persons
F/TDF
13 infections among 1568 persons
52 infections among 1568 persons
TDF
F/TDF
All
0. 33 [67%]
(0.19–0.56)
0.25 [75%]
(0.13–0.45)
Women
0.29 [71%]
(0.13–0.63)
0.34 [66%]
(0.16–0.72)
Men
0.37 [63%]
(0.17–0.80)
0.16 [84%]
(0.06–0.46)
TDF2 (heterosexual men and
women)
9 infections among 601 persons
1.2 infections/100 person-years
24 infections among 599 persons
3.1 infections per 100 person-years
0.38 [62%]
(0.17–0.79)
FEM-PrEP (heterosexual
women)
33 infections among 1024 persons
4.7 infections per 100 person-years
35 infections among 1032 persons
5.0 infections per 100 person-years
0.94 [6%]
a
(0.59–1.52)
West African Trial
(heterosexual women)
2 infections among 427 persons
0.86 infections per 100 person-years
6 infections among 432 persons
2.48 infections per 100 person-years
0.35 [65%]
a
(0.03–1.93)
a
Not statistically significant.
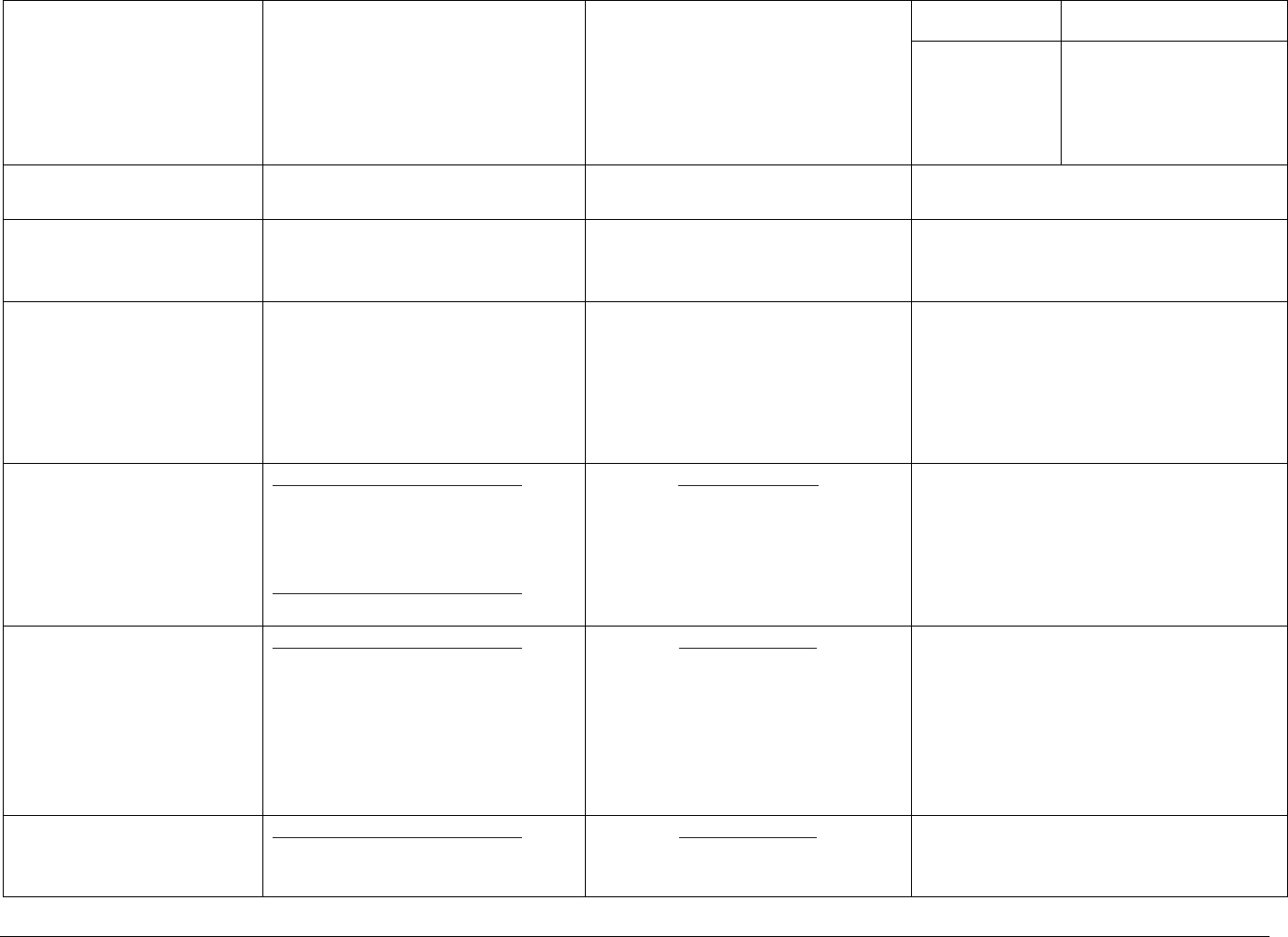

Preexposure Prophylaxis for the Prevention of HIV Infection in the United States – 2021 Update Clinical Practice Guideline
Page 89 of 108
VOICE (heterosexual
women)
TDF
52 infections among 993 persons
6.3 infections per 100 person-years
F/TDF
61 infections among 985 persons
4.7 infections per 100 person-years
35 infections among 999 persons
4.2 infections per 100 person-years
TDF
F/TDF
1.49 [-50 %]
a
(0.97–2.3)
1.04 [-4%]
a
(0.73, 1.5)
BTS (persons who inject
drugs)
17 infections among 1204 persons
0.35 infections per 100 person-years
33 infections among 1207 persons
0.68 infections per 100 person-years
0.51 [49%]
(9.6, 72.2)
DISCOVER (MSM and
TGW)
F/TAF
7 infections among 2670 persons
0.16 infections per 100 person-years
F/TDF
15 infections among 2665 persons
0.34 infections per 100 person-years
0.47 [-53%]
(0.19-1.15)
DISCOVER (TGW)
Not reported
Not reported
Not reported
Included 74 TGW of which 26 prematurely
discontinued study drug (F/TAF 16,
F/TDF 10) and 24 dropped out of the study
by 48 weeks of follow-up
HPTN 077 (men and
women)
Cabotegravir 800 mg injection
1 infection among 82 persons
48 weeks after final injection
Cabotegravir 600 mg injection
0 infections among 69 persons
Placebo injection
0 infections among 151 persons
Not reported
HPTN 083 (MSM and
TGW)
Cabotegravir 600 mg injection
13 infections among 2244 persons
5 during continuous, on-time
injections
3 during oral lead in phase
5 after hiatus of injections
0.41 infections per 100 person-years
daily oral F/TDF
39 infections among 2250 persons
7 after hiatus of pill receipt
32 during continuous, on-time pill
receipt
1.22 infections per 100 person-years
0.34 (0.18-0.62)
HPTN 083 (TGW)
Cabotegravir 600 mg injection
2 infections among 266 persons
0.54 infections per 100 person-years
daily oral F/TDF
7 infections among 304 persons
1.80 infections per 100 person-years
0.34 (.08-1.56)

Preexposure Prophylaxis for the Prevention of HIV Infection in the United States – 2021 Update Clinical Practice Guideline
Page 90 of 108
HPTN 084 (heterosexual
women)
Cabotegravir 600 mg injection
4 infections among 1613 persons
daily oral F/TDF
34 infections among 1613 persons
0.11 (0.04-0.32)
mITT: modified intent to treat analysis; HR: hazard ratio; IRR: incidence rate ratio
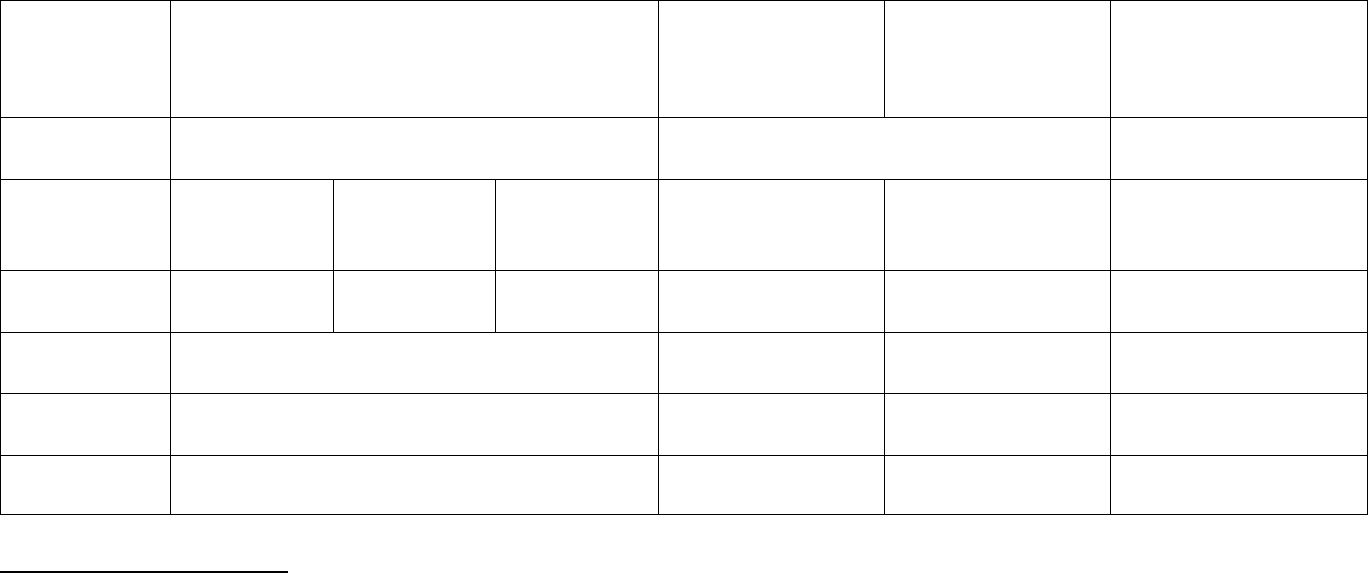
TABLE 14: MEASURES OF EFFICACY, BY MEDICATION ADHERENCE, PERCENTAGE REDUCTION IN HIV INCIDENCE IN
RANDOMIZED CLINICAL TRIALS
Study
Modified Intent-to-Treat Efficacy
Efficacy by
Self-report
Adherence Measures
Efficacy by
Pill-count Adherence
Measures
(95% CI)
Efficacy by
Blood Detection of Drug
Measures
a
(95% CI)
iPrEx
(F/TDF)
44% (15–63%)
>50% 50% (18–70%)
>90% 73% (41–88%)
92% (40–99%)
Partners PrEP
All
TDF: 67%
F/TDF: 75%
Men
TDF: 63%
F/TDF: 84%
Women
TDF: 71%
F/TDF: 66%
NR
100% (87–100%)
TDF: 86% (67–94%)
F/TDF: 90% (58–98%)
TDF2
(F/TDF)
All
63%
Men
80%
Women
49%
b
NR
NR
TDF detected: 85%
b
FEM-PrEP
(F/TDF)
NR
NR
NR
NR
VOICE
(TDF, F/TDF)
NR
NR
NR
NR
BTS
(TDF)
49%
NR
56% (-19 to 86%)
c
74% (17–94%)
NR, not reported.
a
Tenofovir detection assays were done in subsets of persons randomly assigned to receive TDF or TDF/FTC
b
Finding not statistically significant
c
Among participants on directly observed therapy
TABLE 15: EVIDENCE SUMMARY OF RANDOMIZED CLINICAL TRIALS — SAFETY AND TOXICITY
Study
Outcome Analyses
Agent
Control
Grade 3/4 Adverse Clinical Events
a
iPrEx
52 events
59 events
ATN 082
1 event
1 event
TDF2
21 events
32 events
West African Trial
NR
NR
Grade 3/4 Adverse Laboratory Events
a
iPrEx
59 events
48 events
ATN 082
3 events
0 events
TDF2
32 events
32 events
West African Trial
1 event
5 events
Grade 3/4 Adverse Events (Clinical and Laboratory)
a
Partners PrEP
TDF: 323 events
TDF/FTC: 337 events
307 events
FEM-PrEP
NR
NR
US MSM Safety Trial
36 events
26 events
VOICE
NR
NR
BTS
175 events
173 events
DISCOVER
F/TAF: 6% of participants
F/TDF: 5 % of participants
HPTN 077
Not reported
Not reported
HPTN 083
Cabotegravir: 31.8% of participants
F/TDF: 33.6% of participants
HPTN 084
Pending*
Pending*
Injection Site Reactions (≥ Grade 2)
HPTN 077
Cabotegravir: 38.1%
Placebo: 2.3%
HPTN 083
Cabotegravir: 31.8% of participants
Not applicable
HPTN 084
Pending*
Not applicable
NR, not reported.
a
RDBPCT = randomized, double-blind, prospective clinical trial
TABLE 16: EVIDENCE SUMMARY OF RANDOMIZED CLINICAL TRIALS — HIV RESISTANCE FINDINGS
Study
Outcome Analyses
Agent
Control
iPrEx
2 resistant viruses among 2 persons infected at baseline
0 resistant viruses among 36 persons infected after baseline
1 resistant virus among 8 persons infected at baseline
0 resistant viruses among 64 persons infected after baseline
US MSM Safety Trial
0 resistant viruses among 3 persons infected after baseline (in
delayed arm before starting drug)
1 resistant virus among 1 person infected at baseline
0 resistant viruses among 3 persons infected after baseline
Partners PrEP
2 resistant viruses among 5 persons infected at baseline and
randomly assigned to TDF
1 resistant virus among 3 persons infected at baseline and randomly
assigned to F/TDF
0 resistant viruses among 27 persons infected after baseline
0 resistant viruses among 6 persons infected at baseline
0 resistant viruses among 51 persons infected after baseline
TDF2
1 resistant virus in 1 person infected at baseline
0 resistant viruses among 9 persons infected after baseline
1 resistant virus in 1 person infected at baseline (very low
frequency and transient detection)
0 resistant viruses among 24 persons infected after baseline
FEM-PrEP
4 resistant viruses among 33 persons infected after baseline
1 resistant virus in 35 persons infected after baseline
West African Trial
0 resistant viruses among 2 persons infected while on TDF
NR
VOICE
NR
—
BTS
0 resistant viruses among 49 persons infected after baseline
DISCOVER
0 resistant viruses among 1 person infected at baseline and
randomly assigned to F/TAF
0 resistant viruses among 7 persons infected after baseline
4 resistant viruses among 4 persons infected at baseline and
randomly assigned to F/TDF
0 resistant viruses among 11 persons infected after baseline
HPTN 083
1 resistant virus among 4 persons infected at baseline and randomly
assigned to F/TAF
4 resistant viruses among 9 persons infected after baseline
2 resistant viruses among 3 persons infected at baseline and
randomly assigned to F/TDF
4 resistant viruses among 39 persons infected after baseline
HPTN 084
Not yet reported
Not yet reported
NR, not reported.
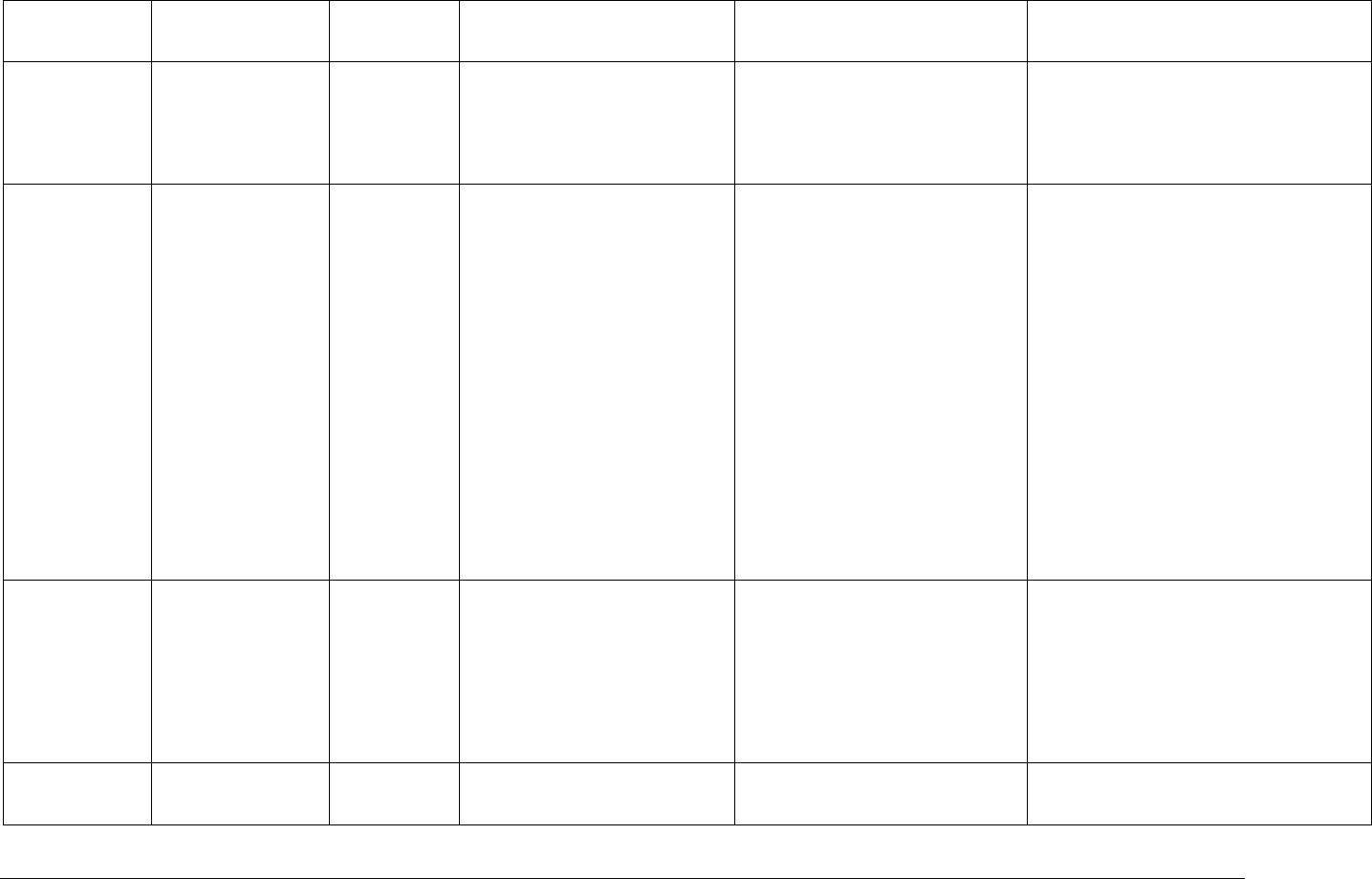

Preexposure Prophylaxis for the Prevention of HIV Infection in the United States – 2021 Update Clinical Practice Guideline
Page 94 of 108
TABLE 17: EVIDENCE SUMMARY OF OPEN-LABEL STUDIES
Study
Design
Population
Effect HR [Efficacy
Estimate]
Efficacy by Blood
Detection of Drug Measure
Resistance
PROUD
Wait-list Control
MSM
[86%] [90% CI: 64%-96%]
comparing immediate vs.
deferred group
Not reported
2 resistant viruses among 3
persons infected at baseline
0 resistant viruses among 23
persons infected after baseline
iPrEx OLE
a
RCT Open-
Label Extension
MSM
0.51 [49%] (95% CI: 0.26-
1.01) comparing those
electing to use PrEP with
those who did not, adjusted
for baseline sexual risk
behavior
Compared with being off
PrEP, HRs for
seroconversion stratified by
weekly dosing inferred from
blood drug levels:
<2 doses/week
0.56 [44%] (0.23-1.31)
2-3 doses/week
0.16 [84%] (0.01-0.79)
4-6 doses/week
0.0 [100%] (0.0-0.21)
7 doses/week
0.0 [100%] (0.0-0.43)
0 resistant viruses among 2
persons infected at baseline (not
started on PrEP)
1 resistant virus among 28 persons
infected after baseline started on
PrEP
0 resistant viruses among 13
persons infected after baseline not
started on PrEP
Demo Project
Clinical Cohort
MSM
b
HIV incidence 0.43 per
100 py (no comparison
group) in a population with
an STI incidence of 90 per
100 py observed during
follow-up.
b
Both seroconverters had
blood drug levels associated
with <2 doses/week
1 resistant virus among 3 persons
infected at enrollment and started
on PrEP
0 resistant viruses among 2
persons infected after baseline
started on PrEP
Kaiser
Permanente
Clinical Cohort
MSM
0 HIV diagnoses in 5104
py of follow-up
Not reported
Not applicable
a
included men who had participated in the iPrEx, CDC Safety, and Adolescent Trials Network 082 PrEP trials
b
653 MSM, 3 heterosexual women, 1 transgender man who has sex with men
References
1. Grohskopf LA, Chillag KL, Gvetadze R, et al. Randomized trial of clinical safety of daily oral
tenofovir disoproxil fumarate (TDF) among HIV-uninfected men who have sex with men (MSM) in
the United States. J Acquir Immune Defic Syndr. 2013; 64(1):79-86.
2. Grant RM, Lama JR, Anderson PL, et al. Preexposure chemoprophylaxis for HIV prevention in men
who have sex with men. N Engl J Med. 2010;363(27):2587-99. doi:10.1056/NEJMoa1011205
3. Food and Drug Administration. FDA Briefing Document, Descovy for PrEP, Meeting of the
Antimicrobial Drugs Advisory Committee. 2019. Accessed 2 February 2020.
https://www.fda.gov/advisory-committees/advisory-committee-calendar/august-7-2019-
antimicrobial-drugs-advisory-committee-meeting-announcement-08072019-
08072019#event-materials
4. Mayer KH, Molina J-M, Thompson MA, et al. Emtricitabine and tenofovir alafenamide vs
emtricitabine and tenofovir disoproxil fumarate for HIV pre-exposure prophylaxis (DISCOVER):
primary results from a randomised, double-blind, multicentre, active-controlled, phase 3, non-
inferiority trial. The Lancet. 2020;396(10246):239-254.
5. Baeten JM, Donnell D, Ndase P, et al. Antiretroviral prophylaxis for HIV prevention in heterosexual
men and women. N Engl J Med. 2012;367(5):399-410. doi:doi:10.1056/NEJMoa1108524
6. Thigpen MC, Kebaabetswe PM, Paxton LA, et al. Antiretroviral preexposure prophylaxis for
heterosexual HIV transmission in Botswana. N Engl J Med. 2012;367(5):423-434.
doi:doi:10.1056/NEJMoa1110711
7. Choopanya K, Martin M, Suntharasamai P, et al. Antiretroviral prophylaxis for HIV infection in
injecting drug users in Bangkok, Thailand (the Bangkok Tenofovir Study): a randomised, double-
blind, placebo-controlled phase 3 trial. Lancet. Jun 15 2013;381(9883):2083-90.
doi:10.1016/S0140-6736(13)61127-7
8. Food and Drug Administration. Truvada approved to reduce the risk of sexually transmitted HIV in
people who are not infected with the virus. 2012; FDA In Brief: FDA continues to encourage
ongoing education about the benefits and risks associated with PrEP, including additional
steps to help reduce the risk of getting HIV | FDA. Accessed 2 29 October 20219.
9. Hosek SG, Landovitz RJ, Kapogiannis B, et al. Safety and feasibility of antiretroviral Preexposure
Prophylaxis for Adolescent Men Who Have Sex With Men Aged 15 to 17 Years in the United
States. JAMA Pediatr. 2017;5:E1-E9.
10. Hosek SG, Rudy B, Landovitz R, et al. An HIV preexposure prophylaxis demonstration project and
safety study for young MSM. J Acquir Immune Defic Syndr. 2017;74(1):21-29.
doi:10.1097/qai.0000000000001179
11. US Preventive Services Task Force. Prevention of Human Immunodeficiency Virus (HIV) Infection:
Preexposure Prophylaxis. Accessed 1 December 2019,
https://www.uspreventiveservicestaskforce.org/Page/Document/RecommendationStatemen
tFinal/prevention-of-human-immunodeficiency-virus-hiv-infection-pre-exposure-
prophylaxis
12. HIV Prevention Trials Network. HPTN 084 Study Demonstrates superiority of CAB LA to oral
FTC/TDF for the prevention of HIV. 2020. Accessed 19 November 2020.
https://www.hptn.org/news-and-events/press-releases/hptn-084-study-demonstrates-
superiority-of-cab-la-to-oral-ftctdf-for

Preexposure Prophylaxis for the Prevention of HIV Infection in the United States – 2021 Update Clinical Practice Guideline
Page 96 of 108
13. Landovitz RJ, Donnell D, Clement ME, et al. Cabotegravir for HIV prevention in cisgender men and
transgender women. N Engl J Med. 2021;385(7):595-608.
14. Smith DK, Van Handel M, Grey J. Estimates of adults with indications for HIV pre-exposure
prophylaxis by jurisdiction, transmission risk group, and race/ethnicity, United States, 2015. Ann
Epidemiol. 2018;28(12):850-857. e9.
15. Harris NS, Satcher Johnson A, Huang YA, et al. Vital Signs: Status of human immunodeficiency virus
testing, viral suppression, and HIV preexposure prophylaxis — United States, 2013–2018. MMWR
Morb Mortal Wkly Rep: Recommendations and Reports. 2019;68(48):1117-1123. Accessed 1
December 2019.
https://www.cdc.gov/mmwr/volumes/68/wr/mm6848e1.htm?s_cid=mm6848e1_w
16. Sullivan PS, Giler RM, Mouhanna F, et al. Trends in the use of oral emtricitabine/tenofovir
disoproxil fumarate for pre-exposure prophylaxis against HIV infection, United States, 2012–2017.
Ann Epidemiol. 2018;28(12):833-840.
17. Harris NS JA, Huang YA, Kern D, et al. . Vital Signs: Status of human immunodeficiency virus
testing, viral suppression, and HIV preexposure prophylaxis — United States, 2013–2018. MMWR
Morb Mortal Wkly Rep. 2019;68:1117–1123.
http://dx.doi.org/10.15585/mmwr.mm6848e1external
18. Centers for Disease Control and Prevention. Estimated HIV incidence and prevalence in the United
States, 2014–2018. HIV Surveillance Supplemental Report. 2020;25(1). Accessed 2 January 2021.
http://www.cdc.gov/hiv/library/reports/hiv-surveillance.html
19. Centers for Disease Control and Prevention. Diagnoses of HIV infection in the United States and
Dependent Areas, 2018 (preliminary). HIV Surveillance Report. 2019;30:1-129. Accessed 1
December 2019. https://www.cdc.gov/hiv/pdf/library/reports/surveillance/cdc-hiv-
surveillance-report-2018-vol-30.pdf
20. Qiao S, Zhou G, Li X. Disclosure of same-sex behaviors to health-care providers and uptake of HIV
testing for men who have sex with men: A systematic review. Am j Mens Health. 2018;12(5):1197-
1214.
21. Petroll AE, Mosack KE. Physician awareness of sexual orientation and preventive health
recommendations to men who have sex with men. Sex Transm Dis. 2011;38(1):63.
22. U.S. Preventive Services Task Force. Screening for Illicit Drug Use. Accessed 20 August 2013,
http://www.uspreventiveservicestaskforce.org/uspstf08/druguse/drugrs.htm#summary
23. McDonell MG, Graves MC, West II, et al. Utility of point of care urine drug tests in the treatment of
primary care patients with drug use disorders. Journal Addict Med. 2016;10(3):196.
24. Chasnoff IJ, Landress HJ, Barrett ME. The prevalence of illicit-drug or alcohol use during pregnancy
and discrepancies in mandatory reporting in Pinellas County, Florida. N Engl J Med.
1990;322(17):1202-1206.
25. White D, Rosenberg ES, Cooper HL, et al. Racial differences in the validity of self-reported drug use
among men who have sex with men in Atlanta, GA. Drug Alcohol Depend. 2014;138:146-153.
26. Barrow RY, Ahmed F, Bolan GA, et al. Recommendations for providing quality sexually transmitted
diseases clinical services, 2020. MMWR Recomm Rep. Jan 3 2020;68(5):1-20.
doi:10.15585/mmwr.rr6805a1
27. Wimberly YH, Hogben M, Moore-Ruffin J, et al. Sexual history-taking among primary care
physicians. J Natl Med Assoc. Dec 2006;98(12):1924-1929.
28. Kurth AERNCNMP, Holmes KKMDP, Hawkins RBA, Golden MRMDMPH. A national survey of clinic
sexual histories for sexually transmitted infection and HIV screening. Sex Transm Dis
2005;32(6):370-376.

Preexposure Prophylaxis for the Prevention of HIV Infection in the United States – 2021 Update Clinical Practice Guideline
Page 97 of 108
29. Laws MB, Bradshaw YS, Safren SA, et al. Discussion of sexual risk behavior in HIV care is infrequent
and appears ineffectual: A mixed methods study. AIDS Behav. 2011;15(4):812-822.
doi:10.1007/s10461-010-9844-3
30. Metsch LR, Pereyra M, del Rio C, et al. Delivery of HIV prevention counseling by physicians at HIV
medical care settings in 4 US cities. Am J Public Health. 2004;94(7):1186-1192.
31. Duffus WA, Barragan M, Metsch L, et al. Effect of physician specialty on counseling practices and
medical referral patterns among physicians caring for disadvantaged human immunodeficiency
virus-infected populations. Clin Infect Dis. Jun 15 2003;36(12):1577-1584.
32. Deutsch MB, Glidden DV, Sevelius J, et al. HIV pre-exposure prophylaxis in transgender women: a
subgroup analysis of the iPrEx trial. Lancet HIV. Dec 2015;2(12):e512-9. doi:10.1016/S2352-
3018(15)00206-4
33. Eaton LA, Earnshaw VA, Maksut JL, et al. Experiences of stigma and health care engagement
among Black MSM newly diagnosed with HIV/STI. J Behavior Medicine. 2018;41(4):458-466.
34. Quinn K, Dickson-Gomez J, Zarwell M, et al. “A gay man and a doctor are Just like, a Recipe for
Destruction”: How Racism and Homonegativity in Healthcare Settings Influence PrEP uptake
among young Black MSM. AIDS Behav. 2019;23(7):1951-1963.
35. Biancarelli DL, Biello KB, Childs E, et al. Strategies used by people who inject drugs to avoid stigma
in healthcare settings. Drug Alcohol Depend. 2019;198:80-86.
36. Horner G, Daddona J, Burke DJ et al. “You’re kind of at war with yourself as a nurse”: Perspectives
of inpatient nurses on treating people who present with a comorbid opioid use disorder. PLoS
One. 2019;14(10)
37. DHHS Panel on Antiretroviral Guidelines for Adults and Adolescents. Guidelines for the Use of
AntiretroviralAgents in HIV-1-Infected Adults and Adolescents. 2019. Accessed 16 August 2019.
http://aidsinfo.nih.gov/contentfiles/AdultandAdolescentGL.pdf
38. Menza TW, Hughes JP, Celum CL et al. Prediction of HIV acquisition among men who have sex
with men. Sex Transm Dis. Sep 2009;36(9):547-555. doi:Doi 10.1097/Olq.0b013e3181a9cc41
39. Smith DK, Pals SL, Herbst JH, et al. Development of a clinical screening index predictive of incident
HIV infection among men who have sex with men in the United States. J Acquir Immune Defic
Syndr. 2012;60(4):421-7. doi:10.1097/QAI.0b013e318256b2f6
40. Chan AW, Pristach EA, Welte JW. Detection by the CAGE of alcoholism or heavy drinking in
primary care outpatients and the general population. J Subst Abuse. 1994;6(2):123-35.
41. Bastiaens L, Riccardi K, Sakhrani D. The RAFFT as a screening tool for adult substance use
disorders. The Am J Drug Alcohol Abuse. Nov 2002;28(4):681-91.
42. Knight JR, Sherritt L, Shrier LA, et al. Validity of the CRAFFT substance abuse screening test among
adolescent clinic patients. Arch Pediatr Adolesc Medicine. Jun 2002;156(6):607-14.
43. Halkitis PN, Pollock JA, Pappas MK, et al. Substance use in the MSM population of New York City
during the Era of HIV/AIDS. Subst UseMisuse. 2011/01/10 2011;46(2-3):264-273.
doi:10.3109/10826084.2011.523265
44. Weller S, Davis K. Condom effectiveness in reducing heterosexual HIV transmission. Cochrane
Database Syst Rev. 2002;(1):CD003255. doi:CD003255 [pii]10.1002/14651858.CD003255
45. Smith DK, Herbst JH, Zhang X, et al. Condom effectiveness for HIV prevention by consistency of
use among men who have sex with men in the United States. J Acquir Immune Defic Syndr. Mar 01
2015;68(3):337-44. doi:10.1097/QAI.0000000000000461
46. Pinkerton SD, Abramson PR. Effectiveness of condoms in preventing HIV transmission. Soc Sci
Medicine. May 1997;44(9):1303-12.
47. Ahmed S, Lutalo T, Wawer M, et al. HIV incidence and sexually transmitted disease prevalence
associated with condom use: a population study in Rakai, Uganda. AIDS. 2001;15(16):2171-9.

Preexposure Prophylaxis for the Prevention of HIV Infection in the United States – 2021 Update Clinical Practice Guideline
Page 98 of 108
48. Reece M, Herbenick D, Schick V, et al. Condom use rates in a national probability sample of males
and females ages 14 to 94 in the United States. JSex Med. 2010;7:266-276. doi:10.1111/j.1743-
6109.2010.02017.x
49. Koblin B, Chesney M, Coates T, et al. Effects of a behavioural intervention to reduce acquisition of
HIV infection among men who have sex with men: the EXPLORE randomised controlled study.
Lancet. 2004;364(9428):41-50. doi:10.1016/S0140-6736(04)16588-4
50. Peterman TA, Tian LH, Warner L, et al. Condom use in the year following a sexually transmitted
disease clinic visit. Int J STD AIDS. 2009;20(1):9-13. doi:10.1258/ijsa.2008.008177
51. Centers for Disease Control and Prevention. -HIV infection, risk, prevention, and testing behaviors
among persons who inject drugs — National HIV Behavioral Surveillance Injection Drug Use, 20
U.S. Cities, 2015. HIV Surveillance Special Report. 2018;18:1-38. Accessed 1 December 2019.
https://www.cdc.gov/hiv/pdf/library/reports/surveillance/cdc-hiv-hssr-nhbs-pwid-2015.pdf
52. Kral AH, Bluthenthal RN, Lorvick J, Gee L, et al. Sexual transmission of HIV-1 among injection drug
users in San Francisco, USA: risk-factor analysis. The Lancet. 2001;357(9266):1397-1401.
53. Strathdee SA, Stockman JK. Epidemiology of HIV among injecting and non-injecting drug users:
current trends and implications for interventions. Curr HIV/AIDS Rep. 2010;7(2):99-106.
54. Cardo DM, Culver DH, Ciesielski CA, et al. A case-control study of HIV seroconversion in health care
workers after percutaneous exposure. N Engl J Med. Nov 20 1997;337(21):1485-1490.
55. Benotsch EG, Zimmerman RS, Cathers L, et al. Non-medical use of prescription drugs and HIV risk
behaviour in transgender women in the Mid-Atlantic region of the United States. IntJournal STD
AIDS. 2016;27(9):776-782.
56. Wilson E, Rapues J, Jin H, et al. . The use and correlates of illicit silicone or “fillers” in a population‐
based sample of transwomen, San Francisco, 2013. Journal Sex Medicine. 2014;11(7):1717-1724.
57. Wilson EC, Jin H, Liu A, et al. . Knowledge, indications and willingness to take pre-exposure
prophylaxis among transwomen in San Francisco, 2013. PLoS One. 2015;10(6)
58. Smith DK, Pan Y, Rose CE, et al. A brief screening tool to assess the risk of contracting HIV infection
among active injection drug users. J Addict Med. 2015;9(3):226-32.
doi:10.1097/ADM.0000000000000123
59. Centers for Disease Control and Prevention. Integrated prevention services for HIV infection, viral
hepatitis, sexually transmitted diseases, and tuberculosis for persons who use drugs illicitly:
summary guidance from CDC and the U.S. Department of Health and Human Services. MMWR
Recomm Rep. Nov 9 2012;61(RR-5):1-40.
60. DiNenno EA. Recommendations for HIV screening of gay, bisexual, and other men who have sex
with men—United States, 2017. MMWR Morb Mortal Wkly Rep. 2017;66
61. US Preventive Services Task Force. Screening For HIV infection: Current recommendations, U.S.
Preventive Services Task Force. Updated 1 December 2019.
https://www.uspreventiveservicestaskforce.org/Page/Document/UpdateSummaryFinal/hum
an-immunodeficiency-virus-hiv-infection-screening1
62. Mimiaga MJ, Reisner SL, Bland S, et al. Health system and personal barriers resulting in decreased
utilization of HIV and STD testing services among at-risk black men who have sex with men in
Massachusetts. AIDS Patient Care STDs. 2009;23(10):825-35. doi:10.1089/apc.2009.0086
63. Wejnert C, Prejean J, Hoots B, et al. Prevalence of missed opportunities for HIV testing among
persons unaware of their infection. JAMA. 2018;319(24):2555-2557.
64. Patel D, Johnson CH, Krueger A, et al. Trends in HIV testing among US adults, aged 18–64 years,
2011–2017. AIDS Behav. 2019:1-8.
65. Stekler JD, Ure G, O'Neal JD, et al. Performance of Determine Combo and other point-of-care HIV
tests among Seattle MSM. J Clin Virol. Mar 2016;76:8-13. doi:10.1016/j.jcv.2015.12.011

Preexposure Prophylaxis for the Prevention of HIV Infection in the United States – 2021 Update Clinical Practice Guideline
Page 99 of 108
66. Centers for Disease Control and Prevention and Association of Public Health Laboratories.
Laboratory testing for the diagnosis of HIV infection : updated recommendations. 2014:1-66.
Accessed 10 December 2019. https://stacks.cdc.gov/view/cdc/23447
67. Powell VE, Gibas KM, DuBow J et al. . Update on HIV preexposure prophylaxis: effectiveness, drug
resistance, and risk compensation. Curr Infect Dis Rep. 2019;21(8):28.
68. Gibas KM, van den Berg P, Powell VE et al. Drug resistance during HIV pre-exposure prophylaxis.
Drugs. 2019;79(6):609-619.
69. McKellar MS, Cope AB, Gay CL, et al. Acute HIV-1 infection in the Southeastern United States: a
cohort study. AIDS Res Human Retroviruses. 2013;29(1):121-128.
70. Hoenigl M, Green N, Camacho M, et al. Signs or symptoms of acute HIV infection in a cohort
undergoing community-based screening. Emerg Infect Dis. 2016;22(3):532.
71. Daar ES, Pilcher CD, Hecht FM. Clinical presentation and diagnosis of primary HIV-1 infection. Curr
Opin HIV AIDS. Jan 2008;3(1):10-5. doi:10.1097/COH.0b013e3282f2e295
01222929-200801000-00004 [pii]
72. Cohen MS, Gay CL, Busch MP, et al. The detection of acute HIV infection. J Infect Dis.
2010;202(Supplement_2):S270-S277.
73. Hecht FM, Busch MP, Rawal B, et al. Use of laboratory tests and clinical symptoms for
identification of primary HIV infection. AIDS. May 24 2002;16(8):1119-1129.
74. Rich JD, Mylonakis E, Flanigan TP. Misdiagnosis of HIV infection - Response. Ann Intern Med. Oct 5
1999;131(7):547-548.
75. Wu H, Cohen SE, Westheimer E, et al. Diagnosing acute HIV infection: The performance of
quantitative HIV-1 RNA testing (viral load) in the 2014 laboratory testing algorithm. J Clin Virol.
2017;93:85-86.
76. Sivay MV, Li M, Piwowar-Manning E, et al. Characterization of HIV seroconverters in a TDF/FTC
PrEP study: HPTN 067/ADAPT. J Acquir Immune Defic Syndr. 2017;75(3):271.
77. Donnell D, Ramos E, Celum C, et al. The effect of oral preexposure prophylaxis on the progression
of HIV-1 seroconversion. AIDS. 2017;31(14):2007.
78. Marzinke MA, Grinsztejn B, Fogel JM, et al. Characterization of human immunodeficiency virus
(HIV) infection in cisgender men and transgender women who have sex with men receiving
injectable cabotegravir for HIV prevention: HPTN 083. Infect Ds. 2021;
79. Workowski iK. Sexually Transmitted Infections Treatment Guidelines, 2021. MMWR
Recommendations and Reports. 2021;70(4):1-187.
80. Centers for Disease Control and Prevention. 2016 Sexually Transmitted Disease Surveillance;
National Profile-Overview: Chlamydia. Accessed 1 December 2019,
https://www.cdc.gov/std/stats18/chlamydia.htm
81. Peterman TA, Newman DR, Maddox L et al. Risk for HIV following a diagnosis of syphilis,
gonorrhoea or chlamydia: 328,456 women in Florida, 2000–2011. International journal of STD &
AIDS. 2015;26(2):113-119.
82. Newman DR, Rahman MM, Brantley A et al. Rates of New Human Immunodeficiency Virus (HIV)
Diagnoses After Reported sexually transmitted infection in women in Louisiana, 2000–2015:
Implications for HIV prevention. Clin Infect Diss. 2020; 70(6), pp.1115-1120.
83. Workowski KA, Bolan GA, Centers for Disease C, Prevention. Sexually transmitted diseases
treatment guidelines, 2015. MMWR Recomm Rep. Jun 05 2015;64(RR-03):1-137.
84. Barbee LA, Tat S, Dhanireddy S et al. Implementation and operational research: effectiveness and
patient acceptability of a sexually transmitted infection self-testing program in an HIV care setting.
J Acquir Immune Defic Syndr. 2016;72(2):e26-e31.

Preexposure Prophylaxis for the Prevention of HIV Infection in the United States – 2021 Update Clinical Practice Guideline
Page 100 of 108
85. Freeman AH, Bernstein KT, Kohn RP et al. Evaluation of self-collected versus clinician-collected
swabs for the detection of Chlamydia trachomatis and Neisseria gonorrhoeae pharyngeal infection
among men who have sex with men. Sex Transm Dis. 2011;38(11):1036-1039.
86. Lunny C, Taylor D, Hoang L, et al. Self-collected versus clinician-collected sampling for Chlamydia
and Gonorrhea screening: a systemic review and meta-analysis. PLoS One. 2015;10(7):e0132776.
87. Harrington P, Onwubiko U, Qi M, et al. Predictive factors for HIV seroconversion among women
attending an urban health clinic in the South: A matched case–control study in Atlanta, GA. 2019:
34(3), pp.124-131
88. Elmes J, Silhol R, Hess KL, et al. Receptive anal sex contributes substantially to heterosexually‐
acquired HIV infections among at‐risk women in Twenty US Cities: results from a modelling
analysis. Am J Reprod Immunol. 2020:e13263. doi:10.1111/aji.13263 Accessed 1 June 2020.
89. Hunte T, Alcaide M, Castro J. Rectal infections with chlamydia and gonorrhoea in women
attending a multiethnic sexually transmitted diseases urban clinic. Int Jf STD AIDS.
2010;21(12):819-822.
90. Trebach JD, Chaulk CP, Page KR et al. Neisseria gonorrhoeae and Chlamydia trachomatis among
women reporting extragenital exposures. Sex Transm Ds. 2015;42(5):233.
91. Danby CS, Cosentino LA, Rabe LK, et al. Patterns of extragenital chlamydia and gonorrhea in
women and men who have sex with men reporting a history of receptive anal intercourse. Sex
Transm dDs 2016;43(2):105-109.
92. Oster AM, Wertheim JO, Hernandez AL et al.. Using molecular HIV surveillance data to understand
transmission between subpopulations in the United States. J Acquir Immune Defic Syndr. Dec 01
2015;70(4):444-51. doi:10.1097/QAI.0000000000000809
93. Hurt CB, Beagle S, Leone PA, et al. Investigating a sexual network of black men who have sex with
men: implications for transmission and prevention of HIV infection in the United States. J Acquir
Immune Defic Syndr. 2012;61(4):515.
94. Copen CE, Chandra A, Febo-Vazquez I. Sexual behavior, sexual attraction, and sexual orientation
among adults aged 18-44 in the United States: Data From the 2011-2013 National Survey of Family
Growth. Natl Health Stat Rep. 2016;(88):1-14.
95. Stannah J, Silhol R, Elmes J, et al. Increases in HIV incidence following receptive anal intercourse
among women: A Systematic review and meta-analysis. AIDS and Behavior. 2020;24(3):667-681.
96. Justman J, Befus M, Hughes J, et al. Sexual behaviors of US women at risk of HIV acquisition: a
longitudinal analysis of findings from HPTN 064. AIDS and behavior. 2015;19(7):1327-1337.
97. Dombrowski JC. Do women need screening for extragenital gonococcal and chlamydial infections?
Sexually Transmitted Diseases. 2015;42(5):240-241.
98. Tao G, Hoover KW, Nye MB et al. Infrequent testing of women for rectal chlamydia and gonorrhea
in the United States. Clin Infect Dis. 2017;
99. American College of Obstetrics and Gynecology. Committee Opinion: Expedited partner therapy in
the management of gonorrhea and chlamydial infection. 12 October 2017,
https://www.acog.org/Resources-And-Publications/Committee-Opinions/Committee-on-
Gynecologic-Practice/Expedited-Partner-Therapy-in-the-Management-of-Gonorrhea-and-
Chlamydial-Infection
100. Centers for Disease Control and Prevention. Guidance on the use of expedited partner therapy in
the treatment of gonorrhea. Accessed 12 October 2017, https://www.cdc.gov/std/ept/gc-
guidance.htm
101. Centers for Disease Control and Prevention. Expedited partner therapy in the management of
sexually transmitted diseases. Accessed 12 October 2017,
https://www.cdc.gov/std/treatment/eptfinalreport2006.pdf

Preexposure Prophylaxis for the Prevention of HIV Infection in the United States – 2021 Update Clinical Practice Guideline
Page 101 of 108
102. Centers for Disease Control and Prevention. Recommendations for partner services programs for
HIV infection, syphilis, gonorrhea, and chlamydial infection. Morbidity and Mortality Reports and
Recommendations. 2008;57(RR09):1-63.
103. Ferreira A, Young T, Mathews C et al. Strategies for partner notification for sexually transmitted
infections, including HIV. Cochrane Database of Syst Rev. 2013;(10)
104. Martin M, Vanichseni S, Suntharasamai P, et al. Renal function of participants in the Bangkok
tenofovir study—Thailand, 2005–2012. Clin infect Dis. 2014;59(5):716-724.
105. Mugwanya KK, Wyatt C, Celum C, et al. Changes i glomerular kidney function among hiv-1–
uninfected men and women receiving emtricitabine–tenofovir disoproxil fumarate preexposure
prophylaxis: A randomized clinical trial. JAMA Intern Med. 2015;175(2):246-254.
106. Marcus JL, Hurley LB, Hare CB, et al. Preexposure prophylaxis for HIV prevention in a large
integrated health care system: Adherence, renal safety, and discontinuation. J Acquir Immune
Defic Syndr. Dec 15 2016;73(5):540-546. doi:10.1097/QAI.0000000000001129
107. Gandhi M, Glidden DV, Mayer K, et al. Association of age, baseline kidney function, and
medication exposure with declines in creatinine clearance on pre-exposure prophylaxis: an
observational cohort study. The lancet HIV. 2016;3(11):e521-e528.
108. Ogbuagu O, Podzamczer D, Salazar LC, et al. Longer-term safety of F/TAF AND F/TDF for HIV PrEP:
DISCOVER Trial Week 96 Results Conference on Retroviruses and Opportunistic Infections (CROI).
Accessed 24 March 2020,
http://www.croiwebcasts.org/console/player/44704?mediaType=audio&&crd_fl=0&ssmsrq
=1585070251708&ctms=5000&csmsrq=5049
109. Cockcroft DW, Gault MH. Prediction of creatinine clearance from serum creatinine. Nephron.
1976;16(1):31-41.
110. Kamis KF, Marx GE, Scott KA, et al. Same-day HIV pre-exposure prophylaxis (PrEP) initiation during
drop-in sexually transmitted diseases clinic appointments is a highly acceptable, feasible, and safe
model that engages individuals at risk for HIV into PrEP care. 2019. Open Forum Infect Dis;6( 7):,
:ofz310.
111. Havens JP, Scarsi KK, Sayles H et al. Acceptability and feasibility of a pharmacist-led HIV pre-
exposure prophylaxis (PrEP) program in the Midwestern United States. 2019. Open Forum Infec
Dis
112. Tung EL, Thomas A, Eichner A et al. Implementation of a community pharmacy-based pre-
exposure prophylaxis service: a novel model for pre-exposure prophylaxis care. Sex Health.
2018;15(6):556-561.
113. Centers for Disease Control and Prevention. Updated guidelines for antiretroviral postexposure
prophylaxis after Ssexual, injection drug use, or other nonoccupational exposure to HIV—United
States, 2016. 2016. Accessed 1 December 2019.
https://www.cdc.gov/hiv/pdf/programresources/cdc-hiv-npep-guidelines.pdf
114. Thomas R, Galanakis C, Vézina S, et al. Adherence to post-exposure prophylaxis (PEP) and
incidence of HIV seroconversion in a major North American cohort. PLoS One. 2015;10(11):
e0142534.
115. Whitlock G, McCormack C, Fearnley J et al. High HIV incidence in men who have sex with men
attending for postexposure prophylaxis: a service evaluation. Sex Transm Infect. 2017;93(3):214-
216.
116. Pilkington V, Hill A, Hughes S et al. How safe is TDF/FTC as PrEP? A systematic review and meta-
analysis of the risk of adverse events in 13 randomised trials of PrEP. J Virus Erad. 2018;4(4):215.
117. Wassner C, Bradley N, Lee Y. A review and clinical understanding of tenofovir: Tenofovir disoproxil
fumarate versus tenofovir alafenamide. J Int Assoc Provid AIDS Care).
2020;19:2325958220919231.

Preexposure Prophylaxis for the Prevention of HIV Infection in the United States – 2021 Update Clinical Practice Guideline
Page 102 of 108
118. US Food and Drug Administration. Truvada Prescribing Information. 2018.
https://www.accessdata.fda.gov/drugsatfda_docs/label/2018/021752s055lbl.pdf
119. Food and Drug Administration. Descovy Prescribing Information. 2019. Accessed 1 December
2019. https://www.accessdata.fda.gov/drugsatfda_docs/label/2019/208215s012lbl.pdf
120. Primary Care Collaborative. Quick COVID-19 primary care survey (Series 15 fielded June 26-29,
2020). 2020. Accessed 8 July 2020.
https://www.pcpcc.org/sites/default/files/news_files/C19%20Series%2015%20National%2
0Executive%20Summary_0.pdf
121. Centers for Disease Control and Prevention. Dear Colleague Letter: PrEP during COVID-19. 2020.
Accessed 8 July 2020. https://www.cdc.gov/nchhstp/dear_colleague/2020/dcl-051520-PrEP-
during-COVID-19.html
122. Abbas UL, Glaubius R, Mubayi A et al. Antiretroviral therapy and pre-exposure prophylaxis:
Combined impact on HIV transmission and drug resistance in South Africa. Journal of Infectious
Diseases. July 15, 2013 2013;208(2):224-234. doi:10.1093/infdis/jit150
123. Celum C, Hallett TB, Baeten JM. HIV-1 prevention with ART and PrEP: Mathematical modeling
insights into resistance, effectiveness, and public health impact. J Infect Dis. 2013;208(2):189-191.
doi:10.1093/infdis/jit154
124. Anderson PL, Glidden DV, Liu A, et al. Emtricitabine-tenofovir concentrations and pre-exposure
prophylaxis efficacy in men who have sex with men. Sci Transl Med. Sep 12 2012;4(151):15-25.
doi:10.1126/scitranslmed.3004006
125. Grant RM, Anderson PL, McMahan V, et al. Uptake of pre-exposure prophylaxis, sexual practices,
and HIV incidence in men and transgender women who have sex with men: a cohort study. Lancet
Infect Dis. Sep 2014;14(9):820-9. doi:10.1016/S1473-3099(14)70847-3
126. Castillo-Mancilla JR, Zheng J-H, Rower JE, et al. Tenofovir, emtricitabine, and tenofovir
diphosphate in dried blood spots for determining recent and cumulative drug exposure. AIDS
research and human retroviruses. 2013;29(2):384-390.
127. Cottrell ML, Yang KH, Prince HMA, et al. A translational pharmacology approach to predicting
outcomes of preexposure prophylaxis against HIV in men and women using yenofovir disoproxil
fumarate with or without emtricitabine. J Infect Dis. 2016;214(1):55-64. doi:10.1093/infdis/jiw077
128. Knobel H, Alonso J, Casado JL, et al. Validation of a simplified medication adherence questionnaire
in a large cohort of HIV-infected patients: the GEEMA Study. AIDS. 2002;16(4):605-613.
129. Golub SA, Operario D, Gorbach PM. Pre-exposure prophylaxis state of the science: empirical
analogies for research and implementation. Curr HIV/AIDS Rep. 2010;7(4):201-9.
doi:10.1007/s11904-010-0057-1
130. Fiscella K, Epstein RM. So Much to Do, So little time: Care for the socially Ddsadvantaged and the
15-minute visit. Arch Intern Med. 2008;168(17):1843-1852. doi:10.1001/archinte.168.17.1843
131. Yarnall KSH, Pollak KI, Ostbye Tet al. Primary care: Is there enough time for prevention? Am J
Public Health. 2003;93(4):635-641. doi:10.2105/ajph.93.4.635
132. Patterson KB, Prince HA, Kraft E, et al. Penetration of tenofovir and emtricitabine in mucosal
tissues: Implications for prevention of HIV-1 transmission. Sci Transl Med. 2011;3(112):112re4.
doi:10.1126/scitranslmed.3003174
133. Anderson P LJ, Buchbinder S, Guanira J et al. and the iPrEx study team. Interpreting detection rates
of intracellular FTC-TP and TFV-DP: The iPrEx trial. presented at: 18th Conference on Retroviruses
and Opportunistic Infections; 2011; Boston, Massachusetts. Accessed 30 May 2011.
http://www.retroconference.org/2011/Abstracts/42612.htm
134. Gandhi M, Bacchetti P, Spinelli MA, et al. Brief Report: Validation of a urine tenofovir
immunoassay for adherence monitoring to PrEP and ART and establishing the cutoff for a point-of-
care test. J Acquir Immune Defic Syndr. 2019;81(1):72-77.

Preexposure Prophylaxis for the Prevention of HIV Infection in the United States – 2021 Update Clinical Practice Guideline
Page 103 of 108
135. Koenig HC, Mounzer K, Daughtridge GW, et al. Urine assay for tenofovir to monitor adherence in
real time to tenofovir disoproxil fumarate/emtricitabine as pre‐exposure prophylaxis. HIV Med.
2017;18(6):412-418.
136. Anderson PL, Liu AY, Castillo-Mancilla JR, et al. Intracellular tenofovir-diphosphate and
emtricitabine-triphosphate in dried blood spots following directly observed therapy.
AntimicrobAgents Chemother. 2018;62(1):e01710-17.
137. Koss CA, Liu AY, Castillo-Mancilla J, et al. Similar tenofovir hair concentrations in men and women
after directly-observed: dosing of TDF/FTC: implications for PrEP adherence monitoring. AIDS.
2018;
138. Seifert SM, Glidden DV, Meditz AL, et al. Dose response for starting and stopping HIV preexposure
prophylaxis for men who have sex with men. Clin Infect Dis. Mar 01 2015;60(5):804-10.
doi:10.1093/cid/ciu916
139. Seifert SM, Chen X, Meditz AL, et al. Intracellular tenofovir and emtricitabine anabolites in genital,
rectal, and blood compartments from first dose to steady state. AIDS Res Hum Retroviruses.
2016;32(10-11):981-991.
140. Marcus JL, Hurley LB, Nguyen DP, Silverberg MJ, Volk JE. Redefining HIV preexposure prophylaxis
failures. Clin Infect Dis. 2017:cix593.
141. Hojilla JC HL, Marcus JL, Silverberg MJ et al. Characterization of HIV preexposure prophylaxis use
behaviors and HIV incidence among U.S. adults in an integrated healthcare system. JAMA Netw
Open, 2021; 4(8):.e2122692-e2122692.
142. Ford SL, Lou Y, Lewis N, et al. Effect of rifabutin on the pharmacokinetics of oral cabotegravir in
healthy subjects. Antivir Ther. 2019;24(4):301-308. doi:10.3851/IMP3306
143. Ford SL, Sutton K, Lou Y, et al. Effect of Rifampin on the single-dose pharmacokinetics of oral
cabotegravir in healthy subjects. Antimicrob Agents Chemother.
2017;61(10)doi:10.1128/AAC.00487-17
144. Ford SL, Lou Y, Lewis N, et al. Effect of rifabutin on the pharmacokinetics of oral cabotegravir in
healthy subjects. Antivir Ther. 2019;24(4):301-308.
145. Trezza C, Ford SL, Gould E, et al. Lack of effect of oral cabotegravir on the pharmacokinetics of a
levonorgestrel/ethinyl oestradiol-containing oral contraceptive in healthy adult women. Br J Clin
Pharmacol. 2017;83(7):1499-1505. doi:10.1111/bcp.13236
146. Yager JL, Anderson PL. Pharmacology and drug interactions with HIV PrEP in transgender persons
receiving gender affirming hormone therapy. Expert Opin on Drug Metab Toxicol. 2020;16(6):463-
474.
147. Landovitz RJ, Donnell D, Clement ME, et al. Cabotegravir for HIV prevention in cisgender men and
transgender women. N Engl J Med. 2021;;385(7):595-608
148. Tolley EE, Zangeneh SZ, Chau G, et al. Acceptability of Long-Acting Injectable Cabotegravir (CAB
LA) in HIV-Uninfected Individuals: HPTN 077. AIDS Behav 2020:1-12.
149. Landovitz RJ, Li S, Eron Jr JJ, et al. Tail-phase safety, tolerability, and pharmacokinetics of long-
acting injectable cabotegravir in HIV-uninfected adults: a secondary analysis of the HPTN 077 trial.
The Lancet HIV. 2020;
150. Radzio-Basu J, Council O, Cong M-e, et al. Drug resistance emergence in macaques administered
cabotegravir long-acting for pre-exposure prophylaxis during acute SHIV infection. Nat Commun.
2019;10(1):1-8.
151. Oliveira M, Ibanescu R-I, Anstett K, et al. Selective resistance profiles emerging in patient-derived
clinical isolates with cabotegravir, bictegravir, dolutegravir, and elvitegravir. Retrovirology.
2018;15(1):56.

Preexposure Prophylaxis for the Prevention of HIV Infection in the United States – 2021 Update Clinical Practice Guideline
Page 104 of 108
152. Harris NS, Johnson AS, Huang Y-LA, et al. Vital signs: status of human immunodeficiency virus
testing, viral suppression, and HIV preexposure prophylaxis—United States, 2013–2018. MMWR
Morb Mortal Wkly Rep. 2019;68(48):1117.
153. Smith DK, Switzer WM, Peters P, et al. A strategy for PrEP clinicians to manage ambiguous HIV test
results during follow-up visits. Open Forum Infect Dis. 2018;, 5(8): ofy180..
154. Stekler JD, Violette LR, Niemann L, et al. Repeated false-positive HIV test results in a patient taking
HIV pre-exposure prophylaxis. In Open forum infectious diseases, 2018;:5(9):ofy197
155. Molina JM, Capitant C, Spire B, et al. On-demand preexposure prophylaxis in men at high risk for
HIV-1 infection. N Engl J Med. 2015;373:2237-46
156. Molina JM, Charreau I, Spire B, et al. Efficacy, safety, and effect on sexual behaviour of on-demand
pre-exposure prophylaxis for HIV in men who have sex with men: an observational cohort study.
Lancet HIV. 2017;4(9):e402-e410. doi:10.1016/S2352-3018(17)30089-9
157. Antoni G, Tremblay C, Delaugerre C, et al. On-demand pre-exposure prophylaxis with tenofovir
disoproxil fumarate plus emtricitabine among men who have sex with men with less frequent
sexual intercourse: a post-hoc analysis of the ANRS IPERGAY trial. The Lancet HIV. 2020;7(2):e113-
20.
158. Dimitrov D, Moore JR, Wood D, et al. Predicted effectiveness of daily and non-daily PrEP for MSM
based on sex and pill-taking patterns from HPTN 067/ADAPT. Clin Infect Dis. 2019;71( 2):249–255,
159. Saag MS, Benson CA, Gandhi RT, et al. Antiretroviral drugs for treatment and prevention of HIV
infection in adults: 2018 recommendations of the International Antiviral Society–USA Panel.
JAMA. 2018;320(4):379-396.
160. Cottrell ML, Prince HM, Schauer AP, et al. Decreased tenofovir diphosphate concentrations in a
transgender female cohort: Implications for human immunodeficiency virus preexposure
prophylaxis. Clin Infect Dis. 2019;69(12):2201-2204.
161. Shieh E, Marzinke MA, Fuchs EJ, et al. Transgender women on oral HIV pre‐exposure prophylaxis
have significantly lower tenofovir and emtricitabine concentrations when also taking oestrogen
when compared to cisgender men. J Int AIDS Society. 2019;22(11)
162. Grant RM, Pellegrini M, Defechereux PA, et al. Sex hormone therapy and tenofovir diphosphate
concentration in dried blood spots: Primary results of the iBrEATHe Study. Clin Infect Dis.
2020;73(7), e2117-e2123.
163. Sevelius JM, Gutierrez-Mock L, Zamudio-Haas S, et al. Research with marginalized communities:
Challenges to continuity during the COVID-19 Pandemic. AIDS Behav. 2020/07/01
2020;24(7):2009-2012. doi:10.1007/s10461-020-02920-3
164. Wilson EC, Turner CM, Arayasirikul S, et al. Disparities in the PrEP continuum for trans women
compared to MSM in San Francisco, California: results from population‐based cross‐sectional
behavioural surveillance studies. J Int AIDS Society. 2020;23:e25539.
165. Becasen JS, Denard CL, Mullins MM, Higa DH, Sipe TA. Estimating the prevalence of HIV and sexual
behaviors among the US transgender population: a systematic review and meta-analysis, 2006–
2017. Am J Public Health. 2019;109(1):e1-e8.
166. Attia S, Egger M, Muller M et al. Sexual transmission of HIV according to viral load and
antiretroviral therapy: systematic review and meta-analysis. AIDS. Jul 17 2009;23(11):1397-404.
doi:10.1097/QAD.0b013e32832b7dca
167. Centers for Disease Control and Prevention. Evidence of HIV treatment and viral suppression in
preventing the sexual transmission of HIV: Technical fact sheet. 2018. Accessed 1 December 2019.
https://www.cdc.gov/hiv/pdf/risk/art/cdc-hiv-art-viral-suppression.pdf
168. Conroy AA, Gamarel KE, Neilands TB et al. Relationship Dynamics and Partner Beliefs About Viral
Suppression: A Longitudinal Study of Male Couples Living with HIV/AIDS (The Duo Project). AIDS
Behav. 2016/07/01 2016;20(7):1572-1583. doi:10.1007/s10461-016-1423-9

Preexposure Prophylaxis for the Prevention of HIV Infection in the United States – 2021 Update Clinical Practice Guideline
Page 105 of 108
169. Stephenson R, Bratcher A, Mimiaga MJ, et al. Brief Report: Accuracy in self-report of viral
suppression among HIV-positive men with HIV-negative male partners. J Acquir Immune Defic
Syndr. 2020;83(3):210-214.
170. Bavinton BR, Pinto AN, Phanuphak N, et al. Viral suppression and HIV transmission in
serodiscordant male couples: an international, prospective, observational, cohort study. Lancet
HIV. 2018;5(8):e438-e447. doi:10.1016/S2352-3018(18)30132-2
171. Rodger AJ, Cambiano V, Bruun T, et al. Risk of HIV transmission through condomless sex in
serodifferent gay couples with the HIV-positive partner taking suppressive antiretroviral therapy
(PARTNER): final results of a multicentre, prospective, observational study. Lancet.
2019;393(10189):2428-2438. doi:10.1016/S0140-6736(19)30418-0
172. Cohen MS, Chen YQ, McCauley M, et al. Antiretroviral therapy for the prevention of HIV-1
transmission. N Engl J Med. 2016;375(9):830-9. doi:10.1056/NEJMoa1600693
173. Cohen MS, McCauley M, Gamble TR. HIV treatment as prevention and HPTN 052. Research
Support, N.I.H., Extramural Review. Curr Opin HIV AIDS. 2012;7(2):99-105.
doi:10.1097/COH.0b013e32834f5cf2
174. Mugo NR, Heffron R, Donnell D, et al. Increased risk of HIV-1 transmission in pregnancy: a
prospective study among African HIV-1-serodiscordant couples. AIDS. 2011;25(15):1887-95.
doi:10.1097/QAD.0b013e32834a9338
175. Thomson KA, Hughes J, Baeten JM, et al. Increased risk of female HIV-1 acquisition throughout
pregnancy and postpartum: a prospective per-coital act analysis among women with HIV-1
infected partners. J Infect Dis. 2018;218(1):16–25.
176. Hoffman RM, Jaycocks A, Vardavas R, et al. Benefits of PrEP as an adjunctive method of HIV
prevention during attempted conception between HIV-uninfected women and HIV-infected male
partners. J Infect Dis. 2015;212(10):1534-1543.
177. Attia S, Egger M, Müller M et al. Sexual transmission of HIV according to viral load and
antiretroviral therapy: systematic review and meta-analysis. AIDS. 2009;23(11):1397-1404.
doi:10.1097/QAD.0b013e32832b7dca
178. Panel on treatment of HIV-infected pregnant women and prevention of perinatal transmission.
Recommendations for Use of Antiretroviral Drugs in Pregnant Women with HIV Infection o and
Interventions to Reduce Perinatal HIV Transmission in the United States. 2020. Accessed 10
January 2021.
https://clinicalinfo.hiv.gov/sites/default/files/guidelines/documents/Perinatal_GL_2020.pdf
179. Mofenson LM, Baggaley RC, Mameletzis I. Tenofovir disoproxil fumarate safety for women and
their infants during pregnancy and breastfeeding. AIDS. 2017;31(2):213-232.
180. Dettinger JC, Kinuthia J, Pintye J, et al. Perinatal outcomes following maternal pre-exposure
prophylaxis (PrEP) use during pregnancy: results from a large PrEP implementation program in
Kenya. Journal of the International AIDS Society. 2019;22(9):e25378. doi:10.1002/jia2.25378
181. Kinuthia J, Pintye J, Abuna F, et al. Pre-exposure prophylaxis uptake and early continuation among
pregnant and post-partum women within maternal and child health clinics in Kenya: results from
an implementation programme. The Lancet HIV. 2020/01/01/ 2020;7(1):e38-e48.
doi:https://doi.org/10.1016/S2352-3018(19)30335-2
182. Siberry GK, Williams PL, Mendez H, et al. Safety of tenofovir use during pregnancy: early growth
outcomes in HIV-exposed uninfected infants. AIDS. 06/ 2012;26(9):1151-1159.
183. Gibb DM, Kizito H, Russell EC, et al. Pregnancy and infant outcomes among HIV-infected women
taking long-term ART with and without tenofovir in the DART Trial. PLoS Med.
2012;9(5):e1001217. doi:10.1371/journal.pmed.1001217
184. Mirochnick M, Best BM, Clarke DF. Antiretroviral pharmacology: special issues regarding pregnant
women and neonates. Clin Perinatol. 2010;37(4):907-27. doi:10.1016/j.clp.2010.08.006

Preexposure Prophylaxis for the Prevention of HIV Infection in the United States – 2021 Update Clinical Practice Guideline
Page 106 of 108
185. The Antiretroviral Pregnancy Registry. Interim Report: 1 January 1989 through 31 January 2019.
Accessed 10 December 2019, http://apregistry.com/forms/exec-summary.pdf
186. Lampe MA, Smith DK, Anderson GJE et al. Achieving safe conception in HIV-discordant couples:
the potential role of oral preexposure prophylaxis (PrEP) in the United States. American Journal of
Obstet Gynecol. 2011;204(6)doi:10.1016/j.ajog.2011.02.026
187. Mugwanya KK, John-Stewart G, Baeten J. Safety of oral tenofovir disoproxil fumarate-based HIV
pre-exposure prophylaxis use in lactating HIV-uninfected women. Exp Opin Drug Safety.
2017;16(7):867-871.
188. Benaboud S, Pruvost A, Coffie PA, et al. Concentrations of tenofovir and emtricitabine in breast
milk of HIV-1-infected women in Abidjan, Cote d'Ivoire, in the ANRS 12109 TEmAA Study, Step 2.
Antimicrob Agents Chemother. 2011;55(3):1315-7. doi:10.1128/AAC.00514-10
189. Waitt C, Olagunju A, Nakalema S, et al. Plasma and breast milk pharmacokinetics of emtricitabine,
tenofovir and lamivudine using dried blood and breast milk spots in nursing African mother–infant
pairs. J Antimicrob Chemother. 2018;73(4):1013-1019.
190. World Health Organization. Programmatic update: Use of antiretroviral drugs for treating
pregnant women and preventing HIV infection in infants. 2012. Accessed 16 August 2013.
http://aidsdatahub.org/dmdocuments/Use_of_Antiretroviral_Drugs__for_Treating_Pregnan
t_Women.pdf
191. Tanner MR, Miele P, Carter W, et al. Preexposure prophylaxis for prevention of HIV acquisition
among adolescents: Clinical considerations, 2020. MMWR Recomm Rep. Apr 24 2020;69(3):1-12.
doi:10.15585/mmwr.rr6903a1
192. Culp L, Caucci L. State adolescent consent laws and implications for HIV pre-exposure prophylaxis.
Am J Prev Med. 2013;44(1 Suppl 2):S119-24. doi:10.1016/j.amepre.2012.09.044
193. Myers JJ, Dufour M-SK, Koester KA, et al. Adherence to PrEP among young men who have sex with
men participating in a sexual health services demonstration project in Alameda County, California.
J Acquir Immune Defic Syndr. 2019;81(4):406-413.
194. Gray WN, Netz M, McConville A et al. Medication adherence in pediatric asthma: A systematic
review of the literature. Pediatr Pulmonol. 2018;53(5):668-684.
195. Venditti EM, Tan K, Chang N, et al. Barriers and strategies for oral medication adherence among
children and adolescents with Type 2 diabetes. Diabetes Res Clin Pract. 2018;139:24-31.
196. Havens PL, Perumean-Chaney SE, Patki A, et al. Changes in bone mass after discontinuation of
preexposure prophylaxis with tenofovir disoproxil fumarate/emtricitabine in young men who have
sex with men: extension phase results of Adolescent Trials Network protocols 110 and 113. Clin
Infect Dis. 2020;70(4):687-91. 197. Havens PL, Tamhane A, Stephensen CB, et al.
Association of vitamin D insufficiency and protective tenofovir diphosphate concentrations with
bone toxicity in adolescent boys and young men using tenofovir disoproxil fumarate/emtricitabine
for HIV pre-exposure prophylaxis. AIDS Res Human Retroviruses. 2019;35(2):123-128.
198. Perkins RB, Guido RS, Castle PE, et al. 2019 ASCCP risk-based management consensus guidelines
for abnormal cervical cancer screening tests and cancer precursors. J Low Genit Tract Dis.
2020;24(2):102-131. doi:10.1097/LGT.0000000000000525
199. Services DoHaH. FAQS About Affordable Care Act Implementation Part 47. 2021. Accessed 13
August 2021. https://www.dol.gov/sites/dolgov/files/EBSA/about-ebsa/our-
activities/resource-center/faqs/aca-part-47.pdf
200. Centers for Disease Control and Prevention, Branson BM, Handsfield HH, et al. Revised
Recommendations for HIV testing of adults, adolescents, and pregnant women in health-care
settings. Morbidity and Mortality Reports and Recommendations. 2006;September 22, 2006 /
55(RR14);1-17

Preexposure Prophylaxis for the Prevention of HIV Infection in the United States – 2021 Update Clinical Practice Guideline
Page 107 of 108
201. Department of Health and Human Services, Panel on Antiretroviral Guidelines for Adults and
Adolescents. Guidelines for the Use of Antiretroviral Agents in Adults and Adolescents with HIV.
2019. Accessed 22 February 2020. https://aidsinfo.nih.gov/guidelines/html/1/adult-and-
adolescent-arv/37/whats-new-in-the-guidelines-
202. Smith DK GL, Black RJ, Auerbach JD et al. Antiretroviral postexposure prophylaxis after sexual,
injection-drug use, or other nonoccupational exposure to HIV in the United States. MMWR
Recomm Rep. 2005;54(RR-2):1-19.
203. Force UPST. Behavioral counseling interventions to prevent sexually transmitted infections: US
Preventive Services Task Force Recommendation Statement. JAMA. 2020;324(7):674-681.
doi:10.1001/jama.2020.13095
204. Schillie S, Wester C, Osborne M, Wesolowski L, Ryerson AB. CDC recommendations for hepatitis C
screening among adults — United States, 2020. MMWR Recomm Rep 2020;69. 2020;69(RR-2):1-
17. Accessed 12 April 2020. http://dx.doi.org/10.15585/mmwr.rr6902a1
205. Chung RT, Davis GL, Jensen DM, et al. Hepatitis C guidance: AASLD-IDSA recommendations for
testing, managing, and treating adults infected with hepatitis C virus. Hepatology. 2015;62(3):932-
954.
206. Guyatt G, Oxman AD, Akl EA, et al. GRADE guidelines: 1. Introduction--GRADE evidence profiles
and summary of findings tables. J Clin Epidemiol. 2011;64(4):383-394.
doi:10.1016/j.jclinepi.2010.04.026
207. Deutsch MB, Glidden DV, Sevelius J, et al. HIV pre-exposure prophylaxis in transgender women: a
subgroup analysis of the iPrEx trial. The lancet HIV. 2015;2(12):e512-e519.
208. Hosek S, Siberry G, Bell M, et al. The acceptability and feasibility of an HIV pre-exposure
prophylaxis (PrEP) trial with young men who have sex with men (YMSM). J Acquir Immune Defic
Syndr. 2012;62(4):447-456. doi:10.1097/QAI.0b013e3182801081
209. McCormack S, Dunn DT, Desai M, et al. Pre-exposure prophylaxis to prevent the acquisition of HIV-
1 infection (PROUD): effectiveness results from the pilot phase of a pragmatic open-label
randomised trial. Lancet. 2016;387(10013):53-60. doi:10.1016/S0140-6736(15)00056-2
210. Volk JE, Marcus JL, Phengrasamy T, et al. No new HIV infections with increasing use of HIV
preexposure prophylaxis in a Ccinical practice setting. Clin Infect Dis. 2015;61(10):1601-3.
doi:10.1093/cid/civ778
211. Liu AY, Cohen SE, Vittinghoff E, et al. Preexposure prophylaxis for HIV infection integrated with
municipal- and community-based sexual health services. JAMA Intern Med. 2016;176(1):75-84.
doi:10.1001/jamainternmed.2015.4683
212. Molina JM, Ghosn J, Algarte-Genin M, et al. Incidence of HIV-infection with daily or on-demand
PrEP with TDF/FTC in Paris area. Update from the ANRS Prevenir Study. 2019. Accessed 24 March
2020.
http://programme.ias2019.org/PAGMaterial/PPT/402_4152/Prevenir%20%20Mexico%202
019%20v10.ppt
213. Cressey TR, Siriprakaisil O, Klinbuayaem V, et al. A randomized clinical pharmacokinetic trial of
Tenofovir in blood, plasma and urine in adults with perfect, moderate and low PrEP adherence:
the TARGET study. BMC Infect Dis. 2017;17(1):496.
214. Van Damme L, Corneli A, Ahmed K, et al. Preexposure prophylaxis for HIV infection among African
women. N Engl J Med. 2012;367(5):411-422.
215. Peterson L, Taylor D, Roddy R, et al. Tenofovir disoproxil fumarate for prevention of HIV infection
in women: A phase 2, double-blind, randomized, placebo-controlled trial. PLoS Clin Trial.
2007;2(5):e27.
216. Marrazzo JM, Ramjee G, Richardson BA, et al. Tenofovir-based preexposure prophylaxis for HIV
infection among African women. N Engl J Med. 2015;372(6):509-18. doi:10.1056/NEJMoa1402269

Preexposure Prophylaxis for the Prevention of HIV Infection in the United States – 2021 Update Clinical Practice Guideline
Page 108 of 108
217. Baeten J. What can the twisted tale of PrEP results teach us? Accessed 21 April 2012,
http://www.retroconference.org/2012b/Abstracts/45269.htm
218. Martin M, Vanichseni S, Suntharasamai P, et al. Factors associated with the uptake of and
adherence to HIV pre-exposure prophylaxis in people who have injected drugs: an observational,
open-label extension of the Bangkok Tenofovir Study. Lancet HIV. 2017;4(2):e59-e66.
doi:10.1016/S2352-3018(16)30207-7
219. Landovitz RJ, Li S, Grinsztejn B, et al. Safety, tolerability, and pharmacokinetics of long-acting
injectable cabotegravir in low-risk HIV-uninfected individuals: HPTN 077, a phase 2a randomized
controlled trial. PLoS Med. 2018;15(11):e1002690.
220. Markowitz M, Frank I, Grant RM, et al. Safety and tolerability of long-acting cabotegravir injections
in HIV-uninfected men (ECLAIR): a multicentre, double-blind, randomised, placebo-controlled,
phase 2a trial. The Lancet HIV. 2017;4(8):e331-e340.
221. Blair CS, Li S, Chau G, et al. Brief Report: Hormonal contraception use and cabotegravir
pharmacokinetics in HIV-uninfected women enrolled in HPTN 077. J Acquir Immune Defic Syndr.
2020;85(1):93-97.
222. Landovitz RJ, Zangeneh SZ, Chau G, et al. Cabotegravir is not associated with weight gain in human
immunodeficiency virus–uninfected individuals in HPTN 077. Clin Infect Diss. 2020;70(2):319-322.
